Abstract
Plasminogen activator inhibitor-1 (PAI-1) is significantly upregulated during inflammatory responses, and elevated PAI-1 levels are associated with poor prognosis in various diseases. However, the precise mechanism through which PAI-1 exacerbates inflammation remains unclear. In the present study, we have investigated the role of PAI-1 in inflammation using a mouse model of skeletal muscle injury. We found that CCR2⁺Ly6C⁺ inflammatory macrophages infiltrated the injured tissues and produced substantial amounts of PAI-1. Notably, PAI-1 deficiency specifically in these macrophages resulted in attenuated inflammation and accelerated tissue repair despite the continued presence of PAI-1 in body fluids, indicating a local macrophage-driven effect. Low-density lipoprotein receptor-related protein-1 (LRP-1), expressed on macrophages, is a common receptor for both PAI-1 and calreticulin (CRT). CRT is exposed on the surface of dying cells and functions as an “eat me” signal recognized by macrophages via LRP-1. We found that PAI-1 binds to LRP-1 with higher affinity than that to CRT, thereby competitively inhibiting CRT recognition and suppressing efferocytosis, the process by which macrophages clear dead cells, ultimately leading to prolonged inflammation. Importantly, administration of a PAI-1 inhibitor, TM5614, restored efferocytosis and significantly improved tissue regeneration. These findings therefore reveal that PAI-1 produced by infiltrating inflammatory macrophages contributes to sustained inflammation by blocking efferocytosis, and that PAI-1 is a promising therapeutic target for the treatment of inflammatory diseases.

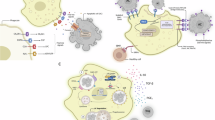
Dead cells expose an “eat-me” signal molecule CRT, which is recognized by the LRP-1 receptor on macrophages, leading to their phagocytosis through a process known as efferocytosis. However, PAI-1, secreted by infiltrating CCR2+Ly6c+ macrophages, impairs tissue regeneration after injury by inhibiting efferocytosis through competitive binding to LRP-1, thereby prolonging inflammation.
Similar content being viewed by others
Data availability
The materials generated for this study can be provided upon reasonable request. Any additional information required to reanalyze the data reported in this paper is available from the corresponding author contact upon request.
References
Nagler-Anderson C. Man the barrier! strategic defences in the intestinal mucosa. Nat Rev Immunol. 2001;1:59–67.
Hajishengallis G, Netea MG, Chavakis T. Trained immunity in chronic inflammatory diseases and cancer. Nat Rev Immunol. 2025;25:497–514.
Esmaeili A, Yazdanpanah N, Rezaei N. LncRNAs orchestrating neuroinflammation: a comprehensive review. Cell Mol Neurobiol. 2025;45:21.
Liang M-H, Wendland JR, Chuang D-M. Lithium inhibits Smad3/4 transactivation via increased CREB activity induced by enhanced PKA and AKT signaling. Mol Cell Neurosci. 2008;37:440–53.
Prado C, Herrada AA, Hevia D, Goiry LG, Escobedo N. Role of innate immune cells in multiple sclerosis. Front Immunol. 2025;16:1540263.
Murray PJ, Wynn TA. Protective and pathogenic functions of macrophage subsets. Nat Rev Immunol. 2011;11:723–37.
Wynn TA, Chawla A, Pollard JW. Macrophage biology in development, homeostasis and disease. Nature. 2013;496:445–55.
Kojima Y, Weissman IL, Leeper NJ. The role of efferocytosis in atherosclerosis. Circulation. 2017;135:476–89.
Doran AC, Yurdagul A, Tabas I. Efferocytosis in health and disease. Nat Rev Immunol. 2020;20:254–67.
Lemke G. How macrophages deal with death. Nat Rev Immunol. 2019;19:539–49.
Gardai SJ, McPhillips KA, Frasch SC, Janssen WJ, Starefeldt A, Murphy-Ullrich JE, et al. Cell-surface calreticulin initiates clearance of viable or apoptotic cells through trans-activation of LRP on the phagocyte. Cell. 2005;123:321–34.
Muller-Taubenberger A. Calreticulin and calnexin in the endoplasmic reticulum are important for phagocytosis. EMBO J. 2001;20:6772–82.
