Abstract
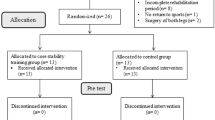
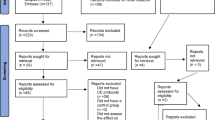
Predicting successful return to play (RTP) during mid-stage rehabilitation after anterior cruciate ligament reconstruction (ACLR) remains a critical, unresolved clinical challenge. High-sports demanders (HSDs)—non-professional athletes participating in level-1 sports (cutting, pivoting, jumping) ≥ 3 times/week with Tegner score > 5—represent a distinct subgroup who face unique rehabilitation challenges yet lack evidence-based mid-stage prediction tools. The primary objective of this study was to identify multidimensional predictors at 24 weeks post-ACLR for successful RTP at 48 weeks, and to construct a clinical scoring tool to guide individualized intervention decisions during mid-stage rehabilitation. This single-blind randomized controlled trial was conducted at the First Affiliated Hospital of Xi’an Medical University, Xi’an, China (April 2024–May 2025). Sixty-four HSDs post-primary ACLR were randomized to a functional rehabilitation model (FRM; n = 32) or traditional rehabilitation model (TRM; n = 32). At 24 weeks, isokinetic strength, hop tests, mSEBT, proprioception, and patient-reported outcomes (IKDC, Lysholm, ACL-RSI) were assessed. Forward stepwise logistic regression with bootstrap internal validation (1,000 iterations) identified independent predictors of 48-week RTP success. Among 57 completers (89.1% follow-up), the overall RTP rate was 75.4%. FRM significantly outperformed TRM (89.3% vs. 62.1%; P = 0.038; NNT = 3.7). Six independent predictors were identified: FRM vs. TRM (OR = 3.49), 60°/s extensor LSI ≥ 77.8% (OR = 2.13), single-leg hop ≥ 68.5 cm (OR = 1.87), ACL-RSI ≥ 67.5 (OR = 1.69), mSEBT anterior ≥ 63.2 cm (OR = 1.39), and 45° proprioceptive error ≤ 6.1° (OR = 0.62). Apparent AUC = 0.87 (95% CI: 0.79–0.95); bootstrap-corrected AUC = 0.81 (95% CI: 0.72–0.90). This exploratory six-factor model demonstrates promising discriminative ability (apparent AUC = 0.87; bootstrap-corrected AUC = 0.81) for mid-rehabilitation RTP prediction in HSDs. The identified predictive associations, rather than established causal relationships, may facilitate early risk identification and individualized intervention planning. External validation in independent, multicenter cohorts is required before clinical implementation.
Similar content being viewed by others
Data availability
The datasets used and/or analysed during the current study available from the corresponding author on reasonable request.
References
McGrath, T. M. et al. Anterior cruciate ligament injury incidence across sex, sport, and competition level: A systematic review and meta-analysis. J. Athl Train. https://doi.org/10.4085/1062-6050-0559.24 (2025).
American Academy of Orthopaedic Surgeons. Decreasing incidence of anterior cruciate ligament tears and reconstruction in the United States: An analysis of a large administrative claims database. Arthroscopy. https://doi.org/10.1016/j.arthro.2024.06.017 (2025).
Lai, C. C. H., Ardern, C. L., Feller, J. A. & Webster, K. E. Return to sport and graft failure rates after primary anterior cruciate ligament reconstruction with a bone-patellar tendon-bone versus hamstring tendon autograft: A systematic review and meta-analysis. Am. J. Sports Med. https://doi.org/10.1177/03635465241226648 (2025).
Delahunt, E. & Remus, A. No difference in return-to-sport rate or activity level in people with anterior cruciate ligament (ACL) injury managed with ACL reconstruction or rehabilitation alone: A systematic review and meta-analysis. Sports Med. 55, 1925–1940 (2025).
Ardern, C. L., Taylor, N. F., Feller, J. A. & Webster, K. E. Fifty-five per cent return to competitive sport following anterior cruciate ligament reconstruction surgery: An updated systematic review and meta-analysis including aspects of physical functioning and contextual factors. Br. J. Sports Med. 48, 1543–1552 (2014).
Lai, C. C., Ardern, C. L., Feller, J. A. & Webster, K. E. Eighty-three per cent of elite athletes return to preinjury sport after anterior cruciate ligament reconstruction: A systematic review with meta-analysis of return to sport rates, graft rupture rates and performance outcomes. Br. J. Sports Med. 52, 128–138 (2018).
Wiggins, A. J. et al. Risk of secondary injury in younger athletes after anterior cruciate ligament reconstruction: A systematic review and meta-analysis. Am. J. Sports Med. 44, 1861–1876 (2016).
