Abstract
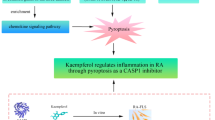
To investigate the mechanism by which Butin inhibits proliferation and pyroptosis in human fibroblast-like synoviocytes of rheumatoid arthritis (HFLS-RA) via the NLRP3/Caspase-1/ GSDMD pyroptosis axis. Flavonoid compounds were extracted from Hei Gu Teng, and Butin was analyzed for its interaction with RA target proteins and signaling pathways using network pharmacology. An in vitro HFLS-RA model was established, and cells were induced with IL-1β. Groups included control, IL-1β-stimulated, IL-1β + Leflunomide, and IL-1β + Butin at low, medium, and high concentrations. Cell inhibition rates were measured using the MTT assay to determine the optimal Butin concentration, while scratch and Transwell assays assessed cell proliferation, migration, and invasion. LDH assays measured cell membrane damage; ELISA, RT-qPCR, and Western blot analyzed the expression of inflammation-related proteins NLRP3, GSDMD, CASP1, CASP3, IL1β, and IL18; Hoechst33342/PI staining and flow cytometry examined the cell cycle and pyroptosis. Hei Gu Teng yielded Butin (> 96% purity). Network pharmacology identified 48 target genes, predominantly involved in pathways like IL-1 signaling, HIF-1 signaling, sphingolipid signaling, and osteoclast differentiation. Cell assays demonstrated significantly reduced proliferation in Butin-treated groups compared to control (P < 0.05). Compared to the IL-1β + Leflunomide group, the Butin group showed decreased LDH release and lower levels of NLRP3, GSDMD, IL-1β, IL-18, CASP1, and CASP3 proteins and mRNAs (P < 0.05). Cell cycle analysis indicated increased DNA content in G0/G1 phases and decreased in G2/S phases for medium and high Butin concentrations (P < 0.05). Butin suppresses the expression of multiple inflammatory factors induced by IL-1β within the NLRP3/CASP-1/GSDMD pyroptosis axis, reducing proliferation and pyroptosis of HFLS-RA, thus alleviating synovial inflammation and representing a potential mechanism for RA treatment.
Similar content being viewed by others
Introduction
Rheumatoid arthritis (RA) is a chronic systemic autoimmune disease characterized by synovial inflammation in multiple joints and progressive joint damage, primarily manifesting clinically as joint pain1, Epidemiological studies indicate a global prevalence of RA ranging from 0.3 to 1%, with an estimated prevalence of 0.4% in China. The disease exhibits a significantly higher incidence in women than in men2. The pathogenesis of RA remains unclear. The underlying pathology involves synovitis and angiogenesis, where aberrant proliferation of vascular granulation tissue progressively destroys articular cartilage and bone, ultimately leading to joint deformity and functional impairment.Without standardized treatment, the disability rate among RA patients reaches approximately 60% within 6–10 years, increasing to as high as 90% after 15 years of disease progression3. According to recent data, cellular pyroptosis plays a significant role in the pathogenesis of RA4. Pyroptosis is a programmed cell death mode dependent on caspase-1/3, exhibiting significant differences in morphological changes and lesion extent compared to apoptosis5. The process is triggered by the release of large amounts of inflammatory cytokines such as interleukin-1β (IL-1β) and interleukin-18 (IL-18), which activate the inflammatory response6,7. These cytokines further recruit inflammatory cells and amplify the inflammatory response8, leading to the proliferation and pyroptosis of human fibroblast-like synoviocytes of rheumatoid arthritis (HFLS-RA), causing abnormal synovial cell growth and the destruction of subchondral bone and cartilage, eventually resulting in joint malformation and functional impairment.
Currently, RA treatment primarily involves non-steroidal anti-inflammatory drugs (NSAIDs) for pain relief in combination with disease-modifying anti-rheumatic drugs (DMARDs), corticosteroids, and biologics to modify disease progression. Although these medications provide rapid symptom relief, their long-term administration frequently induces adverse effects on gastrointestinal, hepatic, and renal functions, often proving intolerable for patients. Notably, certain plant-derived compounds exhibit therapeutic advantages for RA, including enhanced efficacy, reduced costs, and fewer side effects. Hei Gu Teng is a traditional medicinal vine plant widely utilized in Miao ethnomedicine for treating rheumatic disorders. It is derived from the dried vine stems of Periploca forrestii Schltr, a species belonging to the Asclepiadaceae family9. Clinical trials and experimental studies conducted over several years have confirmed the significant efficacy of compound formulations containing Hei Gu Teng. For instance, Jin Wu Jian Gu capsules reduce the expression of IL-1β, interleukin-6 (IL-6), and interleukin-17 (IL-17) in cultured RA synovial cells10. Experimental studies demonstrated that the 60% ethanol extract of Hei Gu Teng significantly reduced serum and inflammatory tissue fluid levels of IL-1β, IL-6, and tumor necrosis factor-α (TNF-α) in adjuvant-induced arthritis (AA) rats, while simultaneously suppressing paw swelling and decreasing the thymus index11. Furthermore, studies have demonstrated that Hei Gu Teng compound formulations effectively suppress paw swelling, reduces thymus index, and downregulate serum levels of IL-1β, IL-6, and TNF-α in AA rats, while increasing kidney, liver, and spleen indices. These findings suggest that Hei Gu Teng may exert anti-rheumatoid effects by modulating immune organ functions12. Hei Gu Teng main components include flavonoids, essential oils, saponins, and coumarins. Butin, a flavonoid compound with significant anti-inflammatory activity, was isolated and screened from Hei Gu Teng. Studies have demonstrated that butin possesses extensive pharmacological effects, including antioxidant, anti-anxiety, hypoglycemic, antitumor, and anti-inflammatory activities. In vivo experiments have shown that butin alleviates lipopolysaccharide (LPS)-induced renal inflammation in mice by suppressing the NF-κB p65 and MAPK signaling pathways through TLR4/Src-mediated mechanisms, consequently reducing inflammatory cytokine expression13. Further studies have demonstrated that butin downregulates the TLR4/MyD88/NF-κB signaling pathway, thereby suppressing lead-induced neuroinflammation and mitigating inflammatory responses14. In LPS-induced human pulmonary artery endothelial cells (HPAECs), butin significantly reduced the expression of IL-1β and cyclooxygenase-2 (COX-2), as well as the release of proinflammatory mediators prostaglandin E2 (PGE2) and nitric oxide (NO)15. Butin also markedly inhibits the expression of IL-6, interleukin-8 (IL-8), TNF-α, and chemokine ligand 2 (CCL2), thereby alleviating inflammatory responses in renal tissues of mice induced by a high-fat diet16. Furthermore, butin suppresses IL-1β release, thereby attenuating inflammation in chondrocytes17. This study builds on previous clinical observations and experimental research conducted by our group. Based on the pharmacological properties of butin, we hypothesize that butin has a similar effect on HFLS-RA and can mitigate HFLS-RA inflammation by inhibiting cell proliferation and pyroptosis. We aim to validate this hypothesis through network pharmacology and explore the mechanisms by which butin regulates the NLRP3/CASP-1/GSDMD axis to inhibit the proliferation and pyroptosis of HFLS-RA in in vitro cell experiments.
