Abstract
Recent advances in our understanding of immune tolerance, particularly the role of immune checkpoints in peripheral tolerance, have opened promising new avenues for therapeutic interventions in immune-related disorders. In this study, we developed a novel class of tolerogenic vaccines based on recombinant virus-like particles (tVLPs), engineered to display the immune checkpoint molecule CTLA-4 on their surface and incorporate specific antigens. These tVLPs promote the differentiation of tolerogenic dendritic cells (DCs) in vitro, characterized by a distinct functional phenotype and associated transcriptomic alterations. Furthermore, tVLPs inhibit DC activation and specifically modulate the antigen-specific T cell compartment, inducing a hyporesponsive state in effector T cells while promoting the activation of regulatory T cells (Tregs). The therapeutic efficacy of tVLPs was demonstrated in a murine model of food allergy, where five consecutive daily injections conferred protection against allergic symptoms and anaphylactic shock. Importantly, this effect was antigen-specific, long-lasting, and dependent on Tregs, as evidenced by the transfer of protection to naïve mice following adoptive transfer of Tregs from vaccinated animals. These findings establish tVLPs as a promising platform for the development of targeted immunotherapies for allergies and autoimmune diseases.
Similar content being viewed by others
Introduction
Immune diseases are a growing public health concern due to their rising incidence. Current therapies for autoimmune diseases and allergies mainly focus on symptom control by reducing inflammation, without restoring long-lasting immune tolerance. These treatments often lack specificity and are associated with significant side effects, including increased susceptibility to infections and malignancies. Advances in the understanding of immune tolerance mechanisms now offer new therapeutic opportunities aimed at inducing long-term, antigen-specific immune tolerance.
Among immune diseases, allergic disorders represent a major and increasing burden, characterized by inappropriate immune responses to harmless environmental antigens. These responses are primarily driven by T helper 2 (Th2) cytokines -including interleukin-4 (IL-4), IL-5, and IL-13- which orchestrate both the initiation and effector phases of allergy. Dendritic cells (DCs), through antigen presentation to naïve T cells, are key regulators of this process, promoting Th2 polarization. However, DCs also have the potential to control allergic inflammation by inducing T cell hyporesponsiveness and regulatory T cells (Tregs), placing them at the intersection of immune activation and tolerance1. Defective Treg function is thought to contribute to allergic sensitization2,3, as observed in immune dysregulation syndromes such as IPEX (immune dysregulation, polyendocrinopathy, enteropathy, X-linked), where Forkhead box P3 (FOXP3) mutations impair Treg development4. Conversely, Tregs play a central role in allergy control5 and allergen-specific immunotherapy (AIT), suppressing multiple facets of Th2-mediated hypersensitivity6. These findings support the development of alternative therapies aimed at enhancing Treg function7,8,9 or modulating Th2 responses. The key role of DCs in these regulation processes was recently shown in epicutaneous allergen immunotherapy (EPIT) where skin DC subsets acquired a distinct phenotype and functional specializations during the EPIT, losing their capacity to prime effector T cells but gaining regulatory T-cell stimulatory properties10. Thus, intervention in the antigen-presenting process and/or activation of the DCs is a strategy for allergic inflammation modulation11,12.
More broadly, DCs are the only antigen-presenting cells (APCs) capable of determining whether an antigenic signal will lead to immunity or tolerance. While fully activated immunostimulatory DCs express high levels of costimulatory molecules (CD80, CD86), produce pro-inflammatory cytokines, and stimulate T cell proliferation, tolerogenic DCs (tolDCs) express low levels of costimulatory molecules, produce immunomodulatory cytokines (IL-10, TGF-β), and impair T cell proliferation13,14. tolDCs also express indoleamine 2,3-dioxygenase (IDO), an enzyme that exhibits an antiproliferative and tolerogenic activity15. Notably, it was shown that expression of IDO in immature DCs reduced Th2 cell activation and allergic airway inflammation in ovalbumin (OVA)-sensitized mice16. Given their ability to promote antigen-specific tolerance, tolDCs are actively being explored as therapeutic tools in transplantation17, autoimmune diseases18, and allergy19.
In addition to costimulatory molecules, immune checkpoints are key regulatory elements that restrict immune cell responses in order to maintain immune homeostasis. While checkpoint inhibitors targeting CTLA-4 (cytolytic T-lymphocyte-associated protein 4) or PD-1 (programmed cell death 1) have revolutionized cancer immunotherapy, strategies that enhance checkpoint signaling are being investigated in autoimmune and allergic diseases20. CTLA-4, expressed on activated T cells and Tregs, competes with CD28 for binding to CD80/CD86, thereby downregulating T cell activation. Mutations in CTLA-4 are associated with various autoimmune diseases21, and certain CTLA-4 polymorphisms have been linked to asthma susceptibility22. Therapeutics targeting CTLA-4, such as the CTLA-4–Ig fusion protein Abatacept®, have shown efficacy in promoting tolerance in autoimmunity and transplantation by blocking co-stimulation and inducing IDO23,24. In murine models of allergic asthma, CTLA-4–Ig has also been shown to potentiate the effects of AIT25.
These findings suggest that enhancing immune checkpoint signaling, particularly through CTLA-4, may be an effective strategy to induce antigen-specific tolerance in allergy.
Nanoparticles and especially virus-like particles (VLPs) are ideal candidates to target DCs and to deliver a signal for immune regulation26. Here, we developed a novel tolerogenic vaccine based on retrovirus-derived VLP (tVLP) carrying a shielded version of OVA as an allergen and expressing a chimeric form of CTLA-4 on its surface. We evaluated the capacity of tVLPs to modulate the phenotype of DCs, their cytokine secretion profile, and thus to inhibit antigen-specific response initiation. Finally, we have evaluated the efficacy of tVLPs to prevent allergic reaction in an experimental mouse model of OVA food allergy and investigated the role of Treg in this protective mechanism.
Results
Design of the tolerogenic vaccines
To develop candidate vaccines for the treatment of immune disorders, we engineered retrovirus-derived murine leukemia virus (MLV) pseudo-particles tVLPOVA displaying the immune checkpoint molecule CTLA-4 on their surface and carrying OVA as a model antigen (Fig. 1A). To optimize CTLA-4 surface expression on tVLPs, we tested several expression strategies using plasmid constructs encoding either the native CTLA-4 sequence or chimeric versions fused with anchoring domains from the vesicular stomatitis virus G protein (VSV-G) or the glycosylphosphatidylinositol (GPI) domain of CD59b. Based on flow cytometry analysis, we observed that the replacement of the native transmembrane and intracellular domains by either those of VSV-G (CTLA-4TM) or CD59b (CTLA-4GPI) significantly enhanced its expression both onto the transfected cells and the resulting tVLPs, with the highest expression using the GPI system (Supplementary Fig. 1).
