Abstract
Antimicrobial photodynamic therapy (aPDT) is a promising strategy to combat resistant microbial strains. However, despite its high in vitro efficacy, clinical outcomes often fall short, largely due to insufficient retention of the photosensitizer (PS) at the target site. Factors such as salivary flow and PS aggregation significantly hinder the effectiveness of aPDT. This study presents the development of a high-viscosity methylene blue (MB) formulation tailored for dental aPDT applications. The increased viscosity aims to enhance PS retention at the treatment site, while carefully selected components address MB aggregation, ultimately improving the clinical efficacy of the therapy. Key formulation strategies included the incorporation of a surfactant, anionic polymers, an acidic pH, and reduced MB concentrations to effectively mitigate aggregation. Stability testing demonstrated that the formulation preserved its organoleptic properties, pH, and MB content over 1 year. Although the formulation exhibited lower MB uptake in Candida albicans biofilms compared to aqueous MB, this did not compromise its antimicrobial activity. In vitro aPDT assays showed comparable efficacy between MB in water and the high-viscosity formulation. These findings highlight the potential of the developed viscous MB formulation to enhance the practicality and clinical success of aPDT in dentistry, without compromising its therapeutic effectiveness.
Similar content being viewed by others
Introduction
The overuse of antimicrobial agents, despite their effectiveness against microbial infections, has led to a significant global health issue known as antimicrobial resistance. This phenomenon results in the emergence of resistant microbial strains, rendering traditional treatments ineffective1,2,3. Consequently, there has been a surge in hospitalizations and deaths due to untreatable infections4. Currently, approximately 35% of common infections exhibit resistance to available antimicrobial drugs, a figure that could escalate to 90%, particularly in low-income countries5. In a report, the World Health Organization frames global oral health as an alarming situation, concluding that it requires urgent measures3. In the United States alone, over 35,000 deaths occur annually due to more than 2.8 million antibiotic-resistant infections, incurring hospital costs of $35–$45 billion. Similarly, in Europe, these costs can reach 7 billion euros6. Urgent adoption of innovative antibacterial treatments is imperative4, including those aimed at oral health care since the relevance related to antimicrobial resistance lies in the fact that antibiotics are among the most prescribed medications for bacterial infections by dentists, with an estimated dental prescription rate of approximately 10% in relation to all prescriptions of this medication class on a global scale3,7.
Antimicrobial photodynamic therapy (aPDT) emerges as a promising avenue, characterized by its non-invasiveness, established safety profile, broad spectrum of action, and lack of association with microbial resistance. Employed across various clinical domains, aPDT employs a non-selective approach, targeting microbial cells through the combined action of a photosensitizer (PS), light, and oxygen.
In this context, methylene blue (MB), a phenothiazinium dye, stands out as a primary PS agent for aPDT8,9,10,11,12. Widely studied for its safety and non-toxic nature13,14, MB’s effectiveness can be compromised by its tendency to aggregate, changing the absorption spectra and reducing its capacity to generate reactive oxygen species (ROS) such as singlet oxygen (1O2)15,16.
There is a huge number of in vitro studies showing MB efficacy against different microorganisms (Gram-positive and Gram-negative bacteria17, fungi18,19,20, and protozoans21,22). Nonetheless, despite its high in vitro efficacy, clinical outcomes often fall short, largely due to insufficient retention of the PS at the target site. Factors such as salivary flow and PS aggregation significantly hinder the effectiveness of aPDT23. Some researchers have been trying to overcome these pitfalls by increasing MB concentration or combining to other agents, such as potassium iodide or sodium dodecyl sulfate (SDS)8,24,25,26.
The MB aggregation is influenced by factors such as medium, concentration and pH, modulating the type and efficacy of the photochemical reactions involved8,27. Monomeric MB tends to produce 1O2, while dimers generate radicals16. Hence, the formation of aggregates diminishes 1O2 generation, impacting photosensitization efficiency. MB monomers are more effective in reducing the number of Candida albicans cells in vitro both in suspension and in biofilm, being more effective in causing cell death via 1O2. Our research group has underscored the importance of developing formulations that mitigate MB aggregation, particularly through the use of SDS8,24,25.
Given that effective PS application and illumination are crucial for treating infected areas, enhancing viscosity has become essential in clinical dental practice. The advantage of increasing the viscosity is the possibility of obtaining the appropriate consistency for application and permanence of the formulation in the desired location. This is an important factor to ensure retention at the application site for gradual release to carry out aPDT action without being quickly neutralized by salivary flow.
Retention can be improved by increasing adhesion time when transporting PS in nanosystems or hydrogels made up of polymers28. Hydrogels are materials made up of a three-dimensional hydrophilic polymer network with the ability to swell in the presence of water, presenting mechanical properties of solids and diffusive transport of liquids and are biomaterials with promising applications as they are biocompatible with biological fluids29. To address this, our study optimized a formulation by incorporating mucoadhesive polymers and pharmacotechnical adjuvant. In order to favor the application of the formulation in the oromucosa, the use of mucoadhesive polymers with bioadhesion properties is desired30, facilitating the maintenance of the formulation in the applied location, increasing the residence time in the oral cavity and improving therapeutic results31. Both polymers hydroxypropylmethylcellulose (HPMC) and carboxymethylcellulose (CMC) are semi-synthetic derivatives of cellulose capable of delivering the necessary rheological properties on the surface of mucosa, increasing drug retention time31.
The incorporation of biopolymers, such as methylcellulose, allows increased viscosity and retention of MB at the site of application by the dentist, overcoming a clinical deficiency when using a fluid formulation, which impairs photoinactivation32. The non-ionic polymer HPMC has a thickening, surfactant and emulsifying action, used to favor drug delivery control and increase the viscosity of formulations33. CMC is an anionic polymer with a thickening and binding function and is present in the composition of toothpastes to increase viscosity and in addition to gel-forming properties, it has good mucoadhesive performance through strong hydrogen bonds between the non-ionized carboxyl groups and mucin, the main glycoprotein found in mucus, responsible for physical and mechanical interactions30. Exposure to higher temperatures will lead to a decrease in the viscosity of the preparation containing CMC34, which is desired when applying the product clinically35. This optimization involved analyzing MB aggregation characteristics, pH, viscosity, density, and active ingredient concentration, alongside assessing effectiveness through microbiological incorporation and in vitro viability in C. albicans biofilms under irradiation parameters. Additionally, the physicochemical stability of the developed formulation was determined.
Results
Physico-chemical properties
For both polymers, the increase in concentration resulted in higher viscosity (Fig. 1). For HPMC, values increased from 14.60 ± 0.51 cP, to 107.50 ± 27.43 cP and finally to 445.02 ± 11.91 cP with concentration ranging from 1, 3 and 5%, respectively. For CMC, a small increase in the concentration caused a pronounced increase in viscosity, going from 32.12 ± 0.85 cP, to 110.78 ± 0.97 cP up to 480.24 ± 20.79 cP with the increase in concentration from 0.25%, 0.50% and 1%, respectively. Considering these parameters, HPMC 1% and CMC 1% (the lowest and highest viscosities, respectively) were excluded from the study.
