Abstract
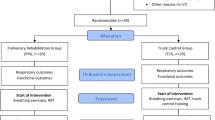
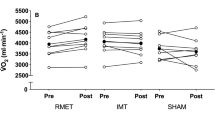
Inspiratory muscle training (IMT) is widely implemented among athletes and patients, but its effects in sedentary adolescent students remain unclear. This randomized controlled trial investigated the effects of 12-week IMT on respiratory function and aerobic capacity in sedentary adolescent boys. For this aim, 41 sedentary male-adolescents (16–18 years) were assigned randomly into IMT (n = 20) or Sham (n = 21) group. IMT was performed 3 days/week, 3 sets of 30 repetitions daily over 12 weeks. The forced vital capacity (FVC), maximal inspiratory pressure (MIP), peak inspiratory flow (PIF), forced inspiratory volume (FIV), maximum expiratory pressure (MEP), estimated maximal oxygen uptake (VO2max), running distance, maximal heart rate and heart rate recovery at 1/3/5 minute (HRR1/3/5) were assessed before and after intervention. Two-way mixed ANOVA or generalized estimating equations was conducted to analyze group×time interactions. Significant group×time interactions were observed for all respiratory function parameters and for VO₂max, running distance, and HRR1 (P < 0.05). Post-intervention, the IMT group showed significantly higher MIP, PIF, FIV, VO₂max, running distance, and HRR1 compared to the Sham group (P < 0.05). The augmentation value was also substantially greater in the IMT group across all outcomes (P < 0.05). These findings suggest 12-week IMT effectively enhances respiratory function and aerobic endurance in sedentary adolescent males. This trial was registered at the Chinese Clinical Trial Registry (Registration ID ChiCTR2600117069, 3/12/2025).
Similar content being viewed by others
Data availability
The datasets used and/or analysed during the current study are available from the corresponding authors on reasonable request.
References
van Sluijs, E. M. et al. Physical activity behaviours in adolescence: Current evidence and opportunities for intervention. Lancet 398, 429–442. https://doi.org/10.1016/S0140-6736(21)01259-9 (2021).
Tremblay, M. S. et al. Sedentary Behavior Research Network (SBRN) - Terminology Consensus Project process and outcome. Int. J. Behav. Nutr. Phys. Act. 75. https://doi.org/10.1186/s12966-017-0525-8 (2017).
Guthold, R., Stevens, G. A., Riley, L. M. & Bull, F. C. Global trends in insufficient physical activity among adolescents: A pooled analysis of 298 population-based surveys with 1· 6 million participants. Lancet. Child. Adolesc. Health. 4, 23–35. https://doi.org/10.1016/s2352-4642(19)30323-2 (2020).
Egan, C. A. et al. Sedentary time and behavior during school: A systematic review and meta-analysis. Am. J. Health. Educ. 50, 283–290. https://doi.org/10.1080/19325037.2019.1642814 (2019).
Chong, K. H., Parrish, A. M., Cliff, D. P., Dumuid, D. & Okely, A. D. Changes in 24-hour movement behaviours during the transition from primary to secondary school among Australian children. Eur. J. Sport. Sci. 22, 1276–1286. https://doi.org/10.1080/17461391.2021.1903562 (2022).
Volpato, L. A. et al. Time reallocations from sedentary behavior to physical activity and cardiovascular risk factors in children and adolescents: A systematic review. J. Phys. Act. Health. 20, 1084–1091. https://doi.org/10.1123/jpah.2022-0471 (2023).
da Silva, B. G. C., Menezes, A. M. B., Wehrmeister, F. C., Barros, F. C. & Pratt, M. Screen-based sedentary behavior during adolescence and pulmonary function in a birth cohort. Int. J. Behav. Nutr. Phys. Act. 14, 82. https://doi.org/10.1186/s12966-017-0536-5 (2017).
Wigna, A. et al. Relationship of objectively measured physical activity, sedentary behavior and sleep time with cardiovascular and mtabolic outcomes in adolescents (a pilot study): ABCD growth study. Matern. Child. Health. J. 26, 2293–2299. https://doi.org/10.1007/s10995-022-03471-w (2022).
