Abstract
Pain is defined as an unpleasant sensory and emotional experience in response to a noxious stimulus. Nowadays, it is increasingly prevalent among adults and may be influenced by past experiences such as child abuse, trauma or psychiatric conditions like anxiety. Thus, this study aims to evaluate the mediating effect of anxiety between child abuse and pain among a sample of Lebanese adults. This cross-sectional study was conducted between March and April 2024. Participants were selected using a snowball sampling method from various Lebanese governorates, and completed a self-administered online questionnaire via Google Forms. All adults over the age of 18 were eligible to participate. The questionnaire included sociodemographic questions, the short form of McGill pain questionnaire, the generalized anxiety disorder-7 (GAD-7), and the child abuse self report scale (CASRS-12). A total of 507 Lebanese adults completed the questionnaire. The mean age was 26.80 ± 10.29 years and 73.2% were female. The results showed that anxiety partially mediated the association between child abuse and pain. Higher levels of child abuse were significantly associated with greater anxiety, which in turn was significantly associated with increased pain. Child abuse was directly associated with higher pain levels. The study highlights the relationship that child abuse has on pain in adults and its relationship with anxiety. Future research delving into the relationship between child abuse and chronic pain in adulthood is essential to better understand the underlying pathways and support effective prevention and intervention strategies.
Similar content being viewed by others
Introduction
Pain in adults is a common complaint in clinical settings1. It is defined as an unpleasant sensory and emotional experience, and is typically classified as either acute or chronic. Acute pain is characterized by a sudden onset (< 1 month) and a limited duration, often resulting from a normal physiological response to injury, trauma or surgery. In contrast, chronic pain persists for longer than three months or beyond the body’s usual healing time, and may arise from an illness, injury, or sometimes an unknown cause1. Pain can diminish an individual’s quality of life, resulting in social isolation, emotional discomfort, and physical restrictions2. Pain is categorized into six types: neuropathic, nociceptive, musculoskeletal, inflammatory, psychogenic, or mechanical3.
The prevalence of pain is more prevalent worldwide4. A study in 2021 showed that 20.9% of adults in the United States experience chronic pain5. Similarly, a systematic review in the United Kingdom revealed that the prevalence of chronic pain is approximately 43%, which rises with increasing age6. Even though pain commonly follows illness or injury, it is increasingly recognized as a distinct medical condition with its own diagnostic and therapeutic considerations.
Child abuse and pain
Notably, pain in adulthood can be related to a history of child abuse. The World Health Organization (WHO) defines child abuse as any form of sexual, physical or emotional abuse or exploitation that may harm a child’s development, health, or dignity4. This includes behaviors such as bruising, scarring, intimidation, criticism, bullying and coercing a child into actions for another person’s benefit. It is a violation of human rights, with estimates suggesting that at least one in seven children experiences a form of abuse each year7. Beyond its psychological toll, child abuse also imposes significant social and economic burden8. Other studies have revealed that child abuse is associated with a range of long-term consequences, including mood disorders9,10,11,12,13, memory impairment14, physical disability15,16, early death17 and suicide attempts9,17,18.
Studies have demonstrated a strong correlation between maltreatment throughout childhood and persistent pain during adulthood19. This may be due to an altered pain sensitivity resulting from of long-term dysregulation of the body’s stress-response systems and neurobiological changes in pain-processing pathways9. A meta-analytic review found that individuals who reported childhood abuse or neglect were significantly more likely to experience pain symptoms and related conditions later in life compared to those without such histories19. In addition, individuals with chronic pain were more likely to report having been abused or neglected as children than healthy controls19. This suggests that individuals who experienced physical, emotional, or sexual abuse or neglect during childhood are at heightened risk not only for chronic pain but also for comorbid mood disorders and functional impairments9,19.
Anxiety and pain
Pain, often associated with a history of child abuse10,19, is frequently accompanied by anxiety9,10, further increasing the overall burden on affected individuals. Anxiety is a physiological state characterized by persistent fear and worry, involving cognitive, physical, emotional, and behavioral components that persist and become more intense, interfering with daily activities20. Physical symptoms may include breathlessness and palpitations, whereas the cognitive aspect involves anticipating vague but realistic threats20. The Diagnostic and Statistical Manual of Mental Disorders–Fifth edition (DSM-5) classifies anxiety disorders into several subtypes, including panic disorder, phobias, and Generalized Anxiety Disorder (GAD)20. The prevalence of anxiety is on the rise globally; according to the World Health Organization (WHO) report21, an estimated 4% of the global population currently experiences an anxiety disorder. In 2019, 301 million people in the world had an anxiety disorder, making it the most common category of mental health disorders21,22.
Pain, child abuse and anxiety
Anxiety has been showed to act as a mediator in various health conditions, like heart failure, coronary artery disease, suicidal ideation, mood disorders23,24,25. It is therefore not surprising that anxiety and chronic pain frequently coexist23,26. Moreover, researchers have gained a deeper understanding of the brain’s functions and how the nervous system interacts with other parts of the body. They have discovered that pain shares several biological mechanisms with anxiety and depression. Specifically, the somatosensory cortex, which interprets sensations such as touch and pain, also plays a role in anxiety and depression23,26. In addition, two neurotransmitters, serotonin and norepinephrine, contribute to pain signaling in the brain and nervous system23,26,27,28. Consequently, the experience of childhood trauma is highly associated with anxiety from the perspective of disruption of emotion regulation as well as more negative emotional states and interpersonal problems. These psychological effects can predispose individuals to higher pain sensitivity and thus, sensation of pain10,28,29.
