Abstract
This study aimed to explore the associations between various lipid parameters and the risk of gallstone disease (GSD). A multicenter cross-sectional study was conducted to explore the associations between nine lipid parameters and the risk of GSD. Multivariable logistic regression models, adjusted for covariates, were employed to evaluate these associations. Stratified analyses by age and sex were performed to assess population-specific effects. Data from multiple centers were integrated using meta-analysis to generate pooled odds ratios with 95% confidence intervals. Trial Sequential Analysis (TSA) was implemented to determine the sufficiency of the sample size and the robustness of the associations under cumulative evidence conditions. This multicenter study included 580,935 participants, with a GSD prevalence of 7.43%. After adjusting for covariables, the combined multi-center results showed that total cholesterol, high-density and low-density lipoprotein cholesterol, and non-HDL cholesterol were negatively associated with GSD risk. In contrast, the Castelli risk index I and II, atherogenic coefficient, and atherogenic index of plasma were positively associated with the risk of GSD. Subgroup analyses and sensitivity analyses yielded consistent results. Stratified analysis revealed distinct lipid-gallstone associations between people with cholecystectomy and gallbladder stones. TSA revealed that the required amount of information has been achieved, and the results are conclusive. This study suggests significant associations between lipid metabolism and the risk of GSD. There are differences in the relationship between blood lipid indexes and cholecystectomy and gallstones. These findings not only enhance our understanding of the relationship between lipid metabolism and GSD but also provide a novel perspective for risk assessment and prevention strategies.
Similar content being viewed by others
Introduction
Gallstone disease (GSD) is one of the most prevalent disorders within the digestive system1. Its global prevalence varies significantly by region, with the highest rates observed in the Americas, followed by Africa, Europe, and Asia2,3. Notably, in China, the prevalence of GSD is significantly higher than the overall level in Asia and is increasing rapidly4. This trend is partly attributed to the acceleration of urbanization and the rise in unhealthy lifestyle patterns, such as high-fat diets and insufficient physical activity, which have contributed to the annual increase in GSD incidence5,6. Although the mortality rate associated with GSD is relatively low, failure to promptly treat and manage GSD and its associated complications can result in severe consequences, including liver damage, liver failure, biliary tract infections (e.g., cholangitis), pancreatitis, diabetes, and increased all-cause mortality7,8,9,10,11. Consequently, early detection, preventive measures, and timely intervention for GSD are of substantial public health significance.
Despite significant advances in hepatobiliary pathophysiology, the precise mechanisms underlying GSD formation remain incompletely understood. Numerous studies have demonstrated that disruptions in serum sterol metabolism, imbalances in bile components, insulin resistance (IR), and other factors are intricately associated with the onset of GSD12. Current epidemiological investigations have predominantly focused on conventional lipid parameters, including total cholesterol (TC), triglycerides (TG), low-density lipoprotein cholesterol (LDL-C), and high-density lipoprotein cholesterol (HDL-C), for GSD risk stratification13. However, these isolated measurements may inadequately capture the complex lipid metabolic derangements associated with GSD risk.
With growing recognition of the association between abnormal lipid profiles and various diseases, non-traditional lipid indicators—such as non-high-density lipoprotein cholesterol (non-HDL), the Castelli risk index, and the atherogenic index—have garnered attention as complementary measures to traditional lipid metrics14,15,16. Previous studies have explored the associations between these non-traditional lipid parameters and the risk of GSD17,18,19. However, due to limitations in data and other factors, the relationships between lipid-related indicators and the risk of GSD still require in-depth validation using large sample sizes. Moreover, most prior research has focused on populations in the United States, with relatively fewer studies conducted on Chinese populations.
Given these gaps, this study conducts a large-scale, multicenter, cross-sectional investigation using population-based data to examine the relationship between both traditional and non-traditional lipid indicators and the risk of GSD formation. This research aims to fill the existing knowledge gaps and provide a more comprehensive understanding of the role of lipid metabolism in GSD, particularly in the Chinese population. Trial Sequential Analysis (TSA) was also implemented to determine the sufficiency and the robustness of the results.
Result
Baseline characteristics of subjects in four hospitals
This cross-sectional study recruited a total of 580,935 participants from four hospitals, including 43,170 individuals diagnosed with gallstone disease (GSD) and 537,765 individuals without GSD. The baseline characteristics and laboratory findings of the participants are presented in Table 1.
Among the 142,088 participants enrolled from the hospital in Liangjiang New Area, 7.66% (10,881 cases) were diagnosed with GSD. In the hospital in Kaizhou District, 8.81% (25,735 cases) of the 292,210 participants were identified with GSD. For the Hospital in Qianjiang District (70,615 participants) and the hospital in Beijing (76,022 participants), the detection rates of GSD were 3.41% (2,413 cases) and 5.45% (4,141 cases), respectively.