Majeti R, Chao MP, Alizadeh AA, Pang WW, Jaiswal S, Gibbs KD, et al. CD47 is an adverse prognostic factor and therapeutic antibody target on human acute myeloid leukemia stem cells. Cell. 2009;138:286–99.
Jaiswal S, Jamieson CHM, Pang WW, Park CY, Chao MP, Majeti R, et al. CD47 is upregulated on circulating hematopoietic stem cells and leukemia cells to avoid phagocytosis. Cell. 2009;138:271–85.
Li Y, Zhang Y, Pan G, Xiang L, Luo D, Shao J. Occurrences and functions of Ly6Chi and Ly6Clo macrophages in health and disease. Front Immunol. 2022;13:901672.
Epelman S, Lavine KJ, Randolph GJ. Origin and functions of tissue macrophages. Immunity. 2014;41:21–35.
Ghosh AK, Vaughan DE. PAI-1 in tissue fibrosis. J Cell Physiol. 2012;227:493–507.
Koh TJ, Bryer SC, Pucci AM, Sisson TH. Mice deficient in plasminogen activator inhibitor-1 have improved skeletal muscle regeneration. Am J Physiol Cell Physiol. 2005;289:C217–C223.
Suelves M, Vidal B, Ruiz V, Baeza-Raja B, Diaz-Ramos A, Cuartas I, et al. The plasminogen activation system in skeletal muscle regeneration: antagonistic roles of urokinase-type plasminogen activator (uPA) and its inhibitor (PAI-1. Front Biosci. 2005;10:2978–85.
Krause MP, Moradi J, Nissar AA, Riddell MC, Hawke TJ. Inhibition of plasminogen activator inhibitor-1 restores skeletal muscle regeneration in untreated type 1 diabetic mice. Diabetes. 2011;60:1964–72.
Rahman FA, Krause MP. PAI-1, the plasminogen system, and skeletal muscle. Int J Mol Sci. 2020;21:7066.
Eren M, Boe A, Klyachko E, Vaughan D. Role of plasminogen activator inhibitor-1 in senescence and aging. Semin Thromb Hemost. 2014;40:645–51.
Vaughan DE, Rai R, Khan SS, Eren M, Ghosh AK. Plasminogen activator inhibitor-1 is a marker and a mediator of senescence. Arterioscler Thromb Vasc Biol. 2017;37:1446–52.
Patsalos A, Pap A, Varga T, Trencsenyi G, Contreras GA, Garai I, et al. In situ macrophage phenotypic transition is affected by altered cellular composition prior to acute sterile muscle injury. J Physiol. 2017;595:5815–42.
Miyata T. Overview: PAI-1 inhibitors and clinical applications. Biomed J. 2025;49:100874.
Yamaoka N, Murano K, Kodama H, Maeda A, Dan T, Nakabayashi T, et al. Identification of novel plasminogen activator inhibitor-1 inhibitors with improved oral bioavailability: structure optimization of N-acylanthranilic acid derivatives. Bioorg Med Chem Lett. 2018;28:809–13.
Yahata T, Ibrahim AA, Hirano K, Muguruma Y, Naka K, Hozumi K, et al. Targeting of plasminogen activator inhibitor-1 activity promotes elimination of chronic myeloid leukemia stem cells. Haematologica. 2020;106:483–94.
Ghosh AK, Soberanes S, Lux E, Shang M, Aillon RP, Eren M, et al. Pharmacological inhibition of PAI-1 alleviates cardiopulmonary pathologies induced by exposure to air pollutants PM2.5. Environ Pollut. 2021;287:117283.
Sasaki K, Fujiwara T, Ochi T, Ono K, Kato H, Onodera K, et al. TM5614, an inhibitor of plasminogen activator inhibitor-1, exerts an antitumor effect on chronic myeloid leukemia. Tohoku J Exp Med. 2022;257:211–24.
Ibrahim AA, Fujimura T, Uno T, Terada T, Hirano K, Hosokawa H, et al. Plasminogen activator inhibitor-1 promotes immune evasion in tumors by facilitating the expression of programmed cell death-ligand 1. Front Immunol. 2024;15:1365894.
Fujimura T, Yoshino K, Kato H, Fukushima S, Ishizuki S, Otsuka A, et al. A phase II multicentre study of plasminogen activator inhibitor-1 inhibitor (TM5614) plus nivolumab for treating anti-programmed cell death 1 antibody-refractory malignant melanoma: TM5614-MM trial. Br J Dermatol. 2024;191:691–7.
