Abstract
With the rising prevalence of mental health issues, depression not only causes significant psychological distress and severely impairs social functioning and quality of life but also heightens the risk of suicide. The Depression Change Expectation Scale (DCES) is an assessment tool designed to evaluate the attitudes of individuals exhibiting depressive tendencies or symptoms regarding their anticipated future changes in depression. Understanding adolescents’ expectations about changes in depression can enable timely and targeted interventions before their mental health deteriorates. However, a Chinese version of the DCES is yet to be developed. This study aimed to translate the DCES, cross-cultural adaptation, and validate the Chinese version of the DCES among college students. Following the Brislin translation model, the initial draft of the DCES was translated and back-translated. The Chinese version was refined through expert localization and a preliminary survey. Using a convenience sampling method, 1,138 students from various universities in Anhui province were surveyed from September to December 2023. Among these, 481 students exhibiting depressive symptoms and tendencies, as identified by the Beck Depression Inventory, were selected for the reliability and validity analysis of the Chinese version of the DCES. The Chinese version of the DCES demonstrated a robust two-factor model fit (Chi-square/degrees of freedom = 2.604; comparative fit index = 0.973; Tucker–Lewis index = 0.970; goodness of fit index = 0.912; normed fit index = 0.958; root mean square error of approximation = 0.058). The scale-level content validity index was 0.898, and item-level content validity indices ranged from 0.830 to 1.000. The internal consistency, as measured by Cronbach’s alpha, was 0.910 for the entire scale and ranged from 0.888 to 0.980 for individual dimensions. The test-retest reliability was 0.985 for the total scale, with individual dimensions’ test-retest reliability ranging from 0.982 to 0.985. This study, supported by previous evidence, indicates that the Chinese version of the DCES possesses excellent validity and reliability. It is a valuable tool for measuring expectations regarding changes in depression and has the potential to predict future trends in depressive symptoms.
Similar content being viewed by others
According to the World Health Organization, approximately 1 billion people worldwide suffer from mental disorders, with around 95 million individuals in China experiencing depressive disorders. The global burden of mental health issues has intensified following the COVID-19 pandemic, with cases of major depression and anxiety disorders increasing by 28% and 26%, respectively. The number of people suffering from depression surged by 53 million, marking a 27.6% increase1. Cross-cultural studies have consistently shown that depression, characterized by pervasive negative emotional experiences, is a prevalent mood disorder among adolescents2,3, with a particularly high prevalence among college students4.
College students are in a critical transitional stage, facing significant academic pressures and the additional stress of entering the workforce5. Compared with their junior and senior high school years, the rhythm of college life changes significantly. Besides managing daily classes, students must navigate more complex interpersonal relationships and handle responsibilities independently, which can easily lead to depressive moods6. Research indicates that college students have a high incidence of depressive symptoms7,8. For example, a 2015 survey conducted at a university in the United States found that 33% of college students experienced depressive moods9. A meta-analysis of the prevalence of depressive moods among Chinese college students revealed a combined detection rate of 29.3%, with rates of 27.4% for boys and 21.6% for girls10. These findings underscore the severity of depressive symptoms in the college student population and highlight the urgent need for addressing their mental health needs.
Depression expectation involves an individual’s anticipations and attitudes regarding their future while grappling with depressive symptoms. Research by Chin et al.11 in Singapore’s primary healthcare sector highlights that the severity of depressive symptoms and specific aspects of disease perception—such as views on chronic illness, personal control, and treatment efficacy—are crucial predictors of positive treatment outcomes. This suggests that patients’ beliefs about their treatment outcomes significantly influence their effectiveness. Eddington et al.12 discovered that optimistic expectations are linked with a greater focus on goal achievement, enhanced engagement with personal objectives, and more significant progress in key life areas. This indicates that changes in expectations are closely related to positive daily experiences and goal pursuit. Moreover, a 2014 evaluation of the DCES’s reliability and validity revealed a strong connection between positive expectations and improvement in depressive symptoms, whereas pessimistic expectations did not show a similar relationship13. Fundamental cognitive features of depression, such as hopelessness, negative self-views, and an external locus of control, often lead individuals to start therapy with low expectations for change14. These negative anticipations, coupled with the motivational deficits characteristic of depression, can result in premature treatment discontinuation—a significant issue15. Hence, it is vital to assess patients’ expectations before initiating treatment. For college students experiencing depressive symptoms, evaluating their expectations using the DCES is crucial for addressing pessimistic views promptly. Understanding change expectations quickly is essential for applying effective supplementary therapies16.