Compared with the non-GSD group, the GSD group exhibited significantly advanced age, higher level of urea nitrogen (UN), uric acid (UA), globulin (GLB), and higher proportion of abnormal blood glucose, kidney stones, fatty liver, and hypertension. In contrast, albumin levels and the albumin-to-globulin ratio (A/G) were significantly higher in the healthy control group. Among the nine lipid profile indicators, all were significantly elevated in the GSD group compared with the non-GSD group, except for high-density lipoprotein cholesterol (HDL-C) (all P < 0.001).
The associations between lipid profile indexes and the risk of GSD
When lipid indicators were analyzed as categorical variables, taking the results from the hospital in Liangjiang New Area as an example, the multivariable logistic regression analysis revealed that, higher level of TC, HDL-C, LDL-C, non-HDL were negatively associated the risk of GSD. In contrast, the CRI1, CRI2, AC, and AIP were positively associated the GSD risk. No significant associations were found between TG and GSD risk (Table 2). The results were not entirely consistent across other centers.
When lipid indicators were analyzed as continuous variables, again taking the results from the hospital in Liangjiang New Area as an example, each unit or standard deviation (SD) increase in TC, HDL-C, LDL-C, non-HDL were negatively associated with GSD risk, Conversely, each unit or SD increase in TG, CRI1, CRI2, AC, and AIP were positively associated with the risk of GSD (Table 2). The results were not completely consistent across other centers.
The pooled associations between lipid profile indexes and GSD risk
The meta-analysis pooled results from four centers demonstrated significant protective associations between elevated levels of conventional lipid markers (TC, HDL-C, LDL-C, and non-HDL cholesterol) and gallstone disease risk. Conversely, higher values of non-traditional indices (CRI1, CRI2, atherogenic coefficient and AIP) demonstrated significant positive associations with GSD risk. Triglyceride levels, however, showed no statistically significant association with gallstone risk in categorical analyses (Fig. 1).
The forest plot for the pooled associations between nine lipid parameters and the risk of GSD.
When analyzed as continuous variables, consistent protective effects were observed in TC, HDL-C, LDL-C, and non-HDL cholesterol, with each unit increment corresponding to significantly reduced GSD risk. In contrast, per-unit increases in TG, CRI1, AC and AIP were significantly associated with elevated GSD risk. No significant association was detected for continuous CRI2 measurements (pooled OR = 1.010; 95%CI: 0.980–1.041).
The direction and significance of associations remained robust when scaled by standard deviation increments. Each standard deviation (SD) increase in conventional lipid parameters persistently correlated with reduced GSD risk, while SD increments in CRI1, AC and AIP maintained significant positive associations. Neither TG nor CRI2 exhibited statistically significant relationships with GSD risk when analyzed per SD increase.
These associations remained consistent when stratified by age and sex (Table 3).
Comparison of results between cholecystectomy and gallstones and sensitivity analysis excluding specific metabolic diseases structure
We further stratified the outcomes into cholecystectomy and gallbladder stones. Due to the unavailability of stratified outcome data from Hospital in Qianjiang District, the analysis was restricted to the three remaining centers, with detailed results presented in Table SW. Meta-analysis of the three centers revealed that when lipids were treated as categorical variables, TC, HDL-C, CRI1, CRI2, AC, and AIP were significantly associated with gallstone formation, with TC and HDL-C acting as protective factors and the remainder as risk factors. These associations were largely consistent with those observed in the cholecystectomy population; however, in the latter, we also identified a positive association between TG and cholecystectomy, as well as inverse associations for LDL-C and non-HDL-C.
To evaluate the robustness of our findings, we conducted a series of sensitivity analyses by systematically excluding specific subpopulations. As detailed in Table SY, exclusion of individuals with fatty liver did not materially alter the observed associations. Similarly, when obese individuals (BMI ≥ 28 kg/m2) were excluded (Table SZ), and when participants with dysglycemia (fasting blood glucose > 7.0 mmol/L) were excluded (Table SX), the results remained largely consistent with those derived from the full population. Hospital in Qianjiang District was excluded from the dysglycemia sensitivity analysis due to lack of glucose data. The consistency of findings across these sensitivity analyses reinforces the robustness of our primary results.
Results of trial sequential analysis (TSA) of lipid indices
The TSA plot revealed that all nine lipid profile indicators crossed both the conventional boundary and the TSA monitoring boundary, achieving the required information size (Fig. 2). This demonstrates that the current study provides robust and conclusive evidence, eliminating the need for additional studies to further validate these findings.
