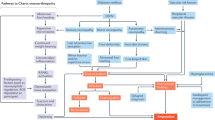
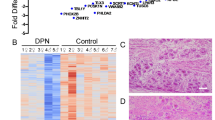
Abstract
Peripheral neuropathy (PN), the most common complication of diabetes, leads to sensory loss and associated health issues as pain and increased fall risk. However, present treatments do not counteract sensory loss, but only partially manage its consequences. Electrical neural stimulation holds promise to restore sensations, but its efficacy and benefits in PN damaged nerves are yet unknown. We designed a wearable sensory neuroprosthesis (NeuroStep) providing targeted neurostimulation of the undamaged nerve portion and assessed its functionality in 14 PN participants. Our system partially restored lost sensations in all participants through a purposely calibrated neurostimulation, despite PN nerves being less sensitive than healthy nerves (N = 22). Participants improved cadence and functional gait and reported a decrease of neuropathic pain after one day. Restored sensations activated cortical patterns resembling naturally located foot sensations. NeuroStep restores real-time intuitive sensations in PN participants, holding potential to enhance functional and health outcomes while advancing effective non-invasive neuromodulation.
Similar content being viewed by others
Introduction
Diabetes is a chronic disease affecting 422 million individuals worldwide1. It can occur as a result of genetic or environmental factors and has been linked to obesity and low physical activity2. Diabetes and its complications have a significant financial impact on the healthcare systems currently globally estimated at US$760 billion, with a projected increase to US$825 billion by 20303. Diabetic peripheral neuropathy is a neurodegenerative disorder, representing the most prevalent complication of diabetes affecting up to 50% of patients over their lifetime4.
Peripheral neuropathy (PN) is slowly progressive5, first affecting long sensory axons causing symptoms such as sensory loss and pain6, followed by autonomic axons, and eventually by larger diameter motor axons4. The mechanisms behind the development and progression of PN are not completely understood but are related to metabolic and micro-vessel alterations which result from chronic hyperglycemia exposure or cardiovascular comorbidities7. Risk factors include insufficient glucose management8,9, poor foot care, lifestyle (obesity, smoking, low physical activity), and cardiovascular comorbidities10,11,12,13. PN can also develop due to many other conditions, as a side effect of chemotherapy, or for unknown reasons14. PN has major health consequences, including foot ulceration, which may lead to lower-limb amputation15,16, and neuropathic pain that often leads to depression, anxiety and sleep disorders, as well as reduced quality of life17. Lower-limb complications of PN and neuropathic pain comprise a significant burden for both patients, increasing morbidity and mortality, and for the healthcare system16,18. Despite this, treatment options are limited. For instance, commercial medications are available for ulcer treatment, aiming at healing the wound once it is already formed, and avoiding infections that lead to necrosis and amputation. However, they do not address the primary mechanism causing the condition, i.e., the lack of sensory feedback. Consequently, they cannot improve the associated walking and balance issues, thus they are unable to prevent the formation of new ulcers. Indeed, the lack of sensory feedback in PN leads to functional deficits during gait, as an increased risk of falls and low balance19,20 and it is considered the strongest risk factor for diabetic foot ulceration12,18. In PN patients, the increased fear of falls, fall-related injuries and the forementioned functional deficits trigger a vicious cycle. Low physical activity and mobility, lead to more progressive diabetes and neuropathy, increased metabolic risks, sensory loss and increased foot ulcerations, which can ultimately lead to limb amputation21.
Restoring sensory feedback has the potential to break this vicious cycle, resulting in several health and functional benefits. While sensory feedback restoration has been tested in amputees with both invasive22,23,24,25 and non-invasive26,27,28,29,30,31,32 approaches, studies in neuropathic groups with similar symptoms (sensory loss), such as non-amputated patients PN, are limited. Oddsson et al.33,34 proposed a solution by providing remapped vibration sensation reflecting plantar pressure measurements at the ankle level. However, vibratory feedback is strongly limited by the bulkiness, rigidity and power consumption of the actuators35, and the remapped approach requires a learning phase to integrate new information during functional tasks, which limits patient adoption29,36. A different approach has been followed by Najafi et al.21,37, who exploited SENSUS, a stimulator designed for pain treatment, to examine the therapeutic effectiveness of plantar electrocutaneous stimulation. They showed some limited improvements in motor performance and plantar-sensation in participants with PN. However, they do not elicit the distal, somatotopic (lost) sensation but rather stimulate in-loco (under the electrodes) where the skin area is poorly sensitive and less excitable, while also preventing the dynamic walking of patients. Transcutaneous Electrical Nerve Stimulation (TENS) at the knee level has been adopted by NeuroMetrix QUELL exclusively to treat neuropathic pain38, with limited results39 and without testing its effects on functions and mobility. Similarly, Bosi and al, tested a long protocol of three series of 10 treatment sessions of frequency-modulated electromagnetic neural stimulation, resulting in only partial pain reduction at the conclusion, limited to a subset of participants. There were no significant improvements in sensory thresholds (vibration, NCV, warm), except for cold sensation, and the effects on function and mobility were not assessed. At the same knee location as in NeuroMetrix QUELL, TENS showed the potential to restore somatotopic sensations30, projected sensations in the foot sole, but only in amputees and limited to statically laying down (no walking ability).
Considering the limits of knee-positioning, we searched for another leg position proximal to damaged insensitive feet, where the nerves are sufficiently close to the skin to be stimulated via superficial stimulation, obtaining the somatotopic sensations in the feet. We hypothesised that this can be achieved close to ankle level. However, it remains unknown if neurostimulation on damaged nerves. such as those in PN participants can elicit perceivable sensations and whether such stimulation could lead to health, pain, or functional benefits in daily activities.
To this aim, we designed a wearable sensory neuroprosthesis (NeuroStep) to restore lost sensations by providing targeted neurostimulation at the ankle level. We tested it in a feasibility study in 14 participants with PN, evaluating the effects on real-time tasks with functional outcomes and pain, and the cortical activation related to the elicited sensations. This is achieved by stimulating the damaged nerves at the ankle level with a purposely designed neuroprosthetic sock to provide somatotopic projected fields (PFs) in the different foot locations. We objectively evaluated the characteristics and responses of the PN-damaged nerves to the injected charge in terms of perceptual threshold and sensitivity to stimulation via psychometric measurements and compared them to measurements in healthy individuals. Then, we tested this neuroprosthesis’s ability to dynamically restore lost foot sensations and improve mobility in functional tasks related to daily life activities. To understand how these artificially restored sensations are processed in the brain, specifically in the primary somatosensory cortex (S1), we used functional MRI (fMRI). We explored whether somatotopic sensations restored through neurostimulation at the proximal nerve level, eliciting PFs in the foot, activate the same S1 areas as when the foot is stimulated directly. Finally, we also assessed reported neuropathic pain after a day of use of the NeuroStep system.
Results
Targeted purposely designed neurostimulation partially restores lost sensation in PN participants
We developed NeuroStep (Fig. 1A), a wearable neurostimulation system restoring lost feet sensation in real-time, and preliminary evaluated its effects during a one-day study in PN participants (N = 14). This is achieved by stimulating the damaged nerves at the ankle level with a purposely designed neuroprosthetic sock (Fig. 1A) to provide PFs in different foot locations. The neuroprosthesis is composed of matrices of multiple electrodes (Fig. 1B) to target three lower-limb nerves: peroneal, posterior tibial (medial plantar, lateral plantar and medial calcaneal branches) and sural. We engineered the optimal position, number and dimension of electrodes to be able to successfully target the desired nerves. The electrodes are placed between the malleoli on the dorsal part of the foot for the peroneal array, between the heel and medial malleolus for the posterior tibial array and between the heel and lateral malleolus for the sural array (Fig. 1B). The number of electrodes and overall dimension of the arrays have been designed considering the average anthropometric measures for each specific key area to in the diverse population of PN participants.
A NeuroStep is a wearable neuroprosthesis for closed-loop neurostimulation of damaged nerves of PN patients. (1) Force-sensitive insole sends foot-ground information. (2) The system controller receives insole data, selects different electrodes and modulates specific stimulation paradigms (found during calibration). (3) Stimulating sock with different electrodes mapped to different insole sensors. During gait, when different sensors are activated, the mapped sock channels are stimulated, and the participant perceives a sensation in the specific areas. B Electrode Sock Array Design. Anthropometric measures for key areas of the foot and ankle and specifications for array design with final number and position of electrodes. C NeuroStep calibration. 1: Quantitative Sensory Testing was performed with a brush, light touch, and a 10 g monofilament to evaluate the sensory loss of PN participants. 2: Electrical stimulation paradigms were calibrated, and appropriate active sites were personalised to achieve targeted sensory restoration. NeuroStep targets three lower-limb nerves: peroneal, posterior tibial (medial plantar, lateral plantar and medial calcaneal branches) and sural. 3: Calibration was performed using a software app to record the user feedback and select the next stimulation paradigm.
For each participant, a personalised calibration phase was performed using a custom-designed software app (Figs. 1C, 2A) developed to wirelessly control the system, to find the combination of electrodes and electrical charge for an optimal somatotopic and pleasant sensory restoration. The app allows the participant and the experimenters to easily control the neuroprosthesis via software by selecting different electrodes and stimulation paradigms, testing them, and directly recording the respective perceived sensations (Figs. 1C, 2A). The experimenter selects the desired parameters (e.g., charge, electrode) and sends them to the system. The experimenter controls via software which electrodes to select; this information is sent to custom-made MUX-PCBs that close the circuit of selected electrodes in each array (Supplementary Fig. S1). The participant reports on a tablet the type, intensity and location of the sensation. This information is used iteratively to modify and optimise the stimulation. When the best parameters were found for a participant (a combination of electrodes and stimulation that elicited pleasant somatotopic sensations in the desired areas of sensory loss), these values were saved for dynamical functional experiments. We achieved a real-time closed-loop wearable system (under 50 msec) by mapping sensors in the insoles to different electrodes in the sock. Specifically, the force-sensitive insole (1) sends wirelessly foot-ground information about gait to a system controller (2). The controller translates the gait pressure information into stimulation parameters. Then it selects and activates via software using a multiplexer the specific electrodes of the stimulating sock and modulates personalised stimulation paradigms (found during personalised calibration) (3). During gait, when different sensors are activated (e.g., a sensor on the back of the insole during heel strike and one on the front of the insole during toe-off), the specific sock channels that elicit a somatotopic sensation in the pressed area (heel and frontal part of the sole sensations) are stimulated. The design of the NeuroStep neuroprosthesis (sensing insoles, processing unit and stimulator with electrodes sock) and its functioning during dynamic walking is shown in Supplementary Movie 1.
A Custom designed software app with interactive GUI. On the left is the experimenter app, and on the right is the participant app to report the sensory feedback in terms of intensity, type and location. B Quantification of the perceived area of sensory loss and electrically evoked stimulation using the interactive GUI. The areas of sensory loss, elicited and restored sensations are then calculated. C Lost sensations are restored with targeted neurostimulation. From left to right: decrease in overall sensory loss after restoring sensation (N = 14 PN participants, Wilcoxon Signed-Rank test alternative two-sided, W = 14 and p = 2.6e-5), percentage of lost area that has been restored with neurostimulation (N = 14 PN participants, One sample Wilcoxon Signed-Rank test, W = 105 and p = 1.2e-4), and type of elicited sensation. D Example participants with lost, evoked, and restored sensation areas. ***p < 0.001. Barplots show the mean ± sem. Boxplots: Boxes: Q1 (25th), median (50th) and Q3 (75th). Whiskers with minimum and maximum: 1.5*IQR below Q1 and above Q3. Outliers outside 1.5*IQR below Q1 or above Q3 are not shown.
