Abstract
The rapid increase in metabolic syndrome (MetS) as a major public health problem may be attributed to changes in population behavior patterns in modern society, including nutritional habits and physical activity. Therefore, this study investigated the association between dietary diversity score (DDS) and adult metabolic syndrome. In this cross-sectional study, 9715 participants aged 35–70 years from the Rafsanjan Cohort Study (RCS) were included. Demographic, medical, and habitual histories were collected. DDS was calculated using a food frequency questionnaire (FFQ). All analyses were performed using Stata 14, with p-values < 0.05. Based on the DDS, subjects were divided into four groups (quartiles). The multivariate-adjusted model showed that the risk of MetS increased by 18% in the third quartile and by 25% in the fourth quartile (OR: 1.18; 98% CI: 1.02–1.36 and OR: 1.25; 98% CI: 1.06–1.48, respectively). Additionally, an increased risk of high serum triglyceride levels was observed in the third quartile (OR: 1.19; 98% CI: 1.05–1.35). The results suggest that there is a relationship between DDS and metabolic syndrome, although this relationship changed after adjusting for confounders.
Similar content being viewed by others
Introduction
Metabolic syndrome (MetS), a clustering of risk factors (central obesity, dyslipidemia, and hypertension)1, is a well-known condition in the causal pathway of cardiovascular disease (CVD). MetS has also been associated with a higher risk of other chronic diseases, such as cancer2and neurodegenerative diseases3. In recent years, the prevalence of MetS has increased worldwide to the point that presently it is considered a major public health problem4. Globally, studies have estimated MetS prevalence rates between 10% and 60%, depending on sex, age, and geographic location. In Asia, the rates generally fall within the range of 32.0–47.6%5. The prevalence of MetS in Iran is 21.1%6.
The rapid increase in MetS prevalence may be attributed to changes in population behavior patterns in modern society7. Previous reports have indicated that lifestyle including nutritional habits and physical activity are the most important independent risk factors for MetS. Among these patterns, diet plays an essential and independent role in the incidence and development of MetS8,9. The dietary diversity score (DDS) is an indicator for assessing diet by counting the number of major food groups consumed, reflecting overall dietary quality compared with the evaluation of single foods or nutrients10,11. Epidemiological studies have indicated that a higher DDS is intimately related to a healthier diet with adequate intake of all food groups, which may provide a wide range of macro- and micro nutrients12,13.
Especially for the Western-style diet high in fat and animal-based foods, a meta-analysis revealed that “Western” dietary patterns were significantly associated with increased MetS risk14. Over the past few decades, there has been a significant shift in Chinese dietary patterns and behaviors, with a move from a predominantly plant-based diet to a Western-style diet. The positive association between the Western dietary pattern and MetS could be attributed in part to the lower amounts of beneficial foods and nutrients that this pattern contains. Higher consumption of refined grains15,16. The review of multiple studies underlined that Mediterranean and plant-based dietary patterns—characterized by high diversity—were consistently linked to reduced MetS risk14. The dietary habits in Rafsanjan, with a focus on traditional, plant-based foods and local agricultural products, can promote a healthy dietary pattern that supports better DDS and potentially reduces the prevalence of MetS.
Some studies suggested that dietary diversity helps to consume more energy and increases the incidence of metabolic syndrome, but other studies indicated that dietary diversity is associated with adequate nutrient intake and reduces the incidence of disease17. No studies have yet explored the relationship between metabolic syndrome and dietary diversity in Rafsanjan city. Therefore, this study investigated the association of dietary diversity score with metabolic syndrome in adults in Rafsanjan.
