Abstract
This study aimed to investigate cervical vessel hemodynamics during 7 days of −6° head-down tilt (HDT) bed rest (BR) and 5 days of recovery in 40 healthy males, focusing on bilateral analysis and dynamic temporal monitoring. Diameter, flow velocity, and blood flow volume (BFV) of bilateral common (CCAs), internal (ICAs), external carotid arteries and vertebral arteries (VAs) were measured at eight time points using ultrasound. Cervical vessels exhibited heterogeneous and lateralized responses. Left VA exhibited the most pronounced BFV and velocity fluctuations, with significant reductions during HDT and recovery to baseline post-HDT, while right VA remained stable. CCAs and ICAs had dynamic diameter and velocity changes, but stable BFVs. Left VA BFV reduction was significantly associated with right VA dominance, elevated heart rate, and increased mean arterial pressure at HDT 3 d. Despite stable total BFV, left VA BFV declined during BR, warranting further monitoring.
Similar content being viewed by others
Introduction
Cerebral perfusion is a critical physiological process that ensures a continuous supply of oxygen and nutrients to the brain while facilitating the removal of metabolic waste, thereby maintaining normal brain function1,2. This process is essential for maintaining normal brain structure and supporting complex neurological functions3,4. However, in microgravity environments, such as those experienced during spaceflight, cerebral perfusion can be significantly disrupted, resulting in physiological symptoms including increased intracranial pressure, dizziness, visual disturbances, and cognitive impairment5,6,7. These symptoms are attributed primarily to fluid redistribution and hemodynamic changes induced by microgravity7. Investigating these mechanisms enhances our understanding of how microgravity affects brain function and plays a vital role in protecting the health and performance of astronauts during long-term space missions.
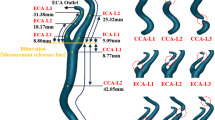
Cerebral blood flow (CBF), a key indicator of cerebral perfusion, quantifies the volume of blood flowing through brain tissue per unit time8. The brain receives its blood supply through two interconnected circulatory systems, the anterior and posterior circulations, which are connected via the circle of Willis at the base of the brain9,10. The anterior circulation originates primarily from the internal carotid artery (ICA) and its branches, including the anterior cerebral artery (ACA) and middle cerebral artery (MCA)11. The ACA supplies the frontal lobe and medial parietal regions, supporting motor control, cognition, and decision-making. In contrast, the MCA supplies the lateral temporal and parietal lobes, as well as the basal ganglia, playing crucial roles in language, sensory perception, and motor functions12,13. The posterior circulation, comprising the vertebral arteries (VAs) and basilar artery, gives rise to the posterior cerebral arteries, which primarily supply the occipital lobe and parts of the temporal lobe essential for visual processing14,15. Total intracranial blood flow is influenced by the combined contributions of the bilateral ICAs and VAs10. Additionally, the common carotid artery (CCA) bifurcates into the ICA and external carotid artery (ECA) simultaneously16, underscoring the importance of cervical vascular health in maintaining adequate cerebral blood supply. Any alterations in cervical blood flow directly impact cerebral perfusion. In our previous study on the effects of dobutamine infusion on cerebral perfusion, we observed heterogeneous CBF responses in the cerebral arteries of volunteers17,18. Such heterogeneous CBF variations are also evident under various physiological conditions, including acute hypotension, hypoxia, orthostatic stress, and dynamic or resistance exercise19,20. These findings highlight the insufficiency of assessing anterior circulation alone to fully capture the regulatory mechanisms of the CBF. A comprehensive evaluation of vascular behavior is therefore essential for understanding these variations. However, the adaptation of the blood flow volume (BFV) within these vessels to microgravity remains inadequately understood, highlighting the need for further investigation.
With increasing interest in microgravity effects, growing attention has been directed toward understanding the CBF under microgravity conditions, including actual spaceflight and ground-based simulated weightlessness, such as head-down tilt (HDT) bed rest (BR), head-out dry immersion, and parabolic flight. Iwasaki et al. examined 6 astronauts during a 16-day space mission and found no significant changes in resting MCA blood flow velocity during or after spaceflight21. Possnig et al. examined BFV changes in the right ICA and VA of 17 volunteers during a 3-day HDT BR and reported a significant decline in BFV in both vessels22. A study in which Doppler ultrasonography was used to measure BFV in the right CCA, ICA, ECA, and VA of 10 healthy males during a 3-day head-out dry immersion reported no significant changes in CBF during or after immersion23. Klein et al. measured right MCA velocity using transcranial Doppler (TCD) during 15 intervals of 22 s of weightlessness in a parabolic flight, assessed 17 participants, and reported no significant differences in velocity between normal gravity and microgravity conditions24. Despite these findings, research on cervical vessels under microgravity conditions remains limited, with inconsistent or unclear patterns of dynamic adaptation and poorly defined turning points, highlighting several gaps that warrant further investigation. First, most studies have focused primarily on the right ICA, with limited attention given to the CCA, ECA, and VA. Second, the predominant focus on unilateral vessels, typically on the right, overlooks potential laterality effects, thereby limiting the comprehensive assessment of the vascular status. Finally, most studies compare discrete time points (e.g., pre-, mid-, and post-HDT BR) without continuous monitoring, potentially missing critical dynamic changes that occur during adaptation to microgravity. Continuous monitoring is essential for capturing the full spectrum of vascular responses.
