Abstract
Objectives
To evaluate trends in neonatal intensive care unit (NICU) admissions, illness acuity, and hospitalization costs among U.S. children’s hospitals from 2017 to 2022.
Methods
This retrospective cohort study used data from the Pediatric Health Information System (PHIS) and included all NICU admissions. We examined trends in patient characteristics (e.g., gestational age, complex chronic conditions), illness severity scores, and standardized hospital costs. Interrupted time series analyses assessed changes in NICU costs over time.
Results
There were 234,571 infants admitted to NICUs in US children’s hospitals between 2017 and 2022. NICU admissions shifted significantly by gestational age with admissions increasing by 10–18% among extremely, very, and late preterm infants. Term infants remained the largest admission group, averaging 45% annually (p < 0.001). Infants with ≥1 complex chronic condition increased from 46.6% in 2017 to 50.9% in 2022 (p < 0.001). NICU-specific illness severity increased modestly over time (1.14–1.24, p < 0.001). Median standardized NICU hospital costs rose by approximately 20% over the study period, with notable inflections in early 2020 and 2021.
Conclusions
Among US children’s hospitals in the PHIS database, NICU admissions were increasingly complex and costly. These findings highlight the importance of ongoing monitoring of resource use and patient mix in specialized NICU settings.
Similar content being viewed by others
Introduction
Neonatal intensive care units (NICUs) play a critical role in managing the care of high-risk infants, with children’s hospitals frequently serving as referral centers for the most complex neonatal conditions. Approximately 10% of all live births in the United States (US) require admission to a NICU with conditions ranging from brief, self-limited illnesses to those requiring prolonged, resource-intensive support [1, 2]. Over the past decade, NICU admission rates have increased by 37% [1]. However, this expansion in care comes with significant costs and longer hospital stays [3,4,5,6], with more than 30% of NICU graduates experiencing chronic health needs post-discharge [7, 8]. As survival improves and the population of NICU graduates becomes more medically complex, it is essential to examine how care needs are evolving in NICU care.
In the United States, there are more than 1400 NICUs with approximately 35,000 beds, most of which are classified as Level III or IV. Higher-acuity NICUs with greater bed capacity are concentrated in children’s and academic hospitals and often located in regions with higher population density [9]. Monitoring epidemiologic trends in NICU admissions is important to understand neonatal care’s evolving landscape and identifying emerging challenges and patterns, given their critical role in the care of high-risk newborns and infants [10]. Previous research has primarily focused on preterm birth and the associated direct medical costs [11, 12], often overlooking the significant proportion of NICU admissions that involve late preterm and full-term infants [13]. For example, between 2016 and 2023, NICU admission rates increased by 9% for full-term and 4% for late-preterm infants [14]. Furthermore, few studies have captured trends in illness severity, complex chronic conditions (CCCs), and length of stay (LOS) within US children’s hospitals, where the most intensive neonatal care is delivered. Such data would be particularly useful given the regionalization of NICU care and increasing complexity.
While NICU utilization and the associated costs have risen nationally, granular trend analyses are limited, particularly for high-acuity tertiary settings. Tertiary children’s hospitals offer a unique vantage point into shifts in neonatal case mix and intensity due to their specialization in complex care, although their neonatal populations may differ from other community hospitals. By focusing on these hospitals [15], our study aims to characterize trends in NICU admissions, patient acuity, and hospitalization costs over a five-year period, including the onset and early recovery phases of the COVID-19 pandemic. These findings may inform planning and resource allocation within tertiary care systems and generate hypotheses for broader population-based research. Thus, we sought to explore trends in NICU admission rates and hospital costs among a cohort of infants at US children’s hospitals between 2017 and 2022.
Methods
Design and data source
We conducted a retrospective cohort study using data from the Pediatric Health Information System (PHIS), an administrative database maintained by the Children’s Hospital Association (Lenexa, KS). PHIS includes inpatient, emergency department, ambulatory surgery, and observation unit data from 48 tertiary children’s hospitals in the United States. The data available in the PHIS dataset includes patient demographic characteristics, procedure codes, and detailed billing information.
Guidelines and ethics statement
This study followed the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) [16] reporting guidelines for cross-sectional studies and determined to be non-human subjects’ research by the Henry Ford Health Institutional Board and exempt from review.