Eaton, C. B. Sedentary behavior and risk of cardiovascular disease. J. Am. Coll. Cardiol. 85, 487–488. https://doi.org/10.1016/j.jacc.2024.11.002 (2025).
Pinto, A. J. et al. Physiology of sedentary behavior. Physiol. Rev. 103, 2561–2622. https://doi.org/10.1152/physrev.00022.2022 (2023).
Owen, N. et al. Sedentary behavior and public health: Integrating the evidence and identifying potential solutions. Annu. Rev. Public Health 41, 265–287. https://doi.org/10.1146/annurev-publhealth-040119-094201 (2020).
Wold, L. E. et al. Cardiopulmonary consequences of vaping in adolescents: A scientific statement from the American Heart Association. Circ. Res. e70–e82. https://doi.org/10.1161/RES.0000000000000544 (2022).
Contardo Ayala, A. M. et al. Effectiveness of intervention strategies to increase adolescents’ physical activity and reduce sedentary time in secondary school settings, including factors related to implementation: A systematic review and meta-analysis. Sports. Med. Open. 25. https://doi.org/10.1186/s40798-024-00688-7 (2024).
Meng, Y., Song, Y. & Li, H. Cardiorespiratory fitness in Chinese children and adolescents: A systematic review and meta-analysis. Ann. Hum. Biol. 52, 2459141. https://doi.org/10.1080/03014460.2025.2459141 (2025).
Mahmoud, O. et al. Association of height growth in puberty with lung function. A longitudinal study. Am. J. Respir. Crit. Care Med. 198, 1539–1548. https://doi.org/10.1164/rccm.201802-0274OC (2018).
Wang, G. et al. Plasticity of individual lung function states from childhood to adulthood. Am. J. Respir. Crit. Care Med. 207, 406–415. https://doi.org/10.1164/rccm.202203-0444OC (2023).
Ingvarsdottir, T. H., Johannsson, E., Rognvaldsdottir, V., Stefansdottir, R. S. & Arnardottir, N. Y. Longitudinal development and tracking of cardiorespiratory fitness from childhood to adolescence. PLoS One 19, e0299941. https://doi.org/10.1371/journal.pone.0299941 (2024).
West, G. B., Brown, J. H. & Enquist, B. J. A general model for the origin of allometric scaling laws in biology. Science 276, 122–126. https://doi.org/10.1126/science.276.5309.122 (1997).
Richardson, R. S., Harms, C. A., Grassi, B. & Hepple, R. T. Skeletal muscle: Master or slave of the cardiovascular system?. Med. Sci. Sports Exerc. 32, 89–93. https://doi.org/10.1097/00005768-200001000-00014 (2000).
Hargreaves, D. et al. Strategies and interventions for healthy adolescent growth, nutrition, and development. Lancet 399, 198–210. https://doi.org/10.1016/S0140-6736(21)01593-2 (2022).
Aimo, A. et al. The ergoreflex: How the skeletal muscle modulates ventilation and cardiovascular function in health and disease. Eur. J. Heart Fail. 23, 1458–1467. https://doi.org/10.1002/ejhf.2298 (2021).
Pate, R. R., O’Neill, J. R. & McIver, K. L. Physical activity and health: Does physical education matter?. Quest 63, 19–35. https://doi.org/10.1080/00336297.2011.10483660 (2011).
Mendonça, F. R. et al. Effects of aerobic exercise combined with resistance training on health-related physical fitness in adolescents: A randomized controlled trial. J. Exerc. Sci. Fit. 20, 182–189. https://doi.org/10.1016/j.jesf.2022.03.002 (2022).
d. S. Silva Filho, R. C., Sasaki, J. E., Gordia, A. P. & Andaki, A. C. R. Effects of a physical exercise program and health advice on sedentary behavior of adolescents. Int. J. Environ. Res. Public Health 20, 1064. https://doi.org/10.3390/ijerph20021064 (2023).
Ferreira Silva, R. M. et al. Barriers to high school and university students’ physical activity: A systematic review. PLoS. One 17, e0265913. https://doi.org/10.1371/journal.pone.0265913 (2022).
Martins, J. Adolescents’ perspectives on the barriers and facilitators of physical activity: An updated systematic review of qualitative studies. Int. J. Environ. Res. Public. Health. https://doi.org/10.3390/ijerph18094954 (2021).
