Abstract
Despite advances in type 2 diabetes (T2D) management, unmet needs remain for therapies that effectively control hyperglycaemia while addressing comorbid metabolic disorders1,2. Here we assessed the efficacy and safety of the dual glucagon receptor (GCGR)/glucagon-like peptide-1 receptor (GLP-1R) agonist mazdutide monotherapy versus placebo in Chinese adults with T2D controlled inadequately with diet and exercise alone. In this phase 3 trial, 320 participants (mean glycated haemoglobin A1c (HbA1c) of 8.24%, body mass index of 28.2 kg m−2 and diabetes duration of 1.9 years) were randomized 1:1:1 to receive weekly subcutaneous injections of mazdutide (4 mg or 6 mg) or placebo for 24 weeks, followed by a 24-week extended mazdutide treatment. At week 24, mazdutide significantly reduced HbA1c versus placebo (primary endpoint): −1.57% with mazdutide 4 mg and −2.15% with mazdutide 6 mg, versus −0.14% with placebo, with treatment differences of −1.43% and −2.02% (both P < 0.0001). Weight loss from baseline at week 24 occurred with −5.61% (4 mg) and −7.81% (6 mg) versus −1.26% (placebo) (both P < 0.0001). Furthermore, more participants with mazdutide achieved HbA1c < 7.0%, weight loss ≥ 5% (all P < 0.0001) and composite endpoints (HbA1c < 7.0% and weight loss ≥ 5%) versus placebo (P = 0.0006 for 4 mg; P < 0.0001 for 6 mg) at week 24. The most common adverse events—diarrhoea, decreased appetite and nausea—were consistent with GLP-1R agonists. These results establish mazdutide monotherapy as an effective intervention providing clinically meaningful glycaemic control and weight reduction alongside a favourable safety profile in this population.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$32.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
De-identified data supporting this study’s findings are available to other qualified researchers upon request. Interested parties may contact the corresponding authors (Dalong Zhu (zhudalong@nju.edu.cn), Jiajun Zhao (jjzhao@sdu.edu.cn) or Lei Qian (cnradium@126.com)). Requests will be reviewed; approved access requires an ethics committee endorsement of the proposed data use and execution of a data access agreement with Innovent Biologics. The clinical study protocol can be found in the Clinical Protocol (Supplementary Information, Clinical Protocol) and the statistical analysis plan is provided in the Supplementary Information.
Code availability
All statistical analyses were completed using SAS v9.4. Data collection was completed using TriaMaster Electronic Data Capture v.5.0.
References
Avogaro, A. & Fadini, G. P. Microvascular complications in diabetes: a growing concern for cardiologists. Int. J. Cardiol. 291, 29–35 (2019).
Davies, M. J. et al. Management of hyperglycaemia in type 2 diabetes, 2022. A consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care 45, 2753–2786 (2022).
International Diabetes Federation. IDF Diabetes Atlas 11th edn (IDF, 2025).
Xu, Y. et al. Diabetes in China part 1: epidemiology and risk factors. Lancet Public Health 9, e1089–e1097 (2024).
Wang, L. et al. Prevalence and treatment of diabetes in China, 2013–2018. JAMA 326, 2498–2506 (2021).
Marso, S. P. et al. Design of the liraglutide effect and action in diabetes: evaluation of cardiovascular outcome results (LEADER) trial. Am. Heart J. 166, 823–830 (2013).
Jendle, J. et al. Efficacy and safety of dulaglutide in the treatment of type 2 diabetes: a comprehensive review of the dulaglutide clinical data focusing on the AWARD phase 3 clinical trial program. Diabetes Metab. Res. Rev. 32, 776–790 (2016).
Sorli, C. et al. Efficacy and safety of once-weekly semaglutide monotherapy versus placebo in patients with type 2 diabetes (SUSTAIN 1): a double-blind, randomised, placebo-controlled, parallel-group, multinational, multicentre phase 3a trial. Lancet Diabetes Endocrinol. 5, 251–260 (2017).
Rosenstock, J. et al. Efficacy and safety of a novel dual GIP and GLP-1 receptor agonist tirzepatide in patients with type 2 diabetes (SURPASS-1): a double-blind, randomised, phase 3 trial. Lancet 398, 212 (2021).