The present study
In the past decades, children were more exposed to different forms of abuse, due to a lack of parenting skills, discipline strategies and child protection measures30. However, its consequences are evident and more prominent in today’s adult population. Child abuse remains a sensitive and underreported issue in Lebanon, making its true prevalence difficult to determine. A study using data between 2017 and 2019 estimated child maltreatment at 3.2%31, although this number likely underrepresents the actual rate due to cultural norms that emphasize endurance and discourage disclosure31. Another national study reported that 27.9% of individuals experienced at least one childhood adversity, with 4.9% reporting two adversities and 2.6% reporting three or more32. Additionally, adults with a history of physical abuse or mental illness are more likely to mistreat their children33. Cultural acceptance of physical punishment as a disciplinary method remains prevalent in Arab societies. For instance, a study in Kuwait showed that the majority of parents endorse physical punishment for child misbehavior34, a practice often unchallenged by law and still present today despite growing awareness of its psychological consequences. However, this method was deemed natural and persisted in modern times, albeit to a lesser extent, considering the spread of parental education and despite the negative repercussions it has on adult life, ranging from pain to psychiatric disorders34. Furthermore, one study showed the prevalence of chronic pain to be higher in elderly populations35. Not to forget the role of anxiety that could arise, later in life, from maltreatment of children36. This added factor could potentially aggravate the pain perceived by adults in the future27. As well, although anxiety has been shown to favor the development of pain, the latter could still manifest as an independent complaint35. Likewise, studies focused on the effect of household overcrowding suggest a 23 to 46% increased risk of child abuse, reflected in urban and poor children37,38. Besides, a Korean study conducted using the data from the 2020 Korean Children and Youth Rights Survey (KCYRS) revealed the protective role of physical activity on child abuse and the decreased negative effects of emotional abuse39. Taking into account the unique cultural dynamics of the Lebanese population and in view of the limited research regarding the negative effects of child maltreatment on adulthood, this study aims to evaluate the mediating effect of anxiety between child abuse and pain among a sample of Lebanese adults.
Methods
Study design and participants
This cross-sectional study was accomplished between March and April 2024, employing a snowball sampling method, where existing participants recruits future participants from social work and acquaintances40. We designed a survey using Google Forms and distributed it to Lebanese adults from diverse background including university students, non-institutionalized individuals and other community members through various messaging platforms and social media channels, including WhatsApp, Instagram, and Messenger. All respondents voluntarily participated in the survey, with no compensation for their participation. All adults over the age of 18 years were eligible to partake in the study. Exclusion criteria were respondents that completely declined participation and those under 18 years.
Minimal sample size calculation
A minimum sample size of 406 was deemed necessary to ensure sufficient statistical power using the formula suggested by Fritz and MacKinnon41 \(n=\frac{L}{f2}+k+1\), where f = 0.14 for small effect size, L = 7.85 for an α error = 5% and power β = 80%, and k = 5 variables that will be included to the mediation model.
Questionnaire
The Arabic questionnaire took an average of 10 min to be completed. The first section gathered sociodemographic information such as sex, age, marital status, and the Household Crowding Index (HCI), which is calculated by dividing the number of people living in the household, excluding newborns, by the total number of rooms, excluding the kitchen and bathrooms42; the higher the household crowding index, the lower the socioeconomic status of the family. The strength, frequency, and duration of physical activity were multiplied to create the physical activity index43.
Short form of McGill pain questionnaire
The short form of McGill pain questionnaire consists of 15 descriptors: 11 sensory items (throbbing, shooting, stabbing, sharp, cramping, gnawing, hot-burning, aching, heavy, tender, and splitting), and 4 affective items (tiring-exhausting, sickening, fearful, and punishing-cruel); rated on a four-point intensity scale: 0 = none, 1 = mild, 2 = moderate or 3 = severe. In addition to the 15-item checklist, two items assess the overall pain experience; patients were asked to rate the level of their current pain on the Present Pain Intensity (PPI) index where 1 = no pain, 2 = mild, 3 = discomfort, 4 = distressing, 5 = horrible, and 6 = excruciating, and described whether their pain was brief, intermittent, or continuous. Also, the SF-MPQ includes a visual analog scale44. It is a reliable qualitative and quantitative assessment tool for pain and has been translated for use among Arabic-speaking patients, with a Cronbach’s α of 0.8545 (Cronbach’s α in this study = 0.92).
Generalized anxiety disorder (GAD-7)
The GAD-7 is a self-administered, 7-item scale, used for identifying likely cases of Generalized Anxiety Disorder over the past 2 weeks. Items are rated on a 4-point Likert-type scale (0 = not at all, 1 = several days, 2 = more than half the days, 3 = nearly every day)46,47. Higher scores indicate a greater risk of anxiety. The scale has been validated in Arabic among adults and adolescents and has demonstrated great psychometric properties46,47. It is short and easy to administer with an internal consistency Cronbach’s α from 0.79–0.9147 (Cronbach’s α in this study = 0.88).
Child abuse self-report scale (CASRS-12)
This scale was developed by Fekih-Romdhane et al.48 and assesses four dimensions of child abuse: physical, psychological and sexual abuse, and neglect using only 12 items. Items are scored on a scale from 0 to 3 (never ∼ always). A higher total score indicates more severe childhood abuse. The scale has been validated in Lebanon, with a McDonald’s ω values ranging from 0.87 to 0.93 for the four subscales48 (Cronbach’s α in this study = 0.86).
