Abstract
Hospitals, traditionally classified within the tertiary sector due to their service-oriented nature, nevertheless exhibit energy demands and technical characteristics akin to those of industrial facilities. Motivated by this, this paper redefines hospital energy demand by emphasizing shared energy forms and consumption processes between healthcare and industry. Methodologically, the study conducts a comparative analysis of energy intensity across regions, highlights process-level similarities and regulatory disparities, proposes a hybrid regulatory framework tailored to healthcare buildings, and reviews the literature on Distributed Energy Systems (DES) in hospitals. To complement these analyses with quantitative evidence, a dynamic TRNSYS 18 mini-scenario is introduced for a representative block of Specialities Operating Theatres (OTs). The simulation provides hourly cooling and electrical loads and yields an annual combined electricity intensity of approximately 780 \(\text{kWh}\cdot\)m\(\vphantom{0}^{-2}\cdot\)yr\(\vphantom{0}^{-1}\), a value that exceeds legacy, medium-size, and even hyperscale data-centre benchmarks. This empirical result supports the claim that critical hospital zones behave energetically as clean-process environments, closer to industrial or infrastructural uses than to conventional tertiary spaces. The findings show that hospitals consume energy at levels closer to industry than to commercial buildings, with critical continuous loads. The industrial sector has already demonstrated rigorous adoption of DES, setting a precedent for their integration in healthcare. Despite progress, the literature lacks comprehensive and region-specific reviews on integrating DES in healthcare, including cogeneration (CHP), trigeneration (CCHP), solar energy systems, and medical waste-to-energy (WtE) recovery. Fully integrated solar–CCHP–WtE systems, in particular, remain underexplored. A novel contribution of this work lies in formulating a hybrid regulatory framework that redefines hospitals as industrial-scale energy hubs, bridging the gap between rigorous industrial DES practices and the specialized operational requirements of the healthcare sector. Overall, the integration of DES presents hospitals with significant opportunities to enhance energy efficiency, improve system reliability, and achieve substantial environmental benefits, all while maintaining the stringent quality standards required in healthcare environments.
Similar content being viewed by others
Introduction
The classification of economic activities into primary, secondary, and tertiary sectors is a globally recognized framework that facilitates the analysis of economic development and resource distribution1,2. The primary sector involves the extraction and harvesting of natural resources (e.g., agriculture, forestry, fishing, and mining). The secondary sector encompasses manufacturing, construction, and industries that process raw materials into finished goods. The tertiary sector comprises service-oriented activities, including healthcare, education, retail, and government services. Hospitals, as an integral part of the healthcare system, fall under the tertiary sector, illustrating their critical role in providing essential services.
In energy-specific contexts, sectors are classified based on end-use consumption patterns. The residential sector addresses household energy consumption, focusing on energy efficiency in appliances and building standards3,4. The commercial sector, including hospitals, hotels, and retail establishments, emphasizes policies targeting energy-efficient heating, ventilation, and air conditioning (HVAC) systems, lighting, and demand management5. The industrial sector is divided into Energy-Intensive (EI) and Non-Energy-Intensive (NEI) industries. EI industries, such as steel, cement, and chemical manufacturing, demand substantial energy inputs and focus on improving process efficiency, reducing emissions, and implementing waste-to-energy solutions. In contrast, NEI industries, like the food industry, demonstrate lower energy dependency but still contribute significantly to overall energy consumption through specific processes such as refrigeration and drying6. These observations underscore the potential for energy efficiency and carbon reduction in non-energy-intensive sectors as well.
The transportation sector involves initiatives for fuel efficiency, electric vehicles, and energy use in public transportation systems. The public sector includes government and public facilities, often targeted by renewable energy mandates and procurement policies. Finally, the energy sector—encompassing power generation, transmission, and distribution—is regulated with a focus on grid management and renewable energy integration7.
Given the unique energy demands of healthcare buildings, which, while generally categorized within the tertiary sector due to their service-oriented function, share more in common with industrial facilities in terms of energy requirements and technical complexity, the conventional classification can be misleading. Hospital infrastructure operates under unique intensity and complexity8. These facilities house a range of technical equipment and energy-intensive systems—such as large-scale boilers, medical gas systems (including compressed air, vacuum systems, nitrous oxide, and oxygen generators), advanced HVAC systems, heat pumps, incinerators, and sometimes multigeneration systems—that support essential hospital functions and ensure a continuous, reliable energy supply critical for patient care9.
In terms of energy consumption, hospitals resemble industrial sites because of their energy-intensive systems and critical operational needs. While residential, office, and commercial buildings significantly contribute to energy consumption and carbon emissions globally, the manufacturing industry remains one of the largest energy consumers and carbon emitters8. Energy efficiency has thus become a critical driver for progress and innovation within the industrial sector10. Although the industrial sector has seen some reductions in final energy consumption (FEC), the tertiary sector has experienced a notable increase—primarily driven by a rising demand for electricity, particularly in sectors reliant on advanced information and communication technologies11. Notably, the industrial sector continues to rely on fossil-based systems9. Recent estimates indicate that fossil fuels accounted for 61% of global electricity production in 2023, though this share is projected to decline to 54% by 2026 as clean energy sources expand their contributions12.
Considering hospitals’ simultaneous needs for cooling, heating, and electricity, and the impact of events such as the COVID-19 pandemic, these facilities have faced a significant increase in energy demands13. The surge in energy consumption—driven by enhanced medical technologies, stricter infection control protocols14, and evolving hospital architectures15—highlights the need for more resilient and sustainable energy systems. Reliable, cost-effective solutions, such as Distributed Energy Systems (DES), are therefore critical to ensure that hospitals can meet these increased energy needs while preparing for future crises16. DES not only mitigates climate change by increasing the share of renewable energy in the mix but also enhances overall energy efficiency through the adoption of more efficient technologies.
A comprehensive review by Zhu17 highlights the benefits of DES, including greater renewable energy use, cost reductions, lowered environmental impact, enhanced energy security, flexibility, and support for smart city development. Polygeneration or multigeneration systems, especially when integrated close to end users and combined with renewable energy sources, represent sustainable DES options. Kasaeian18 demonstrated that optimally designed polygeneration systems outperform traditional energy production in terms of energy, economic, and environmental benefits. Similarly, Alibakhsh’s review18 confirms that solar-integrated polygeneration systems are among the most promising sustainable options. Many DES solutions incorporate renewable sources—such as wind and solar—to produce diverse outputs (thermal energy, cooling, steam, and electricity). Additionally, studies have explored energy recovery from medical waste incineration, drawing inspiration from industrial practices to minimize energy loss. For example, Bujak’s work19 on a hospital complex demonstrated that a medical waste incineration system with heat recovery can reduce environmental impact and improve total energy efficiency to 73%, with positive economic implications.
Table 1 provides the classification of different economic sectors and their associated energy consumption intensities across various energy sectors, as described above, demonstrating the relationship between energy-specific sectors and economic sectors. The color shading represents the intensity of energy consumption, with darker shades indicating higher energy consumption and lighter shades reflecting lower consumption. Economic sectors such as primary (agriculture, mining), secondary (manufacturing, industrial), and tertiary (healthcare, residential, commercial) are classified based on their energy usage levels. The “yes” and “no” labels in the table indicate whether a specific economic sector is relevant to or significantly impacted by a particular energy sector. For instance, a “yes” means that the sector is actively engaged with or heavily reliant on that energy source, whereas “no” indicates minimal or no involvement. This classification helps identify areas with significant energy demands and opportunities for energy efficiency interventions. Although healthcare buildings are traditionally categorized as “low energy consumption” in the tertiary sector, this paper argues that, due to the complex operations and high-energy demands of healthcare facilities, they should be regarded with industry-like energy considerations. This reevaluation emphasizes the need for more accurate energy efficiency measures and for integrating healthcare buildings into energy systems typically designed for industrial sectors.
The purpose of this work is to advocate for reclassifying hospitals’ energy demands by viewing them from an industrial perspective while maintaining strict standards for indoor environmental conditions, thereby enabling policymakers and facility managers to benefit from this approach. The methodological pathway undertaken in this paper supports a reconsideration of the current classification of hospitals within the tertiary sector and draws inspiration from successful strategies implemented in the industrial sector, particularly given their industrial-like energy demands.