Trial Sequential Analysis plot for the associations between nine lipid parameters and the risk of GSD. The plot for TC (A), TG (B), HDL-C (C), LDL-C (D), non-HDL-C (E), CRI 1 (F), CRI 2 (G), AC (H), AIP (I).
Discussion
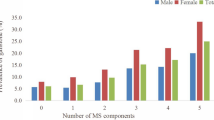
This study employed a multicenter cross-sectional design, enrolling 580,935 participants from four hospitals. Of note, significant variations were observed in both the detection rate of gallstones and the association between blood lipid indicators and gallstone presence across the participating hospitals, with Hospital of Qianjiang district exhibiting the most distinct pattern. These disparities may be attributable to regional epidemiological differences—specifically, a lower incidence of gallstone disease in northern China compared with southwestern China20. Furthermore, the unique dietary habits prevalent among ethnic minority populations in the Qianjiang region may contribute to the differential gallstone incidence observed there. It is also noteworthy that across all study sites, the number of female gallstone patients was significantly higher than that of males, a finding consistent with previously published epidemiological data20,21,22. Because of the heterogeneity across multiple centers, we did not use direct pooling of data for analysis. Instead, a meta-analysis was subsequently conducted to pool the results, aiming to comprehensively and systematically elucidate the associations between traditional and non-traditional lipid profiles and the risk of GSD. The pooled results indicated that TC, LDL-C, and HDL-C were inversely associated with GSD risk, while TG showed no significant overall association. This lack of association may be due to the fact that TG does not directly participate in GSD formation. However, subgroup analyses revealed a positive correlation between TG and GSD in individuals over 60 years of age and in females, which is consistent with previous findings23. This phenomenon may be related to estrogen secretion in women and slower lipid metabolism observed in the elderly population.
The specific mechanisms through which lipids contribute to GSD formation remain unclear. The relationships between TC, LDL-C, and GSD are particularly controversial. Some studies suggest a positive association, while others report an inverse association, and some find no association at all4,19,24,25,26,27. A study by Zhang et al. demonstrated that higher TC and LDL-C levels were significantly associated with a reduced risk of GSD, aligning with our findings13. Similarly, Chen et al. identified lower TC levels and higher TG levels as independent risk factors for GSD, potentially due to compensatory cholesterol secretion by the liver and reduced bile acid secretion19.The inverse associations between TC, LDL-C, and gallstone formation observed in this study are consistent with findings from multiple cross-sectional and Mendelian randomization studies18,28 The large sample size in the present analysis further strengthens the robustness of these results. However, the underlying mechanisms by which TC and LDL-C may confer protection against gallstone development remain unclear. One plausible explanation is that intrahepatic cholesterol levels exert a more direct influence on gallstone pathogenesis than serum cholesterol concentrations19. Additionally, different biological pathways through which plasma LDL-C is reduced may have divergent—and sometimes opposing—effects on gallstone risk29. HDL-C is a well-established protective factor against GSD, facilitating the reverse transport of cholesterol from peripheral tissues (including the gallbladder) to the liver, thereby reducing cholesterol deposition in bile and lowering the risk of gallstone formation4,30,31.
Emerging evidence suggests that non-traditional lipid indices, derived from conventional lipid measurements, demonstrate superior predictive capacity for metabolic disorders compared to individual lipoprotein assessments32,33. These composite biomarkers integrate multifaceted lipid metabolism information, yet their association with cholelithiasis pathogenesis remains insufficiently characterized. Our multi-center pooled analyses demonstrated significant associations between novel atherogenic indices and GSD formation risk, providing critical insights into the pathophysiological interplay between metabolic dysregulation and biliary stone development.
Notably, non-high-density lipoprotein cholesterol (non-HDL-C), calculated as total cholesterol minus HDL-C and encompassing atherogenic lipoproteins including LDL-C, VLDL-C, IDL-C, and Lp(a), exhibited an inverse correlation with cholelithiasis incidence, potentially attributable to its predominant LDL-derived composition (≈70%) modulating cholesterol trafficking and crystallization dynamics.
