Abstract
To compare the performance of first-trimester serum screening (FTSS) and non-invasive prenatal testing (NIPT) in detecting fetal chromosomal aneuploidies trisomy 21 (T21) and trisomy 18 (T18), and to evaluate the cost-effectiveness and clinical feasibility of four screening strategies for the prevention of Down syndrome (DS) from a health economics perspective. This retrospective study included 33,559 pregnant women who underwent DS screening at Fujian Maternity and Child Health Hospital between February 25, 2022, and December 29, 2023. Participants were divided into an FTSS group (n = 23,136) and an NIPT group (n = 10,423) based on the type of screening received. All subjects were followed for eight months postpartum to collect pregnancy outcome data. Screening performance was compared between the two groups based on prenatal diagnostic results. Subsequently, four screening strategies were constructed and assessed using cost-effectiveness analysis and NIPT price sensitivity analysis to determine their health-economic value. A comparison of screening performance between the two groups showed that NIPT had significantly higher specificity (99.96%) and positive predictive value (55.56%) than FTSS (specificity: 92.93%, positive predictive value: 0.91%). Meanwhile, the false-positive rate of NIPT (0.04%) was notably lower than that of FTSS (7.07%). Cost-effectiveness analysis of the four strategies indicated that strategy 2 was the most cost-effective, with a cost-effectiveness ratio (CER) of 1,252,400 CNY and an incremental cost-effectiveness ratio (ICER) of -3,626,700 CNY, achieving improved screening outcomes while reducing costs. Sensitivity analysis further demonstrated that even when the screening scale expanded under strategy 4 or when NIPT prices fluctuated between 700 and 2,100 CNY, strategy 2 maintained the lowest CER. NIPT is superior to FTSS in terms of screening efficacy. Based on a health economic evaluation, among the four strategies, Strategy 2 (using NIPT as conditional screening) offers the best cost-effectiveness while improving detection efficacy, making it the optimal strategy recommended in this study.
Similar content being viewed by others
Introduction
Birth defects are structural, functional, or metabolic abnormalities that occur during fetal development1. And are a major public health problem affecting children’s health2,3. Data indicate that the overall incidence of birth defects in China is approximately 5.6%, with an estimated 900,000 new cases annually. Among these, the incidence of DS is approximately 14.7 per 10,000 live births4. DS is currently incurable5, therefore, it is particularly important to use effective screening tools to prevent the birth of infants with DS. Currently, prenatal screening for DS is primarily conducted using FTSS and NIPT. FTSS estimates the risk of fetal DS by combining maternal serum biochemical markers with basic maternal information such as age and gestational age. This method is cost-effective, easy to implement, and commonly used as a first-line screening approach. Since Lo et al. first identified cell-free fetal DNA (cffDNA) in maternal plasma in 1997, NIPT based on cffDNA has developed rapidly6. Owing to its high sensitivity and specificity—particularly in the detection of chromosomal aneuploidies—NIPT has become a leading technology in the field of prenatal screening7,8. In recent years, some foreign studies have shown that it is more cost-effective to use NIPT as a conditional screening for serologic screening9,10,11. However, it has been proposed that NIPT detects more infants with DS and has a higher health economic value when the economic cost of social burden is considered12,13. A Notice14 was released by the NHLBI in 2016 stating that NIPT applies conditional screening for specific indications following serologic screening. Due to the disparate levels of economic development in different regions and the disproportionate price gap between serologic screening and NIPT, the cost of screening has become a significant factor in determining the value of health economics in China. Currently, different regions in China use different DS screening strategies, and guidelines for the use of NIPT also vary. At the same time, there are few reports of relevant studies on the health economic evaluation of different DS screening strategies in China; thus, it is important to compare the health economic value of different screening strategies used in clinical practice.
With the continuous advancement of prenatal screening technologies and the strengthening of policy support, ensuring screening accuracy while enhancing resource utilization efficiency has become a key challenge in clinical practice. This study included 33,559 pregnant women who underwent DS screening at Fujian Maternity and Child Health Hospital. All participants were followed for eight months postpartum, with prenatal diagnostic results used as the gold standard. Considering the differences in detection accuracy, cost, and clinical feasibility among various prenatal screening methods, this study aims to compare the efficacy of FTSS and NIPT in screening for fetal T21 and T18 and to conduct a health economic evaluation of four screening strategies to assess their clinical applicability and cost-effectiveness.