Effective assessment of change expectations often necessitates focusing on the symptomatic domains of the intervention17. However, in China, there has been limited attention to this due to a lack of targeted tools for accurately assessing change expectations in the psychological realm. Given the high comorbidity between depression and anxiety and their shared risk factors, the Anxiety Change Expectancy Scale (ACES) developed by Dozois and Westra (2005)18 offers valuable insights. Their research demonstrated reported internal consistency and validity in clinical and non-clinical samples19,20 and showed that higher scores on the ACES—indicating more optimistic change expectations—were associated with a faster response to cognitive behavioral therapy in patients with anxiety disorders21. In 2014, Professor Kari M. Eddington and colleagues at the University of North Carolina modified the ACES to create the DCES13. Many of the core concepts covered in the ACES apply to both disorders. However, not all subject areas pertinent to individuals with depression were sufficiently covered by the original scale. Specifically, the measure lacked items assessing expectations about the effectiveness of behavioral activation techniques and participation in enjoyable activities22. To enhance content validity, two items focusing on these areas were introduced, given that behavioral engagement is a crucial intervention strategy linked to expected symptom improvement. Motivational deficits and anhedonia are fundamental characteristics of clinical depression. Consequently, two ACES items related to exposure were removed as they were not relevant to depression. Additionally, items were reworded to focus on expectancies regarding mood control and depression.
Currently, researchers in Singapore have employed a cross-sectional study design to recruit adult patients with depression in primary care settings11. These studies applied regression analysis to determine that symptom severity and specific dimensions of disease perception are significant predictors of positive treatment expectations. In the United States, Kari M. Eddington and colleagues conducted a six-week follow-up study involving 416 depressed college students and 63 adults12. They evaluated the internal consistency of the scale using Cronbach’s alpha and investigated the factor structure of the DCES through principal axis factoring and oblique rotation. Although factor structure models are effective for analyzing complex interactions among multiple factors, their complexity and verification challenges can be limitations23. In the present study, a two-factor model was used to validate the DCES, differentiating between optimistic items (DCES-O) and pessimistic items (DCES-P). This model elucidates two distinct dimensions of expectations regarding treatment outcomes in patients with depression, leading to a more nuanced understanding. According to expectation theory, individuals’ behavior and motivation are influenced by their anticipated outcomes. Positive expectations can trigger beneficial changes, and the DCES aims to forecast changes in mood and behavior by assessing cognitive expectations of improvement in depressive symptoms13. Reflecting the two-factor model and expectation theory, the Chinese version of the DCES encompasses beliefs and expectations related to the enhancement of depressive symptoms, treatment efficacy, self-help strategies, emotional regulation, and involvement in enjoyable activities.
Materials and methods
Study design
In this study, the first draft of DCES was translated according to the Brislin translation model24, and the Chinese version of DCES was formed through expert localization debugging and pre-survey. Then, the cross-sectional survey was used to answer the online questionnaire for college students to understand the depression of college students, select college students with depression tendencies, and continue to answer the Chinese version of DCES to analyze the reliability and effectiveness of DCES in this study.
Scale translation and cross-cultural adaptation
To respect the intellectual property rights of the original scale, we first obtained authorization from the original author before using the DCES13. This study involved localizing the Chinese version of the DCES using the Brislin model24, as illustrated in the following.
-
1.
Translation: The original scale was translated into Chinese by two fluent English speakers: a nursing master’s graduate with an International English Language Testing System score of 6 and an English instructor with a master’s degree in English and a professional English level 8. These translations resulted in two versions, A1 and A2.
-
2.
Integration: After comparing and discussing the two initial translations, a seasoned Ph.D. in psychology collaborated with the research team to produce a revised version, A3.
-
3.
Back-translation: Two psychology specialists performed the back-translation of A3 into English. One specialist held a Ph.D. in psychology with 7 years of teaching experience, while the other was a senior psychological counselor with 39 years of clinical experience. Neither specialist had seen the original scale. Their translations were labeled B1 and B2.