Experimental materials
Experimental cells
Synovial cells were cultured using the tissue explant method, with synovial tissue sourced from patients undergoing active-phase rheumatoid arthritis (RA) total knee arthroplasty at the Second Affiliated Hospital of Guizhou University of Traditional Chinese Medicine. The selection of patients conformed to the 1987 American Rheumatism Association (ARA) revised criteria for RA diagnosis. Patients had not used glucocorticoids or disease-modifying antirheumatic drugs, had given informed consent, and the study received ethical approval (approval number: YJZ2020010093).
Drugs and reagents
Hei Gu Teng plant samples were collected from Qiannan Prefecture(104°35 ‘~ 106°32’ E, 24°38 ‘~ 26°11’ N), Guizhou Province, and identified by Associate Professor Hou Xiaqi as stems of Periploca forrestii Schltr. The specimens are preserved at the Key Laboratory of Natural Product Chemistry of the Chinese Academy of Sciences in Guizhou (specimen voucher number: HGT20200704). Butin (lot number A28IB213681, purity: 99.1%), was obtained from Shanghai Yuan Ye Biotechnology Co, Ltd; Leflunomide (lot number 11752, purity: 99.72%), was purchased from MCE, USA; IL-1β (catalog number: cyt-210-b), from ProSpecbio, USA; Lactate dehydrogenase (LDH) assay kit (catalog number: A020-3), from Nanjing Jiancheng Bioengineering Institute; Annexin V-APC/7-AAD double staining pyroptosis detection kit (catalog number: KGA1030), from Jiangsu Kaiji Biotech Co, Ltd; Hoechst 33,342 (catalog number: C1025), from Shanghai Biyuntian Biotechnology Co, Ltd; Human IL-1β ELISA kit (catalog number: MM-0190H2), Human IL-18 ELISA kit (catalog number: MM-0157H2), Caspase-3 kit (catalog number: MM-1563H2), all from Jiangsu Enzyme Immune Biotech Co, Ltd; and Caspase-1 kit (catalog number: ml058257), from Jiangsu Enzyme-linked Biotech Co, Ltd.
Experimental equipment
Multiskan microplate reader and QE Focus high-resolution mass spectrometer (Thermo Fisher Scientific, USA); Beckman Coulter flow cytometer (CytoFLEX, USA); ECLIPSE Ts2 inverted microscope (Nikon, Japan); DYY-7 C electrophoresis power supply (Beijing Liuyi Instrument Factory); SH-523 chemiluminescence imaging system (Shenhua Science and Technology Co, Ltd, Hangzhou); Bruker AVII-600 MHz and Bruker AV NEO-600 MHz nuclear magnetic resonance spectrometers (Agilent Technologies, Germany); HP-5973 mass spectrometer (Hewlett-Packard, USA); NP7005C semi-preparative liquid chromatograph (Jiangsu Hanbang Science and Technology Co, Ltd.); ZORBAX ODS semi-preparative chromatography column (Agilent Technologies).
Methods
As a commonly used medicine for the treatment of rheumatoid arthritis in Chinese folk, Hei Gu Teng does not belong to the endangered wild plant, and has obtained the collection license of the Second Affiliated Hospital of Guizhou University of Chinese Medicine. The research on it does not violate relevant laws and does not have any conflict of interest.
Extraction of butin
10 kg of dried Hei Gu Teng samples were ground into coarse powder and extracted by heating under reflux with 95% ethanol. The extract was concentrated under reduced pressure to yield 1.7 kg of extract, which was dispersed in water and sequentially extracted with petroleum ether and ethyl acetate, resulting in an ethyl acetate extract weighing 853 g. This extract was mixed with D101 macroporous resin, packed into a column, and eluted with methanol in fractions to obtain components of varying polarity. The 60% methanol fraction (114.5 g) was further purified using polyamide column chromatography, eluted with a methanol gradient, yielding seven fractions (Fr. C1-C7). Fraction C3 (32.3 g) was further purified using dextran gel chromatography.
