Abstract
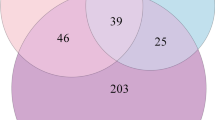
The refugee experience is a known risk factor for psychological stress, cardiovascular disease (CVD) and somatic pain. However, the prevalence and comorbidity of these health outcomes in asylum seekers is not elucidated. Here we performed a retrospective, cross-sectional study in which the forensic medical evaluations of 453 globally representative US asylum seekers were analyzed. Outcomes included the prevalence of symptoms of psychological stress, CVD, somatic pain and their comorbidity. Symptoms of psychological stress, CVD and somatic pain were documented in 94%, 47% and 50% of participants, respectively; 46% reported both CVD and stress symptoms, and 31% reported all three. Palpitations, presyncope/syncope, stroke symptoms and chest pain were reported in 33%, 25%, 20% and 16% of individuals with CVD symptoms, respectively. Furthermore, both stress symptoms and pain symptoms were each strongly predictive of comorbid CVD symptoms. These findings indicate that asylum seekers experience a high burden of comorbid and interrelated psychological stress, CVD and somatic pain.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$79.00 per year
only $6.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
Given the vulnerability of the study population, all of the individual participant data collected during this study, which form the minimum dataset necessary to interpret, verify and extend the research, after deidentification, will be made available by contacting the corresponding author. Statistical analysis plan and analytic code will be made available immediately following publication with no end date for anyone who wishes to access the data for any purposes.
Code availability
GraphPad PRISM 10.2.3 can be downloaded from https://www.graphpad.com/updates. ChartExpo 1.0.0.7 can be downloaded from https://chartexpo.com/. R 4.2.1 can be downloaded from https://www.r-project.org/about.html.
References
Global Trends: Forced Displacement in 2022 (United Nations High Commissioner for Refugees, 2023); https://www.unhcr.org/global-trends-report-2022
Shrestha, N. M. et al. Impact of torture on refugees displaced within the developing world: symptomatology among Bhutanese refugees in Nepal. JAMA 280, 443–448 (1998).
Macfarlane, R. Healthcare and homelessness: remember homeless migrants, especially refused asylum seekers. BMJ 368, m115 (2020).
Darawsheh, W., Bewernitz, M., Tabbaa, S. & Justiss, M. Factors shaping occupational injustice among resettled syrian refugees in the United States. Occup. Ther. Int. 2022, 1–12 (2022).
Lebano, A. et al. Migrants’ and refugees’ health status and healthcare in Europe: a scoping literature review. BMC Public Health 20, 1039 (2020).
Convention and Protocol Relating to the Status of Refugees (United Nations High Commissioner for Refugees, 1951); https://www.unhcr.org/media/convention-and-protocol-relating-status-refugees
Silove, D., Steel, Z. & Mollica, R. Detention of asylum seekers: assault on health, human rights, and social development. Lancet 357, 1436–1437 (2001).
Moreno, A., Piwowarczyk, L. & Grodin, M. A. Human rights violations and refugee health. JAMA 285, 1215 (2001).
Porter, M. & Haslam, N. Predisplacement and postdisplacement factors associated with mental health of refugees and internally displaced persons: a meta-analysis. JAMA 294, 602–612 (2005).
Torpy, J. M., Lynm, C. & Glass, R. M. Chronic stress and the heart. JAMA 298, 1722 (2007).
Marshall, G. N. et al. Diabetes and cardiovascular disease risk in Cambodian refugees. J. Immigr. Minor. Health 18, 110–117 (2016).
Wagner, J. et al. Trauma, healthcare access, and health outcomes among Southeast Asian refugees in Connecticut. J. Immigr. Minor. Health 15, 1065–1072 (2013).
Al-Rousan, T. et al. Epidemiology of cardiovascular disease and its risk factors among refugees and asylum seekers: systematic review and meta-analysis. Int. J. Cardiol. Cardiovasc. Risk Prev. 12, 200126 (2022).
Afari, N. et al. Psychological trauma and functional somatic syndromes: a systematic review and meta-analysis. Psychosom. Med. 76, 2–11 (2013).
Reynolds, C. A. & Minic, Z. Chronic pain-associated cardiovascular disease: the role of sympathetic nerve activity. Int. J. Mol. Sci. 24, 5378 (2023).
Abdallah, C. G. & Geha, P. Chronic pain and chronic stress: two side of the same coin? Chronic Stress 1, 1–10 (2017).
Nissen, A., Hynek, K. A., Scales, D., Hilden, P. K. & Straiton, M. Chronic pain, mental health and functional impairment in adult refugees from Syria resettled in Norway: a cross-sectional study. BMC Psychiatry 22, 571 (2022).
Fleming, P. J. et al. Fear of deportation and associations with mental health among Michigan residents of Middle Eastern & North African descent. J. Immigr. Minor. Health 25, 382–388 (2023).
Gleeson, G. et al. Post-migration factors and mental health outcomes in asylum-seeking and refugee populations: a systematic review. Eur. J. Psychotraumatol. 11, 1793567 (2020).