Study population
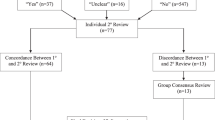
The study cohort included all infants admitted to a PHIS hospital with at least a single day’s room charge for a NICU bed. Infants were included if their discharge date was between January 1, 2017, and December 31, 2022. Encounters were excluded if they originated from a hospital that did not consistently report NICU charges (n = 9 hospitals), or if infants had missing or unknown gestational age or birth weight values. Additionally, children with a recorded NICU charge whose age at admission was greater than 1 year were excluded (see Fig. 1). This exclusion criteria were necessary to confirm the cohort included only those patients who were admitted to the NICU immediately following birth. Infant medical complexity was identified and flagged by diagnosis codes using the Complex Chronic Conditions Classification (CCC) System [17]. This system identifies conditions using codes from the International Classification of Diseases, 10th Revision (ICD-10), and categorized into 10 domains, and widely adopted for research in pediatric populations for over two decades and shown to correlate with healthcare use and mortality risk [18, 19]. The domains of the CCC are allocated by body system. For instance, the ‘cardiovascular domain’ includes all congenital heart defects and conditions related to the heart. The ‘congenital or genetic defect domain’ includes those conditions not otherwise specified in another domain. Examples of CCC diagnoses for each domain are available in supplementary content.
Flow diagram of NICU cohort.
Study outcomes
Patient characteristics included gestational age, birth weight, sex assigned at birth, race/ethnicity, insurance type, discharge disposition, admission source, NICU length of stay (LOS) and Child Opportunity Index (COI). Admission source was defined as follows: ‘inborn’ includes infants admitted to the same facility where they were born versus ‘outborn’ includes infants born at a different facility and transferred to a PHIS hospital with a NICU. The COI is an area-level variable that assesses neighborhood conditions, resources, and environments contributing to healthy development [20]. Illness severity was measured using an adapted, H-RISK score, a PHIS-specific metric that assigns a severity score based on the deviation in length of stay for each All Patient Refined Diagnosis Related Group (APR-DRG) compared to expected values. Increasing values of the score indicate increasing mean NICU LOS for the assigned APR-DRG, suggestive of higher severity of illness [21]. This is a standardized method for stratifying illness severity within PHIS data and has been used in prior neonatal research [21]. Hospital characteristics included admissions rates, hospital length of stay, and NICU-related hospital and total hospitalization costs.
Hospitalization costs
NICU costs were defined as direct medical costs attributable to the NICU stay, from the hospital perspective [22]. Hospital-specific and department-specific cost-to-charge ratios (CCR) were applied to estimate costs, excluding physician fees and indirect costs. CCR are the estimated cost incurred by the hospital. The PHIS dataset uses a standardized unit cost, which is not a direct measure of hospital cost dollars, but a measure of volume related to resources consumed [23]. This standardized unit cost is calculated based on unique hospital median costs for services and developed as a proxy for true resource use that is comparable across hospitals [24]. To adjust for regional variation, costs were standardized using the Centers for Medicare & Medicaid Services wage/price index and inflated to 2022 US dollars using the Producer Price Index for Inpatient Services [25].
Statistical analysis
Patient and hospitalization characteristics were described using frequencies and percentages for categorical variables, medians with interquartile range (IQR) for non-normal continuous variables and means with standard errors (SE) for continuous variables following a normal distribution. Categorical patient and hospitalization characteristics over time were analyzed using generalized linear models (GLM), which included year as the only variable. We assumed a binomial or multinomial distribution with a respective logit or generalized logit link function for categorical variables and a normal or log normal distribution for continuous variables. We also performed an unadjusted time trend analysis of illness severity assuming a Gamma distribution with log link and NICU-related costs with a log-linear model. We summarized NICU admissions, costs, and prevalence of complex diagnoses by gestational age. Gestational age stratification included extremely preterm (22–27 weeks), very preterm (28–33 weeks), late preterm (34–36 weeks), and term ( ≥ 37 weeks). Finally, to assess trends in healthcare costs, we performed an interrupted time series analysis. We a-priori identified discharges for the calendar year 2020 as the interruption period, representing the unique period of COVID-19 and its impacts on the health system. Because NICU-related costs in 2020 were clearly higher than other years, we compared the trend in geometric mean NICU-related costs pre-2020 with the trend in geometric mean NICU-related costs post-2020 using a log-linear interrupted time series (ITS) approach, ignoring NICU-related costs in 2020. Our ITS model included an effect for a pre-2020 slope estimate, an effect for a stepwise change in model intercept at the point of interruption, and an effect for a post-2020 slope estimate. We performed ITS modeling for the entire cohort as well as by gestational age stratification. All statistical analyses were performed using SAS v9.4 (Cary, NC). P values less than 0.05 were considered statistically significant.
