Abstract
Chest physiotherapy, a key component of bronchial hygiene therapy, plays an important role in the overall management and care of patients who require Mechanical Ventilation (MV). We compared the effects of two types of physiotherapy techniques on selected weaning indices of patients requiring MV. We conducted a single-blind randomized controlled clinical trial with pre- and post-measurements in 60 patients requiring MV. Randomization was performed via block randomization with Sequential Numbered Opaque Sealed Envelopes. Participants were randomized into (1) lung squeezing technique (LST) or (2) chest vibration and percussion technique (CVPT). Data collection was carried out using a researcher-created checklist that comprised two sections. The first section gathered patient demographic information, while the second section functioned as a vital sign record sheet. This vital sign record was further divided: the initial part documented systolic and diastolic blood pressure, pulse rate, oxygen saturation, and RSBI prior to the intervention, and the follow-up part captured the same vital signs at intervals of 5- and 25-minutes post-intervention. There was no statistically significant difference between systolic and diastolic blood pressure, respiratory rate, and oxygen saturation scores of the two study groups at baseline and at 5- and 25-minute intervals post-intervention (P > 0.05). However, in terms of rapid, shallow breathing index (RSBI), a significant difference was observed between the two groups scores at baseline (LST: 38.5 (36.2–44.1) vs. CVPT: 35.2 (33.7–38); P < 0.0), 5-minutes post-intervention (LST: 36.6 (34.3–44) vs. CVPT: 34.8 (32.2–36.9); P < 0.05) and 25-minutes post-intervention (LST: 37.1 (32.5–44.4) vs. CVPT: 34 (32.5–35.8); P < 0.05). The results demonstrated that LST outperformed CVPT in enhancing the RSBI, which serves as a weaning index for patients requiring MV. This suggests that LST may facilitate earlier weaning and extubation for these patients. IRCT20091215002861N18, 09/12/2022.
Trial Registration Number: IRCT20091215002861N18, 09/12/2022.
Similar content being viewed by others
Background
Mechanical ventilation (MV), a life-saving intervention, is administered annually to more than 20 million patients globally1. Studies have suggested that a significant proportion, estimated to be around 30%, of individuals admitted to the Intensive Care Unit (ICU) may necessitate MV to assist their respiration during critical illness2,3,4. However, a growing body of evidence has highlighted that extended MV is significantly associated with negative impacts on functional outcomes, extended hospital stays, and increased residual disability, ultimately leading to substantial social and healthcare costs, as supported by various studies5,6,7,8.
Prolonged MV is associated with various detrimental physical and functional effects, including impaired secretion clearance and ICU-acquired weakness (ICU-AW), which leads to physical limitations9. This situation is further exacerbated by malnutrition, chronic cardiac and respiratory problems, and a heightened risk of mental health issues such as depression, anxiety, and delirium5.
In addition to the previously noted physical consequences, patients admitted to the ICU who require prolonged MV may account for a significant portion, over 37%, of the ICU’s overall resource allocation10. In addition, ICU patients requiring MV require at least 6 h per day for at least 21 days, consuming 60% more healthcare resources than non-ventilated patients11. While MV may be necessary for patients experiencing acute respiratory failure, the extended use of MV carries a risk of numerous complications such as ventilator-associated pneumonia (VAP) and pulmonary atelectasis, which may lead to higher mortality12,13.
Given these factors, a patient-centered rehabilitation program designed to enhance the process of weaning from MV should be considered an essential component of managing critically ill ICU patients, ultimately leading to improved physical and psychosocial outcomes, as supported by research14. New research shows that while 70% of patients in the ICU are successfully weaned from MV on the first day, a substantial 30% experience initial failure, creating negative consequences and lengthening the weaning process15. Approximately 3–14% of patients in intensive care units require prolonged MV, defined as ventilation lasting over 96 h or 14 days, and are classified as “difficult to wean.” Notably, around 25% of these patients develop muscle weakness in the initial phases of their recovery16. Several studies17,18,19,20,21 have supported the benefits of early mobilization, as well as respiratory and physical therapy interventions, in various conditions up to the present time.
