Abstract
Childhood maltreatment is a widespread issue worldwide and has a significant impact on the society at multiple levels, as it affects children. Numerous studies have shown the relationship between various forms of child abuse and the development of adverse outcomes in affected individuals. This study aims to assess the mediating role of distress tolerance in the relationship between childhood maltreatment and anxiety among a sample of Lebanese adults. This cross-sectional study was conducted between March and April 2024; 507 participants were recruited using a snowball sampling method. The results of the mediation analysis were adjusted over sex and physical activity. Distress tolerance partially mediated the association between child abuse and anxiety (indirect effect: Beta = 0.01; Boot SE = 0.01; Boot CI 0.001; 0.02). Higher child abuse was significantly associated with less distress tolerance and directly associated with more anxiety. Higher distress tolerance was significantly associated with less anxiety. The mediating role of distress tolerance in the relationship between childhood maltreatment and anxiety as a mental health outcome was established in this study. Thus, this study highlights the importance of enhancing distress tolerance through therapeutic means including Cognitive and Behavioral Therapies and Dialectical Behavioral Therapy. By doing so, individuals can learn to cope with anxiety caused by childhood maltreatment.
Similar content being viewed by others
Introduction
Childhood maltreatment is a widespread issue worldwide impacting society at multiple levels1, and its effects on children are long-lasting, leading to long term psychological consequences2. A recent meta-analysis encompassing 206 studies from 22 countries and 546,458 participants showed that six in ten adults reported having experienced at least one adverse childhood experience, and one in six reported exposures to four or more adverse childhood experiences prior to the age 183. Many instances of childhood abuse and neglect go unreported, meaning actual rates may be higher4.
The prevalence and types of maltreatment can vary significantly based on cultural, societal, and economic factors. In low-income countries, children often face higher rates of neglect due to resource scarcity, limited access to education, and broader societal challenges5. Conversely, in high-income countries, while systems for detecting and reporting maltreatment are more established, stigma, legal barriers, and limited access to resources may still hinder support for at-risk children5.
Different types of child abuse
Childhood maltreatment can have multiple aspects, including physical abuse, emotional abuse, sexual abuse, and neglect6. By definition, domestic physical abuse is the use of intentional force to cause harm or injury to a child7. Minor injuries and severe physical and psychological harm fall within the spectrum of consequences of physical abuse on children7. Psychological or emotional abuse4 includes rejection, threats, destructive criticism, belittling, ignoring and shaming the child8. This pattern impairs the child’s development and sense of self-worth9. Compared to physical abuse, emotional abuse is less recognizable since it does not leave visible harm10. Sexual abuse9 refers to any kind of sexual activity or exploitation that involves a child, including non-contact actions such as voyeurism or involving a child in pornographic materials11. Long-term negative outcomes of sexual abuse include anxiety, trauma and trust issues in relationships12. Neglect can be defined as the failure of the parents to provide the basic needs for their child, like medical care, hygiene, clothing, housing, education and emotional care12. This can lead to emotional difficulties, physical problems and developmental delays12. Although children may experience various forms of abuse, such as bullying or institutional abuse occurring in schools or other institutions13), this study specifically focuses on family-based child abuse and neglect12.
Signs of child abuse
Children who have been maltreated may display a wide range of behavioral, physical, and emotional signs14. Physically, they may present with unexplained injuries such as burns, bruises, scars, or fractures14. Behaviorally, they may withdraw from others, exhibit fearfulness, anxiety, depression, aggression, or even engage in regressive behaviors like bed-wetting14. Emotionally, they may struggle with low self-esteem, difficulty in forming healthy relationships, or frequent emotional outbursts15. Academically, maltreated children often experience challenges in school, including poor performance and a lack of concentration stemming from the trauma15. Emotional maltreatment, while harder to detect due to the absence of physical signs, can be equally damaging, often manifesting in noticeable shifts in a child’s behavior and emotional well-being15.
Causes and risk factors for child abuse
Several factors contribute to the occurrence of childhood maltreatment, ranging from individual characteristics of caregivers to broader social and environmental influences16. Caregiver factors, such as a history of trauma, substance abuse, mental illness, or domestic violence, can increase the likelihood of parents or caregivers abusing or neglecting their children16. Child-related factors also contribute, with very young children, those with disabilities, or children facing behavioral or mental health issues being at higher risk for maltreatment16. Environmental factors, such as poverty, social isolation (as seen during the COVID 19 pandemic), and a lack of support networks, can further heighten the risk of abuse, particularly when children are raised in abusive environments17. Additionally, cultural and societal factors, such as prevailing norms, attitudes, and limited access to support services, may perpetuate the cycle of abuse, making it harder for victims to escape their circumstances18.
Impact of child abuse
Childhood abuse is a condition that shapes the personality of the children and can have multiple adverse effects on their psychological and physiological well-being19. Indeed, childhood abuse disrupts the hypothalamic-pituitary-adrenal gland axis through excessive cortisol secretion triggered by the excessive stress of maltreatment. This dysregulation increases vulnerability to mental health problems20. The psychological effects may include anxiety, depression, post-traumatic stress disorder (PTSD) and substance abuse21. For instance, children suffering from psychological abuse and neglect often report persistent feelings of sadness and excessive worrying22. Moreover, PTSD is a common outcome of childhood abuse, especially in children who are severely and repeatedly abused23. In addition to the latter, maltreated children can develop, later on in life, a personality disorder such as borderline personality disorder (BPD)24 or antisocial personality disorder25. Childhood abuse can also impact the emotional/cognitive development19 and academic performance21. Furthermore, children who have suffered from childhood abuse are more likely to develop behavioral issues, such as aggression, conduct disorders and delinquencies26, as well as unhealthy social relationships22. It is known that brain development is remarkably affected by chronic stress caused by childhood maltreatment especially in the areas related to stress and emotional regulations as well as cognitive functions20. Studies have shown that there is a dose-response relationship between the number of adverse childhood experiences and an increased risk of health and developmental difficulties27. Conversely, children who were reported as affectionate with their parent had decreased risk for health and developmental problems27. It is also of note that the harmful effects of adverse childhood experiences are more pronounced when protective factors, such as mother-child relations, parental health, and community engagement28, are lacking.