Materials and methods
Patient samples
This study retrospectively analyzed 33,559 pregnant women who voluntarily participated in the prenatal screening program at Fujian Maternity and Child Health Hospital from February 25, 2022, to December 29, 2023. Among them, 23,136 cases underwent FTSS, and 10,423 cases underwent NIPT. Pregnancy outcomes were tracked through electronic medical records or telephone follow-ups. All participants were adult pregnant women and provided informed consent.
This study was approved by the Ethics Committee of Fujian Maternity and Child Health Hospital (Approval Number: 2021KLR620), which is responsible for ensuring that all research involving human participants complies with ethical standards and regulations. All experiments were performed according to the Declaration of Helsinki and relevant national and institutional guidelines for human subject research. Informed consent was obtained from all participants before their inclusion in the study.
Research methods
FTSS
2 ml of venous blood samples were collected from pregnant women, centrifuged, separated from serum, and analyzed using the Auto DELFIA automatic time-resolved fluorescence immunoassay. Serologic markers for early pregnancy can be obtained using pregnancy-associated plasma protein A and free chorionic gonadotropin beta-subunit kits. The risk values were calculated with prenatal screening data management software (Life Cycle 5.0 for Prenatal Screening). High-risk thresholds for T21 and T18 were defined as ≥ 1:270 and ≥ 1:350, respectively, while critical-risk thresholds were 1:1000–1:270 for T21 and 1:1000–1:350 for T18.
NIPT
10 ml of venous blood samples were collected from pregnant women, anticoagulated by EDTA, and stored at 4 °C for measurement. Using the accompanying sequencer Next seq CN500, DNA digestion, amplification, purification, fragmentation, labeling signals, hybridization, washing, staining, and scanning were performed according to the microarray operation manual for sequencing to obtain Z values for 23 pairs of chromosomes. According to the sequencing results, specimens with Z-values ≤ -3.0 or ≥ 3.0 were classified as high risk for NIPT, while specimens with − 3.0 < Z-value < 3.0 were classified as low risk.
Prenatal diagnosis
At 18–24 weeks of gestation, 30–40 ml of amniotic fluid was withdrawn, 2 tubes were used for cell culture, and 2 tubes were used for DNA extraction and chromosome microarray analysis. After 7–8 days of cell culture, cell growth was observed under the microscope and harvested when growth reached the appropriate stage, pre-fixed and fixed after hypotonic treatment. Cell suspensions were dropped onto slides to dry for Giemsa staining, and chromosome scanning was performed using a GSL-120, counting 20 split phases and analyzing 5 karyotypes, with increased counting for chimeric abnormalities.
Performance evaluation
Statistics on sensitivity, specificity, positive predictive value, false-positive rate, and false-negative rate to assess screening performance.
Health economics analysis
Screening strategies
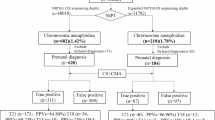
Four screening strategies were proposed based on the screening approach and sample data (Fig. 1).
Screening flowchart.
Strategy 1: Pregnant women received FTSS, T21 high-risk received prenatal diagnosis; continue pregnancy at critical-risk and low-risk.
Strategy 2: Pregnant women received FTSS, T21 high-risk received a prenatal diagnosis, and low-risk continuation of pregnancy; critical-risk received NIPT, T21 high-risk received prenatal diagnosis, and low-risk continuation of pregnancy.
Strategy 3: Pregnant women received FTSS, T21 high-risk received NIPT, NIPT high-risk received prenatal diagnosis, low-risk continuation of pregnancy; early low-risk, critical-risk continuation of pregnancy.
Strategy 4: Pregnant women received NIPT, T21 high-risk received prenatal diagnosis, and low-risk continuation of pregnancy.
Relevant indicators
Cost-effectiveness ratio (CER) = total cost/number of true positives. The lower the cost-effectiveness ratio, the more cost-effective the screening technique is and thus has better health economics.
Incremental Cost Effect Ratio (ICER) = (total cost of strategy 1 screening - total cost of strategy 2 screening) / (strategy 1 detected effect - strategy 2 detected effect). The cost of inputs needed to reflect the increased effect of strategy 1 over strategy 2.