This study used ultrasound technology to systematically examine changes in vascular diameter, blood flow velocity, and BFV in the bilateral CCAs, ICAs, ECAs, and VAs at multiple time points during a 7-day −6° HDT period and a subsequent 5-day recovery phase. The −6° HDT model, a well-established and widely used ground-based method in aerospace medicine, simulates microgravity by positioning participants at a fixed −6° with the head lower than the feet, thereby effectively reproducing the fluid redistribution and hemodynamic changes observed during spaceflight and enabling the study of its physiological effects on the cardiovascular, musculoskeletal, and nervous systems19,25,26,27. The innovation of this study lies in its comprehensive examination of all major cervical vessels through synchronized bilateral vessel assessments and dynamic monitoring across multiple time points. By integrating these approaches, this study aimed to elucidate the dynamic regulatory characteristics of cervical vascular blood flow under simulated microgravity conditions and provide critical insights into cerebral perfusion regulation.
Results
General characteristics
The median age of the 40 healthy male volunteers was 25 years (22, 31), with a range of 19–49 years. The participants’ mean body mass index (BMI) was 23.03 ± 2.49 kg/m2 (range 19.00–29.10 kg/m2). BMI was calculated as weight (kg) divided by the square of height (m²). Among the 40 participants, 30 showed VA dominance, with 20 exhibiting left VA dominance, 10 exhibiting right VA dominance, and the remaining 10 classified as having balanced VA.
Physiological data at different time points
Measurements were performed by trained professionals at multiple time points: baseline (pre-HDT); 12 h (HDT 0.5 d), day 1 (HDT 1 d), day 3 (HDT 3 d), and day 7 (HDT 7 d) during BR; and during recovery on day 1 (R + 1 d), day 3 (R + 3 d), and day 5 (R + 5 d).
Heart rate (HR) significantly decreased during the HDT period, reaching its lowest value at HDT 3 d (62.50 [58.0, 66.75] bpm) before slightly increasing at HDT 7 d. During the recovery phase, HR gradually returned to baseline levels. Systolic blood pressure (SBP) remained stable during the initial HDT period but increased significantly at HDT 7 d (120.80 ± 8.31 mmHg). During the recovery phase, SBP gradually approached baseline levels. Diastolic blood pressure (DBP) exhibited a steady increase during the HDT phase, whereas the mean arterial pressure (MAP) increased significantly, both peaking at HDT 7 d (DBP: 71.98 ± 7.24 mmHg; MAP: 88.20 ± 6.66 mmHg). Both DBP and MAP fluctuated during the recovery phase. Pulse pressure (PP) showed minimal fluctuations, and blood oxygen saturation (SpO2) remained stable throughout the HDT and recovery phases, with no significant differences observed across time points. The detailed physiological data are presented in Table 1.
Differences in total intracranial volume and BFV-related parameters of the CCAs, ICAs, ECAs, and VAs at different time points
BFVs of different vessels and total intracranial volume
The variations in BFV across different vessels and changes in total intracranial volume over time are presented in Table 2. As illustrated in Fig. 1, BFV in the left VA significantly decreased from baseline to HDT 0.5 d (P = 0.021) and HDT 3 d (P = 0.024). However, no significant changes were observed in the bilateral CCAs, ICAs, ECAs, right VA, or overall intracranial BFV across all time points (P > 0.05).
L left, R right, ICA internal carotid artery, VA vertebral artery, BFV blood flow volume, Pre-HDT pre-adaptation period prior to head-down tilt, HDT head-down tilt, R+ recovery time, d day.
Trends in BFV-related parameters in different vessels
BFV-related parameters varied among different vessels and across time points (Table 2). The following sections present a detailed analysis of the trends in changes in the arterial blood flow parameters of peak systolic flow velocity (Vs), end diastolic flow velocity (Vd), mean peak blood flow velocity (Vm-max), and diameter (D) measured by ultrasound.
Bilateral CCAs parameters
The left CCA predominantly showed variations in D, peaking at HDT 0.5 d. A significant increase was observed from pre-HDT to HDT 0.5 d (P = 0.019), followed by a gradual decline during recovery. Significant decreases were observed between HDT 0.5 d and the recovery phase and between HDT 7 d and R + 5 d (P = 0.024). Vs increased significantly from HDT 0.5 d to R + 3 d (P = 0.0080), whereas fluctuations were observed at other time points without notable changes. The right CCA showed a significant decrease in Vd between HDT 7 d and R + 1 d (P = 0.022). Vm-max increased from HDT 3 d to R + 5 d (P = 0.049) and between R + 1 d and R + 5 d (P = 0.036). D significantly declined from HDT 0.5 d to R + 5 d (P = 0.007), whereas the other parameters did not significantly change.
Bilateral ICAs parameters
Among the assessed parameters, blood flow velocity changes were most pronounced in the bilateral ICAs (Fig. 2). Specifically, velocity decreased during BR and returned to baseline by the third day of recovery. For the left ICA, Vs increased significantly from HDT 3 d to R + 3 d (P = 0.0165) and from HDT 7 d to R + 3 d (P = 0.012). Similarly, Vm-max substantially increased from HDT 3 d to R + 5 d (P = 0.028). For the right ICA, Vs increased significantly from HDT 3 d to R + 3 d (P = 0.021) and from HDT 7 d to R + 3 d (P = 0.010). Additionally, Vm-max exhibited a substantial increase from HDT 1 d to R + 3 d (P = 0.024) and from HDT 7 d to R + 3 d (P = 0.039). Regarding D, only the right ICA showed a significant decline from HDT 0.5 d to R + 5 d (P = 0.010) across multiple time points, whereas the left ICA remained unchanged.
L left, R right, ICA internal carotid artery, VA vertebral artery, Vs peak systolic flow velocity, Vm-max mean peak blood flow velocity, Pre-HDT pre-adaptation period prior to head-down tilt, HDT head-down tilt, R+ recovery time, d day.
