Abstract
Low back pain is a leading cause of disability worldwide. Lumbar disc herniation (LDH), a prevalent etiology of low back pain, has various treatment options. This study investigated the impact of health beliefs on decision conflict regarding treatment choices in patients with LDH. A cross-sectional survey was administered to 737 patients with LDH. Three key constructs were assessed using validated instruments: health beliefs (Health Belief Scale), decision conflict (Decision Conflict scale), and treatment expectations (Treatment Expectation Questionnaire). The goodness-of-fit of the hypothesized theoretical framework was evaluated through structural equation modeling. Subsequently, descriptive statistics and Pearson correlation analyses were conducted to examine inter-variable relationships. Finally, the mediation effect of treatment expectations was tested using bias-corrected bootstrap procedures. Health beliefs demonstrated a significant negative association with decision conflict (r = − 0.660, p < 0.001), indicating that stronger health beliefs correlated with reduced decision-making difficulties. Similarly, treatment expectations exhibited a moderate inverse relationship with decision conflict (r = − 0.322, p < 0.001). Mediation analysis identified that treatment expectations were associated with a partial mediating pattern in the relationship between health beliefs and decision conflict (B = − 0.013, SE = 0.005, 95% CI: −0.024 to − 0.006), reflecting an observed correlational pathway that accounted for 19.7% of the total effect of health beliefs on decision conflict. This study found that health beliefs and treatment expectations influence the treatment decisions of patients with lumbar disc herniation (LDH) and reduce decision conflict.
Similar content being viewed by others
Introduction
Lumbar disc herniation (LDH) refers to the rupture of the annulus fibrosus of the intervertebral disc, leading to protrusion of the nucleus pulposus, compression of spinal nerves and cauda equina, and consequent inflammatory reactions, resulting in clinical symptoms such as pain and neurological dysfunction1. Low back pain is the leading cause of disability worldwide, and LDH is one of its most common contributors2, with a global prevalence of 7.62%3. In China, over 300 million individuals have lumbar spine disorders, and approximately 15.2% have been diagnosed with LDH. The peak incidence occurs between the ages of 30 and 50 years, and the prevalence is on the increase due to changing lifestyles and work patterns. The associated pain and functional impairment severely compromise patients’ quality of life4.
Current first-line treatments for LDH include conservative management and surgical interventions5,6. Studies report that symptoms in most patients improve with 6–12 weeks of conservative management7,8. Conservative approaches encompass bed rest, pharmacotherapy, exercise therapy, epidural injections, lumbar traction9,10,11. Surgical treatment is recommended for patients with severe pain that is unresponsive to conservative treatment, signs of cauda equina syndrome, or progressive motor weakness (Medical Research Council scale ≤ 3/5)12,13,14,15. Treatment selection—whether conservative or surgical—is influenced by multiple factors. While conservative management is safer and more suitable for mild or acute cases, its prolonged duration may be a disadvantage to patients with severe pain or disability. On the other hand, surgical intervention, though effective, raises safety concerns for some individuals16. In this context, informed treatment decision-making is critical. However, decision conflict —a psychological state of uncertainty when weighing risks, benefits, and personal values—may hinder optimal choices17,18,19,20.
The Health Belief Model is a core theoretical framework for understanding health behaviors. It posits that an individual’s health-related decisions and behavioral choices are collectively shaped by their perceptions of health threats (including perceptions of susceptibility and severity), as well as their perceptions of treatment benefits and barriers21,22. A study by Alshagrawi et al.23, which focused on COVID-19 vaccination decisions, revealed that perceptions of the severity of the virus and recognition of the protective efficacy of vaccines could significantly and positively predict individuals’ vaccination intentions and behaviors. In contrast, concerns about vaccine side effects reduced the certainty of vaccination decisions. This finding indicates that when individuals have a clearer understanding of disease threats and a more positive evaluation of treatment benefits, their goals regarding treatment decisions become more definite, and they are less likely to fall into the conflict of deciding “whether treatment is needed.” Furthermore, Khalilet al.24 validated this perspective in a study on prostate cancer prevention decisions: after health belief-based educational interventions significantly improved participants’ perceptions of cancer susceptibility and their beliefs in the benefits of screening, they not only showed a greater tendency to proactively choose screening behaviors but also exhibited a significant reduction in hesitation during decision-making processes, such as deciding “whether to undergo screening” and “when to initiate screening,” reflecting the alleviation of decision conflict. Additionally, a study by Taghikhah et al.25 found that patients with stronger health beliefs(HBs) made faster decisions on “whether to seek medical examination” after experiencing suspected symptoms and showed less preoccupation with secondary information such as “medical costs” and “accuracy of examinations” during the decision-making process. Conversely, patients with insufficient HBs ultimately had long-term decision delay. Based on the above evidence, we hypothesize that HBs may be negatively associated with treatment decision conflict (TDC) (Hypothesis 1).
