Abstract
Follow-up care in adult childhood cancer survivors (ACCS) aims to screen for, prevent, and treat potential late effects. The trajectory of ACCS’ health-related quality of life (HRQoL) attending follow-up care is unclear. We investigated changes in HRQoL of ACCS attending a follow-up care program. The primary outcome was the minimal clinically important decrease (MCID) in HRQoL of ≥ 5 points in the mental (MCS) and/or physical component score (PCS) of the 36-item Short Form (SF-36) between baseline and follow-up (3-months after the first visit). We compared baseline characteristics, psychological factors, satisfaction, and distress (measured using the Brief Symptom Inventory). In 47 ACCS (100%), no significant change in the overall median MCS and PCS was observed. In 14 ACCS (29.8%) a MCID in HRQoL was observed. Compared to ACCS without a MCID, they reported lower PCS (median 45.2 [31.7; 51.4] vs. 55.6 [46.1; 57.6], p = 0.007), a higher proportion of low physical health (PCS < 48; 71.4% vs. 27.3%, p = 0.009) and distress (50% vs. 18.8%, p = 0.030) at baseline. Satisfaction was high (94.9%). One in three ACCS experienced a clinically important decrease in HRQoL after follow-up care, with higher rates in those with lower physical health and higher psychological distress at baseline.
Similar content being viewed by others
Introduction
Over the past 30 years, childhood cancer survival rates have improved drastically and exceeded 81% in most European countries for children diagnosed between 2010 and 20141. In Switzerland, survival rate exceeded 85% for children diagnosed between 2014 and 20182. Although overall survival is high, most adult childhood cancer survivors (ACCS) experienced late effects due to the cancer or its treatments3,4,5. Chronic health conditions occurred earlier and more frequently in ACCS compared to peers of the same age groups3,4,5. Psychological distress, fear of cancer recurrence, anxiety, and depressive symptoms were present in ACCS4,6,7,8. They resulted in a high burden of disease during adulthood and may affect health-related quality of life (HRQoL)4,9. Long-term follow-up care aims to reduce the burden of late effects through early detection, treatment, and prevention3,10,11,12,13. Additionally, ACCS may need psychological support and lifestyle counselling3,6,9.
In ACCS who attended structured and tailored follow-up care more late effects were detected compared to ACCS who did not attend follow-up care12,14 or ACCS with follow-up care provided by primary care physicians12,15. The detected follow-up effects ranged from medical conditions such as osteoporosis, endocrinopathy and pulmonary disfunction to secondary malignancies and psychosocial late effect such as higher distress levels12,15. Follow-up care increased the awareness for potential late effects16 and reduced the number of emergency department visits and hospitalizations17. Thus, international guidelines recommend regular follow-up care that is personalized based on the initial cancer and its treatments18,19. Although follow-up care is intended to reassure ACCS and improve outcomes, some ACCS reported that follow-up care visits were associated with stress, anxiety, or fear of detecting new health problems20,21,22. Some ACCS discontinued follow-up care because they “wanted to draw a line under it”23. In a Swiss study, psychological distress persisted or newly occurred in 36% of participants after the follow-up care visit24. Psychological factors were associated with a decreased HRQoL in ACCS9,25,26. However, there is little research on the trajectory of quality of life, psychological variables, fear, and satisfaction in ACCS who attend a follow-up care program12.
Therefore, we aimed to (1) analyze the trajectory of HRQoL in ACCS from before to three months after the first visit in a follow-up care program, and to (2) describe and compare the baseline characteristics of ACCS with a clinically important decrease in HRQoL and ACCS without a MCID in HRQoL three months after the initial visit. Finally (3), we analyzed and report findings from individual feedback to follow-up care visits that may help to improve individualized follow-up care. We hypothesized that ACCS with a MCID in HRQoL have more late effects, experience more psychological distress, and report a lower HRQoL at baseline. We further hypothesized that ACCS with a MCID in HRQoL report lower satisfaction and increased fears and worries since the follow-up care visit.
Methods
Study design, eligibility criteria, and setting
This is a prospective multicenter cohort study of ACCS attending a follow-up care program at two Swiss hospitals (University Hospital Bern, Bern and Kantonsspital Baselland, Liestal). The study is reported following the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement27. The cohort study has been approved by the local ethical committees of North-Eastern Switzerland and Bern (EKNZ, Basec ID 2017 − 00109), and all participants provided informed consent. The study was performed in accordance with the regulations and guidelines of the ethical committee. The prospective cohort trial protocol was designed as a quality improvement project and not registered.
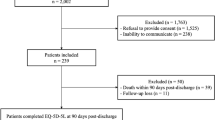
ACCS (≥ 18 years at consent, < 20 years at cancer diagnosis, see prior publication for details28) attending their first visit in a follow-up care program were asked to participate in a cohort study. For the current study, we included all ACCS who consented to the cohort study, attended the first follow-up care visit between February 2017 and May 2021, and completed the 36-item Short Form survey, version 2 (SF-36), at baseline and at three months follow-up. We excluded ACCS with multiple consultations between baseline and follow-up data collection and ACCS with missing baseline and/or follow-up data of the SF-36 (Supplementary Fig. 1).