Bilateral ECAs parameters
The bilateral ECAs remained largely stable across all time points and parameters. However, the left ECA exhibited significant reductions in D, with decreases observed from HDT 1 d to R + 5 d (P = 0.003) and from HDT 7 d to R + 5 d (P = 0.015). In contrast, no significant changes were observed in any parameter for the right ECA across all time points.
Bilateral VAs parameters
Among all the assessed vessels, the left VA exhibited the most pronounced fluctuations in blood flow velocity, with reductions during BR and recovery to baseline levels by R + 3 d, as illustrated in Fig. 3. Vs decreased significantly from pre-HDT to HDT 0.5 d (P = 0.002), HDT 3 d (P = 0.003), and HDT 7 d (P = 0.013). However, it subsequently increased from HDT 0.5 d to R + 3 d (P = 0.0071), HDT 3 d to R + 3 d (P = 0.0129), and HDT 7 d to R + 3 d (P = 0.046). Vd declined significantly from pre-HDT to HDT 3 d (P = 0.024) and R + 1 d (P = 0.006) but increased from R + 1 d to R + 3 d (P = 0.044). Vm-max consistently decreased from pre-HDT to HDT 0.5 d (P = 0.001), HDT 3 d (P = 0.002), HDT 7 d (P = 0.027), and R + 1 d (P = 0.088). However, it significantly increased from HDT 0.5 d and HDT 3 d to R + 3 d (P = 0.013, 0.020). In contrast, the right VA demonstrated relatively stable blood flow velocities, with only Vs showing a significant increase from HDT 3 d to R + 5 d (P = 0.012, Fig. 3).
L left, R right, VA vertebral artery, Vs peak systolic flow velocity, Vd end diastolic flow velocity, Vm-max mean peak blood flow velocity, Pre-HDT pre-adaptation period prior to head-down tilt, HDT head-down tilt, R+ recovery time, d day.
Based on VA dominance subgroups, the left-dominant group showed a significant decrease in Vs, Vd, Vm-max, and BFV of the left VA at HDT 0.5 d compared to baseline (p < 0.05). No significant changes were observed in the right-dominant or balanced groups. For the right VA, none of the three subgroups exhibited significant changes in any parameters across all time points. Details are presented in Table 3.
Relationships between physiological data and decreases in BFV
The results of the binary logistic regression analysis (Table 4) indicated that right VA dominance, HR, and MAP measured at HDT 3 d were associated with a decrease in BFV of the left VA at HDT 3 d. In contrast, age, BMI, as well as baseline HR and MAP, were not significantly correlated. Specifically, right VA dominance (P = 0.026, OR = 59.314) was significantly associated with a decrease in BFV at HDT 3 d. Additionally, although the mean/median HR decreased at the group level from baseline to HDT 3 d, individuals with relatively higher HR at HDT 3 d were more likely to exhibit a reduction in left VA BFV (P = 0.041). Similarly, elevated MAP at HDT 3 d (P = 0.042) may have contributed to the observed reduction in BFV. However, these physiological factors did not correlate with a decrease in BFV at HDT 0.5 d.
Discussion
This study provides a comprehensive analysis of cervical vessel hemodynamics during 7-day −6° HDT BR, revealing heterogeneous and lateralized vascular responses under simulated microgravity. By systematically evaluating all major cervical vessels (bilateral CCAs, ICAs, ECAs, and VAs) across multiple time points, this study addresses a critical research gap. These findings enhance the current understanding of CBF regulation in microgravity. Our findings highlight three key insights. First, the cervical vessels exhibited distinct hemodynamic changes during the −6° HDT and recovery phases. The left VA presented the most pronounced reduction in BFV and velocity, whereas the right VA remained stable, suggesting the lateralization induced by simulated microgravity. The CCAs and ICAs exhibited a general decline in velocity, along with minimal diameter fluctuations, whereas no statistically significant difference was observed in the ECAs. Second, despite localized changes, overall intracranial BFV, as well as BFV in the right VA and bilateral CCAs, ICAs, and ECAs, remained stable, indicating an adaptive mechanism for maintaining cerebral perfusion under short-term simulated microgravity. Third, physiological factors, including right VA dominance, relatively higher individual HR, and elevated MAP at HDT 3 d, were significantly associated with a decrease in BFV in the left VA at the same time point, even though the mean/median HR decreased at the group level.
As a reflection of the body’s fundamental physiological status, systemic cardiovascular changes during HDT should be considered when interpreting alterations in cervical hemodynamics. In the present study, we observed a progressive decrease in HR and a significant increase in DBP and MAP during the HDT period, particularly evident at HDT 7 d. Consistent with our findings, Liang et al. reported that mean HR decreased immediately at the beginning of a 45-day −6° HDT BR28. Similarly, Hirayanagi et al. observed a significant reduction in HR after 6 h of HDT29. The reduction in HR may be associated with the slight inhibition of sympathetic activity during HDBR30, which in turn affects autonomic nervous system function28. With regard to blood pressure, findings under microgravity conditions have been inconsistent, with reports indicating no change, an increase, or a decrease across different studies25,29,31,32,33,34. These discrepancies may be attributed to differences in experimental models and methodologies, including actual spaceflight and ground-based simulated microgravity, such as HDT BR and dry immersion. In a study involving Asian male participants undergoing HDT BR, the MAP gradually increased until day 56 of −6° HDT BR, potentially due to changes in hydrostatic pressure, cardiac preload and afterload, neural activity, and arterial baroreflex function34. Taken together, these systemic cardiovascular responses represent compensatory adjustments to the HDT BR and provide a broader physiological context for understanding cervical vessel dynamics under simulated microgravity.