Butin and RA network pharmacology analysis
Butin and its flavonoid constituents in Hei Gu Teng were not found on the TCMSP platform. Relevant compounds were identified through literature review and depicted using ChemDraw 20.0. The target compounds were screened for activity using the SwissADME database, and their target proteins were converted to standard gene names using Swiss Target Prediction and TCMSP. These genes were then imported into Cytoscape 3.8.2 to construct network diagrams using the STRING 1.7 database. RA disease targets were retrieved from GeneCards, OMIM, and DrugBank databases. Venn diagrams were used to identify common targets between Butin and RA. Hub genes were analyzed using the cytoHubba MCC algorithm, and validation was performed through PPI and degree histograms. GO enrichment and KEGG pathway enrichment analyses were conducted and selected for screening.
Experimental grouping
Based on previous studies by the research group18,19,20, the experimental groups included a control group (Control), an IL-1β-stimulated group (IL-1β), an IL-1β + leflunomide group (IL-1β + Lef), and IL-1β + Butin groups at low (IL-1β + B-L), medium (IL-1β + B-M), and high (IL-1β + B-H) concentrations. The effective concentration range of leflunomide was determined by MTT assay to be 20 mg·L−1, and Butin concentrations were selected based on MTT assay and prior experiments to be 5, 50, and 150 mg·L−1. The concentration of IL-1β for stimulation, based on prior experiments and referenced literature21, was set at 10 mg·L−1.
Culture of HFLS-RA
Synovial tissues from RA patients were obtained postoperatively, rinsed several times with PBS containing double antibiotics, and excess cartilage and adipose tissues were removed. The tissues were minced into approximately 1 mm³ pieces using sterile ophthalmic scissors, spread out in a T25 flask, and incubated for 4 h before flipping the flask and adding 5 mL of complete medium to submerge the tissue pieces. Cultures were maintained at 37 °C with 5% CO2 and passaged until the 3rd to 4th generation for further use.
Wound healing, migration, and invasion assays
Healthy 3rd-generation HFLS-RA cells in the exponential growth phase were used. Using a ruler and marker pen, horizontal lines were uniformly drawn across the back of a 6-well plate, spaced approximately 0.5 to 1 cm apart, crossing at least five lines per well. After enzymatic digestion with trypsin, the cells were counted and seeded at 8105 cells per well in a 6-well plate and cultured overnight. A pipette tip was used to scratch along the ruler-generated lines; the dislodged cells were washed away with PBS, and incomplete medium was added along with taking photographs at 0 h. The plates were then incubated at 37 °C with 5% CO2 for 24 h and photographed again. The migration rate was calculated using the formula: Cell migration rate = (initial scratch width - final scratch width)/initial scratch width × 100%.
For the invasion assays, cell suspensions were added to the upper chamber of a Transwell setup, while the lower chamber was filled with complete medium, including different concentrations of butin for drug-treated groups. After 24 h of incubation, the chambers were dried and stained rapidly. Cells were observed under an inverted microscope, and cells in eight random fields per group were counted, with the experiment repeated three times. This process was also applied to the 3rd generation HFLS-RA treated with a 100 mg·L−1 dilution of Matrigel that coated the chamber and incubated overnight at 37 °C; residual liquid was aspirated, and 100 µL of complete medium was added and incubated for 30 min to hydrate the basement membrane. The subsequent steps were the same as the migration assay.
Detection of NLRP3, GSDMD, IL-1β, IL-18, CASP1, CASP3
Determination of LDH levels in cell culture supernatant
LDH levels in the treated cell sample supernatants were measured according to the instructions provided with the assay kit. Different concentrations of LDH standards were prepared, and 60 µL of LDH assay working solution was added to each well, mixed well, and incubated in the dark at room temperature for 30 min. The optical density at 490 nm was read using a microplate reader. LDH content was calculated based on the standard curve.
ELISA measurement of four biomarkers in cell culture supernatant
After treating the cell sample supernatants, 50 µL of the corresponding standards were added followed by color reagents A and B; the mixture was oscillated to mix thoroughly and incubated in the dark for color development, then stop solution was added. The absorbance at 450 nm was measured for each well.
RT-qPCR analysis of mRNA expression of four biomarkers in cell culture supernatant
Following cell treatment, white RNA precipitate was obtained, mixed with ethanol, centrifuged, and dried. 20 µL of DEPC-treated water was added to measure absorbance and calculate RNA purity and concentration. Reverse transcription conditions were as follows: 50 °C for 15 min, 85 °C for 5 min, and 4 °C for 10 min. Primer sequences are listed in Table 1.
Western blot detection of apoptosis-related protein expression
After treating HFLS-RA samples, protein samples were prepared, and PVDF membranes were soaked in blocking solution followed by BSA for phosphorylated proteins. The membranes were then incubated overnight in diluted primary antibody solution, followed by secondary antibody incubation. After pressing with X-ray film, the film was processed. Grayscale values of the films were analyzed using Image-Pro Plus.
Detection of cell apoptosis
Log-phase cells were adjusted to a concentration of 5 × 108 cells/L and incubated in media containing various concentrations of laccaic acid for 48 h. After digestion with trypsin, cells were collected, washed with PBS, and stained with Hoechst stain at 4 °C in the dark for 30 min. The cells were then filtered through a 200-mesh sieve into flow cytometry tubes for cell cycle analysis. Apoptosis rates were measured using flow cytometry with Hoechst and AnnexinV-APC/7-AAD dual staining. For cells at a concentration of 2 × 108 cells/L, after 24 and 48 h of treatment with different concentrations of laccaic acid and subsequent trypsin digestion, cells were collected and immediately analyzed by flow cytometry following kit instructions.