Methods
Study population
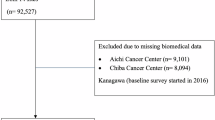
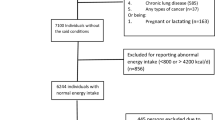
The sample size was 10,000 participants in the Rafsanjan Cohort Study (RCS)18, an arm of the Prospective Epidemiological Research Studies in Iran (PERSIAN). Participants aged 35–70 years residing in Rafsanjan and written informed consent were included in the study (9990). Participants were excluded for incomplete questionnaires regarding demographics, personal habits, dietary habits, and medical history, as well as for unperformed biochemical tests. A total of 9715 participants were considered (Fig. 1: Flow diagram of study participants). Rafsanjan, a city in southeast Iran, have been selected to enroll in this study18. All of the participants had completed questionnaires of demographical, medical, and habitual history. The protocol and questionnaires of this cross-sectional study were designed following the Persian cohort study protocols and under the supervision of the Iranian Ministry of Health and Medical Education (IMHME)19. The accuracy and precision of all methods were achieved using the relevant guidelines and regulations. Written informed consent was obtained from the participants. In addition, they were approved by the Ethics Committee of Rafsanjan University of Medical Sciences with the Ethical Code of IR.RUMS.REC.1400.111. All methods were carried out following the relevant guidelines and regulations.
Data collection
All of the selected participants had filled out the questionnaires approved by the Persian Cohort study under a standardized19. The questionnaires consisted of questions on demographical status (age, gender, education years, and socio-economic status (Wealth score index: WSI)), opium and alcohol consumption, smoking, physical activity (Metabolic equivalent of task: MET), blood pressure, body mass index (BMI), nutritional status, laboratory test, and history of disease. Blood pressure was measured twice for each participant from each arm. Anthropometric parameters including height, weight, and waist circumference were measured according to a standard protocol18. MET was calculated over 24 h using activity-specific MET values from a 22-item questionnaire. WSI was determined through multiple correspondence analysis (MCA) of participants’ economic and social characteristics, based on a 27-question survey18.
Blood samples were collected after 12 h of fasting from all participants. Fasting blood sugar (FBS), triglyceride (TG), and high-density lipoprotein cholesterol (HDL) were measured using Auto Analyzer (BT 1500 Biotechnica, Italy). The CBC assay was also performed using an alpha cell counter (Nihon Kohden, Tokyo, Japan). All experiments were performed in the Rafsanjan cohort laboratory. Physical activity was measured by 22 questions about total hours reported for activities in 24 h and mentioned as Metabolic Equivalent of Task (MET) calculated for 24 h19.
The nutritional status was measured for any subset of variables from the food frequency questionnaire (FFQ). Previous research in Iran has established the reliability and validity of the FFQ20. The socio-economic status (Wealth score index: WSI) was estimated by multiple correspondence analysis (MCA) of the economic variables. The metabolic syndrome prevalence was evaluated in participants according to Adult Treatment Panel III (ATP-III). Based on NCEP-ATP III, metabolic syndrome was defined as the presence of three or more of the following components:
(1) abdominal adiposity (WC ≥ 102 cm in men and ≥ 88 cm in women); (2) low serum HDL-Cholesterol (< 40 mg/dl for men and < 50 mg/dl for women); (3) high serum triglyceride levels (≥ 150 mg/dl); (4) Elevated blood pressure (≥ 130/85 mmHg); (5) abnormal glucose homeostasis (fasting plasma glucose level ≥ 100 mg/dl)21.
Using the 143-item validated FFQ mentioned above, we calculated an energy-adjusted DD score (DDS)22,23. It includes five food groups: Vegetables, fruits, cereals, dairy products, and protein food groups (legumes, meat, fish, eggs, and nuts), based on the food groups. According to Kant’s paper (1995): Foods were grouped into the different groups based on similarities in nutrient composition and uses in the diet. The dairy group was assigned all milk and milk products. The meat group included both animal and plant protein sources. The grain group included all grain products except cakes, pies, cookies, and pastries. The fruit group included all fresh, canned, frozen, dried fruits, fruit juices, and fruit drinks. The vegetable group included all raw, cooked, frozen, and canned vegetables. Food mixtures containing foods from various food groups, for example, mixed dishes with meat, grain, dairy, and vegetables such as lasagna were assigned to all the relevant food groups. Participants had to consume at least half a unit of each food group in a day to be considered a “consumer”. A maximum score of 2 is given to each of the five groups so that each participant receives a score from 0 to 10. To calculate the score of each group, the number of used subgroups is divided by the total number of subgroups in each main group and then multiplied by 2. The total scores of the five main groups were recorded as the total score.
