Abstract
This study aimed to evaluate the association between substituting 10, 30, and 60 min/day of physical activity and sitting time with obesity indicators among workers. It is a cross-sectional study involving 394 adults (76.6% women) from São Paulo, Brazil. Physical activity and sitting time (min/day) were measured using the short version of the International Physical Activity Questionnaire (IPAQ) to determine physical activity levels. Obesity indicators included body mass index (BMI; kg/m²), waist circumference (cm), and body fat (kg). Isotemporal substitution models were analyzed using multivariate linear regression, adjusted for sociodemographic variables. Participants reported median values of 150.0 min/day (IQR: 60.0–360.0) for walking and 445.7 min/day (IQR: 317.1–565.7) for sitting time. The median values for BMI, waist circumference, and body fat were 27.1 kg/m², 91.0 cm, and 23.5 kg, respectively. Substituting 10 min/day of sitting time for 10 min/day of walking was associated with waist circumference (β: -0.216: 95% CI: -0.041; -0.007). In addition, substituting 60 min/day of sitting time for moderate physical activity (β -0.206; 95% CI: -0.123; -0.008) was negatively associated with body fat. The equivalent substitution of different periods of sitting time for more active behaviors was favorably associated with obesity indicators. These findings suggest that lifestyle interventions based on replacing sitting time with physical activity can reduce the obesity epidemic in adults.
Similar content being viewed by others
Introduction
The prevalence of obesity among adults is rising globally1,2. By 2030, it is projected that 3 out of every 10 Brazilian adults will be affected by obesity1. If this trend continues, it could lead to approximately 808,600 deaths from chronic non-communicable diseases associated with excess weight3. Additionally, São Paulo, one of the largest cities in Latin America, has seen a concerning rise in obesity prevalence in recent years4,5,6,7. The prevalence of obesity (defined as a body mass index [BMI] of ≥ 30 kg/m2) increased from 11.1% in 2006 to 19.8% in 20196. Obesity can lead to an increased risk of developing other diseases, including cardiovascular disease8, type 2 diabetes mellitus8 and cancer9.
Non-pharmacological strategies to reduce obesity include engaging in moderate to vigorous physical activity (MVPA) and minimizing sedentary behavior10. According to the World Health Organization (WHO), adults should aim for at least 150 min/week of MVPA to achieve significant health benefits11. However, global estimates show that physical inactivity (< 150 min/week of MVPA) affects 30.3% of adults12. In São Paulo, the prevalence of physical inactivity is even higher, at 38.3%13 .
Several studies on physical activity and obesity have examined only physical activity or sedentary time to predict obesity outcomes, while adjusting for covariates such as age, gender, smoking, and others14,15. However, since a day consists of only 24 h, individuals allocate this time across various behaviors, including sleep, sedentary activities in different contexts (e.g., work, screen time, studying, driving)16, and physical activities across different domains (e.g., work, leisure, transportation)17,18 and intensities (e.g., light, moderate, vigorous)19,20. Due to the finite nature of the 24-hour day, increasing time spent on one behavior (e.g., screen time) often results in a decrease in time allocated to another behavior (e.g., light-intensity physical activity)21.
In this context, isotemporal substitution analysis examines the theoretical effect of “substituting” equal amounts of time spent on one behavior (e.g., 60 min of screen time) with another behavior (e.g., 60 min of light physical activity) on health outcomes22,23,24. Additionally, isotemporal substitution analysis assumes that time-use behaviors, such as sedentary time and physical activity, are interdependent. This approach suggests that reallocating time from one behavior inevitably results in a reduction of another22,23,24.
A growing body of evidence shows that replacing various durations of sedentary behavior (10 min/day or 60 min/day) with physical activity is associated with improvements in various health markers25,26,27,28,29,30,31,32. For instance, Cao and colleagues demonstrated that substituting 60 min/day of sedentary time with 60 min/day of light or vigorous-intensity physical activity was associated with a reduced risk of COPD, depression, and diabetes25. Additionally, another study examining the substitution of 15, 30, 45, and 60 min/day of sedentary time for light and MVPA found negative associations with fat mass (assessed by bioelectrical impedance) and BMI in European adults33. However, most of these studies have been conducted in high-income33,34,35,36.
In contrast, there is limited evidence on the use of isotemporal substitution for obesity markers in Brazil, with most studies focusing on children and adolescents37,38,39. Furthermore, a study that analyzed isotemporal substitution in obesity among Brazilian adults considered only 10 min/day for the analysis40. Therefore, investigating the association between substituting physical activity and sedentary time for different periods could provide further insights into the ideal balance between these behaviors for improving body composition. Thus, the aim of this study was to evaluate the associations between substituting 10, 30 and 60 min/day of physical activity and sitting time with BMI, waist circumference and body fat among workers in São Paulo.
Methods
Study design and sample
This cross-sectional study was conducted among employees of the Regional Health Department (RHD) aged 18 to 73, residing in various regions of the state of São Paulo. Data collection took place between July and September 2018 at each RHD for convenience.
