Abstract
Following traumatic cervical spinal cord injury (SCI), injury-induced functional changes within the perilesional forelimb circuits are an important cause of neurological dysfunction. K+/Cl− cotransporter 2 (KCC2) is a neuron-specific transmembrane protein essential for inhibitory neurotransmission. Reduced KCC2 expression post-SCI disrupts the excitatory/inhibitory ratio in spinal interneurons and blocks supraspinal neurotransmission. Recent advances in AAV9-based gene therapies present a promising approach to upregulate KCC2 and restore functional communication in the injured spinal circuits. This study aims to characterize the neurophysiological changes in a rodent model of bilateral contusion-compression cervical SCI and to assess the functional impact of KCC2 gene therapy in the injured spinal cord. We demonstrate that intrathecal AAV9 delivery of KCC2 enhances long-term forelimb and hindlimb motor recovery and improves neurophysiological outcomes following cervical SCI. This is accompanied by Luminex assay, transcriptional analysis, and immunohistochemical observations suggesting improvements in neuroanatomical preservation and neuroglial alterations in the perilesional circuits.
Similar content being viewed by others
Introduction
Traumatic spinal cord injury (SCI) results in devastating consequences to a patient’s health, independence, mobility, and quality of life1. With more than 15 million patients worldwide suffering from injured spinal cords according to the World Health Organization2, the need for safe, effective, and accessible treatment strategies is urgent. Following traumatic SCI, the presence of spared neural tissue at and adjacent to the injury site is critical for the potential recovery of disrupted spinal circuits3. However, despite retaining this spared neural tissue, the scope of neurological recovery in most SCI patients remains constrained largely due to insufficient functional recuperation in local neural circuits4,5. As such, while patients acutely present with flaccid, areflexic sensorimotor loss, this can progress over time into chronic hyperreflexic spastic paralysis6,7.
Despite the high prevalence of cervical injuries—affecting approximately two-thirds of traumatic SCI patients—our understanding of SCI-induced neuroplastic adaptations in the cervical and forelimb circuits remains limited8,9. The innervation of forelimb muscles arises from the brachial plexus emerging from the C5 to T1 nerve roots10. Neuroplastic alterations taking place in perilesional areas extending rostro-caudal to the cervical lesion core can encompass areas supplying the brachial plexus11. These neuroplastic changes are thought to account for functional alterations within spared cervical circuits. Supporting this, clinical and preclinical neurophysiological assessments, such as motor-evoked potential (MEP), have demonstrated functional disinhibition of the proximal perilesional tissue supplying the brachial plexus12. Strikingly, these neuroplastic changes can extend as far as the lumbar spinal cord after cervical injuries13.
Given the complexity of these neuroplastic changes, therapeutic interventions that modulate spinal interneurons have emerged as promising treatment strategies for activating the spared but dormant neural tissue to further enhance functional recovery—either alone or in combination with other therapeutics14,15. K+/Cl− cotransporter 2 (KCC2) is a neuron-specific symporter that maintains the chloride concentration in inhibitory synapses16. Reduced KCC2 activity post-SCI changes the concentration gradient of chloride ions, thus disabling the hyperpolarizing effects of inhibitory neurotransmitters17. Consequently, this disrupts the control of excitatory/inhibitory (E/I) output by GABAergic and glycinergic interneurons, which blocks the relay of signals in the cervical spinal cord18.
Previous work in a thoracic staggered double hemisection (SDH)19 mouse model, which involves two partial excisions in the spinal cord to completely interrupt the direct ascending and descending neural projections while enabling contralateral transmission in relay networks20, demonstrated the ability of KCC2 agonists to transform dysfunctional spinal circuits into a functional state21. However, KCC2 agonists (such as CLP290 & CLP257) pose potential adverse side effects and currently do not have clinical approval for any other condition22. Additionally, there is a need for continued KCC2 upregulation, and the cessation of agonist administration results in the loss of neurobehavioral improvements21. As such, therapeutic modulation of KCC2 in the injured spinal cord requires an efficacious delivery that minimizes off-target effects and eases clinical translation.
Gene therapy is a fast-evolving therapeutic strategy aimed at the delivery of nucleic acids to selectively alter the transcriptional profile of affected cells23,24. Systemic adeno-associated virus 9 (AAV9) administration is currently in the clinic for spinal muscular atrophy (SMA), and there are ongoing trials to test the efficacy of AAV9 particles for administration through the cisterna magna or via lumbar puncture25. AAV9 has a higher capacity than other serotypes of AAV to cross the blood-brain barrier, and by extension, the blood-spinal cord barrier26. However, challenges with systemic AAV9 administration include its high production cost and off-target transduction of non-specific cell types27. Targeted AAV9 delivery to the injured spinal cord allows sustainable episomal expression of KCC2, mitigating the need for the continued daily administration of KCC2 agonists and avoiding potential adverse off-target effects while improving long-term cost-effectiveness.
The objective of this study is to first characterize the neurophysiological properties of the perilesional forelimb circuits after bilateral contusion-compression cervical SCI and subsequently develop a clinically relevant KCC2 gene therapy approach to modulate these circuits while assessing its functional impact on long-term recovery. With this aim, we developed and optimized an AAV9-based KCC2 upregulation strategy as a targeted molecular approach to alter synaptic function within the injured spinal cord. This study demonstrates that AAV9-mediated KCC2 upregulation ameliorates neurophysiological MEP disinhibition in the cervical circuits, which results in enhanced functional recovery. To our knowledge, this is the first study to report the beneficial impact of KCC2 upregulation in a clinically relevant rat cervical SCI model using neurobehavioral, electrophysiological, molecular, and neuroanatomical readouts.
Results
Forearm neurophysiological disinhibition following cervical SCI
To assess forelimb-specific injury-induced functional neurophysiological alterations, a total of 12 Wistar rats were randomly divided into laminectomized shams and C6/7 SCI cohorts. Following 12 weeks of post-SCI neurobehavioral assessment (Supplementary Fig. 1), forelimb MEPs were recorded from the contralateral forearm in response to electrical stimulation of the sensorimotor cortex via transcranial stimulation with subcutaneous needle electrodes (Fig. 1A). The MEP assessment was conducted at 12 weeks post-SCI to investigate the chronic changes in signal transduction within forelimb circuits proximal to the injury epicenter, which project through the brachial plexus innervating the forearm muscles.
A Schematic overview of the forelimb MEP recording experiment (adapted from BioRender.com with permission). B, C Mean forearm MEP recordings in sham and SCI animals following 10 constant stimuli (10 mA and 0.3 ms). Each line represents the mean of 10 MEPs induced by 10 mA and 0.3 ms pulses in an individual animal. The group average and 95% confidence interval are represented by the central red line and the faded red area, respectively. D C6/7 SCI presents with a significantly higher mean MEP range. E MEP range across varying stimuli intensity. F MEP area under the curve (AUC) across varying stimulus intensities. G MEP range across varying stimulus durations. H MEP AUC across varying stimuli durations. I MEP range following a single pulse and a paired pulse with a 2 ms interval, demonstrating synaptic facilitation. J MEP range following consecutive paired pulses with varying intervals. Statistical inferences were based on unpaired two-tailed t-tests in (D) and repeated-measure two-way ANOVA with Geisser-Greenhouse correction for (E–J). All data in (D–J) are presented as mean ± SEM and were assessed for normality using the Shapiro–Wilk test. (ns: non-significance, *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001).
An average of 10 consecutive MEPs recorded at 10 mA and 0.3 ms was used to measure MEP range, latency, and duration (Fig. 1B–D). SCI animals exhibit a significantly higher MEP range (peak-to-peak amplitude) compared to the control laminectomized animals (1.046 ± 0.442 mV1/2; Mann–Whitney test; U = 4; p = 0.026). This is echoed by a similar increase of the MEP area under the curve (AUC) in C6/7 SCI animals compared to shams (0.038 ± 0.016 mV.s1/2, t(10) = 2.284, p = 0.046). However, no significant change was observed in latency and MEP width (Supplementary Fig. 2A–C).
To further explore the excitability and the stimulus-response profile of the forelimb circuits between injured and control animals, two sets of electrophysiological experiments with varying degrees of stimulus intensity and stimulus duration were conducted. First, varying the intensity of electrical pulses from 1 to 15 mA demonstrated a significant difference in the stimulus-response relationship between sham and SCI animals (Fig. 1E, F, Supplementary Fig. 3). This is evident by both MEP range (repeated-measure two-way ANOVA with the Geisser-Greenhouse correction; stimulus intensity: F(2.928, 29.28) = 16.90, p < 0.0001; cohort: F(1, 10) = 4.684, p = 0.056; interaction: F(12, 120) = 3.377, p = 0.0003) and MEP AUC (repeated-measure two-way ANOVA with the Geisser-Greenhouse correction, stimulus intensity: F(2.397, 23.97) = 16.64, p < 0.0001; cohort: F(1, 10) = 4.376, p = 0.063; interaction: F(12, 120) = 3.413, p = 0.0003). Second, varying stimulus intervals ranging from 0.1 ms to 0.5 ms demonstrated a similar stimulus-response profile difference in both MEP range (repeated-measure two-way ANOVA with the Geisser-Greenhouse correction, stimulus duration: F(2.872, 25.85) = 14.02; p < 0.0001; cohort: F(1, 9): 7.447, p = 0.023; interaction: F(4, 36): 5.215; p = 0.002) and MEP AUC (repeated-measure two-way ANOVA with the Geisser-Greenhouse correction, stimulus duration: F(2.344, 21.10) = 13.31, p < 0.0001; cohort: F(1, 9) = 4.757, p = 0.057; interaction: F(4, 36) = 5.433, p = 0.002) between sham and SCI animals (Fig. 1G, H, Supplementary Fig. 4).