A Schematic representation of tolerogenic virus-like particles (tVLPOVA), composed of retrovirus-derived capsids (Gag) encapsulating the model antigen ovalbumin (OVA), and expressing chimeric CTLA-4 molecules on their surface. CTLA-4 is engineered by fusing its extracellular domain with a membrane anchor domain (e.g., GPI), enabling its display on the particle surface. B–E Modulation of the mDC phenotype and induction of tolerogenic DCs by the tVLPs. B Representative flow cytometry plots showing modulation of CD80 and PD-L1 expression in murine spleen-derived dendritic cells (mDCs; defined as CD11c+MHC-II+ cells) cultured for 24 h with control particles (VLP⁻), particles displaying CTLA-4 alone (tVLP), or tVLPOVA. Numbers indicate the percentage of CD80⁻PD-L1⁺ cells, defined as tolerogenic DCs (tolDCs). C Quantification of CD80, CD86, and PD-L1 mean fluorescence intensity (MFI) in mDCs treated with increasing doses of VLPs. Dashed lines indicate MFI in the medium-only control. LPS treatment (1 μg/mL) was used as a positive activation control. D Percentage of CD80⁻PD-L1⁺ DCs following exposure to indicated VLPs, to evaluate the capacity of the VLPs to induce tolDCs. E Cytokine secretion profiles (IL-10, TGF-β, TNF-α) in culture supernatants after 1 day of stimulation, showing increased production of immunoregulatory cytokines and reduced pro-inflammatory output with tVLPOVA. Data are presented as mean ± SEM, representative of at least two independent experiments. Statistical significance (*p < 0.05; **p < 0.001; n = 6) was determined by the Mann-Whitney test in comparison with medium (C) or VLP- (D, E).
tVLPs induce a tolerogenic phenotype in dendritic cells
We next investigated the effect of tVLPs on dendritic cell (DC) phenotype. Murine spleen-derived DCs (mDCs) were purified (Supplementary Fig. 2) and cultured with increasing concentrations of tVLPOVA, and the expression of costimulatory molecules CD80/CD86 and the immune checkpoint ligand PD-L1 was analyzed by flow cytometry 24 h later. Notably, the PD-L1/CD80 expression ratio is widely used as an indicator of a tolerogenic DCs phenotype27,28. We observed that tVLP treatment led to a dose-dependent downregulation of CD80 and upregulation of PD-L1 expression (Fig. 1B). Interestingly, this effect was antigen-independent, as tVLPs lacking OVA (but still expressing CTLA-4) induced a similar phenotype (Fig. 1C). In control VLPs lacking both CTLA-4 and OVA, failed to promote tolerogenic features and instead slightly increased the expression of costimulatory molecules. To exclude the possibility of steric interference with antibody detection, CD80 and CD86 expression were assessed using multiple antibody clones (clones 16-10A1, 1G10 for anti-CD80 and clones GL-1, PO3.1 for anti-CD86), which yielded comparable staining patterns across all conditions. This confirmed that the observed changes were not due to masking of antibody epitopes by tVLPs. Moreover, with the early-expression analysis and the absence of CD86 modulation at 4 °C (Supplementary Fig. 3), these results strongly support an active, CTLA-4–dependent regulatory mechanism rather than a steric masking artifact. These results highlight the central role of CTLA-4 on tVLPs in counterbalancing the inherent immunogenicity of viral particles and promoting DC tolerogenicity.
When defining tolDCs as CD80-PD-L1+, we observed a significant conversion of mDCs to this tolerogenic phenotype upon tVLP exposure (Fig. 1D). In addition to the phenotypic changes, we detected a shift in cytokine secretion by mDCs: IL-10 and TGF-β, two key immunosuppressive cytokines, were significantly increased in tVLP-treated conditions, whereas TNF-α levels were reduced compared to controls (Fig. 1E).
tVLP induces tolerogenic transcriptional signatures in dendritic cells
To gain deeper insight into the intrinsic molecular changes induced by tVLPs in dendritic cells, we performed transcriptomic profiling of mDCs cultured for 24 hours in the presence of tVLPOVA, control VLP–, or medium alone. Unsupervised clustering of samples based on differentially expressed genes (DEGs) revealed that tVLPOVA-treated DCs displayed a distinct transcriptional profile, clearly separated from both control conditions (Fig. 2A). Of note, DCs exposed to VLP– clustered more closely with the medium-only group, indicating that CTLA-4 expression on the tVLPs is responsible for the major transcriptional reprogramming observed.
A Heatmap showing the relative expressions of differentially expressed genes (DEGs) in murine dendritic cells (mDCs) cultured for 24 h with tVLPOVA, VLP⁻ (lacking CTLA-4 and OVA), or medium alone. A total of 652 DEGs (fold change ≥ 1.2 and p-value < 0.05) were identified, with 305 genes upregulated and 347 downregulated in the tVLPOVA condition. Hierarchical clustering reveals a distinct gene expression profile in tVLPOVA-treated DCs compared to controls. B Volcano plot showing DEGs between tVLPOVA and VLP⁻ conditions. C Selected DEGs showing significant downregulation (left) or upregulation (right) in tVLPOVA-treated DCs compared to VLP⁻. Boxplots showing the expression values for representative genes associated with migration (Cx3cl1, Nod2, Dpp4), metabolic fitness (Kynu, Lpcat2, Srm), immunosuppression (Azin2, Ifi205), and regulatory DC function (Batf, Dusp14, Pilra). D Functional enrichment analysis based on the Gene ontology (GO) of significantly downregulated (top) and upregulated (bottom) gene sets in tVLPOVA-treated DCs. E Boxplots showing the expression values of cytokine-related genes in tVLPOVA-treated DCs. Pro-inflammatory cytokines (Il1a, Il6, Il12a, Il13, Il17a) are downregulated (left), while regulatory cytokines (Il10, Il1rn) are upregulated (right). Expression is shown as log2 normalized counts.
To identify key genes involved in the tolerogenic phenotype, we analyzed the most significantly dysregulated genes using a volcano plot representation (Fig. 2B). tVLPOVA treatment led to the upregulation of several genes associated with immune regulation and metabolic adaptation, including Batf (a transcription factor linked to IL-12 signaling and tolerogenic DC functions), Ifi205 (an interferon-inducible gene implicated in immune tolerance and therapeutic protection), and Srm (a gene involved in polyamine biosynthesis, important for DC metabolic homeostasis). We also observed increased expression of Tnfrsf13b (encoding TACI, which may influence T cell–DC interactions through BAFF signaling) and Azin2, a regulator of the polyamine pathway via antizyme inhibition. Conversely, several genes associated with DC maturation and migration were downregulated in tVLPOVA-treated cells. These included Plet1 and Asb2, both known to promote DC motility, as well as Ifitm1, a marker of activated DCs. Importantly, Csf1r, a receptor involved in mononuclear phagocyte survival and implicated in immune checkpoint pathways, was also downregulated. In addition, we identified decreased expression of Cyp4f16, which may contribute to retinoic acid preservation and favor a tolerogenic environment. A focused analysis of selected DEGs (Fig. 2C) further confirmed the modulation of genes involved in migration (Cx3cl1, Dpp4, Nod2), metabolism (Kynu, Lpcat2, Ryr3), and immune regulation (Dusp14, Pilra), reinforcing the concept that tVLPOVA drives a broad functional reprogramming of DCs.
To functionally interpret these transcriptomic changes, gene ontology (GO)-based functional enrichment was performed. Downregulated genes were linked to pro-inflammatory signaling, DC activation, and cell trafficking, while upregulated genes were significantly associated with pathways involved in metabolic reprogramming and immune regulation (Fig. 2D). These results are in line with the phenotypic changes previously observed and suggest a shift toward a more regulatory DC state.
