Abstract
This study aims to present age-stratified prevalence of women with lower urinary tract symptoms (LUTS) but without cystocele and predict detrusor underactivity (DU) or bladder outlet obstruction (BOO). Between 2005 and 2020, we reviewed women who visited the medical center with LUTS but without cystocele. Positive voiding dysfunction (VD) symptoms were defined as any one or more of the positive descriptions of weak urinary stream, intermittency, strain to urination, and sensation of not emptying. A total of 1,886 women were included in this study. 189 (10.0%) women were diagnosed with DU, and 77 (4.1%) women had BOO. Multivariate logistic regression analysis found that voided volume and VD symptoms were independent predictors for BOO. ROC curve analyses could predict BOO by voided volume ≤ 220 mL derived from uroflowmetry and the presence of VD symptoms with an area under a curve of 0.83. Age and voided volume could predict DU with an area under a curve of 0.82. We found a higher percentage of BOO in women with positive VD symptoms. A non-invasive uroflowmetry with voided volume (≤ 220 mL) and the presence of VD symptoms can predict BOO. DU could be predicted by age and voided volume.
Similar content being viewed by others
Introduction
Female voiding dysfunction (VD) needs a clear and objective definition. The prevalence varies widely from 2.7 to 23% according to various criteria1. Both clinical storage and voiding symptoms correlate with VD, including urgency, frequency, weak stream, and straining. The International Continence Society (ICS) defined VD as “abnormally slow and/or incomplete micturition, based on abnormally slow urine flow rates and/or abnormally high post-void residuals, ideally on repeated measurement to confirm abnormality. Pressure-flow studies can be required to determine the cause of the voiding dysfunction.”2 Nowadays, urodynamic study (UDS) is the gold standard for clarifying female VD and categorized functional detrusor underactivity (DU), and bladder outlet obstruction (BOO)3.
DU has represented a low-pressure-low-flow pattern in UDS with poor voiding efficacy and substantial post-void residual urine. BOO can be anatomical or functional and is characterized by a high-pressure-low-flow pattern in pressure-flow studies4,5. Because of the high complexity of urinary symptoms to correlate with symptoms, Dr. Bates et al. wrote that the bladder is an unreliable witness6. Thus, most women presenting lower urinary tract symptoms (LUTS) require an invasive pressure-flow study, part of the UDS, to differentiate DU or BOO. A non-invasive prediction model including symptoms of DU and BOO is still lacking.
Our study aimed to calculate the age-stratified prevalence of DU and BOO in women with LUTS. We divided the LUTS into the presence or absence of clinical VD symptoms. We utilized four symptoms including weak urinary stream, intermittency, strain to urination, and sensation of not emptying. Patients fulfilled one of the four symptoms were defined positive clinical VD symptom. We aimed to calculate an office-based prediction model to facilitate clinicians’ identification of these patients.
Results
The mean age of the total enrolled 1,886 women was 57.7 years old. For those diagnosed with DU or BOO women, the mean age was 66.2 and 59.5 years old, respectively. The total prevalence of women who presented with LUTS was 10% (189/1886) for DU and 4.1% (77/1886) for BOO. The age-adjusted prevalence rates of DU and BOO are shown in Fig. 1a. The DU patients showed an increasing trend with age, while the BOO patients kept a similar proportion throughout all age stratifications. The proportion did not increase with age in DU patients with clinical VD symptoms. In comparison, DU patients without clinical VD symptoms did increase their prevalence with age (Fig. 1b, p = 0.031). In the BOO groups, women with and without symptoms of VD did not show such trend of DU (Fig. 1c, p = 0.156).
The prevalence of detrusor underactivity (DU) and bladder outlet obstruction (BOO) is divided by age per 10 years. a The age-stratified prevalence of DU and BOO diagnosis in all 1,886 women. b The age-stratified DU population in clinical positive voiding dysfunction (VD) and negative VD symptoms. c The age-stratified BOO population in clinical positive voiding dysfunction (VD) and negative VD symptoms.