Detection of cell cycle arrest
Log-phase cells were adjusted to a concentration of 5 × 108 cells/L and treated with media containing various concentrations of laccaic acid for 48 h. After trypsin digestion, cells were collected, washed with PBS, and stained with Hoechst stain at 4 °C in the dark for 30 min. The cells were then filtered through a 200-mesh sieve into flow cytometry tubes for cell cycle analysis. Apoptosis rates were assessed using flow cytometry with Hoechst and AnnexinV-APC/7-AAD dual staining. Cells in log phase at a concentration of 2 × 108 cells/L were treated with different concentrations of laccaic acid, digested with trypsin after 24 and 48 h, and immediately analyzed by flow cytometry as per kit instructions.
Statistical analysis
Each experiment was repeated at least three times. Experimental data were analyzed using SPSS 26.0 software, and results were expressed as means ± standard deviation (SD; n = 3). All data were tested for normal distribution and, meeting this criterion, were analyzed by one-way ANOVA for multiple group comparisons. Depending on the results of the variance analysis, either LSD or Tamhane’s T2 method was used for post hoc analysis, with P < 0.05 indicating statistically significant differences. Graphs were generated using GraphPad 9.0 and AI drawing software.
Results
Physicochemical data of butin
The compound extracted from Caulis et Folium Millettiae appeared as a yellow powder with the molecular formula C15H12O5 and a purity of ≥ 96% (Fig. 1A). Structural analysis through NMR and MS is as follows: ESI-MS m/z: 295.4 [M + Na]+. 1H-NMR (600 MHz, CD3OD): δ 7.75 (1H, d, J = 8.4 Hz, H-5), 6.96 (1H, d, J = 1.2 Hz, H-2′), 6.83 (1H, d, J = 7.8 Hz, H-5′), 6.82 (1H, dd, J = 8.4, 2.4 Hz, H-6), 6.52 (1H, dd, J = 7.8, 1.2 Hz, H-6′), 6.38 (1H, d, J = 2.4 Hz, H-8), 5.33 (1H, dd, J = 12.6, 3.0 Hz, H-6), 5.33 (1H, dd, J = 12.6, 3.0 Hz, H-2), 3.03 (1H, dd, J = 12.6, 4.2 Hz, H-3a), 2.70 (1H, dd, J = 16.8, 3.0 Hz, H-3b) (Fig. 1B); 13C-NMR (CD3OD): δ 192.2 (CO), 165.4 (C-7), 164.1 (C-8a), 145.4 (C-3′), 145.1 (C-4′), 130.6 (C-1′), 128.5 (CH-5), 117.9 (CH-6′), 114.9 (CH-5′), 113.6 (C-4a), 113.3 (CH-2′), 110.3 (CH-6), 102.4 (CH-8), 79.7 (CH-2), 43.62(CH2-3) (Fig. 1C). These data are consistent with literature values, confirming the compound as (S)−7,3’,4’-trihydroxyflavone, commonly known as butin.
Physicochemical data of compound butin extracted from Periploca forrestii Schltr. (A) Butin chemical structure formula, (B) Butin structure analysis of hydrogen spectrum, (C) Butin structure analysis of carbon spectrum.
Network pharmacology target protein screening and pathway enrichment analysis
Network pharmacology analysis identified 66 target genes (Fig. 2A). GO enrichment analysis revealed major pathways including positive regulation of phosphorus metabolic process, regulation of inflammatory response, response to oxidative stress, perinuclear region of cytoplasm, extracellular matrix, and protein domain-specific binding. Intersection genes were primarily involved in the KEGG enrichment pathways such as the IL-1 signaling pathway, HIF-1 signaling pathway, and sphingolipid signaling pathway, and osteoclast differentiation (Fig. 2B). Based on previous studies by our group on the Jin Wu Jian Gu prescription (containing Caulis et Folium Millettiae) and its effects on HFLS-RA signaling pathways, the CASP-1/3/IL-1β signaling pathway was selected for further research and validation.
Network pharmacology target protein screening and enrichment analysis for butin.
Inhibition of HFLS-RA migration and invasion by butin
Cell identity was confirmed as HFLS-RA based on morphology and tissue origin (Fig. 3). Compared to the blank control group, the IL-1β stimulation group showed increased cell migration. Compared to the IL-1β stimulation group, the IL-1β + leflunomide group exhibited reduced cell migration; relative to the IL-1β + leflunomide group, the low-concentration butin group showed increased cell migration (P < 0.05), while the medium and high-concentration groups showed decreased migration (P < 0.05). The reduction in cell migration was most significant in the high-concentration group (P < 0.01) (Fig. 4A). Invasion assays revealed that, compared to the blank control, the IL-1β stimulation group had increased invasion numbers (P < 0.05). Compared to the IL-1β stimulation group, the IL-1β + CASP-3 inhibitor group showed reduced cell migration (P < 0.05). Relative to the IL-1β + CASP-3 inhibitor group, the low-concentration butin group exhibited increased invasion numbers (P < 0.05), the medium concentration group showed no statistically significant change (P = 0.09), and the high-concentration group showed reduced migration (P < 0.01) (Fig.4B).
Morphology of HFLS-RA cells. (A) Under the microscope, third-generation HFLS-RA cells appear as dense, elongated spindle shapes.(B) With HE staining, HFLS-RA cells exhibit lightly stained cytoplasm and darkly stained nuclei.(C)Immunofluorescence microscopy reveals the morphology of HFLS-RA cells.(D)Post-immunohistochemical staining, the cellular morphology is depicted.
