Abstract
The bone marrow microenvironment influences acute myeloid leukemia (AML) progression. Mesenchymal stem cell–like (MSC-l) populations may exert tumor-modulating effects, but their prognostic role remains uncertain. We retrospectively analyzed 65 adult AML patients (excluding acute promyelocytic leukemia) treated with intensive chemotherapy between 2017 and 2024 at four Spanish institutions. MSC-l cells were identified in BM aspirates at end of treatment by multiparameter flow cytometry (CD13bright/CD45low/CD34neg/CD117neg/CD11bneg/CD16neg/CD71neg/CD64neg). Patients were stratified using a 0.265%cutoff (MSC-lHIGH ≥ 0.265% and MSC-lLOW < 0.265%). Survival was assessed with Kaplan–Meier and Cox regression, adjusting for age and ELN 2017 risk. MSC-lHIGH patients had inferior overall survival (OS) (median 0.66 years vs. not reached; P < 0.001) and relapse-free survival (RFS) (median 1.27 years vs. 1.49 years; P = 0.027). These associations persisted across ELN risk groups. Multivariate analysis confirmed MSC-lHIGH status as an independent predictor of worse OS (HR = 6.43; 95% CI 2.53–16.33; P < 0.001) and RFS (HR = 4.8; 95% CI 1.71–13.47; P = 0.003). MSC-l levels were lower in patients receiving myeloablative conditioning compared with non-transplanted patients, suggesting transplant intensity may influence MSC dynamics. Higher post-treatment MSC-l proportions are associated with poorer survival, independent of ELN risk and age, supporting their potential as a prognostic biomarker in AML.
Similar content being viewed by others
Introduction
Acute myeloid leukemia (AML) is a hematologic neoplasm characterized by the uncontrolled proliferation of abnormal myeloid progenitor cells1. AML arises from a series of genetic and epigenetic changes, primarily affecting hematopoietic stem and progenitor cells (HSPCs)2,3
The pathogenesis of AML, as well as other hematological malignancies, depends not only on intrinsic tumoral factors but is also influenced by the bone marrow (BM) microenvironment4,5. The BM microenvironment includes a complex network of extracellular matrix proteins, soluble growth factors, cytokines and distinct-though possibly overlapping- cellular niches, such as the endosteal (or osteoblastic) and vascular niches. Several studies have demonstrated that blast cells can manipulate the marrow microenvironment to create a permissive conditions that favors disease initiation, progression and therapeuticresistance6,7,8. Mesenchymal stem cells (MSCs) play a decisive role in this process, known as “stromal plasticity”. MSCs are non-hematopoietic multipotent stem cells characterized by their self-renewal capacity, clonogenic efficiency and multilineage differentiation capacity9. Furthermore, MSCs may influence the development of various diseases, including hematological malignancies such as chronic myeloid leukemia, multiple myeloma, and myelodysplastic syndrome/AML10,11,12.However, despite extensive research over the past decade, it remains unclear whether MSCs have tumor-promoting or tumor-suppressive effects, and their precise role in AML is yet to be determined13,14.
CD13, also known as aminopeptidase N, is a transmembrane metalloprotease widely recognized as a surface marker in flow cytometric analysis of MSCs and various progenitor cell populations. Its expression is commonly used as part of a panel of positive markers, including CD73 and CD90, to identify MSCs in accordance with the minimal criteria proposed by the International Society for Cellular Therapy (ISCT)15. Beyond its utility as a phenotypic marker, CD13 plays functional roles in cellular adhesion, migration and differentiation. In flow cytometry, anti-CD13 monoclonal antibodies enable the reliable detection and isolation of MSCs based on differential surface expression, thereby supporting downstream applications in regenerative medicine and cellular therapies16.Recently, our group identified a CD13-bright cell population enriched for canonical MSC markers CD105 and CD90 in myelodysplastic syndromes (MDS) patients at diagnostic. Notably, these MSC-like cells were found to be apredictor of progression to AML17.
In recent years, the introduction of new drugs into the AML therapeutic arsenal has improved the prognosis, but survival rates vary greatly depending on the characteristics of the disease, in particular genetic abnormalities included in the ELN risk score2. However, in every ELN risk group patients show differences in outcome and we should try to refine prognosis of patient as much as possible for appropriate consolidation treatment. In light of these considerations, in this manuscript we explore the potential of MSCs-l as a prognostic factor in intensively treated AML patients.