In women with VD symptoms, 12.8% (36/282) were diagnosed with DU, and 11.3% (32/282) had BOO, according to the criteria7. In those without VD symptoms, 9.5% (153/1604) had DU, and 2.8% (45/1604) had BOO. A significant difference can be found in the diagnosis of BOO (p < 0.001). Women with clinical symptoms of VD had a higher chance of being diagnosed with BOO than those without symptoms (Table 1). On the contrary, DU is relatively hard to determine from the clinical VD symptoms only.
To elucidate the factors predicting BOO, we performed univariate and multivariate analyses (Table 2). Primary demographic data and urodynamic study parameters were included. In the univariate analysis, the volume of strong desire (p = 0.001), maximal urethral closure pressure (MUCP) (p = 0.004), voided volume (p < 0.001), post-void residual urine (PVR) (p < 0.001), and symptoms of VD (p < 0.001) were significantly predicting factors associated with BOO, while the age, parity, pad test weight, functional urethral length, pressure-transmission ratio were not. Further multivariate analysis by stepwise backward logistic analysis identified that MUCP, voided volume, and symptoms of VD were the independent factors predicting BOO. The odds ratio is 3.64 for symptoms of VD, 0.0031 per mL for voided volume, and 1.009 for MUCP, respectively.
A receiver operating characteristic (ROC) curve analysis was used to calculate the optimal predictor’s cut-off combination. Using the single predictor voided volume ≤ 220 mL derived from uroflowmetry, we can obtain a ROC area of 0.80 (Fig. 2a). Combined the predicted logit transformation of the probability of BOO, logit(p), for a voided volume (mL, a) and the presence of symptoms of VD (0 or 1, b) can be denoted by logit(p) = -1.3–1.1 x a + 0.014 x b, with a cut-off value of logit(p) ≥ -2.9 and a ROC area of 0.83 (Fig. 2b) (sensitivity = 75%, specificity = 77%).
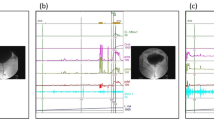
Clinical predictors of bladder outlet obstruction (BOO) and detrusor underactivity (DU) were calculated by receiver operating characteristic (ROC) curve analysis. a The ROC curve analysis using the single predictor voided volume ≤ 220 mL derived from uroflowmetry to predict bladder outlet obstruction. b Prediction of BOO by logit(p). Combined the predicted logit transformation of the probability of BOO, logit(p), for a voided volume (mL, a) and the presence of symptoms of VD (0 or 1, b) can be denoted by logit(p) = -1.3–1.1 x a + 0.014 x b, with a cut-off value of logit(p) ≥ -2.9. The area under the ROC curve is 0.83(95% CI = 0.79 to 0.88, sensitivity = 75%, specificity = 77%). c The ROC curve analysis using the single predictor age ≥ 60 years old to predict detrusor underactivity (95% CI 0.67 to 0.74, sensitivity = 71%, specificity = 58%). d The ROC curve analysis using the single predictor maximum urethral closure pressure ≤ 50 cmH2O to predict detrusor underactivity. (95% CI 0.60 to 0.69, sensitivity = 68%, specificity = 57%). e The ROC curve analysis using the single predictor functional profile length ≤ 2.5 cmH2O to predict detrusor underactivity (95% CI 0.57 to 0.66, sensitivity = 68%, specificity = 51%). f The ROC curve analysis using the single predictor voided volume ≤ 200 mL to predict detrusor underactivity (95% CI 0.76 to 0.82, sensitivity = 69%, specificity = 74%). g The ROC curve analysis using the single predictor post-void residual ≥ 30 mL to predict detrusor underactivity (95% CI 0.59 to 0.66, sensitivity = 83%, specificity = 38%). h Prediction of DU by logit(p). The predicted logit transformation of the probability of DU, logit(p), for age (year-old, a) and voided volume (mL, b) can be denoted by logit(p) = -2.8 + 0.04 x a − 0.01 x b, with a cutoff value of logit(p) ≥ -2.3 and a ROC area of 0.82 ((95% CI 0.79 to 0.84, sensitivity = 76%, specificity = 73%).
