Abstract
Intestinal permeability has been related to colorectal cancer (CRC) development. Zonulin, a protein able to regulate tight junction function and intestinal permeability, emerges as a promising marker to elucidate the contribution of bacterial translocation in CRC. An Italian case-control study included 77 CRC cases, 72 intestinal adenoma and 76 healthy controls (for a total of 148 tumor-free subjects), aged 20–85. Serum zonulin levels were quantified by ELISA kit and blood 16S rRNA gene copies by DNA extraction and polymerase chain reaction. We applied logistic regression models adjusted for center, sex, age and education. There was a positive association between zonulin and CRC risk. The odds ratio (OR) of CRC for the highest versus lowest tertile of zonulin as compared to tumor-free subjects was 2.36 (95% confidence interval, 1.14–4.86). The ORs were similar in colon and rectal cancers. The OR of colon cancer for the highest versus lowest levels of both zonulin and 16S rRNA gene copies was 4.55.
Circulating levels of zonulin were higher in CRC patients compared to tumor-free controls supporting the hypothesis of an interplay of gut barrier dysfunction and bacterial translocation in colorectal carcinogenesis. Zonulin may interact with 16S rRNA gene copies and serve as a further biomarker in the evaluation of CRC diagnosis.
Similar content being viewed by others
Introduction
Colorectal cancer (CRC) is one of the leading causes of cancer-related mortality worldwide, with about 1.8 million new cases diagnosed and about 1 million deaths each year1.
Intestinal microbiome is associated with the development of CRC2,3, and microbial translocation from the gastrointestinal tract to the bloodstream has been suggested to be implicated, too2,4,5,6,7. Intestinal permeability, also known as “leaky gut syndrome,” is a measure of the function of the intestinal barrier, which is responsible for selecting which elements enter the bloodstream from the intestine8. Intestinal dysbiosis, an alteration in the composition and function of intestinal microbiota, has been associated with an increase in intestinal permeability and an increased risk of CRC9,10. Moreover, intestinal permeability can exacerbate gastrointestinal chronic inflammation and inflammatory diseases, such as Crohn’s disease and ulcerative colitis, which are known risk factors for CRC11,12,13.
Zonulin is the only human protein able to (reversibly) regulate intestinal permeability by modulating intercellular tight junctions and is responsible for their opening and closing, allowing for the transit of molecules and fluids in and out of the gut14. In physiological conditions, zonulin plays an important role in regulating paracellular exchanges (e.g. dietary factors), and in protecting the gut barrier from the translocation of microbial cells15,16. In pathological conditions, zonulin has also been implicated in the development of several metabolic diseases, such as type 2 diabetes and obesity, which are also recognised risk factors for CRC12,17,18.
Increased serum levels of zonulin are an indicator of increased intestinal permeability, which can promote higher microbial translocation leading to pro-inflammatory signalling cascades and immune responses in the colorectal carcinogenesis. Serum levels of zonulin have been found to be related with a higher microbial translocation19, measured by bacterial 16S rRNA gene copies in blood, and our previous investigation on 100 CRC cases and 200 controls from Italy reported an over-representation of blood bacterial 16S rRNA gene copies in colon cancer patients compared to tumor-free controls20.
Despite the potential of serum zonulin to elucidate CRC pathways and to serve as a basis to develop new CRC diagnostic strategies, the association between intestinal permeability and CRC has been scarcely investigated21.
The aim of our study is to investigate the relationship between serum zonulin, as a marker of intestinal permeability, and CRC risk using data from a case-control study conducted in Italy20. This analysis will be also evaluated according to bacterial DNA load and profiling in blood.
Materials and methods
Setting and subjects’ recruiting
This case-control study was carried out between 2017 and 2019 in two university hospitals in the metropolitan area of Milan, Italy20. Eligible subjects were 20–85 years old patients, scheduled for a colonoscopy. Subjects with immunodeficiency, selected inflammatory diseases, liver/kidney/heart failure, reported previous cancer, recent hospitalization or colonoscopy, as well as any dietary modifications in the previous month, were excluded. Based on colonoscopies and histological examinations, reviewed by two pathologists, the participants were assigned to different groups. Cases were incident and histologically confirmed CRC. For each CRC case, subject with intestinal adenoma (IA) and a subject free from IA/CRC (hereafter referred to as a healthy control) were frequency-matched (1:1:1) by study center, sex and age (± 5 years).