Martins, J., Marques, A., Sarmento, H. & da Carreiro Costa, F. Adolescents’ perspectives on the barriers and facilitators of physical activity: A systematic review of qualitative studies. Health Educ. Res. 30, 742–755. https://doi.org/10.1093/her/cyv042 (2015).
Abdelghaffar, E.-A., Hicham, E. K., Siham, B., Samira, E. F. & Youness, E. A. Perspectives of adolescents, parents, and teachers on barriers and facilitators of physical activity among school-age adolescents: A qualitative analysis. Environ. Health Prev. Med. 24, 21. https://doi.org/10.1186/s12199-019-0775-y (2019).
Yu, F., Fernandez, R., Chidarikire, S., Mackay, L. & Smith, M. Associated factors, barriers, and interventions to promote physical activity and reduce sedentary time in academics: A systematic review. B.M.C. Public Health 25, 2753. https://doi.org/10.1186/s12889-025-24092-2 (2025).
Illi, S. K., Held, U., Frank, I. & Spengler, C. M. Effect of respiratory muscle training on exercise performance in healthy individuals: A systematic review and meta-analysis. Sports Med. 42, 707–724. https://doi.org/10.1007/bf03262290 (2012).
McConnell, A. K. & Romer, L. M. Respiratory muscle training in healthy humans: Resolving the controversy. Int. J. Sports Med. 25, 284–293. https://doi.org/10.1055/s-2004-815827 (2004).
McConnell, A. Respiratory muscle training: theory and practice (Elsevier Health Sciences, 2013).
Garber, C. E. et al. American College of Sports Medicine position stand. Quantity and quality of exercise for developing and maintaining cardiorespiratory, musculoskeletal, and neuromotor fitness in apparently healthy adults: guidance for prescribing exercise. Med. Sci. Sports Exerc. 43, 1334–1359. https://doi.org/10.1249/MSS.0b013e318213fefb (2011).
Mackała, K. The effect of respiratory muscle training on the pulmonary function, lung ventilation, and endurance performance of young soccer players. Int. J. Environ. Res. Public. Health. https://doi.org/10.3390/ijerph17010234 (2019).
Lin, C. H., Lee, C. W. & Huang, C. H. Inspiratory muscle training improves aerobic fitness in active children. Int. J. Environ. Res. Public. Health. https://doi.org/10.3390/ijerph192214722 (2022).
Enright, S. J. & Unnithan, V. B. Effect of inspiratory muscle training intensities on pulmonary function and work capacity in people who are healthy: A randomized controlled trial. Phys. Ther. 91, 894–905. https://doi.org/10.2522/ptj.20090413 (2011).
Amann, M. Pulmonary system limitations to endurance exercise performance in humans. Exp. Physiol. 97, 311–318. https://doi.org/10.1113/expphysiol.2011.058800 (2012).
Rodrigues, G. D. & McConnell, A. K. The misuse of respiratory resistive loading during aerobic exercises: Revisiting mechanisms of “standalone” inspiratory muscle training. Am. J. Physiol. Lung Cell. Mol. Physiol. 327, L815–L817. https://doi.org/10.1152/ajplung.00396.2023 (2024).
Watson, K. Respiratory muscle training in neuromuscular disease: A systematic review and meta-analysis. Eur. Respir. Rev. https://doi.org/10.1183/16000617.0065-2022 (2022).
Elkins, M. & Dentice, R. Inspiratory muscle training facilitates weaning from mechanical ventilation among patients in the intensive care unit: A systematic review. J. Physiother. 61, 125–134. https://doi.org/10.1016/j.jphys.2015.05.016 (2015).
Araneda, O. F. Systemic and pulmonary inflammation/oxidative damage: Implications of general and respiratory muscle training in chronic spinal-cord-injured patients. Biology https://doi.org/10.3390/biology12060828 (2023).
HajGhanbari, B. et al. Effects of respiratory muscle training on performance in athletes: A systematic review with meta-analyses. J. Strength Cond. Res. 27, 1643–1663. https://doi.org/10.1519/JSC.0b013e318269f73f (2013).
