Abstract
Chimeric antigen receptor (CAR)-T cell therapy has transformed treatment of relapsed/refractory DLBCL, yet resistance driven by regulatory T cells (Tregs) limits its efficacy. Here we identify Timosaponin AIII (TAIII), a clinical-stage natural product, as an effective modulator of CAR-T function that depletes CAR-Tregs while enhancing effector activity. Mechanistically, TAIII acts as an allosteric A2AR inhibitor by competing with cholesterol, suppressing CREB-dependent FoxP3 transcription and disrupting the A2AR-Treg axis. Ablation of A2AR or Tregs in vitro and in vivo abolishes TAIII activity, confirming specificity. Furthermore, TAIII reduces intratumoral Tregs, increases CD8⁺ T cells infiltration, and potentiates PD-1 blockade in solid tumor models. Importantly, TAIII promotes central memory T-cell formation and enhances CAR-T cytotoxic cytokine secretion. Combining or pretreating CAR-T cells with TAIII markedly improves antitumor efficacy and prevents late relapse across preclinical models. These findings establish TAIII as a combinatorial strategy to deplete CAR-Tregs, enhance CAR-T activity, and extend therapeutic durability.
Similar content being viewed by others
Introduction
CD19 chimeric antigen receptor (CAR) T-cell therapy is an effective treatment for relapsed and refractory B-cell malignancies, but in practical clinical application, approximately 60% of patients eventually experience relapse or resistance1,2,3,4,5. Previous investigations suggest that immunosuppressive molecules and cell subsets are critical factors limiting CAR-T efficacy6. The immunosuppressive tumor microenvironment (ITME), including regulatory T cells (Tregs), myeloid-derived suppressor cells (MDSCs), tumor-associated macrophages (TAMs)), and molecules like hypoxia-driven adenosine and IL-107,8, is a major barrier to CAR-T cell efficacy by disrupting immune function. Additionally, CAR-T cell dysfunction or reduced persistence, marked by diminished cytotoxicity and elevated inhibitory receptor expression, is another significant obstacle. Clinical trials evaluating the correlation between CAR-T cell expansion and therapeutic outcomes found that higher CAR-T cell levels post-infusion did not correspond with tumor burden, suggesting that immunosuppressive molecules or cell subsets may play a crucial role in mediating CAR-T therapy response9,10,11. Nevertheless, the precise mechanisms behind this ITME-mediated CAR-T cell dysfunction remain poorly understood12.
Tregs are crucial for maintaining self-tolerance and immune homeostasis, primarily through the high expression of the transcription factor FoxP3, which is essential for their function13,14,15. Tumor-infiltrating Treg cells (TITRs) are particularly immunosuppressive within the tumor microenvironment, impairing anti-tumor immune responses and thus promoting tumor immune evasion8. Two recent studies have highlighted the role of CAR-Treg cells in mediating CAR-T resistance through comprehensive single-cell profiling. Using single-cell proteomics and transcriptomics, Good et al. demonstrated that higher levels of Helios+FoxP3+ CAR-Treg cells are closely associated with poor clinical outcomes, providing insight into why CAR-T cell expansion in vivo does not always correlate with clinical response16,17. Based on single-cell transcriptome and TCR sequencing data, Haradhvala et al.18 analyzed samples from 32 patients treated with CAR-T cell infusion and found that high levels of CAR-Tregs led to clinical non-response, and the addition of just 5% of CAR-Tregs in CAR-T cell products was sufficient to reduce conventional CAR-T (CAR-Tconv) expansion and cause relapse in JeKo-1 lymphoma-engrafted NSG mice. These findings reveal the immunosuppressive impact of CAR-Tregs on CAR-T therapy and suggest that an effective Treg-depleting strategy could optimize CAR-T efficacy19.
Current strategies under development mainly include immune checkpoint inhibitors (ICI) and targeted drug combinations, such as CpG oligonucleotide combined with low-dose anti-OX40/CTLA-420 treatment, or blocking chemokine pathways like anti-CCR421. Additionally, antibodies targeting Treg cell surface receptors, such as anti-APRIL and anti-CD122, have been explored. These neutralizing monoclonal antibodies (mAbs), often combined with ICIs, have shown potential in restoring immune tolerance in animal models22,23. However, no clinically effective strategy for selectively depleting CAR-Tregs to enhance CAR-T efficacy has been developed. One significant limitation is that anti-Treg antibodies lack selective targeting, leading to unintended depletion of antitumor effector T-cell populations or adverse side effects24. Furthermore, certain strategies show modest or marginal effects due to the limitations of monotherapy or inadequate drug delivery approaches24. Therefore, novel approaches to improve the specificity of Treg targeting and enhance anti-tumor efficacy are still under development.
Natural products are characterized by their structural diversity and abundance of bioactive compounds, making them valuable sources for drug discovery and lead compound development in the treatment of major diseases, contributing significantly to human health. Compared to synthetic compounds, natural products often exhibit better bioavailability, biodegradability and safety profiles25. Many successful cases have shown the discovery of lead drugs from natural product extracts, which are subsequently optimized into more effective drugs. With the growing appreciation for functional assays and phenotypic screening, there has been a revitalized interest in natural product-based drug discovery26,27. The combination of CAR-T therapy with small-molecule immunomodulators offers advantages such as high efficiency, flexibility and personalization. Recent studies suggest that using small-molecule immunomodulators to eliminate Tregs and enhance CAR-T cytotoxicity against tumor cells may be a promising strategy to overcome therapy resistance.
To identify potential inhibitors of Treg function, we established a Treg functional assay system and conducted high-throughput screening of an in-house compound library containing over 3000 compounds. This led to the identification of a natural steroidal saponin, Timosaponin AIII (TAIII), which is currently in clinical trials as a safe and effective anti-wrinkle agent due to its anti-inflammatory properties (KCT0002223)28, which also demonstrated inhibitory effects on Tregs. TAIII is derived from Anemarrhena asphodeloides Bunge, a traditional Chinese medicinal herb29. Previous studies suggest that TAIII regulates multiple signal pathways30, including NF-κB, AKT/mTOR, and ERK1/2/MAPKs, exhibiting both anti-inflammatory and anti-tumor activities. Research has shown that TAIII can restore the balance between Treg and Th17 cells in mice with TNBS-induced colitis31. However, the precise mechanisms underlying TAIII’s effects on human T cells and supporting evidence remain unclear.
In this study, we found that TAIII allosterically targets adenosine receptor A2(A2AR) in human T or CAR-T cells, blocking adenosine-mediated immunosuppressive signals by down-regulating key transcriptional markers, including FoxP3 and CTLA-4, and inhibiting Treg recruitment and cholesterol metabolism pathways, thereby reducing the CAR-Treg population. Genetic depletion of A2AR in both Treg and CAR-T cells, along with Treg depletion in CAR-T cells in vitro, and the use of a Treg-depletion CAR-T therapy model (Nalm6-Luc) in vivo, led to the loss of TAIII activity, further reinforcing its selective targeting of the A2AR-Treg axis. By disrupting the adenosine-induced immunosuppressive microenvironment, TAIII significantly suppresses tumor growth and enhances the efficacy of anti-PD-1 immunotherapy by reducing intratumoral Tregs. Importantly, pretreatment or combination with TAIII enhances CAR-T cell expansion, persistence, and antitumor activity, helping to overcome relapses across various tumor models. These findings establish TAIII as a potent CAR-T cell adjuvant and provide evidence that this natural product reduces Tregs, thereby improving CAR-T cell function and preventing therapy resistance.
Results
High-throughput screening identified Timosaponin AIII as a Tregs inhibitor
Given that Treg percentage and function are crucial for CAR-T treatment outcomes, the transcription factor FoxP3a serves as the most important functional marker of Tregs by inhibiting the transcription of genes such as IL-213,14,15. To establish a high-throughput screening platform for Foxp3-mediated Il-2 inhibition, we introduced the human IL-2 promoter region (−326 to +145, 473 bp) containing a FoxP3a (FoxP3) binding site into the Lenti-PGL4 reporter vector. This system was packaged into lentivirus, and the IL-2 promoter-firefly luciferase (Fluc) reporter with a puromycin resistance cassette was transduced into Jurkat T cells. After puromycin selection, monoclonal cells were isolated and tested for luciferase activity upon TCR stimulation. The best-performing clone was selected, and a lentiviral construct for FoxP3a overexpression, containing a BSD resistance cassette, was introduced. Following another round of TCR stimulation and selection, the final monoclonal cell line with optimal performance was chosen, allowing Treg function to be evaluated by Fluc fluorescence intensity (Fig. 1a).
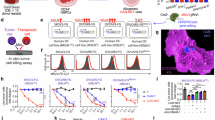
a Schematic illustrating the generation of the high-throughput screening platform for Foxp3-mediated Il-2 inhibition and the inhibitor screening workflow. b Treg functional inhibitor screening identified Timosaponin AIII (TAIII) as a “hit”. c Human PBMCs were activated through TCR stimulation and treated with 1 μM of the indicated compounds for 48 h. IL-2 secretion levels were measured by ELISA (upper panel). Cell viability was measured using the CellTiter-Glo assay (lower panel). d Chemical structure of TAIII. e FoxP3a-IL-2-Fluc-reporter were generated by introducing IL-2-promoter-Fluc-reporter that containing a FoxP3 binding site, into Jurkat T cells, the monoclonal cells were picked out post-puromycin selection, followed delivery of a FoxP3a over-expression lentiviral construct containing a BSD resistance cassette. Cells were treated with or without (w/o) TAIII, the target effect towards Foxp3a-mediated IL-2 suppression were determined by luciferase assay. Data are presented as mean ± SD (n = 3–4 biological replicates); ordinary one-way ANOVA with Dunnett’s test. f TAIII impairs Treg differentiation and functional marker expression in a dose-dependent manner. Human CD4+ Naïve T cells were isolated from umbilical cord blood of healthy donors, and cultured under iTreg polarization conditions for 5 days. iTreg cells were then subjected to TAIII treatment, mRNA levels of indicated genes were assessed post-16 h by qRT-PCR. Data are presented as mean ± SD (n = 3 biological replicates); two-way ANOVA with Dunnett’s test. g–h Naïve human CD4+ T cells were obtained and differentiated into the iTreg lineage as in e. Expression levels of Foxp3 were assessed post-72 h treatment w/o TAIII by flow cytometry. Data are presented as mean ± SD Data are presented as mean ± SD (n = 3 biological replicates); ordinary one-way ANOVA with Dunnett’s test. Source data are provided as a Source Data file.
To identify potential Treg inhibitors, we conducted high-throughput screening of an in-house natural product and FDA-approved drug library (containing over 3000 compounds). The Fluc intensity was normalized to cell viability after 16-hour treatment (Fig. 1a). During the initial screening, over 50 compounds, including Timosaponin AIII (TAIII), exhibited significant modulation of the FOXP3–IL-2 axis (Fig. 1b). To prioritize undisclosed candidates, previously reported compounds such as HDAC inhibitors were excluded through literature and patent database review. The top 10 candidates were subsequently subjected to secondary screening, including single-dose testing in human PBMCs (Fig. 1c, upper panel), with careful consideration of both potency and toxicity. Toxicity was assessed by evaluating the viability of human PBMCs as a surrogate for off-target cytotoxicity (Fig. 1c, lower panel). From this process, TAIII, a natural product derived from Anemarrhena asphodeloides Bunge and also a traditional Chinese medicine, emerged as the lead candidate (Fig. 1d), demonstrating robust dose-dependent efficacy and a favorable safety profile. TAIII significantly reversed FoxP3-mediated IL-2 transcription inhibition in a dose-dependent manner (Fig. 1e). TAIII, a steroidal saponin, has been primarily reported for its anti-cancer, anti-inflammatory, and anti-thrombotic properties30,31. In inflammation models, TAIII reduces cytokines such as IL-6, IL-1β, and TNF-α. However, its role in activating IL-2 or inhibiting human Tregs remains largely unexplored, as do the molecular mechanisms underlying Treg proportion and function.
To verify TAIII’s effect on human Tregs, we isolated human CD4+ naïve T cells and cultured them under iTreg-polarizing conditions. TAIII significantly impaired Treg differentiation and reduced expression of functional markers (FoxP3, CD25, CTLA4) in a dose-dependent manner (Fig. 1f). Similar results were observed when surveying the proportion of FoxP3+ iTreg cells during late differentiation stages (days 5–8) (Fig. 1g, h). These findings suggest that TAIII is a previously unrecognized natural product that inhibits Tregs and reduces their proportion.
TAIII enhances the antitumor efficacy of CAR-T cells by eliminating FoxP3+ Treg cells in vitro
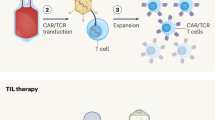
To investigate whether TAIII improves the antitumor efficacy of CAR-T cells, we first generated the CD19 CAR-T by transducing T cells isolated from human peripheral blood mononuclear cells (PBMCs) with lentiviral CAR constructs. We then assessed the baseline T cell phenotypes at the time of CAR-T manufacturing. These included the proportions of CD8, CD4, Tnaive, Tcm, Teff, Temra, and Tregs, assessed by flow cytometry three days post-CAR transduction. T cell subsets were defined as follows: CD45RO⁻CD62L⁺ (Tnaive), CD45RO⁺CD62L⁺ (Tcm), CD45RO⁺CD62L⁻ (Teff), and CD45RO⁻CD62L⁻ (Temra), following established refs. 32,33 (Supplementary Fig. 1a). To evaluate phenotypic changes upon in vitro TAIII exposure, CD19-CAR-T cells were treated with either DMSO or TAIII for 72 hours, followed by flow cytometry analysis. The proportions of CD4⁺ T cells, CD8⁺ T cells and Teff remained largely unchanged, whereas the TAIII-treated group exhibited an increase in Temra cells and a corresponding decrease in Tnaive cells. Notably, TAIII treatment led to a significant reduction (~40%) in Treg proportions (Supplementary Fig. 1b, c, Fig. 2a), suggesting that TAIII may enhance CAR-T efficacy by attenuating immunosuppressive Treg populations.
a CD19 CAR-T cells were generated from human T cells as described in the Methods. After expansion, CAR-T cells were treated with DMSO or TAIII for 72 h. The proportion of FoxP3+ Treg in CD4+ T was then analyzed by flow cytometry. Data are presented as mean ± SD (n = 3 biological replicates); two-sided unpaired t-test. b–c CAR-T and Untransduced T cells (UNT) cells were treated with TAIII (0, 0.5, 1, 2 µM) for 24 and 72 h under non-stimulatory conditions (without tumor cells). T cell proliferation and cell viability/apoptosis were assessed using CellTiter-Glo assays and flow cytometry (PI/Annexin V/7-AAD staining). Data are presented as mean ± SD (n = 3 biological replicates); two-sided unpaired t-test or ordinary one-way ANOVA with Dunnett’s test. CAR-T cells were co-cultured with Raji-Luc (d) or Nalm6-Luc (e) cells at effector-to-target (E:T) ratios of 1:2 or 1:4 under indicated treatments. Cytotoxicity was measured by residual luciferase activity, and IFN-γ, IL-2, and TNF-α levels were determined by ELISA. UNT cells were included as negative controls; Data are presented as mean ± SD (n = 3 biological replicates); two-way ANOVA with Šídák’s multiple comparisons test. f Real-time cytotoxicity of CAR-T cells co-cultured with Raji cells was monitored over 36 h using Incucyte® cytolight red and annexin V staining; Data are presented as mean ± SD (n = 3 biological replicates); two-way ANOVA with Šídák’s multiple comparisons test. g IFN-γ and TNF-α protein levels in CAR-T–Raji co-cultures after 16 h were measured by ELISA; Data are presented as mean ± SD (n = 3 biological replicates); two-sided unpaired t-test. h FoxP3a (FoxP3) mRNA levels in CAR-T–Raji co-cultures were determined by qRT-PCR. Data are presented as mean ± SD from independent experiments (n = 3–4 biological replicates); two-sided unpaired t-test.