Multivariable regression analyses identified four atherogenic indices as independent risk predictors: CRI 1, CRI 2, AC, and AIP, with AIP demonstrating the strongest positive correlation. A large-scale study using the NHANCE database demonstrated a significant non-linear association between elevated AIP and cholelithiasis incidence (adjusted OR: 1.45; 95% CI: 1.09–1.93), with diabetes mellitus identified as a mediating factor33. Meanwhile, Cheng Q et al. found that elevated AC (non-HDL to HDL ratio) was associated with an increased incidence of cholelithiasis using the NHANCE database being consistent with our findings32. The mechanistic convergence of atherogenic indices and GSD formation appears rooted in shared metabolic dysregulation. Multiple plausible mechanisms may account for the positive association between AIP and AC with GSD pathogenesis. First, dyslipidemia induces systemic metabolic perturbations involving hepatic and biliary systems. Specifically, hyperlipidemia promotes hepatic cholesterol hypersecretion while reducing biliary phospholipid content, thereby disrupting cholesterol solubility and creating supersaturated bile conducive to lithogenesis34. Second, insulin resistance emerges as a critical intermediary in this pathophysiological axis. Recent studies have demonstrated a nonlinear dose–response relationship between insulin resistance and AIP levels, characterized by progressive elevation of AIP with declining insulin sensitivity35. This metabolic state enhances biliary cholesterol saturation through dual pathways: (1) hyperlipidemia-induced inactivation of FoxO1 transcription factor upregulates hepatic cholesterol transporters ABCG5/G8, augmenting biliary cholesterol excretion; (2) insulin resistance directly promotes ABCG5/ABCG8 expression, further increasing biliary cholesterol concentration and accelerating crystal nucleation. Concurrently, insulin resistance-mediated downregulation of farnesoid X receptor (FXR) signaling impairs bile acid biosynthesis, exacerbating cholesterol supersaturation and lithogenicity36,37. Collectively, these interrelated pathways establish a mechanistic framework linking dyslipidemia, insulin resistance, and gallstone formation.
Interestingly, stratified analyses in our study revealed distinct associations of TG, LDL-C, non-HDL-C, and atherogenic coefficient (AC) between patients who underwent cholecystectomy and those with gallbladder stones. These differences may be attributed to alterations in lipid metabolism profiles following gallbladder removal, as supported by previous evidence38,39. Moreover, both gallstone patients and those with a history of cholecystectomy exhibited significantly higher atherogenic index of plasma (AIP) compared with healthy controls, suggesting AIP may serve as a valuable and potential predictive marker in both clinical populations.
Notably, existing investigations into the association between novel lipid biomarkers and GSD have been exclusively based on U.S. populations, with no studies conducted in Chinese cohorts31,32. Moreover, prior research has primarily utilized the NHANCE database characterized by limited sample sizes. This large-scale, multicenter study in Chinese populations addresses this critical gap by providing the first evidence from an East Asian cohort. Using TSA, we dynamically monitored cumulative evidence for nine lipid biomarkers. The results demonstrated that all cumulative Z-curves for odds ratios (ORs) crossed both the conventional α-boundary and the pre-specified information boundary, validating the robustness of the findings.
However, several limitations merit acknowledgment. First, the cross-sectional nature of this investigation inherently limits our ability to determine causal associations between GSD and lipid biomarkers, as this design cannot establish temporality or exclude reverse causation. Second, residual confounding from unmeasured variables (e.g., genetic predispositions) persists; critically, lifestyle factors (diet, physical activity), detailed dietary patterns and drugs related to lipid metabolism were unavailable in our retrospective dataset, preventing adjustment. Third, the retrospective nature of the ultrasound data collection imposed constraints: standardized sonographer training protocols and prospective quality control measures for diagnostic criteria were not implemented, potentially introducing inter-observer variability. Future longitudinal cohort studies and randomized controlled trials (RCTs) are necessary to confirm these associations and explore underlying mechanisms.
Method
Study participant
This multicenter cross-sectional study, titled "A Multicenter Cohort Study on the Risk Factors for Gallstone Disease in the Physical Examination Population" (Registration number: ChiCTR2500095891), was conducted across four tertiary care hospital in China from January 2015 to May 2020. The participating centers included a tertiary hospital in Qianjiang District, Chongqing; a tertiary hospital in Kaizhou District, Chongqing; a tertiary hospital in Liangjiang New Area, Chongqing; and a tertiary hospital in Beijing city.
Eligible participants were systematically recruited from the health screening centers of these institutions using strict inclusion criteria: (a) completion of abdominal ultrasonography in accordance with standardized diagnostic protocols; and (b) availability of comprehensive demographic, anthropometric, and biochemical data. The dataset encompassed information on age, sex, height, weight, blood glucose levels, diastolic blood pressure (DBP) and systolic blood pressure (SBP), liver and kidney function indicators, as well as medical histories of conditions such as fatty liver and kidney stones. For participants who had undergone multiple health examinations, only the most recent data were used to ensure the currency and relevance of the information.