Once the back-translations were completed, the entire research team, along with members of a participating expert group, reviewed any discrepancies. A consensus was reached to implement the necessary changes. The original author was consulted to address inconsistencies, and their feedback guided the revisions. The final version, C, in Chinese, was established through this collaborative process.
Expert consultation for the Chinese version C of the DCES involved specialists in clinical psychology, psychoeducation, clinical nursing, and scale development. The expert panel comprised two clinical psychologists, one psychoeducation specialist, one clinical nursing expert, and one scale development expert. Collectively, these experts had an average of 21.50 ± 11.84 years of professional experience, with three having bachelor’s degrees, two having master’s degrees, and 1 having a doctorate. Of these, two held deputy senior professional titles, and three had intermediate professional titles.
Experts evaluated the scale using a 4-point grading system: “1” for irrelevant, “2” for weakly relevant, “3” for strongly relevant, and “4” for very relevant. The assessment considered textual clarity, language expression, item-dimension linkage, and the necessity of any additions or deletions. Based on their professional input, adjustments were made to the scale. Whether to enter the pre-survey was decided after the semantic equivalence of the study group.
In September 2023, a preliminary survey was conducted with 30 students from a medical school in Anhui Province to assess anticipated changes in depression. The purpose and significance of the study were explained to the participants before they began filling out the questionnaire. They were guided and assisted throughout the process, receiving clarifications and advice on the questions. After completing the questionnaire, their responses were recorded, and feedback on the scale was collected. This feedback was used to revise and refine the scale, resulting in Chinese version D.Scale translation and cross-cultural adaptation is shown in Fig. 1.
Structural equation model.
Sample size
Based on the recommendation of the consistency factor analysis (CFA)25,26 for psychometric measures, namely with 10 to 20 samples for each item, We estimated that this study requires 400 college students with depressive symptoms or tendencies. At the same time, based on the prevalence of depression among college students27, We need to investigate at least 1097 college students.
Sampling and procedures
Convenience sampling and an electronic questionnaire were used to survey participants. Data were collected through the platform (https://www.wjx.cn/) from September to December 2023. A total of 1,138 students from various schools in Anhui Province participated in the survey. After the survey, questionnaires with a completion time of less than 90 s and those with regular responses were excluded from the analysis. Messages were sent several times a week by Zhangjing, one of the authors who is a professor in the faculty to other universities, encouraging them to remind their groups to participate in the survey. Additionally, in survey two, a column was added for participants willing to provide their email for re-test purposes to facilitate test-retest reliability. To assess test-retest reliability, a follow-up survey was conducted 2 weeks after the initial survey. The test-retest interval ranged from 2 weeks to 1 month28.
Before filling in the questionnaire, the applicant will answer the questionnaire voluntarily according to the qualified criteria.
Survey One: Inclusion criteria: (1) Age ≥ 18 years; (2) Full-time undergraduate students registered in school; (3) Informed consent and voluntary participation in the study. Exclusion criteria: (1) Those with severe mental illnesses, such as schizophrenia; (2) Those with other life-threatening major illnesses.
Survey Two: For students who completed Survey One and had a score of ≥ 4 on the Beck Depression Inventory, their questionnaire was then linked to the Chinese version of the DCES questionnaire for further completion. Thus, data were collected through a platform from 481 university students in Anhui Province with depressive symptoms or tendencies.
Instruments
Basic information questionnaire:
This questionnaire collected data on the student number, age, sex, and family background of the respondents.
Chinese version of the BDI
The BDI, originally introduced by American psychologist Aaron T. Beck in 1974, was adopted by Chinese scholars29. It includes 13 items with the following scoring ranges: 0–4 points for no depressive symptoms, 5–7 points for mild depressive symptoms, 8–15 points for moderate depressive symptoms, and 16–39 points for major depressive symptoms. This study used this scale to identify students with depressive symptoms or tendencies scoring above 4 points. its Cronbach’s α was 0.83 in this study.
Chinese version of the DCES
The Chinese version of the DCES, which includes 20 items, was developed through localization by the research team. It measures both positive and negative expectations of depression change, with each item rated on a Likert scale from 1 (strongly disagree) to 5 (strongly agree). The total score ranges from 20 to 100 points. The positive change expectation dimension uses reverse scoring, so a higher score indicates more negative expectations regarding changes in depression. Its Cronbach’s α was 0.91 in this study.