Childhood maltreatment and anxiety
Anxiety is one of the resulting mental outcomes of childhood maltreatment29. The correlation between child abuse and anxiety is well-documented in recent literature30, showing that abused individuals during childhood are at a significant higher risk of developing anxiety later in adulthood30. This can be due to various factors like the effect of trauma on the development of the brain, a dysregulation in the hypothalamic-pituitary-adrenal axis, and negative perception on oneself with a low self-esteem31. Despite the existence of extensive literature to suggest the predictive role of childhood abuse on the emergence of anxiety, researchers have called for further investigations of the links between childhood abuse and symptoms of anxiety to better understand the common underlying processes32.
Childhood maltreatment is understood within psychological and neurological frameworks as a significant disruption to normal emotional, cognitive, and social development33. Theories of attachment, such as Bowlby’s, highlight how early abuse or neglect can impair the formation of secure attachments, leading to long-term emotional and behavioral difficulties34. Neurologically, maltreatment has been shown to disrupt the brain’s stress response systems, particularly the hypothalamic-pituitary-adrenal (HPA) axis, resulting in heightened vulnerability to anxiety, depression, and post-traumatic stress disorder34. Early trauma may also impact the development of key brain regions, such as the prefrontal cortex and amygdala, which are involved in emotional regulation and decision-making35. These combined psychological and neurological disruptions can create a cycle of maladaptive coping mechanisms, attachment difficulties, and emotional dysregulation that persist into adulthood35.
Childhood maltreatment, anxiety and distress tolerance
Distress tolerance is defined as the ability of the person to endure emotional distress without trying to escape or avoid it36. In fact, the impact of child abuse can be severe on the ability of the affected individual to tolerate distress. Thus, emotional dysregulation along with chronic stress and learned helplessness caused by abuse result in lowered distress tolerance37. As a consequence, the abused child could develop unfavorable psychological outcomes like anxiety, depression or personality disorders38. These outcomes should then be addressed in therapeutic settings in order to alleviate the effect of child abuse on anxiety39. Therapeutic sessions aim to enhance distress tolerance in order to alleviate anxiety39. The mediating role of distress tolerance can have a positive impact on the relationship between childhood maltreatment and mental health outcomes as shown by several studies40. Whereas individuals with low distress tolerance are more prone to develop maladaptive coping strategies such as self-harm, addiction and delinquency41. This will lead to a poor mental health outcome after being confronted to childhood maltreatment41. On the other hand, negative behaviors can be buffered by high distress tolerance40.
Key aspects of distress tolerance are numerous. Among them, tolerance of emotional pain that is defined by the absence of impulsive reactions or engaging in harmful coping mechanisms in response to uncomfortable emotions like anger, anxiety, sadness, by staying present and serene36. Another aspect of distress tolerance is the acceptance of difficult circumstances despite the fact of them being painful rather than denying or resisting them42. Crisis survival strategies, like Dialectical Behavior Therapy, provide skills to navigate crisis without worsening the situation43. The techniques provided by therapeutic approaches such as CBT and DBT include mindfulness practices, radical acceptance, distraction and delay techniques, and grounding exercises to stay focused on the time present without being driven by negative feelings44. Lastly, many studies have shown the relationship between childhood maltreatment and mental health outcomes and how this relationship is mediated by distress tolerance40.
Rationale and aim of this study
The topic of this study is not only a concern in Lebanon but also globally. In fact, family-based childhood maltreatment is a prevalent issue, which can be found in all countries worldwide2. Given the fact that Lebanon is a Middle Eastern country, and with the absence or strict rules and regulations, childhood abuse could be more prevalent especially in some regions. The Child Rights Situational Analysis for the Middle East and North Africa (MENA) region claimed that “child protection remains a serious issue in every country of the region”. Besides, there is a notable lack of studies on the topic, and a “cultural resistance to addressing the problem (of child abuse)” in all countries of the MENA region, because the subject remains largely taboo45. In Lebanon, the prevalence of child maltreatment established in one study is 3.2%46. Children who were reported as victims of childhood abuse were those who were admitted to the emergency department47. Thus, this low rate could be due to a lack of reporting due to economic, socio-politic and financial problems of the country43. Accordingly, it can be expected to observe high prevalence rates of anxiety related to child abuse in the Lebanese adult population.
Distress tolerance was specifically chosen as a mediator in this study due to its central role in how individuals cope with emotional distress, particularly following traumatic experiences like childhood maltreatment. Research has shown that childhood abuse significantly disrupts emotional regulation, leading to low distress tolerance, which in turn increases vulnerability to anxiety and other mental health issues48. Unlike other psychological mechanisms such as self-esteem or coping strategies, distress tolerance directly impacts an individual’s ability to endure and manage emotional discomfort without resorting to avoidance or maladaptive behaviors48.
The present study aims to assess the mediating role of distress tolerance in the relationship between childhood maltreatment and anxiety among a sample of Lebanese adults. Understanding this relationship can promote therapeutic approaches and preventive efforts that aim to enhance resilience and mental well-being in individuals with history of childhood maltreatment. Based on the following, our research question is the subsequent: To what extent does distress tolerate mediate the association between all types of childhood maltreatment and anxiety among a sample of Lebanese adults? We therefore hypothesize that lower distress tolerance would mediate the association between higher childhood maltreatment and higher anxiety.
Methods
Study design
This cross-sectional study enrolled 507 participants between March and April 2024, recruited via a snowball sampling method from across all Lebanese governorates (Mount Lebanon, South, North, Beirut, and Beqaa). Snowball sampling was used, meaning initial participants were asked to refer others, which allowed for a wider reach but also posed risks of sampling bias, as participants may have referred individuals from similar social networks. Participants were directed to a website providing access to the consent form, an information sheet (detailing the study’s purpose, anonymity, and voluntary participation), and the questionnaire. They were also informed that participation was free of charge and offered no compensation. The study included all Lebanese citizens and residents aged 18 and above with internet access who were willing to participate. Excluded were individuals without internet access, potentially leaving out key demographic groups. Additionally, the inclusion of only those willing to participate could result in self-selection bias, where people with particular interests or motivations are overrepresented.
Minimal sample size calculation
According to Fritz and MacKinnon49 a minimal sample of 408 was deemed necessary based on this formula: \(\:n=\frac{L}{f2}+k+1\), where f=0.14 for small effect size, L=7.85 for an α error of 5% and power β = 80%, and k=6 variables to be entered in the model.
