Abstract
Objective
To investigate the relationship between frailty assessed by the HFRS and in-hospital mortality in ICU patients with sepsis.
Method
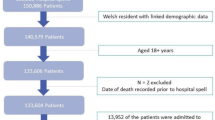
A retrospective analysis of septic ICU patients from the MIMIC-IV database assessed frailty through the Hospital Frailty Risk Score (HFRS). Patients were categorized into non-frail (HFRS < 5, n = 4,882), pre-frail (5 ≤ HFRS < 15, n = 3,134), and frail (HFRS ≥ 15, n = 2,575) groups. The primary outcome was in-hospital mortality. Logistic regression combined with restricted cubic splines (RCS) was employed to evaluate the association between HFRS (categorical and continuous) and mortality. Inverse probability weighting (IPW) validated the results, and subgroup analyses explored frailty-mortality correlations in different patient groups.
Results
A total of 10,591 patients were included, with 4,737 (44.7%) males and median age of 68.9[57.6, 79.6] years. Altogether, 3,024 (28.6%) experienced mortality during hospitalization. Elevated frailty levels were associated with increased in-hospital mortality, consistent across both continuous and categorical HFRS analyses. A linear association between HFRS and mortality risk was indicated by results from RCS. After controlling for potential confounders, both pre-frail and frail statuses were significantly correlated with higher in-hospital mortality risk (pre-frailty, RR = 1.15, 95% CI: [1.06, 1.26], P = 0.002; frailty, RR = 1.29, 95% CI: [1.17, 1.42], P < 0.001). Furthermore, frailty was significantly positively correlated with longer hospital and ICU stays. These findings were confirmed by IPW.
Conclusion
Elevated frailty assessed via HFRS was associated with an increased risk of in-hospital mortality and prolonged hospital and ICU stays in sepsis.
Similar content being viewed by others
Data availability
The datasets used and analysed during the current study available from the corresponding author on reasonable request. The data screening codes used in our analyses, provided by the authors of the MIMIC-IV database, are available on GitHub at (https://github.com/MIT-LCP/ mimic-code).
Abbreviations
- MIMIC-IV:
-
Medical information mart for intensive care IV
- HFRS:
-
Hospital frailty risk score
- ICD:
-
International classification of diseases
- SBP:
-
Systolic blood pressure
- DBP:
-
Diastolic blood pressure
- MBP:
-
Mean blood pressure
- SpO2 :
-
Saturation of peripheral oxygen
- INR:
-
International normalized ratio
- PT:
-
Prothrombin time
- APTT:
-
Activated partial thromboplastin time
- GCS:
-
Glasgow coma scale
- LODS:
-
Logistic organ dysfunction system
- SAPS II:
-
Simplified acute physiology score II
- CRRT:
-
Continuous renal replacement therapy
- MV:
-
Mechanical ventilation
- CI:
-
Confidence interval
- IPW:
-
Inverse probability weighting
- RCS:
-
Restricted cubic splines
- SDM:
-
Standardized mean difference
References
Singer, M. et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 315(8), 801–810 (2016).
Cecconi, M., Evans, L., Levy, M. & Rhodes, A. Sepsis and septic shock. Lancet 392(10141), 75–87 (2018).
Rudd, K. E. et al. Global, regional, and national sepsis incidence and mortality, 1990–2017: analysis for the Global Burden of Disease Study. Lancet 395(10219), 200–211 (2020).
Jones, K. E. et al. Global trends in emerging infectious diseases. Nature 451(7181), 990–993 (2008).
Rhee, C. et al. Prevalence, Underlying Causes, and Preventability of Sepsis-Associated Mortality in US Acute Care Hospitals. JAMA Netw Open. 2(2), e187571 (2019).
Hoogendijk, E. O. et al. Frailty: implications for clinical practice and public health. Lancet 394(10206), 1365–1375 (2019).
Theou, O., Blodgett, J. M., Godin, J. & Rockwood, K. Association between sedentary time and mortality across levels of frailty. CMAJ 189(33), E1056–E1064 (2017).
Soysal, P. et al. Inflammation and frailty in the elderly: A systematic review and meta-analysis. Ageing Res Rev. 31, 1–8 (2016).