Ethical approval for this study was obtained from the ethics committee of West China Fourth Hospital and West China School of Public Health, Sichuan University (approval number: Gwll2021055). The study strictly adhered to the ethical guidelines stipulated in the 1964 Declaration of Helsinki and all subsequent amendments, ensuring the highest standards of ethical conduct in human-subject research. This study is a retrospective analysis of non-identifiable researcher-collected data, human consent to participate statements do not apply. We confirm that: The research does not involve any human experimentation; No identifiable subject data or biological materials were utilized; No personal privacy concerns or commercial interests are implicated in this work.
Laboratory examinations and indices
Fasting blood samples were collected from study participants and analyzed within one hour in the laboratories of the participating hospitals. Using biochemical analyzers, a comprehensive panel of serum biochemical parameters was carefully measured. These parameters included high-density lipoprotein cholesterol (HDL-C), low-density lipoprotein cholesterol (LDL-C), total cholesterol (TC), triglycerides (TG), fasting blood glucose (FBG), systolic blood pressure (SBP), diastolic blood pressure (DBP), total bilirubin (T-bil), direct bilirubin (D-bil), alanine transaminase (ALT), aspartate transaminase (AST), gamma-glutamyl transferase (GGT), creatinine (Cr), uric acid (UA), urea nitrogen (UN), albumin (ALB), globulin (GLB), and the albumin-to-globulin ratio (A/G). However, there are differences in the examination items among different centers, and a few indicators are missing. Each hospital strictly followed internationally recognized standard protocols for biochemical measurements, ensuring the accuracy, reliability, and comparability of the data. Subsequently, several lipid-related indices were calculated using well-established formulas:
-
Non-high-density lipoprotein-cholesterol (non-HDL-C) = (TC—HDL-C);
-
Castelli risk index—I (CRI 1) = (TC/HDL-C);
-
Castelli risk index—II (CRI 2) = (LDL-C/HDL-C);
-
The atherogenic coefficient (AC) = ((TC—HDL—C)/HDL—C).;
-
The atherogenic index of plasma (AIP) = (log(TG/HDL—C)).
Definitions
Ultrasonography examinations were performed by highly experienced radiologists. The diagnosis of GSD was established based on one or both of the following criteria: (i) The presence of one or more hyperechoic structures within the gallbladder or biliary system, which exhibited acoustic shadowing or demonstrated gravity-dependent movement; (ii) In patients who had previously undergone cholecystectomy due to gallstones, the absence of gallbladder visualization on ultrasonography was considered evidence of a prior GSD diagnosis13.
In this cross-sectional study, we defined the fasting blood glucose variable > 7 mmol/L as an abnormal blood glucose level. And lipid markers were categorized into three distinct groups according to the clinical diagnostic criteria. The classification details are as follows: TG (mmol/L): > 5.7, 3.1–5.7, and < 3.1; TG (mmol/L): > 1.7, 0.4–1.7, and < 0.4; LDL-C (mmol/L): > 3.1, 2.07–3.1, and < 2.07; HDL-C (mmol/L): > 2.0, 0.9–2.0, and < 0.9. Additionally, non-HDL cholesterol, CRI1, CRI2, AC, and AIP were divided into three groups based on the interquartile range: > IQR, IQR, and < IQR.
Statistical analysis
In this cross-sectional study, statistical analysis was performed using SPSS software version 19 (IBM, USA). Missing data were addressed using multiple imputation (MI). All continuous variables exhibited non-normal distributions and were thus expressed as medians and interquartile ranges (IQR), denoted as P50 (P25, P75). Comparisons between the GSD and non-GSD groups were conducted using the Wilcoxon rank-sum test. Categorical variables were presented as counts and percentages, with intergroup comparisons performed using the chi-square test.
The adjustment set was selected based on a pre-specified Directed Acyclic Graph (DAG), which was developed by integrating established clinical knowledge with the variables actually available in our retrospective multicenter dataset (Fig. 3). Then a multivariable logistic regression model was employed to evaluate the associations between nine key lipid indicators and the risk of GSD. Lipid parameters were analyzed both as categorical variables and as continuous variables to assess their relationships with the risk of GSD, with subgroup analyses conducted by age and gender. Comprehensive Meta-Analysis (CMA) software was used to pool the results across four hospitals, generating pooled odds ratios (OR) and 95% confidence intervals (CI). Heterogeneity was assessed using Cochran’s Q test, with the magnitude of heterogeneity quantified by the I2 statistic. When significant heterogeneity was present (I2 ≥ 50%), the DerSimonian and Laird random-effects model was applied; otherwise, a fixed-effects model was used. Forest plots were generated using R version 4.3. Trial Sequential Analysis (TSA) was conducted using Stata 17.0 to determine the sufficiency of the sample size and the robustness of the results. TSA was performed based on the pooled data from multiple centers, incorporating both higher-level and highest-level groups. A 2 × 2 contingency table was constructed, and the relative risk reduction (RRR) values were calculated using the combined odds ratios (OR). The statistical power analysis was conducted with a type I error rate (α) of 0.05 and a type II error rate (β) of 0.2.