For the factors affecting DU, multivariate logistic regression analysis found that age, MUCP, FPL, voided volume, and PVR were independent predictors for DU (Table 3). Nevertheless, the clinical symptoms of VD were not. A ROC curve analysis showed the following optimum cut-off value: (1) age ≥ 60 years old, which had a ROC area of 0.70 (Fig. 2c). (2) MUCP ≤ 50 cmH2O, which had a ROC area of 0.64 (Fig. 2d). (3) FPL ≤ 2.5 cmH2O, which had a ROC area of 0.61 (Fig. 2e). (4) Voided volume ≤ 200 mL, which had a ROC area of 0.79 (Fig. 2f). (5) PVR ≥ 30 mL, which had a ROC area of 0.63 (Fig. 2 g). To build a usable clinical model, the logit transformation of the probability of DU, logit(p), for age (year-old, a) and voided volume (mL, b) can be denoted by logit(p) = -2.8 + 0.04 x a − 0.01 x b, with a cutoff value of logit(p) ≥ -2.3 and a ROC area of 0.82 (Fig. 2h). Thus, although a urodynamic study may still be warranted to make a definite diagnosis, women who fulfill these criteria can be screened in an outpatient department.
Discussion
Our study is one of the larger cohorts presenting the uniquely age-stratified prevalence of LUTS women who underwent UDS to evaluate DU and BOO. The total prevalence was 10.0% (189/1,886) of DU regardless of their clinical VD symptoms, and the total prevalence was 4.1% (77/1,886) of BOO in LUTS women. In addition, we developed a model calculated by voided volume and clinical VD symptoms to predict female BOO and DU. In this study, positive clinical VD symptoms were defined as any one or more of the positive descriptions of weak urinary stream, intermittency, strain to urination, and sensation of not emptying. Compared with the ICS definition: “abnormally slow and/or incomplete micturition”8, our positive clinical VD symptoms are slightly broader and clearer. The simple calculation can be implemented in clinical practice and aids doctors in diagnosing and prescribing first-line medication in the office setting.
The DU group showed an increasing trend along with age, while the BOO group kept a similar proportion throughout all age stratifications. Our cohort’s prevalence was 4.1% (77/1,886) of BOO in LUTS women. Farrar et al. reported a 6.7% prevalence of diagnosed BOO based on a sole peak flow rate of < 15 mL/s9. Blaivas and Groutz created a nomogram to diagnose BOO and classified its severity based on pressure-flow criteria of a free Qmax ≤ 12 mL/s and a Pdet. Qmax ≥ 20 cmH2O was associated with radiographic evidence of obstruction and reported a prevalence of 8.3%10. Gammie et al. reported a 9.2% BOO prevalence rate in the cross-section study. They used the same urodynamic criteria and excluded clinical obstruction for the DU and Normal groups women7. In our study, after excluding cystocele, we chose relatively strict criteria to avoid overlap but simple for ease of implementation.
Although there are different criteria to define DU, Jeong et al. compared several DU criteria, and the prevalence of the criteria we chose was 6.4%7,11,12. The result is consistent with another study as well. D’Alessandro et al. reported a prevalence between 3.7%~37% in 2,092 LUTS women attending the urogynecology clinic13. Few studies in the literature reported a detailed age stratification today. We showed that the age-stratified prevalence rate of DU increased from 4.2% at age 41–50 to 12.6% at age 61–70 and 47.5% at age over 70. In Osman’s review, the DU prevalence associated with age ranges from 9% (18–45 years old) to 48% (> 70 years old)14,15.
Our study found that the clinical VD symptoms can predict the diagnosis of BOO. Previous literature showed that storage symptoms like urinary frequency are the most frequent in BOO patients16. Indeed, 88% of BOO and 87% of DU patients in our cohort had storage symptoms such as frequency, urgency, or nocturia (data not shown). The high prevalence of bladder storage symptoms obscures its utilization to differentiate DU from BOO. The clinical VD symptoms in our cohort are more appropriate to predict BOO (p < 0.0001) instead of DU (p = 0.097). Using solely clinical VD symptoms as predictors of BOO has an odds ratio of 3.64 in this study (Table 1). Combined with a low voided volume (≤ 220 mL) by non-invasive uroflowmetry, the prediction of BOO can achieve a 0.83 ROC area.