Statistical analyses
Data analysis was performed using the SPSS software version 26. There was no missing data in our database since all questions were required in the Google Forms. Reliability of the scales was checked using Cronbach’s alpha values. The anxiety score had a normal distribution as shown by the skewness (= 0.459) and kurtosis (= -0.242) values varying between ± 1. The student t-test was used to compare continuous variables between two groups, and Pearson correlation was used for linear correlation between continuous variables. The mediation analysis was conducted using the PROCESS SPSS Macro version 4.2, model 4 for SPSS, a regression-based approach for testing mediation effects. All exposure, mediator, and outcome variables were treated as continuous in the mediation model. Four pathways were generated; Pathway A determined the effect of the child abuse on anxiety (the mediator); Pathway B examined the association between anxiety and pain, and Pathways C and C’ estimated the total and direct effects of child abuse on pain. Mediation significance was determined using Bootstrapped confidence intervals, where an effect was considered significant if the interval did not include zero. The effect ratio was calculated (indirect effect / total effect), which would help quantify how much of the association is shared across variables. Covariates for adjustment in the mediation analysis were selected based on a p value threshold of < 0.25 in the bivariate analyses49. Nagelkerke R2 values were calculated for each model, with values between 0.02–0.13 reflect small effect, whereas values between 0.13–0.26 and ≥ 0.26 indicate medium and large effect respectively50. For all statistical tests, significance was set at p < 0.05.
Results
Five hundred seven adults completed the survey, with a mean age of 26.80 ± 10.29 years [min = 18; max = 70] and 73.2% females. Other description of the sample can be found in (Table 1).
Bivariate analysis
Higher mean pain scores were significantly found in married compared to single participants (Table 2), whereas older age, higher anxiety and child abuse were significantly associated with more pain (Table 3).
Mediation analysis
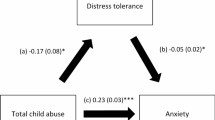
The results of the mediation analysis were adjusted over age and marital status. Excluded from the analysis were the following variables: sex, household crowding index and physical activity. Anxiety partially mediated the association between child abuse and pain (indirect effect: Beta = 0.20; Boot SE = 0.03; Boot CI 0.14; 0.27). Higher child abuse was significantly associated with more anxiety and directly associated with more pain. Finally, higher anxiety was significantly associated with more pain (Fig. 1). The overall model R2 of 0.201, indicates that 20.1% of the variance in pain is accounted for by anxiety (medium effect size). The effect ratio value was 0.203/0.629 = 0.323 [95% CI 0.322; 0.326].
(a) Relation between child abuse and anxiety (R2 = .094); (b) Relation between anxiety and pain (R2 = .382); (c) Total effect of child abuse on pain (R2 = .201); (c’) Direct effect of child abuse on pain. Numbers are displayed as regression coefficients (standard error). ***p < 0.001.
Discussion
The aim of the study was to explore the mediating effect of anxiety in the relationship between child abuse and pain among a sample of Lebanese adults. Anxiety was found to partially mediate the relationship between child abuse and chronic pain. Higher levels of child abuse were significantly linked to higher anxiety and directly associated with greater pain. Additionally, higher anxiety was associated with more pain.
Child abuse and anxiety
Our study results demonstrated that higher exposure to child maltreatment was significantly correlated with aspects of anxiety; findings concurrent with previous evidence36,51,52,53,54. In a Lebanese study conducted on 1810 adolescents to evaluate the association between anxiety and child physical, sexual and psychological abuse, results showed psychological abuse to be a strong determinant of higher anxiety levels in adolescents51. Focusing on adult outcomes, a British cohort study found that a history of child abuse was significantly associated with higher odds of anxiety and depression in adults, which in turn mediated the development of other comorbid conditions53,54. Specifically, social anxiety emerged as the most prominent form of anxiety related to many forms of childhood abuse, as emphasized in a recent meta-analysis that reviewed studies published up to October 2021 across five databases36. In this meta-analysis, emotional abuse was found to be the most significant form of abuse tied with the emergence of social anxiety, while physical and sexual abuse showed milder but still significant effects on psychosocial outcomes36, reinforcing findings from previous studies14,51. Parallel to these outcomes, another meta-analysis conducted across three databases between 2002 and 2012, concluded that adults exposed to childhood physical and sexual abuse were associated with high levels of later anxiety, distress and depression12, suggesting that the psychological consequences of such abuse may persist well into adulthood without a defined time frame for onset. Another article that analyzed the findings of a two-decade longitudinal study about the repercussions of child maltreatment in later life, showed that both emotional abuse and neglect were significantly linked to anxiety and other cognitive and psychosocial derangements14. A reason for the development of the apparent disordered manifestations of child maltreatment may be expressed by the underlying neurobiological consequences of childhood abuse. One study elucidated that the fundamental role of the Hypothalamic–Pituitary–Adrenal (HPA) axis in the regulation of the biological pathways of early life stress may be altered, leading to the emergence of psychiatric disorders and their perpetuation in adult life55. Moreover, a genetic approach was observed to have a positive correlation between the HPA-axis related genes and the drawbacks of child abuse. The presence of specific genes augmented the likelihood of experiencing psychosocial disturbances56.
Anxiety and pain
Our findings demonstrate that more anxiety is strongly linked to higher pain in adults, with anxiety accounting for 20.1% of the variance in pain- reflecting a moderate effect, consistent with a previous meta-analysis results 13 that unveiled a moderate connection between anxiety and pain. This interrelation might be explained by certain brain processing mechanisms reflecting a significant dysregulation of certain brain areas57,58 leading to a perpetual aggravation of the interplay between those two components59. Another cohort study in concordance with our findings showed that accentuation of symptoms of anxiety and/or depression were tightly related to an elevation in pain levels60, a stable effect over time. However, even after remission of anxiety and/or depression, the pain magnitude described was still higher compared to mentally healthy individuals on the long run. This association has been interpreted as part of a negative feedback loop, where chronic depression and anxiety increase pain perception, which in turn exacerbates anxiety and depression60. Similarly, a national longitudinal study conducted in the United States over a four-year period found a significant increase in anxiety levels among older adults experiencing chronic pain61. This association would explain a wider observance of the interplay between the two entities, reflecting that pain might intensify anxiety levels, forming a self-perpetuating cycle where each component amplifies the other. This relationship was corroborated by a recent study carried out on a sample of 1794 adults that demonstrated increased levels of anxiety and depression with increased pain related to childhood maltreatment15. To address this matter, the use of antipsychotics could be beneficial in preventing the evolution of anxiety, thus diminishing the magnitude of pain perception62. Also, one study endorses the use of analgesics and appropriate interventions to restrict the occurrence of pain, which is thought to be an intensifying factor for anxiety60. While combining the effects of analgesics and antipsychotics might modify the dynamics related to anxiety and chronic pain, further studies are needed to verify the nature of the outcome.
