Abstract
Digital mental health interventions (DMHIs) are playing an increasingly important role in supporting mental healthcare. Despite their widespread adoption during and after the COVID-19 pandemic, there has been a lack of review focused on DMHIs available in Chinese. This scoping review aims to enhance understanding of the landscape of DMHIs by examining the available evidence, assessing accessibility, and identifying gaps in both the research and implementation within the Greater China region. Searches across four English and four Chinese databases yielded 28 individual interventions reported across 32 trials in 31 publications. The majority of these interventions were mobile-based and trialed in economically developed regions. While most DMHIs showed significant improvements in reducing mental health symptoms, concerns persist regarding limited public access, high heterogeneity in study quality, and the lack of population-based early interventions. Future research is needed to address these issues within Chinese communities and the mental healthcare system.
Similar content being viewed by others
Introduction
Globally, mental disorders rank as top contributors to the total burden of disease1. People living with mental illness often experience the burden of neglect, discrimination, societal stigma2. A pronounced treatment gap exists worldwide due to a shortage of mental health providers relative to estimated demand3. This shortfall affects both the access to and quality of mental health services, exacerbating the challenges faced by those living with mental illness particularly in low-resource settings. In China, the overall prevalence of mental disorders has risen over the past decades, affecting ~130 million adults. Among these individuals, mood disorders, anxiety disorders, and substance use disorders are particularly prevalent4. Unfortunately, less than 30% of these individuals receive proper treatment due to various factors, including a lack of mental health literacy, mental health providers, stigma, financial concerns, and poor health care service quality5,6.
Since 2010, the Chinese government has prioritized the development of mental health infrastructure to address the rising burden of mental illness, focusing investments on psychiatric hospitals7. Consequently, China’s mental health care system is predominated by hospital-based care8. The vast majority of mental health professionals in China are psychiatric nurses, with relatively few psychiatrists, clinical psychologists, social workers, and occupational therapists9. In 2019, China had 6.8 licensed psychiatric nurses and 2.9 licensed psychiatrists per 100,000 population6, which is significantly lower than the national average of 12.9 psychiatrists per 100,000 population in the United States in 201810. Progress has been made primarily in managing severe mental disorders within hospital settings, but common conditions such as depression and anxiety remain inadequately addressed. Mental health-seeking behavior in China is also lower compared to other countries11. Moreover, investment in the mental health workforce does not meet the growing demand, further exacerbating the barriers to effective mental health care7.
Given these challenges, the rise of digital mental health interventions (DMHIs) offers a promising solution by leveraging the internet’s wide reach to support the overburdened mental healthcare system and provide resources to individuals with mental health symptoms. A mental health intervention is considered digital when it employs technology such as computers, mobile devices, text messaging services, or the Internet to deliver the intervention1. DMHIs can be used for a variety of purposes, including promoting mental health, maintaining mental well-being, providing early intervention, and treating specific conditions. These interventions can be used as standalone solutions or complements to traditional treatments, enhancing current services while introducing innovative prevention and support methods12. Additionally, they offer a layer of anonymity in a climate where mental health stigma is concerning. Within the Chinese context, where 96% of the population owns a smartphone and is proficient with technology8, digital intervention is a particularly promising strategy. These interventions are cost effective, efficacious, and offer a potentially destigmatizing alternative to traditional methods1.
In 2021, Zhang et al. conducted a systematic review of DMHIs in China, reporting on 39 studies encompassing 32 distinct interventions, using various technologies ranging from virtual reality to smartphone applications.8 The review reported generally favorable acceptance and use of digital health technologies among the Chinese population, drawing from both English and Chinese-language studies. Compared to their English counterparts, Chinese DMHI studies focused more prominently on schizophrenia, substance use disorder, and culturally specific presentations of social anxiety, reflecting the previous focus of the Chinese mental healthcare system. Notably, this review excluded studies from Hong Kong, Macao, and Taiwan due to differing healthcare systems and included only participants who met DSM or ICD diagnostic criteria. Since then, the field has evolved rapidly—particularly those emerging during the COVID-19 pandemic, a period marked by rapid growth in DMHIs and increased demand for digital mental health services13. In the current review, we expanded the scope to include these linguistically and culturally related regions and analyzed interventions developed since Zhang’s 2021 review. Differing from the previous review, we focused on self-paced and automated interventions — those delivered by technology itself that can function without human support—which are likely to be more scalable, broadly applicable, and less constrained by regional healthcare contexts14. This type of intervention enhances accessibility, allowing individuals to use it at any time or place, without professional assistance, and while simultaneously maintaining their anonymity. To gain a deeper understanding of the current digital mental health landscape in the Greater China region (mainland China, Hong Kong, Macao, and Taiwan)15, identify sustainable intervention programs available for those in need, and build upon the current literature, it is essential to produce an updated review highlighting the current automatic digital interventions in the region.
Given the high heterogeneity of the studies and the broad scope of the research question, a scoping review is conducted to map the landscape of automated DMHIs in Greater China. The scoping review has three main objectives: (1) to identify the DMHIs available in the Chinese language (both simplified and traditional) within the Greater China region, (2) to assess the efficacy or effectiveness of these interventions, and (3) to determine the public availability of these interventions and their implementation.
Results
Study characteristics
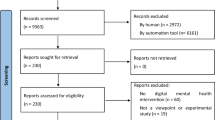
Our literature search retrieved 3472 study records, which were reduced to 2116 after removing duplicates (see Fig. 1). After the title and abstract screening, 102 articles were retained for full-text review. Of these, 89 were excluded, and 13 met the inclusion criteria. Additionally, 18 studies from the previous review on digital mental health in China8 met the inclusion criteria. All full-text records were screened independently by two reviewers (Cohen’s κ = 0.90). In total, 31 publications on 32 trials of 28 unique interventions were deemed eligible and included in the narrative synthesis. One of the included studies reports on three separate trials, two of which met the inclusion criteria16. The collection of included studies involved 24 English-language peer-reviewed studies and 7 Chinese-language peer-reviewed studies.