Darvall, J. N. et al. Impact of frailty on persistent critical illness: a population-based cohort study. Intensive Care Med. 48(3), 343–351 (2022).
Torvik, M. A. et al. Patient characteristics in sepsis-related deaths: prevalence of advanced frailty, comorbidity, and age in a Norwegian hospital trust. Infection 51(4), 1103–1115 (2023).
Proietti, M. et al. Frailty prevalence and impact on outcomes in patients with atrial fibrillation: A systematic review and meta-analysis of 1,187,000 patients. Ageing Res. Rev. 79, 101652 (2022).
Singh, A. et al. Aging and Inflammation. Cold Spring Harb Perspect Med. 14(6), a041197 (2024).
Kim, D. H. & Rockwood, K. Frailty in Older Adults. N Engl J Med. 391(6), 538–548 (2024).
Clegg, A., Young, J., Iliffe, S., Rikkert, M. O. & Rockwood, K. Frailty in elderly people. Lancet 381(9868), 752–762 (2013).
Zhang, L., Zeng, X., He, F. & Huang, X. Inflammatory biomarkers of frailty: A review. Exp. Gerontol. 179, 112253 (2023).
Afilalo, J. et al. Frailty assessment in the cardiovascular care of older adults. J Am Coll Cardiol. 63(8), 747–762 (2014).
Fehlmann, C. A. et al. Frailty assessment in emergency medicine using the Clinical Frailty Scale: A scoping review. Intern. Emerg. Med. 17(8), 2407–2418 (2022).
Navarrete-Villanueva, D. et al. Frailty and physical fitness in elderly people: A systematic review and meta-analysis. Sports Med. 51(1), 143–160 (2021).
Lansbury, L. N. et al. Use of the electronic Frailty Index to identify vulnerable patients: A pilot study in primary care. Br. J. Gen. Pract. 67(664), e751–e756 (2017).
McAlister, F. A., Savu, A., Ezekowitz, J. A., Armstrong, P. W. & Kaul, P. The hospital frailty risk score in patients with heart failure is strongly associated with outcomes but less so with pharmacotherapy. J. Intern. Med. 287(3), 322–332 (2020).
Kwok, C. S. et al. The Hospital Frailty Risk Score and its association with in-hospital mortality, cost, length of stay and discharge location in patients with heart failure short running title: Frailty and outcomes in heart failure. Int J Cardiol. 1(300), 184–190 (2020).
McAlister, F. & van Walraven, C. External validation of the Hospital Frailty Risk Score and comparison with the Hospital-patient One-year Mortality Risk Score to predict outcomes in elderly hospitalised patients: A retrospective cohort study. BMJ Qual. Saf. 28(4), 284–288 (2019).
Ushida, K., Shimizu, A., Hori, S., Yamamoto, Y. & Momosaki, R. Hospital Frailty Risk Score predicts outcomes in chronic obstructive pulmonary disease exacerbations. Arch. Gerontol. Geriatr. 100, 104658 (2022).
Kandula, R. A. et al. Utility of Hospital Frailty Risk Score in predicting postoperative outcomes of sinonasal malignancies. Int. Forum Allergy Rhinol. 14(6), 1097–1100 (2024).
Kumar, V., Barkoudah, E., Jin, D. X., Banks, P. & McNabb-Baltar, J. Hospital Frailty Risk Score (HFRS) predicts adverse outcomes among hospitalized patients with chronic pancreatitis. Dig. Dis. Sci. 68(7), 2890–2898 (2023).
Hao, B. et al. A comparison of three approaches to measuring frailty to determine adverse health outcomes in critically ill patients. Age Ageing 52(6), afad096. https://doi.org/10.1093/ageing/afad096 (2023).
De Biasio, J. C. et al. Frailty in critical care medicine: A review. Anesth. Analg. 130(6), 1462–1473 (2020).
Brummel, N. E. et al. Frailty and Subsequent Disability and Mortality among Patients with Critical Illness. Am J Respir Crit Care Med. 196(1), 64–72 (2017).
Fernando, S. M. et al. Frailty and Associated Outcomes and Resource Utilization Among Older ICU Patients With Suspected Infection. Crit Care Med. 47(8), e669–e676 (2019).
Dent, E. et al. Management of frailty: opportunities, challenges, and future directions. Lancet 394(10206), 1376–1386 (2019).
