Abstract
Childhood exposure to filariasis can confer significant protection against diabetes which is called as “Metabolic Hygiene Hypothesis”. However, the effect of diabetes on anti-filarial immunity is not much studied. In the present study, the role of diabetes on systemic anti-filarial immunity was elucidated. Plasma levels of innate immune cytokines, adaptive immune cytokines, chemokines, hormones and growth factors were quantified by ELISA; Lipid and protein peroxidation and nitrite levels were quantified by spectrophotometry; Peripheral Tregs and exhausted T-cells were quantified by flowcytometry; FoxP3 expression was quantified by qRT-PCR. Anti-filarial immunity was significantly associated with elevated levels of TNF-α, IL-6, IL-1β, IL-10, IL-1Ra, DEF-A1, IL-12, IFN-γ, IL-2, IL-33, IL-9, IL-23, IL-17, IL-8, IP-10, SDF-1, MCP-1 and RANTES and decreased levels of IL-27, IL-4, leptin and FGF-21. Lipid peroxidation, nitrite levels and exhausted T cells were also increased. Chronic diabetes significantly reduced IL-1β, IL-1Ra, DEF-A1 and IL-8 and lipid peroxidation, and increased VEGF levels in DM-LF group. Overall, diabetes was found to downregulate a few critical innate immune components, of anti-filarial immunity, that can promote chronic pathology in LF + subjects.
Similar content being viewed by others
Introduction
Filarial infections in humans as well as animals include lymphatic filariasis, onchocerciasis, loiasis, and mansonellosis1. Lymphatic filariasis is caused by Wuchereria bancrofti, Brugia malayi, and Brugia timori, with W. bancrofti accounting for more than 90% of such infections2. The most prominent pathological manifestations of lymphatic filariasis (LF) are mediated by immune responses against adult worms and infective stage larvae3, leading to lymphedema and hydrocele. Recent epidemiological studies have shown an inverse relationship between the decreasing prevalence of helminth infections and the increasing prevalence of metabolic diseases (“Metabolic Hygiene Hypothesis”)4. Previous research conducted by our lab in the South Indian population has demonstrated a lower prevalence of filariasis among both type-13 and type-2 diabetes patients5. However, the effect of chronic diabetes, on anti-filarial immunity is not clearly known. Diabetes in general, weakens the immune system and increases the susceptibility to infections6. Few studies have shown increased morbidity under conditions of diabetes-filariasis co-morbidity7,8,9. The immune mechanism behind this clinical condition is not clearly known.
Both T and B cells, along with innate immune cells, largely contribute to anti-filarial immunity. T-cell mediated immune responses, during filariasis, depends largely on the phase of the infection: 1. In the acute phase, it is predominantly Th2 (Interleukin-4 (IL-4), IL-5 and IL-13) response10, 2. In the chronic phase, the Th2 response becomes a “modified Th2 response” with T regulatory cells (Tregs) secreting IL-10 and Transforming Growth Factor β (TGF-β)) playing a more prominent role and 3. In the chronic pathology phase, a drastic shift from “modified Th2” to “Th1/Th17” (Interferon-γ (IFN-γ), IL-2 and IL-17) response takes place (which happens only in those who develop lymphatic pathology11). Apart from cytokines, chemokines play an important role in immune cell recruitment and activation12. Indeed, productive worm containment is known to be tightly regulated by chemokines13. Chemokine dysregulation can shift the balance from protection to inflammation and pathology, in LF14. Redox stress is known to induce apoptosis in the filarial parasite and drugs which are capable of inducing redox stress have shown significant anti-filarial activity, at least under in vitro conditions15. However, the effect of systemic redox stress, on anti-filarial immunity is not known. Thus, the anti-filarial immunity in humans is complex and multifaceted.
It is therefore evident that the relationship between diabetes and filariasis is bi-directional. While childhood exposure to filariasis can confer protection against diabetes16, the effect of diabetes on anti-filarial immunity is not much studied. A complex redox-immune-endocrine network is believed to orchestrate the anti-filarial immunity. The effect of diabetes on this network is not known. In the present study, we looked at the effect of diabetes on the circulating levels of cytokines, chemokines, hormones, growth factors, redox markers, peripheral Tregs and exhausted T cells, in LF + subjects.
Results
Clinical characteristics of the study group
S. Table 1 shows the clinical and biochemical characteristics of the study groups. Compared to the control groups (Control and LF), the Diabetes mellitus (DM) groups (DM and DM-LF) had significantly elevated glycemic parameters (Fasting plasma glucose, Postprandial glucose level and glycated Haemoglobin (HbA1c)) and serum triglyceride levels.
Effect of diabetes on the circulating levels of innate immune makers in DM-LF subjects
Figure 1 shows the circulating levels of pro- (Tumour Necrosis Factor (TNF-α), IL-6 and IL-1β) and anti-(IL-10, IL-1Ra, TGF-β and IL-27) inflammatory cytokines, type-1 interferon (IFN-β) and defensin (DEF-A1), in the plasma of the study subjects. The levels of TNF-α, IL-6, IL-1β, IL-10, IL-1Ra, IFN-β and DEF-A1 were significantly higher, while that of IL-27 was significantly lower, in both LF and DM-LF, compared to Control and DM groups, respectively. Interestingly, IL-1β, IL-1Ra and DEF-A1 were the only three markers which were significantly lower in the DM-LF group, compared to the LF group.
Circulating levels of innate immune cytokines in DM-LF subjects. The circulating levels of pro- and anti-inflammatory cytokines, type-1 interferons and defensins in LF + subjects were quantified by ELISA. Bar graph showing the circulating levels of TNF-α (a), IL-6 (b), IL-1β (c), IL-10 (d), IL-1Ra (e), TGF-β (f), IL-27 (g), IFN-β (h), DEF-A1 (i) in the plasma of control, LF, DM and DM-LF subjects. Statistical significance was determined by non-parametric Mann–Whitney U test and p < 0.05 was considered significant. *p < 0.05; **p < 0.01; ***p < 0.001.
Effect of diabetes on the circulating levels of adaptive immune cytokines in DM-LF subjects
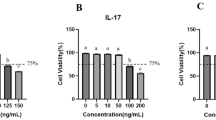
Figure 2 shows the circulating levels of adaptive immune cytokines (Th1-IL-12, IFN-γ, IL-2; Th17-IL-23, IL-17; Th9- IL-9; Th2- IL-33 and IL-4), in the plasma of the study subjects. The plasma levels of IL-12, IFN-γ, IL-2, IL-23, IL-17, IL-9 and IL-33 were significantly higher, while that of IL-4 was significantly lower, in both LF and DM-LF, compared to control and DM groups, respectively.