Treatment expectations (TEX)—patients’ anticipated outcomes regarding cure likelihood, efficacy, and quality of life—also play a pivotal role in decision-making. Expectations significantly shape treatment preferences, adherence, and psychological states. A study reported that in patients with chronic disease, positive expectations correlate with reduced symptoms and improved quality of life26 Furthermore, a study by Smith27 showed that positive preoperative expectations in patients who underwent lumbar spine surgery were associated with lower post-surgical decision regret, directly supporting the critical role of expectation valence. Conversely, unmet expectations may trigger disappointment, depression, or decision-making dilemmas28. Studies propose that treatment expectations may act as a potential bridge in the correlational relationship between HBs and TDC (Fig. 1). Previous studies showed that patients often report selecting therapies that align with their perceived health gains shaped by belief-driven expectations29. This mediating role is further supported by multiple studies: Zhang found that patients with LDH with realistic positive expectations for conservative treatment had lower TDC when choosing between surgery and non-surgery30, while French reported in a systematic review of chronic low back pain that positive physical therapy expectations correlated with higher adherence and lower decision uncertainty31. These findings suggest that expectations may exhibit a mediating pattern in this correlational relationship (Hypothesis 2).
Theoretical framework.
Although previous studies explored factors influencing TDC, the interplay between HBs, TEX, and TDC in LDH remains underexamined. This study aims to clarify the impact of HBs on TDC in patients with LDH, with TEX as a mediator. The findings may provide valuable insights and evidence to support informed decision-making for this population.
Methods
Study participants
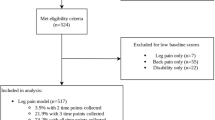
This study recruited participants via convenience sampling for a cross-sectional questionnaire survey. The inclusion criteria were as follows: (1) diagnosis of LDH confirmed by a combination of clinical examination and appropriate imaging (lumbar MRI or CT scans)—specifically, patients must present with clinical symptoms (e.g., low back pain with lower limb radiculopathy, sensory loss, muscle weakness, or hyporeflexia) that correspond to the level of disc herniation identified on imaging; (2) age ≥ 18 years; and (3) voluntary participation. The exclusion criteria included individuals with communication barriers. The survey was anonymous, and all participants provided informed consent prior to completing the questionnaires. A total of 737 questionnaires were collected, with 30 questionnaires excluded as invalid (18 due to incomplete key scale items and 12 due to logical contradictions in responses). Finally, 707 valid responses were obtained (validity rate: 95.93%), and for individual missing scale items (missing rate < 1%), mean imputation by subscale was used to ensure data integrity.
Data collection
Demographic characteristics
Demographic data were collected using a structured questionnaire that covered eight parameters: (a) gender, (b) marital status, (c) age, (d) education level, (e) health insurance type, (f) employment status, (g) annual household income per capita, and (h) residential area.
Measurement of treatment decision conflict
The Decision Conflict Scale (DCS), developed by O’Connor et al.32 and cross-culturally adapted into Chinese by Li33, was used to assess treatment decision conflict. This 16-item scale comprises five subscales: Informed (3 items), Values Clarity (3 items), Support (3 items), Uncertainty (3 items), and Effective Decision-Making (4 items). Responses were rated on a 5-point Likert scale (0 = strongly agree to 4 = strongly disagree). The total scores are calculated by averaging item scores and multiplying them by 25 to yield a 0–100 scale, with higher scores indicating greater decision conflict. The Chinese version demonstrated excellent internal consistency (Cronbach’s α = 0.897).