Flow diagram of study participants.
Statistical analysis
To describe the data, frequency (percentage) and mean ± standard deviation were used for categorical variables and quantitative variables, respectively. The individuals’ baseline characteristics were compared between the groups of our study (quartiles of DDS) using a chi-square test (χ²) and a one-way analysis of variance for categorical and continuous variables, respectively. Cut-points for quartiles of DDS were calculated and subjects were categorized based on quartile cut-points: 1st: ≤1.43; 2nd = 1.44–1.89; 3rd = 1.90–2.39; and 4th = ≥ 2.40. In addition, we used binary logistic analysis to determine the odds ratios (ORs) and the corresponding 95% confidence intervals (CI) for the relationship between MetS and components of metabolic syndrome with quartile categories of dietary diversity score. Besides, we used crude and adjusted models in the regression analysis. Potential confounding parameters were recognized based on subject matter knowledge and relevant epidemiological literature. Next, they were entered into the models sequentially according to their hypothesized strengths of association with MetS and dietary diversity score. To reach this goal, separate models at the bivariate level were run to obtain variables associated with MetS and components of metabolic syndrome. Afterward, variables with a p-value < 0.2 were considered for Multivariate analysis. The baseline (crude) model was stratified based on quartile categories of dietary diversity score. The adjusted models 1 was adjusted for confounding variables, age, gender, education, WSI, smoking, Alcohol and opium consumption, physical activity, total energy intake, and total fat. The adjusted models 2 were adjusted for confounding variables in adjusted model 1 and BMI. All analyses were performed in Stata 14. All p-values were two-sided and p-values < 0.05 and 95% confidence intervals were considered statistically significant.
Results
A total of 9715 subjects who completed the nutrition questionnaire were included in this study. Based on the DDS, subjects were divided into 4 groups (quartiles). The admission characteristics of the four groups are described in Table 1. The mean and standard deviation age of participants in the first group (51.05 ± 9.74) was higher than the other three groups and this difference between them was significant (P < 0.001). The highest percentage of participants in the first and second groups were men and in the third and fourth groups were women (Table 1).
The average education, BMI, and WSI were significantly lower in the first and second groups than in the other groups. The highest percentage of obese people was in the third and fourth groups, and the highest percentage of normal people was in the first group, and this difference was significant (P < 0.001) (Table 1).
The highest average waist circumference was related to subjects of group 4 (96.60 ± 10.96) and this average had a significant difference between the groups (P < 0.001). Among the participants who consumed alcohol and cigarettes, the highest percentage of subjects were in the third and fourth groups (P < 0.001).
The crude model is stratified on the status of DDS.
The adjusted Model 1 is adjusted for confounding variables age, gender, education, WSI, smoking, Alcohol and opium consumption, physical activity, total energy intake, and total fat.
The adjusted model 2 is adjusted for confounding variables in adjusted model 1 and BMI.
P < 0.05 s, 3rd and 4th quartiles compared to the first quartile.
Table 4 shows the Multivariate-adjusted odds ratio for having metabolic syndrome and its features by quartile categories of DDS and DDS continues. The crude model is stratified on the status of DDS.
In adjust model 1, after adjusting confounders such as age, gender, education, WSI, smoking, alcohol and opium consumption, physical activity, total energy and total fat intake, it has been shown that the odds of metabolic syndrome increased 18% in the third group and 25% in the fourth group (OR: 1.18; 95% CI 1.02–1.36 for quartile 3 and OR: 1.25; 95% CI 1.06–1.48 for quartile 4 respectively). Also, an increase in the odds of high-serum triglyceride level was seen in the third group in adjusted model 1 (OR: 1.19; 95% CI 1.05–1.35). The odds of metabolic syndrome increased by about 20% by increasing DDS in adjusted model 1 (DDS continues: OR: 1.20; 95% CI 1.09–1.32).