Lastly, the consequences of child abuse are numerous, and regarding its impact on adult pain, research has found a concurrent relationship, where a rise in childhood maltreatment is linked to higher levels of pain in adulthood62,63,64. The latter relationship had been shown to be reinforced when implying anxiety resulting from childhood trauma as a mediating factor, likely through its amplifying effect on the dysregulation of brain pathways on the short- and long term, demonstrating the complex impact of psychological stressors on the occurrence of pain later in life13,58,59,61. Furthermore, the study showed that anxiety has a partial mediating effect on child abuse and pain, explained by its exacerbating effect on stress pathway dysregulation, significantly contributing to the pathophysiology of chronic pain in adulthood16,63,64,65,66. In instance, other comorbidities like depression also have a mediating effect, further emphasizing the complex interplay between child abuse, mental health, and chronic pain64,67,68,69,70.
Child abuse and pain
The findings of this study revealed a significant association between higher child abuse and higher pain scores in adulthood, aligning with the results of previous research62, which demonstrated that physical or emotional child abuse and early life stressors can result in neurobiological changes, including alterations to the HPA axis that regulates the stress response63. This dysregulation contributes to behavioral disturbances, central pain sensitization, and increased pain perception. Such mechanisms are often linked to comorbid conditions in adulthood, including fibromyalgia and migraines63,71,72. In addition, the socio-economic conditions and cultural perceptions prevalent in Lebanese and Arab societies often normalize child abuse or violence as an acceptable parenting strategy, such as corporal punishment, to enforce discipline within families61,62,65,72,73,74. Research has shown that children who grow up in low-income households are more likely to act violently61,62. Aggressive inclinations can be exacerbated by the stress and challenges of poverty, including restricted access to resources and ongoing financial instability. Parents in these situations often feel overwhelmed and turn to physical punishment as a disciplinary approach, believing it to be the most effective way to establish rules and guarantee their children behave appropriately62,72,73. This is seen in certain cultures, such as the Lebanese one, where corporal punishment is still a frequent and widely accepted practice in many households. However, children who get physical punishment are more likely to face mental health problems, such as chronic anxiety, and personality disorders62,72,73,74. Children could have trouble controlling their emotions and interacting with others. Lastly, depression is another significant outcome for children exposed to physical punishment, as they may internalize feelings of worthlessness and helplessness, leading to emotional distress and long-term mental health damage73,74. Moreover, these cultural attitudes, added to a decline in quality of life and stressors, serve as triggers for pain32, as they contribute to sustained stress pathway activation and heightened pain sensitivity63,75.
Clinical implications
Cognitive behavioral therapy (CBT) is an effective intervention for addressing the psychological impact of child abuse by helping individuals reframe negative thought patterns and develop healthier coping strategies76,77,78. It is widely used in Lebanon, and has shown effectiveness in improving outcomes related to insomnia, anxiety and depression79,80. The use of CBT in primary care patients has indicated a better outcome for treating patients with anxiety and depression79,80. It reduces anxiety, pain pathways dysregulation, and improves emotional and physical well-being76,77,78,81. Also, the incorporation of the mindfulness-based CBT for child abuse can increase the outcomes of the treatment by alleviating anxiety and cognitive triggers that exacerbate pain77,78,81,82. Moreover, educating the public about children’s rights and protection is essential and can be achieved through social media, local programs, and schools. This can help prevent child abuse and enhance their overall protection81. Lastly, family therapy could play a crucial role, as intrafamilial stressors often serve as triggers for child abuse, which can lead to anxiety and other comorbidities in adulthood, ultimately contributing to physical pain.
Limitations
The study has several limitations:
-
1)
Design limitations (cross-sectional design). The cross-sectional design restricts the ability to infer causality, as exposures and outcomes were assessed simultaneously. This limits conclusions about temporal ordering and directionality of observed associations.
-
2)
Information bias. Data were collected through self-administered questionnaires, which may be subject to misinterpretation or recall bias. Given the sensitive nature of the topic, social desirability bias may have influenced responses, potentially leading to underreporting or misclassification. The direction of this bias is uncertain, and while likely moderate, it may have affected the accuracy of the estimated associations.
-
3)
Selection bias. The use of a snowball sampling approach likely resulted in a non-random sample with unknown participation and refusal rates. This method may have introduced systematic differences between the study sample and the broader target population, particularly with respect to gender and marital status. Such differences may bias associations if the over- or under-represented groups differ on key study variables.
-
4)
Generalizability and effect modification. Participation was voluntary and may have attracted individuals with specific experiences or characteristics, particularly due to the sensitive nature of the study. This self-selection, combined with non-random sampling, limits the generalizability of findings. Additionally, interaction effects between sociodemographic variables and key exposures may vary across populations, further restricting external validity.
-
5)
Unmeasured confounding and variable selection. While the analysis adjusted for age, marital status, and socioeconomic status, other potential confounders—such as early-life socioeconomic conditions, education level, family dynamics, and prior mental health—were not included. Moreover, covariate selection was based on a liberal p-value threshold (< 0.25) in bivariate analyses, which may have increased the risk of including non-confounding variables or excluding relevant ones. Although the resulting bias is likely small, this approach may affect the robustness of multivariable estimates.