The clinical VD symptoms cannot predict DU in our study. Our clinical DU prediction model used the age and voided volume by uroflowmetry. Uroflowmetry is a non-invasive measure of voiding pattern and amount. The logit transformation prediction model predicts a 0.82 ROC area. Previous literature used post-void volume (ROC = 0.78) or Qmax (ROC = 0.74) by a pressure-flow study17. The flow rate curve shape was investigated to approach DU and BOO patients. But no patterns can predict female DU, while prolonged and plateau way positively indicates female BOO18. In men with LUTS, a prediction model of DU used older age, smaller prostate volume, two symptoms (less urgency and a weak stream), and a lower maximum flow rate19. Compared with those prediction models, our prediction model is more straightforward, more accessible, and has a similar predictive ability.
Our study showed that MUCP is slightly higher in BOO and lower in DU. These results indicate a potential diagnostic ability to differentiate these two disease entities. The diagnostic value of MUCP had been shown in some types of BOO like high tone non-relaxing urethral sphincter3,20. The DU, on the contrary, was caused by the low detrusor contractility and had never been shown to correlate with the MUCP. Whether it is a physiologic change to the low contractility or secondary to aging is not known now. The role of MUCP in DU requires further research. In our study, we do not intend to incorporate the urethral pressure profilometry into our model because it is invasive and difficult to evaluate in the office-based situation.
The study’s strength is that this is a large cohort with 1,886 women. A sophisticated doctor uses easy-to-remember acronyms to ask about the clinical VD symptoms21, which ensures high inquiry consistency in this study. The limitation of our study is that only women with LUTS visited the hospital. We are unaware of the DU or BOO prevalence in asymptomatic healthy subjects. Second, the DU diagnosis criteria we selected might not be suitable to compare with other studies selecting different criteria. Third, the single voided volume of uroflowmetry may have relatively lower reproducibility. Repeated uroflowmetry or voiding diary is suggested to improve the limit.
Recalling the age-stratified prevalence of our study, the clinicians should be alert to the fact that elderly or menopausal women may have DU or BOO without clinical VD symptoms. A non-invasive uroflowmetry with voided volume can help predict the BOO. A higher percentage of BOO was found in women with the symptoms of VD. BOO can be predicted with low voided volume (less than 220 mL) and the presence of symptoms of VD. The DU could be predicted with the age and voided volume. Other suspicions warrant needing a urodynamic study or referral to a urogynecologic specialty.
Methods
Between February 2005 and December 2020, the medical records of all women with LUTS but without cystocele who visited the urogynecology department of a medical center were reviewed. Our UDS inclusion criteria were LUTS symptoms. The exclusion criteria were cystocele, neurogenic bladder, previous anti-incontinence surgery, bladder tumor or stone, previous cervical cancer surgery, dementia, Parkinson’s disease, and psychotic patients. This study received approval from the National Taiwan University Hospital’s research ethics committee (REC No:202105082RINA). All experiments were performed in accordance with relevant guidelines and regulations. Additionally, this study was registered at ClinicalTrials.gov (NCT04981080).
A total of 1,886 women were included in this study. Informed consent for the examinations was obtained from all the women. Their baseline demographic data had age, parity, and history of overactive bladder syndrome (OAB) and stress urinary incontinence (SUI). OAB was defined as urinary urgency, with or without urgency incontinence, usually accompanied by increased urinary frequency and nocturia for at least three months8. All participants completed a 3-day bladder diary for subjective symptom records, such as daytime frequency, nocturia, urgency, and incontinence episodes22. The urodynamic study (UDS) was performed according to the recommendations of the International Continence Society23. The UDS includes non-instrumented uroflowmetry, filling cystometry was performed with 35 °C distilled water at a rate of 60 mL/sec, a pressure-flow study, and stress urethral pressure profilometry, was performed by an experienced technician with the patient in a sitting position according to the recommendations of the International Continence Society. Multichannel water-filled urodynamic equipment (Life-Tech, Houston, TX, USA) with computer analysis and Urovision (Urolab Janus System V, Houston) was used. Those women who have no complete data on the maximum flow rate (Qmax), voided volume, post-void residual volume (PVR), and detrusor pressure at a maximum flow rate (Pdet.Qmax) were excluded from this study.