The study was conducted according to the guidelines of the Declaration of Helsinki and the protocol was approved by the ethical committees of the involved hospitals: Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico (No. 742–2017; December 14, 2017) and ASST Grande Ospedale Metropolitano Niguarda (No. 477–112016; November 25, 2016). Enrolled subjects signed a written informed consent. Less than 2% of contacted eligible patients declined participation.
Out of 300 recruited subjects, we analysed data on subjects with available serum samples: 77 CRC cases and 72 IA and 76 healthy controls (for a total of 148 tumor-free subjects).
Definition and set up of the interview
The questionnaire was managed by trained and blinded interviewers, and included socio–demographic, education, lifestyle habits, anthropometric data, medical history and daily use of selected drugs. Information on the habitual diet of each participant was collected before the colonoscopy through a reproducible22 and validated23 food frequency questionnaire (FFQ).
Blood and serum collection
Blood samples were collected in 7 mL EDTA tube and in 3 mL blank tube before the colonoscopy. Part of the EDTA sample was immediately stored at − 80 °C for the microbiomic analysis. The sample without anticoagulant was processed and centrifuged (1400 g × 15 min, 4 °C), aliquoted in small vials, and then stored at − 80 °C for the circulating zonulin analysis.
Evaluation of intestinal permeability and 16S rRNA gene copies and profiling
Serum zonulin levels were quantified using the ELISA kit (cat. # K5601) from Immunodiagnostik® (Bensheim, Germany). Aliquots of serum samples were thawed (for the first time) at room temperature. The 96-well plate was pre-coated with a polyclonal anti-zonulin antibody. The competitive ELISA method provided for the addition of a biotinylated zonulin tracer to each sample (including the standards). The peroxidase-labeled streptavidin was added in order to bind the biotinylated zonulin tracer. Finally, following the reaction time, the reading of the fluorescence at 450 nm was performed with a Tecan plate reader (TECAN Infinite F200, Tecan Group Ltd. Mannedorf, Switzerland). The quantification of serum zonulin levels was carried out using a standard curve calculated by a 4-parameter algorithm as reported by the manufacturer.
For 16S rRNA gene copies analyses, DNA extraction, quantitative polymerase chain reaction (qPCR) experiments and sequencing of 16S rRNA gene amplicons were performed by Vaiomer SAS (Labège, France) through an optimized blood-specific technique, described elsewhere20. All samples were analyzed in the same experiment and with the same reagent batches and manipulator.
For both estimates, operators were blinded to the group assignment.
Statistical analysis
We evaluated differences in terms of zonulin by cancer diagnosis using an Anova test. We computed zonulin tertiles among healthy controls. Using multiple logistic regression models adjusted for study center, sex, age and education, we estimated the odds ratios (ORs) of CRC and the corresponding 95% confidence intervals (CIs) as compared to healthy controls, IA and tumor-free subjects (IA and healthy controls combined). We also estimated the ORs for an increment of zonulin equal to one standard deviation (computed among healthy controls; 4.7 ng/ml). In addition, we estimated the ORs of colon and rectal cancer separately. We also considered models further adjusted for body mass index (BMI), diabetes, and drugs use.
We carried out stratified analyses by strata of sex, age (< and ≥ 70) and education (< and ≥ 12 years), using tumor-free subjects as comparison group. Tests for heterogeneity between strata were based on the likelihood ratio test between models with and without interaction terms.
To estimate the relationship between zonulin and 16S rRNA gene copies, we applied a robust linear regression of 16S rRNA gene copies on zonulin using the Huber function24 in order to consider the outliers effect in the model. We then computed the OR of CRC for zonulin tertiles, as compared to tumor-free subjects, further adjusting for quintiles of 16S rRNA gene copies, according to our previous findings20. Using the same model, we estimated the OR of colon cancer for highest tertile of zonulin and the highest quintile of 16S rRNA gene copies compared to the lowest zonulin tertile and the lowest 16S three quintiles. Interaction of zonulin and 16S rRNA gene copies on colon cancer risk was tested comparing models with and without interaction terms.
We identified the genera significantly different according to zonulin tertiles (III vs. I-II) in terms of relative abundance using the Wilcoxon rank sum test and in terms of presence using a chi-square test.
All analyses were performed using SAS 9.4.
Results
Table 1 reports the number and percentages of CRC, IA and healthy controls by study center, sex, age, education, BMI, and diabetes. Their distributions were similar according to these characteristics; 36% of cases, 35% of IA and 33% of controls were women. Mean age was 65.7 (range: 31–85) for CRC, 66.6 (range:32–82) for IA and 65.3 (range: 26–85) for healthy controls.
