Abstract
Background
There is a lack of representation of most racial and ethnic populations in clinical trials in ophthalmology. In 2017, Roche/Genentech began to introduce a range of initiatives to improve the diversity of trial participants.
Objective
To assess whether company initiatives improved the racial/ethnic representation of participants in Roche/Genentech-sponsored phase 3 trials for the indications of neovascular age-related macular degeneration (nAMD)/geographic atrophy (GA), retinal vein occlusion (RVO), and diabetic retinopathy (DR)/diabetic macular oedema (DMO).
Methods
Proportions for each group were calculated and a Chi-Square test with continuity correction used to determine the statistical significance of difference between pre-2017 (2003–2017) and post-2017 (2018–2021) proportions (based on first-patient-in dates). Analyses were conducted for United States (US) sites only and for all global sites (including US).
Results
The noted significant improvements in enrolment were: in the global population, the proportion of Asians/Native Hawaiians/Pacific Islanders included in the trials for each indication increased significantly from pre-2017 to post-2017 (for nAMD/GA by eight-fold, for RVO by seven-fold, for DR/DMO by two-fold); for nAMD/GA trials, both the US and global populations had a significant (about four-fold) increase in the proportion of Black/African American participants from pre-2017 to post-2017, although the proportion was still very low (0.8%); for RVO trials, the proportion of Hispanic participants increased from pre-2017 to post-2017 both in the US and globally.
Conclusions
Company initiatives have improved the racial/ethnic diversity of participants in Roche/Genentech-sponsored phase 3 trials for ophthalmology. Roche/Genentech will continue efforts to enhance the representation of underserved populations in clinical trials.
Similar content being viewed by others
Introduction
In 2022, the United States Food and Drug Administration (FDA) released their “Diversity Plans” [1], thus highlighting the need to improve racial and ethnic representation in clinical trials. Since 2015, the FDA has released Drug Trials Snapshots (for example [2]) of approved therapies to give clear insight into the patient diversity included in these clinical trials and ensure clinicians can provide the most appropriate treatment option for each individual. In addition, both the FDA [1] and the European Medicines Agency (EMA) [3] have recommended that clinical trials include participants who “closely represent the diverse populations for which the drug is intended.” Achieving diversity and inclusion in clinical trials that match disease prevalence is an important step to (i) ensure applicability of trial results and learnings to the wider population and (ii) confirm safety and efficacy among subgroups, which in turn could improve treatment outcomes for all patients.
The increasing awareness of the lack of representation of most racial and ethnic populations in clinical trials [4] has recently extended to the field of ophthalmology. Berkowitz et al. [5] examined clinical trials for FDA-approved drugs for neovascular age-related macular degeneration (nAMD), open-angle glaucoma, and diabetic retinopathy (DR) from 2000 to 2020 (31 trials, 13 drugs, 18,410 participants) [5]. The study found both (i) that the racial/ethnic distribution was different from that expected based on disease prevalence, with non-White participants under-represented, and (ii) that despite increases in enrolment for some races/ethnicities for some conditions from 2000–2010 to 2010–2020 (for example, Asian participants in nAMD and DR trials, Hispanic participants in nAMD and open-angle glaucoma trials), the authors expected under-representation to worsen based on the trends they observed. In support, Kaakour et al. [6] found a discrepancy between demographic data in diabetic macular oedema (DMO) and retinal vein occlusion (RVO) in United States-based trials run from 2004 to 2020 and the 2010 United States census population [6]. These reports are especially concerning given that Black and Hispanic patients have higher rates of prevalence and severity of diabetes and related DR and DMO compared with White Americans [7,8,9,10,11]. Furthermore, in a meta-analysis of five clinical trials of ranibizumab, Black patients with DMO had a significantly lower improvement in best-corrected visual acuity following 24 months of treatment compared with White patients (although this difference was not seen after propensity matching) [12], suggesting that in addition to greater morbidity, evidence for a treatment response to ranibizumab in Black patients is currently inconclusive.