Results
65 AML patients treated with intensive chemotherapy, showed MSCs-l measured by multiparameter flow cytometry (MFC) at the end of treatment (post-induction treatment: induction-1 (n = 18) and induction-2 (4); post-consolidation treatment: consolidation-1 (n = 9), consolidation-2 (n = 5) and consolidation-3 (n = 7) and post-allogeneic hematopoietic stem cell transplantation (allo-HSCT, n = 22) (Fig. 1).The median age of this group was 58 years (range 18–77 years); 32 males and 33 females. Table 1 shows the baseline characteristics of AML, the proportion of MSCs-l at the end of treatment, and the therapies administered to these 65 patients. Six out of 15 (40%), 8 out of 28 (29%)and 8 out of 22 (36%) patients with favorable, intermediate and adverse risk according to ELN 20172 underwent allo-HSCT (P = 0.108).
Flowchart summarizing the distribution of 65 intensively treated adult AML patients with available MSC-l data at the end of treatment. Abbreviations: MSCs-l, mesenchymal stem cells-like; allo-HSCT, allogeneic hematopoietic stem cell transplantation.
Impact of MSCs-l determination at end of treatment
We set 0.265% as the cutoff for MSC-l quantification (MSC-lLOW: < 0.265% and MSC-lHIGH ≥ 0.265%) based on the total analyzed BM cellularity (excluding debris). ROC curve analysis yielded an area under the curve (AUC) of 0.722 (95% CI 0.596–0.848), indicating a fair discriminatory performance of MSC-l levels in relation to survival outcomes. The optimal cutoff value of 0.265% was determined trying to boost its specificity to confidently identify patients with worse outcomes. The resulting J (youden index) value was 0.425, with a sensitivity of 0.48 and specificity of 0.94, thereby defining the threshold for categorizing patients into MSC-lHIGH and MSC-lLOW groups.
In the analysis of OS, theMSCs-l determination showed that 48 patients (74%)were MSCs-lLOW and 17 patients (26%) were MSCs-lHIGH. In the MSCs-lLOW group, the median OS wasnot calculable (NC), while in the MSCs-lHIGH group, the median OS was 0.66 years (95% CI 0.28–1.04). When comparing the two subgroups using a log-rank test, MSCs-lHIGH patients had significantly reduced OS (P < 0.001).The RFS analysis was performed on 51 patients: MSCs-lLOW (n = 40) and MSCs-lHIGH (n = 11). In the MSCs-lLOW group, the median RFS was 1.49 years (95% CI 0.01–3.51), while in the MSCs-lHIGH group, the median RFS was 1.27 years (95% CI 0.02–2.52). A log-rank test showed significantly reduced RFS in MSCs-lHIGH patients (P = 0.027) (Fig. 2).
Clinical outcome stratified according to proportion of MSCs-l at end of treatment for all patients treated with intensive chemotherapy. (A) Overall survival (MSCs-l < 0.265%, n = 48, and MSCs-l ≥ 0.265%, n = 17; HR = 4.941 (95% CI 2.409–10.136). (B) Relapse-free survival (MSCs-l < 0.265%, n = 40, and MSCs ≥ 0.265%, n = 11; HR = 2.630 (95% CI 1.083–6.387). MSCs-l, mesenchymal stem cells-like.
A stratified analysis by the ELN 2017 genetic risk classification2 was performed. In the analysis of OS, the distribution of MSCs-l determination was as follows: 13 patients (20%) with MSCs-lLOWand 2 patients (3%) with MSCs-lHIGHin the favorable-risk group, 20 patients (31%) with MSCs-lLOW and 8 patients (12%) with MSCs-lHIGHin the intermediate-risk group, and 15 patients (23%) with MSCs-lLOW, and 7 patients (11%) with MSCs-lHIGHin the adverse-risk group. The OS in the favorable group was NC in MSCs-lLOW and 0.4 years (95% CI NC) in MSCs-lHIGH. The OS in the intermediate group was 3.4 years (95% CI NC) in MSCs-lLOWand 0.9 years (95% CI:0.3–1.4) in MSCs-lHIGH. The OS in the adverse group was 1.4 years (95% CI:0.1–2.6) in MSC-lsLOW and 0.4 years (95% CI:0.3–0.6) in MSCs-lHIGH. A log-rank test comparing subgroups according to genetic risk showed a reduced OS in MSCs-lHIGH patients (P ≤ 0.001) (Fig. 3).
