Abstract
Maxillofacial fractures, especially those of the mandible, pose a significant risk in microgravity environments because astronauts experience progressive bone loss during long-duration flights because of skeletal unloading. In this study, we explored the biomechanical response of the mandibular angle to high-impact trauma caused by gravity and microgravity. A human mandibular model was subjected to a force of 2000 N at an angle of 45°, which was directed posterosuperiorly at the right-angle region with simulations comparing healthy and osteoporotic bone (bone loses its density in long flights due to skeletal unloading). The results revealed that although stresses remained the same across all conditions, microgravity caused nearly double the strain and deformation, indicating a high risk of fracture. These findings emphasize the need for biomechanical evaluation and protective strategies in space medicine.
Similar content being viewed by others
Introduction
The maxillofacial region is one of the most exposed parts of the body and is highly susceptible to trauma. Common causes of maxillofacial trauma include falls, traffic accidents, interpersonal violence and sports injuries1. Among all maxillofacial traumas, 42% are attributed to mandibular fractures, which include angle fractures (30%), parasymphysis fractures (27%), condylar fractures (27%), body fractures (9%), symphyseal fractures (4%), ramus fractures (3%), and coronoid fractures ( ≤ 1%)2. The biomechanical integrity of the mandible is necessary for proper speech, mastication and protection of the lower airway, and a fracture disrupts this integrity, making them clinically significant3,4.
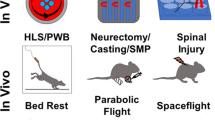
In the context of long-duration spaceflights, fracture biomechanics are more complex. Long exposures to zero gravity/microgravity cause a marked decrease in bone mineral density and disruption of the trabecular pattern due to a condition called spaceflight osteopenia5,6. Studies show that astronauts lose approximately 1–1.5% of their bone mass every month under microgravity conditions because of the absence of mechanical loading, which normally induces bone remodeling7,8. Although not studied extensively, the maxillofacial region is not exempted from these degenerative changes9,10,11.
In addition, there is a risk of traumatic injuries in space, including unintentional collisions with spacecraft equipment, free floating impacts or emergency events. Even minor trauma could have more severe repercussions in spaces where bone weakness is increased and healing is not properly understood12,13. As many space missions extend beyond the low Earth orbit, it is necessary to understand the biomechanics of maxillofacial trauma in microgravity.
With technological advancements, newer methods have been developed to better understand the biomechanics of orthopedic and maxillofacial bones; one such method is finite element analysis (FEA), which is widely used as a predictive tool for evaluating the stress–strain response of bones under various loading conditions14,15,16. The FEA of the mandible has been used to understand fracture risk and fracture fixation stability and to study how occlusal loads are transferred15,16,17. Although FEA studies are highly versatile and efficient, no studies have emphasized the biomechanical behavior of mandible under altered gravitational environments.
To address this gap, this study focused on the use of FEA to compare mandible, specifically the angle subjected to trauma under conditions of gravity and microgravity. Additionally, two different bone qualities of the mandible were used in the present study: a healthy mandible and an osteoporotic mandible. The aim of this study was to evaluate the biomechanical behavior of the mandibular angle under moderate-to-high-impact trauma caused under gravity and microgravity. From the simulations performed on osteoporotic and healthy mandible, we sought to quantify the effects of gravitational unloading on fracture risk, stress distribution, and deformation patterns.
Results
FEA was performed on mandibular models under four distinct conditions. Healthy and osteoporotic bones were tested under Earth’s gravity and microgravity conditions. The results are expressed as the equivalent (von Mises) stress, elastic strain, and total deformation. The summarized results are presented in Table 1.
Under Earth’s gravitational load, both normal and osteoporotic bone possess similar stress values (~1.1 GPa), with less than a 1% difference in deformation and strain. Under microgravity, both the elastic strain and overall deformation nearly doubled compared to those of their Earth counterparts. Despite the increased deformation and strain, the stress values were nearly the same, suggesting that gravity played no role in the internal force distribution but did play a role in the displacement and material extension.
Curiously, osteoporotic bone under microgravity conditions was under lower stress (1.017 × 10⁹ Pa) than healthy bone but with practically the same strain and deformation. This could be indicative of an impaired load-carrying capability due to impaired stiffness and density, demonstrating the vulnerability of impaired bone tissue in low-gravity conditions.