Circulating levels of adaptive immune cytokines in DM-LF subjects. The circulating levels of cytokines in LF + subjects were quantified by ELISA. Bar graph showing the circulating levels of IL-12 (a), IFN-γ (b), IL- 2 (c), IL-23 (d), IL-17 (e), IL-9 (f), IL-33 (g), IL-4 (h) in the plasma of control, LF, DM and DM-LF subjects. Statistical significance was determined by non-parametric Mann–Whitney U test and p < 0.05 was considered significant. *p < 0.05; **p < 0.01; ***p < 0.001.
Effect of diabetes on the circulating levels of chemokines in DM-LF subjects
Figure 3 shows the circulating plasma levels of chemokines (IL-8, IFN γ Induced Protein-10 (IP-10), Regulated upon Activation, Normal T cell Expressed and Secreted (RANTES), Monocyte Chemoattractant Protein-1 (MCP-1) and Stromal Cell Derived Factor-1 (SDF-1)) of the study subjects. The plasma levels of IL-8, IP-10, RANTES, MCP-1 and SDF-1 were significantly higher, in both LF and DM-LF, compared to control and DM groups, respectively. Interestingly, IL-8 was the only chemokine which was significantly reduced in DM-LF compared to LF group.
Circulating levels of chemokines in DM-LF subjects. The circulating levels of chemokines in LF + subjects were quantified by ELISA. Bar graph showing the circulating levels of IL-8 (a), IP-10 (b), SDF-1 (c), MCP-1 (d), RANTES (e) in the plasma of Control, LF, DM and DM-LF subjects. Statistical significance was determined by non-parametric Mann–Whitney U test and p < 0.05 was considered significant. *p < 0.05; **p < 0.01; ***p < 0.001.
Effect of diabetes on the circulating levels of hormones and growth factors in DM-LF subjects
Figure 4 shows the circulating levels of hormones (insulin, adiponectin and leptin) and growth factors (Fibroblast Growth Factor 21 (FGF-21) and Vascular Endothelial Growth Factor (VEGF)), in the plasma of the study subjects. The plasma levels of leptin and FGF-21 were significantly lower, in both LF and DM-LF, compared to control and DM groups, respectively. Interestingly VEGF was significantly higher only in DM-LF compared to the DM group.
Circulating levels of hormones and growth factors in DM-LF subjects. The circulating levels of hormones and growth factors in LF + subjects were quantified by ELISA. Bar graph showing the circulating levels of insulin (a), adiponectin (b), leptin (c), FGF-21 (d), VEGF (e) in the plasma of Control, LF, DM and DM-LF subjects. Statistical significance was determined by non-parametric Mann–Whitney U test and p < 0.05 was considered significant. *p < 0.05; **p < 0.01; ***p < 0.001.
Effect of diabetes on the stress parameters and reactive nitrate levels in LF + subjects
Figure 5 shows the plasma protein (PPO) and lipid peroxidation (LPO) and nitrate levels, of the study subjects. Lipid peroxidation and nitrate levels were found to be significantly higher, in both LF and DM-LF, compared to control and DM groups, respectively. Interestingly, lipid peroxidation was the only marker which was significantly lower in the DM-LF group, compared to the LF group.
Circulating levels of protein and lipid peroxidation and nitrates in DM-LF subjects. The plasma levels of redox parameters and nitrate in LF + subjects were quantified by colorimetric analysis. Bar graph showing the levels of Lipid peroxidation (a), Protein peroxidation (b), Nitrates (c) in the plasma of Control, LF, DM and DM-LF subjects. Statistical significance was determined by non-parametric Mann–Whitney U test and p < 0.05 was considered significant. *p < 0.05; **p < 0.01; ***p < 0.001.
Effect of diabetes on Tregs and exhausted T cells in LF + subjects
Figure 6 shows the percentage of peripheral Tregs and exhausted T cells along with the expression levels of Cytotoxic T Lymphocyte Antigen 4 (CTLA-4), Programmed Cell Death Protein 1 (PD-1) and FoxP3 (Forkhead box P3), in the study population. There was no significant difference in the percentage of peripheral Tregs between the groups. The percentage of exhausted T cells (CD3 + CD4 + CTLA4 + PD-1 +) was significantly higher, in both LF and DM-LF, compared to Control and DM groups, respectively. There was a significant increase in the expression of both CTLA-4 and PD-1 in, both LF and DM-LF, compared to the control and DM groups, respectively. Figure 6e shows the TLR and filarial antigen-induced expression of FoxP3, in the peripheral blood leukocyte cultures. There was no significant difference in the expression of FoxP3, between the groups.
Percentage of peripheral Tregs, exhausted T cells and FoxP3 expression in DMLF subjects. Peripheral Tregs and PD-1 + Th cells was quantified by flow cytometry and FoxP3 expression was quantified by qRT-PCR, respectively in LF + subjects. Bar graph showing peripheral Tregs (a), Exhausted T cells (b), CTLA4 + expression (c) and PD + expression (d) in exhausted Th cells. TLR and BmA induced expression of FoxP3 in LF and DM-LF (e). Statistical significance was determined by non-parametric Mann–Whitney U test and p < 0.05 was considered significant. *p < 0.05; **p < 0.01; ***p < 0.001.
Discussion
Previously, we reported a decrease in the prevalence of lymphatic filariasis among both type-14 and type-25 diabetes patients. This was basically due to LF- mediated immunomodulation, which quenches meta-inflammation16. Meta inflammation is the major etiological factor which drives metabolic diseases17. This phenomenon is now being recognized as the “metabolic hygiene hypothesis”17. While LF infection is known to confer protection against diabetes, the effect of chronic diabetes on LF infection has not been much explored. Previous clinical studies have shown increased morbidity due to LF in diabetes patients7,8,9. However, those studies have not deciphered the immunological mechanism involved. Towards this end, in the present study, the role of diabetes on systemic anti-filarial immunity was elucidated. It is important to note that anti-filarial immunity is complex and multifaceted and involves innate and adaptive immune cytokines and chemokines18. Recent studies have indicated that systemic redox stress, hormones and growth factors determine cytokine/chemokine secretion by immune cells and also determine immune cell exhaustion and Treg population19. This indicates the involvement of a complex redox-immune-endocrine network operating in anti-filarial immunity20. In the present study innate immune response was studied by quantifying the circulating levels of pro-inflammatory cytokines (TNF-α, IL-6 and IL-1β), anti-inflammatory cytokines (IL-10, IL-1Ra, TGF-β and IL-27), Type-1 interferon (IFN-β) and defensin (DEF-A1). Adaptive immune response was studied by quantifying the circulating levels of Th1 (IL-12, IFN-γ and IL-2), Th2 (IL-33 and IL-4), Th9 (IL-9) and Th17 (IL-23 and IL-17), cytokines. We also quantified the circulating levels of the chemokines (IL-8, IP-10, SDF-1, MCP-1 and RANTES), hormones (insulin, adiponectin and leptin), growth factors (FGF-21 and VEGF) and markers of systemic redox stress (LPO, PPO and nitrites). Finally, peripheral Tregs and exhausted T-cells were also quantified. Our major findings were: (1) Compared to LF, in the DM-LF+ group the circulating levels of IL-1β, IL-1Ra, DEF-A1 and IL-8 were reduced; (2) Compared to LF, in the DM-LF + subjects the circulating levels of insulin, adiponectin, leptin and FGF-21 were not affected however VEGF levels were augmented. (3) Compared to LF, Lipid peroxidation was reduced in the DM-LF + group; (4) In LF+ subjects, diabetes co-morbidity did not affect the expression of peripheral Tregs, exhausted T cells or FoxP3; (5) Compared to filariasis, diabetes seem to have very little effect on the immune parameters studied.