To address these concerns, Roche/Genentech has prioritised efforts to enrol diverse populations in clinical trials across all therapeutic areas and is committed to advancing inclusive research to recruit more representative populations and address barriers to clinical trial participation. In 2017, several years before the FDA published the “Diversity Plans,” Genentech, Inc. launched the Advancing Inclusive Research Initiative [13], to underscore the importance of greater representation in clinical research. The initiative expanded by establishing an External Council for Advancing Inclusive Research, where experts in the field help devise solutions to overcome barriers and shape inclusive research. In addition, a range of initiatives within the ophthalmology programme have been introduced over time to enhance diversity among trial participants. As presented in Table 1, initiatives included prioritising diversity by redesigning trials to include disease-specific inclusion/exclusion criteria and study design (that might otherwise have directly or indirectly excluded underserved populations), including a focus on patient-reported outcomes, preparing inclusive patient materials to prevent bias, partnering with external patient advocacy groups to reach additional populations, and selecting new principal investigators at new locations and sites with access to different populations, especially under-represented communities. In ophthalmology, efforts have specifically focused on improving representation of underserved populations for diseases in which there is disproportionate representation. However, the impact of these initiatives has not yet been assessed.
Therefore, the objective of this study was to evaluate the racial/ethnic representation of participants in phase 3 clinical trials sponsored by Roche/Genentech from 2003 to 2021 for the indications of nAMD/geographic atrophy (GA), RVO, and DR/DMO. We assessed whether company initiatives introduced in 2017 improved diversity by comparing clinical trial enrolment demographics pre-2017 to post-2017, and we compared recent clinical trial enrolment to disease prevalence.
Methods
The aim of this study was to assess demographic data (self-reported race and ethnicity) of all patients enroled in all Roche/Genentech phase 3 clinical trials for ophthalmology indications and evaluate the impact of company initiatives that began in 2017. All trials from the ophthalmology programme were included in the study. For nAMD/GA (note that GA was included with nAMD because of the Centers for Disease Control and Prevention [CDC] classification of late-stage AMD [14]) – CHROMA and SPECTRI for lampalizumab (GA), MARINA, ANCHOR, PIER, HARBOR, and ARCHWAY (by port delivery system) for ranibizumab (nAMD), and TENAYA and LUCERNE for faricimab (nAMD). For RVO – BRAVO, CRUISE, and SHORE for ranibizumab, and BALATON and COMINO for faricimab. For DR/DMO – RISE, RIDE, PAGODA (by port delivery system), and Pavilion (by port delivery system) for ranibizumab, and YOSEMITE and RHINE for faricimab. Clinicaltrials.gov registration numbers and first-patient-in dates are provided in Supplementary Table 1.
Outcomes
Statistical analyses examined the change in the proportion of each population subgroup from pre-2017 trials to post-2017 trials for race (American Indian, Asian, Black, and White) and ethnicity (Hispanic or non-Hispanic). Classification of a study as pre- or post-2017 was based on first-patient-in date for 2002–2017 and 2018–2021. All patients with non-missing demographic data were included. Analyses were conducted by indication.
Proportions for each group were calculated by dividing a number of patients by the total number of patients enroled in each set of studies. Chi-square tests with continuity correction were used to determine the significance of the difference between the pre-2017 proportions and post-2017 proportions, and 95% confidence intervals were calculated. P values are provided for the differences in outcomes between the two cohorts included in the model (pre-2017 and post-2017); a value of < 0.05 was considered statistically significant. Analyses were conducted for United States sites only and for all global sites (including the United States). Note, for the purpose of this manuscript, the global data include all sites for each trial and do not include all countries/continents of the world.
The disease prevalence for each population subgroup in post-2017 trials was compared with the most recently reported prevalence in the United States by the CDC. For nAMD/GA, prevalence rates were obtained from the CDC Vision and Eye Health Surveillance System (VEHSS) report based on estimates from 2019 [14]. For RVO, prevalence rates were obtained from the CDC VEHSS using 2019 estimates for “other eye disorders,” “other retinal disorders,” “diagnosed by type,” and “diagnosed BRVO or CRVO” [15]. For DR/DMO, prevalence rates were obtained from the CDC VEHSS report based on estimates from 2021 [16].
Results
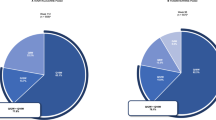
The Roche/Genentech phase 3 ophthalmology clinical trials included first-patient-in dates from 2003 to 2021, with about half occurring after 2017 (Fig. 1A). Most trials included global enrolment sites, although some were based in the United States only (Fig. 1B). All the clinical trials for nAMD/GA, RVO, and DR/DMO included sites in select countries around the world in addition to the United States.