Questionnaire
The questionnaire, administered in Arabic, took an average of 20 min to complete. The first section gathered sociodemographic information such as sex, age, marital status, and the Household Crowding Index (HCI), which is calculated by dividing the number of people living in the household, excluding newborns, by the total number of rooms, excluding the kitchen50. The strength, frequency, and duration of physical activity were multiplied to create the physical activity index51,52.
Measures
Child abuse self report scale—short form (CASRS)
We used the version adapted and validated in Lebanon53, as this concise assessment is derived from the 38-item version, which was also originally developed in an oriental context54, further supporting its cross-cultural validity. Our version consists of 12 statements addressing the primary domains of child abuse that happened within the family: physical (“I witness other family members being beaten”), psychological (“My parents treat me with disrespect”), sexual (“An adult or adults tried to touch my private parts”), and neglect (“My family pays attention to my wishes”). Each item is rated on a 4-point Likert scale ranging from Never (0) to Always (3), with higher scores indicating a greater perceived level of childhood abuse. The current study reports a Cronbach’s α of 0.86.
The distress tolerance scale (DTS)55
This 15-item self-report measure, validated in Arabic56 is designed to assess an individual’s ability to tolerate negative emotions. It includes four subscales: Appraisal of Capacity and Distress Experienced (e.g., “I can tolerate being distressed or upset as well as most people”), Absorption in Negative Emotions (e.g., “When I feel distressed or upset, all I can think about is how bad I feel”), Regulation of Emotions (e.g., “I’ll do anything to stop feeling distressed or upset”), and Tolerance of Distressing Emotions (e.g., “Feeling distressed or upset is unbearable to me”). Participants rate each item on a 5-point Likert scale, ranging from 1 (strongly agree) to 5 (strongly disagree). The Distress Tolerance Scale (DTS) is scored by calculating the mean for each subscale, along with an overall mean score, with item 6 requiring reverse coding. Lower DTS scores indicate a reduced ability to tolerate distress (Cronbach’s α = 0.91 in the current study).
Generalized anxiety scale (GAD-7), validated in Lebanon57,58, it is a 7-item self-report scale used to measure symptoms of anxiety and provide rapid screening for Generalized Anxiety Disorder (GAD). Each item uses a 4-point Likert scale (0–3 points), where respondents are asked to consider the previous two weeks and rate the frequency of their symptoms as ‘not at all’ (0), ‘several days’ (1), ‘more than half the days’ (2), or ‘nearly every day’ (3). The total score ranges from 0 to 217 items, with higher score indicating more anxiety (current Cronbach’s α = .88).
Statistical analysis
Data analysis was performed using the SPSS software version 26. Reliability of the scales was checked using Cronbach’s alpha values. The anxiety score had a normal distribution as shown by the skewness (= .459) and kurtosis ( = − .242) values varying between ± 1. The Student t-test was used to compare continuous variables between two groups, and Pearson correlation was used for linear correlation between continuous variables. The PROCESS SPSS Macro version 3.4, model 4 was used to calculate four pathways; Pathway A determined the effect of the child abuse on the mediator distress tolerance; Pathway B examined the association between distress tolerance and anxiety, and Pathways C and C’ estimated the total and direct effects of child abuse on anxiety. Significance was deemed present if the Bootstrapped confidence interval did not pass by zero. The mediation analysis was adjusted over all variables that showed a p < .25 in the bivariate analysis. Significance was set at p < .05.
Results
Five hundred seven adults completed the survey, with a mean age of 26.80 ± 10.29 years [min = 18; max = 70] and 73.2% females. Other description of the sample can be found in Table 1.
Bivariate analysis
The results of the bivariate analysis are summarized in Tables 2 and 3. Higher child abuse was significantly associated with higher anxiety, whereas more distress tolerance was significantly associated with less anxiety.
Mediation analysis
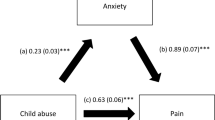
The results of the mediation analysis were adjusted over sex and physical activity. Distress tolerance partially mediated the association between total child abuse and anxiety (indirect effect: Beta = 0.01; Boot SE = 0.01; Boot CI 0.001; 0.02). Higher total child abuse was significantly associated with less distress tolerance and directly associated with more anxiety. Finally, higher distress tolerance was significantly associated with less anxiety (Fig. 1).
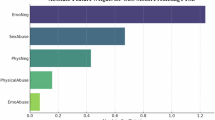
The results of the mediation analysis done by type of child abuse showed that distress tolerance did not mediate the associations between psychological abuse (indirect effect: Beta = 0.01; Boot SE = 0.02; Boot CI − 0.02; 0.05), physical abuse (indirect effect: Beta = 0.002; Boot SE = 0.01; Boot CI − 0.02; 0.03) and sexual abuse (indirect effect: Beta = 0.001; Boot SE = 0.02; Boot CI − 0.02; 0.03) and anxiety, whereas it fully mediated the association between neglect and anxiety (indirect effect: Beta = 0.06; Boot SE = 0.02; Boot CI 0.02; 0.11) (Figs. 2, 3, 4 and 5).
(a) Relation between total child abuse and distress tolerance (R2 = 0.012); (b) Relation between distress tolerance and anxiety (R2 = 0.120); (c) Total effect of total child abuse on anxiety (R2 = 0.049); (c') Direct effect of total child abuse on anxiety. Numbers are displayed as regression coefficients (standard error). *p < .05; ***p < .001.
(a) Relation between psychological child abuse and distress tolerance (R2 = 0.003); (b) Relation between distress tolerance and anxiety (R2 = 0.196); (c) Total effect of psychological child abuse on anxiety (R2 = 0.180); (c') Direct effect of psychological child abuse on anxiety. Numbers are displayed as regression coefficients (standard error). **p < .01; ***p < .001.
(a) Relation between child neglect and distress tolerance (R2 = 0.046); (b) Relation between distress tolerance and anxiety (R2 = 0.035); (c) Total effect of child neglect on anxiety (R2 = 0.013); (c') Direct effect of child neglect on anxiety. Numbers are displayed as regression coefficients (standard error). ***p < .001.