Screening costs
Table 1 presents the key variables and their definitions in the cost model.
Cost1 = NFTSS · CFTSS + NFTSS−HR · CPD + NPD+ · CIT + NDS− · CDS.
Cost2 = NFTSS · CFTSS + NFTSS−HR · CPD + NFTSS−CR · CNIPT + NNIPT−HR · CPD + NPD+ · CIT + NDS− · CDS.
Cost3 = NFTSS · CFTSS+NFTSS−HR · CNIPT+NNIPT−HR · CPD+NPD+ · CIT+NDS− · CDS.
Cost4 = NNIPT · CNIPT + NNIPT−HR · CPD + NPD+ · CIT + NDS− · CDS.
Table 1 Variable Symbols and Their Definitions.
Results
Prenatal screening results by group
A total of 33,559 pregnant women were included in this study, with 23,136 in the FTSS group and 10,423 in the NIPT group. The screening results of each group are as follows:
FTSS group: The average age was 28.87 ± 3.15 years, with 299 cases of advanced maternal age (≥ 35 years), accounting for 1.29%.
T21 screening risk distribution: 1,649 cases were classified as high-risk (7.13%), 3,152 as critical-risk (13.62%), and 18,334 as low-risk (79.24%).
T18 screening risk distribution: 198 cases were classified as high-risk (0.86%), 404 as critical-risk (1.75%), and 22,534 as low-risk (97.40%).
NIPT group: The average age was 32.23 ± 4.53 years, with 3,647 cases of advanced maternal age (≥ 35 years), accounting for 34.99%.
T21 screening risk distribution: 9 cases were classified as high-risk (0.09%), and 10,414 as low-risk (99.90%).
T18 screening risk distribution: 1 case was classified as high-risk, and 10,422 as low-risk.
Results of prenatal diagnosis
A total of 25 cases of chromosomal abnormalities were confirmed in the FTSS group and 7 cases in the NIPT group. The specific detections are as follows:
T21
FTSS group: 19 cases (15 high-risk, 2 critical-risk, and 2 low-risk cases; among them, 1 case was a derivative type: 47, XY, der(21)del(21)(q11.2q21)).
NIPT group: 6 cases (5 high-risk and 1 low-risk case).
T18
FTSS group: 2 cases (1 high-risk and 1 low-risk case; the latter was a special type: 47, XY + i(18)(p10)).
NIPT group: No valid detection (1 high-risk case was confirmed by prenatal diagnosis as a sex chromosome abnormality: 47, XXX).
Sex chromosome abnormalities
FTSS group: 3 cases (including 1 mosaic case: 45, X(12)/46, XX(68)).
NIPT group: 1 case.
Other structural abnormalities
One case of spina bifida with meningocele was detected in each group.
Screening performance of FTSS and NIPT
The screening performance of FTSS and NIPT for T21 is presented in Tables 2 and 3. NIPT demonstrated significantly higher specificity (99.96%) and positive predictive value (55.56%) compared to FTSS (specificity 92.93%, positive predictive value 0.91%), with all differences being statistically significant (P < 0.0001). Meanwhile, the false-positive rate of NIPT (0.04%) was significantly lower than that of FTSS (7.07%) (P < 0.0001). Age-stratified analysis showed that specificity and positive predictive value for both methods remained consistent across different age groups, with statistically significant differences maintained; sensitivity and false-negative rates showed no significant differences among age groups (P = 1.00). Results for T18 screening are shown in Table 4. Due to the limited number of positive T18 cases, some indicators, such as sensitivity, could not be reliably estimated or had wide confidence intervals. Nevertheless, NIPT still outperformed FTSS in specificity and false-positive rate (P < 0.0001). These results should be interpreted with caution considering the sample size and confidence intervals.