The bilateral ICAs are directly associated with anterior cerebral circulation, whereas the CCAs and ECAs are indirectly involved. Previous studies on cervical vessels under microgravity have focused predominantly on ICAs, whereas studies investigating CCAs and ECAs remain limited. Furthermore, the existing results are inconsistent across studies. Consistent with our finding that ICAs blood flow velocity decreases during BR, a phase-contrast magnetic resonance imaging (MRI) study involving nine healthy males revealed that ICA velocity decreased from 22.4 ± 4.3 cm/s at 0° to 18.3 ± 6.13 cm/s at −6° with 1.5 h of HDT (P = 0.01)35. In contrast to our finding that the ICAs BFV remained relatively stable during BR, Possnig et al. reported a significant decline in right ICA BFV by day 3 of a 3-day HDT BR study in 17 participants (10 males and 7 females) via duplex ultrasonography (P < 0.05)22. In line with our findings, a study using ultrasonography to measure BFV in the right CCA, ICA, and ECA in 10 healthy male participants undergoing 3 days of head-out dry immersion reported no significant changes in BFV during or after the intervention23. These inconsistencies may result from variations in study design (e.g., duration and type of microgravity simulation), participant characteristics (e.g., sex and physiological differences), and measurement techniques (e.g., TCD, ultrasound, or MRI). Collectively, the current evidence suggests that microgravity has complex and heterogeneous effects on cervical hemodynamics, necessitating further investigation into the underlying regulatory mechanisms involved.
Anatomically, the vertebrobasilar system, which forms the posterior cerebral circulation, supplies the medulla oblongata and is more closely linked to dizziness, presyncopal symptoms, and autonomic dysfunction than the anterior circulation36,37,38,39,40. Therefore, symptoms commonly experienced by astronauts in microgravity, such as dizziness, balance disorders, and orthostatic intolerance, may be more closely associated with a reduced posterior CBF than with anterior blood flow19. However, prior research has seldom addressed VAs. The VAs exhibited the most pronounced hemodynamic changes among the cervical vessels in this study, with the most evident lateralization. The significant reduction in BFV in the left VA from baseline to both HDT 0.5 d and HDT 3 d suggests a greater sensitivity to microgravity-induced blood flow redistribution than does the relatively stable right VA. Consistent with our findings, Possnig et al. used duplex ultrasonography to examine BFV changes in the VA during 3-day HDT BR and observed a significant reduction after 3 days of BR (P < 0.05)22. Our findings suggest that early blood flow changes in astronauts under the influence of microgravity, as well as potential side-specific differences, particularly in the left VA, warrant close monitoring. Further research is needed to explore the mechanisms underlying these vessel-specific responses and their implications for astronaut health during prolonged space missions.
The regulation of CBF involves multiple factors, including arterial blood pressure, cerebrovascular autoregulation, endothelial function, and regional metabolic activity7,41. In this study, despite fluctuations in left VA BFV under microgravity, overall intracranial blood flow remained stable. Studies on the effects of short-term microgravity on total intracranial blood flow are limited. Inconsistent with our findings, Possnig et al. estimated the total CBF by multiplying the mean blood velocity of the right ICA and VA by the vessel cross-sectional area and then doubling the value to represent both sides22. The results revealed a significant decline in total CBF, from 1078 ± 302 to 853 ± 245 mL/min, after 3 days of BR (P < 0.0001). We speculate that neglecting potential heterogeneity in the left-sided vessels may have affected the results. Future research should consider incorporating multidimensional blood flow measurements and dynamic monitoring, leveraging large-scale datasets to elucidate the mechanisms underlying blood flow homeostasis and enhance our comprehensive understanding of cerebral perfusion.
Our study revealed a significant reduction in BFV in the left VA during the HDT BR period, which was influenced primarily by right VA dominance, as well as relatively higher individual HR and increased MAP at HDT 3 d. VA dominance refers to the asymmetry between the left and right VAs, where one artery is more developed or has a larger diameter than the other42. The identification of right VA dominance underscores the role of vascular laterality in regulating blood flow, which may have contributed to the observed reduction in left VA BFV. This phenomenon can be explained from the perspective of vascular resistance and local physiological regulation. In cases of right VA dominance, the left VA has a smaller caliber, corresponding to higher vascular resistance43. Additionally, smaller vessels are more susceptible to the influence of the sympathetic nervous system, leading to vasoconstriction that further exacerbates reductions in blood flow44,45. Although right VA dominance was identified as a significant factor associated with left VA BFV reduction in the multivariate logistic regression model, subgroup analysis revealed that left VA BFV reduction also occurred in left-dominant individuals. This suggests that dominance may be a marker of underlying vascular asymmetry but not necessarily a causal determinant. Rather, the left VA may inherently exhibit greater physiological responsiveness to posture-induced changes, regardless of dominance configuration. These interpretations should be considered with caution, given the unequal subgroup sizes and potential variability in within-group responses, which may affect the statistical power of subgroup comparisons. The observed association between right VA dominance and reduced left VA BFV further implies that VA dominance may reflect individual variability in vascular adaptation to simulated microgravity. While our study did not directly assess symptoms such as balance disturbances or orthostatic intolerance, this anatomical feature could potentially serve as a physiological marker of susceptibility to microgravity-induced dysfunction. Future research may consider exploratory analyses of VA dominance as a potential marker in astronaut candidate screening and its relevance to spaceflight-related physiological adaptations. In addition to structural asymmetry, autonomic regulation also plays a critical role. Increased HR can affect the cardiovascular system by shortening the diastolic filling time, potentially reducing vascular perfusion46,47. Additionally, a higher HR may reflect heightened sympathetic nervous system activity, which is often linked to cerebral vasoconstriction, particularly in smaller-caliber vessels48,49. According to Ohm’s law, VBF is inversely proportional to vascular resistance50. Thus, vasoconstrictive responses may further contribute to BFV reductions. Similarly, elevated MAP may indicate increased vasoconstriction, particularly in smaller-caliber arteries, thereby reducing BFV51,52. Although this is generally attributed to systemic vascular responses, it is important to note that cerebral vessels possess autoregulatory mechanisms that may respond differently1,53. In our study, the VA was assessed at the V2 segment, which is extracranial but functionally contributes to posterior cerebral circulation and is influenced by both systemic hemodynamics and local regulatory responses. The observed reduction in left VA BFV, despite stable total intracranial flow, therefore speculated to suggest a vessel-specific alteration rather than generalized cerebrovascular constriction. Further studies are warranted to elucidate the underlying mechanisms of this lateralized vascular response under simulated microgravity, including the interplay between structural asymmetry, autonomic regulation, and local hemodynamic control.
