Abstract
The coronavirus disease 2019 (COVID-19) pandemic, which is caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), has been associated with more than 780,000 deaths worldwide (as of 20 August 2020). To develop antiviral interventions quickly, drugs used for the treatment of unrelated diseases are currently being repurposed to treat COVID-19. Chloroquine is an anti-malaria drug that is used for the treatment of COVID-19 as it inhibits the spread of SARS-CoV-2 in the African green monkey kidney-derived cell line Vero1,2,3. Here we show that engineered expression of TMPRSS2, a cellular protease that activates SARS-CoV-2 for entry into lung cells4, renders SARS-CoV-2 infection of Vero cells insensitive to chloroquine. Moreover, we report that chloroquine does not block infection with SARS-CoV-2 in the TMPRSS2-expressing human lung cell line Calu-3. These results indicate that chloroquine targets a pathway for viral activation that is not active in lung cells and is unlikely to protect against the spread of SARS-CoV-2 in and between patients.
Similar content being viewed by others
Main
Chloroquine and hydroxychloroquine are used for the treatment of malaria and have been widely used to treat patients with COVID-19. Both of these drugs are currently under investigation in more than 80 registered clinical trials for the treatment of COVID-19 worldwide2,3. Chloroquine and hydroxychloroquine inhibit the ability of SARS-CoV-2 to infect Vero cells1,5,6, providing a rational for using these drugs for the treatment of COVID-19. However, it is unknown whether these drugs inhibit the infection of lung cells and it is poorly understood how they inhibit infection with SARS-CoV-2.
Chloroquine and hydroxychloroquine increase the endosomal pH of cells and inhibit viruses that depend on low pH for cell entry7. We investigated whether these drugs could also block the cell entry by SARS-CoV-2 and whether entry inhibition accounted for the prevention of infection with SARS-CoV-2. Moreover, we investigated whether entry inhibition is cell-type-dependent, as the virus can use pH-dependent and pH-independent pathways for entry into cells. The spike (S) protein of SARS-CoV-2, which mediates viral entry, is activated by the endosomal-pH-dependent cysteine protease cathepsin L (CTSL) in some cell lines4. By contrast, entry into airway epithelial cells, which express low levels of CTSL8, depends on the pH-independent, plasma-membrane-resident serine protease TMPRSS24. Notably, the use of CTSL by coronaviruses is restricted to cell lines8,9,10, whereas TMPRSS2 activity is essential for the spread and pathogenesis of the virus in the infected host11,12.
We compared the inhibition by chloroquine and hydroxychloroquine of S-mediated entry into Vero (kidney), TMPRSS2-expressing Vero and Calu-3 (lung) cells. Calu-3 cells, as with the airway epithelium, express low amounts of CTSL8 and SARS-CoV-2 entry into these cells is dependent on TMPRSS24. By contrast, entry of SARS-CoV-2 into Vero cells is CTSL-dependent, and both CTSL and TMPRSS2 support entry into TMPRSS2-expressing Vero cells4. As a control, we used camostat mesylate, which inhibits TMPRSS2-dependent entry into cells4.
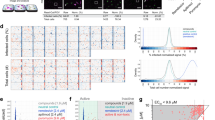
Treatment with camostat mesylate did not interfere with cell viability, whereas chloroquine and hydroxychloroquine slightly reduced the viability of Vero, TMPRSS2-expressing Vero and Calu-3 cells when applied at the highest concentration (Fig. 1a). Inhibition of S-driven entry by camostat mesylate was observed only in TMPRSS2+ cell lines, as expected (Fig. 1a and Table 1). Moreover, chloroquine and hydroxychloroquine inhibited S-driven entry into TMPRSS2− Vero cells with high efficiency whereas the inhibition of entry into TMPRSS2+ Calu-3 and TMPRSS2+ Vero cells was inefficient and absent, respectively (Fig. 1a and Table 1). Therefore, chloroquine and hydroxychloroquine can block S-driven entry, but this inhibition is cell-line-dependent and efficient inhibition is not observed in TMPRSS2+ lung cells.