Borujeni, B. G. & Yalfani, A. Effect of respiratory muscle training session on ankle muscle activity in athletes with chronic low back pain performing overhead squats: A randomized controlled trial. Int. J. Evid. Based Healthc. 18, 256–264. https://doi.org/10.1097/xeb.0000000000000204 (2020).
Lang, J. E., Carrion, V. M., Bhammar, D. M., Howard, J. B. & Armstrong, S. C. A randomized trial of inspiratory training in children and adolescents with obesity. Childh. Obes. 20, 517–525. https://doi.org/10.1089/chi.2023.0183 (2024).
Notter, D. A., Verges, S., Renggli, A. S., Beltrami, F. G. & Spengler, C. M. Similar effects on exercise performance following different respiratory muscle training programs in healthy young men. Sci. Rep. 13, 16135. https://doi.org/10.1038/s41598-023-41580-w (2023).
Kowalski, T., Klusiewicz, A., Rębiś, K., Wilk, A. & Starczewski, M. Comparative study of different respiratory muscle training methods: Effects on cardiopulmonary indices and athletic performance in elite short-track speedskaters. Life https://doi.org/10.3390/life14091159 (2024).
Bull, F. C. et al. World Health Organization 2020 guidelines on physical activity and sedentary behaviour. Br. J. Sports Med. 54, 1451–1462. https://doi.org/10.1136/bjsports-2020-102955 (2020).
Chen, P. et al. Physical activity and health in Chinese children and adolescents: Expert consensus statement (2020). Br. J. Sports Med. 54, 1321–1331. https://doi.org/10.1136/bjsports-2020-102261 (2020).
Migueles, J. H. et al. Accelerometer data collection and processing criteria to assess physical activity and other outcomes: A systematic review and practical considerations. Sports Med. 47, 1821–1845. https://doi.org/10.1007/s40279-017-0716-0 (2017).
Evenson, K. R., Catellier, D. J., Gill, K., Ondrak, K. S. & McMurray, R. G. Calibration of two objective measures of physical activity for children. J. Sports Sci. 26, 1557–1565. https://doi.org/10.1080/02640410802334196 (2008).
Crapo, R. O. Pulmonary-function testing. N. Engl. J. Med. 331, 25–30. https://doi.org/10.1056/NEJM199407073310107 (1994).
Ho, I. M. K., Matković, A. & Matković, B. R. Contemporary methods of predicting maximum oxygen uptake: A brief review. Hrvat. Športskomed. Vjesn. 39, 5–13. https://doi.org/10.69589/hsv.39.1.1 (2024).
Bangsbo, J., Iaia, F. M. & Krustrup, P. The Yo-Yo intermittent recovery test: A useful tool for evaluation of physical performance in intermittent sports. Sports Med. 38, 37–51. https://doi.org/10.2165/00007256-200838010-00004 (2008).
Archiza, B. et al. Effects of inspiratory muscle training in professional women football players: A randomized sham-controlled trial. J. Sports Sci. 36, 771–780. https://doi.org/10.1080/02640414.2017.1340659 (2018).
Cunha, M. et al. The effect of inspiratory muscle training on swimming performance, inspiratory muscle strength, lung function, and perceived breathlessness in elite swimmers: A randomized controlled trial. Porto Biomed. J. 4, e49. https://doi.org/10.1097/j.pbj.0000000000000049 (2019).
de Sousa, M. M. et al. Inspiratory muscle training improves aerobic capacity in amateur indoor football players. Int. J. Sports Med. 42, 456–463. https://doi.org/10.1055/a-1255-3256 (2021).
Rehder-Santos, P. et al. Moderate- and high-intensity inspiratory muscle training equally improves inspiratory muscle strength and endurance-a double-blind randomized controlled trial. Int. J. Sports Physiol. Perform. 16, 1111–1119. https://doi.org/10.1123/ijspp.2020-0189 (2021).
Qin, L. et al. The effect of inspiratory muscle training on health-related fitness in college students. Int J Environ Res Public Health https://doi.org/10.3390/ijerph21081088 (2024).
Fernández-Lázaro, D. et al. Effects on respiratory pressures, spirometry biomarkers, and sports performance after inspiratory muscle training in a physically active population by powerbreath(®): A systematic review and meta-analysis. Biology (Basel) https://doi.org/10.3390/biology12010056 (2022).
