Abstract
As the population of individuals with limited English proficiency (LEP) continues to rise in the United States, language barriers have become an increasingly important yet underrecognized driver of disparities in cancer care. This review aims to synthesize current evidence on how LEP affects the cancer care continuum and to offer actionable strategies to promote equity. We conducted a comprehensive review of the literature spanning communication, diagnosis, treatment, outcomes, prevention, research participation, and policy related to LEP populations in oncology. LEP is associated with poorer cancer outcomes, including delayed diagnosis, lower treatment adherence, decreased access to supportive services, and reduced quality of life. These disparities stem from multilevel communication barriers, underuse of professional interpretation, cultural discordance, and limited institutional support for language-concordant care. LEP patients are also underrepresented in cancer research due to language-based exclusion criteria, inadequate translation resources, and provider burden. A multifaceted framework is needed to address LEP-related disparities in oncology. Key strategies include expanding language-concordant care teams, improving interpreter and translation services, designing inclusive research protocols, and embedding language equity into institutional safety culture and policy. Addressing these disparities is a clinical, ethical, and public health imperative requiring systemic investment and leadership.

Similar content being viewed by others
Background
As of 2023, the U.S. immigrant population reached a record high of 47.8 million [1]. Among individuals aged 5 and older, 68.8 million (22.0%) speak a language other than English at home, with Spanish being the most common (13.4%) [2]. An estimated 26.3 million individuals (8.4%) and 5.4 million households (4.2%) are considered limited English proficient (LEP), indicating difficulty with reading, writing, speaking, or understanding English (Figs. 1 and 2).
a Choropleth map showing the percentage of U.S. residents aged 5 and older with LEP by state. Darker shades indicate states with a higher proportion of LEP individuals, ranging from 0.7% to 17.3%. b Bar graph ranking states by LEP prevalence among individuals aged 5 and older. California (17.3%), New York (13.3%), Texas (12.8%), and New Jersey (12.7%) report the highest proportions. LEP, limited English proficiency.
a Proportion of U.S. residents aged 5 and older with LEP. Of 313.4 million individuals, 26.3 million (8.4%) are classified as LEP. Abbreviations: LEP, limited English proficiency. b Proportion of U.S. households in which no member aged 14 or older (1) speaks only English or (2) speaks a non-English language and speaks English “very well.” Of 127.5 million households, 5.4 million (4.2%) meet the LEP household criteria. c Distribution of LEP households by primary language spoken. Gray bars represent the total number of U.S. households per language group, green bars represent LEP households within each group, and the green line indicates the percentage of LEP households within that group. Spanish-speaking households account for the largest share (3.2 million), while Chinese (31.2%), Korean (30.0%), and Vietnamese (29.8%) households exhibit the highest within-group LEP rates. Abbreviation: LEP, limited English proficiency.
The growing LEP population raises critical concerns about language-related disparities in healthcare. Language barriers impede effective communication with medical staff, hinder understanding of care instructions, and create difficulties with form completion, medication management, and appointment scheduling [3]. Compounding these challenges, many LEP individuals face lower income, limited educational attainment, and employment in low-wage jobs, factors that increase the likelihood of being uninsured and exacerbate disparities in access, adherence, and preventive care [4,5,6,7]. Together, these systemic barriers contribute to poorer health outcomes, including inadequate chronic disease management, greater reliance on emergency department (ED) services, longer hospital stays, and higher rates of readmissions and complications [4,5,6,7].
Despite growing research on healthcare disparities, the impact of LEP on cancer care remains underexplored. Most data come from English-speaking populations, with limited attention to language barriers, inconsistent reporting, and few targeted interventions [8, 9]. As the burden of cancer rises, especially among racial and ethnic minorities, language discordance remains a persistent barrier to effective care, even with federal protections in place [10]. This review outlines the unique challenges LEP patients face in cancer care, highlights disparities across the continuum, and offers actionable strategies to promote language-concordant care and improve outcomes for this underserved population.
Communication disparities across the cancer care continuum
Challenges in communication among patients, caregivers, providers, interpreters, and at the system level contribute significantly to disparities in cancer care for LEP individuals. Patients with LEP often lack awareness of available support, such as free interpreter services, and rely on family members for translation, raising concerns about privacy and accuracy [11]. Access to language-specific materials (e.g., discharge instructions or treatment plans) is limited, and when available, they are frequently overly technical, culturally insensitive, or lacking actionable guidance (e.g., clinic contact information or referrals) [12,13,14].
These challenges are compounded by the complexity of the U.S. healthcare system. LEP patients may be unfamiliar with shared decision-making norms and may hold cultural beliefs (such as respeto and fatalismo among Hispanic populations) that discourage questioning providers [15,16,17]. When combined with low health literacy and limited information-seeking behaviors, these factors can lead to reduced engagement in care and poor adherence to treatment recommendations [11]. LEP patients also face systemic barriers to financial support and may be less likely to receive assistance, further widening existing disparities [18, 19]. Caregivers encounter similar barriers, which may be intensified by undocumented immigration status, financial strain, and limited access to psychosocial resources [18, 20, 21].
On the provider side, language barriers lead to incomplete histories, inadequate consent processes, and missed opportunities for patient education [22]. Reliance on untrained ad hoc interpreters and underuse of professional services, due to time pressure or overestimation of language proficiency, further compromise care [11, 13, 23, 24] Even professional interpreters may lack the training for complex topics like clinical trials or genetic counseling, leading to errors and miscommunication [13, 25,26,27,28]. At the system level, limited interpreter availability, cost barriers, and interpreter delays impede timely, high-quality care [11, 29]. Language barriers are particularly harmful during critical conversations, including end-of-life discussions, where they are linked to poorer quality of life outcomes [30].
National data highlight substantial gaps in institutional compliance with language access standards. In a survey of Medicare providers, 69% reported conducting the four-factor assessment recommended by the Office for Civil Rights, yet only 33% offered services consistent with all four National Culturally and Linguistically Appropriate Services (CLAS) Standards [31]. While 73% acknowledged benefits to providing language access services, nearly half cited obstacles, such as staffing shortages and equipment limitations, and few could provide reliable data on costs [31]. These findings underscore that interpreter and translation services remain inconsistently implemented, with persistent technical barriers and resource constraints reinforcing disparities and hindering equitable cancer care for LEP patients.
Disparities in cancer detection and care delivery
Language discordance contributes to disparities in both cancer incidence and stage at diagnosis. States with high LEP populations, such as California (8.5%) and New York (7.6%), report elevated rates of ovarian and stomach cancers: 10.4 and 9.1 per 100,000 in California, and 11.3 and 10.9 in New York, respectively [32]. LEP patients are also more likely to present with advanced-stage cancers, including pancreatic, head and neck, and breast cancers, as well as higher-risk pediatric malignancies [13, 33,34,35,36]. While some studies note lower odds of late-stage colorectal cancer among Hispanics, the broader evidence highlights diagnostic delays tied to language barriers [37].
These diagnostic disparities extend into treatment and follow-up. LEP patients, especially Spanish-speaking and uninsured individuals, experience delays in initiating care for breast, head and neck, colorectal, and lung cancers [38,39,40]. These delays typically stem from difficulty understanding pre-treatment instructions, managing medications, monitoring symptoms, and navigating follow-up. Although one study found no language effect on radiotherapy timing, LEP remains associated with reduced receipt of cancer-directed therapies and variable treatment plans, particularly in pancreatic and head and neck cancers [33, 34, 41, 42].
During follow-up, LEP patients, especially in pediatrics, show lower adherence to survivorship care and more frequent missed visits [13, 43]. They also have higher ED use, longer hospital stays, and greater readmission rates, particularly in breast, pancreatic, and brain cancers [9, 13, 44,45,46,47]. Higher weekend admission rates suggest delayed care-seeking and more advanced illness [48, 49]. LEP is also independently associated with increased healthcare costs and higher likelihood of discharge to skilled nursing facilities [50].
