Abstract
Background
Attention-deficit/hyperactivity disorder (ADHD) has been linked to unhealthy dietary patterns, but its association with ultra-processed food (UPF) consumption remains underexplored. This study assessed the association between ADHD and UPF intake among children.
Methods
Data were obtained from the 2015–2016 Israeli Kids Health and Nutrition Survey, a nationally representative cross-sectional study. Parents/guardians provided demographic, health, and dietary information via face-to-face interviews. Anthropometrics were measured, and dietary intake was assessed using a 24-hour recall. UPF consumption (grams/day and % of total food weight) was classified by the NOVA system and categorized by the median. Adjusted logistic and linear regressions examined associations between ADHD and UPF.
Results
Of 1135 children aged 6–11 years included, 111 had physician-diagnosed ADHD. Median UPF intake was 342.9 grams/day and 16.7% of total food weight. Adjusted for age, sex, socioeconomic status, and intakes of energy, dietary fiber, and alpha-linolenic acid, ADHD was significantly associated with above-median UPF consumption, as grams/day (OR = 1.622, 95% CI: 1.010–2.604) and as % of total food weight (OR = 1.652, 95% CI: 1.058–2.578). Linear regression models yielded similar associations. No differences in UPF intake were found by stimulant treatment status.
Conclusion
ADHD is associated with higher UPF consumption, with potential influences in either direction.
Impact
-
This study is the first to demonstrate an adjusted association between physician-diagnosed attention-deficit/hyperactivity disorder (ADHD) and higher consumption of ultra-processed foods (UPFs) in children, both in absolute food weight and as a percentage of total food weight intake, independent of stimulant treatment status.
-
Findings add to the literature by moving beyond general unhealthy dietary patterns to focus on UPF intake, a growing public health concern.
-
The observed association may reflect ADHD-related eating behaviors, potential contributions of UPF constituents to ADHD-related symptoms, or both, with implications for ADHD care and child public health.
Similar content being viewed by others
Introduction
Attention-deficit/hyperactivity disorder (ADHD) is one of the most common neurodevelopmental disorders in children, with prevalence steadily increasing in recent years, posing a significant public health concern1. This disorder significantly impairs daily functioning, development, and overall well-being2,3. Previous studies have further demonstrated that ADHD is associated with an increased prevalence of eating disorders, disordered eating behaviors, and unhealthy eating patterns4,5,6. For example, a systematic review and meta-analysis found that ‘unhealthy’ dietary patterns high in refined sugars and saturated fats were associated with greater odds of ADHD, whereas ‘healthy’ patterns rich in fruits and vegetables appeared protective7. Similarly, case–control studies have observed that children with ADHD tend to consume fewer fruits, vegetables, and dairy products but more refined grains and sugary snacks compared to peers without ADHD8. These findings underscore the relevance of overall diet quality to ADHD risk and management.
One of the increasingly concerning dietary exposures in modern diets is the consumption of ultra-processed food (UPF)9. The UPF category, outlined in the NOVA food classification system10,11, is defined as food or beverage formulations resulting from extensive industrial processing and designed to be highly profitable, with low-cost ingredients, extended shelf-life, and appealing taste. These products frequently contain high levels of artificial additives, preservatives, and synthetic ingredients, with little to no whole food components12,13. High UPF intake has been shown to adversely affect overall diet quality, including increased consumption of added sugars, sodium, and saturated fats, and reduced intake of dietary fiber, protein, and essential micronutrients14. Emerging evidence highlights health implications in pediatric populations, with high UPF intake associated with cardiometabolic risk factors, such as increased adiposity, overweight/obesity, insulin resistance, and metabolic-associated fatty liver disease15,16,17,18. UPF exposure has also been linked to a higher prevalence of allergic conditions19, and artificial additives, commonly found in UPF, have been implicated in behavioral disturbances in children20. In adult populations, high consumption of UPF is similarly associated with elevated cardiovascular disease risk and adverse cardiometabolic outcomes21, as well as higher rates of common mental health disorders like depression22. Recent reviews further implicate UPF-heavy diets in autoimmune-mediated inflammation (e.g., increased inflammatory bowel disease activity)23 and in increased incidence of various cancers24. Consistent with these findings, Monteiro et al. reported in a comprehensive Lancet series that UPF-rich diets contribute to the burden of chronic diseases across multiple organ systems in adults25.
The potential association between ADHD and UPF intake may reflect bidirectional influences. On one hand, ADHD-related traits such as impulsivity and sensory sensitivity may predispose individuals to greater consumption of ultra-processed products26. On the other hand, UPF, particularly those high in additives or refined sugars, may contribute to the exacerbation of neurobehavioral symptoms27,28.
Despite the high and increasing prevalence of both ADHD and UPF consumption, their broad implications, and the well-documented associations between ADHD and unhealthy eating behaviors and attitudes, the relationship between ADHD and UPF intake remains understudied.
Notably, focusing on UPF offers a complementary perspective beyond traditional nutrient-based diet assessments. The extent of industrial processing itself may impact health in ways that nutrient composition alone cannot capture. In fact, emerging evidence indicates that UPF can influence appetite regulation and gut microbiota in ways independent of their vitamin or caloric content29. Given the rising consumption of UPF globally and their unique health implications25, examining ADHD in relation to UPF intake (rather than only overall diet quality) is particularly warranted.
Therefore, the aim of the present study was to examine this association in a nationally representative survey of children, adjusting for potential confounders, as it holds considerable importance for public health and health promotion. Additionally, the study aimed to compare UPF consumption between stimulant-treated and non–stimulant-treated children with ADHD.
Methods
Study design, sampling, and procedure
This cross-sectional study was based on data from the 2015–2016 Israeli Kids Health and Nutrition Survey Ages 2–11 Years (1st Rav-Mabat Kids Survey), conducted by the Israel Center for Disease Control in collaboration with the Nutrition Division of the Ministry of Health and the Central Bureau of Statistics. The survey design and operation were detailed elsewhere30.
The survey sample was generated from the 2014 Population Registry and included children aged 2–11 years from all religions in Israel. The sample was generated using a two-stage cluster design. In the first stage, statistical areas were sampled according to geographic strata. In the second stage, 15 children were sampled in each statistical area. The sampling covered 135 localities across seven districts. Of the initial sample, 1792 children (90%) actively participated in the survey, while 199 were excluded due to a lack of parental/guardian informed consent30.
The survey included face-to-face interviews conducted by specially trained personnel with one of the parents/guardians, in the presence of the child, in their home. The interviews collected demographic information, health status, and dietary intake data, and were conducted in Hebrew or Arabic, according to the interviewee’s preference. The survey questionnaire underwent pretesting and construct validity assessment. Furthermore, standardized procedures and continuous monitoring during data collection and entry ensured accuracy and maintained data quality30.
The study population for the current analysis included school-aged children, 6–11 years old, who participated in the 1st Rav-Mabat Kids Survey (n = 1188)30. This age range was selected to reflect elementary school children. Because ADHD diagnosis in preschool-aged children is more complex due to developmental variability31, restricting the analytic sample to ages ≥6 years was intended to reduce misclassification.
Exclusions applied to those with unknown ADHD status (n = 34), incomplete dietary intake information (n = 9), or implausible energy intake (less than 500 kcal/day or more than 4500 kcal/day, n = 12). A child could have been excluded for more than one of these reasons (Supplementary Fig. S1). Socio-demographic characteristics of included (n = 1135) vs. excluded (n = 53) participants were examined, with no significant differences found for age, sex, population group, or SES (p > 0.05 for all; data not shown).
