Abstract
The evidence linking meat intake to early menarche has been contradictory. We aimed to estimate meat intake and time trends among Chinese girls, and to assess the associations between long-term meat intake and menarche. This study used seven rounds of data from the China Health and Nutrition Survey, and 5175 girls aged 6–17 years were analyzed. Cox proportional hazard and restricted cubic spline models were used to analyze the associations and dose-response relationships between meat intake and menarche. Over the 15-year period, total meat intake almost doubled, and meat subtype consumption increased among Chinese girls. Increased total meat, red meat, white meat and poultry intake was significantly associated with the risk of earlier menarche. When extreme tertiles were compared, the multivariable-adjusted hazard ratios (95% confidence intervals) for total meat, red meat, white meat and poultry were 1.28 (1.06–1.54), 1.19 (1.01–1.42), 1.23 (1.02–1.47) and 1.23 (1.06–1.44), respectively. An approximately U-shaped association was observed: compared to the reference (75 g/day), early menarche risk decreased at lower intakes (25–75 g/day), showed no association at moderate intakes (75–175 g/day), and increased significantly at higher intakes (> 175 g/day). Increased long-term meat consumption was associated with an increased risk of early menarche in Chinese girls.
Similar content being viewed by others
Background
A shift toward earlier onset of puberty is of major concern because of its long-term impact on multiple chronic diseases in adulthood, e.g. coronary heart disease1, diabetes/impaired glucose tolerance2,3, and hormone-related cancers2,4. A prospective cohort study with 264, 546 women revealed that early age at menarche is associated with 16% higher all-cause mortality5. Thus, factors influencing puberty timing have been increasingly acknowledged.
Meat is an important part of people’s diets and is a major source of high-quality protein, fat, and vital vitamins and essential minerals. Overall meat intake has continued to rise both in developed and developing countries6,7,8 due to increasing economic development. Increasing evidence has shown that meat consumption is related to puberty timing, but the findings are not entirely consistent9,10,11,12. Prospective studies predominantly based in America9, England13 and Korea14 have consistently reported a positive association between red meat intake and the risk of early menarche, whereas cross-sectional studies conducted in China11 or Iran12 reported a lack of an association. Furthermore, evidence linking processed red meat, poultry or fish intake and pubertal development is limited and remains uncertain. Some epidemiological studies have shown that greater fatty fish intake frequency is associated with later menarcheal age9 whereas others have not reported any associations11,12. A recent cross-sectional study reported that higher consumption of poultry was associated with an earlier age at menarche among Chinese schoolgirls11. Notably, most of these existing studies focused on meat intake frequency via semiquantitative food frequency questionnaires, which cannot reflect the actual amount of meat consumed. As different types of meat have distinct fatty acids and essential minerals, they can exert different metabolic effects on health at different stages of growth, probably including the progression of pubertal timing. Given that a noteworthy secular trend of earlier menarche has been observed in Chinese girls15 investigations on the determinants of menarche in this population are warranted.
To address these foregoing research gaps, the present study aimed to investigate the longitudinal associations between meat intake during prepubertal childhood and menarcheal onset in Chinese girls using collected data from the China Health and Nutrition Survey (CHNS). First, we estimated meat intake and time trends among Chinese girls aged 6–17 years using a series of cross-sectional dietary data from 6 CHNS cycles, covering 15 years from 1997 to 2011. Second, we explored the prospective associations between meat intake (total meat, red meat, white meat, poultry, and fish/shellfish) and timing of menarche using longitudinal data of CHNS.
Methods
Study sample
The CHNS is an ongoing longitudinal cohort study in China that was initiated in 1989. The survey employed a multistage random-cluster process to obtain a sample of over 30,000 individuals in 15 provinces and municipal cities. Data on economic, sociodemographic, nutritional, lifestyle and health issues were collected. Details on the study design and protocol have been documented elsewhere16. The CHNS protocol was approved by the Institutional Review Board at the University of North Carolina, the National Institute of Nutrition and Health, and the Chinese Center for Disease Control and Prevention. All methods were performed in accordance with the relevant guidelines and regulations. Parents provided written informed consent for their children’s participation in the survey.