Clinical outcome stratified according to proportion of MSCs-l at end of treatment for all patients treated with intensive chemotherapy. (A–C) OS according to proportion of MSCs-l and 2017 ELN genetic risk: A, favorable risk, MSCs-l < 0.265%, n = 13 and MSCs-l ≥ 0.265%, n = 2, HR = not significant (NS); B, intermediate risk, MSCs-l < 0.265%, n = 20 and MSCs-l ≥ 0.265%, n = 8, HR = 3.4 (95% CI 1.224–9.447); (C), adverse risk, MSCs-l < 0.265%, n = 15, and MSCs-l ≥ 0.265%, n = 7, HR = 2.972 (95% CI 1.002–8.817). (D–F) RFS according to proportion of MSCs-l and 2017 ELN genetic risk: (D), favorable risk, MSCs-l < 0.265%, n = 12 and MSCs-l ≥ 0.265%, n = 2, HR = NS; (E) intermediate risk, MSCs-l < 0.265%, n = 17 and MSCs-l ≥ 0.265%, n = 5, HR = NS; (F) adverse risk, MSCs-l < 0.265%, n = 11 and MSCs-l ≥ 0.265%, n = 4, HR = NS. MSCs-l, mesenchymal stem cells-like.
In the analysis of RFS, the distribution was as follows: 12 patients (24%) with MSCs-lLOWand 2 patients (4%) with MSCs-lHIGHin the favorable-risk group, 17 patients (33%) with MSC-lsLOW and 5 patients (10%) with MSCs-lHIGHin the intermediate-risk group, and 11 patients (22%) with MSCs-lLOW, and 4 patients (8%) with MSCs-lHIGH in the adverse-risk group.The RFS in the favorable group was 1.47 years (95% CI 0.01–3.42) in MSCs-lLOWand NC inMSCs-lHIGH. The RFS in the intermediate group was 1.49 years (95% CI 0.47–2.50) in MSCs-lLOW and 1.27 years (95% CI NC) in MSCs-lHIGH. The RFS in the adverse group was not calculable in MSCs-lLOW and 0.18 years (95% CI 0.01–1.21) in MSCs-lHIGH(Fig. 2). A log-rank test comparing subgroups according to genetic risk showed a reduction of RFS in MSCs-lHIGH patients (P = 0.05). Cox regression analysis for OS prediction showed that age, ELN 2017 classification2 and the proportion of MSCs-l were independent predictor factors (P = 0.02, HR:0.27, [95% CI 0.09–0.79], P = 0.03, HR: NC, [95% CI NC] and P < 0.01, HR:11.68, [95% CI 3.80–35.9], respectively). Cox regression analysis for the RFS prediction showed that proportion of MSCs-l was an independent predictor factor (P = 0.03, HR:3.38, [95% CI 1.15–9.96]. Age and ELN 2017 classification2were not independent predictors factors (P = 0.37, HR: 0.63, [95% CI 0.23–1.72] and P = 0.87, HR: NC, [95% CI NC], respectively). Proportional hazard assumptions were checked by adding the interaction of every variable with time in every analysis performed.
Multivariate Cox regression analysis for OS identified a MSC-l proportion ≥ 0.265% as an independent predictor of increased mortality (HR = 6.43; 95% CI 2.53–16.33;P < 0.001). Adverse ELN 2017 risk was also associated with worse OS (HR = 15.78; 95% CI 3.36–74.15; P < 0.001), whereas the intermediate-risk category did not reach statistical significance (HR = 4.28; 95% CI 0.96–19.1; P < 0.057) (global P for the variable < 0.001). Age at diagnosis was not significantly associated with overall survival (HR = 0.98; 95% CI 0.96–1.01; P = 0.235), indicating no independent prognostic effect in this cohort. Both reduced-intensity (HR = 0.14; 95% CI 0.04–0.51; P = 0.003) and myeloablative conditioning (HR = 0.15; 95% CI 0.03–0.71; P = 0.017) (global P for the variable = 0.001) were linked to a lower risk of death, suggesting a protective effect of allo-HSCT regardless of conditioning intensity (Fig. 4A).
