Abstract
Prostate cancer (PCa) is one of the most common cancers among men worldwide, and robot-assisted radical prostatectomy (RARP) is a widely used treatment for localized PCa. Achieving pentafecta outcomes, which include continence, potency, cancer control, free surgical margins, and no major complications, is a critical measure of surgical success and long-term prognosis. However, predicting these outcomes remains challenging. In this retrospective, single-center study, we analyzed data from 1,752 patients who underwent RARP for localized prostate adenocarcinoma between August 2009 and April 2023. The pentafecta outcome was achieved in 290 patients (16.6%). Multivariate analysis revealed that bilateral nerve sparing significantly increased the likelihood of achieving the pentafecta outcome (odds ratio 10.36, 95% CI: 5.75–18.66; p < 0.001). Preoperative potency and bilateral nerve sparing were also identified as key predictors. Nomograms were developed using preoperative and postoperative variables, including age, PSA level, biopsy Gleason score, clinical stage, pathological tumor stage, tumor grade, nerve sparing, and preoperative potency. Internal validation of the nomograms was performed using bootstrapping methods, demonstrating robust predictive performance. These nomograms provide valuable tools for personalized surgical planning and patient counseling and may be applicable to broader populations, given the inclusion of universally recognized predictive factors and rigorous validation. This study presents the development and validation of nomograms to predict pentafecta outcomes before and after RARP. These nomograms provide valuable tools for clinicians to estimate the likelihood of achieving postoperative pentafecta outcomes. Incorporating these nomograms into clinical practice may improve patient counseling and shared decision-making.
Similar content being viewed by others
Introduction
Prostate cancer (PCa) is a common malignancy among elderly males1. Radical prostatectomy (RP) is one of the main curative treatment options for patients with localized PCa, with oncological and functional outcomes comparable to those of radiotherapy2,3. The introduction of robotic platforms has led to the widespread adoption of robot-assisted RP (RARP), which has replaced open surgery at many centers4,5.
Recent advancements in robotic surgery have demonstrated significant improvements in surgical precision and patient outcomes, as highlighted by studies focusing on novel robotic platforms and their application in minimally invasive procedures6,7.
After surgical intervention, the assessment of functional and oncological outcomes is crucial for both surgeons and patients. Trifecta outcomes, including erectile function, biochemical recurrence-free survival (BCRFS), and urinary incontinence, have been used to evaluate the quality of RP outcomes8. The inclusion of surgical margins and complication rates in the trifecta resulted in pentafecta outcomes9,10. However, the definitions of functional outcomes such as incontinence and erectile dysfunction lack standardization, and reporting timeframes vary across studies, thereby hindering pooled analyses8. Numerous studies have investigated the predictors of trifecta and pentafecta outcomes after RP9,11,12,13,14.
Factors such as prostate-specific antigen (PSA) level, clinical stage, Gleason score, baseline erectile function, time since RP, and age at RP have been identified as predictors11,12,13,14,15,16.
While existing research has predominantly centered on Western populations, a notable dearth of high-quality data persists regarding outcome predictors in Asian, particularly Japanese, patient cohorts. Recognizing this critical gap, our retrospective study specifically focuses on Japanese patients undergoing Robot-Assisted Radical Prostatectomy (RARP). Our primary goal is the development and validation of nomograms tailored to predict pentafecta outcomes—encompassing urinary continence, margin status, BCRFS, postoperative potency, and complications. Leveraging a substantial patient cohort from our institution, we aim to discern independent predictors, ultimately empowering clinicians with enhanced tools for preoperative counseling and refined decision-making processes.
