Abstract
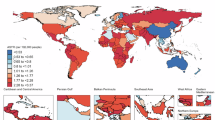
This multicenter study investigated the epidemiological and clinical characteristics of Guillain-Barré syndrome (GBS) during China’s Omicron wave (December 2022–February 2023), and compared the number of GBS hospitalizations with the historical data for the same period from 2018 to 2022. A retrospective analysis was conducted at two tertiary hospitals, categorizing patients into COVID-GBS (case group) and Non-COVID-GBS (control group). During the Omicron wave, the number of GBS hospitalizations was 1.5 times higher compared to the period of 2018–2019 (99 cases vs. 66 cases). Poisson regression analysis confirmed a significant increase in GBS incidence during the Omicron wave (December 2022–February 2023) compared to the 2018–2019 baseline period, with an IRR of 1.541 (95% CI: 1.123–2.129, p = 0.0079). COVID-19-associated GBS patients were significantly older (54.04 vs. 42.06 years, p = 0.002) and exhibited higher rates of cranial nerve involvement (p = 0.014), particularly bulbar involvement (p = 0.009). Acute severity was greater in COVID-19-associated cases, evidenced by elevated ICU admissions, higher peak GBS disability scores (p = 0.048), increased mechanical ventilation needs, and one fatality. The median latency from COVID-19 infection to neurological onset was 9.5 days (IQR: 8–14). Despite these acute differences, 6-month disability outcomes showed no significant divergence between groups, suggesting similar long-term prognoses. The surge in GBS incidence aligns with broader reports of elevated GBS rates during COVID-19 surges, though mechanistic links may involve immune-mediated pathways rather than direct viral causation.
Similar content being viewed by others
Data availability
All data generated or analysed during this study are included in this published article.
References
TAG-VE statement on the meeting of 3 January on the COVID-19. situation in China. https://www.who.int/news/item/04-01-2023-tag-ve-statement-on-the-3rd-january-meeting-on-the-covid-19-situation-in-china
Fu, D. et al. Effectiveness of COVID-19 vaccination against SARS-CoV-2 Omicron variant infection and symptoms - China, December 2022-February 2023. China. CDC. Wkly. 5, 369–373 (2023).
The infection rate of SARS-CoV-2. in Henan province has passed the epidemic peak, and the epidemic strain is mainly BA.5.2 variant _ Media Spotlight _ Portal of Henan Provincial People’s Government. https://www.henan.gov.cn/2023/01-09/2669240.html
Guan, W. J. et al. Clinical Characteristics of Coronavirus Disease 2019 in China. N Engl. J. Med. 382, 1708–1720 (2020).
Zhou, F. et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study. The Lancet 395, 1054–1062 (2020).
Mao, L. et al. Neurologic manifestations of hospitalized patients with Coronavirus Disease 2019 in Wuhan, China. JAMA Neurol. 77, 683–690 (2020).
Montalvan, V., Lee, J., Bueso, T., De Toledo, J. & Rivas, K. Neurological manifestations of COVID-19 and other coronavirus infections: A systematic review. Clin. Neurol. Neurosurg. 194, 105921 (2020).
Fokke, C. et al. Diagnosis of Guillain-Barré syndrome and validation of Brighton criteria. Brain J. Neurol. 137, 33–43 (2014).
Willison, H. J., Jacobs, B. C. & van Doorn, P. A. Guillain-Barré syndrome. The Lancet 388, 717–727 (2016).
Jacobs, B. C. The spectrum of antecedent infections in Guillain-Barré syndrome: A case-control study. Neurology 51, 1110–1115 (1998).
Cao-Lormeau, V.-M. et al. Guillain-Barré syndrome outbreak associated with Zika virus infection in French Polynesia: A case-control study. Lancet 387, 1531–1539 (2016).
Van Den Berg, B. et al. Guillain–Barré syndrome: Pathogenesis, diagnosis, treatment and prognosis. Nat. Rev. Neurol. 10, 469–482 (2014).
Filosto, M. et al. Guillain-Barré syndrome and COVID-19: An observational multicentre study from two Italian hotspot regions. J. Neurol. Neurosurg. Psychiatry. 92, 751–756 (2021).
Fragiel, M. et al. Incidence, clinical, risk factors and outcomes of Guillain-Barré in COVID-19. Ann. Neurol. 89, 598–603 (2021).