The approach begins with a comparative analysis of energy intensity in the healthcare and industrial sectors across various regions, emphasizing shared energy forms and consumption processes. It then highlights the significant disparity in the rigor of the regulatory frameworks governing the industrial and healthcare sectors. Building on this, the paper proposes a hybrid regulatory framework tailored to the unique requirements of healthcare buildings to address this gap. It further translates insights from the industrial sector’s rigorous adoption of Distributed Energy Systems (DES) to promote broader implementation in healthcare settings, thereby enhancing hospital energy efficiency and contributing to decarbonization efforts. Finally, the paper identifies and discusses challenges specific to the healthcare sector in implementing this hybrid framework. To complement these analyses with quantitative evidence, a dynamic TRNSYS 18 mini-scenario is introduced to illustrate the process-like energy behaviour of Specialities Operating Theatres (OTs) under real operating conditions.
Main contributions
-
A reframing that views hospitals as industrial-like energy users—not routine tertiary-service buildings—supported by comparative analyses of energy intensity, shared energy forms, and process-level consumption across healthcare and industry.
-
A hybrid regulatory framework tailored to healthcare buildings that bridges the rigor of industrial practice with hospital operational constraints.
-
Translation of lessons from industry’s adoption of Distributed Energy Systems (DES) to promote broader implementation in healthcare, with implications for energy efficiency and decarbonization.
-
An illustrative dynamic mini-scenario (TRNSYS 18) for a representative block of Specialities Operating Theatres (OTs), providing quantitative evidence of process-like energy behaviour through hourly cooling and electrical loads.
These contributions are intended to capture the attention of decision-makers, policy makers, and managers in both the healthcare sector and energy government.
Paper structure Introduction sets the context, motivates the sector reclassification, and presents the sector mapping. Results then report the outputs of the analytical workflow (Fig. 1)—namely the cross-region energy-intensity comparison for healthcare versus industry, the process-level comparison across key end-uses common to both sectors, the dynamic OT mini-scenario for quantitative validation, the regulatory contrast, and evidence on DES adoption in industry and hospitals. Discussion synthesizes those findings, proposes the hybrid regulatory framework, and examines sector-specific challenges, limitations, and research gaps. Methods documents the datasets, inclusion criteria, harmonization choices, unit conventions, and procedures underlying the Results, and notes any coverage limitations; representative formulas and worked conversions are provided in the Supplementary Information.
Comparative assessment of energy demand in healthcare and industry
Approaching energy intensity in healthcare and industrial sectors beyond regional contexts
As summarized in Table 2, the energy intensity of healthcare and industrial sectors is examined across different economies (U.S. and EU27). For other economies, particularly in the Global South, data limitations prevent a direct comparison. While a similar analysis was intended, challenges such as inconsistent reporting, limited access to detailed energy data, and disparities in healthcare infrastructure and energy supply hinder a comprehensive assessment. The table highlights significant variations and benchmarks. Based on the available data, the verification process has been conducted for the U.S. and Europe, where healthcare facilities demonstrate higher energy intensity compared to the tertiary sector. Large hospitals and inpatient healthcare facilities in the U.S. exhibit energy use exceeding 600–700 kWh/m2, surpassing the typical range observed in commercial and tertiary buildings. In Europe, hospitals also exceed the energy intensity of the tertiary sector, though at lower absolute levels (approximately 320 kWh/m2). Moreover, specific ratios—such as energy consumption per hospital bed (approximately 85,455 kWh/bed/year in the U.S. and approximately 34,000 kWh/bed/year in Europe)—further reinforce the classification of healthcare as an energy-intensive sector.
While GDP-based energy intensity primarily reflects economic productivity per unit of energy consumed, healthcare—unlike light industry—does not generate tangible goods and thus exhibits lower GDP-based energy intensity. However, when measured per unit area, hospitals consume energy at levels comparable to industrial facilities rather than tertiary buildings. This distinction suggests that although healthcare may not match the economic productivity of light industry, its operational energy demand is more aligned with industrial sectors. Hospitals rely on continuous, process-heavy energy loads—including sterilization, medical gas production, HVAC, and advanced medical equipment—which resemble energy-intensive manufacturing rather than typical tertiary activities such as office spaces or retail.
Given these observations, it is reasonable to reconsider the conventional categorization of healthcare within the tertiary sector. Although the tertiary sector already includes healthcare, hospitals exhibit energy consumption far above the tertiary average. Instead, healthcare could be classified under industry—specifically light industry—due to its comparable energy consumption per unit area and its process-driven operational energy demand. This reclassification is further supported by energy intensity figures, which show that hospitals consume far more energy per square meter than commercial tertiary buildings, even if their GDP-based energy intensity remains lower than traditional manufacturing sectors. The methodologies used for calculating GDP-based and area-based energy intensities across different sectors are further detailed in the Supplementary Information (Appendices I–N).
Figure 2 provides a clear visualization of these findings, supporting the need for a revised classification of healthcare within energy benchmarking frameworks.
Similarities in energy forms and consumption per process
The comparative analysis summarized in Table 3 presents an overview of energy consumption in key processes across the healthcare and industrial sectors, as reported in the literature.The table emphasizes similarities in energy carriers—such as electricity, steam, and heat—used for operations like sterilization, cooling, heating, drying, incineration, and compressed air systems. Although the indicators used to quantify energy consumption (e.g., kWh/kg, kWh/m\(\vphantom{0}^2\), or kWh/tonne) vary, they consistently highlight the substantial energy demand in both sectors. In industry, energy use is often tied to production cycles, whereas hospitals require an uninterrupted energy supply to maintain patient care, medical processes, and sterile environments. This continuous demand, combined with stringent environmental control requirements and the operation of specialized medical equipment, contributes to the typically higher energy intensity observed in healthcare facilities.
Illustrative dynamic case study for the specialities operating theatres
Dynamic simulation of the specialities operating theatres
To complement the statistical reclassification of hospital energy demand, a focused dynamic analysis was conducted on a cluster of ten Operating Theatres (OTs) in a Moroccan University Hospital (UH Oujda). The Specialities_Operating_Theatre group occupies a total gross area of \(A_{\text {OT}}={439.602}{\textrm{m}^2}\) and represents one of the most energy-intensive clinical zones of the hospital.
The TRNSYS 18 configuration used for this case study is shown in Fig. 3. Meteorological inputs for Oujda (TMY2 file) are processed through Type 15–3 and supplied to the Type 56 multi-zone thermal model. The Specialities Operating Theatres are represented as an aggregated zone group in TRNBuild, with detailed internal gains and control schedules (Tables 4 and 5).
The simulation produces a full year of high-resolution data (8,760 hourly cooling and electrical load values). These time-series outputs are post-processed through unit converters and integrated using Type 24 to generate the final hourly profiles and the annual totals for cooling and electricity for the Operating Theatres.
The conceptual system boundary within which these OT loads are interpreted is shown in Fig. 4.
A detailed component-level sizing and optimisation of the hospital central plant (boilers, chillers, domestic hot water and auxiliaries) is beyond the scope of this paper. Instead, Fig. 4 serves only to indicate the multi-energy infrastructure in which the dynamic OT results are interpreted. The university hospital operates a multi-utility configuration structurally similar to many industrial sites: central boilers and chillers supply process-like thermal demands (such as high-ventilation Operating Theatres and sterilisation units), while domestic hot water and electrical auxiliaries are distributed across the campus. In this work, the schematic is used solely to illustrate the industrial-like nature of hospital energy infrastructures; all quantitative comparisons with other sectors rely exclusively on the annual specific electricity and cooling intensities derived from the TRNSYS load profiles.
Conceptual representation of the existing multi-energy system at UH Oujda, including boilers, chillers, domestic hot water (DHW) production and auxiliary components. The Operating Theatre cooling and electricity loads imported from TRNBuild are post-processed using Type 24 to obtain high-resolution hourly profiles and annual totals. The topology is comparable to utility systems in light industrial facilities; no detailed component sizing or control optimisation is performed in this work.