In Supplementary Movie 2, it can be observed that PN participants experienced a loss of touch sensation in various parts of their feet. This is illustrated in three distinct participants. The video shows the Quantitative Sensory Testing (QST) being conducted and participants reporting an absence of sensation when touched while blindfolded on different locations of the sole of the foot. Placebo trials were also conducted to verify the accuracy of these responses. QST areas of sensory loss for all participants are shown in Supplementary Fig. S2 (grey areas). Quantitative sensory testing (brush, touch and monofilament) (Figs. 1C, 2B) showed that PN participants had on average 47.4% area of sensory loss in the left and right feet over the dorsal and plantar areas (Fig. 2C). After evaluating sensory loss, we calibrated the neurostimulation to elicit somatotopic sensations overlapping with the sensory loss and we computed the total area of elicited and restored sensations. Neurostimulation consisted of biphasic, charge-balanced, rectangular pulses at a fixed frequency (50 Hz, as previously used in other studies29,40,41) while modulating the amplitude and pulse width. Amplitude was modulated only during the calibration phase to find personalised parameters for each participant. The pulse width was modulated both during the calibration and real-time during functional tasks depending on gait parameters (foot-ground interaction measured through force sensors integrated in the insole of the system). An example of digitalised feet maps is shown in Fig. 2D, with locations of lost, somatotopically evoked and restored sensations. The foot maps and percentages for each participant are shown in Supplementary Figs. S2, S3. In Supplementary Movie 2, we show three PN participants with NeuroStep neurostimulation feedback, able to feel again restored sensations in specific feet locations where previously they reported completely lost sensations. Stimulation successfully partially restored lost sensations, decreasing the foot sensory loss from 47.4 ± 8.4 to 34.0 ± 6.2 (Wilcoxon Signed-Rank test, p = 0.00012) (Fig. 2C). Overall, we elicited a restored sensation (over the area of sensory loss) of 27.0 ± 3.2% (One sample Wilcoxon Signed Rank test, p = 8.30e-06), on the dorsal and plantar sides of the foot (Fig. 2C). Different type of sensations, including physiologically plausible ones were elicited (Fig. 2C). The most common reported sensations were vibration and tingling (26% and 44% respectively), followed by electricity (9%) and touch (6%).
PN participants have higher nerve charge threshold and lower sensitivity compared to healthy controls
To quantitatively evaluate sensory loss and capability to restore some of these sensations in PN nerves (Fig. 3A), we compared the minimal required charge to elicit a reliable sensation, nerve conduction velocities and sensitivity of PN nerves to healthy controls (N = 41, measure from 22 healthy subjects) (Fig. 3B–D). The protocol used to define the charge thresholds similar to the one proposed in refs. 23,42 can be found in Methods, Electrical sensory feedback characterisation. This step is important to understand the feasibility of the device for a large population with differences in perceptual threshold (whether the stimulator and the system deliver enough charge to stimulate different PN participants) and to understand how many different levels of pressure (foot-ground interaction) can be perceived by the participants.
A Protocol to test and compute sensitivity through a tactile discrimination task. The sensitivity is proportional to the number of electrical intensity levels the participants can perceive during a modulated task. B On the left: pa sychometric curve with mean ± std representing the JND of each nerve in PN participants and healthy controls. On the right: boxplot comparison of JND (intensity at 75% probability – point of subjective equality at 50% (PSE)) between neuropathic and healthy participants. N refers to the number of nerves tested: NC = 41, NPN = 13, 12, 14, respectively for peroneal, posterior tibial and sural. Mann Whitney U test alternative two-sided, peroneal (U = 518, p < 0.0001), posterior tibial (U = 471, p < 0.0001), sural (U = 555, p < 0.0001). C Threshold charge to elicit a perceptual sensation in neuropathic and healthy control participants. Number of nerves tested: NC = 41, NPN = 22. Mann Whitney U test alternative two-sided, peroneal (U = 709, p = 0.0002), posterior tibial (U = 813, p < 0.0001), and sural nerves (U = 717, p = 0.0001). D Sensory restoration capabilities of NeuroStep depends on the progression of neuropathy and nerve degeneration. The sural nerve conduction velocity is a predictor of the NeuroStep abilities to elicit or not a sensation. ***p < 0.001. Boxplots (in B and C). Boxes: Q1 (25th), median (50t) and Q3 (75th). Whiskers with minimum and maximum: 1.5*IQR below Q1 and above Q3. Outliers outside 1.5*IQR below Q1 or above Q3 are not shown.
In PN nerves, the mean perceptual charge threshold to elicit a sensation was 4.1 ± 0.9 µC, 9.6 ± 2.9 µC, and 7.2 ± 1.9 µC in the peroneal, posterior tibial, and sural nerves respectively (Fig. 3C). The mean charge threshold in healthy nerves was 1.5 ± 0.1 µC, 1.5 ± 0.1 µC, and 1.2 ± 0.1 µC in the peroneal, posterior tibial, and sural nerves respectively. The threshold charge was significantly higher for PN nerves than healthy controls (Mann Whitney U test peroneal (p = 0.0002), posterior tibial (p = 0.0000), and sural nerves (p = 0.0001)) (Fig. 3C). Similarly, the charge required to elicit a strong sensation (i.e., an 8/10 sensation in a scale where 0 is not felt and 10 is unbearably strong sensation) was significantly higher (Mann Whitney U test, p < 0.0001 for all nerves) for neuropathic nerves than healthy control (Supplementary Fig. S4). We showed that the just noticeable difference (JND), i.e., the discriminability of electrical stimulation43, between PN nerves and healthy controls is significantly higher with neuropathy (Mann Whitney U test, p < 0.0001 for all nerves). The mean JND in PN was 2377.3 ± 1287.5 nC, 1524.3 ± 475.0 nC, and 2762.0 ± 1164.4 nC in the peroneal, posterior tibial, and sural nerve respectively. The mean JND in healthy controls was 104.1 ± 8.0 nC, 104.5 ± 7.7 nC, and 93.8 ± 6.9 nC in the peroneal, posterior tibial, and sural nerves respectively (Fig. 3B). The average Weber Fractions (WF) normalised by reference stimulus44 in each of these nerves are shown in Fig. S5. The WFs were significantly higher for PN participants than healthy controls (Mann Whitney U test, p < 0.0001 for all nerves). Higher WFs indicate a lower sensitivity. The nerve conduction velocities (NCVs) of the neuropathic participants (N = 7) measured in the clinical setting with standard sensorimotor nerve conductions tests in the sural nerve were compared to healthy, age-matched NCVs reported in the literature45,46 and found to be significantly lower (Mann Whitney U test, peroneal p = 2.38e-5, tibial p = 3.31e-8, sural p = 1.00e-8), The mean NCVs of the PN participants included in this study were 39.5 ± 1.0 m/s. The mean NCVs of healthy, age-matched controls were 53.2 ± 5.7 m/s45,46 (Fig. 3D). The sensory NCV (sural) of PN participants was evaluated with respect to the sensations elicited by the neurostimulation in the respective nerve (Fig. 3D). NeuroStep was able to restore sensation when NCV was higher than 33 m/s (Fig. 3D).
Walking ability improved in PN participants using NeuroStep sensory feedback real-time
The artificial sensations were mapped to force sensors in the sensorized insole (e.g., the sensor under the heel was coupled to a specific combination of electrodes in the sock eliciting a sensation on the heel), while the values of the charge were modulated proportionally to the range of force exerted and measured by sensorized insole. The sensations were restored in real time (under 50 ms). Using the previously calibrated electrical sensory feedback and respective charge values, PN participants performed functional tasks (10 m walking test47 and functional gait assessment (FGA)48) with and without the restored sensation, without any prior gait training. One participant did not complete the functional tasks for time reasons. The average FGA score of all participants was significantly improved from 20.7 ± 1.53 without feedback to 23.5 ± 1.16 with feedback (Wilcoxon Signed Rank test, p = 0.008) (Fig. 4A left). Of the 13 participants who completed functional gait testing, 9 had a score lower than 23 indicating a high risk of falls48,49. In this subset of participants, the FGA score improved from 18.6 ± 1.38 without feedback to 22.5 ± 1.36 with feedback (Wilcoxon Signed Rank test, p = 0.0004). Single participant results highlighted that 5 individuals, of 9 with a high risk of falls, had a clinically significant improvement in their FGA score (Fig. 4A right). Examples of FGA tasks with NF and SF are shown in Supplementary Movies 3–4. In Supplementary Movie 3, PN participant S6 significantly improves in two different FGA tasks and explains how the restored sensations through neurostimulation enhanced mobility, coordination and confidence while performing functional tasks. Participant’s acceptability and verbal feedback are also provided. In Supplementary Movie 4, PN participant S13 shows a substantial improvement in balance and speed during a walking task. While initially at risk of falling when using NF, the use of SF enabled S13 to complete the gait task quickly and successfully. The cadence was extracted from the insoles and normalised by walking speed. The median cadence calculated in a 10-metre walk tests (6 repetitions per condition) was found to significantly decrease by 1.16 steps/min with sensory feedback (Repeated Measure ANOVA, p = 1.20e-11), i.e., participants were confident in taking longer steps. A significant decrease in cadence was observed in 7 out of 13 participants (Fig. 4B).
A Functional Gait Analysis (FGA) performance with (SF) and without (NF) sensory feedback. Healthy Age Ranges obtained from Walker et al.107. On the left: Box plots show the median score in all participants (NPN = 13) and in participants at a high risk of falls (NPN = 9) (Baseline FGA < 2349). The individual breakdown shows the raw score and change in score. In box plots on the left: Wilcoxon Signed Rank test alternative two-sided, **p < 0.01 (W = 9, p = 0.008), ***p < 0.001 (W = 1, p = 0.0004). In individual plots on the right: ### clinically significant change33. B Walking Cadence with (SF) and without (NF) sensory feedback during the 10-metre walk test. Box plots show the cadence in each participant with SF and NF. Repeated Measure ANOVA (NPN = 13), ***p < 0.001 (F statistic = 607.98, p = 1.2e-11). For single-subject results (N refers to the number of repetitions per subject, NSF = 6, NNF = 6), the Wilcoxon Signed Rank test ***p < 0.001. S12 did not perform functional tasks and is therefore excluded from this assessment. Boxplots (in A and B). Boxes: Q1 (25th), median (50t) and Q3 (75th). Whiskers with minimum and maximum: 1.5*IQR below Q1 and above Q3. Outliers outside 1.5*IQR below Q1 or above Q3 are not shown. Barplots (in B) show the mean ± sem.
Targeted neurostimulation effects on neuropathic pain
Neuropathic pain was evaluated through the Neuropathic Pain Symptom Inventory questionnaire (NPSI)50 taken before the day of targeted neurostimulation intervention and then again 24 hours later. Cumulative results are shown in (Fig. 5A). Single participant results are shown in (Fig. S6). On the day after the intervention, we measured a clinically significant decrease of 30.4% ± 9.2% of overall NPSI score in the 12 participants who reported pain (Fig. 5B) (Wilcoxon Signed Rank test, p = 0.0048). Clinical significance is defined as a 30% reduction in pain, i.e., the threshold considered to define responders endpoints in clinical trials for pain treatment51,52,53. The dimensions of NPSI mainly responsible for the decrease in pain was burning, paroxysmal pain, and paraesthesia, found to clinically decrease by 37.7% ± 11.2%, 48.1% ± 13.3%, and 31.8% ± 14.1% respectively51,54,55 (Fig. 5C). Changes in spontaneous pain and pain attacks measured through the NPSI were not clinically significant.
A Average Neuropathic Pain Symptom Inventory (NPSI) before and after intervention (NPN = 12 participants). Wilcoxon Signed Rank Test 2-sided, W = 63, p = 0.0049. B Examples of reported areas of pain and evoked sensation. C Constant pain components of the NPSI (NPN = 12 participants). Wilcoxon Signed Rank Test 2-sided, burning: W = 36, p = 0.0078, paroximal: W = 51, p = 0.014, paraesthesia: W = 67, p = 0.026. *p < 0.05, **p < 0.01. ###=clinically significant change (reduction of 30%51,54,55). Barplots (in A and C) show the mean ± sem.