To directly assess the effects of TAIII on untransduced T cells (UNT) and CAR-T cells in the absence of tumor antigen stimulation, we treated these cells with TAIII under non-stimulatory conditions and measured their proliferation, viability, and apoptosis. As shown in revised Fig. 2d–e, TAIII treatment for 24 and 72 h did not significantly affect the proliferation or viability of either cell type, indicating that TAIII’s effects are not due to nonspecific T cell stimulation, but rather are dependent on tumor antigen presence and Treg modulation (Fig. 2b, c).
Given these phenotypic alterations, we next evaluated the functional impact of TAIII on CAR-T cell-mediated tumor cell killing in a co-culture cytotoxicity assay. CAR-T cells were co-cultured with Raji or Nalm6 cells at effector-to-target (E:T) ratios of 1:2 and 1:4, with or without TAIII treatments. TAIII significantly enhanced CAR-T cell-mediated killing of Raji or Nalm6 cells in a dose-dependent manner compared to the CAR-T-only control (Fig. 2d, e). Specifically, TAIII increased the cytotoxicity of CAR-T cells, killing approximately 80% of target Nalm6 cells (Fig. 2e). Additionally, we observed a significant upregulation of T-cell effector cytokine secretion, including IFN-γ, IL-2, and TNF-α, in the TAIII-treated CAR-T group (Fig. 2d, e).
To further investigate the kinetics of TAIII’s effect, CAR-T-cell-mediated killing was monitored over time via immunofluorescence every 2 h for 36 h using the Incucyte® cytolight in a co-culture cytotoxicity assay (E:T = 1:2 or 1:4). Similar results showed that TAIII significantly enhanced CD19 CAR-T activity against Raji cells in a time-dependent manner, with effects observed as early as 4 h (Fig. 2f).
Next, we investigated whether TAIII enhances CAR-T cell cytotoxicity by modulating Tregs. In co-cultures of CAR-T cells with or without TAIII post-activation with Raji (E:T = 1:1), we observed that T-cell effector cytokine secretion, including IFN-γ and TNF-α, was significantly upregulated in the TAIII-treated CAR-T group (Fig. 2g). Moreover, the expression of FoxP3, the key Treg-associated transcription factor, was significantly downregulated (Fig. 2h), consistent with the reduction observed in TAIII-treated CAR-T cells cultured alone (Supplementary Fig. 1b, c, Fig. 2a). These results suggest that TAIII reduces the proportion of FoxP3+ CAR-Treg cells and enhances CAR-T cell cytotoxicity by targeting Tregs.
To specifically evaluate whether TAIII exerts its effects through Treg modulation, we generated Treg-depleted CAR-T (ΔTreg-CAR-T) cells by sorting CD4+CD25+CD127low cells from human PBMCs, reducing their frequency to 1.28% (Supplementary Fig. 2a, b). Notably, flow cytometric analysis was performed 72 h after CAR transduction to capture the dynamic expansion of CAR-T subsets over time, rather than immediately following sorting. Additionally, the Treg depletion strategy targeted <5% of CD4⁺CD25⁺CD127low cells and did not significantly alter the overall CD8/CD4 ratio, reflecting differential expansion post-depletion rather than a loss of CD4⁺ effector cells (Supplementary Fig. 2c). The resulting CAR-T cells were co-cultured with Nalm6-Luc cells for 24 h, and luciferase activity was measured to assess target cell killing. At various E:T ratios, Treg depletion enhanced the short-term killing effect of CAR-T cells, confirming that Tregs negatively influence CAR-T cell function (Supplementary Fig. 2d). This highlights the critical role of CAR-Tregs in modulating CAR-T-mediated cytotoxicity. Purified CD4+ or CD8+ ΔTreg-CAR-T cells were co-cultured with Raji-Luc cells for 24 h. As previously observed, CD8⁺ CAR-T cells were primarily responsible for short-term cytotoxicity11,34. Notably, TAIII treatment did not alter the killing capacity of ΔTreg-CAR-T cells, regardless of subset (Supplementary Fig. 2e–g), indicating that TAIII’s functional enhancement requires Treg presence.
This was further supported by parallel experiments using parental CAR-T cells (5.18% Tregs), in which TAIII significantly enhanced cytotoxicity (Supplementary Fig. 2e), suggesting that TAIII’s functional enhancement is dependent on the presence of Tregs. ELISA analysis revealed no significant differences in IL-2, IFNγ, or TNFα secretion between TAIII-treated and DMSO-treated ΔTreg- or CD4⁺ ΔTreg-CAR-T cells. While TAIII modestly increased cytokine secretion in CD8⁺ ΔTreg-CAR-T cells, this was insufficient to enhance cytotoxic activity (Supplementary Fig. 2g, h).
Collectively, these results demonstrate that TAIII potentiates CAR-T cell efficacy primarily by alleviating Treg-mediated suppression, rather than through direct effects on Teff cells. This targeted mechanism offers therapeutic advantages by preserving intrinsic T cell function while selectively countering immunosuppressive elements within the CAR-T population.
TAIII is a selective allosteric inhibitor of A2AR
To explore the intrinsic mechanism underlying TAIII-mediated Treg inhibition, we sought to identify the direct targets of TAIII using reverse screening methods. We designed and synthesized a biotinylated TAIII probe (Biotin-TAIII-P) with a photoactivatable group using click chemistry35 (Fig. 3a), incorporating a photosensitive fishhook structure for proximity labeling in combination with mass spectrometry (LC-MS) (Supplementary Fig. 3a). This led to the identification of adenosine A2A receptor (A2AR) as a key immunosuppressive target of TAIII (Supplementary Fig. 3b). To further validate this finding, we also used the SwissTargetPrediction online tool, which identified GPCRs as the most prominent class of predicted targets for TAIII. Notably, A2AR (ADORA2A) and A1AR (ADORA1) were identified as the top candidates, reinforcing A2AR as a promising target (Supplementary Fig. 3c–d). Adenosine receptors are members of the rhodopsin-like family of G protein-coupled receptors (GPCRs), which consist of four subtypes: A1R, A2AR, A2BR, and A3R. Each subtype is coupled to distinct intracellular small G proteins, mediating different signaling pathways. To further investigate TAIII’s selectivity, we conducted microscale thermophoresis assays using EGFP-fused adenosine receptor constructs. These assays compared the binding affinity of TAIII for A2AR with that for other adenosine receptor subtypes. The results revealed that TAIII displays high selectivity for A2AR, with negligible or no binding to other receptors and only a modest interaction with A2BR (Supplementary Fig. 3e). A2AR is a well-known immune checkpoint expressed on various immune cells, particularly T cells. Studies show that A2AR plays a critical role in the tumor immunosuppressive microenvironment and promotes tumor immune escape, making it a therapeutic target in immunotherapy. Although its immunosuppressive function via Treg has been established, the molecular mechanisms regulating the activity of Treg remains largely unknown. Moreover, it is unknown whether blocking this signaling pathway improves CAR-T cell manufacturing.
a Photosensitive biotinylated-TAIII (TAIII-P) was generated via click chemistry and used for proximity labeling. b Human T cells isolated from PBMCs were treated with TAIII-P (0–20 μM) for 4 h. Association with A2AR was assessed by avidin-biotin pulldown and western blot (upper), and quantified using ImageJ (lower). Data are presented as mean ± SD from four independent experiments (n = 4 biological replicates); two-way ANOVA with Dunnett’s test. c–d Competition assay in cell lysates pretreated with TAIII, followed by TAIII-P pulldown. Relative A2AR levels were quantified. Data are presented as mean ± SD (n = 3 biological replicates); two-way ANOVA with Dunnett’s test. e 293 T cells were co-transfected with A2AR and a CREB luciferase reporter, followed by treatment with the indicated compounds. CREB transcriptional activity was measured using a luciferase assay. NECA was not included, as A2AR overexpression alone was sufficient to activate the CREB reporter. f 293 T cells transfected with A2AR were incubated with NECA (0.1 μM) and TAIII or AZD4635 for 30 min. cAMP levels were determined by LANCE assay; fluorescence ratios (615/665 nm) were proportional to cAMP. Blank wells were negative controls. Data are presented as mean ± SD from four independent experiments (n = 4 biological replicates); ordinary one-way ANOVA with Dunnett’s test. g 293 T cells transfected with or without A2AR were treated with indicated compounds; cAMP levels were measured by LANCE assay. Data are presented as mean ± SD (n = 3 biological replicates); two-way ANOVA with Dunnett’s test. h Predicted mode of binding of TAIII to A2AR based upon molecular modeling (PDB ID: 4EIY). i–j CREB-Fluc reporters with wild-type or mutant A2AR residues were used to assess the contribution of three residues to TAIII binding (i) and dose-dependent effects (j). Data are presented as mean ± SD (n = 3 biological replicates); two-way ANOVA with Dunnett’s test.
We then confirmed the binding of TAIII to A2AR. Since 293 T cells express low levels of A2AR, we generated the A2AR-overexprssing 293 T cells (293T-A2AR-OE) stably expressing A2AR-GFP. Using a cellular thermal shift assay (CETSA), we investigated the effect of TAIII on A2AR protein stability across different temperatures. As expected, TAIII robustly increased the thermal stability of A2AR (Supplementary Fig. 3f). Moreover, Microscale Thermophoresis assay further confirmed TAIII-A2AR binding. AZD4635, an A2AR inhibitor currently in phase II clinical trials, was used as a positive control (Supplementary Fig. 3g). We then performed a Target engagement assay using biotin-streptavidin pull-down method and demonstrated a dose-dependent interaction between TAIII and A2AR in both overexpression system and primary human T cells (Fig. 3b, Supplementary Fig. 3h). To further confirm the target engagement of A2AR, we performed a competition assay with Biotin-TAIII-P after 4 h of TAIII treatment, and observed that 5 μM TAIII labeled ~50% of A2AR (Fig. 3c, d), confirming A2AR as a direct target of TAIII.
Given that A1R and A3R couple to Gi proteins, while A2AR and A2BR couple to Gs proteins. A2AR activation by ligand binding triggers Gs coupling, activating adenylate cyclase (AC) to produce cAMP and initiates the classic cAMP-PKA-CREB signaling pathway (Supplementary Fig. 4a), which mediates various immunosuppressive responses36,37. To evaluate the functional selectivity of TAIII among the adenosine receptor subtypes, we constructed expression vectors for A1R, A2AR, A2BR, and A3R and over-expressed them in 293 T cells. Using the LANCE cAMP assay, we measured intracellular cAMP levels following A2AR activation with 0.1 μM of the adenosine agonist 5-(N-ethylcarboxamido) adenosine (NECA). The results demonstrated that TAIII exhibited high selectivity for A2AR, with minimal or no effects on the other subtypes and only a modest effect on A2BR (Supplementary Fig. 4b), consistent with previous findings on its binding selectivity (Supplementary Fig. 3e). Considering that A2BR has a substantially lower sensitivity to adenosine compared to A2AR, and its expression is particularly sparse on T cells, especially Tregs, A2BR was not prioritized as a key factor in our analysis. We then compared TAIII’s activity with the phase II A2AR antagonist AZD4635 using both CREB reporter and LANCE cAMP assays. TAIII displayed comparable potency to AZD4635 across various cell models, with cell viability maintained at all tested concentrations, suggesting that TAIII is likely non-toxic to T cells (Fig. 3e, f). To rule out off-target effects on the A2AR-cAMP/PKA/CREB pathway, we assessed TAIII sensitivity in A2AR-overexpressing cells (A2AR-OE) versus parental cells. TAIII exhibited greater sensitivity in A2AR-OE cells, with potency comparable to other A2AR antagonists (Fig. 3g). Taken together, these findings suggest that TAIII is a selective A2AR inhibitor.
To explore TAIII’s binding mode to A2AR, we utilized computer-aided structural analysis to investigate its interaction within the A2AR complex (PDB ID: 4EIY) (Fig. 3h). Studies show that the cholesterol-sensitive motifs (CCM) in the transmembrane region of A2AR are highly conserved. The cholesterol content in the cell membrane modulates the ligand-binding pocket of A2AR, thus affecting its function. Cholesterol depletion or CCM mutations disrupt A2AR structure, impairing orthosteric ligand binding and downstream signaling38,39. As a steroidal saponin, the core structure of TAIII resembles cholesterol and cholesterol replacement with TAIII in the liposome bilayer enhances drug delivery efficiency, highlighting their structural similarity40. Given that membrane cholesterol is crucial for A2AR activation38,39, we hypothesized that TAIII might compete with cholesterol to affect A2AR function. Structural modeling analysis showed the polyhydroxyl head of TAIII extends into a polar pocket formed by Q38, W32, Y43 and K122, allowing stable binding. The other hydrophobic moiety aligns with the non-polar region of the cell membrane along the transmembrane helix, consistent with the phospholipid bilayer model structure (Fig. 3h). To validate this hypothesis, we introduced point mutations into three key CCM residues, which have been reported to bind cholesterol38, and investigated their contribution to the binding of A2AR and TAIII by CREB-luciferase reporter assay. Notably, the W129A mutation retained partial activity, which is an important consideration when interpreting the sensitivity of TAIII in these experiments. Compared to wild-type A2AR, all mutations decrease CREB activity and abolish sensitivity to even increasing doses of TAIII (Fig. 3i, j), indicating that TAIII affects A2AR function by competing with cholesterol and binding allosterically to these critical residues.