Giacco, D. Identifying the critical time points for mental health of asylum seekers and refugees in high-income countries. Epidemiol. Psychiatr. Sci. 29, e61 (2020).
Laban, C. J., Komproe, I. H., Gernaat, H. B. P. E. & de Jong, J. T. V. M. The impact of a long asylum procedure on quality of life, disability and physical health in Iraqi asylum seekers in the Netherlands. Soc. Psychiatry Psychiatr. Epidemiol. 43, 507–515 (2008).
Steel, Z. et al. Impact of immigration detention and temporary protection on the mental health of refugees. Br. J. Psychiatry 188, 58–64 (2006).
Martinez, A. D., Ruelas, L. & Granger, D. A. Household fear of deportation in relation to chronic stressors and salivary proinflammatory cytokines in Mexican-origin families post-SB 1070. SSM Popul. Health 19, 188–200 (2018).
Li, S. S. Y., Liddell, B. J. & Nickerson, A. The relationship between post-migration stress and psychological disorders in refugees and asylum seekers. Curr. Psychiatry Rep. 18, 82 (2016).
Drozdek, B., Kamperman, A. M., Tol, W. A., Knipscheer, J. W. & Kleber, R. J. Is legal status impacting outcomes of group therapy for posttraumatic stress disorder with male asylum seekers and refugees from Iran and Afghanistan? BMC Psychiatry 13, 148 (2013).
Ryan, D. A., Benson, C. A. & Dooley, B. A. Psychological distress and the asylum process: a longitudinal study of forced migrants in Ireland. J. Nerv. Ment. Health Dis. 196, 37–45 (2008).
Laban, C. J., Gernaat, H. B. P. E., Komproe, I. H., Schreuders, B. A. & de Jong, J. T. V. M. Impact of a long asylum procedure on the prevalence of psychiatric disorders in Iraqi asylum seekers in the Netherlands. J. Nerv. Ment. Dis. 192, 843–851 (2004).
Silove, D. et al. The impact of the refugee decision on the trajectory of PTSD, anxiety, and depressive symptoms among asylum seekers: a longitudinal study. Am. J. Disaster Med. 2, 321–329 (2007).
Newham, E. A., Pearman, A., Olinga-Shannon, S. & Nickerson, A. The mental health effects of visa insecurity for refugees and people seeking asylum: a latent class analysis. Int. J. Public Health 64, 763–772 (2019).
Nickerson, A. et al. The association between visa insecurity and mental health, disability and social engagement in refugees living in Australia. Eur. J. Psychotraumatol. 10, 1688129 (2019).
Torres, J. M. et al. Worry about deportation and cardiovascular disease risk factors among adult women: the Center for the Health Assessment of Mothers and Children of Salinas study. Ann. Behav. Med. 52, 186–193 (2018).
Torres, J. M. et al. Deportation worry, cardiovascular disease risk factor trajectories, and incident hypertension: a community-based cohort study. J. Am. Heart Assoc. 8, e013086 (2019).
Ronnegard, A., Nowak, C., Ang, B. & Arnlov, J. The association between short-term, chronic localized and chronic widespread pain and risk for cardiovascular disease in the UK Biobank. Eur. J. Prev. Cardiol. 29, 1994–2002 (2022).
Higson-Smith, C. Updating the estimate of refugees resettled in the United States who have suffered torture. The Center for Victims of Torture https://www.cvt.org/sites/default/files/SurvivorNumberMetaAnalysis_Sept2015_0.pdf (2015).
Kaur, G. et al. Chronic pain diagnosis in refugee torture survivors: a prospective, blinded diagnostic accuracy study. PLoS Med. 17, e1003108 (2020).
Wudeneh, M. et al. Disease burdens and risk factors for diabetes, hypertension, and hyperlipidemia among refugees in Buffalo, New York, 2004–2014. J. Health Care Poor Underserved 30, 1119–1131 (2019).
Amris, K., Jones, L. E. & Williams, A. Pain from torture: assessment and management. Pain Rep. 4, e794 (2019).
Williams, A. & Amris, K. Treatment of persistent pain from torture: review and commentary. Med. Confl. Surviv. 33, 60–81 (2017).
Williams, A. & Baird, E. Special considerations for the treatment of pain from torture and war. Curr. Anesthesiol. Rep. 6, 319–326 (2016).
Istanbul Protocol: manual on effective investigation and documentation of torture and other cruel, inhumane or degrading treatment or punishment. Office of the United Nations High Commissioner for Human Rights https://www.ohchr.org/Documents/Publications/training8Rev1en.pdf (2004).
Grasser, L. R. et al. The fear that remains: associations between trauma, related psychopathology, and fear-potentiated startle in youth resettled as refugees. Dev. Psychobiol. 65, e22385 (2023).
Husain, F. et al. Prevalence of war-related mental health conditions and association with displacement status in postwar Jaffna District, Sri Lanka. JAMA 306, 522–531 (2011).