This investigation used data across 7 waves of CHNS (1997, 2000, 2004, 2006, 2009, 2011 and 2015), including data from Chinese girls aged 6–17 years. In total, 5199 girls completed at least 1 valid 24-hour diet recall between the 1997 and the 2015 survey. Among them, 24 participants with implausible energy intake (< 400 kcal/d or > 4000 kcal/d) were excluded. Thus, 5175 girls were included in the analysis of trends in meat intake. To explore prospective associations between long-term meat intake and timing of menarche, girls who had at least one dietary assessment and who had at least one follow-up visit for menarche thereafter were included in the second analysis. Thus, we excluded 1137 girls without data on menarcheal onset and 2605 girls without dietary data prior to menarche onset. Finally, 1433 girls were eligible for the analysis of associations between long-term meat intake and menarche (Fig. 1).
Flowchart for the study sample.
Dietary intake assessment and meat intake
The dietary intake data in the CHNS were collected via consecutive three-day 24 h dietary recalls to collect individual consumption data. Moreover, seasons such as oil and salt were weighed by a trained investigator at the household level during the same days. Girls aged 12 years or older completed the dietary interview on their own. For girls aged 6 to 11 years, their parents or guardians provided the information on food consumption at home, whereas girls provided the dietary intake information away from home. The majority of school-aged girls in the CHNS 1997–2011 had a complete three-day 24-h recalls (n = 5159, 99.7%); the remainder had either one or two recalls (n = 6 and n = 10, respectively). The average daily intake of total meat, red meat (including unprocessed and processed red meat), white meat (including poultry and and fish/shellfish), poultry, fish/shellfish, and total energy and nutrient intakes were calculated by corresponding versions of the Chinese Food Composition Table (FCT) from consecutive three-day 24 h dietary recalls for each round17,18,19,20 i.e., FCT 1991 for 1997 and 2000 surveys and FCT 2002, FCT 2004 and 2009 (combined) for 2004, 2006, 2009, and 2011 dietary surveys.
Assessment of menarche
Girls aged 8 years or older were asked whether they had begun menstruating at each assessment, and if they had, the month and year of their first menstrual period were recorded. If they provided different menarcheal ages in different waves, only the first reported menarcheal age in the panel data was used for analysis to reduce potential recall bias.
Covariate assessment
The following variables were reported by girls or their parents: date of birth, ethnicity, geographic region, residency, paternal and maternal educational level, and annual household income per capita. Girls’ weight, height, waist circumference and hip circumference were measured at baseline at each visit by research assistants according to standard protocols16. Body mass index (BMI) and waist-to-hip ratio (WHR) were calculated. BMI Z-scores were calculated for each participant using the Chinese reference curves21. Overweight was defined according to the Working Group on Obesity in China (WGOC standard) BMI cutoffs for children22. Maternal or paternal BMI was calculated from self-reported values of height and weight, and was divided into three groups (< 18.5 kg/m2, 18.5–23.9 kg/m2, and ≥ 24.0 kg/m2).
Statistical analysis
Continuous variables are presented as the means (standard deviations [SDs]) or medians (interquartile ranges [IQRs]), and categorical variables are presented as frequencies and percentages. ANOVA, the Kruskal‒Wallis test and the chi‒square test were used to examine differences in characteristics between different groups. The trends of total meat and all kinds of meat intake over time were fitted with a general linear regression model.