Multivariate Cox regression analysis for overall survival (OS) and relapse-free survival (RFS) according to age, ELN 2017 risk classification and allogeneic hematopoietic stem cell transplantation (allo-HSCT). Abbreviations: HR, hazard ratio; CI, confidence interval; RIC, reduced intensity conditioning and MAC, myeloablative conditioning.
Multivariate Cox regression analysis for RFS identified a MSC-l proportion ≥ 0.265% as an independent predictor of increased risk of relapse or death (HR = 4.80; 95% CI 1.71–13.47; P = 0.003), highlighting the adverse prognostic impact of elevated MSC-l levels. Age at diagnosis was not significantly associated with RFS in this model (HR = 1.01; 95% CI 0.98–1.05; P = 0.506).Among transplantation-related factors, reduced-intensity conditioning was significantly associated with a lower risk of relapse or death (HR = 0.14; 95% CI 0.03–0.66;P = 0.013), whereas myeloablative conditioning did not show a significant effect in this model (HR = 1.85; 95% CI 0.59–5.77; P = 0.291) (global P for the variable = 0.022). Neither intermediate ELN 2017 risk (HR = 1.94; 95% CI 0.74–5.12; P = 0.179) nor adverse risk (HR = 2.25; 95% CI 0.77–6.62; P = 0.141) showed predictive power for RFS (global P for the variable = 0.264) (Fig. 4B).
We also explored the prognostic performance of MSC-l quantification at earlier time points. The area under the ROC curve (AUC) for MSC-l levels at diagnosis was 0.653 and after induction therapy was 0.67, both lower than 0.722 observed at the end of treatment.
Impact of allo-HSCT on MSC-l quantification
A one-way ANOVA test was conducted to evaluate differences in MSC-l proportion at the end of treatment according to transplant status and conditioning intensity. The analysis revealed a statistically significant difference among the three groups—non-transplanted patients, patients receiving reduced-intensity conditioning (RIC) and those receiving myeloablative conditioning (MAC) (P = 0.024). Median MSC-l were 0.1, 0.15 and 0.04 in the non-transplanted, RIC and MAC groups respectively. Patients treated with MAC had significantly lower MSC-l percentages compared to non-transplanted patients (P = 0.020). No significant differences were found between the non-transplanted and RIC groups (P = 1) or between the RIC and MAC groups (P = 0.246).
In vitro expansion, and osteogenic, adipogenic and chondrogenicdifferentiation of MSCs-l
In order to identify similarities between MSC-1 and previously described MSC-like cells17 we conducted comparable sorting and culture experiments. MSC-1 cells exhibited similar enrichment of canonical CD105 and CD90 MSC markers and equivalent attachment potential to MSC-like cells (Fig. 5).
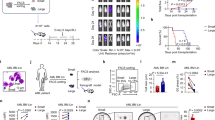
Gating strategy for MSC-l cell sorting. (A) MSC-l cells expressing CD13brightCD45low/negCD105posCD90pos surface markers were isolated from low-density bone marrow samples of AML patients. (B) Brightfield images of culture growth of CD13brightCD45low/neg CD105pos and CD90pos MSC-l cells. The white arrows highlight cells displaying characteristic MSC-l morphologies, such as elongated spindle shapes and cuboidal or polygonal forms, demonstrating successful culture and growth of MSC-l cells. Scale bar 200 µm.