In the present study, it was found that LF infection significantly increased the circulating levels of TNF-α, IL-6, IL-1β, IL-10, IL-1Ra, IFN-β and DEF-A1 and reduced IL-27 levels. Co-morbidity with diabetes specifically reduced IL-1β and DEF-A1 levels. Pro-and anti-inflammatory cytokines, type-1 interferons and defensins together constitute the major component of the innate immune response against LF21. Among the various biomarkers quantified in this study, co-morbidity with diabetes specifically reduced the circulating levels of IL-1β, IL-1Ra and DEF-A1, in LF + subjects. This is in accordance with our previous study, wherein decreased levels of pro-inflammatory cytokines, in LF + diabetic subjects were seen5. While several reports associate pro-inflammatory cytokines with immunopathology, immunization with Brugia malayi adult worm antigens conferred significant protection against infection, in southern African mastomys and Mongolian gerbils and was associated with IL-1β mediated pro-inflammatory cytokine response22. Immunization of Mongolian gerbils with pro-inflammatory fraction of Brugia malayi antigenic extract (that stimulated the secretion of TNF-α, IL-1β and IL-6 from splenocytes) helped in the elimination of the worms. On the other hand, immunization with the anti-inflammatory fraction (that stimulated IL-10 secretion) facilitated the survival of the worms23. Recent studies have shown success in using bioactive macromolecules derived from helminth parasites for treating a variety of inflammatory disorders. Most of these molecules act by binding to innate immune receptors and induce the secretion of anti-inflammatory cytokines24. Secretion of defensins from neutrophils was needed for the rapid elimination of the parasitic Mansonella streptocerca infection, in the skin25. Previously, we have shown significantly reduced basal secretion of DEF-A1 in DM-LF subjects compared to LF subjects21. Thus, the reduced circulating levels of IL-1β, IL-1Ra and DEF-A1, seen in the DM-LF group, indicate impaired systemic innate immune defense mechanism against filariasis.
During the infection with Trichuris muris, a gastrointestinal nematode it was shown that both IL-1α and IL-1β are required for the development of Th2 immune response. Studies on the IL-1α and IL-1β knockout mice lacking either IL-1α or IL-1β were suseptible to persistent T. muris infection and show impaired antigen-specific Th2 responses. This shows the critical role of IL-1 in the regulation of Th2 response during the gastrointestinal nematode infection26. During Heligmosomoides polygyrus bakeri (Hp) infection, IL-1β production by the intestinal epithelial cells along with IL-25 and IL-33 secretion promoted the expansion of type-2 cytokines and type-2 immunity thus revealing the role of IL-1β in protective immunity27. Studies on the circulating levels of proinflammatory cytokines including IL-1β in individuals infected with Strongyloides stercoralis have shown an increased level of Il-1β and other proinflammatory cytokines during the infection which was later reversed following treatment28. Studies on the plasma levels of pro-inflammatory cytokines and chemokines in people with Strongyloides stercoralis infection (Ss +) and type-2 diabetes anti-helmintic treatment showed significantly elevated levels of IL-1Ra29. Studies on the Nippostrongylus brasiliensis (Nb) infected mouse models have shown the production of α-defensins by eosinophils, infiltrating the intestinal mucosa during the helminth infection. Also, the expression of mRNA for α-defensin was also 50-fold higher, suggesting the involvement of defensins in the defense mechanism against helminth infection30. Studies on the skin biopsies of Mansonella streptocerca infected individuals after treatment with a single dose of ivermectin showed degenerated and disintegrating microfilariae (mf) surrounded by immune cells especially neutrophils expressing defensins suggesting the role of defensin as the sign of acute inflammation25.
We found that LF infection significantly increased the circulating levels of IL-12, IFN-γ, IL-2, IL-33, IL-23, IL-17, IL-9 and reduced the IL-4 levels. Co-morbidity with diabetes had no effect on these cytokines. Compared to innate, the adaptive immune response has been well characterized in LF infection31. Unlike innate immune cytokines, adaptive immune cytokines are predominantly secreted either by professional antigen-presenting cells (polarizing cytokines) or T lymphocytes (effector cytokines). While the involvement of Th1 (IL-12, IFN-γ and IL-2) and Th2 (IL-33 and IL-4) cytokines in LF infection has been well characterized32, the importance of Th9 (IL-9) and Th17 (IL-23 and IL-17) cytokines21,33,34 has only recently been elucidated. Adaptive immune response in human filariasis is predominantly of Th2 type and involves the secretion of IL-4, IL-5 and IL-13. IL-4 is the master regulator of Th2 type immunity. Deletion of IL-4R in mice, transformed the highly resistant C57BL strain to a highly susceptible strain, augmenting the growth of Litomosoides sigmodontis35. Immunization of the susceptible Balb/c mice strain with recombinant B. malayi Troponin 1 antigen, induced antigen-specific IL-4 secretion, and was associated with protection against infection36. Infection of IL-4Ra/IL-5-/- BALB/c mice with L. sigmodontis induced strong pleural inflammation and was associated with reduced systemic levels of Th2 cytokines and higher worm burden37. Vaccinating Balb/c mice with recombinant B. malayi ALT-2 antigen, induced a strong Th2 immune response and conferred significant protection against pathogenic challenge38,39. Thus, the reduced IL-4 levels seen in this study might constitute an impaired adaptive immune defense against filariasis. However, IL-4 levels were not altered due to diabetes co-morbidity.