Given the observed modulation of cytokine secretion in tVLP-treated cultures (Fig. 1), we next investigated changes in the expression of cytokine-related genes. As shown in Fig. 2E, tVLPOVA-treated DCs exhibited decreased expression of pro-inflammatory cytokines including Il1a, Il6, Il12, Il13, and Il17. In contrast, genes encoding anti-inflammatory or immunomodulatory cytokines, such as Il10 and Il1rn, were upregulated. These transcriptomic findings support and extend our phenotypic data, confirming that tVLPOVA promotes a transcriptional program consistent with tolerogenic function in DCs.
tVLPs suppress activation of mouse and human dendritic cells
We next evaluated whether tVLPs not only induce a tolerogenic phenotype in dendritic cells but also actively prevent their subsequent activation. To this end, mDCs (Supplementary Fig. 2) were incubated with GFP-recombinant tVLPs and stimulated with lipopolysaccharide (LPS) for 24 hours. GFP fluorescence confirmed that over 99% of DCs had efficiently internalized the tVLPs.
While LPS treatment alone markedly increased the expression of costimulatory molecules CD80 and CD86—as shown by both the proportion of double-positive CD80+CD86+ cells (Fig. 3A) and the upregulation of each marker (Fig. 3B)—tVLP treatment completely abrogated this activation. Importantly, DCs exposed to both tVLP and LPS displayed significantly reduced CD80/CD86 expression levels compared to DCs treated with LPS alone or with control VLPs (VLP–). Strikingly, expression levels in the tVLP + LPS condition were even lower than in unstimulated DCs, indicating that tVLPs not only prevent activation but may also actively suppress basal expression of costimulatory molecules.
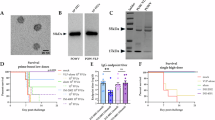
A–C Splenic murine dendritic cells (mDCs) or bone marrow–derived DCs (mBMDCs) were stimulated for 24 h with LPS (1 μg/mL) in the presence or absence of tVLPs (15 μg/mL), control VLPs lacking CTLA-4 (VLP⁻), or soluble CTLA-4-Ig (4-Ig). A Representative flow cytometry contour plots showing CD80 and CD86 expression on splenic mDCs. B Relative mean fluorescence intensity (MFI) of CD80 and CD86 in mDCs (left) and mBMDCs (right) normalized to medium controls. C IL-10 levels in culture supernatants from mDCs measured by ELISA. D, E Human monocyte-derived dendritic cells (hDCs) were cultured for 24 h with or without tVLPs (15 μg/mL) and activated or not with TNF-α (100 ng/mL). D Representative flow cytometry dot plots (left) and quantification (right) showing the proportion of hDCs expressing different levels of CD80 and CD86. Gates for CD80 and CD86 expression were defined using the TNF-α–stimulated condition, where most mDCs display a CD80hiCD86hi phenotype; the same gate positioning was applied consistently across all experimental groups. E Flow cytometry plots and quantification of indoleamine 2,3-dioxygenase (IDO) expression in hDCs, showing that co-treatment with tVLP and TNF-α leads to a strong induction of IDO⁺ in DCs. Data are representative of 2–3 independent experiments. n = 5, 6 per condition. Statistical comparisons were performed using the Mann–Whitney test (*p < 0.05; **p < 0.01, vs. LPS-only condition).
Similar results were observed when tVLPs using the alternative anchorage system of CTLA-4 (CTLA-4TM) were used (Supplementary Fig. 1). Additionally, the importance of the immune checkpoint in these phenotypic modifications is suggested by the similar effect induced by CTLA-4-Ig (“+ 4-Ig”). However, tVLPs were more effective than CTLA-4-Ig at suppressing CD80 expression and uniquely induced a significant increase in IL-10 secretion (Fig. 3C), supporting a broader immunomodulatory effect. To note, tVLPs have no significant impact on the expression of MHC-II and CD40 in comparison to the LPS condition, revealing that their action is selective to the costimulatory axis.
To confirm and extend these findings, similar experiments were renewed with murine bone marrow-derived dendritic cells (mBMDCs; Supplementary Fig. 2). LPS induced stronger CD80/CD86 upregulation in mBMDCs compared to splenic mDCs (Fig. 3B), yet tVLPs were still effective in completely suppressing CD80 and partially reducing CD86 expression. We confirmed that the expression of MHC-II (2.1 vs 2.3-fold increase in +0 and +tVLP, respectively) and CD40 (8.2 vs 8.2-fold increase, respectively) was unaffected.
To explore the translational potential of our findings, we next evaluated the effects of tVLPs on human monocyte-derived DCs (hDCs; Supplementary Fig. 2) activated with TNF-α. Consistent with our murine data, tVLPs significantly blocked TNF-α–induced upregulation of CD80 and CD86 in hDCs (Fig. 3D, left panels). Moreover, quantification of CD80loCD86lo cells revealed a significant increase in the proportion of hDCs with a tolerogenic phenotype, even in the presence of an inflammatory stimulus (Fig. 3D, right panels).
Finally, given the critical role of indoleamine 2,3-dioxygenase (IDO) in the suppression of T cell responses and induction of regulatory T cells, we assessed IDO expression in hDCs. While neither TNF-α nor tVLPs alone induced substantial IDO expression, their combination led to a marked increase in IDO+ hDCs (up to 30%) (Fig. 3E), highlighting the potential of tVLPs to induce human tolDCs.
tVLPs suppress antigen-specific effector T cell proliferation and enhance Treg activation
Given the strong tolerogenic reprogramming observed in DCs following exposure to tVLPs, we next investigated the impact of our vaccine on antigen-specific CD4⁺ T cell responses, distinguishing between conventional effector T cells (Tconv) and regulatory T cells (Tregs).
To this end, we used splenocytes isolated from DO11.10 x Foxp3-GFP transgenic mice, in which OVA-specific CD4⁺ T cells and Foxp3⁺ Tregs can be tracked. Cells were labeled with CellTraceTM Violet (CTV) and cultured for three days in the presence of OVA-recombinant tVLPs (tVLPOVA) or controls (VLPOVA). Initial analyses focused on the percentage of proliferating CD44hi Tconv (representing antigen-experienced T cells) and Treg subsets. This approach allowed us to exclude naïve CD44lo cells and to more accurately evaluate the functional impact of tVLP-induced tolerogenic dendritic cells on relevant T-cell populations. As expected, in the control condition with VLPOVA, both CD44hi Tconv and Treg subsets underwent proliferation, indicative of antigen-specific activation. In contrast, tVLPOVA markedly inhibited the proliferation of CD44hi Tconv cells while significantly promoting the proliferation of CD44hi Tregs (Fig. 4A). These findings were reproduced when analyzing the total CD4⁺ T-cell compartment (Supplementary Fig. 4). To rule out the possibility that tVLPs interfere with antigen presentation by DCs—thus indirectly explaining the reduced Tconv response—we repeated the co-culture experiment in the presence of OVA peptide. Under these conditions, the suppressive effect on Tconv proliferation persisted (Supplementary Fig. 5), suggesting that tVLPs do not impair antigen presentation and that the inhibition of Tconv proliferation is likely due to active immune regulation. To further quantify these effects, we next assessed the absolute numbers of proliferating cells. Consistent with the dilution-based analyses, tVLPOVA induced a significant increase in the total number of proliferating Tregs (Fig. 4A), confirming a true expansion of the regulatory compartment. For Tconv, the absolute number of proliferating cells remained globally similar to the control condition, despite the reduction in their relative frequency. Together, these data indicate that tVLPOVA preferentially expands antigen-specific Tregs while reshaping the phenotypic landscape of Tconv responses, thereby shifting the overall balance of CD4⁺ T-cell activation toward immune regulation.