Kraemer, W. Fundamentals of resistance training: Progression and exercise prescription. Medicine & science in sports & exercise https://doi.org/10.1249/01.MSS.0000121945.36635.61 (2004).
Kowalski, T., Dias Rodrigues, G. & Zanini, M. Application of respiratory muscle training for improved intermittent exercise performance in team sports: A narrative review. Front. Sports Act. Living. 7, 1632207. https://doi.org/10.3389/fspor.2025.1632207 (2025).
Najafi, A. et al. Improvements in soccer-specific fitness and exercise tolerance following 8 weeks of inspiratory muscle training in adolescent males. J. Sports Med. Phys. Fitness 59, 1975–1984. https://doi.org/10.23736/s0022-4707.19.09578-1 (2019).
Tosun, M. I. et al. Respiratory muscle training improves aerobic capacity and respiratory muscle strength in youth wrestlers. Front. Physiol. 16, 1492446. https://doi.org/10.3389/fphys.2025.1492446 (2025).
CHOBISA, C. A., LALWANI, L., VARDHAN, V. & NATHANI, H. Effect of respiratory muscle training on improving respiratory muscle strength in younger population: a systematic review. J. Clin. Diagn. Res. 18 https://doi.org/10.7860/JCDR/2024/69640.19783 (2024).
Mickleborough, T. D., Stager, J. M., Chatham, K., Lindley, M. R. & Ionescu, A. A. Pulmonary adaptations to swim and inspiratory muscle training. Eur. J. Appl. Physiol. 103, 635–646. https://doi.org/10.1007/s00421-008-0759-x (2008).
Berthelot, G. et al. Has athletic performance reached its peak?. Sports Med. 45, 1263–1271. https://doi.org/10.1007/s40279-015-0347-2 (2015).
Fernández-Lázaro, D. et al. Inspiratory muscle training program using the PowerBreath(®): Does it have ergogenic potential for respiratory and/or athletic performance? A systematic review with meta-analysis. Int J Environ Res Public Health https://doi.org/10.3390/ijerph18136703 (2021).
Kaeotawee, P. et al. Effect of threshold inspiratory muscle training on functional fitness and respiratory muscle strength compared to incentive spirometry in children and adolescents with obesity: A randomized controlled trial. Front. Pediatr. 10, 942076. https://doi.org/10.3389/fped.2022.942076 (2022).
Short, T. The pursuit of peak athletic performance. Top. Exerc. Sci. Kinesiol. 4, 3 (2023).
Bailey, S. J. et al. Inspiratory muscle training enhances pulmonary O(2) uptake kinetics and high-intensity exercise tolerance in humans. J. Appl. Physiol. 109, 457–468. https://doi.org/10.1152/japplphysiol.00077.2010 (2010).
Yilmaz, Y. A. et al. Inspiratory muscle warm up improves 400m performance in elite male runners. Sci. Rep. 15, 28879. https://doi.org/10.1038/s41598-025-14797-0 (2025).
Onal, S. N. et al. Evaluation of dynamic respiratory muscle strength, physical fitness, and physical activity in children with asthma and healthy peers. Healthcare 12, 2579. https://doi.org/10.3390/healthcare12242579 (2024).
Pradi, N. et al. Normal values for maximal respiratory pressures in children and adolescents: A systematic review with meta-analysis. Braz. J. Phys. Ther. 28, 100587. https://doi.org/10.1016/j.bjpt.2023.100587 (2024).
Enright, S. J., Unnithan, V. B., Heward, C., Withnall, L. & Davies, D. H. Effect of high-intensity inspiratory muscle training on lung volumes, diaphragm thickness, and exercise capacity in subjects who are healthy. Phys. Ther. 86, 345–354. https://doi.org/10.1093/ptj/86.3.345 (2006).
Kilding, A. E., Brown, S. & McConnell, A. K. Inspiratory muscle training improves 100 and 200 m swimming performance. Eur. J. Appl. Physiol. 108, 505–511. https://doi.org/10.1007/s00421-009-1228-x (2010).
Sonetti, D. A., Wetter, T. J., Pegelow, D. F. & Dempsey, J. A. Effects of respiratory muscle training versus placebo on endurance exercise performance. Respir. Physiol. 127, 185–199. https://doi.org/10.1016/s0034-5687(01)00250-x (2001).