ADHD status and stimulant treatment (independent variables)
The ADHD status of the children was determined based on parental/guardian self-report. Participants were asked if their child had ever been diagnosed with ADHD by a physician. Based on their responses, the children were categorized into ADHD and non-ADHD groups.
For children with ADHD, parents/guardians were asked whether the child was receiving regular pharmacological treatment, defined as use on at least five days per week. Those responding affirmatively were requested to present the medication to the interviewer for verification. Children verified as receiving stimulant medication were classified into the stimulant-treated group. The medications reported included methylphenidate hydrochloride in various formulations: Concerta (18 mg, 36 mg, 54 mg), Ritalin (10 mg tablets), Ritalin Sustained-Release (20 mg tablets), and Ritalin Long-Acting (10 mg, 20 mg, 30 mg, 40 mg modified-release capsules).
UPF consumption (dependent variable)
Dietary intake was assessed using the 24-h recall method, a widely accepted tool in nutritional epidemiology, which has been validated extensively across diverse populations32,33. Through structured interviews, information on the foods and beverages consumed by the children within the previous 24 h was recorded. To improve the accuracy and validity of reporting and quantification, the recall interviews were supported by visual aids, including a food and portion size guide with life-size images. Nutrient intakes were then calculated according to the Israeli food and nutrient database using the Tzameret software program34. Foods and beverages were classified as UPF according to the NOVA food classification system, with NOVA category 4 denoting UPF10,11. This method is widely recognized as both valid and reliable for categorizing foods based on their extent and purpose of industrial processing35,36. It has been endorsed by global organizations, such as the Food and Agriculture Organization and World Health Organization (WHO), for its utility in assessing dietary patterns, informing dietary guidelines, and examining health implications12,37. Its standardized framework ensures comparability across studies, establishing it as a reliable approach for examining the role of UPF in diet and health38.
UPF consumption was primarily characterized by weight, expressed as grams/day and as the percentage of total food weight/day. Intake was analyzed both categorically, with dichotomization at the median (>median vs. ≤median),39,40, and continuously. The weight-derived measures served as the dependent variables in this study, as the potential harm of UPF may also stem from products with low caloric density13,41. Additionally, UPF intake was described by caloric contribution (kcal/day and percentage of total daily energy).
Potential confounders
Sociodemographic variables
Age (years) and sex (boy, girl) were obtained from interview responses. Socioeconomic status (SES) was categorized according to the 2014 National Insurance Institute poverty line as medium-high (above the poverty line) or low (below the poverty line), based on reported monthly income and family size42.
Anthropometric measurements
Height and weight were measured using standard equipment by well-trained personnel. Body mass index (BMI) z-scores, presented as standard deviations (SDs), were calculated, and weight status was categorized according to WHO growth standards: underweight (<−2 SD), normal weight (≥−2 and <1 SD), overweight (≥1 and <2 SD), and obese (≥2 SD)43.
Energy and nutrient intakes
These were derived from the 24-h recall questionnaires. Total energy intake was reported in kcal/day, while macronutrients, sugars, and saturated fat were expressed as percentages of total energy intake and as grams/day. Daily dietary fiber, alpha-linolenic acid (omega-3), and sodium intakes were presented in grams/1000 kcal. These nutrients were used as indicators of overall diet quality. Dietary fiber intake is widely regarded as a marker of a healthy, high-quality diet, as higher fiber consumption typically reflects greater intake of fruits, vegetables, and whole grains44. Similarly, alpha-linolenic acid reflects the quality of fat intake, with higher levels characteristic of diets rich in nutrient-dense plant foods45. Conversely, excessive sodium intake is commonly associated with low-quality dietary patterns and has been inversely correlated with adherence to dietary guidelines46. Accounting for these nutrients allowed for control of general diet quality differences among participants, thereby enabling isolation of the specific associations of interest.
Health behaviors
Participants who performed any physical activity (walking, cycling, running, etc.) for at least an hour per day, on average, were defined as “yes” for physical activity as recommended. Sleep duration was classified as recommended if it fell within the range of 9–12 h per day, on average47.
Statistical analyses
Statistical analyses were conducted using SAS software version 9.4 (SAS Institute, North Carolina). Descriptive statistics characterized the study population by ADHD status. Continuous variables were tested for normality using the Kolmogorov–Smirnov test; normally distributed variables were reported as means and SDs, and non-normally distributed variables as medians and interquartile ranges. Categorical variables were presented as frequencies and percentages. The descriptive statistics were weighted for the total Israeli population by weighting factors provided by the Central Bureau of Statistics, based on population group, geographic residential area, dietary recall day, and sex linked with age groups30.
Comparisons of study participants regarding sociodemographic, anthropometric, and dietary characteristics were conducted according to ADHD status, using t-tests or Mann–Whitney U tests for continuous variables (depending on distribution) and chi-square tests for categorical variables. Among children with ADHD, additional comparisons were made between stimulant-treated and non-stimulant-treated participants.
Multivariable logistic regression models were used to examine the associations between ADHD and above-median daily UPF consumption (grams/day and percentage of total food weight/day). In addition, linear regression models were conducted with continuous UPF variables as the dependent outcomes. Model A was adjusted for all sociodemographic variables, considered basic (core) confounders. Model B was further adjusted for total daily energy intake, given its established importance in nutritional epidemiology. Model C additionally included other variables associated with ADHD in the bivariate analysis (p < 0.05).
Collinearity among variables in the models was examined using Spearman correlation, with a threshold of ≥0.5.
In a sensitivity analysis, logistic regression examined the associations between ADHD and the highest versus lowest quartiles of UPF consumption (Q4 vs. Q1).
In addition, within the ADHD group, children were classified as stimulant-treated vs. non-stimulant-treated. Based on the group-specific median of UPF consumption (grams/day and percentage of total food weight/day), multivariable logistic and linear regression analyses were conducted to examine the association between stimulant treatment and UPF consumption. These analyses were performed using the same modeling strategy and covariate adjustments described above.
Participants with missing data in any of the variables included in the regression models were excluded from the multivariable analyses.
Results from the multivariable logistic regression models were presented as odds ratios (OR) with 95% confidence intervals (CI). Results from the linear regression models were expressed as regression coefficients (β) with 95% CI.
All tests were two-tailed with a significance level of p < 0.05, unless otherwise stated.
Ethics
The 1st Rav-Mabat Kids Survey received approval from the Ethics Committee of the Israeli Ministry of Health (approval number: MOH 043-2012). Written informed consent was obtained from the parents or legal guardians of all participants30.
Results
Characteristics of study participants
A total of 1135 children (51.7% boys, median age 8.4 years, approximately 41% with low SES) were included in the analysis. Of these, 111 (10.5%) were classified in the ADHD group (Table 1). In the overall sample, median total energy intake was 1474.5 kcal/day, with 53.2%, 30.2%, and 15.1% derived from carbohydrates, fat, and protein, respectively. The median BMI z-score was −0.13 SD, and approximately 21% of participants had overweight or obesity. Median UPF intake was 342.9 grams/day and 16.7% of total food weight, while in caloric terms it was 681.5 kcal and 47.3% of total daily energy intake.
Comparison by ADHD status
Characteristics of children with and without ADHD are presented in Table 1. The ADHD group was older and had a higher proportion of boys (p < 0.05 for all). No significant difference was observed for SES. Adherence to physical activity and sleep recommendations did not significantly differ between groups. BMI z-scores and weight status were similar between groups. Total daily energy intake was higher among children with ADHD, although not statistically significant (p = 0.06). Daily dietary fiber intake was lower (p = 0.04) and alpha-linolenic acid intake was higher (p = 0.02) among children with ADHD, with no other differences in daily dietary intake.
