Abstract
YSCH-01, a recombinant L-IFN oncolytic adenovirus based anticancer drug with dual anti-tumor effects, has displayed significant antitumor properties in cancer treatment. However, its specific role in osteosarcoma and the underlying mechanisms remain under studied. Therefore, we analyzed clinical samples and performed experiments using osteosarcoma cell lines in both in vitro and in vivo settings. At the RNA and protein levels, the expression of L-IFN gene carried by YSCH-01 showed the potential antitumor properties. RNA-seq analysis of tumor samples treated with YSCH-01 provided insights into the altered gene expression profiles and signaling pathways, shedding light on the molecular basis of its antitumor effects. Those findings demonstrated that YSCH-01 displayed dose-dependent infectivity with different levels of efficacy and a significant inhibition of osteosarcoma cell proliferation. In both cell line and patient derived xenograft models, YSCH-01 exhibited potent therapeutic effects with the activated type I interferon signaling pathway in tumor tissues, particularly in terms of its distant effects. Furthermore, this study found out the key signal pathways through which YSCH-01 exerts its antitumor effects in osteosarcoma, which pinpointed potential therapeutic targets by identifying the type I interferon signaling pathway as the candidate molecular markers and their correlation with patient outcomes, positioning YSCH-01 as a promising candidate for osteosarcoma treatment.
Similar content being viewed by others
Introduction
Osteosarcoma (OS) is a primary malignant solid tumor characterized by the aggressive proliferation of mesenchymal cells1, primarily affecting children and adolescents. It constitutes about 20% of all primary bone cancers2, with survival rates remaining stagnant despite advancements in chemotherapy and neoadjuvant treatments over recent decades3,4. The complexity of its somatic genome results in diverse molecular aberrations, complicating the identification of universal therapeutic targets. Consequently, OS remains a challenging disease to manage5. The current standard treatments for OS include surgery, chemotherapy, and occasionally radiation therapy6,7,8,9. However, for patients with metastatic or recurrent disease, the prognosis remains particularly poor, with reported five-year survival rates typically ranging from 10% to 30%10,11,12.
One of the major challenges in OS research is the lack of targeted therapies specifically tailored to this disease13. The molecular mechanisms underlying the pathogenesis and progression of OS remain incompletely understood14. The heterogeneity of OS tumors at both the molecular and histological levels complicates treatment strategies and leads to variable responses to existing therapies. Additionally, the development of drug resistance and the potential for metastasis pose significant obstacles to the effective management of this disease15,16.
Oncolytic virotherapy, a form of cancer biotherapy, is considered an effective treatment option. Oncolytic adenoviruses have been extensively studied for clinical cancer treatment due to their potent antitumor effects and reduced toxicity to normal tissues17,18,19. However, systemic administration of oncolytic adenoviruses is limited by factors such as neutralizing antibodies, complement activation, antiviral immunity, and weak tumor tropism, making intra-tumoral administration the most effective method to date20,21. Researchers are exploring alternative delivery methods, including the use of cell carriers, which offer several advantages, such as promoting the escape of loaded viruses from host antiviral immunity and enhancing their effective targeting of distant tumor sites22. Commonly used cell carriers include lymphocyte-like cells (e.g., cytokine-induced killer cells, peripheral blood lymphocytes, dendritic cells), tumor cell-like cells (e.g., tumor-associated macrophages), and stem-like cells (e.g., mesenchymal stem cells, endothelial progenitor cells)23,24.
Oncolytic viruses (OVs), whether naturally occurring or genetically modified, selectively replicate within tumor cells, inducing cell lysis while sparing normal cells. These viruses exert antitumor effects through multiple mechanisms and offer several advantages, including high tumor-targeting efficiency, minimal side effects, broad applicability, and cost-effectiveness25,26. In a previous study, we investigated the efficacy of YSCH-01 in malignant glioblastoma, demonstrating good efficacy27. In another study, the YSCH-01 virus was loaded onto human dental pulp stem cells, demonstrating tumor tropism and a potent antitumor secretome derived from YSCH-01/ human dental pulp stem cells28.
At the current stage of the research stage, several oncolytic adenoviruses have shown therapeutic potential in solid tumors, including OS, with demonstrated oncolytic effects observed in animal models of both localized and metastatic OS. This study aims to investigate the oncolytic activity of YSCH-01 in OS and elucidate its potential mechanisms through in vitro experiments and in vivo models.
Results
Expression patterns of proteins governing YSCH-01 infection in OS cell lines and clinical tissues
We analyzed the expression of key target proteins in four human OS cell lines (143B, MNNG/HOS, MG-63, U-2 OS) and compared them to control human normal bone marrow stromal cells (hBMSC) as control. Western blot analysis was performed using antibodies against CXADR, Survivin, PD-1, RB1, and IFNAR. The results indicated that these proteins were expressed in OS cell lines but were absent in the control group, with expression levels varying among the different OS cell lines (Fig. 1A).
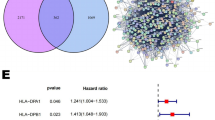
Expression patterns of proteins governing YSCH-01 infection in osteosarcoma cell lines and clinical tissues. (A) Immunoblot analysis of CXADR, IFNAR-1, Survivin, and RB-1 in human osteosarcoma cells compared to normal human bone marrow stromal cells (hBMSC). (B) Immunohistochemistry of CXADR, Survivin, IFNR, RB, PD-1, and PD-L1 in clinical osteosarcoma samples. (C) Heat map analysis of CXADR, Survivin, IFNR, RB, PD-1, and PD-L1 in 26 clinical samples of osteosarcoma. (D) Distribution statistics of patients based on protein expression levels. (E) Recurrence or metastasis after surgical methods and postoperative outcomes in 26 patients.