A higher DDS (continues) was linked to an increased likelihood of abnormal glucose homeostasis (OR: 1.13; 95% CI 1.04–1.23) and high-serum triglyceride level (OR: 1.09; 95% CI 1.01–1.18). This correlation indicates that individuals with higher DDS may be at greater risk for metabolic disorders, potentially leading to type 2 diabetes. These findings highlight the need for early screening and intervention in those with significant dietary distress. Additionally, improving dietary habits could help stabilize blood sugar levels and enhance lipid profiles, ultimately lowering the overall risk of cardiovascular diseases (Table 4).
The adjusted model 2 was adjusted for confounding variables in adjusted model 1 and BMI. The results showed that there was no significant relationship between metabolic syndrome and its components with DDs score. This table showed that adjusted Model 3 incorporated all variables from adjusted Model 2, along with BMI, which was hypothesized as a potential mediator in the DDS–MetS relationship.
Discussion
The present cohort study revealed that DDS was associated with the risk of incident MetS inversely but after adjustment for some confounders such as age, gender, education, WSI, smoking, alcohol and opium consumption, and physical activity, total energy intake and total fat intake, the risk of MetS increased in third quartile (18%) and fourth quartile (24%), and after adjusting of BMI, there wasn’t any correlation between DDS and MetS.
Several potential biological mechanisms have been suggested to explain the association between DDS and the risk of MetS or its components. It has been noted that a greater proportion of the energy intake was contributed by the carbohydrate intake in Asians24. Previous studies proposed higher carbohydrate intakes, have been caused by increased visceral adiposity, and the hepatic de novo lipogenesis upregulating25and related to the prevalence of MetS and its components26. Foods including refined grain that are quickly digested in the gut, have a high glycemic index (GI), that may affect appetite and increase body fat storage and weight gain27. A cross-sectional study showed that a higher dietary GI was associated with the risk of abdominal obesity28. Also, in an Asian-Indian population, a high intake of refined grains was associated with elevated triglyceride and fasting blood glucose levels29.
Some studies found an inverse association between DDS and Mets. In a prospective cohort study among Korean adults aged 40–60 years with a 12 years follow-up, DDS had an inverse association with MetS and its features in men despite women30.Also a cross-sectional study was conducted on 581 healthy adults in Tehran, indicated an inverse correlation with MetS and its components31. DDS is a good indicator for assessing nutrients intake adequacy, quality of diet and relationship between diet and diseases32,33,34. Previous studies have revealed that a more DDS is related to adequate intake of food groups and a healthier diet13,35. However, the association between DDS and Mets depended on the groups of intake foods. Higher DDS may be due to an increase in intake of carbohydrates and refined sweets that is related to obesity and Mets. On the other hand, higher DDS may be related to increasing consumption of vegetables that can reduce obesity and Mets36. Therefore, the components of intake foods are very important to predict the effect of DDS on Mets.
In the present study, after adjusting the confounders, the relationship between DDS and Mets in the third and fourth quartiles was direct. In comparison to other studies, DDS in this study was lower30,31,32, that may be due to differences in DDS determining methods or cultural influence on food intake. For example, the traditional dietary pattern in Iran is refined grain, eggs, potatoes, nuts, vegetables, hydrogenated fats and legumes37. But in China, Korea and Japan (Eastern Asian countries) is kimchi, soybean, seafood, vegetables, fruits and mushrooms14.
On the other hand, due to lower DDS, the consumption of useful foods such as fruits, vegetables and fiber has decreased, in addition to the increase of some components of MetS such as triglycerides, blood pressure and fasting blood sugar in subjects cause beneficial changes in the diet and can distort the relationship between DDS and MetS, and therefore the existence of these confounding factors can increase the consumption of healthy food, which is related to the increase of DDS.