This study has several limitations. First, the cohort consisted of relatively young, male participants, which may limit generalizability across age and sex groups. Second, the 7-day HDT BR duration reflects short-term adaptations and does not capture longer-term effects. Third, ultrasound assessments were performed in different postures across phases (−6° HDT during BR vs. 0° supine during pre- and recovery periods), which may have influenced vascular parameters. Moreover, despite employing standardized imaging protocols and ensuring that the same sonologist examined each participant, slight variation in insonation level across time points, which may have affected measurements of vessel diameter and flow velocity, could not be entirely excluded. This is particularly relevant for the V2 segment of the VA, which was insonated approximately at the same horizontal level as the CCAs. Fourth, while ultrasound provided reliable assessments of cervical vessels, multi-modal imaging (e.g., MRI) could offer complementary insights into intracranial circulation. Finally, symptom-related data (e.g., dizziness or discomfort) were not systematically recorded, limiting our ability to assess the functional relevance of hemodynamic changes. Future studies should incorporate multi-modal imaging, standardized symptom monitoring, and larger, more diverse cohorts, with balanced sex distribution, broader age ranges, and extended HDT durations, to better reflect astronaut demographics and to capture progressive and functional cerebrovascular changes. In addition, the integration of advanced tools such as machine learning may further improve the prediction and interpretation of cerebrovascular dynamics, facilitating more personalized risk assessment and countermeasure development in future spaceflight settings.
In conclusion, this study comprehensively analyzed cervical vessel hemodynamics during 7-day −6° HDT BR, highlighting the heterogeneous and lateralized vascular responses. The left VA exhibited significant reductions in BFV and velocity fluctuations, whereas the right VA remained stable. Overall, BFV in the right VA, CCAs, ICAs, ECAs, and total intracranial remained stable despite some changes in flow velocity and vessel diameter under short-term simulated microgravity. The key factors associated with left VA BFV reduction included right VA dominance, along with relatively higher individual HR and increased MAP at HDT 3 d. These findings provide critical insights into CBF regulation under simulated microgravity, highlighting the role of vascular asymmetry in adaptation. By integrating available astronaut cervical vascular ultrasound data collected before, during, and after spaceflight, we can compare real and simulated responses, supporting personalized monitoring to safeguard astronaut health in the future.
Methods
Study participants
This study was a controlled 7-day −6° HDT BR cohort study. Forty-four healthy, non-smoking Asian male volunteers were initially recruited following rigorous physical and psychological evaluations. The exclusion criteria were as follows: individuals with (1) hypertension; (2) cervical vascular plaques; (3) neurological, cardiovascular, psychiatric, or infectious diseases; (4) severe musculoskeletal or cardiovascular conditions or other significant medical conditions; and (5) morphological abnormalities of the VA, such as focal stenosis, tortuosity, or segmental dilatation, as identified by ultrasound screening. The final cohort comprised 40 participants, 4 of whom were unable to tolerate 7 consecutive days of bed confinement and were subsequently excluded. The experimental protocol was approved by the Research Ethics Committee of Beijing Friendship Hospital, affiliated with Capital Medical University (2024-P2-069-04), and was registered under ChiCTR2500096128. Before participation, all volunteers received a detailed explanation of the study procedures and potential risks, and written informed consent was obtained. The study adhered to the principles of the Declaration of Helsinki and standard clinical practice guidelines.
Study design and procedure
Figure 4 illustrates the study flowchart. Before the experiment, the participants underwent a 2- to 3-day pre-adaptation period to acclimate them to activities such as eating, drinking, defecation, and urination while lying on a 0° tilt bed, ensuring feasibility for the HDT BR study. During the experiment, the participants maintained a strict −6° HDT position without pillows for 7 consecutive days, performing nearly all daily activities in this posture under continuous 24-h video surveillance to ensure compliance. The recovery period lasted 5 days, during which the participants gradually transitioned from lying flat to sitting upright, standing, and walking. Throughout the study and recovery period, the participants adhered to a controlled daily routine and diet. During the experiment, designated personnel from the experimental team provided psychosocial support to the volunteers.
Pre-HDT pre-adaptation period prior to head-down tilt bed rest, HDT BR head-down tilt bed rest, R+ recovery time, d day.