Health economics of different down syndrome screening strategies
Based on the population of pregnant women who underwent DS screening at the Fujian Maternity and Child Health Hospital, this study evaluated the health-economic value of four DS screening strategies. According to the medical service pricing standards of Fujian provincial healthcare institutions and public hospitals, the costs were calculated as follows: 145 CNY per case for FTSS, 1400 CNY per case for NIPT, 1055 CNY per case for prenatal diagnosis, and 3721 CNY per case for induced labor. Other indirect and intangible costs were not included in the analysis. According to a study by Zeng Fang15 from Central South University, Hunan Province’s 2010 per capita GDP of 23,798 CNY was used to estimate the economic burden of each DS baby at 1,100,000 CNY. According to the National Bureau of Statistics of China16, Fujian Province’s GDP per capita in 2022 was 126,829 CNY. The economic cost per missed case of DS infants in Fujian Province was calculated to be approximately 5,860,000 CNY. The comparison results of the four screening strategies are shown in Table 5. Among strategies 1, 2, and 3, strategy 2 had the lowest total cost and per capita cost. To ensure a fair comparison across all four strategies, the original data were standardized and uniformly evaluated per 10,000 individuals. As shown in the cost-effectiveness analysis in Table 6, strategy 2 demonstrated the optimal cost and effectiveness, with the lowest CER of CNY 1,252,400. When comparing strategy 1 with strategy 2, the ICER was CNY − 3,626,700, indicating that strategy 2 not only improved detection effectiveness but also reduced costs, making it more economically advantageous. To further assess the potential impact of clinical implementation changes on the economic evaluation, a sensitivity analysis was conducted. Given that the number of people screened under strategy 4 was relatively small, its screening scale was proportionally expanded to match the other strategies, with an expansion factor of approximately 2.22. The resulting effectiveness and costs after expansion are presented in Table 7. Although the number of true positives increased, the total cost also rose significantly, resulting in a CER of CNY 4,095,500, which remained higher than that of the other three strategies. This suggests that, under current assumptions, scaling up the screening size did not improve its cost-effectiveness ranking. Figure 2 illustrates the sensitivity analysis under NIPT price fluctuations ranging from CNY 700 to CNY 2100. The results showed that strategy 2 consistently maintained the lowest CER, reflecting strong economic performance and robustness.
Sensitivity analysis of cost-effectiveness ratios for four prenatal screening strategies based on NIPT price variation. Although Strategy 1 does not include NIPT, it is retained as a reference to enable comprehensive comparison among all four strategies.
Discussion
This study demonstrates that NIPT significantly outperforms FTSS in screening for common fetal chromosomal aneuploidies while also reducing the risk of invasive procedures for both pregnant women and fetuses. In recent years, NIPT has offered favorable clinical outcomes in screening for fetal chromosomal aneuploidy. With advancements in high-throughput sequencing technology, some domestic scholars have suggested replacing serologic screening with NIPT as the first-line method17. However, due to the high cost and significant regional economic disparities, widespread implementation of NIPT remains challenging. With the full liberalization of the three-child policy in China, there are more and more pregnant women of advanced age. Previous studies have shown that the higher the age of the mother, the higher the incidence of DS18,19. In the current technical specifications14, it is mentioned that pregnant women of advanced age belong to the group of people who are cautious about the use of NIPT. This study found a disparity between maternal age and the selection of screening methods, with advanced-age pregnant women more inclined to choose NIPT—possibly due to concerns about the increased risk of complications associated with invasive prenatal diagnosis in this group. Nevertheless, our findings suggest that NIPT offers high screening performance across both advanced-age and younger pregnant populations.
In this study, the FTSS failed to detect one case of atypical T18 (47, XY + i(18)(p10)), where heterochromatin was observed on the short arm of chromosome 18. This suggests that the sensitivity of FTSS in identifying atypical T18 may be inadequate. 1 low-risk case in both FTSS and NIPT, but subsequent ultrasound findings revealed spina bifida with meningomyelocele, a common phenotype of neural tube defects. The combination of different screening methods, particularly mid-pregnancy ultrasound and FTSS, can more effectively identify fetal abnormalities20. Using FTSS or NIPT alone may result in the missed detection of some abnormal fetuses. Although NIPT demonstrates higher screening performance compared to FTSS, the possibility of false negatives must still be considered. In this study, NIPT missed one case of DS: the pregnant woman underwent further prenatal diagnosis due to an increased NT measurement of 3.2 mm on ultrasound, and the fetus was subsequently confirmed to have T21. Additionally, in our study, two high-risk T21 cases identified by FTSS and one high-risk T18 case identified by NIPT were ultimately diagnosed through prenatal testing as sex chromosome abnormalities (two cases of 47, XXY and one case of mosaicism 45, X(12)/46, XX(68)). These findings suggest that both FTSS and NIPT may also have value in indicating other chromosomal abnormalities. In summary, when FTSS or NIPT results indicate high risk or other abnormalities, prenatal diagnosis remains the gold standard.