Measurement of health beliefs
HBs were measured using the revised Chinese version of the Health Belief Scale (HBS). The original scale, translated by Yuan34, is a widely recognized tool for assessing HBs. Ji et al.35 conducted cross-cultural adaptation and validation, reporting strong reliability (test-retest reliability = 0.889, split-half reliability = 0.936) and internal consistency (Cronbach’s α = 0.967). The 48-item scale includes five subscales: Personal HBs, Perceived Ability to Implement, Perceived Control, Perceived Resource Utilization, and Perceived Threats. Items are rated on a 5-point Likert scale (1 = very weak to 5 = very strong), with higher total scores reflecting stronger HBs.
Measurement of treatment expectations
The Treatment Expectation Questionnaire (TEX-Q), developed by Shedden-Mora et al.36,37 at the University Medical Center Hamburg-Eppendorf (UKE), Germany, and adapted into Chinese by Yang38, was employed. This 15-item tool assesses six dimensions: Treatment Benefit, Positive Impact, Adverse Events, Negative Impact, Treatment Process, and Behavioral Control. Responses are scored on an 11-point Likert scale (0–10). We used the overall mean score of the TEX-Q after reversing the harm expectation subscales (items 7–11), with higher values indicating more positive overall treatment expectations. The Chinese version exhibited excellent reliability (Cronbach’s α = 0.903 overall; 0.842–0.924 for subscales; split-half reliability = 0.958).
Data analysis
Data analysis for this study was conducted using R software (version 4.3.3; R Core Team, 2024) on Windows 11 × 64 (build 26100). Descriptive statistics were used to summarize the key characteristics of patients with LDH. Continuous variables were presented as mean ± standard deviation (M ± SD) and categorical variables as frequencies and percentages. Independent sample t-tests or one-way ANOVA were used to examine the impact of different demographic characteristics on TDC. According to Hair et al.39, the correlation coefficient between individual items and the total scale score needs to be at least 0.5 for scale validity and appropriateness. Mediation analysis was conducted using the mediation package to examine the mediating effects40.
Ethics
This study was approved by the hospital ethics committee (approval number: 2025SZSYLCYJ0404) and complied with the ethical standards of the declaration of Helsinki. Written informed consent was obtained from each patient included in this study prior to participation.
Results
Participant characteristics
The sample comprised 707 consecutively recruited patients with LDH, of whom 63.083% were male and 36.917% were female. Regarding marital status, 68.741% were married while 31.259% were unmarried. Furthermore, regarding the educational background of the participants, 22.631% held a bachelor’s degree or higher, 11.598% had an associate degree, 36.21% completed high school or vocational secondary education, 19.095% had a junior high school education, and 10.467% had an elementary school education or below.
In terms of employment status, 53.890% were employed, 30.127% were retired, and 15.983% were unemployed. Regarding insurance coverage, 54.173% had BMI insurance, 28.854% had NCMS insurance, and 16.973% had URBMI insurance. Residential distribution showed that 59.689% lived in urban areas, while 40.311% resided in non-urban areas.
The time since the first onset of symptoms was distributed as follows: 28.713% within 3 months, 21.358% between 3 and 6 months, 28.854% between 6 and 12 months, and 21.075% over 1 year. Regarding the first medical consultation, 37.907% visited outpatient departments of tertiary hospitals, 34.795% chose to visit the outpatient departments of secondary or community hospitals, 13.861% were hospitalized in secondary hospitals, while 13.437% were hospitalized in tertiary hospitals.
Among all participants, 84.583% had previously sought medical care for lumbar disc herniation-related issues, while 15.417% had not. Regarding the annual income distribution of the participants (Table 1), 21.782% earned over ¥150,000 (approximately over $20,985; upper-class), 20.226% had an annual income between ¥80,000 and ¥150,000 ($11,216–$20,985; solid middle-class), 29.986% earned between ¥30,000 and ¥80,000 ($4,197–$11,216; categorized lower-middle-class), and 28.006% had an annual income of less than ¥30,000 (approximately less than $4,197; low-income).