Disparities in clinical outcomes and quality of life
Despite treatment, patients with LEP may experience worse clinical outcomes. Those with head and neck cancer, for example, have poorer locoregional control following radiation, likely due to missed appointments, misunderstanding of protocols, or underreporting of side effects [51]. Difficulty understanding medication labels and pre-surgical instructions can also lead to dosing errors, improper fasting, and missed warning signs, increasing the risk of serious complications [5, 52, 53].
LEP patients frequently report lower quality of life, higher symptom burden, and greater emotional distress during cancer care. These issues are often rooted in miscommunication surrounding diagnoses, treatment plans, discharge instructions, and follow-up care [54,55,56]. While some studies show no significant differences in hospice or palliative care use, language barriers continue to hinder effective end-of-life communication and decision-making [50, 57,58,59]. In pediatric hospice, Spanish-speaking families have described frustrations with insensitive communication and distressing ED interactions [60]. Insurance challenges further restrict access to supportive services, such as hospice care, visiting nurses, and specialty referrals [11].
Survival disparities have also been documented among LEP patients, particularly in breast, pancreatic and pediatric cancers, where lower overall, disease-free, and disease-specific survival have been observed [13, 33, 38]. However, findings are mixed; some studies show no differences, and certain groups, like Haitian Creole speakers with prostate cancer, have even shown improved survival [45, 61,62,63]. These exceptions may be suggestive of the underlying differences in institutional resources and healthcare infrastructure and present opportunities for targeted interventions [48, 64].
Disparities in prevention and early detection
Language barriers, limited familiarity with preventive care, and systemic inefficiencies reduce awareness and participation in services, such as immunization, genetic counseling, and cancer screenings [65]. English proficiency strongly correlates with HPV awareness, and misconceptions about vaccine-preventable cancers remain prevalent among those with LEP [66]. While LEP patients may access genetic counseling for breast cancer at similar rates to English speakers, reliance on family members as intermediaries can lead to filtered information and loss of patient autonomy [67, 68]. In some cases, family members even withhold diagnoses, complicating decision-making.
LEP is consistently linked to lower cancer screening rates. Urban LEP populations, such as in New York City, show reduced colorectal and cervical screening [69]. Asian Americans with LEP are less likely to be up-to-date on breast, cervical, and colorectal screenings [70,71,72]. Clinics unequipped for translation services exacerbate delays in cervical screening [73]. LEP patients also demonstrate lower completion rates for colorectal, prostate, and lung cancer screenings [74,75,76,77].
Disparities in cancer research participation
LEP individuals remain underrepresented in clinical trials, with enrollment stagnating despite a growing population, particularly in gynecologic oncology [67, 78, 79]. Many U.S. interventional trials exclude non-English speakers, with 40% citing reasons such as unanticipated language needs (51%), difficulty translating materials, and lack of bilingual staff [13, 80, 81]. Limited translated resources and financial constraints further restrict access, disproportionately burdening LEP patients [82]. Notably, when funding for translated consent forms was withdrawn in gynecologic oncology trials, enrollment of Hispanic LEP patients sharply declined [83].
Provider-related factors compound these challenges. Many clinicians may find it burdensome to determine eligibility (75%) or explain trial risks and benefits (68%) to LEP patients [84]. As a result, essential details, such as randomization, withdrawal rights, and consent documentation, are often poorly communicated, leaving patients less informed and deepening mistrust [16, 84,85,86]. This underrepresentation skews data on drug efficacy and safety, limiting the generalizability of trial findings and reinforcing disparities.
Strategies to address disparities in cancer care
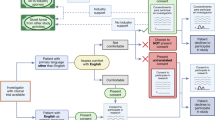
Addressing cancer care disparities among patients with LEP requires a multifaceted strategy (Fig. 3). Here, we discuss and propose interventions to improve access, quality, and outcomes across the cancer care continuum.
Framework highlighting four core domains for reducing cancer care disparities among individuals with LEP: (1) Language Services, including language-concordant care, interpretation, translation, and supplemental strategies; (2) Research Inclusivity, focusing on equitable policy implementation, resource allocation, inclusive study design, and training; (3) Public Education & Engagement, involving digital tools, multilingual resources, and community partnerships; and (4) Safety Culture, emphasizing standardization, reporting, high-risk scenario planning, and team-based training. Abbreviation: LEP, limited English proficiency.
Language access policies
Language access is a civil right rooted in principles of distributive and language justice, ensuring equitable resource allocation and affirming the dignity of linguistic minorities. Creating multilingual spaces enables LEP individuals to fully participate in care and benefit from medical advancements. Over time, key policies have laid a foundation for addressing disparities in cancer care (Fig. 4). By 2019, all U.S. states and D.C. had enacted healthcare language access laws. California leads with 257 provisions, including Medicaid translation requirements [87]. While all states have at least three provisions, their scope varies, ranging from broad mandates to targeted measures for specific providers or populations. Some include detailed implementation guidance; others recognize language access without specifying actions.
Timeline highlighting key federal policies, reports, and initiatives from 1964 to 2023 that have shaped efforts to reduce health disparities and improve language access for individuals with LEP. Abbreviations: CDC, Centers for Disease Control and Prevention; CLAS, Culturally and Linguistically Appropriate Services; CMS, Centers for Medicare & Medicaid Services; HHS, U.S. Department of Health and Human Services; LEP, limited English proficiency; NIH, National Institutes of Health; ODPHP, Office of Disease Prevention and Health Promotion.
Together, these policies form an ethical, legal, and practical framework to reduce disparities. Recognizing language access as a civil right ensures LEP patients are not excluded from health equity efforts. Embedding equity principles in cancer care requires a coordinated, ongoing effort from policymakers and healthcare institutions alike.
Language services
Recognizing language access as a civil right is foundational, but effective implementation requires practical strategies. One such strategy for expanding language-concordant care is to involve providers, navigators, and community health workers who can speak a patient’s preferred language, when feasible.
(1) Language-concordant teams
Language-concordant providers improve satisfaction, communication, and therapeutic relationships [88, 89]. Among Asian Americans, those with language-concordant clinicians reported screening rates comparable to English speakers, highlighting its impact on preventive care [70]. Conversely, the shortage of Spanish-speaking providers contributes to disparities for Hispanic/Latino patients [90]. Culturally competent nurses help patients navigate the U.S. healthcare system, encouraging autonomy and symptom reporting [11]. Patient navigators have successfully recruited and retained underserved Latino adults with advanced cancer in a randomized trial and increased cancer screening rates across multiple populations [91,92,93,94]. Community health workers, such as promotoras in Hispanic communities, further boost screening rates and health literacy through culturally tailored, language-aligned interventions [71, 95,96,97,98,99,100].
In more specialized contexts, language-concordant genetic counselors have been instrumental in improving patient experiences during cancer genetic counseling. Spanish-speaking patients report positive outcomes when counseled in their preferred language, emphasizing the need for linguistic alignment in complex discussions about hereditary cancer risks [101]. Likewise, language-concordant patient family advocates in pediatric oncology have reduced stress and fostered trust, communication, and continuity of care for LEP families [101, 102].
To expand the availability of language-concordant care, several workforce strategies have been proposed. These include targeted recruitment and retention of bilingual medical students and residents, supported by loan forgiveness or pipeline programs aimed at underrepresented linguistic groups, and incentivizing dual certification, such as formal Spanish proficiency testing with CME credit [103]. Embedding community health workers and promotoras directly into oncology care teams ensures culturally aligned navigation throughout the cancer care continuum, while leveraging telemedicine can connect LEP patients to language-concordant specialists across institutions, particularly in settings where local bilingual providers are unavailable [104, 105].
(2) Interpretation services
Full language concordance is not always feasible due to resource constraints, workforce shortages, and linguistic diversity. In such cases, interpretation services play a critical role in bridging communication gaps. Trained interpreters improve comprehension, reduce errors, and enhance clinical outcomes and satisfaction compared to ad hoc alternatives [106,107,108]. In pediatric oncology, interpreters frequently extend beyond their formal roles to support families during complex care [109].