a, Vero, TMPRSS2-expressing Vero and Calu-3 cells were preincubated for 2 h with the respective inhibitors (0 μM, 0.01 μM, 0.1 μM, 1 μM, 10 μM or 100 μM) and then inoculated with replication-defective vesicular stomatitis virus reporter particles bearing the S protein. Top, the transduction efficiency of the virus was assessed. Bottom, cells were not inoculated with virus particles but cell viability after drug treatment was instead assessed at the same time as transduction was quantified. Transduction efficiency was quantified by measuring virus-encoded luciferase activity in cell lysates. Cell viability was measured using the CellTiter-Glo assay. Data are mean ± s.e.m. of three biological replicates, each of which consisted of quadruplicate samples. Data were normalized as the relative entry efficiency or cell viability of inhibitor-treated cells compared with those of untreated cells (set to 100%). The calculated 50% inhibitory concentration (IC50) values are summarized in Table 1. b, Untreated or chloroquine-preincubated Vero and Calu-3 cells were inoculated with SARS-CoV-2 Munich isolate (patient isolate 929, BetaCoV/Munich/BavPat1/2020|EPI_ISL_406862) at a multiplicity of infection (MOI) of 0.001. After inoculation for 24 h, viral RNA was isolated from the culture supernatant (extracellular virus) (dark blue) and the infected cells (intracellular virus) (light blue), and SARS-CoV-2 genome equivalents (GE) were determined by quantitative PCR with reverse transcription. Data are mean ± s.e.m. of three biological replicates, each of which consisted of single samples. c, The experiment was conducted as described in b, but the number of infectious SARS-CoV-2 particles in culture supernatants was determined by plaque titration using Vero E6 cells. PFU, plaque-forming units. Statistical significance was analysed by two-way analysis of variance (ANOVA) with Dunnett’s post hoc test. NS, not significant (P > 0.05); *P ≤ 0.05; **P ≤ 0.01; ***P ≤ 0.001. P values (from left to right) are as follows. a, Entry efficiency (camostat mesylate/chloroquine/hydroxychloroquine), Vero (0.9999/0.8587/0.9997, 0.9842/0.9846/0.3904, 0.6860/0.0991/0.0223, 0.9968/0.0001/0.0001, 0.9997/0.0001/0.0001), TMPRSS2-expressing Vero (0.9999/0.9968/0.9795, 0.1251/0.9962/0.9998, 0.0004/0.9997/0.9999, 0.0001/0.9967/0.9982, 0.0001/0.9981/0.9986; Calu-3 (0.9900/0.9999/0.9986, 0.0003/0.9999/0.9983, 0.0001/0.9988/0.9929, 0.0001/0.1291/0.9938, 0.0001/0.0005/0.0045); cell viability (camostat mesylate/chloroquine/hydroxychloroquine), Vero (0.9273/0.9999/0.9999, 0.9999/0.8710/0.9642, 0.9999/0.9996/0.9999, 0.9999/0.8958/0.4818, 0.9998/0.0838/0.0161), TMPRSS2-expressing Vero (0.9998/0.9999/0.9959, 0.9811/0.9985/0.9362, 0.9998/0.9985/0.9997, 0.9997/0.8835/0.9998, 0.9999/0.0315/0.1422), Calu-3 (0.9986/0.9999/0.9999, 0.9999/0.9997/0.9999, 0.9986/0.9999/0.8134, 0.9924/0.9275/0.7125, 0.9983/0.0492/0.0002). b, (extracellular/intracellular), Vero (0.6844/0.6989, 0.0121/0.0002, 0.0002/0.0001), Calu-3 (0.9434/0.8800, 0.9999/0.8830, 0.0517/0.3924). c, (extracellular/intracellular), Vero (0.9561, 0.0001, 0.0001), Calu-3 (0.1184, 0.9997, 0.0987).
We next investigated whether the cell-type-dependent differences in entry inhibition translated into differential inhibition of authentic SARS-CoV-2. Indeed, chloroquine efficiently blocked SARS-CoV-2 infection of Vero kidney cells, as expected1, but did not efficiently inhibit SARS-CoV-2 infection of Calu-3 lung cells (Fig. 1b, c). A subtle reduction in SARS-CoV-2 infection was seen in the presence of 100 μM chloroquine, consistent with the modest inhibition of cellular entry of S-bearing pseudotypes under those conditions (Fig. 1a), but this effect was not statistically significant. In summary, chloroquine did not efficiently block the infection of Calu-3 cells with S-bearing pseudotypes and authentic SARS-CoV-2, indicating that—in these cells—chloroquine does not appreciably interfere with viral entry or the subsequent steps of the viral replication cycle.
Research to confirm our results in primary respiratory epithelium is ongoing. Moreover, virus production in Calu-3 cells relative to Vero E6 cells was more robust in the present study compared with a previously published study13, potentially due to the use of the Calu-3 subclone 2B4 in the previous but not the present study. Nevertheless, our results suggest that chloroquine and hydroxychloroquine will exert no antiviral activity in human lung tissue and will not be effective against COVID-19, in keeping with the results of recent clinical trials14,15. Moreover, our results highlight the fact that cell lines that mimic important aspects of respiratory epithelial cells should be used when analysing the antiviral activity of compounds that target host cell functions.
