Abstract
An inverse relationship between physical activity and mortality has been observed in epidemiological surveys, but not in randomized clinical trials. This post hoc, not pre-specified analysis of the Italian Diabetes and Exercise Study_2 randomized clinical trial assesses the effect of a physical activity-based counseling intervention on long-term mortality in people with type 2 diabetes. Three hundred physically inactive and sedentary individuals are recruited in three outpatient diabetes clinics in Rome from October 2012 to February 2014. Participants are randomized 1:1 to a Control group receiving standard care and an Intervention group receiving a one-month theoretical and practical counseling targeting both PA and sedentary behavior, each year for 3 years. For this analysis, all-cause and cause-specific mortality are the primary and secondary endpoint, respectively. The vital status is verified on 30 June 2024 and all participants are analyzed. After a 10.3-year follow-up, the number of deaths is significantly lower among Intervention than Control participants (18 vs 35, p = 0.010), mainly due to fewer cancer deaths. Age-and sex-adjusted hazard ratios for mortality are significantly lower in Intervention versus Control participants (0.498 [0.282-0.879], p = 0.016) and between-group differences remain after further adjustment for treatments and baseline cardiometabolic risk profile, major complications, and physical activity and fitness level (0.414 [0.229-0.750], p = 0.004). Limitations include the post hoc type of analysis, a post-trial observational follow-up with no assessment of physical activity and fitness parameters, possible unmeasured confounders, and the non-generalizability to different populations. A behavioral counselling targeting all domains of physical activity and sedentary behavior is associated with reduced long-term mortality risk in people with type 2 diabetes. ClinicalTrials.gov Identifier: NCT01600937.
Similar content being viewed by others
Introduction
Several epidemiological surveys have provided compelling evidence of an inverse independent association between physical activity (PA) level and all-cause and cause-specific mortality1,2,3,4. In addition, PA was found to attenuate the detrimental effect of sedentary time (SED-time) on survival5. An association with mortality was also reported for physical fitness6,7,8, which was shown to be mainly determined by the level of PA9 and to mediate its beneficial effects on survival10. A significant relationship between PA11 or fitness12 and mortality was also reported in people with type 2 diabetes, who have an excess risk of death compared with those without diabetes13. In addition, these individuals are generally poorly adherent to PA recommendations14, indicating the need of identifying and implementing effective behavioral intervention strategies for adoption and maintenance of a physically active lifestyle.
However, at variance with observational studies, no clear evidence has been provided by post hoc analyses of randomized clinical trials that tested lifestyle interventions comprising diet and/or exercise. Of those assessing the efficacy of intervention in preventing type 2 diabetes in people with impaired glucose tolerance (IGT), only the Da Qing Diabetes Prevention Study showed significantly lower all-cause and cardiovascular mortality15,16. Conversely, no between-group difference in mortality was observed in the Finnish Diabetes Prevention Study17 and the Diabetes Prevention Program18. Likewise, the Look AHEAD Study showed no effect of an intensive lifestyle intervention for promoting weight loss in individuals with type 2 diabetes and overweight/obesity on a primary composite endpoint including cardiovascular death19 as well as on all-cause mortality after a post-trial follow-up20. These findings might reflect the failure of such interventions to promote a substantial behavior change that can be maintained in the long term and, hence, favorably impact on survival.
This post hoc, not pre-specified analysis of the Italian Diabetes and Exercise Study (IDES)_2 assessed the effect on long-term mortality of a behavioral counseling aimed at increasing moderate-to-vigorous-intensity PA (MVPA) and decreasing SED-time. This intervention promoted a sustained behavior change characterized by modest increases in MVPA and larger decrements in SED-time with reciprocal increments in light-intensity PA (LPA) (primary endpoint), associated with improvements in physical fitness and cardiometabolic risk profile21.
Results
Patient disposition
As previously reported21, 449 patients were assessed for eligibility from October 2012 to February 2014 in three outpatient diabetes clinics in Rome. After excluding 149 patients for various reasons, the remaining 300 were randomized 1:1 to either an Intervention (INT) group, receiving theoretical and practical counseling for increasing MVPA and decreasing SED-time (n = 150), or a Control (CON) group, receiving standard care (n = 150). The study flow chart is shown in Fig. 1, while the main results have been reported in a previous publication21. Briefly, during the three-year period, there was a relatively modest increase in MVPA in the INT versus CON group (6.4 min day−1, diminished to 3.6 min day−1 at the end of the study), associated with a larger and sustained decrement in SED-time and reciprocal increment in time spent in LPA (0.8 h day−1), with the increase in LPA substantially contributing to the 3.3 METs-hour·week−1 increase in total PA volume21. In addition, changes in both MVPA and SED-time/LPA predicted the improvements in physical fitness and cardiometabolic risk profile22.
Flow of the IDES_2 participants through the study. IDES Italian diabetes and exercise study, INT intervention, CON control, F females, M males.
Primary outcome (all-cause mortality)
The baseline features of participants who were alive ore deceased at censoring are reported in Tables 1 and 2. All participants were analyzed.
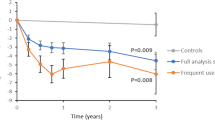
A significantly lower number of participants in the INT versus CON group died over a follow-up of 10.3 ± 2.1 years (range 0.7-11.7) (Table 3). Consistently, crude and age- and sex-adjusted mortality rates (Table 3), Kaplan-Meier estimates (Fig. 2A), and unadjusted and adjusted hazard ratios (HRs) (Fig. 2B, C) were significantly lower in the INT versus CON participants. In addition, the ~50% reduction in mortality risk (0.498 [0.282–0.879], p = 0.016) became even higher ( ~ 60%) when further adjusting for treatments throughout the study and baseline cardiometabolic risk profile, major complications, and PA and fitness parameters (0.414 [0.229-0.750], p = 0.004) (Fig. 2D, E).