For each hourly time step, the TRNSYS deck outputs the total cooling power required by the Specialities Operating Theatres, \(Q_{\text {cool,OT}}(t)\) [kW], together with the internal electric power \(P_{\text {el,OT}}(t)\) [kW] associated with lighting and medical equipment. These loads are normalised by the total OT area to obtain specific power intensities \(q_{\text {cool,OT}}(t)\) and \(p_{\text {el,OT\_spec}}(t)\) [W/m\(\vphantom{0}^{2}\)]:
Rather than focusing on detailed transient behaviour, the present work uses these dynamic profiles to derive annual specific energy intensities for the OT block. Hourly specific electric and cooling power profiles are integrated over the full year (8760 h) using TRNSYS Type 24 to obtain annual specific energy demands \(E_{\text{el,OT}}^{\text{spec}}\) and \(E_{\text{cool,OT}}^{\text{spec}}\) [Wh·m−2]:
The corresponding annual specific energy intensities are obtained by unit conversion:
both expressed in kWh\(\cdot\)m\(\vphantom{0}^{-2}\cdot\)year\(\vphantom{0}^{-1}\). Using the TRNSYS outputs for the Specialities OT block, the resulting annual specific intensities are approximately \(p_{\text{el,OT}}^{\text{year}} \approx{242}{kWh.m^{-2}.year^{-1}}\) for internal electricity (lighting and medical equipment) and \(q_{\text{cool,OT}}^{\text{year}} \approx{1617}{kWh.m^{-2}.year^{-1}}\) for delivered cooling energy.
Data-centre benchmarks used for comparison
Because publicly available, area-normalised electricity and cooling intensities for industrial sectors are scarce and not consistently reported on a kWh\(\cdot\)m\(\vphantom{0}^{-2}\cdot\)year\(\vphantom{0}^{-1}\) basis, the present study uses data centres as a proxy for energy-intensive, process-driven facilities. In the recast EU Energy Efficiency Directive (EED 2023)48, data centres are treated as energy-intensive digital infrastructure subject to detailed energy-performance reporting, and they are often addressed as industrial-like facilities in energy-efficiency policy, reporting frameworks and the research literature. The IEA likewise characterises them as part of the global digital-infrastructure energy system with operational features comparable to industrial clean-process environments. They operate continuously under strict environmental control, high ventilation rates and high internal loads, conditions that closely resemble surgical suites.
Table 6 summarises the reported electricity and cooling intensities for several classes of data centres, alongside the intensities obtained for the Specialities Operating Theatres (OTs) in this study. Figure 5 illustrates this comparison using midpoints of published data-centre ranges and the cooling-electric equivalent for OTs.
Electricity intensities reported for data centres represent total electrical use, including internal process loads, lighting, equipment, ventilation and the electricity consumed by cooling systems. In contrast, the electrical intensity obtained for the Specialities Operating Theatres, \(p_{\text {el,OT}}^{\text {year}}\), reflects only internal electrical loads (lighting and medical devices). The cooling requirement is exported as a thermal load \(E_{\text {cool,OT}}\) and does not include the electricity used to generate that cooling.
To enable a consistent comparison with industrial and data-centre electricity intensities, the associated cooling electricity is estimated as
with hospital chiller coefficients of performance typically ranging from 2.8 to 3.5. Using COP = 3 as a representative value, the combined annual electrical-equivalent intensity of the Specialities Operating Theatres is expressed as:
This value exceeds the electricity intensities reported for room-based legacy data centres and lies well above the ranges typically associated with medium-size and hyperscale facilities (Table 6). While the internal electrical demand of the OTs alone is comparable to medium- to high-density data-centre environments, the magnitude of the cooling-related energy requirement distinguishes Operating Theatres as particularly energy-intensive, process-driven spaces. The similarity in operational constraints—continuous operation, strict environmental control, and dominant process loads—supports the interpretation that Operating Theatres behave energetically as clean-process or infrastructural environments rather than as conventional tertiary spaces. For contextual comparison within the hospital sector, a dynamically modelled and calibrated operating-room case reported in the literature exhibits a total energy intensity of 1685 kWh·m−2·year−1, reflecting similarly stringent hygienic and environmental constraints53.
Regulatory frameworks in industry and healthcare
Globally, the regulatory frameworks for energy efficiency and decarbonization in the industrial and healthcare sectors differ significantly. While industries are subject to rigorous regulations driven by large-scale energy consumption and high carbon emissions, the healthcare sector—despite its high energy intensity—often faces less stringent regulations. This regulatory gap can be attributed to differences in the operational needs of these sectors as well as the common perception of healthcare as part of the tertiary sector rather than as an energy-intensive industry.
Regulatory landscape in industry
Industries, particularly those in manufacturing, heavy industry, and energy production, are typically required to comply with stringent energy efficiency and decarbonization regulations. Because these industries contribute significantly to global emissions, many countries have implemented detailed policies that include mandatory energy audits, renewable energy integration, and carbon reduction strategies. For example, as reported in54, the industrial sector was a major focus for stricter energy efficiency policies in 2024. Many countries have introduced more stringent Minimum Energy Performance Standards (MEPS) for electric motors, MEPS being defined as the Minimum Energy Performance Standards, especially in regions with large industrial sectors and inefficient existing motor stocks. In addition, the industrial sector benefits from financial incentives and supportive government policies that promote energy savings and the adoption of renewable technologies55. This sector gains from tax rebates, financial support, and an emphasis on technological innovation aligned with corporate sustainability goals. For instance, the aluminum industry has achieved energy efficiencies of over 75% through electrification and carbon capture technologies56,57. Moreover, international climate agreements—such as the Paris Climate Accord—further influence these policies by setting clear emissions reduction targets.
Table 7 summarizes key regulatory incentives implemented across various regions to promote energy efficiency in industry, highlighting the specific frameworks, policies, and their tangible benefits in reducing energy consumption and carbon emissions.
Challenges in regulating healthcare facilities
Healthcare facilities, categorized under the tertiary sector, often face less regulatory pressure compared to industrial sectors despite their significant energy consumption. This categorization overlooks the fact that hospitals frequently consume more energy than other tertiary buildings67. The perception of the tertiary sector as less energy-intensive has resulted in less stringent regulations for healthcare, even though their continuous operations and safety-critical systems demand tailored energy efficiency measures. While initiatives such as the European Green Deal68 have begun addressing healthcare decarbonization, the sector’s regulatory environment remains fragmented and insufficiently stringent globally, highlighting the need for more comprehensive and specialized frameworks to address its environmental impact.
Recommendations for bridging the regulatory gap through a hybrid framework
To address the regulatory gap in healthcare energy efficiency, facilities can benefit from adopting key aspects of the industrial approach, including standardized energy audits, performance benchmarks, and financial incentives. These strategies should be complemented by policies specifically tailored to meet the distinct operational and energy challenges inherent to healthcare facilities.
This analysis highlights the importance of introducing a Hybrid Regulatory Framework for Healthcare, which recognizes the dual nature of hospitals. Hospitals combine industrial-scale energy demands with public service responsibilities, complicating their inclusion in traditional regulatory classifications. Developing tailored, hybrid regulations is essential to address these complexities effectively.
Such a framework should:
-
Reflect the unique energy requirements and operational challenges of healthcare facilities, as discussed in the following section on Hybrid Regulatory Framework and Limitations.
-
Incorporate adaptable measures from industrial regulations, such as energy performance metrics and continuous monitoring.
-
Modify existing regulatory categories to align with the hybrid characteristics of hospitals, ensuring both efficiency and compliance with public health mandates.
This hybrid approach not only aligns with sustainability goals but also ensures that hospitals operate effectively while minimizing their environmental footprint. By integrating industrial insights into healthcare-specific regulatory measures, this model can drive significant advancements in energy efficiency and sustainability in the healthcare sector.