Spleen cells from DO11.10 x Foxp3-GFP transgenic mice were labeled with CellTraceTM Violet (CTV) and cultured for 3 days in the absence of exogenous IL-2 with 15 μg/mL of tVLPOVA, VLPOVA (OVA+ only), medium or VLP⁻ (no antigen, no CTLA-4) as controls. Foxp3⁻ (Tconv) and Foxp3⁺ (Treg) OVA-specific CD4⁺ T cells were then analyzed by flow cytometry. A Representative CTV dilution plots showing proliferation of CD44hi antigen-experienced Tconv and Treg cells (left panel). Quantification of proliferated (divided) cells is shown (right panel) as both percentages and absolute numbers. Data are means ± SEM; n = 6; **p < 0.01; Mann–Whitney test, and are representative of 3 independent experiments. B Relative expression of functional surface and intracellular markers in CD44hi Tconv and Treg subsets. Expression levels (MFI) are normalized to the highest value per marker and averaged across groups. C Cytokine profiling by Luminex of culture supernatants collected at day 3. Results are expressed as absolute concentrations (pg/mL). Mean ± SEM are shown; n = 6; *p < 0.05; **p < 0.01; Mann–Whitney test vs. VLPOVA.
To confirm the generality of this observation, we repeated the experiments using splenocytes from OT-II x Foxp3-GFP mice, which recognize OVA in the H-2b context. In this model, the pro-Treg effect of tVLPOVA was again observed, confirming the robustness of the phenomenon across MHC backgrounds (Supplementary Fig. 6).
To assess whether tVLPs not only influence the proliferation but also the functional state of antigen-specific CD4⁺ T cells, we analyzed the expression of phenotypic markers on CD44hi Tconv and Treg populations from DO11.10 x Foxp3-GFP mice after 3 days of co-culture.
Compared to control conditions (medium or VLP–), tVLPOVA induced substantial phenotypic changes in both Tconv and Treg subsets. In the Tconv compartment, we observed a marked upregulation of exhaustion- or anergy-associated markers, including CTLA-4, PD-1, LAG-3, and TIM-3, suggesting that these cells were driven toward a hyporesponsive state. In parallel, Tregs exhibited increased expression of functional suppressive markers, such as CTLA-4, CD39, ICOS, and LAG-3, consistent with an activated and regulatory phenotype (Fig. 4B and Supplementary Fig. 7).
To further characterize the immune environment shaped by tVLPs, we analyzed the cytokine profile in culture supernatants using Luminex multiplex assays. Cytokine levels were normalized to the maximal value detected across all conditions. In medium and VLP– controls, little to no cytokine production was detected. In contrast, cultures stimulated with VLPOVA exhibited a robust pro-inflammatory cytokine signature, characterized by high levels of IFN-γ, TNF-α, IL-2, IL-4, and IL-13, reflecting a mixed Th1/Th2 effector response.
Strikingly, co-cultures with tVLPOVA showed a significant reduction in these pro-inflammatory cytokines compared to VLPOVA, consistent with the suppression of Tconv activation observed earlier. Furthermore, IL-10, a hallmark immunosuppressive cytokine, was increased in the tVLPOVA condition, supporting the emergence of a regulatory milieu (Fig. 4C).
Together, these data indicate that tVLPs exert a dual effect on antigen-specific T cells: they promote functional activation of regulatory T cells while inducing a tolerogenic, anergic-like phenotype in effector T cells, in part through modulation of the cytokine environment.
tVLPs protect against severe allergic reactions in a murine model of OVA-induced food anaphylaxis
To evaluate the therapeutic potential of tVLPs in vivo, we assessed their ability to induce antigen-specific tolerance in a murine model of food allergy. Mice were first sensitized to OVA using OVA/alum injections and then subjected to repeated oral OVA challenges to induce anaphylactic reactions. A cohort of sensitized animals received daily intraperitoneal injections of tVLPOVA over five consecutive days prior to the challenge phase (Fig. 5A). Remarkably, mice treated with tVLPOVA exhibited strong protection against OVA-induced anaphylaxis, with significantly reduced allergic symptoms - such as piloerection and diarrhea - and largely protected from the characteristic drop in body temperature typically associated with anaphylactic shock. Notably, this clinical protection persisted across multiple cycles of OVA challenges (Supplementary Fig. 8) and remained effective up to five months post-vaccination (Day 150; Fig. 5A), indicating long-term immune modulation.
A Experimental scheme and clinical outcomes. Mice were sensitized to ovalbumin (OVA) by two intraperitoneal injections (days –14 and –7), then vaccinated with tVLPOVA or control VLP⁻ (30 μg/injection) daily from day 1 to 5. A group of mice received VLPOVA co-administered with soluble CTLA-4-Ig (4-Ig) as an alternative immunomodulatory strategy. Mice were then challenged orally with OVA on days 15–23 and again on days 150–158. Clinical allergy scores (left) and body temperature changes (right) were recorded 30 minutes after the final OVA challenge of each cycle. Allergic and anaphylactic protection are respectively associated with clinical scores below 2 and temperature drops less than –2 °C. B Specificity of the protective effect. Mice vaccinated with tVLPOVA after OVA sensitization were later sensitized to peanut (days 35 and 42), and subsequently challenged via intraperitoneal injection with OVA (day 50) and peanut extract (day 57). Body temperature was monitored 30 minutes post-injection. Data are representative of three independent experiments. Symbols indicate individual animals; bars represent mean ± SEM. Dashed lines denote thresholds between moderate and severe reactions. *p < 0.05 (Mann–Whitney test); ns, not significant; n = 4–8 mice per group.
To confirm the specificity of the effect and dissect the role of each vaccine component, we included several control groups. Mice treated with CTLA-4+ VLPs lacking OVA (tVLP–), or OVA-recombinant VLPs lacking CTLA-4 (VLPOVA), failed to show significant protection during the initial challenge phase, both in terms of clinical score and hypothermia (Supplementary Fig. 8), underlining the necessity of combining both tolerogenic signal and cognate antigen. Interestingly, we observed a partial but incomplete protection in some animals from both control groups, suggesting that CTLA-4 or OVA alone may exert limited modulatory effects, albeit insufficient for robust clinical protection.
Although a modest reduction in OVA-specific IgE levels was observed at day 160 (Supplementary Fig. 8), this difference did not reach statistical significance and is unlikely to account for the observed protection. To evaluate antigen specificity, we challenged tVLPOVA-vaccinated mice with an unrelated allergen (peanut). While the vaccinated animals remained protected against subsequent OVA challenges, they were not protected from peanut-induced anaphylaxis, as evidenced by comparable hypothermic responses to control mice (Fig. 5B). However, upon a final intravenous challenge with OVA, the same tVLPOVA-vaccinated mice displayed significantly reduced body temperature loss, confirming that the induced immune tolerance was antigen-specific.