This study indicated no association between glucose hemostasis and risk of Mets after adjusting of some confounders. But in adjusted model 1 indicated increased risk of Mets. In contrast, previous studies showed that higher DDS was associated with decreased abnormal glucose hemostasis31,38. However In the current study, consistent with some studies, there was a direct association between DDS and BMI. Previous studies showed when DDS increased, the intake percentage of most food groups was increased that may be cause excess energy intake and increasing BMI39,40. In other study, Mexican men with a more DDS had a higher intake of fat and energy and so overweight41.
In present study, higher DDS associated with excess energy and fat intake. Of course excess energy and total fat may be due to increased consumption of healthy items such as of vegetable oil and whole grain that, there are useful component such as fiber, antioxidants and phytochemicals42,43. In the other hand, contrast with the current study, some studies have showed an inverse association between DDS and BMI17,31. A meta-analysis study of observational studies indicated no relationship between BMI and DDS44. The contradiction in the studies may be related to the type of study conducted, the method of evaluating and determining food diversity, differences in the input or output of some food items and the indicators related to its groups and subgroups that may affect the findings.
In our results, in line with some studies45,46, men consume higher varied diets than women. In some studies, there is no relationship between DDS and gender47,48, and in Cano-Ibáñez et al. study, contrary to our results, the variety of food in women was more than that of men49. Mood and stress, appetite and genetics are included, and even customs and traditions and culture of each region can have a great impact on food diversity46. For example, the environment under our study is located in an area that uses more traditional foods such as stews and refined grain, which is cooked in a traditional way and can affect people’s dietary diversity, as well as traditional sweets that contain a lot of saturated fat and Sugar that is a factor in increasing the incidence of overweight and chronic diseases such as metabolic syndrome50,51,52,53.
In this study, in line with previous studies54,55,56, the relationship between education and DDS was direct, so it can be concluded that as the level of education and awareness increases, attention to food diversity and healthy food consumption increases. Low education can reduce people’s ability to learn nutritional knowledge and understanding. Also, studying more increases in people with higher education, so nutritional awareness may increase in people with higher education55.
Our study has some limitations. We adjusted the potential confounders but there may be residue confounders that didn’t adjust and might affect the Mets risk. Also, the cross-sectional nature of this study cannot establish causal relationships. Additionally, since the FFQ relies on memory, recall bias may occur. However, this study has some strengths such as a large sample size. On the other hand, FFQ was used to assessment of dietary consumption. FFQ may be better for calculating DDS with other tools such as recalls or food records. Analyzing food diversity in each person can help increase the quality of food by increasing the consumption of useful food groups, but according to the results of the studies, it is better to look at the DDS tools and groups, and subgroups based on quality, method of processing and the presence of nutrients in them. Longitudinal and qualitative studies are needed in the future to establish temporal relationships and to understand dietary behaviors contributing to higher DDS and Mets risk. Qualitative studies are suggested to explore dietary behaviors linked to a higher risk of DDS and MetS.
Conclusions
Our findings showed that there is a relationship between DDS and metabolic syndrome, although this relationship has changed after adjusting for confounders, due to the existence of contradictions in the results of different studies, there is a need to review the DDS tool and conduct longitudinal and qualitative studies to confirm our finding.
Data availability
Sequence data supporting this study’s findings have been deposited in the Persian Adult Cohort Study Center, Rafsanjan University of Medical Sciences, Iran. The data is not available publicly. However, the data can be obtained from the corresponding author upon a reasonable request by Email: adilinatlos@gmail.com.
References
DeBoer, M. D. et al. Independent associations between metabolic syndrome severity and future coronary heart disease by sex and race. J. Am. Coll. Cardiol. 69, 1204–1205 (2017).
Micucci, C., Valli, D., Matacchione, G. & Catalano, A. Current perspectives between metabolic syndrome and cancer. Oncotarget 7, 38959 (2016).
Zhang, P. & Tian, B. Metabolic syndrome: an important risk factor for Parkinson’s disease. Oxidative medicine and cellular longevity 2014 (2014).
O’Neill, S. & O’Driscoll, L. Metabolic syndrome: a closer look at the growing epidemic and its associated pathologies. Obes. Rev. 16, 1–12 (2015).