Somatotopic sensations elicit cortical activity similar to cutaneous foot sensations
Next, we aimed to better understand the neural basis of the NeuroStep intervention and how the somatotopic sensations are processed in the brain. Due to the somatotopic organisation of S1, sensations of each body part56,57,58,59 are represented at an anatomically specific cortical location. To investigate the somatosensory processing of restored sensations, we explored whether these restored sensations, though targeted proximal stimulation activate similar cortical representations in S1 as when the foot is stimulated directly. Healthy (n = 12) and PN (n = 5) participants underwent 3 Tesla functional MRIs, while they were neurostimulated in three different conditions (proximal somatotopic, distal in-foot, control on-ankle, which for simplicity will be called somatotopic, in-foot and on-ankle afterwards) (Fig. 6A). The somatotopic condition consists of targeted proximal nerve stimulation at the ankle level to elicit distal PFs in the foot (as used in the previous experiments). The in-foot condition consists of applying electrocutaneous stimulation locally on top of the previously elicited PFs (naturally located locations over the foot sole). The on-ankle condition involves electrocutaneous stimulation at the ankle level while avoiding nerve activation, thereby acting as a control condition, where electrodes are placed at a similar location as in the somatotopic condition, but no PFs were elicited. For each of these conditions, three different locations (i.e., corresponding to the peroneal, tibial and sural nerves in somatotopic stimulation) were stimulated (Fig. 6A and Supplementary Fig. S7). Cortical activity evoked by somatotopic neurostimulation were compared to those elicited by in-foot and on-ankle stimulations. We compared overall activity elicited (i.e., across locations) (Fig. 6B), spatial similarity across conditions (Fig. 6C), and ability to classify (distinguish) the three locations within each condition (peroneal, posterior tibial and sural cortical activation, Fig. 6D) in a functionally defined region of interest (ROI) of the S1 foot and ankle area.
A Experimental Set-Up: The protocol consisted of three different conditions: somatotopic, in-foot, and on-ankle stimulation. Each condition was tested in four different runs of 36 stimulations of 4 s each, in which the three target locations (peroneal [red], tibial [blue], sural [yellow] nerves) were presented in a counterbalanced and predefined random order. During each run, an attentional task (counting gaps in stimulation) was performed. Each trial was performed with 3 T fMRI recorded. The processing is detailed in Methods. B Averaged z-standardised activity in the somatotopic (somato), in-foot and on-ankle conditions in a functionally defined foot and ankle S1 region of interest in healthy (dark colours) and PN (light colours) participants. In-foot activation for PN participants is statistically lower than healthy controls (Mann Whitney test alternative two-sided, NH = 12, NPN = 5, U = 11, *p = 0.048). C Spatial overlap of neural activity in the ROI (expressed using the DOC) between in-foot/somatotopic (Foot-Som; circle), in-foot/on-ankle (Foot-Ank; triangle), and on-ankle/somatotopic (Ank-Som; square) conditions. The DOC ranges from 0 (no spatial overlap) to 1 (perfect spatial overlap). The line plots show the DOC for activity thresholded using a Z threshold ranging from 1 to 3.2, with the line and shaded area representing the mean and standard deviation respectively. Statistical significance between condition pairs was determined for activity thresholded using Z > 2.2, as depicted in the bar plots on the right. For healthy participants, the overlap somatotopic/in-foot was higher than vs in-foot/on-ankle, Friedman test alternative two-sided, NH = 12, Q = 8.90, *p = 0.012. PN participants: Friedman test alternative two-sided, NPN = 5, p > 0.05. D Spatial distinguishability of the different stimulation locations (peroneal, tibial and sural) for each condition (somatotopic (somato), in-foot and on-ankle). The average accuracy of a three-class SVM classifier (Leave One Run Out cross-validation) among participants is reported. For healthy participants, somatotopic stimulation provides higher distinguishable patterns than on-ankle, Friedman post-hoc Nemeny test, test alternative two-sided, NH = 12, Q = 6.94, *p = 0.031. PN participants, Friedman post-hoc Nemeny test, test alternative two-sided, NPN = 5, p > 0.05. Barplots (in B, C and D) show the mean ± sem.
Resulting levels of cortical activation in the ROI (Fig. 6B) during the in-foot condition were significantly lower (Mann Whitney, p = 0.048) for PN participants compared to the healthy controls (Fig. 6B). This was expected, given the reduced or abolished sensations recorded during in-foot stimulation with PN. Instead, the level of somatotopic and on-ankle cortical activation in the ROI was not significantly different between PN and healthy participants (Mann Whitney, p > 0.05), indicating that the proximal somatotopic stimulation targets the NP nerves in a location that is still healthy enough to elicit plausible referred somatotopic sensations. The spatial overlap between representations of the different conditions within the S1 ROI was computed using the DICE Overlap Coefficient (DOC)60,61. The DOC was computed between each pair of conditions (for activity during stimulation of all locations vs rest). The DOC ranged from 0 (no spatial overlap) to 1 (perfect spatial overlap) and were computed for different z-thresholds. For healthy controls, given the overlap in perceived sensations between the somatotopic and foot conditions, we expected the highest spatial overlap in activity between these conditions and the lowest overlap between the foot and ankle conditions. Indeed, we found higher spatial overlap between the somatotopic and in-foot conditions compared to the in-foot vs on-ankle conditions for healthy participants (z-threshold of 2.2, multicomparison with Friedman test p = 0.0116; post-hoc Nemenyi test somatotopic/in-foot vs in-foot/on-ankle p = 0.0118, the other post-hoc comparisons were not significant (p > 0.05) Fig. 6C). Given the low activation of in-foot stimulation for PN subject, we were not expecting a high overlap between the somatotopic stimulation and in-foot stimulation conditions for the PN group. The DOC was not statistically different among condition pairs for PN participants (Friedman test p > 0.05).
Finally, we used multivariate pattern analysis to evaluate the spatial distinguishability of the three stimulated locations in each condition by applying an SVM classification algorithm with a linear kernel (Fig. 6D). For example, the three nerves stimulated in the somatotopic conditions elicit sensations in three distinct areas of the foot and elicit spatially distinct brain activity patterns in our ankle-foot S1 ROI. In healthy participants, classification accuracies in the three conditions were significantly different between the three conditions (Multicompare Friedman test, p = 0.0311). Specifically, the somatotopic condition had a better spatial distinguishability than the ankle condition (Post Hoc Nemenyi test, p = 0.0380) which was most likely driven by spatially distinct PFs in the foot, while sensations at the ankle level are more contiguous. Somatotopic vs in-foot and in-foot vs on-ankle were not significantly different in the post-hoc Nemenyi test. While a trend of higher classification accuracy in the somatotopic compared to in-foot and on-ankle conditions is observed in the 5 diabetic participants, no significant differences were found between conditions (Fig. 6D).
Discussion
In this study, we engineered NeuroStep, a non-invasive wearable sensory neuroprosthesis and we validated its effects in a feasibility study with participants with PN. We demonstrated the feasibility of restoring lost foot sensations in PN participants affected by distal sensory loss, using purposely developed neurostimulation. We showed that PN individuals with impaired plantar sensation and high fall risk had functional improvements (e.g., gait) when assisted with somatosensory neuroprostheses. Furthermore, PN individuals reported a reduction effect on neuropathic pain after one day of use. The brain representation of restored somatotopic sensations had a high overlap with the cortical representations of the corresponding loco foot sensations, allowing for fast and intuitive integration of the artificial feedback without prior training.
We were able to partially restore lost sensations in patients with years of disease progression and, therefore, loss of feeling in several areas of their feet. It was not known a priori whether stimulation of these damaged nerves could elicit distal PFs in the PN feet, within the locations of sensory loss. So, to test this, we designed neurostimulation to target proximal branches of damaged nerves at the ankle level where they are near the skin surface and accessible non-invasively. There, the nerves are still partially healthy since sensorimotor neuropathies affect the most distal parts of the extremities first4,12,62. Achieving sensory restoration in all of the patients tested, in at least one nerve, is the first scientific milestone that validates the viability of this approach.
We then investigated the specific characteristics of the artificially restored sensation in terms of charge threshold and sensitivity, to understand the phenotype of PN with respect to healthy nerves. We observed that the required charge for eliciting a sensation was significantly higher for neuropathic participants than for healthy controls. This is consistent with other studies that found the charge threshold63 and maximum tolerable charge64 to be significantly higher in PN. In addition, the sensitivity to electrical stimuli, as measured by JND experiments, was significantly lower for PN participants than for healthy individuals. Lower sensitivity could negatively affect a PN participant’s ability to recognise the intensity of different stimuli, for example associated with the level of pressure of the heel on the floor. This increase in charge threshold and decrease of nerve sensitivity to stimuli is to be expected due to the degenerative progression of peripheral neuropathy, which evolves through demyelination and loss of nerve fibres65 and is confirmed by a lower nerve conduction velocity.
This neuroprosthesis was able to elicit somatotopic sensations. Regarding the type of sensation, it was able to elicit homologous sensation, i.e., the natural sensation of touch35, only in a limited number of cases. Indeed, most sensations were described as sensations like vibration and tingling. Near-natural tactile sensation has been achieved only through invasive neural technologies both at the peripheral level22,25,66 and at the central level67,68,69. While restoring natural touch information with non-invasive electrical stimulation remains an unresolved challenge27,29,30,35,40, these paresthetic sensations can still be subconsciously integrated into the sensory-motor scheme42. Despite not eliciting natural sensation, non-invasive stimulation technologies, still have many advantages, namely that they do not require a surgical procedure, avoiding extensive post-surgery care and complications35. In addition, they are less expensive and do not have biocompatibility issues70, significantly decreasing the risk of infection which is particularly high for diabetic participants who already have reduced wound healing capabilities35,71,72. The intuitiveness and subconscious integration of NeuroStep targeted neurostimulation was also confirmed by improvements in functional tasks related to daily activities. FGA improved overall, and in particular, it improved in individuals at a high risk of falls (baseline FGA < 2348,49). This is crucial, considering that, after possible falls, PN participants have an occurrence of injuries 15 times higher than healthy individuals73. Moreover, falls can result in serious injuries74,75 requiring medical treatment76, and reducing health and shortening survival77, which can strongly impact the healthcare system78. At the same time, while using NeuroStep, cadence during level-ground walking improved (lower cadence means fewer, longer steps for the same normalised velocity), which is possibly a measurable reflection of higher confidence, and contributes to lower metabolic consumption and lower cardiovascular risk31,79.
After one day of use, PN participants reported a reduction in neuropathic pain, as measured by the NPSI questionnaire 24 hours after use. This may be explainable through the gate control theory stating that the stimulation of large diameter sensory fibres blocks the signalling of small nociceptive fibres to the brain and therefore decreases pain80. Our intervention with neurostimulation targets the sensory components of pain by stimulating these large diameter sensory fibres55,81,82, activating the inhibitory mechanism.
Other studies have explored different approaches to addressing neuropathic symptoms. For instance, Najafi et al.21 studied the effects of plantar stimulation over the area where stimulations and elicitable cells are missing (not proximal somatotopic as in our case) after six weeks of use, while Oddsson et al.33 tested their system (remapped at the level of the ankle eliciting an in loco sensation) for over ten weeks, with initial evaluations and improvements observed after two weeks. Immediate improvements in our system are most probably due to the fact that the restored sensations are somatotopic, matching the position where the sensory information was originally expected, and more comprehensive since we stimulate the proximal fibers, which are yet alive, contrary to what happens at their ending. This is consistent with how somatotopic sensations have been shown to require no training or learning phase for the user35,36. In addition, the high efficacy of our neurostimulation may be attributed to the precise targeting of the damaged nerves responsible for neuropathic pain, unlike the inadequate and imprecise placements of traditional TENS83. In future studies, it would be interesting to evaluate how these short-term effects evolve over a longer time period, to explore further improvements and long-term changes of somatotopic targeted stimulation. To confirm the hypothesis that somatotopic sensations are processed at the brain level spatially similarly to direct foot sensations, we exploited fMRI. We stimulated healthy participants with intact foot sensations and analysed the neural correlates of different stimulations: somatotopic, in-foot, and on-ankle.