Altogether, these data demonstrate that tVLPs act as a potent tolerogenic vaccine, capable of inducing durable, antigen-specific, and dose-dependent protection against severe allergic reactions in vivo.
tVLP-induced protection is mediated by regulatory T cells
To determine whether regulatory T cells (Tregs) contribute to the protective effect induced by tVLPOVA, we performed adoptive transfer experiments. CD4⁺CD25hi T cells were isolated from mice vaccinated one month earlier with tVLPOVA or control VLP-, and post-sort analysis confirmed that 93% of the sorted CD4⁺CD25hi population expressed Foxp3, indicating high-purity Tregs (Fig. 6A). These cells were then transferred into naïve recipient mice, which subsequently underwent the full allergy induction protocol, including sensitization followed by two cycles of oral OVA challenges (Fig. 6A). Strikingly, recipient mice that received Tregs from tVLPOVA-vaccinated donors exhibited complete protection against OVA-induced anaphylaxis. These animals showed significantly reduced clinical scores and no detectable drop in body temperature during both challenge cycles, including the second cycle, which typically triggers the most severe reactions. In contrast, mice that received Tregs from VLP–-treated donors developed robust allergic responses, with pronounced clinical symptoms and hypothermia (Fig. 6B, C).
A Experimental protocol. Donor mice were sensitized to OVA, vaccinated with tVLPOVA, and orally challenged with OVA as described in Fig. 5. At day 30, CD4⁺CD25hi Treg cells were isolated from spleen and mesenteric lymph nodes, purified and transferred intravenously (50,000 cells/mouse) into naïve recipient mice. Post-sort analysis confirmed that 93% of the sorted CD4⁺CD25hi population expressed Foxp3. Recipient mice were subsequently sensitized with OVA and subjected to two independent cycles of oral OVA challenges at days 45 (B) and 60 (C). Clinical scores (left) and body temperature drops (right) were recorded 30 minutes after the final gavage of each cycle. Data represent one of three independent experiments. Symbols indicate individual mice; bars represent mean ± SEM. Dashed lines denote thresholds distinguishing moderate from severe allergic responses (score <2 and temperature drop >–2 °C). *p < 0.05; **p < 0.001 (Mann–Whitney test); n = 7–8 per group.
These results demonstrate that Tregs are essential effectors of the immune tolerance induced by tVLP vaccination, and that their adoptive transfer alone is sufficient to reproduce the protective effect in naïve animals.
Discussion
Our study introduces a new tolerogenic vaccine platform based on VLPs that co-deliver a shielded allergen and the immune checkpoint molecule CTLA-4. We demonstrate that such tVLPs elicit a potent, long-lasting, and antigen-specific protection against food-induced anaphylaxis, mediated through regulatory T cell (Treg)–dependent mechanisms. To our knowledge, this is the first report describing the use of enveloped VLPs as a vector for concurrent antigen delivery and immune modulation via a membrane-anchored checkpoint molecule.
Previous strategies using VLPs have mainly focused on immunogenic applications, or at best, on allergen delivery in the absence of immunosuppressive signals. While surface-exposed29 allergen-bearing VLPs can induce blocking IgG responses, they carry a risk of crosslinking pre-existing IgE and triggering anaphylaxis. In contrast, encapsulating the allergen within the VLP core offers a safer approach for use in sensitized individuals. However, this configuration alone—as shown in our VLPOVA condition—proved insufficient to induce robust tolerance in the context of food allergy. By integrating CTLA-4 onto the surface of the same VLPs, we fundamentally altered their immunological profile and efficacy.
Technical optimization was necessary to achieve stable surface expression of CTLA-4 on retrovirus-derived particles. New systems such as the SpyTag/SpyCatcher technology30 have been recently described to easily display molecules, but are not applicable for retrovirus-derived VLP. The use of a GPI-anchoring system31 allowed efficient incorporation of CTLA-4 into the lipid raft regions from which VLPs bud32, resulting in high-density display of functional molecules. This configuration enabled tVLPs to directly interact with DCs and modulate their function. We showed that tVLPs selectively downregulate costimulatory molecules CD80/CD86, increase IL-10 secretion, and upregulate IDO in human DCs, all features consistent with a tolerogenic DC phenotype33. Importantly, these changes were not observed with particles lacking either CTLA-4 or antigen, highlighting the requirement for both signals. No alteration of CD40 in DCs was observed with tVLPs, but its specific role in tolerance induction is still controversial34,35. However, IL-10 production remains the main characteristic of tolDCs36 as it is a powerful anti-inflammatory cytokine that plays an essential role in dampening immune responses and in preventing chronic inflammatory pathologies, including allergy37,38. By increasing IL-10 production without modulating IL-4 secretion, tVLPs alleviated DC cytokine production to promote tolerance. Indeed, DCs producing high levels of IL-10 have been highlighted as potent inducers of Tr1 cells and therefore dampen immune disorders36. Moreover, we highlighted the role of tVLPs to increase IDO production in human DCs. This modulation mediated by CTLA-4 binding may also be of interest in tolerance induction by promotinga hyporesponsive state through increased tryptophan catabolism39 and Tregs induction40. Indeed, anergic modulation of IDO contributes to tolerance induction during subcutaneous allergen immunotherapy by reducing Th2 cytokine production41. Overall, the results on both murine and human DCs suggest a strong tolerogenic role for tVLPs that was confirmed by our transcriptomic analysis of murine DCs in identifying a unique gene expression signature associated with metabolic adaptation (e.g., Srm), suppression of inflammatory pathways (Csf1r, Ifitm1), and enhancement of regulatory functions (Batf, Ifi205, Azin2). This tolerogenic DC state translated into a coordinated T cell response, with suppression of antigen-specific effector T cells and activation of Foxp3⁺ Tregs. The anergy/exhaustion markers observed in Tconv cells (PD-1, TIM-3, LAG-3) and the acquisition of suppressive phenotype in Tregs (CTLA-4, CD39, ICOS) are consistent with long-term tolerance mechanisms. Importantly, this balance was reflected in the cytokine profile, with a shift from pro-inflammatory cytokines (IFN-γ, IL-4, IL-13) toward IL-10 production, without evidence of generalized immunosuppression.
In vivo, tVLPs provided sustained protection against severe allergic reactions even months after treatment. Neither particles bearing antigen alone nor particles displaying CTLA-4 in the absence of antigen conferred protection, emphasizing the necessity of antigen-specific engagement. The lack of cross-protection against unrelated allergens (peanut versus OVA) further confirmed the specificity of this tolerogenic strategy. Despite previous reports showing that VLPs expressing only antigen have protective effects in a preventive model of pollen allergy42, here we show the requirement to combine VLPs with an immunoregulatory signal to provide efficient and long-term therapeutic effects in a food allergy model.
