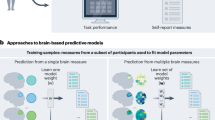
Abstract
Adolescence is a period of increased risk for the onset of depression. However, the neurobiological mechanisms underlying this vulnerability remain poorly understood despite substantial investment and efforts in this research area. In this Perspective, we review existing literature on the links between the adolescent brain and depression risk and development, and discuss methodological and conceptual challenges related to quantifying brain features and measuring depression. We highlight the importance of considering both large-scale longitudinal cohort studies and smaller focused investigator-led studies with deep phenotyping to advance our understanding of the neural basis of depression in adolescence. Emphasizing the need to embrace the developmental context and refine our methodologies, we propose several considerations to help current and future researchers advance our understanding of how the developing brain influences depression risk in today’s youth.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$79.00 per year
only $6.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Solmi, M. et al. Age at onset of mental disorders worldwide: large-scale meta-analysis of 192 epidemiological studies. Mol. Psychiatry 27, 281–295 (2022).
Sawyer, S. M., Azzopardi, P. S., Wickremarathne, D. & Patton, G. C. The age of adolescence. Lancet Child Adolesc. Health 2, 223–228 (2018).
McGorry, P. D. et al. The Lancet Psychiatry Commission on youth mental health. Lancet Psychiatry 11, 731–774 (2024).
Arnett, J. J. Emerging Adulthood: The Winding Road from the Late Teens Through the Twenties (Oxford Univ. Press, 2014).
GBD 2017 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 392, 1789–1858 (2018).
Thapar, A., Eyre, O., Patel, V. & Brent, D. Depression in young people. Lancet 400, 617–631 (2022).
Keyes, K. M. & Platt, J. M. Annual research review: sex, gender, and internalizing conditions among adolescents in the 21st century—trends, causes, consequences. J. Child Psychol. Psychiatry 65, 384–407 (2023).
Ho, T. C. Predicting depression risk in adolescents from multimodal data: current evidence and future directions. Biol. Psychiatry Cogn. Neurosci. Neuroimaging 7, 346–348 (2022).
Tervo-Clemmens, B., Marek, S. & Barch, D. M. Tailoring psychiatric neuroimaging to translational goals. JAMA Psychiatry 80, 765–766 (2023).
Schmaal, L. The search for clinically useful neuroimaging markers of depression—a worthwhile pursuit or a futile quest? JAMA Psychiatry 79, 845–846 (2022).
Gratton, C., Nelson, S. M. & Gordon, E. M. Brain–behavior correlations: two paths toward reliability. Neuron 110, 1446–1449 (2022).
Dhamala, E., Yeo, B. T. T. & Holmes, A. J. One size does not fit all: methodological considerations for brain-based predictive modeling in psychiatry. Biol. Psychiatry 93, 717–728 (2023).
Casey, B. J. et al. The Adolescent Brain Cognitive Development (ABCD) study: imaging acquisition across 21 sites. Dev. Cogn. Neurosci. 32, 43–54 (2018).
Mascarell Maričić, L. et al. The IMAGEN study: a decade of imaging genetics in adolescents. Mol. Psychiatry 25, 2648–2671 (2020).
Bethlehem, Ra. I. et al. Brain charts for the human lifespan. Nature 604, 525–533 (2022).
Edde, M., Leroux, G., Altena, E. & Chanraud, S. Functional brain connectivity changes across the human life span: from fetal development to old age. J. Neurosci. Res. 99, 236–262 (2021).
Blakemore, S. J. Imaging brain development: the adolescent brain. Neuroimage 61, 397–406 (2012).
Paus, T. How environment and genes shape the adolescent brain. Horm. Behav. 64, 195–202 (2013).
Tooley, U. A., Bassett, D. S. & Mackey, A. P. Environmental influences on the pace of brain development. Nat. Rev. Neurosci. 22, 372–384 (2021).