Blanco-Ruiz, M. et al. A nationwide Guillain-Barré syndrome epidemiological study in Spain during the COVID-19 years. Eur. J. Neurol. 31, e16439 (2024).
Keddie, S. et al. Epidemiological and cohort study finds no association between COVID-19 and Guillain-Barré syndrome. Brain J. Neurol. 144, 682–693 (2021).
van Doorn, P. A. et al. European Academy of Neurology/Peripheral Nerve Society Guideline on diagnosis and treatment of Guillain-Barré syndrome. Eur. J. Neurol. 30, 3646–3674 (2023).
Wakerley, B. R., Uncini, A., Yuki, N., Group, G. C., Group, G. C. Guillain-Barré and Miller Fisher syndromes–new diagnostic classification. Nat. Rev. Neurol. 10, 537–544 (2014).
Uncini, A. & Kuwabara, S. The electrodiagnosis of Guillain-Barré syndrome subtypes: Where do we stand?. Clin. Neurophysiol. 129, 2586–2593 (2018).
Hughes, R. A., Newsom-Davis, J. M., Perkin, G. D. & Pierce, J. M. Controlled trial prednisolone in acute polyneuropathy. Lancet 2, 750–753 (1978).
Released by the Taskforce for Joint Prevention and Control Mechanism for COVID-19 under the State Council of P.R. China on December 07, 2022. Prevention and control measures to further optimize COVID‐19 response. Health Care Sci. 2, 7–9 (2023).
Hafsteinsdóttir, B., Dalemo, E., Elíasdóttir, Ó., Ólafsson, E. & Axelsson, M. Decreased incidence of Guillain-Barré Syndrome during the COVID-19 pandemic: A retrospective population-based study. Neuroepidemiology 57, 1–6 (2023).
Censi, S., Bisaccia, G., Gallina, S., Tomassini, V. & Uncini, A. Guillain-Barré syndrome and SARS-CoV-2 infection: A systematic review and meta-analysis on a debated issue and evidence for the ‘Italian factor’. Eur. J. Neurol. 31, e16094 (2024).
W, A., B, S., W, R., R, S. & T, M. Seasonal variation in Guillain-Barré syndrome: A systematic review, meta-analysis and Oxfordshire cohort study. J. Neurol. Neurosurg. Psychiatry https://doi.org/10.1136/jnnp-2014-309056 (2015).
Zheng, P., Tian, D.-C., Xiu, Y., Wang, Y. & Shi, F.-D. Incidence of Guillain-Barré syndrome (GBS) in China: A national population-based study. Lancet Reg. Health 18, 100302 (2022).
COVID-19 Clinical and Surveillance Data — December 9. to January 23, 2023, China. (2022). https://weekly.chinacdc.cn/news/covid-surveillance/bfa0d054-d5bf-42bb-b8b4-f7ce34539b74_en.htm
Luijten, L. W. G. et al. Guillain-Barré syndrome after SARS-CoV-2 infection in an international prospective cohort study. Brain J. Neurol. 144, 3392–3404 (2021).
Li, Y. et al. Relative frequencies and clinical features of Guillain-Barré Syndrome before and during the COVID-19 pandemic in North China. BMC Infect. Dis. 24, 541 (2024).
Cunha, L. L., Perazzio, S. F., Azzi, J., Cravedi, P. & Riella, L. V. Remodeling of the immune response with aging: immunosenescence and its potential impact on COVID-19 immune response. Front. Immunol. 11, 1748 (2020).
Matschke, J. et al. Neuropathology of patients with COVID-19 in Germany: a post-mortem case series. Lancet Neurol. 19, 919–929 (2020).
Yachou, Y., El Idrissi, A., Belapasov, V. & Ait Benali, S. Neuroinvasion, neurotropic, and neuroinflammatory events of SARS-CoV-2: understanding the neurological manifestations in COVID-19 patients. Neurol. Sci. Off J. Ital. Neurol. Soc. Ital. Soc. Clin. Neurophysiol. 41, 2657–2669 (2020).
Ullah, H., Ullah, A., Gul, A., Mousavi, T. & Khan, M. W. Novel coronavirus 2019 (COVID-19) pandemic outbreak: A comprehensive review of the current literature. Vacunas 22, 106–113 (2021).