In the present study, it was found that LF infection significantly increased the circulating levels of the chemokines, IL-8, IP-10, RANTES, MCP-1 and SDF-1. IL-8 was the only chemokine whose levels were significantly reduced under conditions of comorbidity with diabetes, which is in accordance with a previous report40. Previously, early secretion of IL-8 from Peripheral Blood Mononuclear Cells (PBMCs) stimulated with L3 larvae, was noted in LF + subjects41. In filarial infection, macrophages, endothelial cells, and epithelial cells secrete IL-8, which induces neutrophil recruitment42. After recruitment, IL-8 promotes resolution of infection by inducing phagocytosis, oxidative burst and Neutrophil Extracellular Traps (NET/NETosis), in neutrophils42. Thus, IL-8 is the master regulator of neutrophil-mediated immune protection against filariasis, which was reduced in the DM-LF subjects, compared to the LF + subjects. Studies on estimating the circulatory levels of inflammatory biomarkers in 207 subjects in the filariasis endemic area of Orissa showed that the circulating levels of IL-8 were found to be higher in the subjects having the disease compared to the endemic controls. However, asymptomatic individuals showed a level of IL-8 similar to the controls. Thus, it was suggested that the enhanced IL-8 levels were associated with the disease state showing the acute and chronic filarial disease43. Monocytes obtained from filarial- infected (W. bancrofti) individuals showed diminished production of IL-8, compared to uninfected healthy individuals. This was reversed by a single ivermectin- albendazole treatment, suggesting that infection with W. bancrofti, selectively reduces the synthesis of certain cytokines and chemokines44. Also, studies show that filarial infected individuals, who had chronic pathology, with lymphedema, had higher levels of serum IL-840.
In the present study, it was found that LF infection significantly reduced the circulating levels of leptin and FGF-21 and co-morbidity with diabetes specifically augmented the levels of VEGF. Recently, the immune-endocrine network has been identified as a major component of anti-filarial immunity20. The cross-talk between hormones and immune cells determine the metabolic state of the immune cells and henceforth their function (immunometabolism)45. Previously, few studies have reported changes in the levels of metabolic hormones in individuals with obesity46 and diabetes47, infected with filariasis. In this study, both leptin and FGF-21 levels were found to be significantly reduced in the LF and DM-LF subjects. Serum adipocytokine profiling, carried out in obese subjects, infected with Strongyloides stercoralis, showed altered levels of adipocytokines, in these subjects46. Reduced levels of insulin and adiponectin were seen in diabetes patients, infected with Strongyloides stercoralis, which was reversed after treatment47. VEGF-A, VEGF-C and VEGF-D levels were also found to be reduced in these subjects47.
We found that LF infection significantly increased the circulating levels of lipid peroxidation and nitrites and co-morbidity with diabetes specifically reduced the levels of lipid peroxidation (but not nitrite production). The ability of the filarial parasites to survive inside the host partially depends upon the release of antioxidants48. The filarial nematode has evolved a strong antioxidant system, to protect them from the redox stress, produced by the host immune system48. In the present study, there was a significant decrease in lipid peroxidation, in subjects with diabetes-filariasis co-morbidity, while protein peroxidation was largely unaffected. Thus, diabetes might partially affect filarial elimination by reducing the innate redox defense mechanism.
Finally, we looked at Tregs and exhausted T cells in the study subjects. In general, filariasis infections bring about immunomodulation, in the host, by augmenting the activity of regulatory T cells (Tregs)49. However, in the present study, no significant difference was seen in the Treg population between the groups. Filarial infection is also known to induce both CD4 + and CD8 + T cell exhaustion, which is associated with disease pathology50. Recently, PD-1(high) CXCR5+CD4+ Tfh cells were found to play an important role in the production of antibodies against schistosomiasis51. In the present study, LF infection induced Th cell exhaustion, which was not affected by co-morbidity with diabetes. Compared to filariasis, diabetes seems to have very little effect on the immune markers studied, which was quite unexpected. Previously, several articles have indicated the effect of diabetes on immune system6,52. Our previous studies on TLRs have indicated that most of the immune modifying effect of diabetes is predominantly due to hyperglycemia and hence, were seen only in incipient diabetes and not in chronic diabetes patients (who were under treatment). Many of the immune markers which get deranged during incipient diabetes return back to normal rage with the control of blood sugar53,54,55. This could also be due to the anti-inflammatory effect of the anti-diabetic drugs, insulin and metformin56,57. In this study, both DM and DM-LF subjects were under treatment, with controlled blood sugar levels and this could account for the lack of significant impact of diabetes on the immune markers.
During filarial infection, the immune system responds through numerous effector pathways that target the various stages of the parasite58. The typical host immune response to filarial parasites includes the production of cytokines (IL-4, IL-5, IL-9, IL-10, and IL-13), chemokines (IL-8, MCP-1, RANTES, IP-10, MIG) and antibodies with increased eosinophil count and M2 macrophage polarization. Various studies have shown that innate immune cytokines, especially the pro-inflammatory cytokines, play a vital role in the pathology of lymphedema19. Studies have shown increased serum levels of pro-inflammatory cytokines IL-1β, IL-12, TNF-α and IL-6 as well as IL-8, IP-10 etc., which are associated with the immune activation in the filarial pathology19. Leptin promotes Th1, decreases Th2, and can operate as a negative signal for Tregs. These alterations may reverse the helminth-associated type 2 immune responses59. Nitric oxide or nitrate are shown to be cytotoxic for filarial parasite and are shown to participate in the parasite clearance, during a filarial infection, and was found to be increased in this study60. The major processes that influence the regulation of the immune response in filarial infection include the induction of regulatory T cells and exhaution of effector T cells61. It has been suggested that Tregs (both natural and induced), play a key role in the immune evasion by the filarial parasite. This is evidenced by the increased expression of IL-10 and TGF-β in filarial infections, as seen in this study. Also, studies have shown that in murine filarial infections, activity of Tregs have a direct link with the filarial survival, and elimination of Tregs restored the anti-filarial immunity19. Filarial infections are associated with increased expression of CTLA-4 and PD-1, as was seen in this study. Studies have shown that blocking CTLA-4 can partially restore immune response against filariasis19.
The current treatment for lymphatic filariasis include administration of drugs like diethylcarbamazine (DEC), ivermectin or albendazole. Though these drugs are effective in eliminating the microfilariae and block the transmission of the parasite, more efficient drugs are required to target the adult worms62. Hence research is needed to identify biologicals which can completely eliminate the parasite. The adoptive transfer of polyclonal antibodies that were raised against filarial surface antigens (FSAg) in mice, has shown significant reduction in the parasite burden, in infected rats and was also shown to reduce pro-inflammatory cytokines63. A small heat shock protein expressed by Brugia malayi (BmHsp12.6) was shown to bind to IL-10R and was shown to have immunomodulatory functions64. Similarly, filarial antigens like glutathione S- transferase (GST), abundant larval transcript 2 (ALT2), thioredoxin peroxidase (TPX) etc. were shown to have immunomodulatory effect on experimental filarial infections65,66,67. Administration of recombinant Brugia malayi Troponin 1 (rTn1-bm) showed increased cellular proliferation, secretion of pro-inflammatory cytokines and release of NO thereby conferring a protection against the parasite36. This study for the first time identified several key immune mediators involved in anti-filarial immunity and how they are altered under diabetes co-morbidity, and can contribute towards development of immunotherapy against filariasis. The major limitation of this study is that it was conducted with a limited sample size (since the current prevalence of LF among the South Indian population is 1%). Further, being a cross-sectional study, a cause-effect relationship cannot be established. However, the major strength of the study is that, it was conducted in a filarial endemic population, where the prevalence of diabetes is rapidly increasing.