(a) Relation between physical child abuse and distress tolerance (R2 = 0.002); (b) Relation between distress tolerance and anxiety (R2 = 0.140); (c) Total effect of physical child abuse on anxiety (R2 = 0.122); (c') Direct effect of physical child abuse on anxiety. Numbers are displayed as regression coefficients (standard error). **p < .01; ***p < .001.
(a) Relation between sexual child abuse and distress tolerance (R2 = 0.002); (b) Relation between distress tolerance and anxiety (R2 = 0.123); (c) Total effect of sexual child abuse on anxiety (R2 = 0.105); (c') Direct effect of sexual child abuse on anxiety. Numbers are displayed as regression coefficients (standard error). **p < .01; ***p < .001.
Discussion
In this study, findings suggest that higher level of child abuse is associated with higher rates of anxiety43. In fact, individuals who have endured any type of abuse in childhood might be more susceptible to developing higher levels of anxiety. A systematic review and meta-analysis of the association between all forms of child maltreatment and depressive and anxiety disorders41 showed that all forms of child maltreatment were associated with a significantly increased risk of depressive and anxiety disorders30. One prospective cohort study showed that maltreatment in childhood substantially increases the risk of adult depression and anxiety59,60. Other studies have also shown the relationship between childhood maltreatment and negative mental health outcomes other than anxiety, like depression59, PTSD61 and personality disorders62. This correlation can have multiple psychological explanations. In fact, childhood abuse affects the hypothalamic-pituitary-adrenal axis, resulting in increased secretion of cortisol, the stress hormone. With time, chronic stress is able to cause lasting modifications in the amygdala, hippocampus and prefrontal cortex, the regions of the brain involved in fear and anxiety31. Moreover, child abuse could lead to the disruption of secure attachments and often manifests as anxiety later in life30. Impaired emotional regulation, negative cognitive schemas, as well as learned helplessness are also psychological explanations for this correlation30.
In this study, the mediation analysis results showed that distress tolerance partially mediated the association between child abuse and anxiety. In fact, distress tolerance may mediate this relationship by determining the capacity of the individual to cope with emotional pain and stress resulting from childhood trauma. Moreover, the pathway from childhood abuse to anxiety often runs through distress tolerance40. Anxiety is more probable to develop in people with low distress tolerance levels since they do not have the psychological equipment to handle the stress of their abusive experiences63. In contrast, those who have higher distress tolerance levels through any of the mechanisms that enhances this tolerance, are able to better cope with their trauma, thus leading to less anxiety63. Research indicates that childhood anxiety is prevalent among Afghan children, highlighting the significant impact of various stressors on their mental health. Collective violence trauma, particularly related to war, was notably higher in the Afghan sample compared to other countries, with 27.51% reporting personal exposure to such trauma64. These findings align with the study’s observation that higher levels of childhood abuse are associated with increased rates of anxiety. In both contexts, early traumatic experiences, including exposure to violence and abuse, significantly contribute to the development of anxiety disorders. However, the study’s focus on distress tolerance as a mediator between childhood abuse and anxiety may not fully capture the complex interplay of factors influencing mental health outcomes in Afghan children. In Afghanistan, the prevalence of mental health issues among children is exacerbated by factors such as political violence, displacement, and limited access to mental health services65.
The results of the mediation analysis done by type of child abuse showed that distress tolerance did not mediate the associations between psychological abuse physical abuse and sexual abuse and anxiety, whereas it fully mediated the association between neglect and anxiety. This implies that there may be other psychological or environmental factors at play that contribute to the onset of anxiety in individuals who have faced psychological, physical or sexual types of abuse. On the other hand, individuals who experience neglect may have lower levels of distress tolerance, which in turn, increases their likelihood of developing anxiety. In this case, distress tolerance acts as a crucial mechanism through which neglect influences anxiety, potentially indicating that individuals who struggle with tolerating emotional distress may be more vulnerable neglect-induced anxiety. These findings highlight the complexity of how different types of abuse affect mental health outcomes. This suggests that tailored interventions may be necessary, focusing on improving distress tolerance for individuals who have experienced neglect, while exploring other mediators for those who have faced other forms of abuse.
The partial mediation of distress tolerance between child abuse and anxiety suggests that there might be other factors that could mediate this relationship, such as alexithymia, insecure attachment, low self-esteem, social support, chronic stress, etc. Alexithymia, characterized by difficulty in identifying, understanding, and expressing emotions, may play a significant role in mediating the relationship between childhood abuse and anxiety in adulthood66. Childhood maltreatment can impair emotional development, and individuals with alexithymia struggle to process their emotions, which can exacerbate anxiety. This condition may lead to poor emotional regulation, maladaptive coping strategies, and increased stress sensitivity, all of which contribute to anxiety66. Research exploring alexithymia as a mediator could offer valuable insights into how childhood abuse impacts anxiety, potentially guiding therapeutic interventions that focus on improving emotional awareness and regulation to reduce anxiety in individuals with a history of maltreatment66. Secure attachments in early life help develop healthy emotional regulation and coping skills, whereas insecure attachments (such as anxious or avoidant attachment) can lead to difficulties in managing anxiety67. Children who experience abuse or neglect may struggle to form secure attachments, leading to challenges in managing stress and fear in adulthood67. Previous findings have shown that low self-esteem and feelings of worthlessness are often outcomes of childhood maltreatment; people who experience abuse may internalize negative beliefs about themselves, which can exacerbate anxiety68. This lack of self-worth can make it more difficult for them to trust in their ability to cope with stressful situations, leading to greater vulnerability to anxiety disorders68,69. The level of social support available to an individual can influence the development of anxiety in general70and following childhood maltreatment71. Individuals who have supportive relationships or access to social networks may be better able to cope with the emotional fallout of childhood trauma71. Childhood maltreatment often leads to chronic stress, which can disrupt the body’s stress response systems72. Over time, this chronic stress can lead to an overactive sympathetic nervous system (responsible for the “fight or flight” response), making individuals more prone to anxiety72. Additionally, repeated exposure to stress may affect the prefrontal cortex, impairing the individual’s ability to regulate fear and anxiety72.
Concerning the assessment of the different types of child abuse in the relationship with anxiety and distress tolerance as a mediator, this study is the first of its kind to assess such relationship, this is why a comparison with previous studies could not be done.
