Abstract
Background
Speculative claims about COVID-19 vaccines affecting fertility and childbirth have circulated widely. We aimed to examine whether COVID-19 vaccination is causally associated with childbirth in Swedish women.
Methods
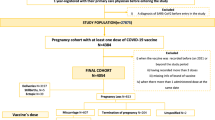
We conducted a cohort study using a representative population of 369,000 to emulate a randomized experiment, comparing childbirth rates between vaccinated and unvaccinated women. Cox proportional hazards models were applied, treating vaccination as a time-varying covariate. Causal modeling was used to adjust for potential bias. To capture vaccine effects on both conception and established pregnancies, the index event was set at an estimated conception date, 280 days prior to childbirth.
Results
We show that with an assumed average pregnancy length of 280 days, there are no statistically significant associations between COVID-19 vaccination and childbirth (unadjusted HR = 0.94 (95% CI 0.89-1.00); adjusted HR = 1.03 (95% CI 0.97-1.09). Assuming a shorter pregnancy length (266 days), the associations between vaccination and childbirth remain insignificant (unadjusted HR = 0.96 (95% CI 0.90-1.02); adjusted HR = 1.04 (95% CI 0.98-1.11)). Neither are there statistically significant associations between COVID-19 vaccination and recorded miscarriages (unadjusted HR = 0.84 (95% CI 0.69-1.03); adjusted HR = 0.86 (95% CI 0.70-1.05).
Conclusions
COVID-19 vaccination is not associated with a decrease in childbirth after adjusting for common confounding factors. These findings provide evidence to support vaccination policies for women of childbearing age.
Plain Language Summary
Early, unfounded rumors spread during the COVID-19 pandemic claimed that mRNA vaccination could cause infertility. Later, suspicions were raised regarding whether reductions in childbirth observed during the pandemic were associated with the novel COVID-19 vaccines. We therefore study effects of COVID-19 vaccination in a representative population of Swedish women, and adjust for any confounding effects. No association is observed between COVID-19 vaccination and childbirth, or between vaccination and recorded miscarriages. We thus find no evidence for any connections between COVID-19 vaccination and the observed decrease in childbirth. Our results are relevant for consideration when vaccination policies involving women of childbearing age are determined.
Similar content being viewed by others
Data availability
The data that support the findings of this study are available on reasonable request five years after article publication from the corresponding author [toomas.timpka@liu.se]. The data are not publicly available due to Swedish legislation. Source Data for Fig. 2 is provided as Supplementary Data.
Code availability
The R code required to replicate our results is available from GitHub at https://doi.org/10.5281/zenodo.18138478.
References
Malik, M., Bauer-Maison, N., Guarna, G. & D’Souza, R. D. Social Media Misinformation about Pregnancy and COVID-19 Vaccines: A Systematic Review. Med Princ. Pr. 33, 232–241 (2024).
Abbasi, J. Widespread misinformation about infertility continues to create COVID-19 vaccine hesitancy. JAMA 327, 1013–1015 (2022).
Berkowitz, H. E. & Vann, J. C. J. Strategies to address COVID-19 vaccine and pregnancy myths. MCN Am. J. Matern Child Nurs. 48, 215–223 (2023).
Vesco, K. K. et al. Obstetric Complications and Birth Outcomes After Antenatal Coronavirus Disease 2019 (COVID-19) Vaccination. Obstet. Gynecol. 143, 794–802 (2024).
Norman, M. et al. Neonatal outcomes after COVID-19 vaccination in pregnancy. JAMA 331, 396–407 (2024).
Fernández-García, S. et al. PregCOV-19 Living Systematic Review Consortium. Effectiveness and safety of COVID-19 vaccines on maternal and perinatal outcomes: a systematic review and meta-analysis. BMJ Glob. Health 9, e014247 (2024).
Manniche, V., Fürst, T., Schmeling, M., Gilthorpe, J. D. & Hansen, P. R. Rates of successful conceptions according to COVID-19 vaccination status: Data from the Czech Republic. Int J. Risk Saf. Med 36, 302–306 (2025).