Aryal, N. & Wasti, S. P. The prevalence of metabolic syndrome in South Asia: a systematic review. Int. J. Diabetes Developing Ctries. 36, 255–262 (2016).
Mazloomzadeh, S., Khazaghi, Z. R. & Mousavinasab, N. The prevalence of metabolic syndrome in Iran: a systematic review and meta-analysis. Iran. J. Public. Health. 47, 473 (2018).
Xu, H., Li, X., Adams, H., Kubena, K. & Guo, S. Etiology of metabolic syndrome and dietary intervention. Int. J. Mol. Sci. 20, 128 (2018).
Song, P., Yu, J., Chang, X., Wang, M. & An, L. Prevalence and correlates of metabolic syndrome in Chinese children: the China Health and Nutrition Survey. Nutrients 9, 79 (2017).
Hosseini, Z., Whiting, S. J. & Vatanparast, H. Current evidence on the association of the metabolic syndrome and dietary patterns in a global perspective. Nutr. Res. Rev. 29, 152–162 (2016).
Qorbani, M. et al. Dietary diversity score and cardio-metabolic risk factors: an updated systematic review and meta-analysis. Eat. Weight Disorders-Studies Anorexia Bulimia Obes., 1–16 (2021).
Patterson, R. E., Haines, P. S. & Popkin, B. M. Diet quality index: capturing a multidimensional behavior. J. Am. Diet. Assoc. 94, 57–64 (1994).
Hatløy, A., Torheim, L. E. & Oshaug, A. Food variety—a good indicator of nutritional adequacy of the diet? A case study from an urban area in Mali, West Africa. Eur. J. Clin. Nutr. 52, 891–898 (1998).
Steyn, N. P., Nel, J. H., Nantel, G., Kennedy, G. & Labadarios, D. Food variety and dietary diversity scores in children: are they good indicators of dietary adequacy? Public Health. Nutr. 9, 644–650 (2006).
Fabiani, R., Naldini, G. & Chiavarini, M. Dietary patterns and metabolic syndrome in adult subjects: a systematic review and meta-analysis. Nutrients 11, 2056 (2019).
Sahyoun, N. R., Jacques, P. F., Zhang, X. L., Juan, W. & McKeown, N. M. Whole-grain intake is inversely associated with the metabolic syndrome and mortality in older adults. Am. J. Clin. Nutr. 83, 124–131 (2006).
Esmaillzadeh, A. et al. Fruit and vegetable intakes, C-reactive protein, and the metabolic syndrome. Am. J. Clin. Nutr. 84, 1489–1497 (2006).
Azadbakht, L. & Esmaillzadeh, A. Dietary diversity score is related to obesity and abdominal adiposity among Iranian female youth. Public Health. Nutr. 14, 62–69 (2011).
Hakimi, H. et al. The profile of Rafsanjan cohort study. Eur. J. Epidemiol. 36, 243–252 (2021).
Poustchi, H. et al. Prospective epidemiological research studies in Iran (the PERSIAN Cohort Study): rationale, objectives, and design. Am. J. Epidemiol. 187, 647–655 (2018).
Mirmiran, P., Esfahani, F. H., Mehrabi, Y., Hedayati, M. & Azizi, F. Reliability and relative validity of an FFQ for nutrients in the Tehran lipid and glucose study. Public Health. Nutr. 13, 654–662 (2010).
Bahar, A. et al. Prevalence of metabolic syndrome using international diabetes federation, National Cholesterol Education Panel-Adult Treatment Panel III and Iranian criteria: results of Tabari cohort study. J. Diabetes Metabolic Disorders. 19, 205–211 (2020).
Kant, A. K., Schatzkin, A., Harris, T. B., Ziegler, R. G. & Block, G. Dietary diversity and subsequent mortality in the first national health and nutrition examination survey epidemiologic follow-up study. Am. J. Clin. Nutr. 57, 434–440 (1993).
Farhangi, M. A. & Jahangiry, L. Dietary diversity score is associated with cardiovascular risk factors and serum adiponectin concentrations in patients with metabolic syndrome. BMC Cardiovasc. Disord. 18, 1–6 (2018).