Currently, the majority of studies on the health economics of prenatal screening in China use the decision tree modeling analysis method. Wang21 discovered that direct NIPT was the most effective, but only the most cost-effective strategy for the given price. Because the proportion of older pregnant women and the cost of NIPT are important factors in strategic decision-making, the incremental age-based cost-effectiveness analysis is most appropriate as the proportion of older pregnant women and acceptance of NIPT rise. Xu et al.22 analyzed the cost-effectiveness of NIPT from a societal standpoint, modeling decisions in a cohort of 10,000 pregnant women simulated with TeeAge Pro software. The study discovered that NIPT was more effective as a first-line screening strategy, detecting more infants with DS, but it was safer and less expensive as a conditional screening strategy than serologic screening. There are fewer studies and health economic analyses of NIPT screening strategies in the country, necessitating the conduct of relevant clinical practice studies to determine the health economic value of prenatal screening strategies. Prenatal screening and diagnostic strategies for DS vary across different regions, and associated costs also differ accordingly. Shang et al.23 conducted a cross-sectional survey of selected prenatal screening and diagnostic institutions across China’s eastern, middle, and western regions. Stated that the current price ranges for NIPT and serological screening in China are 745–2400 CNY and 140–300 CNY, respectively, per case. This study evaluated and compared four DS screening strategies currently implemented in clinical practice in the region, using the prevailing prenatal screening and diagnostic costs in Fujian Province as the basis for economic analysis. After standardizing the original data, the analysis showed that Strategy 2 had the lowest cost per DS case averted, with a CER of CNY 1,252,400, indicating the most favorable cost-effectiveness. The ICER was CNY − 3,626,700, suggesting that this strategy not only improved screening performance but also achieved significant resource savings. In the comparison of Strategy 1 and Strategy 3 with Strategy 2, Strategy 2 adopts a “stratified screening” model of further NIPT for pregnant women at critical risk for FTSS, which not only enhances the identification of high-risk individuals but also avoids the problem of under-testing that may occur in Strategy 1 when pregnant women at critical risk are not assessed. In addition, strategy 2 avoids the waste of resources and unnecessary duplication of testing caused by direct NIPT for all high-risk pregnant women in strategy 3, thus reducing the overall false-positive rate and the resulting excessive clinical interventions. It is worth noting that although Strategy 3 was optimized in terms of screening process compared with Strategy 1, it also failed to implement stratified management of critical-risk pregnant women in FTSS, resulting in two cases of diseased fetuses not being detected, thus limiting the overall efficacy of screening. In contrast, strategy 2 not only improved screening coverage but also still showed significant advantages in cost control. Strategy 4 adopts the NIPT screening model for the entire pregnant women population, which has a wide screening scope, but the CER is as high as CNY 4,091,900, much higher than the other strategies, and the current cost of implementation is high, making it difficult to meet the economic feasibility of routine screening. Combined with the current medical resources and screening budget in Fujian Province, this strategy faces greater challenges in actual promotion. Sensitivity analyses further validated the stability and economic advantages of strategy 2 under different implementation conditions, with strategy 2 consistently maintaining the lowest CER, both in the context of strategy 4 screening scale-up and in the range of NIPT price variation between CNY 700 and CNY 2100. This further suggests that the application of NIPT as a conditional screening tool in FTSS critical-risk pregnant women not only has superior benefits over other strategies but also facilitates earlier identification of chromosomal aneuploidy anomalies in the fetus. In summary, strategy 2 is a more rational and efficient screening strategy under the current health and economic conditions.
Conclusions
Combining the comprehensive analysis of the four screening strategies in this study, we conclude that strategy selection should ensure screening effectiveness while considering economic feasibility to achieve optimal allocation of healthcare resources. Our study found that replacing FTSS with NIPT resulted in a higher cost per detected DS infant than FTSS. Therefore, this study does not recommend generalizing the use of NIPT to all groups of pregnant women but rather applying NIPT as a conditional screening tool to pregnant women with a critical risk of FTSS (strategy 2), which improves the benefits of screening while controlling the cost effectively, demonstrating a higher health economic value.