Kaplan Meier analysis (A) and Cox proportional hazards regression with backward selection of variables, unadjusted (B) or adjusted for age and sex (C), plus UKPDS risk scores, eGFR, ACR, and history of CVD at baseline and treatment with insulin, GLP-1 receptor agonists, SGLT-2 inhibitors, statins and RAS blockers at any time throughout the study (D), plus SED-time, MVPA, LPA, total PA volume, VO2max and lower body muscle strength at baseline (E), according to study arm (INT vs CON). Numbers (percentages) of deaths, number of participants at risk, and HRs (95% CI) for mortality are shown for each group. INT intervention (green lines), CON control (red lines), UKPDS United Kingdom Prospective Diabetes Study, CVD cardiovascular disease eGFR estimated glomerular filtration rate ACR albumin:creatinine ratio, GLP glucagon-like peptide, SGLT sodium-glucose transporter, RAS renin-angiotensin system, SED-time sedentary time, LPA light-intensity physical activity, MVPA moderate-to-vigorous-intensity physical activity, PA physical activity, VO2max maximal oxygen uptake, HR hazard ratio, CI confidence interval.
Sensitivity analysis
The sensitivity analysis including use at baseline of medications showing any imbalance between the two groups yielded virtually identical results (0.418 [0.231–0.755], p = 0.004).
The sensitivity analysis conducted after excluding the 6 CON and 2 INT participants who died during the three-year study period also provided similar results (Fig. 3).
Kaplan Meier analysis (A) and Cox proportional hazards regression with backward selection of variables, unadjusted (B) or adjusted for age and sex (C), according to study arm (INT vs CON) after excluding participants who died during the three-year follow-up. Numbers (percentages) of deaths, number of participants at risk, and HRs (95% CI) for mortality are shown for each group. INT intervention (green lines), CON control (red lines), HR hazard ratio, CI confidence interval.
Secondary outcome (cause-specific mortality)
Regarding the causes of death, a significantly lower number of deaths from cancer, but not from CVD or other causes, was observed in the INT versus CON participants (Table 4).
Post hoc analyses
These exploratory analyses assessed the association of baseline values or mean values throughout the study of PA and fitness parameters with all-cause mortality, regardless of the study arm. Kaplan-Meier estimates showed a trend for decreasing mortality with decreasing SED-time and increasing LPA, MVPA; total PA volume, maximal oxygen uptake (VO2max), and lower body muscle strength, either for baseline values (Fig. 4, significant for LPA, total PA volume, and VO2max) or mean values throughout the study (Fig. 5, significant for VO2max). The same trend was observed for HRs, which were significant for baseline values and/or mean values throughout the study of all PA and fitness parameters, particularly LPA, total PA volume, and VO2max, considered as quartiles and/or continuous variables (Table 5). When baseline values and mean values throughout the study were included in the same model, adjusted for age and sex, a significant association with mortality was observed for baseline values of LPA and mean values throughout the study of MVPA, total PA volume, VO2max, and lower body muscle strength (Table 5).
Kaplan Meier analysis according to quartiles (I=purple; 2=red; III=blue; IV=green) of baseline values of SED-time (A), LPA (B), MVPA (C), total PA volume (D), VO2max (E) and lower body muscle strength (F). Numbers (percentages) of deaths and number of participants at risk are shown for each quartile. PA physical activity, SED-time sedentary time, LPA light-intensity physical activity, MVPA moderate-to-vigorous-intensity physical activity, VO2max maximal oxygen uptake.
Kaplan Meier analysis according to quartiles (I=purple; 2=red; III=blue; IV=green) of mean values throughout the study of SED-time (A), LPA (B), MVPA (C), total PA volume (D), VO2max (E) and lower body muscle strength (F). Numbers (percentages) of deaths and number of participants at risk are shown for each quartile. PA physical activity, SED-time sedentary time, LPA light-intensity physical activity, MVPA moderate-to-vigorous-intensity physical activity, VO2max maximal oxygen uptake.
Discussion
This post hoc, not pre-specified analysis of the IDES_2 showed that a behavioral counseling targeting PA and sedentary behavior was associated with long-term reduction in all-cause mortality versus standard care, which was mainly driven by fewer cancer deaths. This relationship remained after adjustment for treatments and baseline cardiometabolic risk profile, major complications, and PA and fitness level. Moreover, a significant association with mortality was observed for PA and fitness parameters at baseline and throughout the study in the exploratory analyses conducted regardless of study arm.
All-cause mortality
The favorable effect on long-term mortality of the theoretical and practical counseling tested in the IDES_2 may reflect the promotion of a sustained increase in PA and decrease in SED-time, a behavior change that might have been maintained during the post-intervention period, consistent with the well-established efficacy of behavioral counseling interventions in promoting healthy behaviors23. The finding that, in the IDES_2, the moderate but sustained, favorable changes in PA and sedentary behavior and fitness level were associated with progressive improvements in psychological well-being and health related quality of life24 suggests that these changes may have contributed to the perception of the behavioral intervention as less burdensome, consistent with the reported U-shaped relationship between PA and burden perception25, and possibly more enjoyable26. The perceived burden, as well as the tailored and repetitive nature of the intervention, may have facilitated the long-term sustainability of behavior change27 and contributed to the maintenance of associated health benefits even after termination of the study period.