Level of treatment decision conflict, health beliefs, and treatment expectations, and univariate analysis of treatment decision conflict
The scores of DCS, HBS, and TEX-Q of the recruited patients with LDH were 25.748 ± 14.241, 168.356 ± 33.543, and 6.797 ± 0.949, respectively (Table 2). The univariate analysis for TDC revealed that all general categorical variables included in this study showed significant between-group differences (p < 0.05), except for whether the participants had previously sought medical attention for LDH (i.e., consulted a doctor). Specifically, these significant variables included gender, marital status, education level, insurance type, employment status, annual income, residential area, time since symptom onset, and the hospital type for the first medical consultation. All variables demonstrating significant between-group differences were included as covariates in subsequent analyses (Table 3).
Correlations of treatment decision conflict, health beliefs, and treatment expectations
Correlation analysis revealed significant associations among the TDC, HBs, and TEX. HBs (M = 168.356, SD = 33.543) showed a negative correlation with TDCS (r = − 0.660, p < 0.001) and a positive correlation with TEX (r = 0.202, p < 0.001). TEX (M = 101.960, SD = 14.24) were negatively correlated with TDC (r = − 0.322, p < 0.001).
Additionally, age, symptom, operative treatment, having seen a doctor, the form of the first visit and the level of hospital demonstrated significant correlations with either treatment expectations or DCS. health belief were negatively correlated with TDC but positively correlated with treatment expectations. Notably, variables significantly associated with TDC and TEX were also included as covariates in subsequent analyses to control for potential confounding effects (Table 4).
In this study, common method bias (CMB) was not a significant concern, as the first common factor explained only 26.50% of the variance, which is below the critical threshold of 40% set by Harman’s single-factor test, indicating no substantial CMB.
Mediating role of treatment expectations on the relationships between health beliefs and treatment decision conflict
Regression analyses sequentially examined the correlational relationships among HBs, TEX, and TDC. The results demonstrated the following: (1) HBs were significantly and negatively associated with TDC (β = −0.555, p < 0.001), accounting for 50.1% of the variance in DCS; (2) 2) HBs were positively associated with TEX (β = 0.182, p < 0.001), explaining 22.5% of the variance in TEX; (3) Both HBs and TEX negatively predicted TDC with HBs showing a stronger effect (β = −0.595, p < 0.001) compared to TEX (β = −0.163, p < 0.001). Overall, they explained 52.1% of the variance in DCS. All models controlled for covariates in the analyses (Table 5).
The mediation analysis revealed a statistically significant indirect effect of HBs on TDC through TEX (β = −0.013, S.E. = 0.005, 95% CI [− 0.024, − 0.006]). Simultaneously, the model demonstrated that the direct effect of HBs on TDC remained significant after controlling for TEX’s influence on TDC (β = −0.223, S.E.= 0.022, 95% CI [− 0.266, − 0.179]). These findings indicate that treatment expectations exhibit a partial mediating pattern in the correlational relationship between HBs and TDC, based on cross-sectional data. Although mediation was statistically significant, the small effect suggests other unmeasured factors may contribute to TDC (Table 6).
Discussion
This study analyzed 707 patients with LDH to explore the relationship between HBs, TEX, and TDC to assess the interactions among these variables and their impact on patients’ decision-making processes. Consistent with the findings of previous correlational studies, this study’s findings demonstrated that HBs are significantly negatively associated with TDC in patients with LDH21,22. HBs were found to be a significant negative predictor of TDC (β = −0.555, p < 0.001), accounting for 50.1% of the variance in TDC. These findings align with those of previous research21, indicating that stronger HBs are associated with lower feelings of conflict when facing medical decisions. HBs correlate with reduced perceived uncertainty, which may be attributed to patients reporting greater confidence in treatment options, in turn correlating with lower TDC22; however, temporal ordering cannot be established. This result underscores that strengthening patients’ HBs could be an effective strategy to reduce TDC in clinical practice. Additionally, this study found that patients’ perceptions of disease severity, treatment benefits, and treatment barriers significantly influenced their treatment choices. For example, patients who perceived their disease as severe and treatment benefits as significant were more likely to opt for aggressive treatment, whereas those who perceived more treatment barriers tended to choose conservative treatment or delay treatment. A study by Herrmann et al.41 also showed that disease conditions can influence patients’ treatment decisions.