Forbes SJ, Rosenthal N. Preparing the ground for tissue regeneration: from mechanism to therapy. Nat Med. 2014;20:857–69.
Weavers H, Martin P. The cell biology of inflammation: From common traits to remarkable immunological adaptations. J Cell Biol. 2020;219:e202004003.
Horner E, Lord JM, Hazeldine J. The immune suppressive properties of damage associated molecular patterns in the setting of sterile traumatic injury. Front Immunol. 2023;14:1239683.
Zhu H, Shen F, Liao T, Qian H, Liu Y. Immunosenescence and macrophages: From basics to therapeutics. Int J Biochem Cell Biol. 2023;165:106479.
Man SM, Kanneganti T-D. Innate immune sensing of cell death in disease and therapeutics. Nat Cell Biol. 2024;26:1420–33.
Park YJ, Liu G, Lorne EF, Zhao X, Wang J, Tsuruta Y, et al. PAI-1 inhibits neutrophil efferocytosis. Proc Natl Acad Sci USA. 2008;105:11784–9.
Migliorini M, Li S-H, Zhou A, Emal CD, Lawrence DA, Strickland DK. High-affinity binding of plasminogen-activator inhibitor 1 complexes to LDL receptor–related protein 1 requires lysines 80, 88, and 207. J Biol Chem. 2020;295:212–22.
Quail DF, Joyce JA. Microenvironmental regulation of tumor progression and metastasis. Nat Med. 2013;19:1423–37.
Cao C, Lawrence DA, Li Y, Von Arnim CAF, Herz J, Su EJ, et al. Endocytic receptor LRP together with tPA and PAI-1 coordinates Mac-1-dependent macrophage migration. EMBO J. 2006;25:1860–70.
Ichimura A, Matsumoto S, Suzuki S, Dan T, Yamaki S, Sato Y, et al. A small molecule inhibitor to plasminogen activator inhibitor 1 inhibits macrophage migration. Arterioscler Thromb Vasc Biol. 2013;33:935–42.
Kubala MH, Punj V, Placencio-Hickok VR, Fang H, Fernandez GE, Sposto R, et al. Plasminogen activator inhibitor-1 promotes the recruitment and polarization of macrophages in cancer. Cell Rep. 2018;25:2177–91.e7.
Vaughan DE. PAI-1 and atherothrombosis. J Thromb Haemost. 2005;3:1879–83.
Van De Craen B, Declerck PJ, Gils A. The biochemistry, physiology and pathological roles of PAI-1 and the requirements for PAI-1 inhibition in vivo. Thromb Res. 2012;130:576–85.
Ibrahim AA, Yahata T, Onizuka M, Dan T, Ypersele De Strihou C, Miyata T, et al. Inhibition of plasminogen activator inhibitor type-1 activity enhances rapid and sustainable hematopoietic regeneration. Stem Cells. 2014;32:946–58.
Yahata T, Ibrahim AA, Muguruma Y, Eren M, Shaffer AM, Watanabe N, et al. TGF-β–induced intracellular PAI-1 is responsible for retaining hematopoietic stem cells in the niche. Blood. 2017;130:2283–94.
Ibrahim AA, Yahata T, Muguruma Y, Miyata T, Ando K. Blockade of plasminogen activator inhibitor-1 empties bone marrow niche sufficient for donor hematopoietic stem cell engraftment without myeloablative conditioning. Biochem Biophys Res Commun. 2019;516:500–5.
Takahashi N, Kameoka Y, Onizuka M, Onishi Y, Takahashi F, Dan T, et al. Deep molecular response in patients with chronic phase chronic myeloid leukemia treated with the plasminogen activator inhibitor-1 inhibitor TM5614 combined with a tyrosine kinase inhibitor. Cancer Med. 2023;12:4250–8.
Fujimura T, Yoshino K, Nakamura M, Kato H, Ito T, Maekawa T, et al. Efficacy and safety of TM5614 in combination with paclitaxel in the treatment of paclitaxel-resistant cutaneous angiosarcoma: Phase II study protocol. Exp Dermatol. 2024;33:e14976.
Hirai T, Asano K, Ito I, Miyazaki Y, Sugiura H, Agirbasli M, et al. A randomized double-blind placebo-controlled trial of an inhibitor of plasminogen activator inhibitor-1 (TM5614) in mild to moderate COVID-19. Sci Rep. 2024;14:165.