Cox proportional hazard regression models were used to identify the associations of meat intakes and with the event of menarche. Meat intakes were calculated as cumulative means to represent long-term diet and minimize within-person variation. For instance, for a participant with three rounds of dietary data collected in 1997, 2004, and 2009, the cumulative average meat intake was calculated as the arithmetic mean of the individual’s meat intake values across these three waves: (meat intake in 1997 + meat intake in 2004 + meat intake in 2009)/3. The consumption of total meat, red meat, white meat, and poultry were grouped by tertile: tertile 1 (T1), tertile 2 (T2), and tertile 3 (T3). Given that approximately 50% of participants reported no fish/shellfish consumption, we established a distinct non-consumer reference group (0 g/day). For the remaining consumers of fish/shellfish, we subsequently categorized intake into two groups using the weighted median distribution: < median and ≥ median. Hazard ratios (HRs) and their 95% confidence intervals (CIs) were calculated by comparing T2 and T3 to T1 (as the reference category). Cox regression models considered covariates of known or suspected risk factors for early menarche. Multiple imputation was used to impute missing covariates. Each potential confounder was initially considered separately and included if it was associated with both the meat intake and the timing of menarche and substantially altered the estimate by more than 10%. Thus, model 1 was adjusted for geographic region, ethnicity and maternal education level; model 2 was further adjusted for energy intake. In the final model, the BMI Z-score at baseline was also included because it has been proposed that childhood obesity may be related to menarcheal onset. Additionally, the dose-response relationship between total meat intake and menarche timing was analyzed using the restricted cubic spline (RCS) model. All analyses were performed with SAS procedures (version 9.4, 2014, SAS Institute Inc., Cary, NC, USA) and R software (Version 4.3.2, R Foundation for Statistical Computing, Vienna, Austria ). All P values were two-sided, and statistical significance was determined at a P-value < 0.05.
Results
Trends in meat intake
In total, 5175 girls were included in the first analysis. The mean age of the girls was 11.4 ± 3.2 y. Table 1 shows the meat consumption of the Chinese girls from 1997 to 2011. Total meat consumption almost doubled (from 50.0 to 96.7 g/day; difference, + 29.6 [95% CI, 22.1–37.0] g/day; P for trend < 0.0001). Red meat consumption significantly increased from 33.3 to 53.3 g/day (difference, + 15.2 [95% CI, 10.4–20.1] g/day; P for trend < 0.0001), mainly unprocessed meats (difference, + 12.9 [95% CI, 8.2–17.7] g/day; P for trend < 0.0001). White meat consumption significantly increased from 0 to 26.7 g/day (difference, + 14.3 [95% CI, 9.7–19.0] g/day; P for trend < 0.0001), mainly poultry (difference, + 10.7 [95% CI, 7.5–13.9] g/day; P for trend < 0.0001). The median intake of fish/shellfish remained consistently low from 1997 to 2011, with a median value of 0 (0, 33.3) g/day. However, when comparing 2011 to 1997, the absolute difference in intake was 3.6 g/day (95% CI: 0.3, 7.0), suggesting a marginal but significant increase over the 14-year period (P for trend = 0.008).
Baseline characteristics by tertile of meat consumption
The basic demographics and characteristics of Chinese school-aged girls by the tertile of total meat consumption are presented in Table 2. Girls with higher meat intake were more likely to experience menarche at an earlier age, to live in the city, and to have a more highly educated mother or father (all P < 0.0001). Girls with higher meat intake consumed significantly more energy, protein, and fat and fewer carbohydrates (all P < 0.0001). Higher meat intake was associated with a lower waist-to-hip ratio (P < 0.0001).
Cumulative averages of meat intake and menarche
Among the 5175 girls, 1433 girls aged 6–13 y (mean age: 8.2 ± 1.8 y) who had at least one complete dietary data and follow-up visit for menarche onset thereafter were included in the second analysis. Compared with girls who were excluded, those included in the second analysis were younger at baseline. Consequently, they demonstrated significantly lower values across multiple nutritional and anthropometric measures, i.e., energy, carbohydrate, protein and fat; weight Z-score, height Z-score, waist circumference, hip circumference, and waist to hip ratio (data not shown). Cox proportional hazard regression models revealed positive associations of total meat, red meat, white meat, and poultry intake with the risk of earlier menarcheal onset (Table 3), which remained significant after adjustment for total energy intake, ethnicity, residency, maternal education level, and BMI Z-score in the final model. Compared with girls in the lowest tertile of total meat intake, girls in the highest tertile had a 28% higher risk of menarcheal onset at an earlier age (adjusted HR: 1.28, 95% CI: 1.06–1.54, P for trend = 0.01). Similarly, girls with higher red meat or white meat intake were more likely to experience menarche at an earlier age (red meat: adjusted HR: 1.19, 95% CI: 1.01–1.42, P for trend = 0.045; white meat: adjusted HR: 1.23, 95% CI: 1.02–1.47, P for trend = 0.03). We also conducted separate analyses according to kinds of white meat. Positive associations of poultry and fish/shellfish intake with menarche were found (poultry: HR: 1.25, 95% CI: 1.07–1.46, P for trend = 0.005; fish/shellfish: HR: 1.22, 95% CI: 1.02–1.45, P for trend = 0.03). However, no significant association was observed for fish/shellfish after full adjustment for potential confounders in the multivariate-adjusted model (adjusted HR: 1.11, 95% CI: 0.93–1.33, P for trend = 0.22).