However, the finding that the behavioral counseling was successful in reducing all-cause mortality is consistent with only a few trials testing lifestyle interventions. A significant effect was observed in the Da Qing Diabetes Prevention Study, with a 29% and 41% reduction at 23 years15 and a 26% and 33% at 30 years16 in all-cause and cardiovascular mortality, respectively, in the intervention versus control group. Moreover, in older adults with knee osteoarthritis and overweight/obesity participating in the Data from the Arthritis, Diet, and Activity Promotion Trial, intentional weight loss achieved through lifestyle intervention was associated with 50% lower mortality28. In contrast, no between-group difference in mortality risk was observed in the Finnish Diabetes Prevention Study17, the Diabetes Prevention Program18, and the Look AHEAD Study19,20, though in the Finnish Diabetes Prevention Study risk of death in both groups combined was much lower than in the population-based FINRISK IGT reference cohort17. In addition, a recent analysis of the 30-year data from the Da Qing Diabetes Prevention Study showed that the effect of exercise-only intervention was not significant, at variance with diet plus exercise and diet-only interventions29. However, in the Look AHEAD Study, participants who lost ≥10% at one year showed a significant reduction in the primary outcome including cardiovascular death30 and in all-cause mortality20. In addition, in the above trials, lifestyle interventions were effective in improving cardiometabolic risk profile as well as in reducing morbidities associated with increased mortality risk, including CVD, microvascular complications, depression, and physical disability16,17,31,32,33,34,35,36,37,38.
Several reasons might explain the different effects on all-cause mortality in people with type 2 diabetes participating in the IDES_2 and the Look AHEAD, with only the former showing a reduced risk of death in the intervention versus control group despite a much smaller sample size. First, the intervention was PA-based only and aimed at promoting a sustained behavior change in the IDES_2, whereas it was based on both diet and exercise and aimed at promoting a ≥ 7% weight loss in the Look AHEAD. Second, participants in the two trials differed for several clinical features that may affect mortality, such as BMI, sex, ethnicity, and history of CVD. Third, as other counseling interventions designed to promote walking through the provision of pedometers39,40,41, that of the Look AHEAD was of progressively decreasing intensity and focused solely on MVPA, thus resulting in relatively modest and not sustained increases in MVPA, with no change in SED-time and LPA35,42. This is at variance with the IDES_2, in which the counseling was focused on both MVPA and SED-time and promoted reallocation of large amounts of SED-time to LPA, mainly contributing to the large increases in total PA volume and physical fitness, in addition to modest increases in MVPA21. This interpretation is further supported by the strict relationship of values at baseline and throughout the study of PA and fitness parameters with all-cause death. Importantly, though exploratory in nature, these analyses showed that the associations with mortality of mean values throughout the study of MVPA, total PA volume, VO2max, and lower body muscle strength were independent of baseline values, thus arguing in favor of a major role of the intervention in the reduced mortality observed in our study. This is also consistent with a large body of evidence pointing to an important effect on mortality risk of reallocating SED-time to LPA. In fact, a prospective cohort study showed that both the amount and pattern of SED-time were associated with mortality43, and a meta-analysis of observational studies demonstrated an inverse relationship between time spent in daily LPA and all-cause death44. Moreover, prospective studies reported that the association between SED-time or LPA and mortality risk was attenuated, but not abolished by MVPA45, and the number, but not intensity of daily steps was associated all-cause death46,47.
Cause-specific mortality
The finding that the reduced mortality in the IDES_2 was related to fewer deaths from cancer ( ~ 4-fold), but not from CVD is in contrast with the known combined detrimental effect of physical inactivity and sedentary behavior on both cardiovascular and cancer mortality48. However, due to the low number of deaths, the results of the analysis of cause-specific mortality should be interpreted as exploratory, indicating the need for additional studies with larger sample size and/or longer follow-up duration. In any case, this apparent discrepancy might be explained by the pattern of behavior change promoted by the counseling intervention in the IDES_2, which consisted in a decrease in SED-time (with reciprocal increase in LPA) more than an increase in MVPA. In fact, higher PA intensities and volumes were shown to be required to reduce cardiovascular risk49, whereas prolonged sitting time was found to be associated with increased cancer incidence, in addition to (and independently of) a low amount of MVPA, thus suggesting that cancer risk may be decreased by reducing sedentary behaviors50.
Clinical implications
These findings further support the importance of behavioral counseling interventions in promoting the adoption and maintenance of an active lifestyle and suggest the importance of targeting all domains of PA/sedentary behavior in all settings, including not only leisure-time, but also home, work, and commuting. This is crucial for producing a sustained all-round behavior change, including increases in both LPA and MVPA and decreases in SED-time, in order to obtain improvements in physical fitness and long-term survival benefits.
Strengths and limitations
The main strength of this study is the application of an intervention targeting both PA and sedentary-time across all settings, based on theoretical grounds, and using several behavioral change techniques accounting for psychosocial, socio-economic, family, and cultural factors. Other strengths include the lack of missing data for vital status and the assessment of a wide range of parameters to account for, with objective (accelerometer-based) PA measurements.