A Timeline of Roche/Genentech ophthalmology clinical trials and B Map of Roche/Genentech ophthalmology clinical trials. DMO diabetic macular oedema, DR diabetic retinopathy, GA geographic atrophy, nAMD neovascular age-related macular degeneration, RVO retinal vascular occlusion.
Race
American Indian/Alaskan Native
The proportions of American Indian/Alaskan Native participants included in Roche/Genentech ophthalmology trials were low and were similar across the indications (Table 2). The proportion of American Indian/Alaskan Native participants included in the trials for each indication did not change from pre-2017 to post-2017.
Asian/Native Hawaiian/Pacific Islander
In the United States, the proportions of Asian/Native Hawaiian/Pacific Islander participants included in the trials for each indication did not change from pre-2017 to post-2017 (Table 2). In contrast, in the global population, the proportions of Asian/Native Hawaiian/Pacific Islander participants included in the trials for each indication increased significantly from pre-2017 to post-2017 (Table 2). For nAMD/GA, the proportion increased by about eight-fold, for RVO by seven-fold, and for DR/DMO by two-fold. Note that because of data coding and patient responses we are unable to separate the Asian, Native Hawaiian, and Pacific Islander groups.
Black/African American
For nAMD/GA trials, both the United States and global populations had a significant (about four-fold) increase in the proportion of Black/African American participants from pre-2017 to post-2017 (Table 2), although the proportion was still very low (0.8%). For both RVO and DR/DMO trials, the proportion of Black/African American participants included in the trials did not change from pre-2017 to post-2017; however, there was a decrease globally (Table 2). For all indications, the proportions of non-Hispanic Black/African American participants included in recent trials appear to be lower than the estimated prevalence in the United States population (Fig. 2).
For nAMD/GA prevalence rates were obtained from the CDC VEHSS report based on estimates from 2019 [14]. For RVO, prevalence rates were obtained from CDC VEHSS using 2019 estimates for “other eye disorders,” “other retinal disorders,” “diagnosed by type,” “diagnosed BRVO or CRVO” [15]. For DR/DMO, prevalence rates were obtained from the CDC VEHSS report based on estimates from 2021 [16]. BRVO branched retinal vascular occlusion, CDC Centers for Disease Control and Prevention, CRVO central retinal vascular occlusion, DMO diabetic macular oedema, DR diabetic retinopathy, GA geographic atrophy, nAMD neovascular age-related macular degeneration, RVO retinal vascular occlusion, VEHSS Vision and Eye Health Surveillance System.
White
For nAMD/GA and RVO trials, the proportion of White participants did not change from pre-2017 to post-2017 in the United States but did decrease globally (Table 2). For DR/DMO trials, the proportion of White participants did not change from pre-2017 to post-2017 either in the United States or globally (Table 2). For all indications, the proportion of non-Hispanic White participants included in recent trials appears to be higher than the estimated prevalence in the United States population (Fig. 2).
Ethnicity
For nAMD/GA trials, the proportion of Hispanic participants did not change from pre-2017 to post-2017 in the United States but did increase in the global population (Table 2). For RVO trials, the proportion of Hispanic participants increased from pre-2017 to post-2017 both in the United States and globally (Table 2). For DR/DMO trials, the proportion of Hispanic participants did not change from pre-2017 to post-2017 in the United States and decreased slightly in the global population (Table 2). For RVO and DR/DMO, the proportion of Hispanic participants included in recent trials appears to be lower than the estimated prevalence in the United States population (Fig. 2).
Discussion
In 2017, Roche/Genentech introduced the company-wide Advancing Inclusive Research Initiative [13], focused on addressing disparities in clinical research, and over time, additional strategies have been implemented within the ongoing ophthalmology clinical development programmes. The findings of this study suggest that the plan is starting to bring about changes in the conduct of clinical trials, although there is more work to be done. We found that in the United States, although the proportions remain low, there were significant increases in the proportion of Black/African American participants enroled in nAMD/GA trials and in the proportion of Hispanic participants enroled in RVO trials from pre-2017 to post-2017, which we hope is the direct result of our efforts. In addition, although the meta-analysis did not identify any significant changes in DMO/DR enrolment, the recent Pavilion trial includes 41% of participants who identify as Hispanic as a result of initiatives such as targeted site selection [17]. We also observed global increases in Asian enrolment because of increased clinical trial locations in the Asia-Pacific region. However, with a trend to concomitant decreases in Black/African American enrolment, we acknowledge that focusing recruitment on one population may impact another. Overall, we showed that White individuals continue to be overrepresented, and all other races/ethnicities are underrepresented compared with estimated prevalence and overall disease burden in the United States, which is in line with a recent analysis of all ophthalmology trials [18], and is a particular issue for Black Americans who continue to be inadequately represented in all clinical trials [19]. Although some of these findings are encouraging, our study confirms that improving clinical trial participation for underserved populations will remain a high priority and urgent goal.