Chest physiotherapy, a key component of bronchial hygiene, plays an important role in the management of patients requiring MV22. Chest physiotherapy encompasses a wide range of techniques such as body positioning, manual techniques (including mobilization, percussion, vibration, and compression), and specialized methods like lung hyperinflation and intrapulmonary percussion23.
The choice of physiotherapy techniques depends on several factors, including specific injury or condition, ease of expectoration, the level of cooperation, the status of patients requiring MV, the efficacy and safety of the intervention, operational costs, and the preferences of the patients requiring MV24.
Chest vibration and lung squeezing are two popular techniques utilized for enhancing mucociliary clearance in both the central and peripheral airways, proving to be particularly effective in mobilizing secretions that adhere to the bronchial walls25. The lung squeezing technique (LST) is an advanced chest physiotherapy method involving gentle, sustained compression of the chest wall, followed by complete release26. LST helps increase intrathoracic pressure, which can then stimulate the cough mechanism and assist in moving pulmonary secretions, facilitate a more active inhalation, and improve alveolar ventilation27,28.
Also, CVPT is another physiotherapy technique that incorporates chest wall percussion and vibrations, strategic patient positioning to facilitate mucus drainage, and the implementation of effective coughing and breathing techniques to aid the evacuation of secretions that have accumulated in the lungs, boost ventilation and pulmonary perfusion to avoid atelectasis29,30. The effectiveness of these techniques has been investigated in a few studies. Own et al. (2020) in their study found that the two methods of LST and chest percussion can improve the oxygenation parameters of patients requiring MV31. Also, the study by Wong et al. (2003) showed that the LST was more effective than conventional chest vibration for the re-expansion of lung atelectasis among the ventilated pre-term neonates32. Although the effect of these techniques separately and together on respiratory and hemodynamic parameters of different respiratory patients has been investigated, no study has compared the effect of these two techniques on the weaning indices of patients requiring MV. So, this study aimed to compare the effects of two types of physiotherapy techniques on selected weaning indices of patients requiring MV.
Methods
Design
From November 2022 to August 2023, a single-blinded, randomized, controlled trial with pre- and post-measurements was conducted to compare the selected weaning indices in patients requiring MV treated with two distinct physiotherapy techniques: LST and CVPT. In accordance with the Declaration of Helsinki33 and following the approval granted by the Ethics Committee of Shahrekord University of Medical Sciences (No: IR.SKUMS.REC.1401.127), all phases of this research study have been conducted. This study’s protocol is registered with the Iranian Registry of Clinical Trials, accessible online (No: IRCT20091215002861 N18, 09/12/2022). To guarantee that the study met the suggested standards, this study was conducted and its findings were reported in accordance with the Consolidated Standards of Reporting Trials (CONSORT) statement guidelines34.
Patient population and sampling
The participants in this study consisted of patients who were hospitalized in the ICUs of Ayatollah Kashani Hospital affiliated with Shahrekord University of Medical Sciences. Participants were selected using a convenience sampling method based on pre-defined inclusion criteria, and then, to match the groups and control for confounding variables, a block randomization method with sequential numbered opaque sealed envelopes was used for group allocation. In total, sixteen blocks were considered, each comprised of four members. An individual who was not involved with the study selected sealed envelopes to assign participants to one of the two groups: LST and CVPT groups, so the outcome assessor in the two groups was blinded to the randomization codes and the type of administered physiotherapy method during the study.
Inclusion and exclusion criteria
Inclusion criteria included: (1) having a stable hemodynamic status (in terms of blood pressure and pulse), (2) having an endotracheal tube, (3) not having endotracheal suctioning within one hour before each intervention session, and (4) ability to follow commands and take deep breaths during the implementation of the procedures. Exclusion criteria included: (1) chest trauma and (2) ischemia or life-threatening cardiac arrhythmias.
