Abstract
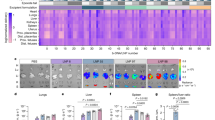
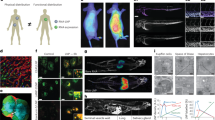
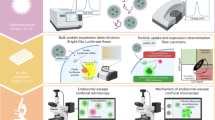
Lipid nanoparticles (LNPs) have garnered tremendous enthusiasm in preclinical and clinical settings for the delivery of nucleic acids such as mRNA. With applications in protein replacement therapies, vaccines and gene editing, mRNA LNPs have only recently been explored in the context of pregnancy disorders. There is a significant need for the design of novel therapeutic technologies such as mRNA LNPs to treat obstetric disorders like pre-eclampsia that are associated with placental pathology and detrimental effects on maternal and fetal health. Here, we present a step-by-step procedure for the preparation and evaluation of placenta-tropic mRNA LNPs for researchers from varied disciplines to explore their application in treating pregnancy disorders. In this Protocol, we describe steps for synthesizing and purifying the key ionizable lipid excipient of the placenta-tropic LNP formulation (4 d) before preparing mRNA LNPs using microfluidic mixing (1 d). Then, we detail in vitro mechanistic evaluations of the effect of protein adsorption on LNP-mediated mRNA transfection to placental trophoblasts (3 d). Finally, we outline methods for isolating reproductive tissues from time-dated pregnant mice to assess in vivo LNP biodistribution and mRNA transfection to the murine placenta (16 d). Compared to alternative LNP formulation procedures, this Protocol focuses on delivering mRNA LNPs to the placenta with a workflow that can be applied for a range of obstetric disorders. This Protocol seeks to increase interdisciplinary work at the interface of nanomedicine, gene modulation and reproductive health.
Key points
-
The procedure covers synthesis and purification of the key ionizable lipid excipient, preparation of mRNA LNPs by microfluidic mixing, assessment of the effect of protein adsorption on LNP transfection to placental trophoblast cells and evaluation of LNP biodistribution and mRNA expression in the placentas of time-dated pregnant mice.
-
The mRNA LNP formulation presented here has demonstrated applications in treating pre-eclampsia in murine models of the condition and has the potential to be expanded for the treatment of other pregnancy disorders.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$32.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The data associated with this Protocol are provided in the article and Supplementary Information. Source data for Figs. 4 and 6 are provided with this paper. Source data are provided with this paper.
References
Vargason, A. M., Anselmo, A. C. & Mitragotri, S. The evolution of commercial drug delivery technologies. Nat. Biomed. Eng. 5, 951–967 (2021).
Swingle, K. L., Hamilton, A. G. & Mitchell, M. J. Lipid nanoparticle-mediated delivery of mRNA therapeutics and vaccines. Trends Mol. Med. 27, 616–617 (2021).
Baden Lindsey, R. et al. Efficacy and safety of the mRNA-1273 SARS-CoV-2 vaccine. N. Engl. J. Med. 384, 403–416 (2021).
Polack Fernando, P. et al. Safety and efficacy of the BNT162b2 mRNA Covid-19 vaccine. N. Engl. J. Med. 383, 2603–2615 (2020).
Fontana, M. et al. CRISPR-Cas9 gene editing with nexiguran ziclumeran for ATTR cardiomyopathy. N. Engl. J. Med. 391, 2231–2241 (2024).
Cullis, P. R. & Felgner, P. L. The 60-year evolution of lipid nanoparticles for nucleic acid delivery. Nat. Rev. Drug Discov. 23, 709–722 (2024).
Love, K. T. et al. Lipid-like materials for low-dose, in vivo gene silencing. Proc. Natl Acad. Sci. USA 107, 1864–1869 (2010).
Hajj, K. A. et al. A potent branched-tail lipid nanoparticle enables multiplexed mRNA delivery and gene editing in vivo. Nano Lett. 20, 5167–5175 (2020).
Wang, X. et al. Preparation of selective organ-targeting (SORT) lipid nanoparticles (LNPs) using multiple technical methods for tissue-specific mRNA delivery. Nat. Protoc. 18, 265–291 (2023).
Omo-Lamai, S. et al. Physicochemical targeting of lipid nanoparticles to the lungs induces clotting: mechanisms and solutions. Adv. Mater. 36, e2312026 (2024).