However, this study has several limitations. First, this was a post hoc, not pre-specified analysis, not powered for the mortality outcome, and including a post-trial observational follow-up, like the other lifestyle intervention trials assessing long-term mortality15,16,17,18,19,20. Therefore, results should be interpreted with caution. Second, the size of the sample and the duration of the intervention were lower than in other trials assessing the effect of lifestyle modification on mortality, thus resulting in a low number of events, which make the interpretation of between-group differences in cause-specific deaths uncertain. However, the sample size was relatively small also in the Da Qing Diabetes Prevention Outcome Study, which reported a significant reduction in mortality with lifestyle intervention15,16, at variance with the much larger Diabetes Prevention Program and Look AHEAD Study18,19,20. Third, PA and fitness parameters as well as cardiovascular risk factors and medication use were not assessed during the post-trial follow-up. Fourth, between group differences in baseline features despite randomization might have affected the results, though they were minimal and were accounted for in the statistical analyses. Fifth, despite the large number of parameters assessed that significantly reduced potential confounding bias, it cannot be excluded that some unmeasured confounders might have also influenced the results. For instance, diet was not considered in data analysis, though patients received dietary prescriptions and adherence to diet was verified at intermediate visits. Finally, the results of this study cannot be readily extrapolated to people with type 2 diabetes with different characteristics or to non-diabetic individuals. Due to these limitations, further studies are required to confirm the beneficial impact on mortality of the intervention strategy tested in the IDES_2 and its generalizability to different populations.
In conclusion, this follow-up analysis of the IDES_2 showed that a three-year behavioral counseling promoting sustained changes in all domains of PA/sedentary behavior was associated with a ~ 50% reduction in all-cause mortality versus standard care. These findings have important clinical implications for the design and implementation of effective counseling interventions to produce a sustained behavior change resulting in reduced long-term mortality in people with type 2 diabetes.
Methods
Design and methods of the IDES_2 are detailed in previous publications21,51 and provided as Supplementary Information.
Design
The IDES_2 was an open-label, assessor-blinded, parallel, superiority randomized clinical trial assessing the efficacy a behavioral counseling intervention for adoption and maintenance of a physically active lifestyle in people with type 2 diabetes.
The research protocol complies with the Declaration of Helsinki and was registered with ClinicalTrials.gov (NCT01600937) on 10 October 2012. It was approved by the Ethics Committee of Sant’Andrea Hospital on 25 September 2012 (n. 212/2012) and participants providinged written informed consent and received no compensation.
Participants
Inclusion criteria were type 2 diabetes of ≥1-year duration; age 40-80 years; body mass index 27-40 kg·m-2; physical inactivity and sedentary behavior for ≥6 months; ability to walk 1.6 Km without assistance; and clearance by a cardiologist. Exclusion criteria were all conditions limiting or contraindicating PA51.
Randomization and blinding
Three hundred eligible patients were recruited in three outpatient diabetes clinics in Rome from October 2012 to February 2014 and subsequently randomized 1:1 to either an INT group, receiving theoretical and practical counseling for increasing MVPA and decreasing SED-time (n = 150), or a CON group, receiving standard care (n = 150).
Randomization was stratified by center and, within each center, by age ( < versus ≥ 65 years) and diabetes treatment (non-insulin versus insulin), using a permuted-block randomization software that randomly varies the block size (range 4–8). To ensure allocation concealment, randomization was centralized at the Department of Clinical Pharmacology and Epidemiology, Consorzio Mario Negri Sud, S. Maria Imbaro, Italy, and implemented by central telephone.
Physicians, exercise specialists, and participants, but not assessors of study parameters, were unblinded to group assignment.
Interventions
The INT group was engaged in a one-month theoretical and practical counseling, once-a-year for 3 years. It consisted of one individual theoretical counseling session, held by a diabetologist, plus eight twice-weekly individual theoretical and practical counseling sessions51.
The 30 min theoretical, individual, face-to-face counseling session was held by a diabetologist and consisted of seven steps52. It was focused on both SED-time/LPA and MVPA across all settings (i.e., leisure-time, transport, household, and occupation). Specifically, it was aimed at assessing patient’s current behavior, increasing his/her awareness of the importance of targeting both domains of PA/sedentary behavior, setting individual goals and programs, identifying internal and external barriers to behavior change in the patient’s personal, family, social, work, and environmental context, and discussing practical solutions for the problems identified.
Each theoretical and practical counseling session was supervised by a certified exercise specialist. The theoretical counseling, which was delivered before the practical counseling and lasted 15 minutes, was aimed at improving patient’s knowledge of the effects of exercise on health, conditions contraindicating exercise, difference between habitual and occasional exercise, essential parameters of wellness such as BP, heart rate, and blood glucose. The practical counseling lasted 75 minutes and consisted of 30 minutes of aerobic exercise followed by 30 minutes of resistance exercise, both at low-to-moderate-intensity depending on the patient’s physical ability, plus additional 15 minutes for warm up and cool down (including stretching). It served to instruct patients to distinguish the different types of exercise, evaluate exercise intensity, monitor and prevent or correct glucose imbalances during and after the session by adjusting medications and/or consuming carbohydrate snacks.
Both physicians and exercise specialists were specifically trained in order to standardize procedures, prevent clustering effect, improve efficacy and safety of intervention, promote patient adherence, and minimize drop-out.
This approach was designed to promote an increase in any kind of PA, based on patient’s preference, and a decrease in SED-time through a two-step behavior change, i.e. decreasing SED-time by substituting and/or interrupting it with LPA and reallocating SED-time and/or time spent in LPA towards gradually increasing amounts of purposeful MVPA. The CON group received only standard care, which included general physician recommendations for increasing daily PA and decreasing SED-time.
Participants in the two group received the same standard care regimen, including dietary prescription, to achieve glycemic, lipid, blood pressure (BP), and body weight targets, according to current guidelines53. Treatment was adjusted using a pre-specified algorithm.