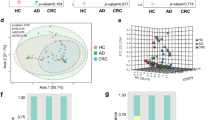
Figure 1 shows the distribution of zonulin among CRC, IA and healthy controls. The mean and median of zonulin were 31.0 ng/ml (SD, 4.2) and 31.0 ng/ml (range IQ, 6.2) in CRC cases, 28.9 ng/ml (SD, 3.7) and 28.6 ng/ml (range IQ, 5.0) in IA and 28.9 ng/ml (SD, 4.6) and 29.2 ng/ml (range IQ, 4.9) in healthy controls. There was heterogeneity between the three groups (p = 0.002), between CRC vs. healthy controls (p = 0.003), and CRC vs. IA (p = 0.002). No heterogeneity was found between IA and healthy controls (p = 0.86).
Plota of serum zonulin distribution among colorectal cancer (CRC) cases (n = 77), intestinal adenoma (IA) (n = 72) and healthy controls (n = 76). aLines indicate first, second and third quartiles.
Table 2 gives the number and the percentage of CRC (including colon and rectal cancer, separately), IA and healthy controls according to tertiles of zonulin. We reported the ORs and the corresponding 95% CIs of CRC for the second and third versus the first zonulin tertile and for an increment of one standard deviation, using as comparison groups: healthy controls, IA and tumor-free subjects (IA and healthy controls combined). There was a positive association between zonulin and CRC risk. The OR of CRC for the highest versus the lowest tertile as compared to healthy controls was 2.55 (95% CI, 1.12–5.82), with a p for trend of 0.018; the OR of CRC as compared to IA was 2.16 (95% CI, 0.91–5.14), with a p for trend of 0.047; the OR of CRC as compared to tumor-free subjects was 2.36 (95% CI, 1.14–4.86), with a p for trend of 0.011. The OR of colon cancer was 2.66 (95% CI, 1.03–6.87), with a p of trend of 0.025, and the OR of rectal cancer was 2.11 (95% CI, 0.83–5.39), with a p of trend of 0.087, considering tumor-free subjects as comparison group.
When we further adjusted for BMI, diabetes and drug use, the OR of CRC was 2.71 (95% CI, 1.27–5.76). We also performed a sensitivity analysis by removing diabetic subjects and found similar results (OR, 2.21; 95% CI, 1.02–4.79).
Figure 2 shows the ORs of CRC for the highest versus the lowest tertile of zonulin in strata of sex, age and education. The associations were apparently stronger in women (OR, 4.86), young individuals (OR, 3.51) and subjects more educated (OR, 3.43), although there was no significant heterogeneity (p = 0.21, 0.20, 0.96, respectively).
Odds ratiosa (ORs) of colorectal cancer (CRC) and 95% confidence intervals (CIs) for the highest versus the lowest zonulin tertile by strata of sex, age and education among 77 CRC and 148 tumor-free subjects. Italy 2017–2019. a Estimated from logistic regression model adjusted for study center, sex, age, education.
When we investigated the relationship between 16S rRNA gene copies and zonulin trough robust regression models, we found that 16S rRNA gene copies tended to increase with higher zonulin levels, with a slope of 136 (p = 0.04) for an increment of a zonulin unit, among healthy subjects (Supplementary Fig. 1). Overall, the slope was 58, not significantly different from 0 (p = 0.18).
Further adjusting for 16S rRNA gene copies, the ORs of CRC for zonulin tertiles did not appreciably change: the ORs were 2.40 for CRC, 2.82 for colon and 2.41 for rectal cancer.
Supplementary Fig. 2 shows the combined effect of zonulin and 16S rRNA gene copies on colon cancer risk. For subjects in the lowest tertile of zonulin and the highest quintile of 16S, the OR of colon cancer was 2.34 (95% CI = 0.76–7.19) as compared to subjects in both the lowest zonulin tertile and the lowest three 16S quintiles, whereas for subjects in the highest tertile of zonulin and the lowest three quintiles of 16S, the OR was 3.33 (95% CI = 1.12–9.87). For subjects in the highest tertile of zonulin and the highest quintile of 16S rRNA, the OR of colon cancer was 4.55 (95% CI = 1.17–17.66). There was no significant interaction (p = 0.51).
When we evaluated the differences of bacteria genera in terms of zonulin, the relative abundances or prevalences of the genera Alkanindiges, Daeguia, Methylobacterium, Limnohabitans, and Sphingobacterium were higher in the highest as compared to the lowest two zonulin tertiles. Conversely, the genera Sphingobium, Corynebacterium 1, and Staphylococcus were lower in the highest zonulin tertile.