Discussion
This study shows that the proportion of MSCs-l at the end of treatment has prognostic impact on survival and relapse in newly diagnosed AML patients treated with front-line intensive regimens. We analyzed the MSCs-l compartment in 65 adult AML patients treated with intensive chemotherapy and evaluated its clinical applicability using a cutoff of 0.265% which showed a high specificity to confidently detect patients with worse outcome. Among demographic, clinical and biological variables evaluated after stratifying by the MSC-l cutoff, only age demonstrated statistical significance in the univariate analysis; however, this association was not retained in the multivariate model. Patients with MSCs-l proportions ≥ 0.265%, regardless of their ELN 2017 genetic risk category2 (favorable, intermediate, or adverse), had significantly shorter OS and RFS in both global and ELN-stratified analyses.We acknowledge that the small number of MSCs-lHIGHpatients in the favorable-risk group (n = 2) limits statistical power in this subgroup; however, the consistent prognostic trend across all ELN categories suggests that the observed impact of MSCs-l is not solely driven by individual strata.In multivariate Cox analysis for OS, MSCs-l ≥ 0.265%, age and ELN 2017 genetic risk classification2 were all independently associated with prognosis. In contrast, for RFS, only the MSCs-l proportion remained an independent prognostic factor.
These data suggest that MSCs-l cells may contribute to AML pathogenesis and prognosis and more importantly, add prognostic value beyond already established factors such as age and ELN risk classification2. To our knowledge, no previous studies have specifically addressed the prognostic significance of MSCs-l in AML. Our findings are consistent with observations in solid tumors, such as glioblastoma, where MSCs-l and fibroblasts have been shown to promote microvascular proliferation and foster an immunosuppressive microenvironment, ultimately contributing to disease progression and poor prognosis18. These parallels suggest that MSC-like cells may exert similar immunomodulatory and pro-survival functions in AML, potentially facilitating immune evasion and the persistence of chemoresistant leukemic clones. Thus, the presence and dynamics of MSCs-l in the bone marrow microenvironment may represent not only a novel prognostic marker, but also a potential therapeutic target in AML.
Our study also highlights the role of allo-HSCT as a modifying factor of MSC-l levels. Moreover, lower MSC-l levels observed in MAC patients suggest that high-intensity regimens may exert a stronger suppressive effect on the mesenchymal niche, potentially disrupting stromal-mediated leukemic support. However, further prospective studies are needed to explore the biological mechanisms underlying these observations.
Although our primary analysis focused on MSC-l assessment at the end of treatment, we also explored their prognostic value at earlier time points (diagnosis and post-induction therapy). In these exploratory analyses, MSC-l levels showed lower predictive accuracy for overall survival, with AUC values of 0.653 at diagnosis and 0.670 after induction therapy, compared with 0.722 at the end of treatment. These results suggest that early MSC-l determination may have limited prognostic value in our cohort.
Our study has some limitations. The flow cytometry panel used did not include classical MSC markers such as CD73, CD90, and CD105 and therefore does not meet the minimal criteria established by the International Society for Cellular Therapy (ISCT) for definitive MSC identification. However, the specificity and reliability of these markers are limited, as they are not exclusive to MSCs and show variable expression depending on donor and spatial context20. Despite the absence of these markers, the CD13bright population—defined by the exclusion of hematopoietic and myeloid lineage markers—displayed mesenchymal characteristics such as plastic adherence and in vitro expansion, although it failed to undergo trilineage differentiation. This may be due to the limited cell numbers available or intrinsic functional alterations in the pathological mesenchymal compartment. Moreover, flow cytometry data indicated that endothelial cells and fibroblasts may also be present within the CD13brightgate; however, these can be distinguished based on CD34 expression and CD13 mean fluorescence intensity (MFI), which are lower than in MSCs-l. Fibroblasts, in particular, require enzymatic digestion for recovery and typically show CD13 MFI values similar to endothelial cells. Hematopoietic cells, in contrast, express minimal or no CD13 and were excluded based on marker expression. Taken together, these findings support the identification of the analyzed population as predominantly mesenchymal in nature.
In summary, in our cohort of 65 intensively treated AML patients, we propose that the proportion of MSCs-l at the end of treatment may serve as an independent prognostic factor. Specifically, the categorical variable MSCs-l enhances risk stratification beyond ELN classification and age for OS and remains the only independent predictor for RFS. These findings warrant validation in larger prospective cohorts. If confirmed, future studies should aim to characterize this population in greater detail, including functional differentiation assays, and explore its therapeutic potential in AML, a disease that remains highly aggressive and prone to relapse.