The current study was based on retrospective data, resulting in a discrepancy in sample sizes between the FTSS and NIPT groups. Future large-scale prospective studies are required to acquire complete data to continue to enhance existing tactics, apply age stratification, investigate ideal screening strategies for different age groups, and optimize the cost-effectiveness and accuracy of DS screening. In the future, as more provinces incorporate NIPT into their public health systems, the acceptance rate of NIPT will continue to rise, with a subsequent decrease in price, and NIPT is expected to replace serologic screening as the first-line screening.
Data availability
The datasets generated during and/or analyzed during the current study are not publicly available due to privacy or ethical restrictions but are available from the corresponding author on reasonable request.
References
Czeizel, A. E. Birth defects are preventable. Int. J. Med. Sci. 2, 91–92. https://doi.org/10.7150/ijms.2.91 (2005).
Kancherla, V., Oakley, G. P., Brent, R. L. & Jr, & Urgent global opportunities to prevent birth defects. Semin. Fetal Neonatal. Med. 19, 153–160. https://doi.org/10.1016/j.siny.2013.11.008 (2014).
Li, X. Y. et al. The congenital birth defects burden in children younger than 14 years of age, 1990–2019: An age-period-cohort analysis of the global burden of disease study. J. Glob. Health. 14, 04012. https://doi.org/10.7189/jogh.14.04012 (2024).
Ministry of Health of the People’s Republic of China. National stocktaking report on birth defect prevention. Ministry of Health of the People’s Republic of China. (2012). http://www.gov.cn/gzdt/att/att/site1/20120912/1c6f6506c7f811bacf9301.pdf. (2012).
Antonarakis, S. E. et al. Down syndrome. Nat. Rev. Dis. Primers. 6, 9. https://doi.org/10.1038/s41572-019-0143-7 (2020).
Neofytou, M. Predicting fetoplacental mosaicism during cfDNA-based NIPT. Curr. Opin. Obstet. Gynecol. 32, 152–158. https://doi.org/10.1097/GCO.0000000000000610 (2020).
Hartwig, T. S., Ambye, L., Sørensen, S. & Jørgensen, F. S. Discordant non-invasive prenatal testing (NIPT)—a systematic review. Prenat Diagn. 37, 527–539. https://doi.org/10.1002/uog.17484 (2017).
Gil, M. M., Accurti, V., Santacruz, B., Plana, M. N. & Nicolaides, K. H. Analysis of cell-free DNA in maternal blood in screening for aneuploidies: Updated meta-analysis. Ultrasound Obstet. Gynecol. Off. J. Int. Soc. Ultrasound. Obstet. Gynecol. 50, 302–314. https://doi.org/10.1002/uog.17484 (2017).
Evans, M. I., Sonek, J. D., Hallahan, T. W. & Krantz, D. A. Cell-free fetal DNA screening in the USA: A cost analysis of screening strategies. Ultrasound Obstet. Gynecol. 45, 74–83. https://doi.org/10.1002/uog.14693 (2015).
Beulen, L. et al. The consequences of implementing non-invasive prenatal testing in Dutch National health care: A cost-effectiveness analysis. Eur. J. Obstet. Gynecol. Reprod. Biol. 182, 53–61. https://doi.org/10.1016/j.ejogrb.2014.08.028 (2014).
Nshimyumukiza, L., Beaumont, J. A., Rousseau, F. & Reinharz, D. Introducing cell-free DNA noninvasive testing in a down syndrome public health screening program: A budget impact analysis. Cost Effect Resour. Alloc. 18, 49. https://doi.org/10.1186/s12962-020-00245-5 (2020).
Walker, B. S., Jackson, B. R., LaGrave, D., Ashwood, E. R. & Schmidt, R. L. A cost-effectiveness analysis of cell free DNA as a replacement for serum screening for down syndrome. Prenat Diagn. 35, 440–446. https://doi.org/10.1002/pd.4511 (2015).
Wang, D. et al. Retrospective and cost-effective analysis of the result of Changsha municipal public welfare program by noninvasive prenatal testing. Chin. J. Med. Genet. 39, 257–263. https://doi.org/10.3760/cma.j.cn511374-20210512-00403 (2022).