Statistical analysis
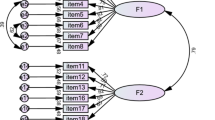
IBM SPSS 25.0 was used to perform statistical analyses, including Cronbach’s alpha for internal consistency and test-retest reliability to evaluate reliability. Confirmatory Factor Analysis (CFA)30 was then conducted using the AMOS 24 software. The empirical strategy included 3 parts. First, descriptive analyses were used to assess the statistical values of the variables that measured the characteristics of the general information. Continuous variables were presented as mean and SD, and categorical variables as numbers and percentages. Second, to examine the reliability of the Chinese version of DCES Cronbach’s alpha was calculated to indicate the internal consistency reliability, where Cronbach’s alpha > 0.70 was considered satisfactory31,32, To ensure the robustness of the scale, items with a reliability coefficient below the acceptable threshold or an item-total correlation coefficient below 0.3 33 were scrutinized and adjusted if necessary. Third, Path analysis was performed using AMOS 24.0 to verify the theoretical structure of the two-factor model, as depicted in Fig. 2. AMOS utilized the maximum likelihood method to estimate the model parameters, providing statistics such as standardized estimates, multivariate correlation R-squared, implied and sample covariance matrices, covariance, and correlation coefficients33. Model fit was evaluated using the following criteria34: root mean square error of approximation < 0.1, normed fit index > 0.8, comparative fit index > 0.8, goodness of fit index > 0.8, and Chi-square/degrees of freedom < 3.
Structural equation model based on two-factor theory.
Results
The Chinese version of DCES was adapted to address cultural differences and feedback from the pre-survey. The modifications are detailed below:
-
1.
Item adjustments for cultural relevance: Certain expressions were revised to better align with Chinese language norms. For example:
-
Item 12 was modified from“Even when I try to talk positively to myself, it doesn’t help me feel better” to “Even if I try to actively talk to myself, I don’t feel better.”
-
Item 4 was changed from “I have had some positive experiences with being able to control my mood by talking positively to myself” to “I have had some success in controlling my emotions by actively talking to myself.”
-
Item 5 was revised from “My depression is too severe to benefit from treatment” to “My depressive symptoms are severe, and the treatment is not effective.”
-
2.
Modification of Statements: Some statements were adjusted for clarity:
-
Item 19 was changed from “If I work hard, I can have a positive impact on my problems with depression” to “Hard work/study has had a positive impact on my depressive issues.” and incorporating feedback from the pre-survey, no items were removed, and the order of items remained consistent with the original scale.
Following these adjustments to fit Chinese linguistic norms and incorporating feedback from the pre-survey, no items were removed, and the order of items remained consistent with the original scale.
General information
The demographic data collected from the questionnaires revealed the following:
-
The sample comprised approximately three times as many females as male students in college schools.
-
A small proportion of participants were only children.
-
The majority of respondents reported having a favorable family environment.
(Table 1 provides a detailed breakdown of these demographic characteristics.)
Internal consistency analysis of the Chinese version of DCES
The internal consistency analysis of the Chinese version of the DCES was assessed using Cronbach’s α coefficient, which was found to be 0.910. This indicates strong overall reliability. Each dimension of the scale also demonstrated high reliability, with coefficients ranging from 0.888 to 0.980. Additionally, a test-retest reliability assessment, conducted with 30 cases 2 weeks later, showed high consistency, with reliability coefficients ranging from 0.982 to 0.985. These results underscore the scale’s robust temporal stability. Detailed reliability results are presented in Table 2.
Content validity of the Chinese version of DCES
Content validity was evaluated using the CVI, which includes item-level CVI and scale-level CVI. Six experts assessed the content validity, considering semantic, equivalence, idiomatic, experience, and conceptual aspects. The item-level CVI ranged from 0.830 to 1.00, and the scale-level CVI was 0.898, with all values exceeding 0.7. These results indicate that the Chinese version of the DCES has strong content validity31.
Pearson correlation analysis of the Chinese version of DCES
Pearson correlation analysis was conducted to examine the relationships among dimensions of the DCES. The correlation coefficients among dimensions ranged from 0.982 to 0.985, indicating a high degree of correlation. Each dimension showed weak to moderate correlations with the others, but all dimensions exhibited a strong correlation with the overall questionnaire. The correlation coefficient between the Chinese version of the BDI and the Chinese version of the DCES was 0.414, reflecting a moderate relationship.