Viscosities (cP) of samples containing 0.005% MB and 0.25% SDS conveyed according to the concentrations (%) of non-ionic (HPMC) and anionic (CMC) polymer.
The formulations whose viscosity was determined were considered to have neutral pH (around of 6.5). Thus, the preparations had their pH adjusted, as acidic and basic to also have the dimer to monomer ratio measured.
Dimer to monomer (D/M) ratio
The D/M ratio was used as a tool to verify the influence of factors in MB aggregation. The D/M values were presented at Fig. 2. On the one hand, there was a significant reduction in MB D/M values with increasing polymers concentrations in the absence of SDS, being higher the D/M values for CMC (Fig. 2A). On the other hand, in formulations containing 0.005% MB associated with 0.25% SDS, the D/M ratio values were significantly lower when compared to absence of SDS. Both polymers showed no strong differences in D/M values with increasing concentrations in the presence of SDS. Thus, it was stablished the need of SDS in the formulations to reduce MB aggregation.
Comparison of the dimer-to-monomer (D/M) ratios of samples containing 0.005% MB conveyed in different concentrations of non-ionic (HPMC)a and anionic (CMC)b polymer. (a) In the absence (gray) or presence (red) of 0.25% SDS at neutral pH. (b) In the presence of 0.25% SDS at acidic (black), neutral (dark gray) and basic (light gray) pH. aD/M(HPMC) = A614/A662. bD/M(CMC) = A623/A663. *Groups sharing the same letters present no statistical differences (p > 0.05) while groups presenting different letters presented significant differences (p < 0.05), Two-way ANOVA followed by Tukey post-test.
In general, the D/M was higher in basic, intermediate in neutral and lower for acidic pHs, both for HPMC and CMC (Fig. 2B). The concentrations of non-ionic and anionic polymers did not interfere in the D/M ratio when considering each pH in isolation and acidic formulations presented lower D/M ratio values. Both concentrations of the non-ionic polymer at acidic pH presented a lower D/M ratio in relation to preparations formulated in basic medium, with a significant reduction in the D/M value in 3% and 5% acidic HPMC compared to the two concentrations of HPMC in basic medium although there is no statistical difference with the same formulations at neutral pH. For the analysis of the anionic polymer, the acidic pH was also able to result in a significant reduction in the D/M ratio compared to the basic pH and neutral pH, remaining in the order of 0.5. The anionic polymer CMC at any concentration and at any pH results in less MB aggregation (smaller D/M values) compared to HPMC.
Figure 3 shows the spectra of MB formulations with SDS at two different concentrations of HPMC (3% and 5%) and CMC (0.25% and 0.5%) at acidic, neutral and basic pH. The formulation with the anionic polymer 0.5% CMC at acidic pH demonstrated less MB aggregation presenting greater viscosity as an additional advantage, thus it was selected as the conditions of choice. The next step was to evaluate the effect of MB concentration. Therefore, the formulations were prepared with different concentrations of MB (0.002%, 0.005% and 0.010%), and the D/M data was presented in Fig. 4. The greatest aggregation was obtained with the highest concentration of MB and the D/M ratio did not show a statistical difference between the two lowest concentrations.
Absorption spectra of triplicate MB formulations with SDS at two different concentrations of each polymer at three different pH. (a) HPMC 3% acidic. (b) HPMC 5% acidic. (c) HPMC 3% neutral. (d) HPMC 5% neutral. (e) HPMC 3% basic. (f) HPMC 5% basic. (g) CMC 0.25% acidic. (h) CMC 0.5% acidic. (i) CMC 0.25% neutral. (j) CMC 0.5% neutral. (k) CMC 0.25% basic. (l) CMC 0.5% basic.
Comparison of the dimer-to-monomer (D/M) ratios of formulations containing 0.5% CMC and 0.25% SDS conveyed at acidic pH with different concentrations of MB: F02 (0.002% MB), F05 (0.005% MB) and F10 (0.010% MB). Groups sharing the same letters present no statistically significant differences (p > 0.05), One-way ANOVA followed by Tukey post-test.
Stability tests
The formulation containing 0.005% MB, 0.25% SDS conveyed in 0.5% CMC (F05) had its stability monitored every 6 months for a period of 1 year, being kept at room temperature (25 °C) and protected from light. The appearance of the formulation was initially determined as a fluid gel with a blue color and a characteristic odor, with such organoleptic assessment of the formulation remaining unchanged throughout the entire period evaluated. The other attributes, such as identification of the MB monomer by spectrophotometry and D/M ratio were quantified and recorded at the initial time (TØ), at 6 months (T6) and 12 months (T12), as shown in the median, minimum and maximum values in Table 1.
The formulation remained stable without significant differences throughout the period evaluated in terms of pH and MB monomer quantification. The increase in the D/M ratio at 12 months was considered statistically significant, in relation to the other two times evaluated, demonstrating that there was an increase in MB aggregation between 6 months and 1 year. Despite this, the numerical difference is quite small, which would possibly not considerably affect the characteristics of the formulation.
Although viscosity stability was not assessed after 1 year, viscosity of the formulations stored during 3 years was measured finding a decrease to approximately 52.7% of the initial value. Considering that 3 years is a long period for formulation stability—typically limited to 6 months in compounding pharmacies and longer in the pharmaceutical industry—future applications should include optimization and more specific stability testing.
MB uptake in biofilms
The spectra of the samples evaluated according to the variable period of incubation in the dark demonstrated, at any of the times evaluated, a higher cellular uptake rate for MB preparation in water (W05) compared to those conveyed in formula (F05). MB conveyed in water (W05) presents greater cellular uptake compared to the formulation in 0.5% CMC (F05) at any of the times analyzed. In the longest incubation time of 60 min approximately 18% uptake was found for F05, with no statistical difference between 60 and 30 min, while cell uptake around 10% was found for 5, 10 and 30 min W05 samples (with no statistical difference between them), as shown in Fig. 5A. For F05, there was no significant difference between any of the times analyzed (approximately 3% uptake).
aPDT biofilm assay. (a) Cellular uptake (%) in Candida albicans biofilm of samples containing 0.005% MB conveyed in water (W05—dark gray) or formula (F05—light gray) after a variable period of incubation time (min). Groups sharing the same letters present no statistically significant differences (p > 0.05), Two-way ANOVA followed by Tukey post-test. (b) Log CFU/mL Viability in 24-h C. albicans biofilm after 27 min of illumination, One-way ANOVA. (c) Comparison Log CFU/mL Viability in 48-h biofilm of C. albicans after 2 treatments of 27 min of illumination or just 1 of 54 min. CT = control in water. FØ = base formulation without MB. W05 = 0.005% MB in water. W10 = 0.010% MB in water. F05 = 0.005% MB in CMC 0.5% formula. F10 = 0.010% MB in CMC 0.5% formula * Groups presenting significant differences between them depending on the illumination time (p < 0.05), Two-way ANOVA followed by Tukey post-test.