In conclusion, we report, the effect of diabetes on anti-filarial immunity, under conditions of diabetes-filariasis co-morbidity. Several important immune biomarkers including cytokines, chemokines, defensins, hormones, growth factors, redox markers, Tregs and exhausted T cells were studied. The most interesting and unexpected finding of this study is that while LF being a parasitic infection brought about major drift in the levels of these immune biomarkers, co-morbidity with diabetes, specifically altered only few of these biomarkers (which were critical for anti-filarial immunity). Importantly the levels of IL-1β, IL-1Ra, IL-8, DEF-A1 and ROI were reduced, while that of VEGF was increased, in DM-LF group, compared to LF group (Fig. 7). Overall, diabetes was found to have significant effect on anti-filarial immunity and neolymphangiogenesis, which can promote chronic pathology, and this needs further validation in a large cohort study.
A model explaining the role played by immune mediators under conditions of DM-LF co-morbidity. During infection, the innate and adaptive arms of the immune response, coordinate to confer protection against filariasis. The activated eosinophils in turn secrete IL-4, which activates and polarizes the resident macrophages (a), to the M2 phenotype. These M2 macrophages secrete IL-8, which attracts the neutrophils (b). They also secrete IL-1β and IL-1Ra which modulates the activation of the neutrophils. The activated eosinophils and neutrophils secrete reactive oxygen intermediates and defensins, which aid in the killing of the parasite. M2 macrophages secrete VEGF (c), which mediates neolymphangiogenesis. All these immune markers were affected in filariasis infected individuals who are diabetic.
Materials and methods
Study subjects
This study is a follow-up of our previous publication wherein we reported a decreased prevalence of LF among diabetic patients compared to normoglycemic subjects5. As a continuation of that study, 1001 outpatients visiting Dr. Mohan’s Diabetes Specialties Centre, Chennai, India, were screened for LF. Out of 1001, only 13 were found to be positive for LF antigen (1.2%). The control subjects were recruited from the healthy volunteers (n = 500) who accompanied the diabetes patients and underwent OGTT testing, as part of this study. Institutional ethical committee approval from the Madras Diabetes Research Foundation Ethics Committee was obtained (Ref No-MDRF-EC/SOC/2009//05) and written informed consent was obtained from all the study subjects. The study was conducted as per the Declaration of Helsinki, following STROBE guidelines. This is the 6th manuscript from the DM-LF study (DM-LF-6).
Diagnosis of T2DM
Diagnosis for T2DM was done following the World Health Organisation (WHO) guidelines68
Detection of bancroftian LF
Filarial antigen level in the sera was quantified using the W. bancrofti Og4C3 antigen-capture ELISA (Tropbio, Australia) according to the manufacturer’s instructions69.
Study groups
The following groups were included.
-
1.
Healthy volunteers who were LF negative and normoglycemic were included as controls (C; n = 12)).
-
2.
Normoglycemic subjects who were LF positive (LF; n = 8).
-
3.
Diabetic subjects who are LF negative (DM; n = 12).
-
4.
Diabetic subjects who were LF positive (DM-LF; n = 13).
Inclusion and exclusion criteria
Only subjects who were aged between 30 and 50 yrs, were included in the study. None of the subjects showed any symptoms of lymphatic filariasis at the time of recruitment. The exclusion criteria were patients with type-1 diabetes and those with a previous diagnosis of urolithiasis, liver cirrhosis, congestive heart failure, chronic lung diseases, chronic infections, or viral hepatitis.
Measurement of cytokines, chemokines, hormones and growth factors by ELISA
The levels of cytokines (TNF-α, IL-6, IL-1β, IL-10, IL-1Ra, TGF-β, IL-27, IFN β, IL-12p70, IFN-γ, IL-2, IL-23, IL-17, IL-9, IL-33, IL-4), chemokines (IL-8, IP-10, SDF-1, MCP-1, and RANTES), hormones (Insulin, adiponectin and leptin), growth factors (FGF-21 and VEGF) and defensin (DEF-A1) were quantified, in the plasma using ELISA (R&D, US) following manufacturer’s protocol. The lower detection limits were: TNF-α = 0.75 pg/ml, IL-6 = 0.32 pg/ml, IL-1β = 0.72 pg/ml, IL-10 = 12.3 pg/ml, IL-1Ra = 0.20 pg/ml, TGF-β = 32.03 pg/ml, IL-27 = 26.3 pg/ml, IFN β = 0.003 pg/ml, IL-12p70 = 2.92 pg/ml, IFN-γ- 0.02 pg/ml, IL-2 = 2.09 pg/ml, IL-23 = 12.19 pg/ml, IL-17 = 1.30 pg/ml, IL-9 = 1.59 pg/ml, IL-33 = 0.31 pg/ml, IL-4 = 0.44 pg/ml, IL-8 = 23.22 pg/ml, IP-10 = 7.15 pg/ml, SDF-1 = 147.79 pg/ml, MCP-1 = 24.52 pg/ml, RANTES = 0.02 pg/ml, Insulin = 0.005 pmol/l, Adiponectin = 24.74 pg/ml, Leptin = 214.84 pg/ml, FGF-21 = 32.01 pg/ml, VEGF = 22.89 pg/ml. and α-defensin = 0.02 pg/ml. The lower detection limits were: The CV was found to be < 10%.
Flow cytometry
2 ml of whole blood was collected in EDTA- coated tubes. After centrifugation, separation of plasma and RBC lysis, the packed cell volume (PCV) was stained with monoclonal antibodies specific for CD3, CD4, CD25, FoxP3, CD152 (CTLA-4) and CD279 (PD-1). Stained cells were analyzed on FACS Canto (BD Biosciences, US). The gating strategy and analysis are illustrated in S. Figure 1.
Peripheral blood leukocyte cultures
Whole blood cultures from the study subjects were performed as described previously54. Briefly, 2 ml of whole blood was collected in EDTA-coated tubes. After centrifugation, the packed cell volume was diluted with RPMI medium (1:1 ratio) containing 10% FCS and was used for in vitro culture. Cells were stimulated with TLR2 ligand-PAM3CSK4 (100 ng/ml) (Invivogen, US), TLR4 ligand-LPS (100 ng/ml) (Invivogen, US), Brugia malayi crude antigen- BmA (10 µg/ml) or were left unstimulated, for 24 h, in parallel cultures. The cell pellets were solubilized in RNAzol and were stored at -80 °C.