Results
Cohort trends
A total of 234,571 infants were admitted to NICUs across 39 US children’s hospitals between 2017 and 2022. Demographic and clinical characteristics are summarized in Table 1. Across the 6-year study period, there were significant changes in the gestational age at birth distribution (p < 0.001). The proportion of infants with unknown gestational age declined from 18.1 to 10.9%. When evaluating absolute numbers for NICU admission across known gestational ages, admissions increased by 10.3% for extremely preterm infants (from 2753 to 3037), 16.0% for very preterm infants (from 5711 to 6626), and 17.8% for late preterm infants (from 7265 to 8556). Term infants remained the largest single category of admissions by volume, averaging 45% annually. The sex distribution remained stable, with approximately 55.7% of infants identified as male. There were statistically significant changes in documented race and ethnicity (p < 0.001), with slight increases in Hispanic infants (16.3% in 2017 to 18.8% in 2022) and decreases in the proportion of infants with unknown race/ethnicity (9.0–6.1%). The complexity of the NICU population also increased. Infants without complex chronic conditions (CCC) declined from 53.4% in 2017 to 49.1% in 2022, while those with ≥2 CCCs increased from 16.9% to 18.2% and infants with ≥4 CCCs rose from 4.7% in 2017 to 5.7% in 2022. Overall, infants with ≥1 CCCs increased from 46.6% in 2017 to 50.9% in 2022 (p < 0.001). Table 2 summarizes the prevalence of medically complex diagnoses by gestational age and CCC domain. The most frequent CCC diagnoses were in the neonatal, cardiovascular, and gastrointestinal domains. Cardiovascular diagnoses were the most prevalent CCC category among very preterm (14.5%), late preterm (11.8%), and term infants (14.2%). Among infants born very preterm, gastrointestinal and respiratory CCC diagnoses increased significantly (p < 0.001), data not shown. Among late preterm and term infants, the prevalence of renal and urologic conditions rose over the study period (p < 0.001), data not shown. Illness severity, measured by the adapted H-RISK score, rose from a mean of 1.14 (SE: 0.01) to 1.24 (SE: 0.01) (p < 0.001).
Outcome trends
For admissions ≥31 days, hospital length of stay (LOS) (range 21.6–24.3%) and NICU-specific LOS (range 17.2–19.5%) increased across the study period (p < 0.001) (Table 1). The proportion of infants admitted for fewer than 7 days in the NICU declined from 45.8 to 40.6% over time. Discharge disposition remained stable over the study period, with approximately 89.2% of infants discharged home each year and in-hospital mortality ranged from 3.5 to 3.7% across all years, data not shown.
NICU cost trends
Total NICU-related costs increased significantly between 2017 and 2022 (p < 0.001) (Table 1). Median cost per NICU hospitalization rose from $24,383 (IQR: $7670–$73,574) in 2017 to $29,234 (IQR: $9953–$85,152) in 2022. Median cost per NICU day also increased, from $3332 to $3779. Correspondingly, mean cost per NICU hospitalization rose from $73,633 (95% CI: 72,094, 75,171) in 2017 and $95,512 (95% CI: 93,570, 97,454). NICU costs represented between 18.2% and 28.1% of total hospital costs. Figure 2 summarizes the distribution of costs by gestational age over the 6-year study period. When stratified by gestational age, extremely preterm infants, though only 7.0% of admissions, accounted for 28.9% of total NICU costs, with a median cost per hospitalization of $275,208 (IQR: $75,232–$462,152) (Table 3). In contrast, term infants comprised 44.7% of admissions and 24.0% of costs, with a substantially lower median cost of $15,449 (IQR: $6,782–$41,746). NICU costs did not significantly change over time for term infants.