The follow-up care visit was planned within an interdisciplinary team led by a physician specialized in general internal medicine and a pediatric oncologist. To ensure evidence-based follow-up care, the Passport for Care® application was used to personalize the Children’s Oncology Long-Term Follow-Up guidelines29.
Procedures
ACCS completed a consent form and baseline questionnaires (SF-36, Brief Symptom Inventory (BSI), demographic and cancer history-related questions) before their first visit in the follow-up care program. ACCS returned the questionnaires by postal mail or e-mail to the follow-up care team. Based on the questionnaires, the follow-up care visit was tailored to meet individual needs. During the follow-up care visit, physicians and specialized nurses collected medical history and physical findings. Further, laboratory tests and other examinations (e.g., echocardiogram) were performed based on the recommendations from the Children’s Oncology Long-Term Follow-Up guidelines and the patient’s history and findings. Approximately, three months after the follow-up care visit, ACCS received a follow-up questionnaire (SF-36, questions about worries, fear, satisfaction, and open-ended feedback questions; no BSI data was obtained three months after the visit) by e-mail or postal mail. Two reminders were sent to non-responders (the first after one month, the second after two months). A research fellow, not involved in the follow-up care visit, entered questionnaires, clinical information from medical reports, and test results into a database. We chose a 3-month follow-up to allow ACCS time to process the information provided during the clinical visit and still be able to provide valuable feedback regarding the clinical visit and their respective needs. The SF-36 items address domains in the preceding four weeks30 and thus, the chosen period represents an adequate distance between the clinical visit and the follow-up assessment.
Primary outcome
The primary outcome was the decrease in HRQoL between baseline and follow-up measured using the reliable and validated SF-3630,31,32,33. The SF-36 assesses eight subscales (physical functioning, physical role function, bodily pain, general health, vitality, social functioning, emotional role function, and mental health) and can be summarized in two summary scales (physical component summary (PCS), mental component summary (MCS). For each subscale, a score is calculated (higher scores indicate better HRQoL; range 0-100) and standardized to the Swiss general population normative data (mean = 50, SD = 10 in the Swiss general population)30,34. We calculated the change between baseline and follow-up in the MCS and PCS scores. A decrease of ≥ 5 points in MCS and/or PCS score from baseline to follow-up was considered a minimal clinically important decrease (MCID) in HRQoL. We compared ACCS with a MCID in HRQoL to ACCS with stable or increased HRQoL. Low physical HRQoL was defined as PCS T-score < 48 points and low mental HRQoL as MCS T-score < 35 points. We used these cut-off values because they have been derived and used in the Swiss Childhood Cancer Survivor Study31.
Additional outcomes
Additional outcomes included satisfaction, worries, and fear. Questions validated in an oncological population35 assessed satisfaction: “There were aspects of my overall visit with the doctor that I was not very satisfied with” and potential for improvement: “There were some things about my visit with the doctor that could have been better”. Answers on a four-point Likert scale (absolutely agree, agree, disagree, absolutely disagree) were dichotomized into “no unsatisfactory aspects”/”no potential for improvement” (absolutely disagree, disagree) and “some unsatisfactory aspects”/”some potential for improvement” (absolutely agree, agree). ACCS were asked to provide feedback to three open questions: “Could certain things have gone better during the consultation?”, “Have there been other topics that were discussed during the consultation?”, and “Open feedback”.
We asked about worries and fears using two questions: “Since the visit, I have been more worried about my health status than before” (worries) and “Since the visit, my fears are greater than before” (fear). Responses on a four-point Likert scale (absolutely agree, agree, disagree, absolutely disagree) were dichotomized into “yes” (absolutely agree, agree) or “no” (disagree, absolutely disagree).
Covariates
Baseline factors included socio-demographic characteristics (age, sex, Swiss / Non-Swiss, education, employment), cancer (based on the prevalence2,36 grouped into CNS tumor, leukemia, lymphoma, sarcoma, and others), age at diagnosis, year of the diagnosis, cancer related treatment (surgery, chemotherapy, and/or radiotherapy) and completion of the treatment, relapse of cancer, health conditions (chronic diseases and chronic medication use), and psychological variables.
Late effects were secondary malignancies, diseases per organ systems with the overall number of affected organ systems based on health records and chronic medication use as a proxy for cardiovascular disease (i.e., diuretics, nitrate, anticoagulant, antihypertensive, and statin use), diabetes (i.e., oral antidiabetics or insulin use), and endocrine disease (i.e., hydrocortisone, mineralocorticoid, desmopressin, and thyroid, sexual or growth hormones use).
