Abstract
Cancer remains the leading cause of mortality and morbidity worldwide, with its associated physical, emotional, and financial burdens contributing to widespread fear among individuals without a cancer diagnosis. This study aimed to estimate the prevalence and identify predictors of fear of cancer (carcinophobia) among the non-cancer population in Saudi Arabia. A cross-sectional study was conducted using an online self-administered survey. The Arabic version of the Fear of Cancer Scale (FOCS) was used to assess cancer-related fear. A total of 413 participants from all five regions of Saudi Arabia were surveyed over a two-month period. The prevalence of high cancer fear was 7.75% (95% CI: 5.17–10.33%). Fear levels ranged from 5.2 to 10.4% across demographic groups. Age and income were significantly associated with cancer fear (p < .05). Older individuals were significantly less likely to report fear, while higher income was associated with a 3.6-fold increase in the odds of reporting fear. The study highlights the substantial prevalence of cancer-related fear in the population in Saudi Arabia and identifies critical predictors that may inform targeted public health strategies. Addressing psychological barriers such as carcinophobia is essential for promoting early detection and preventive healthcare behaviors. The findings suggest the need for culturally tailored cancer education and intervention programs to reduce fear and encourage proactive health management in Saudi Arabia.
Similar content being viewed by others
Introduction
Cancer continues to rank among the leading causes of death and disability worldwide, posing a major public health challenge due to its physical, emotional, and financial toll1. According to global statistics, it remains a top health concern, with millions of new diagnoses and deaths reported each year. In Saudi Arabia, cancer incidence has tripled in recent years, highlighting the urgent need for improved prevention, early detection, and community-based education strategies2.
Alongside its growing medical burden, cancer elicits widespread psychological responses, particularly fear even among individuals who have never been diagnosed. This fear, known as carcinophobia, is defined as an excessive or persistent fear of developing cancer. While fear can be adaptive motivating health-seeking behaviors such as screening; it may also lead to avoidance, denial, and psychological distress, all of which can interfere with timely medical care3,4.
Psychologically, fear is described as an emotional response to a specific, perceived threat. When prolonged, such as in chronic health anxieties, it may negatively impact daily functioning and well-being5. Carcinophobia, in particular, is influenced not only by the threat of illness but also by sociocultural and informational factors. Sensational media portrayals and anecdotal experiences may intensify fear, especially when cancer is depicted as fatal and untreatable6. A U.S.-based survey revealed that 41% of adults ranked cancer as their most feared health condition3, indicating that carcinophobia is among the most common and impactful health-related anxieties globally. Even well-intentioned public health campaigns can inadvertently heighten fear when they emphasize risk without adequate reassurance or support.
Excessive fear may have paradoxical effects. For some, fear promotes proactive behaviors such as regular screenings and healthy lifestyle modifications. For others, it leads to avoidance of healthcare altogether, contributing to delayed diagnoses and reduced treatment efficacy4.
In Saudi Arabia, cancer incidence has increased threefold in recent years2, underscoring the urgency of early detection and public education. However, fear remains a significant barrier to screening. A national study on breast cancer screening behavior revealed that nearly a quarter of Saudi women (23%) avoided screening due to fear of discovering a tumor7. These findings highlight the need to address not only logistical barriers but also the emotional and psychological factors that influence health behaviors in cancer prevention efforts.
Demographic differences also shape cancer fear. Younger adults, women, and individuals with higher education levels tend to report greater anxiety about cancer8. These trends align with psychological models of risk perception, which suggest that perceived vulnerability and emotional salience influence fear. In light of Saudi Arabia’s demographic and epidemiological transition, understanding fear within its social and cultural context is critical.