This study is part of the “Agita São Paulo” program, a state initiative aimed at combating sedentary lifestyles and physical inactivity in São Paulo41. Details of the “Agita São Paulo” program have been published previously41,42,43. As an extension of the program’s efforts, surveys are periodically conducted to assess levels of physical activity, sedentary behavior, and health-related factors (e.g., obesity, hypertension, functionality, and self-perceived health) among the population of São Paulo44.
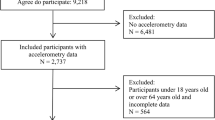
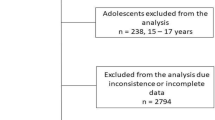
The state of São Paulo is divided into 17 RHD, and 15 15 of these departments from different regions participated in the study. A total of 1,056 workers met the eligibility criteria: (a) aged 18 years or older, (b) employed by an RHD, and (c) without clinical or functional limitations. Individuals with missing or inconsistent data on physical activity (n = 176), sitting time (n = 134), BMI (n = 74), waist circumference (n = 70), body fat (n = 76), age (n = 14), socioeconomic status (n = 51), marital status (n = 36), and educational level (n = 31) were excluded from the analysis. The final sample consisted of 394 adults (76.6% women).
Physical activity and sitting time
Participants reported their levels of physical activity and sitting time using the short version of the International Physical Activity Questionnaire (IPAQ), which has been validated in several countries, including Brazil45,46.
The data collection team instructed participants to report the frequency (days per week) and duration (≥ 10 min performed continuously) of walking, moderate physical activity (MPA), and vigorous physical activity (VPA) performed in the previous week. Average walking time, MPA, and VPA were calculated by multiplying frequency by duration and dividing by 7. IPAQ data were expressed in min/day25,47. Additionally, data where the total sum of walking time, MPA, and VPA exceeded 960 min/day were excluded from the analysis. Finally, data with at least 10 min/day of reported activity were considered valid for analysis48.
Participants also self-reported sitting time spent in various contexts (home, work, free time, studying, lying down watching television) during the last seven days. For the analysis, we used substitutions of 10, 30, and 60 min/day of walking, MPA, VPA, and sitting time. These periods were specifically chosen based on previous studies that have demonstrated significant associations with health outcomes, including type 2 diabetes, metabolic syndrome, glycated hemoglobin, and waist circumference49,50.
Obesity indicators
BMI, waist circumference, and body fat were used as indicators of obesity. Height (cm) was measured using a Seca 213 portable stadiometer (Seca 213®, Hamburg, Germany) with an accuracy of 0.5 cm. Participants were instructed to stand barefoot in an upright position, aligned with the Frankfurt plane.
Body weight (kg) was measured using a Tanita SC-240 bioelectrical impedance device (TANITA Corporation, Japan), which has a maximum capacity of 200 kg. BMI (kg/m²) was calculated by dividing body weight (kg) by height (m²).
Waist circumference (cm) was measured using an inelastic tape measure (Sanny, São Paulo, Brazil) with an accuracy of 0.1 cm. The tape was placed horizontally at the level of the umbilical scar while the participant stood in an upright position. Three measurements were taken, and the average was calculated.
Body fat (kg) was measured using bioelectrical impedance with the Tanita SC-240 portable body composition analyzer (TANITA Corporation, Japan). The analyzer uses four electrodes placed on the feet, with a frequency of 50 kHz and an electric current of 90 milliamps. Participants’ height, age, and gender were entered into the scale’s software before measurement. Once the information was input, participants were instructed to stand straight in the Frankfurt plane. Bioelectrical impedance analysis has demonstrated acceptable validity and reproducibility in adults when compared to dual-energy X-ray absorptiometry51.
Correlates
A standardized questionnaire was used across all departments during the interviews to collect sociodemographic data. Participants were categorized by age (< 65 and ≥ 65 years), sex (male and female), and marital status (single, married, divorced, and widowed). In addition, participants were classified by socioeconomic status (low, medium, and high) according to the Brazilian income classification index52. Educational level was categorized as low (up to elementary school), medium (completed elementary school), and high (university degree, master’s degree, PhD, or post-doctorate).
Statistical analyses
The Kolmogorov-Smirnov test was used to assess the normality of the data distribution. Frequency and percentage (%) were used to describe categorical variables. Given the non-normal distribution of data on physical activity, sitting time, and obesity indicators, continuous variables were reported as medians and interquartile ranges (25th and 75th percentiles).
Multivariate linear regression analysis (β coefficient) and 95% confidence intervals (95% CI) were used to assess the associations between different durations (10, 30, and 60 min/day) of sitting time, walking, MPA, and VPA with obesity indicators (BMI, waist circumference, and body fat). Due to the non-parametric distribution of sitting time, physical activity variables, and obesity indicators, we transformed the non-parametric data using a log10 transformation.
Linear models for single activities, partitioning, and isotemporal substitution were employed, following the method proposed by Merkay and colleagues22. The single-activity model assessed the associations of each behavior independently, adjusting for covariates, without including other behaviors in the statistical model. In contrast, the partition model considers all activities that contribute to the total time spent and evaluates the effect of each time-use behavior on the outcome variable independently. However, the partition model is not isotemporal, as it does not include the total time variable (the sum of sitting time, walking, MPA, and VPA) in the analysis.