Winkler-Dworak, M., Zeman, K. & Sobotka, T. Birth rate decline in the later phase of the COVID-19 pandemic: the role of policy interventions, vaccination programmes, and economic uncertainty. Hum. Reprod. Open 2024, hoae052 (2024).
Jasilioniene, A., Jasilionis, D., Jdanov, D. & Myrskylä, M. Association between the COVID-19 vaccination campaign and fertility trends: a population-level time series analysis for 22 countries. BMJ Public Health 3, e001410 (2025).
Winters, M. et al. Debunking COVID-19 vaccine misinformation with an audio drama in Ghana, a randomized control trial. Sci. Rep. 15, 8955 (2025).
Soucheray, S. RFK Jr says no COVID vaccines for healthy children, pregnant women. CIDRAP News. May 27, 2025. [2026-01-20] https://www.cidrap.umn.edu/covid-19/rfk-jr-says-no-covid-vaccines-healthy-children-pregnant-women#:~:text=News-,RFK%20Jr%20says%20no%20COVID%20vaccines%20for%20healthy%20children%2C%20pregnant,Steven%20J.
Magnus, M. C., Wilcox, A. J., Morken, N. H., Weinberg, C. R. & Håberg, S. E. Role of maternal age and pregnancy history in risk of miscarriage: prospective register based study. BMJ 364, l869 (2019).
Firouzbakht, M., Sharif Nia, H., Kazeminavaei, F. & Rashidian, P. Hesitancy about COVID-19 vaccination among pregnant women: a cross-sectional study based on the health belief model. BMC Pregnancy Childbirth 22, 611 (2022).
Greenland, S. Basic methods for sensitivity analysis of biases. Int J. Epidemiol. 25, 1107–1116 (1996).
Hernán, M. A., Hernández-Díaz, S. & Robins, J. M. A structural approach to selection bias. Epidemiology 15, 615–625 (2004).
Hui, L. et al. Suboptimal care factors and stillbirths during the COVID-19 pandemic in Victoria: A state-wide linkage study of stillbirths and Consultative Council on Obstetric and Paediatric Mortality and Morbidity case reviews. Women Birth 38, 101855 (2025).
Sandoval, M. N. et al. COVID-19 infection history as a risk factor for early pregnancy loss: results from the electronic health record-based Southeast Texas COVID and Pregnancy Cohort Study. BMC Med 23, 274 (2025).
Franklin, JB. et al.; JAMA Summit on Clinical Trials Participants. Modernizing the Data Infrastructure for Clinical Research to Meet Evolving Demands for Evidence. JAMA. 5, https://doi.org/10.1001/jama.2024.0268 (2024).
Socialstyrelsen. Statistics on pregnancies, births and newborns (in Swedish). [2025-06-03] https://www.socialstyrelsen.se/statistik-och-data/statistik/alla-statistikamnen/graviditeter-forlossningar-och-nyfodda/.
Hoem, B. & Hoem, J. M. Sweden’s family policies and roller-coaster fertility. Jinko Mondai Kenkyu 52, 1–22 (1996).
Acknowledgements
This study was supported by grants from the Swedish Research Council (VR 2021-05608, VR 2022-05608, VR 2025-06721), Region Östergötland (ALF-936190), and the Research Council of Southeast Sweden (FORSS-940915).
Funding
Open access funding provided by Linköping University.
Author information
Authors and Affiliations
Contributions
D.N., T.S., and T.T. conceived and designed this study; D.N. analyzed the data; A.S., O.E., J.L., Ö.D., and T.T. verified the results; D.N. and T.T. wrote this paper; T.S., O.E., J.L., A.S., J.H., M.B., D.A., E.G., and Ö.D. revised the manuscript and provided intellectual content. T.T. is the guarantor of the content.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Communications Medicine thanks Victoria Male and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Nordvall, D., Schön, T., Hinkula, J. et al. COVID-19 vaccination carries no association with childbirth rates in Sweden. Commun Med (2026). https://doi.org/10.1038/s43856-026-01396-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s43856-026-01396-x