To further characterize the neuroplastic nature of the injured spinal cord, paired pulses with varying short stimulus intervals were conducted to assess synaptic facilitation and inhibition (Fig. 1I, J). While two pulses with a 2 ms interval exhibits a higher MEP range in both uninjured shams and SCI animals compared to a single pulse, no difference in the MEP range augmentation between sham and SCI was observed (repeated-measure two-way ANOVA; pulse number: F(1, 10) = 14.17, p = 0.004; cohort = F(1, 10) = 3.152, p = 0.106; interaction: F(1, 10) = 0.221, p = 0.648). With varying paired-pulse intervals, there was a greater decline in MEP range in SCI compared to control shams (repeated-measure two-way ANOVA with the Geisser-Greenhouse correction; pulse interval: F(2.955, 29.55) = 16.77, p < 0.0001; cohort: F(1, 10) = 1.552, p = 0.241; interaction: F(19, 190) = 2.890, p = 0.0001).
Intrathecal AAV9 administration enables modulation of cervical interneurons
The increased MEP range is suggestive of impaired inhibitory neurotransmission and imbalanced E/I signaling. KCC2 is an emerging approach to restore inhibitory neurotransmission, but challenges in its pharmacological implementation limit its clinical translatability. As such, we seek to develop an AAV9 approach to augment KCC2 expression. For this purpose, AAV9s expressing either KCC2 or the control EGFP were microinjected (1.0 × 1012 GC kg−1) into the C6/7 subarachnoid space at either 15-min post-SCI (acute) or 1-week post-SCI (subacute) to determine the optimal time point for intrathecal AAV9 administration and to characterize its transgenic expressional pattern following traumatic cervical SCI (Fig. 2A). All transgenic expressions were under human synapsin 1 promoter, which solely targets the neuronal population28 (Supplementary Fig. 5). In addition, both cervical and thoracic spinal cords were isolated to investigate the spread of AAV9 particles following either acute or subacute microinjections.
A Schematic overview of the localized intrathecal AAV9 injection at acute (total n = 16) and subacute (total n = 19) timepoints (adapted from BioRender.com with permission). B Slc12a5 expression at the acute time point in the injury epicenter and caudal thoracic spinal cord. C Slc12a5 expression at the subacute time point in the injury epicenter and caudal thoracic spinal cord. D Difference in Slc12a5 expression between acute and subacute injections. E 10× confocal images of the injured spinal cord demonstrate the efficacy of localized intrathecal AAV9 administration to induce episomal EGFP expression. The cell nucleus is represented by DAPI. All data are presented as mean ± SEM (*p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001).
For the acute time point, a total of 16 Wistar rats were randomly divided into four groups, including 5 C6/7 laminectomized shams, 5 C6/7 clip-compression injured rats, 3 injured rats injected with AAV9-Syn-EGFP, and 3 injured rats injected with AAV9-Syn-KCC2 (Fig. 2B). The AAV9 particles were microinjected at the injury site 15 min following clip-compression injury, and rats underwent transcardial perfusion 1-week post-operation. AAV9-Syn-KCC2 induced a significant increase in Slc12a5 expression compared to AAV9-Syn-EGFP at the lesion site (2.904 ± 0.457 log2RQ; mixed-effects analysis with Sidak’s multiple comparison; adjusted p < 0.0001), evident by reverse transcription-quantitative polymerase chain reaction (RT-qPCR).
For subacute injection, a total of 19 Wistar rats were similarly divided into 5 C6/7 laminectomized shams, 4 C6/7 clip-compression injured rats, 5 injured rats injected with AAV9-Syn-EGFP, and 5 injured rats injected with AAV9-Syn-KCC2 (Fig. 2C). RT-qPCR revealed increased Slc12a5 expression in the AAV9-Syn-KCC2 compared to the AAV9-Syn-EGFP (3.385 ± 0.314 log2RQ; mixed-effects analysis with Sidak’s multiple comparison; adjusted p < 0.0001), and there was a significant downregulation of KCC2 expression in the thoracic cord compared to the injury epicenter due to the decreased viral load (−2.384 ± 0.280 log2RQ; mixed-effects analysis with Sidak’s multiple comparison; adjusted p = 0.0002).
The intrathecal AAV9 injection does not exert any significant change on the SCI-induced downregulated KCC2 expression when injected acutely or subacutely, as evident by comparison to the SCI controls (Fig. 2B, C). Overall, subacute AAV9 injection showed greater transduction and lower variability compared to acute injection (Fig. 2D). Furthermore, a representative immunohistochemical analysis of the injured spinal cord following subacute localized intrathecal administration of AAV9-Syn-EGFP reveals successful EGFP expression at both the perilesional dorsal and ventral horns at 1-week post-injection (Fig. 2E). These observations validate the effectiveness of localized intrathecal AAV9 microinjections to upregulate KCC2 expression locally at the lesioned and perilesional spinal tissue without any adverse effects.
KCC2 upregulation enhances functional neurobehavioral recovery
While the localized intrathecal delivery of KCC2-expressing AAV9 particles provides an exciting clinically relevant approach, the long-term impact of KCC2 upregulation in a bilateral contusion-compression injury is unexplored. Hence, randomly divided C6/7 injured Wistar rats underwent a long-term neurobehavioral assessment by blinded observers to investigate the impact of AAV9-mediated KCC2 upregulation on forelimb and hindlimb functional recovery. The injured rats received 1.0 × 1012 GC kg−1 of either AAV9-Syn-KCC2 (n = 10) or AAV9-Syn-EGFP (n = 9) subacutely at 1-week post-SCI. In addition, three non-injured shams were included as reference points that solely underwent C6/7 laminectomy.
KCC2 upregulation resulted in a significant improvement on the forelimb locomotor assessment scale (FLAS) at 12 weeks post-SCI (Kruskal–Wallis test with Dunn’s multiple comparison; mean rank difference = 6.650, adjusted p = 0.026) (Fig. 3A, B). Similarly, modest improvement in forelimb grip strength was observed over the 12 weeks of recovery after SCI (Fig. 3C, repeated-measure two-way ANOVA; time: F(11, 187) = 64.39, p < 0.0001; cohort: F(1, 17) = 1.209; p = 0.29; interaction: F(11, 187) = 1.861, p = 0.047). Additionally, the inclined plane assessment suggests significantly enhanced trunk stability in the KCC2-treated group compared to the control rats, which translated into 9.44 ± 3.39° of improvement on an inclined plane at 12 weeks post-SCI (Fig. 3D; repeated-measure two-way ANOVA; p = 0.006; q = 0.032). Open-field locomotor BBB assessment also demonstrated significant incremental hindlimb improvement in the rats receiving AAV9-Syn-KCC2 compared to the control AAV9-Syn-EGFP rats (Fig. 3E; repeated-measure two-way ANOVA; time: F(13, 221) = 287.4, p < 0.0001; cohort: F(1, 17) = 2.769, p = 0.114; interaction: F(13, 221) = 4.484, p < 0.0001). This improvement resulted in a 2.61 ± 1.04 BBB score difference at 12 weeks post-SCI between the KCC2-treated rats compared to the EGFP control rats (repeated-measure two-way ANOVA; p = 0.013; q = 0.038). KCC2 upregulation did not have a significant impact on animal weight (repeated-measure two-way ANOVA; time: F(12, 228) = 98.44, p < 0.0001; cohort: F(2, 19) = 1.091, p = 0.356; interaction: F(24, 228) = 1.409, p = 0.103). Strikingly, while previous studies suggest a link between KCC2 function and pain sensitivity29,30,31, no significant difference in hindlimb von Frey pain threshold was observed (Supplementary Fig. 6).
A Representative FLAS images showing enhanced forelimb recovery following KCC2 upregulation. B Averaged FLAS score by two independent observers, compared with one-way ANOVA with Dunnett multiple comparison. C Forelimb grip strength quantified by grip strength meter (SDI Grip strength system) reveals incremental improvement in KCC2-treated rats compared to EGFP control. D Average inclined plane measurement reveals gradual improvements in trunk stability. E Improved hindlimb function recorded by open-field BBB following AAV9-mediated KCC2 upregulation. F Representative CATWALK runs for each group. G, H CatWalkTM analysis demonstrated enhanced recovery in stride length following KCC2 gene therapy (two-way ANOVA using FDR according to the two-stage linear set-up procedure of Benjamini, Krieger, and Yekutieli to correct for multiple comparisons). Time-coursed data analyzed with repeated-measure two-way ANOVA using FDR according to the two-stage linear set-up procedure of Benjamini, Krieger, and Yekutieli to correct for multiple comparisons. Statistically significant changes are illustrated with an asterisk (*). All data were checked for normality using the Shapiro–Wilk test and are presented as mean ± SEM (*p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001).
All rats exhibited weight support (evident by BBB score ≥ 9) at 12 weeks post-SCI and were included in the CatWalkTM Gait Analysis (Fig. 3F). Principal Component Analysis (PCA) identified patterns and structures in the CATWALKTM runs. For forelimb readouts, the first two principal components (Dim1 and Dim2) explained 60.7% and 24.3% of the variance in the data, respectively. In contrast, the first two principal components (Dim1 and Dim2) for the hindlimb explained 58.0% and 15.7% of the variance in the data. Using the first two principal components as the clustering variables, the animals were clustered into the corresponding experimental groups using K-means. The loadings of the original variables on the principal components were plotted and examined (Supplementary Fig. 7). AAV9-mediated KCC2 upregulation increased forelimb stride length by 0.273 ± 0.114 cm compared to the EGFP control group (Fig. 3G; two-way ANOVA; F(1, 17) = 5.768, adjusted p = 0.028). Similarly, KCC2-treated rats demonstrated enhanced hindlimb stride length by 0.670 ± 0.230 cm compared to the EGFP control group (Fig. 3H; two-way ANOVA; F(1, 17) = 8.463, adjusted p = 0.009).
