Abstract
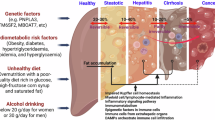
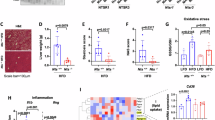
Metabolic dysfunction-associated steatotic liver disease (MASLD), also termed non-alcoholic fatty liver disease (NAFLD), represents the predominant chronic hepatic condition globally, yet remains without successful drug-based interventions. Understanding the molecular mechanisms driving MASLD progression is crucial. DDR2, a recently identified receptor tyrosine kinase, participates in various physiological processes including extracellular matrix remodeling, cell adhesion, and fibrosis. Given that MASLD pathogenesis involves lipid accumulation, inflammation, and progressive fibrotic remodeling of the liver, DDR2 signaling may play a critical role in linking extracellular matrix dynamics to metabolic and inflammatory pathways. However, its precise contribution to MASLD development and progression remains undefined, underscoring the need for mechanistic studies to clarify DDR2’s role and potential as a candidate modulator. DDR2 expression was assessed in liver tissues from both hepatic steatosis and genetically obese mice. RT-qPCR, Western blotting, and Oil Red O staining were utilized to examine DDR2’s role in lipid synthesis within hepatocytes under both cellular and animal models. The impact of DDR2 on MASLD were examined by utilizing db/db mice alongside C57BL/6J mice fed a high-fat diet (HFD). Hepatic DDR2 expression was markedly diminished in HFD-fed and db/db mice relative to controls. DDR2 overexpression resulted in diminished hepatic triglyceride accumulation and downregulated lipid synthesis-related gene expression in vitro and in vivo, whereas DDR2 knockdown exhibited the opposite effect. Mechanistically, DDR2 overexpression enhanced AMPK/ACC phosphorylation in hepatocytes, while its knockdown suppressed these pathways, findings corroborated by the use of AMPK inhibitors and agonists. DDR2 suppresses hepatocyte lipogenesis via activation of the AMPK/ACC pathway, suggesting its prospective role as a potential regulator in MASLD management.
Similar content being viewed by others
Data availability
All data generated or analysed during this study are included in this published article (and its Supplementary Information files).
References
Riazi, K. et al. The prevalence and incidence of NAFLD worldwide: a systematic review and meta-analysis. Lancet Gastroenterol. Hepatol. 7, 851–861. https://doi.org/10.1016/S2468-1253(22)00165-0 (2022).
Eslam, M. et al. A new definition for metabolic dysfunction-associated fatty liver disease: An international expert consensus statement. J. Hepatol. 73, 202–209. https://doi.org/10.1016/j.jhep.2020.03.039 (2020).
Eslam, M., Sanyal, A. J., George, J. & International Consensus, P. M. A. F. L. D. A Consensus-Driven Proposed Nomenclature for Metabolic Associated Fatty Liver Disease. Gastroenterology 158, 1999–2014 e (1991). https://doi.org/10.1053/j.gastro.2019.11.312 (2020).
Adams, L. A. et al. The natural history of nonalcoholic fatty liver disease: a population-based cohort study. Gastroenterology 129, 113–121. https://doi.org/10.1053/j.gastro.2005.04.014 (2005).
White, D. L., Kanwal, F. & El-Serag, H. B. Association between nonalcoholic fatty liver disease and risk for hepatocellular cancer, based on systematic review. Clin. Gastroenterol. Hepatol. 10 (e1342), 1342–1359. https://doi.org/10.1016/j.cgh.2012.10.001 (2012).
Ledford, H. First US drug approved for a liver disease surging around the world. Nature https://doi.org/10.1038/d41586-024-00747-9 (2024).
Sodum, N., Kumar, G., Bojja, S. L., Kumar, N. & Rao, C. M. Epigenetics in NAFLD/NASH: Targets and therapy. Pharmacol. Res. 167, 105484. https://doi.org/10.1016/j.phrs.2021.105484 (2021).