24-hour Migration and invasion counts of HFLS-RA (means ± standard deviation) (SD; n = 3). ▲P < 0.05 vs. control group; ◇P < 0.05 vs. IL-1β group; *P < 0.05, **P < 0.01 vs. IL-1β + Lef; ns: no statistically significant differences.
Reduction of membrane permeability in HFLS-RA by butin
LDH release assays indicated that, compared to the blank control group, the IL-1β stimulation group had increased LDH release (P < 0.05). Compared to the IL-1β stimulation group, the IL-1β + leflunomide group showed a significant reduction in LDH release (P < 0.01). Relative to the IL-1β + leflunomide group, the low-concentration butin group showed a significant increase in LDH release (P < 0.01), whereas the medium and high-concentration groups showed decreased LDH release, with the most significant difference observed in the high-concentration group (P < 0.01) (Fig.5).
Reduction of LDH release in RA-FLS cells by butin (means ± standard deviation (SD; n = 3). ▲P < 0.05 vs. control group; ◇P < 0.05 vs. IL-1β group; *P < 0.05, **P < 0.01 vs. IL-1β + Lef; ns: no statistically significant differences.
Inhibition of NLRP3, GSDMD, IL-1β, IL-18, CASP1, and CASP3 expression by butin
ELISA results showed that compared to the blank control group, expression of NLRP3, GSDMD, IL-1β, IL-18, CASP1, and CASP3 was significantly increased in the IL-1β stimulation group (P < 0.01). Compared to the IL-1β stimulation group, the IL-1β + caspase-3 inhibitor group showed reduced expression of these markers (P < 0.05). Relative to the IL-1β + leflunomide group, the low and medium concentration butin groups showed significant reductions in GSDMD, IL1β, IL-18, CASP1, and CASP3 expression (P < 0.01), while the high-concentration group showed significant reductions in CASP1 and CASP3 expression (P < 0.01), with no statistical difference in NLRP3 and GSDMD expression (P = 0.32, P = 0.074) (Fig. 6).
Inhibition of NLRP3, GSDMD, IL-1β, IL-18, CASP1, and CASP3 expression levels by butin (means ± standard deviation (SD; n = 3). ▲P < 0.05 vs. control group; ◇P < 0.05 vs. IL-1β group; *P < 0.05, **P < 0.01 vs. IL-1β + Lef; ns: no statistically significant differences.
Inhibition of NLRP3, GSDMD, IL-1β, IL-18, CASP1, and CASP3 mRNA expression by butin
RT-qPCR results indicated that compared to the blank control group, expression of NLRP3, GSDMD, IL-1β, IL-18, CASP1, and CASP3 increased in the IL-1β stimulation group (P < 0.05). Relative to the IL-1β stimulation group, the IL-1β + leflunomide group showed decreased expression of these markers (P < 0.05). Compared to the IL-1β + leflunomide group, the low-concentration butin group exhibited a significant increase in expression (P < 0.05). In the medium concentration group, IL-1β expression decreased (P < 0.05), while NLRP3, GSDMD, IL-18, CASP1, and CASP3 expressions showed no statistical difference with P-values of 0.449, 0.074, 0.802, 0.135, and 0.621, respectively (P > 0.05). In the high-concentration group, IL-1β, IL-18, CASP1, and CASP3 expression significantly decreased (P < 0.01), with CASP1 and CASP3 showing no statistical difference (P = 0.184, P = 0.621) (Fig. 7).
Inhibition of mRNA expression of NLRP3, GSDMD, IL-1β, IL-18, CASP1, and CASP3 by Butin (means ± standard deviation (SD; n = 3). ▲P < 0.05 vs. control group; ◇P < 0.05 vs. IL-1β group; *P < 0.05, **P < 0.01 vs. IL-1β + Lef; ns: no statistically significant differences.
Inhibition of NLRP3, GSDMD, IL-1β, IL-18, CASP1, and CASP3 protein expression by butin
Western blot results showed that compared to the blank control group, protein expression of NLRP3, GSDMD, IL-1β, IL-18, CASP1, and CASP3 increased in the IL-1β stimulation group (P < 0.05). Relative to the IL-1β stimulation group, the IL-1β + leflunomide group exhibited decreased protein expression of these markers (P < 0.05). Compared to the IL-1β + leflunomide group, the low and medium concentration butin groups showed a significant increase in the protein expression of NLRP3, GSDMD, IL-18, CASP1, and CASP3 (P < 0.01), whereas in the high-concentration group, protein expression significantly decreased (P < 0.01). For the low and medium concentration groups, IL-1β protein expression showed no statistical difference with P-values of 0.140 and 0.079, respectively (P = 0.31) (Fig. 8).
Inhibition of protein expression of NLRP3, GSDMD, IL-1β, IL-18, CASP1, and CASP3 by butin (means ± standard deviation (SD; n = 3) 1: blank control group. 2: IL-1β stimulation group.3:IL-1β + Lef group. 4:Butin low-dose group. 5:Butin Medium-dose group. 6:Butin High-dose group.▲P < 0.05 vs. control group; ◇P < 0.05 vs. IL-1β group; *P < 0.05, **P < 0.01 vs. IL-1β + Lef; ns: no statistically significant differences.
Effect of butin on IL-1β-induced apoptosis in HFLS-RA cells
Results indicated that following IL-1β induction, both early and late stages of total apoptosis rates increased in the IL-1β stimulation group compared to the blank control group (P < 0.05). Relative to the IL-1β stimulation group, the IL-1β + leflunomide group showed decreased rates of total apoptosis at both stages (P < 0.05). Compared to the IL-1β + leflunomide group, the low concentration butin group exhibited a significant increase in total early and late apoptosis rates (P < 0.01), whereas the medium and high concentration groups showed decreased rates (P < 0.05), with the most significant reduction observed in the high concentration butin group (P < 0.01) (Fig. 9).