Biofilm viability experiments
The treatments carried out in the 24 h biofilm viability experiment (660 nm, 37.3 mW/cm2, 27 min) showed a small significant reduction in the CFU/mL count in relation to CT only for the F05 group (reduction of 0.22 Log CFU/mL) with no statistical differences between the other groups (Fig. 5B).On the other hand, all groups showed increased antimicrobial action after double treatment, and the greatest reduction was obtained with F05 being 4.26 Log, with no statistical differences between other treatments and with a significant reduction compared to the CT and FØ groups, (Fig. 5C).
The experiment also evaluated treatments carried out with 54 min of illumination time, without new application of MB, keeping the other parameters the same (Fig. 5C). With just 1 cycle of illumination (54 min), without reapplication of treatment, Log reductions were significant for all samples compared to CT and all samples with MB also in relation to FØ, but with maximum reductions close to 1 Log CFU/mL.
Discussion
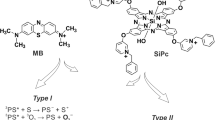
This study focused on the development of a MB formulation with increased viscosity for the application in oral aPDT with the aim of increasing MB retention at the treatment site. Besides the physical–chemical properties and stability, the control of MB aggregation was also considered since our group has been showing that this could be an important strategy to improve antimicrobial action8,24,25,36,37. The aggregation process directly influences reactive oxygen species production. In polar environments, dimerization occurs significantly, leading to a substantial reduction in singlet oxygen generation via the Type II reaction, as dimers are deactivated through the Type I reaction16,38. All these features together could provide improved clinical application.
The literature demonstrates that the aggregation state of MB is influenced by various factors, including its concentration, the pH of the conveying medium, and its interaction with adjunct molecules like surfactants8,16,39,40. Initially, we examined MB aggregation in conjunction with polymers, specifically HPMC and CMC. The increase in the polymer concentrations in formulations lacking SDS led to a slightly decrease in MB aggregation. This reduction can be ascribed to the emulsifying, surfactant, and viscosity-modifying properties of HPMC and CMC polymers33,41. In a study involving gum arabic for hydrogel synthesis, Vilsinski et al.42 attributed MB’s interaction with this anionic polymer to Coulombic, ion–dipole, hydrogen bonding, and hydrophobic forces.
The data on the anionic polymer used in our research, associated to SDS, indicated reduced MB aggregation, prompting consideration of CMC for further investigation. However, analysis depicted in Fig. 2A revealed no significant difference in the D/M ratio at a 1% CMC concentration compared to any HPMC concentration in formulations containing the surfactant. Notably, MB aggregation was higher in CMC than in HPMC formulations, motivating us to proceed with experiments utilizing both polymers, with the exclusion of one concentration of each. The observed D/M ratio values exceeded those observed in SDS-containing formulations, indicative of greater MB aggregation in the absence of the surfactant. The use of the surfactant associated to phenothiazinium dyes has been focus of the research in our group8,24,25,36,37.
The lower D/M ratio of MB in the presence of SDS can be explained by the hindered dimerization resulting from the formation of ion pairs between MB and the surfactant16,30,43. Additionally, reduced hydrophobic interaction between two MB molecules at the micelle’s interfacial region further contributes to this effect.
In literature, viscosity serves as a crucial parameter for evaluating biomaterials used in clinical settings for dentistry, often categorized qualitatively as low, medium, or high viscosity. It reflects the fluidity and flow capacity of the product, with the ideal balance sought to ensure both adequate adaptation to oral tissues and containment at the application site44. The association of antimicrobial agents to polymers is a technique employed to enhance substantivity and efficacy45. Ensuring the delivery of PS in adequate concentration to the infected site is a critical step, and the administration of an appropriate formulation is essential46. For aPDT to effectively combat microorganisms, it is imperative that the PS formulation demonstrates sufficient diffusion to facilitate penetration into anatomical structures and microbial uptake43.
To achieve the desired antimicrobial effect, the PS substance must exhibit substantivity, remaining localized at the site of action and releasing gradually to mitigate the influence of salivary flow. Both HPMC and CMC are mucoadhesive polymers with bioadhesive properties30, making them suitable for increasing the viscosity of dental preparations, thereby prolonging their retention at the application site.
In this context, both polymers could provide the desired consistency at specific concentrations. However, the formulation containing 1% HPMC, a non-ionic polymer, resulted in the lowest viscosity between samples (approximately 14.89 cP), exhibiting a thin and highly liquid appearance that did not significantly enhance viscosity. Conversely, the 1% CMC formulation demonstrated high viscosity (approximately 476.36 cP), potentially posing challenges in manipulation due to its thicker consistency.
The influence of pH on aggregation was assessed at two concentrations of both non-ionic and anionic polymers, since pH is extremely important for photooxidation studies in MB-sensitized biological systems, which are generally carried out in neutral solutions47. Interestingly, the concentrations of these polymers did not impact the D/M ratio when considering each pH independently. Notably, formulations with acidic pH exhibited lower D/M ratio values. This phenomenon can be attributed to the cationic nature of MB, which exhibits enhanced interaction with aqueous molecules in acidic environments compared to non-protonated materials42. The acidic medium was considered more suitable to continue with the experiments, considering the D/M ratio impacting the aggregation and singlet oxygen production. Also, Vilsinski et al.42, who compared simulated fluids at pH 1.2 and 6.8, and observed that an acidic environment facilitated greater release of MB from the hydrogel formed by anionic polymers. Moreover, in the realm of pharmacotechnical formulation development, acidic pH is preferred to enhance preparation stability and reduce degradation risks, particularly through hydrolysis. As elucidated by Luo et al.48, acidity can augment bacterial inactivation by impeding intracellular protein synthesis. Additionally, Gusman et al.49 highlight that the acidic pH of MB solutions exhibits superior biocompatibility with connective tissue compared to neutral pH, thereby promoting the repair and regeneration of periodontal tissue.
Nonetheless, some publications have pointing out that the basic medium provides greater quantum yield of 1O2 production47,50 and better antimicrobial effect40,50. In unbuffered or weakly buffered solutions, the extinction of non-protonated MB species by O2 is much faster than the rate of protonation for any pH values greater than 5 and, therefore, the yield of 1O2 would be similar to that obtained in pH 847,50. Singlet oxygen production quantum yield is inversely proportional to the buffer strength, which may be related to the increase in aggregation at buffered high ionic strength media51. Also, MB pKas values are influenced by the cosolvent52. Considering this potential conflict in the choice of pH for the formulation, further study should compare aggregation, stability, MB release from the formulation and antimicrobial effectivity at different pHs to perform an assertive decision.