Across all four simulations, the equivalent (von Mises) stress consistently concentrated at the right mandibular angle, corresponding to the site of traumatic loading (Figs. 1, 4, 7, and 10). Peak stresses were localized along the lateral cortical plate and inferior border of the angle, with stress progressively diminishing along the ramus and body. Only minimal stress was transmitted to the contralateral side and condylar region, indicating that the impacted angle served as the principal energy-absorbing zone in all models.
Under Earth’s gravity, both healthy and osteoporotic mandibles exhibited a similar focal stress hotspot at the external cortex of the angle, with limited superior or posterior propagation. Osteoporotic bone did not shift the stress concentration site; instead, reduced material stiffness produced a slightly broader region of intermediate stress surrounding the same anatomical focus.The elastic strain distributions for healthy and osteoporotic mandibles under Earth’s gravity are shown in Figs. 2 and 5. The corresponding total deformation patterns under gravity are illustrated in Figs. 3 and 6.
In microgravity, the overall stress-localization pattern remained centered at the right angle, demonstrating that mandibular geometry and loading direction predominantly defined the stress field. However, both healthy and osteoporotic mandibles showed more diffuse stress contours extending along the inferior border and slightly anteriorly toward the body, coinciding with the nearly doubled elastic strain and total deformation. In osteoporotic bone under microgravity, the peak von Mises stress was modestly lower than in healthy bone, but this occurred alongside a wider distribution of intermediate stress—consistent with the impaired stiffness and reduced capacity of osteoporotic bone to concentrate and carry load.The elastic strain distributions under microgravity for healthy and osteoporotic mandibles are shown in Figs. 8 and 11. The corresponding total deformation patterns are illustrated in Figs. 9 and 12.
Below are the FEA results:
Healthy bone under gravity
Figure 1
Equivalent stress of healthy bone under gravity.
Figure 2
Elastic strain of healthy bone under gravity.
Figure 3.
Total deformation of healthy bone under gravity.
Osteoporotic bone under gravity
Figure 4
Equivalent stress of osteoporotic bone under gravity.
Figure 5
Elastic strain of osteoporotic bone under gravity.
Figure 6
Total deformation of osteoporotic bone under gravity.
Healthy bone under microgravity
Figure 7
Equivalent stress of healthy bone under microgravity.
Figure 8
Elastic strain of healthy bone under microgravity.
Figure 9
Total deformation of healthy bone under microgravity.
Osteoporotic bone under microgravity
Figure 10
Equivalent stress of osteoporotic bone under microgravity.
Figure 11
Elastic strain of osteoporotic bone under microgravity.
Figure 12
Total deformation of osteoporotic bone under microgravity.
Figure 13
Force of 2000 N applied at the right-angle posterosuperiorly at an angle of 45° simulating mandibular angle trauma.
Discussion
This finite element analysis demonstrated that microgravity significantly alters the mandibular biomechanical response to trauma and that the effect is enhanced in osteoporotic bone. We present our findings below in the context of the literature.
Experimental data from postmortem human mandibles indicate that fracture thresholds at the condyle and mandibular angle are approximately 2,800 N under restrained impact loading18,19. Finite element and experimental studies with controlled directions and magnitudes of loading always apply forces of approximately 2,000 N at 45° angulation and induce clinically relevant fracture patterns at the mandible angle20,21. These findings justify our choice of a 2,000 N, posterosuperiorly directed, 45° trauma vector to model moderate-to-severe impacts.
Our finding that elastic strain and deformation nearly doubled under microgravity conditions is consistent with known alterations in the bone response in space. While long bones are well described for microgravity-induced bone loss, craniofacial bones such as the mandible are not immune to loss. Simulated microgravity models have shown substantial reductions in mandibular and alveolar bone density and increased resorption markers in males and females11. Similarly, micro-CT analysis of rodents has shown substantial mandibular microstructure alterations under spaceflight conditions10. In gravity, osteoporotic bones show only a minimal increase in deformation compared to healthy bones because the fixed condyle boundary condition dominates the structural response; the same phenomenon occurs in normal and osteoporotic bone in microgravity, as they do not allow any kind of movement.