Although we did not observe significant modulation of IgE or protective IgG subclasses in serum, other mechanisms—such as Tr1 induction, IL-10–dependent suppression, or local tissue-resident tolerance—may contribute and remain to be elucidated. Notably, the modest reduction in OVA-specific IgE observed at day 160 was not statistically significant and is unlikely to account for the protection, suggesting that tVLP-induced tolerance can counteract anaphylaxis despite pre-existing IgE–mast cell sensitization. This indicates that the protective effect of tVLPOVA does not rely on modulation of circulating IgE but instead reflects regulatory mechanisms capable of dampening effector responses. Future studies will be required to clarify the mechanisms underlying protection. Our data suggest that rather than merely inducing immune deviation, tVLPs establish a tolerogenic cellular network involving DCs, Tregs, and cytokine crosstalk. Critically, adoptive transfer of Tregs from vaccinated mice conferred protection to naïve recipients, formally establishing their central role in tVLP-induced tolerance. Further work using improved multimer tools will be needed to characterize the polyclonal OVA-specific Treg repertoire induced by tVLPs.
Collectively, our findings position tVLPs as a promising translational platform for tolerance induction in allergic diseases. Their modular design allows adaptation to other antigens and checkpoints, and their selective immune reprogramming supports their potential application not only in allergy but also in autoimmunity or immune disorders. Future studies will be needed to explore safety, delivery routes, and durability in human settings, but our data establish a clear rationale for clinical development of tVLP-based therapies.
Methods
Plasmids. pGag-pol encoding for core proteins from Murine Leukemia Virus (MuLV) is derived from pHIT6043 by promoter substitution with a minimal CMV promoter using the SacII/Xba1 unique restriction sites. The pGag-OVA DNA was previously described44. The pCTLA-4WT encodes the murine CTLA-4 protein inserted in the pIRES backbone (Clontech®) using the unique EcoRI site of restriction (Position 1102). pCTLA-4TM encodes chimeric mCTLA-4 in which the transmembrane and intracytoplasmic domains were substituted with those of the vesicular stomatitis virus-derived G (VSVG) protein and separated from the extracellular domain of mCTLA-4 by the Gly-Gly-Gly-Gly-Ser flexible linker. pCTLA-4GPI encodes chimeric mCTLA-4 in which the transmembrane and intracytoplasmic domains were substituted with those of the CD59 molecule as an anchoring system.
Cell lines. Human embryo kidney cells (HEK 293 T; CRL-1573, ATCC) were cultured at 37 ◦C in 5% CO2 in DMEM medium supplemented with Glutamax, 100 U/mL of penicillin and streptomycin, 25 mM HEPES and 10% of heat-inactivated fetal calf serum (FCS) (all from Thermo Fischer Scientific). 293T-GagGFP cells (DD7) were obtained after infection of HEK 293 T cells with the recombinant lentiviral vector encoding Gag-GFP previously described.
VLP production, purification and validation. Non-recombinant or OVA-recombinant VLPs were produced in transiently transfected HEK 293 T. Cells were seeded in 175-cm3 culture flasks (15 ×106 cells per flask) in complete DMEM medium and cotransfected 24 h later with 25 μg of plasmid DNA, including pGag-pol / pCTLA-4 at a ratio of 1:4 for tolerogenic VLPs (tVLPs); pGag-pol / pGag-OVA / pCTLA-4 at a ratio of 0.25:0.75:4 for tVLPOVA. pCTLA-4 designates alternatively pCTLA-4TM or pCTLA-4GPI. Plasmids were mixed with PEI (PEI MAX® - Transfection grade; Polysciences) at a ratio of 1:3 and incubated for 6 h. Medium was then replaced with fresh DMEM supplemented with Glutamax and 25 mM HEPES for 60 h before sampling. GFP-recombinant VLPs were collected from DD7 cells cotransfected with 50 μg of pCTLA-4TM or pCTLA-4GP. The purification process was previously described44, including an ultracentrifugation through a 3 mL 20%-60% sucrose gradient (Sigma-Aldrich). The production of VLPs was quantified by protein measurement according to the bicinchoninic acid Assay method (Pierce BCA Protein Assay Kit, Thermo Fischer Scientific). For validation, 20 μg of VLPs were incubated with 5 μL of 4 μm diameter aldehyde/sulfate latex beads (Thermo Fischer Scientific) for 15 min at room temperature, and washed with PBS (qsp 1 mL) for 1 h. Blocking solution was added (20 μL of FCS) for 30 min and after three washings, anti-CD152-PE (eBiosciences) was added in 2% BSA in PBS for 1 h. For intra-VLP staining, beads were incubated in Triton 1% PBS for 1 h and then incubated with primary antibodies: anti-MuLV p30 (clone R187, CRL-1912 cells; ATCC) and anti-OVA (polyclonal rabbit serum, Agro-Bio), and then secondary antibodies in 0.1% Triton PBS. Finally, beads were washed and resuspended in 200 μL PBS for flow cytometry analysis using a Cytoflex (Beckman Coulter). tVLP stability was assessed after storage at 4 °C for up to one month and at −80 °C for up to six months, showing preserved particle size/structure and maintenance of CTLA-4 surface expression by flow cytometry
DC activation assay. Murine DCs were isolated from spleens (mDC) or produced from bone marrow (mBMDC) of BALB/c mice. Spleens were harvested and digested for 30 min in 10% FCS RPMI (Life Technologies) with 0.1 mg/mL DNAse I and 1 mg/mL Collagenase IV (Sigma Aldrich). CD3+, CD8+, B220+, NKp46+, and Ter119+ cells were eliminated using magnetic separation with specific biotinylated antibodies (eBiosciences) and anti-Biotin beads (30 µL/1.108 cells; Miltenyi). Bone marrow cells were cultured for 8 days in RPMI medium supplemented with 2 mM L-Glutamine, 50 µM 2-mercaptoethanol, 100 U/mL penicillin, 100 μg/mL streptomycin, 10% heat-inactivated FCS, and 20 ng/mL GM-CSF (Miltenyi). Medium was replaced every 3 days for 8 days. mDCs or mBMDCs were plated (3.105 cells/ well) and incubated overnight with 10% FCS RPMI, 20 ng/mL of GM-CSF+/− 10 μg/mL LPS (Sigma Aldrich) +/− tVLPs at several concentrations. CTLA-4-Ig was used at concentrations normalized to the surface density of CTLA-4 displayed on tVLPs, as determined by quantifying CTLA-4 levels using an ELISA-based assay with Abatacept as the standard. The expression of activation markers was analyzed by flow cytometry, and cytokine secretion was assessed in culture supernatants by ELISA.
Human-derived DC (hDC) were generated from monocytes purified from PBMC of healthy donors from the Etablissement Français du Sang (EFS), isolated on Percoll (Sigma-Aldrich), and positively selected using CD14 Human Microbeads and LS Columns (Miltenyi). CD14+ cells were then cultured for 5 days at 37 °C, 5% CO2 in RPMI supplemented with 2 mM L-Glutamine, 100 U/mL penicillin, 100 μg/mL streptomycin, 10% heat-inactivated FCS, rIL-4 (20 ng/mL), and rGM-CSF (100 ng/mL). On day 5, hDC were activated or not with TNF-α (100 ng/mL) +/− tVLP. After 24 hours, hDC were analyzed by flow cytometry using HLA-DR-FITC, CD86-APC, CD80-PE, CD11c-PEVio615 (Miltenyi,) and IDO-PC7 (intracellular staining - Thermo Fischer Scientific).