Shi, J. et al. Nutrient patterns and its association and metabolic syndrome among Chinese children and adolescents aged 7–17. Nutrients 15, 117 (2022).
Teff, K. L. et al. Endocrine and metabolic effects of consuming fructose-and glucose-sweetened beverages with meals in obese men and women: influence of insulin resistance on plasma triglyceride responses. J. Clin. Endocrinol. Metabolism. 94, 1562–1569 (2009).
Song, S., Lee, J. E., Song, W. O., Paik, H. Y. & Song, Y. Carbohydrate intake and refined-grain consumption are associated with metabolic syndrome in the Korean adult population. J. Acad. Nutr. Dietetics. 114, 54–62 (2014).
Brand-Miller, J. C., Holt, S. H., Pawlak, D. B. & McMillan, J. Glycemic index and obesity. Am. J. Clin. Nutr. 76, 281S–285S (2002).
Salari-Moghaddam, A., Keshteli, A. H., Haghighatdoost, F., Esmaillzadeh, A. & Adibi, P. Dietary glycemic index and glycemic load in relation to general obesity and central adiposity among adults. Clin. Nutr. 38, 2936–2942 (2019).
Radhika, G., Van Dam, R. M., Sudha, V., Ganesan, A. & Mohan, V. Refined grain consumption and the metabolic syndrome in urban Asian indians (Chennai Urban Rural Epidemiology Study 57). Metabolism 58, 675–681 (2009).
Kim, J. et al. Association between Dietary Diversity score and metabolic syndrome in Korean adults: A Community-based prospective cohort study. Nutrients 14, 5298 (2022).
Azadbakht, L., Mirmiran, P. & Azizi, F. Dietary diversity score is favorably associated with the metabolic syndrome in tehranian adults. Int. J. Obes. 29, 1361–1367 (2005).
Azadbakht, L., Mirmiran, P., Esmaillzadeh, A. & Azizi, F. Dietary diversity score and cardiovascular risk factors in tehranian adults. Public Health. Nutr. 9, 728–736 (2006).
Mirmiran, P., Azadbakht, L., Esmaillzadeh, A. & Azizi, F. Dietary diversity score in adolescents-a good indicator of the nutritional adequacy of diets: Tehran lipid and glucose study. Asia Pac. J. Clin. Nutr. 13, 56–60 (2004).
Drewnowski, A., Renderson, S. A., Driscoll, A. & Rolls, B. J. The Dietary Variety score: assessing diet quality in healthy young and older adults. J. Am. Diet. Assoc. 97, 266–271 (1997).
Habte, T. Y. & Krawinkel, M. Dietary diversity score: a measure of nutritional adequacy or an indicator of healthy diet? (2016).
Khamoushi, A., Mohammadi Sartang, M., Mazloom, Z. & Akbarzadeh, M. Dietary diversity and abdominal obesity among female students of Shiraz University of Medical Sciences, Shiraz, Iran. Int. J. Nutr. Sci. 5, 79–83 (2020).
Falahi, E., Anbari, K., Ebrahimzadeh, F. & Roosta, S. Dietary patterns associated with metabolic syndrome: the Khorramabad Study. J. Nutr. Food Secur. 2, 201–212 (2017).
Gholizadeh, F. et al. The relation of dietary diversity score and food insecurity to metabolic syndrome features and glucose level among pre-diabetes subjects. Prim. Care Diabetes. 12, 338–344 (2018).
Jayawardena, R. et al. High dietary diversity is associated with obesity in Sri Lankan adults: an evaluation of three dietary scores. BMC Public. Health. 13, 1–8 (2013).
Karimbeiki, R. et al. Higher dietary diversity score is associated with obesity: a case–control study. Public. Health. 157, 127–134 (2018).
Ponce, X., Ramirez, E. & Delisle, H. A more diversified diet among Mexican men may also be more atherogenic. J. Nutr. 136, 2921–2927 (2006).