TAIII activates T cell responses through impairing Treg function in an A2AR-dependent manner
Adenosine suppresses immune cells within the tumor microenvironment by inhibiting T cell activation and cytotoxic function41,42,43. Furthermore, as a significant mediator of Treg function, extracellular adenosine contributes to the immunoregulatory activity of Tregs44,45. To evaluate the efficacy of TAIII in enhancing T cell immune responses through A2AR signaling, we isolated PBMCs from healthy donors and cultured them under pan-T cell conditions with NECA (a potent adenosine agonist) or TAIII. Transcriptomic analysis (bulk RNA-seq) of T cells revealed that in the presence of NECA, TAIII treatment significantly upregulated immune activation genes, including TNF, GZMB, IFN-γ and IL-2, while downregulating immunosuppressive genes, such as FoxP3, IKZF2 (Helios), IKZF4 (Eos) and CCR8 (Fig. 4a). Additionally, it enriched immune suppression-related genes and pathways in Tregs, as shown by Reactome pathway enrichment analysis (Supplementary Fig. 5a). To validate these findings, we conducted ELISA and qRT-PCR, demonstrating that TAIII effectively counteracted NECA-mediated suppression of IL-2 and IFN-γ expression, enhancing T cell activation. Moreover, TAIII dose-dependently reduced FoxP3 transcription in T cells, showing greater potency than AZD4635 (Fig. 4b–c, Supplementary Fig. 5b, c). Similar results were observed when evaluating the proportion of FoxP3+ iTreg cells during differentiation. NECA (5 μM) upregulated Treg differentiation and functional markers (FoxP3, CTLA4, CD25, and TGF-β), which were significantly suppressed by TAIII treatment (Fig. 4d, Supplementary Fig. 5d).
a Human PBMCs (1 × 10⁶) were activated with anti-CD3/CD28 beads for 4 days, then treated with NECA ± TAIII for 24 h. Bulk RNA sequencing was performed, and a heatmap displays selected mRNAs and surface markers of Treg and Teff subsets. b PBMCs were stimulated with CD3/CD28 beads and treated with indicated compounds for 48 h. IFN-γ and IL-2 in supernatants were measured by ELISA. Data represent mean ± SEM of three independent experiments, each in triplicate; analyzed by ordinary one-way ANOVA with Dunnett’s test. c T cells were generated as in (a). IFN-γ, IL-2, and FoxP3 transcription (c) and FoxP3 expression during 10-day induced Treg (iTreg) differentiation (d) were determined by qRT-PCR. Data are presented as mean ± SD (n = 3 biological replicates); ordinary one-way ANOVA with Dunnett’s test. e–f Human CD4⁺ naive T cells were skewed to Tregs for 7 days. Suppressive function was assessed by co-culture with CFSE-labeled responder Teff cells; CFSE dilution in CD4⁺CFSE⁺ Teff cells was analyzed by flow cytometry to determine the percentage of undivided Teff cells. Data are presented as mean ± SD (n = 3 biological replicates); ordinary one-way ANOVA with Dunnett’s test. g–h iTreg cells (4-day differentiation) were transduced with shCK or shA2AR constructs (shA2AR-2, -3), and mRNA levels of indicated genes, including FoxP3, were measured by qRT-PCR. Data are presented as mean ± SD (n = 3 biological replicates); One-way ANOVA with Dunnett’s test. i iTreg cells were generated and the recruitment change of CREB on FoxP3a (FoxP3) promoter w/o TAIII treatment was confirmed by CUT & RUN assay. Data are presented as mean ± SD (n = 3 biological replicates); ordinary one-way ANOVA with Dunnett’s test.
Furthermore, we demonstrate that TAIII significantly prevented NECA-mediated immunosuppressive effects of Tregs on effector T cells (Teffs) (Fig. 4e, f, Supplementary Fig. 5e). To assess the direct effects of NECA and TAIII on Teff cell proliferation in the absence of Tregs, we performed CFSE dilution assays. CFSE-labeled Teff cells were cultured with or without NECA or TAIII, and proliferation was measured by CFSE dilution. As shown in Supplementary Fig. 5g, neither NECA nor TAIII significantly affected Teff proliferation under Treg-depleted conditions. These findings suggest that the effects of TAIII on Teff cells in the presence of Tregs are likely mediated through Treg modulation, rather than direct modulation of Teff proliferative capacity. Lentiviral delivery of A2AR-silencing shRNA into primary human iTregs markedly reduced FoxP3 protein levels and increased IL-2 transcription, while non-targeting controls showed no effect (Fig. 4g). To exclude off-target effects, we treated A2AR-depleted Tregs with TAIII and found that TAIII-mediated FoxP3 suppression and cAMP production were significantly attenuated by A2AR depletion, as confirmed by qRT-PCR and LANCE cAMP assays, suggesting that TAIII specifically targets A2AR to regulate FoxP3+ Tregs (Fig. 4h, Supplementary Fig. 5f).
To investigate the mechanism underlying TAIII-mediated FoxP3 transcriptional inhibition, a CUT & RUN assay revealed a robust reduction in CREB occupancy at the FoxP3-CNS-2 promoter region in human iTregs (Fig. 4i), confirming that TAIII inhibits FoxP3+ Tregs and enhances T cell activity through A2AR signaling blockade.
TAIII improves CAR-T cell antitumor activity through blocking A2AR in vitro
To determine whether TAIII improves CAR-T function through A2AR signaling, we performed co-culture cytotoxicity assay (E: T = 1: 2 or 1: 4 in Fig. 5, E: T = 1: 1 to another donor in Supplementary Fig. 6a, b). NECA impaired CAR-T cytotoxicity by increasing of FoxP3+ CAR-Tregs, but TAIII restored cytotoxic function of NECA-treated CAR-T cells against Nalm-6 or Raji cells and upregulated effector cytokines, including IL-2, IFN-γ and TNF-α (Fig. 5a–c, Supplementary Fig. 6a, b). Given the importance of the proportion of CAR-Tregs in determining patient response and outcome to CAR-T therapy17,18, and TAIII’s ability to impair Treg function and differentiation, we then sought to investigate whether TAIII reduces FoxP3+ CAR-Tregs through A2AR signaling. In co-cultures of CAR-T cells and Raji cells in media with or without TAIII, the levels of FoxP3 and the frequency of FoxP3+ Tregs were significantly upregulated by NECA. Importantly, these effects were completely reversed by TAIII treatment without affecting the proportions of total CD4+ and cytotoxic CD8+ T cells (Fig. 5d, Supplementary Fig. 6c). This selective modulation, which aligns with our previous observations (Supplementary Fig. 1), demonstrates TAIII’s target specificity. These findings suggest that TAIII enhances the cytotoxicity of CAR-T cells by blocking A2AR signaling.
a CD19 CAR-T cells were generated as in (Fig. 2) and co-cultured with Raji-Luc or Nalm6-Luc cells under indicated conditions for 24 h; the CD19 levels were assessed by measuring the luciferase signal. Data represent pooled biological replicates; Data are presented as SD (n = 3 biological replicates); two-way ANOVA with Tukey’s test. b–c CAR-T cells from different donors were co-cultured with Raji-Luc or Nalm6-Luc cells under indicated treatments. IFN-γ, IL-2, and TNF-α in supernatants were measured by ELISA. Data are presented as mean ± SD (n = 3 biological replicates); ordinary one-way ANOVA or two-way ANOVA with Dunnett’s test. d CD19 CAR-T cells were co-cultured with Raji cells; FoxP3 mRNA levels were determined by qRT-PCR. Data are presented as mean ± SD (n = 3 biological replicates); ordinary one-way ANOVA with Dunnett’s test. e Effects of TAIII on central memory T cells (CD62L⁺CD45RO⁺, Tcm) were assessed after 48 h co-culture with Raji cells at E:T ratios of 1:1, 1:2, or 1:4 by flow cytometry. Data are presented as mean ± SD (n = 3 biological replicates); two-way ANOVA with Dunnett’s test. f A2AR knockdown (KD) CD19-CAR-T cells were generated via shRNA transduction (GFP⁺), and knockdown efficiency was confirmed by qRT-PCR. Data are presented as mean ± SD (n = 3 biological replicates); two-sided unpaired t-test. g Intracellular cAMP levels in A2AR-KD CAR-T cells were measured to assess TAIII-mediated inhibition of A2AR signaling; Two-way ANOVA with Šídák’s multiple comparisons test. h–i A2AR-KD, parental CD19-CAR-T, and UNT cells were co-cultured with Nalm6-Luc cells for 24 h. Cytotoxicity was measured by residual luciferase activity at E:T ratios of 1:1 and 1:2 (normalized to Nalm6-only controls), and IL-2 secretion was quantified by ELISA at E:T = 1:1. Data are presented as mean ± SD (n = 3 biological replicates); two-way ANOVA or ordinary one-way ANOVA with Tukey’s test.
Give that central memory T cells (Tcm) not only exhibit anti-tumor activity but also prevent recurrence46,47, we further explored the impact of TAIII on Tcm populations (CD62L+CD45RO+) using a co-culture and FACS assay (E:T = 1:1, 1:2 or 1:4). We observed that NECA stimulation robustly reduced the proportion of Tcm cells, while TAIII treatment completely restored Tcm levels across all conditions (Fig. 5e, Supplementary Fig. 6d).
To validate these findings, we conducted single-cell sequencing (scRNA-seq) using 10× Genomics on CAR-T only or co-culture system, with or without TAIII treatment. By clustering and quantifying the proportions of B (Raji) and T (CAR-T) cells, we observed that TAIII robustly enhanced Raji cell (B cell subset) killing (E:T = 1:1) (Supplementary Fig. 7a), consistent with our previous results. By re-clustering the combined T cell single-cell data, we isolated CD4+ T cells and further identified a FOXP3high CD4+ CTLA+ Treg subset (Supplementary Fig. 7b). In the co-culture condition, the proportion of this Treg subset within CD4⁺ T cells decreased by >40% upon TAIII treatment. Likewise, in the CAR-T–only group, the FOXP3highCD4⁺CTLA4⁺ Treg cluster and A2AR⁺CD4⁺ Tregs were both markedly reduced (>40%) following TAIII treatment, underscoring the compound’s consistent suppressive effect on Treg populations (Supplementary Fig. 7c, d). These findings support the modulatory effect of TAIII on Treg populations in the context of NECA stimulation.
Notably, scRNA-seq analysis revealed a significant shift in cytotoxic CD8+ T cells. In CAR-T/Raji co-cultures, CD8+ CAR-T cells exhibited enhanced cytotoxicity after co-culture with tumor cells, which was further amplified in the TAIII-treated group. Differences in cytotoxicity were observed between key cytotoxic subsets, CD8+ GZMB+ Tex (Exhausted T cells) and CD8+ GZMA+ Tem. CellChat analysis revealed the strongest interactions between these subsets and Tregs (Supplementary Fig. 7e–f), suggesting that this increase is a secondary effect resulting from the reduction in Tregs. Additionally, TAIII treatment significantly upregulated the expression of IFNγ and TNFα (Supplementary Fig. 7g), reinforcing our hypothesis that TAIII enhances CAR-T cytotoxicity via Treg modulation, indirectly affecting CD8+ T cells.
Furthermore, bulk RNA-seq results showed that TAIII treatment counteracted NECA’s effects by modulating T cell proliferation and activation, cytotoxic cytokines and Treg immune suppression-related genes and pathways, as shown by Reactome Pathway enrichment analysis (Supplementary Fig. 7h). These findings align with our observations in T cells (Supplementary Fig. 5a). Importantly, TAIII treatment significantly counteracted the effects of NECA by upregulating TNF expression to enhance the T cell immune response, while downregulating the transcription of Treg functional markers, such as FoxP3, CTLA4, and CD25, in CAR-T cells, suggesting resistance to adenosine-mediated transcriptional changes (Supplementary Fig. 7i-j). These results were consistent with our previous T cell data. We also observed significant enrichment of fatty acid metabolism pathways, particularly cholesterol metabolism, following TAIII treatment (Supplementary Fig. 7k), consistent with TAIII’s role in regulating lipid metabolism40,48. Given that membrane cholesterol homeostasis regulates A2AR activity and is essential for Treg stability and function39,49, and considering TAIII’s ability to compete with cholesterol, these results suggest that TAIII modulates A2AR activity through both cholesterol metabolism regulation and allosteric binding to A2AR.
To better assess the specificity of TAIII, we replaced NECA with the high-affinity A2AR agonist CGS-21680. In functional assays (e.g., cytotoxicity and cytokine secretion), CGS-21680 induced significant inhibition, validating that our system responds robustly to a known A2AR agonist. This further ensures that the observed effects of TAIII are due to specific A2AR targeting, rather than non-specific receptor interactions (Supplementary Fig. 8a–b). Building on this, we next aimed to confirm that the effects of TAIII are A2AR-dependent and exclude potential off-target effects. To achieve this, we conducted additional experiments using A2AR knockdown (KD) in CAR-T cells. Briefly, CD19-CAR-T cells were transduced with A2AR-targeting shRNA (GFP+) and sorted by FACS. Knockdown efficiency was confirmed both at the protein level via Western blot and at the mRNA level using qRT-PCR (Supplementary Fig. 8c, Fig. 5f). First, we treated A2AR-KD CAR-T cells with TAIII and observed that TAIII no longer modulated A2AR-mediated cAMP production following A2AR knockdown, further confirming the specificity of TAIII for A2AR (Fig. 5g). A2AR-KD CAR-T cells were subsequently co-cultured with Nalm6-Luc cells, and the results demonstrated that A2AR knockdown enhanced CAR-T cell cytotoxicity compared to the SCR control (GFP-). Importantly, TAIII did not further enhance this cytotoxic effect, confirming that TAIII’s action is dependent on A2AR signaling (Fig. 5h). Furthermore, A2AR-KD CAR-T cells exhibited higher IFN-γ and IL-2 secretion but were unresponsive to both NECA and TAIII treatments, further supporting the A2AR dependence of TAIII’s effects (Fig. 5i, Supplementary Fig. 8d, e). These findings align with data from A2AR-KD Tregs, where TAIII had no impact on Treg activity (Fig. 4g, h, Supplementary Fig. 5f), providing strong evidence that A2AR is a critical mediator of TAIII’s effects on both Treg and CAR-T cell function.
Collectively, these results suggest that TAIII plays an important role in enhancing CAR-T cell function by modulating A2AR signaling and may help prevent relapse after CAR-T therapy.
TAIII suppresses tumor growth through reversing A2AR-FoxP3+Treg mediated immunosuppression
To assess the antitumor efficacy of TAIII in vivo, we treated a syngeneic mouse model (C57BL/6 J) inoculated with MC38 cells with 5 mg/kg TAIII administrated intraperitoneally for 22 days (Supplementary Fig. 9a). TAIII demonstrated a high tumor growth inhibition (TGI = 55.9%) compared to the vehicle group, with no apparent adverse effects, as determined by monitoring body weight over time (Supplementary Fig. 9b–e). Importantly, TAIII treatment significantly increased the levels of CD8, CD4 and GZMB, while downregulating FoxP3 levels in tumor tissues (Supplementary Fig. 9f). Furthermore, TAIII significantly upregulated the expression of activation-associated cell surface molecules, such as CD69, on cytotoxic T lymphocytes (CTL) cells in TDLNs (Supplementary Fig. 9g). Additionally, the IHC staining of excised tumors revealed a significant decrease in FoxP3 protein levels and a marked increase in CD8+ T cells, indicating that blocking A2AR signaling with TAIII reduced infiltrating Tregs while simultaneously enhancing CD8+ T cell infiltration in the TAIII treatment group (Supplementary Fig. 9h). Next, we measured cytokine release in both tumor tissues and serum, finding that TAIII significantly increased the secretion of cytotoxic IFN-γ and IL-2 (Supplementary Fig. 9i).