Considering all the different formulation compositions proposed, the 0.5% CMC formulation, 0.25% SDS and other adjuvants at pH = 5 was chosen to be associated with three different concentrations of MB (0.002; 0.005 and 0.010%, named F02; F05 and F10, respectively). Even associated to SDS, the highest MB concentration (F10) studied exhibited D/M ratio in the order of 0.62 while the two lowest MB concentrations 0.002% (F02) and 0.005% (F05) presented D/M around 0.5, without significant differences between them. Increasing the concentration of MB in a solvent with a high dielectric constant such as water favors dimerization by modifying the electrostatic repulsion between the monomers27 which are held together by the hydrophobic bond that overcomes the electrostatic repulsion between two MB cations, leading to aggregation15.
Regarding the stability of the developed formulation (F05), a period of 12 months is deemed secure. Upon detailed analysis of the D/M ratio data provided in Table 2, it’s observed that the measurements obtained are very close (0.498 and 0.502, difference of 0.004), indicating a lack of real difference even with a found statistical difference, i.e., in practical terms, this minor disparity may not substantially affect the stability of the formulation. Data presented previously showed D/M increase of 0.28 hinders MB antimicrobial efficacy, which is around seventy times higher the D/M difference found in stability test8. The other attributes evaluated remained consistent over a year, including organoleptic characteristics, pH, and the quantification of MB absorption at a wavelength of 663 nm. Further studies are necessary to establish additional stability criteria, particularly considering that increased MB aggregation after 6 months may adversely affect the outcome of aPDT.
The uptake of MB in biofilms presented higher rates for those carried in water (W05) compared to the formulation (F05). Vilsinski et al.42 state that the levels of MB released from hydrogels in water are low, probably due to the presence of the polymer which, by providing greater viscosity to the preparation, favors a modified release of PS30. Chemisorption plays an essential role in the release of MB from the polymer hydrogel, depending on the ability to interact with the PS molecule and support greater content in its structure, which prevents its release due to significant interactions between them42. No influence of the incubation time on the incorporation of MB was observed when the formulation was used.
In water, shorter incubation times resulted in less incorporation, which can be justified by the intrinsic efflux pump system as a defense mechanism of the microorganism, capable of recognizing PS molecules and affecting transport across the membrane53. This mechanism of resistance to several drugs is well known in relation to the species C. albicans, favoring the elimination of PS by pumping it out of the cells and affecting the effectiveness of the treatment. Also, there was greater incorporation with longer incubation times of 30 and 60 min, with no difference between 30 and 60 min. The pre-irradiation time of 30 min was considered by Torres-Hurtado et al.54 more effective for multiple PDT applications in C. albicans. Adequate incubation time seems to have a huge impact on the effectiveness of aPDT, especially in relation to C. albicans strains, due to the size of these cells and the presence of the cell wall55. Collina et al.36 also observed that increasing the pre-irradiation time does not modify the aPDT response when using an aqueous solution of MB with SDS for this same microorganism, probably due to constant uptake.
In the in vitro evaluation of viability in C. albicans biofilm, the base formula without MB (FØ) showed a reduction of 0.39 Log CFU/mL in relation to the control only in the experiment of 54 min of direct illumination, which demonstrates the absence of cytotoxicity of the developed base formulation. This small effect of reduction in CFU/mL can be attributed to the presence of SDS in the formulation, which has been demonstrated in previous works by the group to reduce approximately 1 Log CFU/mL compared to the control in water when radiant exposure of 44.0 J/cm2 was used and irradiance of 26.1 mW/cm2 in a suspension of C. albicans24 or in a biofilm of the same microorganism in the adhesion phase using similar exposure time, but with a higher irradiance of 37.3mW/cm2, reaching a radiant exposure of 60.4J/cm225. The association of SDS with MB promotes an antimicrobial effect superior to MB conveyed in water without the surfactant, achieving inactivation of planktonic C. albicans with irradiance parameters of 26.1 mW/cm2 and radiant exposure of 44 J/cm2 in an experiment carried out in suspension24.
In the biofilm viability test with 24-h growth, small antimicrobial action was found for formulation containing 0.005% MB (F05), with only 0.2 Log CFU/mL reduction. A similar observation was found by Machado et al.25 in aqueous samples of various PS, including MB, evaluated in biofilms in the maturation phase, both in the presence and absence of SDS. Also, Machado showed that the application of successive treatments may improve aPDT efficacy.
Then, carrying out tests on 48-h growth biofilms, it was decided to perform double aPDT treatment. In this double treatment protocol, an antimicrobial effect of approximately 4 Log reduction in CFU/mL was obtained, however, all samples containing MB showed a similar effect, regardless of the convey media (water or formula). Surprisingly, greater uptake in biofilm of MB conveyed in water did not improve antimicrobial action. The hypothesis is that the lower D/M ratio in F05 may result in increased singlet oxygen production and, also, and act at specific intracellular targets8,19,56,57,58. Simultaneously, the higher uptake of MB conveyed in water, increase MB concentration in cells or biofilm matrix resulting in higher D/M ratio, and reduced antimicrobial effect. This change in MB aggregation also occurs in the mitochondria, forming dimers that depend on both the PS concentration and the organelle itself, in addition to the membrane potential that determines the way in which MB binds to the mitochondria58. It was demonstrated in isolated mitochondria, in intracellular medium, the reduction of MB generating the reduced form leuko-MB59. The depth of light penetration, the characteristics of the strain and the biological environment to be treated are factors that influence the antifungal effect of PS used in PDT, with the incubation time being fundamental to determine the incorporation of PS into the cellular structures of the microorganism. The interaction of MB with mitochondria leads to cytotoxic damage59 and is related to the generation of 1O260. George and Kishen43 also observed greater incorporation of MB conveyed in water with a lower rate of associated cell death, considering that different formulations can promote binding of MB in different cell locations, which can result in an increase in the concentration of PS at the site with dimerization and consequent reduction in cell death.
While CMC and HPMC are known mucoadhesive polymers, standardized methodologies for evaluating bioadhesion remain a subject of ongoing research61. Assessing the mucoadhesive properties of a formulation remains a significant challenge due to the diversity of available methods, each based on distinct experimental setups and requiring either animal tissues or synthetic substitutes. The choice of method can significantly influence the conclusions drawn, highlighting the need for a standardized and robust approach to evaluating mucoadhesion61,62. Recent efforts have been made to develop standardized methodologies for this purpose63. In future work, mucoadhesive properties of the F05 hydrogel should be investigated to optimize its antimicrobial potential and enhance its clinical applicability.
This double application of aPDT has been an interesting strategy to improve the antimicrobial action. In vitro, Nunes et al.64 obtained an inhibition rate of 99.991% of C. albicans proliferation. Successive applications of aPDT leads to increased ROS production, probably due to the accumulation of intracellular metabolites that accentuate the oxidative stress suffered by the fungal cell, leading to a reduction in CFU/mL65.