Improving enrolment disparities will be challenging because there are many barriers to participation, especially among underserved populations. A recent comprehensive literature review assessed factors affecting participation in clinical trials in the United States [20]. The barriers to participation (excluding personal interest) included language barriers, perceived risk, trust in the medical community, cultural background, relationship with healthcare providers, lack of education about clinical trials, time commitment, costs, and comorbidities. In addition, a study linked clinical trial site location to driving time and United States census data and found geographic and socio-economic disparities in access to clinical trial sites for rural and non-Northeastern locations and for poorer populations and those with lower education levels [21]. Of note, access to clinical trial sites was also limited for patients with higher levels of self-reported visual impairment, which may be a factor to consider in the future. These barriers are omnipresent for all industry-sponsored clinical trials. A review of clinical trial enrolment by race/ethnicity over a range of clinical trials for other therapies for similar indications (Supplementary Table 2) highlights that the challenges faced by Roche/Genentech are reflected by a similar low representation of underserved populations in trials from other sponsors. Although enroling new sites and increasing the diversity of participants will be complex, Roche/Genentech has plans to overcome barriers and improve equity in clinical trials. Given the challenges of running a global ophthalmology clinical trial, planned and future Roche/Genentech clinical trials are to be focused on expansion of clinical trial sites to include global locations and to recruit suitable patient numbers in each country (to allow subanalyses of data, rather than have country-specific studies) and focused on specific patient populations. The SALWEEN and ELEVATUM studies were initiated to better understand the potential of these initiatives and address inclusion and exclusion criteria that may limit participation (Table 3).
Roche/Genentech initiatives apply to both clinical trials and the broader healthcare community, and match proposals from other stakeholders, including trial sponsors [22,23,24]. One aspect of particular importance is the expansion of trial sites and the addition of new principal investigators (Table 1), especially from under-represented communities, as this enhances the ability to enrol diverse participants. Other considerations include support in multiple languages and differential engagement of caregivers (who may be of different ages, depending on the condition). Interestingly, in a global online survey of all clinical research, Getz et al. [25] found a significant correlation between site personnel diversity and patient enrolment diversity [25]. Furthermore, in a retrospective study of ophthalmic clinical trials, Bains et al. [26] found that concordance between research staff and patients for race and ethnicity was linked to improved enrolment [26]. These studies propose that hiring and supporting investigators and site staff who reflect the patient community may be valuable. Indeed, Woreta et al. [27] have outlined a range of programmes that aim to increase ophthalmology workforce diversity [27]. Roche/Genentech is an invested supporter of this approach with sponsorship and mentoring in the Minority Ophthalmology Mentoring Program run by the American Academy of Ophthalmology and other programmes that are highlighted in Table 3. Another consideration that could improve workplace diversity is investment in and support of residency education programmes [28, 29]. Efforts to improve workforce diversity will also continue to consider the employment of women in key positions.
As a company-wide approach to addressing disparities in clinical research, Roche/Genentech formed an External Council for Advancing Inclusive Research, and the council recently published their recommendations for the future of clinical trials, which address issues at the system level, patient level, and study level [13]. Furthermore, in 2021, the Advancing Inclusive Research Site Alliance was established to enable Roche/Genentech to partner with selected trial sites to identify best practices and address barriers to participation [30]. Within the ophthalmology programme, in 2023, a Diversity & Inclusion Ophthalmology Mini-Council was formed to connect and support cross-functional teams. In line with the FDA “Diversity Plans” recommendations [31], a Diversity Plan will be developed for each clinical trial for each therapy to (i) outline specific strategies to address recruitment barriers and (ii) detail a plan of action to enrol and retain diverse participants who reflect the prevalence of the indication. The plan includes items such as site feasibility and targeted selection, investigator engagement, patient support and engagement, vendor selection, and trial accessibility (also noted in Table 1). For ophthalmology, Diversity Plans have been initiated for vamikibart for uveitic macular oedema (NCT05642312, NCT05642325) and for satralizumab for thyroid eye disease (NCT05987423, NCT06106828), and future studies will assess their benefit. Other outstanding issues to be addressed by Roche/Genentech in the future may include participation of Native American individuals in clinical trials (especially given a high prevalence of DMO [32]), which may require special considerations, for example [33], establishing trust [34]. In addition, infrastructure challenges in some countries may be difficult to overcome (for example, sites in African countries may have limited capacity to support a clinical trial and may lack imaging facilities). The ELEVATUM study is already addressing these issues with current sites engaging both Native American populations and Africans in Kenya.