A total of 26 patients diagnosed with OS between 2022 and 2023 who underwent either limb amputations or tumor segment resection with artificial joint replacement at our hospital were included in this study. To ensure the scientific rigor of the results, we included patients with primary osteosarcoma confirmed by biopsy, all of whom had a pathological classification of conventional osteosarcoma. Tumor specimens from these patients were collected for immunohistochemical analysis of the aforementioned markers. Over half of the cases showed strong positivity for CXADR, Survivin, and PD-1, with staining in more than 80% of the cells. The overall positivity rates were 84.6% (22/26) for CXADR, 76.9% (20/26) for Survivin, and 88.5% (23/26) for PD-1. Although the IFNAR group had a low number of strongly positive cases (7.7%, 2/26), the overall positivity rate was still high at 81% (21/26 cases). In contrast, RB1 showed no strong positivity and a positivity rate of 23.1% (6/26), while PD-L1 exhibited no positivity (0%, Fig. 1B–D).
The analysis of 4 OS cell lines and 26 clinical samples revealed elevated CXADR, Survivin, PD-1, and IFNAR expression, while RB1 and PD-L1 were expressed at very low levels. Notably, CXADR serves as an adenovirus receptor, and the Survivin promoter in the oncolytic adenovirus YSCH-01 specifically targets cells with high Survivin expression. Additionally, YSCH-01 induces the overexpresses of interferon-like protein L-IFN, suggesting potential antitumor effects on OS.
We followed up with the 26 patients to document their surgical methods and postoperative recurrence or metastasis. Among these patients, 12 experienced local recurrence or distant metastasis. We analyzed the correlation between recurrence/metastasis and the positive expression levels of the tumor markers (Fig. 1E). The findings showed no significant correlation between the expression levels of these biomarkers and patient prognosis under traditional treatments.
Efficiency and oncolytic effects of YSCH-01 on OS cell lines in vitro
To explore the potential of oncolytic adenoviruses in targeting OS cells, we used the OncoMul-V2-EGFP virus to infect four OS cell lines (143B, MNNG/HOS, MG-63, U-2 OS) at different concentrations (1, 10, and 50 MOI). After 48 h, the cells were examined under a fluorescence microscope, and fluorescence-positive cells were quantified using flow cytometry (Fig. 2A and B). In 3D cultures, adenoviruses carrying EGFP successfully infect OS tissues after 14 days (Fig. 2C). Our findings showed that the oncolytic adenoviruses effectively infected OS cells, with significant infection rates observed at 1 MOI in U-2 OS, 10 MOI in 143B, MG-63, and MNNG/HOS cells. The infection rate was more than 90% at a dose of 10 MOI, indicating that oncolytic adenoviruses can infect OS cells in a dose-dependent manner, with varying infectivity levels among different cell lines.
Infection of osteosarcoma cells and tissues by OncoMul-V2-EGFP. (A) Fluorescence expression and analysis of the green area in osteosarcoma cells infected with OncoMul-V2-EGFP at multiplicity of infection (MOI) doses of 1, 10, and 50 after 48 h. (B) Flow cytometry analysis showing the proportion of fluorescent cells in osteosarcoma cells infected with OncoMul-V2-GEFP at various doses for 48 h. (C) Fluorescence expression in a 3D-cultured model of osteosarcoma tissue infected with OncoMul-V2-EGFP over time. ns means P > 0.05, * means P < 0.05, ** means P < 0.01, *** means P < 0.001, **** means P < 0.0001.
Further, we infected the four OS cell lines with the oncolytic adenovirus YSCH-01 and measured the overexpression of interferon-like protein L-IFN at both RNA and protein levels using qPCR and Western Blot analysis. After 24 h of infection with 1 and 10 MOI of YSCH-01, qPCR analysis showed significantly increased mRNA levels of L-IFN in U-2 OS, M-G63, and MNNG/HOS cells with the 10 MOI. There was also a trend of increased mRNA levels of L-IFN in 143B at 10 MOI, although this increase was not statistically significant (Fig. 3A). Conversely, the low-dose group (1 MOI) did not exhibit elevated mRNA levels. Following 48 h of infection with 10 MOI of YSCH-01, Western blot analysis demonstrated increased L-IFN protein expression across all four cell lines, which was absent in the Vehicle and OncoMul-V2 control groups (Fig. 3B and C). These in vitro experiments indicate that YSCH-01 infection at certain doses leads to the exogenous overexpression of L-IFN in OS cells. Based on these results, we hypothesize that YSCH-01 might be effective in OS treatment, prompting further pharmacodynamics studies of YSCH-01 both in vitro and in vivo.
L-IFN expression in osteosarcoma cells infected with YSCH-01. (A) qPCR analysis of L-IFN expression in U-2 OS, 143B, MG-63, and MNNG/HOS cells infected with YSCH-01 at doses of 1 MOI and 10 MOI for 24 h. (B) and (C) : Immunoblot analysis of L-IFN in U-2 OS, 143B, MG-63, and MNNG/HOS cells infected with 10 MOI of YSCH-01 or OncoMul-V2 for 48 h. ns means P > 0.05, * means P < 0.05, ** means P < 0.01, *** means P < 0.001, **** means P < 0.0001.
To evaluate the cytotoxic effect of YSCH-01 on OS cells, we infected U-2 OS, MG-63, 143B, and MNNG/HOS cells with YSCH-01 at various MOI (0, 1, 10, 50, 100, 300, 500, and 1000) and stained them with crystal violet after 4 days. The cytotoxic effects of YSCH-01 were also assessed using CCK-8 assay. The in vitro cytotoxic assay demonstrated a dose-dependent cytotoxic effect of YSCH-01 on OS cells (Fig. 4A), with varying IC50 values across different cell lines (Fig. 4B). This dose-response relationship indicates the potential to optimize treatment regimens to maximize therapeutic efficacy while minimizing off-target effects. The observed differential sensitivity of OS cells to YSCH-01 highlights the importance of personalized dosing strategies tailored to individual patient profiles, underscoring the importance of precision medicine in oncology.
Cytotoxic effects of YSCH-01 on osteosarcoma cells. (A) Crystal violet staining of U-2 OS, MG-63, 143B, and MNNG/HOS cells infected with YSCH-01 at doses of 0, 1, 10, 50, 100, 300, 500, and 1000 MOI for 4 days. (B) CCK-8 assay analysis of the cytotoxic effects of YSCH-01 on U-2 OS, MG-63, 143B, and MNNG/HOS cells.