Methods
Data reporting
No statistical methods were used to predetermine sample size. The experiments were not randomized and the investigators were not blinded to allocation during experiments and outcome assessment.
Cells
Vero 76, Vero 76 stably expressing TMPRSS2 (both used for pseudotype experiments)4, the Vero 76 subclone Vero E6 (used for SARS-CoV-2 experiments), HEK293T and Calu-3 cells16 were cultured in Dulbecco’s modified Eagle’s medium (DMEM) or minimum essential medium (MEM, Calu-3) supplemented with 10% fetal bovine serum (FBS) and 1% penicillin–streptomycin. In case of Calu-3 cells, the medium was also supplemented with 1% non-essential amino acids and 1% sodium pyruvate. All cell lines were incubated at 37 °C and 5% CO2 and were obtained from repositories (Vero E6 and HEK293T) or collaborators (Calu-3 and Vero 76). Cell lines were free of mycoplasma, authenticated on the basis of morphology and growth properties and confirmed by PCR to be of the correct species. The cell lines used were not listed as commonly misidentified cell lines by the ICLAC register.
Production of pseudotyped particles
Vesicular stomatitis virus (VSV) particles pseudotyped with SARS-CoV-2 S were generated according to published protocols4,17. At 24 h after transfection, HEK293T cells expressing the S protein were inoculated with a replication-restricted, VSV-G-trans-complemented VSV, which lacks the genetic information for VSV-G but instead encodes the reporter genes eGFP (enhanced green fluorescent protein) and FLuc (firefly luciferase), VSV*ΔG-FLuc18 (provided by G. Zimmer). After 1 h of incubation at 37 °C and 5% CO2, the inoculum was aspirated and the cells were washed with phosphate-buffered saline (PBS) before culture medium was added. The culture medium was further supplemented with the culture supernatant from I1-hybridoma cells (CRL-2700 cells, ATCC) containing anti-VSV-G antibody (1:1,000) to inactivate residual input virus. After an incubation period of 18 h at 37 °C and 5% CO2, the culture supernatant was collected, centrifuged to pellet cellular debris, and the clarified supernatant was aliquoted and stored at −80 °C until further use.
Transduction of target cells with pseudotypes and its inhibition
For transduction experiments, Vero, TMPRSS2-expressing Vero and Calu-3 cells were grown in 96-well plates and allowed to reach about 50–70% confluency. Then, cells were preincubated with medium containing different concentrations (10 nM, 100 nM, 1 μM, 10 μM or 100 μM) of camostat mesylate (Sigma-Aldrich), chloroquine or hydroxychloroquine (both Tocris) or DMSO (Roth, solvent control) for 2 h at 37 °C and 5% CO2, before they were inoculated with S-bearing VSV. At 18 h after transduction, culture supernatants were aspirated and cells were lysed by incubation (30 min, room temperature) with Cell Culture Lysis Reagent (Promega). Cell lysates were subsequently transferred to white, opaque-walled 96-well plates and FLuc activity was quantified as an indicator of transduction efficiency, using the Beetle-Juice substrate (PJK) and a Hidex Sense plate reader (Hidex) operated with Hidex plate reader software (version 0.5.41.0, Hidex). Raw luminescence values (indicating luciferase activity) were recorded as counts per second. For normalization, transduction of DMSO-treated cells was set to 100% and the relative transduction efficiencies in the presence of camostat mesylate, chloroquine or hydroxychloroquine were calculated. Transduction experiments were performed in technical quadruplicates using three separate pseudotype preparations.
SARS-CoV-2 infection of target cells and its inhibition
Virus infections were done with SARS-CoV-2 Munich isolate 929. Vero E6 or Calu-3 cells were seeded at densities of 3.5 × 105 cells per ml or 6 × 105 cells per ml in 12-well plates, respectively. After 24 h, cells were incubated with chloroquine (1 μM, 10 μM or 100 μM) or left untreated (control) for 1 h at 37 °C. Subsequently, cells were infected with an MOI of 0.001 in serum-free OPTIpro medium containing the above-mentioned chloroquine concentrations at 4 °C for 30 min to enable virus attachment. Afterwards, infection medium was removed and the wells were washed twice with PBS and DMEM supplemented with chloroquine was added as described above and the plates were incubated at 37 °C. Samples were taken at 24 h after infection. Infection experiments were conducted with biological triplicates in a biosafety level 3 laboratory.