Probability distribution of total NICU hospitalization costs by gestational age.
ITS analysis revealed that NICU-related costs were relatively stable pre-pandemic (p = 0.491), there was a small but significant change in the model intercept ($38,646 [observed] vs $37,055 [projected], p = 0.031) after 2020 followed by an increase in NICU costs post-pandemic (p < 0.001) (Fig. 3a). Gestational age subgroup analysis suggested varied patterns across GA categories with the increased costs driven by the extremely preterm and term infants (Fig. 3b).
Interrupted time-series analysis of NICU hospitalization costs overal (a) and stratified by gestational age (b).
Discussion
This analysis of NICU admissions across US children’s hospitals reveals an increase in overall admissions, higher acuity scores, and rising hospitalization costs between 2017 and 2022. The findings demonstrate increasing medical complexity, shifting demographic patterns, longer hospitalizations, and rising costs, trends that carry important implications for neonatal care delivery, planning, and policy. Rather than asserting broad policy implications, our results highlight the need for future population-based studies that evaluate NICU care delivery across hospital types, settings, and patient case mix.
Demographic and clinical shifts
Over the 6-year study period, we observed notable shifts in the clinical and demographic profile of NICU admissions. The proportion of infants admitted with complex chronic conditions (CCC) increased, as did median illness severity scores. While full-term infants have traditionally been underrecognized in NICU cost studies, they consistently include nearly half of all NICU admissions in our cohort. Though race and ethnicity distributions shifted significantly, the decline in the proportion of infants with unknown race/ethnicity suggests this may be driven by improved data capture rather than true population change. Likewise, a reduction in unknown gestational age, from 18.1 to 10.9%, improved the precision of gestational age-based analyses. Among infants with known gestational age, the number of admissions increased by 10.3% for extremely preterm, 16.0% for very preterm, and 17.8% for late preterm infants, pointing to both enhanced reporting and increased population-level need. The significant increases in NICU admissions for late preterm infants, alongside the sustained need for complex medical care across all gestational age groups, further emphasize the necessity for adaptive healthcare strategies to meet the changing demands of neonatal care. The NICU population is becoming increasingly medically complex, and improvements in clinical documentation have enhanced our ability to track these trends.
Outcome trends and hospital utilization
Longer hospitalizations and rising medical complexity were also evident. Across the study period, the proportion of short-stay NICU hospitalizations ( < 7 days) declined over time, while the volume of infants requiring longer stays ( > 31 days) increased. These findings suggest a growing cohort of infants requiring prolonged and intensive medical care, likely reflecting improved survival of high-risk infants, evolving clinical practices, and shifting thresholds for NICU admission [26]. Admissions from outside hospitals comprised 69% of the cohort, and most infants (89%) were discharged home, while 6% required transfer and 3.6% died in-hospital. The distribution of medically complex diagnoses also shifted: cardiovascular, gastrointestinal, and respiratory conditions became more prevalent across gestational age groups. Taken together, these outcome patterns indicate increased demand for high-resource neonatal care and reinforce the critical role of children’s hospital NICUs in managing complex, long-stay admissions.
Cost implications and financial burdens
The financial implications of these trends are sizeable as NICU hospitalizations represent a significant portion of pediatric inpatient expenditures. While extremely preterm infants accounted for only 7% of admissions, they represented 29% of NICU-related costs, with median hospitalization costs reaching $275,208. Term infants, while less costly on average ($15,449), represented 45% of admissions and accounted for nearly one-quarter of NICU-related costs—highlighting a previously underappreciated source of spending. NICU costs per hospitalization and per day rose steadily across the study period, and the average cost per hospitalization in 2021 and 2022 exceeded pre-pandemic projections. Interrupted time series analysis confirmed a significant shift in cost trajectories following the COVID-19 pandemic, particularly for extremely preterm and term infants.
Comparatively, recent literature corroborates the high financial demands of neonatal intensive care, especially for preterm and medically complex infants. A 2021 study reported that NICU admissions accounted for 18% of infant hospitalizations, with an average spending of $71,158 per admission, and costs ranging from $4488 to $161,929, reflecting the variability in care complexity [27]. Another study focusing on preterm infants born at or before 30 weeks’ gestation found a median NICU admission cost of $77,132.90, with interquartile ranges between $48,338 and $126,680 [28]. Furthermore, children with medical complexity (CMC), though representing less than 1% of the pediatric population, are responsible for a substantial portion of healthcare expenditures, indicating that CMCs account for almost one-third of all child health spending, with rehospitalization comprising the largest proportion of subsequent costs (27.2%) [29].