The main limitation of this study is the accuracy of demographic reporting, especially for the older studies where patients may have been grouped together or had limited options to self-report their race/ethnicity (of note, in line with recent draft FDA guidance [35], Roche/Genentech have updated the electronic Case Report Form to better capture race and to enable reporting of multi-racial patients; Supplementary Table 3). In addition, this was a post hoc retrospective analysis. We were unable to assess the representation of clinical trial principal investigators or primary manuscript authors, which may offer additional insight in the future. Moreover, we did not consider gender diversity in this manuscript, which is another important aspect that, for example, may be addressed through supporting increased training and selection of female principal investigators. Accurate assessment of the prevalence and disease burden of each condition in specific racial/ethnic groups in each country may also help ensure equity, especially as disease characteristics may be affected by the culture, diet, and lifestyle of the country. However, given the use of company-only data over a range of years, indications, and drugs, we believe that the results are as consistent as possible and reflect a comprehensive assessment of our ophthalmology programme. Our findings are also limited because they are not generalizable to other industry-sponsored programmes, which would be impacted by their own diversity initiatives. A future study evaluating changes in enrollment in retinal clinical trials across sponsors may help to better understand disparities.
In conclusion, Roche/Genentech’s efforts to improvethe diversity of clinical trial participants have been progressing since 2017 and reflect a genuine concern for accurate treatment assessment. Our efforts, although promising, highlight that we have more work to do. In the United States, the proportion of Black/African American participants in nAMD trials and the proportion of Hispanic participants in RVO trials increased, but we did not see any changes in DR/DMO trial enrolment in the meta-analysis, and the extent of any changes did not meet the current disease prevalence. However, we did observe global increases in enrolment of Asian participants because of the addition of clinical trial sites in the region. Roche/Genentech will continue efforts to enhance representation of underserved populations in ophthalmology clinical trials, particularly with the novel ELEVATUM trial, and we hope other government agencies and industry sponsors see this study as an example of positive changes in the pharmaceutical industry, as the field pursues equality, optimised treatment outcomes, and (ultimately) personalised healthcare for all.
Data availability
For up to date details on Roche’s Global Policy on the Sharing of Clinical Information and how to request access to related clinical study documents, see here: https://go.roche.com/data_sharing. Anonymised records for individual patients across more than one data source external to Roche cannot, and should not, be linked due to a potential increase in risk of patient re-identification. Requests for the data underlying this publication require a detailed, hypothesis-driven statistical analysis plan that is collaboratively developed by the requestor and company subject matter experts. Direct such requests to Roche for consideration.
References
U.S. Food and Drug Administration. Diversity plans to improve enrollment of participants from underrepresented racial and ethnic populations in clinical trials guidance for industry. 2022. https://www.fda.gov/media/157635/download.
U.S. Food and Drug Administration. Center for Drug Evaluation and Research: drug trials snapshots summary report 2022. 2022. https://www.fda.gov/media/168662/download.
European Medicines Agency. ICH guideline E8 (R1) on general considerations for clinical studies. 2022. https://www.ema.europa.eu/en/documents/scientific-guideline/ich-e-8-general-considerations-clinical-trials-step-5_en.pdf.
Bibbins-Domingo K, Helman A, Dzau VJ. The imperative for diversity and inclusion in clinical trials and health research participation. JAMA. 2022;327:2283–4.
Berkowitz ST, Groth SL, Gangaputra S, Patel S. Racial/ethnic disparities in ophthalmology clinical trials resulting in US Food and Drug Administration drug approvals from 2000 to 2020. JAMA Ophthalmol. 2021;139:629–37.
Kaakour AH, Hua HU, Rachitskaya A. Representation of race and ethnicity in randomized clinical trials of diabetic macular edema and retinal vein occlusion compared to 2010 US census data. JAMA Ophthalmol. 2022;140:1096–102.