PRISMA flowchart of studies identified for inclusion in the review.
Table 1 provides an overview of the characteristics of studies included organized by intervention. All 32 trials were conducted in the Greater China region, including nine (28%) in Beijing, six (19%) in Hong Kong, four (13%) in Zhejiang, three (9%) in Guangdong, two (6%) in Shanghai, two in Macao (6%), one (3%) in Shandong, one (3%) in Chongqing, and four (13%) in multiple cities in China. Of the 28 interventions, 17 (61%) were in simplified Chinese, four (14%) were in traditional Chinese, one (4%) was in both simplified and traditional Chinese, and six (21%) were in unspecified Chinese (did not clearly indicate simplified or traditional Chinese usage). Twenty-two (79%) were locally developed for Chinese-speaking populations, six (21%) were originally developed internationally and translated into Chinese. Of the six internationally developed interventions, three (50%) were adapted for the Chinese context. Most interventions 22 (79%) were for adults, and six interventions (21%) were conducted amongst individuals less than 18 years old.
Online intervention modalities
A range of digital technologies were utilized for mental health interventions. Among the 28 identified interventions, 12 (43%) were application-based interventions delivered via mobile devices, highlighting the increasing reliance on mobile technology for mental health support in the Greater China region16,17,18,19,20,21,22,23,24,25,26,27. Of these, four interventions utilized existing applications as delivery vehicles: two through WeChat22,26, a widely used social media platform in China, and two through WhatsApp16, a popular messaging application. Additionally, one intervention leveraged automated text messages to provide interventions28. Web-based interventions were employed in seven interventions (25%), reflecting the accessibility and broad reach of internet-based programs29,30,31,32,33,34,35,36,37,38. There is also a growing interest in immersive technologies for mental health treatment, as evidenced by the seven interventions (25%) that used virtual reality-based interventions39,40,41,42,43,44,45. Zhu et al. developed a computer software program to deliver their intervention, demonstrating a unique approach among the reviewed studies46.
Target population
The interventions included in this review targeted a variety of populations. Four (14%) interventions targeted a broad, non-specific universal sample from the public16,18,25. One study specifically recruited participants from university settings, aiming to represent the academic community32. Additionally, one study recruited a healthy sample of seventh-grade Chinese middle school students26. The remaining 27 trials of 22 unique interventions can be grouped into two categories based on the participants’ health conditions: individuals with existing mental health symptoms and individuals with existing physical health symptoms.
Individuals with existing mental health symptoms
Nineteen interventions (68%) targeted individuals with mental health symptoms. Among these, seven (37%) interventions focused on participants with self-reported depressive symptoms or a formal diagnosis of depression20,21,22,24,34,36,39,41,46. Three (16%) interventions derived from five studies addressed individuals with high social anxiety: one targeting adolescents19, one targeting adults23, and one targeting university students29,31,37. One intervention targeted individuals with situational insomnia35, and another focused on those with generalized anxiety disorder44. Additionally, three (16%) interventions derived from five studies included participants with obsessive-compulsive disorder (OCD)45, attention deficit hyperactivity disorder (ADHD)30, and post-traumatic stress disorder (PTSD)38, respectively. Four (21%) interventions derived from five studies aimed at individuals looking to quit smoking or struggling with impulse control and substance use disorders, including one for tobacco users28, one for internet addiction33, and two for broader substance use issues17,27. Of the 19 interventions, four (21%) were implemented to augment usual treatment, which included psychotropic medication use and psychological counseling27,39,41,46.
Individuals with existing physical health symptoms
Three interventions (11%) focused on individuals with physical health symptoms who were undergoing medical treatments that could have mental health impacts. Mao et al. and Wong et al. tested the effects of VR-based interventions on cancer patients undergoing chemotherapy40,42. Ran et al. applied a VR-based intervention to dental patients between the ages of four and eight to reduce anxiety and pain43.
Target outcomes and intervention types
Depression and related symptoms
Among the 28 included interventions, ten (36%) assessed depression as the primary outcome20,21,22,24,25,32,34,35,36,39,41,42, and another three (11%) included depression as the secondary outcome16,38. Of these 13 interventions, six, originating from five studies, employed mindfulness-based techniques16,24,32,39,42. Three interventions derived from four studies used internet-based cognitive behavioral therapy (iCBT)22,34,35,36. Other interventions included attention training41, behavior activation20,21, self-efficacy38, and a lifestyle medicine approach that incorporated psychoeducation, physical activity, nutrition, stress, sleep management, and motivation components. The severity of depression was measured using scales, including the Hamilton Depression Scale35,39,41,42, Beck Depression Inventory39, Patient Health Questionnaire-916,20,21,22, Center for Epidemiologic Studies Depression Scale34,36, Hospital Anxiety and Depression Scale35,42, Symptom Checklist 90-Depression38, and 21-Item Depression, Anxiety, and Stress Scale25,32. Eleven interventions (85%) demonstrated significant improvements in reducing depression in the intervention group post intervention16,20,21,22,24,25,34,35,36,38,39,41,42, with two demonstrating sustained significance beyond the immediate post-treatment period16,38. Among the nine interventions that reported effect sizes, seven had small to medium effects16,22,24,25,32,38. One behavioral activation-based digital intervention for depression “Step-by-step” showed a large effect in the pilot20 but a moderate effect in the full trial21. One iCBT intervention underwent evaluation in trials conducted by Ren et al. and Yeung et al., where Ren et al.’s trial36 exhibited large effect and Yeung et al.’s trial34 found a moderate effect size for the intervention.