Intervention
Following the receipt of the ethical code and all necessary permits, a comprehensive explanation of the research objectives and methodology was provided to the departments’ head nurses and the patient’s legal guardians, emphasizing the voluntary nature of participation and the participant’s right to withdraw at any time; subsequently, the informed consent forms were completed, and the study commenced. We investigated the effect of physiotherapy (LST and CVPT) on airway clearance and the selected weaning indices of patients requiring MV in both groups. Patients in the first group were given LST if they had not already received tracheal suction, bronchodilators, food, or drug gavage. Prior to performing the maneuver, the researcher observed three to five respirations in order to determine the amount of pressure on the thorax. Based on the observed pressure, the amount of pressure during expiration was adjusted accordingly (for all respirations, mechanically assisted or spontaneous). Using the hands unilaterally, on the lower one-third of the thorax (anteriorly and posteriorly), proportionate to the patient’s body, increases the expiratory tidal volume by 30% (as shown on the monitor). At the end of each expiration, the pressure was removed to allow free inspiration, and this procedure was repeated 10 times with an interval of three respiratory cycles between each compression35.
CVPT was performed in the second group; patients initially underwent suction without CVPT, and 3 h later underwent suction with CVPT. Percussion was performed by rhythmically clapping the chest, with a loose wrist and a cupped hand, transferring energy to the peripheral airways. The patient was then placed in a semi-sitting or lateral position, and percussion was applied on the affected area from the lower chest upward, and attempts were made to percuss all points. The mean percussion rate was 2 to 3 per second, which was applied to the lungs continuously for 2 to 4 min. In the CVPT, a series of fine oscillatory movements was performed by a vibrator (Thrive 717 Massager Chest Vibrator) on the chest wall during exhalation after taking a deep breath. The chest wall vibration technique was performed to move secretions towards the larger airways. Vital signs and rapid, shallow breathing index (RSBI) were recorded before the interventions and 5 and 25 min after the interventions in both groups. RSBI, which is also referred to as the ratio of respiratory rate to tidal volume (f/VT), is the most widely used predictor of weaning success36. Prior to the performance of the maneuvers within both experimental groups, the researcher charged with implementing the procedures participated in a concise educational program designed to familiarize him with the LST and CVPT protocols. In addition, an anesthesiologist, blinded to the study, positioned patients before the intervention based on their pulmonary radiologic findings (atelectasis or infiltration), ensuring the most affected lung area (the region exhibiting atelectasis or infiltration) was positioned superiorly37. Before and after suctioning, the patients were given 100% oxygen on a ventilator for 1 min to prevent hypoxia. A Nelaton catheter half the size of an endotracheal tube was used to suction the airways twice for 10 s on the same day at an interval of 3 h, applying a vacuum pressure of 80–120 mmHg using an open suction system applied via central suction to each patient.
Instruments
In this study, a checklist was used to collect data. This checklist consisted of two parts. The first part included patient demographic information such as age, gender, education level, marital status, occupation, and previous hospitalization history and the second part was a vital sign record sheet for patients; the second part of the checklist itself was divided into two parts: the first part included systolic and diastolic blood pressure, pulse rate, oxygen saturation, and RSBI before the intervention, and the second part included systolic and diastolic blood pressure, pulse rate, oxygen saturation, and RSBI 5 and 25 min after the intervention. In order to ensure the validity and reliability of the data collection tool, a Japanese ALPK2 dial sphygmomanometer was used to monitor the systolic and diastolic blood pressure of the patients. Also, a Jumper JPD-500E Fingertip Pulse Oximeter was used to monitor the patient’s oxygen saturation in the blood, a Puritan Bennett 840 ventilator was used to monitor the patient’s RSBI, and an analog watch was used to monitor the patient’s pulse rate.
Ethical considerations
Following a review process, the Ethics Committee of Shahrekord University of Medical Sciences granted approval for this study, which has been assigned the official registration number IR.SKUMS.REC.1401.127. Written informed consent from the patient’s legal guardians was secured only after a detailed explanation of the study’s aims and objectives, clearly outlining that participation was voluntary and that withdrawal from the study was possible at any stage without any repercussions.