Materials and methods
In this retrospective study, we searched our prospectively maintained database of RARP cases from August 2009 to April 2023. Prior to surgery, all patients included in the study underwent clinical, biochemical, and radiological evaluations. The clinical examination followed a standardized approach involving a comprehensive patient history and physical examination. Biochemical investigations included complete blood count, kidney and liver function tests, coagulation profiling, and quantification of PSA levels. Radiological assessments varied among the patients and comprised a combination of multiparametric magnetic resonance imaging (mpMRI), contrast-enhanced computed tomography of the abdomen and pelvis, or a bone scan. The initial diagnosis in all patients was based on transrectal or transperineal ultrasound-guided prostate biopsy. The authors affirm the availability and accessibility of all original data presented in this study. The study protocol was approved by the Ethics Committee of the Fujita Health University Hospital (approval no. HM19-265).
Baseline data
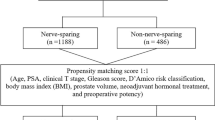
Baseline data for each patient included several factors, including age, body mass index (BMI), preoperative PSA level, clinical stage, neoadjuvant hormonal therapy, prostate volume, and D’Amico risk staging17.
Radiological and biopsy data
Radiological data were retrieved and used to determine the local clinical stage by combining findings from mpMRI with those from digital rectal examination. The biopsy data included important information such as the Gleason score. These data were crucial in assessing the extent and characteristics of PCa in each patient.
Operative technique and variables
Surgical procedures were conducted by skilled robotic surgeons using the da Vinci Si and Xi systems (Intuitive Surgical, Sunnyvale, CA, USA)18,19,20 and the Hinotori system (Medicaroid). Detailed data regarding operative variables, such as operative time, console time, extent of nerve sparing, and estimated blood loss, were also collected for analysis. These parameters provided insights into the surgical technique and intraoperative aspects of the procedures performed.
Postoperative follow‑up
Complications were assessed during a 90-day period according to the Clavien-Dindo classification21. Following discharge, patients underwent scheduled follow-up visits at one week for catheter removal and subsequently at one month for quantification of serum PSA levels. Subsequent monitoring of serum PSA levels was performed in accordance with the guidelines outlined by the European Association of Urology3. Information regarding Gleason score and margin status was obtained from the final biopsy report. These data provided valuable insights into the pathological characteristics and outcomes of patients.
Data collection
Data on patient demographics, preoperative variables (e.g., age, BMI, PSA levels, Gleason score, and clinical stage), surgical details (e.g., surgical approach, surgical time, and blood loss), and postoperative outcomes were obtained from electronic medical records. Pentafecta outcomes were assessed at the following postoperative time points: 3, 6, and 9 months, and 1 year.
Pentafecta outcome
Continence was assessed based on the usage of ‘zero pads’. The daily pad count at three and six months post RARP was monitored to evaluate urinary continence recovery. Potency was defined as the capability to achieve and sustain satisfactory erections or firmness adequate for sexual activity or intercourse. Post RARP, a PSA assay was scheduled every 3 months for the initial 2 years, followed by assessments every 6 months for the subsequent 3 years, and annually thereafter. Biochemical recurrence (BCR) was defined as two consecutive PSA levels exceeding 0.2 ng/mL post RARP. Attainment of pentafecta status necessitated the absence of major perioperative complications (with only 90-day Clavien–Dindo complications (CDC) ≤ 3a considered), as well as negative surgical margins. Only patients meeting all these criteria were classified as having achieved pentafecta.
Statistical analysis
Categorical data were presented as proportions or percentages, whereas continuous data were reported as either means and median with interquartile ranges, as appropriate. Normality of the data was assessed using the Kolmogorov-Smirnov and Shapiro’s tests. For normally distributed data, the Student’s t-test was used to compare the means between the two groups. Non-parametric tests (Mann-Whitney U test or Kruskal-Wallis test) were used for skewed data. Qualitative variables were described in terms of frequency and proportion. The Chi-square test or Fisher’s exact test was used to compare categorical data, depending on its appropriateness.