Real-time PCR analysis
RNA extraction from the stored samples was carried out using RNeasy Mini Kit (Qiagen). 1 µg of RNA was converted to cDNA using reverse transcription and real-time PCR was performed using TaqMan probes (Applied Biosystems, US) specific for FOXP3. 18S rRNA was used as a housekeeping control. Gene expression levels (normalized to 18S rRNA) were analyzed using the StepOnePlus RT-PCR system (Applied Biosystems, Foster City, CA, USA) and 2–ΔΔCt was calculated for all samples with unstimulated sample values as reference.
Statistical analysis
Mann–Whitney U test was used for comparing LF- versus LF + groups. Multiple comparisons were corrected using Holm’s correction. All the analyses were done using GraphPad Prism version 5.0 (GraphPad Software, US). p-value less than 0.05 was considered significant.
Data availability
Data is provided within the manuscript or supplementary information files.
References
Bizhani, N., Hashemi Hafshejani, S., Mohammadi, N., Rezaei, M. & Rokni, M. B. Lymphatic filariasis in Asia: A systematic review and meta-analysis. Parasitol. Res. 120, 411–422. https://doi.org/10.1007/s00436-020-06991-y (2021).
Liu, Q. et al. Helminth infection can reduce insulitis and type 1 diabetes through CD25- and IL-10-independent mechanisms. Infect. Immun. 77, 5347–5358. https://doi.org/10.1128/IAI.01170-08 (2009).
Berbudi, A. et al. Filarial infection or antigen administration improves glucose tolerance in diet-induced obese mice. J. Innate. Immun. 8, 601–616. https://doi.org/10.1159/000448401 (2016).
Aravindhan, V. et al. Decreased prevalence of lymphatic filariasis among subjects with type-1 diabetes. Am. J. Trop. Med. Hyg. 83, 1336–1339. https://doi.org/10.4269/ajtmh.2010.10-0410 (2010).
Aravindhan, V. et al. Decreased prevalence of lymphatic filariasis among diabetic subjects associated with a diminished pro-inflammatory cytokine response (CURES 83). PLoS Negl. Trop. Dis. 4, e707. https://doi.org/10.1371/journal.pntd.0000707 (2010).
Berbudi, A., Rahmadika, N., Tjahjadi, A. I. & Ruslami, R. Type 2 diabetes and its impact on the immune system. Curr. Diabetes Rev. 16, 442–449. https://doi.org/10.2174/1573399815666191024085838 (2020).
Denzinger, S., Watzlawek, E., Burger, M., Wieland, W. F. & Otto, W. Giant scrotal elephantiasis of inflammatory etiology: A case report. J. Med. Case Rep. 1, 23. https://doi.org/10.1186/1752-1947-1-23 (2007).
Ranasinghe, P., Jayawardena, R. & Katulanda, P. Sri Lanka in global medical research: A scientific analysis of the Sri Lankan research output during 2000–2009. BMC Res. Notes 5, 121. https://doi.org/10.1186/1756-0500-5-121 (2012).
Masamatti, S. S., Narasimha, A., Janardhan, J. V. & Chowdappa, V. Lymph node fibrosis in a case of primary lymphedema—A report of two cases. J. Clin. Diagn. Res. 10, ED08–ED09. https://doi.org/10.7860/JCDR/2016/19528.8561 (2016).
Pearce, E. J. et al. Th2 response polarization during infection with the helminth parasite Schistosoma mansoni. Immunol. Rev. 201, 117–126. https://doi.org/10.1111/j.0105-2896.2004.00187.x (2004).
Babu, S. et al. Filarial lymphedema is characterized by antigen-specific Th1 and th17 proinflammatory responses and a lack of regulatory T cells. PLoS Negl. Trop. Dis. 3, e420. https://doi.org/10.1371/journal.pntd.0000420 (2009).
Sokol, C. L. & Luster, A. D. The chemokine system in innate immunity. Cold Spring Harb. Perspect. Biol. 7, a016303. https://doi.org/10.1101/cshperspect.a016303 (2015).
Bouchery, T. et al. The chemokine CXCL12 is essential for the clearance of the filaria Litomosoides sigmodontis in resistant mice. PLoS ONE 7, e34971. https://doi.org/10.1371/journal.pone.0034971 (2012).
Kathamuthu, G. R. et al. Filarial coinfection is associated with higher bacterial burdens and altered plasma cytokine and chemokine responses in tuberculous lymphadenitis. Front. Immunol. 11, 706. https://doi.org/10.3389/fimmu.2020.00706 (2020).
Ray, A. S., Joardar, N., Mukherjee, S., Rahaman, C. H. & Sinha Babu, S. P. Polyphenol enriched ethanolic extract of Cajanus scarabaeoides (L.) Thouars exerts potential antifilarial activity by inducing oxidative stress and programmed cell death. PLoS ONE 13, 0208201. https://doi.org/10.1371/journal.pone.0208201 (2018).
Aravindhan, V. & Anand, G. Cell type-specific immunomodulation induced by helminthes: Effect on metainflammation, insulin resistance and type-2 diabetes. Am. J. Trop. Med. Hyg. 97, 1650–1661. https://doi.org/10.4269/ajtmh.17-0236 (2017).
Aravindhan, V. & Madhumitha, H. Metainflammation in diabetic coronary artery disease: Emerging role of innate and adaptive immune responses. J. Diabetes Res. 2016, 6264149. https://doi.org/10.1155/2016/6264149 (2016).
Ritter, M. & Hubner, M. P. Editorial: Host immune response and protective immune responses during filarial infections. Front. Immunol. 13, 1102121. https://doi.org/10.3389/fimmu.2022.1102121 (2022).
Babu, S. & Nutman, T. B. Immunology of lymphatic filariasis. Parasite Immunol. 36, 338–346. https://doi.org/10.1111/pim.12081 (2014).
Sibi, J. M., Mohan, V., Deepa, M., Babu, S. & Aravindhan, V. Modulatory effect of filarial infection on the systemic hormone levels in subjects with metabolic syndrome (DM-LF5). Front. Endocrinol. 13, 1011942. https://doi.org/10.3389/fendo.2022.1011942 (2022).
Sibi, J. M., Mohan, V., Munisankar, S., Babu, S. & Aravindhan, V. Augmented innate and adaptive immune responses under conditions of diabetes-filariasis comorbidity. Front. Immunol. 12, 716515. https://doi.org/10.3389/fimmu.2021.716515 (2021).
Sahoo, M. K. et al. Immunization with inflammatory proteome of Brugia malayi adult worm induces a Th1/Th2-immune response and confers protection against the filarial infection. Vaccine 27, 4263–4271. https://doi.org/10.1016/j.vaccine.2009.05.015 (2009).