Viral RNA extraction and quantitative RT–PCR
For viral RNA extraction from supernatants, 50 μl of cell culture supernatant was mixed with RAV1 lysis buffer (Macherey-Nagel) followed by an incubation at 70 °C for 10 min. RNA extraction was performed as recommended by the manufacturer (Macherey-Nagel). For intracellular viral RNA extraction, cells were washed with PBS and lysed with TRIzol (Zymo). SARS-CoV-2 genome equivalents were detected by quantitative RT–PCR targeting the SARS-CoV-2 E gene as previously reported19, using the following primers: E_Sarbeco_F, ACAGGTACGTTAATAGTTAATAGCGT; E_Sarbeco_P1, FAM-ACACTAGCCATCCTTACTGCGCTTCG-BBQ; E_Sarbeco_R, ATATTGCAGCAGTACGCACACA. The quantitative RT–PCR experiment and data processing were carried out using the LightCycler 480 Real-Time PCR System (Roche) and LightCycler 480 Software (version 1.5, Roche Molecular Systems). Absolute quantification was performed using SARS-CoV-2-specific in vitro-transcribed RNA standards, as previously described19.
Plaque assay
Infectious SARS-CoV-2 plaque-forming units were quantified by plaque titration on Vero E6 cells, as previously described20, with minor modifications. Vero E6 monolayers were seeded in 24-well plates, washed with PBS, incubated with serial dilutions of SARS-CoV-2-containing cell culture supernatants in duplicates, and overlaid with 1.2% Avicel in DMEM, supplemented as described above. After 72 h, cells were fixed with 6% formaline and visualized by crystal violet staining.
Cell viability assay
The cell viability was quantified using the CellTiter-Glo assay (Promega) and using the same experimental conditions as described above for transduction experiments with the exception that cells were not inoculated with virus particles. In brief, cells were preincubated for 2 h at 37 °C and 5% CO2 with medium containing different concentrations (10 nM, 100 nM, 1 μM, 10 μM or 100 μM) of camostat mesylate, chloroquine or hydroxychloroquine, or DMSO (solvent control), before culture medium was added (instead of medium containing VSV pseudotyped with SARS-CoV-2 S) and cells were further incubated for 18 h. Next, intracellular ATP levels were quantified as an indicator of cell viability. For this, culture supernatants were aspirated and cells were lysed by incubation with CellTiter-Glo substrate for 30 min at room temperature. Cell lysates were subsequently transferred to white, opaque-walled 96-well plates and luminescence was measured using a Hidex Sense plate reader (Hidex). Luminescence values (indicating cell viability) were recorded as absolute counts over a period of 200 ms per well. For normalization, cell viability of control-treated cells was set to 100% and the relative viability of cells incubated in the presence of camostat mesylate, chloroquine or hydroxychloroquine was calculated. Cell viability experiments were performed in technical quadruplicates and repeated with three separately prepared dilution series of the inhibitors.
Statistical analysis
Two-way ANOVA with Dunnett’s post hoc test was performed to analyse statistical significance of differences in transduction efficiencies, SARS-CoV-2 genome equivalents or SARS-CoV-2 titres between control- and inhibitor-treated cells. P > 0.05, not significant; *P ≤ 0.05; **P ≤ 0.01; ***P ≤ 0.001). The IC50 values, which indicate the inhibitor concentration that led to a 50% reduction in transduction, were calculated using a nonlinear regression model with variable slope. Statistical analyses and IC50 calculations were performed using GraphPad Prism (version 8.4.2).
Reporting summary
Further information on research design is available in the Nature Research Reporting Summary linked to this paper.
Data availability
All data are provided with the paper. Source data are provided with this paper.
References
Wang, M. et al. Remdesivir and chloroquine effectively inhibit the recently emerged novel coronavirus (2019-nCoV) in vitro. Cell Res. 30, 269–271 (2020).
Ferner, R. E. & Aronson, J. K. Chloroquine and hydroxychloroquine in covid-19. Br. Med. J. 369, m1432 (2020).
Touret, F. & de Lamballerie, X. Of chloroquine and COVID-19. Antiviral Res. 177, 104762 (2020).
Hoffmann, M. et al. SARS-CoV-2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor. Cell 181, 271–280 (2020).
Yao, X. et al. In vitro antiviral activity and projection of optimized dosing design of hydroxychloroquine for the treatment of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Clin. Infect. Dis. 71, 732–739 (2020).
Liu, J. et al. Hydroxychloroquine, a less toxic derivative of chloroquine, is effective in inhibiting SARS-CoV-2 infection in vitro. Cell Discov. 6, 16 (2020).
Rolain, J. M., Colson, P. & Raoult, D. Recycling of chloroquine and its hydroxyl analogue to face bacterial, fungal and viral infections in the 21st century. Int. J. Antimicrob. Agents 30, 297–308 (2007).
Park, J. E. et al. Proteolytic processing of Middle East respiratory syndrome coronavirus spikes expands virus tropism. Proc. Natl Acad. Sci. USA 113, 12262–12267 (2016).