Psychological baseline variables were based on the reliable and validated Brief Symptom Inventory (BSI)6,37,38. The BSI consists of 53 items and assesses nine subscales: somatization, obsessive-compulsive tendencies, interpersonal sensitivity, depression, anxiety, aggression, phobic anxiety, paranoid ideation, and psychotic tendencies. Each item expresses a statement on how much ACCS suffered from a problem described during the previous 7 days (scores range from 1 = not at all to 5 = very much). The Global Severity Index (GSI) measures general psychological distress, as it portrays the average of all subscale values (range 1–5). The values of the GSI and the subscales were converted to T-scores (higher scores indicating higher distress) using German normative data (mean = 50, SD = 10 in the German general population)37. Psychological distress was defined as GSI T-score ≥ 63 and/or a T-score ≥ 63 in at least two subscales37,38.
Statistical analysis
Descriptive statistics were used to characterize the study population. For continuous variables, we reported the median and interquartile range (IQR). For categorical variables, we reported proportions and frequencies. We compared baseline characteristics between groups using Wilcoxon rank-sum tests for continuous variables, and chi-square or Fisher’s exact tests for categorical variables, as appropriate39. We compared MCS, PCS and SF-36 subscales at baseline and follow-up using the sign-rank test40.
We analyzed free-text feedback according to qualitative content analysis by Mayring41, using QCAmap, an open access program42. Specific aspects of the free-text data were categorized into three main groups (positive feedback, negative feedback, and feedback without emotional connotation). The intra-coder agreement was assessed with a time difference of 60 days.
Missing data was reported in the tables. Missing values were handled according to the respective manuals for the scales: SF-36 User’s Manual30 and the BSI manual37. No further imputation was done. All statistical analyses were performed using STATA 16.0 IC software. Graphics were created using STATA 18.0 IC software (STATA Corp., College Station, TX, USA). All p-values < 0.05 were considered statistically significant. Because all analyses were exploratory, we refrained from adjusting for multiple testing.
Results
Study population and descriptive data
Out of 102 ACCS (100%) who provided informed consent for the cohort study, 47 ACCS (46.1%) met the eligibility criteria for this study and were analyzed (Supplementary Fig. 1). The median age was 25.7 years [IQR 21.3; 38.9], 66.0% were female, and 79.1% were employed (Table 1). The median age at cancer diagnosis was 9.0 years [4.2; 13.2] with a median time since diagnosis of 20.0 years [12.0; 29.0]. The main cancer groups were leukemia (n = 15, 31.9%), lymphoma (n = 11, 23.4%), CNS tumor (n = 9, 19.2%), sarcoma (n = 6, 12.8%), and others (n = 7, 14.8%; Langerhans cell histiocytosis n = 1, neuroblastoma n = 3, retinoblastoma n = 1, germ cell tumor n = 1, and renal tumor n = 1). ACCS reported a median of 5 [4; 8] late effects and the median time between the follow-up care visit and follow-up questionnaire was 132 days [100; 281].
The median MCS score at baseline was 52.5 [43.9; 56.4] and the median PCS score 51.4 [42.5; 56.9] with 8.5% reporting low mental HRQoL and 40.4% low physical HRQoL (Table 1). Baseline psychological distress was present in 28.3% of the overall population with a median GSI T-score of 48.5 [37; 63]. No difference between included and excluded ACCS in the baseline characteristics was observed except for SF-36 subscales for general health (median included 53.7 vs. excluded 46.8, p-value = 0.048) and emotional role functioning (56.4 vs. 52.1, p-value = 0.037) (Supplementary Table 1).
Primary outcome
In the overall group, the median MCS score at follow-up was 51.2 [42.3; 56.8] and the median PCS score was 50.4 [39.7; 57.7] (see Table 2 for SF-36 subscales). The changes between baseline and follow-up in the MCS was − 0.3 (IQR [− 3.4; 2.4], p = 0.882) and in the PCS − 0.2 (IQR [− 3.5; 3.0], p = 0.592; Supplementary Table 2). A total of 14 ACCS (29.8%) reported a MCID in HRQoL between baseline and follow-up (MCS n = 9 (19.2%), PCS n = 8 (17.0%), and in both n = 3 (6.4%)). In this group, the median MCS change was − 7.3 [− 10.7; − 0.5] and the median PCS change − 6.4 [− 11.4; 0.6] (Table 2). Compared to ACCS without a MCID in HRQoL, ACCS with a MCID in HRQoL reported particularly strong decreases in the SF-36 subscales for physical role functioning (median change − 10.6 [− 18.2; − 3.0] vs. 0 [0; 0], p < 0.001), general health (− 7.2 [− 11.5; 0] vs. 0 [− 4.6; 5.5], p = 0.004), social role functioning (− 6.2 [− 12.5; 0] vs. 0 [0; 0], p = 0.001), and emotional role functioning (− 6.5 [− 21.7; 0] vs. 0 [0; 4.3], p = 0.001) (Table 2).
Comparison of baseline characteristics in ACCS with and without MCID in HRQoL
Baseline socio-demographic and cancer-related characteristics were comparable in the two groups (Table 1). Whereas the MCS at baseline was comparable in both groups (Fig. 1a), ACCS with a MCID in HRQoL reported a lower physical HRQoL at baseline (PCS median 45.2 [31.7; 51.4] vs. 55.6 [46.1; 57.6], p = 0.007, Fig. 1b) and a higher proportion of low physical health (PCS < 48) (71.4% vs. 27.3%, p = 0.009). Significant differences in the SF-36 subscales at baseline were found in physical functioning (46.4 [40.5; 52.3] vs. 52.3 [49.3; 55.2], p = 0.037), bodily pain (41.3 [33.3; 41.3] vs. 59.8 [49.8; 59.8], p < 0.001) and social role functioning (44.6 [32.1; 57.1] vs. 57.1 [44.6; 57.1, p = 0.038) (Table 1).