Tong, T. K. et al. The effect of inspiratory muscle training on high-intensity, intermittent running performance to exhaustion. Appl. Physiol. Nutr. Metab. 33, 671–681. https://doi.org/10.1139/h08-050 (2008).
Farthing, J. P., Borowsky, R., Chilibeck, P. D., Binsted, G. & Sarty, G. E. Neuro-physiological adaptations associated with cross-education of strength. Brain Topogr. 20, 77–88. https://doi.org/10.1007/s10548-007-0033-2 (2007).
Latash, M. L. Muscle coactivation: Definitions, mechanisms, and functions. J. Neurophysiol. 120, 88–104. https://doi.org/10.1152/jn.00084.2018 (2018).
Issurin, V. B. Training transfer: Scientific background and insights for practical application. Sports Med. 43, 675–694. https://doi.org/10.1007/s40279-013-0049-6 (2013).
Lavoie, J. L. Noradrenaline and skeletal muscle: Modulation of spillover and potential effects. Can. J. Appl. Physiol. 26, 410–412 (2001).
D’Lima, G. M. Health promotion in multiple domains: Capitalizing on the spillover effect (Old Dominion University, 2014).
Subramanian, T. & Goyal, M. Respiratory muscle strength training for athletes: A narrative review. J. Clin. Diagn. Res. 19, 1. https://doi.org/10.7860/JCDR/2025/76089.20433 (2025).
Lomax, M., Grant, I. & Corbett, J. Inspiratory muscle warm-up and inspiratory muscle training: Separate and combined effects on intermittent running to exhaustion. J. Sports Sci. 29, 563–569. https://doi.org/10.1080/02640414.2010.543911 (2011).
McConnell, A. K. CrossTalk opposing view: Respiratory muscle training does improve exercise tolerance. J Physiol 590, 3397–3398. https://doi.org/10.1113/jphysiol.2012.235572 (2012).
Esposito, F., Limonta, E., Alberti, G., Veicsteinas, A. & Ferretti, G. Effect of respiratory muscle training on maximum aerobic power in normoxia and hypoxia. Respir. Physiol. Neurobiol. 170, 268–272. https://doi.org/10.1016/j.resp.2010.02.004 (2010).
Hagen, T., Taylor, C. T., Lam, F. & Moncada, S. Redistribution of intracellular oxygen in hypoxia by nitric oxide: Effect on HIF1alpha. Science 302, 1975–1978. https://doi.org/10.1126/science.1088805 (2003).
Lomax, M., Epiphaniou, A. & Scott, A. The efficacy of respiratory muscle training in raising the ventilatory threshold: A pilot study. Med. Sci. Sports Exerc. 47, 534. https://doi.org/10.1249/01.mss.0000466095.56279.a8 (2015).
Toneloto, M. G., Terzi, R. G., Silva, W. A., Moraes, A. C. & Moreira, M. M. Effects of different tidal volumes and positive end expiratory pressure on gas exchange in experimental bronchopleural fistula. Rev. Bras. Ter. Intensiva 20, 254–260. https://doi.org/10.1590/s0103-507x2008000300008 (2008).
Verges, S., Kruttli, U., Stahl, B., Frigg, R. & Spengler, C. M. Respiratory control, respiratory sensations and cycling endurance after respiratory muscle endurance training. Adv. Exp. Med. Biol. 605, 239–244. https://doi.org/10.1007/978-0-387-73693-8_42 (2008).
Markov, G., Spengler, C. M., Knöpfli-Lenzin, C., Stuessi, C. & Boutellier, U. Respiratory muscle training increases cycling endurance without affecting cardiovascular responses to exercise. Eur. J. Appl. Physiol. 85, 233–239. https://doi.org/10.1007/s004210100450 (2001).
Edwards, A. M. & Walker, R. E. Inspiratory muscle training and endurance: A central metabolic control perspective. Int. J. Sports Physiol. Perform. 4, 122–128. https://doi.org/10.1123/ijspp.4.1.122 (2009).
Barnes, K. R. & Kilding, A. E. Strategies to improve running economy. Sports Med. 45, 37–56. https://doi.org/10.1007/s40279-014-0246-y (2015).