Remote options via telephone and video expand access and timeliness. Studies show they can match or exceed in-person interpreting for routine tasks like discharge instructions [110,111,112,113,114]. Bilingual phone interventions have increased cancer screening, especially among Spanish-speaking women, and improved Hispanic enrollment in clinical trials [115, 116]. Despite their benefits, providers often prefer in-person interpreters for complex discussions (e.g., device education, advanced care planning) due to the lack of visual cues, background noise, connectivity issues, and limited dialect support with remote options [24, 117].
To optimize interpretation services, hospital administrations should prioritize funding for interpreter infrastructure and training [118,119,120]. They are well-positioned to expand remote options, implement automated scheduling systems that streamline access for LEP patients, and ensure the delivery of standardized interpreter training programs. Requiring at least 100 h of training for interpreters has been shown to reduce clinical errors by up to 70% and significantly improve safety and quality [27, 107, 121]. These programs should also incorporate pre- and post-encounter briefings to align expectations and address challenges [122, 123]. Ultimately, apart from hospital administrations, the responsibility for proper implementation of interpreter services must be shared across different stakeholders: nursing leadership could oversee the implementation of training modules, while professional oncology societies and accrediting bodies can embed language-access standards into quality benchmarks. Frontline clinicians and nurses must also be educated to consistently document interpreter use in the electronic health record [124, 125].
(3) Translation services
While interpretation supports real-time communication, translation services are vital for providing LEP patients with accessible written materials throughout cancer care. One key application is improving medication adherence. The University of Colorado Health translated prescription labels into 26 languages, enhancing understanding and adherence among non-English speakers [126]. Similarly, ConcordantRx used health literacy-informed multilingual instructions to improve dosing accuracy and treatment adherence [127]. Yet, many pharmacies still rely on patient requests. Proactively offering multilingual labels and counseling patients on medication use can significantly enhance safety [128].
Digital tools further expand access. Apps like MediBabble and platforms like Google Translate help providers and LEP patients communicate in urgent settings, improving satisfaction [5, 129,130,131]. Tools like Sisom help children express cancer symptoms in their native language [132]. However, these tools often lack accuracy for complex medical content and should supplement, not replace, professional translation [129, 130]. Federal guidelines stress that machine-generated content must be reviewed by qualified human translators to meet legal standards [133,134,135].
To optimize translation services, systems must ensure accuracy, address cost barriers, and proactively offer multilingual resources. Providers play a key role in assessing comprehension and tailoring materials. Moffitt Cancer Center demonstrates this with an integrated model offering free interpreting and translation services. Between 2011 and 2013, they completed over 25,000 interpretation encounters and 1400 translation projects, earning a 4.8/5 patient satisfaction score [136].
Inclusive research
Sponsors and pharmaceutical companies have a critical role in addressing the underrepresentation of LEP individuals in clinical research. Recommended strategies include mandating dedicated budget lines for translating consent forms and other trial materials, requiring sites to demonstrate interpreter access before trial activation, partnering with community-based organizations for multilingual outreach, and publicly reporting enrollment demographics stratified by language to enhance transparency [137, 138]. Some sponsors have piloted initiatives, such as multilingual enrollment hotlines and the hiring of bilingual research coordinators, which have shown promise in improving participation among LEP patients [138]. Yet these remain isolated examples; broad implementation of such measures is critical to achieving equity goals in clinical trials.
Federal agencies emphasize the ethical importance of inclusive research. The Food and Drug Administration (FDA) recommends that Institutional Review Boards (IRBs) ensure translated consent materials and interpreter support throughout the trial [139]. Informed consent should be treated as an ongoing dialogue, not a one-time event. However, IRB practices vary; some offer comprehensive language access guidelines, while others do not [140]. Initiatives such as the FDA’s Section 907 Action Plan and Drug Trials Snapshots aim to improve demographic representation and highlight differences in treatment outcomes across subgroups [141, 142].
To further promote inclusivity, IRBs should avoid imposing language restrictions unless justified [80]. Journals can support this goal by requiring researchers to explain their inclusion and exclusion criteria [143]. Equipping investigators with the skills to collaborate with interpreters and design linguistically inclusive protocols is critical, and clinicians play a key role in advocating for language access in both clinical care and research settings [137, 138]. Ultimately, creating a more inclusive research environment is not only an ethical and legal responsibility; it is a scientific necessity for producing valid, generalizable findings that reflect the populations served.
Safety culture
Creating a culture of safety for LEP patients requires healthcare organizations to embed language access and cultural competence into every level of care. Language barriers significantly increase the risk of adverse events, underscoring the need to incorporate these priorities into safety protocols, supported by leadership, strategic planning, and dedicated resources. The Agency for Healthcare Research and Quality emphasizes that overcoming language barriers should be central to an institution’s quality and safety mission [144]. Embedding language access into operational policies and learning from LEP-related safety events promotes continuous improvement. Patient and family advisory councils offer important perspectives for guiding targeted interventions.
A strong safety culture also relies on accurate reporting and documentation. Staff, including interpreters, should be trained to report all safety events, including near misses. The FDA’s MedWatch program supports this process with Spanish-language reporting tools [145]. Documenting language preferences and interpreter use in electronic health records enables health systems to monitor outcomes and identify areas for improvement. Certain clinical scenarios, such as medication reconciliation, discharge, informed consent, emergency care, and surgery, pose heightened risks for LEP patients. These moments require qualified interpreters and plain-language translated materials to ensure clarity and prevent miscommunication. The teach-back method can be used to confirm patient understanding.
To support ongoing improvement, organizations should implement structured team training. The Agency for Healthcare Research and Quality’s TeamSTEPPS LEP Module equips interdisciplinary teams to enhance communication and reduce errors [146]. Techniques like briefs, check-backs, and teach-backs foster collaboration and psychological safety among care teams. Ultimately, fostering a robust safety culture for LEP patients requires institutional commitment, regular review of LEP-related data, and sustained investment in language-access infrastructure.
Public education and engagement
Public education is essential for meeting the needs of LEP patients by improving health literacy, navigation, and access to services. Multilingual resources help LEP individuals navigate healthcare systems and address social determinants of health. LEP.gov (available in 21 languages) and the Coverage to Care initiative (in nine languages) provide guidance on coverage, primary care, and preventative services.
Public education also improves cancer literacy. Tools like The Health Communicator support older migrant patients with tailored, multilingual resources. NCCN Guidelines®, available in multiple languages and mobile formats, empower patients and clinicians alike. Language-concordant platforms, such as call centers and websites, boost engagement in clinical trials [147]. Digital tools assist LEP patients in tracking symptoms and managing care. The American Cancer Society’s Personal Health Manager (English/Spanish) and Spanish-language electronic symptom reporting systems improve communication and care continuity [148, 149]. Multimedia interventions, including native-language videos, reminders, and culturally adapted materials, have increased screening rates among refugees and LEP populations [100, 150,151,152]. A Florida cancer center’s multilevel strategy combining interpreters, navigators, and provider training notably boosted lung cancer screening among Hispanic and Black patients [153].
Partnerships with community organizations enhance outreach. FDA-led webinars and advisory committees give LEP communities a voice in health policy. Biweekly updates from the FDA’s Office of Minority Health and Health Equity keep patients and providers informed about safety, funding, and research initiatives.
Conclusion
Disparities in cancer care for LEP patients span the entire care continuum from prevention to survivorship. This review highlights the need for comprehensive, multifaceted strategies to close these gaps. Key approaches include expanding language-concordant care, improving interpretation and translation services, and enhancing public education and engagement. Tailored digital tools, multilingual materials, and culturally adapted interventions have shown success in improving cancer literacy, screening uptake, and treatment adherence. However, these efforts must be paired with systemic changes, such as equitable digital access, targeted workforce training, and strong policy enforcement to ensure sustained impact. Partnering with community organizations, stakeholders, and LEP individuals creates a feedback loop that builds trust, improves communication, and informs culturally relevant programs and policies.