Higher TEX were significantly associated with lower decision conflict (β = -0.163, p < 0.001),aligning with prior studies showing that higher expectations correlate with reduced decision conflict in chronic disease management25,26. This result further supports the importance of treatment expectations in the decision-making process, suggesting that clinicians should fully consider patients’ expectations when formulating treatment plans to reduce TDC; this is consistent with the findings of Oswald26. Treatment expectations influence treatment outcomes by affecting patients’ subjective feelings and behavioral responses. For instance, positive expectations can enhance treatment effects, producing a placebo effect, while negative expectations may lead to a nocebo effect that may hinder treatment efficacy28. Expectations not only influence short-term treatment outcomes but may also have long-term effects on patients’ recovery and quality of life. Research indicates that positive expectations can promote patient recovery and improve treatment satisfaction and adherence27. Therefore, treatment expectations play a significant role in medical decision-making dilemmas by influencing patients’ psychological states, treatment behaviors, and clinicians decision-making processes. Understanding this mechanism can help optimize treatment plans, improve patient satisfaction and treatment outcomes, and reduce ethical dilemmas and complexities in medical decision-making.
HBs exhibited a significant indirect associational pattern with TDC through TEX (β = −0.013, S.E. = 0.005, 95% CI [− 0.024, − 0.006]). Additionally, the model showed that after controlling for the effect of TEX on TDC, the direct effect of HBs on TDC remained significant (β = −0.223, S.E. = 0.022, 95% CI [− 0.266, − 0.179]). These results indicate that TEX show a partial mediating pattern in the correlational relationship between HBs and TDC. However, this pattern reflects observed associations in cross-sectional data and does not imply causation. HBs not only directly influence treatment decisions but also indirectly affect decisions by shaping patients’ TEX. Additionally, patients’ expectations regarding treatment efficacy, process, and behavioral control serve as a bridge between HBs and treatment decisions. HBs were significantly and positively associated with treatment expectations (β = 0.182, p < 0.001), accounting for 22.5% of the variance in treatment expectations in this cross-sectional sample. This suggests that stronger HBs are associated with higher expectations for treatment outcomes. HBs may enhance positive attitudes toward treatment, thereby raising expectations for treatment efficacy. This implies that clinicians should pay attention to patients’ HBs when formulating treatment plans to improve their expectations, potentially enhancing treatment adherence and outcomes.
This study highlights the importance of considering patients’ HBs and TEX in clinical practice. Healthcare professionals should actively assess patients’ HBs, understand their perceptions of disease and treatment, and use effective communication and education to help patients develop positive TEX, thereby facilitating decisions that promote recovery. Strengthening HBs fosters more rational treatment decisions, while positive TEX can influence patients’ HBs and decisions. A comprehensive understanding of the interactions among HBs, treatment decisions, and expectations is crucial for developing personalized treatment plans and interventions in clinical practice.
Study limitations
A key limitation of this study is the use of cross-sectional data to examine mediation, which precludes establishing temporal ordering of variables or definitive causal relationships. Moreover, mediation analyses in cross-sectional designs identifies correlational patterns rather than causal pathways; hence, the observed mediating role of TEX should be interpreted as an associational trend rather than a directional effect. Future longitudinal studies are needed to verify the temporal sequence of HBs, TEX, and TDC, which would strengthen inferences about potential causal relationships.
Furthermore, the study sample was primarily drawn from a specific region, limiting generalizability to other populations. Future research could expand the sample scope to improve generalizability. Additionally, the influence of HBs and TEX may vary across cultural contexts. Future studies should endeavor to stratify patients into cultural geographic subgroups and incorporate longitudinal designs to address temporal limitations. Longitudinal studies could further investigate the causal relationships among HBs, TEX, and TDC, providing new perspectives for medical decision-making support. Future studies should endeavor to stratify patients into cultural geographic subgroups.