Statistical analysis
Utilizing G*Power software, a sample size calculation was conducted considering the study by Own et al.31 which took into account an effect size of 0.8, a significance level (alpha error) of 0.05, a power of 0.80, and an anticipated 20% attrition rate, resulting in a final sample size of 64 participants (32 in each group). Data analysis was conducted based on the principle of intention to treat. All the statistical analyses were conducted using the Statistical Package for the Social Sciences for Windows (SPSS, version 18; IBM Corp, Armonk, NY, USA). The Shapiro–Wilk test was also performed to assess the normal distribution of the data. Data were expressed as means ± SD or as median with interquartile range (IQR) according to the distribution of the data. Group comparisons were made using independent samples t-test and paired samples t-test for normally distributed data, or Mann-Whitney U test and Wilcoxon signed-rank test for non-normally distributed data. Categorical variables were compared using Chi-square or Fisher’s exact test. A p-value less than 0.05 was considered statistically significant.
Results
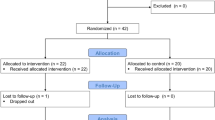
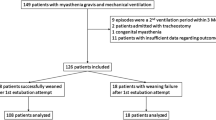
A total of 60 patients requiring MV were included in this study and divided into two groups, including LST (n = 30) and CVPT (n = 30). The CONSORT flow diagram of the participants is presented in Fig. 1. The mean age of patients in the LST and CVPT groups was 51.1 ± 15.44 and 51.66 ± 15.21, respectively. There was no significant difference between the two groups in terms of demographic variables (P > 0.05) (Table 1).
Consort flow diagram of the participants.
According to the results, at the baseline, there was a significant difference in the systolic blood pressure of the two groups at 5 min after the suctioning compared to before the suctioning (LST: 126.2 ± 15.2 vs. 121.7 ± 16.3; P < 0.05 and CVPT: 128.5 ± 9.6 vs. 123.7 ± 12.4; P < 0.05). Also, at the baseline, in the CVPT group, there was a significant difference in diastolic blood pressure at 5 min after the suctioning compared to before the suctioning (79.8 ± 9.9 vs. 75.2 ± 10.3; P < 0.05). However, the mean score of systolic and diastolic blood pressure did not show a significant difference between the two groups in the post-intervention phases compared to the baseline (P > 0.05). In addition, at the baseline, there was a significant difference in the respiratory rate of the two groups at 5 min after the suctioning compared to before the suctioning (LST: 94.4 ± 16.7 vs. 90.8 ± 16.2; P < 0.05 and CVPT: 94.6 ± 12.5 vs. 90.7 ± 13.7; P < 0.05). However, the mean score of the respiratory rate did not show a significant difference between the two groups in the post-intervention phases compared to the baseline (P > 0.05) (Table 2).
The results of the present study showed that in the LST group, there was a significant difference in the oxygen saturation scores at 5 min after the intervention compared to the 5 min before the intervention (96 (95–97) vs. 95 (94.75–96); P < 0.05). However, in other phases of the study, the oxygen saturation scores did not show a significant difference between the two groups (P > 0.05). Also, the findings of our study reported that there was a significant difference between the two groups in terms of RSBI scores at the baseline (LST: 38.5 (36.2–44.1) vs. CVPT: 35.2 (33.7–38); P < 0.05), 5-minutes after the intervention (LST: 36.6 (34.3–44) vs. CVPT: 34.8 (32.2–36.9); P < 0.05) and 25-minutes after the intervention (LST: 37.1 (32.5–44.4) vs. CVPT: 34 (32.5–35.8); P < 0.05). Moreover, after adjusting for the effect of baseline values of systolic and diastolic blood pressure, respiratory rate, and RSBI, the results of the Multivariate analysis of variance indicated no significant difference in the post-intervention values of the two groups (P > 0.05) (Table 3).