YSCH-01-Infected cell supernatants stimulate PBMC inflammatory cytokine secretion
In an in vitro experiment, supernatants from YSCH-01-infected 143B tumor cells (48 h post-infection) were used to stimulate mouse PBMCs for 8 h. The culture supernatant of YSCH-01-infected osteosarcoma cells upregulated the expression of proinflammatory cytokines (IFN-γ, IL-12α, and TNF-α) in mouse PBMCs (see Supplementary Fig. S1 online). These findings suggest that factors such as L-IFN present in the tumor cell supernatant may contribute to immune cell activation.
Oncolytic effects of YSCH-01 in osteosarcoma CDX nude mouse model
In vitro experiments confirmed both the infectivity and cytotoxic effects of the oncolytic adenovirus YSCH-01 in OS cells. To further validate these findings, in vivo experiments were conducted to establish both the CDX and PDX models in nude mice. Subcutaneous CDX models were established using human U2-OS, 143B, and MNNG/HOS cells. YSCH-01 was administered once every 2 days for a total of five administrations (Fig. 5A). The results demonstrated a significant inhibitory effect of YSCH-01 on tumor growth at the administration site in all three OS cell lines, with tumor inhibition rates of 75.16%, 107.45%, and 65.00%, respectively. Additionally, YSCH-01 showed a significant inhibitory effect or a trend toward inhibiting the growth of tumors at non-administration sites (Fig. 5B–D).
Oncolytic effects of YSCH-01 in osteosarcoma cell line-derived xenograft (CDX) nude mouse model. (A) Experimental flowchart of the pharmacological study of YSCH-01 in an osteosarcoma CDX nude mouse model. (B-D) Growth curves of bilateral tumors and relative weight changes in U-2 OS (B), 143B (C), and MNNG/HOS (D) osteosarcoma CDX nude mouse models. ns means P > 0.05, * means P < 0.05, ** means P < 0.01, *** means P < 0.001, **** means P < 0.0001.
By comparison, the OncoMul-V2 control exhibited a significant antitumor effect at the administration site but had no effect on tumors at the non-administration site (Fig. 5B, C and D). No significant differences in the relative body weight were observed across all groups (Fig. 5B, C and D), indicating that the mice tolerated the YSCH-01 treatment well. These findings highlight the potent anti-tumor effects of YSCH-01 across different OS cell lines and its potential as a promising therapeutic agent for OS treatment.
Moreover, YSCH-01 demonstrated distant (abscopal) effects on U-2 OS and 143B xenograft tumors in nude mice, highlighting the need for further research to explore this phenomenon.
Oncolytic effects of YSCH-01 in osteosarcoma clinical PDX model
Similar results were observed in the PDX models, where tumor tissues from two OS patients were established in xenograft models in nude mice. The efficacy of YSCH-01 was evaluated by comparing tumor growth changes at both administration and non-administration sites, along with relative changes in body weight of nude mice (Fig. 6A). In both OS PDX models, YSCH-01 exhibited a highly significant anti-tumor effect at the administration site, with tumor inhibition rates of 155.22% and 170.94%, respectively. Moreover, YSCH-01 also demonstrated significant effects at non-administration sites, with tumor inhibition rates of 163.17% and 95.42%, respectively.
Oncolytic effects of YSCH-01 in osteosarcoma patient-derived xenograft (PDX) models. (A) Experimental flowchart of the pharmacological study of YSCH-01 in an osteosarcoma PDX model. (B-C) Growth curves of bilateral tumors, tumor suppression rates, and relative weight changes in the 0# (B) and 2# (C) osteosarcoma PDX nude mouse models. ns means P > 0.05, * means P < 0.05, ** means P < 0.01, *** means P < 0.001, **** means P < 0.0001.
While the OncoMul-V2 control group also showed tumor inhibitory effects or a trend towards inhibition at both administered and non-administered sites, its efficacy was notably lower than that of YSCH-01(Fig. 6B and C). These results indicate that YSCH-01 significantly inhibited tumor growth at administration sites in OS PDX models and exerted considerable anti-tumor effects at non-administration sites, highlighting the strong in vivo efficacy of YSCH-01 in treating OS.
Activation of the type I interferon signaling pathway in YSCH-01 infected CDX tissue
Based on the in vivo efficacy data shown in Figs. 5 and 6, we prioritized the subcutaneous tumor models (U-2 OS vs. 143B) exhibiting superior abscopal effects for mechanistic investigation. However, given that U-2 OS showed non-typical therapeutic responses in injected tumors compared to the backbone virus OncoMul-V2, it might not adequately reflect the underlying mechanisms. After comprehensive evaluation, we selected 143B cells for preliminary mechanistic studies.
RNA-seq data analysis was conducted on tumor tissue samples from YSCH-01-treated and control groups in the 2# PDX model and the 143B CDX model to investigate differences in gene expression patterns and signaling pathway activity. However, due to the potent tumor-killing effects of YSCH-01 in the 2# PDX model treatment group, the tumors were too small for effective RNA-seq analysis. In contrast, significant differences in gene expression patterns and signaling pathway activities were observed in the CDX model between the treatment and control groups (Fig. 7A).
Activation of the type I interferon signaling pathway in YSCH-01-infected CDX tissue. (A) RNA-seq data analysis of CDX tumor tissue samples using 143B cell line, comparing the YSCH-01 treatment group to control groups. receiving This analysis revealed 394 genes up-regulated and 644 genes down-regulated in the treatment group compared to the control group. (B) Gene Ontology analysis showing significant gene expression enrichment in the ‘ISG15-protein conjugation’ and ‘response to type I interferon’ pathways, which are closely related to type I interferon activation in the YSCH-01 treatment group compared to the control group. (C) qPCR analysis showing the relative expression levels of the selected genes of ‘ISG15-protein conjugation’ and ‘response to type I interferon’ pathway showed in panel B.
The distinct gene expression profiles in the YSCH-01 treatment group indicated extensive regulation of key molecular pathways associated with tumor initiation and progression. Gene Ontology enrichment analysis identified type I interferon-related genes as the most significantly differentially expressed, consistent with YSCH-01 being an oncolytic adenovirus carrying recombinant interferon-like protein gene (L-IFN).