Ultimately, addressing these disparities is both a moral and public health imperative. By advancing inclusive, patient-centered care and embedding equity and safety into healthcare systems, we can ensure all patients, regardless of language proficiency, receive high-quality, compassionate cancer care.
Data availability
The data supporting Figs. 1 and 2 are publicly available from the U.S. Census Bureau, 2019-2023 American Community Survey (ACS) 5-Year Estimates. Data can be accessed through the Census Bureau’s data portal at: https://data.census.gov/. No additional proprietary datasets were generated or analyzed for this study.
References
Passel JG and JS. U.S. immigrant population in 2023 saw largest increase in more than 20 years [Internet]. Pew Res. Cent. 2024 [cited 2025 Mar 13]. Available from: https://www.pewresearch.org/short-reads/2024/09/27/u-s-immigrant-population-in-2023-saw-largest-increase-in-more-than-20-years/
Bureau UC. Language Spoken at Home [Internet]. Census.gov. [cited 2025 Mar 13]. Available from: https://www.census.gov/programs-surveys/acs/
Artiga S, Hamel L, Gonzalez-Barrera A, Montero A, Hill L, Presiado M, et al. Survey on Racism, Discrimination and Health - Findings - 10257 [Internet]. KFF. 2023 [cited 2025 Mar 13]. Available from: https://www.kff.org/report-section/survey-on-racism-discrimination-and-health-findings/
Cano-Ibáñez N, Zolfaghari Y, Amezcua-Prieto C, Khan KS. Physician–Patient Language Discordance and Poor Health Outcomes: A Systematic Scoping Review. Front Public Health [Internet]. 2021 [cited 2025 Mar 13];9. Available from: https://www.frontiersin.org/journals/public-health/articles/10.3389/fpubh.2021.629041/full
Al Shamsi H, Almutairi AG, Al Mashrafi S, Al Kalbani T. Implications of Language Barriers for. Healthcare: A Systematic Review. Oman Med J. 2020;35:e122.
Lu T, Myerson R. Disparities in Health Insurance Coverage and Access to Care by English Language Proficiency in the USA, 2006-2016. J Gen Intern Med. 2020;35:1490–7.
Diamond L, Izquierdo K, Canfield D, Matsoukas K, Gany F. A Systematic Review of the Impact of Patient-Physician Non-English Language Concordance on Quality of Care and Outcomes. J Gen Intern Med. 2019;34:1591–606.
Shaw V, Zhang B, Tang M, Peng W, Amos C, Cheng C. Racial and socioeconomic disparities in survival improvement of eight cancers. BJC Rep. 2024;2:1–9.
Smith KM, Rogers CR, Akinola OO, Holbert NA, Blunt HB, Yen RW. The impact of limited English proficiency on oncological outcomes in the United States: A systematic review. J Eval Clin Pract. 2025;31:e14112.
Smith BD, Smith GL, Hurria A, Hortobagyi GN, Buchholz TA. Future of Cancer Incidence in the United States: Burdens Upon an Aging, Changing Nation. J Clin Oncol. 2009;27:2758–65.
Perez GK, Mutchler J, Yang MS, Fox Tree-Mcgrath C, Park ER. Promoting quality care in patients with cancer with limited English proficiency: perspectives of medical interpreters. Psychooncology. 2016;25:1241–5.
Alvarez AH, Escobar-Domingo MJ, Lee D, Schuster K, Foppiani J, Taritsa I, et al. Beyond the language barrier: Assessing health literacy of Spanish breast cancer surgery resources. Surgery. 2024;176:1029–35.
Robles JM, Ruiz J, Correa R, Dinescu-Munoz N, Patel C, Noyd D, et al. The impact of language discordance on pediatric cancer care outcomes: A systematic review. Pediatr Blood Cancer. 2024;71:e31338.
Chen DW, Banerjee M, He X, Miranda L, Watanabe M, Veenstra CM, et al. Hidden Disparities: How Language Influences Patients’ Access to Cancer Care. J Natl Compr Cancer Netw JNCCN. 2023;21(951-959):e1.
Vanderpool RC, Kornfeld J, Rutten LF, Squiers L. Cancer information-seeking experiences: the implications of Hispanic ethnicity and Spanish language. J Cancer Educ Off J Am Assoc Cancer Educ. 2009;24:141–7.
Simon C, Zyzanski SJ, Eder M, Raiz P, Kodish ED, Siminoff LA. Groups Potentially at Risk for Making Poorly Informed Decisions About Entry into Clinical Trials for Childhood Cancer. J Clin Oncol [Internet]. 2003 [cited 2025 Mar 14]; Available from: https://ascopubs.org/doi/10.1200/JCO.2003.03.003
Zhao X. Cancer Information Disparities Between U.S.- and Foreign-Born Populations. J Health Commun. 2010;15:5–21.
Shi JJ, McGinnis GJ, Peterson SK, Taku N, Chen Y-S, Yu RK, et al. Pilot study of a Spanish language measure of financial toxicity in underserved Hispanic cancer patients with low English proficiency. Front Psychol [Internet]. 2023 [cited 2025 Mar 14];14. Available from: https://www.frontiersin.org/journals/psychology/articles/10.3389/fpsyg.2023.1188783/full
Ragavan MV, Swartz S, Clark M, Lo M, Gupta A, Chino F, et al. to Financial Assistance Programs and Their Impact on Overall Spending on Oral Anticancer Medications at an Integrated Specialty Pharmacy. JCO Oncol Pract. 2024;20:291–9. Access.
Murong M, Giannopoulos E, Pirrie L, Giuliani ME, Fazelzad R, Bender J, et al. The Experience of Informal Newcomer Cancer Caregivers with Limited Language Proficiency: A Scoping Review. J Immigr Minor Health. 2023;25:436–48.
Zamora ER, Kaul S, Kirchhoff AC, Gwilliam V, Jimenez OA, Morreall DK, et al. The impact of language barriers and immigration status on the care experience for Spanish-speaking caregivers of patients with pediatric cancer. Pediatr Blood Cancer. 2016;63:2173–80.
Youdelman M. The High Costs of Language Barriers in Medical Malpractice [Internet]. Natl. Health Law Program. 2013 [cited 2025 Mar 14]. Available from: https://nhelprestordev.wpenginepowered.com/resource/the-high-costs-of-language-barriers-in-medical-malpractice/
Martin FC, Philip J, McLachlan S-A. Healthcare Professionals’ Views of Working with Medical Interpreters in a Cancer Setting: an Exploratory Study. J Cancer Educ. 2022;37:1115–21.
Fiedler J, Pruskil S, Wiessner C, Zimmermann T, Scherer M. Remote interpreting in primary care settings: a feasibility trial in Germany. BMC Health Serv Res. 2022;22:99.
Karliner LS, Pérez-Stable EJ, Gildengorin G. The Language Divide. J Gen Intern Med. 2004;19:175–83.
Lara-Otero K, Weil J, Guerra C, Cheng JKY, Youngblom J, Joseph G. Genetic Counselor and Healthcare Interpreter Perspectives on the Role of Interpreters in Cancer Genetic Counseling. Health Commun. 2019;34:1608–18.
Donelan K, Hobrecker K, Schapira L, Mailhot JR, Goulart BH, Chabner BA. Medical interpreter knowledge of cancer and cancer clinical trials. Cancer. 2009;115:3283–92.
Simon CM, Zyzanski SJ, Durand E, Jimenez XF, Kodish ED. Interpreter accuracy and informed consent among Spanish-speaking families with cancer. J Health Commun. 2006;11:509–22.
Burkle CM, Anderson KA, Xiong Y, Guerra AE, Tschida-Reuter DA. Assessment of the efficiency of language interpreter services in a busy surgical and procedural practice. BMC Health Serv Res. 2017;17:456.