Baker RS. Diabetic retinopathy in African Americans: vision impairment, prevalence, incidence, and risk factors. Int Ophthalmol Clin. 2003;43:105–22.
Harris MI, Klein R, Cowie CC, Rowland M, Byrd-Holt DD. Is the risk of diabetic retinopathy greater in non-Hispanic blacks and Mexican Americans than in non-Hispanic whites with type 2 diabetes? A U.S. population study. Diabetes Care. 1998;21:1230–5.
Varma R, Bressler NM, Doan QV, Gleeson M, Danese M, Bower JK, et al. Prevalence of and risk factors for diabetic macular edema in the United States. JAMA Ophthalmol. 2014;132:1334–40.
Malhotra NA, Greenlee TE, Iyer AI, Conti TF, Chen AX, Singh RP. Racial, ethnic, and insurance-based disparities upon initiation of anti-vascular endothelial growth factor therapy for diabetic macular edema in the US. Ophthalmology. 2021;128:1438–47.
Wong TY, Klein R, Islam FM, Cotch MF, Folsom AR, Klein BEK, et al. Diabetic retinopathy in a multi-ethnic cohort in the United States. Am J Ophthalmol. 2006;141:446–55.
Khan MA, Hill L, Stoilov I, Haller JA. Impact of race on vision outcomes in ranibizumab-treated patients with diabetic macular edema. Annual Meeting of the American Academy of Ophthalmology, New Orleans, LA, number 12, 2021.
Garrick O, Mesa R, Ferris A, Kim ES, Mitchell E, Brawley OW, et al. Advancing inclusive research: establishing collaborative strategies to improve diversity in clinical trials. Ethn Dis. 2022;32:61–8.
Centers for Disease Control and Prevention (CDC), Vision and Eye Health Surveillance System (VEHSS). Prevalence of age-related macular degeneration (AMD). 2022. https://www.cdc.gov/visionhealth/vehss/estimates/amd-prevalence.html.
Centers for Disease Control and Prevention (CDC). Vision and Eye Health Surveillance System (VEHSS). 2019. https://www.cdc.gov/visionhealth/vehss/index.html.
Centers for Disease Control and Prevention (CDC), Vision and Eye Health Surveillance System (VEHSS). Prevalence of diabetic retinopathy (DR). 2023. https://www.cdc.gov/visionhealth/vehss/project/case-definitions-data/diabetic-retinopathy-prevalence.html.
ClinicalTrials.gov. A multicenter, randomized study in participants with diabetic retinopathy without center-involved diabetic macular edema to evaluate the efficacy, safety, and pharmacokinetics of ranibizumab delivered via the port delivery system relative to the comparator arm (PAVILION). 2024. https://www.clinicaltrials.gov/study/NCT04503551.
Montazeri F, Wang M, Atkuru A, Estrada MM, Liu YA, Emami-Naeini P. Racial, ethnic, and gender diversity in United States ophthalmology clinical trials. Ophthalmol Sci. 2023;4:100402.
Green AK, Trivedi N, Hsu JJ, Yu NL, Bach PB, Chimonas S. Despite the FDA’s five-year plan, black patients remain inadequately represented in clinical trials for drugs. Health Aff. 2022;41:368–74.
Allison K, Patel D, Kaur R. Assessing multiple factors affecting minority participation in clinical trials: development of the clinical trials participation barriers survey. Cureus. 2022;14:e24424.
Soares RR, Huang C, Sharpe J, Cobbs L, Gopal A, Rao W, et al. Geographic and socioeconomic access disparities to phase 3 clinical trials in ophthalmology in the United States. Eye. 2023;37:1822–8.
Corneli A, Hanlen-Rosado E, McKenna K, Araojo R, Corbett D, Vasisht K, et al. Enhancing diversity and inclusion in clinical trials. Clin Pharmacol Ther. 2023;113:489–99.
Kelsey MD, Patrick-Lake B, Abdulai R, Broedl UC, Brown A, Cohn E, et al. Inclusion and diversity in clinical trials: actionable steps to drive lasting change. Contemp Clin Trials. 2022;116:106740.
Versavel S, Subasinghe A, Johnson K, Golonski N, Muhlhausen J, Perry P, et al. Diversity, equity, and inclusion in clinical trials: a practical guide from the perspective of a trial sponsor. Contemp Clin Trials. 2023;126:107092.