Discussion
Our study shows an association between circulating levels of zonulin and CRC risk, supporting the hypothesis that an increased intestinal permeability (or leaky gut syndrome) could play a role in CRC development. This novel result, together with the additive effect of serum zonulin and circulating bacterial 16S rRNA gene copies found on colon cancer risk, supports the evidence regarding the interplay between gut barrier dysfunction, microbial translocation, and colon cancer risk.
These results align with the findings from a Russian study, including 152 CRC patients and 134 controls21, which reported that CRC patients had significantly higher levels of serum zonulin compared to healthy subjects and patients with non-tumor inflammatory bowel disease (IBD). That study found that the level of zonulin increased with the progression of the disease. In addition, a nested case-control study from the Health Professionals Follow-Up Study, including 261 incident CRC cases and 261 controls, supported the involvement of microbial translocation, as indicated by plasma sCD14 levels and potentially EndoCAb IgM, in the development of CRC6. In another case-control study, including 26 CRC cases and 41 healthy controls from South Africa, circulating bacterial toxins, such as lipopolysaccharides (LPS), were significantly elevated in the CRC patients compared to healthy controls4. Moreover, a Greek study, including 397 adjuvant or metastatic CRC cases and 32 healthy controls, reported a positive association between microbial translocation, measured by blood bacterial 16S rRNA gene copies, and CRC5, similarly to our previous investigation on these data20.
Increased serum levels of zonulin have been associated with increased blood 16S rRNA gene copies in an elderly Italian population comprising 43 healthy subjects19. Our data were consistent with those findings in healthy controls, but did not show any significant correlation between serum zonulin and 16S rRNA gene copies overall and among CRC cases, suggesting that higher intestinal permeability and higher bacterial DNA translocation independently act on the risk of colon cancer. Zonulin is one of the different markers associated with intestinal permeability, and 16S rRNA gene copies, as a marker for microbial translocation, is grounded in the well-established concept that bacterial DNA in the bloodstream reflects increased permeability of the gut barrier25,26. In CRC patients, compromised intercellular integrity can facilitate bacterial entry into the bloodstream, potentially influencing our observed elevation in 16S rRNA gene copies. Our study also includes information on bacteria in blood in relation to zonulin levels, providing further insights on gut barrier functions.
Zonulin is part of the haptoglobin family proteins27 and the structural and functional diversity within the zonulin family underscores the complexity of its role in regulating intestinal barrier function17,28. It has been reported that the Immunodiagnostik kit does not recognize prohaptoglobin27. However, Fasano and colleagues29 highlighted the broader impact of the zonulin family on intestinal health. Measuring the entire zonulin family could offer a more comprehensive assessment of the dynamic interactions within the intestinal barrier. This integrative approach aligns with emerging research that emphasizes the interconnectedness of various proteins in maintaining gut homeostasis30. In our study, measuring the complete zonulin family allows capturing the collective influence of these proteins on intestinal permeability.
An increasing evidence suggests that the disruption of the protective mucosal barrier in the gastrointestinal tract contributes to the development of CRC2,10,16. The impairment of the colonic barrier integrity leads to heightened exposure of colonocytes and other components of the mucosal immune system to toxins present in the colonic environment, thereby amplifying inflammatory processes and the release of reactive oxygen species16. Zonulin has been implicated in many chronic inflammatory diseases17. Serum zonulin is upregulated in irritable bowel syndrome (IBS) and the levels are comparable to those in celiac disease31. Levels of faecal and serum zonulin were also elevated in patients diagnosed with Crohn’s disease, while no association was observed with ulcerative colitis in a study on 40 IBD patients and 40 healthy subjects32. However, another study based on 118 IBD patients and 23 healthy controls found higher serum zonulin concentrations in patients with Crohn’s disease and ulcerative colitis and an inverse correlation between serum zonulin concentration and disease duration33. Those findings suggest that zonulin dysregulation may be a common feature of gastrointestinal disorders, including CRC.
In addition to the overall association, we explored potential effect modifiers in the zonulin-CRC relationship. The associations between zonulin levels and CRC risk appeared to be stronger in women and young individuals, without however significant heterogeneity. These findings are consistent with a study by Maget et al.34, which reported that females exhibited significantly higher levels of serum zonulin than males, suggesting a gender-related difference in zonulin regulation.