These studies align with our findings, highlighting the significant financial resources required for the care of medically complex infants and confirms this population continues to drive pediatric hospital resource use. The continued increase in NICU admissions among infants with chronic conditions calls for investment in integrated care models (i.e., care coordination programs) that bridge inpatient and outpatient services to ensure smoother transitions post-discharge and address the social determinants shaping neonatal outcomes [30]. Rising NICU costs, particularly among high-acuity and term infants, highlight the critical need for hospital-level resource planning and greater attention to the economic impact of neonatal care.
Importantly, the interpretation of increased admissions and costs should be contextualized within the distinction between utilization and population-level need. While the economic concept of “demand” refers to actual use, this may not equate to the health system’s optimal or equitable provision of care. Moreover, although we observed rising direct hospital costs, these estimates are derived from charge data and do not reflect total family spending, reimbursement, or out-of-pocket expenses. As such, we cannot draw conclusions about family financial burden, and future studies using patient-reported outcomes and payer-level data are needed to assess these dimensions.
While NICUs have traditionally been associated with the care of preterm infants, our data indicate that full-term infants account for nearly half of admissions, underscoring the diverse and evolving nature of neonatal critical care needs at children’s hospitals. This finding is particularly relevant for term infants with complex conditions, for whom cost estimates have historically been limited. Additionally, this study provides a novel contribution by examining NICU costs as a proportion of total children’s hospital expenditures, offering a critical perspective on the financial impact of neonatal intensive care relative to overall hospital costs at US children’s hospitals. This lens is important given the increasing regionalization of neonatal care and closure of community pediatric beds, resulting in a significant shift in the care of term and late-preterm infants towards Children’s Hospital NICUs. These data provide important insights into high-acuity neonatal care that complements, rather than duplicates, national estimates by providing NICU-specific cost data for infants admitted to tertiary care hospitals. Understanding how admissions, complexity, and costs are evolving within children’s hospitals remains a critical step in assessing resource needs and ensuring equity in neonatal outcomes.
Limitations
Our study has a few limitations. Research using administrative data has some degree of error and missingness of patient clinical data. For example, there were many encounters in the PHIS database where the infant had an unknown gestational age and while the change in unknown GA decreased by 7% over the study period, the unknown GA group may account for some of the trends seen in the gestational age categories during the study period. Secondly, our data is specific to children’s hospitals and likely underestimates NICU admissions overall, and the characteristics of neonatal admission in non-children’s hospitals may be different given the variation in level of care [12]. The objective of this study, however, was not to estimate national NICU costs but to characterize trends in a highly specialized subgroup that is underrepresented in other datasets. Lastly, given our study period covers the year(s) of the COVID-19 pandemic, its impact likely influenced some results. Even so, the data is still clinical meaningful as it provides trend information before and after the global pandemic. Further exploration is warranted to better identify the mechanisms driving higher costs during the pandemic that is not related to higher volumes of admissions.
Conclusion
This study provides an updated analysis of NICU admissions and costs in U.S. children’s hospitals. Unlike prior research focused primarily on preterm infants, we show that term infants account for nearly one-quarter of NICU hospitalization costs, highlighting a critical gap in existing estimates. The substantial resources required to care for term infants with complex conditions underscore the need to include this population in future economic evaluations of neonatal care. Although this study did not explicitly examine the role of social determinants of health, our findings point to the importance of future work linking hospital- and population-level datasets to evaluate how factors such as insurance coverage, race/ethnicity, and neighborhood context shape variation in care, outcomes, equity, and costs. While NICU care is resource-intensive, it is important to note that most infants survive and experience positive developmental outcomes. Additionally, NICUs may contribute to overall hospital margin and sustainability, particularly within children’s hospitals; however, the financial implications of neonatal care must be interpreted within an ethical framework that prioritizes infant and family well-being, rather than revenue generation. Ultimately, these findings raise important questions for hospital leaders and researchers working to improve the efficiency, equity, and long-term sustainability of neonatal intensive care.
