Abstract
Despite infectious diseases being a significant threat to global health, there are continuing concerns that regulatory authorities do not prioritize therapeutic strategies for infectious diseases with the same urgency as those for oncological or orphan diseases. This study aims to examine the differences in the productivity of drug development and approval procedures between non-infectious and infectious diseases, and to determine the utilization patterns of acceleration programs. All molecules and biologic products approved between January 1, 2015, and December 31, 2024 (N = 464) were subject to a cross-sectional study. Drugs@FDA, the Federal Register, and ClinicalTrials.gov were used as sources of data to establish median Clinical Development Time (CDT), Regulatory Approval Time (RAT), and cumulative Regulatory Review Time (RRT). Kruskal–Wallis tests were used to compare median values (interquartile range, IQR), and chi-square tests were used for proportions. Time-to-event differences were tested using Kaplan–Meier analyses with log-rank testing, and hazard ratios (HRs) were calculated using Cox proportional hazards models. Multivariable logistic regression with interaction terms was used to model Priority Review, Fast Track, Breakthrough Therapy, and Accelerated Approval, reporting adjusted odds ratios (aOR). Of 464 approvals, 65 (14.0%) targeted infectious diseases. Median CDT was 2.76 years (IQR 1.80–4.25) versus 3.46 years (IQR 2.59–4.66; p = 0.003), and median RRT was 3.54 years (IQR 2.58–5.03) versus 4.22 years (IQR 3.24–5.73; p = 0.006) for infectious and non‑infectious drugs, respectively. Nevertheless, infectious agents were approved 58% faster (HR = 1.58; 95% CI 1.15–2.16; p = 0.0047). Infectious disease products were more likely to receive Fast Track (OR = 4.49; 95% CI 2.39–8.70) and Priority Review (OR = 10.69; 95% CI 4.57–29.50) but less likely to obtain Breakthrough Therapy (OR = 0.42; 95% CI 0.28–0.63) or Accelerated Approval (OR = 0.12; 95% CI 0.016–0.56). Infectious disease treatments outpace non-infectious disease treatments in terms of drug development and approval timelines. Nevertheless, they are less frequently utilized in pathways like Accelerated Approval, which are scientifically less applicable to acute-disease endpoints. Therefore, policy reforms should focus on addressing the underlying economic and scientific barriers to anti-infective innovation.
Similar content being viewed by others
Introduction
Infectious diseases represent a major public health threat, resulting in significant morbidity and mortality globally1. The COVID-19 pandemic heightened human vulnerability, leading to an estimated 14.83 million excess deaths by the end of 2021, and resulting in an economic output of around US$3.8 trillion in 20202,3. At the same time, antimicrobial resistance (AMR) is estimated to cause approximately 4.95 million deaths per year, 1.27 million of which are due to treatment-resistant infections4. Yet new antimicrobial innovation gains have been slowed by scientific hurdles and insufficient commercial incentives4,5. Despite current clinical needs, the number of anti-infective agents successfully marketed remains significantly lower than that for oncology or orphan disease treatments6. Alongside the development of new molecular entities, strategies such as drug repurposing and off-label use are critical in expanding the therapeutic arsenal, particularly during public health crises7,8. To shorten the development process, the US Food and Drug Administration (FDA) implemented four accelerated pathways under the 2012 FDA Safety and Innovation Act (FDASIA); namely, Priority Review, Fast Track, Breakthrough Therapy, and Accelerated Approval9. These mechanisms aim to shorten development time without compromising safety and efficacy. Similar initiatives exist globally, such as the European Medicines Agency’s (EMA) PRIME scheme and Japan’s ‘Sakigake’ designation, reflecting a global consensus on the need for regulatory flexibility to address unmet medical needs10.