Toward the adoption of distributed energy systems in healthcare with the same rigor as industrial precedence
Industry as a pioneer in the adoption of distributed energy systems: lessons for healthcare sector
The concept of Distributed Energy Systems originated in industry primarily with the advent of CHP or cogeneration systems, which gained popularity in the 1980 s and 1990 s as industries sought ways to increase energy efficiency and reduce costs. This early adoption focused on leveraging DES for simultaneous heat and electricity production in industrial facilities, thereby optimizing fuel use and waste heat recovery69,70. A recent study71 reviewed DES, focusing on technological features, application domains, and policy frameworks. Policies such as feed-in tariffs have accelerated DES adoption, with renewable-based systems now accounting for 26% of global power and over 32 countries operating more than 10 GW of renewable-based DES capacity. DES encompasses both renewable and non-renewable technologies. Renewable-based systems include solar (PV and solar thermal), wind, hydro, bioenergy, and geothermal, which produce electrical or thermal energy but often require storage due to intermittency. Non-renewable systems, such as internal combustion engines, CHP, CCHP, gas turbines, and micro-turbines, typically rely on fossil fuels but can integrate renewable sources like solar thermal.
In healthcare, particularly in hospitals, DES adoption grew in the early 2000 s when concerns about energy resilience, efficiency, and sustainability became more prominent. Hospitals, with their critical energy needs and round-the-clock operations, recognized the potential of DES to enhance reliability and reduce emissions72. These systems were increasingly viewed as essential for reducing operational costs and for supporting the stringent environmental conditions required in healthcare environments.
In parallel, waste recovery technologies, particularly Waste-to-Energy (WtE), emerged in the industrial sector in the 1960s—initially in Europe and North America—as part of efforts to reduce landfill use and generate renewable energy. The industry embraced these systems more widely in the 1970 s and 1980s. WtE technologies convert waste into electricity and heat through high-temperature incineration, thereby reducing both waste volume and environmental impact73. Industries also leverage alternative fuels (AFs) such as Refuse-Derived Fuel (RDF) and Solid Recovered Fuel (SRF) to decrease dependence on fossil fuels, enhance sustainability, and reduce operational costs; these fuels not only provide a cost-effective and eco-friendly alternative but also contribute to waste management by reducing landfill pressure74. In healthcare, the adoption of waste recovery technologies was slower, with hospitals initially focusing on waste segregation before gradually implementing systems—such as incineration for medical waste disposal—in the 1990s. This trend gained further traction in the 2000 s, particularly in developed nations, as part of broader sustainability efforts75.
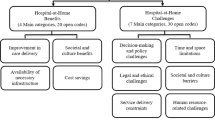
The diagram in Fig. 6 outlines the approach to integrating decentralized energy solutions, emphasizing the roles of cogeneration (CHP), trigeneration (CCHP), and decentralized generation (DG), along with their associated economic and environmental benefits. Additionally, Table 8 highlights the notable adoption of DES in the industrial sector, showcasing its diverse applications and considerable advantages in improving energy efficiency, reducing environmental impact, and supporting sustainable energy practices.
Case studies from the literature on combinations of energy systems implemented in hospitals and performance metrics
The literature lacks a comprehensive review comparing different combinations of distributed energy system (DES) designs in hospitals, even though an increasing number of individual studies focus on energy system integration in these settings. Research has primarily focused on four types of energy systems:
Cogeneration (CHP) systems
Early work in hospital energy integration examined combined heat and power (CHP) systems, which generate electricity and heat simultaneously. For example, Cappiello (2021)79 compared multiple CHP configurations for a hospital in Stuttgart using simulation and economic analysis. Options included a single CHP engine, dual engines, and a configuration combining one engine with a 500 kW photovoltaic field. The results indicated that a single 2 MW engine, optimized for thermal loads, provided the best economic performance with a very short payback period. Building on this foundation, Toughzaoui (2024)80 developed a fuel cell CHP system that integrates solar energy, hydrogen production, and storage. By applying genetic algorithms for optimization, this system minimizes both investment and electricity costs, highlighting the potential for decentralized, renewable-enhanced energy solutions in healthcare.
Trigeneration (CCHP) systems
Expanding on CHP, trigeneration—i.e. combined cooling, heating, and power (CCHP) systems—add cooling and steam production to electricity and heat. Pagliarini (2012)81 analyzed a system combining a gas engine cogeneration unit, a gas-fired auxiliary boiler, an absorption chiller, and an electric chiller. Simulation results underscored that public support is crucial to the economic feasibility of such systems. Complementary research from a field study in Greece82 confirmed that similar CCHP systems can achieve overall efficiencies above 75% with economic viability within eight years. Additionally, Santiago (2022)83 improved a CCHP system by incorporating an Organic Rankine Cycle (ORC) using pentane and R141b, achieving energetic and exergetic efficiencies of 81% and 42%, respectively.
Renewable polygeneration systems
Another approach integrates renewable energy sources with conventional systems to provide multiple outputs. Annamaria and Calise (2014)84 examined a system combining CPVT collectors, a single-stage LiBreH2O absorption chiller, storage tanks, and a gas-turbine CHP. Their TRNSYS simulation revealed a payback period of around 12 years, with potential for higher profitability through feed-in tariffs. In a related study, Swayze (2023)85 presented a decision-making framework comparing solar and natural gas-based trigeneration systems, finding that solar systems yield the fastest payback in hospitals, while natural gas systems may be more appropriate for mixed-use buildings. Further advancing the concept, Chen et al. (2021)86 proposed a hospital-oriented quad-generation system that integrates renewable sources, high-temperature superconducting cables, and cryogenic fluid storage to enhance energy reliability and reduce carbon emissions.
Waste-to-energy solutions
Parallel to energy generation, integrating medical waste management with energy recovery has also received attention. Windfeld and Brooks87 highlighted challenges arising from inconsistent definitions of medical waste, which lead to varying disposal practices. Zhao et al.88 documented a dramatic increase in medical waste due to the COVID-19 pandemic, underscoring the need for sustainable disposal methods. In response, Pokson (2024)39 simulated a waste-to-energy system that incorporated a steam sterilizer, incinerator, hot fluid tank, and multigeneration capabilities, achieving a 12% reduction in environmental impact along with measurable outputs in electricity, cooling, and heating. Similarly, Bujak (2015)19 evaluated a system integrating a heat recovery steam generator, microturbine, and steam/water heat exchanger, which effectively reduced waste volume and improved energy efficiency.
The table 9 summarizes these case studies and their key findings.
Benefits, limitations and research gaps in integrated energy systems for hospitals
Integrated energy systems in hospitals offer substantial benefits while facing significant challenges. On the benefits side, case studies (see Table 9) show that these systems improve energy efficiency—for example, CCHP systems with gas engines and ORC achieve efficiencies exceeding 75%81,83—and reduce operational costs, with CHP systems having payback periods of less than 2 years79 and CCHP systems around 8 years81. Additionally, distributed CCHP and waste-to-energy systems enhance energy supply reliability39,85, while waste-to-energy and solar-based trigeneration systems contribute to environmental benefits by lowering emissions39,85.
Despite these advantages, several challenges must be addressed. For example, clean and pure steam generation—critical for sterilization and patient care—requires strict purity standards89,90. Energy recovery systems integrated into air-handling units (AHUs) can improve overall efficiency by reclaiming energy from exhaust air, but they must ensure that air quality in sensitive areas (such as operating rooms and ICUs) is not compromised91. Maintaining precise indoor conditions (temperature, humidity, and air quality) is essential to safeguard patient care11. Moreover, sensor-based energy management systems face difficulties due to unpredictable occupancy patterns in high-traffic areas like emergency rooms92. High initial capital costs and the need for technology adaptation to meet rigorous operational and regulatory standards further complicate implementation11,93. Additional barriers include regulatory and technical challenges in integrating new technologies (such as waste-to-energy and solar polygeneration), operational complexities in managing multiple energy sources, and space limitations in urban or older hospital facilities91,92.
Furthermore, the literature lacks a fully integrated model that combines solar, combined heat and power (CHP), and waste-to-energy technologies specifically designed for healthcare applications through medical waste recovery94. In addition, the classification of hospitals within the tertiary sector is often insufficiently addressed and can be misleading when based solely on activity type. Bridging the regulatory gap between industry and healthcare in terms of energy efficiency and decarbonization requires the development of hybrid frameworks that account for the unique operational characteristics and complexities of hospitals.