To identify predictors of the pentafecta outcome, backward stepwise logistic regression analysis was performed under a threshold of p < 0.1 to select valuable predictive factors of pentafecta achievement in the training group and to record the odds ratio (OR) and 95% confidence interval (CI). The Akaike’s information criterion (AIC) was calculated and compared for each factor. We hypothesized that the model with the lowest AIC value and the fewest number of variables would be the final model. This analysis began with a full model and gradually eliminated non-significant variables, resulting in a reduced best-fit model. A nomogram was developed based on the aforementioned criteria and internally validated using bootstrapping with 500 replications, and the maximum area under the receiver operating characteristic (ROC) curve (AUC) and goodness of fit were assessed using the Hosmer-Lemeshow test. The nomogram was generated using the “RMS” package in the R program. ROC curves were used to evaluate the predictive ability of the developed pentafecta nomogram, and calibration plots were constructed to assess model calibration by comparing the observed and expected probabilities of the pentafecta. Calibration plots were also generated using the “RMS” package in the R program. All statistical tests were performed with R 4.3.0 (R Foundation for Statistical Computing, Vienna, Austria) with a two-sided significance level set at p < 0.05.
Nomogram development and validation
Nomograms were constructed based on the results of multivariable logistic regression analysis. The predictive accuracy of the nomogram was assessed using discrimination and calibration measures. Internal validation was performed using bootstrap 500 resampling techniques.
Results
A total of 1,752 patients were included in the analysis. The patient characteristics are presented in Table 1. The initial PSA value, biopsy Gleason score, biopsy technique, and other variables differed between patients with and without pentafecta achievement (all p < 0.05, except BMI), with a median age of 67 (IQR 63–71) years, median PSA level of 7.5 (IQR 5.5–10.7) ng/dL, and median BMI of 23.5 (IQR 21.8–25.5) kg/m². The D’Amico risk classification included 249 (14.2%) low-risk, 791 (45.1%) intermediate-risk, and 725 (41.4%) high-risk patients. A total of 290 patients (16.6%) achieved the pentafecta outcome.
Multivariable logistic regression analysis
Multivariate analysis revealed that bilateral nerve sparing was associated with a 10.36-fold (95% CI: 5.75–18.66) higher likelihood of achieving the pentafecta outcome compared to non-nerve sparing (p < 0.001). Preoperative potency and lower pathologic T stage (T1-2b) were also associated with higher likelihoods of achieving the pentafecta outcome, with OR of 66.63 (95% CI: 24.32–182.48) and 1.91 (95% CI: 0.58–6.25), respectively. (Table 2)
Nomogram
Based on the final model, we constructed nomograms to predict the pentafecta achievement of preoperative and postoperative factors. A nomogram was constructed to predict the likelihood of achieving a pentafecta outcome before and after RP based on perioperative clinical parameters.
Preoperative nomogram
The accuracy of the nomogram (Fig. 1), measured as the area under the receiver operating characteristic curve, showed good predictive accuracy. The calibration of the nomogram appeared to be excellent, with a C-index of 0.802 (95% CI 0.801–0.804) (Fig. 2).
Nomogram predicting the likelihood of attaining a pentafecta outcome before RP.
Calibration plot for the preoperative nomogram.
Postoperative nomogram
The accuracy of the nomogram (Fig. 3), measured as the area under the receiver operating characteristic curve, was 0.847, indicating excellent predictive accuracy. The nomogram calibration was excellent, with a C-index of 0.844 (95% CI 0.801–0.804) (Fig. 4).
Nomogram predicting the likelihood of attaining a pentafecta outcome after RP using postoperative factors.
Calibration plot for the postoperative nomogram.
The predictive accuracy of the nomograms was assessed using discrimination measures such as the AUC (Fig. 5) and calibration measures such as calibration plots.
ROC analysis of pentafecta achievement for the (purple) postoperative model and (red) preoperative model. The AUC of the postoperative scoring model developed in the study was greater than preoperative model. ROC, receiver operating characteristic; AUC, area under the curve.
Discussion
Localized PCa can be successfully treated with RP, which has a high success rate for disease-free survival after five years (up to 90%)3. Surgical and radiation therapies have shown equivalent oncological and functional results; therefore, the choice of treatment depends on the specifics of the patient.