HR, SBP, and DBP were recorded using an electronic sphygmomanometer (HBP-1300, Omron, Dalian, China) over the right brachial artery; measurements were taken at the heart level while the participants remained supine. The MAP was calculated using the following formula. \({\rm{MAP}}({\rm{mmHg}})=\left(1/3\times {\rm{SBP}}\right)+\left(2/3\times {\rm{DBP}}\right)\). The PP was determined as follows: \({\rm{PP}}({\rm{mmHg}})={\rm{SBP}}-{\rm{DBP}}\). SpO2 was recorded via a portable pulse oximeter (PM10N; Covidien, MA, USA).
Ultrasound data acquisition and image analysis
Blood flow data from cervical vessels were obtained using a portable pulse-wave Doppler ultrasound device (X5, SonoScape, Shenzhen, China) with a probe frequency of 4.0–16.0 MHz. All ultrasound examinations were performed by two experienced sonologists (Fengxia Yu [FY] and Xia Ma [XM]). For each participant, all repeated scans across different time points were conducted by the same sonologist to ensure intra-subject consistency. During the HDT BR phase, all ultrasound measurements were performed while participants maintained the −6° HDT position. Meanwhile, measurements during the pre-HDT and recovery phases were conducted in the supine position (0° tilt). This ensured that the assessments during HDT BR reflected the physiological state under simulated microgravity.
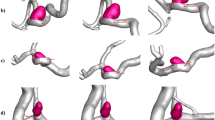
This study employed standardized ultrasound examination protocols to assess the cervical blood vessels, ensuring high-quality imaging and data consistency. Before examination, the participants removed their neck accessories and assumed the supine position to expose and relax the neck region. During the procedure, the participants tilted their heads slightly backward and gently turned them to the contralateral side, ensuring neck muscles relaxation while maintaining a comfortable posture. Ultrasound was performed to assess the bilateral CCAs, ICAs, ECAs, and VAs. Two-dimensional imaging was used to measure the vascular D at specific anatomical sites: 1.0–1.5 cm proximal to the bifurcation of the CCA, 1.0–1.5 cm distal to the ICA origin, 1.0–1.5 cm distal to the ECA origin, and at the V2 segment of the VA, approximately at the same horizontal level as the CCA measurement site. To ensure measurement precision, the images were magnified for clear visualization of the vessel walls and lumen. A VA was considered dominant if its diameter exceeded that of the contralateral VA by at least 0.3 mm54 (Fig. 5). Pulsed wave (PW) Doppler imaging and measurements were conducted at the same locations as those used for the two-dimensional diameter assessments. The beam-vessel angle was adjusted to <60°, with the sampling volume covering the entire lumen and the sampling line positioned at the center of the lumen. PW images were recorded and accompanied by three dynamic video clips (each 2 s long) and saved for analysis. Before analyses, spectral data were preprocessed, including the removal of improperly acquired or noise-affected data. The spectral data sequence was trimmed to generate complete periodic subseries. To improve data quality, sequence averaging and low-pass filtering were employed to reduce noise and eliminate outliers.
The scan shows the bilateral VA diameters in the participant with left VA dominance. VA vertebral artery, L left, R right, D diameter.
The key hemodynamic parameters, including Vs, Vd, and Vm-max, were extracted from the blood flow data (Fig. 6). Vs (cm/s) represents the peak blood flow velocity during systole, whereas Vd (cm/s) corresponds to the blood flow velocity at the end of diastole. Both values were calculated as averages over multiple cardiac cycles and automatically derived from blood flow data. \({\rm{Vm}}-\max ({\rm{cm}}/{\rm{s}})={\int }_{{\rm{i}}=1}^{{\rm{n}}}{{\rm{v}}}_{{\rm{i}}}/{\rm{n}}\), where Vi is the peak blood flow velocity at each sampling point during a cardiac cycle, and n is the number of sampling points. Vm-max represents the average peak flow velocity over the cardiac cycle, integrating both the systolic and diastolic phases. When multiplied by a correction factor of 0.5, Vm-max approximates the mean blood flow velocity (Vm), in cm/s. BFV, defined as the volume of blood passing through a specific vessel cross-section per minute, was calculated as \({\rm{BFV}}({\rm{ml}}/\min )={\rm{\pi }}\times {\left({\rm{D}}/2\right)}^{2}\times {\rm{Vm}}\times 60/100\), with D in mm. Total intracranial blood flow was determined as the sum of the blood flow from the bilateral ICAs and VAs.
Hemodynamic features of the ICA from a left ICA ultrasound Doppler image of the participant. ICA internal carotid artery.
Statistical analysis
All data were analyzed using SPSS (version 20.0; IBM Corp., Armonk, NY, USA). Data normality was assessed using the Shapiro–Wilk test. Normally distributed data are presented as mean ± standard deviation, and non-normally distributed data are presented as the median (lower quartile, upper quartile). To analyze differences between measurements at different time points, we selected differential statistical tests depending on the data distribution. For normally distributed data, repeated-measures analysis of variance was performed, followed by Tukey’s honestly significant difference test for post hoc analysis if the analysis of variance results were significant. For non-normally distributed data, the Friedman test was performed, followed by Dunn’s test for post hoc comparisons when significant differences were detected. Multivariate logistic regression was used to assess the associations between changes in BFV, treated as a binary dependent variable, and physiological parameters (independent variables) during the study period, relative to pre-HDT results. The BFV at each time point was labeled as 1 if it exceeded the pre-HDT values and 0 otherwise. To minimize the impact of confounding factors, including age, BMI, and VA dominance, these variables were included as independent variables in the regression model with categorical settings. Statistical significance was set at a P value of <0.05.
Data availability
The data that support the findings of this study are available from the corresponding authors upon reasonable request.
References
Claassen, J., Thijssen, D., Panerai, R. B. & Faraci, F. M. Regulation of cerebral blood flow in humans: physiology and clinical implications of autoregulation. Physiol. Rev. 101, 1487–1559 (2021).