To cope with the harm caused by childhood abuse, one study had an increased focus on distress tolerance as a mediator between childhood maltreatment and mental health outcome73. For instance, this study suggested that high distress tolerance can have a buffer effect on the impact of childhood abuse, therefore promoting resilience and adaptive coping to get better mental health outcomes74. In fact, higher levels of distress tolerance achieved by any technique like DBT or CBT and exercises like mindfulness have shown to decrease the levels of anxiety in individuals who suffered from child abuse75,76,77. Since therapy is not widely available, other means should be relied on to address distress tolerance in the general population78. This includes education and awareness by teaching individuals to achieve mindfulness by mindfulness practices79. Trauma-Focused Cognitive-Behavioral Therapy (TF-CBT) plays a crucial role in enhancing distress tolerance for children who have experienced childhood abuse, ultimately reducing anxiety80. This therapy helps individuals develop coping strategies, such as emotion regulation and cognitive restructuring, to manage intense emotions and challenging thoughts associated with trauma80. By gradually exposing children to their traumatic memories in a safe and controlled environment, TF-CBT allows them to process these memories without becoming overwhelmed80. By improving distress tolerance, TF-CBT reduces the emotional dysregulation that often leads to anxiety, making it an effective intervention for children and adolescents affected by childhood abuse80. Moreover, child protection laws are essential in many countries, providing frameworks for preventing and responding to childhood maltreatment, with many of these laws including mandatory reporting requirements for professionals who suspect abuse81. Social workers and other professionals may face difficult decisions about when to intervene in family matters while maintaining confidentiality, as these actions can sometimes conflict with the urgency of ensuring a child’s safety and well-being82.
Limitations
This study has several limitations that should be considered when interpreting its findings. First, because the data on childhood abuse were collected retrospectively through a questionnaire, the accuracy of the memories reported by participants may be influenced by their later experiences, potentially leading to recall bias or inaccuracies in the information provided. Second, there is the possibility that some participants may have willfully provided incorrect responses or altered the facts, either consciously or unconsciously, which could affect the validity of the results. The outcomes observed in this study may not be generalizable to other populations, as different cultural, social, and environmental factors could influence the relationship between childhood abuse and anxiety, leading to variations in the results when conducted in different settings or among diverse groups. Moreover, the cross-sectional design of our study limits our ability to establish causality, and reliance on self-reported data may be biased. However, it is important to note that mediation analysis can be appropriate for cross-sectional data when the goal is to explore potential indirect relationships between variables, even though causal inferences cannot be definitively made. A selection bias is possible because of the snowball sampling technique, the unknown refusal rate, and the predominance of females, single and highly educated participants. Diversifying the sample population in future studies can reveal cultural, socioeconomic, and demographic differences that can affect the generalizability of our findings. Future research should use longitudinal designs that can track changes over time and thus better understand the temporal dynamics among these variables, while taking this study’s limitations.
Clinical implications
This study sheds the light on the importance of potentializing distress tolerance by all means including CBT and DBT so the individual can learn to cope with anxiety related to childhood abuse. This should be a call to help children who are suffering from abuse, providing them with earlier support early so they do not have to suffer from anxiety or reduced distress tolerance later in life. Moreover, the role of the physician is crucial in detecting various forms of child abuse to take action and prevent future negative outcomes on the mental health of abused children. Practical recommendations to enhance distress tolerance include behavioral therapies, trauma-focused therapy, promoting mindfulness practices, encouraging healthy coping mechanisms such as journaling, creative arts, physical exercise, and spending time in nature, as well as promoting lifestyle changes.
Conclusion
This study’s results suggest that higher child abuse might be significantly associated with higher anxiety, with more distress tolerance acting as partial mediator in this association. Future research should include policy implications such as integrating distress tolerance training in early childhood interventions. Additionally, future studies should consider a more diverse population and explore comorbidities with other disorders, such as substance abuse, PTSD, and risky behaviors.
Data availability
Because of ethical committee constraints, none of the data collected or analyzed during this study are publicly available. However, the corresponding authors may make the data available upon reasonable request.
References
Stoltenborgh, M. It Should Not Hurt to Be a Child: Prevalence of Child Maltreatment Across the Globe. http://hdl.handle.net/1887/19142.
Perry, B. D. Sharing Ideas to Help Children Thrive Www.Lfcc.on.ca Inaugural Lecture by Maltreatment and the Developing Child: How Early Childhood Experience Shapes Child and Culture. www.lfcc.on.ca (2004).
Madigan, S. et al. Adverse Childhood Experiences: A Meta-analysis of Prevalence and Moderators Among Half a Million Adults in 206 Studies, Vol 22 (2023).
Quiroz, H. J. et al. Identifying populations at risk for child abuse: a nationwide analysis. J. Pediatr. Surg. 55 (1), 135–139. https://doi.org/10.1016/j.jpedsurg.2019.09.069 (2020).
Kecheng, Z. & Hussain, M. The historical origin and public manifestation of public Art. Pak Soc. Sci. Rev. 7 (III), 6. https://doi.org/10.35484/pssr.2023(7-iii)06 (2023).
Jackson, A. M., Kissoon, N. & Greene, C. Aspects of abuse: recognizing and responding to child maltreatment. Curr. Probl. Pediatr. Adolesc. Health Care. 45 (3), 58–70. https://doi.org/10.1016/j.cppeds.2015.02.001 (2015).
Christian, C. W. et al. The evaluation of suspected child physical abuse. Pediatrics 135 (5), e1337–e1354. https://doi.org/10.1542/peds.2015-0356 (2015).
Esser, M. B. et al. Physical abuse, psychological abuse and neglect: evidence of alcohol-related harm to children in five States of India. Drug Alcohol Rev. 35 (5), 530–538. https://doi.org/10.1111/dar.12377 (2016).
Downey, C. & Crummy, A. The impact of childhood trauma on children’s wellbeing and adult behavior. Eur. J. Trauma. Dissoc. 6 (1), 237. https://doi.org/10.1016/j.ejtd.2021.100237 (2022).
Snyder, R. L. No Visible Bruises: What We Don’t Know About Domestic Violence Can Kill Us.
Mathews, B. & Collin-Vézina, D. Child sexual abuse: toward a conceptual model and definition. Trauma. Violence Abuse. 20 (2), 131–148. https://doi.org/10.1177/1524838017738726 (2019).