Chinese Diabetes Society. Guideline for the prevention and treatment of diabetes mellitus in China (2024 edition). Chin. J. Diabetes https://doi.org/10.3760/cma.j.cn115791-20241203-00705 (2025).
American Diabetes Association Professional Practice Committee. Classification and diagnosis of diabetes: Standards of Medical Care in Diabetes—2022. Diabetes Care 45, S17–S38 (2022).
Scheen, A. J. & Lefèbvre, P. J. Glucagon, from past to present: a century of intensive research and controversies. Lancet Diabetes Endocrinol. 11, 129–138 (2023).
Zhang, B. et al. Efficacy and safety of mazdutide in Chinese patients with type 2 diabetes: a randomised, double-blind, placebo-controlled phase 2 trial. Diabetes Care 47, 160–168 (2024).
le Roux, C. W. et al. Glucagon and GLP-1 receptor dual agonist survodutide for obesity: a randomised, double-blind, placebo-controlled, dose-finding phase 2 trial. Lancet Diabetes Endocrinol. 12, 162–173 (2024).
Rosenstock, J. et al. Retatrutide, a GIP, GLP-1 and glucagon receptor agonist, for people with type 2 diabetes: a randomised, double-blind, placebo and active-controlled, parallel-group, phase 2 trial conducted in the USA. Lancet 402, 529–544 (2023).
Expert Group for Expert Consensus on weight management for type 2 diabetes mellitus. Experts consensus on weight management for type 2 diabetes mellitus (2024 edition). Int. J. Endocrinol. Metab. https://doi.org/10.3760/cma.j.cn121383-20240514-00022 (2024).
Li, J. et al. Once-weekly mazdutide in Chinese adults with obesity or overweight. N. Engl. J. Med. 392, 2215–2225 (2025).
Perry, R. J. et al. Hepatic acetyl CoA links adipose tissue inflammation to hepatic insulin resistance and type 2 diabetes. Cell 160, 745–758 (2015).
American Diabetes Association Professional Practice Committee. Glycemic targets: Standards of Medical Care in Diabetes—2022. Diabetes Care 45, S83–S96 (2022).
ICH. ICH Harmonised Guideline: Addendum on estimands and sensitivity analysis in clinical trials. ICH E9(R1) (ICH, 2019).
Acknowledgements
We thank all the participants, their families and all investigators and study site staff who are involved in this study. The study was supported by Innovent Biologics, Suzhou, China.
Author information
Authors and Affiliations
Consortia
Contributions
All authors had full access to all the data in the study and had critically reviewed the manuscript and approved the final manuscript. All authors vouch for data accuracy and fidelity to the protocol. D.Z. and J.Z. are the co-first authors. D.Z., J.Z., F.X., H.D. and L.Q. developed the study concept and design. D.Z., J.Z., H. Cai, X.C., S.X., C.S., Z.C., H. Cao, H.J., L.Z., H.W., B.S., Yanbing Li, M.L. and B.F. acquired the data. D.Z., J.Z., Yue Li and Q.M. drafted the manuscript. H.L. and L.L. performed statistical analysis. F.X., H.D. and L.Q. provided administrative, technical or material support. All authors contributed to the analysis or interpretation of data and critical revisions of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
D.Z., H. Cai and H.J. serve as consultants to Innovent Biologics. F.X., H.D., H.L., L.L., Yue Li, Q.M. and L.Q. are employees of Innovent Biologics. The other authors declare no competing interests.
Peer review
Peer review information
Nature thanks Richard Pratley and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 Subgroup analyses of glycemic and body weight outcomes under the efficacy estimand.
Symbols are LS mean treatment difference and error bars are 95% CI, mITT population. BMI=body mass index. HbA1c=glycated haemoglobin. LS=least squares. mITT=modified intent-to-treat. No.=number. pts=participants. yrs=years. CI=confidence interval.