Despite the recognized importance of cancer fear, its true prevalence and predictors remain underexplored in many regions, including Saudi Arabia. One key barrier has been the lack of culturally sensitive tools to assess cancer-related fear in Arabic-speaking populations. To address this gap, the present study employed a culturally and linguistically adapted Arabic version of the Fear of Cancer Scale (FOCS), which captures both direct fears (e.g., fear of death or diagnosis) and indirect fears (e.g., financial burden or impact on family). This tool was specifically designed to reflect the social and emotional nuances of cancer fear within the Saudi context, ensuring validity and reliability in regional assessments. By using this scale, the study aims to estimate the prevalence of cancer fear among non-cancer adults in Saudi Arabia and identify its sociodemographic predictors. The findings will help inform targeted public health messaging and interventions that reduce fear-driven barriers, promote early detection behaviors, and ultimately improve cancer outcomes.
Significance of the study
This study will provide essential data on the prevalence and predictors of cancer-related fear in Saudi Arabia, offering insights that can help improve cancer prevention efforts, inform public health policy, and guide future research in psychological oncology. By addressing the psychological aspects of cancer fear, this research aims to reduce the negative impact of this fear on health behaviors and overall well-being, ultimately contributing to disease prevention and early detection which in turn lead to better health outcomes in the Saudi population.
Methods
Study design
The current study employed a cross-sectional design to explore the prevalence and predictors of the fear of cancer (carcinophobia) among the non-cancer population in Saudi Arabia.
Research question
What are the prevalence and predictors of the fear of cancer (carcinophobia) among the non-cancer population in Saudi Arabia?
Sample
The optimal sample size was 385 participants, estimated based on the following formula:
where, due to a lack of previous estimates, p is assumed to be 0.5.
A non-probability consecutive sampling approach was used to recruit 413 non-cancer adults aged 18 years and older, residing in Saudi Arabia, over a period of 2 months to explore the prevalence and predictors of the fear of cancer (carcinophobia) among the non-cancer population.
Data collection
The current study used an online survey across all 13 regions of the Kingdom of Saudi Arabia for data collection. The survey included socio-demographic information such as age, gender, occupation, marital status, chronic disease, family history of cancer, education level, income, health status perception, and the Fear of Cancer Scale (FOCS) was used to assess the level of fear of cancer (carcinophobia) among the non-cancer population in Saudi Arabia. FOCS is a self-evaluation questionnaire developed by a Chinese team to examine the level of cancer fear in non-cancer populations9. It includes 17 items in two subscales; the first one assesses direct fear that includes 8 items, and the second one assesses indirect fear including 9 items. FOCS has good reliability and validity, in which the Kendall Concordance coefficient for the content validity of the items from 7 experts in the Delphi consultation was 0.542 (p < .001) suggesting good reliability, and the I-CVI score ranged between 0.807 and 0.990 suggesting good content validity. The questionnaire was translated and modified to Arabic by the study team, validity and reliability of the Arabic version was published in a previous study.
Data analysis and management
To describe the demographics of the sample, categorical variables were summarized using frequency and percentages, whereas numerical variables were summarized using mean and standard deviation. The percentage of fear-of-cancer was estimated using a 95% confidence interval. In addition, the distribution of low/high fear of cancer was cross tabulated among demographic factors. Furthermore, to assess the strength of association, multivariable binary logistic regression was utilized. Statistical analyses were conducted using IBM SPSS Statistics version 30 and statistical significance was sent at p-value < 0.05.
Ethical considerations
Approval from the King Abdullah International Medical Research Centre (KAIMRC) in Riyadh was obtained on March 3, 2024, prior to initiating the study (IRB # 000007724, Study # NRR24/017/5). Participants’ consent to participate was granted by answering the survey questions. Informed consent was obtained from all subjects. The study’s aim was clearly communicated to the participants, along with an assurance that there are no expected risks linked to their involvement. Participants were informed of their right to withdraw from the research at any point without facing any adverse consequences. To safeguard privacy and confidentiality, all participant information was kept anonymous, and no personal details were disclosed. All methods were carried out in accordance with relative guidelines and regulations.