Conclusion
By analyzing data from 707 participants, this study revealed the relationships between HBs, TEX, and TDC. The results showed that HBs were significantly negatively associated with TDC and positively associated with TEX in this cross-sectional sample. Treatment expectations partially mediated the relationship between HBs and TDC. These findings highlight that enhancing patients’ HBs and calibrating realistic TEX may be associated with reduced TDC in clinical practice, based on observed correlations; however, causal claims are not supported by cross-sectional data. Future research could explore other potential mediating variables and the stability of these relationships across different cultural contexts.
Clinicians should strengthen patients’ HBs through education and communication to reduce conflicts in medical decision-making. When formulating treatment plans, clinicians should consider patients’ expectations and use proactive communication and information provision to improve their expectations of treatment outcomes. Given patients’ diverse socioeconomic backgrounds and health conditions, individualized treatment plans should be developed to meet specific needs and reduce TDC. This study provides new insights into the relationships among HBs, TEX, and TDC and offers valuable guidance for clinical practice.
Data availability
The data that support the findings of this study are not publicly available due to privacy or ethical restrictions but are available from the corresponding author upon reasonable request.
References
Kreiner, D. S., Hwang, S. W. & Easa, J. E. North American Spine Society. An evidence-based clinical guideline for the diagnosis and treatment of lumbar disc herniation with radiculopathy. Spine J. 14, 180–191. https://doi.org/10.1016/j.spinee.2013.08.003 (2013).
Vialle, L. R., Vialle, E. N., Suárez Henao, J. E. & Giraldo, G. Lumbar disc herniation. Revista Brasileira De Ortop. (English Edition). 45, 17–22. https://doi.org/10.1016/s2255-4971(15)30211-1 (2010).
Knezevic, N. N., Candido, K. D. & Vlaeyen, J. W. S. Low back pain. Lancet 398, 78–92 (2021).
Peng, J., Liu, Y., Liu, J., Li, J. & Zeng, X. Burden of disease in the chinese population from. (2005).
Chinese Orthopaedic Association of Orthopaedic Rehabilitation Group. Clinical practice guideline for diagnosis and treatment of lumbar disc herniation. Chin. J. Orthop. 40, 477–487. https://doi.org/10.3760/cma.j.cn121113-20200402-00213 (2020).
Støttrup, C., Andresen, A., Ernst, C. & Andersen, M. Ø. Surgical treatment of lumbar disc herniation. Ugeskr Laeger (2018).
Deyo, R. A. & Mirza, S. K. Herniated lumbar intervertebral disk. N Engl. J. Med. 374, 1763–1772. https://doi.org/10.1056/nejmcp1512658 (2016).
Deyo, R. A., Diehl, A. K. & Rosenthal, M. How many days of bed rest for acute low back pain? N Engl. J. Med. 315, 1064–1070. https://doi.org/10.1056/nejm198610233151705 (1986).
Weiner, B. Treatment of lumbar disc herniation: evidence-based practice. Int. J. Gen. Med. 3, 209–214. https://doi.org/10.2147/ijgm.s12270 (2010).
Buy, X. & Gangi, A. Percutaneous treatment of intervertebral disc herniation. Semin Intervent Rad. 27, 148–159. https://doi.org/10.1055/s-0030-1253513 (2010).
Sun, K. et al. A systematic review and meta-analysis for Chinese herbal medicine duhuo jisheng decoction in treatment of lumbar disc herniation. Medicine 99, e19310. https://doi.org/10.1097/md.0000000000019310 (2020).
Haro, H. et al. Japanese orthopaedic association (joa) clinical practice guidelines on the management of lumbar disc herniation, third edition - secondary publication. J. Orthop. Sci. 27, 31–78. https://doi.org/10.1016/j.jos.2021.07.028 (2021).
Haiqing, M., Feifei, Z. & Siyi, C. Expert consensus on the implementation process of percutaneous lumbar endoscopic surgery for accelerated rehabilitation surgery. Chin. J. Bone Joint Surg. 12, 641–651 (2019).