Nascimbeni, F. et al. From NAFLD in clinical practice to answers from guidelines. J. Hepatol. 59, 859–871. https://doi.org/10.1016/j.jhep.2013.05.044 (2013).
Keating, S. E. et al. Effect of aerobic exercise training dose on liver fat and visceral adiposity. J. Hepatol. 63, 174–182. https://doi.org/10.1016/j.jhep.2015.02.022 (2015).
Larson-Meyer, D. E. et al. Effect of 6-month calorie restriction and exercise on serum and liver lipids and markers of liver function. Obes. (Silver Spring). 16, 1355–1362. https://doi.org/10.1038/oby.2008.201 (2008).
Donnelly, K. L. et al. Sources of fatty acids stored in liver and secreted via lipoproteins in patients with nonalcoholic fatty liver disease. J. Clin. Invest. 115, 1343–1351. https://doi.org/10.1172/JCI23621 (2005).
Siddiqui, M. S. et al. Severity of nonalcoholic fatty liver disease and progression to cirrhosis are associated with atherogenic lipoprotein profile. Clin Gastroenterol Hepatol 13, 1000–1008 e1003, (2015). https://doi.org/10.1016/j.cgh.2014.10.008
Fabbrini, E. et al. Alterations in adipose tissue and hepatic lipid kinetics in obese men and women with nonalcoholic fatty liver disease. Gastroenterology 134, 424–431. https://doi.org/10.1053/j.gastro.2007.11.038 (2008).
Adiels, M., Olofsson, S. O., Taskinen, M. R. & Boren, J. Overproduction of very low-density lipoproteins is the hallmark of the dyslipidemia in the metabolic syndrome. Arterioscler. Thromb. Vasc Biol. 28, 1225–1236. https://doi.org/10.1161/ATVBAHA.107.160192 (2008).
Diraison, F., Moulin, P. & Beylot, M. Contribution of hepatic de novo lipogenesis and reesterification of plasma non esterified fatty acids to plasma triglyceride synthesis during non-alcoholic fatty liver disease. Diabetes Metab. 29, 478–485. https://doi.org/10.1016/s1262-3636(07)70061-7 (2003).
Lambert, J. E., Ramos-Roman, M. A., Browning, J. D. & Parks, E. J. Increased de novo lipogenesis is a distinct characteristic of individuals with nonalcoholic fatty liver disease. Gastroenterology 146, 726–735. https://doi.org/10.1053/j.gastro.2013.11.049 (2014).
Ju, G. X., Hu, Y. B., Du, M. R. & Jiang, J. L. Discoidin domain receptors (DDRs): potential implications in atherosclerosis. Eur. J. Pharmacol. 751, 28–33. https://doi.org/10.1016/j.ejphar.2015.01.033 (2015).
Matsuyama, W., Kamohara, H., Galligan, C., Faure, M. & Yoshimura, T. Interaction of discoidin domain receptor 1 isoform b (DDR1b) with collagen activates p38 mitogen-activated protein kinase and promotes differentiation of macrophages. FASEB J. 17, 1286–1288. https://doi.org/10.1096/fj.02-0320fje (2003).
Zhang, Y. et al. An essential role of discoidin domain receptor 2 (DDR2) in osteoblast differentiation and chondrocyte maturation via modulation of Runx2 activation. J. Bone Min. Res. 26, 604–617. https://doi.org/10.1002/jbmr.225 (2011).
Zhang, Y. et al. Nrp1, a Neuronal Regulator, Enhances DDR2-ERK-Runx2 Cascade in Osteoblast Differentiation via Suppression of DDR2 Degradation. Cell. Physiol. Biochem. 36, 75–84. https://doi.org/10.1159/000374054 (2015).
Lin, K. L. et al. Transcriptional upregulation of DDR2 by ATF4 facilitates osteoblastic differentiation through p38 MAPK-mediated Runx2 activation. J. Bone Min. Res. 25, 2489–2503. https://doi.org/10.1002/jbmr.159 (2010).