The isotemporal model, however, assumes the effect of substituting one specific behavior for another within the same time period. For instance, when analyzing the effect of substituting 60 min/day of sitting time with 60 mi/day of walking or VPA on BMI, sitting time is excluded from the analysis. The coefficients generated for walking and VPA represent the effect of replacing sitting time with these activities, while keeping covariates and total time within the analysis.
The single-activity, partition, and isotemporal models were applied to the periods of 10, 30, and 60 min per day of sitting time and physical activity to assess obesity outcomes. All analyses were adjusted for age, sex, marital status, socioeconomic status, and educational level. A significance level of p < 0.05 was considered, and analyses were conducted using SPSS, version 24 (SPSS Inc., IBM Corp., Armonk, Nova York, NY, EUA).
Ethics approval and consent to participate
All aspects of the study were in accordance with the Declaration of Helsinki. The study was approved by the Ethics Committee of Universidade Municipal de São Caetano do Sul under protocol number 2.531.002. All participants provided written informed consent or assent before participating in the study. To ensure confidentiality, participants’ data was anonymized using numeric identification codes instead of names.
Results
The characteristics of the participants are summarized in Table 1. Overall, the sample was predominantly female (76.6%), with a medium socioeconomic level (59.1%), married (52.5%), and highly educated (63.2%). Participants self-reported a median of 150 min/day of walking (IQR: 60.0 − 360.0), 180 min/day of MPA (IQR: 78.7 − 450.0), and 60 min/day of VPA (IQR: 0.0 − 240.0). In contrast, the median sitting time was 445.7 min/day (IQR: 317.1 − 565.7).
Table 2 presents the results of the single and partial activity analyses examining the associations between different patterns of physical activity and sitting time with obesity indicators. In the single activity models, both 10 and 60 min/day of walking were negatively associated with waist circumference (β: -0.125; 95% CI: -0.025; -0.004; β: -0.135; 95% CI: -0.026; -0.005, respectively) and body fat (β: -0.101; 95% CI: -0.067; -0.001; β: -0.111; 95% CI: -0.068; -0.003, respectively). No significant associations were found between 30 min/day of physical activity or sitting time and obesity indicators. In the partitioned model, only 10 min/day of walking was negatively associated with waist circumference (β: -0.129; 95% CI: -0.028; -0.001).
No statistically significant association was found between substituting 10 min/day of physical activity or sitting time with BMI (Table 3). On the other hand, substituting 10 min/day of MPA and 10 min/day of VPA for 10 min/day of walking (β: -0.176; 95% CI: -0.037; -0.002; β: -0.183; 95% CI: -0.037; -0.004) was associated with waist circumference. Additionally, substituting 10 min/day of sitting time for 10 min/day of walking (β: -0.216; 95% CI: -0.041; -0.007) was negatively associated with waist circumference. Similarly, substituting 10 min/day of VPA with 10 min/day of walking (β: -0.172; 95% CI: -0.106; -0.005) was associated with a decrease in body fat. Furthermore, substituting 10 min/day of sitting time for 10 min/day of walking (β: -0.203; 95% CI: -0.119; -0.012) or MPA (β: -0.208; 95% CI: -0.127; -0.008) was negatively associated with body fat (Table 3).
No associations were found between substituting 30 min/day of physical activity or sitting time with BMI, waist circumference, or body fat (Table 4).
Table 5 shows the associations between the substitution of 60 min/day of physical activity and sitting time with indicators of obesity. Substituting 60 min/day of VPA for 60 min/day of walking (β: -0.151; 95% CI: -0.033; -0.001) was negatively associated with waist circumference. In addition, substituting 60 min/day of sitting time for MPA (β: -0.206; 95% CI: -0.123; -0.008) was negatively associated with body fat.
Discussion
The present study examined the associations between substituting 10, 30 and 60 min/day of physical activity and sitting time with BMI, waist circumference and body fat among workers in São Paulo. Overall, the results of this study suggest that substituting different patterns of sitting time with various forms of physical activity may be associated with a reduction in obesity indicators in São Paulo workers.
Both 10 min/day and 60 min/day of walking were associated with lower waist circumference and body fat in the single and partition models, but no associations were found with higher-intensity activities. These findings are consistent with studies in high- and middle-income countries33,40,53,54, which have shown that light-intensity physical activity (10 and 60 min/day), as measured by accelerometry and self-report, is negatively associated with BMI, body fat, and waist circumference. Walking, in particular, can be a more accessible form of physical activity, as it requires no prior experience and involves no financial cost55. Furthermore, the potential benefits of light physical activity on obesity and cardiovascular risk, as well as its significance for public health, have already been well established19,56.