Shirato, K., Kawase, M. & Matsuyama, S. Wild-type human coronaviruses prefer cell-surface TMPRSS2 to endosomal cathepsins for cell entry. Virology 517, 9–15 (2018).
Shirato, K., Kanou, K., Kawase, M. & Matsuyama, S. Clinical isolates of human coronavirus 229E bypass the endosome for cell entry. J. Virol. 91, e01387-16 (2016).
Iwata-Yoshikawa, N. et al. TMPRSS2 contributes to virus spread and immunopathology in the airways of murine models after coronavirus infection. J. Virol. 93, e01815-18 (2019).
Zhou, Y. et al. Protease inhibitors targeting coronavirus and filovirus entry. Antiviral Res. 116, 76–84 (2015).
Matsuyama, S. et al. Enhanced isolation of SARS-CoV-2 by TMPRSS2-expressing cells. Proc. Natl Acad. Sci. USA 117, 7001–7003 (2020).
Boulware, D. R. et al. A randomized trial of hydroxychloroquine as postexposure prophylaxis for COVID-19. N. Engl. J. Med. 383, 517–525 (2020).
Kupferschmidt, K. Big studies dim hopes for hydroxychloroquine. Science 368, 1166–1167 (2020).
Klemm, C. et al. Mitogen-activated protein kinases (MAPKs) regulate IL-6 over-production during concomitant influenza virus and Staphylococcus aureus infection. Sci. Rep. 7, 42473 (2017).
Kleine-Weber, H. et al. Mutations in the spike protein of Middle East respiratory syndrome coronavirus transmitted in Korea increase resistance to antibody-mediated neutralization. J. Virol. 93, e01381-18 (2019).
Berger Rentsch, M. & Zimmer, G. A vesicular stomatitis virus replicon-based bioassay for the rapid and sensitive determination of multi-species type I interferon. PLoS ONE 6, e25858 (2011).
Corman, V. M. et al. Detection of 2019 novel coronavirus (2019-nCoV) by real-time RT-PCR. Eurosurveill. 25, 2000045 (2020).
Herzog, P., Drosten, C. & Müller, M. A. Plaque assay for human coronavirus NL63 using human colon carcinoma cells. Virol. J. 5, 138 (2008).
Acknowledgements
This work was supported by the Bundesministerium für Bildung und Forschung (RAPID Consortium, 01KI1723A and 01KI1723D to C.D. and S.P., respectively). We thank A. Maisner (Vero 76 cell line), S. Ludwig (Calu-3 cell line) and G. Zimmer (VSV pseudotype system) for providing cell lines and reagents.
Author information
Authors and Affiliations
Contributions
M.H. and S.P. designed the study. M.H., K.M., H.H.-W., A.K., H.K.-W., N.K., N.C.G. and M.A.M. performed research. M.H., M.A.M., C.D. and S.P. analysed the data. C.D. provided essential reagents. M.H. and S.P. wrote the manuscript. All authors revised the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Source data
Rights and permissions
About this article
Cite this article
Hoffmann, M., Mösbauer, K., Hofmann-Winkler, H. et al. Chloroquine does not inhibit infection of human lung cells with SARS-CoV-2. Nature 585, 588–590 (2020). https://doi.org/10.1038/s41586-020-2575-3
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41586-020-2575-3
This article is cited by
-
Drug repurposing: a promising drug discovery strategy for the treatment of emerging epidemic infectious disease
Molecular Diversity (2026)
-
Targeting PANoptosis: a promising therapeutic strategy for ALI/ARDS
Apoptosis (2025)
-
Multi-omics analysis uncovered systemic lupus erythematosus and COVID-19 crosstalk
Molecular Medicine (2024)
-
COVID-19 drug discovery and treatment options
Nature Reviews Microbiology (2024)
-
Nanoparticulate curcumin spray imparts prophylactic and therapeutic properties against SARS-CoV-2
Emergent Materials (2024)



John H Abeles
First, hydroxychloroquine should be the drug examined as several studies point out its potency, and dew if any clinicians reply chloroquine itself
Second, the initial entry of virus is in nasophyngeal tissue not in lungs, and the best results reported ising hydroxychloroquine in multiple Covid19 studies - both large scale observational and some double blind studies- are when used early on in the disease.