National Health and Family Planning Commission Office. Notice of the general office of the national health and family planning commission on the standardization and orderly carrying out of prenatal screening and diagnosis of fetal free DNA in maternal peripheral blood. (2016). http://www.nhc.gov.cn/fys/s3581/201611/0e6fe5bac1664ebda8bc28ad0ed68389.shtml
Zeng, F. An economic evaluation on prenatal screening strategies for Down’s syndrome in Hunan Province. M.Sc. Thesis, Central South University. (2012). https://kns.cnki.net/kcms2/article/abstract?v=CdHX_LbaUYyPCNM_5BJVgShm53-6iEV3uZSA0dvzU4i9CzEUsKOEtYsHPJX-VzR4JFRlzfShsK4AJeEDN5vBwIboKxOP4V9IJHtW_i9tNKI-FBEJOGopNZj22FSF9_pyODX_XkB3gPm-IdwWnRRki8fUN2ZvhqyinKEimsQlukHWQbgqn1z_zGdjZ3MiNjXkMLfjaZh2nZU=&uniplatform=NZKPT&language=CHS
National Bureau of Statistics. China Statistical Year Book. China Statistics Press. (2023). https://www.stats.gov.cn/sj/ndsj/2023/indexch.htm
Liu, Y. et al. Clinical performance of non-invasive prenatal screening as a first-tier screening test for trisomy 21, 18, 13 and sex chromosome aneuploidy in a pilot City in China. Hum. Genomics. 14, 21. https://doi.org/10.1186/s40246-020-00268-2 (2020).
Irving, C., Richmond, S., Wren, C., Longster, C. & Embleton, N. D. Changes in fetal prevalence and outcome for trisomies 13 and 18: A population-based study over 23 years. J. Maternal-fetal Neonatal. Med. 24, 137–141. https://doi.org/10.3109/14767051003758879 (2011).
Kurtovic-Kozaric, A. et al. Ten-year trends in prevalence of down syndrome in a developing country: Impact of the maternal age and prenatal screening. Eur. J. Obstet. Gynecol. Reprod. Biol. 206, 79–83. https://doi.org/10.1016/j.ejogrb.2016.08.038 (2016).
Chen, Y. et al. The diagnostic accuracy of maternal serum alpha-fetoprotein variants (AFP-L2 and AFP-L3) in predicting fetal open neural tube defects and abdominal wall defects. Clin. Chim. Acta. 507, 125–131. https://doi.org/10.1016/j.cca.2020.03.044 (2020).
Wang, S., Liu, K., Yang, H. & Ma, J. A cost-effectiveness analysis of screening strategies involving non-invasive prenatal testing for trisomy 21. Front. Public. Health. 10, 870543. https://doi.org/10.3389/fpubh.2022.870543 (2022).
Xu, Y. et al. Cost-effectiveness analysis of non-invasive prenatal testing for down syndrome in China. Int J. Technol. Assess Health Care. 35, 237–242. https://doi.org/10.1017/S0266462319000308 (2019).
Shang, W., Wan, Y. & Huang, J. Cross-sectional investigation on the utilization of prenatal screening and diagnostic services for down syndrome in China. Chin. J. Woman Child. Health Res. 32, 1529–1536. https://doi.org/10.3969/ji.ssn.1673-5293.2021.10.025 (2021).
Acknowledgements
We would like to thank the Medical Genetic Diagnosis and Therapy Center and Fujian Maternity and Child Health Hospital for providing data support.
Funding
This work was supported by the Joint Funds for the Innovation of Science and Technology, Fujian Province (Grant number: 2024Y9557 to Lin Zheng).
Author information
Authors and Affiliations
Contributions
L.Z. designed the study. M.W., S.Z., and L.S. performed the experimental work. H.H. and L.X. were responsible for quality control of the experiments. N.Y. conducted the data analysis and wrote the manuscript. All authors have read and approved the final manuscript. Funding This work was supported by the Joint Funds for the Innovation of Science and Technology, Fujian Province (Grant number: 2024Y9557 to Lin Zheng).
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Zheng, L., Yin, N., Wang, M. et al. Comparative performance and health economic analysis of prenatal screening for down syndrome in Fujian province, China. Sci Rep 15, 23940 (2025). https://doi.org/10.1038/s41598-025-08592-0
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-08592-0