Abstract
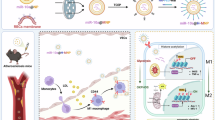
Precise regulation of mitochondrial reactive oxygen species (mtROS) in macrophages is essential for reducing inflammation and promoting diabetic wound healing. However, achieving targeted and responsive mtROS modulation in specific cell remains challenging. Herein, we report a macrophage-mitochondria hybrid membrane derived artificial extracellular vesicle platform (C@AH-EV). C@AH-EV integrates biomimetic dual-targeting membranes with an mtROS activatable prodrug. It leverages membrane protein-mediated targeting of macrophage mitochondria to offer highly selective intracellular delivery. The payload is a ROS sensitive antioxidant prodrug, which incorporates lipid tails that enhance its drug loading efficiency in vesicles. Upon mtROS-triggered cleavage of the boronate ester bond, potent antioxidants were locally released within the mitochondria to restore redox balance. In vitro and in vivo studies demonstrate that C@AH-EVs effectively reprogram macrophages from an inflammatory toward an anti-inflammatory phenotype, thereby attenuating inflammation and accelerating diabetic wound repair. This work offers a promising direction for treating chronic inflammatory conditions.
Similar content being viewed by others
Data availability
The data that support the findings of this study are available within the article and its Supplementary Information files. Source data are available for Figs. 2d–g, i, 3e, g–i, 5b, h, k, 6b, c, g, h, 7b, c, e, f, 8a–f and 9d, Supplementary Figs. 16, 19, 21, 22, 26–30 and 34–43. Source data are provided with this paper.
References
Zhang, Y. et al. Global disability burdens of diabetes-related lower-extremity complications in 1990 and 2016. Diabetes Care 43, 964–974 (2020).
Powers, J. G., Higham, C., Broussard, K. & Phillips, T. J. Wound healing and treating wounds: chronic wound care and management. J. Am. Acad. Dermatol. 74, 607–625 (2016).
Lipsky, B. A. A current approach to diabetic foot infections. Curr. Infect. Dis. Rep. 1, 253–260 (1999).
Osterman, F. A. Jr The use of angioplasty, bypass surgery, and amputation in the management of peripheral vascular disease. N. Engl. J. Med. 326, 414 (1992).
da Silva, A. F. et al. Audit Committee of the Vascular Surgical Society of Great Britain and Ireland The management and outcome of critical limb ischaemia in diabetic patients: results of a national survey. Diabet. Med. 13, 726–728 (1996).
Saluja, S. et al. Foot ulceration and its association with mortality in diabetes mellitus: a meta-analysis. Diabet. Med. 37, 211–218 (2020).
Monaghan, M. G., Borah, R., Thomsen, C. & Browne, S. Thou shall not heal: overcoming the non-healing behaviour of diabetic foot ulcers by engineering the inflammatory microenvironment. Adv. Drug Deliv. Rev. 203, 115120 (2023).
Li, M., Hou, Q., Zhong, L., Zhao, Y. & Fu, X. Macrophage related chronic inflammation in non-healing wounds. Front. Immunol. 12, 681710 (2021).
Vikram, A., Tripathi, D. N., Kumar, A. & Singh, S. Oxidative stress and inflammation in diabetic complications. Int. J. Endocrinol. 2014, 679754 (2014).
Bullon, P., Newman, H. N. & Battino, M. Obesity, diabetes mellitus, atherosclerosis and chronic periodontitis: a shared pathology via oxidative stress and mitochondrial dysfunction?. Periodontology 2000 64, 139–153 (2014).
Puleston, D. J. et al. Polyamines and eIF5A hypusination modulate mitochondrial respiration and macrophage activation. Cell Metab. 30, 352–363.e8 (2019).
Glorieux, C., Liu, S., Trachootham, D. & Huang, P. Targeting ROS in cancer: rationale and strategies. Nat. Rev. Drug Discov. 23, 583–606 (2024).
Formentini, L. et al. Mitochondrial ROS production protects the intestine from inflammation through functional M2 macrophage polarization. Cell Rep. 19, 1202–1213 (2017).