Anxiety
Generalized, mixed, and situational (non-social) anxiety was assessed as the primary outcome in eight interventions (29%)25,26,32,35,40,42,43,44, and five (18%) as the secondary outcome16,20,21,22,24. Among the eight interventions that measured anxiety as the primary outcome, one used relaxation and physical activity26, one employed mindfulness-based cognitive therapy (MBCT)42, one adopted mindfulness-based intervention32, two utilized distraction interventions40,43, one implemented exposure therapy44, one used iCBT35, and one took a lifestyle medicine approach25. The severity of anxiety was assessed using the Spence Children’s Anxiety Scale26, General Anxiety Disorder 7-item16,20,21,22,24, Hamilton Anxiety Rating Scale44, and the State Anxiety Scale for Children40. Ran et al. assessed the application of a VR intervention to improve operative anxiety and behavior management during short-term dental procedures among children using the Children’s Fear Survey Schedule-Dental Subscale and Wong-Baker FACES Pain Rating Scale43. Additionally, two studies utilized the Hospital Anxiety and Depression Scale to concurrently measure the severity of depression and anxiety35,42, while two other studies25,32 utilized the anxiety subscale from the 21-item versions of the Depression, Anxiety, and Stress Scale. With one exception, all interventions that measured anxiety as the primary outcome reported significant improvements in anxiety levels post intervention. The exception was an internet-based mindfulness intervention that incorporated principles from the Health Action Process Approach and assessed anxiety using the short version of the Depression Anxiety Stress Scale32. Additionally, of the eight interventions reporting effect size, seven interventions showed small effects16,21,22,24,25,32, while one had large effects40. The Step-by-Step pilot20 reported a large effect size while the full trial21 reported a small effect.
Social anxiety
Three of the included interventions (11%) focused on social anxiety19,23,29,31,37. These studies used the Social Interaction Anxiety Scale29,31,37, Social Phobia Scale29,31,37, Social Anxiety Scale19, Liebowitz Social Anxiety Scale23, and State-Trait Anxiety Inventory23. All three interventions—one web-based cognitive behavioral therapy (CBT)31,37 and two mobile-based cognitive bias modification for interpretation19,23—significantly reduced social anxiety. However, one of the three trials examining the web-based CBT treatment only investigated the predictors of treatment adherence and outcomes but did not report the effects on outcomes29. Another one of these three trials reported large effect sizes37. Lin et al. also measured the level of Taijin Kyofusho (TKS), a culturally specific form of social anxiety common in Eastern cultures where individuals worry that their behaviors, expressions, or physical characteristics might offend or discomfort others31, as the primary outcome measure using the 31-item Taijin Kyofusho Scale (TKSS). The study found that participants in the intervention group with higher pretreatment TKS levels showed significant reductions in TKSS scores posttreatment.
Mental wellbeing
Four mindfulness-based interventions (MBI) (14%) assessed general mental health and well-being, two as the primary outcome18,32 and two as the secondary outcome16. All four interventions used the World Health Organization Five Well-Being Scale (WHO-5), a short, self-administered, and positively worded scale that measures subjective well-being over the past two weeks. Wong et al. investigated an intervention based on the lifestyle medicine approach, using the Depression, Anxiety, and Stress Scale – 21 Items to assess overall mental health as the primary outcome measure25. Additionally, the Step-by-step intervention trials conducted by Sit et al.20 and Li G et al.21 measured subjective wellbeing as the secondary outcome using WHO-5. Six interventions16,18,21,25,32 significantly improved mental well-being following the interventions and reported small to moderate effect sizes.
Cognitive function
Four of the included interventions (14%) measured cognitive function as the primary outcome27,30,41,46 and one measured it as the secondary outcome45. These studies evaluated the efficacy of different interventions: a VR-based exposure and response prevention intervention for female OCD patients45, a computer-assisted cognitive remediation intervention for adult patients with major depression46, a web-based executive function training intervention for pediatric ADHD patients30, a mobile-based attention training intervention for pediatric patients with depressive episodes41, and a cognitive training and cognitive bias modification-based intervention for males with methamphetamine use disorder27. Cognitive function was assessed using screening tests including Montreal Cognitive Assessment-Basic45, Wisconsin Card Sorting Test46, Trail Making Test, Stroop Color and Word Test, the CogState Battery27, objective evaluation30, and the Mini Mental State Evaluation Scale41. Four interventions27,41,45,46 significantly improved cognitive function and performance for participants in the intervention group, but no effect sizes were reported in the original articles. Additionally, the web-based executive function training intervention for pediatric ADHD patients did not demonstrate significant effects on executive function based on objective evaluations30.
Sleep
Two interventions, one utilizing CBT35 and one a MBI16, measured sleep-related indicators as primary outcome measures. Four other interventions, one employing relaxation and physical activity26, one using MBCT24, one implementing CBT22, and one adopting a lifestyle-medicine approach25, measured sleep-related indicators as secondary measures. The assessment measures included the Insomnia Severity Index16,22,25,35, Pre-sleep Arousal Scale16,35, Dysfunctional Beliefs and Attitudes about Sleep Scale16, Pittsburgh Sleep Quality Index24, and the Patient-Reported Outcomes Measurement Information System26. Both interventions that targeted sleep-related concerns as the primary outcome reported significant improvements in the intervention group post-intervention16,35; of these one reported large effect size16.
COVID-19 related outcomes
Four of the included studies directly addressed pandemic-related mental health challenges. Among these, one CBT-based intervention measured the severity of situational insomnia35, three other interventions examined COVID-19 related depression or anxiety symptoms as the outcome measures22,26,44. Zhang et al. documented three cases of patients with generalized anxiety disorder, who were primarily concerned with COVID-19 infection anxiety and reported that exposure therapy significantly reduced their anxiety levels44. Zheng et al. used an intervention promoting relaxation and physical activity and significantly reduced anxiety and eye strain among Chinese middle school students under home confinement26. Song et al. tested the efficacy of an iCBT intervention on reducing COVID-19 related mental health problems and reported medium effect sizes22.