In the isotemporal substitution model, beneficial associations were found when substituting at least 10 min/day of sitting time with 10 min/day of walking and 10 min/day of MPA, which were linked to lower waist circumference and body fat, respectively. A study by Gonze and colleagues40, conducted with 780 Brazilian adults (493 women), found that substituting 10 min/day of sedentary time with 10 min/day of light physical activity or MVPA was associated with reductions in BMI (β = -0.104) and fat percentage (β = -0.383). Sitting time, a form of sedentary behavior, is strongly associated with an increase in waist circumference, visceral adipose tissue, and body fat, which in turn are linked to the development of certain cancers (including digestive system and colorectal cancers) and all-cause mortality14,57,58. Our findings suggest that reducing sitting time and increasing physical activity levels can positively impact obesity indicators and may help reduce the risk of adverse health outcomes.
Curiously, our results showed that substituting 10 min/day of MPA and VPA with 10 min/day of walking was associated with a reduction in obesity indicators (waist circumference and body fat). These findings are not consistent with the WHO’s recommendation of at least 60 min/day of MVPA11. This discrepancy may be due to the discomfort higher-intensity activities may cause compared to light physical activity59,60. Additionally, walking is a natural activity that helps break sedentary behavior, improves lipid metabolism, and can be sustained for long periods61,62,63. However, it is important to highlight the potential benefits of higher-intensity activities, such as greater energy expenditure and improved health markers, which have been widely demonstrated in the literature34,39,64,65.
We found no association between substituting 30 min/day of physical activity and sitting time with obesity indicators. These results contrast with existing literature49,50,66,67. Additionally, a systematic review study49 examining the effect of isotemporal substitution on various obesity indicators found that some studies included in the review analyzed the effects of 30 min/day and reported associations with different obesity indicators, such as BMI, waist circumference, and body fat percentage. We hypothesize that methodological differences between our study and the cited studies may explain the discrepancies. For example, the sample size in our study was smaller than in other studies50,66. Additionally, objective methods, such as accelerometry, were used to measure physical activity in these studies50,67, which was not feasible in our study. While questionnaires are commonly used in large-scale studies due to their practicality, accelerometry helps reduce memory bias by directly measuring physical activity and sedentary time without relying on self-reports68,69. Finally, the studies mentioned above50 estimated body composition objectively, which was not possible in our study. These differences in measurement methods could lead to variations in body composition estimates and impact the analysis70.
Finally, a previous population-based study found that substituting 60 min/day of MVPA for sedentary time (assessed using accelerometry) was negatively associated with fat mass and body fat, as measured by bioelectrical impedance33. Similarly, Wang and colleagues observed beneficial effects on overweight and obesity when sedentary time was replaced with MVPA, as assessed by the IPAQ34. These findings support our results and emphasize the need for effective strategies to encourage reallocating sedentary time to more active behaviors.
Educating the public about the distribution of time spent on various behaviors can have positive implications for public health71. Given the challenges middle-aged and older adults face in performing VPA for extended periods72,73, replacing sedentary time with at least 10 min/day of light physical activity could be a useful starting point for reducing overweight and obesity.
This study has several limitations. Due to its cross-sectional design, we cannot establish causal relationships. Additionally, our results may not be generalizable to other populations, as the sample consisted mainly of Brazilian workers with a high socioeconomic status and education level. We also could not assess the amount of sleep as part of the full 24-hour movement cycle. While the IPAQ’s validity has been established, memory bias may have led participants to over report physical activity levels and underreport sedentary time74. Body fat was measured indirectly using bioelectrical impedance, so the estimates are prone to error75,76. Finally, we were unable to account for other potential confounders, such as race/ethnicity, household income, energy consumption, and the built environment.
Conclusion
The results of this study suggest that substituting 10 min/day and 60 min/day of sitting time for 60 min/day of walking or MPA is beneficial for reducing waist circumference and body fat. These findings align with existing literature on the positive effects of walking on body composition and support lifestyle interventions that promote replacing sitting time with physical activity to reduce and prevent obesity. Furthermore, our results underscore the need for longitudinal studies to evaluate the long-term effects of these time-use behavior substitutions on obesity indicators.
Data availability
The datasets generated and/or analyzed during the current study are not publicly available due the terms of consent/assent to which the participants agreed but are available from the corresponding author on reasonable request. Please contact the corresponding author to discuss availability of data and materials.
References
Estivaleti, J. M. et al. Time trends and projected obesity epidemic in Brazilian adults between 2006 and 2030. Sci. Rep. 12, 12699. https://doi.org/10.1038/s41598-022-16934-5 (2022).
Phelps, N. H. et al. Worldwide trends in underweight and obesity from 1990 to 2022: a pooled analysis of 3663 population-representative studies with 222 million children, adolescents, and adults. Lancet https://doi.org/10.1016/S0140-6736(23)02750-2 (2024).
Nilson, E. A. F., Gianicchi, B., Ferrari, G. & Rezende, L. F. M. The projected burden of non-communicable diseases attributable to overweight in Brazil from 2021 to 2030. Sci. Rep. 12, 22483. https://doi.org/10.1038/s41598-022-26739-1 (2022).
Assis Comaru, F. & Faria Westphal, M. Housing, urban development and health in latin America: contrasts, inequalities and challenges. Rev. Environ. Health. 19, 329–346. https://doi.org/10.1515/reveh-2004-19-3-410 (2021).