Notably, the use of expedited programs shows significant variation: between 2015 and 2019, 73% of oncology approvals received Priority Review designation, compared to only 45% of infectious disease-related products11. Various scientific and logistical hurdles; such as surrogate endpoint validation, complexities in large trials across geographically diverse areas, and the need for tight safety controls in essentially healthy populations; have been cited as factors in the slower progress of anti-infective treatments12,13. By comparison, regulatory authorities are flexible amid crises, proactively adjusting procedures to meet public health crises14.
To determine if the regulatory issues described lead to significant delays, we conducted a systematic analysis of Clinical Development Time (CDT), Regulatory Approval Time (RAT), and Regulatory Review Time (RRT) for all pharmaceuticals and biologics approved by the FDA between 2015 and 2024. Based on information from the FDA database, ClinicalTrials.gov, and previous meta-analyses, our analyses were stratified by infectious versus non-infectious indications, examined the use of expedited designations (including Priority Review, Breakthrough Therapy, Fast Track, and Orphan Drug), and examined pertinent trial-design characteristics. Extending the correlation between expedited pathways and development efficiency described by Hwang et al.15 and the framework of Sacks et al., emphasizing disease-specific regulatory decision-making considerations16, this research examines the application of regulatory pathways between different therapeutic classes, specifically testing whether treatments for infectious diseases achieve structural alignment with the eligibility criteria of expedited programs. We hypothesize that a structural difference exists, in which treatments for infectious diseases provide scientific evidence (e.g., from acute trial designs) that is less compatible with the eligibility criteria for certain expedited designations. If this disparity is confirmed, it would indicate a structural misalignment between program eligibility criteria and the scientific realities of anti-infective drug development, requiring policy change.
Methods
Data sources and cohort definition
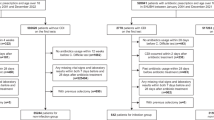
This is a cross-sectional examination that evaluates new molecular entities (NMEs) and new therapeutic biological products approved by the US FDA from January 1, 2015, through December 31, 2024. The study employed publicly available sources, including the Drug@FDA database17, the Federal Register18, and ClinicalTrials.gov19. Products were included if they were designated as NMEs or therapeutic biologics and were approved by the US FDA between January 1, 2015, and December 31, 2024. Products were excluded if they were generics, veterinary medications, or approved beyond the study period. Detailed inclusion/exclusion criteria are provided in the Supplementary Methods.
Study objectives
The study’s objectives were structured as follows:
Primary objective
To compare the regulatory timelines (Clinical Development Time (CDT) and Regulatory Review Time (RRT)) for infectious versus non-infectious therapeutics.
Secondary objectives
(1) To compare the utilization rates of the four primary FDA expedited pathways (Priority Review, Fast Track, Breakthrough Therapy, and Accelerated Approval) between the two therapeutic areas; and (2) To identify the independent predictors associated with receiving each expedited designation.
Exploratory objective
To evaluate the interaction effects between the infectious disease indication and the expedited pathway designations on the overall time-to-approval.
Cohort definition and analytical subsets
The final dataset included 457 products (51 infectious and 406 non-infectious), after exclusions for withdrawn, diagnostic, or literature-based approvals (7 drugs in total; 1.5%). Disease classifications were based on primary therapeutic indication. This sample was handled similarly for all Cox regression20 and Kaplan–Meier21 Analyses.
Outcome measures
Three main periods were computed. CDT is the duration from the Investigational New Drug (IND) effective date to the New Drug Application (NDA) or Biologic License Application (BLA) submission date. Meanwhile, RAT is the duration from NDA or BLA submission to FDA approval. Moreover, RRT is the duration from the IND effective date to the FDA approval. CDT represents the time from Investigational New Drug (IND) application approval, which is simply an FDA authorization to initiate human clinical trials, to the submission of either a New Drug Application (NDA) for small-molecule drugs or a Biologics License Application (BLA) for biologic products. RAT is the time from the NDA/BLA submission to final FDA Approval, while RRT reflects the whole time from the IND Approval to the product’s Approval.