Impact of butin on IL-1β-induced apoptosis in HFLS-RA cells (means ± standard deviation (SD; n = 3). ▲P < 0.05 vs. control group; ◇P < 0.05 vs. IL-1β group; *P < 0.05, **P < 0.01 vs. IL-1β + Lef; ns: no statistically significant differences.
Effect of butin on the cell cycle of IL-1β-induced HFLS-RA cells
Cell cycle analysis revealed that compared to the blank control group, the IL-1β stimulation group showed a decreased proportion of cells in the G0/G1 phase (P < 0.05) and an increased proportion in the G2/M phase (P < 0.05), with no significant change in the S phase proportion (P = 0.075). Relative to the IL-1β stimulation group, the IL-1β + leflunomide group exhibited an increased proportion of cells in the G0/G1 phase (P < 0.05), a decrease in the S phase proportion (P < 0.05), and a decrease in the G2/M phase proportion (P < 0.05). Compared to the IL-1β + leflunomide group, all concentration groups of butin showed a decreased proportion of cells in the G0/G1 phase (P < 0.01), and a significant increase in the S phase proportion (P < 0.01). The low concentration butin group showed a significant increase in the G2/M phase proportion (P < 0.01), the medium concentration group showed a decreased proportion (P < 0.05), and the high concentration group showed no statistical difference (P = 0.573) (Fig. 10).
Effect of butin on the cell cycle of IL-1β-induced HFLS-RA cells (means ± standard deviation (SD; n = 3). ▲P < 0.05 vs. control group; ◇P < 0.05 vs. IL-1β group; *P < 0.05, **P < 0.01 vs. IL-1β + Lef; ns: no statistically significant differences.
Discussion
The primary pathological feature of RA is the persistent inflammation of the synovial membrane and abnormal proliferation of its lining, which plays a crucial role in the proliferation, migration, invasion, and consequent destruction of cartilage surfaces during the development and progression of RA15,16. Our research group, aiming to clarify the effects of butin on HFLS-RA migration and invasion, has confirmed through migration and invasion assays that butin effectively inhibits these processes as well as proliferation. Abnormal cell cycle regulation is one of the internal causes of immune diseases. Cell cycle arrest provides additional time for cells to repair damage, thereby reducing the release and activation of intracellular inflammatory factors17. Flow cytometry results indicate that butin treatment reduces both early and late total apoptosis rates. It is hypothesized that butin may decrease the expression of CASP1 and CASP3 in the upstream apoptosis pathway of HFLS-RA, resulting in cell cycle arrest at the G0/G1 phase. The effect of cell cycle arrest is more pronounced at a high concentration of butin (150 mg/L), elucidating the specific phase of the cell cycle affected by butin in HFLS-RA. Current research on the mechanisms of the cell cycle and apoptosis in HFLS-RA is limited; therefore, further studies on these mechanisms could become an effective approach for treating RA.
NLRP3 inflammasomes play a crucial role in inflammation, acting as tissue damage sensors in the human body. Their core function is to process and promote the release of IL-1β and IL-18. Overactivation of NLRP3, stimulated by pathogens or danger signals within the body, can lead to apoptosis and disrupt the autoimmune system, potentially resulting in various autoimmune diseases such as RA, systemic lupus erythematosus, and ankylosing spondylitis22,23,24,25. Studies have shown that NLRP3 and its downstream products are significantly involved in the pathological mechanisms of RA. Experiments have demonstrated that during exacerbations of RA, levels of NLRP3 and ASC proteins in the peripheral blood and synovial fluid of patients are significantly higher than in controls. The inhibition of NLRP3 and CASP1 significantly reduces IL-1β expression26. CASP3, through its interaction with the N-terminal of GSDME and the cell membrane, participates in apoptosis, thereby alleviating the exacerbation of RA inflammation27.
Butin may directly inhibit CDK6 kinase activity, thereby reducing apoptosis28. In a setting where ASC and pro-Caspase1 expression remain stable, the quantity of NLRP3 is closely related to its regulation and activation. NLRP3 is expressed in various cell types, including neutrophils, monocytes, dendritic cells, and some macrophages. Clinical observations have noted elevated levels of NLRP3 mRNA and NLRP3-related proteins in RA patients29. Expression of ASC varies by cell type under different stimuli30, and in RA animal studies, ASC not only facilitates the modeling of CIA rats but also plays a role in the early immune response31. Key apoptotic proteins CASP1 activate IL-1β and IL-18 and can also perforate the cell membrane, thereby increasing the intracellular presence of IL-1β and IL-1832. Studies suggest that in the Caspase family, CASP3 also participates in GSDMD/GSDME-mediated membrane perforation, leading to apoptosis33,34. Our experimental results found a strong positive correlation between CASP1 expression and GSDMD, IL-1β, IL-18, further confirming the validity and authenticity of our experiment. Following IL-1β stimulation, elevated expression of NLRP3, GSDMD, CASP1, CASP3, IL-1β, and IL-18 in HFLS-RA cells and significantly increased LDH levels in the culture supernatant were observed, with a massive release of CASP1, CASP3, IL-1β, IL-18. RT-qPCR and WB experiments showed that Butin intervention significantly reduced the expression of NLRP3, GSDME, CASP3, IL-1β, IL-18. Thus, Butin inhibits upstream apoptosis axis activation of CASP1, CASP3, reduces NLRP3, GSDMD production, decreases membrane perforation, and limits the outflow of intracellular inflammatory factors, effectively preventing apoptosis. By reducing immune stress within and outside the body of RA patients, butin helps restore natural immunity balance, a significant mechanism in treating RA.