Silva MD, Genoff M, Zaballa A, Jewell S, Stabler S, Gany FM, et al. Interpreting at the End of Life: A Systematic Review of the Impact of Interpreters on the Delivery of Palliative Care Services to Cancer Patients With Limited English Proficiency. J Pain Symptom Manage. 2016;51:569–80.
Guidance And Standards On Language Access Services: Medicare Providers [Internet]. Off. Insp. Gen. Gov. Overs. US Dep. Health Hum. Serv. 2010 [cited 2025 Mar 14]. Available from https://oig.hhs.gov/reports/all/2010/guidance-and-standards-on-language-access-services-medicare-providers/
Toraih EA, Hussein MH, Malik MS, Malik AN, Kandil E, Fawzy MS. Unraveling the link between language barriers and cancer risk. Cancer Causes Control [Internet]. 2024 [cited 2025 Mar 14]; Available from: https://doi.org/10.1007/s10552-024-01946-5
Calvillo-Ortiz R, Polanco-Santana JC, Castillo-Angeles M, Allar BG, Anguiano-Landa L, Ghaffarpasand E, et al. Language Proficiency and Survival in Pancreatic Cancer: a Propensity Score–Matched Analysis. J Gastrointest Surg. 2022;26:94–103.
Duraiswamy S, Rubin SJ, Kim Y, Mur T, Edwards HA. Limited English proficiency and head and neck cancer outcomes. Am J Otolaryngol. 2022;43:103470.
Balazy KE, Benitez CM, Gutkin PM, Jacobson CE, von Eyben R, Horst KC. Association between primary language, a lack of mammographic screening, and later stage breast cancer presentation. Cancer. 2019;125:2057–65.
Oliveira K, Clark S, Dunn E, Mangram A. Spanish As a Primary Language and Its Effect on Breast Cancer Presentation. J Oncol Pract. 2011;7:165–7.
Mojica CM, Glenn BA, Chang C, Bastani R. The Relationship between Neighborhood Immigrant Composition, Limited English Proficiency, and Late-Stage Colorectal Cancer Diagnosis in California. BioMed Res Int. 2015;2015:460181.
Spiegel D, Willcox J, Modest AM, Bhargava N, Recht A. Impact of Limited English Proficiency on Breast Cancer Outcomes. Int J Radiat Oncol Biol Phys. 2024;120:e67.
Sheni R, Qin J, Viswanathan S, Castellucci E, Kalnicki S, Mehta V. Predictive Factors for Cancer Treatment Delay in a Racially Diverse and Socioeconomically Disadvantaged Urban Population. JCO Oncol Pract. 2023;19:e904–15.
Chen AM, Harris JP, Tjoa T, Haidar Y, Armstrong WB. Racial disparities in the timely receipt of adjuvant radiotherapy for head and neck cancer. Oral Oncol. 2023;147:106611.
Koerner SA, Arber S. Overcoming barriers to radiotherapy in at-risk urban populations: primary language as a driver of initiation disparity. J Radiat Oncol. 2018;7:91–6.
Polednak AP. Identifying newly diagnosed Hispanic cancer patients who use a physician with a Spanish-language practice, for studies of quality of cancer treatment. Cancer Detect Prev. 2007;31:185–90.
Williams KM, Dougherty D, Plagens C, Shah NR, Tubbs D, Ehrlich PF. Limited English Proficiency can Negatively Impact Disease/Treatment in Children With Cancer Compared to Those Who are English Proficient-an Institutional Study. J Pediatr Surg. 2024;59:800–3.
Diamond L, Gany F, Pottinger TD, Samedy P, Dong A, Martin S, et al. Influence of language barriers on hospital readmissions in cancer patients. J Clin Oncol. 2015;33:e17583–e17583.
Williams C, Chong G, Tacey M, Barnett F, Mooi J, Jalali A, et al. Addressing disparities in health outcomes for patients with advanced pancreatic cancer and limited English proficiency. Asia Pac J Clin Oncol. 2024;20:531–6.
John-Baptiste A, Naglie G, Tomlinson G, Alibhai SMH, Etchells E, Cheung A, et al. The effect of English language proficiency on length of stay and in-hospital mortality. J Gen Intern Med. 2004;19:221–8.
Witt EE, Eruchalu CN, Dey T, Bates DW, Goodwin CR, Ortega G. The role of patient primary language in access to brain tumor resection: Evaluating emergent admission and hospital volume. J Cancer Policy. 2021;30:100306.
Feeney T, Cassidy M, Tripodis Y, McAneny D, Kavanah M, Sachs T, et al. Association of Primary Language with Outcomes After Operations Typically Performed to Treat Cancer: Analysis of a Statewide Database. Ann Surg Oncol. 2019;26:2684–93.
Manuel SP, Chia ZK, Raygor KP, Fernández A. Association of Language Barriers With Process Outcomes After Craniotomy for Brain Tumor. Neurosurgery. 2022;91:590.
Laronne A, Granek L, Wiener L, Feder-Bubis P, Golan H. “Some things are even worse than telling a child he is going to die”: Pediatric oncology healthcare professionals perspectives on communicating with children about cancer and end of life. Pediatr Blood Cancer. 2022;69:e29533.
Qureshi MM, Romesser PB, Jalisi S, Zaner KS, Cooley TP, Grillone G, et al. The influence of limited English proficiency on outcome in patients treated with radiotherapy for head and neck cancer. Patient Educ Couns. 2014;97:276–82.
Cohen AL, Rivara F, Marcuse EK, McPhillips H, Davis R. Are language barriers associated with serious medical events in hospitalized pediatric patients?. Pediatrics. 2005;116:575–9.
Witt EE, Eruchalu CN, Dey T, Bates DW, Goodwin CR, Ortega G. Non-English Primary Language Is Associated with Short-Term Outcomes After Supratentorial Tumor Resection. World Neurosurg. 2021;155:e484–502.
Bonilla J, Escalera C, Santoyo-Olsson J, Samayoa C, Ortiz C, Stewart AL, et al. The importance of patient engagement to quality of breast cancer care and health-related quality of life: a cross-sectional study among Latina breast cancer survivors in rural and urban communities. BMC Womens Health. 2021;21:59.
Yi JK, Swartz MD, Reyes-Gibby CC. English Proficiency, Symptoms, and Quality of Life in Vietnamese- and Chinese-American Breast Cancer Survivors. J Pain Symptom Manage. 2011;42:83–92.
Acosta E, Agbayani C-JG, Jenkins BN, Cortes HG, Kain ZN, Fortier MA. The Impact of Primary Language Spoken on the Pain Experience of Children With Cancer. J Pediatr Hematol Oncol. 2022;44:135–41.
Leung B, Wong SK, Ho C. End-of-Life Health Resource Utilization for Limited English-Proficient Patients With Advanced Non–Small-Cell Lung Cancer. JCO Oncol Pract. 2022;18:e1716–24.
Brock KE, Steineck A, Twist CJ. Trends in End-of-Life Care in Pediatric Hematology, Oncology, and Stem Cell Transplant Patients. Pediatr Blood Cancer. 2016;63:516–22.
Jaramillo S, Hui D. End-of-Life Care for Undocumented Immigrants With Advanced Cancer: Documenting the Undocumented. J Pain Symptom Manage. 2016;51:784–8.
Thienprayoon R, Marks E, Funes M, Martinez-Puente LM, Winick N, Lee SC. Perceptions of the Pediatric Hospice Experience among English- and Spanish-Speaking Families. J Palliat Med. 2016;19:30–41.
Parikh DA, Chudasama R, Agarwal A, Rand A, Qureshi MM, Ngo T, et al. Race/Ethnicity, Primary Language, and Income Are Not Demographic Drivers of Mortality in Breast Cancer Patients at a Diverse Safety Net Academic Medical Center. Int J Breast Cancer. 2015;2015:835074.
Sridhar P, Misir P, Kwak H, deGeus SW, Drake FT, Cassidy MR, et al. Impact of Race, Insurance Status, and Primary Language on Presentation, Treatment, and Outcomes of Patients with Pancreatic Adenocarcinoma at a Safety-Net Hospital. J Am Coll Surg. 2019;229:389.