Improved neurophysiological outcomes with KCC2 upregulation after cervical SCI
Following neurobehavioral assessments, electrophysiological recordings were conducted at 12 weeks post-SCI to assess the influence of KCC2 upregulation on signal transduction across the injured spinal cord and on functional changes within the cervical circuits. Similar to the previous experiment, forelimb MEPs were recorded from the contralateral forearm in response to electrical stimulation of the sensorimotor cortex. An average of 10 consecutive MEPs recorded at 10 mA and 0.3 ms was used to measure MEP range, AUC, latency, and duration (Fig. 4A–D, Supplementary Fig. 8A, B). KCC2 upregulation significantly reduced MEP range (0.812 ± 0.361 mV1/2; Kruskal–Wallis test with Dunn’s multiple comparison; adjusted p: 0.048) and AUC (0.031 ± 0.013 mV.s1/2; Kruskal–Wallis test with Dunn’s multiple comparison; adjusted p: 0.024). Additionally, MEP latency was significantly reduced in the KCC2-treated rats compared to the EGFP control (2.698 ± 1.051 ms; one-way ANOVA with Holm–Sidak’s multiple comparison; adjusted p: 0.019), but no difference in MEP duration was observed.
A Mean forearm MEP recordings in sham, AAV9-Syn-EGFP, and AAV9-Syn-KCC2, using 10 MEPs involving pulses with 10 mA and 0.3 ms in duration. B MEP range quantification in the mean forearm MEP. C MEP AUC quantification in the mean forearm MEP. D Peak latency quantification in mean forearm MEP. E, F Increasing stimulus intensity at 0.1 ms pulse duration increases the MEP range and AUC. KCC2 gene therapy restores the MEP range and AUC. G, H Increasing stimulus duration at 10 mA intensity similarly increases MEP range and AUC. KCC2 gene therapy restores the forelimb MEP range back to an uninjured level. I, J Paired-pulse quantifications. Statistical analysis included the Shapiro–Wilk test to assess Gaussian distribution, followed by either one-way ANOVA or repeated-measure two-way ANOVA with Geisser-Greenhouse correction. All data are presented as mean ± SEM (*p < 0.05, **p < 0.01).
To determine the excitability and maximal response, the stimulus-response relationship was obtained by varying the intensity of electrical pulses from 1 to 15 mA (Fig. 4E, F, Supplementary Fig. 8C). Consistent with the previous findings, the threshold to induce an MEP response was lower in injured compared to non-injured rats, indicating higher excitability of the forelimb circuits after C6/7 SCI. Notably, KCC2-upregulation significantly lowered the MEP range, reflecting a restoration of spinal excitability (repeated-measure two-way ANOVA with the Geisser-Greenhouse correction; stimulus intensity: F(1.804, 30.66) = 12.57, p = 0.0002; cohort: F(1, 17) = 4.569, p = 0.047; interaction: F(12, 204) = 3.366, p = 0.0002). This is also echoed by restored MEP AUC in the KCC2-treated group compared to the EGFP control group (repeated-measure two-way ANOVA with the Geisser-Greenhouse correction, stimulus intensity: F(12, 204) = 11.94, p < 0.0001; cohort: F(1, 17) = 4.269, p = 0.054; interaction: F(12, 204) = 3.213, p = 0.0003).
Similarly, increasing the pulse duration from 0.1 ms to 0.5 ms increased the MEP range and demonstrated a similar pattern (repeated-measure two-way ANOVA with the Geisser-Greenhouse correction; stimulus duration: F(2.430, 41.31) = 13.73, p < 0.0001; cohort: F(1, 17) = 6.538, p = 0.020; interaction: F(5, 85) = 2.238, p = 0.059), but it plateaued in the AAV9-Syn-EGFP rats after pulse duration exceeded 0.4 ms (Fig. 4G, H, Supplementary Fig. 8D). This is also echoed by similar changes in MEP AUC following varying pulse duration (repeated-measure two-way ANOVA with the Geisser-Greenhouse correction; stimulus duration: F(2.040, 34.68) = 17.35, p < 0.0001; cohort: F(1, 17) = 6.738, p = 0.019; interaction: F(5, 85) = 3.093, p = 0.013).
To assess the impact of KCC2 upregulation on synaptic facilitation and depression, paired pulses with varying intervals were used (Fig. 4I, J). Paired stimuli with 6 ms intervals demonstrate restored MEP range following KCC2 upregulation (repeated-measure two-way ANOVA; pulse number: F(1, 17) = 16.01, p = 0.0009; cohort = F(1, 17) = 7.893, p = 0.012; interaction: F(1, 17) = 0.458, p = 0.508). Similarly, KCC2 upregulation suggests the restoration of the synaptic depression profile (Fig. 4J). This is evident by the impact of varying paired-pulse intervals on the MEP range (repeated-measure two-way ANOVA with the Geisser-Greenhouse correction, pulse interval: F(2.069, 35.17) = 36.73, p < 0.0001; cohort: F(1, 17) = 10.67, p = 0.005; interaction: F(3, 51) = 2.393, p = 0.079).
Neuroanatomical effects of KCC2 upregulation on cervical circuits
To examine the long-term impact of localized AAV9 injection and its diffusion in the spinal cord parenchyma, the spinal cords were isolated at 12 weeks post-SCI and randomly sectioned in either sagittal (n = 4) or axial planes (n = 5). These sectioned cords were stained for NeuN and imaged to visualize the AAV9-expressed EGFP in relation to the preserved neuronal nuclei. The results illustrate localized EGFP expression in the injured spinal cord at 12 weeks post-SCI, in addition to validating the long-term expression of virally expressed proteins following AAV9 administration (Fig. 5A–D). To test whether KCC2 upregulation causes any alterations in sprouting near the lesion core, the spinal cords cut in the sagittal direction were stained for serotonin (5HT) and β3-tubulin (Fig. 5E–H). There was no statistically significant difference in the 5HT+ and β3-tublin+ areas (unpaired t-test on averaged 5HT+/β3-tublin+ areas, p = 0.97).
A The transgenic expression of EGFP demonstrates the extent of AAV9 diffusion in the injured spinal cord in a longitudinal slide. B, C Higher magnification images of regions shown in (A). D Axial section at the injury epicenter demonstrating the extent of AAV9-induced EGFP expression. E Representative confocal images of the cervical spinal cord stained for β3-tubulin (Blue) and 5HT (Red) in sham, EGFP/non-treated, and KCC2-treated rats, collected 12 weeks post-SCI. The intensity of F β3-tubulin and G 5HT staining was quantified using Fiji software. H The ratio of 5HT and β3-tubulin was calculated across the rostro-caudal region 2 mm from the SCI epicenter in EGFP/non-treated and KCC2-treated spinal cords. All data are presented as mean ± SEM.
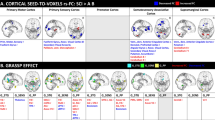
To further explore the neuroplastic alterations to spinal neural circuits at the injured spinal cord, the axial total NeuN count, glutamate decarboxylase (GAD67)+ area, vesicular GABA transporter (VGAT)+ area, and vesicular glutamate transporter 2 (VGluT2)+ area were quantified at −1920 µm, −960 µm, 0 µm, 960 µm, and 1920 µm relative to the injury epicenter (Fig. 6, Supplementary Fig. 9A–D). KCC2 upregulation increased the neuronal count compared to the EGFP control (0.358 ± 0.111 log2 sham-normalized NeuN+ cell count; unpaired t-test; t(8) = 3.239; p = 0.012). GAD67 and VGAT are important markers of inhibitory interneurons. GAD67 is one of the two isoforms of glutamate acid decarboxylase, which catalyzes the conversion of L-glutamic acid to γ-aminobutyric acid (GABA)32. VGAT is highly concentrated in GABAergic and glycinergic nerve endings33, and is responsible for the vesicular packaging and exocytosis of neurotransmitters34. KCC2 upregulation increased preservation of GAD67+ area (0.378 ± 0.113 log2 sham-normalized GAD67+ area; unpaired t-test; t(8) = 3.33; p = 0.010) and VGAT+ area (0.820 ± 0.289 log2 sham-normalized VGAT+ area; Welch’s t-test; t(4.02) = 2.837; p = 0.047). VGluT2 was expressed in excitatory interneurons. However, no significant observation in the VGluT2+ area was observed (unpaired t-test; t(8) = 0.183; p = 0.859).
A Representative confocal images for NeuN, GAD67 (threshold), VGAT (threshold), and VGlut2 (threshold) at 960 µm. B–E The mean quantification across −1920 µm, −960 µm, 0 µm, 960 µm, and 1920 µm relative to the SCI epicenter. B Elevated NeuN cell counts at and around the lesion site. Total NeuN+ cell count. C GAD67+ area is significantly higher in the KCC2-treated group compared to the EGFP control. D Similarly, the VGAT+ area is significantly higher in the KCC2-treated group compared to the EGFP control. E No statistically significant alteration in the Vglut2+ area was observed. All data are presented as mean ± SEM, normalized to the uninjured sham group, checked for Gaussian distribution using the Shapiro–Wilk test, and analyzed using t-test following log2 transformation (ns: non-significant, *p < 0.05, **p < 0.01).