Secondary outcomes included assessment of regulatory designations, including Priority Review, Breakthrough Therapy, Fast Track, and Orphan Drug designation. Secondary outcomes included subgroup analysis by application type (NDA vs. BLA), regulatory designation (Priority vs. Standard Review, Orphan vs. Non-Orphan), and trial phase (Phase 2, 3, or 4).
Trial characteristics and covariates
For each approved product, the attributes of the clinical trials were derived, including trial phase, enrollment size, endpoint type (clinical or surrogate), and orphan drug designation status. The approval year was also recorded to examine temporal trends and external events, such as the COVID-19 pandemic.
Statistical analyses
Continuous variables, such as CDT, RAT, and RRT, were reported as medians with interquartile ranges (IQR) and compared using the Kruskal–Wallis test. The chi-squared test evaluated categorical measurements as proportions. Temporal trends were assessed with the aid of the Cochran–Armitage trend tests. Time-to-event analyses (Kaplan–Meier and Cox regression) were used to model regulatory timelines. This approach is well-suited to the non-normal, right-skewed nature of regulatory data and properly accommodates censored observations. It provides a more dynamic measure of approval probability (hazard) over time, and its use is consistent with established methodological precedents in regulatory science. Kaplan–Meier curves were used to assess time-to-event distributions for CDT, RAT, and RRT, and comparisons were made using log-rank tests with follow-up. As the cohort comprised only successfully approved products, withdrawal or rejection was not considered a competing event.
Multivariable logistic regression models were constructed to identify the independent predictors for each accelerated designation. To evaluate predictors of FDA expedited designations, we developed separate multivariable logistic regression models for each of the FDA expediting programs. Additionally, a single logistic interaction model was constructed to examine the interaction effects between infectious disease indication and each expedited program. Cox proportional hazards regression models were used to examine the predictors of the time until approval (RRT), reporting hazard ratios (HR) with 95% confidence intervals (CI) ; proportional hazards assumptions were checked and confirmed by Schoenfeld residual analysis. No imputation was performed. Our final cohort had complete timeline data based on the unified start-date metric (IND effective date), thus no imputation for missing data was necessary. The statistical analysis is more detailed in the supplementary methods.
Machine learning analysis: random forest classifier
A Random Forest classifier22 was used to predict the probability of a Priority Review. Full methodology, hyperparameters, and performance metrics (including AUC and variable importance) are presented in Supplementary Methods. Supplementary Figure S6 reports the ROC and precision-recall (PR) curves for reference.
Subgroup and sensitivity analyses
Subgroup analyses grouped according to application type NDA versus BLA, orphan status, trial stage, and approvals before versus after 2020 were conducted as a means of testing the strength of inferences across diverse settings. Sensitivity analyses included exclusion of extreme values (the upper and lower 2.5% of CDT and RAT) and alternative gamma regression modeling of RRT. To specifically address the potential confounding effect of the COVID-19 pandemic, a detailed sensitivity analysis was performed by excluding all 12 COVID-19-related approvals; the full results of this analysis are provided in the Supplementary Information (Supplementary Results, Table S6). Each statistical comparison was two-sided, with a threshold of significance of p < 0.05. Results were calculated using R 4.2.1 and Python 3.9.
Results
Cohort characteristics and approval trends
Figure 1 illustrates the large-scale FDA approvals of new molecular entities and biologics between January 1, 2015, and December 31, 2024. In this period, a cumulative 464 products obtained approval, comprising 65 (14.0%) treatments for infectious diseases and 399 (86.0%) for non-infectious diseases. In the non-infectious approval category, oncology accounted for the largest share with 134 approvals (28.9%), followed by neurology with 82 approvals (17.7%), with the remaining 183 approvals (39.5%) divided among rare diseases, cardiology, and other non-infectious disease groups. Yearly approvals increased steadily from 28 in 2015 to 42 in 2021, then decreased to 36 in 2024; in contrast, infectious disease approvals showed greater volatility. They progressed from 3 in 2015 to 10 in 2022 (Fig. 1), a spike largely attributable to the regulatory response to the COVID-19 pandemic.