Data availability
The data that support the findings of this study may be available from Children’s Hospital Association, but restrictions apply to the availability of these data, which were used under license for the current study, and so are not publicly available.
References
Kim Y, Ganduglia-Cazaban C, Chan W, Lee M, Goodman DC. Trends in neonatal intensive care unit admissions by race/ethnicity in the United States, 2008–2018. Sci Rep. 2021;11:23795. https://doi.org/10.1038/s41598-021-03183-1.
March of Dimes. Peristats: United States Perinatal Data Snapshots. Accessed September 29, 2014, http://www.marchofdimes.org/Peristats/pdflib/999/pds_99_1.pdf.
Vance AJ, Henderson J, Yin Z, Costa DK, Meghea C. Healthcare utilization and costs among commercially insured infants with and without medically complex conditions. Adv Neonatal Care. 2025;25:138–48. https://doi.org/10.1097/ANC.0000000000001251.
Speer RR, Schaefer EW, Aholoukpe M, Leslie DL, Gandhi CK. Trends in costs of birth hospitalization and readmissions for late preterm infants. Children (Basel). 2021;8 https://doi.org/10.3390/children8020127.
Sharma D, Murki S. Making neonatal intensive care: cost effective. J Matern Fetal Neonatal Med. 2021;34:2375–83. https://doi.org/10.1080/14767058.2019.1660767.
Waitzman NJ, Jalali A, Grosse SD. Preterm birth lifetime costs in the United States in 2016: an update. Semin Perinatol. 2021;45:151390. https://doi.org/10.1016/j.semperi.2021.151390.
Hannan KE, Bourque SL, Palmer C, Tong S, Hwang SS. Prevalence and predictors of medical complexity in a national sample of VLBW infants. Hosp Pediatr. 2021;11:525–35. https://doi.org/10.1542/hpeds.2020-004945.
Kieran E, Sara R, Claydon J, Hait V, de Salaberry J, Osiovich H, et al. Outcomes of neonates with complex medical needs. Adv Neonatal Care. 2019;19:275–84. https://doi.org/10.1097/anc.0000000000000639.
Pineda R, Kati K, Breault CC, Rogers EE, Mack WJ, Fernandez-Fernandez A. NICUs in the US: levels of acuity, number of beds, and relationships to population factors. J Perinatol. 2023;43:796–805. https://doi.org/10.1038/s41372-023-01693-6.
Bettegowda VR, Lackritz E, Petrini JR. Epidemiologic Trends in Perinatal Data. In: Oh W, editor., Toward Improving the outcome of pregnancy III. March of Dimes; 2010.
Brown CC, Moore JE, Tilford JM. Rates of preterm birth and low birthweight: an analysis of racial and ethnic populations. Health Aff (Millwood). 2023;42:261–7. https://doi.org/10.1377/hlthaff.2022.00656.
Boghossian NS, Geraci M, Phibbs CS, Lorch SA, Edwards EM, Horbar JD. Trends in resources for neonatal intensive care at delivery hospitals for infants born younger than 30 weeks’ gestation, 2009–2020. JAMA Netw Open. 2023;6:e2312107 https://doi.org/10.1001/jamanetworkopen.2023.12107.
Vance AJ, Henderson J, Yin Z., Costa DK, Meghea C. Healthcare Utilization and Costs Among Commercially Insured Infants With and Without Medically Complex Conditions. Advances in Neonatal Care. 2025;25:138–148.
Martin J, Osterman MK. Increases in neonatal intensive care admissions in the United States, 2016–2023. NCHS Data Brief. 2025; https://doi.org/10.15620/cdc/174581.
Markham JL, Hall M, Stephens JR, Richardson T, Gay JC. A pediatric hospital medicine primer for performing research using administrative data. Hosp Pediatr. 2022;12:e319–e325. https://doi.org/10.1542/hpeds.2022-006691.
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. Strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. BMJ. 2007;335:806–8. https://doi.org/10.1136/bmj.39335.541782.AD.
Feudtner C, Feinstein JA, Zhong W, Hall M, Dai D. Pediatric complex chronic conditions classification system version 2: updated for ICD-10 and complex medical technology dependence and transplantation. BMC Pediatr. 2014;14:199 https://doi.org/10.1186/1471-2431-14-199.