Confirmatory factor analysis of the Chinese version of DCES
Confirmatory factor analysis using AMOS demonstrated a good fit for the model, as depicted in Fig. 2. The model fitting indices are detailed in Table 3, confirming that the factor structure of the DCES aligns well with the theoretical framework.
Discussion
This study aimed to address the gap in Chinese research by cross-cultural adaptation and we validated the DCES among Chinese college students in the early stages of depression. The test-retest reliability, a crucial measure of the scale’s consistency, was above 0.6 in both surveys, suggesting that the DCES version is reliable32. Confirmatory factor analysis results indicated that nearly all items had loadings above 0.4 on their respective factors, and the model fit indices were acceptable (see Table 2), supporting the structural validity of the scale.
Compared with previous studies, the internal consistency of the DCES in this study differs from the original scale developed by Eddington KM in 201413. Several factors may contribute to these differences35,36: (1). Personality Differences: Chinese respondents may exhibit more neutral response tendencies, while Americans may show more individualistic preferences. (2) Timing: The survey was administered to students shortly after their enrollment, a period potentially influenced by psychological adjustments post-holidays. (3) Cultural and Environmental Factors: Variations may arise from differences in social roles and academic environments between the two populations.
Given the increasing attention to mental health promotion, especially regarding depression37, understanding how negative expectations during treatment can lead to adverse effects is crucial16,38. Addressing mental health issues requires a reliable, objective basis for self-evaluation to mitigate potential risks and errors. Therefore, it is necessary to scientifically and effectively measure changes in expectations of depression. Hence, this study aims to localize the scale for measuring changes in expectations of depression. This study focuses on cross-cultural adaptation, testing the reliability, and validating a scale for measuring in depression change expectations, with the goal of future clinical application. Insights into change expectations can help clinicians gauge individuals’ readiness for action-oriented strategies, such as cognitive therapy, or identify the need for interventions like motivational interviews39.
The DCES has the potential to significantly contribute to the treatment process by providing a deeper understanding of patients’ change expectations. This can enhance adherence to therapeutic homework, improve therapist effectiveness, and facilitate dynamic interactions within multidisciplinary treatment teams. Using reliable and effective assessment tools such as the DCES, medical professionals can enhance early assessment, anticipate patient needs, and implement timely interventions to improve patient care40. This study meticulously translated the DCES into Chinese using the Brislin translation model, ensuring cultural relevance through expert review and adjustments based on pre-survey feedback. The Chinese version of the DCES, like the original, contains two dimensions and twenty items based on the two-factor theory model. Its features clear, concise items and a straightforward scoring system, allowing completion in just 3–5 min. This design demonstrates both practicality and ease of use.
Nevertheless, the study has limitations. First, the survey was conducted exclusively in selected universities in Anhui Province due to resource constraints, which may not completely represent the diverse regional economic backgrounds and university environments across China, potentially introducing sample bias. Second, for the college students with depression status in this study, we did not ask about their treatment status or about medical illness and mental illness in the family, which might affect their change expectations. Third, because predictive research requires a longer time span, this study has not yet conducted predictive validity testing.
Conclusion
The Chinese version of the DCES, consisting of 20 items across two categories, exhibits strong reliability and validity. It is a valuable tool for psychiatrists, psychological counselors, psychotherapists, and social workers to assess changes in patients’ expectations regarding psychological depression. Nonetheless, the study’s representativeness is limited by its focus on college students, which may impact the generalizability of the findings. In the future, we plan to further conduct predictive validity testing and hope to expand the application population, applying this scale to clinical depression patients.
Data availability
The datasets generated and/or analyzed during the current study are not publicly available due to the private information collected but are available from the corresponding authors at reasonable request.