Similar results were observed in a dose-escalation experiment, where doses ranged from 5 mg/kg to 20 mg/kg (once daily, QD) in the MC38 tumor model, with 50 mg/kg of AZD4635 (twice daily, BID) used as a positive control (Fig. 6a). TAIII exhibited dose-dependent tumor growth suppression, achieving a TGI = 50.5% without noticeable body weight loss, and showed higher potency than AZD4635 (TGI = 34.6%) (Fig. 6b–c, Supplementary Fig. 10a). Moreover, immunohistochemistry (IHC) staining of tumor-draining lymph nodes (TDLNs) revealed a robust decrease in FoxP3 protein levels and a reduction in infiltrated Treg cell numbers in a dose-dependent manner (Fig. 6d, Supplementary Fig. 10b), suggesting that TAIII suppresses tumor growth by impairing Foxp3+ Tregs in vivo. Furthermore, TAIII significantly enhanced the secretion of cytotoxic IFN-γ and IL-2 in both tumor tissues and serum (Fig. 6e). Collectively, these results suggest that TAIII suppresses tumor growth in vivo by blocking A2AR-mediated FoxP3+ Treg signaling.
a C57BL/6 J mice were injected subcutaneously with 1 × 106 MC38 cells. Six days later, TAIII (5-20 mg/kg, QD) or AZD4635 (50 mg/kg, BID) was administered intraperitoneally (n = 7–8 mice). Tumor growth over time (b) and tumor growth inhibition (TGI) after 16 days (c) were determined. Data are presented as mean ± SD (n = 7–8 mice); two-way or one-way ANOVA with Dunnett’s test. d Effects of treatments on FoxP3⁺ Tregs in tumor-draining lymph nodes (TDLNs) were measured by IHC, and relative positive area was quantified using ImageJ. Data are presented as mean ± SD (n = 3 mice); ordinary one-way ANOVA with Dunnett’s test. e IFN-γ levels in excised tumors and serum were measured by ELISA. Data are presented as mean ± SD (n = 7–8 mice); ordinary one-way ANOVA with Dunnett’s test. f Combination study: MC38 tumor-bearing mice were treated with isotype control, anti-PD-1 (5 mg/kg, BIW), TAIII (10 mg/kg, QD), or anti-PD-1 + TAIII (combo) for 22 days (n = 6 mice). Tumor size over time (g–h) and tumor growth after 22 days (i) were monitored. Data represent pooled biological replicates; Data are presented as mean ± SD (n = 6 mice); two-way ANOVA with Dunnett’s test (i) or ordinary one-way ANOVA with Tukey’s test (g). IFN-γ (j) and pCREB (k) levels in excised tumors were measured by ELISA and western blot; band intensity was quantified using ImageJ. Data represent pooled biological replicates; Data are presented as mean ± SD (n = 4–6 mice); ordinary one-way ANOVA with Tukey’s test. l The proportion of Tcm cells in tumor-infiltrating lymphocytes (TILs) were assessed by flow cytometry. Data represent pooled biological replicates; Data are presented as mean ± SD (n = 4 mice); ordinary one-way ANOVA with Tukey’s test. m–n Tumor infiltration of Tregs and CD8⁺ T cells was assessed by IHC; relative positive area was quantified using ImageJ (scale bar 20 μm). Data represent 3 mice (3 fields per tumor; n = 9 fields); Data are presented as mean ± SD; one-way ANOVA with Tukey’s test.
A recent study demonstrated that PD-1 blockade expands Tregs in tumors, limiting the efficacy of immunotherapy50. To determine whether TAIII enhances the antitumor activity of PD-1 therapy, we treated MC38 tumor-bearing mice (C57BL/6 J) with isotype control, anti-PD-1 (5 mg/kg, twice weekly, BIW), TAIII alone (10 mg/kg) administrated intraperitoneally, or the combination of TAIII and PD-1 therapy for 22 days (Fig. 6f). TAIII significantly enhanced the efficacy of anti-PD-1 therapy compared to monotherapy, without apparent adverse effects, as evidenced by body weight monitoring (Fig. 6g–i, Supplementary Fig. 10c, d). Moreover, TAIII significantly increased the production of antitumor cytokines IFN-γ and IL-2 in both tumor tissues and serum (Fig. 6j). Similarly, western blotting of excised tumors showed a marked reduction in A2AR-downstream signaling (pCREB) (Fig. 6k, Supplementary Fig. 10e), demonstrating that the observed therapeutic benefits were mediated through A2AR pathway blockade. Although CREB is relatively evenly expressed across different tissues, it is expressed at higher levels in immune cells, reflecting its key role in immune responses (The Human Protein Atlas database). We acknowledge the limitation that differential CREB expression across cell types in the tumor microenvironment could influence the observed changes in pCREB levels. Future studies will address this by analyzing cell-type-specific responses to TAIII and anti-PD-1 treatment.
Flow cytometric analysis of tumor-infiltrating lymphocytes (TILs) revealed a significant increase in the proportion of Tcm cells in the combination therapy group, relative to the anti-PD-1 monotherapy group (Fig. 6l), suggesting that TAIII + anti-PD-1 therapy potentiates T cell responses by promoting Tcm differentiation. Consistent with this, IHC staining demonstrated a marked reduction in FoxP3+ Tregs, along with an increase in CD8+ T cells within TILs, further corroborating the enhanced antitumor efficacy of the combination treatment (Fig. 6m–n).
Taken together, these results highlight the role of TAIII in enhancing the efficacy of PD-1 immunotherapy by reducing intratumoral Tregs through combination treatments.
TAIII prevents relapse after CAR-T therapy in various preclinical models by targeting A2AR-Treg signaling
Given the importance of FoxP3+ CAR-Treg levels in determining prognosis after CAR-T infusion17,18, we analyzed clinical samples from databases of patients who received CAR-T therapy. CD19 CAR-T products were collected pre-infusion from patients with B-lymphoblastic leukemia who experienced either long-term remission (R, over 8 years, n = 25) or no objective response to the therapy (NR, n = 6), and these were analyzed using scRNA-seq (GSE262072). The analysis revealed that the ratios of A2AR+FOXP3+ cells within total CAR-T populations are significantly correlated with the percentage of cytotoxic cells, cytokine production and clinical response, consistent with findings from Good and Haradhvala et al.17,18 (Fig. 7a–b). Specifically, A2AR signaling and Tregs-related pathways, such as NF-κB1, TGF-β1, and the CD8+ T cell-related gene CRTAM (Class-I MHC-restricted T-cell associated molecule)51,52, are closely associated with tumor response following CAR-T infusion (Fig. 7b), positioning A2AR-FoxP3 as a potential biomarker for predicting therapeutic response and suggesting that A2AR blockade by TAIII may enhance CAR-T cell efficacy in patients.
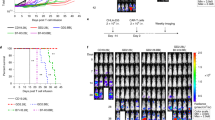
Analysis of CAR-T cell products from patients (GSE262072): proportion of ADORA2A⁺ FOXP3⁺/FOXP3⁺ Tregs (a) and expression of indicated genes (b). Boxes indicate median and interquartile range (IQR); whiskers denote min–max. Each dot represents one patient-derived CAR-T product (n = 31). Two-sided unpaired t-test or Welch’s t-test. c–e NSG mice engrafted with Raji-Luc cells received CAR-T or UNT cells ± TAIII (5 mg/kg); tumor burden was monitored by bioluminescence imaging (d–e). Data are presented as mean ± SD (n = 5 mice); two-way ANOVA with Dunnett’s test. f Survival curves were compared using the log rank Mantel–Cox test. g–h CAR-T persistence and phenotype in bone marrow and peripheral blood were assessed by flow cytometry on the last study day, including CAR⁺, CD62L⁺ T cells, and FoxP3⁺ Tregs. Data are presented as mean ± SD (n = 3–4 mice); two-sided unpaired t-test. i–k NSG mice (n = 6–7) engrafted with Nalm6 cells (3×10⁶) received CAR-T or UNT cells ± TAIII (5 mg/kg). Survival was analyzed by log-rank (Mantel–Cox) test (j) and CAR⁺/FOXP3⁺ proportions in blood and spleen were evaluated on day 4 or 7 post-engraftment; two-sided unpaired t-test (k). l–n Immunocompetent C57BL/6 J mice bearing MC38-mCD19 tumors received lymphodepletion (CTX + FLU) on day 6 and CAR-T or UNT cells ± TAIII (10 mg/kg, daily) on day 7. Tumor growth (m), TGI, and infiltration of FoxP3⁺ Tregs and CD8⁺ T cells were analyzed by IHC (n). Data are presented as mean ± SD (n = 5 mice); two-sided unpaired t-test. o–p NSG mice were subcutaneously injected with Nalm6-Luc cells and treated with CAR-T ± TAIII-pretreated CAR-T cells (1 μM, 72 h). Leukemia burden was assessed by bioluminescence, and CAR⁺ (day 7) /CAR-Treg (day 14) populations in blood and bone marrow were quantified. Data are presented as mean ± SD (n = 3 mice; 6 Treg measurements); two-sided unpaired t-test. q–t Patient-derived CD19 CAR-T cells (n = 8) were co-cultured with Raji-Luc (E:T = 1:2) under indicated treatments for 24 h. Cytotoxicity was quantified by luciferase loss (q–r), cytokine secretion measured by ELISA (s), and FoxP3 expression analyzed by qRT-PCR (t). Data are presented as mean ± SD; two-sided paired (r, s) or unpaired (t) t-tests.
Our findings further demonstrate that TAIII effectively reduces Treg proportions and function by blocking A2AR signaling, thereby potentially enhancing the efficacy of CAR-T cells in preventing tumor relapse. To test this hypothesis, we investigated the effect of TAIII on tumor relapse following CAR-T cell therapy in vivo. Raji-Luc cells were intravenously injected into NSG immunocompromised mice, followed by treatment with CAR-T or UNT cells two days later, with or without TAIII combination treatment (QD), starting at day 3 (post-Raji cells engraftment) through day 58 (Fig. 7c). Both CD19-CAR-T cells alone and the combination group effectively cleared Raji cells within a week. However, relapse occurred after remission in the CAR-T-only group two weeks later, whereas no relapse was observed in the combination group. In the CAR-T only group, 4 out of 5 mice died following the reappearance of lymphoma cells at 8 weeks (Fig. 7d, e, Supplementary Fig. 11a). The combination of TAIII and CAR-T significantly extended mouse survival compared to the vehicle and CAR-T-only groups (Fig. 7f). Moreover, the combination therapy significantly upregulated CAR-T and Tcm cell populations while downregulating FoxP3+ Tregs in both the bone marrow and blood, compared to all other conditions (Fig. 7g, h). These findings suggest that TAIII combination therapy is an effective and affordable therapeutic strategy to prevent relapse after CAR T-cell therapy in lymphoma.
To further validate our findings and demonstrate the broader applicability of TAIII in enhancing CAR-T cell potency, we assessed its effects in a Nalm6 intravenous xenograft model. NSG immunocompromised mice were intravenously injected with 3×10⁶ Nalm6 lymphoma cells (n = 6–7), followed by infusion of 6 × 10⁶ CAR-T cells or UNT controls on day 3. TAIII (5 mg/kg, QD) was co-administered starting on day 3 post-inoculation and continued through day 16 (Fig. 7i). In this model, all control groups ultimately succumbed, whereas CAR-T treatment significantly prolonged survival. Importantly, the combination of CAR-T and TAIII therapy resulted in the longest survival time, with no mice in the CAR-T + TAIII group succumbing to the disease by the end of the experiment, while five out of seven mice (5/7) in the CAR-T only group had died (Fig. 7j). In contrast, TAIII did not prolonged the survival of UNT group, suggesting that its effects are antigen-specific rather than nonspecific. This combination therapy also enhanced CAR-T cell persistence and reduced Treg frequencies (Fig. 7k), with no significant effect on the CD8/CD4 ratio. These findings provide direct evidence of durable, antigen-specific tumor control and improved survival, without apparent toxicity, as indicated by stable body weight (Supplementary Fig. 11b, c).
We further extended our analysis to an immunocompetent MC38-mCD19 solid tumor model, where TAIII synergized with murine CD19-CAR-T therapy (Fig. 7l). C57BL/6 J immunocompetent mice were subcutaneously injected with 1 × 10⁶ MC38-mCD19 cells (n = 5). On day 6, mice were treated with 4.5 mg cyclophosphamide (CTX) and 0.75 mg/200 μL fludarabine (FLU) via intraperitoneal injection for lymphodepletion. On day 7, mice were treated with the optimal dose of CAR-T cells (4 × 10⁶), TAIII (10 mg/kg, daily), or a combination of both. Mice receiving the combination treatment showed more rapid tumor eradication, with a TGI of 90% (Fig. 7m). Tumor microenvironment profiling revealed a significant increase in intratumoral antigen-specific CD8⁺ T cells, accompanied by a reduction in Tregs, providing direct in vivo evidence that TAIII enhances CAR-T efficacy through immune modulation rather than nonspecific activation (Fig. 7n). In addition, we assessed cytokine release in mouse serum and found that TAIII significantly increased the secretion of cytotoxic TNF-α. Flow cytometry analysis also revealed an increase in CD8⁺CD45.1⁺ T cells in the spleen (SP) and bone marrow (BM) of MC38-mCD19-bearing mice on day 6 post-engraftment (Supplementary Fig. 11d–e). These findings indicate that TAIII selectively targets Tregs in vivo, and modulates their population to enhance CAR-T cell expansion and persistence. This likely contributes to the improved antitumor efficacy and survival observed in the combination therapy group, and no apparent toxicity, as evidenced by stable body weight (Supplementary Fig. 11c, f). These results align with our observations in the Raji-Luc model, reinforcing TAIII’s role as a potent adjunct to CAR-T therapy and its potential to improve outcomes in both leukemia and solid tumors. Together, these findings support the generalizability of TAIII’s immunomodulatory effects.
To assess whether TAIII pretreatment enhances CAR-T cell antitumor activity in vivo, we treated Raji-Luc-bearing mice with CD19-CAR T cells six days post-tumor engraftment (heavy tumor burden). Mice were treated CD19-CAR T cells either with or without TAIII pretreatment (1 μM, 36 h) (Supplementary Fig. 12a). TAIII-pretreated group—which exhibited reduced FoxP3 levels both in vitro and in vivo (Supplementary Fig. 12b, c) —demonstrated significantly lower Raji-Luc cell percentages in vivo compared to CAR-T alone and the vehicle control groups. The pretreatment group exhibited greater potency and achieved earlier tumor clearance than the CAR-T only group (Supplementary Fig. 12d).