Schmaal, L. et al. Cortical abnormalities in adults and adolescents with major depression based on brain scans from 20 cohorts worldwide in the ENIGMA Major Depressive Disorder Working Group. Mol. Psychiatry 22, 900–909 (2017).
Schmaal, L. et al. ENIGMA MDD: seven years of global neuroimaging studies of major depression through worldwide data sharing. Transl. Psychiatry 10, 172–172 (2020).
Shen, X. et al. Brain structural associations with depression in a large early adolescent sample (the ABCD study®). eClinicalMedicine 42, 101204 (2021).
Opel, N. et al. Mediation of the influence of childhood maltreatment on depression relapse by cortical structure: a 2-year longitudinal observational study. Lancet Psychiatry 6, 318–326 (2019).
Skranes, J. et al. Cortical surface area and IQ in very-low-birth-weight (VLBW) young adults. Cortex 49, 2264–2271 (2013).
Ho, T. C. et al. Subcortical shape alterations in major depressive disorder: findings from the ENIGMA Major Depressive Disorder Working Group. Hum. Brain Mapp. 43, 341–351 (2022).
Schmaal, L. et al. Subcortical brain alterations in major depressive disorder: findings from the ENIGMA Major Depressive Disorder Working Group. Mol. Psychiatry 21, 806–812 (2016).
Weissman, D. G. et al. Reduced hippocampal and amygdala volume as a mechanism underlying stress sensitization to depression following childhood trauma. Depress. Anxiety 37, 916–925 (2020).
Rao, U. et al. Hippocampal changes associated with early-life adversity and vulnerability to depression. Biol. Psychiatry 67, 357–364 (2010).
Hubachek, S. et al. Hippocampal subregion volume in high-risk offspring is associated with increases in depressive symptoms across the transition to adolescence. J. Affect. Disord. 281, 358–366 (2021).
Hurtado, H. et al. Polygenic risk for depression and anterior and posterior hippocampal volume in children and adolescents. J. Affect. Disord. 344, 619–627 (2024).
Toenders, Y. J. et al. Neuroimaging predictors of onset and course of depression in childhood and adolescence: a systematic review of longitudinal studies. Dev. Cogn. Neurosci. 39, 100700 (2019).
Nelson, B. D., Perlman, G., Klein, D. N., Kotov, R. & Hajcak, G. Blunted neural response to rewards as a prospective predictor of the development of depression in adolescent girls. Am. J. Psychiatry 173, 1223–1230 (2016).
Stringaris, A. et al. The brain’s response to reward anticipation and depression in adolescence: dimensionality, specificity, and longitudinal predictions in a community-based sample. Am. J. Psychiatry 172, 1215–1223 (2015).
Foland‐Ross, L. C. et al. Cortical thickness predicts the first onset of major depression in adolescence. Int. J. Dev. Neurosci. 46, 125–131 (2015).
Vulser, H. et al. Early variations in white matter microstructure and depression outcome in adolescents with subthreshold depression. Am. J. Psychiatry 175, 1255–1264 (2018).
Luby, J. L., Barch, D., Whalen, D., Tillman, R. & Belden, A. Association between early life adversity and risk for poor emotional and physical health in adolescence: a putative mechanistic neurodevelopmental pathway. JAMA Pediatr. 171, 1168 (2017).
Papmeyer, M. et al. Cortical thickness in individuals at high familial risk of mood disorders as they develop major depressive disorder. Biol. Psychiatry 78, 58–66 (2015).
Little, K. et al. Association between serotonin transporter genotype, brain structure and adolescent-onset major depressive disorder: a longitudinal prospective study. Transl. Psychiatry 4, e445 (2014).
Luby, J. L. et al. Developmental trajectories of the orbitofrontal cortex and anhedonia in middle childhood and risk for substance use in adolescence in a longitudinal sample of depressed and healthy preschoolers. Am. J. Psychiatry 175, 1010–1021 (2018).
