Abstract
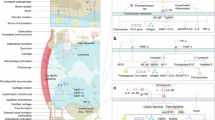
Inflammatory osteolysis is primarily characterized by an extensive macrophage-mediated inflammatory response coupled with osteoclast (OC) formation, triggered by bacterial byproducts and/or environmental stressors. And Osteoarthritis (OA) is one of the most common degenerative diseases in clinical medicine. Currently, anti-inflammatory drugs and intra-articular drug injection are mainly used, but the treatments only relieve symptoms. Punicalagin (PUN), a hydrolyzable tannin derived from pomegranate extract, the suppression of pro-inflammatory cytokine production in macrophages. The therapeutic potential of PUN in alleviating inflammatory osteolysis remains inadequately elucidated. PUN demonstrated favourable biocompatibility and therapeutic potential in vitro, including potent anti-osteoclastic activity, ROS scavenging capacity, and epigenetic regulatory functions. PUN was found to inhibit bromodomain-containing protein 4 (Brd4)-mediated chromatin space remodeling, consequently upregulating the production of endogenous anti-inflammatory factors and antioxidant factors. This study reveals a new therapeutic mechanism that PUN exerts anti-inflammatory effects and regulates epigenetic regulation by influencing Brd4-mediated chromatin remodeling. These findings showed the therapeutic potential of PUN for inflammatory diseases, especially inflammatory osteolysis. Notably, our work identifies a new strategy that synergistically combines osteoclast inhibition with epigenetic regulation, providing a promising direction for the therapies for bone-related inflammatory diseases.
Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request. The datasets generated and/or analyzed during the current study are available in https://www.ncbi.nlm.nih.gov/sra/PRJNA1328197, BioProject ID: PRJNA1328197.
References
Wu, H. et al. Artemether attenuates LPS-induced inflammatory bone loss by inhibiting osteoclastogenesis and bone resorption via suppression of MAPK signaling pathway. Cell Death Dis. 9(5), 498. https://doi.org/10.1038/s41419-018-0540-y (2018).
Kassem, A. et al. Porphyromonas gingivalis stimulates bone resorption by enhancing RANKL (Receptor Activator of NF-κB Ligand) through activation of toll-like receptor 2 in osteoblasts. J. Biol. Chem. 290(33), 20147–20158. https://doi.org/10.1074/jbc.M115.655787 (2015) (In Eng).
Matheus, H. R., Ozdemir, S. D. & Guastaldi, F. P. S. Stem cell-based therapies for temporomandibular joint osteoarthritis and regeneration of cartilage/osteochondral defects: A systematic review of preclinical experiments. Osteoarthr. Cartil. 30(9), 1174–1185. https://doi.org/10.1016/j.joca.2022.05.006 (2022).
Wang, D. et al. Recent advances in animal models, diagnosis, and treatment of temporomandibular joint osteoarthritis. Tissue Eng. Part B Rev. 29(1), 62–77. https://doi.org/10.1089/ten.TEB.2022.0065 (2023).
Cardoneanu, A. et al. Temporomandibular joint osteoarthritis: Pathogenic mechanisms involving the cartilage and subchondral bone, and potential therapeutic strategies for joint regeneration. Int. J. Mol. Sci. https://doi.org/10.3390/ijms24010171 (2022).
Li, B., Guan, G., Mei, L., Jiao, K. & Li, H. Pathological mechanism of chondrocytes and the surrounding environment during osteoarthritis of temporomandibular joint. J. Cell. Mol. Med. 25(11), 4902–4911. https://doi.org/10.1111/jcmm.16514 (2021).
Mbalaviele, G., Novack, D. V., Schett, G. & Teitelbaum, S. L. Inflammatory osteolysis: A conspiracy against bone. J. Clin. Invest. 127(6), 2030–2039. https://doi.org/10.1172/JCI93356 (2017).
Kandahari, A. M. et al. A review of UHMWPE wear-induced osteolysis: The role for early detection of the immune response. Bone Res. 4, 16014. https://doi.org/10.1038/boneres.2016.14 (2016).