Outcome measures
The primary outcome of IDES-2 was to assess the effect of a behavioral intervention versus standard care on the adoption and maintenance of a physically active lifestyle and included four coprimary endpoints, i.e., SED-time, time spent in LPA and MVPA, and total PA volume over the three-year period.
Other outcomes included the effect of the intervention on physical fitness, modifiable cardiovascular risk factors, musculo-skeletal disturbances, psychological well-being, and health related quality of life (secondary) and the relationship between change in behavior and change in the secondary endpoints (ancillary).
The results for these outcomes have been reported in previous publications21,22,24,54,55, except for those regarding musculo-skeletal disturbances, which were not analyzed due to the high percentage of unfilled questionnaires.
The primary outcome of this post hoc, not pre-specified analysis was all-cause mortality. The vital status of study participants on 30 June 2024 was verified by interrogating the Italian Health Card database https://sistemats4.sanita.finanze.it/simossHome/login.jsp)56.
Causes of death were assessed as secondary outcome in the IDES_2 only, retrieved from medical records obtained from the patient’ relatives or general practitioner.
Measurement of study parameters
The study parameters were measured every 4 months (12 months for fitness).
Total PA volume, time spent in LPA and MVPA, and SED-time were measured by the use of an accelerometer (MyWellness Key, Technogym, Cesena, IT) and a daily diary for reporting the time spent sleeping, wearing the instrument, and performing non-accelerometer recordable activities. Participants were asked to wear the device in waking hours (except if swimming) from awakening to bedtime. In this way, it was possible to assume that the accelerometer non-wear time in the awake state was spent in routine morning and evening sedentary activities and it was therefore added to the accelerometer-based SED-time to calculate total SED-time. Matthews’ cut-points was used to identify time spent in LPA (100–1951 counts/min corresponding to 1.5–2.9 METs)57, whereas Freedson’s cut-points were used to determine time spent in PA of moderate (1952–5724 counts/min corresponding to 3–5.9 METs) and vigorous ( ≥ 5725 counts/min corresponding to ≥6 METs) intensity58. Diary-reported time spent in non-accelerometer recordable activities was added to that recorded by the accelerometer, according to the intensity of each activity59.
Physical fitness was evaluated by assessing cardiorespiratory fitness by estimating maximal oxygen uptake (VO2max) from peak oxygen uptake during a maximal treadmill test, muscular fitness, as upper and lower body strength by isometric tests, and flexibility by a standard bending test.
Cardio-respiratory fitness was assessed by a maximal treadmill exercise test using a Balke protocol60. Patients were instructed not to hold the treadmill rails and were verbally encouraged to reach volitional exhaustion, as reported by the patient or by the physician for medical reasons. The time to exhaustion was used to estimate maximal oxygen uptake (VO2max), given the high correlation between these two parameters.
For strength assessment, isometric muscle strength was measured by means of a strain gauge tensiometer (Digimax, Mechatronic GmbH, Germany)51. The muscles chains involved in fundamental activities of daily living were tested. Upper body muscle strength was assessed by maximal voluntary contractions (MVCs) performed at a shoulder press (Technogym) along the sagittal plane, with a 90° and 45° angle at the elbow and between the upper arm and the trunk, respectively. Lower limb muscle strength was assessed by MVCs performed at a costumed leg extension machine (Technogym). The angle at the knee and the hip was fixed at 90°. Subjects were asked to exert their maximal force with both limbs simultaneously and to maintain it for at least 2-3 seconds before relaxing. For each exercise, three MVCs were performed, with 3-min rest interval between contractions. During the MVCs, verbal encouragement was provided.
For hip and trunk flexibility assessment, a standard bending test was executed51. Standing on a step with the legs fully extended, patients were asked to bend the torso forward to try to touch the ground with their fingertips. The test was performed three times and the distance between the finger and the ground was measured by the exercise specialist at the third attempt.
Modifiable cardiovascular risk factors included clinical and biochemical parameters. Body weight and height were measured using scale and stadiometer and BMI was then calculated as weight (kg)/height (m2), while waist circumference was taken at the umbilicus and BP was recorded with a sphygmomanometer after a five-minute rest with the patient seated with the arm at the heart level. Hemoglobin A1c (HbA1), fasting plasma glucose, triglycerides, total, HDL, and LDL cholesterol, serum creatinine, and albumin/creatinine ratio. Biochemical tests were centralized at the Laboratory of Clinical Chemistry of Sant’Andrea University Hospital. Glomerular filtration rate (GFR) was then estimated from serum creatinine by the use of the Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) equation [31], whereas global and fatal CHD and stroke 10-year risk scores were calculated using the United Kingdom Prospective Diabetes Study (UKPDS) risk engine61.
Statistical analysis
Data are presented as mean ± SD, for continuous variables, and number of cases and percentage, for categorical variables. Between-group differences were assessed by unpaired two-sided Student’s t test, for continuous variables, and Pearson’s χ2 test or Fisher’s exact test, as appropriate, for categorical variables.