Masuda T, Hirata T, Sakamoto T, Tsubata Y, Ichihara E, Kozuki T, et al. Treatment rationale and protocol design: an investigator-initiated phase II study of combination treatment of nivolumab and TM5614, a PAI-1 inhibitor for previously treated patients with non-small cell lung cancer. J Thorac Dis. 2024;16:3381–8.
Kleemann J, Schilling B. Multicentre phase II trial of plasminogen activator inhibitor-1 inhibitor (TM5614) plus nivolumab in Japanese advanced melanoma patients: immune resistance remains one of the major efforts in melanoma research. Br J Dermatol. 2024;191:654–5.
Concordet J-P, Haeussler M. CRISPOR: intuitive guide selection for CRISPR/Cas9 genome editing experiments and screens. Nucleic Acids Res. 2018;46:W242–W245.
Gurumurthy CB, Sato M, Nakamura A, Inui M, Kawano N, Islam MA, et al. Creation of CRISPR-based germline-genome-engineered mice without ex vivo handling of zygotes by i-GONAD. Nat Protoc. 2019;14:2452–82.
Hasegawa A, Mochida K, Nakamura A, Miyagasako R, Ohtsuka M, Hatakeyama M, et al. Use of anti-inhibin monoclonal antibody for increasing the litter size of mouse strains and its application to in vivo-genome editing technology. Biol Reprod. 2022;107:605–18.
Misharin AV, Cuda CM, Saber R, Turner JD, Gierut AK, Haines GK, et al. Nonclassical Ly6C− monocytes drive the development of inflammatory arthritis in mice. Cell Rep. 2014;9:591–604.
Pinto AR, Godwin JW, Chandran A, Hersey L, Ilinykh A, Debuque R, et al. Age-related changes in tissue macrophages precede cardiac functional impairment. Aging. 2014;6:399–413.
Smith AJ, Clutton RE, Lilley E, Hansen KEA, Brattelid T. PREPARE: guidelines for planning animal research and testing. Lab Anim. 2018;52:135–41.
Percie du Sert N, Hurst V, Ahluwalia A, Alam S, Avey MT, Baker M, et al. The ARRIVE guidelines 2.0: Updated guidelines for reporting animal research. PLoS Biol. 2020;18:e3000410.
Acknowledgements
We are grateful to Aki Kurosaki for genotyping; to the Life Science Support Center of Tokai University for technical assistance,especially Ayaka Nakamura for gene-modified mice generation. We also thank Editage (www.editage.jp) for English language editing.
Funding
This work was supported in part by MEXT/JSPS KAKENHI under Grant Numbers JP23K07820, JP23K21386, and JP25K22562; JST Adaptable and Seamless Technology transfer Program through Target-driven R&D (A-STEP) under Grant Number JPMJTM22C4; Research and Study Project of Tokai University Research Organization; Tokai University School of Medicine Research Aid; Research Grant of the Princess Takamatsu Cancer Research Fund; Research Grant of the Kobayashi Foundation.
Author information
Authors and Affiliations
Contributions
AAI, TT, MK, NW, and HH performed the experiments and analyzed the data. A.A.I. and TY drafted the manuscript and prepared figures. H.M. and M.O. generated the genetically modified mouse. T.M. provided the materials for the study. T.Y. designed and supervised the study. All the authors contributed to the article and approved the submitted version for publication.
Corresponding author
Ethics declarations
Competing interests
TM discloses research funding from Astellas, Daiichi Sankyo, Kowa, and Renascience, Inc. The authors declare that the research was conducted in the absence of commercial or financial relationships that could be construed as potential conflicts of interest.
Ethics approval statement
All animal experimental procedures and protocols were designed according to the PREPARE guidelines [58] and reviewed and approved by the Institutional Animal Care and Use Committee at Tokai University (approval number: 243008). Animal handling and experimental procedures were performed in compliance with the ARRIVE guidelines 2.0 [59] and other relevant guidelines and regulations.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ibrahim, A.A., Miura, H., Terada, T. et al. Inflammatory macrophage-derived plasminogen activator inhibitor-1 exacerbates inflammation through efferocytosis inhibition. Cell Death Discov. (2026). https://doi.org/10.1038/s41420-026-03076-0
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41420-026-03076-0