Dose-response relationship between total meat intake and menarche
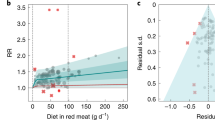
RCS analysis revealed a U-shaped association between total meat intake and menarche (Fig. 2). The overall and nonlinear associations between meat intake and the risk of menarche were statistically significant (P = 0.006 and P = 0.048). Using 75 g/day of meat intake as the reference, we observed a significantly reduced risk of early menarche for intakes between 25 and 75 g/day. No significant association was found for consumption between 75 and 175 g/day. However, the risk of early menarche increased significantly with meat intake over 175 g/day.
Dose-response relationship of total meat intake with menarche. RCS, restricted cubic spline. The RCS model was used to examine the dose-response relationship between total meat intake and meanarche timing. The data shown are HRs and 95% CIs adjusted for geographic region, ethnicity, maternal education level, energy intake and BMI Z-score at baseline.
Discussion
In this nationally representative cohort study, we found that from 1997 to 2011, meat consumption increased among Chinese school-aged girls, especially the consumption of unprocessed red meat and poultry. The intake of fish has remained low, with only a small increase over time. Girls with higher intakes of total meat, red meat, white meat, and poultry, experienced their menarcheal timing at an earlier age. These relationships were independent of potential sociodemographic confounders and prepubertal body size.
The increasing trend in different types of meat among Chinese girls could be due to the dietary transition that China has undergone over the past 20 years25. Wang et al. reported that the consumption rates of meat and meat subtypes among Chinese adults increased from 1991 to 20117. Like in adults, red meat, mainly pork, is the main type of meat consumed by girls, followed by other meats and poultry6,7. On the basis of the current high rate of meat consumption worldwide8, the impacts of long-term meat intake on type 2 diabetes6, elevated blood pressure26 and cancer risk27,28,29 have been widely investigated. However, the evidence for an overall association of meat and meat subtypes with children’s growth is not clear enough.
Previous studies have shown that the frequency of meat intake is associated with age at menarche9,11. Our study substantially extends previous findings by examining the amounts of specific categories of meat by using the cumulative average values of meat intake. The negative associations of total meat and red meat with age at menarche in our study are in agreement with the findings of a previous study9. The reasons for the adverse effects of meat on the timing of menarche have not been clarified. It is usually assumed that there are several factors that act individually or in combination. An oversupply of zinc found in red meat could signal the body to initiate puberty30,31. Another mechanism may involve the production of the toxic substances, such as heterocyclic amines produced during the preparation of red meat at high temperatures32. Nevertheless, no significant correlation was observed between meat consumption and menarche in some studies10,11 which, in our opinion, may be related to the timing of dietary assessment or dietary assessment methods. Whereas dietary assessment in our study was conducted repeatedly in girls with a mean age of 8.2 y using three-day 24 h dietary recalls, girls in the US study had a mean age of 11.3 y at baseline, and their meat consumption was calculated with the use of self-administered semiquantitative food frequency questionnaires9. Given that the habitual intake of children may not be stable during childhood, cumulative consumption is a more accurate reflection of long-term meat intake than a one-time dietary assessment.
In our study, the dose-response relationship between total meat intake and menarche was explored. An approximately U-shaped relationship was found for total meat intake and the risk of early menarche. Using 75 g/day of meat intake as the reference, we observed a significantly reduced risk of early menarche for intakes between 25 and 75 g/day. No significant association was found for consumption between 75 and 175 g/day. However, the risk of early menarche increased significantly with meat intake over 175 g/day. The findings of our study are consistent with the recommended intake of meat in the Chinese Dietary Guidelines (version 2022), which suggests a recommended meat intake for children aged 6–13 y of 280–350 g/week (i.e., 40–70 g/d).