Jiang-Xie, L. F., Drieu, A. & Kipnis, J. Waste clearance shapes aging brain health. Neuron 113, 71–81 (2025).
Hochberg, A. R. & Young, G. S. Cerebral perfusion imaging. Semin. Neurol. 32, 454–465 (2012).
Wu, D. et al. Trajectories and sex differences of brain structure, oxygenation and perfusion functions in normal aging. Neuroimage 302, 120903 (2024).
Gupta, U., Baig, S., Majid, A. & Bell, S. M. The neurology of space flight; How does space flight effect the human nervous system?. Life Sci. Space Res. 36, 105–115 (2023).
Hupfeld, K. E., Mcgregor, H. R., Reuter-Lorenz, P. A. & Seidler, R. D. Microgravity effects on the human brain and behavior: dysfunction and adaptive plasticity. Neurosci. Biobehav. Rev. 122, 176–189 (2021).
Du, J. et al. Alterations in cerebral hemodynamics during microgravity: a literature review. Med. Sci. Monitor 27, e928108 (2021).
Cai, L. et al. A machine learning approach to predict cerebral perfusion status based on internal carotid artery blood flow. Comput. Biol. Med. 164, 107264 (2023).
Rosner, J., Reddy, V. & Lui, F. Neuroanatomy, circle of willis. In: StatPearls. StatPearls Publishing, Treasure Island (FL). Available at: https://europepmc.org/article/NBK/nbk534861 (2023).
Willie, C. K., Tzeng, Y. C., Fisher, J. A. & Ainslie, P. N. Integrative regulation of human brain blood flow. J. Physiol.592, 841–859 (2014).
Giotta, L. A. et al. Microsurgical neurovascular anatomy of the brain: the anterior circulation (Part I). Acta Biomed. 92, e2021412 (2021).
Jobson, D. D., Hase, Y., Clarkson, A. N. & Kalaria, R. N. The role of the medial prefrontal cortex in cognition, ageing and dementia. Brain Commun. 3, fcab125 (2021).
Pierce, J. E. & Peron, J. The basal ganglia and the cerebellum in human emotion. Soc. Cogn. Affect. Neurosci. 15, 599–613 (2020).
Palejwala, A. H. et al. Anatomy and white matter connections of the lateral occipital cortex. Surg. Radiol. Anat. 42, 315–328 (2020).
Giotta, L. A. et al. Microsurgical neurovascular anatomy of the brain: the posterior circulation (part ii). Acta Biomed. 92, e2021413 (2021).
Marshall, I., Papathanasopoulou, P. & Wartolowska, K. Carotid flow rates and flow division at the bifurcation in healthy volunteers. Physiol. Meas. 25, 691–697 (2004).
Yu, F. et al. Dobutamine-induced alterations in internal carotid artery blood flow and cerebral blood flow in healthy adults. Brain Res. Bull. 221, 111204 (2025).
Zhang, T. et al. Dobutamine-induced alternations in cerebral blood flow of healthy adults: a 3d pseudocontinuous arterial spin labeling study. BMC Med. 21, 238 (2023).
Ogoh, S., Sato, K., de Abreu, S., Denise, P. & Normand, H. Arterial and venous cerebral blood flow responses to long-term head-down bed rest in male volunteers. Exp. Physiol. 105, 44–52 (2020).
Hashimoto, T. et al. Maintained exercise-enhanced brain executive function related to cerebral lactate metabolism in men. FASEB J. 32, 1417–1427 (2018).
Iwasaki, K. et al. Human cerebral autoregulation before, during and after spaceflight. J. Physiol.579, 799–810 (2007).
Possnig, C. et al. Regional changes in cerebral blood flow between the upright and supine posture and over 3 days of bed rest. Exp. Physiol. https://physoc.onlinelibrary.wiley.com/doi/full/10.1113/EP091820 (2025).
Ogoh, S., Hirasawa, A., de Abreu, S., Denise, P. & Normand, H. Internal carotid, external carotid and vertebral artery blood flow responses to 3 days of head-out dry immersion. Exp. Physiol. 102, 1278–1287 (2017).
Klein, T. et al. The influence of microgravity on cerebral blood flow and electrocortical activity. Exp. Brain Res. 237, 1057–1062 (2019).
Amirova, L. et al. Cardiovascular system under simulated weightlessness: head-down bed rest vs. dry immersion. Front. Physiol. 11, 395 (2020).
Boutouyrie, P. et al. Impact of 60 days of head-down bed rest on large arteries. J. Hypertens. 40, 2058–2067 (2022).
Kramer, L. A. et al. Artificial gravity: an effective countermeasure for microgravity-induced headward fluid shift?. J. Appl. Physiol. 137, 1071–1081 (2024).
Liang, X. et al. Effects of a 45-day head-down bed rest on the diurnal rhythms of activity, sleep, and heart rate. Biol. Rhythm Res. 45, 591–601 (2014).
Hirayanagi, K. et al. Autonomic cardiovascular changes during and after 14 days of head-down bed rest. Auton. Neurosci. 110, 121–128 (2004).
Shiraishi, M. et al. Blood pressure variability during 120-day head-down bed rest in humans. Biomed. Pharmacother. 57(Suppl 1), 35s–38s (2003).
Baevsky, R. M. et al. Autonomic cardiovascular and respiratory control during prolonged spaceflights aboard the international space station. J. Appl. Physiol. 103, 156–161 (2007).
Modak, S. & Banerjee, P. K. Studies of left ventricular functions by systolic time intervals on exposure to dry immersion. Indian J. Aerosp. Med. 48, 48–56 (2004).