Results
A consecutive sample over a period of 2 months of 413 non-cancer participants were recruited from the five regions and the 13 major cities of Saudi Arabia. Most of the participants were from the middle region (74.8%), residing in Riyadh city (76.8%), female (72.2%), under 35 years old (72.4%), married (63.7%), and holding a bachelor’s, master’s, or Ph.D. degree (74.5%), who are employed (61.3%). A sizable percentage of them (43.3%) earn 5000 SAR or more monthly. The vast majority do not have chronic diseases (82.8%) but have acquaintance with cancer through a relative or a friend (87.4%). The average self-rating of health out of 10 is 8.22 ± 1.72. Refer to Table 1 for more details about the sample characteristics (n = 413).
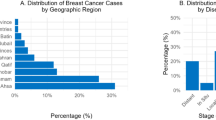
Figure 1 below presents the distribution of responses to the 17 items of the Arabic Fear of Cancer Scale (AFOCS). A notable trend emerged: items reflecting indirect fears—such as pain (Q10), family distress (Q14), financial burden (Q9), and stigma or isolation (Q16)—elicited the highest levels of agreement. For example, more than 180 participants strongly agreed that cancer is very painful, and over 160 agreed they would seek screening after hearing about others’ diagnoses (Q13), reflecting a reactive coping response.
In contrast, items representing direct fears—such as fear of diagnosis (Q12), associating with cancer patients (Q15), or visiting hospitals (Q11)—showed more varied responses, often with substantial levels of disagreement. The lowest agreement was seen in statements reflecting misconceptions, such as the belief that cancer is contagious (Q3), which was strongly disagreed with by a majority (n = 272). These patterns suggest that cancer fear in the Saudi population is more strongly tied to emotional and social consequences than to the disease itself.
Distribution of the participants’ responses to the AFOCS.
The cancer-fear score (CFS) is calculated by adding the responses to Q1-Q17. Furthermore, it was categorized into low fear if CFS < 51 and high fear if CFS ≥ 51. Doing so, we can capture the overall high fear of cancer attributed to direct reasons (Items 1, 2, 4, 8, 9, 10, 12, 13) or indirect ones (the remaining items), according to9.
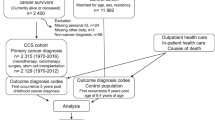
With that in mind, the prevalence of carcinophobia (Fear of Cancer) is 7.75% with 95% CI = (5.17%, 10.33%). Figure 2 below depicts the distribution of the participants’ responses to the carcinophobia categories.
Prevalence of carcinophobia.
Table 2 below depicts the high fear of cancer across the sample demographics. Verily, the prevalence of high fear of cancer ranges from 5.2 to 10.4%. In fact, the high fear of cancer is largest among participants living in other regions and other cities, who are males, with age 35–44, who are unmarried, holding postgraduate degree, working in non-health sectors, earning 5000 or more, having chronic diseases, and who have no acquaintance with cancer.
To identify factors significantly associated with fear of cancer and adjust for confounders, we employed a multivariable logistic regression. As depicted in Table 3 below, the age and income were significantly associated with the fear of cancer. Specifically, older age (25–34 and 45 or above) was associated with at least a 75% lower likelihood of reporting cancer fear compared to younger participants (18–24), suggesting a possible protective effect. In contrast, participants with a monthly income of 5000 SAR or more had 3.6 times odds of reporting fear of cancer compared to those with lower income.
Discussion
This study provides new evidence on the psychological burden of cancer fear among non-cancer adults in Saudi Arabia. The prevalence of high cancer fear (7.75%) is noteworthy and warrants attention from public health authorities. This percentage reflects a meaningful psychological concern, particularly considering its potential impact on healthcare-seeking behaviors and quality of life. The findings align with international literature, which suggests that younger individuals are more likely to perceive themselves as vulnerable to serious illnesses, and that those with higher income may experience heightened health consciousness due to greater access to health information5,10,11.