Bohland, H. K. et al. Depression and anxiety in female refugees from East Africa and the Middle East displaced to Germany: cross-sectional results of the female refugee study, taking sociodemographic and migration-related factors into account. Front. Psychiatry 14, 1303009 (2023).
Hinchey, L. M. et al. The predictive utility of trauma subtypes in the assessment of mental health outcomes for persons resettled as refugees. J. Immigr. Minor. Health 25, 274–281 (2023).
Pathways to Wellness: Integrating Refugee Health and Well-being. Refugee Health Screener – 15 (RHS-15) https://www.refugeehealthta.org/wp-content/uploads/2012/09/RHS15_Packet_PathwaysToWellness-1.pdf (Pathways to Wellness, 2011).
Sternberg, R. M. et al. Development of the Stress of Immigration Survey (SOIS): a field test among Mexican immigrant women. Fam. Community Health 39, 40–52 (2016).
Malm, A., Tinghog, P., Narusyte, J. & Saboonchi, F. The refugee post-migration stress scale (RPMS)—development and validation among refugees from Syria recently resettled in Sweden. Conflict Health 14, 2 (2020).
Kaur, G., Pryor, K. O., Milewski, A. R., Weinberg, R. & Hemmings, H. C. Torture mechanisms and chronic somatic pain in US refugees. Br. J. Anaesth. 131, e41–e43 (2023).
Abubakar, I. et al. The UCL–Lancet Commission on Migration and Health: the health of a world on the move. Lancet 392, 2606–2654 (2018).
Harris, P. A. et al. Research electronic data capture (REDCap)—a metadata-driven methodology and workflow process for providing translational research informatics support. J. Biomed. Inf. 42, 377–381 (2009).
Stress a major health problem in the U.S., warns APA. American Psychological Association https://www.apa.org/news/press/releases/2007/10/stress (2007).
Kent, M. et al. The ACTTION-APS-AAPM Pain Taxonomy (AAAPT) multidimensional approach to classifying acute pain conditions. Pain Med. 18, 947–958 (2017).
Fillingim, R. et al. The ACTTION-American Pain Society Pain Taxonomy (AAPT): an evidence-based and multidimensional approach to classifying chronic pain conditions. J. Pain 15, 241–249 (2014).
Ornato, J. P. & Hand, M. M. Warning signs of a heart attack. Circulation 129, e393–e395 (2014).
Jurgens, C. Y. et al. State of the science: the relevance of symptoms in cardiovascular disease and research: a scientific statement from the American Heart Association. Circulation 146, e173–e184 (2022).
Sustainable Development Goals Indicators: regional groupings used in Report and Statistical Annex. United Nations Statistical Division https://unstats.un.org/sdgs/indicators/regional-groups/ (2024).
Acknowledgements
Research reported in this publication was supported by the National Institute Of Neurological Disorders And Stroke of the National Institutes of Health (award number K23NS116114; G.K.). This study was also supported by grants from the National Institute of General Medical Sciences (T32GM007739 to the Weill Cornell/Rockefeller/Sloan Kettering Tri-Institutional MD-PhD program; H.L.P.) and a Predoctoral Fellowship from the National Cancer Institute (F30CA257282; H.L.P.). The content of this study is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. The study sponsors had no role in the study design; in the collection, analysis and interpretation of data; in the writing of the report; or in the decision to submit the paper for publication.
Author information
Authors and Affiliations
Contributions
J.M.L.: data curation, methodology, writing—original draft, and writing—review and editing; H.L.P.: data curation, methodology, visualization, writing—original draft, and writing—review and editing; C.H.: conceptualization, methodology, data curation and project administration; R.B.: conceptualization, data curation, formal analysis, methodology, software, validation, visualization, writing—original draft, and writing—review and editing; F.T.: conceptualization, data curation, formal analysis, methodology, software, validation, visualization, writing—original draft, and writing—review and editing; A.L.: conceptualization, methodology, data curation and project administration; S.V.: methodology and formal analysis; C.G.: data curation, methodology and project administration; T.O.: methodology and formal analysis; A.R.M.: methodology, formal analysis, and writing—review and editing; G.K.: conceptualization, data curation, methodology, validation, writing—original draft, writing—review and editing, project administration, funding acquisition, resources and supervision.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Mental Health thanks Omid Dadras, Amanda C. de C. Williams and the other, anonymous, reviewers for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information (download PDF )
Supplementary Fig. 1 and Tables 1 and 2.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lurie, J.M., Pietz, H.L., Hatef, C. et al. Psychological stress, cardiovascular disease and somatic pain in asylum seekers: a retrospective cross-sectional study. Nat. Mental Health 2, 1442–1450 (2024). https://doi.org/10.1038/s44220-024-00312-3
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s44220-024-00312-3
This article is cited by
-
Post-migration Social Determinants of Health in Asylum Seekers: A Retrospective Qualitative Study
Journal of Immigrant and Minority Health (2025)