Strathearn, L. et al. Long-term cognitive, psychological, and health outcomes associated with child abuse and neglect. Pediatrics 146 (4), 438. https://doi.org/10.1542/peds.2020-0438 (2020).
Blakemore, T., Herbert, J. L., Arney, F. & Parkinson, S. The impacts of institutional child sexual abuse: A rapid review of the evidence. Child. Abuse Negl. 74, 35–48. https://doi.org/10.1016/j.chiabu.2017.08.006 (2017).
McTavish, J. R. et al. Identifying children exposed to maltreatment: A systematic review update. BMC Pediatr. 20 (1), 4. https://doi.org/10.1186/s12887-020-2015-4 (2020).
Vizard, E., Gray, J. & Bentovim, A. The impact of child maltreatment on the mental and physical health of child victims: a review of the evidence. BJPsych Adv. 28 (1), 60–70. https://doi.org/10.1192/bja.2021.10 (2022).
Vial, A., van der Put, C., Stams, G. J. J. M., Kossakowski, J. & Assink, M. Exploring the interrelatedness of risk factors for child maltreatment: A network approach. Child. Abuse Negl. 107, 622. https://doi.org/10.1016/j.chiabu.2020.104622 (2020).
Đapić, M. R., Flander, G. B. & Prijatelj, K. Children behind closed doors due to covid-19 isolation: abuse, neglect and domestic violence. Archives Psychiatry Res. 56 (2), 181–192. https://doi.org/10.20471/dec.2020.56.02.06 (2020).
Al-Saadoon, M., Al-Adawi, M. & Al-Adawi, S. Socio-cultural constraints in protecting child rights in a society in transition: a review and synthesis from Oman. Child. Indic. Res. 14 (1), 239–267. https://doi.org/10.1007/s12187-020-09759-z (2021).
Oh, D. L. et al. Systematic review of pediatric health outcomes associated with childhood adversity. BMC Pediatr. 18 (1), 7. https://doi.org/10.1186/s12887-018-1037-7 (2018).
The_effects_of_childhood_maltreatment_on.
Kisely, S. et al. Child maltreatment and mental health problems in adulthood: birth cohort study. Br. J. Psychiatry. 213 (6), 698–703. https://doi.org/10.1192/bjp.2018.207 (2018).
Jaffee, S. R. Child maltreatment and risk for psychopathology in childhood and adulthood. Annu. Rev. Clin. Psychol. 13, 525–551. https://doi.org/10.1146/annurev-clinpsy-032816-045005 (2017).
Barboza, G. E. & Dominguez, S. Longitudinal growth of post-traumatic stress and depressive symptoms following a child maltreatment allegation: an examination of violence exposure, family risk and placement type. Child. Youth Serv. Rev. 81, 368–378. https://doi.org/10.1016/j.childyouth.2017.08.029 (2017).
Mainali, P., Rai, T. & Rutkofsky, I. H. From child abuse to developing borderline personality disorder into adulthood: exploring the neuromorphological and epigenetic pathway. Cureus. https://doi.org/10.7759/cureus.9474 (2020).
Johnson, S. A. Understanding the violent personality: antisocial personality disorder, psychopathy, & sociopathy explored. Foresic Res. Criminol. Int. J. 7 (2), 267. https://doi.org/10.15406/frcij.2019.07.00267 (2019).
Augustyn, M. B., Thornberry, T. P. & Henry, K. L. The reproduction of child maltreatment: an examination of adolescent problem behavior, substance use, and precocious transitions in the link between victimization and perpetration. Dev. Psychopathol. 31 (1), 53–71. https://doi.org/10.1017/S0954579418001633 (2019).
Webster, E. M. The impact of adverse childhood experiences on health and development in young children. Glob Pediatr. Health. 9, 708. https://doi.org/10.1177/2333794X221078708 (2022).
Touloumakos, A. K. & Barrable, A. Adverse childhood experiences: the protective and therapeutic potential of nature. Front. Psychol. 11, 935. https://doi.org/10.3389/fpsyg.2020.597935 (2020).
Hovens, J. G. F. M. Emotional Scars Impact of Childhood Trauma on Depressive and Anxiety Disorders.
Gardner, M. J., Thomas, H. J. & Erskine, H. E. The association between five forms of child maltreatment and depressive and anxiety disorders: A systematic review and meta-analysis. Child. Abuse Negl. 96, 82. https://doi.org/10.1016/j.chiabu.2019.104082 (2019).
The_effects_of_childhood_maltreatment_on (2).
Kascakova, N., Furstova, J., Hasto, J., Geckova, A. M. & Tavel, P. The unholy trinity: childhood trauma, adulthood anxiety, and long-term pain. Int. J. Environ. Res. Public. Health. 17 (2), 414. https://doi.org/10.3390/ijerph17020414 (2020).
Teicher, M. H., Gordon, J. B. & Nemeroff, C. B. Recognizing the importance of childhood maltreatment as a critical factor in psychiatric diagnoses, treatment, research, prevention, and education. Mol. Psychiatry. 27 (3), 1331–1338. https://doi.org/10.1038/s41380-021-01367-9 (2022).
Grady, M. D., Levenson, J. S. & Bolder, T. Linking adverse childhood effects and attachment: a theory of etiology for sexual offending. Trauma. Violence Abuse. 18 (4), 433–444. https://doi.org/10.1177/1524838015627147 (2017).
Cross, D., Fani, N., Powers, A. & Bradley, B. Neurobiological development in the context of childhood trauma. Clin. Psychol. Sci. Pract. 24 (2), 111–124. https://doi.org/10.1111/cpsp.12198 (2017).
Kraemer, K. M., Luberto, C. M., O’Bryan, E. M., Mysinger, E. & Cotton, S. Mind–body skills training to improve distress tolerance in medical students: a pilot study. Teach. Learn. Med. 28 (2), 219–228. https://doi.org/10.1080/10401334.2016.1146605 (2016).
Jeffries, E. R., McLeish, A. C., Kraemer, K. M., Avallone, K. M. & Fleming, J. B. The role of distress tolerance in the use of specific emotion regulation strategies. Behav. Modif. 40 (3), 439–451. https://doi.org/10.1177/0145445515619596 (2016).