Rand AE, Agarwal A, Ahuja D, Ngo T, Qureshi MM, Gupta A, et al. Patient Demographic Characteristics and Disease Stage as Drivers of Disparities in Mortality in Prostate Cancer Patients Who Receive Care at a Safety Net Academic Medical Center. Clin Genitourin Cancer. 2014;12:455–60.
Feeney T, Park C, Godley F, Cassidy M, Sachs T, McAneny D, et al. Provider–patient Language Discordance and Cancer Operations: Outcomes from a Single Center Linked to a State Vital Statistics Registry. World J Surg. 2020;44:1.
Bruce KH, Schwei RJ, Park LS, Jacobs EA. Barriers and facilitators to preventive cancer screening in Limited English Proficient (LEP) patients: Physicians’ perspectives. Commun Med. 2014;11:235–47.
Lee HY, Luo Y, Neese J, Daniel C, Hahm HC. The Role of English Proficiency in HPV and HPV Vaccine Awareness: A Cross-Sectional Study Across Race/Ethnicity. Asian Pac J Cancer Prev APJCP. 2021;22:349–57.
Roy M, Purington N, Liu M, Blayney DW, Kurian AW, Schapira L. Limited English Proficiency and Disparities in Health Care Engagement Among Patients With Breast Cancer. JCO Oncol Pract. 2021;17:e1837–45.
Baars JE, van Dulmen AM, Velthuizen ME, van Riel E, Ausems MGEM. Breast cancer genetic counseling among Dutch patients from Turkish and Moroccan descent: participation determinants and perspectives of patients and healthcare professionals. J Community Genet. 2017;8:97–108.
Van Manh AL, Blondeau-Lecomte E, Makoni N, Jandorf L, Perumalswami P. Identifying Factors Associated with Cancer Screening in Immigrant Populations Living in New York City. J Community Health. 2020;45:1027–9.
Xie Z, Chen G, Suk R, Dixon B, Jo A, Hong Y-R. Limited English Proficiency and Screening for Cervical, Breast, and Colorectal Cancers among Asian American Adults. J Racial Ethn Health Disparities. 2023;10:977–85.
Ridgeway JL, Njeru JW, Breitkopf CR, Mohamed AA, Quirindongo-Cedeño O, Sia IG, et al. Closing the Gap: Participatory Formative Evaluation to Reduce Cancer Screening Disparities among Patients with Limited English Proficiency. J Cancer Educ. 2021;36:795–803.
Cataneo JL, Meidl H, Ore AS, Raicu A, Schwarzova K, Cruz CG. The Impact of Limited Language Proficiency in Screening for Breast Cancer. Clin Breast Cancer. 2023;23:181–8.
Haas JS, Vogeli C, Yu L, Atlas SJ, Skinner CS, Harris KA, et al. Patient, provider, and clinic factors associated with the use of cervical cancer screening. Prev Med Rep. 2021;23:101468.
Hill JC, Njeru JW, Wieland ML, Rutten LJ, Jacobson DJ, Jenkins GD, et al. Disparities Among Limited English Proficient Patients in Colon Cancer Screening with Multi-target DNA Stool Test. J Immigr Minor Health. 2022;24:556–9.
Bayly JE, Trivedi S, Mukamal KJ, Davis RB, Schonberg MA. Limited English proficiency and reported receipt of colorectal cancer screening among adults 45–75 in 2019 and 2021. Prev Med Rep. 2024;39:102638.
Stone BV, Labban M, Beatrici E, Filipas DK, Frego N, Qian Z. Jason), et al. The effect of limited english proficiency on prostate-specific antigen screening in American men. World J Urol. 2024;42:54.
Lung Cancer Screening Completion Rates Demonstrate Disparity Between Patient Populations | A21. HEALTH SERVICES RESEARCH: HIGHLIGHTS OF EPIDEMIOLOGY, POPULATION HEALTH, COST, AND OUTCOMES. Am Thorac Soc Int Conf Meet Abstr Am Thorac Soc Int Conf Meet Abstr [Internet]. [cited 2025 Mar 14]Available from https://www.atsjournals.org/doi/abs/10.1164/ajrccm-conference.2024.209.1_MeetingAbstracts.A1091
Disparities in Clinical Research and Cancer Treatment - CDPR24 [Internet]. Cancer Prog. Rep. [cited 2025 Mar 14]. Available from: https://cancerprogressreport.aacr.org/disparities/cdpr24-contents/cdpr24-disparities-in-clinical-research-and-cancer-treatment/
Jorge S, Masshoor S, Gray HJ, Swisher EM, Doll KM. Participation of Patients With Limited English Proficiency in Gynecologic Oncology Clinical Trials. 2023 [cited 2025 Mar 14]; Available from: https://jnccn.org/view/journals/jnccn/21/1/article-p27.xml
Muthukumar AV, Morrell W, Bierer BE. Evaluating the frequency of English language requirements in clinical trial eligibility criteria: A systematic analysis using ClinicalTrials.gov. PLOS Med. 2021;18:e1003758.
Frayne SM, Burns RB, Hardt EJ, Rosen AK, Moskowitz MA. The exclusion of non-English-speaking persons from research. J Gen Intern Med. 1996;11:39–43.
Velez MA, Glenn BA, Garcia-Jimenez M, Cummings AL, Lisberg A, Nañez A, et al. Consent document translation expense hinders inclusive clinical trial enrolment. Nature. 2023;620:855–62.
Guo XM, Neuman MK, Vallejo A, Matsuo K, Roman LD. An absence of translated consent forms limits oncologic clinical trial enrollment for limited English proficiency participants. Gynecol Oncol. 2024;180:86–90.
Nguyen TT, Somkin CP, Ma Y. Participation of Asian-American Women in Cancer Chemoprevention Research. Cancer. 2005;104:3006–14.
Aristizabal P, Nataraj S, Ma AK, Kumar NV, Perdomo BP, Martinez ME, et al. Social Determinants of Health and Informed Consent Comprehension for Pediatric Cancer Clinical Trials. JAMA Netw Open. 2023;6:e2346858.
Giarelli E, Bruner DW, Nguyen E, Basham S, Marathe P, Dao D, et al. Research participation among Asian American women at risk for cervical cancer: exploratory pilot of barriers and enhancers. J Immigr Minor Health. 2011;13:1055–68.
Youdelman M. Summary of State Law Requirements Addressing Language Needs in Health Care [Internet]. Natl. Health Law Program. 2019 [cited 2025 Mar 13]. Available from: https://nhelprestordev.wpenginepowered.com/resource/summary-of-state-law-requirements-addressing-language-needs-in-health-care-2/
Seible DM, Kundu S, Azuara A, Cherry DR, Arias S, Nalawade VV, et al. The Influence of Patient-Provider Language Concordance in Cancer Care: Results of the Hispanic Outcomes by Language Approach (HOLA) Randomized Trial. Int J Radiat Oncol Biol Phys. 2021;111:856–64.
Bregio C, Finik J, Baird M, Ortega P, Roter D, Karliner L, et al. Exploring the Impact of Language Concordance on Cancer Communication. JCO Oncol Pract. 2022;18:e1885–98.
Balderas-Medina Anaya Y, Hsu P, Martínez LE, Hernandez S, Hayes-Bautista DE. Latina Women in the U.S. Physician Workforce: Opportunities in the Pursuit of Health Equity. Acad Med. J Assoc Am Med Coll. 2022;97:398–405.
Fischer SM, Kline DM, Min S-J, Okuyama S, Fink RM. Apoyo con Cariño: Strategies to Promote Recruiting, Enrolling, and Retaining Latinos in a Cancer Clinical Trial. J Natl Compr Canc Netw. 2017;15:1392–9.
Genoff MC, Zaballa A, Gany F, Gonzalez J, Ramirez J, Jewell ST, et al. Navigating Language Barriers: A Systematic Review of Patient Navigators’ Impact on Cancer Screening for Limited English Proficient Patients. J Gen Intern Med. 2016;31:426–34.