Toenders, Y. J. et al. Predicting depression onset in young people based on clinical, cognitive, environmental, and neurobiological data. Biol. Psychiatry Cogn. Neurosci. Neuroimaging 7, 376–384 (2022).
Zhi, D. et al. Triple interactions between the environment, brain, and behavior in children: an ABCD study. Biol. Psychiatry 95, 828–838 (2024).
Yoon, L. et al. Frontolimbic network topology associated with risk and presence of depression in adolescents: a study using a composite risk score in Brazil. Biol. Psychiatry Cogn. Neurosci. Neuroimaging 8, 426–435 (2023).
Jin, J. et al. Structural connectivity between rostral anterior cingulate cortex and amygdala predicts first onset of depressive disorders in adolescence. Biol. Psychiatry Cogn. Neurosci. Neuroimaging 7, 249–255 (2022).
Tse, N. Y. et al. A mega-analysis of functional connectivity and network abnormalities in youth depression. Nat. Ment. Health 2, 1169–1182 (2024).
Shen, X. et al. A phenome-wide association and Mendelian Randomisation study of polygenic risk for depression in UK Biobank. Nat. Commun. 11, 2301 (2020).
Bos, M. G. N., Peters, S., van de Kamp, F. C., Crone, E. A. & Tamnes, C. K. Emerging depression in adolescence coincides with accelerated frontal cortical thinning. J. Child Psychol. Psychiatry 59, 994–1002 (2018).
Albaugh, M. D. et al. Age-related volumetric change of limbic structures and subclinical anxious/depressed symptomatology in typically developing children and adolescents. Biol. Psychol. 124, 133–140 (2017).
Schmaal, L. et al. Brain structural signatures of adolescent depressive symptom trajectories: a longitudinal magnetic resonance imaging study. J. Am. Acad. Child Adolesc. Psychiatry 56, 593–601.e9 (2017).
Strikwerda-Brown, C. et al. Mapping the relationship between subgenual cingulate cortex functional connectivity and depressive symptoms across adolescence. Soc. Cogn. Affect. Neurosci. 10, 961–968 (2015).
Davey, C. G. et al. Functional brain-imaging correlates of negative affectivity and the onset of first-episode depression. Psychol. Med. 45, 1001–1009 (2015).
Jalbrzikowski, M. et al. Development of white matter microstructure and intrinsic functional connectivity between the amygdala and ventromedial prefrontal cortex: associations with anxiety and depression. Biol. Psychiatry 82, 511–521 (2017).
Ooi, L. Q. R. et al. Comparison of individualized behavioral predictions across anatomical, diffusion and functional connectivity MRI. Neuroimage 263, 119636 (2022).
Winter, N. R. et al. Quantifying deviations of brain structure and function in major depressive disorder across neuroimaging modalities. JAMA Psychiatry 79, 879 (2022).
Uhlhaas, P. J. et al. Towards a youth mental health paradigm: a perspective and roadmap. Mol. Psychiatry 28, 3171–3181 (2023).
Rolle, C. E. et al. Cortical connectivity moderators of antidepressant vs placebo treatment response in major depressive disorder: secondary analysis of a randomized clinical trial. JAMA Psychiatry 77, 397 (2020).
Cattarinussi, G., Delvecchio, G., Maggioni, E., Bressi, C. & Brambilla, P. Ultra-high field imaging in major depressive disorder: a review of structural and functional studies. J. Affect. Disord. 290, 65–73 (2021).
Makowski, C. et al. Leveraging the Adolescent Brain Cognitive Development study to improve behavioral prediction from neuroimaging in smaller replication samples. Cereb. Cortex 34, bhae223 (2024).
Marek, S. et al. Reproducible brain-wide association studies require thousands of individuals. Nature 603, 654–660 (2022).
Hubbard, N. A. et al. The Human Connectome Project of adolescent anxiety and depression dataset. Sci. Data 11, 837 (2024).