To further substantiate the potentiating effect of TAIII pretreatment on CAR-T cell-mediated cytotoxicity and its broader applicability, we employed the Nalm6-Luc subcutaneous tumor model. NSG mice were subcutaneously injected with 1 × 10⁶ Nalm6-Luc lymphoblastic leukemia cells, and six days later, 5 × 10⁶ CAR-T cells or TAIII-pretreated CAR-T cells (1 μM, 72 h) were infused. As anticipated, TAIII pretreatment significantly enhanced CAR-T cell antitumor activity in vivo. Compared to the CAR-T-only group, the TAIII-pretreated group exhibited a rapid reduction in tumor burden and achieved tumor eradication earlier, underscoring the potentiating effect of TAIII pretreatment on CAR-T cell-mediated cytotoxicity (Fig. 7o and Supplementary Fig. 12e). Subsequently, we tracked T cell frequencies and phenotypes in peripheral blood (on days 4, 7, and 14 post-CAR-T infusion), bone marrow and spleen (on day 14 post-CAR-T infusion) through flow cytometry. The results revealed that the TAIII pretreatment group exhibited a marked expansion of CAR-T cells and a significant reduction in CAR⁺ FoxP3+ Tregs in both peripheral blood (BL) and bone marrow (BM) compared to the CAR-T-only group (Fig. 7p). From day 4 to day 7, we observed an increase in the overall number of CD3+ T, CD4+ T, CD8+ T, Tcm, and effector memory T cells (Temra) cells in peripheral blood in the TAIII pretreatment group. Importantly, the CD4/CD8 ratio remained unchanged in the combination group compared to the CAR-T-only therapy group (Supplementary Fig. 12f–k). Notably, the sustained alterations in T cell populations suggest that TAIII’s modulation of Tregs provides long-term benefits, enhancing CAR-T cell persistence and functionality well beyond the initial treatment phases. These results are consistent with our findings in the Raji-Luc model and further underscore the generalizability of TAIII’s effects.
Additionally, we collected CD19 CAR-T products from 8 patients with B-lymphoblastic malignancies experiencing uncontrolled disease progression after CAR-T infusion (Table 1) and evaluated them with TAIII in coculture models. CAR-T cells from patients were co-cultured with Raji-Luc cells at E:T ratios of 1:1 to 1:4, with or without TAIII treatment (Fig. 7q). TAIII significantly enhanced CAR-T cell-mediated killing of Raji-Luc cells compared to the CAR-T-only group, with the killing efficiency in some patients increasing by several folds (Fig. 7r, Supplementary Fig. 13a, b). To determine whether TAIII enhances CAR-T cell cytotoxicity by targeting Tregs, we cocultured Raji-activated CAR-T cells with or without TAIII (E:T = 1:2). TAIII treatment significantly increased T cell-derived cytokine secretion (IL-2, IFN-γ) (Fig. 7s) and markedly decreased FoxP3 expression levels (Fig. 7t), indicating a reduction in FoxP3+ CAR-Tregs. To investigate whether TAIII improves patient-derived CAR-T function through A2AR signaling, we performed co-culture assay (E:T = 1:2) and found that NECA treatment significantly impaired CAR-T cell cytotoxicity. However, TAIII restored the cytotoxic function of NECA-treated CAR-T cells, enabling effective Raji cell killing (Supplementary Fig. 13c, d). These findings demonstrate that TAIII pretreatment and combination with CAR-T cells enhances antitumor activity, accelerating tumor clearance and reducing recurrence in preclinical models compared to CAR-T monotherapy.
To test whether the immune-modulatory effects of TAIII are dependent on immune cells (e.g., T cells), Raji-Luc cells were intravenously injected into NSG immunocompromised mice, followed by treatment with or without TAIII. TAIII exhibited minimal effect on Raji cell growth in T cell-deficient mice (Supplementary Fig. 14a–c), with no significant survival benefit (Supplementary Fig. 14d). Additionally, no apparent body weight loss was observed, confirming that TAIII’s safety in immunocompromised mice (Supplementary Fig. 14e).
To further investigate the role of TAIII in modulating Tregs during CAR-T cell therapy in vivo, we performed additional experiments using the Nalm6-Luc xenograft model with ΔTreg-CAR-T cells (Tregs reduced to 1.28%). NSG immunodeficient mice were intravenously injected with Nalm6-Luc cells, followed by CAR-T cell infusion on day 2. TAIII treatment (QD) was initiated concurrently and continued through day 18 (Supplementary Fig. 15a). We ensured the inclusion of appropriate controls, such as the UNT cell control, in the study design. Consistent with our in vitro findings (Supplementary Fig. 2), depletion of Tregs abrogated the therapeutic benefit of TAIII. While CAR-T therapy alone induced partial tumor regression, the addition of TAIII to ΔTreg-CAR-T cells conferred no further tumor suppression (Supplementary Fig. 15b, c) and did not significantly improve survival (Supplementary Fig. 15d). In the Treg-depleted CAR-T + TAIII group, the apparent loss of therapeutic benefit after day 19 is not due to a late-onset effect, but rather reflects the absence of TAIII’s primary target, Tregs. Notably, TAIII did not enhance CAR-T efficacy at any time point in the absence of Tregs, highlighting the essential role of Tregs in mediating TAIII’s therapeutic effects. Flow cytometry analysis of peripheral blood, bone marrow, and spleen on day 7 post-CAR-T infusion revealed that TAIII had no significant effect on CAR-T expansion or persistence in the Treg-depleted model, with no changes observed in the Tcm population or overall CAR-T contraction (Supplementary Fig. 15e–f). These findings underscore that TAIII enhances CAR-T efficacy primarily through Treg modulation, rather than by directly promoting CAR-T persistence. By selectively modulating Treg activity without impairing other immune components, TAIII improves CAR-T function while preserving systemic immune balance, thereby improving therapeutic outcomes.
Collectively, these findings reveal that TAIII, through Treg-targeting mechanisms, augments CAR-T cell efficacy and reduces relapse when used as a pretreatment or in combination therapy, offering a promising approach to optimize CAR-T therapeutic outcomes and production.
Discussion
CAR-T cell therapy has become an established treatment for patients with relapsed and/or refractory B cell lymphomas, achieving durable remissions in a significant proportion of patients. However, approximately half of treated patients develop resistance. The mechanisms of resistance include CD19 loss and T-cell dysfunction, which can be mitigated by targeting alternative antigens and improving manufacturing processes53. Recent studies have shown that the proportion of Tregs in CAR-T products affects CAR-T cells function post-infusion and correlates with patient’s responses and outcomes17,18. Current strategies to counteract Treg-mediated suppression include Treg cell neutralization, destabilization, and conferring T-cell resistance to Treg suppression54. However, these strategies face limitations due to incomplete understanding of in situ Treg suppression mechanisms. Moreover, poor targeting specificity often results in concurrent depletion of cytotoxic T cells or adverse effects24. Therefore, selectively blocking Treg-mediated immunosuppression remains a challenge for enhancing CAR-T immunotherapy efficacy and overcoming resistance.
Natural products offer distinct advantages compared to conventional synthetic molecules and have played a pivotal role in drug discovery, particularly in cancer therapy55,56. With higher bioavailability, broader mechanisms in action, and lower toxicity, natural products hold significant potential as targeted immune modulators in various processes of both adaptive and innate immunity57. In this study, using a Treg functional screen system and high-throughput screening of an in-house natural products library, we identified TAIII as a lead compound that impairs Tregs differentiation and function while activating the T-cell immune response during CAR-T therapy. TAIII is a steroidal saponin derived from Anemarrhena asphodeloides Bunge, and has garnered attention for its potent therapeutic properties, particularly in cancer and anti-inflammatory treatments30,58. TAIII has shown promising anti-cancer effects across various cancer types by inducing apoptosis, triggering autophagy, and inhibiting metastasis30. Some studies have demonstrated that TAIII enhances the efficacy of chemotherapies, suggesting its potential as an adjunct in cancer treatment, likely due to its immunoregulatory properities59. In line with this, although TAIII significantly suppressed tumor growth over time, the discrepancy between longitudinal tumor inhibition and endpoint tumor weight likely reflects its dynamic and immune-dependent activity (Supplementary Fig. 9d), reinforcing the rationale for combination strategies to enhance therapeutic durability. In our study, TAIII exhibited minimal impact on Raji cell growth and the survival of mice in an NSG immunocompromised model (Supplementary Fig. 14), while showing high potency in immunocompetent xenograft models or NSG mice receiving CAR-T cell infusion (Figs. 6 and 7, Supplementary Figs. 9–12). Notably, its antitumor activity was not observed in models infused with ΔTreg-CAR-T cells, and TAIII showed no specific modulatory effects on non-Treg T cell subsets in vitro (Supplementary Figs. 2 and 15). These findings reinforce the notion that TAIII primarily acts through Treg-targeted immunoregulation. Consistently, an independent study has shown that TAIII modulates the Treg/Th17 balance in colitis models by inhibiting NF-κB and MAPK signaling pathways31, highlighting the importance of further mechanistic studies to define its selective immunomodulatory properties.
Here, we identified A2AR as a key molecular target of TAIII through a combination of experimental validation and computational predictions. To begin, we synthesized a Biotin-TAIII probe for proximity labeling, followed by LC-MS analysis, which confirmed A2AR as a direct binding partner of TAIII. Further experiments, including biotin-pull-down assays, competition assays, and docking modeling, reinforced this interaction. In parallel, to further support these findings, we used the online target prediction tool SwissTargetPrediction, which revealed G protein-coupled receptors (GPCRs) as the most frequent class of predicted targets, with A2AR (ADORA2A) and A1AR (ADORA1) at the top of the list (Supplementary Fig. 3c–d). Functionally, we demonstrated that TAIII inhibits A2AR signaling by downregulating CREB activation using a CREB-reporter assay. Importantly, when A2AR ligands were added in combination with TAIII, the inhibitory effect was reversed, suggesting that TAIII can counteract the suppressive effects of A2AR ligands. Furthermore, A2AR knockdown in CAR-T cells eliminated TAIII’s enhancing effect on CAR-T potency, confirming the essential role of A2AR in mediating TAIII’s effects on Treg inhibition and CAR-T cell function (Fig. 5f–i, Supplementary Fig. 8). These findings provide strong evidence for A2AR as a critical target of TAIII in modulating immune responses and enhancing CAR-T cell efficacy.
Building upon these findings, we further demonstrate that TAIII specifically blocks A2AR signaling in CAR-T cells by acting as a previously unrecognized allosteric inhibitor, reducing the proportion of CAR-Tregs without significantly depleting cytotoxic T cells. This occurs through the suppression of FoxP3, CTLA4, CD25, Helios, Eos and CCR8 transcription (Fig. 4, Supplementary Figs. 5 and 7). To our knowledge, this is the first report of TAIII targeting and blocking immune checkpoints (ICPs), which supports the notion that TAIII is an immunoregulatory molecule. Moreover, TAIII reduces Tregs from CAR-T cells while simultaneously activating immune responses, without causing excessive inflammatory cytokine secretion, which could lead to toxicity. This suggests that TAIII carries a low risk of triggering cytokine release syndrome (CRS), a common side effect associated with CAR-T cell therapy. Importantly, TAIII increases the percentage of Tcm and Temra cells upon tumor antigen stimulation in vitro and in vivo, enhancing T-cell expansion and persistence (Figs. 5e, 6l, 7g and Supplementary Fig. 12j, k). As a result, it improves outcomes in patients receiving CAR-T products post-infusion.
Furthermore, we demonstrated that TAIII suppresses tumor growth by blocking A2AR-mediated FoxP3+Treg immunosuppressive barriers and prevents relapses after CAR-T therapy in various models by eliminating CAR-Tregs. However, our multi-omics studies revealed that TAIII affects CAR-T products through multiple mechanisms, include direct targeting of A2AR to modulate factors such as FoxP3, CTLA4, as well as influencing essential chemokines that recruit Tregs, notably the CCL1-CCR8 axis. Additionally, pathway enrichment analysis provided mechanistic insights into the metabolic reprogramming effect of TAIII on both Tregs and CAR-T cells, particularly regarding lipid metabolism. For example, TAIII regulates cholesterol metabolism (Supplementary Fig. 7k), which is crucial for A2AR signaling and Treg activity39,49, indicating the multifunctional role of TAIII in Treg regulation. These findings shed light on future studies investigating the intrinsic mechanisms of TAIII.
Given its immunoregulatory properties and ability to downregulate CTLA4 expression in T cells, TAIII holds promise as an adjuvant to immune checkpoint inhibitors (ICIs) such as anti-PD-1 antibodies. Notably, PD-1 blockade alone has been shown to paradoxically expand intratumoral Tregs, thereby limiting therapeutic efficacy50. Our study demonstrates that TAIII counteracts this effect by reducing Tregs through A2AR signaling inhibition, thereby enhancing the antitumor activity of PD-1 immunotherapy (Fig. 6, Supplementary Fig. 10). The combination of TAIII and anti-PD-1 not only reduces tumor burden but also reshapes the tumor microenvironment by suppressing Tregs while promoting the expansion and activation of CD8⁺ T cells and Tcm, ultimately overcoming a major barrier to PD-1-based therapies in solid tumors. Upregulation of key cytotoxic cytokines such as IFN-γ and downregulation of A2AR-related signaling pathways (e.g., pCREB) further indicate that TAIII enhances CD8+ T cell function while suppressing immunosuppressive Tregs. These findings suggest that TAIII could be a valuable adjuvant to PD-1 therapy, addressing Treg-mediated immune evasion and improving tumor control. The combination could offer a potent and cost-effective approach for treating solid tumors, particularly those resistant to conventional therapies. Given the promising preclinical results, further clinical studies are warranted to explore the therapeutic potential of this combination across a broader range of cancers.
TAIII also has clinical potential as a standalone or combination therapy for patients with chemotherapy-refractory or relapsed cancers. Additionally, we found that pretreating or combining patient-derived CAR-T products with TAIII significantly enhanced tumor cell killing in vitro and accelerated tumor clearance in vivo compared to CAR-T-only group (Fig. 7, Supplementary Figs. 11–13). This effect is likely mediated through its impact on ICP signaling, including A2AR and CTLA4, or by affecting CAR-T cell metabolism. Notably, the pretreatment results suggest that TAIII could offer an alternative strategy for patients who are intolerant to ongoing treatment, providing a promising approach to enhance CAR-T therapy efficacy. Collectively, these findings highlight the potential for translating TAIII-based approaches from preclinical to clinical settings.