Bascuas, P. J., Gutiérrez, H., Piedrafita, E., Bataller-Cervero, A. V. & Berzosa, C. Study of physiological adaptations in vertical kilometer runners: Focus on cardiorespiratory and local muscle demands. J. Funct. Morphol. Kinesiol. 9, 230. https://doi.org/10.3390/jfmk9040230 (2024).
Stickford, A., Stickford, J., Tanner, D., Stager, J. & Chapman, R. Runners maintain locomotor-respiratory coupling following isocapnic voluntary hyperpnea to task failure. Eur. J. Appl. Physiol. 115, 2395–2405. https://doi.org/10.1007/s00421-015-3220-y (2015).
Chulani, V. L. & Gordon, L. P. Adolescent growth and development. Prim. Care 41, 465–487. https://doi.org/10.1016/j.pop.2014.05.002 (2014).
Lewis, M. E. Exploring adolescence as a key life history stage in bioarchaeology. Am. J. Biol. Anthropol. 179, 519–534. https://doi.org/10.1002/ajpa.24615 (2022).
Varghese, M., Ruparell, S. & LaBella, C. Youth athlete development models: A narrative review. Sports Health 14, 20–29. https://doi.org/10.1177/19417381211055396 (2022).
Fernando, R. J., Ravichandran, K. & Vaz, M. Aerobic fitness, heart rate recovery and heart rate recovery time in Indian school children. Indian J. Physiol. Pharmacol. 59, 407–413 (2015).
Mongin, D., Chabert, C., Courvoisier, D. S., García-Romero, J. & Alvero-Cruz, J. R. Heart rate recovery to assess fitness: Comparison of different calculation methods in a large cross-sectional study. Res. Sports Med. 31, 157–170. https://doi.org/10.1080/15438627.2021.1954513 (2023).
Akram, M. Heart rate recovery (HRR). J. Microbes Res. 10, 2836–2187. https://doi.org/10.58489/2836-2187/024 (2024).
Rodrigues, G. D., Gurgel, J. L., Gonçalves, T. R. & da Silva Soares, P. P. Inspiratory muscle training improves physical performance and cardiac autonomic modulation in older women. Eur. J. Appl. Physiol. 118, 1143–1152. https://doi.org/10.1007/s00421-018-3844-9 (2018).
Watson, A. M., Brickson, S. L., Prawda, E. R. & Sanfilippo, J. L. Short-term heart rate recovery is related to aerobic fitness in elite intermittent sport athletes. J. Strength Cond. Res. 31, 1055–1061. https://doi.org/10.1519/jsc.0000000000001567 (2017).
Radhakrishnan, K., Sharma, V. K. & Subramanian, S. K. Does treadmill running performance, heart rate and breathing rate response during maximal graded exercise improve after volitional respiratory muscle training? Br. J. Sports Med. https://doi.org/10.1136/bjsports-2017-097827.3 (2017).
Ladriñán-Maestro, A., Sánchez-Infante, J., Martín-Vera, D. & Sánchez-Sierra, A. Influence of an inspiratory muscle fatigue protocol on healthy youths on respiratory muscle strength and heart rate variability. A randomized controlled trial. Front. Physiol. 15, 1457019. https://doi.org/10.3389/fphys.2024.1457019 (2024).
Ladriñán-Maestro, A., Sánchez-Infante, J., Rodríguez-Sanz, D. & Sánchez-Sierra, A. Short-term effects of inspiratory muscle warm-up and fatigue on diaphragmatic function in professional basketball players: A randomized clinical trial. Eur. J. Appl. Physiol. https://doi.org/10.1007/s00421-025-06116-2 (2026).
Antonelli, C. B. B., Hartz, C. S., Santos, S. D. S. & Moreno, M. A. Effects of inspiratory muscle training with progressive loading on respiratory muscle function and sports performance in high-performance wheelchair basketball athletes: A randomized clinical trial. Int. J. Sports Physiol. Perform. 15, 238–242. https://doi.org/10.1123/ijspp.2018-0979 (2020).