Fan, J. et al. Frailty index and all-cause and cause-specific mortality in Chinese adults: a prospective cohort study. Lancet Public Health. 5(12), e650–e660 (2020).
Xu M, Gong Y, Yin X. Association of Frailty With Risk of Incident Hospital-Treated Infections in Middle-Aged and Older Adults: A Large-Scale Prospective Cohort Study. J Gerontol A Biol Sci Med Sci. 2024 Aug 1;79(8):glae146.
Muscedere, J. et al. The impact of frailty on intensive care unit outcomes: A systematic review and meta-analysis. Intensive Care Med. 43(8), 1105–1122 (2017).
Li, Q., Shang, N., Gao, Q., Guo, S. & Yang, T. Prevalence of sarcopenia and its association with frailty and malnutrition among older patients with sepsis-a cross-sectional study in the emergency department. BMC Geriatr. 25(1), 377 (2025).
Lee, H. Y. et al. Preexisting Clinical Frailty Is Associated With Worse Clinical Outcomes in Patients With Sepsis. Crit Care Med. 50(5), 780–790 (2022).
Patrizio, E. et al. Assessing the mortality risk in older patients hospitalized with a diagnosis of sepsis: the role of frailty and acute organ dysfunction. Aging Clin Exp Res. 34(10), 2335–2343 (2022).
Dong, J., Chen, R., Song, X., Guo, Z. & Sun, W. Quality of life and mortality in older adults with sepsis after one-year follow up: A prospective cohort study demonstrating the significant impact of frailty. Heart Lung 60, 74–80 (2023).
de Souto Barreto, P., Rolland, Y., Maltais, M. & Vellas, B. Associations of multidomain lifestyle intervention with frailty: Secondary analysis of a randomized controlled trial. Am. J. Med. 131(11), 1382.e7-1382.e13 (2018).
Apóstolo, J. et al. Effectiveness of interventions to prevent pre-frailty and frailty progression in older adults: A systematic review. JBI Database Syst. Rev. Implement. Rep. 16(1), 140–232 (2018).
Gilbert, T. et al. Development and validation of a Hospital Frailty Risk Score focusing on older people in acute care settings using electronic hospital records: an observational study. Lancet 391(10132), 1775–1782 (2018).
Renedo, D. et al. Higher Hospital Frailty Risk Score is associated with increased risk of stroke: Observational and genetic analyses. Stroke 54(6), 1538–1547 (2023).
Lim, Z. et al. Delirium is significantly associated with Hospital Frailty Risk Score derived from administrative data. Int. J. Geriatr. Psychiatry 38(1), e5872 (2023).
Detsky, M. E. et al. Using the Hospital Frailty Risk Score to assess mortality risk in older medical patients admitted to the intensive care unit. CMAJ Open 11(4), E607–E614 (2023).
Veronese, N. et al. Prevalence of multidimensional frailty and pre-frailty in older people in different settings: A systematic review and meta-analysis. Ageing Res. Rev. 72, 101498 (2021).
Acknowledgements
The authors would like to thank all those who contributed to the completion of this work.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
YLX Contributed to data curation, conceptualization, data analysis, and manuscript writing. XYW and ADL Contributed to methodology and data curation. XM reviewed the initial draft. SBG supervised and reviewed the manuscript. All authors approved the fi6nal manuscript and are responsible for its content.
Corresponding authors
Ethics declarations
Ethical approval
Ethical approval for this study was obtained from the Ethics Committee of Beijing Chaoyang Hospital, affiliated with Capital Medical University. The dataset used in this research was obtained from the MIMIC-IV 3.1 database. We have completed the CITI Program courses on "Human Research and Data" and "Specimen-Only Research" to apply for access to the database (Record ID: 66067288). The individual patient information in this database was anonymized, and therefore, ethical review and informed consent requirements were waived. All methods employed in our study were carried out in accordance with the relevant guidelines and regulations.
Consent for publication
Not Applicable.
Competing interests
The authors declare no competing interests.
Clinical trial number
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Xu, Y., Wang, X., Li, A. et al. Association between hospital frailty risk score and in-hospital mortality in critically ill patients with sepsis: results from MIMIC-IV database. Sci Rep (2026). https://doi.org/10.1038/s41598-026-47654-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-026-47654-9