Lastly, one of the principal actions of HCQ is as a zinc ionophore. Zinc has been shown potently active against virus replication. Without added zinc, any laboratory study is not adequately assessing clinical utility in which adjunctive zinc is used ( populations studies often show consistent zinc deficiencies in most Western populations)
Here below are some pertinent positive references for further reading on the question of HCQ plus zinc plus either doxycycline ( my preferred choice because it isn’t associated with further small cardiac risk) or azithromycin
Note : Most of the successful reports of the use of HCQ plus zinc etc are in early stage, outpatients and not in late stage, hospitalised patients
The first link is a large data base (more than 50 studies ) on HCQ in Covid19 treatment
The second reference is an important review from a Yale University professor ...
The third and fourth are on a recent, large, well conducted observational study from Henry Ford Hospital ...
The fifth is an important outpatient study ...
https://c19study.com/
https://academic.oup.com/aj...
https://www.ijidonline.com/...
https://www.henryford.com/n...
https://www.preprints.org/m...
https://www.ijidonline.com/...
https://www.preprints.org/m...
https://aapsonline.org/hcq-...
https://www.medrxiv.org/con...
https://www.preprints.org/m...
https://www.evms.edu/media/...
https://link.springer.com/a...
https://pjmedia.com/news-an...
https://www.medrxiv.org/con...
https://www.medrxiv.org/con...
https://www.middleeasteye.n...
http://www.ijmr.org.in/prep...
https://aapsonline.org/hydr...
decide/
https://www.indiatoday.in/i...
ohminus Replied to John H Abeles
If the mechanism doesn't work, the mechanism doesn't work. Hydroxychloroquine doesn't work via substantially different pathways.
And a large, well conducted observational study is still weak evidence.
The review is from May and as such already quite outdated.
As for the use in outpatients, that may well be, but doesn't adress the problem with COVID-19 and only poses new questions whether it is ethically defensible to use a drug that has substantial toxicity especially dangerous to the high risk group in patients that do not yet have a serious problem. All the more since data on long-term consequences is missing. Given that COVID-19 can damage the heart, giving a cardiotoxic drug may just exacerbate the long-term problems.
Add to that that it's scarce and already running out in many places for patients it is proven to help
Your linkspamming is decidedly unhelpful - all the more when it lists preprints, some posted months ago, without regard for peer review, and also lists studies not concerned with the specific issue at hand.
Jordan Geller Replied to ohminus
That is the tactic of all the Trump Neo-Luddites, obfuscate and cause confusion, bury in 'proof' (poor quality links) to maintain 'hope' in the the face of ever more conclusive proof of its ineffectiveness. This Arthritis/Malaria drug simply doesn't work for Sars-Cov-2 prophylaxis at any stage of exposure.
Globalist Juice Replied to Jordan Geller
My goodness, *orange man bad* ...EEEeeek!
- do you even have any broader thoughts, or has his mere presence muted every spark in your brain?
Julien Chavanton Replied to ohminus
"providing this early
version of the manuscript as a service to our authors and readers."
Well, this one is not reviews yet ...
ohminus Replied to Julien Chavanton
Try reading properly:
"This is an unedited manuscript that has been accepted for publication"
The only reviews still to come are those of the typeset final version - not for content but to see if anything was screwed up in editing.
Julien Chavanton Replied to ohminus
Once more you are quite arrogant in your comments.
Also it seems you are simply choosing to ignore the facts.
"The manuscript will undergo copyediting,
typesetting and a proof review before it is published in its final form. Please note that during
the production process errors may be discovered which could affect the content, and all legal
disclaimers apply."
ohminus Replied to Julien Chavanton
And you're projecting again.
But please, tell us how the fact that typesetting hasn't been done yet invalidates the content.
The one who chooses to ignore facts is you - the fact that it has been peer-reviewed.
Annoyed Citizen Replied to ohminus
The only thing you have proven here:
You don't even recognize an apple - bike - comparison scam when it's so obviously floating around in front of your nose:
1)
ncbi.nlm.nih.gov/pmc/articl...
https://pubmed.ncbi.nlm.nih...
2)
If anything should have been proven here, except empty gibberish:
This is what a reasonable test setup would have looked like:
Calu-3 - ACEII/ TMPRSSII+ - HBEC - HCQ - Comparison
Calu 3 - ACEII/ TMPRSSII+ - A549 - HCQ - Comparison
HBEC - ACEII/ TMPRSSII+ - A549 - HCQ - Comparison.
Optimal:
Calu-3 - ACEII/ TMPRSSII+- AECII - HCQ - Comparison
Calu 3 - ACEII/ TMPRSSII+ - AECII- HCQ - Comparison
HBEC - ACEII/ TMPRSSII+ - AECII- HCQ - Comparison
And in vitro doesn't really say anything anyway:
Remember, for example, the interferon success (non)story
Funny Update:
https://ijidonline.com/arti... (pr)
https://link.springer.com/a... (pr)
https://medrxiv.org/content... (pr)
https://ijmr.org.in/article... (pr)
https://academic.oup.com/aj... (pr)
ohminus Replied to Annoyed Citizen
The only thing you have proven here is that you believe you get to invent your own scientific standards so you can "lecture" people infinitely more qualified than you to assess the issue.