Annual trends in the number of FDA-approved drugs by therapeutic class between 2015 and 2024.
Temporal trends of expedited designations by indication are provided in Fig. 2. Use of expedited mechanisms between 2015 and 2024 demonstrated an upward trend, along with ongoing imbalances in approvals for infectious and non-infectious diseases (Fig. 2; Supplementary Figure S2; Table S3). Moving towards Priority Review, median annual designation rates for products developed against infectious diseases were 92% (IQR 83–100%), compared with 60% (IQR 55–68%) for products developed against non-infectious diseases (Wilcoxon rank-sum p < 0.001). In Fast Track, median values reflected 75% (IQR 50–100%) of approvals for infectious diseases, compared with 35% (30–40%) for non-infectious diseases (p < 0.001). In Breakthrough Therapies, no statistical difference was present—35% (15–50%) of infectious products vs 30% (25–40%) of non-infectious products (p = 0.18)—notwithstanding increased variability recorded annually across infectious agents. Accelerated Approval was most underused among infectious products, with a median rate of 5% (IQR 0–10%), compared with 20% (15–25%) for non-infectious products (p = 0.002). Over time, Priority Review of infectious products increased from 75% in 2015 to 100% in 2019, prior to the pandemic. This high utilization was maintained during the pandemic (2020–2022) before normalizing in 2023–2024 (Fig. 2). Fast Track reached its maximum at 100% in 2019 and 2022; Breakthrough Therapies reached 65% in 2020; and Accelerated Approval never exceeded 15% in any given year.
Temporal trends in the proportion of drugs receiving expedited FDA designations, stratified by infectious diseases versus non-infectious diseases.
Regulatory timelines comparisons
A comparative analysis of the timelines surrounding regulatory procedures showed that there was no considerable difference in median development and approval times for infectious versus non-infectious treatments; however, time-to-event analyses revealed faster movement for infectious products (Fig. 3; Table 1; Supplementary Figure S3; Table S4). The reported CDT was 2.76 years (IQR 1.80–4.25) compared to 3.46 years (IQR 2.59–4.66) for non-infectious drugs (Kruskal–Wallis p = 0.003). The RAT, the period from submission to approval, had a median of 243 days (IQR 232–300) for infectious treatments, compared with 331 days (IQR 238–366) for non-infectious treatments (p = 0.008). Additionally, the median RRT was 3.54 years (IQR 2.58–5.03) for infectious treatments and 4.22 years (IQR 3.24–5.73) for non-infectious treatments (p = 0.006).
Kaplan–Meier survival curves comparing infectious and non-infectious diseases across three time-to-event outcomes: CDT, RAT, and RRT.
Confirming the median values comparison, Kaplan–Meier analyses indicated a significantly accelerated progression through CDT (log-rank p = 0.012), RAT (p = 0.0018), and overall RRT (p = 0.0073) for infectious disease-related products. In the multivariable Cox proportional hazards model for RRT (Supplementary Table S1), therapies for infectious disease showed a significantly higher hazard of receiving approval (HR = 1.58; 95% CI 1.15–2.16; p = 0.0047), representing a 58% higher probability of achieving the endpoint at any given time compared to non-infectious drugs. Two Cox models were constructed to analyze time to regulatory approval. In the main-effects model (Supplementary Table S1), therapies for infectious disease showed a significantly higher hazard of approval (HR = 1.58; 95% CI 1.15–2.16; p = 0.0047). In a separate interaction-adjusted model (Table 2) that included infectious × pathway interaction terms, the HR was higher (HR = 2.98; 95% CI 1.30–6.80; p = 0.0096), suggesting potential amplification effects across specific expedited programs. In addition, Breakthrough Therapy designation was associated with a faster RRT independently (HR = 1.41; 95% CI 1.11–1.78; p = 0.0041). An interaction term with Accelerated Approval suggested a reduced effect of infectious disease therapies (HR for infectious × Accelerated Approval = 0.49; 95% CI 0.20–1.19; p = 0.115), though the result did not attain statistical significance. These results are visually summarized in Fig. 4, which presents a forest plot of the hazard ratios from the interaction-adjusted Cox regression model. Subgroup analysis post-2020 showed a 15% reduction in RAT for infectious disease-related target products during the COVID-19 pandemic (p = 0.032).