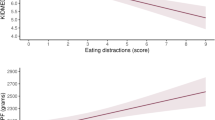
For UPF intake expressed as grams/day, the median in the ADHD group (419.0 grams/day) was significantly higher than in the comparison group (334.0 grams/day, p = 0.006). When categorized by the overall sample median, 65.7% of children with ADHD consumed above-median daily UPF weight intake, compared with 48.1% of children without ADHD. Similarly, when UPF intake was expressed as a percentage of total daily food weight, median values were higher in the ADHD group compared with the non-ADHD group (20.8% vs. 16.4%, respectively; p = 0.003). When categorized by the 50th percentile of total daily food weight, 65.3% of children with ADHD consumed above the median percentage, compared with 48.3% of children without ADHD (p = 0.007) (Fig. 1).
a Ultra-processed food consumption (grams/day). b Proportion of participants with ultra-processed food consumption (grams/day) above the median. c Ultra-processed food consumption (grams as a percentage of total food weight). d Proportion of participants with ultra-processed food consumption (grams as a percentage of total food weight) above the median. Calculated with the application of sample weights of the 2015–2016 Israeli Kids Health and Nutrition Survey (1st Rav-Mabat Kids Survey). Abbreviations: ADHD attention-deficit and hyperactivity disorder, UPF ultra-processed food.
Multivariable models
In the multivariable analyses, Model A was adjusted for age, sex, and SES, while Model B was further adjusted for total daily energy intake. Model C was additionally adjusted for dietary fiber and alpha-linolenic acid intake. No substantial collinearity was observed among the variables included in the models. In the logistic regression analyses (Fig. 2), children with ADHD consistently showed significantly higher odds of above-median UPF consumption across all models. In the fully adjusted model (Model C), the odds ratio was 1.622 (95% CI: 1.010, 2.604; p = 0.045) for daily UPF intake in grams and 1.652 (95% CI: 1.058, 2.578; p = 0.027) for UPF percentage of total food weight. Similar associations between ADHD and higher UPF intake were observed in the linear regression analyses (Table 2). In Model C, ADHD was associated with an additional 57.285 grams/day of UPF consumption (95% CI: 5.904, 108.665; p = 0.029) and with a 3.837 percentage-point increase in UPF as a proportion of total food weight (95% CI: 1.201, 6.474; p = 0.004).
a Outcome: above-median ultra-processed food consumption, expressed as weight ( > 342.9 grams/day). P-values: Model A = 0.012, Model B = 0.037, Model C = 0.045. b Outcome: above-median ultra-processed food consumption, expressed as a percentage of total food weight ( > 16.7%). P-values: Model A = 0.008, Model B = 0.015, Model C = 0.027. Model A: adjusted for age, sex, and socioeconomic status. Model B: adjusted for age, sex, socioeconomic status, and total energy intake. Model C: adjusted for: age, sex, socioeconomic status, total energy intake, dietary fiber intake, and alpha-linolenic acid intake. Abbreviations: ADHD attention-deficit and hyperactivity disorder.
The sensitivity analysis yielded broadly similar results, with point estimates indicating a positive association between ADHD and UPF consumption in the highest compared with the lowest quartile (Supplementary Table S1). In selected models, the observed associations were of borderline statistical significance, possibly reflecting the smaller sample size (Table 1).
Comparison of ADHD participants by stimulant treatment status
Of the 111 participants with ADHD, 37 (33.3%) reported receiving regular stimulant treatment. No significant differences were observed between children according to stimulant treatment status in demographics, anthropometric measures, health behaviors, or nutritional intake (Table 3).
UPF consumption also did not differ significantly between the groups when expressed as weight, percent weight, energy, or percent energy. Multivariable logistic and linear regression analyses likewise showed no association between stimulant treatment and UPF consumption (Supplementary Table S2).
Discussion
Main findings
In this nationally representative sample of Israeli children, ADHD was associated with higher UPF intake when measured both as daily weight (grams/day) and as the percentage of total daily food weight. The associations persisted in analyses using continuous UPF variables and were largely consistent in the sensitivity analysis, supporting the robustness of the findings. No differences in UPF consumption were observed by stimulant treatment status among children with ADHD. To the best of our knowledge, this is the first study to examine the association between physician-diagnosed ADHD and UPF consumption in children, a contribution of particular importance given the high prevalence and significant implications of both.
Notably, the magnitude of the association was modest. In fully adjusted models, ADHD was associated with roughly 1.6-fold higher odds of high UPF intake and an average increase of about 57 grams of UPF per day. However, even a modest increase in UPF consumption could be meaningful given the prolonged duration of exposure across the lifespan, and the broad range of detrimental health outcomes associated with these products25.
ADHD prevalence and group characteristics
ADHD prevalence in the current study (10.5%) is higher than global estimates. An umbrella review of meta-analyses by Ayano et al. reported a worldwide prevalence of 8.0% (95% CI: 6.0–10.0%)48. Nevertheless, Israeli studies have consistently shown higher rates across a range of ages. Cohen et al., based on medical records of children aged 6–13 in Israel’s second-largest health fund, reported a prevalence of 12.3%, which increased with age (3.7% at age 6; 16% at age 11; 17.1% at age 13)49. Pinhas-Hamiel et al. reported a high prevalence of ADHD among Israeli adolescents (20.1%), based on a nationwide analysis of medical records50, further suggesting elevated rates in Israel compared with global estimates.
Other characteristics of the ADHD group in this study were a higher proportion of boys, in line with the existing literature51, and no significant difference in SES compared with the non-ADHD group. This lack of difference may reflect a counterbalance between evidence linking ADHD to lower SES52 and, conversely, greater awareness and access to diagnosis in higher SES groups53. In addition, no differences were observed between the ADHD group and the comparison group in overall macronutrient intake. Nevertheless, children with ADHD demonstrated a lower dietary fiber intake, a finding that may indicate poorer dietary quality. Additionally, a higher intake of alpha-linolenic acid was observed in the ADHD group, which may reflect greater awareness of its documented association with symptom regulation54. Both groups’ macro- and micronutrient intakes were within the acceptable distribution ranges according to the Dietary Reference Intakes55.
To note, no differences were observed between the ADHD and comparison group in either total daily caloric intake from UPF or the percentage of UPF calories relative to overall energy intake. However, a significant difference was noted in UPF consumption when measured by food weight. This apparent discrepancy may be explained by the fact that not all UPFs are calorically dense; rather, they vary significantly in energy density. Some formulations contain ingredients with little or no caloric contribution, such as artificial colorants, preservatives, or non-nutritive sweeteners. In addition, many ultra-processed products are specifically manufactured to be low-calorie or marketed as “light” alternatives, including artificially sweetened beverages (which add substantial weight due to liquid content), sugar-free gelatin desserts, and low-fat snack products13,41. These items can increase the overall weight of UPF consumed without proportionally raising caloric intake.
At the same time, a considerable proportion of commonly consumed UPF, such as sweet baked goods, confectionery, fried snacks, and certain breakfast cereals, are highly energy-dense and contribute disproportionately to total caloric intake despite their relatively low physical weight. When such items coexist in the diet alongside energy-dilute UPF, population-level UPF intake may appear high when expressed as calories yet comparatively lower when expressed as grams (and vice versa). This heterogeneity in energy density provides a plausible explanation for the divergence between calorie-based and weight-based UPF measures observed in our study: it suggests that the greater weight of UPF consumed by the ADHD group may be primarily driven by a higher intake of low-energy-density products.