Additionally, evidence shows that osteoporosis lowers bone stiffness and density, which renders it more susceptible to deformation during loading. Experimental testing revealed that the cortical bone density in osteoporotic human mandibles was much lower than that in healthy control mandibles, corresponding to a reduced elastic modulus ( < 10 GPa) and bone mineral density. These results favor both the modulus and density differences used by our model22,23,24.
Although the condyles were modelled with rigid boundary conditions, the unilateral impact generated substantial local deformation and stress concentration at the mandibular angle. This localized absorption of energy limited the amount of stress transmitted across the mandibular arch to the contralateral condyle. The observed distribution is therefore a combined outcome of the impact direction, patient-specific geometry, and regional stiffness characteristics rather than an inaccuracy in the reconstructed model.
Most FEA trauma analyses ignore gravity because high-magnitude forces dominate gravity’s effects in brief simulations. However, a comparison of the results suggested that the exclusion of the preload under gravity causes greater displacement and strain under identical external loads. Facial bones do not support weight in the conventional sense, so facial structures react differently when gravity is ignored that is the mandible is more freely mobile, with no counterforce to dissipate impact energy; this removes baseline tissue resistance and allows more deformation.
The microgravity-induced doubling of strain and deformation poses important concerns about fracture tolerance thresholds in astronauts, particularly those with osteopenia due to spaceflight. Even small impact events such as equipment strikes, floating strikes, or inadvertent drops could be beyond the tolerance of weakened craniofacial bones. This compelling evidence supports the use of protective craniofacial equipment, trauma prevention protocols, and prelaunch screening of astronauts for bone mineral density.
This study has several limitations that should be considered when interpreting the results. The mandibular bone in our model was represented as homogeneous and isotropic; incorporating cortical–cancellous differentiation would likely improve the realism of stress localization. Muscle forces were not included, although in vivo they may provide stabilizing preload that influences mandibular response to impact. In addition, the model predicts stress, strain, and displacement but does not simulate true crack initiation or fracture propagation. Experimental validation under actual or simulated microgravity is also lacking, and future cadaveric or in vitro studies may help corroborate these findings. Although the condyles were fully fixed to standardize loading, this boundary condition does not reflect the physiological compliance of the temporomandibular joint and may underestimate differences between normal and osteoporotic mandibles. Microgravity was simulated by removing gravitational acceleration alone and did not account for systemic adaptations such as altered remodeling or fluid shifts that occur during spaceflight. Minor geometric discrepancies may also arise from CT slice thickness, segmentation smoothing, and mesh optimization; however, these do not affect the true anatomical dimensions used in the simulation. Despite these limitations, the model retained accurate cortical and cancellous boundaries and patient-specific geometry, ensuring that the overall mechanical behavior remained physiologically reasonable. Finally, although fixed condylar constraints generally promote broader stress transfer, the impact direction in this study produced substantial local energy absorption at the angle, reducing contralateral stress; alternative loading vectors or TMJ modeling approaches may therefore yield different patterns and warrant further investigation.
Overall, this study examined the biomechanical behavior of mandibular angle fractures under traumatic loading in both Earth gravity and microgravity using finite element analysis. By applying a 2000 N force in a 45° posterosuperior direction to simulate moderate-to-severe impacts, we compared healthy and osteoporotic mandibles and found that stress distribution was largely insensitive to gravity, whereas strain and total deformation nearly doubled in microgravity. In osteoporotic bone, reduced stiffness corresponded with greater deformation, suggesting compounded vulnerability during spaceflight. These findings highlight the importance of gravitational loading in maxillofacial biomechanics and support the need for protective measures and targeted screening to mitigate fracture risk in astronauts during long-duration missions.
Methods
Model acquisition and preparation
A CT scan of a human mandible was obtained as a DICOM file, which was imported to the CAD software Fusion 360 (Autodesk, San Rafael, USA). The 3D volume was converted to a surface mesh so that the entire mandible would be recognized as a solid by FEA software (Ansys, Canonsburg, USA), which was then exported as a STEP file.
Geometric refinements and meshing
The STEP file was imported into ANSYS Workbench 2025 R1 (Ansys, Canonsburg, USA) using SpaceClaim (SpaceClaim Corporation (Ansys), Concord, USA), where geometric refinements and mesh optimizations were performed. Modeling was performed using a tetrahedral patch-independent mesh with an elemental size of 0.3 mm to ensure adequate resolution at structurally significant areas, such as the angle and condyles.