KCC2 upregulation alters the synaptic microenvironment
To further examine the impact of KCC2 upregulation on local synapses after injury, the immediate neuroglial response in the injured spinal cord at 1-week post-KCC2 induction was analyzed using a multiplex Luminex assay. AAV9 did not alter the local inflammatory response in the injured spinal cord (Fig. 7A, B). KCC2 upregulation elevated the Interferon gamma-induced protein 10 (IP-10; also referred to as C-X-C motif chemokine ligand 10; CXCL10) cytokine level in the injured spinal cord compared to the EGFP control (1.406 ± 0.387 log2 fold change; one-way ANOVA with Holm–Sidak multiple comparison; adjusted p = 0.012). This was echoed by upregulation of the Cxcl10 gene (2.325 ± 0.727 log2RQ; one-way ANOVA with Holm–Sidak multiple comparison; adjusted p = 0.017), which encodes for IP-10 protein (Fig. 7C). To further investigate the long-term impact of such chemokine alteration, immunohistochemical analysis at 12 weeks post-SCI revealed reduced IBA1+ cells (unpaired t-test; -0.822 ± 0.283 log2 sham-normalized IBA1+ cells; p = 0.020) and no change in GFAP+ area (unpaired t-test; −0.052 ± 0.170 log2 sham-normalized GFAP+ area; p = 0.768) in the injured spinal cord following KCC2 upregulation (Fig. 7D–F, Supplementary Fig. 9E, F).
A Heatmap with hierarchical clustering performed based on cosine similarity. Statistically significantly altered cytokines/chemokines are indicated by asterisks (*), as determined by ANOVA using FDR according to the two-stage linear set-up procedure of Benjamini, Krieger, and Yekutieli to correct for multiple comparisons. B KCC2 upregulation elevates the level of IP-10. C Cxcl10 expression coding for IP-10 expression was significantly upregulated in the injured spinal cord receiving AAV9-Syn-KCC2. D Representative images of GFAP and IBA1 immunohistochemical staining at 1920 µm rostral to the SCI epicenter. E KCC2 upregulation does not alter GFAP+ area. F KCC2 upregulation significantly reduces IBA1+ area. G, H AAV9-mediated KCC2 upregulation reduces the expression of KCC2-related genes and alters the expression of Mecp2 transcription factor. All data are presented as mean ± SEM (ns: non-significant, *p < 0.05).
Pursuing this further, selective transcriptional characterization of the KCC2 interactome at 7 days post-injection demonstrated the ability of AAV9-mediated KCC2 upregulation to alter the expressional pattern of other chloride cotransporters, such as Slc12a2 (0.357 ± 0.097 log2RQ; one-way ANOVA with Holm–Sidak multiple comparison; adjusted p = 0.007) and Slc12a4 (0.278 ± 0.094 log2RQ; one-way ANOVA with Holm–Sidak multiple comparison; adjusted p = 0.026). KCC2 upregulation also changes the expression of Jam2 (0.496 ± 0.122 log2RQ; one-way ANOVA with Holm–Sidak multiple comparison; adjusted p: 0.004) and Gabrg1 (0.425 ± 0.156 log2RQ; one-way ANOVA with Holm–Sidak multiple comparison; adjusted p = 0.039). Furthermore, KCC2 upregulation altered the expression of the Mecp2 transcription factor (0.207 ± 0.076 log2RQ; one-way ANOVA with Holm–Sidak multiple comparison; adjusted p = 0.043) (Fig. 7G, H, Supplementary Fig. 10).
Discussion
This translationally focused research builds upon strong foundational proof-of-concept data to address the necessary knowledge gaps for clinical translation of KCC2-based therapeutics21,35. To the best of our knowledge, this is the first study to examine the impact of KCC2 upregulation in traumatic cervical SCI and to utilize a localized AAV9 approach to upregulate the KCC2 gene in the injured spinal cord. This is also the first study to compare and contrast acute and subacute AAV9 injections into the cerebrospinal fluid at the subarachnoid space on top of the lesion core to induce KCC2 expression. This approach focuses the viral load at the site of injury, reducing both cost and off-target effects. Using this approach, we demonstrated that KCC2 upregulation can enhance functional recovery incrementally over time. Importantly, the observed improvements in electrophysiological response and immunohistochemical markers suggest that the observed enhanced recovery is through neuromodulatory and neuroplastic effects.
The findings of this study have important clinical implications for individuals sustaining cervical SCIs. With a life expectancy spanning several decades from the time of injury, cervical SCI can lead to a prolonged life with permanent disability, along with an estimated direct lifetime cost of up to 5 million USD per patient36. Furthermore, there is a critical knowledge gap on the elucidation of cervical-specific neuroplastic alterations, as most preclinical studies to date have utilized thoracic injury models aimed at assessing hindlimb recovery37, despite traumatic SCI most often occurring at the cervical level1. This highlights the need for the characterization of cervical-specific changes and developing neuromodulatory treatments for cervical SCIs.
Many cervical SCI patients with complete sensorimotor dysfunction, classified as ASIA Impairment Scale grade A, possess spared neural tissue at the site of injury21. Yet, these patients often show complete paralysis with minimal recovery over time4,38,39,40. Decades of research have attempted to improve sensorimotor recovery in these patients by reconstituting the precise neural circuits lost due to the injury. However, recent observations and evidence of synaptic plasticity, axonal sprouting, and spontaneous circuit reorganization after SCI have put forward a new approach to neuromodulate the spared neural circuits to regain function and result in the formation of new circuits to bypass the injury site3,41. In recent years, there has been attention directed towards the therapeutic potential of KCC2, yet the impact of KCC2 modulation in a clinically relevant SCI model has not been investigated, and in particular, no studies to date have been undertaken in models of cervical injury.
The present study demonstrates neuroplastic changes in the injured cervical spinal cord, which are highlighted by both the restored MEP response and the altered immunohistochemical markers of different neuronal populations. The electrophysiological findings of this study are in line with a recent study that examined the MEP response in large animal models and humans with traumatic SCI12. According to these large animal models and human observations, the amplitude of MEP recording in the abductor digiti minimi muscle—which is innervated by the ulnar nerve originating from C8/T1 and located above the injury site—is greater compared to the uninjured control in neural circuits at and above the injury site12. Our findings expand on this by utilizing a wide range of stimulus intensities and durations, optimized from previously described protocols42,43. We demonstrate that the threshold to induce a response is lower in the injured spinal cord, which results in a significantly higher MEP amplitude following traumatic SCI. This could be due to the altered inhibitory neurotransmission caused by KCC2 downregulation following traumatic SCI. Interestingly, AAV9-mediated KCC2 upregulation lowers the MEP amplitude and restores the MEP threshold to near uninjured levels. Furthermore, the decrease in MEP latency following KCC2 gene therapy suggests that restored inhibitory neurotransmission enhances signal transduction in the injured spinal cord and ultimately improves functional outcomes.
Our neurobehavioral findings demonstrate that KCC2 upregulation significantly enhances both forelimb and hindlimb recovery following traumatic cervical SCI. Forelimb-specific readouts that suggest improved recovery following KCC2 upregulation include FLAS44, forelimb grip strength45, and forelimb stride length (gait analysis)46. Similarly, hindlimb-specific readouts that demonstrate improved recovery include open-field BBB and hindlimb stride length46,47. Other readouts, such as inclined plane assessment, which primarily assesses trunk stability, involve both forelimb and hindlimb function and suggest improvements in overall postural control and coordinated motor output following KCC2 upregulation48. These enhancements in hindlimb locomotor recovery may reflect E/I balance reconstitution and functional activation of spared neurons, resulting in improved descending control over lumbar circuits via the corticospinal tract49. Furthermore, enhancement in forelimb readouts suggests improved functional neurotransmission at or near the lesion site involving extrapyramidal tracts50,51.
In line with these functional changes in the cervical circuits, our results also suggest that restoring inhibitory neurotransmission through KCC2 upregulation led to lasting neuroanatomical changes to the injured cervical spinal cord. As we did not observe any changes in axonal sprouting—which is often evident following rehabilitation training—we can further differentiate the neuroplastic mechanism behind KCC2 gene therapy from other neuromodulatory treatments, such as rehabilitation or epidural stimulation20,21,52. Instead, we observed enhanced neuronal preservation mostly in inhibitory interneurons. This echoes the findings of neurodevelopmental studies in which interneuron survival is influenced by balanced E/I neurotransmission, neuronal activity, and activity-dependent signaling53,54. These parallels suggest that KCC2-driven functional improvements may engage similar survival-promoting mechanisms in the injured spinal cord. Furthermore, while the underlying mechanisms behind delayed neuronal pathologies in the injured spinal cord are not entirely elucidated, recent findings highlight reduced neuronal swelling as a mechanism for delayed neuronal survival following Na+-K+-Cl− cotransporter 1 (NKCC1) modulation55.
This study also demonstrates that AAV9-mediated KCC2 upregulation induces distinct local molecular and cellular changes that may contribute to neuroglial modulation and synaptic remodeling in the injured spinal cord microenvironment. Transcriptional changes were also observed in other members of the Solute Carrier 12 (SLC12) family of cation-chloride cotransporters, such as Slc12a2 and Slc12a4, which encode NKCC1 and KCC1, respectively56. These findings suggest that KCC2 upregulation affects the regulation of other chloride cotransporters. Furthermore, changes in Jam2 and Gabrg1 indicate changes in cell adhesion and inhibitory synaptic regulation, potentially reflecting circuit-level reorganization post-injury. Moreover, the upregulation of Mecp2, a transcription factor associated with synaptic plasticity and epigenetic control, hints at a broader role for KCC2 in influencing gene regulatory networks involved in neuronal adaptation and repair. Additionally, changes in IP-10 level57,58, particularly given the concurrent reduction in IBA1+ microglia/macrophages and unchanged GFAP+ astrocytic reactivity at 12 weeks post-SCI59, hint at potentially close involvement of other cell types in regulating inhibitory synapses. Collectively, these findings highlight the complex role of KCC2 in the post-SCI spinal cord milieu.