IBGE. Censo Demográfico. https://www.ibge.gov.br/ Accessed March 2022 (2022).
Lima, A. P., Nunes, A., Nicoletti, C. F. & Benatti, F. B. Trend in the prevalence of overweight and obese adults in Sao Paulo, Brazil: analysis between the years 2006 and 2019. Int. J. Environ. Res. Public. Health. 21 https://doi.org/10.3390/ijerph21040502 (2024).
Greene, J. & Guanais, F. An examination of socioeconomic equity in health experiences in six latin American and Caribbean countries. Rev. Panam. Salud Publica. 9, 42:e127. https://doi.org/10.26633/RPSP.2018.127 (2018).
Riaz, H. et al. Association between obesity and cardiovascular outcomes: a systematic review and meta-analysis of mendelian randomization studies. JAMA Netw. Open. 1, e183788. https://doi.org/10.1001/jamanetworkopen.2018.3788 (2018).
Parra-Soto, S. et al. Associations of six adiposity-related markers with incidence and mortality from 24 cancers-findings from the UK Biobank prospective cohort study. BMC Med. 19, 7. https://doi.org/10.1186/s12916-020-01848-8 (2021).
O’Donoghue, G., Blake, C., Cunningham, C., Lennon, O. & Perrotta, C. What exercise prescription is optimal to improve body composition and cardiorespiratory fitness in adults living with obesity? A network meta-analysis. Obes. Rev. 22, e13137. https://doi.org/10.1111/obr.13137 (2021).
Bull, F. C. et al. World Health Organization 2020 guidelines on physical activity and sedentary behaviour. Br. J. Sports Med. 54, 1451–1462. https://doi.org/10.1136/bjsports-2020-102955 (2020).
Strain, T. et al. National, regional, and global trends in insufficient physical activity among adults from 2000 to 2022: a pooled analysis of 507 population-based surveys with 5.7 million participants. Lancet Glob Health. 12, e1232–e1243. https://doi.org/10.1016/S2214-109X(24)00150-5 (2024).
Ministério da Saúde. Vigitel Brasil 2006–2023: vigilância de fatores de risco e proteção para doenças crônicas por inquérito telefônico : estimativas sobre frequência e distribuição sociodemográfica de prática de atividade física nas capitais dos 26 estados brasileiros e no Distrito Federal entre 2006 e 2023 : prática de atividade física. Ministério da Saúde, Secretaria de Vigilância em Saúde e Ambiente, Departamento de Análise Epidemiológica e Vigilância de Doenças não Transmissíveis. – Brasília : Ministério da Saúde. (2024).
Silveira, E. A. et al. Sedentary behavior, physical inactivity, abdominal obesity and obesity in adults and older adults: a systematic review and meta-analysis. Clin. Nutr. ESPEN. 50, 63–73. https://doi.org/10.1016/j.clnesp.2022.06.001 (2022).
Biddle, S. J. H. et al. Erratum to: screen time, other sedentary behaviours, and obesity risk in adults: a review of reviews. Curr. Obes. Rep. 6, 352. https://doi.org/10.1007/s13679-017-0267-6 (2017).
Saunders, T. J. et al. Sedentary behaviour and health in adults: an overview of systematic reviews. Appl. Physiol. Nutr. Metab. 45, S197–S217. https://doi.org/10.1139/apnm-2020-0272 (2020).
Kazemi, A. et al. Leisure-time and occupational physical activity and risk of cardiovascular disease incidence: a systematic-review and dose-response meta-analysis of prospective cohort studies. Int. J. Behav. Nutr. Phys. Act. 21, 45. https://doi.org/10.1186/s12966-024-01593-8 (2024).
Paluch, A. E. et al. Daily steps and all-cause mortality: a meta-analysis of 15 international cohorts. Lancet Public. Health. 7, e219–e228. https://doi.org/10.1016/S2468-2667(21)00302-9 (2022).
Ross, R., Janssen, I. & Tremblay, M. S. Public health importance of light intensity physical activity. J. Sport Health Sci. 13, 674–675. https://doi.org/10.1016/j.jshs.2024.01.010 (2024).
Rey Lopez, J. P., Sabag, A., Martinez Juan, M., Rezende, L. F. M. & Pastor-Valero, M. Do vigorous-intensity and moderate-intensity physical activities reduce mortality to the same extent? A systematic review and meta-analysis. BMJ Open. Sport Exerc. Med. 6, e000775. https://doi.org/10.1136/bmjsem-2020-000775 (2020).
Dumuid, D. et al. Compositional data analysis for physical activity, sedentary time and sleep research. Stat. Methods Med. Res. 27, 3726–3738. https://doi.org/10.1177/0962280217710835 (2018).
Mekary, R. A., Willett, W. C., Hu, F. B. & Ding, E. L. Isotemporal substitution paradigm for physical activity epidemiology and weight change. Am. J. Epidemiol. 170, 519–527. https://doi.org/10.1093/aje/kwp163 (2009).
Mekary, R. A. Isotemporal substitution model for physical activity and osteoarthritis outcomes. Osteoarthr. Cartil. 26, 1571–1572. https://doi.org/10.1016/j.joca.2018.07.003 (2018).
