Abstract
To evaluate the effectiveness of the integrated people-centered eye car"365 Eye Care,” in controlling myopia among children and adolescents in northeast China. Additionally, the study aimed to explore the model’s impact on different subgroups. A retrospective analysis was conducted on the changes in spherical equivalent(∆SE) within one year of 427 participants and 494 control participants who underwent the “365 Eye Care"project at He Eye Specialist Hospital from January 2021 to December 2023. The effectiveness of “365 Eye Care"on vision protection was analyzed. The difference between the two groups was further analyzed when the baseline SE was constant. The project included the analysis of the causes of myopia and the formulation of individualized myopia prevention and control plans, monthly vision examination and visual status monitoring, and assessing the eye environment (including diet, light, table and chair selection, etc.) The 1-year change in SE(∆SE) was − 0.46 ± 0.36 for the “365 eyecare” group and- 1.82 ± 1.14 for the control group (P < 0.001). The SE for pre-myopia, low myopia, and moderate myopia were significantly lower than the control group(P < 0.001), and the difference was − 1.25D, - 1.38D, - 0.81D, respectively. There was no difference between the two groups in high myopia. The results showed that the comprehensive eye care intervention helped slow down the progression of myopia, and the average effect level was 0.71. The integrated people-centered eye care model, “365 eyecare,” holds promise for myopia control. And the earlier the children participated in the comprehensive intervention, the better the myopia prevention and control effect.
Similar content being viewed by others
Introduction
Myopia is the most prevale which of refractive error1. High myopia is associated with severe complications, including retinal detachment and myopic macular degeneration, which can result in irreversible vision loss2,3,4,5. The widespread use of electronic devices reduced outdoor activity, which contribute to the exacerbation of myopia during adolescence6. Therefore, implementing effective prevention and control measures for myopia at this stage is crucial for maintaining normal ocular development and refractive status7,8,9,10.
Myopia in children and adolescents has become one of the major public health problems17. Many randomized controlled trial showed the effectiveness of low-dose atropine, ortho-k, DIMS-like spectacles, etc. on reducing myopia progression11. Exploring effective preventive measures has become the key to preventing and controlling myopia. The occurrence and development of myopia are the results of the combined action of multiple factors, and the single-factor study has limited impact on the progression of myopia, so the combined intervention of multiple factors may have great potential11,12.
In 2019, the World Health Organization (WHO) released its first World Vision Report, which mainly recommends that integrated people-centered eye care be the preferred healthcare model. A new 2020 World Health Assembly resolution focuses on integrated people-centered eye care13,14,15. A cross-sectional study in India evaluated the effect of integrated person-centered eye care on eye care behavior in the community population15, and some scholars in Africa discussed the application and implementation of integrated person-centered eye care in Africa16,17. However, no relevant studies have been retrieved on myopia prevention and control among children and adolescents.
In this study, a real-world study (RWS) was conducted to evaluate the effect of people-centered comprehensive eye care on myopia prevention and control in children and adolescents by matching the retrospective cohort study method. The changes in spherical equivalent after one year of people-centered comprehensive eye care were compared between the two groups17.
Materials and methods
This study was a retrospective cohort analysis involving 921 patients (921 right eyes) who attended He Eye Specialist Hospital from January 2021 to December 2023 were included. The intervention group consisted of 427 patients (427 right eyes), who engaged in the person-centered comprehensive eye care model known as “365 Eye Care”, while the control group consisted of 494 patients (494 right eyes). All patients underwent cycloplegic refraction using ARK- 1 (Nidek, Gamagori, Japan) by a professional optometrist. All patients wearing orthokeratology lenses underwent a washout period prior to measurements.
This study desensitized the identifiable information in the data. It was approved by the Ethics Committee of He Eye Specialist Hospital (IRB (2023) K018.01) and adhered to the tenets of the Declaration of Helsinki. All patients underwent a comprehensive examination conducted by qualified ophthalmologists and certified optometrists. Informecconsent was obtained from all subiects and their legal guardians.
Inclusion–exclusion criteria
Patients were eligible for this study if they met the following criteria: Between 3 and 17 years of age; No undergone eye surgery; Medical records were obtained 1 year (± 3 months) after the first visit. The data of spherical and cylindrical refraction were complete at the first and last visits.
The exclusion criteria were spherical equivalent (SE) degree greater than + 0.75D at the first visit, combined with other eye diseases such as strabismus and amblyopia; Participation in other similar research projects; Missing data of the right eye; Important records that could affect the results were missing (SE, date of birth, sex, time of visit, type of lens worn, etc.).
Grouping criteria
The participants were divided into the intervention and control groups according to whether they participated in the IPEC program.
Intervention group: The intervention contents of the IPEC program included establishing vision health records (Table 1), and the detailed suggestions are provided in Attachment 1.