Charlot M, Santana MC, Chen CA, Bak S, Heeren TC, Battaglia TA, et al. Impact of patient and navigator race and language concordance on care after cancer screening abnormalities. Cancer. 2015;121:1477–83.
Percac-Lima S, Ashburner JM, Bond B, Oo SA, Atlas SJ. Decreasing Disparities in Breast Cancer Screening in Refugee Women Using Culturally Tailored Patient Navigation. J Gen Intern Med. 2013;28:1463–8.
O’Brien MJ, Halbert CH, Bixby R, Pimentel S, Shea JA. Community Health Worker Intervention to Decrease Cervical Cancer Disparities in Hispanic Women. J Gen Intern Med. 2010;25:1186–92.
Nuño T, Martinez ME, Harris R, García F. A Promotora-administered group education intervention to promote breast and cervical cancer screening in a rural community along the U.S.-Mexico border: a randomized controlled trial. Cancer Causes Control. CCC. 2011;22:367–74.
Wasserman MR, Bender DE, Lee S-Y, Morrissey JP, Mouw T, Norton EC. Social Support Among Latina Immigrant Women: Bridge Persons as Mediators of Cervical Cancer Screening. J Immigr Minor Health. 2006;8:67–84.
Watson-Johnson LC, Bhagatwala J, Reyes-Garcia C, Hinojosa A, Mason M, Meade CD, et al. Refinement of an Educational Toolkit to Promote Cervical Cancer Screening among Hispanic Immigrant Women in Rural Southern Georgia. J Health Care Poor Underserved. 2012;23:1704–11.
Springer R, Erroba J, O’Malley JP, Huguet N. Differences in up-to-date colorectal and cervical cancer screening rates by ethnicity and preferred language: An analysis across patient-, clinic-, and area-level data sources. SSM - Popul Health. 2024;25:101612.
Fang CY, Ragin CC. Addressing Disparities in Cancer Screening among U.S. Immigrants: Progress and Opportunities. Cancer Prev Res (Phila Pa). 2020;13:253–60.
Jimenez S, Matthews A, Darrah R, Schreiber A, Ricker C, Wolfe Schneider K. Perspectives on Spanish language concordant cancer genetic counseling sessions from the Spanish-speaking population. J Genet Couns. 2023;32:111–27.
Gil S, Hooke MC, Niess D. The Limited English Proficiency Patient Family Advocate Role: Fostering Respectful and Effective Care Across Language and Culture in a Pediatric Oncology Setting. J Pediatr Oncol Nurs. 2016;33:190–8.
MSN GT, Lanza O, Rodriguez FM, Chang A. The Kaiser Permanente Clinician Cultural and Linguistic Assessment Initiative: Research and Development in Patient–Provider Language Concordance. Am J Public Health. 2011;101:205–8.
Roland KB, Milliken EL, Rohan EA, DeGroff A, White S, Melillo S, et al. Use of Community Health Workers and Patient Navigators to Improve Cancer Outcomes Among Patients Served by Federally Qualified Health Centers: A Systematic Literature Review. Health Equity. 2017;1:61–76.
Sharma AE, Lisker S, Fields JD, Aulakh V, Figoni K, Jones ME, et al. Language-Specific Challenges and Solutions for Equitable Telemedicine Implementation in the Primary Care Safety Net During COVID-19. J Gen Intern Med. 2023;38:3123–33.
Karliner LS, Jacobs EA, Chen AH, Mutha S. Do professional interpreters improve clinical care for patients with limited English proficiency? A systematic review of the literature. Health Serv Res. 2007;42:727–54.
Flores G, Abreu M, Barone CP, Bachur R, Lin H. Errors of medical interpretation and their potential clinical consequences: a comparison of professional versus ad hoc versus no interpreters. Ann Emerg Med. 2012;60:545–53.
Ibrahim EM, Al-Saad R, Wishi AL, Khafaga YM, El Hussainy G, Nabhan A, et al. Appraisal of communication skills and patients’ satisfaction in cross-language encounters in oncology practice. J Cancer Educ Off J Am Assoc Cancer Educ. 2002;17:216–21.
Granhagen Jungner J, Tiselius E, Blomgren K, Lützén K, Pergert P. The interpreter’s voice: Carrying the bilingual conversation in interpreter-mediated consultations in pediatric oncology care. Patient Educ Couns. 2019;102:656–62.
Wofford JL, Campos CL, Johnson DA, Brown MT. Providing a Spanish interpreter using low-cost videoconferencing in a community health centre: a pilot study using tablet computers. Inform Prim Care. 2012;20:141–6.
Mottelson IN, Sodemann M, Nielsen DS. Attitudes to and implementation of video interpretation in a Danish hospital: A cross-sectional study. Scand J Public Health. 2018;46:244–51.
Nápoles AM, Santoyo-Olsson J, Karliner LS, O’Brien H, Gregorich SE, Pérez-Stable EJ. Clinician Ratings of Interpreter Mediated Visits in Underserved Primary Care Settings with Ad hoc, In-person Professional, and Video Conferencing Modes. J Health Care Poor Underserved. 2010;21:301–17.
Joseph C, Garruba M, Melder A. Patient satisfaction of telephone or video interpreter services compared with in-person services: a systematic review*. Aust Health Rev. 2017;42:168–77.
Crossman KL, Wiener E, Roosevelt G, Bajaj L, Hampers LC. Interpreters: Telephonic, In-Person Interpretation and Bilingual Providers. Pediatrics. 2010;125:e631–8.
Beach ML, Flood AB, Robinson CM, Cassells AN, Tobin JN, Greene MA, et al. Can language-concordant prevention care managers improve cancer screening rates? Cancer Epidemiol Biomark Prev Publ Am Assoc Cancer Res Cosponsored Am Soc Prev. Oncol. 2007;16:2058–64.
Sanossian N, Rosenberg L, Liebeskind DS, Starkman S, Eckstein M, Stratton S, et al. A Dedicated Spanish Language Line Increases Enrollment of Hispanics Into Prehospital Clinical Research. Stroke. 2017;48:1389–91.
Lee JS, Nápoles A, Mutha S, Pérez-Stable EJ, Gregorich SE, Livaudais-Toman J, et al. Hospital discharge preparedness for patients with limited English proficiency: A mixed methods study of bedside interpreter-phones. Patient Educ Couns. 2018;101:25–32.
Feiring E, Westdahl S. Factors influencing the use of video interpretation compared to in-person interpretation in hospitals: a qualitative study. BMC Health Serv Res. 2020;20:856.
Jacobs B, Ryan AM, Henrichs KS, Weiss BD. Medical Interpreters in Outpatient Practice. Ann Fam Med. 2018;16:70–6.
Jaeger FN, Pellaud N, Laville B, Klauser P. Barriers to and solutions for addressing insufficient professional interpreter use in primary healthcare. BMC Health Serv Res. 2019;19:753.
Gany FM, Gonzalez CJ, Basu G, Hasan A, Mukherjee D, Datta M, et al. Reducing clinical errors in cancer education: interpreter training. J Cancer Educ Off J Am Assoc Cancer Educ. 2010;25:560–4.
Norris WM, Wenrich MD, Nielsen EL, Treece PD, Jackson JC, Curtis JR. Communication about end-of-life care between language-discordant patients and clinicians: insights from medical interpreters. J Palliat Med. 2005;8:1016–24.
Trube CL, Yeo TP. Patients With Limited English Proficiency: A Challenge for Oncology Nursing Providers. Clin J Oncol Nurs. 2023;27:147–53.
Jones J, Rice K, Cueto V, Mojica CDV, Stawitcke M, Salem S, et al. Increasing Health Care Workers’ Proficiency With Using Professional Medical Interpretation: A Workshop. MedEdPORTAL. 16:11017.
Bloom L. Improving Communication for Surgical Patients With Cancer With Limited English Proficiency. Clin J Oncol Nurs. 2023;27:359–63.