Dietary and nutritional aspects of ADHD
Prior literature linked ADHD to eating disorders and disordered eating. A meta-analysis of 12 studies (ADHD n = 4013; controls n = 29,404) by Nazar et al. found markedly higher odds of eating disorders among individuals with ADHD (pooled OR ≈ 3.8)4. A systematic review by Kaisari et al. concluded that there is moderate strength of evidence for a positive association between ADHD and disordered eating, particularly overeating5. A nationally representative school-based study in Israel (Namimi-Halevi et al.) found that adolescents with ADHD had significantly elevated odds of disordered eating, defined via a positive SCOFF screener: 50.2% versus 43.9% in non-ADHD peers (adjusted OR = 1.41; 95% CI: 1.17–1.70)56.
Evidence also indicates that ADHD is associated with variations in dietary intake and nutritional patterns, generally characterized as less healthy compared with peers without the diagnosis. Rojo Marticella et al. conducted a study across preschool and elementary populations (n = 734) and identified that the ADHD group was negatively associated with a healthy dietary pattern and positively associated with a Western-like diet6. A case–control study (n = 390) by Akin et al. found that children with ADHD consumed more processed meat products, milk-based desserts, and chocolate sweets than controls26. Wolff et al.; n = 1187) demonstrated that children and adolescents with ADHD reported more frequent and higher consumption of candy and fruit gums compared with the comparison group57. Findings from Salvat et al. also indicated that children with ADHD consumed more simple sugars and ready-made meals compared with their peers58.
Collectively, the evidence underscores distinct dietary behaviors among children with ADHD. Nevertheless, the present study addresses an existing knowledge gap concerning the association between ADHD and UPF consumption. To the best of our knowledge, only two studies have examined the association between UPF and ADHD. Both differed from the present study in two important aspects: they examined whether UPF intake predicts ADHD-related symptoms rather than investigating the reverse direction, and they focused on symptoms of ADHD rather than a clinical diagnosis of ADHD. The first study, a large Norwegian cohort study by Borge et al., investigated 77,768 mother–child pairs and reported that a one SD increase in maternal UPF intake during pregnancy was associated with a 3.0% higher ADHD symptom score at age eight (95% CI: 1.5–4.5%)59. The second, a longitudinal Brazilian study by Ferreira et al., followed children from infancy to adolescence (n = 173 at age 12–13 years) and found that higher UPF consumption at ages three to four predicted subsequent hyperactivity/inattention symptoms. Specifically, each 10-gram, 10-kcal, and 10% increase in UPF intake at preschool age conferred relative risks of ADHD symptoms of 1.01 (95% CI: 1.00–1.02), 1.02 (95% CI: 1.01–1.02), and 1.25 (95% CI: 1.04–1.51), respectively, for later hyperactivity/inattention60.
Health implications of UPF
UPF exposure in childhood has been linked to higher risks of obesity, metabolic disturbances, allergy outcomes, and adverse behavioral outcomes15,16,17,18,19, while in adults it has been associated with obesity, type 2 diabetes, cardiovascular disease, common mental disorders, auto-immune diseases, cancer, and mortality21,22,23,24,25,61,62. Although causal mechanisms remain under investigation, several pathways have been proposed: displacement of nutrient-dense foods; excess sugars and high glycemic load leading to dopaminergic dysregulation and metabolic strain; the impact of food additives (e.g., colorants, preservatives, emulsifiers) on neurobehavioral and inflammatory processes; exposure to packaging-derived contaminants such as phthalates and bisphenols; and modulation of the gut–brain axis through changes in microbiota composition and function19,63,64,65.
Nevertheless, it is important to emphasize that UPF represents a heterogeneous group, ranging from items that may carry some nutritional benefits to products that are consistently considered unhealthy, such as sugar-sweetened beverages, ready meals, and confectionery13,66.
Stimulant treatment
Stimulant medications for ADHD are known to improve executive functioning and may also suppress appetite, potentially reducing consumption of UPF67. However, the current study found no differences in UPF consumption between stimulant-treated and untreated children with ADHD. These findings should be interpreted cautiously, given the relatively small subsample. It is possible that children receiving stimulants represent those with more severe or definite ADHD, whereas the remaining children may have varying degrees of behavioral disturbance31, with treatment potentially restoring dietary patterns to a level comparable to those of peers with ADHD who are not treated with stimulants. In addition, while one might expect stimulant-treated children to consume less UPF, given that ADHD stimulants often suppress appetite during the day and may enhance inhibitory control over food selection67, many children experience “rebound effect” as medication effects wear off in the evening68, potentially leading to increased intake of convenient, ultra-processed snacks later in the day. Such compensatory overeating, individual variability in response, and family practices may further mask differences in net daily consumption68,69. Additional studies are required to further explore this issue.
ADHD and UPF consumption
Several explanations may underlie the observed association between ADHD and increased UPF consumption. On the one hand, ADHD symptoms themselves can drive dietary choices. Impulsivity, emotional dysregulation, and reward-processing difficulties bias individuals toward immediately gratifying foods, strongly flavored, and visually appealing, while devaluing minimally processed options that require planning, preparation, or delayed reward70. Evidence of dopaminergic and opioid system dysfunction in ADHD supports this explanation, as disturbances in the brain reward cascade foster heightened reward dependence and may increase preference for foods that rapidly stimulate dopamine release71. Parental feeding practices may contribute to higher UPF consumption in children with ADHD, as parents sometimes provide readily available UPF at mealtimes to avoid conflicts72. Moreover, behavior management strategies often rely on immediate edible rewards, frequently involving ultra-processed sugary foods, which may further reinforce preferences for rapidly gratifying options73. In addition, children with ADHD may exhibit atypical sensory processing and selective eating, which narrows dietary variety and promotes reliance on familiar packaged products74. Finally, distractions and difficulties in daily self-regulation may lead children with ADHD to postpone eating during the day, resulting in increased evening consumption of ready-to-eat and conveniently available UPF75.
UPF and ADHD symptoms
Mechanisms underlying the observed association may also operate in the reverse direction, whereby UPF contribute to ADHD-related symptoms. Interest in diet’s role in ADHD dates back to the 1970s when Dr. Benjamin Feingold hypothesized that eliminating certain additives (salicylates, artificial colors/flavors) could alleviate hyperactivity76. Early controlled studies provided mixed results; a National Institutes of Health panel in 1982 found only a “limited positive association” between Feingold-type elimination diets and reduced hyperactivity, with no consistent or widespread effect77. An early meta-analysis in 1983 similarly reported negligible overall benefits of dietary modification (reviewing 23 studies, it found no significant behavioral improvements)78. However, more recent evidence from rigorous trials has identified a small but significant link between artificial food additives and hyperactive behavior. A 2004 meta-analysis of 15 double-blind, placebo-controlled trials reported that artificial food colorings have an adverse effect on children’s behavior, with an overall effect size of ~0.21 (a modest increase in hyperactivity)79. Likewise, single-trial data confirm this pattern: in one placebo-controlled challenge, the removal of artificial colors and preservatives from the diet of preschoolers led to reduced hyperactivity, and these children showed significantly increased hyperactive behavior when given a drink containing those additives, an effect observed even in children without ADHD80. Another large trial in both preschool-age and school-age children found that consuming a mix of artificial food colorings and a sodium benzoate preservative resulted in increased hyperactivity in 3-year-olds and 8/9-year-olds from the general population81. Notably, the magnitude of these effects was small, but the findings have been robust across studies. This history, from Feingold’s initial diet hypothesis to modern trials, underscores that while diet is not a primary cause of ADHD, certain dietary components (particularly synthetic food additives) can subtly exacerbate hyperactive behaviors, warranting consideration in the overall context of ADHD symptoms.