Forest plot showing hazard ratios from Cox regression with interaction terms (e.g., infectious × accelerated approval).
Predictive modeling of expedited program designation
To better identify the predictors underlying the FDA’s expedited pathway designations, we employed two complementary approaches: multivariable logistic regression and a Random Forest classifier. The variables included in the models included indication (infectious vs. non-infectious), orphan designation, trial phase, and endpoint classification. As shown in Table 3, infectious disease indication was the best predictor of Priority Review (adjusted odds ratio [aOR] = 10.69; 95% CI 5.4–27.3; p < 0.0001), followed in turn by orphan designation (aOR = 3.7; 95% CI 2.1–6.5; p < 0.0001) and surrogate endpoints (aOR = 1.9; 95% CI 1.1–3.2; p = 0.02). Fast Track designation was associated with infectious indications (aOR = 4.49; 95% CI 2.8–9.6; p < 0.0001) and Phase II/III trials (aOR = 2.3; 95% CI 1.4–3.8; p = 0.001) and yielded an area under the curve (AUC) of 0.81. Breakthrough Therapy designation was affected by surrogate endpoints (aOR = 2.5; 95% CI 1.6–3.9; p = 0.0002) and orphan designation status (aOR = 2.2; 95% CI 1.3–3.7; p = 0.003). While Accelerated Approval revealed an inverse association for the infectious indication (aOR = 0.12; 95% CI 0.03–0.66; p = 0.013), it showed a significant positive association with surrogate endpoints (aOR = 4.7; 95% CI 2.3–9.6; p < 0.0001). All models had excellent discrimination (AUCs between 0.79 and 0.85) and good calibration (Hosmer–Lemeshow p > 0.10).
We further optimized a Random Forest classifier using trial-level features, namely infectious status, orphan designation (frequency of 51.1%), trial phase (mean of 2.8 ± 0.6), enrolment size (median of 342; inter-quartile range of 161–605), and approval year (mean of 2019.7 ± 2.9), using an 80:20 train: test ratio (n = 371/93) with 500 trees. Optimized performance was 75.6% accurate (95% CI 65.4–84.0%; p = 0.0028 relative to no-information rate of 61.1%), with an area under the curve (AUC) of 0.794, 71.4% sensitivity, 78.2% specificity, balanced accuracy of 74.8%, and Cohen’s Kappa of 0.491. Permutation importance testing revealed a higher effect of orphan status (mean Gini decrease = 28.4), followed by infectious status (22.7), trial phase (15.2), enrolment size (9.8), and approval year (4.1; Supplementary Figure S9).
Subgroup and sensitivity analyses
Subgroup analyses revealed differences in trial duration and enrollment size by application type, orphan designation, review pathway, and trial phase. For example, BLAs had longer trial durations and smaller enrollment than NDAs, and Priority Review was consistently associated with faster regulatory timelines. Sensitivity analyses confirmed the robustness of findings after excluding COVID-related products and statistical outliers. Full results and subgroup comparisons are provided in Supplementary Results and Supplementary Tables S6 and S7.
Discussion
The 10-year analysis of 464 FDA approvals reveals program-specific regulatory alignment that reflects underlying scientific and clinical characteristics of infectious versus non-infectious diseases. One key finding is the variation in the utilization of expedited programs. This variation, which is not a sign of neglect but rather a reflection of the FDA’s adaptability to different disease contexts, underscores the importance of context-specific regulatory strategies. These findings are further supported by our regression models, which demonstrate that Fast Track and Priority Review are preferentially applied to infectious disease products addressing urgent public health needs.