Mekary, R. A. et al. Isotemporal substitution analysis for physical activity, television watching, and risk of depression. Am. J. Epidemiol. 178, 474–483. https://doi.org/10.1093/aje/kws590 (2013).
Cao, Z., Xu, C., Zhang, P. & Wang, Y. Associations of sedentary time and physical activity with adverse health conditions: outcome-wide analyses using isotemporal substitution model. EClinicalMedicine 48, 101424. https://doi.org/10.1016/j.eclinm.2022.101424 (2022).
Sun, Y. et al. Isotemporal substitution of sedentary behavior for physical activity on cardiorespiratory fitness in children and adolescents. Med. (Baltim). 99, e21367. https://doi.org/10.1097/MD.0000000000021367 (2020).
Boyle, T., Vallance, J. K., Buman, M. P. & Lynch, B. M. Reallocating time to sleep, sedentary time, or physical activity: associations with waist circumference and body mass index in breast cancer survivors. Cancer Epidemiol. Biomarkers Prev. 26, 254–260. https://doi.org/10.1158/1055-9965.EPI-16-0545 (2017).
Sadarangani, K. P. et al. Exchanging screen for non-screen sitting time or physical activity might attenuate depression and anxiety: a cross-sectional isotemporal analysis during early pandemics in South America. J. Sci. Med. Sport. 26, 309–315. https://doi.org/10.1016/j.jsams.2023.04.007 (2023).
Lai, T. F. et al. Effect of isotemporal substitution of sedentary behavior with different intensities of physical activity on the muscle function of older adults in the context of a medical center. BMC Geriatr. 23, 130. https://doi.org/10.1186/s12877-023-03819-z (2023).
Moura, B. P., Rufino, R. L., Faria, R. C., Sasaki, J. E. & Amorim, P. R. S. Can replacing sitting time with standing time improve adolescents’ cardiometabolic health? Int. J. Environ. Res. Public. Health. 16 https://doi.org/10.3390/ijerph16173115 (2019).
Feter, N. et al. Association between 24-hour movement behavior and cognitive function in Brazilian middle-aged and older adults: findings from the ELSA-Brasil. Innov. Aging. 7, igad030. https://doi.org/10.1093/geroni/igad030 (2023).
Freire, A. et al. Isotemporal substitution of sedentary behavior by different physical activity intensities on pain and disability of patients with chronic low back pain: a cross-sectional study. Arch. Phys. Med. Rehabil. 103, 1944–1950. https://doi.org/10.1016/j.apmr.2022.03.017 (2022).
Farrahi, V. et al. Replacing sedentary time with physical activity and sleep: associations with cardiometabolic health markers in adults. Scand. J. Med. Sci. Sports. 33, 907–920. https://doi.org/10.1111/sms.14323 (2023).
Wang, J. et al. Isotemporal substitution of different behaviour patterns with the presence of MAFLD in Chinese adults. Liver Int. 42, 2683–2695. https://doi.org/10.1111/liv.15439 (2022).
Dumuid, D. et al. Relationships between older adults’ use of time and cardio-respiratory fitness, obesity and cardio-metabolic risk: a compositional isotemporal substitution analysis. Maturitas 110, 104–110. https://doi.org/10.1016/j.maturitas.2018.02.003 (2018).
Swindell, N. et al. Compositional analysis of the associations between 24-h movement behaviours and cardio-metabolic risk factors in overweight and obese adults with pre-diabetes from the PREVIEW study: cross-sectional baseline analysis. Int. J. Behav. Nutr. Phys. Act. 17, 29. https://doi.org/10.1186/s12966-020-00936-5 (2020).
Volpato, L. A. et al. Associations between substitution of sedentary behavior patterns with physical activity and cardiovascular risk factors in adolescents: a 3-year longitudinal study. J. Phys. Act. Health. 21, 1114–1120. https://doi.org/10.1123/jpah.2024-0149 (2024).
Domingues, S. F., Diniz da Silva, C., Faria, F. R., de Sa Souza, H. & Dos Santos Amorim, P. R. Sleep, sedentary behavior, and physical activity in Brazilian adolescents: achievement recommendations and BMI associations through compositional data analysis. PLoS One. 17, e0266926. https://doi.org/10.1371/journal.pone.0266926 (2022).
Moura, B. P., Rufino, R. L., Faria, R. C. & Amorim, P. R. S. Effects of isotemporal substitution of sedentary behavior with light-intensity or moderate-to-vigorous physical activity on cardiometabolic markers in male adolescents. PLoS One. 14, e0225856. https://doi.org/10.1371/journal.pone.0225856 (2019).
Gonze, B. B. et al. Effects of substituting sedentary behavior with light-intensity or moderate-to-vigorous physical activity on obesity indices in adults: a prospective short-term follow-up study. Int. J. Environ. Res. Public. Health. 18 https://doi.org/10.3390/ijerph182413335 (2021).
Matsudo, V. et al. Promotion of physical activity in a developing country: the Agita Sao Paulo experience. Public. Health Nutr. 5, 253–261. https://doi.org/10.1079/phn2001301 (2002).