Abbreviations
- CVI:
-
Content Validity Index
- S-CVI:
-
Scale-level CVI
- I-CVI:
-
Item-level CVI
- CFI:
-
Comparative fit index
- GFI:
-
Goodness-of-fit index
- NFI:
-
Normed fit index
- DCES:
-
Depression Change Expectancy Scale
- RMSEA:
-
Root-mean-square errors of approximation
- TLI:
-
Tucker-Lewis index
References
The 2022 National Mental Health Survey Report. Current Status, Impact Factors, and Service Status. (2023). http://psy.china.com.cn/node_1013711.htm(
Liu, C. H. et al. The prevalence and predictors of mental health diagnoses and suicide among U.S. College students: implications for addressing disparities in service use. Depress. Anxiety. 36 (1), 8–17 (2019).
Wang, Y. H. et al. Progress in emotion analysis based on emotion dictionary in depression. Chin. J. Health Psychol. 32 (01), 24–29 (2024).
Li, W. et al. Prevalence and associated factors of depression and anxiety symptoms among college students: a systematic review and meta-analysis. J. Child Psychol. Psychiatry Allied Discip. 63 (11), 1222–1230 (2022).
Cheema, S. et al. Factors associated with perceived stress in middle Eastern university students. J. Am. Coll. Health. 70 (8), 2462–2469 (2022).
Alkhawaldeh, A. et al. Stress factors, stress levels, and coping mechanisms among university students. Sci. World J. 29 (6), 2026971 (2023).
Flesch, B. D. et al. Major depressive episode externalizing symptoms among university students. PLoS One. 16 (6), e0252027 (2021).
Yang, T. et al. The interplay of personality traits, anxiety, and depression in Chinese college students: a network analysis. Front. Public. Health. 11 (3), 1204285 (2023).
Beiter, R. et al. The prevalence and correlates of depression, anxiety, and stress in a sample of college students. J. Affect. Disord. 173, 90–96 (2015).
Tang, H. et al. Meta-analysis of the detection rate of depressed mood among Chinese college students from 2002 to 2011. Journal of Jilin University (Medical edition). 39 (05),965–969 (2013).
Chin, S. et al. Depression outcome expectancy in primary care in Singapore: symptom severity as a mediating determinant. Indian J. Psychol. Med. 42 (1), 39–45 (2020).
Eddington, K. M. et al. Individual differences in expectancies for change in depression: associations with goal pursuit and daily experiences. J. Soc. Clin. Psychol. 35 (8), 629–642 (2016).
Eddington, K. M. et al. Evaluation of the internal consistency, factor structure, and validity of the depression change expectancy scale. Assessment 21 (5), 607–617 (2014).
Roiser, J. P., Elliott, R. & Sahakian, B. J. Cognitive mechanisms of treatment in depression. Neuropsychopharmacology 37(1), 117–136 (2012).
Disner, S. G. et al. Neural mechanisms of the cognitive model of depression. Nat. Rev. Neurosci. 12 (8), 467–477 (2011).
Yang, L. Signalization of the treatment expectation questionnaire TEX-Q and use in colorectal cancer patients. Nanchang Univ. 6(2), 1–3 (2023).
Boussageon, R. et al. How do they add up? The interaction between the placebo and treatment effect: A systematic review. Br. J. Clin. Pharmacol. 88 (8), 3638–3656 (2022).
Dozois, D. J. et al. Development of the anxiety change expectancy scale (ACES) and validation in college, community, and clinical samples. Behav. Res. Ther. 43 (12), 1655–1672 (2005).
Dozois, D. J. A. et al. Development of the anxiety change expectancy (ACES)and validation in college, behaviour community, and clinical samples. Res. Therapy. 43, 1655–1672 (2005).
Westra, H. A. et al. Preparing clients for cognitive behavior therapy: A randomized pilot study of motivational interviewing for anxiety. Cogn. Therapy Res. 30, 481–498 (2006).
Westra, H. A. et al. Marcus M. Expectancy, homework compliance, and initial change in cognitive-behavioral the Rap for anxiety. J. Consult. Clin. Psychol. 75, 363–373 (2007).
Dimidjian, S. et al. Randomized trial of behavioral activation, cognitive therapy, and antidepressant medication in the acute treatment of adults with major depression. J. Consult Clin. Psychol. 74 (4), 658–670 (2006).
Han, X. Estimation and inference of dynamic structural factor models with over-identifying restrictions. J. Econ. 202(2), 145–148 (2018).
Shi, G. L. et al. Sinicization and reliability validity test of ICU fall risk assessment tool. Chin. Nurs. J. 58, 763–768 (2023).