Hodges, N. A., Sussman, E. M. & Stegemann, J. P. Aseptic and septic prosthetic joint loosening: Impact of biomaterial wear on immune cell function, inflammation, and infection. Biomaterials 278, 121127. https://doi.org/10.1016/j.biomaterials.2021.121127 (2021).
Gruber, R. Osteoimmunology: Inflammatory osteolysis and regeneration of the alveolar bone. J. Clin. Periodontol. 46(21), 52–69. https://doi.org/10.1111/jcpe.13056 (2019).
Kwak, S. C. et al. Umbelliferone prevents lipopolysaccharide-induced bone loss and suppresses RANKL-induced osteoclastogenesis by attenuating Akt-c-Fos-NFATc1 signaling. Int. J. Biol. Sci. 15(11), 2427–2437. https://doi.org/10.7150/ijbs.28609 (2019).
O’Brien, W. et al. RANK-independent osteoclast formation and bone erosion in inflammatory arthritis. Arthritis Rheumatol. 68(12), 2889–2900. https://doi.org/10.1002/art.39837 (2016).
Wei, S., Kitaura, H., Zhou, P., Ross, F. P. & Teitelbaum, S. L. IL-1 mediates TNF-induced osteoclastogenesis. J. Clin. Invest. 115(2), 282–290. https://doi.org/10.1172/JCI23394 (2005).
Zeng, C. et al. Relative efficacy and safety of topical non-steroidal anti-inflammatory drugs for osteoarthritis: A systematic review and network meta-analysis of randomised controlled trials and observational studies. Br. J. Sports Med. 52(10), 642–650. https://doi.org/10.1136/bjsports-2017-098043 (2018).
Cooper, C. & Jordan, K. M. Topical NSAIDs in osteoarthritis. BMJ 329(7461), 304–305. https://doi.org/10.1136/bmj.329.7461.304 (2004).
Kloppenburg, M. Hand osteoarthritis-nonpharmacological and pharmacological treatments. Nat. Rev. Rheumatol. 10(4), 242–251. https://doi.org/10.1038/nrrheum.2013.214 (2014).
Jones, I. A., Togashi, R., Wilson, M. L., Heckmann, N. & Vangsness, C. T. Jr. Intra-articular treatment options for knee osteoarthritis. Nat. Rev. Rheumatol. 15(2), 77–90. https://doi.org/10.1038/s41584-018-0123-4 (2019).
Ishii, K. A. et al. Coordination of PGC-1beta and iron uptake in mitochondrial biogenesis and osteoclast activation. Nat. Med. 15(3), 259–266. https://doi.org/10.1038/nm.1910 (2009).
Wu, Z., Qu, J., Zhang, W. & Liu, G. H. Stress, epigenetics, and aging: Unraveling the intricate crosstalk. Mol. Cell 84(1), 34–54. https://doi.org/10.1016/j.molcel.2023.10.006 (2024).
Rice, S. J., Beier, F., Young, D. A. & Loughlin, J. Interplay between genetics and epigenetics in osteoarthritis. Nat. Rev. Rheumatol. 16(5), 268–281. https://doi.org/10.1038/s41584-020-0407-3 (2020).
Nunez-Carro, C., Blanco-Blanco, M., Villagran-Andrade, K. M., Blanco, F. J. & de Andres, M. C. Epigenetics as a therapeutic target in osteoarthritis. Pharmaceuticals (Basel) https://doi.org/10.3390/ph16020156 (2023).
Min, J., Feng, Q., Li, Z., Zhang, Y. & Xu, R. M. Structure of the catalytic domain of human DOT1L, a non-SET domain nucleosomal histone methyltransferase. Cell 112(5), 711–723. https://doi.org/10.1016/s0092-8674(03)00114-4 (2003).
Assi, R. et al. Inhibition of KDM7A/B histone demethylases restores H3K79 methylation and protects against osteoarthritis. Ann. Rheum. Dis. 82(7), 963–973. https://doi.org/10.1136/ard-2022-223789 (2023).
Loughlin, J. & Reynard, L. N. Osteoarthritis: Epigenetics of articular cartilage in knee and hip OA. Nat. Rev. Rheumatol. 11(1), 6–7. https://doi.org/10.1038/nrrheum.2014.189 (2015).