The gating strategy and post-gating purity of the different dendritic-cell populations are shown in Supplementary Fig. 2
RNAseq. mDCs were obtained as previously described, stained with CD11c and MHC II, and the double-positive cells were sorted on a FACS ARIA. 3 × 105 cells were plated and incubated overnight with 25 µg/mL of tVLPOVA, VLP- or medium as a control. Total RNA was isolated with the RNAqueous™- Kit (Invitrogen) according to the manufacturer’s recommendations. RNA concentration was measured on a NanoDrop1000 (Thermo Fisher Scientific), and RNA integrity was determined on a Bioanalyzer (Agilent) with measurements higher than 8.
RNA-seq libraries were prepared from low-input RNA using the SMARTer cDNA synthesis kit, followed by purification and library construction with the Nextera XT DNA Library Preparation Kit (Illumina). Final libraries were qualified and quantified using a TapeStation system and the Quantifluor dsDNA System to verify fragment size distribution and concentration. Sequencing was performed on an Illumina NextSeq 500 instrument using a NextSeq 500 High Output Kit v2 (2 × 75 bp; 150 cycles; 400 million reads; ~50 Gb). Raw sequencing reads were quality-filtered and trimmed using Trim Galore. The trimmed reads were then aligned to the mouse reference transcriptome using Salmon. Differentially expressed genes (DEGs) were identified with DESeq2, applying a fold-change threshold of ≥1.2 and a p-value cutoff of 0.05. Functional enrichment analysis was performed using the Enrichr database based on Gene Ontology (GO) terms.
Impact of tVLP on antigen-specific CD4 + T cells. Spleen cells were collected from DO11.10xFOXP3-GFP (H-2d) or OT-IIxFOXP3-GFP (H-2b) mice. T cells were enriched after CD8+, B220+, NKp46+, and Ter119+ magnetic depletion. Cells were stained with CellTrace Violet (CTV, Thermo Fischer Scientific) according to the manufacturer’s recommendations and then cultured in 96-well plates (3 × 105 cells/well) in complete RPMI medium in the presence of different concentrations of tVLPs or medium as a control. No exogenous IL-2 was added to the proliferation assays. After 3 days, proliferation and activation of CTV+ T cells (Tconv and Treg) were analyzed by flow cytometry.
Flow cytometry. Cells were stained with the antibodies listed in the Supplementary Fig. 9. Intracellular detection was performed on fixed and permeabilized cells using Foxp3/Transcription Factor Staining Buffer Set (eBioscience). All cytometry experiments were performed on a Cytoflex (Beckman Coulter) cytometer, and data were analyzed using Cytexpert (Beckman Coulter) or FlowJo Software (Treestar Inc).
Mice. Seven-week-old BALB/C (AnNR/j) female mice were purchased from Janvier Labs. DO11.10xFOXP3-GFP (H-2d) or OT-IIxFOXP3-GFP (H-2b) mice were generated and maintained in our animal facility under specific pathogen-free conditions in agreement with current European Union legislation on animal care, housing, and scientific experimentation. All procedures were approved by the local ethics animal committee and national authorities (APAFIS #32149-2021082617476358 v3).
Food allergy model and treatment. Mice were sensitized twice at 1-wk interval by i.p. injection (100 µL) of 10 μg of OVA (A5503; Sigma-Aldrich) mixed with 500 μg aluminum hydroxide (Imject Alum; Thermo Fischer Scientific). Eight days after sensitization, mice were daily i.p. injected with 30 μg of tVLPs for 5 days. Allergic reactions were then induced 10 days later by OVA p.o administrations (20 mg/mouse) every two to three days. Severity of allergic response was assessed 30 min after the last induction by measuring changes in body temperature using a rectal thermometer (Bioseb) and by evaluating clinical score as previously described8. Mice sera were collected at different time points and stored at −20 °C until their analysis by ELISA for immunoglobulins.
Multiplex cytokine analysis by Luminex
Cytokines were quantified in culture supernatants at day 3. Preliminary attempts to generate temporal cytokine kinetics were limited by reduced cell viability beyond day 5. Multiplex cytokine quantification was performed using MILLIPLEX® Mouse Cytokine/Chemokine Magnetic Bead Panel kits (Merck, Darmstadt, Germany) according to the manufacturer’s instructions. Briefly, standards, controls, and samples were incubated with fluorescently labeled magnetic capture beads in 96-well filter plates. After washing, biotinylated detection antibodies were added, followed by incubation with streptavidin-phycoerythrin. Plates were then analyzed using a MAGPIX® analyzer (Luminex, Austin, TX, USA). Cytokine concentrations were determined by interpolation from standard curves generated for each analyte using known concentrations.
Statistical analysis. Statistical significance was evaluated with GraphPad Prism (GraphPad Software) using the Mann-Whitney U test (comparison of rank, unpaired, nonparametric test, two-tailed, α risk = 5%) with *p < 0.05 taken as statistical significance (**p < 0.01; ***p < 0.001).
Data availability
All data and materials are available upon request.
References
Ruiter, B. & Shreffler, W. G. The role of dendritic cells in food allergy. J. Allergy Clin. Immunol. 129, 921–928 (2012).
Ling, E. M. et al. Relation of CD4 + CD25+ regulatory T-cell suppression of allergen-driven T-cell activation to atopic status and expression of allergic disease. Lancet 363, 608–615 (2004).
Stoumpos, A., Heine, G., Saggau, C. & Scheffold, A. The role of allergen-specific regulatory T cells in the control of allergic disease. Curr. Opin. Immunol. 92, 102509 (2025).
Torgerson, T. R. et al. Severe food allergy as a variant of IPEX syndrome caused by a deletion in a noncoding region of the FOXP3 gene. Gastroenterology 132, 1705–1717 (2007).
Conrad, M. L. et al. Regulatory T cells and their role in allergic disease. Allergy 80, 77–93 (2025).
Yamashita, H., Takahashi, K., Tanaka, H., Nagai, H. & Inagaki, N. Overcoming food allergy through acquired tolerance conferred by transfer of Tregs in a murine model. Allergy 67, 201–209 (2012).
Rosenzwajg, M. et al. Low-dose IL-2 in birch pollen allergy: A phase-2 randomized double-blind placebo-controlled trial. J. Allergy Clin. Immunol. 155, 650–655 (2025).
Bonnet, B. et al. Low-dose IL-2 induces regulatory T Cell-mediated control of experimental food allergy. J. Immunol. 197, 188–198 (2016).
Bonnet, B., Vinot, P. A. & Bellier, B. Cibles et immunothérapies innovantes dans le traitement de l’allergie alimentaire. Rev. Franç. Allergol. 57, 327–336 (2017).
Laoubi, L. et al. Epicutaneous allergen immunotherapy induces a profound and selective modulation in skin dendritic-cell subsets. J. Allergy Clin. Immunol. 150, 1194–1208 (2022).
Lombardi, V. & Akbari, O. Dendritic cell modulation as a new interventional approach for the treatment of asthma. Drug N. Perspect. 22, 445–451 (2009).
Xu, J. et al. The role of DC subgroups in the pathogenesis of asthma. Front. Immunol. 15, 1481989 (2024).