Xue, L. et al. Rational design of bisphosphonate lipid-like materials for mRNA delivery to the bone microenvironment. J. Am. Chem. Soc. 144, 9926–9937 (2022).
Melamed, J. R. et al. Ionizable lipid nanoparticles deliver mRNA to pancreatic β cells via macrophage-mediated gene transfer. Sci. Adv. 9, eade1444 (2023).
Billingsley, M. M. et al. In vivo mRNA CAR T cell engineering via targeted ionizable lipid nanoparticles with extrahepatic tropism. Small 20, e2304378 (2024).
Rurik, J. G. et al. CAR T cells produced in vivo to treat cardiac injury. Science 375, 91–96 (2022).
Ni, H. et al. Piperazine-derived lipid nanoparticles deliver mRNA to immune cells in vivo. Nat. Commun. 13, 4766 (2022).
Palanki, R. et al. In utero delivery of targeted ionizable lipid nanoparticles facilitates in vivo gene editing of hematopoietic stem cells. Proc. Natl Acad. Sci. USA 121, e2400783121 (2024).
Breda, L. et al. In vivo hematopoietic stem cell modification by mRNA delivery. Science 381, 436–443 (2023).
Funding research on women’s health. Nat. Rev. Bioeng. 2, 797–798 (2024).
Moley, K. Closing the gender health gap is a $1 trillion opportunity. Biopharm. Deal. https://doi.org/10.1038/d43747-024-00021-x (2024).
It’s about time to focus on women’s health. Nat. Rev. Bioeng. 1, 379 (2023).
Bilinski, A. & Emanuel, N. Fewer than 1% of United States clinical drug trials enroll pregnant participants. Am. J. Obstet. Gynecol. 232, e136–e139 (2025).
Prasad, S. et al. Systematic review and meta-analysis of the effectiveness and perinatal outcomes of COVID-19 vaccination in pregnancy. Nat. Commun. 13, 2414 (2022).
Shimabukuro, T. T. et al. Preliminary findings of mRNA Covid-19 vaccine safety in pregnant persons. N. Engl. J. Med. 384, 2273–2282 (2021).
Dagan, N. et al. Effectiveness of the BNT162b2 mRNA COVID-19 vaccine in pregnancy. Nat. Med. 27, 1693–1695 (2021).
Klein, S. L., Creisher, P. S. & Burd, I. COVID-19 vaccine testing in pregnant females is necessary. J. Clin. Invest. 131, e147553 (2021).
Swingle, K. L. et al. Ionizable lipid nanoparticles for in vivo mRNA delivery to the placenta during pregnancy. J. Am. Chem. Soc. 145, 4691–4706 (2023).
Safford, H. C. et al. Orthogonal design of experiments for engineering of lipid nanoparticles for mRNA delivery to the placenta. Small 20, 2303568 (2023).
Geisler, H. C. et al. EGFR-targeted ionizable lipid nanoparticles enhance in vivo mRNA delivery to the placenta. J. Control. Release 371, 455–469 (2024).
Swingle, K. L. et al. Placenta-tropic VEGF mRNA lipid nanoparticles ameliorate murine pre-eclampsia. Nature 637, 412–421 (2025).
Safford, H. C. et al. Probing the role of lipid nanoparticle elasticity on mRNA delivery to the placenta. Nano Lett. 25, 4800–4808 (2025).
Young, R. E. et al. Systematic development of ionizable lipid nanoparticles for placental mRNA delivery using a design of experiments approach. Bioact. Mater. 34, 125–137 (2024).
Chaudhary, N. et al. Lipid nanoparticle structure and delivery route during pregnancy dictate mRNA potency, immunogenicity, and maternal and fetal outcomes. Proc. Natl Acad. Sci. USA 121, e2307810121 (2024).
Hofbauer, S. I. et al. Cytokine mRNA delivery and local immunomodulation in the placenta using lipid nanoparticles. Adv. Ther. 8, e00148 (2025).
Jayaraman, M. et al. Maximizing the potency of siRNA lipid nanoparticles for hepatic gene silencing in vivo. Angew. Chem. Int. Ed. Engl. 51, 8529–8533 (2012).
Francia, V., Schiffelers, R. M., Cullis, P. R. & Witzigmann, D. The biomolecular corona of lipid nanoparticles for gene therapy. Bioconjug. Chem. 31, 2046–2059 (2020).