Stevenson et al. showed a potential gene-diet interaction in behavioral responses to challenge mixtures containing food colorants and sodium benzoate, proposing non-IgE-dependent histamine release triggered by specific additives as a biologically plausible mechanism82. Central histamine H3 receptor activity has been implicated in inhibitory learning, increased hyperactivity in murine models, and enhanced dopamine release in the frontal cortex83, supporting the hypothesis that histamine may mediate the effects of food additives on ADHD-related symptoms. In particular, azo dyes have been reported to provoke urticaria in some individuals irrespective of aspirin sensitivity, providing clinical evidence consistent with additive-induced histamine release84,85,86. Building on this mechanistic rationale, individual susceptibility may be partly explained by polymorphisms in the histamine N-methyltransferase (HNMT) gene, which may impair histamine degradation and thereby moderate a child’s behavioral response to additive challenges82. The interplay between environmental triggers and genetic vulnerability could help explain the heterogeneity of responses observed in the general population.
While not all UPF contain high levels of sugar or additives, many products are characterized by formulations that combine refined carbohydrates, added sugars, artificial colorants, preservatives, or flavor enhancers13. Emerging evidence suggests that diets high in refined sugars may contribute to destabilization of circulating glucose levels and impair prefrontal inhibitory control and attention regulation87,88. Certain additives, including colorants and preservatives, may exacerbate hyperactivity in susceptible children89. UPF may also influence biological pathways relevant to ADHD through the gut. For instance, emulsifiers and some artificial sweeteners can increase intestinal permeability, allowing pro-inflammatory molecules to enter circulation and contribute to neuroinflammatory processes90,91. Similarly, UPF-driven alterations of the gut microbiota may disrupt the production of neurotransmitters and signaling along the gut–brain axis, mechanisms implicated in attentional control and emotional regulation65. At the same time, reliance on UPF displaces nutrient-dense foods and may lead to lower intake of omega-3 fatty acids, iron, and zinc—nutrients shown to support cognitive function and mitigate ADHD symptoms92.
Taken together, these bidirectional explanations suggest a potentially self-perpetuating vicious cycle, whereby ADHD symptoms increase susceptibility to UPF consumption, and high UPF exposure in turn may exacerbate symptom severity and functional impairment.
Public health implications
Given that prior research from Israel and other countries has consistently demonstrated associations between ADHD and unhealthy lifestyle behaviors across the lifespan (such as smoking and alcohol consumption)3,93,94, UPF consumption may likewise represent a lifestyle characteristic of children with ADHD. Reducing children’s UPF burden is reasonable as part of comprehensive ADHD care. In practice, clinicians, parents, and educators can integrate several complementary approaches. Brief screening for UPF-heavy dietary patterns during ADHD evaluations and follow-up visits may help identify children at risk. When such patterns are detected, professionals should encourage practical substitutions with minimally processed, ready-to-eat options and promote the establishment of family-based routines such as shared meals and structured snack times, which provide a more stable nutritional environment. Parents play a central role in shaping daily food availability and choices, while schools and other educational settings strongly influence children’s eating patterns through meal provision, peer modeling, and exposure to food marketing. Health education programs can further enhance awareness of the risks associated with UPF and motivate children and parents to adopt healthier choices in daily life. Finally, policy-level actions, including improving school food environments, setting procurement standards, and regulating marketing to children, can reinforce these efforts, creating a supportive ecosystem for sustained dietary change.
The implications of the current study extend beyond children with ADHD, highlighting a broader child public health relevance in the general population. The cumulative evidence from Schab and Trinh’s systematic review and subsequent double-blind, placebo-controlled challenge studies indicates that artificial food colorants and benzoate preservatives, commonly found in UPFs, are associated with increases in hyperactive behavior in children, irrespective of a prior ADHD diagnosis or baseline levels of hyperactivity79,80,81. Consistent with this interpretation, the current study found comparable effects among children with and without stimulant medication use, which is consistent with the possibility that components of UPF may have a broadly acting effect on child behavior. In children with pre-existing behavioral difficulties, such dietary exposures may exacerbate symptoms to a clinically meaningful extent. Accordingly, the regulation and management of artificial additives in the diet can be considered a population-level child public health concern, rather than an issue confined to clinical subgroups.
Limitations and strengths
The study had several limitations. Selection bias may have occurred, as ~10% of eligible candidates did not participate, and children with missing ADHD or nutrition data, as well as those with implausible energy intakes, were excluded. To mitigate non-response effects, survey weights were applied, and sociodemographic characteristics of included and excluded participants were compared, with no differences found.
Information bias was another concern. ADHD status was determined by a physician’s diagnosis as reported by parents, lacking independent clinical verification. Relying on parent-reported diagnoses could introduce misclassification of ADHD status. However, previous research suggests that a parent-reported provider diagnosis of ADHD is fairly reliable for epidemiological purposes95, and the observed prevalence was consistent with Israeli data from medical records49,50. Nonetheless, over-diagnosis cannot be ruled out, as the distinction between simple behavioral difficulties and clinically defined ADHD is often challenging to delineate, particularly amid broad diagnostic trends in recent years, including an increase in diagnoses among children with milder symptomatology96. Consequently, the inclusion of misclassified or borderline cases within the ADHD group may have diluted the true magnitude of the associations observed.
Dietary intake was self-reported as well, but the use of validated questionnaires and visual aids32,33, together with exclusion of children with extreme energy intake values, helped mitigate this bias. In addition, the use of a single 24-h recall may have limited the ability to capture habitual patterns and normal day-to-day variation in diet32,33, potentially misrepresenting usual intake. Nonetheless, using one recall per person is a common approach in surveys and can be sufficient for estimating mean dietary intakes at the population level (as the estimates of the group’s intake are statistically robust and less affected by day-to-day within-person variation)97, and the large sample size, year-round data collection, and careful scheduling of interviews across different days of the week increased representativeness.
It should be noted that the NOVA classification has recognized limitations. The UPF group encompasses diverse foods, some of which are not uniformly harmful66. However, it remains a widely used and accepted system for classifying UPF in contemporary nutritional epidemiology25. The results need to be interpreted with appropriate nuance, and the NOVA classification should be viewed as a general indicator of highly processed dietary patterns rather than as a blanket condemnation of all NOVA 4 items.
Interviewer bias was also a possible concern, but this was reduced through standardized protocols and specially trained interviewers. Social desirability bias was likely non-differential between exposure groups, thereby attenuating rather than exaggerating observed associations.
As a cross-sectional study, causal inference cannot be drawn. It remains unclear whether ADHD symptoms influenced food choices or vice versa. Accordingly, the findings were interpreted as associations, with a recognition that the directionality of the relationship remains unclear; both the possibility that ADHD may contribute to higher UPF intake, and that UPF consumption may exacerbate ADHD-related symptoms, warrant consideration. Longitudinal studies are needed to clarify the temporal and causal nature of this association. In addition, dietary changes following ADHD diagnosis, such as adopting healthier eating habits98, may also have affected associations, but this effect is likewise expected to attenuate the observed relation. Finally, the focus on Israeli school-aged children further limits generalizability to other age groups or cultural settings.