Kawai, I. et al. Discoidin domain receptor 2 (DDR2) regulates body size and fat metabolism in mice. Transgenic Res. 23, 165–175. https://doi.org/10.1007/s11248-013-9751-2 (2014).
Yang, X. et al. Targeting adipocytic discoidin domain receptor 2 impedes fat gain while increasing bone mass. Cell. Death Differ. 29, 737–749. https://doi.org/10.1038/s41418-021-00887-9 (2022).
Lachkar, F., Papaioannou, A., Ferre, P. & Foufelle, F. [ER stress and NAFLD]. Biol. Aujourdhui. 214, 15–23. https://doi.org/10.1051/jbio/2020007 (2020).
Mors, K. et al. Anti-inflammatory Effects of Alcohol Are Associated with JNK-STAT3 Downregulation in an In Vitro Inflammation Model in HepG2 Cells. Dis Markers 6622701, (2021). https://doi.org/10.1155/2021/6622701 (2021).
Farese, R. V. Jr., Zechner, R., Newgard, C. B. & Walther, T. C. The problem of establishing relationships between hepatic steatosis and hepatic insulin resistance. Cell. Metab. 15, 570–573. https://doi.org/10.1016/j.cmet.2012.03.004 (2012).
Biddinger, S. B. et al. Hepatic insulin resistance is sufficient to produce dyslipidemia and susceptibility to atherosclerosis. Cell. Metab. 7, 125–134. https://doi.org/10.1016/j.cmet.2007.11.013 (2008).
Parekh, S. & Anania, F. A. Abnormal lipid and glucose metabolism in obesity: implications for nonalcoholic fatty liver disease. Gastroenterology 132, 2191–2207. https://doi.org/10.1053/j.gastro.2007.03.055 (2007).
Loomba, R. & Sanyal, A. J. The global NAFLD epidemic. Nat. Rev. Gastroenterol. Hepatol. 10, 686–690. https://doi.org/10.1038/nrgastro.2013.171 (2013).
Mariadoss, A. V. A. & Wang, C. Z. Exploring the Cellular and Molecular Mechanism of Discoidin Domain Receptors (DDR1 and DDR2) in Bone Formation, Regeneration, and Its Associated Disease Conditions. Int. J. Mol. Sci. 24 https://doi.org/10.3390/ijms241914895 (2023).
Coelho, N. M., Wang, A. & McCulloch, C. A. Discoidin domain receptor 1 interactions with myosin motors contribute to collagen remodeling and tissue fibrosis. Biochim. Biophys. Acta Mol. Cell. Res. 1866, 118510. https://doi.org/10.1016/j.bbamcr.2019.07.005 (2019).
Ornitz, D. M. & Itoh, N. New developments in the biology of fibroblast growth factors. WIREs Mech. Dis. 14, e1549. https://doi.org/10.1002/wsbm.1549 (2022).
Wang, L. T., Zhang, B. & Chen, J. J. Effect of anti-fibrosis compound on collagen expression of hepatic cells in experimental liver fibrosis of rats. World J. Gastroenterol. 6, 877–880. https://doi.org/10.3748/wjg.v6.i6.877 (2000).
Xie, B. et al. DDR2 facilitates hepatocellular carcinoma invasion and metastasis via activating ERK signaling and stabilizing SNAIL1. J. Exp. Clin. Cancer Res. 34, 101. https://doi.org/10.1186/s13046-015-0218-6 (2015).
Hawley, S. A. et al. Use of cells expressing gamma subunit variants to identify diverse mechanisms of AMPK activation. Cell. Metab. 11, 554–565. https://doi.org/10.1016/j.cmet.2010.04.001 (2010).
Um, J. H. et al. AMP-activated protein kinase-deficient mice are resistant to the metabolic effects of resveratrol. Diabetes 59, 554–563. https://doi.org/10.2337/db09-0482 (2010).
Dzamko, N. et al. AMPK beta1 deletion reduces appetite, preventing obesity and hepatic insulin resistance. J. Biol. Chem. 285, 115–122. https://doi.org/10.1074/jbc.M109.056762 (2010).