Conclusion
By adopting industrial strategies for energy management—particularly Distributed Energy Systems (DES)—the healthcare sector can unlock significant opportunities to enhance energy efficiency. Integrated energy systems such as combined heat and power (CHP), combined cooling, heat, and power (CCHP), solar polygeneration, and waste-to-energy (WtE) technologies allow hospitals to effectively manage energy demand, lower operational costs, and reduce environmental impacts. These technologies, already widely implemented in the industrial sector due to established decarbonization policies and incentives, have positioned industries as leaders in energy transformation.
However, research that fully integrates solar, CHP, and WtE technologies for healthcare applications, particularly through medical waste recovery, remains limited. Optimizing the configuration, scalability, and performance of such systems for hospitals requires further exploration. Moreover, the classification of hospitals within the tertiary sector often fails to address their unique operational complexities, which can misguide energy strategies based solely on activity type. The illustrative dynamic case study presented in this work further highlights the process-like energy behaviour of critical hospital areas, reinforcing the argument for treating hospitals as industrial-scale energy users.
Bridging the regulatory and operational gap between industry and healthcare necessitates the development of hybrid frameworks that reflect the distinct energy needs of hospitals. Addressing challenges such as high initial costs, regulatory constraints, and spatial limitations requires tailored policies and incentives modeled on those in the industrial sector. Pilot projects and policy reforms will be crucial to refine these systems for healthcare environments, ensuring that hospitals achieve both energy efficiency and environmental sustainability. By doing so, the healthcare sector can actively contribute to global climate objectives while overcoming its unique challenges.
Methods
Study design and scope This is a non-experimental, observational, desk-based, data-driven comparative study that combines quantitative benchmarking, deterministic conversions, engineering-based process alignment, documentary analysis of regulatory instruments, and a narrative evidence synthesis on distributed energy systems (DES)/polygeneration. The study uses publicly available datasets and peer-reviewed sources, applies prespecified inclusion and harmonization rules, and documents procedures for reproducibility.
Sector mapping used for interpretation We clarify terminology and boundaries (primary/secondary/tertiary; energy-intensive vs. non-energy-intensive industry; healthcare within the tertiary sector) and construct a mapping that relates hospital functions to industrial-like processes based on energy carriers and operational roles (e.g., sterilization \(\leftrightarrow\) thermal processing; drying \(\leftrightarrow\) dehydration; refrigeration \(\leftrightarrow\) cold-chain). The mapping guides comparability and does not reassign official statistics.
Cross-region energy-intensity comparison To compare healthcare and industry beyond a single country, we compiled region-level indicators where reporting is consistent and verifiable. For the U.S. and EU27, we extracted:
-
GDP-based energy intensity (quads per trillion dollars or equivalent);
-
area-based intensity for buildings (kWh/m\(\vphantom{0}^{2}\); for hospitals and selected industrial subsectors);
-
sector-specific ratios where available (e.g., kWh/bed\(\cdot\)yr).
We harmonized units to SI (kWh, MJ; 1 kWh = 3.6 MJ) and applied transparent conversions documented in the Supplementary Information (SI). Numerical derivations are reproducible from the SI; due to non-comparable reporting, verified cross-region results are restricted to the U.S. and EU27 (this coverage limitation applies only to this subsection).
Process-level alignment of common energy forms We compared processes present in both sectors—sterilization, cooling, heating/space heat, drying, incineration, and compressed air/medical gases—focusing on energy carriers (electricity, steam/thermal) and the most comparable intensity metrics available in the literature (e.g., kWh/kg, kWh/article, kWh/m\(\vphantom{0}^{2}\!\cdot\)year, kWh/tonne). For each process, we verified that operational envelopes (e.g., temperature level, duty cycle) were comparable and converted reported metrics to a common basis where required. Worked calculations and unit conversions are provided in the SI.
Dynamic OT mini-scenario (TRNSYS) for quantitative validation To complement the desk-based comparisons, we developed an illustrative dynamic model of the Specialities Operating Theatres (OTs) using TRNSYS 18. The model incorporates climate inputs (TMY2), building-physics parameters from TRNBuild, internal gains and schedules calibrated from hospital operational data, and an hourly HVAC load evaluation. Outputs include cooling load \(Q_{\text {cool,OT}}(t)\), electrical demand \(P_{\text {el,OT}}(t)\), and their associated specific intensities (\(q_{\text {cool,OT}}(t)\) and \(p_{\text{el,OT}}(t)\)). Annual aggregates are used to compute electricity intensity (EI) and cooling-electric equivalents, enabling comparison with published benchmarks for data centres. The scenario is illustrative rather than predictive, and its purpose is to demonstrate the process-like energy behaviour of OTs under realistic operational constraints.
Regulatory contrast We reviewed energy-management and decarbonization instruments applicable to industrial establishments and to hospitals in the jurisdictions considered. For each, we recorded the presence or absence of audits, performance standards, incentives, recovery obligations, and monitoring/reporting provisions. The comparison is descriptive and informs the framework developed in the Discussion.
Evidence synthesis on DES and polygeneration We conducted a narrative synthesis of peer-reviewed studies and technical reports on CHP/CCHP, solar thermal/PV, and medical waste-to-energy relevant to both hospital loads and industrial analogs. Records were screened for operational relevance and transparent performance data. For each included item we extracted system scope (components), reported performance (efficiency, energy coverage, reliability contributions), and any economic indicators (e.g., simple payback). No meta-analysis was performed. Unit conventions and any necessary conversions for DES case values follow the Methods conventions above. The aim is to document industry’s established leadership and earlier, more rigorous adoption of DES and to assess feasibility for hospitals.
Integration step for healthcare-specific challenges We integrated the outputs from the cross-region comparison, process alignments, regulatory contrast, and DES evidence to articulate two overarching conclusions: (i) hospitals should not be treated as routine tertiary services but as facilities with industrial-like energy demand profiles, and (ii) a sector-appropriate, hybrid regulatory framework is needed to reflect hospital-specific constraints (e.g., indoor environmental quality and hygiene requirements, steam purity, redundancy and uptime, occupancy unpredictability, capital intensity, and space limitations). This synthesis provides the basis developed further in the Discussion.
Data handling, units, and conversions All indicators are reported in SI units. Where original sources used alternative units or economic bases (e.g., toe, MJ, local currencies, constant-price series), we converted them using stated factors in the SI and, for economic denominators, used the constant-price or currency-normalized series available in the cited datasets. Every arithmetic step shown or implied in the Results is reproduced in the SI so values can be checked and updated if a source is revised.
Coverage limitation The comparative assessment of healthcare and industry is restricted to the U.S. and EU27 because these are the only economies where energy-intensity indicators for both sectors are sufficiently documented, consistently reported, and methodologically compatible for cross-region comparison. For many other regions—particularly in the Global South—official statistics on hospital and industrial energy use remain incomplete, heterogeneous, or reported using non-comparable metrics, which prevents extending the cross-region analysis beyond the U.S.–EU27 dataset.
At the process level, however, publicly available electricity and cooling intensities for industrial facilities are generally scarce worldwide and are not reported in a harmonised manner. For this reason, data centres are adopted as the proxy for energy-intensive, process-driven environments: they are one of the few sectors with robust, internationally published intensity benchmarks, and they are formally recognised in EU legislation and IEA digital-infrastructure statistics as industrial-like facilities.
The dynamic TRNSYS modelling included in this work is similarly bounded in scope. It focuses exclusively on the Specialities Operating Theatres—the hospital’s most cooling-dominated and process-driven clinical area—while modelling broader healthcare structures lies beyond the purpose of this illustrative validation step.
Reproducibility Dataset names, access dates/versions, indicator definitions, and unit conversions are documented in the paper and/or SI, enabling exact reproduction of the numerical transformations reported and straightforward updates when sources are revised. The TRNSYS workflow used for the dynamic Operating Theatre mini-scenario is fully described through its model structure, parameter definitions, and governing equations, allowing independent replication of the resulting annual electricity and cooling intensities.