Also, the successive illuminations, it is possible to reduce the light energy density and the amount of MB to inactivate C. albicans54. The successive applications of PDT are preferable in regard of increasing the illumination time or irradiance, since increased irradiance may lead to photobleaching, and longer irradiation times may make the protocol unfeasible in clinics25.
In this sense, the data obtained corroborate these principles since the single application of 54 min of illumination culminated in an antimicrobial effect of only 1 Log reduction in CFU/mL, while the double treatment presented an antimicrobial effect of 4 Log CFU/mL. The greatest effectiveness of inactivating UFC/mL lies in the incremental damage caused to the cells at each stage of illumination, since in the first exposure to light the cell may suffer small damage, and a new treatment with the MB followed by light exposure, greater damage will be promoted, making self-repair mechanisms impossible54,66. According to Baptista et al.19 there is a close relationship between the physiological state of C. albicans and the efficiency of photoinactivation, since the extracellular matrix of fungal cells with 48 h of growth appears to be the first target of aPDT. This yeast is even more resistant to photodynamic inactivation due to its size and the presence of a nuclear membrane that can present an additional barrier to the penetration of PS, requiring higher doses of both light and PS67. Dias et al.65 suggest that aPDT can reduce the virulence of the fungus and confirm that cells in biofilms are more tolerant to aPDT than in planktonic cultures, since the extracellular polymeric matrix in fungal biofilms provides additional protection to the cells, protecting them from those of oxidative stress, making it difficult for PS to penetrate the biofilm multilayers and the consequent inactivation.
As stated by Machado et al.25 we maintain the hypothesis that the double treatment potentiated the effect of aPDT in the dispersion phase of the C. albicans biofilm, based on the possibility that the initial application was capable of sensitizing the biofilm and causing a slight disruption of the extracellular matrix with inactivation of dispersed cells of yeast and, with the second application of PDT, achieve a deeper penetration of MB into the biofilm, leading to a more effective antimicrobial effect. Considering also that application in the oral cavity will result in the product mixing with saliva leading to the dilution of the PS and consequent reduction of the PDT effect, double application can increase the antimicrobial action in clinical practice. Also, further studies should consider measuring the D/M ratio after diluting the MB formulation with simulated salivary fluid.
It is well-established that the clinical application of aPDT using MB dissolved in water within the oral cavity often does not achieve the same level of efficacy as observed in vitro. This discrepancy is primarily attributed to the low retention of MB at the treatment site, as well as its dilution and aggregation caused by saliva. Consequently, given that the formulation demonstrated increased viscosity without compromising antimicrobial activity in the in vitro model, it warrants further evaluation in clinical settings. Although the irradiation protocol utilized in this study cannot be directly applied to clinical practice, the use of a laser with a higher intensity than the LED employed here may be advantageous for optimizing a clinical treatment protocol.
Further studies should stablish the rheological properties of the formulation, shear and bioadhesion analysis, while optimization of light parameters is also essential.
Conclusions
Thus, the formulation was prepared successfully, increased viscosity was achieved with control of MB aggregation and antimicrobial action similar to MB delivered in water. In this sense, we believe this formulation may improve the aPDT clinical protocols in dentistry, with easy application and similar antimicrobial effects than the water MB.
Methods
Chemicals
MB, SDS and Xylitol were acquired from Sigma-Aldrich (Sant Louis, Missouri, USA), CMC 80% of –COOH functionalization, from Nutrifarm do Brasil (São Paulo, Brazil) and HPMC 7.61% hydroxypropoxyl functionalization and 29.3% of methoxyl, from Lepuge Insumos Farmacêuticos (São Paulo, Brasil, BR). Methylparaben, Propylene glycol, HCl, NaOH and the salts to prepare phosphate buffer saline (PBS) at pH 7.2 (137 mM NaCl, 2.7 mM KCl, 8.1 mM Na2HPO4 and 1.47 mM KH2PO4) were purchased from Synth (Diadema, Brazil).
Stock solutions of 1 mg/mL of MB and 50 mg/mL of SDS were prepared with deionized water. Preservative solution of 100 mg/mL of methylparaben was prepared with propylene glycol. The stock solutions were stored in the dark at room temperature.
Development of formulations
Formulations containing 0.005% MB associated to non-ionic (HPMC) or anionic (CMC) polymers, in three different concentrations (1%, 3% or 5% (w/w) of HPMC and 0.25%, 0.5% or 1% (w/w) of CMC) were prepared in triplicate, as scheme shown in Fig. 6. Other components such as sweetener (5% xylitol), preservative solution (0.1% methylparaben at propylene glicol) and SDS (0.25%) were also added. Also, the formulation with 0.5% CMC and 0.25% SDS was prepared in triplicate in three concentrations of MB: 0.002% (F02), 0.005% (F05) and 0.010% (F10) at pH 5.0 (n = 9).
Scheme presenting different formulations tested. At each line the parameters testes were informed: Line 1: Polymer type; Line 2 Polymer concentration; Line 3: SDS concentration; Line 4: pH; Line 5: MB concentration.
The formulations were prepared by solubilizing xylitol in water and homogenized with MB stock solution. For those with non-ionic polymer, SDS stock solution was added in half the quantity. Separately, one third of the total purified water of the formulation was heated to boiling with the preservative solution and HPMC (1%, 3% and 5%) was added. After cooling, the MB preparations containing or not SDS were added (n = 18).
For formulations with the anionic polymer, CMC (0.25%, 0.5% and 1%) was dispersed in the preservative solution and homogenized with MB preparations. Then, SDS stock solution was added in half the quantity (n = 18). All formulations, at this point, were prepared with 0.005% MB (n = 36).
Also, in order to evaluate the influence of pH, formulations containing 0.005% MB and 0.25% SDS were prepared in triplicate with HPMC (3% and 5%) or CMC (0.25% and 0.5%) at pH 6.5. One part was acidified to pH 5.0 with 0.1 M HCl and another part was alkalinized with 0.1 M NaOH to pH 8.0.
Physico-chemical properties
The viscosity and density of the formulations were determined by sinewave vibro viscometer SV-10 (A&D Company Limited) and density meter DMA 4500 M (Anton-Paar). The calculation of the absolute viscosity based on the results obtained from the specific density, determined with a concentration density meter, was carried out in the same three concentrations of the non-ionic or anionic polymers of the formulations containing, 0.005% MB and 0.25% SDS.
The pH was measured/adjusted using a bench top digital pH meter MPA-210-MS (CAAL). 0.1 M HCl and 0.1 M NaOH were used to adjust pH as acidic (5.0), neutral (6.5) and alkaline (8.0).
Determining the dimer to monomer (D/M) ratio
The absorption spectra of the MB conveyed in formulations were recorded between 250 and 800 nm with a UV–visible spectrophotometer UV-1800 (Shimadzu, Japan), in triplicate, using a 2 mm pathway quartz cuvette. To evaluate aggregation, the dimer to monomer (D/M) ratios were determined by absorption wavelength values at 614 nm (D) and at 662 nm (M), or 623 nm (D) and at 663 nm (M), for formulations containing HPMC or CMC, respectively8.