One of the key strategies of “365 Eye Care” is the management of myopia in children and adolescents through a collaborative approach. For people seeking to prevent and control myopia, it is important to first inform them about the occurrence of myopia and how to properly control the development of myopia, so that integrated eye care services can be available and sustainable myopia management means.
The control group maintained the original lifestyle and eye habits without any other intervention.
Statistical analysis
This study used Stata17 (StataMP- 64) software for statistical analysis. P < 0.05 was considered to indicate statistical significance.
The data were tested for normality and homogeneity of variance. Mann-Whitney test was used for measurement data that did not conform to normal distribution, and the student t-test was used to compare the differences between groups for measurement data with normal distribution and homogeneity of variance. The difference-in-difference (DID) method was used to analyze the myopia prevention and control effect of participation in IPEC.
Results
Table 2 shows the baseline demographic characteristics of the two groups. There were no significant differences in gender, age of enrollment, baseline SE, myopia degree, and type of wearing glasses between the two groups (P > 0.05).
Table 3 shows the baseline and one-year SE for the two groups of patients. There was no statistically significant difference in baseline SE between the two groups (P = 0.12). After one year, the mean level of SE decreased in both groups, and the difference was statistically significant (P < 0.01). The decrease in SE was − 1.51D less in the intervention group than in the control group.
Figure 1 shows the difference in one-year change in SE(∆SE) between the two groups (P < 0.01). The ∆SE of the intervention group is − 0.46 ± 0.36 and that of the control group is − 1.82 ± 1.14.
Comparison of one-year SE change of participants(∆SE) between the intervention group and control group.
Figure 2 shows statistically significant differences between the two groups in pre-myopia, low myopia, and moderate myopia subgroups (P < 0.01). The ∆SE of the intervention group was − 1.25D, − 1.38D, − 0.81D lower than that of the control group, respectively. There was no significant difference in SE for high myopia participants between the intervention group and the control group (P > 0.05).
Differences in one-year SE change of participants(∆SE) between the two groups according to the degree of baseline myopia.
Table 4 shows the DID analyses of SE at enrollment and after 1 year for the intervention and control groups. Before the intervention, the difference in effect size between the intervention group and the control group was 0.04, which was not statistically significant (P = 0.17). After the intervention, the difference effect value between the intervention group and the control group was 0.75, and there was a significant difference (P < 0.01). The difference was 0.71; the results showed that the comprehensive intervention helped slow down the progression of myopia, and the average effect level was 0.71.
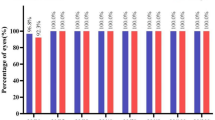
Table 5 shows the percentage of patients with ∆SE ≦ − 0.50 D after one year in the intervention group and control groups. The results indicate statistically significant differences between the two groups in the pre-myopia, low-myopia, and moderate-myopia categories (p < 0.001), with the intervention group exhibiting a higher percentage of patients with ∆SE ≦ − 0.50 D compared to the control group across all categories.
Discussion
In this study, we conducted a real-world cohort study to evaluate the impact of a “365 Eye Care” program on myopia prevention and control in children and adolescents. Our findings demonstrated that participants in the intervention group, who received comprehensive guidance on lifestyle factors such as diet, sleep, and screen time, achieved better myopia control outcomes compared to the control group. These results align with and extend the findings of previous studies, highlighting the importance of early and holistic interventions in myopia management18,19.
The reduction of time spent outdoors significantly increases the incidence of myopia in children and adolescents19,20. Prolonged close reading was also significantly associated with the development of myopia, which is consistent with our observation that participants in the “365 Eye Care” program, who were advised to balance screen time with outdoor activities, showed better myopia control outcomes.
Our study also supports the growing body of evidence emphasizing the role of early intervention in myopia management. Morgan et al. emphasize in their study that myopia progresses most rapidly during childhood and adolescence, so this period is critical for intervention21,22. By providing personalized lifestyle adjustments and recommendations for regular follow-up, our “365 Eye Care” program effectively delayed the progression of myopia, which is consistent with the findings of Huang et al., who demonstrated that structured eye care programs can significantly reduce the incidence of myopia in school-age children23,24,27.
The findings of this study revealed no significant difference between the high myopia group and the control group in terms of the effectiveness of people-oriented comprehensive eye care. The percentage of patients with ∆SE≦− 0.50 D was significantly higher in the intervention group than in the control group after 1 year. This suggests that the benefits of comprehensive myopia intervention are not limited to the severity of myopia at baseline but are instead influenced by the timing of intervention initiation. Specifically, the earlier children participate in comprehensive myopia prevention and control programs, the more effective these interventions are in slowing myopia progression and reducing the risk of developing high myopia. This underscores the importance of early intervention, as timely and consistent eye care can significantly alter the trajectory of myopia development in children.