Webster, K. E. & Feller, J. A. Exploring the high reinjury rate in younger patients undergoing anterior cruciate ligament reconstruction. Am. J. Sports Med. 44, 2827–2832 (2016).
Paterno, M. V., Rauh, M. J., Schmitt, L. C., Ford, K. R. & Hewett, T. E. Incidence of second ACL injuries 2 years after primary ACL reconstruction and return to sport. Am. J. Sports Med. 42, 1567–1573 (2014).
Ma, X. et al. Correlations of strength, proprioception, and tactile sensation to return-to-sports readiness among patients with anterior cruciate ligament reconstruction. Front. Physiol. 13, 1046141 (2022).
Agel, J., Rockwood, T. & Klossner, D. Collegiate ACL injury rates across 15 sports: National collegiate athletic association injury surveillance system data update (2004–2005 through 2012–2013). Clin. J. Sport Med. 26, 518–523 (2016).
Van Melick, N. et al. Evidence-based clinical practice update: Practice guidelines for anterior cruciate ligament rehabilitation based on a systematic review and multidisciplinary consensus. Br. J. Sports Med. 50, 1506–1515 (2016).
Burland, J. P. et al. Decision to return to sport after anterior cruciate ligament reconstruction, part I: A qualitative investigation of psychosocial factors. J. Athl Train. 53, 452–463 (2018).
Brewer, B. et al. Rehabilitation adherence and anterior cruciate ligament reconstruction outcome. Psychol. Health Med. 9, 163–175 (2004).
Lynch, A. D. et al. Consensus criteria for defining successful outcome after ACL injury and reconstruction: A Delaware-Oslo ACL cohort investigation. Br. J. Sports Med. 49, 335–342 (2015).
Barber-Westin, S. D. & Noyes, F. R. Factors used to determine return to unrestricted sports activities after anterior cruciate ligament reconstruction. Arthroscopy 27, 1697–1705 (2011).
Nagelli, C. V. & Hewett, T. E. Should return to sport be delayed until 2 years after anterior cruciate ligament reconstruction? Biological and functional considerations. Sports Med. 47, 221–232 (2017).
Grindem, H., Arundale, A. J. & Ardern, C. L. Alarming underutilisation of rehabilitation in athletes with anterior cruciate ligament reconstruction: Four ways to change the game. Br. J. Sports Med. 52, 1162–1163 (2018).
Davies, W. T., Myer, G. D. & Read, P. J. Is it time we better understood the tests we are using for return to sport decision making following ACL reconstruction? A critical review of the hop tests. Sports Med. 50, 485–495 (2020).
Kotsifaki, A., Korakakis, V., Whiteley, R., Van Rossom, S. & Jonkers, I. Measuring only hop distance during single leg hop testing is insufficient to detect deficits in knee function after ACL reconstruction: A systematic review and meta-analysis. Br. J. Sports Med. 54, 139–153 (2020).
Welling, W. et al. Low rates of patients meeting return to sport criteria 9 months after anterior cruciate ligament reconstruction: A prospective longitudinal study. Knee Surg. Sports Traumatol. Arthrosc. 26, 3636–3644 (2018).
Grindem, H., Snyder-Mackler, L., Moksnes, H., Engebretsen, L. & Risberg, M. A. Simple decision rules can reduce reinjury risk by 84% after ACL reconstruction: The Delaware-Oslo ACL cohort study. Br. J. Sports Med. 50, 804–808 (2016).
Kyritsis, P., Bahr, R., Landreau, P., Miladi, R. & Witvrouw, E. Likelihood of ACL graft rupture: Not meeting six clinical discharge criteria before return to sport is associated with a four times greater risk of rupture. Br. J. Sports Med. 50, 946–951 (2016).
Toole, A. R. et al. Young athletes cleared for sports participation after anterior cruciate ligament reconstruction: How many actually meet recommended return-to-sport criterion cutoffs? J. Orthop. Sports Phys. Ther. 47, 825–833 (2017).
Webster, K. E. & Feller, J. A. Development and validation of a short version of the anterior cruciate ligament return to sport after injury (ACL-RSI) scale. Orthop. J. Sports Med. 6, 2325967118763763 (2018).
Ardern, C. L., Taylor, N. F., Feller, J. A., Whitehead, T. S. & Webster, K. E. Psychological responses matter in returning to preinjury level of sport after anterior cruciate ligament reconstruction surgery. Am. J. Sports Med. 41, 1549–1558 (2013).
Petersen, W., Taheri, P., Forkel, P. & Zantop, T. Return to play following ACL reconstruction: A systematic review about strength deficits. Arch. Orthop. Trauma. Surg. 134, 1417–1428 (2014).
Dingenen, B. & Gokeler, A. Optimization of the return-to-sport paradigm after anterior cruciate ligament reconstruction: A critical step back to move forward. Sports Med. 47, 1487–1500 (2017).