Khairnar, S. J., Rudrapal, M., Ahire, E. D., Jagtap, M. R. & Kshirsagar, S. J. Overview of Functional Foods. in Applications of Functional Foods in Disease Prevention 1–31Apple Academic Press, (2024).
Agrawal, R., Ranveer, R., Rathod, N. & Nirmal, N. P. Phytochemicals as bioactive ingredients for functional foods. in Recent Frontiers of Phytochemicals 95–108Elsevier, (2023).
Salehi-Abargouei, A., Akbari, F., Bellissimo, N. & Azadbakht, L. Dietary diversity score and obesity: a systematic review and meta-analysis of observational studies. Eur. J. Clin. Nutr. 70, 1–9 (2016).
Gómez, G. et al. Diet quality and diet diversity in eight latin American countries: results from the Latin American Study of Nutrition and Health (ELANS). Nutrients 11, 1605 (2019).
Marla, K. S. & Padmaja, R. Analyzing gender differentials in dietary diversity across urban and peri-urban areas of Hyderabad, India. BMC Nutr. 9, 1–10 (2023).
Zhang, J. & Zhao, A. Dietary diversity and healthy aging: a prospective study. Nutrients 13, 1787 (2021).
Tian, X., Xu, X., Zhang, K. & Wang, H. Gender difference of metabolic syndrome and its association with dietary diversity at different ages. Oncotarget 8, 73568 (2017).
Cano-Ibáñez, N. et al. Dietary diversity and nutritional adequacy among an older Spanish population with metabolic syndrome in the PREDIMED-plus study: a cross-sectional analysis. Nutrients 11, 958 (2019).
Guimarães, V. H. D. et al. Comparative study of dietary fat: lard and sugar as a better obesity and metabolic syndrome mice model. Arch. Physiol. Biochem. 129, 449–459 (2023).
Nikniaz, L. et al. Nutrient pattern analysis of mineral based, simple sugar based, and fat based diets and risk of metabolic syndrome: a comparative nutrient panel. BMC Endocr. Disorders. 22, 1–13 (2022).
Clifton, P. Metabolic syndrome—role of dietary fat type and quantity. Nutrients 11, 1438 (2019).
Harrison, S., Couture, P. & Lamarche, B. Diet quality, saturated fat and metabolic syndrome. Nutrients 12, 3232 (2020).
Hiza, H. A., Casavale, K. O., Guenther, P. M. & Davis, C. A. Diet quality of americans differs by age, sex, race/ethnicity, income, and education level. J. Acad. Nutr. Dietetics. 113, 297–306 (2013).
O’Meara, L., Williams, S. L., Hickes, D. & Brown, P. Predictors of dietary diversity of indigenous food-producing households in rural Fiji. Nutrients 11, 1629 (2019).
Wilcox, S., Sharpe, P. A., Liese, A. D., Dunn, C. G. & Hutto, B. Socioeconomic factors associated with diet quality and meeting dietary guidelines in disadvantaged neighborhoods in the Southeast United States. Ethn. Health. 25, 1115–1131 (2020).
Funding
The Iranian Ministry of Health and Medical Education has contributed to the funding used in the PERSIAN Cohort through Grant No. 700/534. This study has also been supported by the Vice Chancellery for Research & Technology of Rafsanjan University of Medical Sciences. The context of this article is the views of the authors and the funder had no role in the design of the study and collection, analysis, and interpretation of data, the decision to publish, and the writing of the manuscript.
Author information
Authors and Affiliations
Contributions
Sh.H. contributed to the design of the study and drafting of the manuscript; P.K. contributed to the design of the study and statistical analysis. F.A collected the data and prepared tables. M.K & M.GH contributed to the drafting of the manuscript. L.S contributed to the design of the study and critical review of the draft manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Heidari, S., Kahnooji, M., Ayoobi, F. et al. Relationship between metabolic syndrome and dietary diversity in the Rafsanjan cohort study. Sci Rep 15, 10579 (2025). https://doi.org/10.1038/s41598-025-90086-0
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-90086-0