Material and methods
Patients and samples
The primary patient and disease characteristics were collected retrospectively, including: age, sex, cytomorphological assessment, AML diagnosis confirmation (according to the site´s routine practice), cytogenetics, molecular studies, description of the front-line treatment approach, disease response assessments and disease follow-up19. Patients diagnosed with acute promyelocytic leukemia (APL) were excluded. We reviewed data collected from 65 intensively treated adult AML patients with available MSC-l data measured by flow cytometry (MFC) at the end of treatment. These patients were diagnosed between 2017 and 2024 at Hospital Universitario Fundación Jiménez Díaz, Hospital Universitario Rey Juan Carlos, Hospital Universitario General de Villalba, and Hospital Universitario Infanta Elena, all in Madrid (Spain).
Written informed consent was obtained from all study participants. Approval of the study was obtained from the Clinical Research Ethics Committee of the Hospital Universitario Fundación Jiménez Díaz (TFG017-19_FJD). The study complied with the Declaration of Helsinki.
MSCs-l screening
MFC immunophenotypic studies were performed on BM aspirate samples, processed under sterile conditions within 24 h of collection. The pre-filtered bone marrow sample (EDTA) is incubated for 15 min with a combination of eight pre-selected monoclonal antibodies (MoAb) which were used to identify and characterize BM MSCs-l (Table 2). Erythrocytes were subsequently lysed with BD FACS™ solution for 10 min (BD Biosciences), followed by two washes with PBS (Inova Diagnostics). The FACS Canto II flow cytometer (Becton Dickinson Biosciences, San Jose, CA, USA) was used to acquire a minimum of 500.000 events per tube (two tubes analyzed). Infinicyt™ software (Cytognos SL, Salamanca, Spain) was used to analyze the main leukocyte subpopulations in the generated FCS files. Regarding MSCs-l gating strategy, a retrospective search for phenotypic information on MSCs-l was performed in the flow cytometry files of 65 AML patients. The phenotypic analysis of AML MSCs-l was adjusted from Muñiz et al21 considering that CD105 and CD90 were not routinely included in our routine AML monitoring panel. A bright CD13-positive population was identified, which was negative for CD34, CD45, CD117, CD11b, CD16, CD71 and CD64. This population is referred to as the MSC-like (MSC-l) compartment (Fig. 6). Gates were set according to the appropriate isotype control, and the expression of each marker was reported as the percentage of positive cells of total BM nucleated cells, excluding debris.
Gating strategy to identify the mesenchymal stem cells-like (pink cells).
In vitro expansionof MSCs-l
The same sorting strategy and culture methods described by the group (17) were employed based on the CD13brightCD45low/negCD105posCD90pos population for further studies on MSC-like cells to confirm their MSC identity. A total of three samples were analyzed to isolate the MSC-like phenotype from erythrocyte-depleted low-density bone marrow cells. Then, cells were stained for phycoerythrin (PE) anti-CD13 (clone WM15) (Beckton Dickinson), fluorescein (FITC) anti-CD45 (clone T29/33) (Dako), allophycocyanin (APC) anti-CD105 (clone 43/A3) (Beckton Dickinson) and violet 450 anti-CD90 (clone 5E10) (Beckton Dickinson). Cell sorting was conducted using a FACSMelody™ Cell Sorter (Becton Dickinson) equipped with three lasers and FACSChorus™ software. Subsequent flow cytometry analysis was performed using FlowJo v.10.9.0.
Statistical analysis
Quantitative variables were compared with Mann–Whitney test. Qualitative variables were compared by Chi-square test or Monte Carlo simulation in case expected frequencies in cells were below. One-way ANOVA test was employed to compare the proportion of MSC-l in non-transplanted patients vs allo-HSCT with RIC and MAC conditioning regimens. Overall survival (OS) was defined as the time from the date of AML diagnosis to the date of death due to any cause. Relapse free survival (RFS) was calculated from the date of achieving complete response (CR) or CR with incomplete hematologic recovery (CRi) until the date of relapse or death from any cause. CR and CRi were defined according to the current 2017 ELN guidelines2. ROC curve analysis was performed to determine the optimal cutoff value for MSC-l proportion based on its sensitivity and specificity, trying to boost its specificity to confidently identify patients with worse outcome. Kaplan–Meier and log-ranks test were used to compare OS and RFS between groups. Intensively-treated patients were analyzed globally and in a stratified analysis by the ELN 2017 genetic risk classification2.In addition, exploratory ROC curve for OS prediction were performed to assess the prognostic value of MSC-l quantification at diagnosis and after induction therapy, in order to compare these time points with the end-of-treatment assessment.