Directed acyclic graphs between blood lipid indexes and gallstones.
Conclusion
This study underscores the pivotal role of lipid metabolic dysregulation in GSD pathogenesis, revealing that TC, HDL-C, LDL-C, and non-HDL-C are negatively correlated with the risk of GSD. Conversely, elevated levels of the CRI1, CRI2, AC, and AIP are significantly associated with an increased risk of GSD. The above results were different between cholecystectomy and gallbladder stones. These findings not only elucidate the underlying mechanisms of GSD, but also establish a comprehensive risk stratification framework that integrates lipid homeostasis biomarkers. This framework holds substantial potential for clinical translation, offering a novel and practical approach for early risk assessment, targeted prevention, and personalized management of GSD. By integrating these lipid parameters into clinical practice, our study provides actionable insights to enhance the precision of GSD prevention and improve patient outcomes.
Data availability
The datasets generated during and analysed during the current study are not publicly available due to the confidentiality of multi-center collaboration but are available from the corresponding author on reasonable request.
Abbreviations
- GSD:
-
Gallstone disease
- TC:
-
Total cholesterol
- TG:
-
Triglycerides
- LDL-C:
-
Low-density lipoprotein cholesterol
- HDL-C:
-
High-density lipoprotein cholesterol
- non-HDL-C:
-
Non-high-density lipoprotein-cholesterol
- CRI 1:
-
Castelli risk index–I
- CRI 2:
-
Castelli risk index–II
- AC:
-
Atherogenic coefficient
- AIP:
-
Atherogenic index of plasma
- FBG:
-
Fasting blood glucose
- SBP:
-
Systolic blood pressure
- DBP:
-
Diastolic blood pressure
- T-bil:
-
Total bilirubin
- D-bil:
-
Direct bilirubin
- ALT:
-
Alanine transaminase
- AST:
-
Aspartate transaminase
- GGT:
-
Gamma-glutamyl transferase
- Cr:
-
Creatinine
- UA:
-
Uric acid
- UN:
-
Urea nitrogen
- ALB:
-
Albumin
- GLB:
-
Globulin
- (A/G):
-
Albumin-to-globulin ratio
References
Wang, X. et al. Global epidemiology of gallstones in the 21st century: a systematic review and meta-analysis. Clin. Gastroenterol. Hepatol. 22(8), 1586–1595 (2024).
Abdu, S. M., Assefa, E. M. Prevalence of gallstone disease in Africa: a systematic review and meta-analysis. BMJ Open Gastroenterol. 12(1), (2025).
Aerts, R. & Penninckx, F. The burden of gallstone disease in Europe. Aliment Pharmacol. Ther. 18(Suppl 3), 49–53 (2003).
Wang, J. et al. Serum lipid levels are the risk factors of gallbladder stones: a population-based study in China. Lipids Health Dis. 19(1), 50 (2020).
Lammert, F. et al. Gallstones. Nat. Rev. Dis. Primers. 2, 16024 (2016).
Portincasa, P., Moschetta, A. & Palasciano, G. Cholesterol gallstone disease. Lancet 368(9531), 230–239 (2006).
Yu, W. et al. Establishment and validation of a predictive model for gallstone disease in the general population: a multicenter study. Sichuan Da Xue Xue Bao Yi Xue Ban. 55(3), 641–652 (2024).
Wan, Y. et al. Elevated serum triglyceride levels may be a key independent predicting factor for gallbladder cancer risk in gallbladder stone disease patients: a case-control study. BMC Endocr. Disord. 22(1), 270 (2022).
Ang, Y. et al. Causal effects of gallstone disease on risk of gastrointestinal cancer in Chinese. Br. J. Cancer 124(11), 1864–1872 (2021).
Wang, F. et al. Gallstone disease and type 2 diabetes risk: A mendelian randomization study. Hepatology 70(2), 610–620 (2019).
Lv, J. et al. Gallstone disease and the risk of type 2 diabetes. Sci. Rep. 7(1), 15853 (2017).
Zhang, X. et al. Prevalence and risk factors of gallbladder stones and polyps in Liaoning, China. Front. Med. (Lausanne). 9, 865458 (2022).