To further validate these findings, we performed qPCR analysis on tumor tissues from the CDX model’s control and experimental groups, focusing on genes associated with type I interferon (Fig. 7B). The results showed significantly elevated expression levels of Interferon Stimulated Gene 15 (ISG-15), Bone Marrow Stromal Cell Antigen 2 (BST2), IFITM1 (Interferon Induced Transmembrane Protein 1), Interferon Induced Protein With Tetratricopeptide Repeats 3 (IFIT3), 2’-5’-Oligoadenylate Synthetase 1(OSA1), and MX Dynamin Like GTPase 2 (MX2) in the YSCH-01 treatment group compared to the control group, indicating activation of the type I interferon signaling pathway. These changes in signaling pathway activities highlighted that YSCH-01 disrupts oncogenic pathways and promotes robust anti-tumor responses. These findings provide a comprehensive molecular understanding of the impact of YSCH-01 treatment on tumor biology, elucidating its mechanisms of action and therapeutic potential in OS.
Discussion
This preclinical study evaluated the safety and efficacy of YSCH-01, an oncolytic adenovirus carrying L-IFN gene, in treating OS. Immunohistochemical analysis of tumor samples from 26 OS patients revealed that 84.6% of cases showed positivity for CXADR and 76.9% for Survivin, with more than half of the cases exhibiting strong expression of these markers. Given that CXADR is an adenovirus receptor and that the Survivin promoter selectively targets cells with high Survivin expression, combined with the external overexpression of Interferon-like protein L-IFN by YSCH-01, we hypothesize that YSCH-01 exerts anti-tumor effects on OS. Based on this, we conducted both in vitro and in vivo experiments.
The in vitro experiments confirmed that YSCH-01 could infect human OS cells, varying infectivity among different cell lines. MG-63 and U-2 OS cells were significantly infected at lower concentrations, while the MNNG/HOS cells required higher concentrations for significant infection, and 143B cells required even higher concentrations. Furthermore, the experimental group demonstrated overexpression of the antitumor protein L-IFN at both the RNA and protein levels, reinforcing the notion that YSCH-01 can infect different OS cell types. CCK8 assay results also demonstrated that YSCH-01 exhibited cytotoxicity against OS cells in vitro, with varying potencies across cell lines. The IC50 values ranged from 18.49 MOI for U-2 OS to 198.3 MOI for MG-63, indicating a 10.72-fold difference in sensitivity.
In the pharmacodynamic experiments involving nude mice transplanted with OS cell lines (U-2 OS, 143B, and MNNG/HOS) were injected with either empty vector OncoMul-V2 or the oncolytic adenovirus YSCH-01 carried L-IFN gene. YSCH-01 and OncoMul-V2 demonstrated significant tumor inhibition at the administration site, with YSCH-01 showing superior anti-tumor effects compared to OncoMul-V2 in the 143B and MNNG/HOS groups. Additionally, YSCH-01 exhibited an inhibitory effect on the non-administered side of the tumor, known as an abscopal effect, in the U-2 OS and 143B groups. In contrast, the empty virus did not produce any abscopal effect in the three groups. These results confirm that YSCH-01 has more potent anti-tumor effects than the empty vector virus and induces abscopal effects in certain OS cell lines. In PDX models, YSCH-01 also significantly inhibited tumor growth at the administration site. Also, it showed some inhibitory effect on non-injected tumors, consistent with results from the CDX model.
YSCH-01 is a multifunctional oncolytic adenovirus developed using the CTGVT strategy, which employs adenoviruses as gene delivery vectors to transfer therapeutic genes into host cells. YSCH-01 is engineered with a dual regulatory strategy to achieve targeted replication: its wild-type E1A promoter is replaced with a truncated optimized Survivin promoter, and the CR2 region of the 24 bp E1A gene has a deleted base pair sequence. These modifications enhance the virus’s ability to selectively target tumor cells while minimizing its effect on normal cells. As a result, YSCH-01 demonstrates high efficiency, stability, safety, broad infectivity, and large payload capacity during the targeted replication of the oncolytic adenovirus in tumor cells. Besides, the L-IFN gene carried by YSCH-01, which was designed with a signal peptide sequence, can be highly expressed during adenovirus replication. As reported in our earlier studies (Shan Jiang et al., 2023)29, the L-IFN protein expressed by YSCH-01-infected tumor cells can be secreted extracellularly, which contributing to the anti-tumor effects. L-IFN protein is known to exert multiple anti-tumor effects, including activating the immune response of host cells, enhancing viral resistance, promoting the activation of the natural immune system, inhibiting viral replication and transmission, and directly inducing anti-tumor effects30. A series of comprehensive clinical and non-clinical studies, including those conducted by our team, have shown that YSCH-01 has significant anti-tumor activity. The proposed mechanisms by which YSCH-01 exerts its anti-tumor effects include replicating extensively in tumor cells to induce tumor cell apoptosis and autophagy, regulating the immune microenvironment in tumors, such as promoting immune cell infiltration and increasing cytokine secretion, upregulating the expression of MHC-I proteins on the surface of tumor cells to promote the presentation of tumor antigens, inhibiting tumor angiogenesis, and activating specific intracellular signaling pathways that affect the survival and proliferation of tumor cells31.
Our research confirms YSCH-01’s significant anti-tumor effects on OS in both in vitro and in vivo experiments. However, several questions remain that warrant further investigation. In the pharmacodynamic experiments conducted on the CDX model, YSCH-01 demonstrated differential effects on OS cell lines, showing distal efficacy in U-2 OS and 143B cells but not in MNNG/HOS cells. Additional studies are needed to clarify the underlying reasons for this discrepancy and to optimize the treatment protocol. In the PDX model, YSCH-01 significantly inhibited tumor growth in OS xenografts and also showed a notable anti-tumor effect on the non-treated side. However, due to time and cost constraints, only two PDX models were successfully established in this study. Further research should aim to establish a more significant number of PDX models to support our findings more robustly. Moreover, the RNA sequencing of tumors in the PDX model presents another area for improvement. The strong killing effect of the experimental group resulted in tumors that were too small for RNA sequencing. Although CDX model tumors confirmed our hypothesis, further exploration is necessary to determine if similar results would be observed in the PDX model. Adjusting the treatment dosage or duration in the future may help achieve a more optimal balance between tumor response and sample availability for sequencing.