Dixit, S. et al. Inflammatory antigens of Brugia malayi and their effect on rodent host Mastomys coucha. Parasite Immunol. 26, 397–407. https://doi.org/10.1111/j.0141-9838.2004.00725.x (2004).
Chakraborty, P., Aravindhan, V. & Mukherjee, S. Helminth-derived biomacromolecules as therapeutic agents for treating inflammatory and infectious diseases: What lessons do we get from recent findings?. Int. J. Biol. Macromol. 241, 124649. https://doi.org/10.1016/j.ijbiomac.2023.124649 (2023).
Fischer, P., Bamuhiiga, J. & Buttner, D. W. Treatment of human Mansonella streptocerca infection with ivermectin. Trop. Med. Int. Health 2, 191–199. https://doi.org/10.1046/j.1365-3156.1997.d01-233.x (1997).
Helmby, H. & Grencis, R. K. Interleukin 1 plays a major role in the development of Th2-mediated immunity. Eur. J. Immunol. 34, 3674–3681. https://doi.org/10.1002/eji.200425452 (2004).
Zaiss, M. M. et al. IL-1beta suppresses innate IL-25 and IL-33 production and maintains helminth chronicity. PLoS Pathog. 9, e1003531. https://doi.org/10.1371/journal.ppat.1003531 (2013).
Anuradha, R. et al. Systemic cytokine profiles in strongyloides stercoralis infection and alterations following treatment. Infect. Immun. 84, 425–431. https://doi.org/10.1128/IAI.01354-15 (2016).
Rajamanickam, A. et al. Helminth infection modulates systemic pro-inflammatory cytokines and chemokines implicated in type 2 diabetes mellitus pathogenesis. PLoS Negl. Trop. Dis. 14, e0008101. https://doi.org/10.1371/journal.pntd.0008101 (2020).
Khatun, A., Sakurai, M., Okada, K., Sakai, Y. & Morimoto, M. Detection of alpha-defensin in eosinophils in helminth-infected mouse model. J. Vet. Med. Sci. 80, 1887–1894. https://doi.org/10.1292/jvms.18-0601 (2018).
Sahu, B. R., Mohanty, M. C., Sahoo, P. K., Satapathy, A. K. & Ravindran, B. Protective immunity in human filariasis: A role for parasite-specific IgA responses. J. Infect. Dis. 198, 434–443. https://doi.org/10.1086/589881 (2008).
Hoerauf, A. & Brattig, N. Resistance and susceptibility in human onchocerciasis–beyond Th1 vs. Th2. Trends Parasitol. 18, 25–31. https://doi.org/10.1016/s1471-4922(01)02173-0 (2002).
Anuradha, R. et al. IL-4-, TGF-beta-, and IL-1-dependent expansion of parasite antigen-specific Th9 cells is associated with clinical pathology in human lymphatic filariasis. J. Immunol. 191, 2466–2473. https://doi.org/10.4049/jimmunol.1300911 (2013).
Anuradha, R. et al. Modulation of CD4+ and CD8+ T-cell function by interleukin 19 and interleukin 24 during filarial infections. J. Infect. Dis. 213, 811–815. https://doi.org/10.1093/infdis/jiv497 (2016).
Le Goff, L., Lamb, T. J., Graham, A. L., Harcus, Y. & Allen, J. E. IL-4 is required to prevent filarial nematode development in resistant but not susceptible strains of mice. Int. J. Parasitol. 32, 1277–1284. https://doi.org/10.1016/s0020-7519(02)00125-x (2002).
Kushwaha, V., Tewari, P., Mandal, P., Tripathi, A. & Murthy, P. K. Troponin 1 of human filarial parasite Brugia malayi: cDNA cloning, expression, purification, and its immunoprophylactic potential. Parasitol. Res. 118, 1849–1863. https://doi.org/10.1007/s00436-019-06316-8 (2019).
Ritter, M. et al. IL-4/5 signalling plays an important role during Litomosoides sigmodontis infection, influencing both immune system regulation and tissue pathology in the thoracic cavity. Int. J. Parasitol. 47, 951–960. https://doi.org/10.1016/j.ijpara.2017.06.009 (2017).
Dakshinamoorthy, G. & Kalyanasundaram, R. Evaluating the efficacy of rBmHATalphac as a multivalent vaccine against lymphatic filariasis in experimental animals and optimizing the adjuvant formulation. Vaccine 32, 19–25. https://doi.org/10.1016/j.vaccine.2013.10.083 (2013).
Kalyanasundaram, R. & Balumuri, P. Multivalent vaccine formulation with BmVAL-1 and BmALT-2 confer significant protection against challenge infections with Brugia malayi in mice and jirds. Res. Rep. Trop. Med. 45–56, 2011. https://doi.org/10.2147/RRTM.S13679 (2011).
Babu, S., Blauvelt, C. P., Kumaraswami, V. & Nutman, T. B. Chemokine receptors of T cells and of B cells in lymphatic filarial infection: A role for CCR9 in pathogenesis. J. Infect. Dis. 191, 1018–1026. https://doi.org/10.1086/427658 (2005).
Semnani, R. T., Law, M., Kubofcik, J. & Nutman, T. B. Filaria-induced immune evasion: Suppression by the infective stage of Brugia malayi at the earliest host-parasite interface. J. Immunol. 172, 6229–6238. https://doi.org/10.4049/jimmunol.172.10.6229 (2004).
Brattig, N. W., Buttner, D. W. & Hoerauf, A. Neutrophil accumulation around Onchocerca worms and chemotaxis of neutrophils are dependent on Wolbachia endobacteria. Microbes Infect. 3, 439–446. https://doi.org/10.1016/s1286-4579(01)01399-5 (2001).
Satapathy, A. K. et al. Human bancroftian filariasis: Immunological markers of morbidity and infection. Microbes Infect. 8, 2414–2423. https://doi.org/10.1016/j.micinf.2006.05.003 (2006).
Semnani, R. T. et al. Filaria-induced monocyte dysfunction and its reversal following treatment. Infect. Immun. 74, 4409–4417. https://doi.org/10.1128/IAI.01106-05 (2006).
Crowe, J. et al. The parasitic worm product ES-62 promotes health- and life-span in a high calorie diet-accelerated mouse model of ageing. PLoS Pathog. 16, e1008391. https://doi.org/10.1371/journal.ppat.1008391 (2020).
Rajamanickam, A. et al. Impact of helminth infection on metabolic and immune homeostasis in non-diabetic obesity. Front. Immunol. 11, 2195. https://doi.org/10.3389/fimmu.2020.02195 (2020).
Rajamanickam, A., Munisankar, S., Menon, P. A., Nutman, T. B. & Babu, S. Diminished circulating levels of angiogenic factors and rage ligands in helminth-diabetes comorbidity and reversal following anthelmintic treatment. J. Infect. Dis. 224, 1614–1622. https://doi.org/10.1093/infdis/jiab170 (2021).