Others
An expert system intervention for college students with internet addiction found a significant decrease in self-reported hours spent online per week and online satisfaction after the intervention. The intervention was found to have large effect sizes33. Two CBT-based interventions for substance use—one targeting smoking cessation28 and the other for adults with recent substance use17—reported significant improvements in addiction levels following smartphone-based interventions using measures including self-reported cigarette consumption and the timeline follow-back survey on primary drug use. Li A et al. measured eating behaviors with the Three-Factor Eating Questionnaire and the Power of Food Scale after a mindfulness-based intervention with eating-specific exercises and found significant improvements16.
Public availability
Of the 28 interventions reviewed, only one (4%) remained publicly available after the conclusion of the study18. Mak et al. designed the “Living with Heart” intervention, a mobile-based intervention in Hong Kong that offers mindfulness, self-compassion, and cognitive behavioral psychoeducation training for the general public18. The Android mobile version of this intervention is publicly accessible47.
The effective web-based CBT intervention for Chinese depression patients, MoodGYM, was reported by Yeung et al. and Ren et al.34,36. Although originally developed in Australia and translated into Chinese for the studies, only the English and the German version are currently available48. Additionally, the smartphone-based lifestyle medicine intervention developed by Wong et al., to address overall mental health for the general public in Hong Kong is expected to become available later this year25. All other interventions (86%) reported in the reviewed studies are not publicly available.
Study design
According to the Oxford Centre for Evidence-Based Medicine levels of evidence49, this review included 25 (78%) randomized controlled trials (RCTs), six (19%) quasi-experimental designs, and one case series.
Randomized controlled trials
Six RCTs used an active control group, including four trials with “treatment as usual”27,39,41,46 and two trials as “enhanced treatment as usual”18,21. Three trials used a “no treatment”31,40,43 group. Four trials used attention control by adding components such as mental health education or basic counseling17,24,26,28. Ten trials utilized a waitlisted control group, granting participants in the control group access to the intervention after the trial’s completion16,19,25,32,33,34,36,37,38. Two trials used a mock intervention like the experimental intervention23,30. Among all RCT trials, two employed a three-arm design18,32.
Quasi-experimental designs
Of the six trials that adopted a quasi-experimental design, three employed a non-randomized approach. One trial evaluated cognitive behavioral therapy for COVID-19-related mental health problems, demonstrating its impact on reducing symptoms associated with the pandemic22. The other trials focused on treating social anxiety29 and OCD45 respectively. Additionally, three trials utilized a single group, pre-post uncontrolled design to evaluate the effectiveness of interventions20,35,42.
Case series
One case series study explored the role of virtual reality exposure therapy in treating psychiatric illness in three patients who had chief complaints of fear of COVID-19 infection44.
Quality assessment and acceptance
Quality assessments were conducted using the JBI critical appraisal tools. Results for the 31 publications included in Tables 2–4. While the review includes 32 trials, the quality assessment for the two RCTs from Li A et al., was based on that publication as a whole, resulting in 31 quality assessments16. Among the 24 RCTs reviewed, five (21%) had a low risk of bias21,24,25,26,27, 16 (67%) had a moderate risk of bias16,18,19,23,28,30,31,32,34,40,41,43,46, three (13%) had a high risk of bias17,33,39. Studies with moderate or high bias risk often showed weaknesses in selection, allocation, intervention administration, and outcome assessment methods, primarily due to unspecified randomization procedures or lack of participant and outcome assessor blinding. Due to the nature of psychotherapy interventions, double-blind designs were rarely feasible, with only two studies24,28 employing them. If the blinding of the participants and personnel rating were removed from the assessment, the risk of bias for these eight trials would be reduced significantly16,18,25,32,36,38,40,43. Of the six quasi-experimental studies reviewed, two (33%) had low risk of bias29,45, two (33%) had moderate risks20,22, and two (33%) had high risks35,42, primarily due to issues in selection and allocation, particularly the absence of a control group. The case series study had a high risk of bias as it lacked information regarding inclusion criteria and demographics of the patients.
Additionally, seven interventions (25%) reported the acceptability or satisfaction levels of participants using a combination of questionnaires25, self-designed surveys17,34,38,40,42, and qualitative interviews20,21,40. All seven interventions reported high levels of acceptability and satisfaction among participants, indicating a positive reception and perceived value of the interventions.
Discussion
This review systematically examined 31 publications that reported 28 unique DMHIs in Chinese. The interventions tackled a wide range of mental health issues including depression, anxiety, cognitive function, mental well-being, insomnia, substance-related addictive disorders, and COVID-19-related symptoms. Most interventions (19/28) were either mobile or internet-based, and about one-third utilized virtual reality technology, underscoring an area of growing research interest. Predominantly, examined studies employed randomized controlled trials (25/32). Seven interventions that examined acceptability reported high levels. Most interventions (27/28) demonstrated significant improvements in at least one primary mental health outcome post-intervention. Effect-size statistics were provided for 14 interventions with most laying in the small to moderate range. The results on sustained effectiveness of the interventions over time were mixed, only eight interventions reported follow-up data, and four showed sustained post-treatment gains across all primary mental health outcomes. Only one intervention remained publicly available and fully functional after the study conclusion.
Research on DMHIs for children is gaining traction. Among the six interventions that targeted children, three addressed anxiety, one targeted depression, one focused on ADHD, and one was aimed at social anxiety. Although studies on children and adolescents included in this review remain less common compared to adults, their representation has notably increased since the previous review in 20218. This rising interest can be attributed to several key factors. First, digital interventions are inherently aligned with the younger generation’s proficiency in technology, making these tools especially engaging and practical for children and adolescents. Second, the privacy and confidentiality provided by these interventions can be valuable for adolescents who may be more sensitive to stigma and peer perception when dealing with mental health issues. For instance, Mao et al.19, demonstrated the effectiveness of a mobile-based intervention for adolescents with social anxiety, highlighting the importance of reducing stigma in this context. Third, digital interventions can be seamlessly integrated into school systems, offering direct support within educational settings. Zheng et al.’s online streaming intervention, implemented as a course for grade seven students during COVID-19 home confinement, displayed how such resources can be utilized within schools to address mental health needs26.