Notably, we found that white meat (mainly poultry) intake was related to an earlier age at menarche. Our results are in agreement with findings from a prospective study of 241 Iranian girls (mean age at baseline: 9.6 y)12 and a cross-sectional study of 986 Chinese girls (mean age: 11.97 y)11 which revealed that girls who consumed poultry had a 35-39% greater risk of menarche at an earlier age. The potential explanation for these results could be related to the poultry intake including the intake of fried chicken (additional adjustment for total fat intake in our study nullified the statistical significance of the association, data not shown)27 or hormone residues, such as diethylstilboestrol, in poultry33. Poultry products, particularly those from industrial farming, may contain residual growth-promoting hormones or endocrine-disrupting chemicals (EDCs) that mimic endogenous sex hormones. These substances can prematurely activate the hypothalamic-pituitary-gonadal (HPG) axis by binding to estrogen or androgen receptors, thereby accelerating menarcheal timing34. To our knowledge, poultry has been less studied in relation to the health of children. Recent studies have revealed positive associations between poultry intake and blood pressure35, incident cardiovascular disease27, and pancreatic cancer risk36. Thus, the influences of poultry intake on human health, especially the health of children, require further investigation.
Fish/shellfish are an abundant source of marine omega-3 polyunsaturated fatty acids with anti-inflammatory properties and were recently reported to have a beneficial effect on dysmenorrhea pain37. Jansen et al. reported that girls with tuna/sardine intake > 1 time/week (n = 75, 16.6%) had a later age at menarche (HR = 0.62) than those with intake < 1 time/month (n = 144, 31.2%)9. However, no significant correlation was observed in our study or other studies12. A possible reason is that the fish/shellfish consumption in CHNS girls may be too low (average intake: 4.2 g/day) to detect a significant association with menarche. In fact, approximately half of the girls did not consume fish or shellfish during the three-day 24-hour dietary interview in our study. As the consumption of fish has been gradually increasing over time, further research is needed to address the prospective effects of fish intake on menarcheal timing in the Chinese girl population.
For the analysis of temporal trends in meat consumption, this study’s strengths included nationally representative sample and investigation of the trends of various meat subtypes. For the examination of meat intake-menarche associations, the strengths of our study include prospective longitudinal follow-up (median: 4.0 years) and use of cumulative consumption metrics to capture long-term meat consumption, which accounted for within-subject variability. To our knowledge, this is the first comprehensive dose-response analysis of meat intake and menarche timing in Chinese girls. Furthermore, the comprehensive and detailed data allowed us to simultaneously take a number of potential confounders or mediators into account and thus to reliably examine the relationships of meat and meat subtypes with menarcheal onset.
Some limitations of our study should also be noted. First, 24-h dietary recall cannot generally evaluate usual dietary intake, but the average intake from three 24-h dietary recalls and the cumulative mean of meat intake can reduce random variation and provide estimates close to usual meat consumption. Second, as our temporal trend analysis relies on repeated cross-sectional data, it captures population-level shifts in meat consumption rather than individual dietary trajectories. Third, our assessment of meat-puberty associations relied on menarche as the outcome measure, which reflects a late-stage pubertal milestone rather than the initiation of puberty. The effects of meat intake on earlier events of puberty (e.g., age at Tanner stage 2 for breast development in girls or initiation of gonadal growth in boys) may differ from those on menarche. Fourth, there may be some unmeasured confounding factors (e.g., maternal age at menarche) in this study, although as many potential covariates as possible have been adjusted by us.
Conclusions
Our study revealed continued growth trends in total meat and meat subtype intake among girls in China over 15 years from 1997 to 2011. Higher intakes of total meat, red meat, white meat, and poultry, but not fish/shellfish, were associated with an increased risk of early menarche. An approximately U-shaped association between total meat intake and the risk of early menarche was observed in our study. A total meat intake of more than 175 g/day might be a threshold point for experiencing menarche at an early age. Further research is needed to address the prospective effects of meat intake on earlier stages of pubertal development in the Chinese girl population.
Data availability
The data supporting the findings of this study are available from CHNS (https://www.cpc.unc.edu/projects/china/data/datasets).