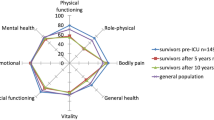
(a) Baseline mental HRQoL (MCS T-score) for the overall study population (n = 47), ACCS with a MCID in HRQoL (n = 14), and ACCS without a MCID in HRQoL (n = 33). MCID, Minimally clinically important decrease; HRQoL, Health Related Quality of Life; MCS, Mental Component Score; ACCS, Adult Childhood Cancer Survivors. Higher MCS values indicate better mental HRQoL. p = 0.340, Wilcoxon rank-sum test. (b) Baseline physical HRQoL (PCS T-score) for the overall study population (n = 47), ACCS with a MCID in HRQoL (n = 14), and ACCS without a MCID in HRQoL (n = 33), p = 0.007. MCID, Minimally clinically important decrease; HRQoL, Health Related Quality of Life; PCS, Physical Component Score; ACCS, Adult Childhood Cancer Survivors. Higher PCS values indicate better physical HRQoL. p = 0.007, Wilcoxon rank-sum test.
Psychological distress at baseline was present in a higher proportion of ACCS with a MCID in HRQoL (50% vs. 18.8%, p = 0.030; higher median GSI T-score (56 [52; 65] vs. 44 [35; 54], p = 0.008) compared to ACCS who did not experience a MCID in HRQoL (Table 1, Supplementary Fig. 2).
Additional outcomes
At follow-up, 94.9% of ACCS reported no aspects they were not satisfied with during the follow-up care visit and most ACCS (85.4%) reported no potential for improvement for the follow-up care visit. There was no difference between ACCS with and without a MCID in HRQoL. There was a trend, albeit not significant, towards more worries (53.9% vs. 21.7%, p = 0.061) and fear (38.5% vs. 16.0%, p = 0.229) in ACCS with a MCID in HRQoL compared to ACCS without a MCID (Supplementary Table 3).
Qualitative responses
In total, we analyzed 44 free text answers written by 29 ACCS (19 answers by ACCS with a MCID in HRQoL, 21 answers by ACCS without a MCID in HRQoL) with 49 positive and 25 negative aspects. Supplementary Table 4 provides a summary of the reported aspects. Strong emotional responses included “With the new knowledge […] I realize that the unconscious pressure to be “normal”, healthy, like everyone else, has become much smaller.” and “For me, the annual examinations are a horror, because I get very scared.” Further examples are provided in Supplementary Table 5. ACCS with a MCID in HRQoL provided more often free text answers and mentioned more positive aspects (gratitude, holistic view, and relief).
Discussion
This study analyzed the trajectory of HRQoL of 47 ACCS attending their first visit in a follow-up care program. Overall, mental and physical HRQoL showed no significant difference from before to three months after the visit. However, one-third of ACCS reported a MCID in HRQoL three months after the follow-up care visit. ACCS with a clinically important decrease in HRQoL, reported at baseline lower physical health scores, a higher proportion of low physical health and psychological distress compared to ACCS without a clinically important decrease in HRQoL. Despite their decrease in HRQoL, most ACCS were satisfied with the follow-up care visit. ACCS reported a wide variation in strong emotions related to the follow-up care visit which may be addressed by clinicians.
The underlying reasons for the varying trajectories in HRQoL and particularly the decrease in HRQoL among a third of the study population, remain unknown and warrant further studies. According to a systematic review published in 2017, only little is known about the psychosocial impact of follow-up care in ACCS12. Our study shows that one-third of ACCS attending the follow-up care program reported a clinically relevant decrease in HRQoL over the following three months. Whether this finding is a result of the follow-up care visit or occurs independently from the visit needs to be assessed in future studies. One may hypothesize that follow-up care visits might, although well intended, be associated with distress and anxiety. Previous studies showed, that the discussion and findings during the follow-up care visits may contribute to psychological distress among attendees by increasing nervousness, generating stress, and provoking fears of cancer recurrence and new late effects20,21,22,43. In adolescent childhood cancer survivors follow-up care visits were associated with a decrease in overall psychological distress24. However, one-third of survivors reported persistent psychological distress, and some adolescents reported new distress after the follow-up care visit. ACCS in our study reported strong emotions due to the re-experiencing of cancer-related memories when entering medical institutions or the thoughts about late effects that will persist or may develop. However, preexisting psychological factors and lower physical health may indicate that these ACCS are at risk of a further decline in HRQoL.