Minokoshi, Y. et al. Leptin stimulates fatty-acid oxidation by activating AMP-activated protein kinase. Nature 415, 339–343. https://doi.org/10.1038/415339a (2002).
Canto, C. & Auwerx, J. AMP-activated protein kinase and its downstream transcriptional pathways. Cell. Mol. Life Sci. 67, 3407–3423. https://doi.org/10.1007/s00018-010-0454-z (2010).
Arconzo, M. et al. Hepatic-specific Pgc-1alpha ablation drives fibrosis in a MASH model. Liver Int. 44, 2738–2752. https://doi.org/10.1111/liv.16052 (2024).
Yang, Y. et al. Dihydromyricetin ameliorates hepatic steatosis and insulin resistance via AMPK/PGC-1alpha and PPARalpha-mediated autophagy pathway. J. Transl Med. 22, 309. https://doi.org/10.1186/s12967-024-05060-7 (2024).
Li, Y. et al. AMPK phosphorylates and inhibits SREBP activity to attenuate hepatic steatosis and atherosclerosis in diet-induced insulin-resistant mice. Cell. Metab. 13, 376–388. https://doi.org/10.1016/j.cmet.2011.03.009 (2011).
Foretz, M. et al. Short-term overexpression of a constitutively active form of AMP-activated protein kinase in the liver leads to mild hypoglycemia and fatty liver. Diabetes 54, 1331–1339. https://doi.org/10.2337/diabetes.54.5.1331 (2005).
Lebeaupin, C. et al. Endoplasmic reticulum stress signalling and the pathogenesis of non-alcoholic fatty liver disease. J. Hepatol. 69, 927–947. https://doi.org/10.1016/j.jhep.2018.06.008 (2018).
Liu, Q. et al. Ablation of myeloid discoidin domain receptor 2 exacerbates arthritis and high fat diet induced inflammation. Biochem. Biophys. Res. Commun. 649, 47–54. https://doi.org/10.1016/j.bbrc.2023.01.074 (2023).
Kanehisa, M., Furumichi, M., Sato, Y., Matsuura, Y. & Ishiguro-Watanabe, M. KEGG: biological systems database as a model of the real world. Nucleic Acids Res. 53, D672–D677. https://doi.org/10.1093/nar/gkae909 (2025).
Kanehisa, M. Toward understanding the origin and evolution of cellular organisms. Protein Sci. 28, 1947–1951. https://doi.org/10.1002/pro.3715 (2019).
Kanehisa, M. & Goto, S. KEGG: kyoto encyclopedia of genes and genomes. Nucleic Acids Res. 28, 27–30. https://doi.org/10.1093/nar/28.1.27 (2000).
Funding
This research was funded by the Anhui Science Fund for Distinguished Young Scholars (No. 2208085J45), the National Natural Science Foundation of China (Grants No. 82370878 and 81870402), the Key Research and Development Program of Anhui Province (No. 2022i01020023), the Natural Science Foundation of Anhui Province (No. 2308085QH270) and Natural Science Foundation of Colleges and Universities in Anhui Province (No. 2025AHGXZK40536).
Author information
Authors and Affiliations
Contributions
Guo Manyu: Conceptualization, Methodology, Software. Lin Li: Data curation, Writing-Original draft preparation. Wang Yiming: Validation, Visualization, Investigation. Gao Jingya: Formal analysis, Software. Wei Xiang: Validation, Writing-Review&Editing. Hua Hongting: Investigation, Data Curation. Wang Dong: Investigation, Data Curation. Huang Can: Visualization, Resources. Wang Xiuyun: Visualization, Resources. Zou Bingbing: Visualization, Resources, Data Curation. Zhang Lei: Supervision, Project administration. Zhang Huabing: Supervision, Project administration, Funding acquisition. Chen Qi: Supervision, Project administration.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
All experimental procedures were approved by the Ethics Committee of Anhui Medical University and were carried out in strict accordance with the ARRIVE guidelines. We further confirm that every experiment adhered to all applicable ethical regulations and standards.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.