Conclusion
Child abuse is a serious topic that is more frequent nowadays in its different types. It is potentially linked to long-term consequences that may be both psychological and physical, including chronic pain in adulthood. This relationship should be examined in the scope of longitudinal studies to establish causality. Children often develop anxiety, depression and other comorbidities that may mediate the development of pain through different pathways. Additional investigations of child abuse and pain in adulthood should improve the comprehension of these different pathways, which may lead to the treatment or prevention of pain-particularly by considering the mediating role of anxiety. Future studies should explore other potential mediators that may contribute to the development of pain.
Data availability
Because of ethical committee constraints, none of the data collected or analyzed during this study are publicly available. However, the corresponding authors may make the data available upon reasonable request.
References
Dahlhamer, J. et al. Prevalence of chronic pain and high-impact chronic pain among adults—United States, 2016. MMWR Morb. Mortal. Wkly. Rep. 67 (36), 1001–1006. https://doi.org/10.15585/mmwr.mm6736a2 (2018).
Moreno-Ligero, M., Moral-Munoz, J. A., Salazar, A. & Failde, I. mHealth intervention for improving pain, quality of life, and functional disability in patients with chronic pain: Systematic review. JMIR Mhealth Uhealth 11, e40844. https://doi.org/10.2196/40844 (2023).
Dydyk, A. M. & Conermann, T. Chronic pain. In StatPearls (eds Dydyk, A. M. & Conermann, T.) (StatPearls Publishing, 2025).
World Health Organization. Child maltreatment. (accessed 16 August 2024); https://www.who.int/news-room/fact-sheets/detail/child-maltreatment
Rikard, S. M., Strahan, A. E., Schmit, K. M. & Guy, G. P. Chronic pain among adults—United States, 2019–2021. MMWR Morb. Mortal. Wkly. Rep. 72 (15), 379–385. https://doi.org/10.15585/mmwr.mm7215a1 (2023).
Fayaz, A., Croft, P., Langford, R. M., Donaldson, L. J. & Jones, G. T. Prevalence of chronic pain in the UK: A systematic review and meta-analysis of population studies. BMJ Open 6 (6), e010364. https://doi.org/10.1136/bmjopen-2015-010364 (2016).
Finkelhor, D., Turner, H. A., Shattuck, A. & Hamby, S. L. Prevalence of childhood exposure to violence, crime, and abuse: Results from the national survey of children’s exposure to violence. JAMA Pediatr. 169 (8), 746–754. https://doi.org/10.1001/jamapediatrics.2015.0676 (2015).
Preventing child maltreatment: A guide to taking action and generating evidence. World Health Organization (2006). Preventing child maltreatment: A guide to taking action and generating evidence. (accessed 25 March 2025); https://iris.who.int/bitstream/handle/10665/43499/9241594365_eng.pdf;sequence=1
Lippard, E. T. C. & Nemeroff, C. B. The devastating clinical consequences of child abuse and neglect: Increased disease vulnerability and poor treatment response in mood disorders. Am. J. Psychiatr. 177 (1), 20–36. https://doi.org/10.1176/appi.ajp.2019.19010020 (2020).
Huh, H. J., Kim, K. H., Lee, H. & Chae, J. The relationship between childhood trauma and the severity of adulthood depression and anxiety symptoms in a clinical sample: The mediating role of cognitive emotion regulation strategies. J. Affect. Disord. 213, 44–50. https://doi.org/10.1016/j.jad.2017.02.009 (2017).
Lindert, J. et al. Sexual and physical abuse in childhood is associated with depression and anxiety over the life course: Systematic review and meta-analysis. Int. J. Public Health 59 (2), 359–372. https://doi.org/10.1007/s00038-013-0519-5 (2014).
Strathearn, L. et al. Long-term cognitive, psychological, and health outcomes associated with child abuse and neglect. Pediatrics 146 (4), e20200438. https://doi.org/10.1542/peds.2020-0438 (2020).
Gerrits, M. M. J. G., van Marwijk, H. W. J., van Oppen, P., van der Horst, H. & Penninx, B. W. J. H. Longitudinal association between pain, and depression and anxiety over four years. J. Psychosom. Res. 78 (1), 64–70. https://doi.org/10.1016/j.jpsychores.2014.10.011 (2015).
Neigh, G. N., Gillespie, C. F. & Nemeroff, C. B. The neurobiological toll of child abuse and neglect. Trauma Violence Abuse 10 (4), 389–410. https://doi.org/10.1177/1524838009339758 (2009).
Baagil, H., Baagil, H. & Gerbershagen, M. U. Preoperative anxiety impact on anesthetic and analgesic use. Medicina (Kaunas) 59 (12), 2069. https://doi.org/10.3390/medicina59122069 (2023).
Ellsberg, M., Jansen, H. A. F. M., Heise, L., Watts, C. H. & Garcia-Moreno, C. Intimate partner violence and women’s physical and mental health in the WHO multi-country study on women’s health and domestic violence: An observational study. Lancet 371 (9619), 1165–1172. https://doi.org/10.1016/S0140-6736(08)60522-X (2008).
Lee, C. & White, H. R. Effects of childhood maltreatment on violent injuries and premature death during young adulthood among urban high-risk men. Arch. Pediatr. Adolesc. Med. 166 (9), 814–820. https://doi.org/10.1001/archpediatrics.2012.244 (2012).
Brown, J., Cohen, P., Johnson, J. G. & Smailes, E. M. Childhood abuse and neglect: Specificity of effects on adolescent and young adult depression and suicidality. J. Am. Acad. Child Adolesc. Psychiatr. 38 (12), 1490–1496. https://doi.org/10.1097/00004583-199912000-00009 (1999).
Davis, D. A., Luecken, L. J. & Zautra, A. J. Are reports of childhood abuse related to the experience of chronic pain in adulthood? A meta-analytic review of the literature. Front. Pain Res. (Lausanne) 21 (5), 398–405. https://doi.org/10.1097/01.ajp.0000149795.08746.31 (2005).