Crude mortality rates in each group were described as events per 1000 patient-years from start of follow-up to censoring, with 95% exact Poisson confidence intervals (CIs), and adjusted for age and sex by a Poisson regression model. Between-group differences were assessed by generalized linear models. Kaplan-Meier survival probabilities for all-cause mortality were estimated according to study arm. The hazard ratios (HRs) and their 95% CIs were estimated by Cox proportional hazards regression with backward selection of variables. These analyses were either unadjusted or sequentially adjusted for age and sex (model 1), UKPDS risk scores, estimated glomerular filtration rate, albumin: creatinine ratio, and history of cardiovascular disease (CVD) at baseline and treatment with insulin, glucagon-like peptide-1 receptor agonists, sodium-glucose transporter-2 inhibitors, statins, and blockers of the renin-angiotensin system at any time throughout the study (model 2), SED-time, MVPA, LPA, PA volume, VO2max and lower body muscle strength at baseline (model 3). Use of cardioprotective medications throughout the study was included as covariate (yes/no) instead of use at baseline to fully account for the higher, though not statistically significant, exposure to these agents during the three-year study period in the CON versus the INT group21, which was required to achieve comparable glucose, lipid and BP levels because of the lower energy expenditure. However, a sensitivity analysis including baseline treatment with medications showing any imbalance between the two groups was conducted. Finally, a sensitivity analysis was conducted after excluding participants who died during the three-year study period.
The above analyses were also run according to baseline values or mean values throughout the study of SED-time, LPA, MVPA, total PA volume, VO2max, and lower body muscle strength, either as quartiles or continuous variables, regardless of the study arm. The mean values throughout the study were calculated for each participant as the average of all measures obtained from baseline to end-of-study (i.e., either at 3 years or when patients dropped out for any reason, including death).
All p values were two-sided, and a p < 0.05 was considered statistically significant. Statistical analyses were performed using SPSS version 13.0 (SPSS Inc., Chicago, IL, USA).
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
The raw data are available under restricted access due to the inclusion of confidential information. For strictly research purposes, access can be obtained by the corresponding author (giuseppe.pugliese@uniroma1.it) on reasonable request within 3 months. Source data are provided with this paper.
References
Paffenbarger, R. S., Hyde, R. T. Jr, Wing, A. L. & Hsieh, C. C. Physical activity, all-cause mortality, and longevity of college alumni. N. Engl. J. Med. 314, 605–613 (1986).
Fishman, E. I. et al. Association between objectively measured physical activity and mortality in NHANES. Med. Sci. Sports Exerc 48, 1303–1311 (2016).
Moore, S. C. et al. Leisure time physical activity of moderate to vigorous intensity and mortality: a large pooled cohort analysis. PLoS Med. 9, e1001335 (2012).
Ekelund, U. et al. Dose-response associations between accelerometry measured physical activity and sedentary time and all-cause mortality: systematic review and harmonised meta-analysis. BMJ 366, l4570 (2019).
Ekelund, U. et al. Does physical activity attenuate, or even eliminate, the detrimental association of sitting time with mortality? A harmonised meta-analysis of data from more than 1 million men and women. Lancet 388, 1302–1310 (2016).
Blair, S. N. et al. Physical fitness and all-cause mortality. A prospective study of healthy men and women. JAMA 262, 2395–2401 (1989).
Myers, J. et al. Exercise capacity and mortality among men referred for exercise testing. N. Engl. J. Med. 346, 793–801 (2002).
Ruiz, J. R. et al. Association between muscular strength and mortality in men: prospective cohort study. BMJ 337, a439 (2008).
Church, T. S., Earnest, C. P., Skinner, J. S. & Blair, S. N. Effects of different doses of physical activity on cardiorespiratory fitness among sedentary, overweight or obese postmenopausal women with elevated blood pressure: a randomized controlled trial. JAMA 297, 2081–2091 (2007).
Celis-Morales, C. A. et al. The association between physical activity and risk of mortality is modulated by grip strength and cardiorespiratory fitness: evidence from 498135 UK-Biobank participants. Eur. Heart J. 38, 116–122 (2017).
Hu, G. et al. Physical activity, cardiovascular risk factors, and mortality among Finnish adults with diabetes. Diab. Care 28, 799–805 (2005).
Church, T. S., LaMonte, M. J., Barlow, C. E. & Blair, S. N. Cardiorespiratory fitness and body mass index as predictors of cardiovascular disease mortality among men with diabetes. Arch. Intern. Med. 165, 2114–2120 (2005).
Tancredi, M. et al. Excess mortality among persons with type 2 diabetes. N. Engl. J. Med. 373, 1720–1732 (2015).
Resnick, H. E., Foster, G. L., Bardsley, J. & Ratner, R. E. Achievement of American Diabetes Association clinical practice recommendations among U.S. adults with diabetes, 1999-2002: the National Health and Nutrition Examination Survey. Diab. Care 29, 531–537 (2006).
Li, G. et al. Cardiovascular mortality, all-cause mortality, and diabetes incidence after lifestyle intervention for people with impaired glucose tolerance in the Da Qing Diabetes Prevention Study: a 23-year follow-up study. Lancet Diab. Endocrinol. 2, 474–480 (2014).
Gong, Q. et al. Morbidity and mortality after lifestyle intervention for people with impaired glucose tolerance: 30-year results of the Da Qing Diabetes Prevention Outcome Study. Lancet Diab. Endocrinol. 7, 452–461 (2019).
Uusitupa, M. et al. Ten-year mortality and cardiovascular morbidity in the Finnish Diabetes Prevention Study-secondary analysis of the randomized trial. PLoS One 4, e5656 (2009).
Lee, C. G. et al. Effect of Metformin and Lifestyle Interventions on Mortality in the Diabetes Prevention Program and Diabetes Prevention Program Outcomes Study. Diab. Care 44, 2775–2782 (2021).
Look AHEAD Research Group, W. ingR. R. et al. Cardiovascular effects of intensive lifestyle intervention in type 2 diabetes. N. Engl. J. Med. 369, 145–154 (2013).