We showed that somatotopic stimulation elicited cortical activations that spatially overlapped with the ones elicited by foot stimulation, supporting somatotopic stimulation as a valid physiologically accurate alternative to provide foot sensations. As expected, it was not possible to elicit plausible sensations in loco in the foot of PN participants, i.e., when stimulating the foot directly, which is attributed to the distal neuropathy and consequent sensory loss of these participants. The PN participants reported lower or no (consciously) perceptions and exhibited lower cortical activation during foot stimulation. This further supports the use of stimulation on proximal - still partially healthy - PN nerves, to elicit lost distal foot sensations. Furthermore, fMRI results show the limitation of in-loco electrocutaneous approaches like SENSUS21, which stimulates under the sole of the foot, where PN patients did not perceive sensations both at the conscious level (no sensation reported) and unconscious (low fMRI cortical S1 activation) and where it is not possible to stimulate dynamically during walking.
In addition, somatotopic stimulation in healthy controls elicited three distinct brain activity patterns corresponding to the three different stimulated nerves. These somatotopic activities could be decoded with higher classification accuracy than the on-ankle condition. This better distinguishability of locations together with the higher overlap between somatotopic/in-foot (physiologically accurate) with respect to in-foot/on-ankle, make NeuroStep stimulation a better alternative than remapped approaches such as those used by Walkasins33. Indeed, re-mapped sensations at the ankle, not only require a further learning step by the user to match the artificial sensations with the original expected input but also elicit cortical activations which are less distinguishable36. Different levels of nerve and mechanoreceptor damage in PN participants make it difficult to predict results from the cortical activity of fMRI. This, in combination with a smaller sample size, may explain why the results in the PN participants were not consistent.
The somatotopic stimulation we provide allows for intuitive, physiologically accurate, cognitive integration28,84. These benefits combined with pain decrease highlight the wide range of functional and health benefits which this wearable and safe neuroprosthesis has the potential to provide.
Neuropathy is typically progressive5,6, therefore it is important to understand the extent of validity of the present intervention. The success or failure of sensory restoration depends on the severity of the disease, defined by a critical level of demyelination and nerve fibre loss as measured by NCV. We showed that NeuroStep is functional prior to an NCV decrease to ~ 33 m/s. This threshold was defined considering only the patients with available clinical NCV. Since the time (potentially infinite) for calibration was limited by patient availability, we might have been able to find a somatotopic sensation in patients with failed nerve characterisation by performing a longer and more specific calibration process. Considering this conservative estimate of disease severity for NeuroStep use and the typical slow progression of PN over decades5 (approximate rate of NCV decrease at 0.55 m/s per year19,85,86,87,88), we estimate that the device could restore sensation for several years before the progressive neuropathy becomes too severe (Fig. 3D).
Limitations
The limitations of this work include its short-term nature, the absence of a control condition in clinical outcome measures, and the short follow-up, which makes it difficult to draw conclusions about the therapeutic effect and clinical outcomes of the device yet provides sufficient evidence to support its short-term assistive use. The device was tested in a one-day single-session feasibility study, and the current findings require further validation through a longer clinical trial with multiple sessions. Given the lack of control condition and the complex experience of pain89, we cannot rule out that other mechanisms, such as participant engagement, may have contributed to a placebo effect in the decrease of pain. Indeed, a significant reduction in pain could also be achieved through placebo alone86. While the single-group assignment is a standard study design for neurostimulation applications, incorporating a control group in future research would strengthen the conclusions about NeuroStep’s effects on neuropathic pain reduction. It would be relevant to evaluate also possible long-term substantial (50%) pain decreases51, helping to rule out the potential influence of placebo effects. However, developing a credible sham control and proper blinding for neurostimulation is technically challenging90 and raises ethical concerns, especially if the condition being treated is severe or if effective treatments are withheld from the control group. We were also limited in our ability to restore sensation due to the severity of nerve damage. This could be related to the diverse population of neuropathic subjects with different levels of neuropathy and symptoms. Future selection criteria could include NCV to focus on participants who can be better assisted by NeuroStep. Functional improvements should be evaluated depending on the severity of the disease to identify the participants who could better benefits. In a larger patient cohort, confounding factors beyond the severity of neuropathy, such as patient characteristics (e.g., age, gender), should be controlled and their effects evaluated to ensure accurate results. In addition to this, participants were not properly blinded to the conditions, which could have impacted the results. However, proper blinding is not possible in sensory feedback studies since the prerequisite for participants is to clearly perceive the sensations during SF. While this study provides valuable insights into the preliminary effectiveness of NeuroStep, it did not include specific data on patient acceptability. Future studies should incorporate patient acceptability assessments to ensure a comprehensive evaluation of the intervention’s impact91,92. Finally, the expert-guided calibration required to successfully target nerves that innervate the foot at a proximal level is currently very time-intensive and can be automatised in the future to make long-term testing more feasible93,94. Overall, a long-term clinical trial assessing the effects of multiple sessions of targeted neurostimulation on functional, sensory, and clinical outcomes, along with comparisons to a control group, will be crucial to further validate the current findings. Incorporating additional measures (e.g., physiological changes, EEG) and tasks (e.g., VR for multimodal sensory feedback) could also provide a more comprehensive evaluation of participants’ improvements and the device’s effectiveness.
In conclusion, this work showed the design and validation of a wearable somatosensory neuroprostheses to target different neuropathic symptoms. The targeted stimulation showed the potential to tackle functional, health and pain drawbacks of PN and pave the way for further long-term investigations. Future work that focuses on a long-term at-home evaluation with a bigger cohort of patients, would be able to examine more clinical outcomes of use of this device over time and the effect of adherence and compliance on functional and health benefits. Through this, different functional and health outcomes (improvement in tactile sensitivity, ulcers’ prevention capabilities among others) will be tested together with possible plastic changes at the brain level.
Methods
NeuroStep system
We developed the NeuroStep system (Fig. 1) a wearable neuroprosthesis to deliver non-invasive neurostimulation (Supplementary Movie 1). The system was used to provide real-time feedback during functional task performance and is composed of three main components:
-
1.
A Force Sensing Component including:
-
2.
A system controller (ODROID-C2, Hardkernel Co., South Korea) that (1) receives the information from the force sensors (2) encodes the information into stimulation parameters that are sent to the stimulator (3) selects active electrodes in an array via software and send the information to the stimulator;
-
3.
A stimulation component includes:
-
A CE approved portable stimulator (RehaMove 3, Hasomed, Germany) that provides modulated sensory feedback to the user through neurostimulation.
-
Two custom-made MUX-PCBs select active electrodes in each array for personalised calibration (Supplementary Fig. S1);
-
Two smart stimulation socks with three matrices of textile electrodes placed in anatomically plausible positions to target nerves that innervate the foot (peroneal, posterior tibial (medial plantar, lateral plantar and medial calcaneal branches), sural) (Fig. 1B);
-
In addition, the NeuroStep system includes a custom-made graphical user interface (GUI) which can be used to intuitively interact with the system by selecting the stimulation parameters, controlling the stimulation, and selecting the active electrode(s) in the MUX-PCB and socks. The full calibration can be performed via software without changes to the system. The GUI can also save user feedback such as the perceived sensation location, intensity, and type, as described in the section titled “Electrical sensory feedback characterisation”. Parameters and personalised electrodes can be saved to be used after calibration.
Participant recruitment and study design
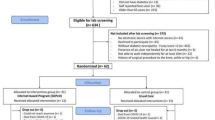
18 participants were recruited (recruitment is detailed in the Ethics section). 4 participants were excluded due to not meeting inclusion criteria upon evaluation (no sensory loss (n = 2) and inability to walk without assistance (n = 1)) or declining to participate (n = 1). A total of 14 PN participants were included in the final protocol of the study. All 14 participants had diagnosed neuropathy with sensory loss, and 12 out of the 14 had neuropathic pain. The study design is shown in Fig. 7. The timeline between enrolment and the first day of testing depended on the availability of the participant but was typically within 2 weeks. The participants were preliminary assessed for eligibility through a questionnaire for pain, qualitative sensory loss as perceived by the participant, and NCV when available from clinical routine (Fig. 7A). The feasibility study is an interventional, not masked, single group assignment study. All participants were assigned to the same intervention (sensory feedback SF restored by targeted stimulation), which was compared to the case in which the same participants were not provided with sensory feedback NF (within-subject comparison or control condition). Intervention and control conditions were presented in a random order. A summary of the participants included in the study is presented in Table 1. Further details are presented in Supplementary Table S2. Sample size (n = 11) was computed a priori using an effect size from mobility effects of 1.1321, α error probability 0.05, 1-β error probability 0.95. The sample size for pain effects (n = 12) was computed using an effect size of 1.0555, α error probability 0.05, 1-β error probability 0.95. Power estimation and effect sizes were based on pairwise comparisons relative to the baseline.
A Study design. First, enrolment was performed at the clinical sites, followed by an assessment for eligibility (see flow diagram in Supplementary Fig. S8 for detailed information). Then patients that satisfied the inclusion and exclusion criteria were allocated to intervention. The timeline between enrolment and the first day of testing depended on the availability of the participant but was typically within 2 weeks. Then, participants performed a full day of tests with (SF) and without (NF) electrically induced sensory feedback. 24 hours later, a follow-up NPSI to assess pain was performed. Available participants that satisfied the inclusion criteria for fMRI testing were then enrolled for a further half a day of scanning. The fMRI scanning was performed up to one month after the first day of stimulation depending on the availabilities of participants and of the scanners. B Detailed protocol of one day of NeuroStep use and fMRI scanning. The time range of each step is shown.
Participants filled out a comprehensive information form including personal data (age, height, weight, shoe size, education level, etc.) and a full description of the location, type, and intensity of neuropathic pain including the Neuropathic Pain Syndrome Inventory (NPSI). Participants’ clinical data, such as medical records and clinical test results were also obtained with permission from their doctors. Types of clinical data included, when available, were nerve conduction velocity (NCV) of the sensory sural, motor peroneal, and motor tibial nerves, diabetes onset time (if applicable), and HbA1c levels over time. All forms recorded on paper were stored in a locked room and when digitalised, were stored on an encrypted hard drive.
PN participants (N = 14) participated in one full day of tests and use of NeuroStep (Fig. 7B). The full day of tests was performed in the laboratory and controlled by experimenters. Full adherence to stimulation was ensured. None of the participants dropped out during the study. One participant did not complete the full set of functional tests due to time limitations and was excluded from functional analysis. The protocol started with the participant filling out an NPSI focused on the 24 h before. Then continued with (i) Quantitative Sensory Testing (QST) for sensory loss assessment, (ii) neurostimulation calibration for sensory restoration, (iii) Just Noticeable Difference (JND) to test sensory sensitivity and (iv) functional tests. Study aims for each phase are shown in Fig. 7. The functional assessments consisted of standard tasks performed either with intervention, (i.e., sensory feedback restored with neurostimulation), or without sensory feedback (i.e., with the system not stimulating). During the control condition the participants wore the neuroprosthesis that was not providing any neurostimulation. The intervention and control conditions were presented in a random order determined before each task. The number of control and intervention trials was balanced for each task. The NPSI was taken again 24 hours after the one taken at the beginning of the testing day. Healthy participants performed the full calibration and the JND test for sensory sensitivity (N = 22). Considering that some of the healthy participants perform the JND test and full calibration of both feet, the final number of available nerve data is N = 41. After the one-day intervention, five out of 14 PN participants and 12 healthy controls were recruited for another half day including calibration of somatotopic, in-foot and on-ankle sensations and fMRI testing. Participant-specific information of the testing session is available in Supplementary Tables S2 and S4. The functional assessments consisted of standard tasks performed either with intervention, (i.e., sensory feedback restored with neurostimulation), or without sensory feedback (i.e., with the system turned off). During the control condition, the participants were asked to wear neuroprostheses that did not provide any neurostimulation. The intervention and control conditions were presented in a random order determined before each task by the experimenter. The number of control and intervention trials was balanced for each task. The NPSI was taken again 24 hours after the one taken at the beginning of the testing day. Healthy participants performed the full calibration and the JND test for sensory sensitivity (N = 22) and the fMRI testing (N = 12). Considering that some of the healthy participants perform the JND test and full calibration of both feet, the final number of available nerve data is N = 41.