Furthermore, we computed the ORs by BMI categories and found that the OR of CRC was 1.48 among subjects with BMI < 25 and 4.06 among subjects with BMI ≥ 25 kg/m2, without a significant heterogeneity (p = 0.43). In other studies using zonulin as intestinal permeability marker, a positive association was found between intestinal permeability alteration and obesity35,36. Additionally, a study on obese children patients found that zonulin levels were associated with HDL-C and leptin levels, even after adjusting for age and BMI36. These results indicate a potential interaction between zonulin, obesity, and CRC risk. The well-known association between obesity and increased CRC risk37 can at least in part be mediated by a gut barrier dysfunction and an altered gut microbiota. Dietary habits can influence that interaction, but intervention studies are not univocal to date in supporting the influence of dietary modifications on circulating zonulin levels38,39,40. Investigating (dietary) interventions targeting zonulin and bacterial translocation may offer promising avenues for personalized preventative strategies in individuals at high risk of CRC.
In our study, the data on serum zonulin aim to shed a light on the underlying mechanisms of microbial translocation in CRC, indicating the importance of considering both host and microbial factors in CRC development. When we considered the relationship between zonulin and CRC risk by stage, we found an OR of 1.25 for I-II stage and of 9.18 for III-IV stage. Our findings could also offer innovative data useful to conceive new non-invasive strategy for the detection of CRC diagnosis and severity. Circulating levels of biological markers have been widely studied in relation to CRC, with the aim of identifying potential biomarkers for early detection applicable to screening and early diagnosis of the disease41,42. In line with our study, most of the proposed diagnostic tests for CRC are increasingly based on microbial signatures in faecal or blood samples3,5,43.
Given the lack of data on faecal microbiota, we were not able to evaluate as a whole the pathway linking gut microbiota, intestinal permeability, and inflammation in CRC carcinogenesis. However, we identified blood bacterial DNA that were different according to zonulin levels and assessed the ORs of colon cancer according to combined levels of zonulin and 16S rRNA gene copies. Another limitation is that our results cannot distinguish whether the elevated zonulin is a consequence or a predictor of the disease, and we cannot infer on a direct causal relationship between intestinal permeability and CRC. However, most cases were detected at the first CRC-diagnosing colonoscopy, allowing us to recruit incident cases from the very beginning of the diagnostic process.
With reference to selection bias, CRC cases, healthy and IA subjects were recruited in the same hospital among patients admitted for colonoscopy. An ad hoc data collection was applied to recruit all patients according to the same procedures (e.g. similar setting, catchment areas). We took care to exclude subjects with history of cancer or with selected chronic and inflammatory diseases. However, we cannot rule out residual selection bias due to the characteristics of the population undergoing colonoscopy. The participation rate was satisfactory.
Our questionnaire was administered by trained interviewers, reducing information bias. Interviewers and investigators were blinded to the group assignment, as data collection was performed before endoscopy. In addition, our cases were unaware of the cancer diagnosis at the time of the interview, ideally removing the over-reporting bias of cases. With reference to confounding, we were able to adjust for study center, sex, age, education, BMI, diabetes, and use of selected drugs. Further controlling for 16S rRNA gene copies in the models did not modify the associations with zonulin. In addition, the use of healthy controls, IA or tumor-free subjects as comparison group did not change the results. A major limitation of this study remains the relatively small sample size. The fact that results from this case-control study are in line with previous findings involving different modifiable factors associated with CRC risk is partially reassuring44,45,46,47. Additional biological experiments could provide further evidence to the current findings.
In conclusion, circulating levels of zonulin, which is considered a measure of intestinal permeability, were higher in CRC patients compared to tumor-free controls supporting the hypothesis that intestinal permeability may contribute to the development of this neoplasm. Future prospective studies are needed to elucidate the underlying mechanisms and validate the clinical utility of zonulin as a potential biomarker for CRC risk stratification.
Data availability
All the reads are publicly available in the European Nucleotide Archive (ENA) with the accession number: PRJEB46474.
References
Rawla, P., Sunkara, T. & Barsouk, A. Epidemiology of colorectal cancer: incidence, mortality, survival, and risk factors. Prz Gastroenterol. 14, 89–103. https://doi.org/10.5114/pg.2018.81072 (2019).
Janney, A., Powrie, F. & Mann, E. H. Host-microbiota maladaptation in colorectal cancer. Nature. 585, 509–517. https://doi.org/10.1038/s41586-020-2729-3 (2020).