Kreiner, D. S. et al. An evidence-based clinical guideline for the diagnosis and treatment of lumbar disc herniation with radiculopathy. Spine J. 14, 180–191. https://doi.org/10.1016/j.spinee.2013.08.003 (2014).
Glocker, F. X. Deutsche gesellschaft für neurologie (eds.). Leitlinien für diagnostik und therapie in der neurologie—lumbale radikulopathie. (2018).
Watters, W. C. & McGirt, M. J. An evidence-based review of the literature on the consequences of Conservative versus aggressive discectomy for the treatment of primary disc herniation with radiculopathy. Spine J. 9, 240–257. https://doi.org/10.1016/j.spinee.2008.08.005 (2008).
Wosny, M. et al. Factors guiding clinical decision-making in genitourinary oncology. Cancer Med. 13, 70304. https://doi.org/10.1002/cam4.70304 (2024).
Andkhoie, M., Meyer, D. & Szafron, M. Factors underlying treatment decision-making for localized prostate cancer in the u.s. And canada: a scoping review using principal component analysis. CUAJ 13 https://doi.org/10.5489/cuaj.5538 (2019).
Basile, F. W. et al. Uncertainty in tuberculosis clinical decision-making: an umbrella review with systematic methods and thematic analysis. PLOS Glob Public. Health. 4, e0003429. https://doi.org/10.1371/journal.pgph.0003429 (2024).
Zambri, F. et al. Health belief model efficacy in explaining and predicting intention or uptake influenza vaccination during pregnancy. Ann. Ist Super Sanita. 58, 285–292. https://doi.org/10.4415/ANN_22_04_09 (2022).
Pecanac, K. E., Brown, R. L. & Kremsreiter, H. B. Decisional conflict during major medical treatment decision-making: a survey study. J. Gen. Intern. Med. 36, 55–61. https://doi.org/10.1007/s11606-020-06125-1 (2020).
Rosenstock, I. M. Historical origins of the health belief model. Health Educ. Quart. 2, 328–335. https://doi.org/10.1177/109019817400200403 (1974).
Alshagrawi, S. S. Predicting covid-19 vaccine uptake: comparing the health belief model and theory of planned behavior. Hum. Vaccin Immunother. 20, 2361503. https://doi.org/10.1080/21645515.2024.2361503 (2024).
Khalil, M. I. et al. Effect of health belief model-based educational intervention on prostate cancer prevention; knowledge, practices, and intentions. BMC Cancer. 24, 289. https://doi.org/10.1186/s12885-024-12044-9 (2024).
Taghikhah, F. R., Jabbari, A., Desouza, K. C., Malik, A. & Khorshidi, H. A. Understanding delayed diabetes diagnosis: an agent-based model of health-seeking behavior. Med. Decis. Mak. 45, 399–425. https://doi.org/10.1177/0272989X251326908 (2025).
Oswald, L. B. et al. Patient expectations of benefit from systemic treatments for metastatic prostate cancer. Cancer Med. 9, 980–987. https://doi.org/10.1002/cam4.2783 (2019).
Smith, R. A. & Johnson, T. L. The impact of preoperative expectations on post-surgical decision regret in lumbar spine surgery. Spine 44, 867–873 (2019).
Yang, M. et al. Nocebo expectations rather than placebo expectations affect topical pain relief: a randomized clinical trial. Biomed. Pharmacother. 175, 116728. https://doi.org/10.1016/j.biopha.2024.116728 (2024).
Buergler, S., Sezer, D., Gaab, J. & Locher, C. The roles of expectation, comparator, administration route, and population in open-label placebo effects: a network meta-analysis. Sci. Rep. 13, 11827. https://doi.org/10.1038/s41598-023-39123-4 (2023).
Zhang, L. & Wang, Y. Treatment expectations and decisional conflict in lumbar disc herniation: a pilot study. J. Clin. Nurs. 31, 562–570 (2022).