The visual protection and health are equally important1,25,26. Because children’s visual system has not yet fully developed, the ability of the eye to adapt to external stimuli is limited, so it is easy to be affected by bright light, television, computers and other adverse visual environment26,27,28,29. During the COVID- 19 pandemic, reduced outdoor activities due to online courses and increased digital screen time contributed to the occurrence and development of myopia30. Therefore, in the critical period and sensitive period of visual development of children and adolescents, timely and appropriate treatment and training can prevent and treat myopia. We should pay more attention to integrated people-centered eye care, to achieve early detection, early intervention and early treatment.
This study has some limitations. Firstly, the observation period of this study was one year, and the IPEC can effectively delay myopia progression in children and adolescents. In further studies, as the IPEC is increasingly popular, long-term follow-up can be conducted to explore its long-term effect further. Secondly, in the future, prospective randomized controlled trials should be conducted to control the influence of confounding factors on the results of the study and include axial length measurement. Furthermore, our study only records the outdoor activity time, controlling and evaluating the intensity of outdoor ambient light will be valuable in further studies.
The integrated people-centered eye care model, “365 eyecare,” holds promise for myopia control. And the earlier the children participated in the comprehensive intervention, the better the myopia prevention and control effect.
Data availability
Anonymized datasets generated and analyzed during the current study will be made available on reasonable request by the corresponding author (Guanghao Qin, qinguanghao2020@163.com.
Change history
12 September 2025
A Correction to this paper has been published: https://doi.org/10.1038/s41598-025-18787-0
References
Bullimore, M. A. et al. The risks and benefits of myopia control. Ophthalmology 128 (11), 1561–1579. https://doi.org/10.1016/j.ophtha.2021.04.032 (2021).
Zhang, X. et al. Optic neuropathy in high myopia: glaucoma or high myopia or both? Prog Retin Eye Res. 99, 101246. https://doi.org/10.1016/j.preteyeres.2024.101246 (2024).
Ikuno, Y. & Overview of the complications of high MYOPIA Retina ;37(12):2347–2351. doi:https://doi.org/10.1097/IAE.0000000000001489 (2017).
Haarman, A. E. G. et al. The complications of myopia: A review and Meta-Analysis. Invest. Opthalmology Visual Sci. 61 (4), 49. https://doi.org/10.1167/iovs.61.4.49 (2020).
Liu, L. et al. Analysis of morphological and quantitative changes in pathological myopia and perioperative changes in posterior scleral reinforcement using three-dimensional magnet resonance imaging. Front. Bioeng. Biotechnol. 11 https://doi.org/10.3389/fbioe.2023.1242440 (2023).
Foreman, J. et al. Association between digital smart device use and myopia: a systematic review and meta-analysis. Lancet Digit. Health. 3 (12), e806–e818. https://doi.org/10.1016/S2589-7500(21)00135-7 (2021).
Wolffsohn, J. S., Whayeb, Y., Logan, N. S. & Weng, R. IMI—Global trends in myopia management attitudes and strategies in clinical Practice—2022 update. Invest. Opthalmology Visual Sci. 64 (6), 6. https://doi.org/10.1167/iovs.64.6.6 (2023).
Naidoo, K. S. et al. Potential lost productivity resulting from the global burden of myopia. Ophthalmology 126 (3), 338–346. https://doi.org/10.1016/j.ophtha.2018.10.029 (2019).
Logan, N. S. et al. IMI accommodation and binocular vision in myopia development and progression. Invest. Opthalmology Visual Sci. 62 (5), 4. https://doi.org/10.1167/iovs.62.5.4 (2021).
Ma, Y. et al. Healthcare utilization and economic burden of myopia in urban China: A nationwide cost-of-illness study. J. Glob Health. 12, 11003. https://doi.org/10.7189/jogh.12.11003 (2022).
Tariq, F. et al. Advances in myopia prevention strategies for school-aged children: a comprehensive review. Front. Public. Health. 11 https://doi.org/10.3389/fpubh.2023.1226438 (2023).
Lawrenson, J. G. et al. Interventions for myopia control in children: a living systematic review and network meta-analysis. Cochrane Database Syst. Reviews. 2023 (2). https://doi.org/10.1002/14651858.CD014758.pub2 (2023).
Marques, A. P. et al. The economics of vision impairment and its leading causes: A systematic review. EClinicalMedicine 46, 101354. https://doi.org/10.1016/j.eclinm.2022.101354 (2022).
Burton, M. J. et al. The lancet global health commission on global eye health: vision beyond 2020. Lancet Glob Health. 9 (4), e489–e551. https://doi.org/10.1016/S2214-109X(20)30488-5 (2021).