While TAIII pretreatment significantly enhances CAR-T cell-mediated tumor clearance and delays relapse in the short term (Fig. 7o–p and Supplementary Fig. 12), our findings suggest that long-term therapeutic benefits may require sustained in vivo administration of TAIII. Although TAIII potently modulates the tumor microenvironment and boosts CAR-T efficacy (Figs. 6–7 and Supplementary Figs. 9–13), its immune-modulating effects appear transient once the drug is cleared from the system. These results underscore the potential need for continuous or intermittent TAIII treatment to sustain CAR-T cell persistence and prevent tumor recurrence. Future studies should optimize the dosing regimen and explore the combined effects of TAIII on both tumor microenvironment dynamics and CAR-T cell function, further enhancing the clinical application of this therapeutic strategy.
Currently, many new strategies are being explored to overcome the limitations of CAR T-cells and improve their efficacy by increasing their expansion capacity, persistence, and cytotoxic activity60. In addition to designing new CAR structures, optimizing cell culture conditions, and incorporating homeostatic cytokines during the expansion, recent studies demonstrate that small-molecule compounds in combination with CAR-T cell therapies show promising results in preclinical and clinical studies61,62,63,64, thereby expanding their therapeutic potential for refractory diseases.
In comparison to existing A2AR-targeting technologies, such as synthetic inhibitors, genetic silencing, and Treg depletion, TAIII offers several unique advantages. While synthetic inhibitors like AZD4635 show potent A2AR blockade, TAIII acts as an allosteric inhibitor, providing a multifaceted mechanism by not only inhibiting A2AR activity but also modulating cholesterol-related pathways crucial for A2AR activation. This broader mechanism enhances its therapeutic potential, making it a more versatile option than traditional A2AR antagonists. Furthermore, TAIII’s reversible modulation allows flexible dosing and fine-tuning of immune responses, providing distinct advantages over the permanent alterations caused by genetic silencing of A2AR. Additionally, while Treg depletion from infusion products can improve CAR-T efficacy, it often affects both Tregs and effector T cells, potentially compromising overall immune function. In contrast, TAIII selectively targets Tregs, enhancing CAR-T function without severely impacting other immune cell subsets (Supplementary Figs. 1, 2, 6 and 11). By selectively modulating Tregs and indirectly enhancing CD8⁺ T cell function while preserving overall immune homeostasis, TAIII emerges as a promising adjuvant for immunotherapy. It offers a more targeted, reversible, and immune-compatible alternative to conventional A2AR-targeting strategies.
In summary, our findings highlight that TAIII is a potent immune adjuvant that selectively impairs Treg function, improves CAR-T cell activity, and prevents relapse through allosterically binding and metabolic inhibition of A2AR signaling. While clinical trials on topical applications have shown no significant toxicity28, data on oral or intravenous administration remain limited. Preclinical rodent studies report no dose-limiting toxicity at doses up to 50 mg/kg (i.p.), and minimal adverse effects at 0.5% dermatological application29 or 5-10 mg/kg doses in our experiments (Figs. 6, 7 and Supplementary Figs. 9–11). Notably, pretreating CAR-T cells with TAIII before infusion enhances CAR-T efficacy, potentially reducing toxicity from direct drug infusion (Fig. 7, Supplementary Figs. 12 and 13). These findings suggest that TAIII could provide a safer and more targeted approach for improving CAR-T therapy, offering a valuable foundation for future clinical trials. As a safe and effective immune adjuvant currently under clinical evaluation (KCT0002223)28, TAIII could be used as a supplement in CAR-T cell products manufacturing, offering enhanced potency compared to standard culture media. While other approaches are being developed to deprive cholesterol or inhibit A2AR signaling in CAR-T products, our data suggest that approaches designed to combine or pretreat CAR-T cells with natural products like TAIII may prove more effective in enhancing antitumor activity and overcoming CAR-Treg-mediated therapeutic resistance. Further clinical investigations are needed to validate this concept and assess its efficacy in patients.
Methods
Ethics statement
All animal experiments were approved by the Institutional Animal Care and Use Committee of the Chinese Academy of Sciences (Approval Nos: DWLL(p)-2023-23, DWLL(E)-2024-34, DWLL(E)-2025-35). The maximal permitted tumor burden was 2000 mm³ in volume or 2 cm in diameter per animal, as specified by the committee guidelines. Tumors were measured every 2 days, and animals were closely monitored for signs of distress. If tumor volume approached or exceeded the approved limit at the time of measurement, animals were immediately euthanized humanely. We confirm that no animal was allowed to maintain a tumor exceeding the permitted burden for any extended period. All procedures complied with the NIH Guide for the Care and Use of Laboratory Animals and the ARRIVE guidelines.
For human samples, this study was approved by the Ethics Committee of Tongji Hospital (Approval Nos: TJ1537, NCT02537977) for the collection and use of clinical samples, and by the Ethics Committee of the Chinese Academy of Sciences (Approval No: YXLL-2023-17) for the isolation and use of PBMCs and naive T cells from healthy donors. Written informed consent was obtained from all participants prior to sample collection. The study was conducted in compliance with the principles of the Declaration of Helsinki and all relevant institutional guidelines.
Cell lines and cell culture
The HEK-293T and Jurkat T cell lines were obtained from the ATCC (Manassas, VA, USA) Cell Line Bank. Jurkat T cells used in this study were cultured with 5% CO2 at 37 °C, at a concentration of 2 × 105 to 5 × 105 in RPMI (Gibco, Thermofisher), with 10% FBS (VivaCell, C04002) and supplemented with 1% penicillin/streptomycin. Human T or CAR-T cells were cultured in X-VIVO (Lonza, 04-418Q) with 10% FBS (Gibco, 10100-147), 1% GlutaMAX (Gibco, 35050061), 1% NEAA (Gibco, 11140050), 1% Antibiotic-Antimycotic (Gibco, 15240062), 100 IU IL-2 (R&D Systems, 202-IL) and Dynabeads Human T-activator CD3/CD28 (Gibco, 1132D). HEK-293T cells were cultured in DMEM with 10% FBS (VivaCell, C04001) and 1% penicillin/streptomycin. Human cell lines were authenticated within 6 months of manuscript preparation through cell line short tandem repeat (STR) profiling conducted by a certified Contract Research Organization (CRO), SHANGHAI BIOWING BIOTECHNOLOGY Co. LTD. All cell lines tested matched >85% with the STR profiles of their corresponding lines listed in the ATCC or DSMZ Cell Line Bank and were confirmed to be virus- and mycoplasma-free.
Biological reagents
For immunoblotting, the following primary antibodies were used: β-Actin (Yeason, 30101ES60, 1:5000), CREB (Cell Signaling Technology, 9197 T, 1:1000), phospho-CREB (Ser133; Cell Signaling Technology, 9198 T, 1:1000), A2AR (Santa Cruz Biotechnology, sc-32261, 1:1000), and GAPDH (Cell Signaling Technology, #2118, 1:5000). The secondary antibodies (Goat anti-Rabbit lgG antibody, M21002L) and (Goat anti-Mouse IgG HRP, M21001L) were obtained from Abmart. Streptavidin beads magnetic beads were purchased from MedChemExpress (MCE, Shanghai). The cell viability detection kit (Cell Counting-Lite 2.0 Luminescent Cell Viability Assay) was obtained from Vazyme (DD1101-02). The Bright-Glo™ Assay Reagent was obtained from Promega (E2620). The immobilon western HRP substrate was purchased from Millipore (WBKLS0500). The LANCETM cAMP 384 Kit was purchased from PerkinElmer (AD0262E) and One Step qRT-PCR SYBR Green Kit was purchased from Yeasen (11143ES80). The chemical compound library comprised both in-house synthesized compounds and commercially acquired compounds from MCE and TargetMol (Shanghai). NECA was purchased from MCE (Shanghai). AZD4635, CPI-444 and Timosaponin AIII were purchased from TargetMol (Shanghai). Inhibitors were dissolved in DMSO to obtain 10 mM stock solutions. Serial dilutions were then made to obtain final dilutions for cellular assays with a final concentration of DMSO between 0.2% and 0.5%. All buffer solutions were prepared using pH adjustment calculations performed with Mettler Toledo (FE28-Standard).
TAIII probe synthesis
To a mixture of Timosaponin AIII (74 mg, 0.1 mmol) and 3-(3-(but-3-yn-1-yl)-3H-diazirin-3-yl) propanoic acid (17 mg, 0.1 mmol) in 2 mL DMF were added HATU (38 mg, 0.1 mmol) and DIEA (26 mg, 0.2 mmol). The mixture was stirred for 2 h at room temperature in the dark. Subsequently, the reaction was quenched by water (10 mL), and the mixture was extracted by CH2Cl2. The organic phases were combined together and dried over anhydrous Na2SO4. Upon solvent evaporation, the residue was purified by flash column chromatography to yield TAIII probe (7 mg, 8%) as a white solid.
Click Chemistry and proximity labeling proteomics
293 T cells were cultured in a 10 cm dish until 80–90% confluence was reached. The cells were washed with PBS and lysed by 1 ml of NP-40 lysis buffer. Centrifugation (13,000 g; 10 min; 4 °C) was applied to remove the insoluble fraction from the cell lysate. DMSO or TAIII-P was added into cellular lysates, followed by incubation at 4 °C for 2 h and all samples were UV (365 nM)-irradiated for 30 min using a UV crosslinker, then biotin-azide (10 μM), TCEP (1 mM), TBTA (100 μM), and CuSO4 (1 mM) were added sequentially to the lysate, followed by 1 h incubation at room temperature, protected from light. The proximity labeled proteins were then acetone-precipitated and air-dried, then resolubilized in a 1.5% SDS solution. The sample was incubated with avidin-agarose beads at room temperature for 2 hours before centrifugation, the supernatant was removed and the beads were washed with PBS three times, finally subjected to LC-MS/MS based proteomics analysis or western blotting. The raw mass spectrometry data generated has been deposited in the PRIDE public repository under accession code: PXD060766.
Cellular thermal shift assays
A2AR OE 293 T cells were harvested and freeze-thawed for three cycles, centrifuged to remove the precipitates (13,000 g; 10 min; 4 °C). TAIII or DMSO was added to cell lysates in a dose-dependent manner and incubated for 1 h. Samples were then divided into 100 μL aliquots in 0.2 ml PCR tubes and transiently heated in a PCR machine for 3 min at indicated temperatures, followed by 3 min of cooling at RT. Samples were then centrifuged (13,000 g; 10 min; 4 °C) to separate the soluble proteins from the cell debris and aggregates. The supernatant was transferred to new tubes and analyzed by western blotting.
LANCE cAMP assay
cAMP levels were measured by LANCE™ cAMP 384 kit (PerkinElmer, AD0262) according to the manufacturer protocol. Briefly, cells were harvested and resuspended in Stimulation Buffer (PBS with 0.1% BSA and 0.5 mmol/L IBMX) at a concentration of 6 × 105 cells per mL, and then transferred 5 μL of cell suspension to each well of a 384-well plate. Then stimulated cells with TAIII dilutions for 30 min in the presence of 0.1 μM NECA. After that add Detection Mix and incubate for 60 min at room temperature in the dark. Then, reading 340/665 nm and 340/615 nm fluorescence intensity, the ratio of 665 nm/615 nm is inversely proportional to cAMP concentration.
Pan-T cells activation and expansion
PBMC were isolated from fresh human peripheral blood by density gradient centrifugation. For inducing PBMC into pan-T cells, PBMC were cultured in a suitable tissue culture plate or dish at a concentration of 1 × 106/ml, and added Dynabeads Human T-Activator CD3/CD28 (Gibco, 11131D) at a bead-to-cell ratio of 1:1, 100 IU/ml IL-2 was also added into the culture medium. Dynabeads were removed on day 5, and after 48 h of removal of the beads, the pan-T cells were harvested for further analysis.
For assessed cytokine secretion and mRNA expression, PBMC or T cells were cultured at a concentration of 1 × 105 cells per mL in 96-well or 6-well flat-bottom plates, cells were activated by 1:1 Dynabeads and treated with indicated TAIII or AZD4635 in the present of 5 μM NECA. After 16 h treatment, PBMC were collected for qRT-PCR analysis (Yeason), and the secretion levels of IFN-γ and IL-2 were analyzed by an ELISA kit (MultiSciences) after 48 h of culture.
Treg induction
Human PBMCs (n = 3) were obtained from blood samples of healthy donors (Shanghai Blood Center) with ethical approval from the Shanghai Blood Center Ethics Committee. Monocytes were first isolated from fresh umbilical cord blood (n = 3) by density gradient centrifugation using Ficoll-Paque Plus (GE Healthcare), and then isolated CD4+ Naïve T cells by using Human Naïve CD4+ T Cell Isolation Kit II (Miltenyi Biotec, 130-094-131). Subsequently, naïve T cells were activated by Dynabeads Human T-Activator CD3/CD28 (Gibco, 11131D) and cultured under Treg-induced conditions as previously described: IL-2(100 IU/ml), TGF-β1 (5 ng/ml), indicated drug treatments were also administered. 5 days later, removing the TGF-β1 from the culture medium, differentiation efficiency was detected by FACS before subsequent experiments. The PBMCs and naive T cells used in our experiments were sourced from different healthy donors (Ethics approval number: YXLL-2023-17), ensuring that the data reflects variability across individuals and is representative of the general population. This approach enhances the robustness and generalizability of our findings.
Treg suppression assay
Human CD4+CD25highCD127lowCD45RA- Teff cells were sorted from healthy adult PBMC by BD FACSAria III flow cytometer. Teff cells were incubated with 2.5 μM CFSE (Invitrogen, C34570) at 37 °C for 20 min, and then added five times the original staining volume of complete culture medium and incubated for 5 min. After that, remove the supernatant by centrifugation and resuspend cells in pre-warmed culture medium. These stained cells were stimulated by CD3/CD28 Dynabeads (bead-to-cell ratio is 1:4) and then co-cultured with Treg cells at the indicated ratio in 200 μL medium in a round bottom 96-well plate (20,000 Teff cells per well). After 96 h of co-culture, the proliferating peaks were analyzed by FACS.
Flow cytometry (FACS)
For surface protein staining, cells were harvested and incubated with the fluorochrome-conjugated antibodies for 30 min at room temperature and protected from light.