Writers Uch. UCHealth launches program to translate prescription medication labels into 26 languages [Internet]. UCHealth Today. 2023 [cited 2025 Mar 13]. Available from: https://www.uchealth.org/today/uchealth-launches-program-to-translate-prescription-medication-labels-into-26-languages/
Bailey SC, Sarkar U, Chen AH, Schillinger D, Wolf MS. Evaluation of Language Concordant, Patient-Centered Drug Label Instructions. J Gen Intern Med. 2012;27:1707–13.
Zargarzadeh AH, Law AV. Access to multilingual prescription labels and verbal translation services in California. Res Soc Adm Pharm. 2011;7:338–46.
Panayiotou A, Gardner A, Williams S, Zucchi E, Mascitti-Meuter M, Goh AM, et al. Language Translation Apps in Health Care Settings: Expert Opinion. JMIR MHealth UHealth. 2019;7:e11316.
Panayiotou A, Hwang K, Williams S, Chong TWH, LoGiudice D, Haralambous B, et al. The perceptions of translation apps for everyday health care in healthcare workers and older people: A multi-method study. J Clin Nurs. 2020;29:3516–26.
Narang B, Park S-Y, Norrmén-Smith IO, Lange M, Ocampo AJ, Gany FM, et al. The Use of a Mobile Application to Increase Access to Interpreters for Cancer Patients With Limited English Proficiency: A Pilot Study. Med Care. 2019;57 Suppl 6 Suppl 2:S184–9.
Tsimicalis A, Le May S, Stinson J, Rennick J, Vachon M-F, Louli J, et al. Linguistic Validation of an Interactive Communication Tool to Help French-Speaking Children Express Their Cancer Symptoms. J Pediatr Oncol Nurs. 2017;34:98–105.
45 CFR 92.201 -- Meaningful access for individuals with limited English proficiency. [Internet]. [cited 2025 Mar 13]. Available from: https://www.ecfr.gov/current/title-45/part-92/section-92.201
Youdelman M. What is required under Title VI and Section 1557 to ensure Language Access for Individuals with Limited English Proficiency? [Internet]. Natl. Health Law Program. 2024 [cited 2025 Mar 13]. Available from: https://healthlaw.org/resource/what-is-required-under-title-vi-and-section-1557-to-ensure-language-access-for-individuals-with-limited-english-proficiency/
Office for Access to Justice | Department of Justice Language Access Plan [Internet]. 2023 [cited 2025 Mar 13]. Available from: https://www.justice.gov/atj/department-justice-language-access-plan
Ramos R, Davis JL, Antolino P, Sanz M, Grant CG, Green BL. Language and communication services: a cancer centre perspective. Divers Equal Health Care. 11:0–0.
Staples JN, Lester J, Li A, Walsh C, Cass I, Karlan BY, et al. Language as a barrier to cancer clinical trial accrual: assessing consenting team knowledge and practices for cancer clinical trial consent among low English fluency patients. Appl Cancer Res. 2018;38:14.
Alhalel J, Francone N, Post S, O’Brian CA, Simon MA. How Should Representation of Subjects With LEP Become More Equitable in Clinical Trials?. AMA J Ethics. 2022;24:319–25.
Commissioner O of the. Informed Consent [Internet]. FDA; 2024 [cited 2025 Mar 13]. Available from: https://www.fda.gov/regulatory-information/search-fda-guidance-documents/informed-consent
Resnik DB, Jones CW. Research subjects with limited English proficiency: ethical and legal issues. Account Res. 2006;13:157–77.
Commissioner O of the. FDASIA Section 907: Inclusion of Demographic Subgroups in Clinical Trials. FDA [Internet]. 2019 [cited 2025 Mar 13]; Available from: https://www.fda.gov/regulatory-information/food-and-drug-administration-safety-and-innovation-act-fdasia/fdasia-section-907-inclusion-demographic-subgroups-clinical-trials
Research C for DE and. Drug Trials Snapshots. FDA [Internet]. 2025 [cited 2025 Mar 13]; Available from: https://www.fda.gov/drugs/drug-approvals-and-databases/drug-trials-snapshots
Coakley M, Fadiran EO, Parrish LJ, Griffith RA, Weiss E, Carter C. Dialogues on diversifying clinical trials: successful strategies for engaging women and minorities in clinical trials. J Womens Health. 2012;21:713–6. 2002.
Improving Patient Safety Systems for Patients With Limited English Proficiency [Internet]. [cited 2025 Mar 13]. Available from: https://www.ahrq.gov/health-literacy/professional-training/lepguide/index.html
Craigle V. MedWatch: The FDA Safety Information and Adverse Event Reporting Program. J Med Libr Assoc. 2007;95:224–5.
Wasserman M, Renfrew MR, Green AR, Lopez L, Tan-McGrory A, Brach C, et al. Identifying and Preventing Medical Errors in Patients With Limited English Proficiency: Key Findings and Tools for the Field. J Healthc Qual Off Publ Natl Assoc Healthc Qual. 2014;36:5–16.
Wallington SF, Luta G, Noone A-M, Caicedo L, Lopez-Class M, Sheppard V, et al. Assessing the awareness of and willingness to participate in cancer clinical trials among immigrant Latinos. J Community Health. 2012;37:335–43.
Garcia Farina E, Rowell J, Revette A, Haakenstad EK, Cleveland JLF, Allende R, et al. Barriers to Electronic Patient-Reported Outcome Measurement Among Patients with Cancer and Limited English Proficiency. JAMA Netw Open. 2022;5:e2223898.
Tofthagen C, Halpenny B, Melendez M, Gonzalez L, Sanchez Varela V, Negrón R, et al. Evaluating the Linguistic Appropriateness and Cultural Sensitivity of a Self-Report System for Spanish-Speaking Patients with Cancer. Nurs Res Pract. 2014;2014:702683.
Zhang Y, Ornelas IJ, Do HH, Magarati M, Jackson JC, Taylor VM. Provider Perspectives on Promoting Cervical Cancer Screening Among Refugee Women. J Community Health. 2017;42:583–90.
Tu S-P, Yip M-P, Chun A, Choe J, Bastani R, Taylor V. Development of Intervention Materials for Individuals With Limited English Proficiency: Lessons Learned From “Colorectal Cancer Screening in Chinese Americans. Med Care. 2008;46:S51.
Reuland DS, Ko LK, Fernandez A, Braswell LC, Pignone M. Testing a Spanish-language colorectal cancer screening decision aid in Latinos with limited English proficiency: Results from a pre-post trial and four month follow-up survey. BMC Med Inform Decis Mak. 2012;12:53.
Gay NA, Da Silva MT, Vega VP, Thomassen A, MacIntyre J, Valls-Delgado G, et al. A multi-level system quality improvement project to reduce disparities in lung cancer screening: The Sylvester Lung Screening Project. J Clin Oncol. 2023;41:6518–6518.
Acknowledgements
None.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
H.S.K. contributed to the literature survey/data collection, interpretation, figure design, manuscript writing/editing, and final proofreading. A.S.U contributed to the figure design. C.I. contributed to the conception, design, and supervision. S.D. contributed to the conception, design, supervision, manuscript editing, and final proofreading. All authors reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
SD received honoraria from Astra Zeneca (advisory and speaking), Johnson and Johnson (advisory and speaking), Lilly (advisory), Boehringer Ingelheim(advisory), Daiichi Sankyo(advisory), Takeda (advisory), Nuvation Bio (advisory), Oncohost (advisory), Caris (advisory), Acrotech (advisory) and Apollomics (advisory). CI received honorarium from Nuvation Bio (advisory).
Ethics approval and consent to participate
Not applicable.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kim, H.S., Irwin, C., Ulag, A.S. et al. Cancer care disparities among patients with limited English proficiency: challenges and strategies for equity. BJC Rep 3, 80 (2025). https://doi.org/10.1038/s44276-025-00187-6
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s44276-025-00187-6