There were relatively few interventions (5/28) targeting the general adult population, which highlights a gap in the application of DMHIs for broader population-based detection and early prevention in the Greater China region. Most interventions (19/28) targeted individuals with specific mental health conditions, with six designed to augment traditional psychotropic medication and psychological counseling. This indicates that DMHIs are often used to enhance rather than replace existing treatment methods. The integration of DMHIs alongside traditional care emphasizes their role as complementary tools that can expand upon current mental health services. By enhancing traditional approaches and providing additional support, DMHIs offer new avenues for improving mental health care delivery and accessibility, rather than substituting existing systems. While designing, rolling out and evaluating DMHIs for the general adult population are important next steps, developing targeted interventions for vulnerable groups such as the elderly, migrants, and the LGBTQ community should also be priorities for future research. The use of DMHIs can break down major barriers faced by these populations in accessing mental health services including privacy and confidentiality, filling a critical gap in care by significantly enhancing the inclusivity and effectiveness of the digital mental health landscape.
This review showed that while DMHIs are increasingly employed to address specific mental health outcomes, there is limited information on whether participants utilized other interventions concurrently. This points to an opportunity for developing a poly-digital ecosystem, where individuals can personalize their use of various digital interventions to optimize their mental health outcomes12. In considering the effectiveness of DMHIs, while there is variability in the effect of different interventions on individual users, most studies included in this review reported small to moderate effects. If different DMHIs are used in tandem, there is a possibility that their effects would compound, potentially leading to greater overall effectiveness and sustained benefits over time. Exploration of the possibility of such synergistic interaction between different DMHIs could contribute to the development of personalized and effective mental health care solutions.
In examining the distribution of DMHIs across Greater China, it became evident that most have been tested or conducted in provinces or regions characterized by higher income and greater development. This concentration in more affluent areas may skew the perceived effectiveness and accessibility of these interventions, as they are not being widely tested in lower-income, less developed regions where digital infrastructure and healthcare resources are more limited. The primary advantage of DMHIs, especially those that are mobile or web-based, lies in their potential to expand the reach and accessibility of traditional mental healthcare50. This is especially important in the geographically, demographically, and culturally diverse Greater China regions, where regional disparities in healthcare provision are pronounced and national and regional strategies could benefit from digitally scalable solutions that can reach underserved areas, where traditional in-person mental health services are scarce or non-existent. However, the current focus on high-income regions raises concerns about the applicability and effectiveness of these interventions in diverse socioeconomic environments. Moreover, our review focused exclusively on self-guided interventions, which inherently possess a greater potential for scalability due to their lower reliance on continuous professional oversight. Self-guided DMHIs could be crucial in democratizing mental health support, making basic care accessible to a broader audience at a significantly reduced cost. Nevertheless, the challenge remains to be how these technologies are made adaptable and relevant to the cultural and social contexts of users across development contexts.
A trend identified in this review was the adaptation of internationally developed DMHIs for the Chinese context. Six of the included studies investigated interventions originating from countries including the United States, Switzerland, and Australia. While some research teams took a straightforward approach by translating these effective interventions into Chinese, three interventions incorporated some degree of cultural adaptation. Despite the differences in adaptation levels, these interventions generally demonstrated significant positive outcomes among the target populations.
Among the three interventions that included cultural modifications, only one described a rigorous adaptation process based on the Ecological Validity Model20, while the others relied more on expert opinion for guidance23,29,31. The lack of detailed descriptions of the adaptation process in the majority of the studies raises concerns about the adequacy and appropriateness of these adaptations for the Chinese population. This oversight highlights a critical gap in ensuring that these interventions are culturally relevant and effective in the adapted context. Additionally, this field faces an issue with transparency, as the full contents and methodologies of DMHIs often remain undisclosed and are frequently inaccessible to the broader community. Open source DMHIs can significantly improve transparency, which allows for a greater and more flexible iteration by the wider scientific and clinical communities, thus improving the quality, cultural relevance, and accessibility of such interventions51.
DMHIs have a well-established track record of development and validation in Western countries. However, their introduction to China has been more recent, with a notable exponential increase over the past decade8. With aims towards the broader implementation of DMHIs in China, it is crucial that future research focuses on developing robust frameworks for comprehensive cultural adaptation. This will help ensure the interventions are not only relevant but also effective for the Chinese population, thereby maximizing their efficacy and impact. Moreover, enhancing cultural adaptation may not only boost the effectiveness of DMHIs within China but also increase their appeal and applicability to Chinese communities abroad.
Seven interventions used virtual reality as the medium and were all conducted in hospital settings. Among these, two studies incorporated mindfulness techniques, ranging from mindfulness training to stress reduction therapy. Feng et al.’s39 reported that VR-based mindfulness intervention improved depression symptoms in Parkinson’s patients, Mao et al.42 observed reductions in depressive and anxiety symptoms among ovarian cancer patients. These positive outcomes suggest that MBI delivered through virtual reality have the potential to be developed for broader public use, potentially offering significant benefits to individuals who can access these resources.
Wong et al.40 and Ran et al.’s43 VR interventions were both distraction interventions where VR was used on pediatric patients to ease their anxiety symptoms with positive outcomes. The interventions provided real-time distraction and emotional support for pediatric patients undergoing chemotherapy or dental treatments, complementing traditional medical treatments, and improving patient well-being and compliance40,43. This innovative use of VR-based DMHIs extends their application beyond traditional mental health settings into multidisciplinary healthcare environments. Integrating VR-based DMHIs into such diverse settings demonstrates their versatility and their potential to bridge gaps between mental health and general healthcare. The positive outcomes observed suggest that integrating VR-based DMHIs into routine clinical practice could potentially improve patient care in medical disciplines, leading to more holistic and patient-centered approaches to health.