Multivariate Cox regression analysis was used to predict OS and RFS, with MSC-l quantification (categorized as explained above), age (categorized in < 60 years or ≥ 60 years), allo-HSCT (with RIC and MACconditionings codified in different variables) and the ELN 2017 genetic risk model as covariates. Statistical analyses were perfomed using SPSS 19.0 (IBM, Arkmon, NY). The confidence interval was set at 95% and the P-values were bilateral, considered significant if ≤ 0.05.
Data availability
The datasets used and/or analysed during the current study available from the corresponding author on reasonable request.
References
Shimony, S., Stahl, M. & Stone, R. M. Acute myeloid leukemia: 2023 update on diagnosis, risk-stratification, and management. Am. J. Hematol. 98, 502–526 (2023).
Döhner, H. et al. Diagnosis and management of AML in adults: 2017 ELN recommendations from an international expert panel. Blood 129, 424–447 (2017).
Prada-Arismendy, J., Arroyave, J. C. & Röthlisberger, S. Molecular biomarkers in acute myeloid leukemia. Blood Rev. 31, 63–76 (2017).
Pittenger, M. F. et al. Mesenchymal stem cell perspective: Cell biology to clinical progress. npj Regen. Med. 4, 1–15 (2019).
Jovic, D. et al. A brief overview of global trends in MSC-based cell therapy. Stem Cell Rev. Rep. 18, 1525–1545 (2022).
Shafat, M. S., Gnaneswaran, B., Bowles, K. M. & Rushworth, S. A. The bone marrow microenvironment—Home of the leukemic blasts. Blood Rev. 31, 277–286 (2017).
Menter, T. & Tzankov, A. Tumor microenvironment in acute myeloid leukemia: Adjusting niches. Front. Immunol. 13, 811144 (2022).
Pimenta, D. B. et al. The bone marrow microenvironment mechanisms in acute myeloid leukemia. Front. Cell Dev. Biol. 19(9), 764698 (2021).
Tan, L., Liu, X., Dou, H. & Hou, Y. Characteristics and regulation of mesenchymal stem cell plasticity by the microenvironment—Specific factors involved in the regulation of MSC plasticity. Genes Dis 9, 296–309 (2020).
Contribution to myeloma bone disease and therapeutics. Garcia-Gomez, A., Sanchez-Guijo, F., Del Cañizo, M. C., San Miguel, J. F. & Garayoa, M. Multiple myeloma mesenchymal stromal cells. World J Stem Cells 6, 322–343 (2014).
Chandia, M. et al. Involvement of primary mesenchymal precursors and hematopoietic bone marrow cells from chronic myeloid leukemia patients by BCR-ABL1 fusion gene. Am. J. Hematol. 89, 288–294 (2014).
Lopez-Villar, O. et al. Both expanded and uncultured mesenchymal stem cells from MDS patients are genomically abnormal, showing a specific genetic profile for the 5q-syndrome. Leukemia 23, 664–672 (2009).
Lee, M. W. et al. Mesenchymal stem cells in suppression or progression of hematologic malignancy: Current status and challenges. Leukemia 33, 597–611 (2019).
Galland, S. & Stamenkovic, I. Mesenchymal stromal cells in cancer: a review of their immunomodulatory functions and dual effects on tumor progression. J. Pathol. 250, 555–572 (2020).
Dominici, M. et al. Minimal criteria for defining multipotent mesenchymal stromal cells. The international society for cellular therapy position statement. Cytotherapy 8, 315–317 (2006).
Rahman, M. M. et al. CD13 promotes mesenchymal stem cell-mediated regeneration of ischemic muscle. Front. Physiol. 9(4), 402 (2014).
Atance, M. et al. Flow cytometry analysis of mesenchymal stem cells: a predictive biomarker for leukemia transformation in myelodysplastic syndrome. EJHaem 6, e70059 (2025).
Poon, C. C. et al. Mesenchymal stem cells and fibroblasts contribute to microvascular proliferation in glioblastoma and are correlated with immunosuppression and poor outcome. Cancer Immunol. Res. 13, 804–820 (2025).