Data availability
All external datasets used in this study (including the U.S. Energy Information Administration, Eurostat, the Joint Research Centre, and the International Energy Agency) are publicly available from the cited sources. All derived indicators, calculations and conversions supporting the analysis are provided within the manuscript and the Supplementary Information. The TRNSYS-based dynamic case study is illustrative and follows standard modelling procedures; the resulting annual electricity and cooling intensities are part of the modelling outputs reported in the manuscript, and additional modelling details are available from the corresponding author upon reasonable request.
Abbreviations
- ACH:
-
Air Changes per Hour
- AHU:
-
Air Handling Unit
- AD:
-
Anaerobic Digestion
- CBECS:
-
Commercial Buildings Energy Consumption Survey
- CCHP:
-
Combined Cooling, Heating, and Power
- CHP:
-
Combined Heat and Power
- COP:
-
Coefficient of Performance (chiller)
- CPVT:
-
Concentrating Photovoltaic–Thermal
- DC:
-
Data Centre
- DES:
-
Distributed Energy Systems
- DG:
-
Distributed Generation
- DOE:
-
U.S. Department of Energy
- EIA:
-
U.S. Energy Information Administration
- EI:
-
Energy Intensity
- EUI:
-
Energy Use Intensity
- FEC:
-
Final Energy Consumption
- GDP:
-
Gross Domestic Product
- HRSG:
-
Heat Recovery Steam Generator
- IMW:
-
Infectious Medical Waste
- JRC:
-
Joint Research Centre
- KGOE:
-
Kilogram of Oil Equivalent
- LCA:
-
Life Cycle Assessment
- LCOE:
-
Levelized Cost of Energy
- OT:
-
Operating Theatre
- ORC:
-
Organic Rankine Cycle
- PV:
-
Photovoltaic
- RDF:
-
Refuse-Derived Fuel
- SRF:
-
Solid Recovered Fuel
- SFP:
-
Specific Fan Power
- TMY2:
-
Typical Meteorological Year (Version 2)
- TRNSYS:
-
Transient System Simulation Tool
- TRNBuild:
-
TRNSYS Building Preprocessor
- WHO:
-
World Health Organization
- WtE:
-
Waste-to-Energy
- \(A_{\text {OT}}\) :
-
Total floor area of the Specialities Operating Theatres [m\(\vphantom{0}^{2}\)]
- \(E_{\text {cool,el}}\) :
-
Cooling-electric equivalent energy (\(E_{\text {cool,OT}}/\text {COP}\)) [kWh\(\vphantom{0}_{\text {el}}\)]
- \(E_{\text {cool,OT}}^{\text{spec}} \) :
-
Annual specific cooling energy of OTs (Type 24 output) [\(\text{Wh}\cdot\)\(\text{m}^{-2}\)]
- \(E_{\text {el,OT}}^{\text{spec}}\) :
-
Annual specific cooling energy of OTs (Type 24 output) [\(\text{Wh}\cdot\)\(\text{m}^{-2}\)]
- \(EI_{\text{OT,total}}\) :
-
Total electrical-equivalent energy intensity of OTs (internal electricity + cooling-electric) [\(\text{kWh}\cdot\)\(\text{m}^{-2}\cdot\)\(\text{yr}^{-1}\)]
- \(P_{\text{el,OT}}(t)\) :
-
Instantaneous total electrical demand of the OT block [kW]
- \(p_{\text{el,OT}}(t)\) :
-
Specific instantaneous electrical demand of OTs [\(\text{W}\cdot\)\(\text{m}^{-2}\)]
- \(p_{\text{el,OT}}^{\text{year}}\) :
-
Annual specific electricity intensity of OTs [\(\text{kWh}\cdot\)\(\text{m}^{-2}\cdot\)\(\text{yr}^{-1}\)]
- \(Q_{\text {cool,OT}}(t)\) :
-
Instantaneous total cooling load of the OT block at time t [kW]
- \(q_{\text {cool,OT}}(t)\) :
-
Specific instantaneous cooling demand of OTs [\(\text{W}\cdot\)\(\text{m}^{-2}\)]
- \(q_{\text{cool,OT}}^{\text{year}}\) :
-
Annual specific cooling energy intensity of OTs [\(\text{kWh}\cdot\)\(\text{m}^{-2}\)\(\cdot\)\(\text{yr}^{-1}\)][
References
Investopedia. Economic sectors: An overview. https://www.investopedia.com/terms/s/sectors-of-the-economy.asp. Accessed: 2023-12-20.
Bank, W. World development indicators. https://data.worldbank.org/indicator (2023). Accessed: 2023-12-20.
U.S. Energy Information Administration. Energy use basics. https://www.eia.gov/consumption/residential/. Accessed: 2023-12-20.
U.S. Environmental Protection Agency. Electricity customers and energy use. https://www.epa.gov/energy/energy-efficiency. Accessed: 2023-12-20.
U.S. Department of Energy. Energy intensity indicators. https://www.energy.gov/eere/slsc/commercial-buildings-energy-consumption-survey-cbecs. Accessed: 2023-12-20.
Qin, C. et al. China’s non-energy-intensive sectors have greater carbon reduction potential: Based on a three-tier sda approach from energy substitution perspective. Environ. Impact Assess. Rev. 112, 107771. https://doi.org/10.1016/j.eiar.2024.107771 (2025).
United Nations Statistics Division. International standard industrial classification of all economic activities (isic). https://unstats.un.org/unsd/classifications. Accessed: 2023-12-20.
Grimaz, S., Ruzzene, E. & Zorzini, F. Situational assessment of hospital facilities for modernization purposes and resilience improvement. Int. J. Disaster Risk Reduct. 66, 102594. https://doi.org/10.1016/j.ijdrr.2021.102594 (2021).
Wang, J., Yang, W., Zhang, Y., Ren, T. & Liang, S. Research on energy consumption evaluation and energy saving and carbon reduction measures for typical general hospitals in hot summer and warm winter regions. Energy Sustain. Dev. 79, 101381. https://doi.org/10.1016/j.esd.2024.101381 (2024).
Räikkönen, M. et al. Economic and environmental indicators for assessing energy efficiency improvements in smart manufacturing processes. In Proceedings of the 16th World Congress on Engineering Asset Management (WCEAM), 602–611 (Springer International Publishing, Cham, 2023).
Tzeiranaki, S. T., Bertoldi, P., Economidou, M., Clementi, E. L. & Gonzalez-Torres, M. Determinants of energy consumption in the tertiary sector: Evidence at european level. Energy Rep. 9, 5125–5143. https://doi.org/10.1016/j.egyr.2023.03.122 (2023).
International Energy Agency. World energy outlook 2024 (2024).
Hervás-Zaragoza, J., Colmenar-Santos, A., Rosales-Asensio, E. & Colmenar-Fernández, L. Microgrids as a mechanism for improving energy resilience during grid outages: A post covid-19 case study for hospitals, https://doi.org/10.1016/j.renene.2022.08.132 (Publisher: Pergamon, 2022).
Squire, M. M., Munsamy, M., Lin, G., Telukdarie, A. & Igusa, T. Modeling hospital energy and economic costs for covid-19 infection control interventions. Energy Build. 242, 110948. https://doi.org/10.1016/j.enbuild.2021.110948 (2021).
Acehan, Z. & Sarikaya, Ö. S. Assessment of healthcare buildings in terms of spatial requirements in disaster cases: The case of adana city hospital emergency department during the covid-19 pandemic. Int. J. Disaster Risk Reduct. 108, 104577. https://doi.org/10.1016/j.ijdrr.2024.104577 (2024).
Jin, M., Feng, W., Marnay, C. & Spanos, C. Microgrid to enable optimal distributed energy retail and end-user demand response. Appl. Energy 210, 1321–1335. https://doi.org/10.1016/j.apenergy.2017.05.103 (2018).
Zhu, X., Zhang, X., Gong, P. & Li, Y. A review of distributed energy system optimization for building decarbonization. J. Build. Eng. 73, 106735. https://doi.org/10.1016/j.jobe.2023.106735 (2023).
Kasaeian, A., Bellos, E., Shamaeizadeh, A. & Tzivanidis, C. Solar-driven polygeneration systems: Recent progress and outlook. Appl. Energy 264, 114764. https://doi.org/10.1016/j.apenergy.2020.114764 (2020).