In recent years, components of traditional Chinese medicine have also played a crucial role in apoptosis. Pomegranate polyphenols can inhibit the NF-κB signaling pathway, reducing CASP1 expression in a collagen-induced arthritis mouse model, thereby decreasing apoptosis and improving synovial inflammation19. Paeoniflorin derivatives can inhibit the proliferation of macrophages in adjuvant-induced arthritis rats within the TLR4/NLRP3/GSDMD signaling pathway, thereby alleviating joint inflammation35. Triptolide can suppress cell inflammation by inhibiting mitochondrial autophagy and inflammasome activation36. This study, by constructing an HFLS-RA model and employing various experimental methods to examine classical apoptotic pathway inflammatory factors NLRP3, GSDMD, CASP1, CASP3, IL-1β, and IL-18, found that butin significantly inhibits their expression, particularly at high concentrations. A comparative analysis revealed that the most pronounced inhibitory effects of butin on inflammatory factors were on CASP1 and CASP3, followed by IL-1β and IL-18. This indicates that the extent of inflammation in HFLS-RA is closely related to its proliferation and apoptosis. High activation of CASP1 is a primary factor inducing apoptosis, as apoptotic cells release large amounts of inflammatory factors, which then promote the abnormal proliferation of HFLS-RA. Thus, by inhibiting CASP1 activation, butin reduces cell apoptosis and lowers the release of inflammatory factors, stimulating abnormal proliferation of synovial cells, which is one of its mechanisms of action in treating RA. Additionally, the study found that HFLS-RA apoptosis is not only dependent on CASP1 but also involves CASP3. Using leflunomide as a control in clinical RA treatment, experimental results showed that butin’s medium concentration has a comparable inhibitory effect on HFLS-RA apoptosis and proliferation to leflunomide, while its high concentration has a superior effect.
Conclusion
In summary, butin exhibits effective inhibition of HFLS-RA proliferation in vitro and induces cell cycle arrest at the G0/G1 phase, thereby effectively inhibiting HFLS-RA proliferation. Butin regulates the NLRP3/CASP-1/GSDMD apoptosis axis, inhibiting the activity of the upstream core protease CASP1, reducing the production and release of NLRP3, IL-1β, and IL-18. It also inhibits the synthesis of the membrane-perforating protein GSDMD, decreasing the outflow of inflammatory factors, and reducing the release of pro-inflammatory factors induced by apoptosis that contribute to the abnormal proliferation of HFLS-RA, which is one of the potential mechanisms in its treatment of RA. This study has limitations as it only involved cellular experiments. The research group plans to further substantiate these results through animal experiments in subsequent studies.
Data availability
The datasets generated during and/or analyzed during the current study are available upon request from the corresponding author.Acknowledgments.
References
Alivernini, S., Firestein, G. S. & McInnes, I. B. The pathogenesis of rheumatoid arthritis. Immunity 55(12), 2255–2270 (2022).
Hasan, A. A., Khudhur, H. R. & Hameed, A. K. Rheumatic autoimmune diseases (focus on RA): prevalence, types, causes and diagnosis. Karbala J. Pharm. Sci., 1(20). (2022).
Tian, X. P. & Zeng, X. F. Relying on the guidelines, standardize the diagnosis and treatment of rheumatoid arthritis, and implement thestandard treatment. Chin. J. Intern. Med. 57(4), 2404–241 (2018).
Mao, J. et al. Neutrophil extracellular traps induce pyroptosis of rheumatoid arthritis fibroblast-like synoviocytes via the NF-κB/caspase 3/GSDME pathway. Inflammation 47(3), 921–938 (2024).
Li, Z. T. et al. The role of synovial fibroblast pyroptosis in the pathogenesis of rheumatoid arthritis and its intervention of Chinese medicine . Rheum. Arthritis 12(04), 37–41 (2023).
Abu Khweek, A. & Amer, A. O. Pyroptotic and non-pyroptotic effector functions of caspase-11. Immunol. Rev. 297(1), 39–52 (2020).
Weir, A. & Vince, J. E. No longer married to inflammasome signaling: the diverse interacting pathways leading to pyroptotic cell death. Biochem. J. 479(10), 1083–1102 (2022).
Liu, Z. et al. Caspase-1 engages full-length gasdermin D through two distinct interfaces that mediate caspase recruitment and substrate cleavage. Immunity 53(1), 106–114 (2020).
Wang, P. et al. Thrombospondin-1 as a potential therapeutic target: multiple roles in cancers. Curr. Pharm. Design 26(18), 2116–2136 (2020).
Ma, W. K. et al. Study on the anti-inflammatory effect of total extract on synovial cells in rheumatoid arthritis. J. Guiyang Coll. Traditional Chin. Med. 39(3), 58–61 (2017).
Huang, M. J. et al. Anti-rheumatoid arthritis effect of black vine and its molecular mechanism. Chin. J. Experimental Formula 17(12), 174–177 (2011).
Hou, Y. T. et al. Study on the effect and mechanism of compound black vine against rheumatoid arthritis. Sichuan Normal Univ. J. 39(1), 124–126 (2016).
Ren, Q. et al. Flavonoid Fisetin Alleviates Kidney Inflammation and Apoptosis Via Inhibiting Src-mediated NF-κB p65 and MAPK Signaling Pathways in Septic AKI mice[J]122109772 (Biomedicine & Pharmacotherapy, 2020).
Yang, W. et al. Fisetin improves lead-induced neuroinflammation, apoptosis and synaptic dysfunction in mice associated with the AMPK/SIRT1 and autophagy pathway. Food Chem. Toxicol. 134, 110824 (2019).