Nam, J.-H. et al. Functional ambivalence of dendritic cells: tolerogenicity and immunogenicity. Int. J. Mol. Sci. 22, 4430 (2021).
Dao Nyesiga, G. et al. Tolerogenic dendritic cells generated in vitro using a novel protocol mimicking mucosal tolerance mechanisms represent a potential therapeutic cell platform for the induction of immune tolerance. Front Immunol. 14, 1045183 (2023).
Pallotta, M. T. et al. Indoleamine 2,3-dioxygenase is a signaling protein in long-term tolerance by dendritic cells. Nat. Immunol. 12, 870–878 (2011).
An, X. J. et al. Immature dendritic cells expressing indoleamine 2,3-dioxygenase suppress ovalbumin-induced allergic airway inflammation in mice. J. Investig. Allergol. Clin. Immunol. 21, 185–192 (2011).
Que, W., Guo, W.-Z. & Li, X.-K. Manipulation of regulatory dendritic cells for induction transplantation tolerance. Front. Immunol. 11, 582658 (2020).
Horton, C., Shanmugarajah, K. & Fairchild, P. J. Harnessing the properties of dendritic cells in the pursuit of immunological tolerance. Biomed. J. 40, 80–93 (2017).
de Aragão-França et al. Tolerogenic dendritic cells reduce airway inflammation in a model of dust mite-triggered allergic inflammation. Allergy Asthma Immunol. Res 10, 406–419 (2018).
Mohammadi, P., Hesari, M., Chalabi, M., Salari, F. & Khademi, F. An overview of immune checkpoint therapy in autoimmune diseases. Int. Immunopharmacol. 107, 108647 (2022).
Waterhouse, P. et al. Lymphoproliferative disorders with early lethality in mice deficient in Ctla-4. Science 270, 985–988 (1995).
Zheng, Y. et al. A meta-analysis of the association between CTLA-4 genetic polymorphism and susceptibility of asthma. Medicine 97, e11380 (2018).
Rudd, C. E. & Schneider, H. Unifying concepts in CD28, ICOS and CTLA4 co-receptor signalling. Nat. Rev. Immunol. 3, 544–556 (2003).
Grohmann, U. et al. CTLA-4-Ig regulates tryptophan catabolism in vivo. Nat. Immunol. 3, 1097–1101 (2002).
Maazi, H. et al. Cytotoxic T lymphocyte antigen 4-immunoglobulin G is a potent adjuvant for experimental allergen immunotherapy. Clin. Exp. Immunol. 172, 113–120 (2013).
Puricelli, C. et al. Cutting-edge delivery systems and adjuvants in tolerogenic vaccines: a review. Pharmaceutics 14, 1782 (2022).
Unger, W. W. J., Laban, S., Kleijwegt, F. S., van der Slik, A. R. & Roep, B. O. Induction of Treg by monocyte-derived DC modulated by vitamin D3 or dexamethasone: differential role for PD-L1. Eur. J. Immunol. 39, 3147–3159 (2009).
Obregon, C., Kumar, R., Pascual, M. A., Vassalli, G. & Golshayan, D. Update on Dendritic Cell-Induced Immunological and Clinical Tolerance. Front Immunol. 8, 1514 (2017).
Engeroff, P. et al. Allergens displayed on virus-like particles are highly immunogenic but fail to activate human mast cells. Allergy: Eur. J. Allergy Clin. Immunol. 73, 341–349 (2018).
Brune, K. D. et al. Plug-and-Display: decoration of Virus-Like Particles via isopeptide bonds for modular immunization. Sci. Rep. 6, 19234 (2016).
Wojta-Stremayr, D. et al. CD8+ T cell fate and function influenced by antigen-specific virus-like nanoparticles co-expressing membrane tethered IL-2. Plos One 10, e0126034 (2015).
Chazal, N. & Gerlier, D. Virus entry, assembly, budding, and membrane rafts. Microbiol. Mol. Biol. Rev. 67, 226–237 (2003).
Maldonado, R. & Von Andrian, U. How tolerogenic dendritic cells induce regulatory T cells. Adv. Immunol. 108, 111–165 (2010).
Tuettenberg, A., Fondel, S., Steinbrink, K., Enk, A. H. & Jonuleit, H. CD40 signalling induces IL-10-producing, tolerogenic dendritic cells. Exp. Dermatol. 19, 44–53 (2010).
Flórez-Grau, G., Zubizarreta, I., Cabezón, R., Villoslada, P. & Benitez-Ribas, D. Tolerogenic dendritic cells as a promising antigen-specific therapy in the treatment of multiple sclerosis and neuromyelitis optica from preclinical to clinical trials. Front. Immunol. 9, 1–10 (2018).
Comi, M., Amodio, G. & Gregori, S. Interleukin-10-producing DC-10 is a unique tool to promote tolerance via antigen-specific T regulatory Type 1 cells. Front. Immunol. 9, 682 (2018).
Akdis, C. A. & Akdis, M. Mechanisms of immune tolerance to allergens: role of IL-10 and Tregs. J. Clin. Investig. 124, 4678–4680 (2014).
Coomes, S. M. et al. CD4 + Th2 cells are directly regulated by IL-10 during allergic airway inflammation. Mucosal Immunol. 10, 150–161 (2017).
Platten, M., Wick, W. & Van Den Eynde, B. J. Tryptophan catabolism in cancer: Beyond IDO and tryptophan depletion. Cancer Res. 72, 5435–5440 (2012).
Baban, B. et al. IDO activates regulatory T cells and blocks their conversion into Th17-like T cells. J. Immunol. 183, 2475–2483 (2009).
Taher, Y. A. et al. Indoleamine 2,3-dioxygenase-dependent tryptophan metabolites contribute to tolerance induction during allergen immunotherapy in a mouse model. J. Allergy Clin. Immunol. 121, 16–18 (2008).
Kratzer, B. et al. Prevention of allergy by virus-like nanoparticles (VNP) delivering shielded versions of major allergens in a humanized murine allergy model. Allergy 74, 246–260 (2018).
Soneoka, Y. et al. A transient three-plasmid expression system for the production of high-titer retroviral vectors. Nucleic Acids Res 23, 628–633 (1995).
Pitoiset, F. et al. Retrovirus-based virus-like particle immunogenicity and its modulation by toll-like receptor activation. J. Virol. 91. (2017).
Acknowledgements
We thank the staff at Centre d’Experimentation Fonctionnelle (UMS 28 – Sorbonne UniversitéSite Pitié-Salpêtrière) for taking care of the mice, Wing Yan Yuen and Bruno Gouritin fortechnical assistance.
Author information
Authors and Affiliations
Contributions
B.B. conceptualized the study and supervised the project. The methodology was developed by B.B., P.A.X., J.V., B.L., and D.K. Experiments were conducted by P.A.X., J.V., B.L., J.M. Analysis and visualization were handled by P.A.X., J.V., B.L., N.T. Funding was acquired by B.B. The original draft was written by P.A.X, J.V. and B.B., before being reviewed and edited by all authors.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Vinot, PA., Vigneron, J., Marsande, J. et al. Immune checkpoint-engineered virus-like particles induce antigen-specific immune tolerance and protect against food allergy. npj Vaccines 11, 43 (2026). https://doi.org/10.1038/s41541-026-01379-y
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41541-026-01379-y