Preexisting psychological distress may also persist in some cancer survivors after a follow-up care visit24 and independently decrease HRQoL. In a U.S. childhood cancer survivor study, high psychological distress scores (measuring anxiety, depression, and somatization) were associated with lower HRQoL in all domains26. Psychological distress seems to coexist with low HRQoL25,44 and could independently lead to a further decrease in HRQoL. Compared to the Swiss population (high distress in 18.1%45) and the Swiss Childhood Cancer Survivor Study (high distress in 14.4%6 and 13%8), a higher proportion of ACCS in our study reported high psychological distress (28.3%) at baseline, which may also explain some of the observed decrease in HRQoL. Whether ACCS with more severe late effects13 and psychological distress46 are more likely to seek out follow-up care and therefore, are at risk for decreased HRQoL remains unknown. Thus, further studies should assess the causal pathways that result in these findings.
Although our study population was young (median age: 25.7 years), a median of five chronic late effects requiring medical care were reported. Childhood cancer survivors attending follow-up care programs were more likely to self-report late effects compared to survivors without follow-up care13. During follow-up care visits new late effects are frequently discovered12,15. New or persisting medical late effects negatively influence HRQoL31,47,48 and result in psychological distress6. In our study, we observed no difference in the number of late effects and chronic medication use between ACCS with and without a MCID in HRQoL. It is hypothesized that somatic late effects do not affect HRQoL per se but rather via high psychological distress26,33. American ACCS with a higher burden of chronic health conditions at baseline reported a lower HRQoL later on during the St. Jude Lifetime Cohort Study49. The timeframe of change, as well as any causal pathway, remains still unclear and warrants further research.
While both MCS and PCS assess HRQoL, they measure distinct aspects. Late effects and cancer experiences can influence both scales negatively, positively and not at all31,44,47. In the Swiss Childhood Cancer Survivor Study, all health problems reduced HRQoL across all scales, but the PCS was more affected31. Whereas no difference between the MCS in ACCS compared to their siblings was observed in the U.S., ACCS reported lower PCS scores47. Due to the small patient cohort, we were not able to compare differences between ACCS with a MCID in MCS to those with a MCID in the PCS. Future research in a larger cohort is warranted to explore the differences in health trajectories and baseline characteristics between these groups.
Only limited evidence is available on how to approach psychological and HRQoL related aspects during follow-up care. Studies suggest that identifying and addressing distress and aspects that affect quality of life may improve HRQoL over time24,50. Adolescent childhood cancer survivors perceived greater benefits from distress screening when their identified issues were discussed, compared to when the screened issues remained undiscussed24. One aspect observed in our study population showed that there may were unmet or unrealistic expectations. Although the follow-up care visit lasted a whole day in our setting, some answers indicate that expectations were not always met (missing answers, insufficient time, or a perceived lack of care after the follow-up care visit). Other studies also observed a need for more psychosocial support, information, and individualized content20,23,51,52. An unfulfilled information need is associated with higher psychological distress and lower HRQoL in ACCS52,53. Thus, providing information could mitigate distress following the follow-up care visit.
Overall, satisfaction with the follow-up care visit and the doctor encounter was high in our study and also in a study in pediatric cancer survivors50. A recent study from Geneva showed similar results as most ACCS perceived a follow-up care visit reassuring and satisfactory20.
Limitations
Although the study addresses an important topic, several limitations need to be discussed. First, the main limitation of our study is the small sample size, the short follow-up duration, and that we had no control group to compare ACCS with to those without follow-up care. The high proportion of baseline distress compared to previous studies suggest that a selected ACCS population with specific needs attended the follow-up care program. Thus, our findings may be limited to our program and not generalizable to other follow-up care settings and all ACCS. Second, a response rate of 46.1% indicates a substantial proportion of ACCS who did not or were not able to return a follow-up questionnaire. Although there were no relevant differences in the baseline characteristics between ACCS who completed the questionnaires and ACCS who did not, our findings may not be generalizable to all survivors attending the follow-up care program. Furthermore, our study was exploratory, and these findings warrant validation in other settings and with larger patient samples. Thus, we cannot infer causality. Finally, given the small patient cohort, we were not able to assess differences between ACCS with a MCID in the MCS compared to those with a MCID in the PCS. The MCS and the PCS are different health related quality of life outcomes. Thus, future studies need to assess differences between the two outcomes, the causal pathways on how HRQoL is influenced and what appropriate and effective preventive interventions are. Finally, ACCS completed baseline and follow-up questionnaires at different times before and after the follow-up care visit. Thus, recall bias and other factors may have influenced the results.
Implication for clinical practice
Low physical HRQoL and the presence of psychological distress at baseline may identify ACCS who are vulnerable to a MCID in HRQoL following the first clinical follow-up care visit in a follow-up care program. Clinicians need to be aware of psychological aspects that are associated with the attendance at follow-up care visits and eventually may influence HRQoL. The presence of low physical HRQoL and psychological distress may be modifiable factors that have been shown in other studies to influence HRQoL. In ACCS experiencing increased distress, inquiring about the reasons for their distress and discussing HRQoL problems may improve HRQoL trajectories and subjective well-being24,50.