Abbreviations
- CHNS:
-
China Health and Nutrition Survey
- FCT:
-
food composition table
- BMI:
-
body mass index
- WHR:
-
waist-to-hip ratio
- WGOC:
-
Working Group on Obesity in China
- SD:
-
standard deviation
- IQR:
-
interquartile range
- HR:
-
hazard ratio
- CI:
-
confidence interval
- T:
-
tertile
- RCS:
-
restricted cubic spline
References
Ota, K. et al. Relationships between age at menarche and risk of cardiovascular disease mortality among Japanese women: The Japan collaborative cohort study for evaluation of Cancer risk (JACC) study. J. Atheroscler Thromb. 30, 247–254 (2023).
Lee, J. S. et al. Long-term health outcomes of early menarche in women: an umbrella review. QJM 115, 837–847 (2022).
Jung, H. et al. Relationship between age at menarche and metabolic diseases in Korean postmenopausal women: The Korea National health and nutrition examination survey 2016–2018. PloS One. 18, e0280929 (2023).
Lv, Y. et al. Health outcomes of age at menarche in European women: A two-sample Mendelian randomization study. Postgrad. Med. J. 99, 993–999 (2023).
Liang, Z. et al. Joint associations of actual age and genetically determined age at menarche with risk of mortality. JAMA Netw. Open. 4, e2115297 (2021).
Liu, M. et al. Trajectories of meat intake and risk of type 2 diabetes: findings from the China health and nutrition survey (1997–2018). Nutrients 15, 3277 (2023).
Wang, Z. H. et al. Secular trends in meat and seafood consumption patterns among Chinese adults, 1991–2011. Eur. J. Clin. Nutr. 69, 227–233 (2015).
Sui, Z. et al. Changes in meat/poultry/fish consumption in australia: from 1995 to 2011–2012. Nutrients 8, 753 (2016).
Jansen, E. C. et al. Higher childhood red meat intake frequency is associated with earlier age at menarche. J. Nutr. 146, 792–798 (2015).
Carwile, J. L. et al. Milk consumption after age 9 years does not predict age at menarche. J. Nutr. 145, 1900–1908 (2015).
Wu, Y. et al. Higher poultry consumption was associated with an earlier age at menarche. Acta Paediatr. 110, 889–895 (2021).
Moslehi, N. et al. Longitudinal association of dietary sources of animal and plant protein throughout childhood with menarche. BMC Pediatr. 21, 206 (2021).
Rogers, I. S. et al. Diet throughout childhood and age at menarche in a contemporary cohort of British girls. Public. Health Nutr. 13, 2052–2063 (2010).
Li, S. J., Paik, H. Y. & Joung, H. Dietary patterns are associated with sexual maturation in Korean children. Br. J. Nutr. 95, 817–823 (2006).
Ma, N. et al. Secular trends and urban-rural disparities in the median age at menarche among Chinese Han girls from 1985 to 2019. World J. Pediatr. 19, 1162–1168 (2023).
Popkin, B. M., Du, S., Zhai, F. & Zhang, B. Cohort profile: the China health and nutrition Survey–monitoring and Understanding socio-economic and health change in china, 1989–2011. Int. J. Epidemiol. 39, 1435–1440 (2010).
Wang, G. China Food Composition 1st edn (People’s Medical Publishing House, 1991).
Yang, Y. X., Wang, G. Y. & Pan, X. C. China Food Composition 1st edn (Peking University Medical Press, 2002).
Yang, Y. X., He, M. & Pan, X. C. China Food Composition 1st edn (Peking University Medical Press, 2004).
Yang, Y. X., Wang, G. Y. & Pan, X. C. China Food Composition 2nd edn (Peking University Medical Press, 2009).
Li, H. et al. Body mass index growth curves for Chinese children and adolescents aged 0 to 18 years. Zhonghua Er Ke Za Zhi. 47, 493–498 (2009).
Force GoCOT [Body mass index reference norm for screening overweight and obesity in Chinese children and adolescents]. Zhonghua Liu Xing Bing Xue Za Zhi. 25, 97–102 (2004).
de Onis, M. et al. Development of a WHO growth reference for school-aged children and adolescents. Bull. World Health Organ. 85 (9), 660–667 (2007).
Cole, T. J., Bellizzi, M. C., Flegal, K. M. & Dietz, W. H. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 320 (7244), 1240–1243 (2000).