You clearly neither know how to do an actual literature research, instead cherrypicking your sources, nor do you know how to actually assess the quality of a study. You simply copy stuff someone else told you to copy and then try to drown the net in linkspam. Unfortunately, copy/paste doesn't substitute for graduate school.
Annoyed Citizen Replied to ohminus
You bubble so much mental garbage together here and ramble down your would-be expertise without a single source and accuse others of cherrypicking. There are countless sources that prove that the cell lines in in vitro studies are chosen with care and differences are to be considered, that the literature on this should slay you!
https://www.frontiersin.org...
"..."lecture" people infinitely more qualified than you to assess the issue."
You're NONE of them. And you obviously don't even know the reading you're rambling about here, otherwise you wouldn't fabricate so much verbal diarrhea.
ohminus Replied to Annoyed Citizen
Cute, coming from someone who believes defamation substitutes for arguments. Your attempt to assess my credentials is hilarious, but only underscores you have as little respect for the law as for science.
Googling yourself the world you'd like to have does not constitute literature research. It's clear you have no means to assess the quality of studies and the rigor of scientific journals.
Annoyed Citizen Replied to ohminus
Bla, bla, bla. Nothing new from you: No Source, nothing else, only "bla..."
ohminus Replied to Annoyed Citizen
Nothing new from you - insults and standards you refuse to meet yourself. Just the certainty that you are right and all experts in the field are wrong.
Falko Seger Replied to ohminus
Still waiting for quote. ;-)
Annoyed Citizen Replied to Falko Seger
As I have already announced to you:
https://www.ncbi.nlm.nih.go...
"While it has been shown that CQ does not block SARS-CoV-2 infection in the human lung cell line Calu-3 (Hoffmann et al., 2020b), it does greatly reduce viral infection in Huh7-ACE2 cells in our study. This inconsistency can be explained by that SARS-CoV-2 entry into Calu-3 cells is independent of endosomal acidification because of its high expression level of TMPRSS2, which activates spike at the plasma membrane; while the Huh7.5 (a derivative cell line of Huh7) cells heavily rely on the endosomal low pH for SARS-CoV-2 entry (Dittmar et al., 2021), resulting in a high dependence on lysosomes whose function can be inhibited by CQ. "
Your stupidity and your biological lack of understanding are now finally proven.
And still waiting and waiting and waiting...I'm still waiting for quotes! Where are right again your sources - not that there could be such, which would support your stupidity?!
ohminus Replied to Annoyed Citizen
Cute. Still nothing but insults, ignorance, and cherrypicked and misrepresented sources.
The only stupidity and biological lack of understanding you have proven are your own. Huh7.5 is a hepatocyte cell line - ie. liver cells.
Have fun proving to the world your belief that sufficient criminal drive can substitute for studying a topic. Meanwhile, I write actual biomedical publications.
Annoyed Citizen Replied to ohminus
Nobrainer after nobrainer. Not even grasping what I am talked about. Oh... btw: Good luck with NRP-1 and stupid antibodies versus HKNNKS... Laughing my ass of: An endosomal entry inhibitor should block ACEII/TMPRSSII? And babbling something about "You all have no idea and cherrypicking" Gnihihi! Your really dumb like hell, friend. No content and since almost 2 years "You don't nothing and I know something, without any study, any quote... No content.... Laughing my ass of.
Annoyed Citizen Replied to ohminus
I bet with you that you could not even bring me the citation, why the comparison with a verocell culture was possible at all, and why already by this no relevant significance can be made, because this process is not described in more detail and therefore BIAS would have to be assumed? Please quote for me, you funny little man.
Annoyed Citizen Replied to ohminus
And funniest thing:
YOU blustered that the studies were not peer reviewed. Now 5 of them are already through and you are still rambling!
Proves only one thing:
You're full of mental illness.
ohminus Replied to Annoyed Citizen
Still trying to substitute expertise with insults, I see. Peer review doesn't end like that, it continues even after a manuscript has been accepted for publication. The fact that a paper has been accepted in some journal does not mean its scientific craftsmanship is solid.
The only thing you prove is that you lack any and all pertinent expertise and simply smear and insult anyone who has said expertise.
Criminal energy does not substitute for years of training, I'm afraid.
ohminus Replied to Julien Chavanton
"Well, this one is not reviews yet ..."
Except it has, as evidenced by the fact that it's been accepted.