Del Valle, D. M. et al. An inflammatory cytokine signature predicts COVID-19 severity and survival. Nat. Med. 26, 1636–1643 (2020).
Jacobs, B. C., van Doorn, P. A., Groeneveld, J. H., Tio-Gillen, A. P. & van der Meché, F. G. Cytomegalovirus infections and anti-GM2 antibodies in Guillain-Barré syndrome. J. Neurol. Neurosurg. Psychiatry. 62, 641–643 (1997).
Sharma, A., Sharma, A. & Soubani, A. O. A Study on the Epidemiology of COVID-19-Related Guillain-Barré Syndrome in the United States. J. Clin. Neuromuscul. Dis. 25, 178–183 (2024).
Ergin Beton, O., Ozturk Tan, O. & Bilen, S. The potential association between COVID-19 disease and Guillain-Barré syndrome. Neurol. Res. 44, 855–860 (2022).
Kuwabara, S. & Yuki, N. Axonal Guillain-Barré syndrome: Concepts and controversies. Lancet. Neurol. 12, 1180–1188 (2013).
Ho, T. W. et al. Guillain-Barré syndrome in northern China. Relationship to Campylobacter jejuni infection and anti-glycolipid antibodies. Brain 118(Pt 3), 597–605 (1995).
Yamana, M. et al. Guillain-Barré syndrome and related diseases after influenza virus infection. Neurol. Neuroimmunol. Neuroinflamm 6, e575 (2019).
Leonhard, S. E. et al. Guillain-Barré syndrome related to Zika virus infection: A systematic review and meta-analysis of the clinical and electrophysiological phenotype. PLoS. Negl. Trop. Dis. 14, e0008264 (2020).
Ke, Z. et al. Structures and distributions of SARS-CoV-2 spike proteins on intact virions. Nature 588, 498–502 (2020).
Fantini, J., Di Scala, C., Chahinian, H. & Yahi, N. Structural and molecular modelling studies reveal a new mechanism of action of chloroquine and hydroxychloroquine against SARS-CoV-2 infection. Int. J. Antimicrob. Agents 55, 105960 (2020).
Negi, G. et al. SARS-CoV-2 evolved variants bind to sialylated gangliosides and are inhibited by a tetravalent sialo-glycocluster. ACS Infect. Dis. 11, 3036–3049 (2025).
Dey, M. et al. Synergistic binding of SARS-CoV-2 to ACE2 and gangliosides in native lipid membranes. ACS. Infect. Dis. 10, 907–916 (2024).
Hussain, F. S., Eldeeb, M. A., Blackmore, D. & Siddiqi, Z. A. Guillain Barré syndrome and COVID-19: Possible role of the cytokine storm. Autoimmun. Rev. 19, 102681 (2020).
Ubogu, E. E. Biology of the human blood-nerve barrier in health and disease. Exp. Neurol. 328, 113272 (2020).
Acknowledgements
We sincerely thank the patients who participated in this study and all of those who contributed to this study. We thank the Reviewers for their valuable comments and suggestions. We thank the First Affiliated Hospital of Zhengzhou University and Luoyang Central Hospital for their support.
Funding
This work was supported by China Postdoctoral Science Foundation, Special Funding Project, (2020T130111ZX), Key Project of Luoyang Science & Technology Development Program(2302004 A), Henan Province Health Commission Co-Construction Project (LHGJ20230806).
Author information
Authors and Affiliations
Contributions
Jiwei Zhang: Conceptualization, Supervision, Writing – review & editing. Yifan Guo: Data collection and analysis, Writing – original draft, Writing – review & editing. Liting Wei: Data collection, Writing – review & editing. Jinshun Liu: Writing – review & editing. Shibo Li: Writing – review & editing. Shuo Zhang: Writing – review & editing.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This study was approved by the Ethics Committees of the First Affiliated Hospital of Zhengzhou University(2024-KY-1665) and Luoyang Central Hospital affiliated with Zhengzhou University. These studies were conducted in accordance with the local legislation and institutional requirements. As this study is retrospective, written informed consent was waived by the First Affiliated Hospital of Zhengzhou University.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhang, J., Guo, Y., Wei, L. et al. Post-COVID-19 surge in Guillain-Barré syndrome during the Omicron wave in China with clinical characteristics and potential immune-mediated pathways. Sci Rep (2026). https://doi.org/10.1038/s41598-026-44136-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-026-44136-w