Previous research on KCC2 in the context of SCI supports and complements our findings. Bilchak et al. demonstrated that CLP257 (KCC2 agonist) administration to Sprague Dawley rats with a T12 spinal cord transection restores endogenous inhibition and alleviates spastic symptoms35. This was evident by improvements in H-reflex depression as well as reduced phasic and tonic electromyography responses35. Interestingly, these CLP257 improvements resemble improvements observed by rehabilitative interventions, such as bicycle training35. In a follow-up study, the same group demonstrated that KCC2 augmentation improves stepping ability by normalizing reflex responses in multiple pathways and reducing muscle co-contraction without weakening motor output60. Similarly, Beverungen et al. demonstrated that both KCC2 and brain-derived neurotrophic factor (BDNF) play critical roles in mediating the anti-spastic effects of rehabilitation61. In the study by Beverungen et al., rats with a T12 transection received either the KCC2 inhibitor VU0240551 or the BDNF scavenger TrkB-IgG during daily rehabilitation sessions61. At four weeks post-injury, blockade of either pathway impaired frequency-dependent depression of the H-reflex, a key marker of hyperreflexia, thereby confirming the importance of KCC2 and BDNF in the modulation of spinal reflex excitability during recovery61.
Further research into pathway-specific changes following KCC2 upregulation would be of great interest. While the intricate connections of ascending and descending pathways and the role of spinal interneurons on the modulation of signal processing continue to be active areas of research, our understanding of how these networks contribute to differential functional changes remains limited. For instance, the unchanged hindlimb von Frey threshold and sensitivity following KCC2 upregulation in cervical SCI highlights this point. One potential explanation is that hindlimb von Frey examines the somatic mechanical allodynia or hyperalgesia from hindlimb circuits, decussating at the level of innervation and carried by the spinothalamic tract to the ventral posterior nucleus of the thalamus and subsequently the somatosensory cortex62. A potential explanation is that the spinothalamic tract, either the myelinated lateral or the unmyelinated ventral spinothalamic tract, is unaffected by the changes in inhibitory neurotransmission at the perilesional cervical level following KCC2 upregulation63. This does provide an intriguing avenue for future research to further understand the forelimb-specific pain pathways and the role of KCC2 modulation in alleviating such forelimb-specific pain after cervical injuries.
The localized intrathecal AAV9 delivery optimized in this study can have diverse applicability for future experiments and clinical translation. In the past decade, six gene therapies have gained clinical approval. Adeno-associated viral (AAV) particles are based on naturally occurring non-pathogenic small parvoviruses, which are capable of introducing a gene of interest, such as KCC2, into mammalian cells64. However, to ensure translational feasibility, the development of AAV-based therapeutics needs to consider viral packing, viral tropism, viral toxicity, and expression dynamics65. In contrast to lentiviral vectors, AAVs are well-suited for widespread clinical use as they do not integrate into the host genome66. AAVs have a packaging capacity of around 4.7 kb, which is considerably lower than the lentiviral capacity66. The AAV capsid can vary according to the serotype, ranging from AAV1 to AAV10, with recombinant alterations that can enable enhanced CNS penetrance or diminished immunoreactivity25,67,68,69,70. Importantly, these viruses are all replication-defective and non-enveloped viruses, which can be handled under Biosafety level 1 (BSL1) if they are not produced using a helper virus and do not express an oncogenic or toxic protein.
The clinical approval of AAV2-based and AAV9-based therapeutics for Leber congenital amaurosis and spinal muscular atrophy, respectively, has accelerated the development of gene therapy agents, particularly for neurological conditions. While AAV9 demonstrates a moderate ability to cross the blood-spinal cord barrier, the high financial costs limit its applicability for systemic injection into adult SCI patients71. Additionally, systemic AAV administration increases the risk of inflammation and adverse off-target effects. Therefore, an alternative approach would be to inject the AAV9 particles intrathecally to minimize off-target effects and overall costs by reducing the viral load. This has shown to be quite effective, but previous intrathecal injections of AAV9 into the cisterna magna have demonstrated pathology in the dorsal root ganglia25,72. Subpial injection provides an alternative but can cause damage due to the close proximity of the pia mater to the parenchyma73.
The present study aimed to examine the injection of AAV9s intrathecally at the site of injury to upregulate KCC2 expression. This strategy demonstrates a targeted AAV9 delivery that minimizes off-target effects and holds great promise for future clinical translation of AAV9-based gene therapies for traumatic SCI patients. The AAV9-Syn-EGFP and AAV9-Syn-KCC2 viruses used in this study have been previously validated at the protein level in earlier work, including Chen et al., where increased KCC2 expression was demonstrated using immunohistochemistry21. Our study builds on this foundation by applying the same vector in a clinically relevant cervical SCI model and by assessing the effects of acute and subacute delivery timing.
Previous characterizations of KCC2 expression in clinically relevant traumatic cervical SCI models in our lab demonstrate prolonged KCC2 downregulation in both the thoracic and cervical injured spinal cord74. Furthermore, previous research demonstrates that while daily KCC2 agonist administration can improve functional recovery over a long period of time, the cessation of agonists results in the loss of neurobehavioral improvements21. Hence, there is a need for continued agonist administration, which favors gene therapy over pharmacological candidates to continuously increase KCC2 expression in the injured spinal cord.
Despite their potential, current pharmacological strategies for KCC2 upregulation face significant limitations. Direct KCC2 agonists are not clinically approved and have an increased risk of toxicity. CLP290 is a potent KCC2 agonist, which can improve functional recovery in the thoracic SDH murine model. However, CLP290, or its related drugs, are known to have off-target effects that can complicate its clinical translation75. Two recent studies have aimed to discover KCC2 gene expression‑enhancing compounds by performing a wide drug screening investigation. Both studies have discovered that therapeutics targeting GSK3β have the ability to potently increase KCC2 expression. Several of these therapeutics are FDA-approved for cancer patients, such as kenpaullone76,77. However, because GSK3β is ubiquitously present in all cell types, these agents can exhibit several off-target effects78.
Similar to KCC2, other members of the SLC12 family of cation-chloride cotransporters play a critical role in regulating the intracellular chloride levels necessary for defining the inhibitory effects of the neurotransmitters GABA and glycine. This includes NKCC1, which has gained significant interest in recent years due to the availability of clinically approved NKCC1 modulators, such as various loop diuretics. Overall, the balance between NKCC1 and KCC2 activity is crucial for maintaining the appropriate chloride gradients in neurons79. In a recent study, the intrathecal administration of a clinically approved NKCC1 inhibitor, butanamide, showed improved functional recovery in mice with thoracic SCI55. Interestingly, butanamide also prevents prolonged excitatory neuronal swelling and subsequent neuronal death after SCI, in addition to restoring stepping ability in SCI mice55. These findings highlight the therapeutic potential of targeting NKCC1 for neuromodulation and functional repair, and suggest that such an approach could offer promising therapeutic avenues for cervical SCI as well79.
Lastly, KCC2 gene therapy is a strong candidate for combinatorial treatment strategies, as it can enhance the effectiveness of other therapeutic strategies. For instance, rehabilitative training can improve neurological readouts in both SCI patients80,81,82,83 and SCI animal models84,85,86,87,88,89,90. However, improved recovery following rehabilitation remains highly contingent on injury severity, injury location, and the rehabilitation training protocol. Furthermore, the underlying mechanism behind rehabilitation-induced neuroplastic changes is yet to be fully deciphered. KCC2 gene therapy is an excellent approach to augment the reliability and effectiveness of rehabilitation following traumatic SCI. Similarly, transplantation of stem cells shows exciting promise to regenerate lost neural tissue91. However, translation of stem cell therapy from the bench to the clinic has been hindered in part due to poor neural integration of the transplanted stem cells. Restored balanced E/I transmission through KCC2 gene therapy is an interesting approach to enhance the integration of stem cells into functional circuits92.
Methods
Animal purchase and housing
All animal experiments were performed on inbred female Wistar rats weighing between 230 and 280 g and aged between 12 and 13 weeks (obtained from Charles River Laboratories, Wilmington, MA, http://www.criver.com). The sample size was based on previous publications37,71,93,94 and power calculations to achieve an 80% likelihood (Type 2 error rate of 20%) of detecting an effect size at a Type 1 error rate of 5%. Injured rats underwent a clip-compression injury (1-min, 23.6 g) after laminectomy at the cervical region (C6/7), as previously described95. Sham rats followed the same laminectomy procedure without undergoing a clip-compression injury. Rats were housed individually in a hygienic environment at 23 ± 3 °C and 40–60% relative humidity. They were exposed to a 12 h light/dark cycle with unrestricted access to food and water. All animal experiments received ethical approval and were conducted in compliance with the University Health Network (UHN) and the Canadian Council on Animal Care guidelines. For all surgical operations, 5% inhalant isoflurane in O2 carrying gas was used to anesthetize the rats, and 2% isoflurane was used to maintain anesthesia throughout the surgeries. Post-operation, rats were subcutaneously administered with 0.05 mg/kg of buprenorphine BID for three days and received 5 mL of subcutaneous 0.9% saline for 1 week. All rats were placed in a warm room post-operation in separate individual cages.
AAV9 injection
AAV9 capsids were obtained from the University of Pennsylvania Gene Therapy Program and Boston Children’s Hospital Viral Core, which were modified to express KCC2 under the human synapsin promoter 1. All AAV9 intrathecal injections were performed using an automated Hamilton Syringe with a bevelled 32G needle at a 45° angle to minimize CSF leakage. Following injection, the dura was immediately covered with SURGIFOAM™ Absorbable Gelatin.