Matsudo, S. M. et al. The Agita Sao Paulo Program as a model for using physical activity to promote health. Rev. Panam. Salud Publica. 14, 265–272. https://doi.org/10.1590/s1020-49892003000900007 (2003).
Matsudo, V. The role of partnerships in promoting physical activity: the experience of Agita Sao Paulo. Health Place. 18, 121–122. https://doi.org/10.1016/j.healthplace.2011.09.011 (2012).
Silva, L. J. et al. The prevalence of physical activity and its associated effects among students in the Sao Paulo public school network, Brazil. Cien Saude Colet. 21, 1095–1103. https://doi.org/10.1590/1413-81232015214.19792015 (2016).
Craig, C. L. et al. International physical activity questionnaire: 12-country reliability and validity. Med. Sci. Sports Exerc. 35, 1381–1395. https://doi.org/10.1249/01.MSS.0000078924.61453.FB (2003).
Matsudo, S. et al. QUESTIONÁRIO INTERNACIONAL DE ATIVIDADE FÍSICA (IPAQ): ESTUDO DE VALIDADE E REPRODUTIBILIDADE NO BRASIL. Revista Brasileira De Atividade Física Saúde 6, 5–18. doi:https://doi.org/10.12820/rbafs.v.6n2p5-18 (2012).
Liu, Y., Lin, H., Zhang, H., Zhang, X. & Yin, S. Correlation analysis between physical activity and depressive tendencies among occupational groups: an isotemporal substitution approach. BMC Public. Health. 23, 2241. https://doi.org/10.1186/s12889-023-17134-0 (2023).
COMMITTEE I R. Guidelines for the Data Processing and Analysis of the International Physical Activity Questionnaire [EB/OL]. (2005). https://sites.google.com/site/theipaq. Accessed December 2024.
Grgic, J. et al. Health outcomes associated with reallocations of time between sleep, sedentary behaviour, and physical activity: a systematic scoping review of isotemporal substitution studies. Int. J. Behav. Nutr. Phys. Act. 15, 69. https://doi.org/10.1186/s12966-018-0691-3 (2018).
Galmes-Panades, A. M. et al. Isotemporal substitution of inactive time with physical activity and time in bed: cross-sectional associations with cardiometabolic health in the PREDIMED-Plus study. Int. J. Behav. Nutr. Phys. Act. 16, 137. https://doi.org/10.1186/s12966-019-0892-4 (2019).
Jensky-Squires, N. E. et al. Validity and reliability of body composition analysers in children and adults. Br. J. Nutr. 100, 859–865. https://doi.org/10.1017/S0007114508925460 (2008).
Pesquisa, A. B. d. E. d. & Pesquisa, A. B. d. E. d. Critério de classificação econômica Brasil. (2014). http://www.abep.org/criterio-brasil Accessed April 2024.
Sadarangani, K. P. et al. Substituting sedentary time with physical activity domains: an isotemporal substitution analysis in Chile. J. Transp. Health. 14, 100593. https://doi.org/10.1016/j.jth.2019.100593 (2019).
Stamatakis, E. et al. All-cause mortality effects of replacing sedentary time with physical activity and sleeping using an isotemporal substitution model: a prospective study of 201,129 mid-aged and older adults. Int. J. Behav. Nutr. Phys. Act. 12, 121. https://doi.org/10.1186/s12966-015-0280-7 (2015).
Hansen, B. H. et al. Step by step: Association of device-measured daily steps with all-cause mortality-A prospective cohort study. Scand. J. Med. Sci. Sports. 30, 1705–1711. https://doi.org/10.1111/sms.13726 (2020).
Chastin, S. F. M. et al. How does light-intensity physical activity associate with adult cardiometabolic health and mortality? Systematic review with meta-analysis of experimental and observational studies. Br. J. Sports Med. 53, 370–376. https://doi.org/10.1136/bjsports-2017-097563 (2019).
Dhawan, D. & Sharma, S. Abdominal obesity, adipokines and non-communicable diseases. J. Steroid Biochem. Mol. Biol. 203, 105737. https://doi.org/10.1016/j.jsbmb.2020.105737 (2020).
Jayedi, A., Khan, T. A., Aune, D., Emadi, A. & Shab-Bidar, S. Body fat and risk of all-cause mortality: a systematic review and dose-response meta-analysis of prospective cohort studies. Int. J. Obes. (Lond). 46, 1573–1581. https://doi.org/10.1038/s41366-022-01165-5 (2022).
Ekkekakis, P., Parfitt, G. & Petruzzello, S. J. The pleasure and displeasure people feel when they exercise at different intensities. Sports Med. 41, 641–671. https://doi.org/10.2165/11590680-000000000-00000 (2011).
Niedermeier, M., Ledochowski, L., Leitner, H., Zingerle, H. & Kopp, M. Acute effects of a single bout of walking on affective responses in patients with major depressive disorder. Int. J. Environ. Res. Public. Health. 18 https://doi.org/10.3390/ijerph18041524 (2021).