Dilliard, S. A., Cheng, Q. & Siegwart, D. J. On the mechanism of tissue-specific mRNA delivery by selective organ targeting nanoparticles. Proc. Natl Acad. Sci. USA 118, e2109256118 (2021).
Bashiri, G. et al. Nanoparticle protein corona: from structure and function to therapeutic targeting. Lab Chip 23, 1432–1466 (2023).
Chappell, L. C., Cluver, C. A., Kingdom, J. & Tong, S. Pre-eclampsia. Lancet 398, 341–354 (2021).
Turanov, A. A. et al. RNAi modulation of placental sFLT1 for the treatment of preeclampsia. Nat. Biotechnol. 36, 1164–1173 (2018).
Zhang, R. et al. Helper lipid structure influences protein adsorption and delivery of lipid nanoparticles to spleen and liver. Biomater. Sci. 9, 1449–1463 (2021).
Voke, E. et al. Protein corona formed on lipid nanoparticles compromises delivery efficiency of mRNA cargo. Nat. Commun. 16, 8699 (2025).
King, A. et al. Tumor-homing peptides as tools for targeted delivery of payloads to the placenta. Sci. Adv. 2, e1600349 (2016).
Zhang, B. et al. Placenta-specific drug delivery by trophoblast-targeted nanoparticles in mice. Theranostics 8, 2765–2781 (2018).
Li, L. et al. Trophoblast-targeted nanomedicine modulates placental sFLT1 for preeclampsia treatment. Front. Bioeng. Biotechnol. 8, 64 (2020).
Cureton, N. et al. Selective targeting of a novel vasodilator to the uterine vasculature to treat impaired uteroplacental perfusion in pregnancy. Theranostics 7, 3715–3731 (2017).
Alfaifi, A. A. et al. Megalin-targeting liposomes for placental drug delivery. J. Control. Release 324, 366–378 (2020).
Renshall, L. J. et al. Targeted delivery of epidermal growth factor to the human placenta to treat fetal growth restriction. Pharmaceutics 13, 1778 (2021).
Wilson, R. L. et al. Nanoparticle mediated increased insulin-like growth factor 1 expression enhances human placenta syncytium function. Placenta 93, 1–7 (2020).
Li, L. et al. Nanoparticle-mediated simultaneous downregulation of placental Nrf2 and sFlt1 improves maternal and fetal outcomes in a preeclampsia mouse model. ACS Biomater. Sci. Eng. 6, 5866–5873 (2020).
Irvin-Choy, N. S., Nelson, K. M., Dang, M. N., Gleghorn, J. P. & Day, E. S. Gold nanoparticle biodistribution in pregnant mice following intravenous administration varies with gestational age. Nanomedicine 36, 102412 (2021).
Ma, Y., VanKeulen-Miller, R. & Fenton, O. S. mRNA lipid nanoparticle formulation, characterization and evaluation. Nat. Protoc. 20, 2618–2651 (2025).
Swingle, K. L., Ricciardi, A. S., Peranteau, W. H. & Mitchell, M. J. Delivery technologies for women’s health applications. Nat. Rev. Bioeng. 1, 408–425 (2023).
Furukawa, S., Kuroda, Y. & Sugiyama, A. A comparison of the histological structure of the placenta in experimental animals. J. Toxicol. Pathol. 27, 11–18 (2014).
Han, X. et al. An ionizable lipid toolbox for RNA delivery. Nat. Commun. 12, 7233 (2021).
Li, B. et al. Accelerating ionizable lipid discovery for mRNA delivery using machine learning and combinatorial chemistry. Nat. Mater. 23, 1002–1008 (2024).
Billingsley, M. M. et al. Ionizable lipid nanoparticle-mediated mRNA delivery for human CAR T cell engineering. Nano Lett. 20, 1578–1589 (2020).
Han, X. et al. Plug-and-play assembly of biodegradable ionizable lipids for potent mRNA delivery and gene editing in vivo. Preprint at bioRxiv https://doi.org/10.1101/2025.02.25.640222 (2025).
Li, B. et al. Combinatorial design of nanoparticles for pulmonary mRNA delivery and genome editing. Nat. Biotechnol. 41, 1410–1415 (2023).
Padilla, M. S. et al. Branched endosomal disruptor (BEND) lipids mediate delivery of mRNA and CRISPR-Cas9 ribonucleoprotein complex for hepatic gene editing and T cell engineering. Nat. Commun. 16, 996 (2025).