The following fluorescent dye-conjugated antibodies were used for flow cytometric analysis: For human T cell staining, the abundance of distinct cell populations and the corresponding flow cytometry gating strategies were applied to delineate CD4⁺ T (CD4-FITC, BD222346; CD4-Alexa Fluor 700, BD561030), CD8⁺ T (CD8-PC5.5, BD560662), CD3⁺ T (CD3-PE, BD561803), CAR⁺ T (CAR-Alexa Fluor 647, BIOSWAN, 200102), regulatory T (Treg), naïve T (Tnaive), central memory T (Tcm), effector T (Teff), and terminally differentiated effector memory T (Temra) cells. CAR-T cells were gated on the basis of CD3 or CD4 in combination with CD19-CAR (CD19-BV421, BD562440) expression. Tregs were defined as CD4⁺FoxP3⁺ cells. For intranuclear FoxP3 staining, cells were fixed and permeabilized after surface staining, by using a Foxp3/Transcription Factor Staining Buffer Set (eBioscience) according to the manufacturer’s instructions and then stained with anti-FoxP3-PE-Cy7 (eBioscien, 25-4776-41) or FoxP3-PE (BD Pharmingen™, 560082). Human T cell subsets were classified according to surface markers as follows: CD45RO⁻CD62L⁺ (Tnaive), CD45RO⁺CD62L⁺ (Tcm), CD45RO⁺CD62L⁻ (Teff), and CD45RO⁻CD62L⁻ (Temra). For Treg depletion experiments, natural Tregs (nTregs) within PBMCs were identified as CD4⁺CD25⁺CD127low cells. For mouse T cell subsets, we used CD44 as a substitute for CD45RO. CD45RO-PE (BD 555493), CD62L-BV421 (BD 563862), and CD44-BV421 (BD 563970) were employed. Cell proliferation was tracked using CFSE (Invitrogen, C34554), and viability was assessed with Fixable Viability Stain 660 (BD 564405) or Fixable Viability Stain 520 (BD 564407). For mouse T cell staining, anti-mouse CD45-FITC (BD 553080), CD3-APC-Cy7 (BD 557596), CD4-APC (BD 553051), CD8-PC5.5 (BD 551162), FoxP3-PE (BD 560408), CD44-BV421 (BD 563970), and CD62L-Alexa Fluor 700 (BD 560517) were employed. Data were collected by Beckman CytoFLEX and analyzed with FlowJo V10.8.1 software.
Microscale Thermophoresis assay
MST assay was done as previously described65, A2AR OE 293 T cells were lysed by RIPA buffer added PMSF, centrifuged to remove the precipitates (13,000 g; 10 min; 4 °C), and then 10 μL cellular lysates were incubated with 10 μL serial dilution of TAIII or AZD4635 at room temperature for 30 min. Then the mixture was loaded into capillaries supplied by Nano-Temper, and thermophoresis was scanned by Monolith (Nano-Temper).
Human samples for scRNA-seq & bulk RNA-seq
Human CAR-T products were obtained under the approval of the Tongji Hospital Review Board (Clinical Trial No: NCT02537977, Sponsor: Shanghai Tongji Hospital, Tongji University School of Medicine) and written informed consent was obtained from all participants or their legally authorized representatives. Clinical characteristics of B-lymphoblastic malignancy patients can be found in Table 1. The scRNA-seq and bulk RNA-seq were performed and carried out by Novogene Co., Ltd. following the manufacturer’s instructions. The raw data generated in this study have been deposited in the GEO database under accession numbers GSE289388 and GSE302847.
Cut & Run assay
The Cut & Run assays were performed as previously described66, carried out and analyzed by Novogene Co., Ltd. following the manufacturer’s instructions. Details provided in Supplementary and methods.
Molecular modeling
The crystal structure of A2AR was obtained from Protein Data Bank (PDB ID: 4EIY). Then, water molecules and original ligands were manually removed by using PyMol software. This docking job to predict the binding pose of Timosaponin AIII was carried out by Autodock (version 4.2.6). To the beginning, prepare_ligand4.py and prepare_recptor4.py scripts from AutoDockTools 1.5.6 were used to prepare the initial files, including adding charges and hydrogen atoms. Next, a grid box of 60 × 60 × 60 with a spacing of 0.375 Å was set to enclose the whole binding site38. The Lamarckian genetic algorithm (LGA) was adopted to search for the best binding poses. The specific docking settings were as follows: trials of 100 dockings, 300 individuals per population with a crossover rate of 0.8, and the local search rate was set to 0.06. Other parameters were set as default during the docking.
CAR-T cell production
CD19 CAR-T cells were generated from human T cells. Briefly, human pan-T cells (CD3 T) were isolated from PBMC (n = 3) with a human pan-T isolated kit (Miltenyi Biotec, 130-096-535) and incubated with CD3/CD28 cross-linking antibody beads, CAR lentiviral constructs were delivered into T cells at MOI = 5-10 on the 3rd day, cells then were expanded in vitro in the presence of 100 U/ml IL-2 for 7 days. During the expansion, the medium was replenished every other day to a density of 1 × 106. The CAR-T cells were co-cultured with Raji cells (E:T at 2:1 or 4:1) under indicated treatments for 16 h, then analyzed by flow cytometry.
CAR-T cell functional assay
For assessing CAR-T cell cytotoxicity function, 2 × 104 Raji cells were co-cultured with CD19-CAR-T cells in 1640 with 5% FBS at the indicated ratio in 96-well round-bottom plates, under 1 μM TAIII treatment in the presence or absence of 5 μM NECA. After 16 h co-culture, cells were harvested for qRT-PCR and FACS, the frequency of CD19 positive cells was considered to be the remaining frequency of Raji cells, and the CAR-T cell killing percentage = (Initial frequency - Remaining frequency) ÷ Initial frequency. After 16 h co-culture, collect culture supernatant to measure the secretion level of IL-2, IFN-γ and TNF-α by ELISA (MultiSciences). We acknowledge that variability in cytokine levels, such as IL-2, may arise between experiments due to differences in the donor-derived CAR-T cells and the sensitivity of the ELISA assay kits used. These factors should be taken into account when interpreting the data. Nevertheless, all experiments were conducted under consistent conditions to ensure the reliability of the results within each specific setup. And, the frequency of CD62L+CD45RO+ Tcm cell subsets were determined after 48 h co-culture.
The process of CD19-CAR-T killing was monitored by Incucyte® S3 Live-Cell Analysis System (Sartorius). For this assay, Raji cells were stained with Incucyte® cytolight rapid red dye (Sartorius, #4706) prior to seeding at a density of 10,000 cells per well in a 96-well flat-bottom plate. Then different numbers of CAR-T cells were added to obtain the indicated E:T ratio, and a suggested concentration of Incucyte® Annexin V Green Dye (Sartorius, #4642) was added into culture medium for mark cells undergoing apoptosis. Fluorescence images at 10× zoom of each well were collected every 2 h during 36-h co-culture process; the colocalization of red and green fluorescent areas indicates the apoptotic Raji cells. The data was analyzed using Incucyte® Spheroid Analysis Software Module.
Knockdown assay
The A2AR-shRNA pLKO.1-GFP-puro lentiviral particles against A2AR were obtained from Tsingke Biotechnology Co., Ltd., Treg cells were incubated with the viral particles in the presence of 5–8 μg/ml Polybrene (Hanbio) for 24 h, and then fresh medium was added. 72 h post-infection, the cells were selected with 0.3 μg/ml puromycin for 48 h. Following selection, cells were collected after 3–5days of selection, GFP+ and GFP- cells were isolated by sorting, and protein as well as mRNA levels were determined by immunoblotting and qRT-PCR, respectively.
The sequences of the shRNAs are as follows:
Name | Target sequences |
A2AR-sh1 | GCCTCTTCATTGCCTGCTTCG |
A2AR-sh2 | GCCAAGTGGCCTGTCTCTTTG |
A2AR-sh3 | GCTAAGGGCATCATTGCCATC |
High-throughput screening platform for Foxp3-mediated IL-2 inhibition
To generate a high-throughput screening platform for Foxp3-mediated IL-2 inhibition, the human IL-2 promoter region (−326- + 145, 473 bp), which contains a FoxP3 binding site, was introduced into the Lenti-PGL4 delivery vector. In this approach, lentivirus was packaged by Hanbio, and the IL-2 promoter-Fluc reporter was introduced into the Jurkat T cells followed the lentivirus transduction protocol in the presence of 5–8 μg/ml Polybrene (Hanbio) for 24 h, and then fresh medium was added. 72 h post-infection, the cells were selected with 0.3 μg/ml puromycin for 48 h. Following puromycin selection, monoclonal cells were isolated. These clones were tested for luciferase activity upon TCR stimulation, and the best-performing monoclonal clone was selected. Subsequently, a lentiviral construct for FoxP3a overexpression, containing a BSD resistance cassette, was introduced into the selected clone. After another round of TCR stimulation and selection, the final monoclonal cell line was chosen based on optimal performance. Treg function was evaluated by measuring the fluorescence intensity of Fluc.
Animal models
(1) Syngeneic transplant models:
Six-week-old male C57BL/6 J mice (Gem Pharmatech, Nanjing, China) were housed in IVC cages in SPF facility and used according to the animal care regulations of Hefei Institutes of Physical Science, Chinese Academy of Sciences (Hefei, China). After a week of adaptive feeding, 1 × 106 MC38 cells in PBS harvested during exponential growth were injected into the subcutaneous space on the right flank of mice. Daily oral administration was initiated when the tumor volume had reached about 50 mm3. TAIII was delivered intraperitoneally daily in 5% DMSO/0.5% Methocel/0.4% Tween80 solution at 5 mg/kg, 10 mg/kg, and 20 mg/kg, or anti-PD-1 (5 mg/kg in saline, BIW), and its vehicle was administered as control. The reference compound AZD4635 was delivered orally twice a day in 5% DMSO corn oil at 50 mg/kg. Body weight and tumor growth were measured every two days. Tumor volume (mm3) = [(W2 × L)/2], in which the width (W) is defined as the smaller of the two measurements and length (L) is defined as the larger of the two measurements. The harvested tumor-draining lymph nodes or the tumor tissues were further evaluated by the IHC assay using Foxp3 and CD8 staining according to the instructions. Briefly, after fixing in 4% neutral buffered formalin and processing in paraffin, the tumor-draining lymph nodes or the tumor tissues were sectioned into 4 μm sections, and then stained with FoxP3 or CD8 antibody.
(2) Non-invasive in vivo bioluminescence model:
5.5-week-old NSG mice were injected intravenously with 3 × 106 Raji-Luc or Nalm6-Luc cells (Shanghai Model Organisms Center, Inc., NM-B07-1). Two or six days later, 6 × 106 of CAR-T cells manufactured from day 6-10 were given intravenously. Effect of CAR-T only or TAIII combination treatment (5 mg/kg, IP, HKI) on Raji-Luc+ or Nalm6-Luc+ cell growth in a non-invasive in vivo bioluminescence model of lymphoma (n = 5 or 6). For a pretreatment model, the CD19-CAR T cells with or without TAIII pretreatment (1 μM, 36 h) were infused post-6 days of injection of Raji-Luc to mice. Correlation between luciferase-positive lymphoma burden as measured by Bright-Glo assay and luminoskan every 3 days or every week and bioluminescent images of representative mice with matched starting lymphoma burden were taken. Survival curves were compared using the log rank Mantel–Cox test. The percentage of Luc (CD19) and CAR-T cells, along with other T cell subsets, was measured by flow cytometry using the indicated antibodies in blood or bone marrow or spleen samples from transplanted mice (n = 5 or 6). The body weights of mice transplanted were measured every two days.
In the MC38-mCD19 subcutaneous tumor model, C57BL/6 J immunocompetent mice were subcutaneously injected with 1 × 10⁶ MC38-mCD19 cells (n = 5). On day 6, mice were treated with 4.5 mg cyclophosphamide (CTX) and 0.75 mg/200 μL fludarabine (FLU) via intraperitoneal injection for lymphodepletion. On day 7, mice were treated with the optimal dose of CAR-T cells (4 × 10⁶), TAIII (10 mg/kg, daily), or a combination of both. Tumor size was measured after treatment. Subsequent assays, including tumor growth inhibition (TGI) calculations, tumor tissue staining, flow cytometry, and ELISA, were performed following procedures similar to those used in the syngeneic transplant models. TGI = ((MTVcontrol-MTVtreated)/MTVcontrol)×100%. MTV: Mean Tumor Volume.
For the Nalm6-Luc subcutaneous tumor model with pretreatment, NSG mice (n = 3) were subcutaneously injected with 1 × 10⁶ Nalm6-Luc lymphoblastic leukemia cells. Six days later, 5 × 10⁶ CAR-T cells or TAIII-pretreated CAR-T cells (1 μM, 72 h) were infused. Correlation analysis was performed between the luciferase-positive leukemia burden, measured by the Bright-Glo assay and Luminoskan. Total flux was quantified and plotted. T-cell frequencies and phenotypes were assessed in peripheral blood (on days 4, 7, and 14 post-CAR-T infusion), bone marrow and spleen (on day 14 post-CAR-T infusion) via flow cytometry.
Mice were sacrificed according to the experimental protocols or when they met prespecified endpoints defined by the IACUC. All animal studies were performed by blinded personnel in specific-pathogen-free, Helicobacter-free facilities in Tongji University and the Chinese Academy of Sciences Animal Resource Center following national, state, and institutional guidelines, including the ARRIVE guidelines, and according to protocols approved by the Institutional Animal Care and Use Committee of Tongji University and the Chinese Academy of Sciences (DWLL(p)-2023-23, DWLL(E)-2024-34, DWLL(E)-2025-35).
ELISAs on tumor samples
ELISAs on tumor samples were performed as described before67,68. Briefly, the procedure involved two main steps:
(1) Tumor Tissue Preparation: Tumor tissues were excised immediately post-sacrifice and placed on ice to minimize protein degradation. The tissues were minced and homogenized in a tissue lysis buffer optimized for protein extraction. After homogenization, samples were centrifuged at 4 °C to collect the supernatant containing soluble proteins.
(2) ELISA Procedure: The supernatant was analyzed using commercially available ELISA kits (MultiSciences), following the manufacturer’s instructions, to quantify IL-2, IFN-γ, and other cytokines of interest in both tumor homogenates and serum samples.
Statistical analysis
Each experiment was conducted independently three times, with three technical replicates per experiment. Biological replicates are defined as independent experiments performed on different days using distinct cell passages or animals. For in vitro experiments, each replicate represents cells from a separate culture batch; for in vivo studies, each replicate represents an individual mouse. Technical replicates (e.g., multiple wells from the same culture) were not used for statistical analysis. Standard deviation (SD) was used for all data unless otherwise specified. Normality of the data was assessed using the Shapiro-Wilk test. Parametric tests (Student’s t-test or ANOVA) were applied only to data that passed the normality test. For data that did not follow a normal distribution, non-parametric tests, such as the Mann-Whitney U test or Kruskal-Wallis test, were used as appropriate. Statistical significance was determined accordingly, with exact P values reported in the figures for clarity. All analyses were conducted using GraphPad Prism (Version 9).
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
The datasets generated in this study, including scRNA-seq and bulk RNA-seq, have been deposited in the Gene Expression Omnibus (GEO) database under accession numbers GSE289388 and GSE302847, respectively. The LC-MS/MS-based proteomics data have been deposited in the PRIDE repository under accession code PXD060766. Source data are provided with this paper. All other relevant data are available within the article, its Supplementary Information, or the Source Data file. Source data are provided with this paper.
References
Sehn, L. H. & Salles, G. Diffuse large B-cell lymphoma. N. Engl. J. Med. 384, 842–858 (2021).
Schuster, S. J. et al. Chimeric antigen receptor T cells in refractory B-cell lymphomas. N. Engl. J. Med. 377, 2545–2554 (2017).
