Introduction
Empiric antibiotics are given to about 80% of very low birth weight (VLBW) infants in the United States for concern of early-onset sepsis (EOS) [1]. We previously reported that implementing a delivery-based risk-stratification guideline for EOS evaluation among preterm infants in1 our level III neonatal intensive care unit (NICU), consistent with American Academy of Pediatrics (AAP) recommendations, was associated with reduced early antibiotic use without safety concerns [2, 3].
Infants are classified as low-risk if born by cesarean delivery for maternal indications (e.g., preeclampsia), without labor or attempted induction of labor, and with rupture of membranes at delivery [2, 4, 5]. In this study, we assessed the sustainability and safety of this guideline over a four-year period following its initial implementation.
Methods
We conducted a retrospective cohort study of VLBW infants (<1500 g) admitted to the NICU from January 2009 to April 2025. The study was approved by the University of Pennsylvania IRB.
Three study periods were defined: pre-implementation (January 2009–March 2017), post-implementation (April 2017–January 2020), and sustainability (February 2020–April 2025). Clinical data were extracted from the electronic medical record. The primary outcome was the proportion of VLBW infants (overall and low-risk) with antibiotic initiation on days 0–3 after birth. Balancing measures included antibiotic initiation on days 4–7, blood or spinal fluid culture-confirmed infection on days 4–7, and death or transfer by day 7.
Comparisons were made across periods using descriptive statistics. Annual rates of antibiotic initiation among low-risk VLBW infants were displayed graphically.
Results
The study included 1253 VLBW infants: 727 during pre-implementation, 191 during post-implementation, and 335 during the sustainability period (Supplementary Table 1). Baseline characteristics were similar across cohorts. The proportion classified as low-risk was 41%, 44%, and 35% across the three periods.
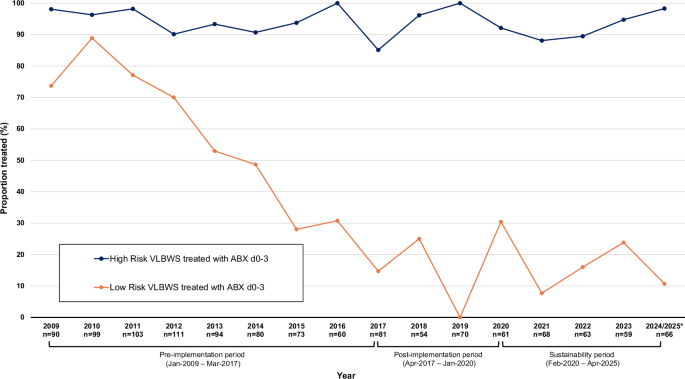
Among low-risk infants, early antibiotic initiation decreased from 185/298 (62.1%) pre-implementation to 11/83 (13.3%) post-implementation and remained low in the sustainability period at 21/122 (17.2%), with no significant difference between post-implementation and sustainability (p = 0.4, Supplementary Table 2). For days 4–7, rates of blood culture collection, antibiotic initiation, bacteremia, and death or transfer were similar across periods. As rates of early antibiotic initiation among low-risk infants declined, the rate among high-risk infants was unchanged over the study period (Fig. 1).
Annual proportions of very low birth weight (VLBW) infants receiving antibiotics on days 0–3 after birth from 2009 through April 2025 are shown by delivery risk category. The orange line represents low-risk infants (delivered by cesarean for maternal indications, without labor or rupture of membranes before delivery), and the blue line represents higher-risk infants. * Data for 2024–2025 were combined, as the sustainability period includes infants born through April 2025 only.
To assess whether changes were limited to low-risk infants or reflected broader practice shifts, we compared antibiotic use among all VLBW infants. Antibiotic initiation increased in the sustainability period compared to post-implementation (113/191 [59.2%] vs. 221/335 [66.0%], p = 0.04), though the proportion of low-risk infants was lower (43.5% vs. 36.4%, p = 0.05). During days 4–7, both antibiotic initiation (11.5% vs. 6%, p = 0.03) and blood culture collection (13.1% vs. 7.2%, p = 0.02) were lower in the sustainability period. Rates of death, transfer, and culture-confirmed EOS were similar across periods. Overall, 18/738 (2.4%) high-risk infants had culture-confirmed EOS, while no cases occurred among 488 low-risk infants (p < 0.001).