Our time-to-event analyses and median-based analyses demonstrate significantly shorter CDT, RAT, and RRT for infectious diseases compared with non-infectious treatments (all p-values < 0.01). This observation highlights an advantage for infectious disease treatments. Infectious disease treatments exhibit significantly higher odds of receiving Fast Track (OR = 4.49) and Priority Review (OR = 10.69) designations, but are less frequently utilized for Breakthrough Therapy (OR = 0.42) and Accelerated Approval (OR = 0.12). These patterns suggest strong support for expedited programs, despite persistent program-specific imbalances across several therapeutic arenas. Such a differential approach to regulation demonstrates a system for selectively prioritizing responses to infectious threats through specific programs, but not through other available incentives.
The current results confirm and extend those of prior literature. In agreement with studies from Hwang et al.15, We conclude that clinical trials of infectious diseases feature shorter study periods and lower participant enrollments. However, where prior studies may have identified this as an inequality in program application11, our findings reframe this as a logical, context-dependent alignment. Whereas prior studies of review timelines showed a clearing of around 20% of review time following the FDA Safety and Innovation Act (FDASIA) provision enactment, our study finds a 15% fall of RAT for infectious products after 2020, a trend likely aggravated by countermeasures taken during the COVID-19 pandemic, consistent with prior trends.23. This observation further highlights contextual determinants of regulatory efficiency. In addition, this trend aligns with our broader finding that infectious disease treatments had significantly shorter RATs overall. This shorter review time results from two factors working in concert: it is influenced by the intrinsic nature of ID trials (e.g., more focused data packages from shorter, acute-disease studies), and it is also formally codified by explicit regulatory policy via the high utilization of Priority Review (88% vs 58%). This designation explicitly commits the FDA to an accelerated review clock. Therefore, the shorter RAT results from both intrinsic trial properties and explicit regulatory policy working in alignment.
Crucially, our use of Kaplan–Meier tests combined with Cox regression models reinforces the trend observed in median comparisons, offering additional support for the robustness of the observed differnces. These findings suggest that, despite the apparent congruence of median timelines, infectious disease therapies gain an advantage from accelerated regulatory processes when their data are analyzed using time-dependent strategies. By combining regression methods, time-to-event analyses, and machine learning procedures, our study goes beyond descriptive benchmarking and proposes a rich, program-specific analysis of regulatory practice. These results support the contention that orphan and infectious designations have a primary influence on expedited pathway designation and illustrate the utility of machine learning methods for regulatory prioritization in antimicrobial resistance. These differential patterns likely reflect inherent differences in disease course and outcome measurability rather than lapses in regulatory attention.
The program-specific differences demand a mechanistic approach. The deliberate targeting of therapeutics to specific delivery for infectious diseases is evident in the Priority Review and Fast Track programs, which demonstrate a conscious approach to addressing antimicrobial resistance and other public health threats. In contrast, the applicability of the Accelerated Approval and Breakthrough Therapy programs in infectious disease development is inherently limited. Most infectious diseases feature short, clearly defined clinical endpoints, such as pathogen clearance or survival, which reduces the necessity for surrogate endpoints or long-term efficacy markers that typically support Accelerated Approval. Similarly, the Breakthrough Therapy designation requires demonstrating substantial improvements over existing therapies, which can be challenging in areas where established standards of care are already in place. In this context, the relatively low frequency of these designations for infectious products (OR = 0.12 for Accelerated Approval; OR = 0.42 for Breakthrough Therapy) reflects a careful scientific alignment rather than a lapse in regulatory practices.