Castaño-Bonilla, T. et al. No evidence that CD33 rs12459419 polymorphism predicts gemtuzumab ozogamicin response in consolidation treatment of acute myeloid leukemia patients: Experience of the PETHEMA group. Dis. Markers 2022, 3132941 (2022).
Bandyopadhyay, S. et al. Mapping the cellular biogeography of human bone marrow niches using single-cell transcriptomics and proteomic imaging. Cell 187, 3120-3140.e29 (2024).
Muñiz, C. et al. Ex vivo identification and characterization of a population of CD13high CD105+ CD45—Mesenchymal stem cells in human bone marrow. Stem Cell Res. Ther. 6, 169 (2015).
Acknowledgements
T.C. is a PhD candidate at the Universidad Autónoma de Madrid (UAM), and this work is submitted in partial fulfillment of the requirements for the doctoral degree. The authors gratefully acknowledge the technical assistance of Raquel Gonzalo and Susana Castañón in performing the experiments with mesenchymal stem cells using multiparametric flow cytometry . We also extend our sincere gratitude to the research team at the Hospital Universitario Fundación Jiménez Díaz for their contributions to the expansion, culture, and differentiation of MSCs into various cell subtypes.
Funding
This research received no external funding.
Author information
Authors and Affiliations
Contributions
Formal analysis : Tamara Castaño Bonilla, Raquel Mata, Carlos Blas, Cristina Serrano, Juan Manuel Alonso Domínguez, Juana Serrano, Gonzalo Castellanos, Raquel Capellán, Rocío Salgado, Laura Pardo, Laura Solán, Alvaro V. Arriero, Belén Rosado, Daniel Laínez, María Yuste, Pilar Beltran, Eva Oliva, Pilar Llamas, Rocío Olivera and Mireia Atance. Investigation : Tamara CastañoBonilla. Methodology: Tamara Castaño Bonilla, Raquel Mata, Carlos Blas, Cristina Serrano, Juan Manuel Alonso Domínguez, Juana Serrano, Gonzalo Castellanos, Raquel Capellán, Rocío Salgado, Laura Pardo, Laura Solán, Alvaro V. Arriero, Belén Rosado, Daniel Laínez, María Yuste, Pilar Beltran, Eva Oliva, Pilar Llamas, Rocío Olivera, Ignacio Mahillo and Mireia Atance. Supervision : Juana Serrano, Daniel Lainez, Raquel Mata, Cristina Serrano, Mireia Atance, Alberto Lázaro, Pilar Llamas and Juan Manuel AlonsoDomínguez. Visualisation : Tamara Castaño Bonilla, Juan Manuel Alonso Domínguez and Daniel Láinez González. Data curation : Raquel Mata, Carlos Blas, Cristina Serrano, Juan Manuel Alonso Domínguez, Juana Serrano, Gonzalo Castellanos, Raquel Capellán, Rocío Salgado, Laura Pardo, Laura Solán, Alvaro V. Arriero, Belén Rosado, Daniel Laínez, María Yuste, Pilar Beltran, Eva Oliva, Pilar Llamas, Rocío Olivera and Mireia Atance. Writing—original draft : Tamara Castaño. Writing—review and editing : Raquel Mata, Carlos Blas, Cristina Serrano, Juan Manuel Alonso Domínguez, Juana Serrano, Gonzalo Castellanos, Raquel Capellán, Rocío Salgado, Laura Pardo, Laura Solán, Alvaro V. Arriero, Belén Rosado, Daniel Laínez, María Yuste, Pilar Beltran, Ignacio Mahillo, Eva Oliva, Pilar Llamas, Rocío Olivera and Mireia Atance.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
All participants provided written informed consent. The study protocol was approved by the Clinical Research Ethics Committee of the Hospital Universitario Fundación Jiménez Díaz (TFG017-19_FJD) and was conducted in accordance with the Declaration of Helsinki.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Castaño-Bonilla, T., Láinez-González, D., Serrano, J. et al. Mesenchymal stem cells-like as a prognostic biomarker in patients diagnosed with acute myeloid leukemia. Sci Rep 15, 42680 (2025). https://doi.org/10.1038/s41598-025-26852-x
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-26852-x