Shukla, P., Vashist, P., Suraj Ss, Gupta, V., Gupta, N. & Bharadwaj, A. Effect of integrated people-centred eye care (IPEC) model on eye care seeking behaviour of community. Indian J. Public. Health. 66 (3), 282. https://doi.org/10.4103/ijph.ijph_1391_21 (2022).
Van Staden, D. & Munsamy, A. Integrated, people-centred eye care: why South Africa needs to prioritise scaling up refractive services. South. Afr. Med. J. 111 (10), 924. https://doi.org/10.7196/SAMJ.2021.v111i10.15918 (2021).
Xie, J. et al. Real-World data for healthcare research in China: call for actions. Value Health Reg. Issues. 27, 72–81. https://doi.org/10.1016/j.vhri.2021.05.002 (2022).
Charvériat, M. et al. Use of real-world evidence in translational Pharmacology research. Fundam Clin. Pharmacol. 36 (2), 230–236. https://doi.org/10.1111/fcp.12734 (2022).
Chen, L. & Zhang, X. W. Which lamp will be optimum to eye? Incandescent, fluorescent or LED etc. Int. J. Ophthalmol. 7 (1), 163–168. https://doi.org/10.3980/j.issn.2222-3959.2014.01.30 (2014).
Guo, Y. et al. [Outdoor activity and myopia among 681 primary students in urban and rural regions of Beijing]. Zhonghua Yi Xue Za Zhi. 94 (3), 191–194 (2014).
Morgan, I. G. et al. The epidemics of myopia: aetiology and prevention. Prog Retin Eye Res. 62, 134–149. https://doi.org/10.1016/j.preteyeres.2017.09.004 (2018).
Pan, W. et al. Lancet Reg. Health West. Pac. ;55:101484. doi:https://doi.org/10.1016/j.lanwpc.2025.101484 (2025).
Zhou, W. J. et al. Five-Year progression of refractive errors and incidence of myopia in School-Aged children in Western China. J. Epidemiol. 26 (7), 386–395. https://doi.org/10.2188/jea.JE20140258 (2016).
French, A. N., Morgan, I. G., Burlutsky, G., Mitchell, P. & Rose, K. A. Prevalence and 5- to 6-Year incidence and progression of myopia and hyperopia in Australian schoolchildren. Ophthalmology 120 (7), 1482–1491. https://doi.org/10.1016/j.ophtha.2012.12.018 (2013).
Bullimore, M. A. & Johnson, L. A. Overnight orthokeratology. Contact Lens Anterior Eye. 43 (4), 322–332. https://doi.org/10.1016/j.clae.2020.03.018 (2020).
Huang, D. et al. Fundus tessellated density assessed by deep learning in primary school children. Transl Vis. Sci. Technol. 12 (6), 11. https://doi.org/10.1167/tvst.12.6.11 (2023).
Chen, J. et al. Axial length changes in progressive and non-progressive myopic children in China. Graefe’s Archive Clin. Experimental Ophthalmol. 261 (5), 1493–1501. https://doi.org/10.1007/s00417-022-05901-5 (2023).
Lu, T. et al. Refractive lens power and lens thickness in children (6–16 years old). Sci. Rep. 11 (1), 19284. https://doi.org/10.1038/s41598-021-98817-9 (2021).
Wang, Y. & Ma, J. Future developments in SMILE: higher degree of myopia and hyperopia. Asia-Pacific J. Ophthalmol. 8 (5), 412–416. https://doi.org/10.1097/01.APO.0000580128.27272.bb (2019).
Jonas, J. B. et al. IMI prevention of myopia and its progression. Invest. Opthalmology Visual Sci. 62 (5), 6. https://doi.org/10.1167/iovs.62.5.6 (2021).
Acknowledgements
We thank the participants in this study. The authors have no proprietary interest in any of the products mentioned in this article.
Funding
This study was supported by Foundation of Liaoning He University [LHYX(2023)19].
Author information
Authors and Affiliations
Contributions
Conception and design of the research: GQ, XH, SY; Analysis and interpretation of the data: FY; Writing original draft preparation: FY, XH; Data collection: ZR, CY, JC; Critical revision of the manuscript: GQ, SY; Supervision: WH, SY, XH. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Consent for publication
Not Applicable.
Ethical approval
This study was approved by the Ethics Committee of He Eye Specialist Hospital (IRB (2023) K018.01) and conducted by the Department of Clinical Research.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this Article was revised: The original version of this Article contained an error in Figure 1. Full informationregarding correction can be found in the correction published with this article.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
He, X., Yang, F., Zhang, R. et al. The impact of the integrated people-centered eye care model on myopia control among children and adolescents in China. Sci Rep 15, 12838 (2025). https://doi.org/10.1038/s41598-025-97253-3
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-97253-3