Implication for research
Future studies should assess the causal pathways between distress, late effects and HRQoL in ACCS. Our findings need to be confirmed in a larger survivor population. A decrease in HRQoL over time has been observed in the American St. Jude Lifetime Cohort Study49 in ACCS with more somatic late effects. Thus, studies with longer follow-up duration should assess HRQoL trajectories in ACCS. Finally, future studies should focus on developing and implementing interventions aimed at reducing the potential negative impact of follow-up care visits on HRQoL in ACCS and subsequently evaluate their efficacy.
Conclusion
In ACCS attending a follow-up care visit, one in three ACCS reported a clinically relevant decrease in HRQoL from before to three months after the visit. ACCS with a clinically important decrease in HRQoL reported lower physical health and higher psychological distress at baseline. These ACCS may profit from being flagged for extra care. The causal pathway between a decrease in HRQoL after a follow-up care visit and low physical health and high psychological distress at baseline, however, is still unknown and warrants further investigation.
Data availability
Data privacy laws apply. The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Botta, L. et al. Long-term survival and cure fraction estimates for childhood cancer in Europe (EUROCARE-6): Results from a population-based study. Lancet Oncol. https://doi.org/10.1016/S1470-2045(22)00637-4 (2022).
Pasquale et al. Schweizerischer Krebsbericht 2021 (Bundesamt für Statistik, 2022).
Oeffinger, K. C. et al. Chronic health conditions in adult survivors of childhood cancer. N Engl. J. Med. 355 (15), 1572–1582. https://doi.org/10.1056/NEJMsa060185 (2006).
Geenen, M. M. et al. Medical assessment of adverse health outcomes in long-term survivors of childhood cancer. JAMA 297 (24), 2705–2715. https://doi.org/10.1001/jama.297.24.2705 (2007).
Bhakta, N. et al. The cumulative burden of surviving childhood cancer: An initial report from the St Jude lifetime cohort study (SJLIFE). Lancet 390 (10112), 2569–2582. https://doi.org/10.1016/S0140-6736(17)31610-0 (2017).
Michel, G. et al. Psychological distress in adult survivors of childhood cancer: The Swiss childhood cancer survivor study. J. Clin. Oncol. 28 (10), 1740–1748. https://doi.org/10.1200/JCO.2009.23.4534 (2010).
Cupit-Link, M., Syrjala, K. L. & Hashmi, S. K. Damocles’ syndrome revisited: Update on the fear of cancer recurrence in the complex world of today’s treatments and survivorship. Hematol. Oncol. Stem Cell. Ther. 11 (3), 129–134. https://doi.org/10.1016/j.hemonc.2018.01.005 (2018).
Gianinazzi, M. E. et al. Adolescent survivors of childhood cancer: Are they vulnerable for psychological distress? Psychooncology 22 (9), 2051–2058. https://doi.org/10.1002/pon.3249 (2013).
Michel, G. et al. Quality of life, and neurocognitive functioning in survivors of childhood cancer and their parents. Pediatr. Clin. North. Am. 67 (6), 1103–1134. https://doi.org/10.1016/j.pcl.2020.07.005 (2020).
Otth, M. et al. Cancer knowledge and health-consciousness in childhood cancer survivors following transition into adult care-results from the ACCS project. Front. Oncol. 12, 946281. https://doi.org/10.3389/fonc.2022.946281 (2022).
Schindler, M. et al. Cause-specific long-term mortality in survivors of childhood cancer in Switzerland: A population-based study. Int. J. Cancer. 139 (2), 322–333. https://doi.org/10.1002/ijc.30080 (2016).
Signorelli, C. et al. The impact of long-term follow-up care for childhood cancer survivors: A systematic review. Crit. Rev. Oncol. Hematol. 114, 131–138. https://doi.org/10.1016/j.critrevonc.2017.04.007 (2017).
Rebholz, C. E. et al. Follow-up care amongst long-term childhood cancer survivors: A report from the Swiss childhood cancer survivor study. Eur. J. Cancer 47 (2), 221–229. https://doi.org/10.1016/j.ejca.2010.09.017 (2011).
Ford, J. S., Chou, J. F. & Sklar, C. A. Attendance at a survivorship clinic: Impact on knowledge and psychosocial adjustment. J. Cancer Surviv. 7 (4), 535–543. https://doi.org/10.1007/s11764-013-0291-9 (2013).
Staba Hogan, M. J., Ma, X. & Kadan-Lottick, N. S. New health conditions identified at a regional childhood cancer survivor clinic visit. Pediatr. Blood Cancer. 60 (4), 682–687. https://doi.org/10.1002/pbc.24360 (2013).
Landier, W. et al. Impact of tailored education on awareness of personal risk for therapy-related complications among childhood cancer survivors. J. Clin. Oncol. 33 (33), 3887–3893. https://doi.org/10.1200/JCO.2015.62.7562 (2015).
Sutradhar, R. et al. Specialized survivor clinic attendance is associated with decreased rates of emergency department visits in adult survivors of childhood cancer. Cancer 121 (24), 4389–4397. https://doi.org/10.1002/cncr.29679 (2015).