Nevertheless, the study has several notable strengths. It included a large, nationally representative sample with a high response rate. Internal validity was strengthened by the use of validated measurement tools, standardized protocols, and interviews conducted by trained personnel. Comprehensive dietary information was obtained from all participants, along with detailed information on pharmacological treatment. The consistency of the results across various statistical approaches supports the robustness of the observed associations. Moreover, the analyses were rigorously adjusted for a wide range of potential confounders, reducing the likelihood of residual confounding. Nonetheless, the risk of residual confounding and the existence of an unmeasured third factor that is linked to both ADHD and UPF consumption still remains.
Conclusion
In this nationally representative cross-sectional sample of Israeli children, physician-diagnosed ADHD was associated with higher UPF consumption, independent of stimulant treatment status. Given the observational design, directionality cannot be determined; the association may reflect ADHD-related eating behaviors, potential contributions of UPF constituents to hyperactive behaviors, or both. These findings support considering UPF intake within a broader child public health context and underscore the need for further studies to clarify temporality and clinical relevance.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Xu, G., Strathearn, L., Liu, B., Yang, B. & Bao, W. Twenty-year trends in diagnosed attention-deficit/hyperactivity disorder among US children and adolescents, 1997-2016. JAMA Netw. Open. 1, e181471 (2018).
Cabral, M. D. I., Liu, S. & Soares, N. Attention-deficit/hyperactivity disorder: diagnostic criteria, epidemiology, risk factors and evaluation in youth. Transl. Pediatr. 9, S104–S113 (2020).
French, B. et al. The impacts associated with having ADHD: an umbrella review. Front Psychiatry 15, 1343314 (2024).
Nazar, B. P. et al. The risk of eating disorders comorbid with attention-deficit/hyperactivity disorder: a systematic review and meta-analysis. Int. J. Eat. Disord. 49, 1045–1057 (2016).
Kaisari, P., Dourish, C. T. & Higgs, S. Attention Deficit Hyperactivity Disorder (ADHD) and disordered eating behaviour: a systematic review and a framework for future research. Clin. Psychol. Rev. 53, 109–121 (2017).
Rojo-Marticella, M. et al. Do children with attention-deficit/hyperactivity disorder follow a different dietary pattern than that of their control peers? Nutrients https://doi.org/10.3390/NU14061131 (2022).
Del-Ponte, B., Quinte, G. C., Cruz, S., Grellert, M. & Santos, I. S. Dietary patterns and attention deficit/hyperactivity disorder (ADHD): a systematic review and meta-analysis. J. Affect Disord. 252, 160–173 (2019).
Jamshidnia, A., Tavallaei, M. & Hosseinzadeh, M. Food intake and attention-deficit/hyperactivity disorder in children: a case control study. Clin. Nutr. ESPEN 44, 342–347 (2021).
Baker, P. et al. Ultra-processed foods and the nutrition transition: Global, regional and national trends, food systems transformations and political economy drivers. Obes. Rev. https://doi.org/10.1111/OBR.13126 (2020).
Monteiro, C. A. et al. NOVA. The star shines bright. World Nutr. 7, 28–38 (2016).
Moubarac, J. C., Parra, D. C., Cannon, G. & Monteiro, C. A. Food classification systems based on food processing: significance and implications for policies and actions: a systematic literature review and assessment. Curr. Obes. Rep. 3, 256–272 (2014).
Monteiro, C. A., Levy, R. B., Claro, R. M., de Castro, I. R. R. & Cannon, G. A new classification of foods based on the extent and purpose of their processing. Cad. Saude Publica 26, 2039–2049 (2010).
Monteiro, C. A. et al. Ultra-processed foods: what they are and how to identify them. Public Health Nutr. 22, 936 (2019).
Martini, D., Godos, J., Bonaccio, M., Vitaglione, P. & Grosso, G. Ultra-processed foods and nutritional dietary profile: a meta-analysis of nationally representative samples. Nutrients https://doi.org/10.3390/NU13103390 (2021).
Khoury, N. et al. Ultraprocessed food consumption and cardiometabolic risk factors in children. JAMA Netw. Open 7, E2411852 (2024).
Petridi, E. et al. The impact of ultra-processed foods on obesity and cardiometabolic comorbidities in children and adolescents: a systematic review. Nutr. Rev. 82, 913–928 (2024).
De Amicis, R. et al. Ultra-processed foods and obesity and adiposity parameters among children and adolescents: a systematic review. Eur. J. Nutr. 61, 2297–2311 (2022).
Lee, G. Y., Lim, J. H., Joung, H. & Yoon, D. Association between ultraprocessed food consumption and metabolic disorders in children and adolescents with obesity. Nutrients https://doi.org/10.3390/NU16203524 (2024).
Berni Canani, R. et al. Ultra-processed foods, allergy outcomes and underlying mechanisms in children: an EAACI task force report. Pediatric Allergy Immunol. https://doi.org/10.1111/PAI.14231 (2024).
Warner, J. O. Artificial food additives: Hazardous to long-term health?. Arch. Dis. Child 109, 882–885 (2024).
Mendoza, K. et al. Ultra-processed foods and cardiovascular disease: analysis of three large US prospective cohorts and a systematic review and meta-analysis of prospective cohort studies. Lancet Regional Health Am. https://doi.org/10.1016/j.lana.2024.100859 (2024).
Lane, M. M. et al. Ultra-processed food consumption and mental health: a systematic review and meta-analysis of observational studies. Nutrients https://doi.org/10.3390/NU14132568 (2022).
Soublette Figuera, A. et al. Effects of ultra-processed foods and food additives on disease activity in adults with inflammatory bowel disease: a scoping review. J. Clin. Med. https://doi.org/10.3390/JCM14217798 (2025).
Isaksen, I. M. & Dankel, S. N. Ultra-processed food consumption and cancer risk: a systematic review and meta-analysis. Clin. Nutr. 42, 919–928 (2023).
Monteiro, C. A. et al. Ultra-processed foods and human health: the main thesis and the evidence. Lancet 406, 2667–2684 (2025).
Akin, S. et al. Processed meat products and snacks consumption in ADHD: a case–control study. North Clin. Istanb. 9, 266–274 (2022).
Ríos-Hernández, A., Alda, J. A., Farran-Codina, A., Ferreira-García, E. & Izquierdo-Pulido, M. The Mediterranean diet and ADHD in children and adolescents. Pediatrics https://doi.org/10.1542/PEDS.2016-2027 (2017).
Johnson, R. J. et al. Attention-deficit/hyperactivity disorder: is it time to reappraise the role of sugar consumption?. Postgrad. Med. 123, 39–49 (2011).
Vadiveloo, M. K. et al. Ultraprocessed foods and their association with cardiometabolic health: evidence, gaps, and opportunities: a science advisory from the American Heart Association. Circulation 152, e245–e263 (2025).
Israel Center for Disease Control (Israel Ministry of Health). Rav Mabat Kids First National Health and Nutrition Survey Ages 2-11 Years 2015-2016. 391. https://www.gov.il/BlobFolder/reports/mabat-kids2-11-2015-2016-full/en/files_publications_units_ICDC_rav_mabat_kids_en.pdf (2025).
Wolraich, M. L. et al. Clinical practice guideline for the diagnosis, evaluation, and treatment of attention-deficit/hyperactivity disorder in children and adolescents. Pediatrics https://doi.org/10.1542/PEDS.2019-2528 (2019).