Stability tests
The formulation containing 0.005% MB, 0.5% CMC, 0.25% SDS (F05), sweetener and preservative, pH 5.0 (the chosen one), was subjected to physicochemical stability tests (organoleptic assessment, determination of pH, monomer quantification at 663 nm and D/M ratio)68 at room temperature (25 °C) for 12 months and to evaluate photochemical effectiveness through in vitro microbiological experiments of uptake and viability in Candida albicans biofilm as described below.
Microbiologial assays
Biofilm formation
The Candida albicans yeast (ATCC 10231) was grown at 37 °C for 24 h on a Sabouraud Dextrose Agar Medium (Kasvi, Curitiba, Brazil). After preparing a suspension in PBS, the number of cells were counted in a Neubauer Chamber and the suspension diluted to reach 1.0 × 108 cells/mL for uptake experiments and 5.0 × 107 cells/mL for viability experiments8,36.
The 24 and 48-well plates were treated with Bovine Fetal Serum (Vitrocell, São Paulo, Brazil) for 24 h. After that, it was removed and 0.20 mL of the yeast suspension were added to the wells, along with Sabouraud Dextrose Broth Medium (Kasvi, Curitiba, Brazil). The plates were incubated at 37 °C, 50 rpm, for 24 h (maturation phase) or 48 h (dispersion phase) for the biofilm formations. The supernatant was discarded and the adhered biofilms were washed with PBS25.
MB uptake in biofilms
The biofilms were exposed to the 1 mL of MB, in water (W05) or F05, and they were kept for 5, 10, 30 and 60 min under dark conditions. After that, 0.8 mL of supernatant were collected in microtubes. Water samples received 0.04 mL of SDS 5%. Samples were centrifuged (5 min at 5.000 rpm) and the absorption spectra were recorded between 250 and 800 nm using a UV–visible UV-1800 spectrophotometer (Shimadzu, Japan), a 2 mm path length cuvette. The samples were tested in triplicate, in two independent experiments. In order to determine the cellular uptake, this formula was used:
where Ic was the initial concentration of MB and Fc meant the final concentration recorded, considering the maximum absorption at 663 nm36.
Biofilm viability experiments
The biofilms were exposed to the 0.2 mL of formulations with MB 0.005% (F05) and MB 0.010% (F10), without MB (FØ), water at pH 5 as control (CT) and water with MB 0.005% (W05) or MB 0.010% (W10) at pH 5. They were kept for 5 min under dark conditions at 25 °C. After this period, the treatments were removed and the biofilms were washed with the PBS and kept at 0.3 mL of PBS to be illuminated with an LED device (Biolambda, São Paulo, Brazil) following the light parameters24,25 presented in Table 2.
Three different experimental conditions were evaluated: 27 min illumination, 54 min illumination and with double application of treatment and illumination for 27 min in each cycle, i.e., application of the PS, washing biofilm, 27 min illumination, PBS removal and another exposure to PS, washing and another 27 min illumination under the same parameters25.
Then, the biofilms were disrupted by multiple pipetting and vortexing for 1 min. An aliquot of 20 µL of each sample was diluted (10–1 to 10–5) and 15 µL of each dilution was seeded in lines into Petri dishes containing Sabouraud dextrose agar culture medium (Kasvi, Curitiba, Brazil). The plates were incubated for 24 h at 37 °C and the number of colony-forming units (CFU/mL) was counted. The samples were tested in triplicate, in three independent experiments25.
Statistical analysis
The statistical analysis was performed by using IBM SPSS Statistics version 22 software. Shapiro–Wilk test was employed to evaluate the data normality. The parametric data were expressed as mean ± standard deviation (viscosity, density and log CFU/mL). The nonparametric data were expressed as median, minimum and maximum (D/M ratio and pH) and these values underwent logarithmic transformation. The one-way or two-way ANOVA tests were performed, depending upon the experiment design followed by the Tukey post-test with a confidence level of 95% (p < 0.05).
Data availability
The datasets used and/or analysed during the current study available from the corresponding author on reasonable request.
References
PAHO. Pan-Americana Health Organization. Annual Report of the Director 2019: Advancing the Sustainable Health Agenda for the Americas 2018–2030. Preprint at (2019).
ANVISA. Confira dados mundiais sobre resistência microbiana. Notícias: Conscientização e Mobilização, 23/11/2021. (Agência Nacional de Vigilância, 2021) Sanitária. https://www.gov.br/anvisa/pt-br/assuntos/noticias-anvisa/2021/confira-dados-mundiais-sobre-resistencia-microbiana#:~:text=Dados da OMS mostram,ou septisemia e pneumonia evitáveis).
WHO. Global Oral Health Status Report: Towards Universal Health Coverage for Oral Health by 2030. https://www.who.int/publications/i/item/9789240061484 (2022).
WHO. 2020 Antibacterial Agents in Clinical and Preclinical Development. (World Health Organization, 2021).
ANVISA. Programa Nacional de Prevenções e Controle de Infecções Relacionadas à Assistência à Saúde (PNPCIRAS) 2021 a 2025. Preprint at https://www.gov.br/anvisa/pt-br/centraisdeconteudo/publicacoes/servicosdesaude/publicacoes/pnpciras_2021_2025.pdf (2021).
CDC. Centers for Disease Control and Prevention. Antibiotic Resistance Threats in the United States, 2019. (U.S Department of Health and Human services, 2019).
Thompson, W. et al. The Essential Role of the Dental Team in Reducing Antibiotic Resistance (FDI World Dental Federation, 2020).
da Collina, G. A. et al. Controlling methylene blue aggregation: A more efficient alternative to treat Candida albicans infections using photodynamic therapy. Photochem. Photobiol. Sci. 17, 1355–1364 (2018).
Filipini, S. M. R. et al. Adjunctive antimicrobial photodynamic therapy using methylene blue/ethanol formulation in experimental periodontitis in diabetic rats: Short-term results. Lasers Med. Sci. 34, 1253–1260 (2019).
Cecatto, R. B. et al. Methylene blue mediated antimicrobial photodynamic therapy in clinical human 11 studies: The state of the art. Photodiagn. Photodyn. Ther. 27, 101828 (2020).
Sousa, J. N. L. et al. Photoinactivation of Candida albicans using methylene blue as photosensitizer. Rev. Gaúch. Odontol. 63, 411–417 (2015).
Teodoro, P. & Fernandes, H. V. The use of photodynamic therapy as an alternative method of treating oral candidiasis. Revista Arquivos Científicos (IMMES) 3, 14–23 (2020).
Prochnow, E. P. et al. Antimicrobial photodynamic effect of phenothiazinic photosensitizers in formulations with ethanol on Pseudomonas aeruginosa biofilms. Photodiagnosis Photodyn. Ther. 13, 291–296 (2016).