Discussion
The present study was conducted to compare the effects of two types of physiotherapy techniques on selected weaning indices of patients requiring MV. The results of this study showed that there was no significant difference in the systolic and diastolic blood pressure, respiratory rate, and oxygen saturation values of both groups at baseline and 5 and 25 min after the intervention. The results of the study by Zeng et al. found that after chest physiotherapy there was no significant difference in vital signs and respiratory parameters (tidal volume (VT), respiratory rate (RR), peak airway pressure (Ppeak), and mean airway pressure (Pmean)) of patients requiring MV in both groups compared to the baseline and only a significant difference was observed in the oxygen saturation values of patients in the intervention group38, which is in agreement with the present study findings. However, the findings of other studies revealed that chest physiotherapy, including various types, including squeezing39,40 and chest vibration and percussion41,42, was effective in improving the hemodynamic and respiratory parameters of patients requiring MV. The difference in results of the studies may be attributed to the variation in the type of physiotherapy methods, sample size, age group, and duration of the intervention and the study.
Given the results of the current study, there was a significant difference in the RSBI scores of the LST and CVPT groups at the baseline and 5 and 25 min after the intervention. The effectiveness of physiotherapy techniques on ventilator weaning indices of patients requiring MV was explored in the previous studies. For example, Yang et al. (2010) and Farghaly et al. (2019) in their studies investigated the efficacy of physical therapy intervention on ventilator weaning indices of patients requiring MV and showed that there were no significant differences in the RSBI values of these patients after the intervention compared to the baseline43,44. Their studies yielded different results than ours, possibly because of the inadequate impact that physiotherapy interventions have on patients requiring MV; the patients may not respond properly to these interventions because of their clinical characteristics and condition.
Although, another study conducted by Yazdani et al. investigated the effectiveness of the manual hyperinflation (MHI) technique on weaning indices of patients with abdominal surgeries and indicated that there was a significant difference in the RSBI values of the intervention and control groups at 5 and 25 min after the intervention45, which is consistent with the present study results.
The findings of this study also demonstrated that the LST was more effective than the CVPT in improving RSBI as a weaning index for patients requiring MV. According to the physiological basis, LST involves gentle, sustained chest compressions to help restore homogeneous lung inflation, whereas conventional techniques like postural drainage, percussion, and vibration (PDPV) use gravity, manual percussion, and vibration to move mucus46. In their study, Wong et al. showed that LST was more effective for correcting respiratory parameters and re-expansion of lung atelectasis in pre-term neonates. However, there was no significant difference between the two groups in terms of hemodynamic parameters (systolic and diastolic blood pressure and oxygen saturation)32, which was consistent with the present study. Also, the results of the study by Own et al. found that both methods of chest percussion and squeezing were effective in improving the oxygenation parameters (Pulmonary oxygenation capacity index (PaO2/FiO2 readings), SpO2, PaO2, and FiO2) and ventilatory and respiratory parameters (tidal volume, amount and viscosity of secretions, respiratory inspection, and auscultation) of patients requiring MV31. The difference in results of the studies may be attributed to the different inclusion criteria and different target populations in these studies.
In addition, Khalil et al. in their study compare the effects of MHI and expiratory rib cage compression (ERCC) on arterial blood gas parameters in patients requiring MV and demonstrated a significant difference in ABG parameters before and after MHI and ERCC47.
One of the limitations of this study was the small sample size, which could affect the results because the study was conducted at one of the general educational hospitals located in Shahrekord City. Therefore, it is suggested that future studies in this field be done with a larger sample size. The use of a convenience sampling method in this study was also a major limitation because it is associated with a significant risk of selection bias. It is recommended that future studies include other sampling methods. Since this study was not a multi-center trial, it led to low generalizability of the study results. Furthermore, the inherent design of the study precluded blinding of the patients and the therapist; consequently, only the data assessor remained unaware of the treatment assignments. In general, it is suggested that future studies investigate the effects of other physiotherapy methods on the weaning indices of patients requiring MV and compare the effects of these methods with each other.