We also intend to investigate additional factors that may enhance the anti-tumor effects of YSCH-01 and to further understand the underlying reasons for its variable efficacy across different OS cell lines. Preliminary findings by our team revealed that the combination of gemcitabine with YSCH-01 exhibited synergistic anti-tumor effects in the HCC1806 human breast squamous cell carcinoma CDX model (data not shown). Given gemcitabine’s established role in treating osteosarcoma, future studies will explore its combination with YSCH-01 as a potential therapy for OS. Additionally, we aim to elucidate the specific mechanisms by which YSCH-01 exerts anti-osteosarcoma effects and to identify the key components contributing significantly to its anti-tumor activity. Finally, we plan to conduct clinical trials to evaluate the efficacy of YSCH-01 in patients with advanced OS. These future research directions will enhance our understanding of YSCH-01’s anti-osteosarcoma effects and pave the way for its potential clinical application in treating this challenging malignancy.
Interferons are a group of signaling cytokines, secreted by host cells to induce protection against various disorders, including directly impacting tumor cells or indirectly causing the immune system to protect host cells. The efficacy of anticancer therapies is correlated to Interferon signaling32. Potent antiproliferative, proapoptotic, antiangiogenic, and immunomodulatory effects of interferons prompted their use for anticancer treatment33. Besides, single-cell RNA sequencing studies at serial time points during immune therapy also showed that peripheral immune cell phenotypes were linked to the increased strength of patients’ tumor-immune cell interaction, including increased cytotoxic differentiation and strong activation of interferon signaling in peripheral T cells in responder patients34, which revealed the important impact of interferon signal pathways in tumor therapy. Despite the potent antitumorigenic properties of natural and pharmacologic type I interferons, these agents achieved only a limited success in cancer therapy, which is often attributed to the downregulation of type I interferon receptor35. L-IFN, a novel recombinant type I Interferon derived from human IFNa-2b and other type I interferon subtypes by mutagenesis, can be expressed by our oncolytic adenovirus YSCH-01 in the tumor cells and exert immune cell stimulation and antitumor effect. Previous research by Zhang et al. revealed that sIFN-I, an first-generation interferon-like protein similar to L-IFN, has been demonstrated to robustly inhibit tumoral angiogenesis, activate immune cells, and suppress the growth of transplantable and genetically engineered tumors in mouse models36.
In order to reveal the main mechanism of YSCH-01, we carried out the RNAseq analysis and the following validation with mouse CDX tumor tissue after YSCH-01 therapy. The results showed that the type I interferon-related genes were the most significantly differentially expressed compared with the vehicle group, preliminarily revealing the related mechanism of YSCH-01 against osteosarcoma, which is consistent with the previous clinical research on circulating immune cell phenotype markers after immune therapy34.
As shown in Fig. 5, the control virus without L-IFN expression exhibited minimal therapeutic effect in untreated distant tumors. This aligns with our previous finding36, supporting the proposed mechanism that YSCH-01’s distant therapeutic effect is primarily mediated by extracellularly secreted L-IFN and subsequent immune cell activation. To test this hypothesis, CCK-8 cytotoxicity assays were performed using supernatants from YSCH-01-infected 143B tumor cells. Consistent with our speculation, the supernatants exhibited minimal in vitro cytotoxicity against tumor cells (data not shown). Concurrently, an in vitro experiment using supernatants from YSCH-01-infected 143B cells to stimulate mouse PBMCs revealed that YSCH-01-infected osteosarcoma cell supernatants upregulated proinflammatory cytokine expression (IFN-γ, IL-12α, and TNF-α) in PBMCs. This suggests that factors like L-IFN in the supernatant contribute to immune cell activation. Collectively, these results highlight L-IFN’s critical role in YSCH-01’s abscopal effect. Future studies should characterize the specific immune cell subsets activated by L-IFN and their migration to distant tumors.
In conclusion, our findings, validated through both in vivo and in vitro experiments, underscore the potential of YSCH-01 as a promising therapeutic agent for OS. This study also provides valuable insights into the potential antitumor mechanisms of the oncolytic adenovirus YSCH-01 in the context of OS. These results warrant further investigations to explore the clinical applications of YSCH-01 in OS treatment and to fully characterize its therapeutic potential.
Materials and methods
Oncolytic adenovirus
The Oncolytic adenoviruses we used in this study were OncoMul-V2, OncoMul-V2-EGFP, and YSCH-01, all constructed by Shanghai Yuansong Biotechnology Co., Ltd. OncoMul-V2 served as the oncolytic adenovirus vector, in which the E1A promoter of the human wild adenovirus type 5 was replaced with a truncated Survivin promoter and a 24-base pair sequence of the CR2 region of the E1A gene was deleted. OncoMul-V2-EGFP was a derivative of OncoMul-V2 that carried an exogenous green fluorescent protein (EGFP) sequence. YSCH-01, also known as Recombinant L-IFN Adenovirus, incorporated the multifunctional therapeutic gene L-IFN into the OncoMul-V2 backbone. All viruses were stored at -80℃ and thawed on ice before use.
In our previous preclinical studies, we did not prioritize researching the effects of YSCH-01 on the osteosarcoma immune microenvironment. However, recent laboratory data from our ongoing Phase I/IIa clinical trials of YSCH-01 for pan-cancer treatment (Clinical Trial No. CTR20241362) indeed show an increase in peripheral blood NK cell counts following YSCH-01 administration. This finding suggests that YSCH-01 may activate NK cells, a hypothesis we will prioritize for in-depth investigation in future studies.