American Psychiatric Association (2013). Diagnostic and Statistical Manual of Mental Disorders (Fifth ed.). Arlington, VA: American Psychiatric Publishing.
World health organization. anxiety disorders. World Health Organization. Anxiety Disorders. World Health Organization. (accessed 16 August 2024); https://www.who.int/news-room/fact-sheets/detail/anxiety-disorders.
Institute for health metrics and evaluation. GBD results. (accessed 25 March 2025); https://www.healthdata.org/data-tools-practices/interactive-visuals/gbd-results.
Mullins, P. M., Yong, R. J. & Bhattacharyya, N. Associations between chronic pain, anxiety, and depression among adults in the United States. Pain Pract. 23 (6), 589–594. https://doi.org/10.1111/papr.13220 (2023).
Stanley, I. H. et al. Anxiety sensitivity and suicidal ideation/suicide risk: A meta-analysis. J. Consult. Clin. Psychol. 86 (11), 946–960. https://doi.org/10.1037/ccp0000342 (2018).
Vongmany, J., Hickman, L. D., Lewis, J., Newton, P. J. & Phillips, J. L. Anxiety in chronic heart failure and the risk of increased hospitalisations and mortality: A systematic review. Eur. J. Cardiovasc. Nurs. 15 (7), 478–485. https://doi.org/10.1177/1474515116635923 (2016).
Arango-Dávila, C. A. & Rincón-Hoyos, H. G. Depressive disorder, anxiety disorder and chronic pain: Multiple manifestations of a common clinical and pathophysiological core. Rev. Colomb. Psiquiatr. (Engl. Ed.) 47 (1), 46–55. https://doi.org/10.1016/j.rcp.2016.10.007 (2018).
Tang, J. & Gibson, S. J. A psychophysical evaluation of the relationship between trait anxiety, pain perception, and induced state anxiety. J. Pain 6 (9), 612–619. https://doi.org/10.1016/j.jpain.2005.03.009 (2005).
Choi, J. Y. & Oh, K. J. Cumulative childhood trauma and psychological maladjustment of sexually abused children in Korea: Mediating effects of emotion regulation. Child Abuse Negl. 38 (2), 296–303. https://doi.org/10.1016/j.chiabu.2013.09.009 (2014).
Wright, M. O., Crawford, E. & Del Castillo, D. Childhood emotional maltreatment and later psychological distress among college students: The mediating role of maladaptive schemas. Child Abuse Negl. 33 (1), 59–68. https://doi.org/10.1016/j.chiabu.2008.12.007 (2009).
Whipple, E. E. & Richey, C. A. Crossing the line from physical discipline to child abuse: How much is too much?. Child Abuse Negl. 21 (5), 431–444. https://doi.org/10.1016/s0145-2134(97)00004-5 (1997).
Bakhos J.J et al. Child Maltreatment in Lebanon: Prevalence, Screening and Upgrade of ESCAPE. World Journal of Public Health. 7 (1), 14–21. https://doi.org/10.11648/j.wjph.20220701.13 (2022).
Itani, L., Haddad, Y. C., Fayyad, J., Karam, A. & Karam, E. Childhood adversities and traumata in lebanon: A national study. Clin. Pract. Epidemiol. Ment. Health 10, 116–125. https://doi.org/10.2174/1745017901410010116 (2014).
Christian, C. W. The evaluation of suspected child physical abuse. Pediatrics 135 (5), 1337. https://doi.org/10.1542/peds.2015-0356 (2015).
Qasem, F. S., Mustafa, A. A., Kazem, N. A. & Shah, N. M. Attitudes of kuwaiti parents toward physical punishment of children. Child Abuse Negl. 22 (12), 1189–1202. https://doi.org/10.1016/s0145-2134(98)00097-0 (1998).
Tsang, A. et al. Common chronic pain conditions in developed and developing countries: Gender and age differences and comorbidity with depression-anxiety disorders. J. Pain 9 (10), 883–891. https://doi.org/10.1016/j.jpain.2008.05.005 (2008).
Liu, J., Deng, J., Zhang, H. & Tang, X. The relationship between child maltreatment and social anxiety: A meta-analysis. J. Affect. Disord. 329, 157–167. https://doi.org/10.1016/j.jad.2023.02.081 (2023).
Cant, R. L., O’Donnell, M., Sims, S. & Harries, M. Overcrowded housing: One of a constellation of vulnerabilities for child sexual abuse. Child Abuse Negl. 93, 239–248. https://doi.org/10.1016/j.chiabu.2019.05.010 (2019).
Gao, Y., Mi, X., Wang, Y., Zou, S. & Zhou, H. Association between household crowding and violent discipline and neglect of children: Analysis of multiple indicator cluster surveys in 26 low- and middle-income countries. Int. J. Environ. Res. Public Health 18 (4), 1685. https://doi.org/10.3390/ijerph18041685 (2021).
Ryu, S. & Gao, Z. The moderating effects of physical activity on the relationships between child maltreatment and health outcomes among korean adolescents: A secondary analysis of the 2020 Korean children and youth rights survey. J. Clin. Med. 12 (14), 4574. https://doi.org/10.3390/jcm12144574 (2023).
Handcock, M. S. & Gile, K. J. Comment: On the concept of snowball sampling. Soc. Methodol. 41 (1), 367–371. https://doi.org/10.1111/j.1467-9531.2011.01243.x (2011).
Fritz, M. S. & Mackinnon, D. P. Required sample size to detect the mediated effect. Psychol. Sci. 18 (3), 233–239. https://doi.org/10.1111/j.1467-9280.2007.01882.x (2007).
Melki, I. S., Beydoun, H. A., Khogali, M., Tamim, H. & Yunis, K. A. Household crowding index: A correlate of socioeconomic status and inter-pregnancy spacing in an urban setting. J. Epidemiol. Commun. Health 58 (6), 476–480. https://doi.org/10.1136/jech.2003.012690 (2004).