Children’s Oncology Group. Long-Term Follow-Up Guidelines for Survivors of Childhood, Adolescent, and Young Adult Cancers Version 5.0. October (2018). http://www.survivorshipguidelines.org. Accessed 17 Nov 2022.
Michel, G. et al. Evidence-based recommendations for the organization of long-term follow-up care for childhood and adolescent cancer survivors: A report from the pancaresurfup guidelines working group. J. Cancer Surviv. 13 (5), 759–772. https://doi.org/10.1007/s11764-019-00795-5 (2019).
Babecoff, S. et al. Long-term follow-up for childhood cancer survivors: The Geneva experience. Swiss Med. Wkly. 152, w30153. https://doi.org/10.4414/smw.2022.w30153 (2022).
Michel, G. et al. Can health beliefs help in explaining attendance to follow-up care? The Swiss childhood cancer survivor study. Psychooncology 20 (10), 1034–1043. https://doi.org/10.1002/pon.1823 (2011).
Baughan, C. A. et al. Follow-up in stage I cutaneous malignant melanoma: An audit. Clin. Oncol. (R Coll. Radiol.) 5 (3), 174–180. https://doi.org/10.1016/s0936-6555(05)80321-8 (1993).
Earle, E. A. et al. Follow-up care for childhood cancer survivors: A focus group analysis. Eur. J. Cancer 41 (18), 2882–2886. https://doi.org/10.1016/j.ejca.2005.08.028 (2005).
Harju, E. et al. Psychological distress in survivors of childhood cancer and their parents before and after a follow-up appointment: The need for screening and validation of the emotion thermometer. J. Psychos. Oncol. Res. Pract. 5 (2). https://doi.org/10.1097/or9.0000000000000097 (2023).
de Beurs, E., Carlier, I. & van Hemert, A. Psychopathology and health-related quality of life as patient-reported treatment outcomes: Evaluation of concordance between the brief symptom inventory (BSI) and the short form-36 (SF-36) in psychiatric outpatients. Qual. Life Res. 31 (5), 1461–1471. https://doi.org/10.1007/s11136-021-03019-5 (2022).
Huang, I. C. et al. Emotional distress impacts quality of life evaluation: A report from the childhood cancer survivor study. J. Cancer Surviv 11 (3), 309–319. https://doi.org/10.1007/s11764-016-0589-5 (2017).
von Elm, E. et al. The strengthening the reporting of observational studies in epidemiology (STROBE) statement: Guidelines for reporting observational studies. Lancet 370 (9596), 1453–1457. https://doi.org/10.1016/s0140-6736(07)61602-x (2007).
Tinner, E. M. E. et al. Characteristics and feedback of adult survivors of childhood cancer seen in Swiss comprehensive follow-up clinics led by general internists: A prospective cohort study. BMJ Open 14 (7), e081823. https://doi.org/10.1136/bmjopen-2023-081823 (2024).
Horowitz, M. E. et al. Passport for care: Implementing the survivorship care plan. J. Oncol. Pract. 5 (3), 110–112. https://doi.org/10.1200/jop.0934405 (2009).
Ware, J. E. & Keller, K. M. SD SF-36 physical and mental component summary measures: A user’s manual. (1994). https://www.researchgate.net/profile/John-Ware-6/publication/292390260_SF-36_Physical_and_Mental_Health_Summary_Scales_a_User%27s_Manual/links/5af580264585157136caee31/SF-36-Physical-and-Mental-Health-Summary-Scales-a-Users-Manual.pdf. Accessed 13 May 2024.
Rueegg, C. S. et al. Health-related quality of life in survivors of childhood cancer: The role of chronic health problems. J. Cancer Surviv. 7 (4), 511–522. https://doi.org/10.1007/s11764-013-0288-4 (2013).
Essig, S. et al. Health-related quality of life in long-term survivors of relapsed childhood acute lymphoblastic leukemia. PLoS One 7 (5), e38015. https://doi.org/10.1371/journal.pone.0038015 (2012).
Reulen, R. C. et al. The use of the SF-36 questionnaire in adult survivors of childhood cancer: Evaluation of data quality, score reliability, and scaling assumptions. Health Qual. Life Outcomes. 4, 77. https://doi.org/10.1186/1477-7525-4-77 (2006).
Roser, K. et al. Health-related quality of life in Switzerland: Normative data for the SF-36v2 questionnaire. Qual. Life Res. 28 (7), 1963–1977. https://doi.org/10.1007/s11136-019-02161-5 (2019).
Loblaw, D. A., Bezjak, A. & Bunston, T. Development and testing of a visit-specific patient satisfaction questionnaire: The Princess Margaret hospital satisfaction with doctor questionnaire. J. Clin. Oncol. 17 (6), 1931–1938. https://doi.org/10.1200/jco.1999.17.6.1931 (1999).
Michel, G. et al. Incidence of childhood cancer in Switzerland: The Swiss childhood cancer registry. Pediatr. Blood Cancer 50 (1), 46–51. https://doi.org/10.1002/pbc.21129 (2008).