Although not statistically significant (p = .052), the data suggest that married individuals may be less likely to report fear of cancer, with an estimated 65.4% lower odds compared to unmarried individuals. This trend is consistent with findings from12] and [13, which suggest that social support may buffer health-related fear and anxiety. Marriage may offer both emotional reassurance and practical support, making health threats feel more manageable. Additionally, married individuals are more likely to adopt healthier lifestyles and engage in preventive healthcare behaviors, which may reduce uncertainty and fear14,15.
In the Saudi context, cultural factors add further complexity. Although cancer incidence has increased substantially in the past decade2, fear-driven avoidance behaviors remain prevalent. A recent national study found that fear of discovering a tumor was a prominent barrier to breast cancer screening participation among Saudi women7, This highlights how rising cancer rates—when not accompanied by adequate public education—can exacerbate fear and discourage early detection.
Cancer fear exists along a continuum, ranging from constructive motivation to maladaptive avoidance. Moderate levels of fear may encourage protective behaviors, such as screening participation and healthier living16,17. However, excessive or unaddressed fear can impair rational decision-making, foster denial, and lead to delays in care18,19. Indirect exposure to cancer—such as caregiving or bereavement—can also contribute to persistent anticipatory fear20, further intensifying emotional distress at the community level.
The item-level response patterns in this study provide further insight into the nature of cancer fear in this population. The strongest levels of agreement were observed for items reflecting indirect or socially mediated fears, such as pain, emotional impact on family, isolation, and financial burden. This suggests that cancer fear among Saudi adults may be shaped more by concerns about suffering, stigma, and relational disruption than by the biological disease process itself.
In contrast, items reflecting direct clinical fears—such as receiving a diagnosis, visiting hospitals, or associating with patients—elicited more neutral or disagreeing responses. Notably, misconceptions such as cancer being contagious were strongly rejected by most respondents, indicating relatively accurate medical knowledge, despite strong emotional reactions to the broader implications of cancer. These findings highlight the importance of designing public health interventions that go beyond medical education alone. Programs should also address emotional, familial, and financial concerns, and include supportive messaging that frames cancer as a treatable and manageable condition, rather than a death sentence. Psychological reassurance and de-stigmatization are likely key to reducing excessive fear and promoting early screening behaviours.
To mitigate the negative effects of carcinophobia, public health strategies must strike a balance between raising awareness and reducing anxiety. Educational campaigns should normalize cancer as a manageable condition, while also providing access to psychological support. Evidence-based messaging that validates public concerns—without amplifying distress—is essential for encouraging timely health-seeking behaviors. As demonstrated by recent campaigns in the UK and other countries, integrating emotional reassurance into cancer education can help reduce fear and improve screening participation21.
This study contributes to the growing field of psycho-oncology in Saudi Arabia by estimating the prevalence and identifying key predictors of cancer fear in a non-cancer adult population. However, several limitations should be considered. First, the online survey method may have led to underrepresentation of older adults and those with limited internet access. Second, the use of non-random sampling limits the generalizability of findings. Third, the cross-sectional design precludes causal inference between demographic characteristics and cancer fear.
Implications for practice
The findings of this study highlight the need for focused interventions targeting carcinophobia within specific demographic segments—particularly younger individuals and those with higher income levels. Healthcare practitioners and policymakers can use these insights to design culturally sensitive public health initiatives that reduce cancer-related anxiety and disseminate accurate, reassuring information. Incorporating mental health resources and evidence-based coping strategies into cancer education may help reduce emotional barriers and improve psychological well-being among individuals who experience elevated cancer fear.
Conclusion
This study offers important insights into the prevalence and predictors of cancer fear among non-cancer adults in Saudi Arabia. The findings reveal that 7.75% of respondents reported high levels of cancer fear, with elevated fear more common among younger adults, unmarried individuals, and those with higher incomes. These demographic factors can help inform targeted public health interventions aimed at mitigating cancer-related fear and its influence on healthcare-seeking behaviors.