Material properties
Within the enginseering data module of ANSYS (Ansys, Canonsburg, USA), two custom material profiles were created to represent healthy and osteoporotic bones. These materials were assigned the material properties shown in Table 225,26,27,28.
Simulation conditions
The prepared model was then imported to the static structural environment within ANSYS (Ansys, Canonsburg, USA), and four of the following simulations were tested:
-
Healthy bone under Earth’s gravitational force (1 g)
-
Osteoporotic bone under Earth’s gravitational load
-
Healthy bone under microgravity (0 g)
-
Osteoporotic bone under microgravity
In all the patients, fixed supports were applied at the condyles to simulate the temporomandibular joint. For models involving gravity, the standard earth gravity (9.81 m/s²) setting was applied, which resulted in a gravitational force in the negative Z direction.
Microgravity simulation
Microgravity was simulated within ANSYS by disabling the gravitational acceleration component in the environment settings. For the 0 g condition, the standard Earth gravity value (9.81 m/s²) applied in the negative Z-axis was set to zero, resulting in a neutral gravitational field. No additional inertial or centrifugal forces were introduced, ensuring that the model experienced a true gravity-independent load state. This approach follows established finite-element protocols for microgravity approximation, where the absence of gravitational preload allows evaluation of pure load-driven stress distribution in craniofacial structures.
Loading conditions and outcome measures
To simulate trauma, a force of 2000 N at an angle of 45° posterosuperiorly was applied at the right mandibular angle, corresponding to the vector of a moderate to a high impact blow that may occur during interpersonal violence or accidental impact20,21.A schematic representation of the applied load and direction is shown in Fig. 13.
After the boundary conditions were set, the models were solved under linear elastic assumptions, and the outcomes of each simulation were described in terms of
-
Equivalent (von Mises) stress
-
Elastic strain
-
Total deformation
These results were compared to understand the role of bone quality and gravitational forces on mandibular biomechanics during trauma.
Ethics and informed consent statement
This study did not involve human participants, animal experiments, or clinical data. Therefore, ethical approval was not needed.
Data availability
All the data generated or analyzed during this study are included in this published article.
References
Srinivasan, B., Balakrishna, R., Sudarshan, H., Veena, G. & Prabhakar, S. Retrospective analysis of 162 mandibular fractures: an institutional experience. Ann. Maxillofac. Surg. 9, 124 (2019).
Rashid, A., Eyeson, J., Haider, D., van Gijn, D. & Fan, K. Incidence and patterns of mandibular fractures during a 5-year period in a London teaching hospital. Br. J. Oral. Maxillofac. Surg. 51, 794–798 (2013).
Choi, A. H., Conway, R. C., Taraschi, V. & Ben-Nissan, B. Biomechanics and functional distortion of the human mandible. J. Investig. Clin. Dent. 6, 241–251 (2015).
Vijayaraghavan, N. V., Ramesh, G., Thareja, A. & Patil, S. Masticatory efficiency after rehabilitation of acquired maxillary and mandibular defects. Indian J. Dent. 6, 139 (2015).
Man, J., Graham, T., Squires-Donelly, G. & Laslett, A. L. The effects of microgravity on bone structure and function. npj Microgravity 8, 1–15 (2022).
Gabel, L. et al. Incomplete recovery of bone strength and trabecular microarchitecture at the distal tibia 1 year after return from long-duration spaceflight. Sci. Rep. 12, 9446 (2022).
Stavnichuk, M., Mikolajewicz, N., Corlett, T., Morris, M. & Komarova, S. V. A systematic review and meta-analysis of bone loss in space travelers. npj Microgravity 6, 5 (2020).
Baran, R. et al. Microgravity-related changes in bone density and treatment options: a systematic review. Int. J. Mol. Sci. 23, 8650 (2022).
Moussa, M. S., Goldsmith, M. & Komarova, S. V. Craniofacial bones and teeth in spacefarers: systematic review and meta-analysis. JDR Clin. Trans. Res. 7, 238008442210849 (2022).
Ghosh, P., Stabley, J. N., Behnke, J. B., Allen, M. R. & Delp, M. D. Effects of spaceflight on the murine mandible: possible factors mediating skeletal changes in non-weight-bearing bones of the head. Bone 83, 156–161 (2016).