For acute injections, the AAV9 solutions were microinjected during the initial operation at 15 min following C6/7 injury. For subacute injections, the EGFP and KCC2-expressing AAV9 solutions were microinjected at 1 week following the injury operation. For the subacute injection, anesthesia was induced with 5% isoflurane in 100% O2 and then maintained via a nose cone (2% isoflurane, 100% O2) throughout the surgery. All operations were performed in a sterile environment with a stereotaxic instrument. Following the operation, the rats were subcutaneously administered 0.05 mg/kg of buprenorphine BID for three days.
Immunohistochemistry
Wistar rats were transcardially perfused with phosphate-buffered saline (PBS) followed by 4% paraformaldehyde (PFA) in PBS. The spinal cords were then dissected out (0.5 cm rostral and 0.5 cm caudal from the lesion epicenter), post-fixed, and cryoprotected in 30% sucrose/PBS for 48 h. The sampled spinal cords were then randomly divided for either longitudinal or axial 30-μm-thick slicing using a Cryostat and stored in a −80° freezer. A block solution (5% normal serum, 1% bovine serum albumin, 0.3% Triton X-100 in PBS) was applied for 1 h at room temperature (RT) to prepare the sectioned spinal cords for immunohistochemical staining. Subsequently, primary antibody incubation was performed overnight at 4 °C, followed by a triple 1× PBS wash. Secondary antibody incubation was accompanied by 4′,6-diamidino-2-phenylindole (DAPI, 1:200, Sigma) application for 90 min at RT. For the longitudinal sections, the sectioned cords were stained for 5HT, B3 tubulin, and NeuN. For the axial sections, the sectioned cords were stained for NeuN, VGAT, GAD67, VGlut2, IBA1, and GFAP. All primary and secondary antibody concentrations are listed in Supplementary Table 1. All images were acquired using a 20× objective lens with a Nikon Eclipse Ti C2 + inverted confocal microscope with the NIS Element imaging software version 4.20. The acquired images were analyzed in Fiji.
RNA and protein extraction
Wistar rats were sacrificed for molecular analysis using intracardial perfusion (infused with 250 ml of phosphate buffer solution). For molecular analysis, the injury epicenter spanning 5 mm in length was extracted and snap-frozen in liquid nitrogen. RNA and protein were extracted using mirVanaTM PARISTM Kit and stored at −80 °C. The total protein concentration was measured using Micro BCA™ Protein Assay Kit, and the total RNA concentration and purity were measured using DeNovix DS-11FX+ Spectrophotometer/Flourometer nanodrop.
RT-qPCR gene expression analysis
A Bioline SensiFASTTM cDNA Synthesis Kit (Cat#: BIO-65053, Toronto, Canada, www.uoftmedstore.com) reverse transcribed the extracted RNA into cDNA at 1 ng µL−1 concentration. The TaqMan primers for the selected genes were mixed with Bioline SensiFAST™ Probe Hi-ROX (Cat#: BIO-82020, Toronto, Canada, www.uoftmedstore.com). All primers were purchased from Applied Biosystems (Foster City, CA, USA, www.thermofisher.com). PPIA was used as an endogenous housekeeping gene control. Each sample was examined using 3 technical replicates and followed by 40 cycles. Subsequent analysis was performed with 2−ΔΔCT (relative quantification) recordings using Applied Biosystems SDS RQ Manager (version 2.1).
Multiplex Luminex assay
Following total protein quantification using a Micro BCA™ Protein Assay Kit, 200 µg of the isolated protein was diluted in 60 μL of PBS. The samples were sent to Eve Technologies (Calgary, Canada, www.evetechnologies.com) for Rat Cytokine Array/Chemokine Array 27 Plex (RD27)TM analysis, which consists of eotaxin, EGF, fractalkine, IFN-γ, IL-1α, IL-1β, IL-2, IL-4, IL-5, IL-6, IL-10, IL-12(p70), IL-13, IL-17A, IL-18, IP-10, GRO/KC, TNF-α, G-CSF, GM-CSF, MCP-1, Leptin, LIX, MIP-1α, MIP-2, RANTES, and VEGF. The protein concentration (pg mL−1) was calculated based on a standard curve.
Neurobehavioral assessments
Three days following cervical SCI, the BBB locomotor rating scale of 21 points was used to assess each rat’s hindlimb function in an open-field environment47. Rats were placed individually and scored by two blinded and independent researchers. For inclined plane trunk stability assessment, SCI rats were placed on an inclined plane platform, both leaning on the right and left sides, and the angle was gradually increased by 5° until the rat was unable to hold its position for 3 s without sliding, and the angle was recorded for both the left and right sides. For forelimb grip strength assessment, a grip strength meter (SDI Grip Strength System, model DFM-10; San Diego Instruments, San Diego, California) was used to measure the maximum grip strength. Hind paw sensitivity was assessed by mechanical von Frey allodynia, involving Touch TestTM Sensory Kit. Ten consecutive trials with 5.18, 5.46, 5.88, and 6.10 filaments were performed on each rat, placed in individual cages, to examine paw withdrawal reflex and tactile sensitivity. The threshold to induce a response and the % positive response were recorded for each rat.
CatWalkTM XT (Noldus, Version 10.6) was used for gait and locomotion assessment at 12 weeks post-SCI. Each rat underwent 3 successful runs on the CatWalkTM apparatus, as previously described93. PCA was performed on the CatWalkTM data using the prcomp function in R. The number of principal components to retain was chosen based on the Scree plot, which plotted the variance explained by each principal component. The animals were clustered into the corresponding experimental groups using the k-means function in R and the first two principal components as the clustering variables. The results of the PCA and clustering were visualized using the fviz_pca_ind and fviz_pca_var functions from the factoextra package in R. The fviz_pca_ind function was used to create a scatterplot of the principal components, with ellipses of type “normal” to indicate the clusters. The fviz_pca_var function was used to create a plot of the loadings of the original variables on the principal components. The results of the PCA and clustering were interpreted to understand the relationships among the variables in the catwalk data and to identify patterns and structures in the data. The loadings of the variables on the principal components were used to determine which variables had the greatest influence on the construction of the principal components. The clustering results were used to distinguish the experimental groups based on their gait patterns.
Electrophysiological assessment
Electrophysiological recordings were carried out at 12 weeks post-SCI under ketamine anesthesia, with animals positioned in a stereotactic holder in a prone position. MEPs were initiated by transcranial stimulation with two needle-electrodes placed subcutaneously over the skull at the sensorimotor cortex, whereas recording electrodes were placed in the forearm extensor muscles, as previously reported96. Stimulation intensity ranged between 1 and 15 mA, with stimulation pulse duration ranging between 0.1 and 0.5 ms in duration. The average MEP following 10 pulses was recorded at 10 mA for 0.3 ms. Paired pulses were recorded with either 6 ms or 20 ms intervals. The data was acquired with the Clampex module of pClamp 8.2 software (Axon Instruments) and analyzed with the Clampfit module of the same program. Since the variance for MEP range and AUC increases as the MEP range increases, square root normalization was used to ensure homoscedasticity for statistical analysis.
Statistics and reproducibility
All data were reported and visualized as mean ± SEM. The statistical analyses were performed and illustrated on GraphPad Prism 8. Schematic illustrations were created using BioRender (BioRender.com) with permission. All measurements were examined for normality using the Shapiro–Wilk test. Homoscedasticity was checked with the Brown–Forsythe test and F-test for analysis of variance (ANOVA) and t-tests, respectively. For comparison between two independent samples, unpaired t-tests were used for parametric and homoscedastic analysis, whereas Welch’s t-tests were used for parametric and non-homoscedastic analysis. For comparing means among more than two groups, ANOVAs were used on parametric data, and the Kruskal–Wallis tests were used for non-parametric data. Additionally, two-way repeated measures ANOVAs followed by post-hoc tests were performed to compare the differences in stimulus-response electrophysiological recordings and longitudinal neurobehavioral scores between control and study groups. For two-way repeated measures ANOVAs, Mauchly’s test in IBM SPSS Statistics Version 29 was used to assess for the assumption of sphericity, and the Geisser-Greenhouse correction in GraphPad Prism 8 was used were applicable. For level-specific epicenter and thoracic RT-qPCR experimentation, mixed effect analyses with Sidak multiple comparison was used. For acute and subacute RT-qPCR comparison, two-way ANOVA with Sidak multiple comparison was used. Heatmaps and correlation matrices were created in Morpheus (Broad Institute, Cambridge, MA, USA, https://software.broadinstitute.org/morpheus), and hierarchical clustering was based on cosine similarity. A p < 0.05 was considered statistically significant.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
All source data underlying the graphs and charts presented in the main figures is uploaded in Supplementary Data 1. Furthermore, all datasets are available from the corresponding author upon request.
Code availability
The Fiji macros used for image analysis are available from the corresponding author upon request.
References
Ahuja, C. S. et al. Traumatic spinal cord injury. Nat. Rev. Dis. Prim. 3, 17018 (2017).
World Health Organization. Spinal cord injury. www.who.int/news-room/fact-sheets/detail/spinal-cord-injury (2024).
Hutson, T. H. & Di Giovanni, S. The translational landscape in spinal cord injury: focus on neuroplasticity and regeneration. Nat. Rev. Neurol. 15, 732–745 (2019).
Fawcett, J. W. et al. Guidelines for the conduct of clinical trials for spinal cord injury as developed by the ICCP panel: spontaneous recovery after spinal cord injury and statistical power needed for therapeutic clinical trials. Spinal Cord. 45, 190–205 (2007).
Fouad, K., Popovich, P. G., Kopp, M. A. & Schwab, J. M. The neuroanatomical–functional paradox in spinal cord injury. Nat. Rev. Neurol. 17, 53–62 (2021).