Fan, L. et al. Exosome-based mitochondrial delivery of circRNA mSCAR alleviates sepsis by orchestrating macrophage activation. Adv. Sci. 10, e2205692 (2023).
Wang, Y. A.-O. et al. Extracellular vesicles from 3D cultured dermal papilla cells improve wound healing via Krüppel-like factor 4/vascular endothelial growth factor A-driven angiogenesis. Burns Trauma 30, tkad034 (2023).
Wen, Y. et al. Cell-derived nanovesicles prepared by membrane extrusion are good substitutes for natural extracellular vesicles. Extracell. Vesicle 1, 100004 (2022).
Jang, S. C. et al. Bioinspired exosome-mimetic nanovesicles for targeted delivery of chemotherapeutics to malignant tumors. ACS Nano 7, 7698–7710 (2013).
Lai, J., Huang, C., Guo, Y. & Rao, L. Engineered extracellular vesicles and their mimics in cardiovascular diseases. J. Control. Release 347, 27–43 (2022).
Gong, H. et al. Nanomaterial biointerfacing via mitochondrial membrane coating for targeted detoxification and molecular detection. Nano Lett. 21, 2603–2609 (2021).
Nakayama, T. Suppression of hydroperoxide-induced cytotoxicity by polyphenols. Cancer Res. 54, 1991s–1993s (1994).
Pavlíková, N. Caffeic acid and diseases—mechanisms of action. Int. J. Mol. Sci. 24, 588 (2022).
Chatterjee, S., Anslyn, E. V. & Bandyopadhyay, A. Boronic acid based dynamic click chemistry: recent advances and emergent applications. Chem. Sci. 12, 1585–1599 (2021).
Wang, P., Gong, Q., Hu, J., Li, X. & Zhang, X. Reactive oxygen species (ROS)-responsive prodrugs, probes, and theranostic prodrugs: applications in the ROS-related diseases. J. Med. Chem. 64, 298–325 (2020).
Larcher, A., Lebrun, A., Smietana, M. & Laurencin, D. A multinuclear NMR perspective on the complexation between bisboronic acids and bisbenzoxaboroles withcis-diols. New J. Chem. 42, 2815–2823 (2018).
Meadows, M. K., Roesner, E. K., Lynch, V. M., James, T. D. & Anslyn, E. V. Boronic acid mediated coupling of catechols and N-hydroxylamines: a bioorthogonal reaction to label peptides. Org. Lett. 19, 3179–3182 (2017).
Kolb, H. C., Finn, M. G. F., Sharpless, K. B. & Sharpless, K. B. Click Chemistry: diverse chemical function from a few good reactions. Angew. Chem. Int. Ed. 40, 2004–2021 (2001).
Baker, P. J. et al. Molecular structures that influence the immunomodulatory properties of the lipid A and inner core region oligosaccharides of bacterial lipopolysaccharides. Infect. Immun. 62, 2257–2269 (1994).
Fahy, E. et al. A comprehensive classification system for lipids. J. Lipid Res. 46, 839–861 (2005).
Oprea, T. I. Property distribution of drug-related chemical databases. J. Comput Aided Mol. Des. 14, 251–264 (2000).
Dekant, W., Fujii, K., Shibata, E., Morita, O. & Shimotoyodome, A. Safety assessment of green tea based beverages and dried green tea extracts as nutritional supplements. Toxicol. Lett. 277, 104–108 (2017).
Magnani, C., Isaac, V. L. B., Correa, M. A. & Salgado, H. R. N. Caffeic acid: a review of its potential use in medications and cosmetics. Anal. Methods 6, 3203–3210 (2014).
Gandin, V., Khalkar, P., Braude, J. & Fernandes, A. P. Organic selenium compounds as potential chemotherapeutic agents for improved cancer treatment. Free Radic. Biol. Med. 127, 80–97 (2018).