Gupta, S. & Srivastava, A. K. Glutathione metabolism of filarial worms: A vulnerable target for the design and synthesis of new antifilarial agents. Med. Sci. Monit. 12, HY1–HY9 (2006).
Wammes, L. J. et al. Regulatory T cells in human lymphatic filariasis: Stronger functional activity in microfilaremics. PLoS Negl. Trop. Dis. 6, e1655. https://doi.org/10.1371/journal.pntd.0001655 (2012).
Horn, S. et al. Filarial lymphedema patients are characterized by exhausted CD4(+) T cells. Front. Cell Infect. Microbiol. 11, 767306. https://doi.org/10.3389/fcimb.2021.767306 (2021).
Zhang, Y. et al. Higher frequency of circulating PD-1(high) CXCR5(+)CD4(+) Tfh cells in patients with chronic schistosomiasis. Int. J. Biol. Sci. 11, 1049–1055. https://doi.org/10.7150/ijbs.12023 (2015).
Geerlings, S. E. & Hoepelman, A. I. Immune dysfunction in patients with diabetes mellitus (DM). FEMS Immunol. Med. Microbiol. 26, 259–265. https://doi.org/10.1111/j.1574-695X.1999.tb01397.x (1999).
Madhumitha, H. et al. Impaired toll-like receptor signalling in peripheral B cells from newly diagnosed type-2 diabetic subjects. Cytokine 76, 253–259. https://doi.org/10.1016/j.cyto.2015.04.010 (2015).
Madhumitha, H., Mohan, V., Babu, S. & Aravindhan, V. TLR-induced secretion of novel cytokine IL-27 is defective in newly diagnosed type-2 diabetic subjects. Cytokine 104, 65–71. https://doi.org/10.1016/j.cyto.2017.09.032 (2018).
Shruthi, S. et al. Decreased leukocyte exhaustion is associated with decreased IFN-beta and increased alpha-defensin-1 levels in type-2 diabetes. Cytokine 156, 155918. https://doi.org/10.1016/j.cyto.2022.155918 (2022).
Saisho, Y. Metformin and inflammation: Its potential beyond glucose-lowering effect. Endocr. Metab. Immune Disord. Drug Targets 15, 196–205. https://doi.org/10.2174/1871530315666150316124019 (2015).
Dandona, P., Chaudhuri, A., Mohanty, P. & Ghanim, H. Anti-inflammatory effects of insulin. Curr. Opin. Clin. Nutr. Metab. Care 10, 511–517. https://doi.org/10.1097/MCO.0b013e3281e38774 (2007).
Nutman, T. B. & Kumaraswami, V. Regulation of the immune response in lymphatic filariasis: Perspectives on acute and chronic infection with Wuchereria bancrofti in South India. Parasite Immunol. 23, 389–399. https://doi.org/10.1046/j.1365-3024.2001.00399.x (2001).
Tahapary, D. L. et al. Effect of anthelmintic treatment on leptin, adiponectin and leptin to adiponectin ratio: A randomized-controlled trial. Nutr. Diabetes 7, e289. https://doi.org/10.1038/nutd.2017.37 (2017).
Winkler, S., El Menyawi, I., Linnau, K. F. & Graninger, W. Short report: Total serum levels of the nitric oxide derivatives nitrite/nitrate during microfilarial clearance in human filarial disease. Am. J. Trop. Med. Hyg. 59, 523–525. https://doi.org/10.4269/ajtmh.1998.59.523 (1998).
Maizels, R. M. & Yazdanbakhsh, M. Immune regulation by helminth parasites: Cellular and molecular mechanisms. Nat. Rev. Immunol. 3, 733–744. https://doi.org/10.1038/nri1183 (2003).
Melrose, W. D. Chemotherapy for lymphatic filariasis: Progress but not perfection. Expert Rev. Anti. Infect. Ther. 1, 571–577. https://doi.org/10.1586/14787210.1.4.571 (2003).
Das, N. C., Ray, A. S., Bayry, J. & Mukherjeee, S. Therapeutic efficacy of anti-bestrophin antibodies against experimental filariasis: Immunological. Immune-Inform. Immune Simul. Investig. Antibodies https://doi.org/10.3390/antib10020014 (2021).
Dakshinamoorthy, G. et al. Biochemical characterization and evaluation of a Brugia malayi small heat shock protein as a vaccine against lymphatic filariasis. PLoS ONE 7, e34077. https://doi.org/10.1371/journal.pone.0034077 (2012).
Veerapathran, A., Dakshinamoorthy, G., Gnanasekar, M., Reddy, M. V. & Kalyanasundaram, R. Evaluation of Wuchereria bancrofti GST as a vaccine candidate for lymphatic filariasis. PLoS Negl. Trop. Dis. 3, e457. https://doi.org/10.1371/journal.pntd.0000457 (2009).
Gregory, W. F., Atmadja, A. K., Allen, J. E. & Maizels, R. M. The abundant larval transcript-1 and -2 genes of Brugia malayi encode stage-specific candidate vaccine antigens for filariasis. Infect Immun. 68, 4174–4179. https://doi.org/10.1128/IAI.68.7.4174-4179.2000 (2000).
Anand, S. B. et al. Comparison of immunogenicity, protective efficacy of single and cocktail DNA vaccine of Brugia malayi abundant larval transcript (ALT-2) and thioredoxin peroxidase (TPX) in mice. Acta Trop 107, 106–112. https://doi.org/10.1016/j.actatropica.2008.04.018 (2008).
World Health, O. & International Diabetes, F. (World Health Organization, Geneva, 2006).
Pion, S. D. et al. Positivity of antigen tests used for diagnosis of lymphatic filariasis in individuals without Wuchereria Bancrofti infection but with high Loa Loa Microfilaremia. Am. J. Trop. Med. Hyg. 95, 1417–1423. https://doi.org/10.4269/ajtmh.16-0547 (2016).
Acknowledgements
Some of the experiments were carried using the DHR supported Multi-Disciplinary Research Unit. The Dept of Genetics, University of Madras has received funds for infrastructural support from DST-FIST and UGC-SAP programs. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
VA, SB and VM conceived and designed the experiment. JMS and SS performed the experiment. JMS and VA analyzed the data. JMS and VA drafted the manuscript. All the authors contributed to the discussion and reviewed the manuscript. VA is the guarantors of the data.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
The human experimental procedures were approved by the Madras Diabetes Research Foundation Ethics Committee (Ref No-MDRF-EC/SOC/2009//05).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Sibi, J.M., Shruthi, S., Mohan, V. et al. Immunoendocrine network under conditions of diabetes-filariasis co-morbidity DMLF6. Sci Rep 15, 35060 (2025). https://doi.org/10.1038/s41598-025-02862-7
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-02862-7