Auerbach, R. P. et al. Reward-related neural circuitry in depressed and anxious adolescents: a human connectome project. J. Am. Acad. Child Adolesc. Psychiatry 61, 308–320 (2022).
Fan, S., Wang, Y., Wang, Y. & Zang, Y. Revisiting resting-state functional connectivity of the amygdala and subgenual anterior cingulate cortex in depressed adolescents and adults. Biol. Psychiatry Cogn. Neurosci. Neuroimaging https://doi.org/10.1016/j.bpsc.2024.11.004 (2024).
Wolfers, T. et al. Mapping the heterogeneous phenotype of schizophrenia and bipolar disorder using normative models. JAMA Psychiatry 75, 1146 (2018).
Mills, K. L. et al. Inter-individual variability in structural brain development from late childhood to young adulthood. Neuroimage 242, 118450 (2021).
Tamnes, C. K., Bos, M. G. N., van de Kamp, F. C., Peters, S. & Crone, E. A. Longitudinal development of hippocampal subregions from childhood to adulthood. Dev. Cogn. Neurosci. 30, 212–222 (2018).
McGrath, J. J. et al. Age of onset and cumulative risk of mental disorders: a cross-national analysis of population surveys from 29 countries. Lancet Psychiatry 10, 668–681 (2023).
Marquand, A. F., Rezek, I., Buitelaar, J. & Beckmann, C. F. Understanding heterogeneity in clinical cohorts using normative models: beyond case-control studies. Biol. Psychiatry 80, 552–561 (2016).
Rutherford, S. et al. The normative modeling framework for computational psychiatry. Nat. Protoc. 17, 1711–1734 (2022).
Sun, X. et al. Mapping neurophysiological subtypes of major depressive disorder using normative models of the functional connectome. Biol. Psychiatry 94, 936–947 (2023).
Lv, J. et al. Individual deviations from normative models of brain structure in a large cross-sectional schizophrenia cohort. Mol. Psychiatry 26, 3512–3523 (2021).
Wolfers, T. et al. Replicating extensive brain structural heterogeneity in individuals with schizophrenia and bipolar disorder. Hum. Brain Mapp. 42, 2546–2555 (2021).
Segal, A. et al. Regional, circuit and network heterogeneity of brain abnormalities in psychiatric disorders. Nat. Neurosci. 26, 1613–1629 (2023).
Carrera, E. & Tononi, G. Diaschisis: past, present, future. Brain 137, 2408–2422 (2014).
Fornito, A., Zalesky, A. & Breakspear, M. The connectomics of brain disorders. Nat. Rev. Neurosci. 16, 159–172 (2015).
Maciejewski, D. F. et al. Most fare well—but some do not: distinct profiles of mood variability development and their association with adjustment during adolescence. Dev. Psychol. 55, 434–448 (2019).
Kjelkenes, R. et al. Deviations from normative brain white and gray matter structure are associated with psychopathology in youth. Dev. Cogn. Neurosci. 58, 101173 (2022).
Mulder, J. D. & Hamaker, E. L. Three extensions of the Random Intercept Cross-Lagged Panel Model. Struct. Equ. Modeling 28, 638–648 (2021).
Westlin, C. et al. Improving the study of brain–behavior relationships by revisiting basic assumptions. Trends Cogn. Sci. 27, 246–257 (2023).
Tiego, J. et al. Precision behavioral phenotyping as a strategy for uncovering the biological correlates of psychopathology. Nat. Ment. Health 1, 304–315 (2023).
Diagnostic and Statistical Manual of Mental Disorders: DSM-5 (American Psychiatric Association, 2013).
International Classification of Diseases 11th Revision (World Health Organization, 2022); https://icdcdn.who.int/icd11referenceguide/en/html/index.html
Kotov, R. et al. The Hierarchical Taxonomy of Psychopathology (HiTOP): a dimensional alternative to traditional nosologies. J. Abnorm. Psychol. 126, 454–477 (2017).