Getz K, Florez M, Botto E, Ribeiro K, Goller G, Robinson L, et al. Global investigative site personnel diversity and its relationship with study participant diversity. Ther Innov Regul Sci. 2022;56:777–84.
Bains A, Osathanugrah P, Sanjiv N, Chui C, Fiorello MG, Siegel NH, et al. Diverse research teams and underrepresented groups in clinical studies. JAMA Ophthalmol. 2023;141:1037–44.
Woreta FA, Gordon LK, Knight OJ, Randolph JD, Zebardast N, Pérez-González CE. Enhancing diversity in the ophthalmology workforce. Ophthalmology. 2022;129:e127–36.
Ledesma Vicioso N, Woreta F, Sun G. Presence of diversity or inclusion information on US ophthalmology residency program websites. JAMA Ophthalmol. 2022;140:606–9.
Lee EY, Farrokhyar F, Bakshi N, Levin LA, Ahuja N. Equity, diversity, and inclusion landscape in Canadian postgraduate medical education for ophthalmology. Can J Ophthalmol. 2024;59:31–9.
Vidal GA, Chalela P, Curry AN, El-Rayes B, Halmos B, Herrera AF, et al. Advancing Inclusive Research (AIR) Site Alliance: facilitating the inclusion of historically underrepresented people in oncology and ophthalmology clinical research. Contemp Clin Trials. 2024;137:107416.
Genentech, Inc. Our commitment to diversity and inclusion. 2022. https://www.gene.com/stories/our-commitment-to-diversity-inclusion.
Lundeen EA, Andes LJ, Rein DB, Wittenborn JS, Erdem E, Gu Q, et al. Trends in prevalence and treatment of diabetic macular edema and vision-threatening diabetic retinopathy among Medicare Part B fee-for-service beneficiaries. JAMA Ophthalmol. 2022;140:345–53.
Urban Indian Health Institute. Clinical trial participation guide for American Indians and Alaska Natives: partner toolkit. 2023. https://www.uihi.org/resources/clinical-trial-toolkit/.
Mainous AG 3rd, Kelliher A, Warne D. Recruiting indigenous patients into clinical trials: a circle of trust. Ann Fam Med. 2023;21:54–6.
U.S. Department of Health and Human Services, U.S. Food and Drug Administration. Collection of race and ethnicity data in clinical trials and clinical studies for FDA-regulated medical products: guidance for industry. 2024. https://www.fda.gov/media/175746/download.
Acknowledgements
The authors thank Daniela Ferrara, Jacqueline Travaso, Manuel Amador, Veronica Sandoval, Jacqueline Ackerman, Ashley Iyer, DeAnna Kovach, and Shirley Dang, all from Genentech, Inc., for their valuable contributions to the study and the manuscript.
Funding
The trials included in this analysis were funded by Genentech, Inc. and/or F. Hoffmann-La Roche Ltd. (Basel, Switzerland). Medical writing assistance was provided by Janelle Keys, PhD, of Envision Pharma Group, and funded by Genentech, Inc. Envision’s services complied with international guidelines for Good Publication Practice. Roche/Genentech was involved in designing the analysis, conducting the analysis, and preparation and review of the manuscript.
Author information
Authors and Affiliations
Contributions
AC, AJP, and SB designed the analysis and prepared the data. SB conducted the statistical analysis. All authors provided critical review of manuscript drafts and approved the final draft.
Corresponding author
Ethics declarations
Competing interests
AWS reports research support from Roche/Genentech, consulting for Apellis, Astellas, EyePoint, Iveric Bio, Regeneron, Roche/Genentech, and honoraria from Allergan AbbVie and DORC. JB reports research support from Allergan AbbVie, Apellis, Astellas, Character Biosciences, Iveric Bio, Outlook Therapeutics, Roche/Genentech, consulting for Roche/Genentech, and speaker bureaus for Apellis, Astellas, Iveric Bio, and Roche/Genentech. AJP, OOI, SB, CQR, AM, and CB are employees of, and may be stockholders in, Genentech, Inc.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Scott, A.W., Brown, J., Prager, A.J. et al. Racial and ethnic diversity in ophthalmology: a meta-analysis of industry-sponsored phase 3 clinical trials from a single company. Eye Open 1, 3 (2025). https://doi.org/10.1038/s44440-025-00002-8
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s44440-025-00002-8