Cell lines and culture conditions
The OS cell lines MNNG/HOS, 143B, MG-63, and U-2 OS, along with normal human bone marrow stromal cells (hBMSC), were used in this study. All cell lines were obtained from the Cell Bank of the Chinese Academy of Sciences (Shanghai, China). The MNNG/HOS, MG-63, and U-2 OS cell lines were cultured in Dulbecco’s Modified Eagle’s Medium (DMEM), and the 143B cell line was cultured in DMEM/F12. Both culture mediums were supplemented with 10% fetal bovine serum (FBS, Gibco, USA). The hBMSC was cultured in a 1:1 mixture of Ham’s F12 medium and DMEM, supplemented with 10% FBS (Gibco, USA). All culture media were additionally supplemented with 1% penicillin and streptomycin (Sigma-Aldrich, St Louis, MO, USA).
Human osteosarcoma samples
All patients were treated at the Department of Orthopaedic, Shanghai Jiao Tong University Affiliated Sixth People’s Hospital. OS tissue samples were collected from patients between 2022 and 2023. The protocol of this study was approved by the Ethics Committee of Shanghai Sixth People’s Hospital (NO. 2020 − 131). All methods were carried out in accordance with relevant guidelines and regulations. We followed the ethical guidelines outlined in the Helsinki Declaration for conducting research involving human subjects. We guaranteed the protection of data anonymity and confidentiality and utilizing it solely for purposes stated above. Informed consent was obtained from all subjects and/or their legal guardian(s).
RNA extraction and the quantitative real-time PCR (qPCR) analysis
Total RNA was extracted from tissue samples and cultured cells using TRIzol reagent (Invitrogen, Carlsbad, CA, USA). Reverse transcription was performed with the RevertAid First Strand cDNA Synthesis Kit (Invitrogen, USA). The qPCR experiments were conducted on an ABI Prism 7900HT real-time system (Applied Biosystems). All reactions were carried out in triplicate in a final reaction volume of 10 µL. The relative mRNA expression of different genes was calculated using the 2^-ΔΔCt approach.
Protein extraction and Western blotting analysis
Protein lysates were prepared from cultured cells using RIPA buffer (EpiZyme, PC102) containing a protease inhibitor (Invitrogen, 36978) and PhosSTOP (Roche, Switzerland). The lysates were placed on the ice for 30 min, followed by centrifugation at 13,000 × g for 15 min at 4℃ to remove precipitates. Proteins were then separated by electrophoresis and transferred onto a PVDF membrane. At room temperature, the membrane was blocked with 5% nonfat milk for one hour. Subsequently, the following primary antibodies were added: CXADR, Survivin, IFNAR, PD1, RB, PD-L1, actin, L-IFN (custom-made), and β-tubulin. The membrane was incubated overnight with these primary antibodies on a shaker at 4℃. Afterward, HRP-linked anti-rabbit IgG (1:2000) or HRP-linked anti-mouse IgG (1:1000) was used as the secondary antibody. Protein bands were visualized using Super Signal West Femto Maximum Sensitivity Substrate (Thermo Fisher Scientific).
Fluorescence activating cell sorting (FACS)
Osteosarcoma cells were cultured in 12-well plates at a density of 2 × 105 cells/well overnight. The cells were then treated with empty vector oncolytic adenoviruses carrying EGFP at multiplicities of infection (MOIs) of 1, 10, and 50 or with vehicle control. After 48 h, the cells were photographed and digested by Accutase (#40506ES60, YEASEN), washed once with phosphate-buffered saline (PBS), and resuspended in PBS for FACS analysis.
The PDX and CDX model establishment
-
1.
Experimental animals:
Female NOG mice (4 weeks old) were purchased from Shanghai Lingchang Biotechnology Co., Ltd, and female Balb/c nude mice (4–5 weeks old) were obtained from Beijing Vital River Laboratory Animal Technology Co., Ltd., Shanghai Subsidiary. All mice were specific pathogen-free (SPF) grade and housed in an SPF-grade facility, maintained at a temperature of 20–26℃, with 40–70% humidity, on a 12 h light/dark cycle. No more than five mice were kept in each cage, with free access to food and water. All animal experimental protocols were approved by the Experimental Animal Care Commission of Shanghai LIDE biotech Co. Ltd (the reference number LDIACUC 006). All the methods were performed in accordance with the relevant guidelines and regulations including ARRIVE guidelines.
-
2.
The PDX model:
Tumor samples from OS patients were collected during biopsy surgeries and cut into small fragments (approximately 2 × 2 × 2 mm). These fragments were implanted subcutaneously into NOG mice. Tumor growth was monitored regularly, and once the tumors reached a volume of approximately 200 mm3, they were removed, cut into smaller pieces, and passaged into Balb/c nude mice to maintain the PDX model.
-
3.
The CDX model:
OS cell lines (U-2 OS, 143B, MNNG/HOS) were cultured during their logarithmic growth phase. Cells were resuspended in a suitable medium and injected subcutaneously into the flanks of nude mice at a density of 3 × 106 cells per side. Tumor growth was monitored, and when the tumors reached a specific size, they were harvested for further analysis.
-
4.
Treatment administration:
When tumor volumes reached approximately 150 mm3 in the PDX model and 80–120 mm3 in the CDX model, treatment with YSCH-01 oncolytic adenovirus was initiated. Mice were divided into 3 groups: two treatment groups received intratumoral injections of YSCH-01 or the empty vector virus OncoMul-V2, while the control groups received intratumoral injections of vehicles. The frequency of administration are once every 2 days for 5 times (Q2D X 5). Tumor volume and body weight were measured every 3 days and the overall health of the mice was monitored throughout the treatment period.
-
5.
Tumor volume calculation:
Tumor volumes were measured regularly using calipers. Statistical analysis was performed to compare tumor growth inhibition, treatment response, and overall efficacy among different treatment groups in both the PDX and CDX model experiments. Tumor Growth Inhibition Rate (TGI): When Ti-T0 > 0, TGI(%)=[1 - (Ti - T0) / (Ci - C0)] × 100, When Ti-T0 < 0, TGI % = [1 - (Ti - T0) / T0] × 100. Ti is the average tumor volume in the treatment group on the assessment day, T0 is the average tumor volume in the treatment group on the grouping day, Ci is the average tumor volume in the solvent control group on the assessment day, and C0 is the average tumor volume in the solvent control group on the grouping day.