Wirbel, J. et al. Meta-analysis of fecal metagenomes reveals global microbial signatures that are specific for colorectal cancer. Nat. Med. 25, 679–689. https://doi.org/10.1038/s41591-019-0406-6 (2019).
de Waal, G. M., de Villiers, W. J. S., Forgan, T., Roberts, T. & Pretorius, E. Colorectal cancer is associated with increased circulating lipopolysaccharide, inflammation and hypercoagulability. Sci. Rep. 10, 8777. https://doi.org/10.1038/s41598-020-65324-2 (2020).
Messaritakis, I. et al. The Prognostic Value of the detection of Microbial translocation in the blood of colorectal cancer patients. Cancers (Basel). 12 https://doi.org/10.3390/cancers12041058 (2020).
Shi, M. et al. Circulating markers of microbial translocation and host response to bacteria with risk of colorectal cancer: a prospective, nested case-control study in men. EBioMedicine. 91, 104566. https://doi.org/10.1016/j.ebiom.2023.104566 (2023).
Xiao, Q. et al. Alterations of circulating bacterial DNA in colorectal cancer and adenoma: a proof-of-concept study. Cancer Lett. 499, 201–208. https://doi.org/10.1016/j.canlet.2020.11.030 (2021).
Camilleri, M. Leaky gut: mechanisms, measurement and clinical implications in humans. Gut. 68, 1516–1526. https://doi.org/10.1136/gutjnl-2019-318427 (2019).
Round, J. L. & Mazmanian, S. K. The gut microbiota shapes intestinal immune responses during health and disease. Nat. Rev. Immunol. 9, 313–323. https://doi.org/10.1038/nri2515 (2009).
Yu, L. C. Microbiota dysbiosis and barrier dysfunction in inflammatory bowel disease and colorectal cancers: exploring a common ground hypothesis. J. Biomed. Sci. 25, 79. https://doi.org/10.1186/s12929-018-0483-8 (2018).
Coussens, L. M. & Werb, Z. Inflammation and cancer. Nature. 420, 860–867. https://doi.org/10.1038/nature01322 (2002).
Keum, N. & Giovannucci, E. Global burden of colorectal cancer: emerging trends, risk factors and prevention strategies. Nat. Rev. Gastroenterol. Hepatol. 16, 713–732. https://doi.org/10.1038/s41575-019-0189-8 (2019).
Loftus, E. V., Sandborn, W. J. & Jr. & Epidemiology of inflammatory bowel disease. Gastroenterol. Clin. North. Am. 31, 1–20. https://doi.org/10.1016/s0889-8553(01)00002-4 (2002).
Fasano, A. Zonulin and its regulation of intestinal barrier function: the biological door to inflammation, autoimmunity, and cancer. Physiol. Rev. 91, 151–175. https://doi.org/10.1152/physrev.00003.2008 (2011).
Fasano, A. & Zonulin Regulation of tight junctions, and autoimmune diseases. Ann. N Y Acad. Sci. 1258, 25–33. https://doi.org/10.1111/j.1749-6632.2012.06538.x (2012).
Genua, F., Raghunathan, V., Jenab, M., Gallagher, W. M. & Hughes, D. J. The role of gut barrier dysfunction and microbiome dysbiosis in colorectal cancer development. Front. Oncol. 11, 626349. https://doi.org/10.3389/fonc.2021.626349 (2021).
Fasano, A. All disease begins in the (leaky) gut: role of zonulin-mediated gut permeability in the pathogenesis of some chronic inflammatory diseases. F1000Res. 9 https://doi.org/10.12688/f1000research.20510.1 (2020).
Sturgeon, C. & Fasano, A. Zonulin, a regulator of epithelial and endothelial barrier functions, and its involvement in chronic inflammatory diseases. Tissue Barriers. 4, e1251384. https://doi.org/10.1080/21688370.2016.1251384 (2016).
Gargari, G. et al. Bacterial DNAemia is associated with serum zonulin levels in older subjects. Sci. Rep. 11, 11054. https://doi.org/10.1038/s41598-021-90476-0 (2021).
Mutignani, M. et al. Blood bacterial DNA load and profiling differ in colorectal cancer patients compared to tumor-free controls. Cancers (Basel). 13. https://doi.org/10.3390/cancers13246363 (2021).
Kushlinskii, N. E. et al. Blood serum zonulin in colorectal cancer, autoimmune Bowel diseases, and irritable bowel syndrome. Bull. Exp. Biol. Med. 173, 376–379. https://doi.org/10.1007/s10517-022-05552-w (2022).