Conclusion
The results demonstrated that LST outperformed CVPT in enhancing the RSBI, which serves as a weaning index for patients requiring MV. This suggests that LST may facilitate earlier weaning and extubation for these patients. It is recommended that future studies examine the impact of chest physiotherapy and its various types on early extubation of patients requiring MV more thoroughly.
Data availability
Upon request, the corresponding authors will make available the datasets that have been utilized and analyzed in this current research study.
References
Walter, K. Mechanical ventilation. Jama 326 (14), 1452 (2021).
Grasselli, G. et al. Mechanical ventilation parameters in critically ill COVID-19 patients: a scoping review. Crit. Care. 25 (1), 115 (2021).
Orso, D. et al. Mechanical ventilation management during mechanical chest compressions. Respir. Care. 66 (2), 334–346 (2021).
Trudzinski, F. C. et al. Risk factors for prolonged mechanical ventilation and weaning failure: a systematic review. Respiration 101 (10), 959–969 (2022).
Bissett, B., Gosselink, R. & Van Haren, F. M. P. Respiratory muscle rehabilitation in patients with prolonged mechanical ventilation: a targeted approach. Annual Update in Intensive Care and Emergency Medicine. 2020:595–609. (2020).
Ferrando, C., Vallverdú, J., Zattera, L., Tusman, G. & Suárez-Sipmann, F. Improving lung protective mechanical ventilation: the individualised intraoperative open-lung approach. Br. J. Anaesth. 281–287. (2024).
Pinto, C. B., Leite, D., Brandão, M. & Nedel, W. Clinical outcomes in patients undergoing invasive mechanical ventilation using NAVA and other ventilation modes-A systematic review and meta-analysis. J. Crit. Care. 76, 154287 (2023).
Rubulotta, F. et al. Mechanical ventilation, past, present, and future. Anesth. Analgesia. 138 (2), 308–325 (2024).
Taylor, C. Intensive care unit acquired weakness. Anaesth. Intensive Care Med. 22 (2), 81–84 (2021).
Lippi, L. et al. Efficacy of physiotherapy interventions on weaning in mechanically ventilated critically ill patients: a systematic review and meta-analysis. Front. Med. 9, 889218 (2022).
Surani, S. et al. Weaning from mechanical ventilator in a long-term acute care hospital: a retrospective analysis. Open. Respiratory Med. J. 14, 62–66 (2020).
Sklar, M. C. et al. Association of low baseline diaphragm muscle mass with prolonged mechanical ventilation and mortality among critically ill adults. JAMA Netw. Open. 3 (2), e1921520 (2020).
Windisch, W. et al. Prolonged weaning from mechanical ventilation: results from specialized weaning centers—a registry-based study from the WeanNet initiative. Deutsches Ärzteblatt Int. 117 (12), 197 (2020).
Pelosi, P. et al. Personalized mechanical ventilation in acute respiratory distress syndrome. Crit. Care. 25, 1–10 (2021).
Ríaseos, L. E. & Garcia-Perdomo, H. A. Risk factors associated with failed weaning from mechanical ventilation in septic patients admitted to an intensive care unit: a case-control study. Revista De La. Facultad De Med. 70 (4), e94464 (2022).
Huang, H-Y., Huang, C-Y. & Li, L-F. Prolonged mechanical ventilation: outcomes and management. J. Clin. Med. 11 (9), 2451 (2022).
Carda, S. et al. The role of physical and rehabilitation medicine in the COVID-19 pandemic: the clinician’s view. Annals Phys. Rehabilitation Med. 63 (6), 554–556 (2020).
Carda, S. et al. COVID-19 pandemic. What should physical and rehabilitation medicine specialists do? A clinician’s perspective. Eur. J. Phys. Rehabil. Med. 56 (4), 515–524 (2020).
Huang, D. et al. Effect of mechanical ventilation and pulmonary rehabilitation in patients with ICU-acquired weakness: a systematic review and meta-analysis. Annals Palliat. Med. 10 (9), 9594606–9599606 (2021).