Kauffman, K. J. et al. Optimization of lipid nanoparticle formulations for mRNA delivery in vivo with fractional factorial and definitive screening designs. Nano Lett. 15, 7300–7306 (2015).
Akinc, A. et al. Targeted delivery of RNAi therapeutics with endogenous and exogenous ligand-based mechanisms. Mol. Ther. 18, 1357–1364 (2010).
McDonnell, T. et al. The role of beta-2-glycoprotein I in health and disease associating structure with function: more than just APS. Blood Rev. 39, 100610 (2020).
Di, S. et al. Pathogenic role of anti-ß2-glycoprotein I antibodies in antiphospholipid associated fetal loss: characterisation of ß2-glycoprotein I binding to trophoblast cells and functional effects of anti-ß2-glycoprotein I antibodies in vitro. Ann. Rheum. Dis. 64, 462–467 (2005).
Zhang, Y. et al. TMEM16F phospholipid scramblase mediates trophoblast fusion and placental development. Sci. Adv. 6, eaba0310 (2020).
Riddell, M. R., Winkler-Lowen, B., Jiang, Y., Davidge, S. T. & Guilbert, L. J. Pleiotropic actions of forskolin result in phosphatidylserine exposure in primary trophoblasts. PLoS One 8, e81273 (2013).
Chamley, L. W., Allen, J. L. & Johnson, P. M. Synthesis of β2 glycoprotein 1 by the human placenta. Placenta 18, 403–410 (1997).
Pennington, K. A., Schlitt, J. M. & Schulz, L. C. Isolation of primary mouse trophoblast cells and trophoblast invasion assay. J. Vis. Exp. 2012, e3202 (2012).
Swingle, K. L., Hamilton, A. G. & Mitchell, M. J. Flow cytometric analysis of the murine placenta to evaluate nanoparticle platforms during pregnancy. Placenta 166, 132–138 (2024).
Wice, B., Menton, D., Geuze, H. & Schwartz, A. L. Modulators of cyclic AMP metabolism induce syncytiotrophoblast formation in vitro. Exp. Cell Res. 186, 306–316 (1990).
Shepherd, S. J. et al. Scalable mRNA and siRNA lipid nanoparticle production using a parallelized microfluidic device. Nano Lett. 21, 5671–5680 (2021).
Chen, D. et al. Rapid discovery of potent siRNA-containing lipid nanoparticles enabled by controlled microfluidic formulation. J. Am. Chem. Soc. 134, 6948–6951 (2012).
Geisler, H. C., Safford, H. C. & Mitchell, M. J. Rational design of nanomedicine for placental disorders: birthing a new era in women’s reproductive health. Small 20, 2300852 (2023).
Author information
Authors and Affiliations
Contributions
K.L.S. designed and conducted experiments, analyzed the data, wrote the original draft of the manuscript, and contributed to reviewing and editing the manuscript. M.J.M. supervised the experiments and overall study, was responsible for funding acquisition for the experiments, and contributed to reviewing and editing the manuscript.
Corresponding author
Ethics declarations
Competing interests
K.L.S. and M.J.M. have filed a patent application based on this work. M.J.M. is an inventor on a patent related to this work filed by the Trustees of the University of Pennsylvania.
Peer review
Peer review information
Nature Protocols thanks Yusuke Sato and the other, anonymous reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key references
Swingle, K. L. et al. Nature 637, 412–421 (2025): https://doi.org/10.1038/s41586-024-08291-2
Swingle, K. L. et al. J. Am. Chem. Soc. 145, 4691–4706 (2023): https://doi.org/10.1021/jacs.2c12893
Geisler, H. C. et al. J. Control. Release 371, 455–469 (2024): https://doi.org/10.1016/j.jconrel.2024.05.036
Supplementary information
Supplementary Information (download PDF )
Supplementary Figures 1–7 and Supplementary Table 1
Supplementary Data 1 (download XLSX )
Supplementary Data 1
Source data
Source Data Fig. 4 and Fig. 6 (download XLSX )
Statistical Source Data
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Swingle, K.L., Mitchell, M.J. Preparation of placenta-tropic mRNA lipid nanoparticles for pregnancy disorders. Nat Protoc (2026). https://doi.org/10.1038/s41596-025-01325-7
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41596-025-01325-7