Ditunno, J., Little, J., Tessler, A. & Burns, A. Spinal shock revisited: a four-phase model. Spinal Cord 42, 383-95 (2004).
Stampas, A. et al. Evidence of treating spasticity before it develops: a systematic review of spasticity outcomes in acute spinal cord injury interventional trials. Ther. Adv. Neurol. Disord. 15, 17562864211070657 (2022).
Singh, A., Tetreault, L., Kalsi-Ryan, S., Nouri, A. & Michael, F. Global prevalence and incidence of traumatic spinal cord injury. CLEP https://doi.org/10.2147/CLEP.S68889 (2014).
Gonzalez-Rothi, E. J. et al. Spinal interneurons and forelimb plasticity after incomplete cervical spinal cord injury in adult rats. J. Neurotrauma 32, 893–907 (2015).
Calancie, B. et al. Evidence that alterations in presynaptic inhibition contribute to segmental hypo- and hyperexcitability after spinal cord injury in man. Electroencephalogr. Clin. Neurophysiol. Evoked Potentials Sect. 89, 177–186 (1993).
O’Shea, T. M., Burda, J. E. & Sofroniew, M. V. Cell biology of spinal cord injury and repair. J. Clin. Investig. 127, 3259–3270 (2017).
Jutzeler, C. R. et al. Sensorimotor plasticity after spinal cord injury: a longitudinal and translational study. Ann. Clin. Transl. Neurol. 6, 68–82 (2019).
Aisen, M. L., Brown, W. & Rubin, M. Electrophysiologic changes in lumbar spinal cord after cervical cord injury. Neurology 42, 623–623 (1992).
Edgerton, V. R. et al. Training locomotor networks. Brain Res. Rev. 57, 241–254 (2008).
Rossignol, S. & Frigon, A. Recovery of locomotion after spinal cord injury: some facts and mechanisms. Annu. Rev. Neurosci. 34, 413–440 (2011).
Chamma, I., Chevy, Q., Poncer, J. C. & Lévi, S. Role of the neuronal K-Cl co-transporter KCC2 in inhibitory and excitatory neurotransmission. Front. Cell. Neurosci. 6, 1-15 (2012).
Boulenguez, P. et al. Down-regulation of the potassium-chloride cotransporter KCC2 contributes to spasticity after spinal cord injury. Nat. Med. 16, 302–307 (2010).
Zavvarian, M.-M., Hong, J. & Fehlings, M. G. The functional role of spinal interneurons following traumatic spinal cord injury. Front. Cell. Neurosci. 14, 127 (2020).
Courtine, G. et al. Recovery of supraspinal control of stepping via indirect propriospinal relay connections after spinal cord injury. Nat. Med. 14, 69–74 (2008).
Brand et al. Restoring voluntary control of locomotion after paralyzing spinal cord injury. Science 336, 1182–1185 (2012).
Chen, B. et al. Reactivation of dormant relay pathways in injured spinal cord by KCC2 manipulations. Cell 174, 521–535.e13 (2018).
Gagnon, M. et al. Chloride extrusion enhancers as novel therapeutics for neurological diseases. Nat. Med. 19, 1524–1528 (2013).
High, K. A. & Roncarolo, M. G. Gene therapy. N. Engl. J. Med. 381, 455–464 (2019).
Dunbar, C. E. et al. Gene therapy comes of age. Science 359, eaan4672 (2018).
Hordeaux, J. et al. The neurotropic properties of AAV-PHP.B are limited to C57BL/6J mice. Mol. Ther. 26, 664–668 (2018).
Lykken, E. A., Shyng, C., Edwards, R. J., Rozenberg, A. & Gray, S. J. Recent progress and considerations for AAV gene therapies targeting the central nervous system. J. Neurodev. Disord. 10, 16 (2018).
Collins, L. T., Ponnazhagan, S. & Curiel, D. T. Synthetic biology design as a paradigm shift toward manufacturing affordable adeno-associated virus gene therapies. ACS Synth. Biol. 12, 17–26 (2023).
Kügler, S., Kilic, E. & Bähr, M. Human synapsin 1 gene promoter confers highly neuron-specific long-term transgene expression from an adenoviral vector in the adult rat brain depending on the transduced area. Gene Ther. 10, 337–347 (2003).
Lorenzo, L.-E. et al. Enhancing neuronal chloride extrusion rescues α2/α3 GABAA-mediated analgesia in neuropathic pain. Nat. Commun. 11, 869 (2020).
Shi, M. et al. EA participates in pain transition through regulating KCC2 expression by BDNF-TrkB in the spinal cord dorsal horn of male rats. Neurobiol. Pain. 13, 100115 (2023).
Mapplebeck, J. C. S. et al. Chloride dysregulation through downregulation of KCC2 mediates neuropathic pain in both sexes. Cell Rep. 28, 590–596.e4 (2019).
Tavazzani, E. et al. Glutamic acid decarboxylase 67 expression by a distinct population of mouse vestibular supporting cells. Front. Cell. Neurosci. 8, 1-9 (2014).
Chaudhry, F. A. et al. The vesicular GABA transporter, VGAT, localizes to synaptic vesicles in sets of glycinergic as well as GABAergic neurons. J. Neurosci. 18, 9733–9750 (1998).
Juge, N., Omote, H. & Moriyama, Y. Vesicular GABA transporter (VGAT) transports β-alanine. J. Neurochem. 127, 482–486 (2013).
Bilchak, J. N., Yeakle, K., Caron, G., Malloy, D. & Côté, M.-P. Enhancing KCC2 activity decreases hyperreflexia and spasticity after chronic spinal cord injury. Exp. Neurol. 338, 113605 (2021).
National Spinal Cord Injury Statistical Center. Traumatic Spinal Cord Injury Facts and Figures at a Glance (University of Alabama at Birmingham, 2023).
Hong, J. et al. Level-specific differences in systemic expression of pro- and anti-inflammatory cytokines and chemokines after spinal cord injury. Int. J. Mol. Sci. 19, 2167 (2018).
Adams, M. & Cavanagh, J. F. R. International Campaign for Cures of Spinal Cord Injury Paralysis (ICCP): another step forward for spinal cord injury research. Spinal Cord 42, 273–280 (2004).
Tuszynski, M. H. et al. Guidelines for the conduct of clinical trials for spinal cord injury as developed by the ICCP Panel: clinical trial inclusion/exclusion criteria and ethics. Spinal Cord. 45, 222–231 (2007).
Steeves, J. D. et al. Guidelines for the conduct of clinical trials for spinal cord injury (SCI) as developed by the ICCP panel: clinical trial outcome measures. Spinal Cord. 45, 206–221 (2007).
Courtine, G. & Sofroniew, M. V. Spinal cord repair: advances in biology and technology. Nat. Med. 25, 898–908 (2019).
Fehlings, M. G., Tator, C. H., Linden, R. D. & Piper, I. R. Motor and somatosensory evoked potentials recorded from the rat. Electroencephalogr. Clin. Neurophysiol. 69, 65–78 (1988).
Fehlings, M. G., Tator, C. H. & Linden, R. D. The relationships among the severity of spinal cord injury, motor and somatosensory evoked potentials and spinal cord blood flow. Electroencephalogr. Clin. Neurophysiol. 74, 241–259 (1989).
Anderson, K. D. et al. Forelimb locomotor assessment scale (FLAS): novel assessment of forelimb dysfunction after cervical spinal cord injury. Exp. Neurol. 220, 23–33 (2009).
Anderson, K. D., Gunawan, A. & Steward, O. Spinal pathways involved in the control of forelimb motor function in rats. Exp. Neurol. 206, 318–331 (2007).
Hamers, F. P. T., Koopmans, G. C. & Joosten, E. A. J. CatWalk-assisted gait analysis in the assessment of spinal cord injury. J. Neurotrauma 23, 537–548 (2006).
Basso, D. M., Beattie, M. S. & Bresnahan, J. C. A sensitive and reliable locomotor rating scale for open field testing in rats. J. Neurotrauma 12, 1–21 (1995).
Rivlin, A. S. & Tator, C. H. Objective clinical assessment of motor function after experimental spinal cord injury in the rat. J. Neurosurg. 47, 577–581 (1977).
Ghosh, A. et al. Rewiring of hindlimb corticospinal neurons after spinal cord injury. Nat. Neurosci. 13, 97–104 (2010).
Zaaimi, B., Edgley, S. A., Soteropoulos, D. S. & Baker, S. N. Changes in descending motor pathway connectivity after corticospinal tract lesion in macaque monkey. Brain 135, 2277–2289 (2012).
Weishaupt, N., Hurd, C., Wei, D. Z. & Fouad, K. Reticulospinal plasticity after cervical spinal cord injury in the rat involves withdrawal of projections below the injury. Exp. Neurol. 247, 241–249 (2013).
Fenrich, K. K. et al. Self-directed rehabilitation training intensity thresholds for efficient recovery of skilled forelimb function in rats with cervical spinal cord injury. Exp. Neurol. 339, 113543 (2021).
Priya, R. et al. Activity regulates cell death within cortical interneurons through a calcineurin-dependent mechanism. Cell Rep. 22, 1695–1709 (2018).
Wong, F. K. et al. Pyramidal cell regulation of interneuron survival sculpts cortical networks. Nature 557, 668–673 (2018).
Li, Q. et al. Reduction of prolonged excitatory neuron swelling after spinal cord injury improves locomotor recovery in mice. Sci. Transl. Med. 16, eadn7095 (2024).
Hebert, S. C., Mount, D. B. & Gamba, G. Molecular physiology of cation-coupled Cl? cotransport: the SLC12 family. Pflug. Arch. Eur. J. Physiol. 447, 580–593 (2004).