Zhang, M. et al. Blood lipid metabolism and the risk of gallstone disease: a multi-center study and meta-analysis. Lipids Health Dis. 21(1), 26 (2022).
Shukla, A. et al. Effect of furocyst on lipid profile and insulin resistance across different categories of body mass index in women with polycystic ovarian syndrome (PCOS). Cureus. 16(11), e74571 (2024).
Roever, L., Biondi-Zoccai, G. & Chagas, A. C. Non-HDL-C vs. LDL-C in Predicting the Severity of Coronary Atherosclerosis. Heart Lung Circ. 25(10), 953–954 (2016).
Sniderman, A. D. et al. A meta-analysis of low-density lipoprotein cholesterol, non-high-density lipoprotein cholesterol, and apolipoprotein B as markers of cardiovascular risk. Circ. Cardiovasc. Qual. Outcomes 4(3), 337–345 (2011).
Shi, A. et al. Metabolic abnormalities, liver enzymes increased risk of gallstones: a cross-sectional study and multivariate mendelian randomization analysis. Intern. Emerg. Med. 20(2), 501–508 (2025).
Yuan, X. et al. Causal associations between changes in lipid profiles and risk of gallstone disease: a two-sample Mendelian randomization study. Ann. Transl. Med. 10(15), 818 (2022).
Chen, L. et al. Novel insights into causal effects of serum lipids and lipid-modifying targets on cholelithiasis. Gut 73(3), 521–532 (2024).
Song, Y. et al. Age, gender, geographic and clinical differences for gallstones in China: a nationwide study. Ann. Transl. Med. 10(13), 735. https://doi.org/10.21037/atm-21-6186.PMID:35957733 (2022) (PMCID:PMC9358507).
Rodriguez Gatta, D. et al. Sex disparities in gallstone disease: insights from the MAUCO prospective population-based cohort study. BMJ Open Gastroenterol. 11(1), e001457 (2024).
Ning, Q. et al. Estimating global prevalence of gallbladder stones in general population from 2000 to 2024: systematic review and meta-analysis. Ann. Med. 57(1), 2570795. https://doi.org/10.1080/07853890.2025.2570795 (2025) (Epub 2025 Oct 10. PMID: 41069192; PMCID: PMC12517418).
Kim, S. B. et al. Sex differences in prevalence and risk factors of asymptomatic cholelithiasis in Korean health screening examinee: A retrospective analysis of a multicenter study. Medicine (Baltimore) 96(13), e6477 (2017).
Zhao, G. et al. Elevated LDL-c may warn of the risk of gallbladder stones in the patients with metabolic dysfunction-associated steatotic liver disease: A case-control study. Clin. Res. Hepatol. Gastroenterol. 48(6), 102363 (2024).
Chen, L. et al. Insights into modifiable risk factors of cholelithiasis: A Mendelian randomization study. Hepatology 75(4), 785–796 (2022).
Zeng, D. et al. High Levels of Serum Triglyceride, Low-density Lipoprotein Cholesterol, Total Bile Acid, and Total Bilirubin are Risk Factors for Gallstones. Clin. Lab. 67(8), (2021).
Stender, S. et al. Low-density lipoprotein cholesterol and risk of gallstone disease: a Mendelian randomization study and meta-analyses. J. Hepatol. 58(1), 126–133 (2013).
Andreotti, G. et al. Serum lipid levels and the risk of biliary tract cancers and biliary stones: A population-based study in China. Int. J. Cancer 122, 2322–2329 (2008).
Yang, G., Mason, A. M., Gill, D., Schooling, C. M. & Burgess, S. Multi-biobank Mendelian randomization analyses identify opposing pathways in plasma low-density lipoprotein-cholesterol lowering and gallstone disease. Eur. J. Epidemiol. 39(8), 857–867 (2024).
Kim, Y. K., Kwon, O. S. & Her, K. H. The grade of nonalcoholic fatty liver disease is an independent risk factor for gallstone disease: An observational Study. Med. (Baltimore) 98(27), e16018 (2019).
Banim, P. J. et al. The aetiology of symptomatic gallstones quantification of the effects of obesity, alcohol and serum lipids on risk. Epidemiological and biomarker data from a UK prospective cohort study (EPIC-Norfolk). Eur. J. Gastroenterol. Hepatol. 23(8), 733–740 (2011).
Cheng, Q. et al. Association of non-high-density lipoprotein cholesterol to high-density lipoprotein cholesterol ratio (NHHR) and gallstones among US adults aged ≤ 50 years: a cross-sectional study from NHANES 2017–2020. Lipids Health Dis. 23(1), 265 (2024).