Lippard, E. T. C. & Nemeroff, C. B. The devastating clinical consequences of child abuse and neglect: increased disease vulnerability and poor treatment response in mood disorders. Am. J. Psychiatry. 177 (1), 20–36. https://doi.org/10.1176/appi.ajp.2019.19010020 (2020).
Crowe, K. & McKay, D. Efficacy of cognitive-behavioral therapy for childhood anxiety and depression. J. Anxiety Disord. 49, 76–87. https://doi.org/10.1016/j.janxdis.2017.04.001 (2017).
Robinson, M. et al. Mediating Role of Distress Tolerance The Mediating Role of Distress Tolerance in the Relationship between Childhood Maltreatment and Mental Health Outcomes Among University Students.
Babaeifard, M. et al. Early maladaptive schemas, distress tolerance and self-injury in Iranian adolescents: serial mediation model of transdiagnostic factors. BJPsych Open. 10 (3), 708. https://doi.org/10.1192/bjo.2024.708 (2024).
Glassman, L. H. et al. A brief report on the assessment of distress tolerance: are we measuring the same construct? J. Ration. Emotive Cogn. Behav. Therapy. 34 (2), 87–99. https://doi.org/10.1007/s10942-015-0224-9 (2016).
Andrushko, Y. Working with trauma in dialectical behavioral therapy: literature review. Polonia Univ. Sci. J. 2, 8–19. https://doi.org/10.23856/5701 (2023).
Webb, C. A., Beard, C., Kertz, S. J., Hsu, K. J. & Björgvinsson, T. Differential role of CBT skills, DBT skills and psychological flexibility in predicting depressive versus anxiety symptom improvement. Behav. Res. Ther. 81, 12–20. https://doi.org/10.1016/j.brat.2016.03.006 (2016).
Polonko, K. A. Child Sexual Abuse in the Middle East and North Africa: A Review. https://www.researchgate.net/publication/261177004.
Joel Bakhos, J. et al. Child maltreatment in Lebanon: prevalence, screening and upgrade of ESCAPE. World J. Public. Health. 7 (1), 14. https://doi.org/10.11648/j.wjph.20220701.13 (2022).
Hovdestad, W., Campeau, A., Potter, D. & Tonmyr, L. A systematic review of childhood maltreatment assessments in population-representative surveys since 1990. PLoS ONE. 10 (5), 366. https://doi.org/10.1371/journal.pone.0123366 (2015).
Paulus, F. W., Ohmann, S., Möhler, E., Plener, P. & Popow, C. Emotional dysregulation in children and adolescents with psychiatric disorders. A narrative review. Front. Psychiatry. 12, 52. https://doi.org/10.3389/fpsyt.2021.628252 (2021).
Fritz, M. S. & MacKinnon, D. P. Required sample size to detect the mediated effect. Psychol. Sci. 18 (3), 233–239. https://doi.org/10.1111/j.1467-9280.2007.01882.x (2007).
Melki, I. S., Beydoun, H. A., Khogali, M., Tamim, H. & Yunis, K. A. Household crowding index: A correlate of socioeconomic status and inter-pregnancy spacing in an urban setting. J. Epidemiol. Community Health. 58 (6), 476–480. https://doi.org/10.1136/jech.2003.012690 (2004).
Anne, K. Validation of the Physical Activity Index (PAI) as a Measure of Total Activity Load and Total Kilocalorie Expenditure During Submaximal Treadmill Walking (2003).
Assaf, M. et al. Arabic Translation and Psychometric Testing of the Physical Activity Index (PAI). https://doi.org/10.21203/rs.3.rs-5945662/v1 (2025).
Fekih-Romdhane, F. et al. Development and validation of a shortened version of the child abuse self report scale (CASRS-12) in the Arabic Language. Child. Adolesc. Psychiatry Ment Health. 16 (1), 3. https://doi.org/10.1186/s13034-022-00533-3 (2022).
Mohammadkhani, P., Mohammadi, M. R., Nazari, M. A., Salavati, M. & Razzaghi, O. M. Development, validation and reliability of child abuse self report scale (CASRS) in Iranian students. Med. J. Islamic Repub. Iran. 17, 51 (2003).
Brown, R. J., Burton, A. L. & Abbott, M. J. The relationship between distress tolerance and symptoms of depression: validation of the distress tolerance scale (DTS) and short-form (DTS-SF). J. Clin. Psychol. 78 (12), 2609–2630. https://doi.org/10.1002/jclp.23370 (2022).
Noureddine, A. et al. Validation of the Arabic versions of the long (15 items) and short (4 items) forms of the Distress Tolerance Scale (DTS), 11 October 2024, PREPRINT (Version 1) available at Research Square [https://doi.org/10.21203/rs.3.rs-4909439/v1].
Sawaya, H., Atoui, M., Hamadeh, A., Zeinoun, P. & Nahas, Z. Adaptation and initial validation of the patient health questionnaire-9 (PHQ-9) and the generalized anxiety disorder-7 questionnaire (GAD-7) in an Arabic speaking Lebanese psychiatric outpatient sample. Psychiatry Res. 239, 245–252. https://doi.org/10.1016/j.psychres.2016.03.030 (2016).
Khoury-Malhame, M. et al. Psychometric Validation of the Arabic Version of the GAD-7 Among Lebanese Adolescents. https://doi.org/10.21203/rs.3.rs-4486990/v1 (2024).
Li, M., D’Arcy, C. & Meng, X. Maltreatment in childhood substantially increases the risk of adult depression and anxiety in prospective cohort studies: systematic review, meta-analysis, and proportional attributable fractions. Psychol. Med. 46 (4), 717–730. https://doi.org/10.1017/S0033291715002743 (2016).
Guo, L. et al. Childhood maltreatment predicts subsequent anxiety symptoms among Chinese adolescents: the role of the tendency of coping styles. Transl Psychiatry. 11 (1), 1. https://doi.org/10.1038/s41398-021-01463-y (2021).
Rameckers, S. A. et al. The Smpact of childhood maltreatment on the severity of childhood-related posttraumatic stress disorder in adults. Child. Abuse Negl. 120, 208. https://doi.org/10.1016/j.chiabu.2021.105208 (2021).
Kounou, K. B. et al. Childhood maltreatment and personality disorders in patients with a major depressive disorder: A comparative study between France and Togo. Transcult Psychiatry. 52 (5), 681–699. https://doi.org/10.1177/1363461515572001 (2015).