Extended Data Fig. 2 Changes in FPG and seven-point SMBG.
a. Change from baseline in FPG over time under the efficacy estimand. Symbols and error bars are LS means and 95% CI, and numbers are LS mean changes at scheduled visits, from an MMRM analysis, mITT population. At week 24, n = 89 in the mazdutide 4 mg group, n = 86 in the mazdutide 6 mg group, and n = 82 in the placebo group had FPG measures. b. Seven-point SMBG profiles at baseline and week 24. Data are observed means and standard errors from descriptive analyses of the mITT population. At week 24, n = 92 with mazdutide 4 mg, n = 91 with mazdutide 6 mg, and n = 98 with placebo had pre-breakfast SMBG measures; n = 91 with mazdutide 4 mg, n = 89 with mazdutide 6 mg, and n = 98 with placebo had 2 h post breakfast SMBG measures; n = 92 with mazdutide 4 mg, n = 91 with mazdutide 6 mg, and n = 97 with placebo had pre-lunch SMBG measures; n = 91 with mazdutide 4 mg, n = 89 with mazdutide 6 mg, and n = 94 with placebo had 2 h post lunch SMBG measures; n = 92 with mazdutide 4 mg, n = 90 with mazdutide 6 mg, and n = 97 with placebo had pre-dinner SMBG measures; n = 89 with mazdutide 4 mg, n = 88 with mazdutide 6 mg, and n = 95 with placebo had 2 h post dinner SMBG measures; n = 90 with mazdutide 4 mg, n = 86 with mazdutide 6 mg, and n = 95 with placebo had bedtime SMBG measures. FPG=fasting plasma glucose. LS=least squares. mITT= modified intent-to-treat. MMRM=mixed model repeated measures. SMBG=self-measured blood glucose. CI=confidence interval. ***Nominal p < 0.0001 versus placebo. All p values were two-sided.
Extended Data Fig. 3 Changes in SMBG at week 24 under the treatment-policy estimand.
Bars are LS means and error bars are 95% CI, from an ANCOVA analysis, mITT population. At week 24, n = 92 in the mazdutide 4 mg group, n = 91 in the mazdutide 6 mg group, and n = 97 in the placebo group had daily mean SMBG, pre-meal SMBG, 2 h post-meal SMBG, and glucose excursions measures. LS=least squares. mITT=modified intent-to-treat. ANCOVA=analysis of covariance. SMBG=self-measured blood glucose. CI=confidence interval. H=hour. **Nominal p < 0.01, ***nominal p < 0.0001 versus placebo. All p values were two-sided.
Extended Data Fig. 4 Changes in blood pressure and pulse rate over time.
a. Change from baseline in SBP over time under the efficacy estimand. b. Change from baseline in DBP over time under the efficacy estimand. For a and b, symbols and error bars are LS means and 95% CI, and numbers are LS mean changes at week 24, from an MMRM analysis, mITT population. At week 24, n = 89 in the mazdutide 4 mg group, n = 86 in the mazdutide 6 mg group, and n = 82 in the placebo group had blood pressure measures. c. Change from baseline in pulse rate over time. Data are observed means and standard errors from descriptive analyses of the mITT population. n = 93 in the mazdutide 4 mg group, n = 96 in the mazdutide 6 mg group, and n = 103 in the placebo group had pulse rate measures. DBP=diastolic blood pressure. LS=least squares. mITT=modified intent-to-treat. MMRM=mixed model repeated measures. SBP=systolic blood pressure. CI=confidence interval. min=minute. *Nominal p < 0.05, **nominal p < 0.01 versus placebo. All p values were two-sided.
Extended Data Fig. 5 Prevalence of nausea (a), vomiting (b), and diarrhea (c) over time (safety population).
a. The proportion of participants with nausea throughout the study. b. The proportion of participants with vomiting throughout the study. c. The proportion of participants with diarrhea throughout the study.
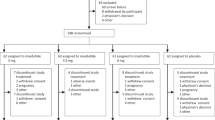
Extended Data Fig. 6 Study design.
This study included a 4-week screening period, a 6-week lead-in period, a 24-week treatment period, a 24-week extended treatment, and a 4-week off-treatment follow-up period.
Supplementary information
Supplementary Information (download PDF )
The Supplementary Information file contains: inclusion and exclusion criteria of the DREAMS-1 trial; list of investigators in the DREAMS-1 trial; list of ethics committees approving the DREAMS-1 Trial; Supplementary Tables 1–6 and the statistical analysis plan.
Supplementary Information (download PDF )
Clinical Protocol.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhu, D., Zhao, J., Cai, H. et al. Mazdutide versus placebo in Chinese adults with type 2 diabetes. Nature 652, 174–180 (2026). https://doi.org/10.1038/s41586-025-10026-w
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41586-025-10026-w