Rasooly IR, Shults J, Guevara JP, Feudtner C. State variation in posthospital home nursing for commercially insured medically complex children. Pediatrics. 2020;146 https://doi.org/10.1542/peds.2019-2465.
Berry JG, Ash AS, Cohen E, Hasan F, Feudtner C, Hall M. Contributions of children with multiple chronic conditions to pediatric hospitalizations in the United States: a retrospective cohort analysis. Hosp Pediatr. 2017;7:365–72. https://doi.org/10.1542/hpeds.2016-0179.
Noelke C, McArdle N, Baek M, Huntington N, Huber R, Hardy E, et al. Child Opportunity Index 2.0 Technical Documentation. 2020. Accessed 05/15/ 2024. https://www.diversitydatakids.org/research-library/research-report/coi-30-technical-documentationdiversitydatakids.org/researchlibrary/research-brief/how-we-built-it.
King BC, Richardson T, Patel RM, Lee HC, Bamat NA, Hall M, et al. Prioritization framework for improving the value of care for very low birth weight and very preterm infants. J Perinatol. 2021;41:2463–73. https://doi.org/10.1038/s41372-021-01114-6. Oct.
Shwartz M, Young DW, Siegrist R. The ratio of costs to charges: how good a basis for estimating costs? Inquiry. 1995;32:476–81.
Hall M, Duda P. Comparing cost methodologies: what’s available in PHIS. Accessed May 1, 2023, https://www.childrenshospitals.org/Member-Center/Groups-Products/PHIS/Resources/Webinars/Research/Comparing-Cost-Methodologies-Nov-2018.
Keren R, Luan X, Localio R, Hall M, McLeod L, Dai D, et al. Prioritization of comparative effectiveness research topics in hospital pediatrics. Arch Pediatr Adolesc Med. 2012;166:1155–64. https://doi.org/10.1001/archpediatrics.2012.1266.
US Bureau of Labor Statstics. Consumer Price Index. Accessed August 2, 2022, https://www.bls.gov/cpi/.
King BC, Richardson T, Patel RM, Lee HC, Bamat NA, Patrick SW, et al. Cost of clinician-driven tests and treatments in very low birth weight and/or very preterm infants. J Perinatol. 2021;41:295–304. https://doi.org/10.1038/s41372-020-00879-6.
Valencia Z, Aditi Sen K. NICU Admissions and Spending Increased Slightly from 2017–2021. Health Care Cost Institue. Accessed 12-05 2024, https://healthcostinstitute.org/hcci-originals-dropdown/all-hcci-reports/nicu-use-and-spending-1.
Rolnitsky A, Unger S, Urbach D, Bell CM. The price of neonatal intensive care outcomes - in-hospital costs of morbidities related to preterm birth. Front Pediatr. 2023;11:1068367 https://doi.org/10.3389/fped.2023.1068367.
Cohen E, Berry JG, Camacho X, Anderson G, Wodchis W, Guttmann A. Patterns and costs of health care use of children with medical complexity. Pediatrics. 2012;130:e1463–70. https://doi.org/10.1542/peds.2012-0175.
Vance AJ, Benjamin A, Hsu J, Berry JG. Care coordination programs for infants with complex conditions: a systematic review. Pediatrics. 2023;152. https://doi.org/10.1542/peds.2022-061083.
Author information
Authors and Affiliations
Contributions
AJV, TR, JGK conceptualized and designed the study, drafted the initial manuscript, interpreted findings, and revised the manuscript. TR completed data extraction and conducted analysis. BK, JL, KL, AL, HL, TL, RP interpreted findings, critically reviewed and revised the manuscript. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
JGK received funding from the National Institutes of Health (K12TR004374). AJV was supported by an Internal Mentored Award from Henry Ford Health. All other authors have indicated they do not have any conflicts of interest relevant to this article to disclose.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Article Summary This article investigated trends in NICU admissions, clinical demographics, and costs among U.S. children’s hospitals over a six-year period from 2017 - 2022.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Vance, A.J., Richardson, T., King, B. et al. Trends in admissions and costs for neonatal intensive care in US children’s hospitals, 2017–2022. J Perinatol (2026). https://doi.org/10.1038/s41372-026-02619-8
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41372-026-02619-8