Naser, A. et al. Validity of adult psychopathology model using psychiatric patient sample from a developing country: confirmatory factor analysis. Mental Illn. https://doi.org/10.1155/2022/9594914 (2022).
Sabah, A. et al. Psychometric properties of the perceived collective family efficacy scale in Algeria. Healthcare 11 (19), 2691. https://doi.org/10.3390/healthcare11192691 (2023).
Wang, M. Y. et al. Meta-analysis of the prevalence of depression among Chinese college students in the last decade. J. Hainan Med. Coll. 26 (9), 686–693699. https://doi.org/10.13210/j.cnki.jhmu (2020).
Gomez, R. & Stavropoulos, V. Confirmatory factor analysis and exploratory structural equation modeling of the structure of attention-deficit/hyperactivity disorder symptoms in adults. Assessment 28 (6), 1570–1582. https://doi.org/10.1177/1073191120905892 (2021).
Shek, D. T. L. Reliability and factorial structure of the Chinese version of the Beck depression inventory. J. Clin. Psychol. 46 (1), 35–43. https://doi.org/10.1002/1097-4679(199001)46:13.0.CO;2-W( (1990).
Sabah, A. et al. Psychometric properties of the perceived collective family efficacy scale in Algeria. Healthc. (Basel). 11 (19), 2691. https://doi.org/10.3390/healthcare11192691 (2023).
Zhang, D. et al. Reliability and validity of the Chinese version of the Brief Emotion and Regulation Beliefs Scale in Chinese nursing students. Bmc Nurs. 21(1), 221 (2022).
Boparai, J. K. et al. How to design and validate a questionnaire: a guide. Curr. Clin. Pharmacol. 13 (4), 210–215 (2018).
Sabah, A. et al. Psychometric properties of the perceived collective family efficacy scale in Algeria. Healthcare 11, 2691. https://doi.org/10.3390/healthcare11192691 (2023).
Sabah, A. et al. The associations between sibling victimization, sibling bullying, parental Acceptance–Rejection, and school bullying. Int. J. Environ. Res. Public Health. 19 (23), 16346. https://doi.org/10.3390/ijerph192316346( (2022).
Liu, C. H. et al. Factors associated with depression, anxiety, and PTSD symptomatology during the COVID-19 pandemic: clinical implications for U.S. Young adult mental health. Psychiatry Res. 290, 113–172 (2020).
Zornitsa Kalibatseva & Frederick, T. L. Leong.Cultural factors, depressive and somatic symptoms among Chinese American and European American college students. J. Cross-Cult. Psychol. 49(10):002202211880318 https://doi.org/10.1177/0022022118803181(2018).
Wang, J. et al. Association of recent violence encounters with suicidal ideation among adolescents with depression. JAMA Netw. Open. 6 (3), e231190 (2023).
Heisig, S. R. et al. What do women with breast cancer expect from their treatment? Correlates of negative treatment expectation about endocrine therapy. Psychooncology 25 (12), 1485–1492 (2016).
Ludwig, M. et al. High expectations: from treatment to prevention. Acta Physiol. (Oxf). 215 (1), 2–4 (2015).
Kim, J. K. et al. Effect of pre-treatment expectations on post-treatment expectation fulfillment or outcomes in patients with distal radius fracture. J. Hand Ther. 36 (1), 97–102 (2023).
Acknowledgements
The authors would like to acknowledge Bengbu Medical University and all participants in this study.
Funding
Anhui Province Fund for High-level Teaching Team (2018jxtd105).
Author information
Authors and Affiliations
Contributions
S.L., JZ, P.Y., F.C.: study design and critical revision of the manuscript. S.L.,W.W., R.B., Q.L.: collection and interpretation of data; L.C., W.D.: drafting and revising of the manuscript. All authors reviewed the manuscript. All authors approved the final version for publication.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The present study has been approved by the Research Ethics Committee of Bengbu Medical University (No. 2022 − 128). The study was conducted following the principles of the Helsinki Declaration. All participants provided their written informed consent before the research. The data were collected and analyzed anonymously.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Li, S., Ye, P., Du, W. et al. The reliability and validity of the depression change expectancy scale in college students: a cross-sectional study in China. Sci Rep 15, 8198 (2025). https://doi.org/10.1038/s41598-025-92573-w
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-92573-w