VR interventions can also deliver another means of exposure therapy, as evidenced by studies such as Zhu et al’s study45 on female OCD patients and Zhang et al.’s study44 on anxiety patients with COVID-19-specific symptoms. Unlike traditional imaginal exposure methods, VR can simulate environments that trigger symptoms, providing patients with a fully immersive experience. Both studies observed positive results, including significant symptom reduction. This indicates that VR exposure therapy holds considerable potential for enhancing treatment outcomes by creating more engaging and realistic therapeutic experiences. The ability to replicate and control symptom-inducing scenarios in a virtual setting could also lead to more effective and personalized treatment options.
None of the virtual reality interventions reviewed are publicly available, as they were specifically developed for use in the intervention and have not been commercialized. Accessibility of VR interventions is also limited due to the requirement for VR equipment or headsets. Despite the growth of the VR industry, headsets remain relatively costly and are not easily accessible to most households. Furthermore, most VR interventions were examined in hospital settings with the necessary resources, and it was not specified whether the VR interventions were compatible with specific headset models.
The evolving landscape of DMHIs in Greater China calls for continued research to explore digital innovations such as poly-digital interventions that integrate multiple tools to create personalized care pathways. Future studies are recommended to focus on developing scalable and adaptable solutions that address the needs of diverse populations, particularly those in low-resource or rural areas, ensuring these interventions are both accessible and cost-effective. As DMHIs continue to evolve, their successful integration into existing health systems, particularly in primary care settings, is likely to be crucial for sustainability and bridging gaps in mental health service delivery. Furthermore, research should prioritize evaluating the long-term effectiveness of DMHIs, assessing not only their immediate impact but also their ability to sustain improvements over time. Rigorous cultural adaptation of successful international DMHIs can be a promising approach to ensure these tools are relevant and effective within the Chinese context. Ultimately, with further research in these key areas, DMHIs have the potential to transform the mental health care in Greater China, providing scalable, accessible solutions to meet the diverse mental health needs of local populations.
Methods
Search strategy and selection criteria
Zhang et al.8 reviewed the digital mental health landscape in China up to June 2021. This review builds on their work by incorporating the latest progresses in the field. To do this, four English-language databases (MEDLINE, PsycINFO, EMBASE, Cochrane Central Register of Controlled Trials via Ovid) and four Chinese-language databases (CNKI, Weipu, Wanfang, and Sinomed) were searched for peer-reviewed articles reporting DMHIs interventions available in the Chinese language published between January 1, 2021, and February 24, 2024. Search terms including “mental health”, “telehealth”, and “Chinese” or “China” were used to search the databases. The search strategy (Supplementary Table 1) focused on mental health disorders to prioritize interventions targeting diagnosable outcomes that are commonly reported in clinical trials. Additionally, the Cochrane Central Register of Controlled Trials database was further examined for the publication of complete trials, and only the published articles of the complete trials were included. During manuscript revision, we identified one additional publication evaluating the same intervention as an included pilot via a targeted supplementary check; this study was added for completeness and is reported in the PRISMA diagram under “Others.”
To be included in the current review, the mental health interventions should (i) enroll Chinese-speaking participants residing in Greater China (mainland China, Hong Kong, Macao, Taiwan); (ii) have at least one peer-reviewed publication reporting quantitative efficacy or effectiveness data in human participants (i.e., evidence-based); (iii) be enabled by digital technology; (iv) be fully automated and self-paced—meaning that all therapeutic content could be delivered without real-time, individualized clinician or coach contact, although one-off orientation or automated reminders were acceptable; (v) be available in either simplified or traditional Chinese; and (vi) include at least one of the mental health problems as the outcome. Any comparator or none was accepted. Interventions that are designed for severe mental conditions, including schizophrenia, psychosis, Alzheimer’s disease, and autism are not included in the current review. No additional exclusion criteria, such as age restrictions, were applied to capture a broad scope of the digital mental health literature for this scoping review. When multiple studies report on different clinical trials of the same mental health intervention, we included all papers that met our inclusion criteria. This approach allows us to assess how intervention has been applied across various settings and populations, enhancing our understanding of its generalizability and effectiveness. However, in cases where several publications report on the same trial, only those studies that contribute unique insights relevant to our primary interest in mental health outcomes associated with the intervention were included. Additionally, we prioritized studies that analyzed large original samples to ensure a comprehensive understanding of the intervention. This scoping review follows the Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews (PRISMA-ScR) guideline (see the Supplementary Table 2), and the protocol has been registered with the Research Registry (#reviewregistry1861).
Data extraction and analysis
Studies were screened firstly based on titles and abstracts, with this initial screening conducted independently by three researchers (J.H., Y.L., V.S.), each reviewing a subset of the studies. Title and abstract screening was conducted as single screening. Following this, full-text reviews of 141 papers was conducted, with each paper independently double screened by Y.L. and V.S. Any disagreements in the full-text screening process were resolved through discussions facilitated by a senior reviewer (J.H.). Data of the eligible papers were then extracted using a custom spreadsheet to record the study population, trial design, the intervention name, online intervention modalities and therapeutic model, region of development, content of intervention, study outcomes, and public availability (see Supplementary Table 3 for the final data collection form).
Each peer-reviewed study included in this review underwent quality assessment using the Joanna Briggs Institute (JBI) critical appraisal tools conducted by E.J. and Y.L. This approach involved examining items including study design, participant selection criteria, methods of intervention allocation, blinding procedures, and outcome measurement techniques. Each item was coded as “Yes” (“Y”, meeting the criterion), “No” (“N”, not meeting the criterion), and “Unclear” (“U”, not reported). If an item was not applicable to the study, its coding was left blank. The overall risk of bias for each study was determined by items on internal validity, excluding those on statistical validity. Thus, items 11–13 from the RCT appraisal tool and item 9 from the quasi-experimental appraisal tool were omitted from consideration. The risk of bias percentage was calculated from the number of “Yes” responses out of all applicable items—excluding any that were left blank. Based on this percentage, studies were categorized as high risk if fewer than 50% of the items are scored as “Y”, moderate risk if between 50% and 79% were scored as “Y”, and low risk if between 80% and 100% were scored as “Y”. The review’s compliance against the PRISMA-ScR guideline was assessed by J.H. and W.Y.Z. All the authors critically reviewed and approved the manuscript. Due to the heterogeneity among the studies, we organized the descriptive statistics based on interventions, creating separate entries for each eligible intervention within publications and combining studies that employed the same intervention or reported on the same trial into one entry.