Ostojic, S. M., Stojanovic, M. D. & Calleja-Gonzalez, J. Ultra short-term heart rate recovery after maximal exercise: Relations to aerobic power in sportsmen. Chin. J. Physiol. 54, 105–110. https://doi.org/10.4077/cjp.2011.amm018 (2011).
Esco, M., Williford, H., Olson, M., Russell, A. & Gaston, K. The relationship between selected anthropometric variables, VO2max, and heart rate recovery. J. Strength Cond. Res. 25, S78. https://doi.org/10.1097/01.JSC.0000395703.59589.73 (2011).
Haraldsdottir, K., Brickson, S., Sanfilippo, J., Dunn, W. & Watson, A. In-season changes in heart rate recovery are inversely related to time to exhaustion but not aerobic capacity in rowers. Scand. J. Med. Sci. Sports. 28, 418–424. https://doi.org/10.1111/sms.12934 (2018).
Buchheit, M., Papelier, Y., Laursen, P. B. & Ahmaidi, S. Noninvasive assessment of cardiac parasympathetic function: Postexercise heart rate recovery or heart rate variability?. Am. J. Physiol. Heart Circ. Physiol. 293, H8-10. https://doi.org/10.1152/ajpheart.00335.2007 (2007).
Bosquet, L., Gamelin, F. X. & Berthoin, S. Reliability of postexercise heart rate recovery. Int. J. Sports Med. 29, 238–243. https://doi.org/10.1055/s-2007-965162 (2008).
Grässler, B., Thielmann, B., Böckelmann, I. & Hökelmann, A. Effects of different training interventions on heart rate variability and cardiovascular health and risk factors in young and middle-aged adults: A systematic review. Front. Physiol. 12, 657274. https://doi.org/10.3389/fphys.2021.657274 (2021).
Speer, K. E., Naumovski, N. & McKune, A. J. Heart rate variability to track autonomic nervous system health in young children: Effects of physical activity and cardiometabolic risk factors. Physiol. Behav. 281, 114576. https://doi.org/10.1016/j.physbeh.2024.114576 (2024).
Sheel, A. W., Richards, J. C., Foster, G. E. & Guenette, J. A. Sex differences in respiratory exercise physiology. Sports Med. 34, 567–579. https://doi.org/10.2165/00007256-200434090-00002 (2004).
Kowalski, T. et al. Respiratory muscle training induces additional stress and training load in well-trained triathletes-randomized controlled trial. Front. Physiol. 14, 1264265. https://doi.org/10.3389/fphys.2023.1264265 (2023).
Acknowledgements
We would like to thank the participants for volunteering their time and efforts for this study. We also thank all the athletes for their time and effort. This research was supported by Fundamental Research Funds for the Central Universities (Exercise Rehabilitation Science Laboratory, No.2024KFZX007). The experiments comply with the current laws of the country in which they were performed. The authors have no conflict of interest to declare. The datasets generated during and/or analyzed during the current study are not publicly available but are available from the corresponding author who was an organizer of the study.
Funding
This work was supported by Fundamental Research Funds for the Central Universities (Exercise Rehabilitation Science Laboratory, No.2024KFZX007).
Author information
Authors and Affiliations
Contributions
Guangxin Li and Yueming Zhao contributed to conceptualization, data curation, formal analysis, investigation, methodology, and writing—original draft preparation and reviewing. Ting Mo contributed to software and methodology. Zhanjia Zhang contributed to visualization and methodology. Xin Zhang and Shilun Hou contributed to conceptualization, resources, supervision, validation, writing-review & editing and final approval. All authors have approved publishment of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
The study was approved by the Sports Science Experiment Ethics Committee of Beijing Sport University (Approval No. :2024382 H), and written informed consent was obtained from all participants and their parents before allocation. All procedures performed in the present study involving human participants were in accordance with the ethical standards of the institutional and national research committees and with the 1964 Helsinki Declaration and its later amendments, or with comparable ethical standards. This trial was registered at the Chinese Clinical Trial Registry (ChiCTR2600117069, 3/12/2025).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Li, G., Zhao, Y., Mo, T. et al. The effects of inspiratory muscle training on respiratory function and aerobic capacity in sedentary adolescents: A single-blind randomized controlled trial. Sci Rep (2026). https://doi.org/10.1038/s41598-026-44416-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-026-44416-5