Baranowski, T. 24-hour recall and diet record methods. Nutr. Epidemiol. https://doi.org/10.1093/ACPROF:OSO/9780199754038.003.0004 (2012).
National Cancer Institute (Dietary Assessment Primer). 24-hour Dietary Recall (24HR) At a Glance. https://dietassessmentprimer.cancer.gov/profiles/recall/ (2025).
Israel Ministry of Health. Tzamert Software (Hebrew). https://www.gov.il/he/pages/nutrition-professionals?chapterIndex=3 (2025).
Huybrechts, I. et al. Characterization of the degree of food processing in the European Prospective Investigation into Cancer and Nutrition: application of the Nova classification and validation using selected biomarkers of food processing. Front Nutr. 9, 1035580 (2022).
Dickie, S., Woods, J., Machado, P. & Lawrence, M. A novel food processing-based nutrition classification scheme for guiding policy actions applied to the Australian food supply. Front. Nutr. https://doi.org/10.3389/FNUT.2023.1071356 (2023).
Food and Agriculture Organization of the United Nations. Guidelines on the Collection of Information on Food Processing through Food Consumption Surveys. https://openknowledge.fao.org/items/b8033ea6-184e-4eca-a7a2-8123e2c4103f (2025).
Monteiro, C. A., Cannon, G., Lawrence, M., Costa Louzada, M. L. & Machado, P.P. Ultra-processed foods, diet quality, and health using the NOVA classification system. https://openknowledge.fao.org/server/api/core/bitstreams/5277b379-0acb-4d97-a6a3-602774104629/content (2025).
Rodrigues, J. et al. Adherence to the Mediterranean diet, sodium and potassium intake in people at a high risk of dementia. Nutrients https://doi.org/10.3390/NU16101419 (2024).
Su, X. et al. The association between PURE healthy diet score and all-cause mortality in Chinese adults: a nationwide cohort study. Precis. Nutr. 3, e00087 (2024).
Vitale, M. et al. Ultra-processed foods and human health: a systematic review and meta-analysis of prospective cohort studies. Adv. Nutr. 15, 100121 (2023).
Endeweld, M., Barkali, N., Gottlieb, D. & Heller, O. Poverty and Social Gaps in 2014, annual report. https://www.btl.gov.il/English%20Homepage/Publications/Poverty_Report/Pages/oni2014e0721-3829.aspx (2025).
World Health Organization. Child growth standards. https://www.who.int/tools/child-growth-standards (2025).
Dahl, W. J. & Stewart, M. L. Position of the academy of nutrition and dietetics: health implications of dietary fiber. J. Acad. Nutr. Diet. 115, 1861–1870, (2015).
Pan, A. et al. α-Linolenic acid and risk of cardiovascular disease: a systematic review and meta-analysis1. Am. J. Clin. Nutr. 96, 1262 (2012).
Gowrishankar, M., Blair, B. & Rieder, M. J. Dietary intake of sodium by children: Why it matters. Paediatr. Child Health 25, 47–61 (2020).
US Center for Disease Control. Physical Activity Guidelines for School-Aged Children and Adolescents. https://www.cdc.gov/physical-activity-education/guidelines/index.html (2025).
Ayano, G., Demelash, S., Gizachew, Y., Tsegay, L. & Alati, R. The global prevalence of attention deficit hyperactivity disorder in children and adolescents: an umbrella review of meta-analyses. J. Affect Disord. 339, 860–866 (2023).
Cohen, R. et al. Prevalence of epilepsy and attention-deficit hyperactivity (ADHD) disorder: a population-based study. J. Child Neurol. 28, 120–123 (2013).
Pinhas-Hamiel, O. et al. Attention-deficit/hyperactivity disorder and obesity: a national study of 1.1 million Israeli adolescents. J. Clin. Endocrinol. Metab. 107, E1434–E1443 (2022).
Quinn, P. O. & Madhoo, M. A review of attention-deficit/hyperactivity disorder in women and girls: uncovering this hidden diagnosis. Prim. Care Companion CNS Disord. 16, PCC.13r01596 (2014).
Russell, A. E., Ford, T., Williams, R. & Russell, G. The association between socioeconomic disadvantage and attention deficit/hyperactivity disorder (ADHD): a systematic review. Child Psychiatry Hum. Dev. 47, 440–458, https://doi.org/10.1007/S10578-015-0578-3 (2016).
Pearce, A. et al. Childhood attention-deficit hyperactivity disorder: socioeconomic inequalities in symptoms, impact, diagnosis and medication. Child Adolesc. Ment. Health 29, 126–135 (2024).
Chang, J. P. C., Su, K. P., Mondelli, V. & Pariante, C. M. Omega-3 polyunsaturated fatty acids in youths with attention deficit hyperactivity disorder: a systematic review and meta-analysis of clinical trials and biological studies. Neuropsychopharmacology 43, 534–545 (2018).
National Institutes of Health. Nutrient Recommendations and Databases. https://ods.od.nih.gov/HealthInformation/nutrientrecommendations.aspx (2025).
Namimi-Halevi, C. et al. Attention-deficit hyperactivity disorder is associated with disordered eating in adolescents. Pediatr. Res 96, 1068–1075 (2024).
Wolff, N. et al. On the positive association between candy and fruit gum consumption and hyperactivity in children and adolescents with ADHD. Z. Kinder Jugendpsychiatr Psychother. 47, 228–238 (2019).
Salvat, H. et al. Nutrient intake, dietary patterns, and anthropometric variables of children with ADHD in comparison to healthy controls: a case-control study. BMC Pediatr. https://doi.org/10.1186/S12887-022-03123-6 (2022).
Borge, T. C. et al. The associations between maternal and child diet quality and child ADHD – findings from a large Norwegian pregnancy cohort study. BMC Psychiatry https://doi.org/10.1186/S12888-021-03130-4 (2021).
Ferreira, R. C., Marin, A. H., Vitolo, M. R. & Campagnolo, P. D. B. Early ultra-processed foods consumption and hyperactivity/inattention in adolescence. Rev. Saude Publica 58, 46 (2024).
Nilson, E. A. F. et al. Premature mortality attributable to ultraprocessed food consumption in 8 countries. Am. J. Prev. Med. 68, 1091–1099 (2025).
Lane, M. M. et al. Ultra-processed food exposure and adverse health outcomes: umbrella review of epidemiological meta-analyses. BMJ https://doi.org/10.1136/BMJ-2023-077310 (2024).
Morys, F. et al. Ultra-processed food consumption affects structural integrity of feeding-related brain regions independent of and via adiposity. npj Metab. Health Dis. 3, 1–9 (2025).
Mottis, G., Kandasamey, P. & Peleg-Raibstein, D. The consequences of ultra-processed foods on brain development during prenatal, adolescent and adult stages. Front. Public Health 13, 1590083 (2025).
Rondinella, D. et al. The detrimental impact of ultra-processed foods on the human gut microbiome and gut barrier. Nutrients 17, 859 (2025).
Louie, J. C. Y. Are all ultra-processed foods bad? A critical review of the NOVA classification system. Proc. Nutrition Soc. https://doi.org/10.1017/S0029665125100645 (2025).
Stevens, J. R., Wilens, T. E. & Stern, T. A. Using stimulants for attention-deficit/hyperactivity disorder: clinical approaches and challenges. Prim. Care Companion CNS Disord. 15, PCC.12f01472 (2013).
López, F. A. et al. ADHD symptom rebound and emotional lability with lisdexamfetamine dimesylate in children aged 6 to 12 years. J. Atten. Disord. 21, 52–61 (2017).