Predicting favorable outcomes after surgical intervention is crucial for guiding treatment decisions. Several factors have been identified as predictive indicators across different patient populations and surgical methods (such as open or robotic procedures), leading to the development of trifecta and pentafecta outcomes as quality measures for assessing the effectiveness of RP outcomes.
To predict preoperative and postoperative pentafecta outcomes, we built useful and instructive nomograms that considered various aspects. The calibration plots showed significant concordance between the predicted and actual probabilities, and both nomograms displayed excellent fit statistics. The use of numerous variables in the regression analysis may raise concerns about overfitting; however, the application of Akaike’s Information Criterion (AIC) for model selection helps mitigate this risk by prioritizing model parsimony and predictive accuracy.Additionally, both models showed modest diagnostic accuracy in predicting pentafecta outcomes after RARP, as demonstrated by the AUC values of 0.807 and 0.847. Consequently, our models predicted the pentafecta outcomes with a reasonable level of accuracy.
For instance, Eastham et al. created a nomogram that included six factors, including age at RP, Gleason score, PSA level, clinical stage, and erectile function15. In patients with PCa who underwent RARP, Jazayeri et al. discovered that the Gleason score was the only predictor of trifecta and pentafecta outcomes12. Similarly, Patel et al. found that age was the only factor that could predict pentafecta results after RARP10. In a study by Novara et al., age and preoperative International Index of Erectile Function score were prognostic factors for trifecta results14. We found that serum PSA level, clinical stage, grade, and lymph node status were independent predictors of pentafecta outcomes, which is consistent with earlier investigations. In contrast to other studies, age at RP did not appear to be a feature in our prediction models because the univariate analysis revealed no statistically significant age difference between the two groups. Furthermore, according to our data, the Charlson Comorbidity Index (CCI) was a predictor of pentafecta outcomes after RARP. CCI has been shown to predict survival in some cancers, including PCa22. Our findings contribute to the growing corpus of research on factors that can predict RP outcomes, particularly in achieving the pentafecta. Clinicians may benefit from the compilation of nomograms and identification of relevant predictors in the formulation of treatment plans for patients with PCa undergoing RARP. Several notable characteristics distinguish our study from others23,24,25,26,27. Compared with previous studies, the rates of trifecta and pentafecta outcomes following RP in our study were notably lower (30.8%) during the median follow-up period of 21 months. This discrepancy can be attributed to the fact that the majority of patients in our series had high-risk and locally advanced disease, distinguishing them from the cohorts in the previously mentioned studies. In addition, we employed a stringent zero-pad criterion to assess urinary continence. Furthermore, as mentioned earlier, most patients in our series were sexually inactive, and baseline erectile function has been reported to be a predictor of trifecta outcomes. Given the lack of sexual activity at baseline in our patient cohort, we excluded potency outcomes from the originally proposed pentafecta outcomes. However, we acknowledge that sexual function is an essential aspect and one of the least satisfying parameters after RP. Also, it is noteworthy that our previous study demonstrated a substantial advantage in pentafecta achievement associated with nerve-sparing (NS) over non-nerve-sparing (non-NS) robot-assisted radical prostatectomy (RARP), underscoring the clinical significance of NS in optimizing outcomes in prostatectomy28. Limitations, the retrospective design may introduce selection bias and discussed its potential impact on results and conclusions.We recommended that future research incorporate preoperative planning for nerve-sparing (NS) surgery through surgeon questionnaires to enhance the understanding of decision-making processes and their impact on functional outcomes, thereby improving the predictive accuracy and clinical relevance of pentafecta models. Although Body Mass Index (BMI) showed no significant association with pentafecta outcomes in this study, its potential as a predictive factor warranted further exploration, particularly in the context of metabolic health and prostate cancer outcomes.