Importantly, the study highlights that cancer fear is not solely based on the disease itself but is shaped by personal experiences, emotional vulnerability, and sociocultural factors. While some individuals may avoid screenings due to anxiety, others may engage in excessive health monitoring—both of which can negatively impact health outcomes. These findings underscore the need for culturally sensitive cancer education programs that reduce fear while promoting proactive behaviors such as early detection.
To foster a healthier and more balanced approach, future public health strategies should focus on delivering accurate, reassuring, and accessible information about cancer and its treatment. Additionally, future research should explore patterns of cancer-related fear in greater depth, evaluate the effectiveness of intervention strategies, and examine how sociocultural variables—such as education, social class, and income—influence public perceptions of cancer.
Data availability
Data are available upon reasonable request by contacting the author at his email: sarisr@ksau-hs.edu.sa.
References
Centers for Disease Control and Prevention. Leading causes of death (2023). https://www.cdc.gov/nchs/fastats/leading-causes-of-death.htm.
Alqahtani, W. S. et al. Epidemiology of cancer in Saudi Arabia thru 2010–2019: a systematic review with constrained meta-analysis. AIMS Public. Health. 7 (3), 679–696. https://doi.org/10.3934/publichealth.2020053 (2020).
Shen, L. & Callejas, M. L. A. Fear of cancer, its antecedents, correlates, and disease risk estimates. Communication Public. 8 (4), 343–356. https://doi.org/10.1177/20570473231197297 (2023).
Tarrant, G. Fear of cancer (carcinophobia): Symptoms, causes, treatment, advice - PsychoTreat. PsychoTreat. (2023). https://psychotreat.com/what-is-carcinophobia-or-fear-of-cancer/.
Dubayova, T. et al. The impact of the intensity of fear on patients’ delay regarding health care-seeking behavior: a systematic review. Int. J. Public. Health. 55 (5), 459–468. https://doi.org/10.1007/s00038-010-0149-0 (2010).
He, R. & Li, Y. Media exposure, cancer beliefs, and cancer-related information-seeking or avoidance behavior patterns in China. Int. J. Environ. Res. Public Health. 18 (6), 3130. https://doi.org/10.3390/ijerph18063130 (2021).
Alkarak, S. et al. Factors affecting breast cancer screening behavior among women in Saudi arabia: a retrospective cross-sectional study. Cureus 16 (4), e58324. https://doi.org/10.7759/cureus.58324 (2024).
Murphy, P. J., Marlow, L. A. V., Waller, J. & Vinet, C. What is it about a cancer diagnosis that would worry people? A population-based survey of adults in England. BMC Cancer. 18, 86. https://doi.org/10.1186/s12885-017-3963-4 (2018).
Feng, L. S. et al. Development and reliability and validity test of the fear of cancer scale (FOCS). Ann. Med. 54 (1), 2353–2361. https://doi.org/10.1080/07853890.2022.2113914 (2022).
Ferrer, R. A., Klein, W. M. P., Persoskie, A., Avishai-Yitshak, A. & Sheeran, P. The tripartite model of risk perception (TRIRISK): distinguishing deliberative, affective, and experiential components of perceived risk. Ann. Behav. Med. 50 (5), 653–663. https://doi.org/10.1007/s12160-016-9790-z (2016).
Vrinten, C., McGregor, L. M., Heinrich, M., von Wagner, C. & Waller, J. What do people fear about cancer? A systematic review and meta-synthesis of cancer fears in the general population. Psycho-Oncology 26 (8), 1070–1079. https://doi.org/10.1002/pon.4287 (2017).
Hall, A. G. et al. Breast cancer fatalism: the role of women’s perceptions of the health care system. J. Health Care Poor Underserved. 19, 1321–1335. https://doi.org/10.1353/hpu.0.0091 (2008).