Cell counting kit-8 (CCK-8) assay
Cell proliferation was assessed using the CCK-8 assay. OS cells (U-2 OS, 143B, MNNG/HOS) were seeded at a density of 2000 cells/100 µl/well and MG-63 cells at 2500 cells/100 µl/well in a 96-well plate. The cells were incubated in a humidified cell culture incubator at 37 °C with 5% CO2 for 18 h. Subsequently, cells were treated with varying doses of the YSCH-01 virus. After 96 h, 10 µl of CCK-8 reagent (#40203ES80, Yeasen Biotechnology, Shanghai, China) was added to each well, followed by further incubation at 37 °C with 5% CO2 for 1 h. Finally, absorbance at 450 nm was measured using a microplate reader.
RNA-seq sequencing and data analysis
The human 143B CDX nude mouse received intratumoral injections of YSCH-01, while the control groups received intratumoral injections of vehicles. The frequency of administration were once every 2 days for 5 times. After therapy with YSCH-01 or vehicle for 15 days, tumor tissues from two groups were collected and put into liquid nitrogen for quick freezing. All the experiments were done by triplicate. RNA was extracted using the RNeasy Plus Mini kit (QIAGEN, Hilden, Germany). The RNA integrity was assessed with an Agilent 2100 Bioanalyzer (Agilent Technologies). The corresponding RNA libraries construction, sequencing and data analysis were carried out by the JingZhou Gene company.
Immunohistochemistry (IHC)
OS tissues from clinical patients and subcutaneous tumor models were embedded in paraffin. Standard 4 μm sections were cut from the paraffin-embedded tissues and de-paraffinized, followed by antigen retrieval, blocking, and overnight incubation. The samples were then washed with phosphate-buffered saline (PBS) and incubated with an HRP-linked anti-IgG antibody at 37℃ for 30 min. Following three additional PBS washes, the samples were stained with 3,3’-diaminobenzidine (DAB) for 5–10 min. After counterstaining and dehydrating, the samples were observed using a DM6B microscope (Leica Microsystems).
Statistical evaluation
All data were analyzed using GraphPad Prism 8 software (San Diego, CA, USA). Student’s t-test or a one-way analysis of variance was performed to calculate the differences between the experimental group and the control group, and P < 0.05 was considered statistically significant (*P < 0.05; **P < 0.01; ***P < 0.001).
Data availability
Data from all RNA-seq are uploaded to the NCBI Gene Expression Omnibus (GEO) database with GEO Series accession number GSE294206 (https://www.ncbi.nlm.nih.gov/geo/query/acc.cgi?acc=GSE294206) and available from the corresponding author on reasonable request.
References
Hannah, C. B. et al. Osteosarcoma. Nat. Rev. Dis. Primers 8, 1 (2022).
Theresa, H. M. K., Renata, A. & Elysia, M. A. Survival trends among adolescents and young adults diagnosed with cancer in the united states: comparisons with children and older adults. J. Clin. Oncol. 42, 6 (2023).
Gill, J. & Gorlick, R. Advancing therapy for osteosarcoma. Nat. Rev. Clin. Oncol. 18 (10), 609–624 (2021).
Panagi, M., Pilavaki, P., Constantinidou, A. & Stylianopoulos, T. Immunotherapy in soft tissue and bone sarcoma: unraveling the barriers to effectiveness. Theranostics 12 (14), 6106–6129 (2022).
Yan, P., Wang, J., Yue, B. & Wang, X. Unraveling molecular aberrations and pioneering therapeutic strategies in osteosarcoma. Biochim. Et Biophys. Acta Rev. Cancer. 1879 (5), 189171 (2024).
Alannah, S. et al. Future directions in the treatment of osteosarcoma. Cells 10, 1 (2021).
Hana Lim, M. et al. Tandem High-Dose chemotherapy increases the risk of secondary malignant neoplasm in pediatric solid tumors. Cancer Res. Treat. 56 (2), 642–651 (2024).
Ju, H. Y. et al. Vincristine, Irinotecan, and Temozolomide as a salvage regimen for relapsed or refractory sarcoma in children and young adults. Cancer Res. Treat. 54 (2), 563–571 (2022).
Zhengbo, H. et al. Enrichment of Wee1/CDC2 and NF-κB signaling pathway constituents mutually contributes to CDDP resistance in human osteosarcoma. Cancer Res. Treat. 54 (1), 277–293 (2022).
Crompton, J. et al. Local control of soft tissue and bone sarcomas. J. Clin. Oncol. 36 (2), 111–117 (2018).
Hannah, C. et al. Osteosarcoma. Nat. Rev. Dis. Primers 8 (1), 77 (2022).
Isakoff, M., Bielack, S., Meltzer, P. & Gorlick, R. Osteosarcoma: current treatment and a collaborative pathway to success. J. Clin. Oncol. 33 (27), 3029–3035 (2015).
Shi, P. et al. Active targeting schemes for nano-drug delivery systems in osteosarcoma therapeutics. J. Nanobiotechnol. 21 (1), 103 (2023).
Lisa, M. et al. Frequency of pathogenic germline variants in Cancer-Susceptibility genes in patients with osteosarcoma. JAMA Oncol. 6, 5 (2020).
Liu, Y. et al. Single-cell and Spatial transcriptomics reveal metastasis mechanism and microenvironment remodeling of lymph node in osteosarcoma. BMC Med. 22 (1), 200 (2024).
Lizardo, M. et al. Pharmacologic Inhibition of eIF4A blocks NRF2 synthesis to prevent osteosarcoma metastasis. Clin. Cancer Res. 30 (19), 4464–4481 (2024).
Russell, S., Peng, K. & Bell, J. Oncolytic virotherapy. Nat. Biotechnol. 30 (7), 658–670 (2012).
Bommareddy, P., Shettigar, M. & Kaufman, H. Integrating oncolytic viruses in combination cancer immunotherapy. Nat. Rev. Immunol. 18 (8), 498–513 (2018).
Shalhout, S., Miller, D., Emerick, K. & Kaufman, H. Therapy with oncolytic viruses: progress and challenges. Nat. Rev. Clin. Oncol. 20 (3), 160–177 (2023).