Lauterbach, M. A. et al. Toll-like receptor signaling rewires macrophage metabolism and promotes histone acetylation via ATP-citrate lyase. Immunity 51(6), 997-1011 e7. https://doi.org/10.1016/j.immuni.2019.11.009 (2019).
Ji, Q. et al. Hematopoietic PBX-interacting protein mediates cartilage degeneration during the pathogenesis of osteoarthritis. Nat. Commun. 10(1), 313. https://doi.org/10.1038/s41467-018-08277-5 (2019).
Haynes, S. R. et al. The bromodomain: A conserved sequence found in human, Drosophila and yeast proteins. Nucleic Acids Res. 20(10), 2603. https://doi.org/10.1093/nar/20.10.2603 (1992).
Jang, M. K. et al. The bromodomain protein Brd4 is a positive regulatory component of P-TEFb and stimulates RNA polymerase II-dependent transcription. Mol. Cell 19(4), 523–534. https://doi.org/10.1016/j.molcel.2005.06.027 (2005).
Yang, Z. et al. Recruitment of P-TEFb for stimulation of transcriptional elongation by the bromodomain protein Brd4. Mol. Cell 19(4), 535–545. https://doi.org/10.1016/j.molcel.2005.06.029 (2005).
Itzen, F., Greifenberg, A. K., Bosken, C. A. & Geyer, M. Brd4 activates P-TEFb for RNA polymerase II CTD phosphorylation. Nucleic Acids Res. 42(12), 7577–7590. https://doi.org/10.1093/nar/gku449 (2014).
Nicodeme, E. et al. Suppression of inflammation by a synthetic histone mimic. Nature 468(7327), 1119–1123. https://doi.org/10.1038/nature09589 (2010).
Filippakopoulos, P. et al. Selective inhibition of BET bromodomains. Nature 468(7327), 1067–1073. https://doi.org/10.1038/nature09504 (2010).
Wang, Z. Q. et al. Bromodomain and extraterminal (BET) proteins: Biological functions, diseases, and targeted therapy. Signal Transduct. Target. Ther. 8(1), 420. https://doi.org/10.1038/s41392-023-01647-6 (2023).
Park-Min, K. H. et al. Inhibition of osteoclastogenesis and inflammatory bone resorption by targeting BET proteins and epigenetic regulation. Nat. Commun. 5, 5418. https://doi.org/10.1038/ncomms6418 (2014).
Tao, X., Yin, L., Xu, L. & Peng, J. Dioscin: A diverse acting natural compound with therapeutic potential in metabolic diseases, cancer, inflammation and infections. Pharmacol. Res. 137, 259–269. https://doi.org/10.1016/j.phrs.2018.09.022 (2018).
Atanasov, A. G. et al. Discovery and resupply of pharmacologically active plant-derived natural products: A review. Biotechnol. Adv. 33(8), 1582–1614. https://doi.org/10.1016/j.biotechadv.2015.08.001 (2015).
Ge, G. et al. Punicalagin ameliorates collagen-induced arthritis by downregulating M1 macrophage and pyroptosis via NF-κB signaling pathway. Sci. China Life Sci. 65(3), 588–603. https://doi.org/10.1007/s11427-020-1939-1 (2022).
Wang, W. et al. Protective effects of Punicalagin on osteoporosis by inhibiting osteoclastogenesis and inflammation via the NF-κB and MAPK pathways. Front. Pharmacol. 11, 696. https://doi.org/10.3389/fphar.2020.00696 (2020).
Olajide, O. A., Kumar, A., Velagapudi, R., Okorji, U. P. & Fiebich, B. L. Punicalagin inhibits neuroinflammation in LPS-activated rat primary microglia. Mol. Nutr. Food Res. 58(9), 1843–1851. https://doi.org/10.1002/mnfr.201400163 (2014).
Xu, X. et al. Punicalagin Inhibits Inflammation in LPS-Induced RAW264.7 Macrophages via the Suppression of TLR4-Mediated MAPKs and NF-κB Activation. Inflammation 37(3), 956–965. https://doi.org/10.1007/s10753-014-9816-2 (2014).
Glyn-Jones, S. et al. Osteoarthritis. Lancet 386(9991), 376–387. https://doi.org/10.1016/S0140-6736(14)60802-3 (2015).