The aims of the study were as follows (Fig. 7). AIM1) Functionality of the NeuroStep device to restore SF in participants with damaged neuropathic nerves. AIM2) Changes in areas of sensation and loss with stimulation (SF) and without (NF). AIM3) Changes between functional tasks with SF and NF. AIM4) changes from baseline in pain level as reported by the participant. AIM5) changes in brain activity (fMRI) in the primary somatosensory area between somatotopic and non-somatotopic stimulation. gg
In this feasibility study, we did not test the effect of Virtual Reality (VR) measured with electroencephalography (EEG) as defined in the initial protocol, focusing on the use of the device and the short-term effects (a single day session) of a wearable targeted neuroprostheses on functional tasks and pain. The effects of the combination of targeted neurostimulation and VR will be tested in a long-term trial (multiple sessions) in the future.
Ethics
The experiments were designed and conducted in accordance with the Declaration of Helsinki and following a protocol approved by ETH Zurich’s ethics commission (EK 2019-N-97). The purpose of this study is to test the device and not to provide a diagnosis (the patients were recruited with a known diagnosis of neuropathy) nor to modify the participants’ therapy. 18 PN participants were recruited, 4 were excluded, and 14 performed the experiments. No compensation was provided. Healthy participants were recruited (N = 22), and all of them performed the JND and charge experiments. All participants read and signed the informed consent form including the use of identifiable images and access to medical records. PN participants were recruited through the University Hospital Zurich and Balgrist University Hospital in Zurich, between July 2021 and October 2023, with recruitment of PN participants concluding in October 2023. Inclusion and exclusion criteria are specified in Supplementary Table S1. The overall recruitment, starting from enrolment, allocation, follow-up, and analysis is shown in the CONSORT flow diagram one arm intervention in Supplementary Fig. S8.
Sensation characterisation
Quantitative Sensory Testing (QST)
Quantitative Sensory Testing was performed on each participant to assess their residual nerve function and understand their areas of sensory loss. The participant was blindfolded while the touch receptors on the sole and dorsum of the foot and around the ankle were stimulated with a gloved finger (light touch), cotton swab (brushing) and a 10 mg monofilament. Light touch and brush were tested on the entire area of the foot while monofilament followed the standardised 10-points around the foot95. The participant was then asked to report if and where the touch was felt (Supplementary Movie 2). The area of sensory loss (incorrect answers in Supplementary Movie 2) was saved using a GUI by drawing the loss area on four different views of each foot. Locations, where stimulations were not felt or felt in the wrong location (more than 2 mm from the tested area96) were considered as locations of sensory loss. Then, the area of lost sensation over the dorsal and plantar views of the foot was calculated as a sum of the three different modalities of QST and computed as a percentage with respect to the entire dorsal and plantar foot area (Fig. 2 and Supplementary Fig. S3).
Electrical sensory feedback characterisation
The calibration of neurostimulation parameters in neuroprosthetics is highly participant-specific since the perceived sensation relies on the relative position of the superficial electrodes to the underlying nerve and is sensitive to different nerve conditions (e.g., nerve tissue damage in peripheral neuropathy97,98). In addition, this may change over time due to neural adaptation99 and/or displacement of the electrodes. To address this, we used a personalised calibration phase to find the optimal electrode positions and stimulation parameters for each participant. The NeuroStep sock was purposely designed to be able to target superficial nerves eliciting three differently located, distal sensations in the foot. Each of the sock’s three arrays was designed considering anthropometric measures100,101 to ensure there were enough electrodes (e.g., active sites) to cover the intended target area (Fig. 1B). Each electrode in the array can be defined by software as disconnected, cathodic, or anodic. In this way, several combinations of electrodes with different locations and dimensions can be tested until a proper somatotopic sensation is achieved. During the calibration phase, the experimenters chose the cathode and anode electrodes in the sock using the NeuroStep interactive GUI. Participants were instructed to report the intensity of the stimulation they felt on a scale from 0–10 where 0 is not perceived, 1 is barely perceivable, and 10 is a very strong, not bearable sensation31,32. Then, a series of electrical pulse trains increasing in amplitude were delivered until the participant reported a clear, but non-painful sensation with 5/10 intensity. If the electrically elicited sensation was good (somatotopic and, overlapping with the area of sensory loss if possible), the location was selected. If the perceived sensation was mainly under the electrodes or in the wrong location, the experimenters selected different electrodes until an optimal location was achieved. After the electrodes were fixed, a calibration procedure similar to the one described in refs. 22,31,32 was conducted to find the perceptual (minimum, 2/10 intensity) and maximum threshold (below pain, 8/10 intensity) for each nerve for each participant (Table 2). Since TENS can elicit different types of sensations42, each paradigm was also qualitatively described by reporting which sensation described the sensation best. The descriptors were: light touch, vibration, tingling, pressure, slow pulsation, twitching, electricity, pain or other sensation as described by the participant102. Pulse trains consisted of biphasic, rectangular pulses at a fixed frequency (50 Hz, as previously used in other studies29,40,41) while modulating the amplitude and pulse width. Each pulse train lasted for 2 s with a 1 s pause. The software automatically increases the amplitude or pulse width of consecutive pulses from the minimum to the maximum possible value by a step that is specified by the experimenter. When either the perceptual or maximum threshold was reached, the participant described the perceived sensation in terms of type (vibration, pressure, tingling, warm, electricity, etc), area elicited (dorsal and ventral), and intensity (1–10) in the GUI. For each nerve, the calibration was repeated six times, and the charge values were averaged across all trials; the reported sensation area was requested only during the first three trials for each nerve and averaged among them. The electrode position, stimulation parameters and reported sensation were saved for each nerve of each participant using the customised GUI. The area of reported sensation was saved by drawing on four different views of each foot in the GUI. Then, the area of reported sensations was defined as the total area over three different neurostimulation trials for each location/nerve. The total area of artificially evoked sensations was computed with respect to the entire dorsum, plantar and foot area (Fig. 2D). Then, the area of restored sensation was computed as the intersection between evoked sensation and lost sensation with respect to the entire lost area.
Just noticeable difference (JND)
The just noticeable difference (JND) is the smallest difference (i.e., the sensitivity) between two stimuli that can be reliably discriminated by the participant103. To determine the JND, two 1-second bursts of stimulation were delivered separated by a break of 1 s31. The range of stimuli was fixed between the perceptual (2/10) and maximum threshold (8/10) found during calibration. The pairs of stimuli consisted of a reference stimulus (average value of the charge range) and a test stimulus (a value between perceptual and maximum thresholds). Test stimuli values were computed by modulating the pulse width to find eight equally distributed values between the perceptual and maximum threshold levels around the reference stimulus. Pairs of test stimuli were presented eight times each in a random order with the participant asked to identify whether the first or second stimulus was stronger. This test was performed with 41 nerves in 22 healthy participants and 22 nerves in 13 neuropathic participants. Depending on the time available, each participant did either both or a single foot. One participant did not perform the JND test for the limited time available. Then, the probability of judging the test stimulus as larger than the reference stimulus was computed and, a psychometric function was fitted to the probability points (Fig. 3A). Then, we computed the point of subjective equality (PSE), i.e., the PW that was perceived higher in at least 50% of the trials and the JND as the difference between the PSE and the PW that was perceived stronger in 75% of the trials104,105. For each JND, we computed the WF, which is the JND divided by the reference stimulus. Smaller WFs indicate a higher sensitivity, i.e., a smaller difference in input (PW modulation) is needed to perceive a difference in intensity. Each PN participant performed a different number of JND tests (side and nerves) depending on which nerves were elicited during the calibration and time availability. The overview of the JNDs test is summarised in Supplementary Table S3.
Functional assessments
The participant was firstly asked to perform a few steps (min 10 steps) to measure the minimum and maximum force exerted on each pressure sensor. Then, each nerve (stimulation channel) with a successfully restored sensation, was matched to the sensor closer to the elicited location. Then, for each pair sensor/stimulation, the perceptual (2/10) and maximum charge (8/10) found during electrical calibration were mapped to the minimum and maximum force exerted on the force insole for functional use31. During functional use, the stimulation was modulated between these two values depending on the foot-ground force.
Standard functional tests (the Functional Gait Analysis (FGA)48, and 10 m walking test47) were performed in both SF and NF conditions. During the NF condition, the participants were wearing the system, but the stimulation was turned off. The FGA is a 10-item test that has been shown to be effective at predicting fall risk in older adults48 and has been recommended as an outcome measure of adults with neurologic conditions106. Each item is scored from 0 to 3 (3 = normal, 2 = mild impairment, 1 = moderate impairment, 0 = severe impairment) with a maximum score of 30. It was performed once per condition per participant in a random order, and it was scored independently by two scorers. Scorers were blinded to the experiment condition (SF or NF). If scores conflicted (> 1 point difference per task), the recorded videos were revisited by a third scorer to determine the correct score. Final scores were computed as the average between the two independent scorers and compared to the average score for each age group107. The 10 m walking test was performed 6 times in each condition in a randomised order. The time from the 2 m to the 8 m mark was recorded to determine the speed of each trial. The time recorded was averaged between experimenters. Tasks were video-recorded and checked by a third experimenter in case of inconsistencies between experimenters (time difference > 0.5 s). During functional assessment, foot-ground force information containing gait events was recorded and saved. Cadence was later extracted from these gait events by counting the number of steps taken between the 2 m and 8 m mark and dividing by time. All cadence values were normalised by walking speed to compare between feedback and no feedback conditions.
Neuropathic pain
The Neuropathic Pain Symptom Inventory (NPSI)50, a new self-questionnaire specifically validated to evaluate the different symptoms of neuropathic pain for a 24-hour interval, was taken at the start of the one-day of intervention and again 24 h later. NPSI scores were further sub-grouped in spontaneous pain vs pain attacks and in five pain type categories, i.e., burning, evoked, paroxysmal, pressing/deep, paraesthesia.