Look AHEAD Research Group. Effects of intensive lifestyle intervention on all-cause mortality in older adults with type 2 diabetes and overweight/obesity: results from the look AHEAD study. Diabetes Care. 45, 1252–1259 (2022).
Balducci, S. et al. Effect of a behavioral intervention strategy on sustained change in physical activity and sedentary behavior in patients with type 2 diabetes: the IDES_2 Randomized Clinical Trial. JAMA 321, 880–890 (2019).
Balducci, S. et al. Relationships of changes in physical activity and sedentary behavior with changes in physical fitness and cardiometabolic risk profile in individuals with type 2 diabetes: the Italian diabetes and exercise Study 2 (IDES_2). Diab. Care 45, 213–221 (2022).
O’Connor, E. A., Evans, C. V., Rushkin, M. C., Redmond, N. & Lin, J. S. Behavioral counseling to promote a healthy diet and physical activity for cardiovascular disease prevention in adults with cardiovascular risk factors: updated evidence report and systematic review for the US Preventive Services Task Force. JAMA 324, 2076–2094 (2020).
Nicolucci, A. et al. Effect of a behavioural intervention for adoption and maintenance of a physically active lifestyle on psychological well-being and quality of life in patients with type 2 diabetes: the IDES_2 Randomized Clinical Trial. Sports Med. 52, 643–654 (2022).
Watkins, K. W. et al. Effect of adults’ self–regulation of diabetes on quality-of-life outcomes. Diab. Care 23, 1511–1515 (2000).
Teixeira, D. S., Rodrigues, F., Cid, L. & Monteiro, D. Enjoyment as a predictor of exercise habit, intention to continue exercising, and exercise frequency: the intensity traits discrepancy moderation role. Front. Psychol. 13, 780059 (2022).
Middleton, K. R., Anton, S. D. & Perri, M. G. Long-Term Adherence to Health Behavior Change. Am. J. Lifestyle Med. 7, 395–404 (2013).
Shea, M. K. et al. The effect of randomization to weight loss on total mortality in older overweight and obese adults: the ADAPT Study. J. Gerontol. A Biol. Sci. Med. Sci. 65, 519–525 (2010).
Yu, L. et al. Influence of a diet and/or exercise intervention on long-term mortality and vascular complications in people with impaired glucose tolerance: Da Qing Diabetes Prevention Outcome study. Diab. Obes. Metab. 26, 1188–1196 (2024).
Look AHEAD Research Group, G. reggE. W. et al. Association of the magnitude of weight loss and changes in physical fitness with long-term cardiovascular disease outcomes in overweight or obese people with type 2 diabetes: a post-hoc analysis of the Look AHEAD randomised clinical trial. Lancet Diab. Endocrinol. 4, 913–921 (2016).
Gong, Q. et al. Long-term effects of a randomised trial of a 6-year lifestyle intervention in impaired glucose tolerance on diabetes-related microvascular complications: the China Da Qing Diabetes Prevention Outcome Study. Diabetologia 54, 300–307 (2011).
Lindström, J. et al. The Finnish Diabetes Prevention Study (DPS): Lifestyle intervention and 3-year results on diet and physical activity. Diab. Care 26, 3230–3236 (2003).
Ratner, R. et al. Impact of intensive lifestyle and metformin therapy on cardiovascular disease risk factors in the diabetes prevention program. Diab. Care 28, 888–894 (2005).
Diabetes Prevention Program Research Group. Long-term effects of lifestyle intervention or metformin on diabetes development and microvascular complications over 15-year follow-up: the Diabetes Prevention Program Outcomes Study. Lancet Diabetes Endocrinol. 3, 866–875 (2015).
Look AHEAD Research Group, W. ingR. R. Long-term effects of a lifestyle intervention on weight and cardiovascular risk factors in individuals with type 2 diabetes mellitus: four-year results of the Look AHEAD trial. Arch. Intern. Med. 170, 1566–1575 (2010).
Look AHEAD Research Group. Effect of a long-term behavioural weight loss intervention on nephropathy in overweight or obese adults with type 2 diabetes: a secondary analysis of the Look AHEAD randomised clinical trial. Lancet Diab. Endocrinol. 2, 801–809 (2014).
Faulconbridge, L. F. et al. One-year changes in symptoms of depression and weight in overweight/obese individuals with type 2 diabetes in the Look AHEAD study. Obesity 20, 783–793 (2012).
Gregg, E. W. et al. Impact of Intensive Lifestyle Intervention on Disability-Free Life Expectancy: The Look AHEAD Study. Diab. Care 41, 1040–1048 (2018).
Harris, T. et al. Physical activity levels in adults and older adults 3-4 years after pedometer-based walking interventions: long-term follow-up of participants from two randomised controlled trials in UK primary care. PLoS Med. 15, e1002526 (2018).
Khunti, K. et al. Promoting physical activity in a multi-ethnic population at high risk of diabetes: the 48-month PROPELS randomised controlled trial. BMC Med 19, 130 (2021).
Andrews, R. C. et al. Diet or diet plus physical activity versus usual care in patients with newly diagnosed type 2 diabetes: the Early ACTID randomised controlled trial. Lancet 378, 129–139 (2011).
Unick, J. L. et al. Four-year physical activity levels among intervention participants with type 2 diabetes. Med Sci. Sports Exerc 48, 2437–2445 (2016).
Diaz, K. M. et al. Patterns of Sedentary Behavior and Mortality in U.S. Middle-Aged and Older Adults: a national Cohort Study. Ann. Intern Med 167, 465–475 (2017).
Chastin, S. F. M. et al. How does light-intensity physical activity associate with adult cardiometabolic health and mortality? Systematic review with meta-analysis of experimental and observational studies. Br. J. Sports Med. 53, 370–376 (2019).