Jin, Y., Di, J. & Wang, X. Early rehabilitation nursing in ICU promotes rehabilitation of patients with respiratory failure treated with invasive mechanical ventilation. Am. J. Translational Res. 13 (5), 5232–5239 (2021).
Liu, K. et al. Implementation of the ABCDEF bundle for critically ill ICU patients during the COVID-19 pandemic: a multi-national 1-day point prevalence study. Front. Med. 8, 735860 (2021).
Shkurka, E., Wray, J., Peters, M. & Shannon, H. Chest physiotherapy for mechanically ventilated children: a systematic review. J. Pediatr. Intensive Care. 13 (02), 109–118 (2024).
Main, E. & Rand, S. Conventional chest physiotherapy compared to other airway clearance techniques for cystic fibrosis. Cochrane Database Syst. Reviews 2023(5).
Battaglini, D. et al. Chest physiotherapy: an important adjuvant in critically ill mechanically ventilated patients with COVID-19. Respir. Physiol. Neurobiol. 282, 103529 (2020).
Abdelrazek, M. A., Kassem, H., AbuShady, M. & Heneidy, W. Reflex rolling versus lung squeezing techniques on pulmonary functions in premature neonate with pneumonia. Benha Int. J. Phys. Therapy. 2 (2), 101–108 (2024).
Mishra, R. & Samuel, A. J. Thoracic squeeze technique: an advanced chest physiotherapy technique for hospitalized neonates. Indian J. Thorac. Cardiovasc. Surg. 34 (3), 449–450 (2018).
Basith, A. et al. A comparative on the effects of thoracic squeeze technique versus manual diaphragm release technique on sputum clearance among patient with chronic obstructive pulmonary disease. Indian J. Physiotherapy Occup. Therapy. 18 (5), 381–384 (2024).
Zhang, W., Taihuan, W., Zhang, B. & Luo, H. Multiple squeezing based on velocity synchronous chirplet transform with application for bearing fault diagnosis. Mech. Syst. Signal Process. 188, 110006 (2023).
Audsavachulamanee, B. et al. The Flow-Pressure and cardiopulmonary responses of manual chest percussion with different ranges of Oscillation frequency in healthy subjects. Trends Sci. 21 (3), 7345 (2024).
Papadopoulou, O. et al. The effectiveness of respiratory physiotherapy in children with severe respiratory problems: literature review. Int. J. Sci. Res. Archive. 12 (2), 103–109 (2024).
Own, D. G., Mohamed, N. T., ProfOsama Hassan, A. S., ProfFatma, A. & El-Fattah, A. R. Effect of chest percussion and squeezing on respiratory status for mechanically ventilated patients. Int. J. Novel Res. Healthc. Nurs. 7 (3), 119–130 (2020).
Wong, I. & Fok, T. F. Randomized comparison of two physiotherapy regimens for correcting atelectasis in ventilated pre-term neonates. Hong Kong Physiotherapy J. 21 (1), 43–50 (2003).
World Medical, A. World medical association declaration of Helsinki: ethical principles for medical research involving human subjects. Jama 310 (20), 2191–2194 (2013).
Schulz, K. F., Altman, D. G. & Moher, D. CONSORT 2010 statement: updated guidelines for reporting parallel group randomised trials. J. Pharmacol. Pharmacotherapeutics. 1 (2), 100–107 (2010).
Gosselink, R. et al. Physiotherapy in the intensive care unit. Neth. J. Crit. Care. 15 (2), 66–75 (2011).
Rittayamai, N., Ratchaneewong, N., Tanomsina, P. & Kongla, W. Validation of rapid shallow breathing index displayed by the ventilator compared to the standard technique in patients with readiness for weaning. BMC Pulm. Med. 21 (1), 310 (2021).
Kohan, M., Mohammad, T. N., Rahimi, E., Javadi, M. & Momtahen, H. The effects of expiratory rib cage compression before endotracheal suctioning on airway-secretion removal in mechanically ventilated patients. Iran. J. Nurs. Res. 4 (12–13), 55–62 (2009).