Banducci, A. N., Lejuez, C. W., Dougherty, L. R. & MacPherson, L. A prospective examination of the relations between emotional abuse and anxiety: moderation by distress tolerance. Prev. Sci. 18 (1), 20–30. https://doi.org/10.1007/s11121-016-0691-y (2017).
Kovess-Masfety, V., Keyes, K., Karam, E., Sabawoon, A. & Sarwari, B. A. A National survey on depressive and anxiety disorders in Afghanistan: A highly traumatized population. BMC Psychiatry. 21 (1), 4. https://doi.org/10.1186/s12888-021-03273-4 (2021).
Neyazi, A. et al. Health survey on anxiety, depression, and stress in Afghanistan: A large-scale cross-sectional study amid ongoing challenges. Discover Mental Health. 4 (1), 5. https://doi.org/10.1007/s44192-024-00090-5 (2024).
Anagnostopoulou, T., Kalaitzaki, A., Tsouvelas, G. & Tamiolaki, A. The long-term effect of childhood trauma and alexithymia on mental distress during the COVID-19 pandemic in Greece. Psychology 29 (2), 57–78. https://doi.org/10.12681/psy_hps.28172 (2024).
Lee Raby, K., Labella, M. H., Martin, J., Carlson, E. A. & Roisman, G. I. Childhood abuse and neglect and insecure attachment States of Mind in adulthood: prospective, longitudinal evidence from a high-risk sample. Dev. Psychopathol. 29 (2), 347–363. https://doi.org/10.1017/S0954579417000037 (2017).
Weindl, D. & Lueger-Schuster, B. Coming to terms with oneself: A mixed methods approach to perceived self-esteem of adult survivors of childhood maltreatment in foster care settings. BMC Psychol. 6 (1), 7. https://doi.org/10.1186/s40359-018-0259-7 (2018).
Obeid, S. et al. Correlates of emotional intelligence among Lebanese adults: the role of depression, anxiety, suicidal ideation, alcohol use disorder, alexithymia and work fatigue. BMC Psychol. 9 (1), 6. https://doi.org/10.1186/s40359-021-00525-6 (2021).
Mahfoud, D., Fawaz, M., Obeid, S. & Hallit, S. The co-moderating effect of social support and religiosity in the association between psychological distress and coping strategies in a sample of Lebanese adults. BMC Psychol. 11 (1), 9. https://doi.org/10.1186/s40359-023-01102-9 (2023).
Rehan, W., Antfolk, J., Johansson, A., Jern, P. & Santtila, P. Experiences of severe childhood maltreatment, depression, anxiety and alcohol abuse among adults in Finland. PLoS ONE. 12 (5), 252. https://doi.org/10.1371/journal.pone.0177252 (2017).
Hinds, J. A. & Sanchez, E. R. The role of the hypothalamus–pituitary–adrenal (HPA) axis in test-induced anxiety: assessments, physiological responses, and molecular details. Stresses 2 (1), 146–155. https://doi.org/10.3390/stresses2010011 (2022).
Berenz, E. C. et al. A multimodal study of childhood trauma and distress tolerance in young adulthood. J. Aggress. Maltreat Trauma. 27 (7), 795–810. https://doi.org/10.1080/10926771.2017.1382636 (2018).
Su, Y., Meng, X., Yang, G. & D’Arcy, C. The relationship between childhood maltreatment and mental health problems: coping strategies and social support act as mediators. BMC Psychiatry. 22 (1). https://doi.org/10.1186/s12888-022-04001-2 (2022).
Komarati, M., Motlagh, F. Z. & Pirani, Z. Comparison of the Effectiveness Acceptance and Commitment Therapy (ACT) and Mindfulness-Based Cognitive Therapy on Distress Tolerance of Female Adolescents with Self-Injury Behaviors, Vol 15 (Winter & Spring, 2021).
Afshari, B. & Hasani, J. Study of dialectical behavior therapy versus cognitive behavior therapy on emotion regulation and mindfulness in patients with generalized anxiety disorder. J. Contemp. Psychother. 50 (4), 305–312. https://doi.org/10.1007/s10879-020-09461-9 (2020).
Lagdon, S. et al. Assessing the mediating role of social support in childhood maltreatment and psychopathology among college students in Northern Ireland. J. Interpers. Violence. 36 (3–4), 2112–2136. https://doi.org/10.1177/0886260518755489 (2021).
Rush, A. J. Making therapy widely available: clinical research triumph or existential catastrophe? Am. J. Psychiatry. 179 (2), 79–82. https://doi.org/10.1176/appi.ajp.2021.21121201 (2021).
Bockmann, J. O. & Yu, S. Y. Using mindfulness-based interventions to support self-regulation in young children: A review of the literature. Early Child. Educ. J. 51 (4), 693–703. https://doi.org/10.1007/s10643-022-01333-2 (2023).
Landolt, M. A., Cloitre, M. & Schnyder, U. Evidence-Based Treatments for Trauma Related Disorders in Children and Adolescents.
Mathews, B. Developing Countries and the Potential of Mandatory Reporting Laws to Identify Severe Child Abuse and Neglect.
Kousholt, D. & Juhl, P. Situated Ethics in Collaborative Research. https://doi.org/10.1007/s42087-021 (2021).
Acknowledgements
The authors would like to thank all participants.
Author information
Authors and Affiliations
Contributions
SO, SH and FFR designed the study; EM drafted the manuscript; SH carried out the analysis and interpreted the results; FS and MD collected the data. DM, RH and TS reviewed the paper for intellectual content; all authors reviewed the final manuscript and gave their consent.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
The Lebanese International University’s School of Pharmacy ethics committee granted this study ethics permission. When filling out the online form, each participant provided written informed consent, as did their parents or legal guardian(s) if they were study participants under the age of sixteen. All methods were performed in accordance with the relevant guidelines and regulations (in accordance with the Declaration of Helsinki).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Mattar, E., Sawma, T., Hallit, R. et al. The mediating role of distress tolerance in the relationship between childhood maltreatment and anxiety in a sample of Lebanese adults. Sci Rep 15, 13570 (2025). https://doi.org/10.1038/s41598-025-98417-x
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-98417-x