French, D. P. & Sim, J. Treatment expectations and adherence to physical therapy in chronic low back pain: a systematic review. J. Orthop. Sports Phys. Ther. 50, 241–251 (2020).
O’Connor, A. M., Llewellyn-Thomas, H. & Flood, A. Decision conflict scale: development and evaluation of a tool to measure decisional uncertainty. Med. Decis. Mak. 19 (1), 25–30 (1999).
Li, Y. Research on the construction and application of a treatment decision-making aid plan for patients with early primary liver cancer. Dissertation. Shanghai: Second Military Medical University, (2017).
Wang, L. H. et al. Mediating effect of HBs between health knowledge and health behavior in patients with hypertension and stroke. Chin. J. Behav. Med. Brain Sci. 26, 847–851. https://doi.org/10.3760/cma.j.issn.1674-6554.2017.09.016 (2017).
Ji, S. & Hui, Y. Cross-cultural debugging and reliability and validity evaluation of health belief scale. China Med. Innov. 139–141. https://doi.org/10.3969/j.issn.1674-4985.2013.09.075 (2013).
Alberts, J. et al. Development of the generic, multidimensional treatment expectation questionnaire (tex-q) through systematic literature review, expert surveys and qualitative interviews. BMJ Open. 10, e036169. https://doi.org/10.1136/bmjopen-2019-036169 (2020).
Shedden-Mora, M. C. et al. The treatment expectation questionnaire (TEX-Q): validation of a generic multidimensional scale measuring patients’ treatment expectations. PLoS One. 18 (1), e0280472. https://doi.org/10.1371/journal.pone.0280472 (2023).
Yang, L. N. The sinicization of the treatment expectation questionnaire (tex-q) and its application in colorectal cancer patients. Dissertation. Nanchang: Nanchang University, (2023).
Hair, J. F., Anderson, R. E., Tatham, R. L. & Black, W. C. Multivariate Data Analysis 7th edn (Pearson Prentice Hall, 2010).
Tingley, D., Yamamoto, T., Hirose, K., Keele, L. & Imai, K. Mediation: r package for causal mediation analysis. J. Stat. Soft. 59, 1–38. https://doi.org/10.18637/jss.v059.i05 (2014).
Herrmann, A., Hall, A. & Proietto, A. Using the health belief model to explore why women decide for or against the removal of their ovaries to reduce their risk of developing cancer. BMC Women’s Health. 18, 184. https://doi.org/10.1186/s12905-018-0673-26 (2018).
Acknowledgements
The authors delivered their appreciations to all the personnel involved in the study and Patients with lumbar intervertebral disc protrusion participated in this study. Special thanks were given to Health Commission of Henan Province, to provide grant support for the Program.
Funding
This study received funds from the Key Research and Development Project of Henan Province (No. 241111313800) and National Key Clinical Specialty Construction Project (Yu Wei Medical Letter [2023] No.30).
Author information
Authors and Affiliations
Contributions
•Yuan Tian : Conceptualization, Methodology, Data curation, Formal analysis, Writing- Original draft preparation, Writing- Reviewing and Editing, Project administration•Shao-Hua Chen: Conceptualization, Writing- Original draft preparation, Writing- Reviewing and Editing, Supervision, Methodology•Gao-Ding Jia : Conceptualization, Data curation, Software, Formal analysis•Rui-Peng Song: Validation, Resources, Funding acquisition•Shi-Na Cheng: Investigation, Data curation•Bei-Bei Chen: Conceptualization, Investigation, Data curation•Jia-Ying Song: Investigation, Data curation•Jing-Yi Yang :Investigation, Datacuration.
Corresponding author
Ethics declarations
Ethical approval
Ethical approval was granted by Ethics Committee of The Third People’s Hospital of Henan Province (2025SZSYLCYJ0404)and complied with the ethical standards of the declaration of Helsinki. Written informed consent was obtained from all participants.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Tian, Y., Chen, SH., Song, RP. et al. The impact of health beliefs on treatment decision conflict through treatment expectations mediation in patients with lumbar disc herniation. Sci Rep 15, 42802 (2025). https://doi.org/10.1038/s41598-025-27025-6
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-27025-6