Assaf, M. et al. Arabic translation and psychometric testing of the physical activity index (PAI). Res. Square https://doi.org/10.21203/rs.3.rs-5945662/v1 (2025).
Melzack, R. The short-form McGill pain questionnaire. Pain 30 (2), 191–197. https://doi.org/10.1016/0304-3959(87)91074-8 (1987).
Terkawi, A. S. et al. Development and validation of arabic version of the short-form McGill pain questionnaire. Saudi J. Anaesth. 11 (1), S2–S10. https://doi.org/10.4103/sja.SJA_42_17 (2017).
Spitzer, R. L., Kroenke, K., Williams, J. B. W. & Löwe, B. A brief measure for assessing generalized anxiety disorder: The GAD-7. Arch. Intern Med. 166 (10), 1092–1097. https://doi.org/10.1001/archinte.166.10.1092 (2006).
Sawaya, H., Atoui, M., Hamadeh, A., Zeinoun, P. & Nahas, Z. Adaptation and initial validation of the patient health questionnaire - 9 (PHQ-9) and the generalized anxiety disorder - 7 questionnaire (GAD-7) in an arabic speaking lebanese psychiatric outpatient sample. Psychiatr. Res. 239, 245–252. https://doi.org/10.1016/j.psychres.2016.03.030 (2016).
Fekih-Romdhane, F. et al. Development and validation of a shortened version of the child abuse self report scale (CASRS-12) in the arabic language. Child Adolesc. Psychiatr. Ment. Health 16 (1), 100. https://doi.org/10.1186/s13034-022-00533-3 (2022).
Bursac, Z., Gauss, C. H., Williams, D. K. & Hosmer, D. W. Purposeful selection of variables in logistic regression. Sour. Code Biol. Med. 3, 17. https://doi.org/10.1186/1751-0473-3-17 (2008).
Cohen, J. Statistical Power Analysis for the Behavioral Sciences (Routledge, 2013).
Merhy, G., Azzi, V., Salameh, P., Obeid, S. & Hallit, S. Anxiety among lebanese adolescents: Scale validation and correlates. BMC Pediatr. 21 (1), 288. https://doi.org/10.1186/s12887-021-02763-4 (2021).
Haddad, C. et al. Prevalence and associated factors of social anxiety among lebanese adolescents. Prim. Care Companion CNS Disord. 24 (3), 21m03061. https://doi.org/10.4088/PCC.21m03061 (2022).
Berber Çelik, Ç. & Odacı, H. Does child abuse have an impact on self-esteem, depression, anxiety and stress conditions of individuals?. Int. J. Soc. Psychiatr. 66 (2), 171–178. https://doi.org/10.1177/0020764019894618 (2020).
Sarkar, N., Zainal, N. H. & Newman, M. G. Self-esteem mediates child abuse predicting adulthood anxiety, depression, and substance use symptoms 18 years later. J. Affect. Disord. 365, 542–552. https://doi.org/10.1016/j.jad.2024.08.107 (2024).
Cao, C., Chen, M., Yang, S., Xu, Y. & Gu, J. Childhood maltreatment, multilocus HPA-axis genetic variation and adolescent comorbidity profiles of depressive and anxiety symptoms. Child Abuse Negl. 149, 106683. https://doi.org/10.1016/j.chiabu.2024.106683 (2024).
Dalechek, D. E., Caes, L., McIntosh, G. & Whittaker, A. C. Anxiety, history of childhood adversity, and experiencing chronic pain in adulthood: A systematic literature review and meta-analysis. Eur. J. Pain 28 (6), 867–885. https://doi.org/10.1002/ejp.2232 (2024).
Campbell, C. M. & Edwards, R. R. Mind-body interactions in pain: The neurophysiology of anxious and catastrophic pain-related thoughts. Transl. Res. 153 (3), 97–101. https://doi.org/10.1016/j.trsl.2008.12.002 (2009).
Mutschler, I., Ball, T., Wankerl, J. & Strigo, I. A. Pain and emotion in the insular cortex: Evidence for functional reorganization in major depression. Neurosci. Lett. 520 (2), 204–209. https://doi.org/10.1016/j.neulet.2012.03.095 (2012).
Borsook, D., Sava, S. & Becerra, L. The pain imaging revolution: Advancing pain into the 21st century. Neuroscientist. 16 (2), 171–185. https://doi.org/10.1177/1073858409349902 (2010).
Bierman, A. & Lee, Y. Chronic pain and psychological distress among older adults: A national longitudinal study. Res. Aging 40 (5), 432–455. https://doi.org/10.1177/0164027517704970 (2018).
Craner, J. R., Lake, E. S., Barr, A. C., Kirby, K. E. & O’Neill, M. Childhood adversity among adults with chronic pain: Prevalence and association with pain-related outcomes. Clin. J. Pain 38 (9), 551–561. https://doi.org/10.1097/AJP.0000000000001054 (2022).
El Bcheraoui, C., Kouriye, H. & Adib, S. M. Physical and verbal/emotional abuse of schoolchildren, lebanon, 2009. East. Mediterr. Health J. 18 (10), 1011–1020. https://doi.org/10.26719/2012.18.10.1011 (2012).
Mills, S. E. E., Nicolson, K. P. & Smith, B. H. Chronic pain: A review of its epidemiology and associated factors in population-based studies. Br. J. Anaesth. 123 (2), e273–e283. https://doi.org/10.1016/j.bja.2019.03.023 (2019).
Nicolson, K. P., Mills, S. E. E., Senaratne, D. N. S., Colvin, L. A. & Smith, B. H. What is the association between childhood adversity and subsequent chronic pain in adulthood? A systematic review. BJA Open 6, 100139. https://doi.org/10.1016/j.bjao.2023.100139 (2023).