Challenges in defining functional outcomes, such as erectile dysfunction and incontinence, contributed to variability in reported results and should have been addressed in future studies. While robust internal validation methods, including bootstrapping, were applied, the lack of external validation limited the generalizability of our findings, highlighting the need for multicenter studies to confirm the nomograms’ applicability across diverse populations.
In addition to quantitative measures like pentafecta outcomes, future research should have incorporated patient-reported outcome measures to assess satisfaction and quality of life after RARP, providing a more comprehensive evaluation of surgical success. Finally, the exclusion of long-term outcomes restricted insights into the durability of pentafecta results; extended follow-up studies were essential to evaluate the sustainability and long-term impact of these outcomes.”
Conclusion
Our study has successfully established and validated preoperative and postoperative nomograms designed to predict pentafecta achievement after RARP for localized PCa, presenting a significant advancement for clinical application. While both models demonstrated fair accuracy in forecasting pentafecta outcomes, it is worth noting that our operational prediction model stands as one of the most comprehensive in this domain. Despite certain limitations, the model exhibited satisfactory discrimination and calibration performances overall. Importantly, our findings indicate that a substantial majority of men undergoing RP have the potential to attain the pentafecta status. Our developed nomogram, leveraging individualized pre-treatment and post-treatment data, provides a valuable tool for men to assess their likelihood of achieving an excellent outcome following RP, thereby offering crucial insights for clinical practice and informed treatment decisions.
Data availability
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Sung, H. et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 71, 209–249 (2021).
Hamdy, F. C. et al. 10–year outcomes after monitoring, surgery, or radiotherapy for localized prostate cancer. N. Engl. J. Med. 375, 1415–1424 (2016).
Mottet, N. et al. EAU–ESTRO–SIOG guidelines on prostate cancer. Part 1: Screening, diagnosis, and local treatment with curative intent. Eur. Urol. 71, 618–629 (2017).
van Poppel, H., Everaerts, W., Tosco, L. & Joniau, S. Open and robotic radical prostatectomy. Asian J. Urol. 6, 125–128 (2019).
Singh, I. & Hemal, A. K. Robotic–assisted radical prostatectomy in 2010. Expert Rev. Anticancer Ther. 10, 671–682 (2010).
Brassetti, A. et al. Robotic surgery in urology: History from PROBOT® to HUGO™. Sensors (Basel). 23 (16), 7104 (2023).
Ragusa, A. et al. Safety and feasibility of three arms settings robot-assisted radical prostatectomy using the Hugo RAS system: Surgical set-up in a double-center large case series. World J. Urol. 42 (1), 517 (2024).
Borregales, L. D. et al. Trifecta’ after radical prostatectomy: Is there a standard definition? BJU Int. 112, 60–67 (2013).
Patel, V. R. et al. Critical review of ‘pentafecta’ outcomes after robot–assisted laparoscopic prostatectomy in high–volume centres. BJU Int. 108, 1007–1017 (2011).
Patel, V. R. et al. Pentafecta: A new concept for reporting outcomes of robot–assisted laparoscopic radical prostatectomy. Eur. Urol. 59, 702–707 (2011).
Inoue, S., Hieda, K., Hayashi, T., Teishima, J. & Matsubara, A. Longitudinal analysis of trifecta outcome in Japanese patients with prostate cancer following robot–assisted laparoscopic radical prostatectomy. World J. Urol. https://doi.org/10.1007/s00345-020-03515-2 (2020).
Jazayeri, S. B., Weissman, B. & Samadi, D. B. Outcomes following robotic–assisted laparoscopic prostatectomy: Pentafecta and Trifecta achievements. Minerva Urol. Nefrol. 70, 66–73 (2018).
Ou, Y. C. et al. Pentafecta outcomes of 230 cases of robotic–assisted radical prostatectomy with bilateral neurovascular bundle preservation. Anticancer Res. 35, 5007–5013 (2015).
Novara, G. et al. Trifecta outcomes after robot–assisted laparoscopic radical prostatectomy. BJU Int. 107, 100–104 (2011).