Du, W. et al. Diabetes Mellitus Mediates the Relationship Between Atherogenic Index of Plasma and Gallstones: A Population-Based Cross-Sectional Study. Diabetes Metab. Syndr. Obes. 17, 317–332 (2024).
Chen, H., et al. Metabolomics reveals the effects of high dietary energy density on the metabolism of transition angus Cows. Animals (Basel). 12(9), (2022).
Yin, B. et al. Non-linear association of atherogenic index of plasma with insulin resistance and type 2 diabetes: a cross-sectional study. Cardiovasc. Diabetol. 22(1), 157 (2023).
Ye, X. et al. FXR Signaling-Mediated Bile Acid Metabolism Is Critical for Alleviation of Cholesterol Gallstones by Lactobacillus Strains. Microbiol. Spectr. 10(5), e0051822 (2022).
Yu, X. H. et al. Cholesterol transport system: An integrated cholesterol transport model involved in atherosclerosis. Prog. Lipid Res. 73, 65–91 (2019).
Osman, A. et al. Is cholecystectomy in patients with symptomatic uncomplicated Cholelithiasis beneficial in improving the lipid profile?. Cureus 12, e6729 (2020).
Chavez-Tapia, N. C. et al. Association between cholecystectomy for gallstone disease and risk factors for cardiovascular disease. Ann. Hepatol. 11(1), 85–89 (2012).
Acknowledgements
We sincerely thank all study participants. We are deeply grateful to the leadership, staff, and medical teams of the following hospitals for providing essential physical examination data: First Affiliated Hospital of Chongqing Medical University Jinshan Hospital (Chongqing), The People’s Hospital of Kaizhou District (Chongqing), Qianjiang Central Hospital of Chongqing (Chongqing), and Beijing Xiaotangshan Hospital (Beijing). We are grateful to our colleagues from West China School of Public Health and West China Fourth Hospital of Sichuan University, as well as all the authors, for their support, especially for their technical assistance in data analysis. This work has received support from multiple funds. Finally, we express our gratitude to the ethics committees of all participating institutions for their approval. Finally, we sincerely thank the medical reviewers, proofreaders and editors for their assistance.
Funding
This research was supported by the Natural Science Foundation of Sichuan Province Project (2026NSFSC0589, 2023NSFSC1927); the National Natural Science Foundation of China (81903398); the research start- up fund for the introduction of talents of Sichuan University (YJ2021112); Medical Youth Innovation Research Project of Sichuan Province (Q21016); “From 0 to 1” Innovation Project, Sichuan University (2023SCUH0026); Sichuan Provincial Science and Technology Department 2023 Central Guide Local Project (2023ZYD0097); the Sichuan Tianfu Emei Plan for Young Talents (No.Emei-1841); the Sichuan Health Commission’s Popularization and Application Project (No.2025- 2401); Research Project on High- Quality Development of Clinical Nutrition Work (2025–3-Y-15); and Medical Research Project of Chengdu City 2025129.
Author information
Authors and Affiliations
Contributions
XW, YJ, LZ: conceptualization, and investigation, writing original draft, revision. YJ, HYL, MLH: methodology, assisted in the conceptualization, contributed to the draft writing. YJ: software, imaging analysis, and revision. YJ, CLW, XYZ, HYL, WQY, XW, XB, YTX, LJX: contributed to the methodology, writing, and data curation. MLH, XW, WQY, HYL, GHJ, JL: contributed to the conception, and draft writing. XW, YJ, YY,YML: writing, review, and editing. XW, CLW, XYZ, GCL, XFS, GHJ, LZ, FL, YML, YY: data collection, revision. All authors reviewed the final draft and agreed on its content and conclusions. All authors had full access to all the data in the study and had final responsibility for the decision to submit for publication. XW, CLW, YML, FL, YY and LZ accessed and verified the data.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
Ethical approval for this study was obtained from the ethics committee of West China Fourth Hospital and West China School of Public Health, Sichuan University (approval number: Gwll2021055). This study is a retrospective analysis of non-identifiable researcher-collected data. The requirement for informed consent from the study subjects was waived by the IRB of Ethical Approval of Ethics Committee of West China Fourth Hospital and West China School of Public Health, Sichuan University due to the retrospective study design. We confirm that: The research does not involve any human experimentation; No identifiable subject data or biological materials were utilized; No personal privacy concerns or commercial interests are implicated in this work.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Jiang, Y., Wang, C., Lou, Y. et al. Lipid metabolism and gallstone disease risk: a multicenter study. Sci Rep 16, 6530 (2026). https://doi.org/10.1038/s41598-026-37603-x
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-026-37603-x