Vrinten, C., van Jaarsveld, C. H., Waller, J., von Wagner, C. & Wardle, J. The structure and demographic correlates of cancer fear. BMC Cancer. 14, 597. https://doi.org/10.1186/1471-2407-14-597 (2014).
Ruiz-Marin, C. M., Molina-Barea, R., Slim, M. & Calandre, E. P. Marital adjustment in patients with cancer: association with psychological distress, quality of life, and sleep problems. Int. J. Environ. Res. Public Health. 18 (13), 7089. https://doi.org/10.3390/ijerph18137089 (2021).
National Cancer Institute. Facing cancer with your spouse or partner (2025). https://www.cancer.gov/about-cancer/coping/adjusting-to-cancer/spouse-or-partner.
Simard, S., Thewes, B. & Humphris, G. Fear of cancer recurrence in adult cancer survivors: a systematic review of quantitative studies. J. Cancer Survivorship: Res. Pract. 7 (3), 300–322. https://doi.org/10.1007/s11764-013-0272-z (2013).
Dijkstra, A. & Brosschot, J. F. Worry about health in smoking behaviour change. Behav. Res. Ther. 41 (9), 1081–1092. https://doi.org/10.1016/S0005-7967(02)00244-9 (2003).
Cancer Research, U. K. Fear, anxiety, panic and cancer (2020). https://www.cancerresearchuk.org/about-cancer/coping/mental-health-cancer/how-cancer-make-you-feel/fear-anxiety-panic/fear-anxiety-panic-cancer.
Thewes, B., Butow, P., Bell, M. L., Beith, J. & Wilson, K. Fear of cancer recurrence in young early-stage breast cancer survivors: the role of metacognitive style and disease-related factors. Psycho-Oncology 22 (9), 2059–2063. https://doi.org/10.1002/pon.3252 (2013).
Smith, S. G., Vrinten, C., Kobayashi, L. C. & Wardle, J. Bereaved cancer carers’ fear of developing cancer: a neglected but important concern. Psycho-Oncology 23 (4), 402–408. https://doi.org/10.1002/pon.3444 (2014).
NHS England. NHS chief launches new campaign to combat the fear of cancer. NHS Engl. News (2022). https://www.england.nhs.uk/2022/03/nhs-chief-launches-new-campaign-to-combat-the-fear-of-cancer/.
Acknowledgements
The authors would like to express their sincere gratitude to the Publication Office at the King Abdullah International Medical Research Center for their assistance and support. Additionally, they would like to thank the Office of Research at the College of Public Health and Health Informatics, King Saud bin Abdulaziz University for Health Sciences, for their help in reviewing and proofreading the manuscript.
Funding
None of the authors have funding.
Author information
Authors and Affiliations
Contributions
R.A, A.I, A.A, S.S, and M.R.A, were involved in the study’s conception, design, and conduct. R.A, D.A, A.I, A.A, M.R.A, M.A, F.A, M.A.A, and S.S. were involved in data collection and analysis. A.A and M.R.A contributed to the discussion. R.A, D.A, A.I, A.A, M.R.A, M.A, F.A, M.A.A, and S.S wrote, reviewed, and edited the manuscript. R.A. conducted the analysis and interpretation of the results. All Authors contributed equally to writing the first draft of the manuscript, and all authors edited, reviewed, and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
At King Saud bin Abdulaziz University for Health Sciences (KSAU-HS), King Abdullah International Medical Research Center (KAIMRC) (https://www.ksau-hs.edu.sa/English/About-Us/Pages/UniversityChart.aspx ) is the entity in charge of the Institutional Review board (IRB) approvals. Furthermore, the IRB approval was obtained from KAIMRC on March 3, 2024 (IRB # 000007724, Study # NRR24/017/5).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Abusaris, R., Alsaqabi, D., Ibrahim, A.F.A. et al. Prevalence and predictors of carcinophobia among the non cancer population in Saudi Arabia. Sci Rep 15, 29356 (2025). https://doi.org/10.1038/s41598-025-15181-8
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-15181-8