Data availability
All data generated or analyzed in this study are provided in the published article and its supplementary information files.
References
Fu, Z., Burger, H., Arjadi, R. & Bockting, C. L. H. Effectiveness of digital psychological interventions for mental health problems in low-income and middle-income countries: a systematic review and meta-analysis. Lancet Psychiatry 7, 851–864 (2020).
Vigo, D., Thornicroft, G. & Atun, R. Estimating the true global burden of mental illness. Lancet Psychiatry 3, 171–178 (2016).
Eaton, J. et al. Scale up of services for mental health in low-income and middle-income countries. Lancet 378, 1592–1603 (2011).
Huang, Y. et al. Prevalence of mental disorders in China: a cross-sectional epidemiological study. Lancet Psychiatry 6, 211–224 (2019).
Shi, W., Shen, Z., Wang, S. & Hall, B. J. Barriers to professional mental health help-seeking among chinese adults: a systematic review. Front. Psychiatry 11, 442 (2020).
Xu, Z. et al. The state of mental health care in China. Asian J. Psychiatry 69, 102975 (2022).
Fang, M., Hu, S. X. & Hall, B. J. A mental health workforce crisis in China: a pre-existing treatment gap coping with the COVID-19 pandemic challenges. Asian J. Psychiatr. 54, 102265 (2020).
Zhang, X., Lewis, S., Firth, J., Chen, X. & Bucci, S. Digital mental health in China: a systematic review. Psychol. Med 51, 2552–2570 (2021).
Liu, J. et al. Mental health system in China: history, recent service reform and future challenges. World Psychiatry 10, 210–216 (2011).
University of Michigan Behavioral Health Workforce Research Center. Estimating the Distribution of the U.S. Psychiatric Subspecialist Workforce (University of Michigan School of Public Health, 2018).
Yin, H., Wardenaar, K. J., Xu, G., Tian, H. & Schoevers, R. A. Help-seeking behaviors among Chinese people with mental disorders: a cross-sectional study. BMC Psychiatry 19, 373 (2019).
Bond, R. R. et al. Digital transformation of mental health services. npj Ment. Health Res. 2, 13 (2023).
Liu, S. et al. Online mental health services in China during the COVID-19 outbreak. Lancet Psychiatry 7, e17–e18 (2020).
Groot, J. et al. The effectiveness of fully automated digital interventions in promoting mental well-being in the general population: systematic review and meta-analysis. JMIR Ment. Health 10, e44658 (2023).
Rongxing, G. in How the Chinese Economy Works (ed Guo Rongxing) 296–314 (Palgrave Macmillan UK, 2009).
Li, A. C., Wong, K. K., Chio, F. H., Mak, W. W. & Poon, L. W. Delivering mindfulness-based interventions for insomnia, pain, and dysfunctional eating through a text messaging app: three randomized controlled trials investigating the effectiveness and mediating mechanisms. J. Med Internet Res 24, e30073 (2022).
Liang, D., Han, H., Du, J., Zhao, M. & Hser, Y. I. A pilot study of a smartphone application supporting recovery from drug addiction. J. Subst. Abus. Treat. 88, 51–58 (2018).
Mak, W. W. et al. Efficacy and moderation of mobile app-based programs for mindfulness-based training, self-compassion training, and cognitive behavioral psychoeducation on mental health: randomized controlled noninferiority trial. JMIR Ment. Health 5, e60 (2018).
Mao, N. et al. Smartphone-based training of cognitive bias modification: efficacy for reducing social anxiety in chinese adolescents. J. Child Fam. Stud. 32, 2394–2405 (2023).
Sit, H. F. et al. A feasibility study of the WHO digital mental health intervention step-by-step to address depression among chinese young adults. Front. Psychiatry 12, https://doi.org/10.3389/fpsyt.2021.812667 (2022).
Li, G. et al. A WHO digital intervention to address depression among young Chinese adults: a type 1 effectiveness-implementation randomized controlled trial. Transl. Psychiatry 14, 102 (2024).
Song, J. et al. Self-help cognitive behavioral therapy application for COVID-19-related mental health problems: a longitudinal trial. Asian J. Psychiatr. 60, 102656 (2021).
Sun, X. et al. Cognitive bias modification for interpretation training via smartphones for social anxiety in Chinese undergraduates. J. Exp. Psychopathol. 10, 2043808719875274 (2019).
Sun, Y. et al. Effectiveness of smartphone-based mindfulness training on maternal perinatal depression: randomized controlled trial. J. Med. Internet Res. 23, e23410 (2021).
Wong, V. W.-H. et al. Smartphone-delivered multicomponent lifestyle medicine intervention for improving mental health in a nonclinical population: a randomized controlled trial. Front. Public Health 11, https://doi.org/10.3389/fpubh.2023.1231981 (2024).
Zheng, Y. et al. A peer-to-peer live-streaming intervention for children during COVID-19 homeschooling to promote physical activity and reduce anxiety and eye strain: cluster randomized controlled trial. J. Med. Internet Res. 23, e24316 (2021).
Zhu, Y. et al. A newly designed mobile-based computerized cognitive addiction therapy app for the improvement of cognition impairments and risk decision making in methamphetamine use disorder: randomized controlled trial. JMIR Mhealth Uhealth 6, e10292 (2018).