Amagasa, S. et al. Is objectively measured light-intensity physical activity associated with health outcomes after adjustment for moderate-to-vigorous physical activity in adults? A systematic review. Int. J. Behav. Nutr. Phys. Act. 15, 65. https://doi.org/10.1186/s12966-018-0695-z (2018).
Collings, P. J. et al. Substituting device-measured sedentary time with alternative 24-hour movement behaviours: compositional associations with adiposity and cardiometabolic risk in the ORISCAV-LUX 2 study. Diabetol. Metab. Syndr. 15, 70. https://doi.org/10.1186/s13098-023-01040-x (2023).
Duvivier, B. et al. Reducing sitting time versus adding exercise: differential effects on biomarkers of endothelial dysfunction and metabolic risk. Sci. Rep. 8, 8657. https://doi.org/10.1038/s41598-018-26616-w (2018).
Cao, Y. et al. The effect of different intensity physical activity on cardiovascular metabolic health in obese children and adolescents: an isotemporal substitution model. Front. Physiol. 14, 1041622. https://doi.org/10.3389/fphys.2023.1041622 (2023).
Galmes-Panades, A. M. et al. Targeting body composition in an older population: do changes in movement behaviours matter? Longitudinal analyses in the PREDIMED-Plus trial. BMC Med. 19, 3. https://doi.org/10.1186/s12916-020-01847-9 (2021).
Larsen, S. C. et al. Substituting sedentary time with sleep or physical activity and subsequent weight-loss maintenance. Obes. (Silver Spring). 31, 515–524. https://doi.org/10.1002/oby.23631 (2023).
Lai, T. F. et al. Substituting sedentary time with physical activity in youngest-old to oldest-old community-dwelling older adults: associations with body composition. Front. Public. Health. 10, 837213. https://doi.org/10.3389/fpubh.2022.837213 (2022).
Ferrari, G. L. et al. Comparison of self-report versus accelerometer – measured physical activity and sedentary behaviors and their association with body composition in latin American countries. PLOS ONE. 15, e0232420. https://doi.org/10.1371/journal.pone.0232420 (2020).
Colley, R. C., Butler, G., Garriguet, D., Prince, S. A. & Roberts, K. C. Comparison of self-reported and accelerometer-measured physical activity among Canadian youth. Health Rep. 30, 3–12. https://doi.org/10.25318/82-003-x201900700001-eng (2019).
Kuriyan, R. Body composition techniques. Indian J. Med. Res. 148, 648–658. https://doi.org/10.4103/ijmr.IJMR_1777_18 (2018).
Dumuid, D. et al. The compositional isotemporal substitution model: a method for estimating changes in a health outcome for reallocation of time between sleep, physical activity and sedentary behaviour. Stat. Methods Med. Res. 28, 846–857. https://doi.org/10.1177/0962280217737805 (2019).
Manas, A. et al. Reallocating accelerometer-assessed sedentary time to light or moderate- to vigorous-intensity physical activity reduces frailty levels in older adults: an isotemporal substitution approach in the TSHA study. J. Am. Med. Dir. Assoc. 19, 185e181–185e186. https://doi.org/10.1016/j.jamda.2017.11.003 (2018).
Shi, H. et al. Sedentary behaviors, light-intensity physical activity, and healthy aging. JAMA Netw. Open. 7, e2416300. https://doi.org/10.1001/jamanetworkopen.2024.16300 (2024).
Biskup, M. et al. Agreement between accelerometer-assessed and self-reported physical activity and sedentary behavior in female breast cancer survivors. Diagnostics (Basel). 13. https://doi.org/10.3390/diagnostics13223447 (2023).
Marra, M. et al. Assessment of body composition in health and disease using bioelectrical impedance analysis (BIA) and dual energy x-ray absorptiometry (DXA): a critical overview. Contrast Media Mol Imaging. 2019, 3548284. https://doi.org/10.1155/2019/3548284 (2019).
Gaba, A., Kapus, O., Cuberek, R. & Botek, M. Comparison of multi- and single-frequency bioelectrical impedance analysis with dual-energy X-ray absorptiometry for assessment of body composition in post-menopausal women: effects of body mass index and accelerometer-determined physical activity. J. Hum. Nutr. Diet. 28, 390–400. https://doi.org/10.1111/jhn.12257 (2015).
Acknowledgements
We would like to thank all the staff at the Regional Health Department. We would also like to thank the researchers and the collection team for developing this study and the Agita São Paulo program.
Author information
Authors and Affiliations
Contributions
JPSJ, RRB and AS carried out the study, collected and interpreted the data. DS, GF, JPSJ, RRB, PPOM, AS and MS helped to write and revise the manuscript; VM was responsible for coordinating the overall study and contributed to the intellectual content. All the authors contributed to the study design, critically reviewed the manuscript and approved the final version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Sales, D., Ferrari, G., da Silva Junior, J.P. et al. Isotemporal substitution of physical activity patterns and sitting time with obesity indicators among workers in São Paulo. Sci Rep 15, 1684 (2025). https://doi.org/10.1038/s41598-025-85601-2
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-85601-2