Insel, T. et al. Research Domain Criteria (RDoC): toward a new classification framework for research on mental disorders. Am. J. Psychiatry 167, 748–751 (2010).
Borsboom, D. A network theory of mental disorders. World Psychiatry 16, 5–13 (2017).
Eaton, N. R. et al. A review of approaches and models in psychopathology conceptualization research. Nat. Rev. Psychol. 2, 622–636 (2023).
Kessler, R. C. et al. Anxious and non-anxious major depressive disorder in the World Health Organization World Mental Health Surveys. Epidemiol. Psychiatr. Sci. 24, 210–226 (2015).
Simms, L. J. et al. Development of measures for the Hierarchical Taxonomy of Psychopathology (HiTOP): a collaborative scale development project. Assessment 29, 3–16 (2022).
Levin‐Aspenson, H. F. & Greene, A. L. Rethinking trauma‐related psychopathology in the Hierarchical Taxonomy of Psychopathology (HiTOP). J. Trauma. Stress 37, 361–371 (2024).
Ringwald, W. R., Forbes, M. K. & Wright, A. G. C. Meta-analysis of structural evidence for the Hierarchical Taxonomy of Psychopathology (HiTOP) model. Psychol. Med. 53, 533–546 (2023).
Tackett, J. L. & Hallquist, M. The need to grow: developmental considerations and challenges for modern psychiatric taxonomies. J. Psychopathol. Clin. Sci. 131, 660–663 (2022).
Forbes, M. K. et al. A hierarchical model of the symptom-level structure of psychopathology in youth. Clin. Psychol. Sci. 13, 278–300 (2024).
Waszczuk, M. A. et al. The prognostic utility of personality traits versus past psychiatric diagnoses: predicting future mental health and functioning. Clin. Psychol. Sci. 10, 734–751 (2022).
Sunderland, M. & Slade, T. The relationship between internalizing psychopathology and suicidality, treatment seeking, and disability in the Australian population. J. Affect. Disord. 171, 6–12 (2015).
Kim, H. et al. Internalizing psychopathology and all‐cause mortality: a comparison of transdiagnostic vs. diagnosis‐based risk prediction. World Psychiatry 20, 276–282 (2021).
Levin-Aspenson, H. F., Watson, D., Clark, L. A. & Zimmerman, M. What Is the general factor of psychopathology? Consistency of the p factor across samples. Assessment 28, 1035–1049 (2021).
Fried, E. I. Studying mental health problems as systems, not syndromes. Curr. Dir. Psychol. Sci. 31, 500–508 (2022).
Scheffer, M. et al. A dynamical systems view of psychiatric disorders—theory: a review. JAMA Psychiatry 81, 618–623 (2024).
Borsboom, D., Haslbeck, J. M. B. & Robinaugh, D. J. Systems‐based approaches to mental disorders are the only game in town. World Psychiatry 21, 420–422 (2022).
Weavers, B. et al. The antecedents and outcomes of persistent and remitting adolescent depressive symptom trajectories: a longitudinal, population-based English study. Lancet Psychiatry 8, 1053–1061 (2021).
Kuppens, P. It’s about time: a special section on affect dynamics. Emot. Rev. 7, 297–300 (2015).
Fried, E. I., Proppert, R. K. K. & Rieble, C. L. Building an early warning system for depression: rationale, objectives, and methods of the WARN-D study. Clin. Psychol. Eur. 5, e10075 (2023).
Schoevers, R. A. et al. Affect fluctuations examined with ecological momentary assessment in patients with current or remitted depression and anxiety disorders. Psychol. Med. 51, 1906–1915 (2021).
Silk, J. S. et al. Daily emotional dynamics in depressed youth: a cell phone ecological momentary assessment study. J. Exp. Child Psychol. 110, 241–257 (2011).