Al-Fayez, G. A., Ohaeri, J. U. & Gado, O. M. Prevalence of physical, psychological, and sexual abuse among a nationwide sample of arab high school students: Association with family characteristics, anxiety, depression, self-esteem, and quality of life. Soc. Psychiatr. Psychiatr. Epidemiol. 47 (1), 53–66. https://doi.org/10.1007/s00127-010-0311-2 (2012).
Sachs-Ericsson, N., Kendall-Tackett, K. & Hernandez, A. Childhood abuse, chronic pain, and depression in the national comorbidity survey. Child Abuse Negl. 31 (5), 531–547. https://doi.org/10.1016/j.chiabu.2006.12.007 (2007).
Fayyad, J. A., Farah, L., Cassir, Y., Salamoun, M. M. & Karam, E. G. Dissemination of an evidence-based intervention to parents of children with behavioral problems in a developing country. Eur. Child Adolesc. Psychiatr. 19 (8), 629–636. https://doi.org/10.1007/s00787-010-0099-3 (2010).
Jordan, K. P., Thomas, E., Peat, G., Wilkie, R. & Croft, P. Social risks for disabling pain in older people: A prospective study of individual and area characteristics. Pain 137 (3), 652–661. https://doi.org/10.1016/j.pain.2008.02.030 (2008).
Macfarlane, G. J. The epidemiology of chronic pain. Pain 157 (10), 2158–2159. https://doi.org/10.1097/j.pain.0000000000000676 (2016).
Nelson, S., Simons, L. E. & Logan, D. The incidence of adverse childhood experiences (ACEs) and their association with pain-related and psychosocial impairment in youth with chronic pain. Clin. J. Pain 34 (5), 402–408. https://doi.org/10.1097/AJP.0000000000000549 (2018).
Raphael, K. G., Widom, C. S. & Lange, G. Childhood victimization and pain in adulthood: A prospective investigation. Pain 92 (1–2), 283–293. https://doi.org/10.1016/s0304-3959(01)00270-6 (2001).
Ibrahim, N. K., Jalali, E. A., Al-Ahmadi, J. R. & Al-Bar, A. A. Prevalence, risk factors and outcome of childhood abuse reported by female university students in Jeddah. J. Egypt Public Health Assoc. 83 (5–6), 329–351 (2008).
Usta, J., Farver, J. M. & Danachi, D. Child maltreatment: The Lebanese children’s experiences. Child Care Health Dev. 39 (2), 228–236. https://doi.org/10.1111/j.1365-2214.2011.01359.x (2013).
Afifi, T. O., Fortier, J., Sareen, J. & Taillieu, T. Associations of harsh physical punishment and child maltreatment in childhood with antisocial behaviors in adulthood. JAMA Netw. Open 2 (1), e187374. https://doi.org/10.1001/jamanetworkopen.2018.7374 (2019).
Youssef, R. M., Attia, M. S. & Kamel, M. I. Children experiencing violence. I: Parental use of corporal punishment. Child Abuse Negl. 22 (10), 959–973. https://doi.org/10.1016/s0145-2134(98)00077-5 (1998).
Xian-Yu, C. et al. Cognitive behavioral therapy for children and adolescents with post-traumatic stress disorder: Meta-analysis. J. Affect. Disord. 308, 502–511. https://doi.org/10.1016/j.jad.2022.04.111 (2022).
Muñoz-Solomando, A., Kendall, T. & Whittington, C. J. Cognitive behavioural therapy for children and adolescents. Curr. Opin. Psychiatr. 21 (4), 332–337. https://doi.org/10.1097/YCO.0b013e328305097c (2008).
Cuijpers, P. et al. A meta-analysis of cognitive-behavioural therapy for adult depression, alone and in comparison with other treatments. Can. J. Psychiatr. 58 (7), 376–385. https://doi.org/10.1177/070674371305800702 (2013).
Geagea, L. et al. Assessing cognitive behavioral therapy for insomnia in individuals with cannabis use disorder utilizing actigraphy and serum biomarkers: A pilot study. Sleep Med. 100, 434–441. https://doi.org/10.1016/j.sleep.2022.09.017 (2022).
Khoury, B. & Ammar, J. Cognitive behavioral therapy for treatment of primary care patients presenting with psychological disorders. Libyan J. Med. 9 (1), 24186. https://doi.org/10.3402/ljm.v9.24186 (2014).
Alharbi, I. et al. A cross-sectional study on public awareness about child sexual abuse in Makkah, Saudi Arabia. Cureus 15 (2), e34931. https://doi.org/10.7759/cureus.34931 (2023).
Bitar, Z., Rogoza, R., Hallit, S. & Obeid, S. Mindfulness among lebanese university students and its indirect effect between mental health and wellbeing. BMC Psychol. 11 (1), 114. https://doi.org/10.1186/s40359-023-01155-w (2023).
Acknowledgements
The authors would like to thank all participants.
Author information
Authors and Affiliations
Contributions
FFR, SH and SO designed the study; EK and GC drafted the manuscript; SH carried out the analysis and interpreted the results; FS and MD collected the data. DM and SEK reviewed the paper for intellectual content; all authors reviewed the final manuscript and gave their consent.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The Lebanese International University’s School of Pharmacy ethics committee granted this study ethics permission (Reference number: 2024ERC-023-LIUSOP). When filling out the online form, each participant provided written informed consent. All methods were performed in accordance with the relevant guidelines and regulations (in accordance with the Declaration of Helsinki).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Kesrewani, E., Chammas, G., Malaeb, D. et al. The mediating role of anxiety between child abuse and pain among a sample of Lebanese adults. Sci Rep 15, 16559 (2025). https://doi.org/10.1038/s41598-025-01689-6
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-01689-6