Bujak, J. W. Production of waste energy and heat in hospital facilities. Energy 91, 350–362 (2015).
International Energy Agency. Tracking clean energy progress 2023 (2023). Accessed: 2024-12-30.
McMillan, C. 2018 industrial energy data book. National Renewable Energy Laboratory. https://doi.org/10.7799/1575074 (2019).
U.S. Energy Information Administration. Manufacturing energy consumption survey (mecs), 2018 (2021). Released: February 2021.
U.S. Energy Information Administration. Mecs 2018 – enclosed floorspace and number of establishment buildings. Table 9.1 (2021). Released: September 2021.
U.S. Energy Information Administration. Electricity data browser: Average retail price of electricity (2022). Accessed: 2025-02-03.
Associates, G. . B. Hospital energy and water benchmarking survey, 2022 (2022). Accessed: 2025-02-03.
U.S. Energy Information Administration. Energy characteristics and energy consumed in large hospital buildings in the united states (2007 & 2018) (2018). Accessed: 2025-02-03.
Energy information administration (eia) - commercial buildings energy consumption survey (cbecs). Accessed: 2025-02-26.
Doe buildings energy consumption survey. Accessed: 2025-02-26.
Eurostat. Eurostat database (2023). Accessed 23 Feb 2025.
Tzeiranaki, S. T. et al. Energy consumption and energy efficiency trends in the eu, 2000–2020. Tech. Rep., Publications Office of the European Union, Joint Research Centre https://doi.org/10.2760/727548. (EU Energy Efficiency Report, 2022).
González, A. G., García-Sanz-Calcedo, J. & Salgado, D. R. A quantitative analysis of final energy consumption in hospitals in spain. Sustainability 10, 1696 (2018).
Ubigreen. Hospital energy bill: How to stop the bleeding? (2024). Accessed: 2025-02-25.
Balaras, C. A. et al. Energy use intensities for non-residential buildings. In Proceedings of the 48th International HVAC&R Congress and Exhibition, 369, https://doi.org/10.24094/kghk.017.48.1.369 (Belgrade, Serbia, 2017).
McGain, F., Moore, G. & Black, J. Steam sterilisation’s energy and water footprint: A hospital case study. Aust. Health Rev. 40, 333–339. https://doi.org/10.1071/AH15163 (2017).
Gil, A. G., González, O. A. O., Sepúlveda, L. F. C. & Torres, P. N. A. Venting stage experimental study of food sterilization process in a vertical retort using temperature distribution tests and energy balances. Case Stud. Therm. Eng. 22, 100736. https://doi.org/10.1016/j.csite.2020.100736 (2020).
Bai, X., Ma, W., Huang, J., Liang, C. & Zhang, X. Performance assessment and improvement of a district cooling system: A case study of enhancing energy efficiency of hospital buildings. Case Stud. Therm. Eng. 56, 104187. https://doi.org/10.1016/j.csite.2024.104187 (2024).
Judith, E. 15 - minimising energy consumption associated with chilling, refrigerated storage and cooling systems in the food industry. In Klemeš, J., Smith, R. & Kim, J.-K. (eds.) Handbook of Water and Energy Management in Food Processing, 449–480, https://doi.org/10.1533/9781845694678.4.449 (Woodhead Publishing, 2008).
Shen, C., Zhao, K., Ge, J. & Zhou, Q. Analysis of building energy consumption in a hospital in the hot summer and cold winter area. Energy Procedia 158, 3735–3740. https://doi.org/10.1016/j.egypro.2019.01.883 (2019).
Pokson, C. & Chaiyat, N. Energy, economic, and environmental analysis of a novel combined cooling, heating, and power (cchp) system from infectious medical waste. Clean. Waste Syst. 8, 100155. https://doi.org/10.1016/j.clwas.2024.100155 (2024).
John, J., Collins, M., O’Flynn, K. et al. Carbon footprint of hospital laundry: A life-cycle assessment. BMJ Open 14, https://doi.org/10.1136/bmjopen-2023-080838 (2024).
Mondal, M. H. T. & Sarker, M. S. H. Comprehensive energy analysis and environmental sustainability of industrial grain drying. Renew. Sustain. Energy Rev. 199, 114442. https://doi.org/10.1016/j.rser.2024.114442 (2024).
Rizan, C., Bhutta, M. F., Reed, M. & Lillywhite, R. The carbon footprint of waste streams in a uk hospital. J. Clean. Prod. 286, 125446. https://doi.org/10.1016/j.jclepro.2020.125446 (2021).
Tao, Y., Feng, Q. & Chen, Y. Improving long-term operation performance of hazardous waste rotary kiln incineration facilities: An evaluation with a dea model. Water Res. 174, 575–584. https://doi.org/10.1016/j.wasman.2023.11.034 (2024).
Energy portal: Energy information. Accessed: 2024-11-18.
Compressed air challenge. Accessed: 2024-11-18.
Abd Rahman, N. M., Lim, C. H. & Fazlizan, A. Optimizing the energy saving potential of public hospital through a systematic approach for green building certification in malaysia. J. Build. Eng. 43, 103088. https://doi.org/10.1016/j.jobe.2021.103088 (2021).
Golmohamadi, H. Demand-side management in industrial sector: A review of heavy industries. Renew. Sustain. Energy Rev. 156, 111963. https://doi.org/10.1016/j.rser.2021.111963 (2022).
Directive (EU) 2023/1791 of the European Parliament and of the Council of 13 September 2023 on energy efficiency and amending Regulation (EU) 2023/955 (recast) (Text with EEA relevance) (2023).
European Commission Joint Research Centre. Eu code of conduct for data centres: Best practice guidelines, 13th edition. Tech. Rep. JRC128184, Joint Research Centre, European Commission (2022). Accessed: 2025-12-08.
IEA 4E – Electronic Devices and Networks Annex (EDNA). Metrics for data centre energy efficiency: A critical review of models and results. Tech. Rep., International Energy Agency (IEA), 4E – Electronic Devices and Networks Annex (2020). Accessed: 2025-12-08.
Davis, J. Uptime institute global data center survey 2022. https://uptimeinstitute.com/resources/research-and-reports/uptime-institute-global-data-center-survey-results-2022 (2022). Industry survey report.
Masanet, E., Shehabi, A., Lei, N., Smith, S. & Koomey, J. Recalibrating global data center energy-use estimates. Science 367, 984–986. https://doi.org/10.1126/science.aba3758 (2020).
González-Gil, A., López-González, J. L., Fernández, M., Eguía, P., Erkoreka, A., Granada, E. Thermal energy demand and potential energy savings in a Spanish surgical suite through calibrated simulations. Energy Buildings 174, 513–526. https://doi.org/10.1016/j.enbuild.2018.06.035 (2018).
International Energy Agency. Energy efficiency 2024 (2024). Accessed: 2024-12-18.
International Energy Agency. Clean energy progress: Energy efficiency 2023 (2023).
International Energy Agency. Energy efficiency in emerging markets report (2020).
Industrial deep decarbonization: Modeling approaches and challenges. https://www.rff.org/publications/reports/industrial-deep-decarbonization-modeling-approaches-and-data-challenges/. Accessed: 17 Nov. 2024.
Malinauskaite, J. et al. Energy efficiency in industry: Eu and national policies in italy and the uk. Energy 172, 255–269. https://doi.org/10.1016/j.energy.2019.01.130 (2019).
Bayssi, O. et al. Green hydrogen landscape in north african countries: Strengths, challenges, and future prospects. Int. J. Hydrog. Energy 84, 822–839. https://doi.org/10.1016/j.ijhydene.2024.08.277 (2024).
International Energy Agency. International energy agency publishes new review of morocco’s energy policies. https://www.iea.org/news/international-energy-agency-publishes-new-review-of-moroccos-energy-policies (2019). Accessed 17 November 2024.
Decree n. 2-17-746: Mandatory energy audits and energy audit organisations. https://www.iea.org/policies/8571-decree-n-2-17-746-on-mandatory-energy-audits-and-energy-audit-organisations. Accessed: 18 Nov. 2024.