Neelapu, S. S. et al. Axicabtagene ciloleucel CAR T-cell therapy in refractory large B-cell lymphoma. N. Engl. J. Med. 377, 2531–2544 (2017).
Maude, S. L. et al. Tisagenlecleucel in children and young adults with B-cell lymphoblastic leukemia. N. Engl. J. Med. 378, 439–448 (2018).
Maude, S. L. et al. Chimeric antigen receptor T cells for sustained remissions in leukemia. N. Engl. J. Med. 371, 1507–1517 (2014).
Nakamura, K. et al. Targeting an adenosine-mediated “don’t eat me signal” augments anti-lymphoma immunity by anti-CD20 monoclonal antibody. Leukemia 34, 2708–2721 (2020).
Rodriguez-Garcia, A., Palazon, A., Noguera-Ortega, E., Powell, D. J. Jr. & Guedan, S. CAR-T cells hit the tumor microenvironment: strategies to overcome tumor escape. Front Immunol. 11, 1109 (2020).
Togashi, Y., Shitara, K. & Nishikawa, H. Regulatory T cells in cancer immunosuppression—implications for anticancer therapy. Nat. Rev. Clin. Oncol. 16, 356–371 (2019).
Locke, F. L. et al. Tumor burden, inflammation, and product attributes determine outcomes of axicabtagene ciloleucel in large B-cell lymphoma. Blood Adv. 4, 4898–4911 (2020).
Jacobson, C. A. et al. Axicabtagene ciloleucel in the non-trial setting: outcomes and correlates of response, resistance, and toxicity. J. Clin. Oncol. 38, 3095–3106 (2020).
Sterner, R. C. & Sterner, R. M. CAR-T cell therapy: current limitations and potential strategies. Blood Cancer J. 11, 69 (2021).
Ruella, M., Korell, F., Porazzi, P. & Maus, M. V. Mechanisms of resistance to chimeric antigen receptor-T cells in haematological malignancies. Nat. Rev. Drug Discov. 22, 976–995 (2023).
Sakaguchi, S. et al. Regulatory T cells and human disease. Annu. Rev. Immunol. 38, 541–566 (2020).
Rudensky, A. Y. Regulatory T cells and Foxp3. Immunol. Rev. 241, 260–268 (2011).
Zheng, Y. & Rudensky, A. Y. Foxp3 in control of the regulatory T cell lineage. Nat. Immunol. 8, 457–462 (2007).
Schuster, S. J. et al. Tisagenlecleucel in adult relapsed or refractory diffuse large B-cell lymphoma. N. Engl. J. Med. 380, 45–56 (2019).
Good, Z. et al. Post-infusion CAR TReg cells identify patients resistant to CD19-CAR therapy. Nat. Med. 28, 1860–1871 (2022).
Haradhvala, N. J. et al. Distinct cellular dynamics associated with response to CAR-T therapy for refractory B cell lymphoma. Nat. Med. 28, 1848–1859 (2022).
Saini, N. & Neelapu, S. S. CAR Treg cells: prime suspects in therapeutic resistance. Nat. Med. 28, 1755–1756 (2022).
Marabelle, A. et al. Depleting tumor-specific Tregs at a single site eradicates disseminated tumors. J. Clin. Invest 123, 2447–2463 (2013).
Wang, R. et al. Blocking migration of regulatory T cells to leukemic hematopoietic microenvironment delays disease progression in mouse leukemia model. Cancer Lett. 469, 151–161 (2020).
Tai, Y.-T. et al. APRIL signaling via TACI mediates immunosuppression by T regulatory cells in multiple myeloma: therapeutic implications. Leukemia 33, 426–438 (2019).
Sharma, M. et al. Bempegaldesleukin selectively depletes intratumoral Tregs and potentiates T cell-mediated cancer therapy. Nat. Commun. 11, 661 (2020).
Dees, S., Ganesan, R., Singh, S. & Grewal, I. S. Regulatory T cell targeting in cancer: emerging strategies in immunotherapy. Eur. J. Immunol. 51, 280–291 (2021).
Luo, Y., Cobb, R. E. & Zhao, H. Recent advances in natural product discovery. Curr. Opin. Biotechnol. 30, 230–237 (2014).
Harvey, A. L., Edrada-Ebel, R. & Quinn, R. J. The re-emergence of natural products for drug discovery in the genomics era. Nat. Rev. Drug Discov. 14, 111–129 (2015).
Atanasov, A. G. et al. Natural products in drug discovery: advances and opportunities. Nat. Rev. Drug Discov. 20, 200–216 (2021).
Im, A. R. et al. Clinical evaluation of the safety and efficacy of a timosaponin A-III-based antiwrinkle agent against skin aging. J. Cosmet. Dermatol 19, 423–436 (2020).
Lin, Y. et al. Pharmacological activity, pharmacokinetics, and toxicity of timosaponin AIII, a natural product isolated from Anemarrhena asphodeloides Bunge: a review. Front. Pharmacol. 11, 764 (2020).
Tu, H. et al. Anti-tumor effect and mechanisms of Timosaponin AIII across diverse cancer progression. Biochem. Pharmacol. 228, 116080 (2024).
Lim, S.-M. et al. Timosaponin AIII and its metabolite sarsasapogenin ameliorate colitis in mice by inhibiting NF-κB and MAPK activation and restoring Th17/Treg cell balance. Int. Immunopharmacol. 25, 493–503 (2015).
Tong, C. et al. Optimized tandem CD19/CD20 CAR-engineered T cells in refractory/relapsed B-cell lymphoma. Blood 136, 1632–1644 (2020).
Klysz, D. D. et al. Inosine induces stemness features in CAR-T cells and enhances potency. Cancer Cell 42, 266–282.e268 (2024).
Raskov, H., Orhan, A., Christensen, J. P. & Gögenur, I. Cytotoxic CD8+ T cells in cancer and cancer immunotherapy. Br. J. Cancer 124, 359–367 (2021).
Wang, Y. et al. Pharmacological targeting of Vacuolar H(+)-ATPase via subunit V1G combats multidrug-resistant cancer. Cell Chem. Biol. 27, 1359–1370.e1358 (2020).
Sheth, S., Brito, R., Mukherjea, D., Rybak, L. P. & Ramkumar, V. Adenosine receptors: expression, function and regulation. Int. J. Mol. Sci. 15, 2024–2052 (2014).
Carpenter, B. & Lebon, G. Human adenosine A2A receptor: molecular mechanism of ligand binding and activation. Front. Pharmacol. 8, 898 (2017).
McGraw, C., Koretz, K.S., Oseid, D., Lyman, E. & Robinson, A.S.J.M. Cholesterol dependent activity of the adenosine A2a receptor is modulated via the cholesterol consensus motif. Molecules 27, 3529 (2022).
McGraw, C., Yang, L., Levental, I., Lyman, E. & Robinson, A. S. Membrane cholesterol depletion reduces downstream signaling activity of the adenosine A(2A) receptor. Biochim Biophys. Acta Biomembr. 1861, 760–767 (2019).
Zhang, L. et al. Novel timosaponin AIII-based multifunctional liposomal delivery system for synergistic therapy against hepatocellular carcinoma cancer. Int. J. Nanomed. 16, 5531–5550 (2021).
Wang, L. et al. The inhibitory effect of adenosine on tumor adaptive immunity and intervention strategies. Acta Pharmaceutica Sin. B 14, 1951–1964 (2024).
Xing, J., Zhang, J. & Wang, J. The immune regulatory role of adenosine in the tumor microenvironment. Int. J. Mol. Sci. 24, 14928 (2023).
Whiteside, T. L. Targeting adenosine in cancer immunotherapy: a review of recent progress. Expert Rev. Anticancer Ther. 17, 527–535 (2017).
Ohta, A. & Sitkovsky, M. Extracellular adenosine-mediated modulation of regulatory T cells. Front Immunol. 5, 304 (2014).
Ernst, P. B., Garrison, J. C. & Thompson, L. F. Much Ado about adenosine: adenosine synthesis and function in regulatory T cell biology. J. Immunol. 185, 1993–1998 (2010).
Gitto, S., Natalini, A., Antonangeli, F. & Di Rosa, F. The emerging interplay between recirculating and tissue-resident memory T cells in cancer immunity: lessons learned from PD-1/PD-L1 blockade therapy and remaining gaps. Front. Immunol. 12 755304 (2021).
Ahmed, H. et al. Role of T cells in cancer immunotherapy: Opportunities and challenges. Cancer Pathogenesis Ther. 1, 116–126 (2023).
Park, J.-H. et al. Timosaponin A3 induces anti-obesity and anti-diabetic effects in vitro and in vivo. Int. J. Mol. Sci. 25, 2914 (2024).
Zeng, H. et al. mTORC1 couples immune signals and metabolic programming to establish T(reg)-cell function. Nature 499, 485–490 (2013).
Geels, S. N. et al. Interruption of the intratumor CD8+ T cell:Treg crosstalk improves the efficacy of PD-1 immunotherapy. Cancer Cell 42, 1051–1066.e1057 (2024).
Cortez, V. S. et al. CRTAM controls residency of gut CD4+CD8+ T cells in the steady state and maintenance of gut CD4+ Th17 during parasitic infection. J. Exp. Med. 211, 623–633 (2014).
Boles, K. S., Barchet, W., Diacovo, T., Cella, M. & Colonna, M. The tumor suppressor TSLC1/NECL-2 triggers NK-cell and CD8+ T-cell responses through the cell-surface receptor CRTAM. Blood 106, 779–786 (2005).
Salas-Benito, D., Berger, T.R. & Maus, M.V. Stalled CARs: Mechanisms of Resistance to CAR T Cell Therapies. 7, 23-42 (2023).
Han, S., Toker, A., Liu, Z. Q. & Ohashi, P. S. Turning the tide against regulatory T cells. Front Oncol. 9, 279 (2019).
Huang, M., Lu, J.-J. & Ding, J. Natural products in cancer therapy: past, present and future. Nat. Products Bioprospecting 11, 5–13 (2021).
Ali Abdalla, Y. O. et al. Natural products for cancer therapy: a review of their mechanism of actions and toxicity in the past decade. J. tropical Med. 2022, 5794350 (2022).
Wang, K., Conlon, M., Ren, W., Chen, B. B. & Bączek, T. Natural products as targeted modulators of the immune system. J. Immunol. Res. 2018, 7862782 (2018).
Ji, K. Y. et al. The enhancing immune response and anti-inflammatory effects of Anemarrhena asphodeloides extract in RAW 264.7 cells. Phytomedicine Int. J. Phytother. Phytopharmacol. 59, 152789 (2019).
Song, X. Y. et al. Timosaponin AIII, a steroidal saponin, exhibits anti-tumor effect on taxol-resistant cells in vitro and in vivo. Steroids 146, 57–64 (2019).
López-Cantillo, G., Urueña, C., Camacho, B.A. & Ramírez-Segura, C. CAR-T Cell Performance: How to Improve Their Persistence? Front Immunol. 13, 878209 (2022).
Zhang, H. et al. The magic of small-molecule drugs during ex vivo expansion in adoptive cell therapy. Front Immunol. 14, 1154566 (2023).
Cao, X. et al. Small-molecule compounds boost CAR-T cell therapy in hematological malignancies. Curr. Treat. options Oncol. 24, 184–211 (2023).
Harrer, D.C., Dörrie, J. & Schaft, N. CARs and Drugs: pharmacological ways of boosting CAR-T-cell therapy. Int. J. Mol. Sci. 24, 2342 (2023).
Park, S. et al. Direct control of CAR T cells through small molecule-regulated antibodies. Nat. Commun. 12, 710 (2021).
Huang, L. & Zhang, C. Microscale thermophoresis (MST) to detect the interaction between purified proteins and small molecules. in Plant Chemical Genomics: Methods and Protocols (eds. Hicks, G.R. & Zhang, C.) 187–193 (Springer US, New York, NY, 2021).
Mei, H. et al. Discovery of IHMT−337 as a potent irreversible EZH2 inhibitor targeting CDK4 transcription for malignancies. Signal Transduct. Target. Ther. 8, 18 (2023).
Hsu, E. J. et al. A cytokine receptor-masked IL2 prodrug selectively activates tumor-infiltrating lymphocytes for potent antitumor therapy. Nat. Commun. 12, 2768 (2021).
García-Mendoza, M. G. et al. Neutrophils drive accelerated tumor progression in the collagen-dense mammary tumor microenvironment. Breast Cancer Res. 18, 49 (2016).
Acknowledgements
The authors gratefully acknowledge the generous and valuable scientific support of Dr. James D. Griffin and Prof. Sara Buhrlage at the Dana-Farber Cancer Institute, Harvard Medical School, and Prof. Caiwen Duan at Shanghai Children’s Medical Center, Shanghai Jiao Tong University School of Medicine. The author is especially grateful to Mr. Guangzhen Wang for his steadfast support, selfless contributions and constant encouragement throughout the course of this study. Our work was supported and funded by the National Natural Science Foundation of China (82373937 to J.Y., 82370158 to W.Z., and 82304784 to R.J.), the National Key R&D Program of China (2021YFA1100800 to A.L.), the Fundamental Research Funds for the Central Universities (22120240435 to J.Y.), and the Major Science and Technology Project of Anhui Province (202303a07020007 to Q.L.). We are also grateful for the support of the Youth Innovation Promotion Association of CAS support for J.Y. (No. 2022453). Figures were created with BioRender.com and published under license (u3ikt9k, ooqqw8l, grxl0cd).
Author information
Authors and Affiliations
Contributions
M.H., W.Z., Z.Q. and G.L. conceptualized, designed, and performed the studies. M.H., Z.Q. and G.L. carried out data analyses and wrote the manuscript. Z.Q., G.L. and H.M. performed the animal studies, S.Q., Y.Z., X.C. and C.Q. helped with animal studies. H.M. prepared a schematic illustration of the compound screening workflow. W.Z., Y.Z., X.T. and X.L. helped with CAR-T generation and analysis. R.J., C.H. and L.Y. helped with cell lines and system generation. Z.X., D.L. and R.L. provided human PBMCs and helped with the Treg induction assay. W.Z. and B.X. performed the analysis of the human clinical databases. C.W. and B.W. helped with molecular modeling/docking. Y.H. helped with cell culturing and FACS. Y.C. and A.W. helped with the click chemistry assay. J.L., W.W., B.L., J.L. and P.L. provided valuable scientific feedback and guidance. A.L., Q.L. and J.Y. conceptualized and designed the studies, carried out data analyses, and wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks Sebastian Kobold, Francesco Marangoni, Lilach Soreq and the other anonymous reviewers for their contribution to the peer review of this work. [A peer review file is available].
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Hou, M., Zhang, W., Qi, Z. et al. Timosaponin AIII enhances CAR-T cell potency and prevents relapse through impairing CAR-Tregs. Nat Commun 17, 3045 (2026). https://doi.org/10.1038/s41467-026-70867-5
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41467-026-70867-5