Limitations
Our study has several limitations. First, using multiple public data repositories may lead to timeline inconsistencies, though we unified metrics using the pivotal trial’s IND effective date. Second, this study analyzes only successfully approved products, which introduces an approval bias by excluding applications that were withdrawn or rejected. Third, the significant cohort imbalance (N = 406 vs. N = 51) limits statistical power, widening confidence intervals and potentially underpowering our models to detect complex interaction effects. Fourth, confounding by therapeutic area (e.g., acute vs. chronic endpoints) was not fully adjusted for in all models. Furthermore, our models do not account for key omitted variables, such as sponsor type or the underlying economic incentives for a given drug. Our data also reflects the final outcome of a designation and cannot differentiate between sponsor-driven requests and the FDA’s regulatory judgment on those requests, which is a significant confounder. Lastly, no formal multiple-testing correction (e.g., Bonferroni) was applied in this study due to its exploratory nature; therefore, results were interpreted conservatively. These findings pertain solely to the U.S. FDA and may not generalize to other agencies. Finally, the inclusion of the 2020–2022 pandemic period is a limitation; however, a sensitivity analysis excluding all pandemic-related approvals confirmed our primary conclusions remained robust.
Conclusion
In conclusion, the overall review of the FDA approval process for anti-infective treatments reveals a system of rational, program-specific alignment that effectively accelerates treatment approvals. The less frequent utilization of Breakthrough and Accelerated Approval pathways is not a sign of regulatory neglect but a logical consequence of the scientific realities of acute infectious diseases, which often have definitive clinical endpoints, making surrogate-based pathways less applicable. The primary barrier undermining future innovation is therefore not regulatory misalignment, but the limited economic incentives for anti-infective development.
To address this, the key is to deploy economic “pull” mechanisms, such as subscription payments proposed in the PASTEUR Act, to decouple revenue from sales volume, thus incentivizing research and development spending.
In parallel, policies may mandate and incentivize adaptive, platform-approach trial designs that leverage the inherent efficiencies of shorter, smaller infectious disease trials. Furthermore, policies should also create streamlined pathways to rapidly validate and approve repurposed drugs, which remains a key strategy for expanding the anti-infective pipeline. Key, too, is to deploy economic “pull” mechanisms, such as subscription payments proposed in the PASTEUR Act24, to decouple revenue from sales volume, thus incentivizing research and development spending.
Further, integrating machine learning-based predictive models into regulatory designs could enable early identification of frequently neglected candidates. Harmonizing expedited pathway criteria internationally, in addition to enhancing real-world surveillance, is critical to align regulatory timelines with long-term safety and efficacy considerations. Future studies should leverage disclosures under the Freedom of Information Act and conduct cross-agency comparisons to evaluate these reforms and track their impact on the global anti-infective pipeline through the year 2030 and beyond.
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author, Ahmed M. Sayed (soliman1@purdue.edu), upon reasonable request.
References
Khan, M. et al. COVID-19: A global challenge with old history, epidemiology and progress so far. Molecules 26(1), 39 (2020).
Sharma, S. et al. Exploring the COVID-19 journey and cutting-edge biosensing approaches. In Functionalized Nanomaterials for Biosensing and Bioelectronics Applications 173–187 (Elsevier, 2024).
Gayathri, R., Vijayabanu, C. & Theresa, C. Economic disruption and global obscurity-insights and challenges. In Economic Uncertainty in the Post-Pandemic Era 1–26 (Routledge, 2024).
Fong, I. Antimicrobial resistance: A crisis in the making. In New Antimicrobials: For the Present and the Future, 1–21 (2023).
Alara, J. A. & Alara, O. R. An overview of the global alarming increase of multiple drug resistant: A major challenge in clinical diagnosis. Infect. Disord. Drug Targets Disord. 24(3), 26–42 (2024).
Miller, K. L., Fermaglich, L. J. & Maynard, J. Using four decades of FDA orphan drug designations to describe trends in rare disease drug development: Substantial growth seen in development of drugs for rare oncologic, neurologic, and pediatric-onset diseases. Orphanet J. Rare Dis. 16(1), 265 (2021).
Aloni-Grinstein, R., Mamroud, E. & Gal, Y. New frontiers for old medications: Repurposing approved drugs against gram-negative bacterial infections. Microorganisms 13(9), 2115 (2025).