DU was defined as when the detrusor pressure at the maximum flow rate (Pdet.Qmax) was < 20 cmH2O, the maximum flow rate (Qmax) was < 15 mL/s, and the bladder voiding efficiency (BVE, voided volume/ (voided volume + postvoid residual volume)) was less than 90% 7. BOO was defined when the detrusor pressure at the maximum flow rate (Pdet.Qmax) was ≥ 40 cmH2O and the maximum flow rate (Qmax) was < 12 mL/s7. Women who met the above diagnostic criteria were allocated to the DU or BOO group. Those women without DU or BOO were distributed to the non-DU and non-BOO groups.
The presence of clinical symptoms defines the VD symptoms. Formulated questions were asked in the outpatient department. The formulated questions are in two main categories: OAB and VD. Frequency, urgency, and nocturia (acronym FUN) were asked to evaluate the bladder storage symptoms. Weak urinary stream, intermittency, strain to urination, and sensation of not emptying (acronym WISE) of the bladder symptoms were used to define VD according to the FUN-WISE acronym21. Women with any one or more of the positive descriptions of WISE were recorded as with clinical symptoms of VD.
The primary outcome of this study was the correlation of DU, BOO, non-DU, and non-BOO in women with or without clinical symptoms of voiding dysfunction. Age-specific prevalence in women with and without VD was collected and analyzed. The secondary outcomes were the prediction factors among these four groups in subjective VD symptoms and objective UDS parameters. A prediction model was built.
STATA software (Stata Corp., College Station, TX, USA) was used for statistical analysis. One-way ANOVA was performed using GraphPad Prism version 10.0.0 for MacOS (GraphPad Software, Boston, Massachusetts USA, www.graphpad.com). The chi-square, univariate, and multivariable logistic regression tests were used for statistical analysis as appropriate. A p-value of less than 0.05 was considered statistically significant.
Data availability
The datasets analyzed during this study are available from the corresponding author upon reasonable request.
Abbreviations
- BOO:
-
Bladder outlet obstruction
- DU:
-
Detrusor underactivity
- ICS:
-
International Continence Society
- LUTS:
-
Lower urinary tract symptoms
- MUCP:
-
Maximum urethral closure pressure
- OAB:
-
Overactive bladder syndrome
- Pdet.Qmax:
-
Detrusor pressure at a maximal flow rate
- POP:
-
Pelvic organ prolapse
- POP-Q:
-
Pelvic organ prolapse quantification
- PVR:
-
Post-void residual urine
- Qmax:
-
Maximal flow rate
- ROC curve:
-
Receiver operating characteristic curve
- SUI:
-
Stress urinary incontinence
- UDS:
-
Urodynamic study
- VD:
-
Voiding dysfunction
References
Choi, Y. S. et al. Analysis of female voiding dysfunction: A prospective, multi-center study. Int. Urol. Nephrol. 45, 989–994 (2013).
Doumouchtsis, S. K. et al. An International Continence Society (ICS)/ International Urogynecological Association (IUGA) joint report on the terminology for the assessment and management of obstetric pelvic floor disorders. Int. Urogynecol. J. 34, 1–42 (2023).
Sinha, S., Yang, C. C., Arlandis, S. & Goldman, H. B. Female voiding dysfunction: A review of clinical presentation, urodynamic diagnosis and management. Continence. 6, 100578 (2023).
Panicker, J. N. et al. Do we understand voiding dysfunction in women? Current understanding and future perspectives: ICI-RS 2017. Neurourol. Urodyn. 37, S75–S85 (2018).
Hsiao, S. M., Lin, H. H. & Kuo, H. C. Videourodynamic studies of women with voiding dysfunction. Sci. Rep. 7, 6845 (2017).
Bates, C. P., Whiteside, C. G. & Turner‐Warwick, R. Synchronous cine/pressure/flow/cysto‐urethrography with special reference to stress and urge incontinence. Br. J. Urol. 42, 714–723 (1970).
Gammie, A., Kaper, M., Dorrepaal, C., Kos, T. & Abrams, P. Signs and symptoms of Detrusor Underactivity: An analysis of clinical presentation and urodynamic tests from a large group of patients undergoing pressure Flow studies. Eur. Urol. 69, 361–369 (2016).