Frank, G. H. Brief Symptom Inventory Von L. R. Derogatis (Kurzform Der SCL-90-R): Manual, in Deutsche Version (Beltz Test GmbH, 2000).
Derogatis, L. R. & Melisaratos, N. The brief symptom inventory: An introductory report. Psychol. Med. 13 (3), 595–605 (1983).
Kim, H. Y. Statistical notes for clinical researchers: Chi-squared test and Fisher’s exact test. Restor. Dent. Endod. 42 (2), 152–155. https://doi.org/10.5395/rde.2017.42.2.152 (2017).
stata.com Signrank. - Equality test on matched data. https://www.stata.com/manuals/rsignrank.pdf. Accessed 24 July 2024.
Philipp, M. Qualitative content analysis [28 paragraphs]. Forum: Qualit. Soc. Res. 1 (2). https://doi.org/10.17169/fqs-1.2.1089 (2000).
QCA, QCAmap // a software for Qualitative Content Analysis. p. QCAmap is an open access web application for systematic text analysis in scientific projects based on the techniques of qualitative content analysis (Mayring, 2022). https://www.qcamap.org/ui/en/home.
Götze, H. et al. Fear of cancer recurrence across the survivorship trajectory: Results from a survey of adult long-term cancer survivors. Psychooncology 28 (10), 2033–2041. https://doi.org/10.1002/pon.5188 (2019).
Zeltzer, L. K. et al. Psychological status in childhood cancer survivors: A report from the childhood Cancer survivor study. J. Clin. Oncol. 27 (14), 2396–2404. https://doi.org/10.1200/jco.2008.21.1433 (2009).
Michel, G. et al. The brief symptom inventory in the Swiss general population: Presentation of norm scores and predictors of psychological distress. PLoS One 19 (7), e0305192. https://doi.org/10.1371/journal.pone.0305192 (2024).
Recklitis, C., O’Leary, T. & Diller, L. Utility of routine psychological screening in the childhood cancer survivor clinic. J. Clin. Oncol. 21 (5), 787–792. https://doi.org/10.1200/jco.2003.05.158 (2003).
Zeltzer, L. K. et al. Psychosocial outcomes and health-related quality of life in adult childhood cancer survivors: A report from the childhood cancer survivor study. Cancer Epidemiol. Biomark. Prev. 17 (2), 435–446. https://doi.org/10.1158/1055-9965.Epi-07-2541 (2008).
Sedmak, M., Bogdanić, A. & Grubić, M. Correlates of quality of life in pediatric cancer survivors. Psychiatr. Danub. 32 (Suppl 4), 533–539 (2020).
Horan, M. R. et al. Determinants of health-related quality-of-life in adult survivors of childhood cancer: Integrating personal and societal values through a health utility approach. EClinicalMedicine 58, 101921. https://doi.org/10.1016/j.eclinm.2023.101921 (2023).
Engelen, V. et al. Reporting health-related quality of life scores to physicians during routine follow-up visits of pediatric oncology patients: Is it effective? Pediatr. Blood Cancer 58 (5), 766–774. https://doi.org/10.1002/pbc.23158 (2012).
Hendriks, M. J., Harju, E. & Michel, G. The unmet needs of childhood cancer survivors in long-term follow-up care: A qualitative study. Psychooncology 30 (4), 485–492. https://doi.org/10.1002/pon.5593 (2021).
Gianinazzi, M. E. et al. Information provision and information needs in adult survivors of childhood cancer. Pediatr. Blood Cancer 61 (2), 312–318. https://doi.org/10.1002/pbc.24762 (2014).
Christen, S. et al. Perceived information provision and information needs in adolescent and young adult cancer survivors. Eur. J. Cancer Care (Engl) 28 (1), e12892. https://doi.org/10.1111/ecc.12892 (2019).
Acknowledgements
We thank Helen Affolter und Marinela Velikova Bayha, who were involved in patient care and ensured that all ACCS were able to complete baseline and follow-up questionnaires.
Funding
This work was supported by the science funds of the University Institute of Internal Medicine of the cantonal hospital Baselland (grant number: N/A), the Basel Region Childhood Cancer Foundation (grant number: #2020-F009) and the “Berner Stiftung für krebskranke Kinder und Jugendliche” (grant number: N/A).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by L.V, K.R, E.M.T, C.B, C.E.K and M.M.W. The analysis was done by C.E.K., C.B., and K.R. All authors interpreted the results and contributed to the interpretation. The first draft of the manuscript was written by C.E.K and M.M.W. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
The study involves human participants and was approved by ethics committee of Northwestern and Central Switzerland (EKNZ, 2017 − 00109).
Consent to participate
All participants provided informed consent prior to the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Kull, C.E., Vifian, L., Leuppi, J.D. et al. A prospective cohort study on the trajectory of health-related quality of life in adult childhood cancer survivors attending a follow-up care program. Sci Rep 15, 8332 (2025). https://doi.org/10.1038/s41598-025-92820-0
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-92820-0
Keywords
This article is cited by
-
Long-term quality of life in head and neck cancer: the role of postdiagnosis smoking behavior
Journal of Cancer Survivorship (2025)