Ghezzi, M. et al. Polymeric micelles in drug delivery: an insight of the techniques for their characterization and assessment in biorelevant conditions. J. Control. Release 332, 312–336 (2021).
Wacławek, S. et al. Chemistry of persulfates in water and wastewater treatment: a review. Chem. Eng. J. 330, 44–62 (2017).
Wu, X. J. et al. A catalyst-free co-reaction system of long-lasting and intensive chemiluminescence applied to the detection of alkaline phosphatase. Mikrochim. Acta 189, 181 (2022).
Zielonka, J. et al. Mitochondria-targeted triphenylphosphonium-based compounds: syntheses, mechanisms of action, and therapeutic and diagnostic applications. Chem. Rev. 117, 10043–10120 (2017).
Bock, F. A.-O. & Tait, S. A.-O. X. Mitochondria as multifaceted regulators of cell death. Nat. Rev. Mol. Cell Biol. 21, 85–100 (2020).
Giacco, F. & Brownlee, M. Oxidative stress and diabetic complications. Circ. Res 107, 1058–1070 (2010).
Iversen, T.-G., Skotland, T. & Sandvig, K. Endocytosis and intracellular transport of nanoparticles: present knowledge and need for future studies. Nano Today 6, 176–185 (2011).
Leitinger, B. & Hogg, N. The involvement of lipid rafts in the regulation of integrin function. J. Cell Sci. 115, 963–972 (2002).
McMahon, H. T. & Boucrot, E. Molecular mechanism and physiological functions of clathrin-mediated endocytosis. Nat. Rev. Mol. Cell Biol. 12, 517–533 (2011).
Bag, N., Yap, D. H. X. & Wohland, T. Temperature dependence of diffusion in model and live cell membranes characterized by imaging fluorescence correlation spectroscopy. Biochim. Biophysica Acta Biomembr. 1838, 802–813 (2014).
Gao, S. & Hu, J. Mitochondrial fusion: the machineries in and out. Trends Cell Biol. 31, 62–74 (2021).
Jiang, L. et al. Mitochondrion-specific dendritic lipopeptide liposomes for targeted sub-cellular delivery. Nat. Commun. 12, 2390 (2021).
Gao, C. et al. Treatment of atherosclerosis by macrophage-biomimetic nanoparticles via targeted pharmacotherapy and sequestration of proinflammatory cytokines. Nat. Commun. 11, 2622 (2020).
Choi, D. et al. Quantitative proteomic analysis of trypsin-treated extracellular vesicles to identify the real-vesicular proteins. J. Extracell. Vesicles 9, 1757209 (2020).
Acknowledgements
This work was supported by the National Natural Science Foundation of China (Grant No. 82402908 to L.F., Grant No. 82372523 to J.T.H., Grant No. 62475216 to B.P., Grant No. 82272261 to X.K.Y.), Key Research and Development Program of Shaanxi (Grant No. 2024SF-ZDCYL-04-10 to H.G., Grant No. 2024GH-ZDXM-37 to B.P., Grant No. 2022JC-58, 2024SF-ZDCYL-03-26 to X.K.Y.), Shaanxi Province Health Science Research and Innovation Capacity Enhancement Project (Grant No. 2025PT-03 to H.G.).
Author information
Authors and Affiliations
Contributions
L.F. and C.H.Z. collaborated to complete the study and drafted the manuscript. Z.G.X., Z.L.L., and B.Z. assisted with the preparation of nanovesicles. H.L. and J.X.W. assisted with animal experiments. Z.W., J.T.H., and H.G. provided technical help for this study. B.P., N.H.V., and X.K.Y. reviewed and edited the manuscript. All authors discussed the results and implications and commented on the paper.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks Yun Liu and the other anonymous reviewers for their contribution to the peer review of this work. [A peer review file is available].
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Fan, L., Zhang, C., Xu, Z. et al. Hybrid macrophage-mitochondria extracellular vesicles for mitochondrial ROS regulation in diabetic wounds. Nat Commun (2026). https://doi.org/10.1038/s41467-026-69383-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-026-69383-3