Liao, Y. et al. Effectiveness of a text-messaging-based smoking cessation intervention (“Happy Quit”) for smoking cessation in China: a randomized controlled trial. PLoS Med. 15, e1002713 (2018).
Chen, H. et al. Predictors of treatment outcomes and adherence in internet-based cognitive behavioral therapy for social anxiety in China. Behav. Cogn. Psychother. 48, 291–303 (2020).
Li, Y., Liao, W., Zhou, X., Wang, Y. & Qian, Q. An exploratory randomized controlled study of multidimensional computerized executive function training for children with attention deficit hyperactivity disorder. Chin. J. Psychiatry 50, 45–452 (2017).
Lin, L.-Y. et al. An internet-based intervention for individuals with social anxiety and different levels of Taijin Kyofusho in China. J. Cross-Cult. Psychol. 51, 387–402 (2020).
Mak, W. W., Chan, A. T., Cheung, E. Y., Lin, C. L. & Ngai, K. C. Enhancing Web-based mindfulness training for mental health promotion with the health action process approach: randomized controlled trial. J. Med. Internet Res. 17, e8 (2015).
Su, W., Fang, X., Miller, J. K. & Wang, Y. Internet-based intervention for the treatment of online addiction for college students in China: a pilot study of the Healthy Online Self-helping Center. Cyberpsychol. Behav. Soc. Netw. 14, 497–503 (2011).
Yeung, A. et al. Outcomes of an online computerized cognitive behavioral treatment program for treating chinese patients with depression: a pilot study. Asian J. Psychiatr. 38, 102–107 (2018).
Zhang, C. et al. One-week self-guided internet cognitive behavioral treatments for insomnia in adults with situational insomnia during the COVID-19 outbreak. Front. Neurosci. 14, https://doi.org/10.3389/fnins.2020.622749 (2021).
Ren, Z. et al. Effectiveness and mechanism of internet-based self-help intervention for depression: The Chinese version of MoodGYM. Acta Psychol. Sin. 48, 818–832 (2016).
Wang, H. et al. The effect of shame on patients with social anxiety disorder in internet-based cognitive behavioral therapy: randomized controlled trial. JMIR Ment. Health 7, e15797 (2020).
Wang, Z., Wang, J. & Maercker, A. Chinese My Trauma Recovery, a Web-based intervention for traumatized persons in two parallel samples: randomized controlled trial. J. Med. Internet Res. 15, e213 (2013).
Feng, X., Chai, X., Li, H., Cao, L. & Wang, J. The effect of virtual reality technology on the level of depression in patients with Parkinson's with depression. Zhejiang. Clin. Med 24, 248–250 (2022).
Lee Wong, C. et al. Effects of immersive virtual reality for managing anxiety, nausea and vomiting among paediatric cancer patients receiving their first chemotherapy: An exploratory randomised controlled trial. Eur. J. Oncol. Nurs. 61, 102233 (2022).
Li, B., Huang, G. & Ye, X. Effects of virtual reality-based attention training combined with sertraline treatment on cognitive function and brain area ratio low-frequency amplitude in minor depressed patients. Clin. Educ. Gen. Pract 21, 309–312 (2023).
Mao, W., Chen, W. & Wang, Y. Effect of virtual reality-based mindfulness training model on anxiety, depression, and cancer-related fatigue in ovarian cancer patients during chemotherapy. Technol. Health Care 32, 1135–1148 (2024).
Ran, L. et al. Application of virtual reality on non-drug behavioral management of short-term dental procedure in children. Trials 22, 562 (2021).
Zhang, W. et al. Virtual reality exposure therapy (VRET) for anxiety due to fear of COVID-19 Infection: a Case Series. Neuropsychiatr. Dis. Treat. 16, 2669–2675 (2020).
Zhu, J., Huang, N. & Wu, E. The effect of virtual reality technology combined with virtual scene exposure response/ritual blocking therapy technique on treatment adherence in female patients with obsessive-compulsive disorder. Matern. Child Health CareChina 38, 2101–2104 (2023).
Zhu, C., Sun, J. & Wang, Y. Efficacy of computer-assisted cognitive remediation therapy combined with antidepressants on cognitive functioning in patients with remitted depression. Chin. J. Health Manag 14, 142–147 (2020).
Living with Heart, <https://livingwithheart.psy.cuhk.edu.hk/ktf/> (2024).
moodgym, <https://www.moodgym.com.au>.
OCEBM Levels of Evidence Working Group. The Oxford Levels of Evidence 2. Oxford Centre for Evidence-Based Medicine https://www.cebm.ox.ac.uk/resources/levels-of-evidence/ocebm-levels-of-evidence.
Lattie, E. G., Stiles-Shields, C. & Graham, A. K. An overview of and recommendations for more accessible digital mental health services. Nat. Rev. Psychol. 1, 87–100 (2022).
Cuijpers, P., Boyce, N. & van Ommeren, M. Why treatment manuals of psychological interventions should be freely available. Lancet Psychiatry 11, 325–326 (2024).
Acknowledgements
The team expressed gratitude to all the research groups that shared information about their studies.
Author information
Authors and Affiliations
Contributions
J.H., B.J.H., and Y.L. concepted the study. JH developed search strategies with assistance from Y.L., V.S., B.J.H., and E.J. Y.L., V.S., and J.H. conducted data analysis and created charts. Y.L. and E.J. performed quality assessments. J.H. and W.Y.Z. reviewed the manuscript to ensure compliance with the PRISMA-ScR guidelines. Y.L. and V.S. wrote the initial draft of the manuscript under J.H.’s supervision. All authors contributed to the manuscript revision and approved the final version submitted.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Liu, Y., Shen, V.W., Jaime, E. et al. Digital mental health interventions in Chinese: a scoping review. npj Digit. Med. 8, 756 (2025). https://doi.org/10.1038/s41746-025-02129-5
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41746-025-02129-5