Vlkolinský, R., Siggins, G. R., Campbell, I. L. & Krucker, T. Acute exposure to CXC chemokine ligand 10, but not its chronic astroglial production, alters synaptic plasticity in mouse hippocampal slices. J. Neuroimmunol. 150, 37–47 (2004).
Kodangattil, J. N., Möddel, G., Müller, M., Weber, W. & Gorji, A. The inflammatory chemokine CXCL10 modulates synaptic plasticity and neuronal activity in the hippocampus. Eur. J. Inflamm. 10, 311–328 (2012).
Sasaki, Y., Ohsawa, K., Kanazawa, H., Kohsaka, S. & Imai, Y. Iba1 is an actin-cross-linking protein in macrophages/microglia. Biochem. Biophys. Res. Commun. 286, 292–297 (2001).
Bilchak, J. N., Caron, G., Danner, S. M. & Côté, M.-P. KCC2 enhancers normalize reflex responses and improve locomotor function after chronic spinal cord injury. Preprint at bioRxiv https://doi.org/10.1101/2023.10.21.563363 (2023).
Beverungen, H., Klaszky, S. C., Klaszky, M. & Côté, M.-P. Rehabilitation decreases spasticity by restoring chloride homeostasis through the brain-derived neurotrophic factor–KCC2 pathway after spinal cord injury. J. Neurotrauma 37, 846–859 (2020).
Detloff, M. R., Fisher, L. C., Deibert, R. J. & Basso, D. M. Acute and chronic tactile sensory testing after spinal cord injury in rats. J. Vis. Exp. https://doi.org/10.3791/3247 (2012).
Kang, J. H. & Im, S. Functional anatomy of the spinal tracts based on evolutionary perspectives. Korean J. Neurotrauma 19, 275 (2023).
Mingozzi, F. & High, K. A. Immune responses to AAV vectors: Overcoming barriers to successful gene therapy. Blood 122, 23–36 (2013).
Nectow, A. R. & Nestler, E. J. Viral tools for neuroscience. Nat. Rev. Neurosci. 21, 669–681 (2020).
Wang, D., Tai, P. W. L. & Gao, G. Adeno-associated virus vector as a platform for gene therapy delivery. Nat. Rev. Drug Discov. 18, 358–378 (2019).
Chan, K. Y. et al. Engineered AAVs for efficient noninvasive gene delivery to the central and peripheral nervous systems. Nat. Neurosci. 20, 1172–1179 (2017).
Hardcastle, N., Boulis, N. M. & Federici, T. AAV gene delivery to the spinal cord: serotypes, methods, candidate diseases, and clinical trials. Expert Opin. Biol. Ther. 18, 293–307 (2018).
Chen, X. et al. Engineered AAVs for non-invasive gene delivery to rodent and non-human primate nervous systems. Neuron 110, 2242–2257.e6 (2022).
Goertsen, D. et al. AAV capsid variants with brain-wide transgene expression and decreased liver targeting after intravenous delivery in mouse and marmoset. Nat. Neurosci. 25, 106–115 (2022).
Brommer, B. et al. Improving hindlimb locomotor function by non-invasive AAV-mediated manipulations of propriospinal neurons in mice with complete spinal cord injury. Nat. Commun. 12, 781 (2021).
Hordeaux, J. et al. Adeno-associated virus-induced dorsal root ganglion pathology. Hum. Gene Ther. 31, 808–818 (2020).
Bravo-Hernandez, M. et al. Spinal subpial delivery of AAV9 enables widespread gene silencing and blocks motoneuron degeneration in ALS. Nat. Med 26, 118–130 (2020).
Hong, J. Y.-L. A Comparison between Cervical and Thoracic Spinal Cord Injury: Critical Level-Dependent Differences in Pathobiology (University of Toronto, 2020).
Duy, P. Q., He, M., He, Z. & Kahle, K. T. Preclinical insights into therapeutic targeting of KCC2 for disorders of neuronal hyperexcitability. Expert Opin. Ther. Targets 24, 629–637 (2020).
Tang, X. et al. Pharmacological enhancement of KCC2 gene expression exerts therapeutic effects on human Rett syndrome neurons and Mecp2 mutant mice. Sci. Transl. Med. 11, eaau0164 (2019).
Yeo, M. et al. Repurposing cancer drugs identifies kenpaullone which ameliorates pathologic pain in preclinical models via normalization of inhibitory neurotransmission. Nat. Commun. 12, 6208 (2021).
Phukan, S., Babu, V., Kannoji, A., Hariharan, R. & Balaji, V. GSK3b: role in therapeutic landscape and development of modulators. Br. J. Pharmacol. 160, 1–9 (2010).
Talifu, Z. et al. The role of KCC2 and NKCC1 in spinal cord injury: From physiology to pathology. Front. Physiol. 13, 1045520 (2022).
Beekhuizen, K. S. & Field-Fote, E. C. Massed practice versus massed practice with stimulation: effects on upper extremity function and cortical plasticity in individuals with incomplete cervical spinal cord injury. Neurorehabil. Neural Repair 19, 33–45 (2005).
Harkema, S. J. Neural plasticity after human spinal cord injury: application of locomotor training to the rehabilitation of walking. Neuroscientist 7, 455–468 (2001).
Hicks, A. et al. Long-term body-weight-supported treadmill training and subsequent follow-up in persons with chronic SCI: effects on functional walking ability and measures of subjective well-being. Spinal Cord 43, 291-298 (2005).
Kowalczewski, J., Chong, S. L., Galea, M. & Prochazka, A. In-home tele-rehabilitation improves tetraplegic hand function. Neurorehabil. Neural Repair 25, 412–422 (2011).
Tashiro, S. et al. BDNF induced by treadmill training contributes to the suppression of spasticity and allodynia after spinal cord injury via upregulation of KCC2. Neurorehabil. Neural Repair 29, 677–689 (2015).
Barbeau, H. & Rossignol, S. Recovery of locomotion after chronic spinalization in the adult cat. Brain Res. 412, 84–95 (1987).
Battistuzzo, C. R., Callister, R. J., Callister, R. & Galea, M. P. A systematic review of exercise training to promote locomotor recovery in animal models of spinal cord injury. J. Neurotrauma 29, 1600–1613 (2012).
García-Alías, G., Barkhuysen, S., Buckle, M. & Fawcett, J. W. Chondroitinase ABC treatment opens a window of opportunity for task-specific rehabilitation. Nat. Neurosci. 12, 1145–1151 (2009).
Starkey, M. L. et al. High-impact, self-motivated training within an enriched environment with single animal tracking dose-dependently promotes motor skill acquisition and functional recovery. Neurorehabil. Neural Repair 28, 594–605 (2014).
Torres-Espín, A., Beaudry, E., Fenrich, K. & Fouad, K. Rehabilitative training in animal models of spinal cord injury. J. Neurotrauma 35, 1970–1985 (2018).
Torres-Espín, A. et al. Eliciting inflammation enables successful rehabilitative training in chronic spinal cord injury. Brain 141, 1946–1962 (2018).
Khazaei, M., Siddiqui, A. & Fehlings, M. The potential for iPS-derived stem cells as a therapeutic strategy for spinal cord injury: opportunities and challenges. J. Clin. Med. 4, 37–65 (2014).
Fischer, I., Dulin, J. N. & Lane, M. A. Transplanting neural progenitor cells to restore connectivity after spinal cord injury. Nat. Rev. Neurosci. 21, 366–383 (2020).
Wilcox, J. T. et al. Generating level-dependent models of cervical and thoracic spinal cord injury: exploring the interplay of neuroanatomy, physiology, and function. Neurobiol. Dis. 105, 194–212 (2017).
Hordeaux, J. et al. Toxicology study of intra-cisterna magna adeno-associated virus 9 expressing human alpha-L-iduronidase in rhesus macaques. Mol. Ther. Methods Clin. Dev. 10, 79–88 (2018).
Zavvarian, M.-M. et al. The protein kinase inhibitor midostaurin improves functional neurological recovery and attenuates inflammatory changes following traumatic cervical spinal cord injury. Biomolecules 11, 972 (2021).
Krishnan, V. S. et al. Multimodal evaluation of TMS - induced somatosensory plasticity and behavioral recovery in rats with contusion spinal cord injury. Front. Neurosci. 13, 387 (2019).
Acknowledgements
M-M.Z. would like to thank the contributions of Dr. Phillipe Monnier and Dr. Isabelle Aubert as advisory committee members. M-M.Z. was awarded the Crother’s Family Fellowship, Ontario Graduate Scholarship, and Margaret and Howard Gamble Fellowship. M.G.F. wishes to acknowledge support from the Robert Campeau Family Foundation/Dr. C.H. Tator Chair in Brain and Spinal Cord Research at UHN. The authors would like to thank Dr. Tim Worden for copyediting this article.
Author information
Authors and Affiliations
Contributions
M-M.Z.: Conception and design, collection and assembly of data, data analysis, data interpretation, manuscript writing, final approval of manuscript. A.M.; M.K.; Z.L.; A.V.; O.H.; Z.P.: Collection and assembly of data, final approval of manuscript. J.H.; C.S.A; M.H.; Z.H.: Data interpretation, manuscript editing, and final approval of manuscript. M.G.F.: Conception and design, data analysis and interpretation, manuscript writing and editing, final approval of manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Communications Biology thanks Atiyeh Mohammadshirazi and the other anonymous reviewer(s) for their contribution to the peer review of this work. Primary Handling Editors: Claudia Kathe and Benjamin Bessieres.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Zavvarian, MM., Modi, A.D., Khazaei, M. et al. AAV9-mediated KCC2 upregulation enhances functional recovery following cervical spinal cord injury. Commun Biol 8, 1489 (2025). https://doi.org/10.1038/s42003-025-08734-0
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s42003-025-08734-0