Schulz, K. F., Altman, D. G. & Moher, D. CONSORT 2010 statement: Updated guidelines for reporting parallel group randomised trials. BMJ 340, c332 (2010).
Turk, R. et al. Return to sport after anterior cruciate ligament reconstruction requires evaluation of more than 2 functional tests, psychological readiness, quadriceps/hamstring strength, and time after surgery of 8 months. Arthroscopy 39, 790–801 (2023).
Buckthorpe, M. & Della Villa, F. Optimising the mid-stage training and testing process after ACL reconstruction. Sports Med. 50, 657–678 (2020).
Schmitt, L. C., Paterno, M. V. & Hewett, T. E. The impact of quadriceps femoris strength asymmetry on functional performance at return to sport following anterior cruciate ligament reconstruction. J. Orthop. Sports Phys. Ther. 42, 750–759 (2012).
Palmieri-Smith, R. M. & Lepley, L. K. Quadriceps strength asymmetry after anterior cruciate ligament reconstruction alters knee joint biomechanics and functional performance at time of return to activity. Am. J. Sports Med. 43, 1662–1669 (2015).
Labanca, L. et al. Neuromuscular electrical stimulation superimposed on movement early after ACL surgery. Med. Sci. Sports Exerc. 50, 407–416 (2018).
Hopkins, J. T., Ingersoll, C. D., Krause, B. A., Edwards, J. E. & Cordova, M. L. Effect of knee joint effusion on quadriceps and soleus motoneuron pool excitability. Med. Sci. Sports Exerc. 33, 123–126 (2001).
Grooms, D., Appelbaum, G. & Onate, J. Neuroplasticity following anterior cruciate ligament injury: A framework for visual-motor training approaches in rehabilitation. J. Orthop. Sports Phys. Ther. 45, 381–393 (2015).
Riemann, B. L. & Lephart, S. M. The sensorimotor system, part I: The physiologic basis of functional joint stability. J. Athl Train. 37, 71–79 (2002).
Vlaeyen, J. W. & Linton, S. J. Fear-avoidance and its consequences in chronic musculoskeletal pain: A state of the art. Pain 85, 317–332 (2000).
Meier, M. L. et al. The impact of pain-related fear on neural pathways of pain modulation in chronic low back pain. Pain Rep. 2, e601 (2017).
Reid, A., Birmingham, T. B., Stratford, P. W., Alcock, G. K. & Giffin, J. R. Hop testing provides a reliable and valid outcome measure during rehabilitation after anterior cruciate ligament reconstruction. Phys. Ther. 87, 337–349 (2007).
Plisky, P. J., Rauh, M. J., Kaminski, T. W. & Underwood, F. B. Star Excursion Balance Test as a predictor of lower extremity injury in high school basketball players. J. Orthop. Sports Phys. Ther. 36, 911–919 (2006).
Riemann, B. L., Guskiewicz, K. M. & Shields, E. W. Relationship between clinical and forceplate measures of postural stability. J. Sport Rehabil. 8, 71–82 (1999).
Fleming, B. C. et al. The effects of compressive load and knee joint torque on peak anterior cruciate ligament strains. Am. J. Sports Med. 31, 701–707 (2003).
Relph, N., Herrington, L. & Tyson, S. The effects of ACL injury on knee proprioception: A meta-analysis. Physiotherapy 100, 187–195 (2014).
Georgoulis, A. et al. ACL injury and reconstruction: Clinical related in vivo biomechanics. Orthop. Traumatol. Surg. Res. 96, S119–S128 (2010).
Zazulak, B. T., Hewett, T. E., Reeves, N. P., Goldberg, B. & Cholewicki, J. Deficits in neuromuscular control of the trunk predict knee injury risk: Prospective biomechanical-epidemiologic study. Am. J. Sports Med. 35, 1123–1130 (2007).
Funding
This work was supported by Xi’an Medical University Research Fund [grant number 2024QN16].
Author information
Authors and Affiliations
Contributions
FH: Conceptualization, Methodology, Formal analysis, Writing - original draft, Writing - review & editing, Supervision, Project administration, Funding acquisition.NY: Conceptualization, Methodology, Investigation, Data curation, Validation, Writing - review & editing.YX: Methodology, Investigation, Formal analysis, Visualization, Writing - review & editing.CM: Investigation, Data curation, Validation, Writing - original draft, Writing - review & editing.LQ: Resources, Validation, Visualization, Writing - review & editing.All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Hao, F., Yuhong, N., Xuyuan, Y. et al. 24-week multidimensional predictors of return to play post-ACLR in high-sports demanders: a randomized trial. Sci Rep (2026). https://doi.org/10.1038/s41598-026-43911-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-026-43911-z