Cousins, J. C. et al. The bidirectional association between daytime affect and nighttime sleep in youth with anxiety and depression. J. Pediatr. Psychol. 36, 969–979 (2011).
Walsh, R. J. et al. Social contexts, momentary mood and affective variability in early adolescence: an exploratory ecological momentary assessment study. J. Early Adolesc. 44, 59–95 (2024).
Henderson, C., Robinson, E., Evans-Lacko, S. & Thornicroft, G. Relationships between anti-stigma programme awareness, disclosure comfort and intended help-seeking regarding a mental health problem. Br. J. Psychiatry 211, 316–322 (2017).
Sampogna, G. et al. The impact of social marketing campaigns on reducing mental health stigma: results from the 2009–2014 Time to Change programme. Eur. Psychiatry 40, 116–122 (2017).
Collishaw, S. Annual research review: secular trends in child and adolescent mental health. J. Child Psychol. Psychiatry 56, 370–393 (2015).
Orben, A., Meier, A., Dalgleish, T. & Blakemore, S.-J. Mechanisms linking social media use to adolescent mental health vulnerability. Nat. Rev. Psychol. 3, 407–423 (2024).
Högberg, B. Educational stressors and secular trends in school stress and mental health problems in adolescents. Soc. Sci. Med. 270, 113616 (2021).
Foulkes, L. & Andrews, J. L. Are mental health awareness efforts contributing to the rise in reported mental health problems? A call to test the prevalence inflation hypothesis. New Ideas Psychol. 69, 101010 (2023).
Foulkes, L. What Mental Illness Really Is … (and What It Isn’t) (Vintage, 2022).
McCashin, D. & Murphy, C. M. Using TikTok for public and youth mental health—a systematic review and content analysis. Clin. Child Psychol. Psychiatry 28, 279–306 (2023).
Driven into the Darkness: How TikTok’s ‘For You’ Feed Encourages Self-Harm and Suicidal Ideation (Amnesty International, 2021); https://www.amnesty.org/en/documents/POL40/7350/2023/en/
MacSweeney, N., Bowman, S. & Kelly, C. More than just characters in a story: effective and meaningful involvement of young people in mental health research. J. Public Ment. Health 18, 14–16 (2019).
Toenders, Y. J. et al. From developmental neuroscience to policy: a novel framework based on participatory research. Dev. Cogn. Neurosci. 67, 101398 (2024).
Crone, E. A. & Achterberg, M. Prosocial development in adolescence. Curr. Opin. Psychol. 44, 220–225 (2022).
Acknowledgments
N.M. and C.K.T. are supported by the South-Eastern Norway Regional Health Authority (number 2023012). Y.J.T. is supported by Convergence | Healthy Start, a program of the Convergence Alliance—Delft University of Technology, Erasmus University Rotterdam and Erasmus Medical Center. C.K.T. is supported by the South-Eastern Norway Regional Health Authority (number 2021070 and number 500189) and the Research Council of Norway (number 288083 and number 323951).
Author information
Authors and Affiliations
Contributions
N.M.: conceptualization; writing—original draft, writing—review and editing; visualization, project administration. Y.J.T.: conceptualization; writing—original draft, writing—review and editing. C.K.T.: conceptualization; writing—review and editing; funding acquisition.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Mental Health thanks Nicholas Hubbard and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
MacSweeney, N., Toenders, Y.J. & Tamnes, C.K. Neuroimaging insights into adolescent depression risk and development. Nat. Mental Health 3, 772–779 (2025). https://doi.org/10.1038/s44220-025-00453-z
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s44220-025-00453-z
This article is cited by
-
Symptom-specific links between internalizing problems and functional connectivity in adolescents: a network analysis
European Child & Adolescent Psychiatry (2026)
-
The nature of the relation between mental well-being and ill-being
Nature Human Behaviour (2025)