Wu, Y. L. et al. Propionate and butyrate attenuate macrophage pyroptosis and osteoclastogenesis induced by CoCrMo alloy particles. Mil. Med. Res. 9(1), 46. https://doi.org/10.1186/s40779-022-00404-0 (2022).
Yoshimoto, T. et al. Osteocytes directly regulate osteolysis via MYD88 signaling in bacterial bone infection. Nat. Commun. 13(1), 6648. https://doi.org/10.1038/s41467-022-34352-z (2022).
Li, Y. et al. Urolithin B suppressed osteoclast activation and reduced bone loss of osteoporosis via inhibiting ERK/NF-kappaB pathway. Cell Prolif 55(10), e13291. https://doi.org/10.1111/cpr.13291 (2022).
Devaiah, B. N. et al. BRD4 is a histone acetyltransferase that evicts nucleosomes from chromatin. Nat. Struct. Mol. Biol. 23(6), 540–548. https://doi.org/10.1038/nsmb.3228 (2016).
Lamoureux, F. et al. Selective inhibition of BET bromodomain epigenetic signalling interferes with the bone-associated tumour vicious cycle. Nat. Commun. 5, 3511. https://doi.org/10.1038/ncomms4511 (2014).
Cerda, B., Llorach, R., Ceron, J. J., Espin, J. C. & Tomas-Barberan, F. A. Evaluation of the bioavailability and metabolism in the rat of punicalagin, an antioxidant polyphenol from pomegranate juice. Eur. J. Nutr. 42(1), 18–28. https://doi.org/10.1007/s00394-003-0396-4 (2003).
Wang, Q. et al. Punicalagin ameliorates wear-particle-induced inflammatory bone destruction by bi-directional regulation of osteoblastic formation and osteoclastic resorption. Biomater. Sci. 8(18), 5157–5171. https://doi.org/10.1039/d0bm00718h (2020).
Iwatake, M., Okamoto, K., Tanaka, T. & Tsukuba, T. Punicalagin attenuates osteoclast differentiation by impairing NFATc1 expression and blocking Akt- and JNK-dependent pathways. Mol. Cell. Biochem. 407(1–2), 161–172. https://doi.org/10.1007/s11010-015-2466-3 (2015).
Chen, X. et al. Ultrasmall PtAu(2) nanoclusters activate endogenous anti-inflammatory and anti-oxidative systems to prevent inflammatory osteolysis. Theranostics 13(3), 1010–1027. https://doi.org/10.7150/thno.80514 (2023).
Chen, X. et al. LY411575, a potent gamma-secretase inhibitor, suppresses osteoclastogenesis in vitro and LPS-induced calvarial osteolysis in vivo. J. Cell. Physiol. 234(11), 20944–20956. https://doi.org/10.1002/jcp.28699 (2019).
Chen, X. et al. Nirogacestat suppresses RANKL-induced osteoclast formation in vitro and attenuates LPS-induced bone resorption in vivo. Exp. Cell Res. 382(1), 111470. https://doi.org/10.1016/j.yexcr.2019.06.015 (2019).
Yao, H. et al. Sulforaphene suppresses RANKL-induced osteoclastogenesis and LPS-induced bone erosion by activating Nrf2 signaling pathway. Free Radic. Biol. Med. 207, 48–62. https://doi.org/10.1016/j.freeradbiomed.2023.07.009 (2023).
Acknowledgements
The authors would like to thank Editage (www.editage.cn) for the professional English language editing service. There is no founding.
Author information
Authors and Affiliations
Contributions
Dr. Huiping Li contributes to conceptualization, the project administration and supervision; Dr. Qilin Li and Dr. Tianhao Wan contribute to data curation and formal analysis; Dr. Yexin Wang and Prof. Shanyong Zhang contribute to investigation, original draft writing, review and editing.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Li, H., Li, Q., Wan, T. et al. Punicalagin with anti-inflammatory activities affects Brd-4 mediated chromatin remodeling for attenuating inflammatory osteolysis. Sci Rep (2026). https://doi.org/10.1038/s41598-026-41262-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-026-41262-3