Cortical imaging
Scanning procedures
Twelve healthy participants (43 ± 5.53 years old) and five of the original fourteen PN participants (72 ± 2.63 years old) (Supplementary Table S2) participated in the functional magnetic resonance imaging (fMRI) investigation of sensation perception. The fMRI scanning was conducted solely for observational purposes. The results of fMRI did not affect PN participants’ therapy. The fMRI scanning is part of a separate long-term, still ongoing clinical trial. fMRI studies were performed in accordance with the Declaration of Helsinki and approved by the local ethics board Kantonale Ethikkommission Zürich - KEK (2021-02258). Further exclusion criteria for recruiting fMRI participants included standard MRI contraindications. For fMRI contraindications, we complied with the established imaging centre’s routine, and in case of doubt, we excluded the participant from this part of the study. The three distinct target regions or locations innervated by the peroneal, posterior tibial, and sural nerves were characterised and stimulated separately in three main conditions: somatotopic, in-foot, and on-ankle (Fig. 6A). Stimulation was applied to one foot. The foot for healthy participants was chosen randomly, while for PN participants, the foot was preferred where the previous characterisation achieved a complete characterisation (all three nerves). Instead of the custom sock, sticky electrodes were used and were fixated to the participant’s skin using adhesive tape. Stimulation did not elicit noticeable noise artefacts in preliminary fMRI testing. The somatotopic condition was characterised by the functional calibration described above. Electrodes were placed at the ankle level to elicit distal PFs in the foot. In the in-foot condition, electrodes were placed directly over the location (i.e., the PFs) of the mechanoreceptors where somatotopic sensation was elicited. In the on-ankle conditions, electrodes were placed at the ankle level with the goal of eliciting no distal somatotopic sensation, while still being close to the location of the somatotopically stimulating electrodes. Stimulation intensity was determined as follows: participants were given 2 s of stimulation in increasing amplitude (pulse width and frequency fixed at 300 µs and 50 Hz) until the stimulation was perceived to be strong but not painful. In six of twelve healthy participants and four PN participants, this corresponded to a numerical intensity rating of 7 or 8/10 and in six of twelve healthy participants and in one PN participant, this corresponded to a numerical intensity rating of 5/10. In neuropathic participants who do not perceive sensation in the foot condition due to their neuropathy, the appropriate foot charge to stimulate with was calculated a priori. A charge ratio between somatotopic and in-foot charge was calculated from the first eight healthy participants’ data (Supplementary Fig. S9), and this was used to determine the appropriate charge for the in-foot condition of PN participants108 (Supplementary Table S3). The PN participants were then tested with stimulation up to 2 standard deviations above this ratio to confirm their level of loss. Supplementary Table S2 displays the perceived intensity for the in-foot condition at the charge limit in the five participants. Each condition (somatotopic, in-foot, and on-ankle) was tested in four separate fMRI runs. In each run, the three target locations (correspondent to peroneal, tibial posterior and sural nerves in the somatotopic condition) were stimulated in a counterbalanced order, with a different order of target locations per run. The four runs testing a condition were executed consecutively to minimise the need to switch electrodes. The order of the conditions was balanced across participants to avoid order effects.
During an fMRI run, participants saw a white fixation cross via a visual display viewed through a mirror mounted on the head coil. During stimulation, the fixation cross turned red. A stimulation trial lasted 4 s with a jittered pause (2–4 s) between stimuli for a total of 12 stimuli per location and per run. To ensure stable attention to the stimulation during the fMRI runs, the stimulation was interrupted in a small number of stimulation trials (2–4 trials per run). In these interrupted trials, stimulation was provided for 2 s, after which a 1 s silent period was introduced, followed by another 1 s of stimulation. Care was taken to ensure that the interrupted stimulation trials were equally distributed across the stimulation locations within each run. Participants were instructed to count the number of interrupted stimulation trials and verbally reported this at the end of each run. This attentional task was added to ensure stable attention to the stimulation during the fMRI runs. Head motion was minimised using over-ear MRI-safe headphones or padded cushions. Unity 2020.1.13 was used to deliver stimuli and display the fixation cross.
MRI acquisition
MRI data was acquired using a Philips 3 tesla Ingenia system (Best, The Netherlands) with a 32-channel head coil. Task-fMRI data was acquired using an echo-planar-imaging (EPI) sequence using the following acquisition parameters: 40 slices, 2.7 mm109 resolution, TR: 2500 ms, TE: 30 ms, flip angle: 85°, SENSE factor: 2. Anatomical T1-weighted images were acquired using the following acquisition parameters: 1 mm109 resolution, repetition time (TR): 7.7 ms, echo time (TE): 3.6 ms, flip angle: 8°.
MRI preprocessing
Data collected for individuals of whom we tested the left foot was flipped on the midsagittal plane prior to data preprocessing and analysis. fMRI preprocessing was implemented using FSL v5.0.7 (https://fsl.fmrib.ox.ac.uk/fsl/fslwiki). Cortical surface reconstructions and visualisations were realised using FreeSurfer v6.0 (https://surfer.nmr.mgh.harvard.edu/)110,111 and Connectome Workbench v1.3.2 (https://www.humanconnectome.org/software)112. Common preprocessing steps for fMRI data were applied using FSL’s Expert Analysis Tool (FEAT): motion correction using MCFLIRT113, brain extraction using automated brain extraction tool BET114, spatial smoothing using a 3 mm full-width-at-half-maximum (FWHM) Gaussian kernel, and high-pass temporal filtering with a 90 s cutoff. Each participant’s functional data was registered to the corresponding T1-weighted image, initially using 6 degrees of freedom and the mutual information cost function, and then optimised using boundary-based registration (BBR)109.
MRI analysis
Univariate analysis
First-level parameter estimates were computed using a voxel-based general linear model (GLM) based on the gamma hemodynamic response function and its temporal derivatives. Time series statistical analysis was carried out using FILM (FMRIB’s Improved Linear Model) with local autocorrelation correction. To reduce noise artefacts, cerebrospinal fluid and white matter scan-wise time series were added to the model as nuisance regressors. Data were further assessed for excessive motion, and volumes with an estimated absolute mean displacement greater than 1.35 mm (half of the functional voxel size) were scrubbed (maximum percentage of volumes scrubbed in a scan = 5.6%). Contrasts were defined per the main condition for stimulation versus rest and, additionally, for overall stimulation versus rest (i.e., across conditions). A fixed-effects second-level analysis, as implemented in FSL’s FEAT, was used to average across each main condition’s stimulation runs and across all runs per participant. For optimal coregistration and functional signal alignment across participants’ univariate analysis was performed on the cortical surface. Cortical surface projections were constructed from each participant’s T1-weighted images. The statistical map results resulting from each individual’s second-level analysis were projected onto the cortical surface using cortical-ribbon mapping and finally to the fs-LR surface template brain. To create a functional ankle-foot S1 area region of interest (ROI), we calculated a whole-brain group average for the healthy participants. We conducted a one-sample t test for the contrast overall stimulation versus rest (i.e., across conditions) using permutation testing available in PALM115, using 4096 permutations. The activity was thresholded using cluster-based thresholding corrected for multiple comparisons with Z > 2.3. The resulting activity blob at the anatomical ankle and foot area in the primary somatosensory cortex was then extracted as an ankle-foot S1 area ROI. Averaged z-standardised activity was extracted from each participant’s second-level analysis to examine activity elicited by stimulation in each condition in this ankle-foot S1 ROI.
Spatial overlap analysis
The DICE overlap coefficient (DOC)116 was used to quantify the spatial overlap between each pair of conditions. The DOC calculates the spatial overlap between two representations relative to the total area of these representations. The DOC ranges from 0 (no spatial overlap) to 1 (perfect spatial overlap). If A and B represent the areas of two representations, then the DOC is expressed as:
We closely followed previously described procedures60,61,117,118. Activity maps were identified using the contrast stimulation > rest of each participant’s and each condition’s 2nd level analysis (i.e., after averaging across the 4 runs). These activity maps were transformed to the cortical surface (template space), thresholded at Z > 2.2, and masked using both the functional ROI specified above119. To investigate how the choice of threshold influences the spatial overlap results, the DOC was further calculated as a function of z thresholds ranging from 1 to 3 (in steps of 0.2). In-vertex volume between the white matter and pial surfaces was used to calculate the volume covered by the thresholded representations and the resulting DOCs.
Classification analysis
To investigate whether the stimulation of the three target locations (peroneal, posterior tibial, and sural nerves) elicits distinct voxel-wise activity patterns in the ankle-foot S1 ROI within each condition, we aimed to decode the stimulated target location from the trial-wise parameter estimates using Multivariate pattern analysis (MVPA). For this, single-trial parameter estimates were computed with an HRF-based first-level GLM in SPM12 (http://www.fil.ion.ucl.ac.uk/spm/) using SPM’s default parameters. The design matrix consisted of individual regressors for each stimulation trial. This resulted in 144 parameter estimates per condition and participant. Within each condition, i.e., there were 48 trials per target location. The ankle-foot S1 ROI in the fs-LR template surface space was resampled to each participant’s native 3D space, i.e., the same space as the parameter estimates. Any holes were filled. Next, the voxel-wise parameter estimates below the specified ankle-foot S1 ROI were extracted for each trial and participant.
To investigate whether the stimulation of the three target locations (peroneal, posterior tibial, and sural nerves) elicits distinct activity patterns in the ankle-foot S1 ROI within a condition, we aimed to decode the stimulated target location from the parameter estimates. These extracted 144 trials were used in a machine learning pipeline to decode the three target locations from the neural activity patterns. Separately for each participant and each condition, a Leave one Run Out (LORO) cross-validation was performed. To do so, the dataset was split into four fMRI runs. For each fold, data from three runs were used for training and data from the left-out run (i.e., the fourth run) were used for testing. This procedure was repeated four times so that each run served as the testing set once. This ensures the independence of the test set from the training set, allowing it to prevent overfitting and to generalise the performance of the classifier to new and unseen data. At each step, we performed standard scaling, fit on the training set and applied it to the test set. The processed dataset was given as input to an SVM classifier with a linear kernel. Hyperparameters were set at default values. Models were evaluated in terms of average accuracy on each LORO test set. The average classification accuracies for each condition (somatotopic, in-foot and on-ankle) were compared, separately for healthy controls and neuropathic participants.
Data collection and statistical analysis
Plotting, data processing and analysis were performed in Matlab (R2022b, The MathWorks, Natick, MA, U.S.A.) and Python 3.9. Results among patients are presented as average ± standard error. Barplots show the average and standard error. Boxplots show the interquartile range with median, and the whiskers of the rest of the distribution excluded outliers. Statistical analysis was performed using built-in Matlab and Python functions. For clinical measures, published standards for clinically meaningful difference were used to compare baseline and stimulation trials. Non-paired two-group comparison was performed using the Mann-Whitney test (e.g., to compare healthy vs PN participants). Within the subject, paired comparisons were performed using the Wilcoxon Signed-Rank test. If not specified otherwise, an alterative two-sided was used. Single group comparison against mean was performed using One sample Wilcoxon Signed-Rank test. For functional task comparison at the group level, Repeated Measures ANOVA was used. Multicomparison analyses were performed with the Friedman Multicompare test and Post-hoc Nemenyi tests. Post-hoc Nemenyi test accounts for correction for multiple comparisons. Asterisks on plots indicate the following statistical significance levels: p < 0.05 (*), p < 0.01(**), p < 0.001 (***). Exact p-values are reported in the text except for p > 0.05. ### indicates clinical significance from the literature.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
All data supporting the findings of this study are available within the article and its supplementary files. Any additional requests for information can be directed to the corresponding authors. Source data are provided in this paper.
Code availability
Codes used in the analysis are available upon request from the corresponding author.
References
WHO. Global report on diabetes. https://www.who.int/publications-detail-redirect/9789241565257 (2016).
Marx, J. Unraveling the causes of diabetes. Science 296, 686–689 (2002).
Williams, R. et al. Global and regional estimates and projections of diabetes-related health expenditure: Results from the International Diabetes Federation Diabetes Atlas, 9th edition. Diabetes Res. Clin. Pract. 162, 108072 (2020).
Feldman, E. L. et al. Diabetic neuropathy. Nat. Rev. Dis. Prim. 5, 1–18 (2019).
Lehmann, H. C., Wunderlich, G., Fink, G. R. & Sommer, C. Diagnosis of peripheral neuropathy. Neurol. Res. Pract. 2, 20 (2020).
Said, G. Diabetic neuropathy—a review. Nat. Rev. Neurol. 3, 331–340 (2007).
Tesfaye, S. Neuropathy in diabetes. Medicine 34, 91–94 (2006).
Lai, Y.-R. et al. HbA1C Variability is strongly associated with the severity of peripheral neuropathy in patients with type 2 diabetes. Front. Neurosci. 13, 90 (2019).
Su, J. et al. HbA1c variability and diabetic peripheral neuropathy in type 2 diabetic patients. Cardiovasc Diabetol. 17, 47 (2018).