Tang, W., Xu, H., Kopelman, R. & Philbert, M. A. Photodynamic characterization and in vitro application of methylene blue-containing nanoparticle platforms. J. Photochem. Photobiol. 81, 242–249 (2005).
Bergmann, K. & O’Konski, C. T. A spectroscopic study of methylene blue monomer, dimer, and complexes with montmorillonite. J. Phys. Chem. 67, 2169–2177 (1963).
Junqueira, H. C. C., Severino, D., Dias, L. G. G., Gugliotti, M. S. S. & Baptista, M. S. S. Modulation of methylene blue photochemical properties based on adsorption at aqueous micelle interfaces. Phys. Chem. Chem. Phys. 4, 2320–2328 (2002).
Pires, B. R. B., de Paoli, F., Mencalha, A. L. & de SouzadaFonseca, A. Photodynamic therapy on mRNA levels in bacteria. Lasers Med. Sci. 39(1), 229 (2024).
Ambrósio, J. A. R. et al. BSA nanoparticles loaded-methylene blue for photodynamic antimicrobial chemotherapy (PACT): Effect on both growth and biofilm formation by Candida albicans. J. Biomater. Sci. Polym. Ed. 31, 2182–2198 (2020).
Baptista, A. et al. Photodynamic damage predominates on different targets depending on cell growth phase of Candida albicans. J. Photochem. Photobiol. B 177, 76–84 (2017).
Silva, A. R. et al. New insights in phenothiazinium-mediated photodynamic inactivation of Candida Auris. J. Fungi 9(7), 717 (2023).
Cabral, F. V. et al. New insights in photodynamic inactivation of Leishmania amazonensis: A focus on lipidomics and resistance. PLoS ONE 18(9), e0289492 (2023).
Cabral, F. V. et al. Photodynamic therapy offers a novel approach to managing miltefosine-resistant cutaneous leishmaniasis. Biomed. Pharmacother. 177, 116881 (2024).
Nuñez, S. C., Garcez, A. S., Gomes, L., Baptista, M. S. & Ribeiro, M. S. Methylene blue aggregaton in the presence of human saliva. Proc. SPIE 6846, 1–7 (2008).
Gonçalves, J. M. L. A., Monteiro, C. M., Machado, G. B. & Pavani, C. The combination of methylene blue and sodium dodecyl sulfate enhances the antimicrobial photodynamic therapy of Candida albicans at lower light parameters. Photodiagnosis Photodyn. Ther. 42, 103583 (2023).
Machado, G. B., Monteiro, C. M., Gonçalves, J. M. L. A. & Pavani, C. Enhancing antimicrobial photodynamic therapy with phenothiazinium dyes and sodium dodecyl sulfate against Candida albicans at various growth stages. Photodiagnosis Photodyn. Ther. 42, 103628 (2023).
Farias-da-Silva, F. F., Benine-Warlet, J., Groppo, F. C. & Steiner-Oliveira, C. Potentiation of antimicrobial photodynamic therapy with potassium iodide and methylene blue: Targeting oral biofilm viability. Photochem. Photobiol. Sci. 23(12), 2255–2263 (2024).
Lewis, G. N., Goldschmid, O., Magel, T. T. & Bigeleisen, J. Dimeric and other forms of methylene blue: Absorption and fluorescence of the pure monomer. J. Am. Chem. Soc. 65, 1150–1154 (1943).
Silvestre, A. L. P. et al. Current applications of drug delivery nanosystems associated with antimicrobial photodynamic therapy for oral infections. Int. J. Pharm. 592, 120078 (2021).
Feksa, L. R. et al. Hydrogels for biomedical applications. In Nanostructures for the Engineering of Cells, Tissues and Organs, From Design to Application 403–438 (Elsevier, 2018).
Villanova, J. C. O., Oréfice, R. L. & Cunha, A. S. Pharmaceutical applications of polymers. Polímeros 20, 51–64 (2010).
Garg, A., Agrawal, R., Singh Chauhan, C. & Deshmukh, R. In-situ gel: A smart carrier for drug delivery. Int. J. Pharm. 652, 123819 (2024).
da Silva, J. B. et al. Boosting the photodynamic activity of erythrosine B by using thermoresponsive and adhesive systems containing cellulose derivatives for topical delivery. Int. J. Biol. Macromol. 245, 125491 (2023).
Thompson, J. E. & Davidow, L. W. A Practical Guide to Contemporary Pharmacy Practice (Lippincott Williams and Wilkins, 2009).
Sigma-Aldrich. Product Specification: Carboxymethylcellulose sodium salt - Medium viscosity. C4888 https://www.sigmaaldrich.com/BR/pt/product/sigma/c4888 (2023).
da Silva, J. B., Cook, M. T. & Bruschi, M. L. Thermoresponsive systems composed of poloxamer 407 and HPMC or NaCMC: Mechanical, rheological and sol-gel transition analysis. Carbohyd. Polym. 240, 1162683 (2020).
da Collina, G. A. et al. Photodynamic antimicrobial chemotherapy action of phenothiazinium dyes in planktonic Candida albicans is increased in sodium dodecyl sulfate. Photodiagnosis Photodyn. Ther. 29, 101612 (2020).
da Collina, G. A. et al. The importance of combining methods to assess Candida albicans biofilms following photodynamic inactivation. Photodiagnosis Photodyn. Ther. 38, 102769 (2022).
Xu, J. et al. Matrix effect on singlet oxygen generation using methylene blue as photosensitizer. Inorganics 12(6), 155 (2024).
Nuñez, S. C. et al. Urea enhances the photodynamic efficiency of methylene blue. J. Photochem. Photobiol. B 150, 31–37 (2015).
Huang, T.-C., Chen, C.-J., Ding, S.-J. & Chen, C.-C. Antimicrobial efficacy of methylene blue-mediated photodynamic therapy on titanium alloy surfaces in vitro. Photodiagnosis Photodyn. Ther. 25, 7–16 (2019).
Allen Jr, L. V., Adejare, A., Desselle, S. P., Felton, L. A. & Moffat, A. C. Remington: The Science and Practice of Pharmacy. (Pharmaceutical Press, 2012).
Vilsinski, B. H. et al. Photophysics and drug delivery behavior of methylene blue into Arabic-gum based hydrogel matrices. Mater. Today Commun. 26, 1–9 (2021).
George, S. & Kishen, A. Photophysical, photochemical, and photobiological characterization of methylene blue formulations for light-activated root canal disinfection. J. Biomed. Opt. 12(3), 1–10 (2007).
De Vito, A., Romão Júnior, W. Manipulação Dos Biomateriais Odontológicos Diretos - Guia Prático Visual V.1. 345, (Universidade Nove de Julho – UNINOVE, São Paulo, 2022).
Sakae, L. O. et al. An in vitro study on the influence of viscosity and frequency of application of fluoride/tin solutions on the progression of erosion of bovine enamel. Arch. Oral Biol. 89, 26–30 (2018).