Morocco: A new legal framework for independent power producers (2023). Accessed: 2024-11-18.
Zhang, Z., Li, R., Song, Y. & Sahut, J.-M. The impact of environmental regulation on the optimization of industrial structure in energy-based cities. Res. Int. Bus. Finance 68, 102154. https://doi.org/10.1016/j.ribaf.2023.102154 (2024).
Guang, F., Wen, L. & Sharp, B. Energy efficiency improvements and industry transition: An analysis of china’s electricity consumption. Energy 244, 122625. https://doi.org/10.1016/j.energy.2021.122625 (2022).
Bhagwan, N. & Evans, M. A review of industry 4.0 technologies used in the production of energy in china, germany, and south africa. Renew. Sustain. Energy Rev. 173, 113075, https://doi.org/10.1016/j.rser.2022.113075 (2023).
Hassan, Q. et al. Adapting german energy transition rules for iraq through industry, flexibility, and demand management. Futures 161, 103411. https://doi.org/10.1016/j.futures.2024.103411 (2024).
U.S. Department of Energy. Usdoe 2020 energy report (2020).
The european green deal. Accessed: 2024-11-18.
Kalam, A., King, A., Moret, E. & Weerasinghe, U. Combined heat and power systems: economic and policy barriers to growth. Chemistry Central Journal 6, S3, https://doi.org/10.1186/1752-153X-6-S1-S3 (2012). PMID: 22540988; PMCID: PMC3332257.
eBooks.com. Energy efficiency and management for engineers. https://www.ebooks.com/en-us/book/209934971/energy-efficiency-and-management-for-engineers/mehmet-kanoglu/. Accessed: 2024-11-09.
Nadeem, T. B., Siddiqui, M., Khalid, M. & Asif, M. Distributed energy systems: A review of classification, technologies, applications, and policies. Energy Strategy Rev. 48, 101096. https://doi.org/10.1016/j.esr.2023.101096 (2023).
U.S. Department of Energy. Hospitals discover advantages to using chp systems. https://www1.eere.energy.gov/buildings/publications/pdfs/alliances/hea_chp.pdf (2011). Accessed: 2024-11-09.
Shareefdeen, Z. & Al-Najjar, H. Waste-to-energy technologies. In Hazardous Waste Management: Advances in Chemical and Industrial Waste Treatment and Technologies, 207–232, https://doi.org/10.1007/978-3-030-95262-4_8 (Springer International Publishing, 2022).
Shehata, N. et al. Role of refuse-derived fuel in circular economy and sustainable development goals. Process Saf. Environ. Prot. 163, 558–573. https://doi.org/10.1016/j.psep.2022.05.052 (2022).
World Health Organization. Safe Management of Wastes from Health-Care Activities (World Health Organization, Geneva, 2005).
Mobarakeh, M. R. & Kienberger, T. Climate neutrality strategies for energy-intensive industries: An austrian case study. Clean. Eng. Technol. 10, 100545. https://doi.org/10.1016/j.clet.2022.100545 (2022).
Eardley, G. S., Choi, J.-K., Hong, T. & An, J. Decarbonization potential of regional combined heat and power development. Renew. Sustain. Energy Rev. 189, 114038. https://doi.org/10.1016/j.rser.2023.114038 (2024).
Gupta, A. K. et al. Green chemistry revolutionizing sustainability in the food industry: A comprehensive review and call to action. Sustain. Chem. Pharm. 42, 101774. https://doi.org/10.1016/j.scp.2024.101774 (2024).
Cappiello, F. L. & Erhart, T. G. Modular cogeneration for hospitals: A novel control strategy and optimal design. Energy Convers. Manag. 237, 114131. https://doi.org/10.1016/j.enconman.2021.114131 (2021).
Toughzaoui, Y. et al. Advances in hospital energy systems: Genetic algorithm optimization of a hybrid solar and hydrogen fuel cell combined heat and power. Int. J. Hydrog. Energy 86, 1310–1325. https://doi.org/10.1016/j.ijhydene.2024.09.001 (2024).
Pagliarini, G., Corradi, C. & Rainieri, S. Hospital CHCP system optimization assisted by TRNSYS building energy simulation tool. Appl. Therm. Eng. 44, 150–158. https://doi.org/10.1016/j.applthermaleng.2012.04.001 (2012).
Papadimitriou, A., Tosios, A. & Giannini, E. Techno-economic performance assessment of a trigeneration system operating in a hospital. Energies 14, https://doi.org/10.3390/en14165105 (2021).
Santiago, T. S. A., Achiles, A. E. & Dangelo, J. V. H. Thermodynamic performance analysis and optimization of a trigeneration system with different configurations applied to a medium-sized hospital. Energy 239, 122195. https://doi.org/10.1016/j.energy.2021.122195 (2022).
Buonomano, A., Calise, F., Ferruzzi, G. & Vanoli, L. A novel renewable polygeneration system for hospital buildings: Design, simulation and thermo-economic optimization. Appl. Therm. Eng. 67, 43–60 (2014).
Swayze, E. & Singh, K. Techno-economic-environmental decision-making approach for the adoption of solar and natural gas-based trigeneration systems. Energy Convers. Manag. 289, 117189. https://doi.org/10.1016/j.enconman.2023.117189 (2023).
Chen, X. et al. Hospital-oriented quad-generation (HOQG)—A combined cooling, heating, power and gas (CCHPG) system. Appl. Energy 300, 117382, https://doi.org/10.1016/j.apenergy.2021.117382 (2021). Publisher: Elsevier.
Windfeld, E. S. & Brooks, M.S.-L. Medical waste management - A review. J. Environ. Manag. 163, 98–108. https://doi.org/10.1016/j.jenvman.2015.08.013 (2015).
Zhao, H.-L. et al. Energy, environment and economy assessment of medical waste disposal technologies in China. Sci. Total Environ. 796, 148964. https://doi.org/10.1016/j.scitotenv.2021.148964 (2021).
Jamshidmofid, M. et al. Solar-assisted clean steam generator, a cleaner production approach for sustainable healthcare facilities. J. Clean. Prod. 452, 142132. https://doi.org/10.1016/j.jclepro.2024.142132 (2024).
Green, G. & Nordholm, L. M. Hospital steam system functions and operations. Health Facilities Management Magazine (2024).
Sanz-Calcedo, J. G., Al-Kassir, A. & Yusaf, T. F. Thermal energy recovery in critical areas of hospitals. Energy Procedia 158, 3726–3731 (2019).
Wang, X. Heat/energy recovery technologies in buildings. In Wang, R. & Zhai, X. (eds.) Handbook of Energy Systems in Green Buildings, 1–41, https://doi.org/10.1007/978-3-662-49088-4_24-1 (Springer Berlin Heidelberg, Berlin, Heidelberg, 2017).
Garcés, H. O. et al. Monitoring of Thermal Comfort and Air Quality for Sustainable Energy Management inside Hospitals Based on Online Analytical Processing and the Internet of Things. International Journal of Environmental Research and Public Health 19, 12207,https://doi.org/10.3390/ijerph191912207 (2022). Number: 19 Publisher: Multidisciplinary Digital Publishing Institute.
Lakjiri, S., Ouassaid, M. & Cherkaoui, M. Enhancement of the energy efficiency in moroccan public hospitals through solar polygeneration system https://doi.org/10.1109/CISTEM.2016.8066774 (2016).
Acknowledgements
The authors acknowledge the support of various stakeholders in the healthcare and energy sectors in Morocco. Their insights and collaboration have contributed to the contextual understanding of energy efficiency and sustainability challenges in hospital infrastructures.
Funding
The authors received no funding for this work.
Author information
Authors and Affiliations
Contributions
S.L. conceived the study, developed the conceptual framework, and conducted the analysis. M.O. supervised the research design and contributed to the review and interpretation of results. Both authors reviewed and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Lakjiri, S., Ouassaid, M. Reclassifying hospital energy demand toward industry-like requirements for hygienic and resilient indoor environments. Sci Rep 16, 3904 (2026). https://doi.org/10.1038/s41598-025-33606-2
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-33606-2