Boulton, A. J. M. Management of diabetic peripheral neuropathy. Clin. Diabetes 23, 9–15 (2005).
Tesfaye, S. et al. Vascular risk factors and diabetic neuropathy. N. Engl. J. Med. 352, 341–350 (2005).
Sloan, G., Selvarajah, D. & Tesfaye, S. Pathogenesis, diagnosis and clinical management of diabetic sensorimotor peripheral neuropathy. Nat. Rev. Endocrinol. 17, 400–420 (2021).
Jahantigh Akbari, N., Hosseinifar, M., Naimi, S. S., Mikaili, S. & Rahbar, S. The efficacy of physiotherapy interventions in mitigating the symptoms and complications of diabetic peripheral neuropathy: A systematic review. J. Diabetes Metab. Disord. 19, 1995–2004 (2020).
Callaghan, B. C., Price, R. S. & Feldman, E. L. Distal symmetric polyneuropathy: A review. JAMA 314, 2172–2181 (2015).
Dietrich, I., Braga, G. A., de Melo, F. G. & da Costa Silva Silva, A. C. C. The diabetic foot as a proxy for cardiovascular events and mortality review. Curr. Atheroscler. Rep. 19, 44 (2017).
Vadiveloo, T. et al. Amputation-free survival in 17,353 people at high risk for foot ulceration in diabetes: a national observational study. Diabetologia 61, 2590–2597 (2018).
Kioskli, K., Scott, W., Winkley, K., Kylakos, S. & McCracken, L. M. Psychosocial factors in painful diabetic neuropathy: A systematic review of treatment trials and survey studies. Pain. Med. 20, 1756–1773 (2019).
Armstrong, D. G., Boulton, A. J. M. & Bus, S. A. Diabetic foot Ulcers and their recurrence. N. Engl. J. Med. 376, 2367–2375 (2017).
Brown, M. J. et al. Natural progression of diabetic peripheral neuropathy in the zenarestat study population. Diabetes Care 27, 1153–1159 (2004).
Hanewinckel, R. et al. Polyneuropathy relates to impairment in daily activities, worse gait, and fall-related injuries. Neurology 89, 76–83 (2017).
Najafi, B. et al. Using plantar electrical stimulation to improve postural balance and plantar sensation among patients with diabetic peripheral neuropathy: A randomized double blinded study. J. Diabetes Sci. Technol. 11, 693–701 (2017).
Petrini, F. M. et al. Enhancing functional abilities and cognitive integration of the lower limb prosthesis. Sci. Transl. Med. 11, https://doi.org/10.1126/scitranslmed.aav8939 (2019).
Petrini, F. M. et al. Sensory feedback restoration in leg amputees improves walking speed, metabolic cost and phantom pain. Nat. Med. 25, 1356–1363 (2019).
Valle, G. et al. Mechanisms of neuro-robotic prosthesis operation in leg amputees. Sci. Adv. 7, eabd8354 (2021).
Valle, G. et al. Biomimetic computer-to-brain communication enhancing naturalistic touch sensations via peripheral nerve stimulation. Nat. Commun. 15, 1151 (2024).
Pena, A. E., Abbas, J. J. & Jung, R. Channel-hopping during surface electrical neurostimulation elicits selective, comfortable, distally referred sensations. J. Neural Eng. 18, 055004 (2021).
Shin, H. et al. Evoked haptic sensations in the hand via non-invasive proximal nerve stimulation. J. Neural Eng. 15, 046005 (2018).
Chee, L. et al. Cognitive benefits of using non-invasive compared to implantable neural feedback. Sci. Rep. 12, 16696 (2022).
D’Anna, E. et al. A somatotopic bidirectional hand prosthesis with transcutaneous electrical nerve stimulation based sensory feedback. Sci. Rep. 7, 10930 (2017).
Pan, L. et al. Evoking haptic sensations in the foot through high-density transcutaneous electrical nerve stimulations. J. Neural Eng. 17, 036020 (2020).
Chee, L. et al. Optimally-calibrated non-invasive feedback improves amputees’ metabolic consumption, balance and walking confidence. J. Neural Eng. 19, 046049 (2022).
Basla, C., Chee, L., Valle, G. & Raspopovic, S. A non-invasive wearable sensory leg neuroprosthesis: mechanical, electrical and functional validation. J. Neural Eng. 19, 016008 (2022).
Oddsson, L. I. E. et al. The effects of a wearable sensory prosthesis on gait and balance function after 10 weeks of use in persons with peripheral neuropathy and high fall risk – the walk2Wellness trial. Front. Aging Neurosci. 12, 409 (2020).
Oddsson, L. I. E. et al. Extended effects of a wearable sensory prosthesis on gait, balance function and falls after 26 weeks of use in persons with peripheral neuropathy and high fall risk—The walk2Wellness trial. Front. Aging Neurosci. 14, 931048 (2022).
Bensmaia, S. J., Tyler, D. J. & Micera, S. Restoration of sensory information via bionic hands. Nat. Biomed. Eng. 7, 443–445 (2020).
Raspopovic, S., Valle, G. & Petrini, F. M. Sensory feedback for limb prostheses in amputees. Nat. Mater. 20, 925–939 (2021).
Najafi, B., Crews, R. T. & Wrobel, J. S. A novel plantar stimulation technology for improving protective sensation and postural control in patients with diabetic peripheral neuropathy: A double-blinded, randomized study. GER 59, 473–480 (2013).
Jamison, R. N., Wan, L., Edwards, R. R., Mei, A. & Ross, E. L. Outcome of a high-frequency transcutaneous electrical nerve stimulator (hfTENS) device for low back pain: a randomized controlled trial. Pain Practice 19, 466–475 (2019).
Federal Trade Commission. Marketers of pain relief device settle FTC false advertising complaint. Federal Trade Commission https://www.ftc.gov/news-events/news/press-releases/2020/03/marketers-pain-relief-device-settle-ftc-false-advertising-complaint (2020).
Chai, G., Sui, X., Li, S., He, L. & Lan, N. Characterization of evoked tactile sensation in forearm amputees with transcutaneous electrical nerve stimulation. J. Neural Eng. 12, 066002 (2015).
Chai, G. H. et al. Phantom finger perception evoked with transcutaneous electrical stimulation for sensory feedback of prosthetic hand. In 2013 6th International IEEE/EMBS Conference on Neural Engineering (NER) 271–274 (2013).
Bucciarelli, V. et al. Multiparametric non-linear TENS modulation to integrate intuitive sensory feedback. J. Neural Eng. 20, https://doi.org/10.1088/1741-2552/acd4e8 (2023).
Risso, G. et al. Multisensory stimulation decreases phantom limb distortions and is optimally integrated. iScience 25, 104129 (2022).
Norwich, K. H. On the theory of Weber fractions. Percept. Psychophys. 42, 286–298 (1987).
Palve, S. S. & Palve, S. B. Impact of aging on nerve conduction velocities and late responses in healthy individuals. J. Neurosci. Rural Pr. 9, 112–116 (2018).
Saeed, S. & Akram, M. Impact of anthropmetric measures on sural nerve conduction in healthy subjects. J. Ayub Med. Coll. Abbottabad 20, 112–114 (2008).
Perera, S., Mody, S. H., Woodman, R. C. & Studenski, S. A. Meaningful change and responsiveness in common physical performance measures in older adults. J. Am. Geriatr. Soc. 54, 743–749 (2006).
Wrisley, D. M., Marchetti, G. F., Kuharsky, D. K. & Whitney, S. L. Reliability, internal consistency, and validity of data obtained with the functional gait assessment. Phys. Ther. 84, 906–918 (2004).
Wrisley, D. M. & Kumar, N. A. Functional gait assessment: Concurrent, discriminative, and predictive validity in community-dwelling older adults. Phys. Ther. 90, 761–773 (2010).
Bouhassira, D. et al. Development and validation of the neuropathic pain symptom inventory. Pain 108, 248–257 (2004).
Dworkin, R. H. et al. Interpreting the clinical importance of treatment outcomes in chronic pain clinical trials: IMMPACT recommendations. J. Pain. 9, 105–121 (2008).
Dworkin, R. H., Evans, S. R., Mbowe, O. & McDermott, M. P. Essential statistical principles of clinical trials of pain treatments. PAIN Rep. 6, e863 (2021).
Farrar, J. T., Young, J. P., LaMoreaux, L., Werth, J. L. & Poole, R. M. Clinical importance of changes in chronic pain intensity measured on an 11-point numerical pain rating scale. PAIN 94, 149–158 (2001).
Villoria, J., Rodríguez, M., Berro, M. J., Stern, A. & Sánchez-Magro, I. Psychometric validation of the neuropathic pain symptom inventory for its use in Spanish. J. Pain. Symptom Manag. 42, 134–146 (2011).
Aurucci, G. V., Preatoni, G., Damiani, A. & Raspopovic, S. Brain-computer interface to deliver individualized multisensory intervention for neuropathic pain. Neurotherapeutics 20, 1316–1329 (2023).
Gordon, E. M. et al. A somato-cognitive action network alternates with effector regions in motor cortex. Nature 617, 351–359 (2023).
Kikkert, S., Sonar, H. A., Freund, P., Paik, J. & Wenderoth, N. Hand and face somatotopy shown using MRI-safe vibrotactile stimulation with a novel soft pneumatic actuator (SPA)-skin interface. NeuroImage 269, 119932 (2023).
Sanchez Panchuelo, R. M., Besle, J., Schluppeck, D., Humberstone, M. & Francis, S. Somatotopy in the human somatosensory system. Front. Hum. Neurosci. 12, https://doi.org/10.3389/fnhum.2018.00235 (2018).
PENFIELD, W. & BOLDREY, E. Somatic motor and sensory representation in the cerebral cortex of man as studied by electrical stimulation1. Brain 60, 389–443 (1937).
Kikkert, S., Pfyffer, D., Verling, M., Freund, P. & Wenderoth, N. Finger somatotopy is preserved after tetraplegia but deteriorates over time. ELife 10, e67713 (2021).
Kikkert, S. et al. Revealing the neural fingerprints of a missing hand. ELife 5, e15292 (2016).
Sugimoto, K., Murakawa, Y. & Sima, Aa. F. Diabetic neuropathy – a continuing enigma. Diabetes Metab. Res. Rev. 16, 408–433 (2000).
INCEU, G. V. & VERESIU, I. A. Measurement of current perception thresholds using the Neurometer® – applicability in diabetic neuropathy. Clujul Med. 88, 449–452 (2015).
Suzuki, C. et al. Elevated pain threshold in patients with asymptomatic diabetic neuropathy: an intraepidermal electrical stimulation study. Muscle Nerve 54, 146–149 (2016).
Sharma, K. R. Demyelinating neuropathy in diabetes mellitus. Arch. Neurol. 59, 758 (2002).
Tan, D. W. et al. A neural interface provides long-term stable natural touch perception. Sci. Transl. Med. 6, https://doi.org/10.1126/scitranslmed.3008669 (2014).
Fifer, M. S. et al. Intracortical somatosensory stimulation to elicit fingertip sensations in an individual with spinal cord injury. Neurology 98, e679–e687 (2021).
Flesher, S. N. et al. Intracortical microstimulation of human somatosensory cortex. Sci. Transl. Med. 8, 361ra141–361ra141 (2016).
Armenta Salas, M. et al. Proprioceptive and cutaneous sensations in humans elicited by intracortical microstimulation. ELife 7, e32904 (2018).
Christensen, M. B. et al. The foreign body response to the Utah Slant Electrode Array in the cat sciatic nerve. Acta Biomater. 10, 4650–4660 (2014).
Martin, E. T. et al. Diabetes and risk of surgical site infection: A systematic review and meta-analysis. Infect. Control Hosp. Epidemiol. 37, 88–99 (2016).
Wagner, F. W. The dysvascular foot: A system for diagnosis and treatment. Foot Ankle 2, 64–122 (1981).