Come back when you have an idea about scientific publishing, rather than trying to invalidate a study based on typeface.
Fred_EM
Chloroquine alone does not inhibit infection of human lung cells with SARS-CoV-2
Chloroquine is recommended to be used together with zinc for treatment.
The study's authors should comment on that in their paper.
K Bruce
This paper skips over zinc and its roll as an ionophore.
Seems like they are leaping to conclusions based on upregulating one gene.
ohminus Replied to K Bruce
Seems like you don't understand molecular biology.
Julien Chavanton Replied to ohminus
another empty arrogant comment from you ... (not even an argument)
ohminus Replied to Julien Chavanton
It's cute when someone who believes himself qualified to lecture experts calls others "arrogant".
Julien Chavanton Replied to ohminus
Sarcasms, is your new best argument.
I may not be qualified to lecture experts in this field, but I can identify false statements like yours, it does not require much knowledge to do so.
ohminus Replied to Julien Chavanton
Cute. You believe yourself capable of a lot of things and prove the precise opposite every time you make a comment.
If you are not qualified to lecture experts, you are evidently on the wrong page, you have done nothing but pompously dismissing experts and claiming greater expertise than even some of the most respected researchers in the field on the entire planet.
Julien Chavanton Replied to ohminus
Right, best to trust the opinion of a self proclaimed expert, blinded, arrogant.
I did not dismiss anything, I guess you tend to be always right as you argument with yourself.
I look at your comments on other topics just to see who you are, wow you are pretending to be an expert at everything.
ohminus Replied to Julien Chavanton
Cute, coming from someone who doesn't even trust the certified and world-wide renowned experts responsible for the publication, nor those deemed qualified by "Nature" to review this publication.
Your waffling about "self-proclaimed expert" is just your usual resorting to fabrication because you lack substance. Defamation is the only game you can play, and you don't even realize when you're way out of your league. Totally aside from the fact that I happen to have a biomedical research doctorate, your suggestion that I was the expert at issue in my post only underscores you lack any and all understanding of the scientific sector and are merely here to throw mud.
Annoyed Citizen Replied to ohminus
Still didn't grasp the point: Narf....
Why would a drug, that inhibits ENDOSOMAL ENTRY -NOT ACE2/TMPRSS2 entry?! Uuuuuh!
Good luck with your stupidity and your selling of nothing burger.
As I have already announced to you:
https://www.ncbi.nlm.nih.go...
"While it has been shown that CQ does not block SARS-CoV-2 infection in the human lung cell line Calu-3 (Hoffmann et al., 2020b), it does greatly reduce viral infection in Huh7-ACE2 cells in our study. This inconsistency can be explained by that SARS-CoV-2 entry into Calu-3 cells is independent of endosomal acidification because of its high expression level of TMPRSS2, which activates spike at the plasma membrane; while the Huh7.5 (a derivative cell line of Huh7) cells heavily rely on the endosomal low pH for SARS-CoV-2 entry (Dittmar et al., 2021), resulting in a high dependence on lysosomes whose function can be inhibited by CQ. "
Your stupidity and your biological lack of understanding are now finally proven.
https://www.ncbi.nlm.nih.go...
Mysteryposter
Quote "Moreover, we report that chloroquine does not block SARS-CoV-2 infection of the TMPRSS2-positive lung cell line Calu-3"
-------------
Calu-3 is a human lung cancer cell line
https://en.wikipedia.org/wi...
So what this in vitro study proves is that (hydroxy)chloroquine doesn't protect cancer cells against virusses. And it does protect healthy cells, like proved in vitro for healthy kidney cells
https://twitter.com/richard...
ohminus Replied to Mysteryposter
I'm afraid the only thing you have proven is that you do not understand cell culture. And pointing at kidney cells is hilarious when the point of the paper is that the molecular mechanism doesn't exist in lung cells.
Jay_J Jacob
Frontline Doctor who is an Ophthalmologist thinks this drug can cure lung cancer.
The medicine protects normal cells, at the same time as ALLOWS the COVID-19 virus to annihilate cancer cells.
This study is almost a COVER-UP for the cure for cancer!
ohminus Replied to Jay_J Jacob
Ophthalmologist? Yeah, because that's certainly a pertinent specialist.
Robert Clark Replied to Jay_J Jacob
:)
Jean-Claude Jeanine Jamoulle
Thanks for your article : Your abstract ... "Here, we show that engineered expression of TMPRSS2, a cellular protease that activates SARS-CoV-2 for entry into lung cells4, renders SARS-CoV-2 infection of Vero cells insensitive to chloroquine ... This suggests that chloroquine would be active in the presence of a drug inhibitor of the cellular protease ... Thanks for your answer . KR Jean-Claude