Borovik, A. S., Orlova, E. A., Tomilovskaya, E. S., Tarasova, O. S. & Vinogradova, O. L. Phase coupling between baroreflex oscillations of blood pressure and heart rate changes in 21-day dry immersion. Front. Physiol. 11, 455 (2020).
Liu, J. et al. Orthostatic intolerance is independent of the degree of autonomic cardiovascular adaptation after 60 days of head-down bed rest. Biomed. Res. Int. 2015, 896372 (2015).
Marshall-Goebel, K. et al. Effects of short-term exposure to head-down tilt on cerebral hemodynamics: a prospective evaluation of a spaceflight analog using phase-contrast MRI. J. Appl. Physiol. 120, 1466–1473 (2016).
Al Aiyan, A. et al. Vertebrobasilar contribution to cerebral arterial system of dromedary camels (Camelus dromedarius). Front. Vet. Sci. 8, 696707 (2021).
Sciacca, S., Lynch, J., Davagnanam, I. & Barker, R. Midbrain, pons, and medulla: anatomy and syndromes. Radiographics 39, 1110–1125 (2019).
Zhang, Y., Zhang, L. & Wang, J. Analysis of prognosis of infarction in different areas of medulla oblongata. J. Apoplexy Nerv. Dis. 37, 623–628 (2020).
Memmedova, F. et al. Progression rates of medulla oblongata infarcts in clinical follow-up: a retrospective study. Clin. Neurol. Neurosurg. 219, 107329 (2022).
Iordanova, R. & Reddivari, A. K. R. Neuroanatomy, Medulla Oblongata (StatPearls Publishing, 2025).
Aaslid, R. Cerebral autoregulation and vasomotor reactivity. Front. Neurol. Neurosci. 21, 216–228 (2006).
Vural, A. & Derin, C. E. Is the asymmetry between the vertebral arteries related to cerebral dominance?. Turk. J. Med. Sci. 49, 1721–1726 (2019).
Mahajan, S. et al. Hemodynamic phenotypes of hypertension based on cardiac output and systemic vascular resistance. Am. J. Med. 133, e127–e139 (2020).
Aalkjaer, C., Nilsson, H. & De Mey, J. Sympathetic and sensory-motor nerves in peripheral small arteries. Physiol. Rev. 101, 495–544 (2021).
Chen, S. P. & Wang, S. J. Pathophysiology of reversible cerebral vasoconstriction syndrome. J. Biomed. Sci. 29, 72 (2022).
Kagami, K. et al. Diastolic filling time, chronotropic response, and exercise capacity in heart failure and preserved ejection fraction with sinus rhythm. J. Am. Heart Assoc. 11, e26009 (2022).
Namani, R. et al. Effects of myocardial function and systemic circulation on regional coronary perfusion. J. Appl. Physiol. 128, 1106–1122 (2020).
Esler, M. et al. Evaluation of elevated heart rate as a sympathetic nervous system biomarker in essential hypertension. J. Hypertens. 38, 1488–1495 (2020).
Koep, J. L. et al. Autonomic control of cerebral blood flow: fundamental comparisons between peripheral and cerebrovascular circulations in humans. J. Physiol.600, 15–39 (2022).
Widrich, J. & Shetty, M. Physiology, pulmonary vascular resistance. StatPearls [Internet]. StatPearls Publishing. Available at: https://www.ncbi.nlm.nih.gov/sites/books/NBK554380/ (2024).
Moller, P. W. et al. The effects of vasoconstriction and volume expansion on veno-arterial ECMO flow. Shock 51, 650–658 (2019).
Lankadeva, Y. R., May, C. N., Bellomo, R. & Evans, R. G. Role of perioperative hypotension in postoperative acute kidney injury: a narrative review. Br. J. Anaesth. 128, 931–948 (2022).
Franco, F. A. Cerebral autoregulation and syncope. Prog. Cardiovasc. Dis. 50, 49–80 (2007).
Jeng, J. S. & Yip, P. K. Evaluation of vertebral artery hypoplasia and asymmetry by color-coded duplex ultrasonography. Ultrasound Med. Biol. 30, 605–609 (2004).
Acknowledgements
This study was supported by grants from the Space Medical Experiment Project of the China Manned Space Program [No. HYZHXMH01005]; Beijing Hospital Authority Innovation Studio of Young Staff Funding Support [No. 202302]; Beijing Postdoctoral Research Foundation; the postdoctoral launch project of the Beijing Friendship Hospital, Capital Medical University (No. yybsh2024002); Beijing Scholar 2015 [Z.W.]. The authors sincerely thank all the volunteers who participated in this study. The authors would like to thank Editage (www.editage.cn) for English language editing.
Author information
Authors and Affiliations
Contributions
F.Y., X.M., Y.L., R.W. and J.Z. conducted the experiments and collected the data. F.Y., Z.H., Y.W. and W.Z. analyzed and interpreted the data. F.Y. drafted the initial manuscript. P.Q., R.D., L.Q. and Z.C. contributed to the study design and coordination, supervised the overall study, and provided critical feedback. Z.W. and P.R. revised the draft article and secured financial funding for the project. All the authors have read and approved the final version of the manuscript. They agree to be accountable for all aspects of the work. All individuals listed meet the criteria for authorship, and all those who qualify for authorship are included.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Yu, F., Ma, X., Liu, Y. et al. Heterogeneous and lateralized cervical vascular responses to a 7-day head-down tilt bed rest. npj Microgravity 11, 70 (2025). https://doi.org/10.1038/s41526-025-00524-6
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41526-025-00524-6