During the sustainability period, 21 low-risk infants (17.2%) received early antibiotics. Documented reasons included clinical change (n = 10), hypotension (n = 5), gastrointestinal pathology (n = 4), poor biophysical profile (n = 1), and hyperglycemia (n = 1).
Discussion
Implementation of a delivery-based EOS risk-stratification guideline based on AAP recommendations for VLBW infants was sustained for over seven years without safety concerns. Early antibiotic initiation among low-risk infants remained stable and low through the sustainability period, and no cases of culture-confirmed EOS occurred in this group at any time during the study. The continued reduction in antibiotic initiation and blood culture collection during days 4–7 suggests growing provider confidence in the guideline.
These findings build on prior work demonstrating that delivery-based risk stratification can reduce the use of early empiric antibiotics in preterm infants [3,4,5]. Sustained reductions indicate that this approach is durable and adaptable within a high-volume NICU. Delivery-based criteria are simple, reproducible, and rely on routine obstetric data. Broader adoption may help reduce antibiotic exposure in very preterm infants, where empiric use remains common [1]. Further, adoption of this approach helps clinicians recognize not only those VLBW at very low risk of EOS, but also highlights the characteristics of VLBW infants at highest risk of EOS, a potentially fatal complication of preterm birth.
Conclusion
Sustained reductions in early empiric antibiotics among VLBW infants highlight the feasibility of risk-stratified stewardship as a long-term practice standard.
Data availability
De-identified data are available from the corresponding author upon reasonable request.
References
Flannery DD, Ross RK, Mukhopadhyay S, Tribble AC, Puopolo KM, Gerber JS. Temporal trends and center variation in early antibiotic use among premature infants. JAMA Netw Open. 2018;1:e180164. https://doi.org/10.1001/jamanetworkopen.2018.0164.
Puopolo KM, Benitz WE, Zaoutis TE. Management of neonates born at ≤34 6/7 weeks’ gestation with suspected or proven early-onset bacterial sepsis. Pediatrics. 2018;142:e20182896.
Garber SJ, Dhudasia MB, Flannery DD, Passarella MR, Puopolo KM, Mukhopadhyay S. Delivery-based criteria for empiric antibiotic administration among preterm infants. J Perinatol. 2020. https://doi.org/10.1038/s41372-020-00784-y.
Flannery DD, Mukhopadhyay S, Morales KH, Dhudasia MB, Passarella M, Gerber JS, et al. Delivery characteristics and the risk of early-onset neonatal sepsis. Pediatrics. 2022;149. https://doi.org/10.1542/PEDS.2021-052900/1232648/PEDS_2021052900.PDF
Puopolo KM, Mukhopadhyay S, Hansen NI, Cotton CM, Stoll BJ, Sanchez PJ, et al. Identification of extremely premature infants at low risk for early-onset sepsis. Pediatrics. 2017;140:e20170925.
Author information
Authors and Affiliations
Contributions
MFM conceptualized the study, drafted the initial manuscript, revised the manuscript for important intellectual content, and approved the final version. AZB conceptualized the study, managed and analyzed the data, revised the manuscript for important intellectual content, and approved the final version. KMP conceptualized the study, revised the manuscript for important intellectual content, and approved the final version. SM conceptualized the study, revised the manuscript for important intellectual content, and approved the final version. SJG conceptualized the study, managed and analyzed the data, revised the manuscript for important intellectual content, and approved the final version. DDF conceptualized the study, drafted the initial manuscript, revised the manuscript for important intellectual content, and approved the final version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
May, M.F., Zevallos Barboza, A., Garber, S.J. et al. Long-term sustainability and safety of a delivery-based early-onset sepsis evaluation strategy for very low birth weight infants. J Perinatol (2026). https://doi.org/10.1038/s41372-026-02607-y
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41372-026-02607-y