Matthews, C. E. et al. Accelerometer-measured dose-response for physical activity, sedentary time, and mortality in US adults. Am. J. Clin. Nutr. 104, 1424–1432 (2016).
Lee, I. M. et al. Association of step volume and intensity with all-cause mortality in older women. JAMA Intern Med 179, 1105–1112 (2019).
Saint-Maurice, P. F. et al. Association of daily step count and step intensity with mortality among US Adults. JAMA 323, 1151–1160 (2020).
Ekelund, U. et al. Do the associations of sedentary behaviour with cardiovascular disease mortality and cancer mortality differ by physical activity level? A systematic review and harmonised meta-analysis of data from 850 060 participants. Br. J. Sports Med. 53, 886–894 (2019).
Dempsey, P. C. et al. Physical activity volume, intensity, and incident cardiovascular disease. Eur. Heart J. 43, 4789–4800 (2022).
Biswas, A. et al. Sedentary time and its association with risk for disease incidence, mortality, and hospitalization in adults: a systematic review and meta-analysis. Ann. Intern. Med. 162, 123–132 (2015).
Balducci, S. et al. The Italian Diabetes and Exercise Study 2 (IDES-2): a long-term behavioral intervention for adoption and maintenance of a physically active lifestyle. Trials 16, 569 (2015).
Di Loreto, C. et al. Validation of a counseling strategy to promote the adoption and the maintenance of physical activity by type 2 diabetic subjects. Diab. Care 26, 404–408 (2003).
American Diabetes Association. Standards of medical care in diabetes--2012. Diab. Care 35, S11–S63 (2012).
Balducci, S. et al. Sustained decreases in sedentary time and increases in physical activity are associated with preservation of estimated β-cell function in individuals with type 2 diabetes. Diab. Res. Clin. Pr. 193, 110140 (2022).
Balducci, S. et al. Sustained increase in physical fitness independently predicts improvements in cardiometabolic risk profile in type 2 diabetes. Diab. Metab. Res Rev. 39, e3671 (2023).
Orsi, E. et al. Haemoglobin A1c variability is a strong, independent predictor of all-cause mortality in patients with type 2 diabetes. Diab. Obes. Metab. 20, 1885–1893 (2018).
Matthews CE. Calibration of accelerometer output for adults. Med. Sci. Sports Exerc. 37, S512–S522 (2005).
Freedson, P. S., Melanson, E. & Sirard, J. Calibration of the Computer Science and Applications, Inc. accelerometer. Med. Sci. Sports Exerc 30, 777–781 (1998).
Ainsworth, B. E. et al. Compendium of physical activities: classifications of energy costs of human physical activities. Med. Sci. Sports Exerc 25, 71–80 (1993).
Blair, S. N. et al. Changes in physical fitness and all-cause mortality: a prospective study of healthy and unhealthy men. JAMA 273, 1093–1098 (1995).
Stevens, R. J., Kothari, V., Adler, A. I. & Stratton, I. M. United Kingdom Prospective Diabetes Study (UKPDS) Group. The UKPDS risk engine: a model for the risk of coronary heart disease in Type II diabetes (UKPDS 56). Clin. Sci. 101, 671–679 (2001).
Acknowledgements
The Authors thank the IDES and IDES_2 Investigators for participating in the trials (see Supplementary Information). This work was supported by the Metabolic Fitness Association, Monterotondo (Rome), Italy to SB and the Ministero della Salute grant PNRR-MAD-2022-12375970 funded by the European Union - Next Generation EU - NRRP M6C2 - Investment 2.1 Enhancement and strengthening of biomedical research in the NHS to GP. The funders had no role in study design, data collection, data analysis, data interpretation, or writing of the report.
Author information
Authors and Affiliations
Consortia
Contributions
S.B., J.H., and G.P. conceived the study. S.B., J.H., M.V., L.M., F.C., M.M., E.C., F.A., A.G., M.S., G.O., S.Z., and G.P. acquired the data. A.N. and G.P. performed the statistical analysis. All authors were involved in the interpretation of the data. G.P. drafted the manuscript, which was critically revised by all authors, who approved the final version and agree to be accountable for it. S.B., J.H., and G.P. have directly accessed and verified the underlying data reported in this manuscript. All authors had full access to all the data in the study and had final responsibility for the decision to submit for publication.
Corresponding author
Ethics declarations
Competing interests
SB received personal fees from Astra-Zeneca, Eli Lilly, Novo Nordisk, and Takeda; JH received personal fees from Boehringer Ingelheim; MV received personal fees from MundiPharma and Novo Nordisk; SZ is an employer of Technogym; AN received grants from Artsana, Astra-Zeneca, Eli Lilly, Novo Nordisk, and Sanofi Aventis and personal fees from Eli Lilly and Novo Nordisk; GP received personal fees from Astra-Zeneca, Boehringer Ingelheim, Eli Lilly, Merck Sharp & Dome, Mylan, Sigma-Tau, and Takeda. No other disclosures were reported.
Peer review
Peer review information
Nature Communications thanks Richard Woodman and the other anonymous reviewer(s) for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Balducci, S., Haxhi, J., Vitale, M. et al. Effect of a behavioral counseling for adoption and maintenance of a physically active lifestyle on long-term mortality in people with type 2 diabetes: post hoc analysis of the Italian Diabetes and Exercise Study_2. Nat Commun 17, 1930 (2026). https://doi.org/10.1038/s41467-026-68618-7
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41467-026-68618-7