Zhai, F. Y. et al. Dynamics of the Chinese diet and the role of urbanicity, 1991–2011. Obes. Rev. 15 (Suppl 1), 16–26 (2014).
Wang, Z. et al. Moderate intake of lean red meat was associated with lower risk of elevated blood pressure in Chinese women: results from the China health and nutrition survey, 1991–2015. Nutrients 12, 1369 (2020).
Zhong, V. W. et al. Associations of processed meat, unprocessed red meat, poultry, or fish intake with incident cardiovascular disease and all-cause mortality. JAMA Intern. Med. 180, 503–512 (2020).
Cheung, H. S. et al. Association of red meat intake and colorectal cancer among east-Asians: a systematic review and meta-analysis of observational studies performed between 2011–2021. J. Gastrointestin Liver Dis. 32, 377–383 (2023).
Kim, S. R. et al. Effect of red, processed, and white meat consumption on the risk of gastric cancer: an overall and dose⁻response meta-analysis. Nutrients ;11(4). (2019).
Nguyen, N. T. K. et al. Nutrient intake through childhood and early menarche onset in girls: Systematic review and Meta-Analysis. Nutrients 12, 826 (2020).
Villamor, E. & Jansen, E. C. Nutritional determinants of the timing of puberty. Annu. Rev. Public. Health. 37, 33–46 (2016).
Püssa, T. Toxicological issues associated with production and processing of meat. Meat Sci. 95, 844–853 (2013).
Li, Y. Y. et al. Residues of veterinary drugs in livestock and poultry meat and their meal intake in Guangzhou. Chin. Prev. Med. 10, 268–271 (2009).
Predieri, B., Iughetti, L., Bernasconi, S. & Street, M. E. Endocrine Disrupting Chemicals’ Effects in Children: What We Know and What We Need to Learn? Int. J. Mol. Sci. ;23(19). (2022).
Oude Griep, L. M. et al. Relation of unprocessed, processed red meat and poultry consumption to blood pressure in East Asian and Western adults. J. Hypertens. 34, 1721–1729 (2016).
Gao, Y. et al. Poultry and fish intake and pancreatic cancer risk: A systematic review and meta-analysis. Nutr. Cancer. 74, 55–67 (2022).
Snipe, R. M. J. et al. Omega-3 long chain polyunsaturated fatty acids as a potential treatment for reducing dysmenorrhoea pain: Systematic literature review and meta-analysis. Nutr. Diet. 81, 94–106 (2024).
Acknowledgements
This research uses data from the China Health and Nutrition Survey (CHNS). We thank all of the participants for their involvement in the survey. We also thank the National Institute for Nutrition and Food Safety, China Center for Disease Control and Prevention, Carolina Population Center, the University of North Carolina at Chapel Hill, the NIH and the Fogarty International Center, NIH, for providing financial support for the CHNS data collection and analysis of files from 1989 to 2015 and future surveys.
Funding
This research was supported by research grants from the National Natural Science Foundation of China (82404270), Shanxi Province Basic Research Plan (202203021212093), Shanxi Bethune Hospital Talent Introduction Scientific Research Project (2021RC031), and Strategy Research Special Project of Science and Technology of Shanxi Province (202304031401134).
Author information
Authors and Affiliations
Contributions
R.D. and Y.W. designed the study. R.D. conducted the data analysis and wrote the manuscript. D.L., T.R., L.W., R.D., F.G. and Z.L. contributed to the analysis and interpretation of the data. All the authors have critically reviewed the manuscript for important intellectual content, and approved the final version for publication.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
The CHNS protocol was approved by the Institutional Review Board at the University of North Carolina, the National Institute of Nutrition and Health, and the Chinese Center for Disease Control and Prevention. Parents provided written informed consent for their children’s participation in the survey.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Duan, R., Li, D., Ren, T. et al. Trends in meat consumption and its association with menarche timing: findings from CHNS 1997–2015. Sci Rep 15, 24219 (2025). https://doi.org/10.1038/s41598-025-07942-2
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-07942-2
Keywords
This article is cited by
-
Current State of Research on the Prevalence of Microplastics in Aquatic Fish and Their Impact on Health
Reviews of Environmental Contamination and Toxicology (2025)