Toulmonde, M. et al. Reshaping the tumor microenvironment of cold soft-tissue sarcomas with oncolytic viral therapy: a phase 2 trial of intratumoral JX-594 combined with avelumab and low-dose cyclophosphamide. Mol. Cancer. 23 (1), 38 (2024).
Ferguson, M. et al. Transient Inhibition of PI3Kδ enhances the therapeutic effect of intravenous delivery of oncolytic vaccinia virus. Mol. Therapy: J. Am. Soc. Gene Therapy. 28 (5), 1263–1275 (2020).
Willmon, C. et al. Cell carriers for oncolytic viruses: fed ex for cancer therapy. Mol. Therapy: J. Am. Soc. Gene Therapy. 17 (10), 1667–1676 (2009).
Kim, C. et al. N-acetylcysteine amide augments the therapeutic effect of neural stem cell-based antiglioma oncolytic virotherapy. Mol. Therapy: J. Am. Soc. Gene Therapy. 21 (11), 2063–2073 (2013).
Jennings, V. et al. Lymphokine-activated killer and dendritic cell carriage enhances oncolytic reovirus therapy for ovarian cancer by overcoming antibody neutralization in Ascites. Int. J. Cancer. 134 (5), 1091–1101 (2014).
Ilett, E. et al. Internalization of oncolytic reovirus by human dendritic cell carriers protects the virus from neutralization. Clin. Cancer Res. 17 (9), 2767–2776 (2011).
Kaufman, H., Kohlhapp, F. & Zloza, A. Oncolytic viruses: a new class of immunotherapy drugs. Nat. Rev. Drug Discovery. 14 (9), 642–662 (2015).
Kelly, E. & Russell, S. History of oncolytic viruses: genesis to genetic engineering. Mol. Therapy: J. Am. Soc. Gene Therapy. 15 (4), 651–659 (2007).
Ma, X., Hill, B., Hoang, T. & Wen, F. Virus-inspired strategies for cancer therapy. Sem. Cancer Biol. 86, 1143–1157 (2022).
Shan Jiang, H. H. & Chai, X. L. Double-modified oncolytic adenovirus armed with a recombinant interferon-like gene enhanced abscopal effects against malignant glioma. Neurooncol. Adv. 28 (1), vdad117 (2023).
Xu He, W. Y. et al. Potent antitumor efficacy of human dental pulp stem cells armed with YSCH–01 oncolytic adenovirus. J. Transl. Med. 21 (1), 688 (2023).
He, Y. et al. Preliminary efficacy and safety of YSCH01 in patients with advanced solid tumors: an investigator-initiated trial. J. Immunother. Cancer 12 (5), e008999 (2024).
Abdolvahab, M. H. et al. Interferons: role in cancer therapy. Immunotherapy 12 (11), 833–855 (2020).
Borden, E. C., Lindner, D., Dreicer, R., Hussein, M. & Peereboom, D. Secondgeneration interferons for cancer: clinical targets. Semin. Cancer Biol. 10, 125–144 (2000).
Jason, I. et al. Circulating immune cell phenotype dynamics reflect the strength of tumor-immune cell interactions in patients during immunotherapy. Proc. Natl. Acad. Sci. U S A 117 (27), 16072–16082 (2020).
Serge, Y. Fuchs Hope and fear for interferon: the receptor-centric outlook on the future of interferon therapy. J. Interferon Cytokine Res. 33, 211–225 (2013).
Zhang, K. J. et al. A potent in vivo antitumor efficacy of novel Recombinant type I interferon. Clin. Cancer Res. 23 (8), 2038–2049 (2017).
Funding
This work was supported by National Natural Science Foundation of China (82173343), Shanghai Oriental Talent Program(CYQN2023030), Academician Expert Workstation Grants (No.19R1002275468, 20R9004076411, 21R4007547098, S182023110190129357) in Shanghai Yuansong Biotechnology Co., Shanghai science and technology support project on biomedicine in the action plan of Science and Technology innovation (Grant No.19431904200).
Author information
Authors and Affiliations
Contributions
Qingcheng Yang, Shumin Zhou, Ning Li, Jin Huang and Kang-jian Zhang conducted the conception and design of study; Hanqiang Jin, Ruoyu Chen, Yonggang Wang, Jin Huang and Ning Li conducted the experiments; Hanqiang Jin, Ruoyu Chen, Qingcheng Yang, Shumin Zhou and Ning Li conducted the analysis and/or interpretation of data; Ruoyu Chen, Hanqiang Jin, Xue-ping Cao, Xian-long Fang and Yonggang Wang drafted the manuscript; Shumin Zhou, Ning Li and Hafiz Khuram Raza revised the manuscript criticaly for important intellectual content.
Corresponding authors
Ethics declarations
Competing interests
Kang-jian Zhang and Xian-long Fang hold an ownership interest (including patents of YSCH-01) in Yuansong Biotechnology. Other authors report no conflict of interest.
Human ethical approval
The protocol of the human tumor tissues study was approved by the Ethics Committee of Shanghai Sixth People’s Hospital (NO. 2020 − 131). All methods were carried out in accordance with relevant guidelines and regulations. We followed the ethical guidelines outlined in the Helsinki Declaration for conducting research involving human subjects. We guaranteed the protection of data anonymity and confidentiality and utilizing it solely for purposes stated above. Informed consent was obtained from all subjects and/or their legal guardian(s).
Animal ethics approval
All animal experimental protocols were approved by the Experimental Animal Care Commission of Shanghai LIDE biotech Co. Ltd (the reference number LDIACUC 006). All methods of animal study were carried out in accordance with relevant guidelines and regulations. This study is reported in accordance with the ARRIVE guidelines. Mice were monitored every other day for humane endpoints, specifically tumor size, activity levels, and weight loss exceeding 15%. At the time of sacrifice, none of the animals had reached these humane endpoints. The mice were euthanized in a CO₂ environment via cervical dislocation.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.

Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Jin, H., Chen, R., Wang, Y. et al. Therapeutic efficacy of oncolytic adenovirus YSCH-01 in osteosarcoma evaluated in PDX and CDX mouse models. Sci Rep 15, 43565 (2025). https://doi.org/10.1038/s41598-025-27137-z
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-27137-z