Eastham, J. A., Scardino, P. T. & Kattan, M. W. Predicting an optimal outcome after radical prostatectomy: The trifecta nomogram. J. Urol. 179, 2207–2210 (2008).
Cappelleri, J. C. & Rosen, R. C. The sexual Health Inventory for men (SHIM): A 5–year review of research and clinical experience. Int. J. Impot. Res. 17, 307–319 (2005).
D’Amico, A. V. et al. Biochemical outcome after radical prostatectomy, external beam radiation therapy, or interstitial radiation therapy for clinically localized prostate cancer. JAMA 280, 969–974 (1998).
Tamhankar, A. S., Patil, S. R., Ahluwalia, P. & Gautam, G. Does continuation of low–dose aspirin during robot–assisted radical prostatectomy compromise surgical outcomes? J. Endourol. 32, 852–858 (2018).
Batra, V. et al. Predictive factors for lymph node positivity in patients undergoing extended pelvic lymphadenectomy during robot assisted radical prostatectomy. Indian J. Urol. 31, 217–222 (2015).
Carbin, D. D., Tamhankar, A. S., Ahluwalia, P. & Gautam, G. Robot-assisted radical prostatectomy in Indian men of age 75 years and above: A propensity score-matched analysis. J. Robot Surg. 16 (4), 799–806 (2022).
Dindo, D., Demartines, N. & Clavien, P. A. Classification of surgical complications: A new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann. Surg. 240, 205–213 (2004).
Guzzo, T. J. et al. Prediction of mortality after radical prostatectomy by Charlson comorbidity index. Urology 76, 553–557 (2010).
Sallami, S. Predictive factors of urinary incontinence after radical prostatectomy: Systematic review. Tunis Med. 95, 229–235 (2017).
Shao, I. H., Chang, Y. H., Hou, C. M., Lin, Z. F. & Wu, C. T. Predictors of short–term and long–term incontinence after robot–assisted radical prostatectomy. J. Int. Med. Res. 46, 421–429 (2018).
Eastham, J. A. et al. Risk factors for urinary incontinence after radical prostatectomy. J. Urol. 156, 1707–1713 (1996).
Matsushita, K. et al. Preoperative predictive model of recovery of urinary continence after radical prostatectomy. BJU Int. 116, 577–583 (2015).
Novara, G. et al. Evaluating urinary continence and preoperative predictors of urinary continence after robot assisted laparoscopic radical prostatectomy. J. Urol. 184, 1028–1033 (2010).
Bejrananda, T. et al. Comparing pentafecta outcomes between nerve sparing and non nerve sparing robot-assisted radical prostatectomy in a propensity score-matched study. Sci. Rep. 13 (1), 15835 (2023).
Acknowledgements
We wish to thank Rie Hayakawa the assistance rendered during data collection. The authors sincerely thank the entire staff of our department for offering their assistance with the medical service and manuscript writing processes.
Funding
This study had no funding.
Author information
Authors and Affiliations
Contributions
Project development: TB, KT, DS, TM, KY, WN, MS, TN, MT, KZ, MI, HS, MS and RS. Clinical Information: TB, KT, DS, TM, KY, WN, MS, TN, MT, KZ, MI, HS, MS and RS. Basic research Information: TB, KT, DS, TM, KY, WN, MS, TN, MT, KZ, MI, HS, MS and RS. Manuscript writing/editing: TB and KT.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This study was approved by the Ethics Committee of the Fujita Health University Hospital (approval no. HM19-265). All procedures were performed in accordance with the ethical standards of the institutional and national research committees and the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all patients according to the local ethics policy for retrospective analysis of our own anonymised clinical data.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Bejrananda, T., Takahara, K., Sowanthip, D. et al. Development and validation of nomograms for predicting pentafecta outcomes before and after robot-assisted radical prostatectomy: a retrospective study. Sci Rep 15, 2079 (2025). https://doi.org/10.1038/s41598-025-86120-w
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-86120-w