Cavanagh, P. R., Derr, J. A., Ulbrecht, J. S., Maser, R. E. & Orchard, T. J. Problems with gait and Posture in neuropathic patients with insulin-dependent diabetes mellitus. Diabet. Med. 9, 469–474 (1992).
Sterling, D. A., O’Connor, J. A. & Bonadies, J. Geriatric falls: Injury severity is high and disproportionate to mechanism. J. Trauma Acute Care Surg. 50, 116 (2001).
DeMott, T. K., Richardson, J. K., Thies, S. B. & Ashton-Miller, J. A. Falls and gait characteristics among older persons with peripheral neuropathy. Am. J. Phys. Med. Rehabil. 86, 125 (2007).
Bergen, G. Falls and Fall Injuries Among Adults Aged ≥65 Years — United States, 2014. MMWR Morb. Mortal. Wkly. Rep. 65, 993–998 (2016).
Jónsdóttir, H. L. & Ruthig, J. C. A longitudinal study of the negative impact of falls on health, well-being, and survival in later life: the protective role of perceived control. Aging Ment. Health 25, 742–748 (2021).
Florence, C. S. et al. Medical costs of fatal and nonfatal falls in older adults. J. Am. Geriatr. Soc. 66, 693–698 (2018).
Barreira, T. V., Katzmarzyk, P. T., Johnson, W. D. & Tudor-Locke, C. Walking cadence and cardiovascular risk in children and adolescents. Am. J. Prev. Med. 45, e27–e34 (2013).
Melzack, R. & Wall, P. D. Pain mechanisms: a new theory. Science 150, 971–979 (1965).
Kuhn, A., Keller, T., Lawrence, M. & Morari, M. A model for transcutaneous current stimulation: simulations and experiments. Med Biol. Eng. Comput 47, 279–289 (2009).
Johnson, M. Transcutaneous electrical nerve stimulation: Mechanisms, clinical application and evidence. Rev. Pain. 1, 7–11 (2007).
Johnson, M. I. & Bjordal, J. M. Transcutaneous electrical nerve stimulation for the management of painful conditions: focus on neuropathic pain. Expert Rev. Neurother. 11, 735–753 (2011).
Raspopovic, S. et al. Restoring natural sensory feedback in real-time bidirectional hand prostheses. Sci. Transl. Med. 6, https://doi.org/10.1126/scitranslmed.3006820 (2014).
Partanen, J. et al. Natural history of peripheral neuropathy in patients with non-insulin-dependent diabetes mellitus. N. Engl. J. Med. 333, 89–94 (1995).
Laudadio, C. & Sima, A. A. F. Progression rates of diabetic neuropathy in placebo patients in an 18-month clinical trial. J. Diabetes Complications 12, 121–127 (1998).
Azmi, S. et al. Early nerve fibre regeneration in individuals with type 1 diabetes after simultaneous pancreas and kidney transplantation. Diabetologia 62, 1478–1487 (2019).
Gibbons, C. H. et al. The evolving natural history of neurophysiologic function in patients with well-controlled diabetes. J. Peripher. Nerv. Syst. 18, 153–161 (2013).
Gozzi, N. et al. Unraveling the physiological and psychosocial signatures of pain by machine learning. Med https://doi.org/10.1016/j.medj.2024.07.016 (2024).
Carroll, D. et al. Transcutaneous electrical nerve stimulation (TENS) for chronic pain. Cochrane Database Syst. Rev. https://doi.org/10.1002/14651858.CD003222 (2000).
Sekhon, M., Cartwright, M. & Francis, J. J. Development of a theory-informed questionnaire to assess the acceptability of healthcare interventions. BMC Health Serv. Res. 22, 279 (2022).
Graczyk, E. L., Resnik, L., Schiefer, M. A., Schmitt, M. S. & Tyler, D. J. Home use of a neural-connected sensory prosthesis provides the functional and psychosocial experience of having a hand again. Sci. Rep. 8, 9866 (2018).
Borda, L., Gozzi, N., Preatoni, G., Valle, G. & Raspopovic, S. Automated calibration of somatosensory stimulation using reinforcement learning. J. Neuroeng. Rehabil. 20, 131 (2023).
Aiello, G., Valle, G. & Raspopovic, S. Recalibration of neuromodulation parameters in neural implants with adaptive Bayesian Optimization. J. Neural Eng. 20, https://doi.org/10.1088/1741-2552/acc975 (2023).
Booth, J. & Young, M. J. Differences in the performance of commercially available 10-g monofilaments. Diabetes Care 23, 984–988 (2000).
Stevens, J. C. & Choo, K. K. Spatial acuity of the body surface over the life span. Somatosens. Mot. Res. 13, 153–166 (1996).
Zhang, G. Y. et al. Diabetic peripheral neuropathy increases electrical stimulation threshold of sciatic nerve: A prospective parallel cohort study. Diabetes Metab. Syndr. Obes. 13, 4447–4455 (2020).
Keyl, C., Held, T., Albiez, G., Schmack, A. & Wiesenack, C. Increased electrical nerve stimulation threshold of the sciatic nerve in patients with diabetic foot gangrene: A prospective parallel cohort study. Eur. J. Anaesthesiol. 30, 435–440 (2013).
Graczyk, E. L., Delhaye, B. P., Schiefer, M. A., Bensmaia, S. J. & Tyler, D. J. Sensory adaptation to electrical stimulation of the somatosensory nerves. J. Neural Eng. 15, 046002 (2018).
Hajaghazadeh, M., Emamgholizadeh Minaei, R., Allahyari, T. & Khalkhali, H. Anthropometric dimensions of foot in Northwestern Iran and comparison with other populations. Health Scope 7, https://doi.org/10.5812/jhealthscope.14063 (2018).
Jurca, A., Žabkar, J. & Džeroski, S. Analysis of 1.2 million foot scans from North America, Europe and Asia. Sci. Rep. 9, 19155 (2019).
Valle, G. et al. A psychometric platform to collect somatosensory sensations for neuroprosthetic use. Front. Med. Technol. 3, https://doi.org/10.3389/fmedt.2021.619280 (2020).
Ernst, M. O. & Banks, M. S. Humans integrate visual and haptic information in a statistically optimal fashion. Nature 415, 429–433 (2002).
Preatoni, G., Valle, G., Petrini, F. M. & Raspopovic, S. Lightening the perceived prosthesis weight with neural embodiment promoted by sensory feedback. Curr. Biol. 31, 1065–1071 (2021).
Graczyk, E. L. et al. The neural basis of perceived intensity in natural and artificial touch. Sci. Transl. Med. 8, 362ra142–362ra142 (2016).
Moore, J. L. et al. A core set of outcome measures for adults with neurologic conditions undergoing rehabilitation: A CLINICAL PRACTICE GUIDELINE. J. Neurol. Phys. Ther. 42, 174–220 (2018).
Walker, M. L. et al. Reference group data for the functional gait assessment. Phys. Ther. 87, 1468–1477 (2007).
Hughes, N., Bennett, M. I. & Johnson, M. I. An investigation into the magnitude of the current window and perception of transcutaneous electrical nerve stimulation (TENS) sensation at various frequencies and body sites in healthy human participants. Clin. J. Pain. 29, 146–153 (2013).
Greve, D. N. & Fischl, B. Accurate and robust brain image alignment using boundary-based registration. NeuroImage 48, 63–72 (2009).
Dale, A. M., Fischl, B. & Sereno, M. I. Cortical surface-based analysis: I. segmentation and surface reconstruction. NeuroImage 9, 179–194 (1999).
Fischl, B., Liu, A. & Dale, A. M. Automated manifold surgery: constructing geometrically accurate and topologically correct models of the human cerebral cortex. IEEE Trans. Med. Imaging 20, 70–80 (2001).
Marcus, D. et al. Informatics and data mining tools and strategies for the human connectome project. Front. Neuroinform. 5, https://doi.org/10.3389/fninf.2011.00004 (2011).
Jenkinson, M., Bannister, P., Brady, M. & Smith, S. Improved optimization for the robust and accurate linear registration and motion correction of brain images. NeuroImage 17, 825–841 (2002).
Smith, S. M. Fast robust automated brain extraction. Hum. Brain Mapp. 17, 143–155 (2002).
Winkler, A. M., Ridgway, G. R., Webster, M. A., Smith, S. M. & Nichols, T. E. Permutation inference for the general linear model. NeuroImage 92, 381–397 (2014).
Dice, L. R. Measures of the amount of ecologic association between species. Ecology 26, 297–302 (1945).
Kolasinski, J. et al. Investigating the stability of fine-grain digit somatotopy in individual human participants. J. Neurosci. 36, 1113–1127 (2016).
Sanders, Z. et al. Similar somatotopy for active and passive digit representation in primary somatosensory cortex. Hum. Brain Mapp. 44, 3568–3585 (2023).
Glasser, M. F. et al. A multi-modal parcellation of human cerebral cortex. Nature 536, 171–178 (2016).
Acknowledgements
The authors are immensely grateful to the volunteers who freely donated their time to the advancement of knowledge and to a better future for neuropathy patients. The authors thank Alex Meyer, Aiden Xu, Marc Reitz, and Lara Zamboni for their help in developing the system, Daniel Woolley for writing the Unity programme, Manuel Schulthess-Lutz for helping with fMRI data collection and preprocessing, and Jana Hajkova for helping in characterisation of fMRI experiments. The funder had no role in the experimental design, analysis, manuscript preparation or submission. All authors had complete access to data. All authors authorised the submission of the manuscript, but the final submission decision was made by the corresponding author. This project has received the following funding: European Research Council (ERC) under the European Union’s Horizon 2020 research and innovation programme (FeelAgain grant agreement No. 759998). S.R. Swiss National Science Foundation (SNSF) (MOVEIT No. 197271) S.R. Innosuisse ICT programme (n. 47462.1 IP-ICT). S.R. IDEJE by Science Fund of the Republic of Serbia (DiabeticReTrust no. 7753949). S.R. National Science Foundation (SNF 320030_175616). N.W. Swiss National Science Foundation Ambizione Grant (PZ00P3_208996). S.K.
Author information
Authors and Affiliations
Contributions
N.G. and L.C. designed the device, performed all the experiments and all the analyses, made the figures and wrote the manuscript; S.K. and I.O. performed the fMRI experiments and the analyses and wrote the fMRI part of the manuscript; G.P. performed the experiments and prepared the ethical protocol; G.V. co-designed calibration of stimulation; F.B. and N.P. recruited participants; N.W. supervised the fMRI analysis; C.Z. recruited participants, discussed the protocol and results; S.R. designed the device, designed and supervised the experiments, supervised the analyses, discussed the results and wrote the manuscript. All the authors authorised the submission of the manuscript, while the final submission decision was taken by the corresponding author.
Corresponding author
Ethics declarations
Competing interests
The authors do not have anything to disclose.
Peer review
Peer review information
Nature Communications thanks Bijan Najafi, Max Ortiz-Catalan, and the other anonymous reviewer(s) for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
41467_2024_55152_MOESM3_ESM.mp4 (download MP4 )
Supplementary Movie 2: NeuroStep restores missing foot sensations in Diabetic Peripheral Neuropathy Patients. (S2, S3, S5)
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Gozzi, N., Chee, L., Odermatt, I. et al. Wearable non-invasive neuroprosthesis for targeted sensory restoration in neuropathy. Nat Commun 15, 10840 (2024). https://doi.org/10.1038/s41467-024-55152-7
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41467-024-55152-7
This article is cited by
-
Mechanomedicine
Nature Reviews Bioengineering (2026)
-
Diabetic Peripheral Neuropathy: New Diagnostics and Treatment Perspectives
Drugs & Aging (2026)
-
Comfort, consistency, and efficiency of garments with textile electrodes versus hydrogel electrodes for neuromuscular electrical stimulation in a randomized crossover trial
Scientific Reports (2025)