Zeng, H., Zhang, Z., Gong, Y. & Chen, M. Effect of chest physiotherapy in patients undergoing mechanical ventilation: a prospective randomized controlled trial. Chin. Crit. Care. 29 (5), 403–406 (2017).
Aherrao, S., Sharath, H. V. & Sharath, H. V. Effect of thoracic squeezing technique and expiratory flow increase technique on neonates with neonatal respiratory distress syndrome: a case report. Cureus 16(9), (2024).
Thenmozhi, P., Dineshkumar, P., Bhuvaneswari, G., Minolin, T. M. & Tamilselvi, S. Thoracic squeezing on airway secretion and respiratory parameters in mechanically ventilated patients: an interventional study. J. Educ. Health Promotion. 14 (1), 69 (2025).
Ahmed, I. M. Effect of mechanical chest vibration during chest physiotherapy on ventilator parameters and oxygen saturation in mechanically ventilated patients. Int. Egypt. J. Nurs. Sci. Res. 4 (2), 199–211 (2024).
Chen, Y-C. et al. Using chest vibration nursing intervention to improve expectoration of airway secretions and prevent lung collapse in ventilated ICU patients: a randomized controlled trial. J. Chin. Med. Association. 72 (6), 316–322 (2009).
Farghaly, A., Ismail, S. M. & El-Sheikh, M. S. N. Efficacy of manual hyperinflation with expiratory rib cage compression on weaning from mechanical ventilation. New. York Sci. J. 12 (9), 55–63 (2019).
Yang, P-H. et al. Outcome of physical therapy intervention on ventilator weaning and functional status. Kaohsiung J. Med. Sci. 26 (7), 366–372 (2010).
Yazdani, M., Malekzadeh, J., Sedaghat, A. & Mazlom, S. R. The effects of manual lung hyperinflation on pulmonary function after weaning from mechanical ventilation among patients with abdominal surgeries: randomized clinical trial. J. Caring Sci. 10 (4), 216 (2021).
Bush, A. et al. Hodson and Geddes’ Cystic Fibrosis. CRC (2023).
Khalil, N. S., Ismaeel, M. S., Askar, A. H. & Sayed, M. S. Effects of manual hyperinflation with rib cage compression and endotracheal suctioning on arterial blood gas parameters in mechanically ventilated patients at a university hospital, Egypt. Egypt. J. Bronchol. 15, 1–7 (2021).
Acknowledgements
This article’s content originates from a nursing master’s thesis, a work that received approval from the Research and Ethics Committee at the Shahrekord University of Medical Sciences. The researchers wish to express their profound thanks to the Dean of the nursing school and the highly respected Research Vice President of Shahrekord University of Medical Sciences, acknowledging their vital role in enabling and supporting this important research work.
Funding
The research was funded by a grant from Shahrekord University of Medical Sciences, which covered all stages of the project, including the design of the study, data gathering and analysis, interpretation of findings, and the preparation of the manuscript for publication.
Author information
Authors and Affiliations
Contributions
Design of the study: F.A., AM.N., R.M., SH.E., F.Y.; data collection: F.A., F.Y.; analysis and interpretation of data: S.KH., AM.N; manuscript preparation: F.A., AM.N., R.M.; manuscript revision: F.A., AM.N., R.M. All authors checked and confirmed the final manuscript before submission. The author(s) read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval and consent to participate
A detailed explanation was given to the patient’s legal guardians, covering the study’s objectives, the protection of patient privacy and confidentiality, and the voluntary nature of participation, including the right to withdraw at any time; this was followed by the signing of consent forms prior to study involvement. Furthermore, the research project received approval from the Review Board of Shahrekord University of Medical Sciences (IR.SKUMS.REC.1401.127).
Consent for publication
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Azimi, F., Nazari, A.M., Yadollahi, F. et al. The comparison of two types of physiotherapy techniques on selected weaning indices of patients requiring mechanical ventilation: a single blind randomized controlled trial. Sci Rep 15, 18489 (2025). https://doi.org/10.1038/s41598-025-03701-5
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-03701-5