Rai, B., Kaur, J. & Catalina, M. Bone mineral density, bone mineral content, gingival crevicular fluid biomarkers and osteocalcin levels in human mandible and alveolar bone under simulated microgravity. J. Oral. Sci. 52, 385–390 (2010).
National Academies of Sciences, Engineering, and Medicine. Review of NASA’s Evidence Reports on Human Health Risks. (National Academies Press, 2018).
Kirchen, M. E. et al. Effects of microgravity on bone healing in a rat fibular osteotomy model. Aviat. Space Environ. Med. 66, 231–242 (1995).
Lisiak-Myszke, M. et al. Application of finite element analysis in oral and maxillofacial surgery: a literature review. Materials 13, 3063 (2020).
Hedeșiu, M. et al. Three-dimensional finite element analysis on mandibular biomechanics simulation under normal and traumatic conditions. Oral 2, 221–237 (2022).
Wang, H. et al. Three-dimensional finite element analysis of mechanical stress in symphyseal fractured human mandible reduced with miniplates during mastication. J. Oral. Maxillofac. Surg. 68, 1585–1592 (2010).
Arbag, H., Korkmaz, H. H., Ozturk, K. & Uyar, Y. Comparative evaluation of different miniplates for internal fixation of mandible fractures using finite element analysis. J. Oral. Maxillofac. Surg. 66, 1225–1232 (2008).
Unnewehr, M. et al. Fracture properties of the human mandible. Int. J. Leg. Med. 117, 326–330 (2003).
Daniel, R. W. et al. Fracture injury risk of the restrained mandible to anterior–posterior blunt impacts. J. Biomech. Eng. 143, 041003 (2021).
Sancar, B., Çetiner, Y. & Dayı, E. Evaluation of fracture formation patterns in the human mandible with finite element analysis: Part 2 – Corpus and angle regions. Dent. Traumatol. 39, 437–447 (2023).
Liu, Y., Wang, R., Baur, D. A. & Jiang, X. A finite element analysis of stress distribution in the mandible from impact forces with various orientations of third molars. J. Zhejiang Univ. Sci. B 19, 38–48 (2018).
Zimmermann, E. A. et al. Intrinsic mechanical behavior of femoral cortical bone in young, osteoporotic and bisphosphonate-treated individuals in low- and high-energy fracture conditions. Sci. Rep. 6, 2363 (2016).
Duncea, I. et al. Association of systemic and mandibular bone mineral density in postmenopausal females with osteoporosis. Medicina 60, 1313 (2024).
Gulsahi, A. Osteoporosis and jawbones in women. J. Int. Soc. Prev. Community Dent. 5, 263–268 (2015).
Turner, C. H., Rho, J., Takano, Y., Tsui, T. Y. & Pharr, G. M. The elastic properties of trabecular and cortical bone tissues are similar: results from two microscopic measurement techniques. J. Biomech. 32, 437–447 (1999).
Subit, D., Velazquez-Ameijide, J., Arregui-Dalmases, C. & Crandall, J. Tensile material properties of human rib cortical bone under quasi-static and dynamic loading and influence of microstructure on failure characteristics. arXiv (2011).
Beisekenov, N., Sadenova, M., Azamatov, B. & Syrnev, B. Analysis of biomechanical characteristics of bone tissues using a Bayesian neural network: a narrative review. J. Funct. Biomater. 16, 168 (2025).
Jimenez-Palomar, I., Shipov, A., Shahar, R. & Barber, A. H. Mechanical behavior of osteoporotic bone at sub-lamellar length scales. Front. Mater. 2, 13 (2015).
Acknowledgements
We sincerely thank our friends and peers for their encouragement and moral support throughout the course of this project. No external funding or institutional support was involved in the completion of this study.
Author information
Authors and Affiliations
Contributions
S.M. wrote the main manuscript text and analyzed the collected data. V.D. helped in collecting the data. M.K. helped oversee the project and edited the manuscript. All the authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Manoj, S., K.P, M.K. & A.P, V.D. Behavior of mandibular fractures under earth and microgravity conditions: a finite element analysis. npj Microgravity 12, 36 (2026). https://doi.org/10.1038/s41526-025-00558-w
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41526-025-00558-w