Jean, S.-S. et al. Off-label use versus formal recommendations of conventional and novel antibiotics for the treatment of infections caused by multidrug-resistant bacteria. Int. J. Antimicrob. Agents 61(5), 106763 (2023).
Jae, V. S. Simplifying FDASIA: The fast track to expedited drug approval efficiency. Admin. L. Rev. 66, 173 (2014).
Hu, R., et al., New drugs approved by European medicines agency during 2024. Eur. J. Med. Chem. 294 117761,ISSN 0223-5234, https://doi.org/10.1016/j.ejmech.2025.117761 (2025).
Batta, A., Kalra, B. S. & Khirasaria, R. Trends in FDA drug approvals over last 2 decades: An observational study. J. Fam. Med. Primary Care 9(1), 105–114 (2020).
Brown, E. D. & Wright, G. D. Antibacterial drug discovery in the resistance era. Nature 529(7586), 336–343 (2016).
Kesselheim, A. & Darrow, J. FDA designations for therapeutics and their impact on drug development and regulatory review outcomes. Clin. Pharmacol. Ther. 97(1), 29–36 (2015).
Klein, K. et al. Regulatory flexibilities and guidances for addressing the challenges of COVID-19 in the EU: What can we learn from company experiences?. Therap. Innov. Regul. Sci. 56(2), 366–377 (2022).
Hwang, T. J., Darrow, J. J. & Kesselheim, A. S. The FDA’s expedited programs and clinical development times for novel therapeutics, 2012–2016. JAMA 318(21), 2137–2138 (2017).
Sacks, L. V. et al. Scientific and regulatory reasons for delay and denial of FDA approval of initial applications for new drugs, 2000–2012. JAMA 311(4), 378–384 (2014).
Administration, U.S.F.a.D. Drugs@FDA: FDA-Approved Drugs. 2023 April 14, 2025]. http://www.accessdata.fda.gov/scripts/cder/daf/index.cfm.
Administration, N.A.a.R. Federal Register. 2023 April 14, 2025]. http://www.federalregister.gov/.
Medicine, U.S.N.L.o. ClinicalTrials.gov. 2023 April 14, 2025]. http://clinicaltrials.gov/.
Benítez-Parejo, N., del Águila, M. R. & Pérez-Vicente, S. Survival analysis and Cox regression. Allergol. Immunopathol. 39(6), 362–373 (2011).
Rich, J. T. et al. A practical guide to understanding Kaplan-Meier curves. Otolaryngol. Head Neck Surg. 143(3), 331–336 (2010).
Chaudhary, A., Kolhe, S. & Kamal, R. An improved random forest classifier for multi-class classification. Inf. Process. Agric. 3(4), 215–222 (2016).
DiMasi, J. A. et al. Development times and approval success rates for drugs to treat infectious diseases. Clin. Pharmacol. Ther. 107(2), 324–332 (2020).
Bennet, U. S. M. & Young, T. The PASTEUR Act. (Reference Source, 2020).
Acknowledgements
Grammarly was used to refine and correct some of the writing in this version of the manuscript.
Funding
This work was supported by the Shenzhen Basic Research Program (JCYJ20241202124859016). Data were retrieved from publicly available FDA and clinical trial databases.
Author information
Authors and Affiliations
Contributions
NTT and AMS conceptualized the study and designed the research framework. AMS, NTT, and MND performed data analysis and statistical modeling. MND, RE, and JMAA contributed to data verification, collection, and curation. AG, TTHN, PT, and ZZ contributed to drafting, revising, and refining the manuscript. AMS also coordinated collaboration between co-authors and led the manuscript preparation. NO and NTH provided critical scientific feedback and supervised the entire project. All authors reviewed and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Tam, N.T., Sayed, A.M., Dadam, M.N. et al. Regulatory alignment in FDA expedited pathways for infectious diseases: a decadal review with predictive modeling insights. Sci Rep 16, 860 (2026). https://doi.org/10.1038/s41598-025-30452-0
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-30452-0