Sharma, M., Dube, A. & Majumder, S. K. Antibacterial photodynamic activity of photosensitizer-embedded alginate-pectin-carboxymethyl cellulose composite biopolymer films. Lasers Med. Sci. 36, 763–772 (2021).
Bonneau, R., Pottier, R., Bagno, O. & Joussot-Dubien, J. pH dependence of singlet production in aqueous solutions using thiazine dyes as photosensitizers. Photochem. Photobiol. 21, 159–163 (1975).
Luo, Y. et al. Visible light mediated killing of multidrug-resistant bacteria using photoacids. J. Mater. Chem. B 1(7), 997–1001 (2013).
Gusman, D. J. R. et al. pH influences the biocompatibility of methylene blue solutions. Clin. Oral Investig. 22, 361–367 (2018).
Chen, J., Cesario, T. C. & Rentzepis, P. M. Effect of pH on methylene blue transient states and kinetics and bacteria photoinactivation. J. Phys. Chem. A 115, 2702–2707 (2011).
Núñez, S. C. et al. Effects of ionic strength on the antimicrobial photodynamic efficiency of methylene blue. Photochem. Photobiol. Sci. 13(3), 595–602 (2014).
Hemdan, S. S. The shift in the behavior of methylene blue toward the sensitivity of medium: Solvatochromism, solvent parameters, regression analysis and investigation of cosolvent on the acidity constants. J. Fluoresc. 33(6), 2489–2502 (2023).
Prates, R. A., Kato, I. T., Ribeiro, M. S., Tegos, G. P. & Hamblin, M. R. Influence of multidrug efflux systems on methylene blue-mediated photodynamic inactivation of Candida albicans. J. Antimicrob. Chemother. 66, 1525–1532 (2011).
Torres-Hurtado, S. A. et al. Efficient in vitro photodynamic inactivation using repetitive light energy density on Candida albicans and Trichophyton mentagrophytes. Photodiagnosis Photodyn. Ther. 26, 203–209 (2019).
Wiench, R. et al. Influence of incubation time on ortho-toluidine blue mediated antimicrobial photodynamic therapy directed against selected candida strains—An in vitro study. Int. J. Mol. Sci. 22, 10971 (2021).
Tasso, T. T. & Baptista, M. S. Photosensitized oxidation of intracellular targets: Understanding the mechanisms to improve the efficiency of photodynamic therapy. Methods Mol. Biol. 2451, 261–283 (2022).
Liang, P., Kolodieznyi, D., Creeger, Y., Ballou, B. & Bruchez, M. P. Subcellular singlet oxygen and cell death: Location matters. Front. Chem. 8, 592941 (2020).
Oliveira, C. S., Turchiello, R., Kowaltowski, A. J., Indig, G. L. & Baptista, M. S. Major determinants of photoinduced cell death: Subcellular localization versus photosensitization efficiency. Free Radic. Biol. Med. 51, 824–833 (2011).
Gabrielli, D., Belisle, E., Severino, D., Kowaltowski, A. J. & Baptista, M. S. Binding, aggregation and photochemical properties of methylene blue in mitochondrial suspensions. Photochem. Photobiol. 79, 227–232 (2007).
Severino, D., Junqueira, H. C., Gugliotti, M., Gabrielli, D. S. & Baptista, M. S. Influence of negatively charged interfaces on the ground and excited state properties of methylene blue. Photochem. Photobiol. 77, 459–468 (2003).
Woertz, C., Preis, M., Breitkreutz, J. & Kleinebudde, P. Assessment of test methods evaluating mucoadhesive polymers and dosage forms: An overview. Eur. J. Pharm. Biopharm. 85(3), 843–853 (2013).
Bassi da Silva, J., Ferreira, S. B. S., Reis, A. V., Cook, M. T. & Bruschi, M. L. Assessing mucoadhesion in polymer gels: The effect of method type and instrument variables. Polymers (Basel) 10(3), 254 (2018).
Amorós-Galicia, L. et al. Development of a standardized method for measuring bioadhesion and mucoadhesion that is applicable to various pharmaceutical dosage forms. Pharmaceutics 14(10), 1995 (2022).
Nunes, I. P. F. et al. Evaluation of dual application of photodynamic therapy — PDT in Candida albicans. Photodiagnosis Photodyn. Ther. 42, 1–10 (2023).
Dias, L. M. et al. The effect of sub-lethal successive applications of photodynamic therapy on Candida albicans biofilm depends on the photosensitizer. J. Fungi 9, 111 (2023).
Melendez-Celis, U. et al. Organic light emitting diode for in vitro antimicrobial photodynamic therapy of Candida strains. Photodiagnosis Photodyn. Ther. 36, 102567 (2021).
Demidova, T. N. & Hamblin, M. R. Effect of cell-photosensitizer binding and cell density on microbial photoinactivation. Antimicrob. Agents Chemother. 49, 2329–2335 (2005).
BRASIL. Farmacopeia Brasileira. vol. I (Ministério da Saúde. Agência Nacional de Vigilância Sanitária, Brasília, 2019).
Acknowledgements
The authors would like to express their sincere gratitude to Professors Iolanda Midea Cuccovia and Omar Abdel Moneim Abou El Seoud, from the Institute of Chemistry at the University of São Paulo (USP), for kindly granting access to the laboratory equipment used for the viscosity and density measurements of the formulations. The authors thank the São Paulo Research Foundation (FAPESP) for the financial support of this research (Grant Numbers 2016/03037–0); CP thanks National Council for Scientific and Technological Development—CNPq for the Research Fellowship (305373/2023-4) and Coordination for the Improvemente of Higher Education Personnel (CAPES) - PROEX 1294/2023 - Postgraduate Program in Biophotonics applied to Health Sciences/Biophotonics Medicine. This study was financed in part by the Coordination of Higher Education Personnel Improvement—Brasil (CAPES)—Finance Code 001, CMM thanks CAPES for the fellowship (88887.940996/2024-00).
Author information
Authors and Affiliations
Contributions
CMM: Investigation; Resources; Data curation, Formal analysis; Funding acquisition; Visualization; Writing—Original Draft. JMLAG: Investigation; Writing—Original Draft. GBM: Investigation; Writing—Original Draft. OCN: Methodology; Writing—Review & Editing. RAP: Investigation; Methodology; Writing—Review & Editing. CF: Methodology; Formal analysis; Visualization; Supervision; Writing—Review & Editing. CP: Investigation; Methodology; Conceptualization, Formal analysis; Funding acquisition; Project administration; Supervision; Validation; Writing—Review & Editing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Monteiro, C.M., Gonçalves, J.M.L.A., Machado, G.B. et al. Viscous methylene blue formulation for antimicrobial photodynamic therapy in dentistry. Sci Rep 15, 15751 (2025). https://doi.org/10.1038/s41598-025-98568-x
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-98568-x
Keywords
This article is cited by
-
Beta-lactam antibiotics under light: optical and photochemical characterization
Photochemical & Photobiological Sciences (2025)