Franceschi, S. et al. Reproducibility of an Italian food frequency questionnaire for cancer studies: results for specific food items. Eur. J. Cancer. 29A, 2298–2305. https://doi.org/10.1016/0959-8049(93)90225-5 (1993).
Decarli, A. et al. Validation of a food-frequency questionnaire to assess dietary intakes in cancer studies in Italy. Results for specific nutrients. Ann. Epidemiol. 6, 110–118. https://doi.org/10.1016/1047-2797(95)00129-8 (1996).
Yu, C. & Yao, W. X. Robust linear regression: a review and comparison. Commun. Stat-Simul C. 46, 6261–6282. https://doi.org/10.1080/03610918.2016.1202271 (2017).
Fukui, H. Increased intestinal permeability and decreased barrier function: does it really influence the risk of inflammation? Inflamm. Intest Dis. 1, 135–145. https://doi.org/10.1159/000447252 (2016).
Skinner, C., Thompson, A. J., Thursz, M. R., Marchesi, J. R. & Vergis, N. Intestinal permeability and bacterial translocation in patients with liver disease, focusing on alcoholic aetiology: methods of assessment and therapeutic intervention. Th. Adv. Gastroenterol. 13, 1756284820942616. https://doi.org/10.1177/1756284820942616 (2020).
Ajamian, M., Steer, D., Rosella, G. & Gibson, P. R. Serum zonulin as a marker of intestinal mucosal barrier function: may not be what it seems. PLoS One. 14, e0210728. https://doi.org/10.1371/journal.pone.0210728 (2019).
Scheffler, L. et al. Widely used commercial ELISA does not detect precursor of Haptoglobin2, but recognizes properdin as a potential second member of the Zonulin family. Front. Endocrinol. (Lausanne). 9, 22. https://doi.org/10.3389/fendo.2018.00022 (2018).
Fasano, A. Zonulin measurement conundrum: add confusion to confusion does not lead to clarity. Gut. 70, 2007–2008. https://doi.org/10.1136/gutjnl-2020-323367 (2021).
Ternet, C. & Kiel, C. Signaling pathways in intestinal homeostasis and colorectal cancer: KRAS at centre stage. Cell. Commun. Signal. 19, 31. https://doi.org/10.1186/s12964-021-00712-3 (2021).
Singh, P. et al. Serum zonulin is elevated in IBS and correlates with stool frequency in IBS-D. United Eur. Gastroenterol. J. 7, 709–715. https://doi.org/10.1177/2050640619826419 (2019).
Malickova, K. et al. Fecal zonulin is elevated in Crohn’s disease and in cigarette smokers. Pract. Lab. Med. 9, 39–44. https://doi.org/10.1016/j.plabm.2017.09.001 (2017).
Caviglia, G. P. et al. Serum zonulin in patients with inflammatory bowel disease: a pilot study. Minerva Med. 110, 95–100. https://doi.org/10.23736/S0026-4806.18.05787-7 (2019).
Maget, A. et al. Sex differences in zonulin in affective disorders and associations with current mood symptoms. J. Affect. Disord. 294, 441–446. https://doi.org/10.1016/j.jad.2021.07.021 (2021).
Bona, M. D. et al. Intestinal barrier permeability in obese individuals with or without metabolic syndrome: a systematic review. Nutrients. 14 https://doi.org/10.3390/nu14173649 (2022).
Kume, T. et al. The relationship between serum zonulin level and clinical and laboratory parameters of childhood obesity. J. Clin. Res. Pediatr. Endocrinol. 9, 31–38. https://doi.org/10.4274/jcrpe.3682 (2017).
Mandic, M. et al. Is the association of overweight and obesity with colorectal cancer underestimated? An umbrella review of systematic reviews and meta-analyses. Eur. J. Epidemiol. 38, 135–144. https://doi.org/10.1007/s10654-022-00954-6 (2023).
Del Bo, C. et al. A polyphenol-rich dietary pattern improves intestinal permeability, evaluated as serum zonulin levels, in older subjects: the MaPLE randomised controlled trial. Clin. Nutr. 40, 3006–3018. https://doi.org/10.1016/j.clnu.2020.12.014 (2021).
Linsalata, M. et al. The effects of a very-low-calorie ketogenic diet on the intestinal barrier integrity and function in patients with obesity: a pilot study. Nutrients. 15 https://doi.org/10.3390/nu15112561 (2023).