Haylen, B. T. et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic organ prolapse (POP). Int. Urogynecol. J. 27, 165–194 (2016).
FARRAR, D. J. et al. A urodynamic view of bladder outflow obstruction in the female: factors influencing the results of treatment. Br. J. Urol. 47, 815–822 (1975).
Blaivas, J. G. & Groutz, A. Bladder outlet obstruction nomogram for women with lower urinary tract symptomatology. Neurourol. Urodyn. 19, 553–564 (2000).
Jeong, S. J. et al. How do we diagnose detrusor underactivity? Comparison of diagnostic criteria based on an urodynamic measure. Investig Clin. Urol. 58, 247–254 (2017).
Osman, N. I., Esperto, F. & Chapple, C. R. Detrusor Underactivity and the underactive bladder: A systematic review of preclinical and clinical studies. Eur. Urol. 74, 633–643 (2018).
D’Alessandro, G. et al. Detrusor underactivity prevalence and risk factors according to different definitions in women attending urogynecology clinic. Int. Urogynecol. J. 33, 835–840 (2022).
Drake, M. J., Williams, J. & Bijos, D. A. Voiding dysfunction due to detrusor underactivity: An overview. Nat. Rev. Urol. 11, 454–464 (2014).
Osman, N. I. et al. Detrusor underactivity and the underactive bladder: A new clinical entity? A review of current terminology, definitions, epidemiology, aetiology, and diagnosis. Eur. Urol. 65, 389–398 (2014).
Malde, S. et al. Female bladder outlet obstruction: Common symptoms masking an uncommon cause. LUTS: Low Urin Tract. Symptoms. 11, 72–77 (2019).
Chow, P. M., Hsiao, S. M. & Kuo, H. C. Identifying occult bladder outlet obstruction in women with detrusor-underactivity-like urodynamic profiles. Sci. Rep. 11, 23242 (2021).
Kocadag, H. et al. A comparison of flow rate curve shape and video-urodynamic findings in women with lower urinary tract symptoms: Can flow rate curve shape predict female bladder outflow obstruction or detrusor underactivity? World J. Urol. 39, 1591–1595 (2021).
Namitome, R. et al. A prediction model of Detrusor Underactivity based on symptoms and noninvasive test parameters in men with lower urinary tract symptoms: An analysis of a large group of patients undergoing pressure-flow studies. J. Urol. 203, 779–785 (2020).
Kim, S. J., Choo, H. J. & Yoon, H. Diagnostic value of the Maximum Urethral closing pressure in women with overactive bladder symptoms and functional bladder outlet obstruction. Int. Neurourol. J. 26, S1–7 (2022).
Huang, W. J. RE: Third year medical student attitudes toward learning urology. J. Urol. 166, 1011 (2001).
Wu, P. C., Hsiao, S. M. & Lin, H. H. Prevalence and predictors of nocturnal polyuria in females with overactive bladder syndrome. World J. Urol. 40, 519–527 (2022).
Abrams, P. et al. The standardisation of terminology in lower urinary tract function: Report from the standardisation sub-committee of the International Continence Society. Urology. 61, 37–49 (2003).
Acknowledgements
Thanks to the research assistant, Mrs. Hsin-Yi Ho, who communicated with our patients.
Funding
This research received no external funding.
Author information
Authors and Affiliations
Contributions
Conceptualization, C-J W and H-H L; methodology, C-J W and S-M H; software, S-M H; validation, B-C S and H-H L; formal analysis, S-M H; investigation, T-C C, C-H C, and H-H L; resources, H-H L; data curation, C-J W, S-M Hs and P-C W; writing—original draft preparation, C-J W; writing—review and editing, H-H L; visualization, C-J W; supervision, B-C S; project administration, H-H Lin; All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Institutional Review Board Statement
This study received approval from the National Taiwan University Hospital research ethics committee (REC No:202105082RINA) and was registered at ClinicalTrials.gov (NCT04981080).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wu, CJ., Hsiao, SM., Wu, PC. et al. Prevalence and predictors of detrusor underactivity and bladder outlet obstruction in women with lower urinary tract symptoms. Sci Rep 14, 25141 (2024). https://doi.org/10.1038/s41598-024-76242-y
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-024-76242-y