Bowling, A., Davison, K., Haneuse, S., Beardslee, W. & Miller, D. P. ADHD medication, dietary patterns, physical activity, and BMI in children: a longitudinal analysis of the ECLS-K Study. Obesity 25, 1802–1808 (2017).
Dufour, R. et al. Childhood hyperactivity, eating behaviours, and executive functions: Their association with the development of eating-disorder symptoms in adolescence. J. Eat. Disord. 11, 1–11 (2023).
MacDonald, H. J., Kleppe, R., Szigetvari, P. D. & Haavik, J. The dopamine hypothesis for ADHD: an evaluation of evidence accumulated from human studies and animal models. Front. Psychiatry 15, 1492126 (2024).
Matthews, Z., Pigden-Bennett, D., Tavassoli, T. & Snuggs, S. Comparing eating and mealtime experiences in families of children with autism, attention deficit hyperactivity disorder and dual diagnosis. Autism 29, 518–535 (2025).
Bauer, J. M. et al. Rewarding behavior with a sweet food strengthens its valuation. PLoS ONE 16, e0242461 (2021).
Kaşak, M. et al. Selective eating and sensory sensitivity in children with ADHD: a comparative study of ARFID symptom profiles. Int. J. Eating Disorders. https://doi.org/10.1002/EAT.24512 (2025).
Ptacek, R. et al. Disruptive patterns of eating behaviors and associated lifestyles in males with ADHD. Med. Sci. Monit. 20, 608 (2014).
Stare, F. J., Whelan, E. M. & Sheridan, M. Diet and hyperactivity: is there a relationship?. Pediatrics 66, 521–525 (1980).
Skypala, I. & Venter, C. Food hypersensitivity: diagnosing and managing food allergies and intolerance. Blackwell Publishing Ltd. https://alameed.edu.iq/DocumentPdf/Library/eBook/5887.pdf#:~:text=National%20Institutes%20of%20Health%20,triggering%20hyperactivity%20and%20its%20biological (2025).
Kavale, K. A. & Forness, S. R. Hyperactivity and diet treatment: a meta-analysis of the Feingold hypothesis. J. Learn Disabil. 16, 324–330 (1983).
Schab, D. W. & Trinh, N. H. T. Do artificial food colors promote hyperactivity in children with hyperactive syndromes? A meta-analysis of double-blind placebo-controlled trials. J. Dev. Behav. Pediatr. 25, 423–434 (2004).
Bateman, B. et al. The effects of a double blind, placebo controlled, artificial food colourings and benzoate preservative challenge on hyperactivity in a general population sample of preschool children. Arch. Dis. Child 89, 506–511 (2004).
McCann, D. et al. Food additives and hyperactive behaviour in 3-year-old and 8/9-year-old children in the community: a randomised, double-blinded, placebo-controlled trial. Lancet 370, 1560–1567 (2007).
Stevenson, J. et al. The role of histamine degradation gene polymorphisms in moderating the effects of food additives on children’s ADHD symptoms. Am. J. Psychiatry 167, 1108–1115 (2010).
Fox, G. B. et al. Pharmacological properties of ABT-239 [4-(2-{2-[(2R)-2-Methylpyrrolidinyl]ethyl}-benzofuran-5-yl)benzonitrile]: II. Neurophysiological characterization and broad preclinical efficacy in cognition and schizophrenia of a potent and selective histamine H3 receptor antagonist. J. Pharm. Exp. Ther. 313, 176–190 (2005).
Supramaniam, G. & Warner, J. O. Artificial food additive intolerance in patients with angio-oedema and urticaria. Lancet 2, 907–909 (1986).
Murdoch, R. D., Pollock, I., Young, E. & Lessof, M. H. Food additive-induced urticaria: studies of mediator release during provocation tests. J. R. Coll. Physicians Lond. 21, 262–266 (1987).
Murdoch, R. D., Lessof, M. H., Pollock, I. & Young, E. Effects of food additives on leukocyte histamine release in normal and urticaria subjects. J. R. Coll. Physicians Lond. 21, 251–256 (1987).
Davidson, T. L., Jones, S., Roy, M. & Stevenson, R. J. The cognitive control of eating and body weight: It’s more than what you “think. Front. Psychol. 10, 430726 (2019).
Gillespie, K. M. et al. The impact of free and added sugars on cognitive function: a systematic review and meta-analysis. Nutrients 16, 75 (2024).
Arnold, L. E., Lofthouse, N. & Hurt, E. Artificial food colors and attention-deficit/hyperactivity symptoms: conclusions to dye for. Neurotherapeutics 9, 599 (2012).
Shil, A. et al. Artificial sweeteners disrupt tight junctions and barrier function in the intestinal epithelium through activation of the sweet taste receptor, T1R3. Nutrients 12, 1862 (2020).
Bevilacqua, A. et al. Ultra-Processed food and gut microbiota: do additives affect eubiosis? a narrative review. Nutrients 17, 2 (2024).
Ryu, S. A. et al. Associations between Dietary Intake and Attention Deficit Hyperactivity Disorder (ADHD) Scores by Repeated Measurements in School-Age Children. Nutrients 14, 2919 (2022).
Gudjonsson, G. H., Sigurdsson, J. F., Sigfusdottir, I. D. & Young, S. An epidemiological study of ADHD symptoms among young persons and the relationship with cigarette smoking, alcohol consumption and illicit drug use. J. Child Psychol. Psychiatry 53, 304–312 (2012).
Namimi-Halevi, C., Dor, C., Dichtiar, R., Bromberg, M. & Sinai, T. Attention-deficit hyperactivity disorder is associated with risky and unhealthy behaviours among adolescents. Public Health 237, 51–56 (2024).
Cree, R. A. et al. Surveillance of ADHD among children in the united states: validity and reliability of parent report of provider diagnosis. J. Atten. Disord. 27, 111–123 (2023).
Kazda, L. et al. Overdiagnosis of attention-deficit/hyperactivity disorder in children and adolescents: a systematic scoping review. JAMA Netw. Open 4, e215335–e215335 (2021).
Thompson, F. E., Subar, A. F. Dietary assessment methodology. Nutr. Prev. Treat. Dis. https://doi.org/10.1016/B978-0-12-802928-2.00001-1 (2017).
Lange, K. W. Micronutrients and diets in the treatment of attention-deficit/hyperactivity disorder: chances and pitfalls. Front. Psychiatry 11, 102 (2020).
Acknowledgements
The authors would like to acknowledge the diligent work of our study staff that was involved in conducting the survey and/or collecting data across the country, and thank all study participants for their valuable contribution.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors. Open access funding provided by Hebrew University of Jerusalem.
Author information
Authors and Affiliations
Contributions
C.N.H. was involved in designing the study, interpreted the data, and drafted the manuscript; C.D. was involved in designing the study, performed the statistical analyses and interpreted the data; V.K.S was involved in designing the study and revised the manuscript; R.D. supervised and performed the statistical analyses; M.B. interpreted the data and revised the manuscript. T.S. conceptualized, designed, and supervised the study, interpreted the data, was involved in the initial manuscript drafting and revised the manuscript critically for important intellectual content.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Consent to participate
Written informed consent was obtained from the parents or legal guardians of all participants.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Namimi-Halevi, C., Dor, C., Kaufman-Shriqui, V. et al. Attention-deficit/hyperactivity disorder is associated with increased consumption of ultra-processed foods among children. Pediatr Res (2026). https://doi.org/10.1038/s41390-026-04844-5
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41390-026-04844-5