Riviere, A. J., Smith, K. S., Schaberg, M. N., Greene, M. W. & Fruge, A. D. Plasma and fecal zonulin are not altered by a high green leafy vegetable dietary intervention: secondary analysis of a randomized control crossover trial. BMC Gastroenterol. 22, 184. https://doi.org/10.1186/s12876-022-02248-3 (2022).
Loktionov, A. Biomarkers for detecting colorectal cancer non-invasively: DNA, RNA or proteins? World J. Gastrointest. Oncol. 12, 124–148. https://doi.org/10.4251/wjgo.v12.i2.124 (2020).
Ransohoff, D. F. Evaluating a new cancer screening blood test: Unintended consequences and the need for clarity in policy making. J. Natl. Cancer Inst. 113, 109–111. https://doi.org/10.1093/jnci/djaa104 (2021).
Poore, G. D. et al. Microbiome analyses of blood and tissues suggest cancer diagnostic approach. Nature. 579, 567–574. https://doi.org/10.1038/s41586-020-2095-1 (2020).
Rossi, M. et al. Flavonoids and colorectal cancer in Italy. Cancer Epidemiol. Biomarkers Prev. 15, 1555–1558. https://doi.org/10.1158/1055-9965.EPI-06-0017 (2006).
Speciani, M. C. et al. Flavonoid intake in relation to colorectal cancer risk and blood bacterial DNA. Nutrients. 14 https://doi.org/10.3390/nu14214516 (2022).
Speciani, M. C. et al. Garlic consumption in relation to colorectal cancer risk and to alterations of blood bacterial DNA. Eur. J. Nutr. 62, 2279–2292. https://doi.org/10.1007/s00394-023-03110-2 (2023).
Turati, F., Guercio, V., Pelucchi, C., La Vecchia, C. & Galeone, C. Colorectal cancer and adenomatous polyps in relation to allium vegetables intake: a meta-analysis of observational studies. Mol. Nutr. Food Res. 58, 1907–1914. https://doi.org/10.1002/mnfr.201400169 (2014).
Acknowledgements
The authors would like to express their sincerest gratitude to all participants and collaborators to this study, without whose effort this work would not have been feasible. A special thanks to Margherita Cozzi for her valuable involvement in this study. We thank Elena Tansi, Cinzia Della Noce, Rosa Restieri, Nadia Zaretti as well as all the nursing staff at the Digestive and Interventional Endoscopy Unit, ASST Grande Ospedale Metropolitano Niguarda, Milan, and at the Gastroenterology and Endoscopy Unit, Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico, Milan. A thankful mention to Luisa De Simone e Giuseppe Giovenzana for their constant and accurate help in the preparation of the laboratory material. The authors acknowledge support from the Department of Clinical Sciences and Community Health, University of Milan through the APC initiative.
Funding
Data collection was supported by the Italian Foundation for Cancer Research (AIRC) (My First AIRC grant No. 17070). Data analysis was supported by the grant PRIN 2022 PNRR (no. P20229A9S5) from the Italian Ministry of University and Research (MUR).
Author information
Authors and Affiliations
Contributions
MR and PR conceived the work. MR and CLV designed the work. MC, RP, GG, CC, PL, AA, MV, RB, BO, PC, MVa, MMu and MR acquired data. MM, SM, KM, MF, LP, CDB, SG, PR, CLV and MR interpreted the results. MM, GG, CDB and RB contributed to data elaboration. SM and MR conducted statistical analysis. MM, SM and MR drafted the manuscript. All authors critically revised and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
The study was conducted according to the guidelines of the Declaration of Helsinki, and ap-proved by the Ethics Committees of ASST Grande Ospedale Metropolitano Niguarda (No. 477–112016; November 25, 2016) and Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico (No. 742–2017; December 14, 2017). Written informed consent was obtained from all subjects involved in the study.
Consent for publication
All authors consent to the publication of the present version of the manuscript.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Figure 1. (download DOCX )
Scatterplot of zonulin and 16S rRNA gene copies among 76 healthy controls. Supplementary Figure 2. Odds ratiosa (ORs) and 95% confidence intervals (CIs) according to combination of zonulin tertiles and 16S rRNA gene copies quintiles among 39 colon cancer cases and 148 tumor-free subjects; Italy 2017–2019.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Marino, M., Mignozzi, S., Michels, K. et al. Serum zonulin and colorectal cancer risk. Sci Rep 14, 28171 (2024). https://doi.org/10.1038/s41598-024-76697-z
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-024-76697-z
This article is cited by
-
Gut dysbiosis in oncology: a risk factor for immunoresistance
Cell Research (2026)