Sim, H. et al. Fisetin suppresses pulmonary inflammatory responses through Heme oxygenase-1 mediated downregulation of inducible nitric oxide synthase. J. Med. Food 23(11), 1163–1168 (2020).
Chenxu, G. et al. Fisetin protects against high fat diet-induced nephropathy by inhibiting inflammation and oxidative stress via the blockage of iRhom2/NF-κB signaling. Int. Immunopharmacol. 92, 107353 (2021).
Wang, X. et al. Fisetin suppresses chondrocyte senescence and attenuates osteoarthritis progression by targeting Sirtuin 6. Chemico-Biol. Interact. 390, 110890 (2024).
Ma, W. K. et al. Effects of Miao medicine Jinwu Jiangu formula on synovial angiogenesis in rheumatoid arthritis. China J. Tradit Chin. Med. Pharm. 34(10), 4571–4575 (2019).
Ma, W. K. et al. The effect of Miao medicine Jinwu Jiangu Decoction on the autophagy regulation of synovial cells in rheumatoid arthritis. J. Chin. Med. Mater. 42(4), 891–896 (2019).
Ma, W. K. et al. Effects of medicated serum frozen powder of Jinwu Jiangu formula on synovial cell proliferation in rheumatoid arthritis. China J. Tradit Chin. Med. Pharm. 32(4), 1739–1742 (2017).
Hu, Y. et al. Periplogenin suppresses the growth of esophageal squamous cell carcinoma in vitro and in vivo by targeting STAT3. Oncogene 40(23), 3942–3958 (2021).
Kim, H. Y., Kim, S. J. & Lee, S. M. Activation of NLRP 3 and AIM2 inflammasomes in Kupffer cells in hepatic ischemia/reperfusion. FEBS J. 282(2), 259–270 (2015).
Liu, H. et al. NLRP3 inflammasome induced liver graft injury through activation of telomere-independent RAP1/KC axis. J. Pathol. 242(3), 284–296 (2017).
Shen, H. H. et al. NLRP3:A promising therapeutic target for autoimmune diseases. Autoimmun. Rev. 17(7), 694–702 (2018).
Marie, W. H. & Thomas, D. Immunopathogenic mechanisms of systemic autoimmune disease. Lancet 382(9894), 819–831 (2013).
Zhao, Z. Q. & Xu, J. Progress in the nucleotide-binding oligomerization of the domain-like receptor 3 inflammasome in rheumatoid arthritis. Chin. J. Rheum. 21(5), 352–355 (2017).
Wang, Y. et al. Chemotherapy drugs induce pyroptosis through caspase-3 cleavage of a gasdermin. Nature 547(7661), 99–103 (2017).
Lu, H. et al. Crystal structure of a human cyclin-dependent kinase 6 complex with a flavonol inhibitor, fisetin. J. Med. Chem. 48(3), 737–743 (2005).
Shen, H. et al. NLRP3:A promising therapeutic target for autoimmune diseases. Autoimmunity. Reviews. 17(7), 694–702 (2018).
Agrawal, I. & Jha, S. Comprehensive review of ASC structure and function inimmune homeostasis and disease. Mol. Biol. Rep. 47(4), 3077–3096 (2020).
Yamazaki, H. et al. ASC plays a role in the priming phase of the immune response to type II collagen in collagen-induced arthritis. Rheumatol 32(6), 1625–1632 (2012).
Marzano, A. V. et al. A dermatologic perspective on autoinflamma -tory diseases. Clin. Exp. Rheumatol. 36(1), 32–38 (2018).
Toldo, S. et al. Inflammasome,pyroptosis,and cytokines in myocardial ischemia-reperfusion injury. Am J Physiol Heart Circ Physiol, 315(6): H1553-H1 568. (2018).
Julien, O. & Wells, J. A. .Caspases and their substrates. Cell. Death Differ. 24(8), 1380–1389 (2017).
Ge, G. et al. Punicalagin ameliorates collagen-induced arthritis by downre -gulating M1 macrophage and pyroptosis via NF-κB signaling pathway. Sci. China Life Sci. 65(3), 588–603 (2022).
Kang, Y. H. et al. Effect of triptolide on mitochondrial autophagy, activation of NLRP3 inflammatome and pyroptosis of fibroblast synoviocytes in rheumatoid arthritis. Drugs Clin. 39(2), 290–295 (2024).
Acknowledgements
Figures were generated with BioRender.com under the agreement.
Funding
This work was supported by grants from The National Natural Science Foundation of China (No.82274678, No.82405366); Young Science and Technology Talent Growth Project of Guizhou Education Department (Guizhou Education Technology [2024] No.123).
Author information
Authors and Affiliations
Contributions
H. L. and Y.Z. Y. : developing the conceptual framework, investigating the methodology, gathering data, Cell experiments, and writing the original draft.X.L. Y. developing the conceptual framework, investigating the methodology, and gathering data. X. M.and Y. L.: investigation, review, and editing. W.K. M.: conceptualizing, reviewing, and editing. All authors contributed to the article and approved the submitted version. Final approval of the manuscript was given by all authors.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests..
Ethics approval and consent to participate
This study was approved by The Second Affiliated Hospital of Guizhou University of Chinese Medicineand(YJZ2020010093) adhered to the Helsinki Declaration guidelines Verbal.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Li, H., Yang, Y., Ma, X. et al. Butin regulates the NLRP3/CASP-1/GSDMD pyroptosis axis to inhibit proliferation and pyroptosis in human fibroblast-like synoviocytes of rheumatoid arthritis. Sci Rep 15, 33090 (2025). https://doi.org/10.1038/s41598-025-17239-z
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-17239-z